Introduction
Lung cancer is a type of malignant tumor derived
from the respiratory system that is further classified into
non-small cell lung cancer (NSCLC) and small cell lung cancer
(SCLC). NSCLC accounts for ~80% of lung cancer cases (1). NSCLC includes squamous cell carcinoma,
adenocarcinoma and large cell carcinoma; of which adenocarcinoma
presents with an increased onset. Adenocarcinoma demonstrates a
reduced degree of malignancy compared with SCLC. The clinical
symptoms of NSCLC differ depending on tumor size, location and
metastatic range (2), and early NSCLC
is often insidious, producing no visible symptoms until the disease
is at an advanced stage. Due to the high degree of malignancy and
rapid progression, the majority of patients are already in the
mid-late stage of disease by the time of diagnosis. At this
advanced stage of disease, surgical procedures are of no benefit to
patients and therefore lung cancer is the principal cause of
cancer-associated mortality worldwide (3,4). Due to
the changes of lifestyle and environmental pollution aggravation,
lung cancer presents an increasing rate of mortality, and younger
trend (5,6). As the occurrence and development of lung
cancer is multi-factorial, polygenic and multi-level process, there
is still a requirement for an accurate diagnosis method in the
early stages. However, the effects of treatments for advanced lung
cancer are not favorable, with a poor prognosis (7,8). Thus,
early detection, early diagnosis, and early treatment are essential
to improve the quality of life and survival of patients with lung
cancer.
In previous years, vitamin D has been demonstrated
to exert a range of biological functions, which include promoting
calcium absorption, maintaining bone formation and reducing tumor
occurrence and development (9,10).
Ultraviolet irradiation and appropriate vitamin D intake help
reduce tumor incidence, including breast cancer, prostate cancer,
lung cancer and colon cancer (11,12).
Conversely, Vitamin D deficiency is associated with an increased
incidence of cancer, suggesting that vitamin D content is
negatively associated with tumor progression. The primary sources
of vitamin D are nutritional or from sunlight.
1α,25-Dihydroxyvitamin D3
(1α,25(OH)2D3) is the main active metabolite
of vitamin D which can inhibit lung cancer cell proliferation,
activation and progression through promoting apoptosis (13,14).
However, 1α,25(OH)2D3 requires activation by
the vitamin D metabo1ic pathway (15). Therefore, it is postulated that the
aberrant expression of the essential enzymes CYP27A1, CYP27B1, and
CYP24A1 may be associated with lung cancer. However, no previous
research has been conducted to clarify the association between
CYP27A1, CYP27B1 and CYP24A1 expression with NSCLC.
The aim of the present study was to investigate CYP27A1,
CYP27B1, and CYP24A1 expression in NSCLC.
Materials and methods
Patient selection
A total of 180 patients with NSCLC identified by
pathological diagnosis were enrolled in the present study from the
Affiliated Hospital of Qingdao University (Qingdao, China) between
October 2013 and October 2015. All the selected patients with NSCLC
received surgical treatment and included 92 males and 88 females.
The age of the patients ranged between 45–87 years, with an average
of 62.2±6.1 years of age. A total of 62 cases were diagnosed at
stage I, 57 cases at stage II, 34 cases at stage III and 27 cases
at stage IV of the disease. Pathologically, 51 patients presented
with squamous cell carcinoma, 82 patients with adenocarcinoma and
47 patients with large cell carcinoma. There were 42 cases of poor
differentiation, 71 cases of moderate differentiation, and 67 cases
of well differentiation. Inclusion criteria for the study were as
follows: All subjects were newly diagnosed with lung cancer; all
subjects received surgery for the first time; no chemotherapy or
radiotherapy was conducted prior to surgery; all subjects had
signed an informed consent prior to the study. Exclusion criteria
were as follows: Recurrent lung cancer; previously received
surgery; previously received chemotherapy or radiotherapy; combined
with other disease, including infectious disease, malignant tumor,
severe diabetes, severe renal and liver disease, pulmonary
fibrosis, bone metabolic disease and systemic autoimmune disease.
Cancer tissues and para-carcinoma tissues (defined as controls)
were collected and stored at −80°C. The experimental protocols for
the present study were pre-approved by the Ethical Committee of the
Affiliated Hospital of Qingdao University and written informed
consent was obtained from all patients prior to the study.
Chemicals and reagents
The RNA extraction kit and reverse transcription kit
were from R & D systems, Inc. (Minneapolis, MN, USA). Other
common reagents were from Sangon Biotech Co., Ltd., (Shanghai,
China). Real time PCR kit was from Thermo Fisher Scientific, Inc.,
(Waltham, MA, USA). The real time PCR amplifier was from ABI
(Applied Biosystems; Thermo Fisher Scientific, Inc.). DNA amplifier
was the PE Gene Amp PCR System 2400 (Applied.Biosystems; Thermo
Fisher Scientific, Inc.).
Reverse transcription quantitative
polymerase chain reaction (RT-qPCR)
Total RNA was extracted from patient lung tissues
using TRIzol® reagent, according to the manufacturer's
protocol. Total RNA was reverse transcribed to cDNA using
Superscript III reverse transcriptase (Invitrogen; Thermo Fisher
Scientific, Inc.). qPCR was performed to detect CYP24A1,
CYP27A1 or CYP27B1 relative gene expression using a qPCR
kit (Power SYBR™ Green PCR Master Mix; Thermo Fisher Scientific,
Inc.), run on the Perkin Elmer Gene Amp PCR System 2400 thermal
cycler. The reaction conditions were as follows; 92°C for 1 min,
followed by 35 cycles of 90°C for 30 sec, 58°C for 50 sec and 72°C
for 35 sec. Glyceraldehyde 3-phosphate dehydrogenase (GAPDH) was
selected as an internal reference gene. Melting curve analysis was
performed to verify the target specificity of primers. Relative
gene expression levels were quantified using the 2−ΔΔCq
method.
Clinical data collection
Patients' age, sex, clinical stage, pathological
type, differentiation status and prognosis were recorded and
followed up.
