Introduction
Gastric cancer is one of the most common types of
malignant tumor globally. In China, the incidence of gastric cancer
is the second highest of all the malignant tumors (1,2). Early
symptoms in the majority of patients with gastric cancer are not
detected (3). The prognosis remains
poor in patients with intermediate- and advanced-stage gastric
cancer and the total 5-year survival rate is ~20% (3).
The poor prognosis of patients with gastric cancer
is associated with increased invasiveness and metastasis (4,5).
Epithelial-mesenchymal transition (EMT) is a biological process in
which epithelial cells are transformed into mesenchymal-like cells
under certain physiological or pathological conditions (6,7). It has
been suggested that EMT serves a key function in tumor invasion and
metastasis (8). Future studies
investigating the molecular mechanism underling EMT in tumor
invasion and metastasis are required.
Nicotinamide N-methyltransferase (NNMT) is an
S-adenosyl-L-methionine-dependent cytoplasmic enzyme that is mainly
expressed in the human liver (9,10). NNMT is
mainly involved in the biotransformation of drugs and other
xenobiotic chemicals (11). Recent
studies have demonstrated that NNMT is aberrantly expressed in a
number of tumors, suggesting that NNMT serves an important function
in tumor development (12,13). Additionally, the serum levels of NNMT
were significantly increased in patients with colorectal, lung and
renal cell carcinoma compared with those in the control group
(10,14,15).
Previous studies have also demonstrated that the upregulation of
NNMT is associated with poor prognosis, advanced tumor stage, tumor
cell migration and invasion (9,16,17). Although, overexpression of NNMT has
been identified in gastric cancer (18), the underlying molecular mechanism
remains unclear.
The present study aims to evaluate the expression of
NNMT in gastric cancer cell lines and the underlying mechanism by
which NNMT is involved in the progression of gastric cancer,
thereby exploring novel therapeutic targets for gastric cancer
patients.
Materials and methods
Cell culture
Gastric cancer MKN45, MGC-803, AGS and BGC-823 cell
lines, and normal gastric epithelial GES-1 cells were obtained from
the China Center for Type Culture Collection (Beijing, China). All
cell lines were cultured in RPMI-1640 (GE Healthcare, Chicago, IL,
USA) supplemented with 10% fetal bovine serum (FBS) (GE
Healthcare), streptomycin (100 mg/ml) (Invitrogen; Thermo Fisher
Scientific, Inc., Waltham, MA, USA) and penicillin (100 IU/ml)
(Invitrogen; Thermo Fisher Scientific, Inc.) at 37°C in a
humidified atmosphere containing 5% CO2.
Transient transfection
In brief, BGC-823 cells were seeded at the density
of 105 cells/well in a 6-well plate. BGC-823 cells were
transfected with small interfering RNA (siRNA) targeting NNMT
(GCTCAAGAGCAGCTACTACAT) or a non-specific siRNA
(TTCTCCGAACGTGTCACGT) (GenChem, Jiangsu, China), which was used as
a negative control (NC), at a final concentration at 20 nM. Cells
were pre-incubated at room temperature for 10 min with HiPerfect
transfection reagent (Qiagen GmbH, Hilden, Germany). For subsequent
experiments, BGC-823 cells were used at 48 h post-transfection.
Adenoviral vector construction
Recombinant adenoviruses expressing NNMT (Ad-NNMT)
or a NC-adenovirus vector containing green fluorescent protein
(Ad-Con) were obtained from Shanghai GeneChem Co., Ltd. (Shanghai,
China). Briefly, BGC-823 cells were seeded at 10×105
cells/well in a 6-well plate. At 80% confluence, Ad-NNMT or Ad-Con
was transfected into BGC-823 cells at a multiplicity of infection
of 30.
RNA extraction and reverse
transcription-quantitative polymerase chain reaction (RT-qPCR)
Total RNA was isolated from MKN45, MGC-803, AGS and
BGC-823 cells using TRIzol reagent (Life Technologies; Thermo
Fisher Scientific, Inc., Waltham, MA, USA) according to the
manufacturer's protocol. RNA was reversed-transcribed into cDNA
using the TaqMan RNA Reverse Transcription kit (Applied Biosystems;
Thermo Fisher Scientific, Inc.). qPCR was performed using SYBR
Green Supermix (Bio-Rad Laboratories, Inc., Hercules, CA, USA) and
the iCycleriQ Real-Time PCR system (Bio-Rad Laboratories, Inc.) as
described previously (19). The
thermocycling conditons were as followd: at 95°C for 10 min
followed by 50 cycles of 95°C for 10 sec, 55°C for 10 sec and 72°C
for 5 sec; 99°C for 1 sec; 59°C for 15 sec; 95°C for 1 sec; then
cooling to 40°C. Relative mRNA expression was normalized against
the endogenous control, GAPDH, using the 2−ΔΔCt method
(20). The primers used in the
current study was listed as follows: NNMT, forward,
CTGCCTAGACGGTGTGAAGG, and reverse, CTTGACCGCCTGTCTCAACT, and GAPDH,
forward, GAGAAGGCTGGGGCTCATTT, and reverse,
AGTGATGGCATGGACTGTGG.