Western blot
Total proteins were extracted from tissues by the
addition of RIPA lysis buffer (Thermo Fisher Scientific, Inc.) and
incubated at 4°C for 30 min, followed by centrifugation at 12,000 ×
g for 10 min at 4°C. Supernatants were transferred to new tubes for
quantification of extracted protein concentrations using a BCA
assay. Total proteins (20 µg) were separated on 8–12% SDS-PAGE gel,
and transferred to a PVDF membrane. Membranes were blocked by
incubation with 5% skimmed milk for 1 h at 25°C. The membranes were
incubated with primary antibodies, rabbit polyclonal to CYP24A1
(cat. no. ab96691, Abcam, Cambridge, UK), Rabbit polyclonal to
CYP27A1 (cat. no. ab64889, Abcam) or Rabbit monoclonal to CYP27B1
(cat. no. EPR20271, Abcam), (1:1,000) at 4°C overnight. The
following day, membranes were further incubated in horseradish
peroxidase-conjugated goat anti-rabbit secondary antibody (cat. no.
ab6721, Abcam; 1:1,000) at 37°C for 1 h. Proteins were detected
using enhanced chemiluminescence reagents (Thermo Fisher
Scientific, Inc.).
Statistical analysis
Statistical analyses were performed using SPSS
v.16.0 software (SPSS; Inc., Chicago, IL, USA) and data were
presented as the mean ± standard deviation. Multiple group
comparisons were performed using one-way analysis of variance and
Fishers's least significant difference test. Enumerate data were
presented as percentage and compared by χ2 test.
Survival was assessed by Kaplan-Meier analysis. A Cox proportional
hazards regression model was used for univariate and multivariate
analysis. P<0.05 was considered to indicate a statistically
significant difference.
Results
CYP24A1, CYP27A1 and CYP27B1 mRNA
expression in lung cancer
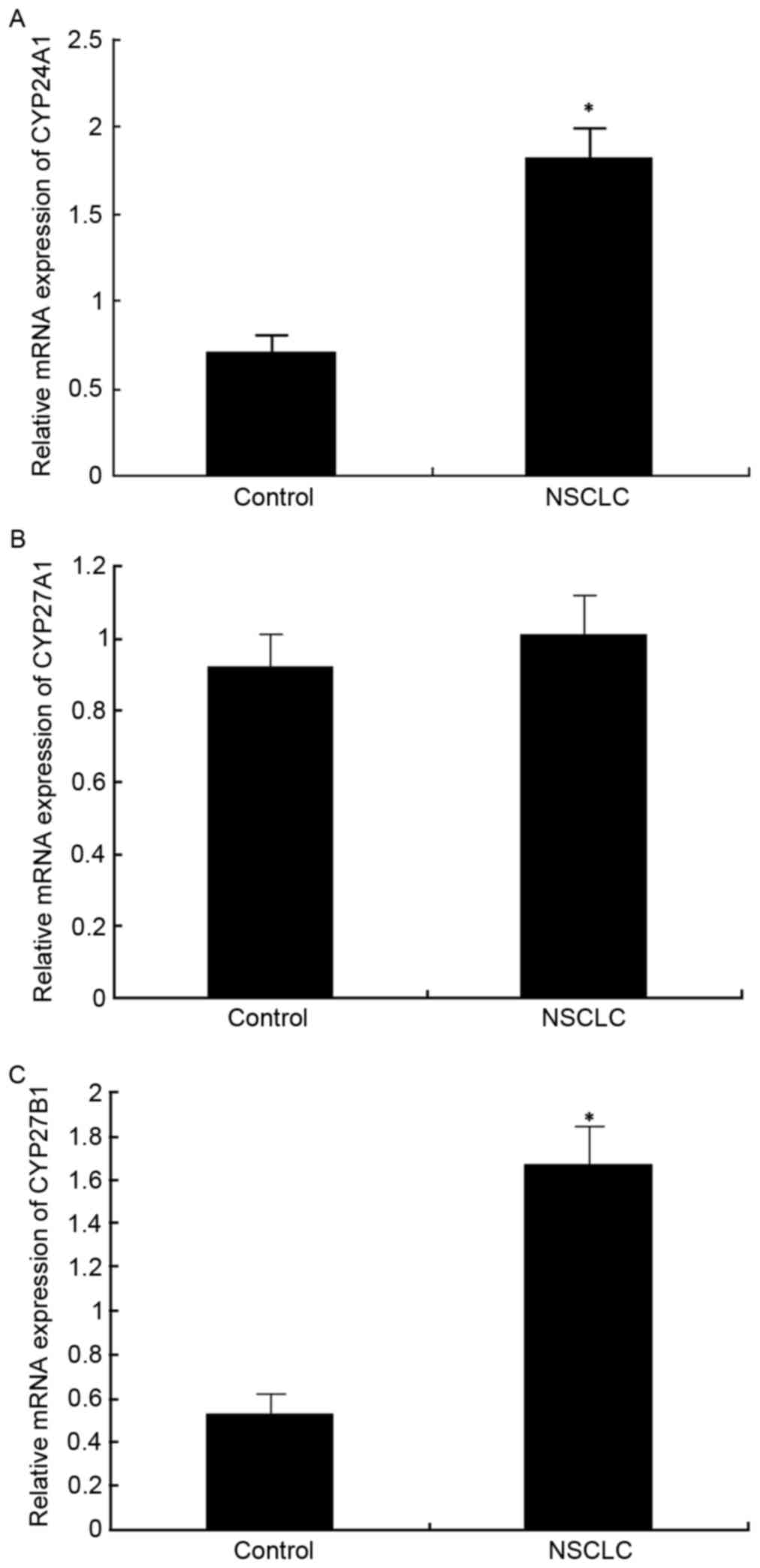
qPCR was conducted to analyze CYP24A1 mRNA
expression in cancer tissue compared with para-carcinoma control
tissue. The results demonstrated that CYP24A1 mRNA
expression was significantly upregulated in cancer tissues compared
with controls (P<0.05; Fig. 1A).
Conversely, CYP27A1 mRNA levels were marginally elevated in
cancer tissues compared with controls, but no significant
differences were observed (Fig. 1B).
However, relative CYP27B1 mRNA expression levels were
significantly upregulated in cancer tissues compared with
para-carcinoma control tissues (P<0.05; Fig. 1C).
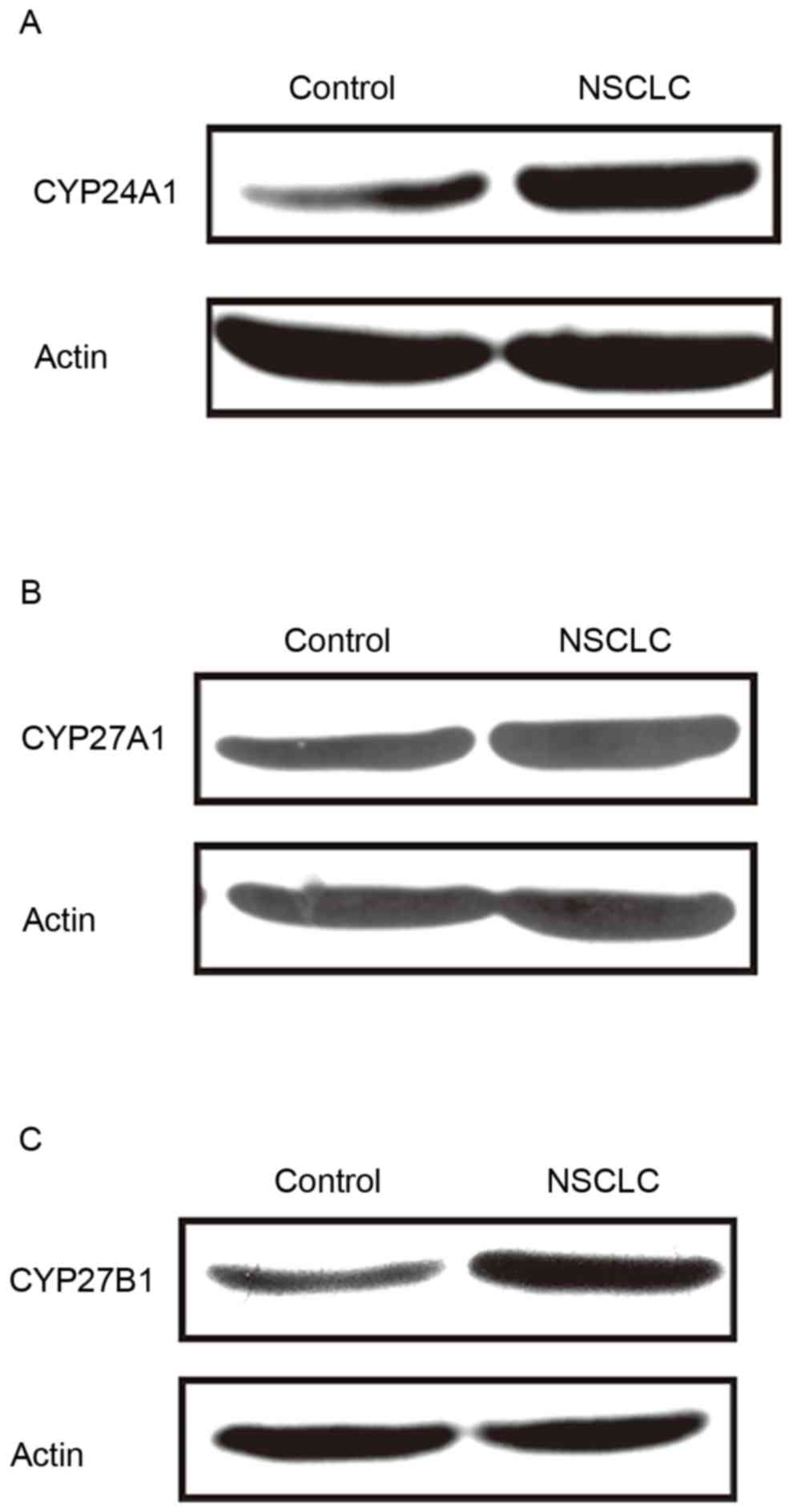
CYP24A1, CYP27A1 and CYP27B1 protein
expression in lung cancer
Comparable to the mRNA expression profiles, the
protein expression of CYP24A1, CYP27A1 and CYP27B1 was elevated in
cancer tissues compared with controls (Fig. 2).