Western blot analysis
Proteins samples were isolated from BGC-823 cells
using radioimmunoprecipitation assay buffer [1% TritonX-100, 15
mmol/l NaCl, 5 mmol/l EDTA and 10 mmol/l Tris/HCl (pH 7.0); Beijing
Solarbio Science & Technology Co., Ltd., Beijing, China]
supplemented with a protease and phosphatase inhibitor cocktail
(Merck KGaA, Darmstadt, Germany). A bicinchoninic protein assay kit
(Pierce; Thermo Fisher Scientific, Inc.) was used to determine the
protein concentration. Equal quantities of protein (15 µg) were
separated by 12% SDS-PAGE. Electrophoresed proteins were then
transferred onto polyvinylidene fluoride membranes. The membranes
were blocked with 8% skimmed milk in Tris-buffered saline with
Tween-20 (TBST; pH 7.5) for 2 h at room temperature and were
incubated with the following primary antibodies at 4°C overnight:
Anti-NNMT (1:1,000; cat no., ab119758; Abcam, Cambridge, UK),
anti-TGFβ (1:1,000; cat no., ab92486; Abcam), anti-Smad2, (1:1,000;
cat no., ab40855; Abcam), anti-epithelial (E)-cadherin (1:1,000;
cat no., ab76055; Abcam), anti-SMA (1:1,000; cat no., ab7817;
Abcam), anti-fibronectin (1:1,000; cat no., ab2413; Abcam),
anti-vimentin (1:1,000; cat no., ab8978; Abcam) and anti-GAPDH
(1:4,000; cat no., 5174; Cell Signaling Technology, Inc., Danvers,
MA, USA). Following multiple washes with tris-buffered saline with
Tween, the membranes were incubated with horseradish-peroxidase
(HRP)-conjugated goat anti-rabbit and anti-mouse IgG or
HRP-conjugated mouse anti-goat IgG (all 1:5,000; Origene
Technologies, Inc.) for 2 h at room temperature prior to another
wash in TBST. Protein bands were visualized using enhanced
chemiluminescence (EMD Millipore, Billerica, MA, USA) according to
the manufacturer's protocol. GAPDH was used as an internal
control.
Cell migration and invasion
assays
Cell migration assays were performed using Boyden
chambers (8-µm pore filter; Corning Inc., Corning, NY, USA). For
the cell invasion assay, the filter surfaces were precoated with
Matrigel (BD Biosciences, Franklin Lakes, NJ, USA). In brief,
BGC-823 cells were seeded at a density of 1×106
cells/well for 24 h and then transfected with Ad-NC or Ad-NNMT were
plated in the upper chamber in RPMI-1640 medium without FBS.
RPMI-1640 medium (600 µl) with 20% FBS was plated in the lower
chamber. After 48 h of incubation, non-migratory and non-invading
cells were removed with cotton swabs. The migratory or invasive
cells located on the lower side of the chamber were fixed in
methanol for 30 min at 37°C and stained with 0.5% crystal violet
for 1 h at 37°C. Stained cells were counted in 5 random fields
using fluorescence microscopy (magnification, ×40). All experiments
were performed in triplicate.
Wound healing assay
In brief, BGC-823 cells were seeded at a density of
1×106 cells/well for 24 h. The confluent monolayer of
cells was then wounded using a p200 pipette tip. The existing media
was replaced and fresh RPMI-1640 (GE Healthcare) supplemented with
10% fetal bovine serum (FBS; GE Healthcare), streptomycin (100
mg/ml) (Invitrogen; Thermo Fisher Scientific, Inc.) and penicillin
(100 IU/ml) were then added. The BGC-823 cells were then
transfected with Ad-NC or Ad-NNMT for 24 and 48 h immediately
following wounding, as per the aforementioned methodology. For each
well, 3 images were captured with a microscope at 0 and 24 h after
wounding.
Treatment with TGF-β1
In order to further validate the effects of NNMT in
EMT, In brief, BGC-823 cells were seeded at a density of
1×106 cells/well for 24 h. BGC-823 cells were
pre-incubated with 20 nM TGF-β1 (cat no. SRP0300; Sigma-Aldrich;
Merck KGaA) or distilled water for 24 h. si-NNMT or NC was
transfected into BGC-823 cells following TGF-β1 treatment in the
presence or absence of TGF-β1. BGC-823 cells were treated with
si-NNMT or NC, as per the aforementioned methodology.
Statistical analysis
Data were analyzed using SPSS software (version
13.0; SPSS, Inc., Chicago, IL, USA). Data are expressed as the mean
± standard error of the mean. Results were analyzed using Student's
t-test or one-way analysis of variance followed by Tukey's honest
significant difference test. P<0.05 was considered to indicate a
statistically significant difference.