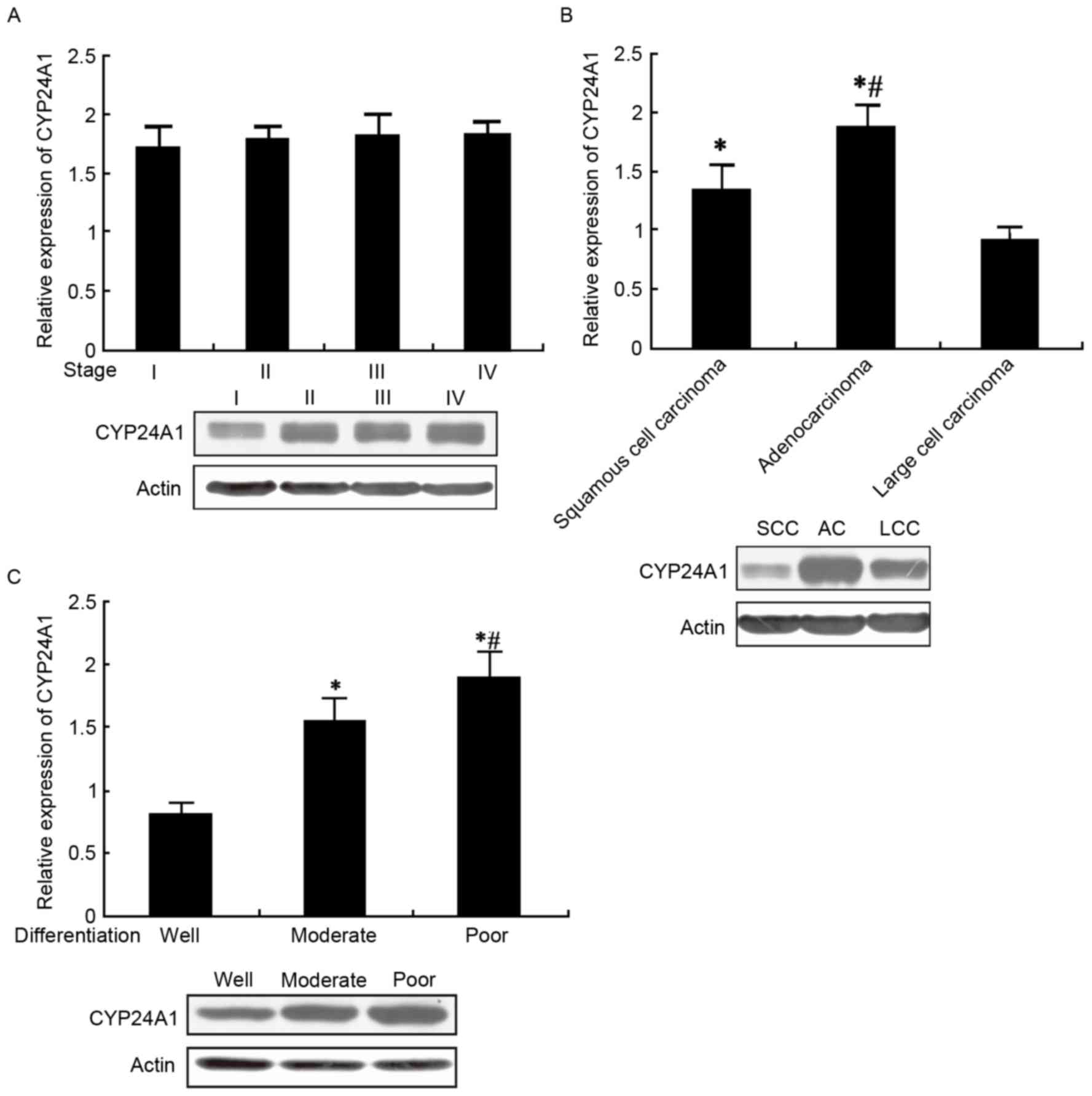
CYP24A1 expression in patients with
NSCLC with different pathological characteristics
qPCR and western blot analysis were used to detect
CYP24A1 mRNA and protein expression in patients with NSCLC with
different TNM stage, pathological type and differentiation status.
The results from the present study suggested that CYP24A1 mRNA and
protein levels increased with increasing TNM stages, although no
statistical differences were observed. CYP24A1 levels were markedly
elevated in adenocarcinoma compared with squamous cell carcinoma
and large cell carcinoma (P<0.05), but there was no significant
difference between squamous and large cell carcinoma. CYP24A1
demonstrated increased expression in the poorly differentiated
group, followed by the moderately differentiated compared with
well-differentiated groups (P<0.05; Fig. 3A-C).
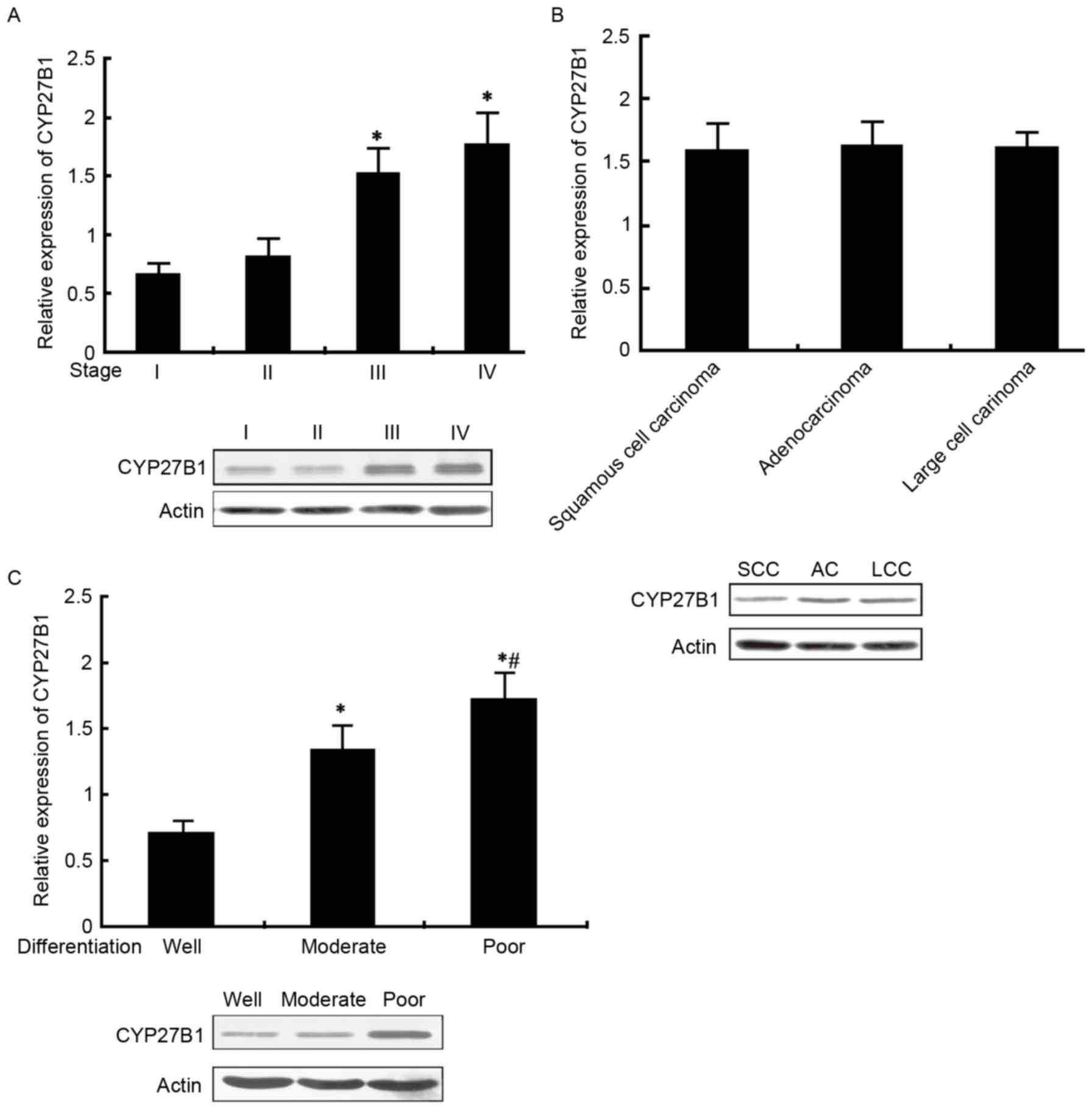
CYP27B1 expression in patients with
NSCLC with different pathological characteristics
Analysis by qPCR and western blot was applied to
measure CYP27B1 mRNA and protein expression in patients with NSCLC
with different TNM stage, pathological type and differentiation
status. The results from the present study revealed that CYP27B1
mRNA and protein levels were significantly elevated with increasing
TNM stage (III and IV vs. I and II, P<0.05). However, the levels
of CYP27B1 were not significantly different between different
pathological types. Furthermore, CYP24A1 levels were increased in
the poorly differentiated group, followed by moderately
differentiated and well differentiated (P<0.05; Fig. 4A-C).
CYP24A1 and CYP27B1 mRNA expression
levels in patients with NSCLC
The differences in CYP24A1 and CYP27B1
mRNA expression in patients with NSCLC in association with age,
sex, smoking and prognosis were compared. The results from the
present study demonstrated that comparisons of CYP24A1 mRNA
levels in patients with different age, sex and smoking presented no
significant differences (Table II).
In the prognosis analysis, patients with a survival time of <5
years had increased CYP24A1 mRNA levels compared with
patients with a survival time ≥5 years (P<0.05). Similar with
CYP24A1, CYP27B1 mRNA levels demonstrated no significant
differences in patients with different sex, gender or smoking
status. In the prognosis analysis, CYP27B1 mRNA levels were
increased in patients with a survival time of <5 years compared
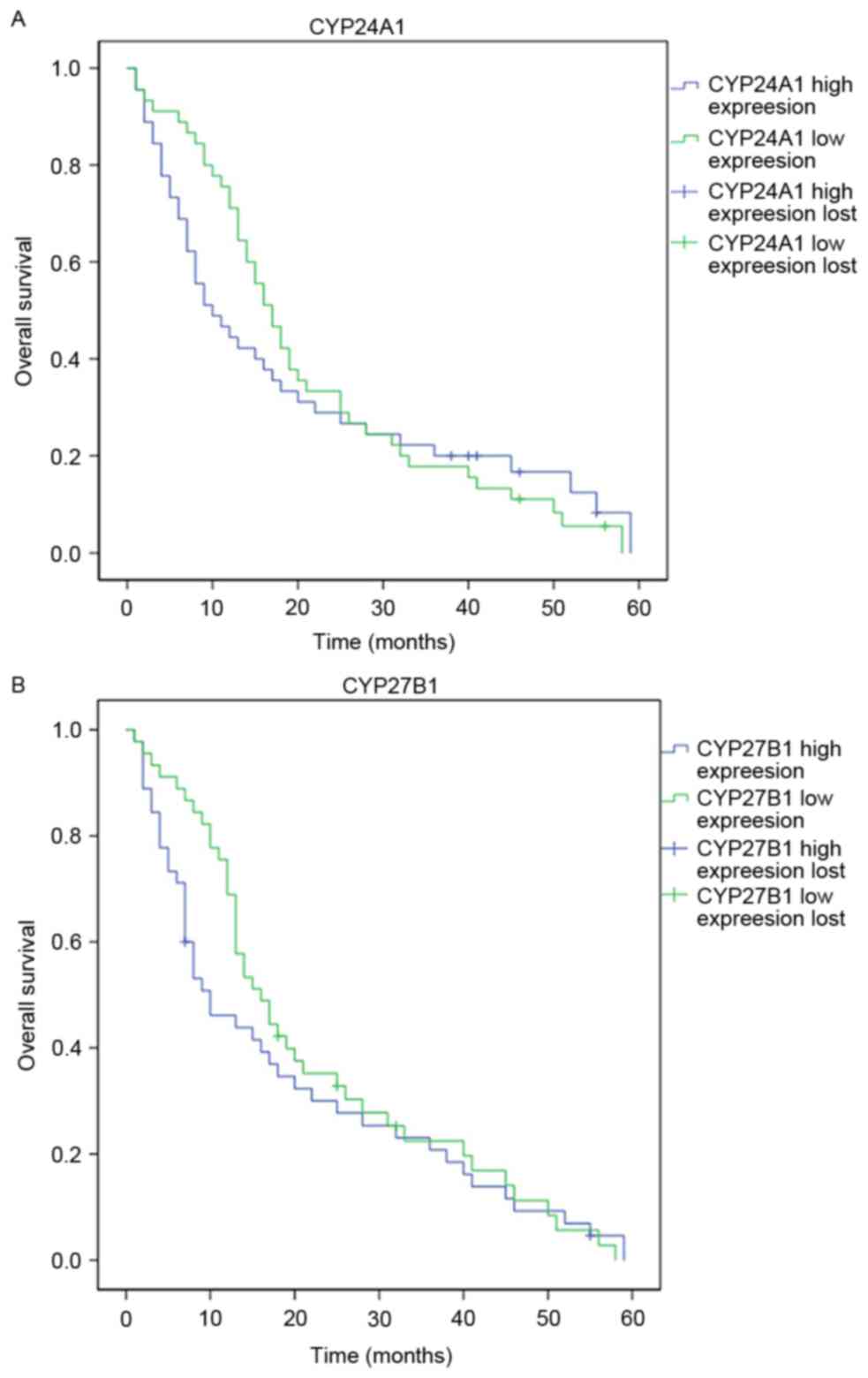
with a survival time of ≥5 years (P<0.05; Table II). To compare the differences in
survival time between patients with varying CYP24A1 or
CYP27B1 expression levels, Kaplan-Meier curve analysis was
performed. Patients with increased CYP24A1 or CYP27B1
expression demonstrated a significantly shorter survival time
compared with patients with reduced CYP24A1 or
CYP27B1 expression (Fig. 5A and
B; P<0.05).
 | Table II.Comparison of CYP24A1 and
CYP27B1 mRNA expression in patients with NSCLC in
association with age (60 years-cut off value), sex, smoking and
survival time (5 years-cut off value). |
Table II.
Comparison of CYP24A1 and
CYP27B1 mRNA expression in patients with NSCLC in
association with age (60 years-cut off value), sex, smoking and
survival time (5 years-cut off value).
| Variable | CYP24A1 mRNA
levels | CYP27B1 mRNA
levels |
|---|
| Age, years |
|
|
|
<60 | 1.78±0.31 | 1.61±0.25 |
|
≥60 | 1.82±0.19 | 1.68±0.91 |
| Sex |
|
|
|
Male | 1.81±0.55 | 1.71±0.61 |
|
Female | 1.79±0.13 | 1.65±0.53 |
| Smoking |
|
|
| No | 1.80±0.17 | 1.62±0.47 |
|
Yes | 1.83±0.22 | 1.70±0.74 |
| Survival time,
years |
|
|
|
<5 | 1.87±0.91 | 1.79±0.78 |
| ≥5 |
1.32±0.26a |
1.21±0.15a |
Discussion
Lung cancer is the most common type of cancer and
recurrent respiratory tract malignant tumor worldwide, and NSCLC
accounts for the majority of lung cancer cases with poor prognosis
(1). The average survival period for
patients with NSCLC is short even following surgery, chemotherapy
and radiotherapy (16). Following an
in-depth investigation of lung cancer biology and pathogenesis over
previous years, there have been notable advances in the diagnosis
and treatment of lung cancer. However, the identification of
specific biomarkers for the early diagnosis and prognosis of lung
cancer is still required (17). The
most bioactive metabolite of vitamin D,
1α,25(OH)2D3 has been confirmed to contribute
various non-endocrine functions in addition to maintaining calcium
stability; including anti-proliferative activity, induction of cell
differentiation, promotion of cell cycle stagnation and apoptosis,
inhibiting cytopoiesis and regulating tumor occurrence and
development (18,19). Vitamin D generates
1α,25(OH)2D3 through the metabolic pathway.
CYP27A1, mainly expressed in the liver and intestinal tract,
encodes for 25-hydroxylase which metabolizes vitamin D to 1,25(OH)D
(20). CYP27B1, widely expressed in
multiple organs, encodes 25-hydroxy vitamin D 1-α hydroxylase to
catalyze 1,25(OH)D to active 1α,25(OH)2D3
(21). CYP24A1 encodes 25-hydroxy
vitamin D3-24-hydroxylase that converts active metabolites to
inactive 24,25-dihydroxy vitamin D (21). Thus, CYP27A1, CYP27B1, and CYP24A1 are
three key enzymes in the vitamin D metabolic pathway. However, the
association between CYP27A1, CYP27B1, and CYP24A1 and NSCLC have
not been fully elucidated.
CYP27A1, CYP27B1, and CYP24A1 belong to the
cytochrome P450 (CYP450) family. CYP450 is an important microsomal
multi-functional oxidase family of hemoglobin enzymes. CYP450 is
expressed in various tissues and organs, and has a variety of
biological functions, including oxidation and metabolism of
endogenous and exogenous substances. Previous studies have
demonstrated that CYP24A1 is overexpressed in skin (22), colon (23), ovarian (24), prostate (25) and lung cancer (26). It promotes tumorigenesis through the
stimulation of signaling pathways and is associated with poor
prognosis (27,28). However, there is still a lack of
evidence to support the association of CYP27A1 and CYP27B1 with
lung cancer. The present study confirmed that CYP27B1 and
CYP24A1 mRNA expression were significantly elevated in
patients with NSCLC. CYP24A1 expression was not associated
with age, sex, smoking or TNM stage, but with pathological type,
differentiation and prognosis. CYP27B1 expression was
significantly associated with TNM stage, differentiation and
prognosis, as opposed to age, sex, smoking status and pathological
type. However, a previous study revealed that increased
CYP27B1 expression in tumors was significantly associated
with improved overall survival (29).
However, this association was attenuated when covariates and
confounding variables were adjusted in the regression model. The
discrepancies between the present study and the Kong et al
(29) study may be due to the
clinical characteristics of enrolled patients, including age, sex
and disease stage.
It has been suggested that the effect of
1α,25(OH)2D3 on tumor cell development was
dependent on CYP27B1 and CYP24A1 activity. In addition, the
polymorphism of CYP24A1 and CYP27B1 has been
demonstrated to be involved in the modulation of vitamin D
metabolism in colon cancer, evidenced by marked changes in
enzymatic activity in colon cancer cells, resulting from the
polymorphism of CYP24A1 and CYP27B1 (30). These alterations may possibly cause
differential 1,25D exposure in colonic cells, which may render
individuals more susceptible to the development of colon
cancer.
In conclusion, CYP27B1 and CYP24A1 may be treated as
independent prognostic factors of NSCLC, and may be new therapeutic
targets to assist clinical diagnosis, treatment and prognosis of
disease. However, the exact mechanism by how CYP27B1 and CYP24A1
are involved in the pathogenesis of NSCLC remains unclear and
requires further investigation.
Acknowledgements
The present study was funded by an Academic Fund for
Young Scientist Award, The Affiliated Hospital of Qingdao
University, Qingdao, China (grant no. 2208).
References
|
1
|
Gudala S, Khan U, Kanungo N, Bandaru S,
Hussain T, Parihar M, Nayarisseri A and Mundluru HP: Identification
and pharmacological analysis of high efficacy small molecule
inhibitors of EGF-EGFR interactions in clinical treatment of
non-small cell lung carcinoma: A computational approach. Asian Pac
J Cancer Prev. 16:8191–8196. 2015. View Article : Google Scholar : PubMed/NCBI
|
|
2
|
Xia M, Duan ML, Tong JH and Xu JG: MiR-26b
suppresses tumor cell proliferation, migration and invasion by
directly targeting COX-2 in lung cancer. Eur Rev Med Pharmacol Sci.
19:4728–4737. 2015.PubMed/NCBI
|
|
3
|
Paz-Ares L, Hirsh V, Zhang L, de Marinis
F, Yang JC, Wakelee HA, Seto T, Wu YL, Novello S, Juhász E, et al:
Monotherapy administration of sorafenib in patients with non-small
cell lung cancer (MISSION) trial: A phase III, multicenter,
placebo-controlled trial of sorafenib in patients with relapsed or
refractory predominantly nonsquamous non-small-cell lung cancer
after 2 or 3 previous treatment regimens. J Thorac Oncol.
10:1745–1753. 2015. View Article : Google Scholar : PubMed/NCBI
|
|
4
|
Guerrera F, Tabbò F, Bessone L, Maletta F,
Gaudiano M, Ercole E, Annaratone L, Todaro M, Boita M, Filosso PL,
et al: The Influence of tissue ischemia time on RNA integrity and
patient-derived xenografts (PDX) engraftment rate in a non-small
cell lung cancer (NSCLC) biobank. PLoS One. 11:e01451002016.
View Article : Google Scholar : PubMed/NCBI
|
|
5
|
Tai CJ, Wang CK, Tai CJ, Tzao C, Lien YC,
Hsieh CC, Hsieh CI, Wu HC, Wu CH, Chang CC, et al: Evaluation of
safety and efficacy of salvage therapy with sunitinib, docetaxel
(Tyxane) and cisplatinum followed by maintenance vinorelbine for
unresectable/metastatic nonsmall cell lung cancer: Stage 1 of a
simon 2 stage clinical trial [Corrected]. Medicine (Baltimore).
94:e23032015. View Article : Google Scholar : PubMed/NCBI
|
|
6
|
Robinson AG, Young K, Balchin K, Owen T
and Ashworth A: Reasons for palliative treatments in stage III
non-small-cell lung cancer: What contribution is made by
time-dependent changes in tumour or patient status? Curr Oncol.
22:399–404. 2015. View Article : Google Scholar : PubMed/NCBI
|
|
7
|
Sasaki S, Yoshioka Y, Ko R, Katsura Y,
Namba Y, Shukuya T, Kido K, Iwakami S, Tominaga S and Takahashi K:
Diagnostic significance of cerebrospinal fluid EGFR mutation
analysis for leptomeningeal metastasis in non-small-cell lung
cancer patients harboring an active EGFR mutation following
gefitinib therapy failure. Respir Investig. 54:14–19. 2016.
View Article : Google Scholar : PubMed/NCBI
|
|
8
|
Kepka L and Socha J: PET-CT limitations in
early stage non-small cell lung cancer: To whom more aggressive
approach in radiotherapy and surgery should be directed? J Thorac
Dis. 7:1887–1890. 2015.PubMed/NCBI
|
|
9
|
Piotrowska A, Wierzbicka J, Nadkarni S,
Brown G, Kutner A and Żmijewski MA: Antiproliferative activity of
double point modified analogs of 1,25-dihydroxyvitamin
D2 against human malignant melanoma cell lines. Int J
Mol Sci. 17:pii: E76. 2016. View Article : Google Scholar
|
|
10
|
Aguirre M, Manzano N, Salas Y, Angel M,
Díaz-Couselo FA and Zylberman M: Vitamin D deficiency in patients
admitted to the general ward with breast, lung, and colorectal
cancer in buenos aires, argentina. Arch Osteoporos. 11:42016.
View Article : Google Scholar : PubMed/NCBI
|
|
11
|
Wen Y, Da M, Zhang Y, Peng L, Yao J and
Duan Y: Alterations in vitamin D signaling pathway in gastric
cancer progression: A study of vitamin D receptor expression in
human normal, premalignant, and malignant gastric tissue. Int J
Clin Exp Pathol. 8:13176–13184. 2015.PubMed/NCBI
|
|
12
|
Vashi PG, Edwin P, Popiel B and Gupta D:
The relationship between circulating 25-hydroxyvitamin D and
survival in newly diagnosed advanced non-small-cell lung cancer.
BMC Cancer. 15:10122015. View Article : Google Scholar : PubMed/NCBI
|
|
13
|
Christakos S, Dhawan P, Verstuyf A,
Verlinden L and Carmeliet G: Vitamin D: Metabolism, molecular
mechanism of action, and pleiotropic effects. Physiol Rev.
96:365–408. 2016. View Article : Google Scholar : PubMed/NCBI
|
|
14
|
Khayatzadeh S, Feizi A, Saneei P and
Esmaillzadeh A: Vitamin D intake, serum Vitamin D levels, and risk
of gastric cancer: A systematic review and meta-analysis. J Res Med
Sci. 20:790–796. 2015. View Article : Google Scholar : PubMed/NCBI
|
|
15
|
Hibler EA, Molmenti Sardo CL, Dai Q,
Kohler LN, Anderson Warren S, Jurutka PW and Jacobs ET: Physical
activity, sedentary behavior, and vitamin D metabolites. Bone.
83:248–255. 2016. View Article : Google Scholar : PubMed/NCBI
|
|
16
|
Huang Z, Yi X, Luo B, Zhu J, Wu Y, Jiang
W, Chu H, Yang Z, Li S, Zhu H, et al: Induced sputum deposition
improves diagnostic yields of pulmonary alveolar proteinosis: A
clinicopathological and methodological study of 17 cases.
Ultrastruct Pathol. 40:7–13. 2016. View Article : Google Scholar : PubMed/NCBI
|
|
17
|
Ortakoylu MG, Iliaz S, Bahadir A, Aslan A,
Iliaz R, Ozgul MA and Urer HN: Diagnostic value of endobronchial
ultrasound-guided transbronchial needle aspiration in various lung
diseases. J Bras Pneumol. 41:410–414. 2015.(In English,
Portuguese). View Article : Google Scholar : PubMed/NCBI
|
|
18
|
Yin K, You Y, Swier V, Tang L, Radwan MM,
Pandya AN and Agrawal DK: Vitamin D protects against
atherosclerosis via regulation of cholesterol efflux and macrophage
polarization in hypercholesterolemic swine. Arterioscler Thromb
Vasc Biol. 35:2432–2442. 2015. View Article : Google Scholar : PubMed/NCBI
|
|
19
|
Fedorova OV, Zernetkina VI, Shilova VY,
Grigorova YN, Juhasz O, Wei W, Marshall CA, Lakatta EG and Bagrov
AY: Synthesis of an endogenous steroidal na pump inhibitor
marinobufagenin, implicated in human cardiovascular diseases, is
initiated by CYP27A1 via bile acid pathway. Circ Cardiovasc Genet.
8:736–745. 2015. View Article : Google Scholar : PubMed/NCBI
|
|
20
|
Gascon-Barré M, Demers C, Ghrab O,
Theodoropoulos C, Lapointe R, Jones G, Valiquette L and Ménard D:
Expression of CYP27A, a gene encoding a vitamin D-25 hydroxylase in
human liver and kidney. Clin Endocrinol (Oxf). 54:107–115. 2001.
View Article : Google Scholar : PubMed/NCBI
|
|
21
|
Adams JS and Hewison M: Extrarenal
expression of the 25-hydroxyvitamin D-1-hydroxylase. Arch Biochem
Biophys. 523:95–102. 2012. View Article : Google Scholar : PubMed/NCBI
|
|
22
|
Mast N, Lin JB and Pikuleva IA: Marketed
drugs can inhibit cytochrome P450 27A1, a potential new target for
breast cancer adjuvant therapy. Mol Pharmacol. 88:428–436. 2015.
View Article : Google Scholar : PubMed/NCBI
|
|
23
|
Brożyna AA, Jochymski C, Janjetovic Z,
Jóźwicki W, Tuckey RC and Slominski AT: CYP24A1 expression
inversely correlates with melanoma progression: Clinic-pathological
studies. Int J Mol Sci. 15:19000–19017. 2014. View Article : Google Scholar : PubMed/NCBI
|
|
24
|
Horváth HC, Lakatos P, Kósa JP, Bácsi K,
Borka K, Bises G, Nittke T, Hershberger PA, Speer G and Kállay E:
The candidate oncogene CYP24A1: A potential biomarker for
colorectal tumorigenesis. J Histochem Cytochem. 58:277–285. 2010.
View Article : Google Scholar : PubMed/NCBI
|
|
25
|
Anderson MG, Nakane M, Ruan X, Kroeger PE
and Wu-Wong JR: Expression of VDR and CYP24A1 mRNA in human tumors.
Cancer Chemother Pharmacol. 57:234–240. 2006. View Article : Google Scholar : PubMed/NCBI
|
|
26
|
Whitlatch LW, Young MV, Schwartz GG,
Flanagan JN, Burnstein KL, Lokeshwar BL, Rich ES, Holick MF and
Chen TC: 25-Hydroxyvitamin D-1alpha-hydroxylase activity is
diminished in human prostate cancer cells and is enhanced by gene
transfer. J Steroid Biochem Mol Biol. 81:135–140. 2002. View Article : Google Scholar : PubMed/NCBI
|
|
27
|
Chen G, Kim SH, King AN, Zhao L, Simpson
RU, Christensen PJ, Wang Z, Thomas DG, Giordano TJ, Lin L, et al:
CYP24A1 is an independent prognostic marker of survival in patients
with lung adenocarcinoma. Clin Cancer Res. 17:817–826. 2011.
View Article : Google Scholar : PubMed/NCBI
|
|
28
|
Shui IM, Mondul AM, Lindström S, Tsilidis
KK, Travis RC, Gerke T, Albanes D, Mucci LA, Giovannucci E and
Kraft P: Breast and Prostate Cancer Cohort Consortium Group:
Circulating vitamin D, vitamin D-related genetic variation, and
risk of fatal prostate cancer in the national cancer institute
breast and prostate cancer cohort consortium. Cancer.
121:1949–1956. 2015. View Article : Google Scholar : PubMed/NCBI
|
|
29
|
Lee WR, Ishikawa T and Umetani M: The
interaction between metabolism, cancer and cardiovascular disease,
connected by 27-hydroxycholesterol. Clin Lipidol. 9:617–624. 2014.
View Article : Google Scholar : PubMed/NCBI
|
|
30
|
Kong J, Xu F, Qu J, Wang Y, Gao M, Yu H
and Qian B: Genetic polymorphisms in the vitamin D pathway in
relation to lung cancer risk and survival. Oncotarget. 6:2573–2782.
2014. View Article : Google Scholar
|
|
31
|
Jacobs ET, Van Pelt C, Forster RE, Zaidi
W, Hibler EA, Galligan MA, Haussler MR and Jurutka PW: CYP24A1 and
CYP27B1 polymorphisms modulate vitamin D metabolism in colon cancer
cells. Cancer Res. 73:2563–2573. 2013. View Article : Google Scholar : PubMed/NCBI
|