Results
Increased expression of NNMT in
gastric cancer cells
First, the expression of NNMT was investigated in
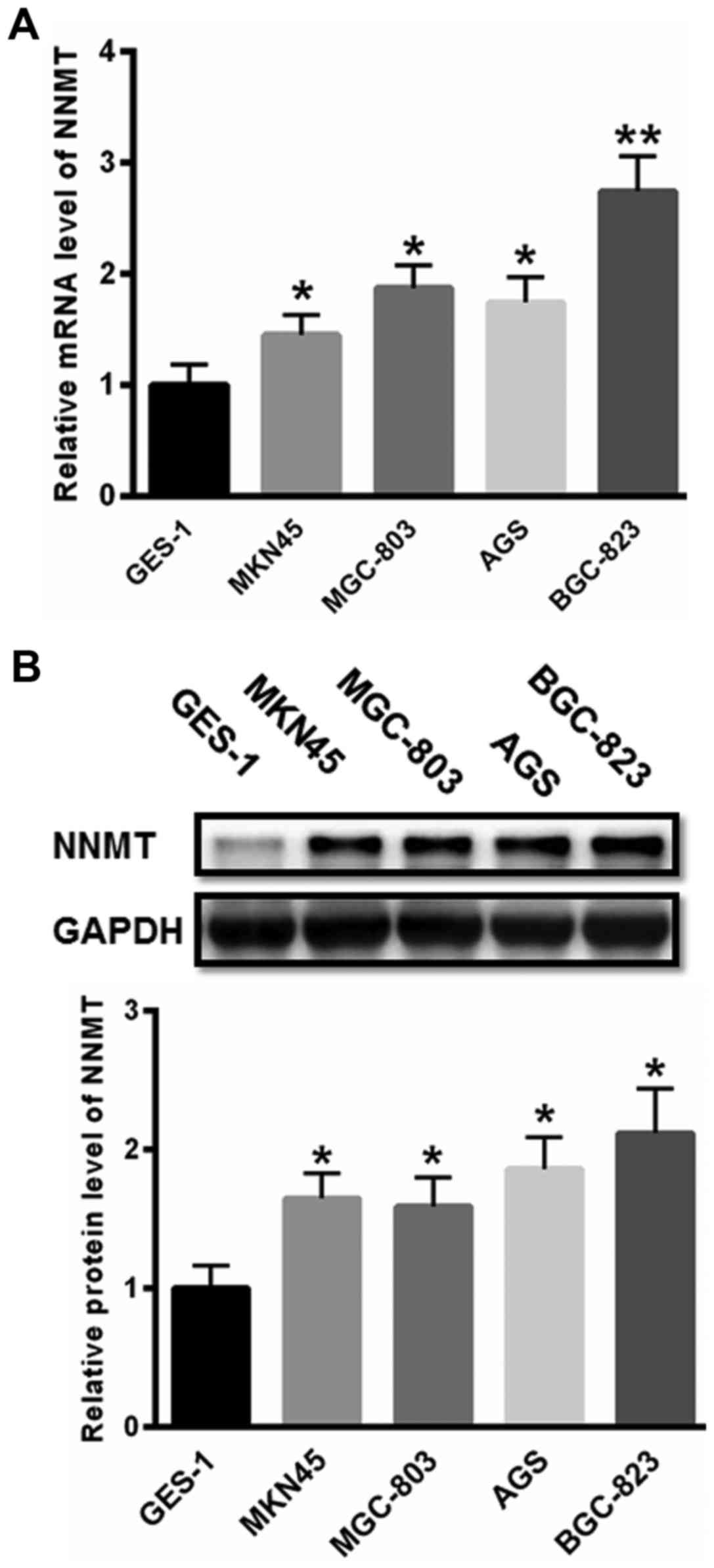
gastric cancer cells. As presented in Fig. 1A, the mRNA level of NNMT was
significantly increased in MKN45, MGC-803, AGS and BGC-823 cells
compared with that in normal GES-1 cells. Additionally, the protein
expression levels of NNMT were also significantly increased in
gastric cancer MKN45, MGC-803, AGS and BGC-823 cells compared with
that in the GES-1 cells (Fig. 1B).
The expression of NNMT was highest in the BGC-823 cells. Hence,
BGC-823 cells were selected for further study.
NNMT promotes EMT in BGC-823
cells
The present study investigated whether NNMT may
induce EMT in BGC-823 cells. The results demonstrated that
overexpression of NNMT in BGC-823 cells (achieved using Ad-NNMT)
led to significant changes in the morphology of the BGC-823 cells,
which acquired an elongated and spindle-shaped phenotype (Fig. 2A). Additionally, upregulation of NNMT
significantly increased the expression of mesenchymal markers,
including α-SMA, vimentin and fibronectin, but decreased the levels
of the epithelial marker E-cadherin (Fig.
2B). Furthermore, upregulation of NNMT significantly increased
the migration of the BGC-823 cells at 24 and 48 h, as assessed
using an in vitro wound healing assay (Fig. 2C). Treatment with Ad-NNMT increased
the migratory and invasive abilities of the BGC-823 cells compared
with that of the Ad-NC group, as assessed using Boyden chamber
assays (Fig. 2D). Collectively, these
results suggest that NNMT may exert an oncogenic function in
gastric cancer cells.
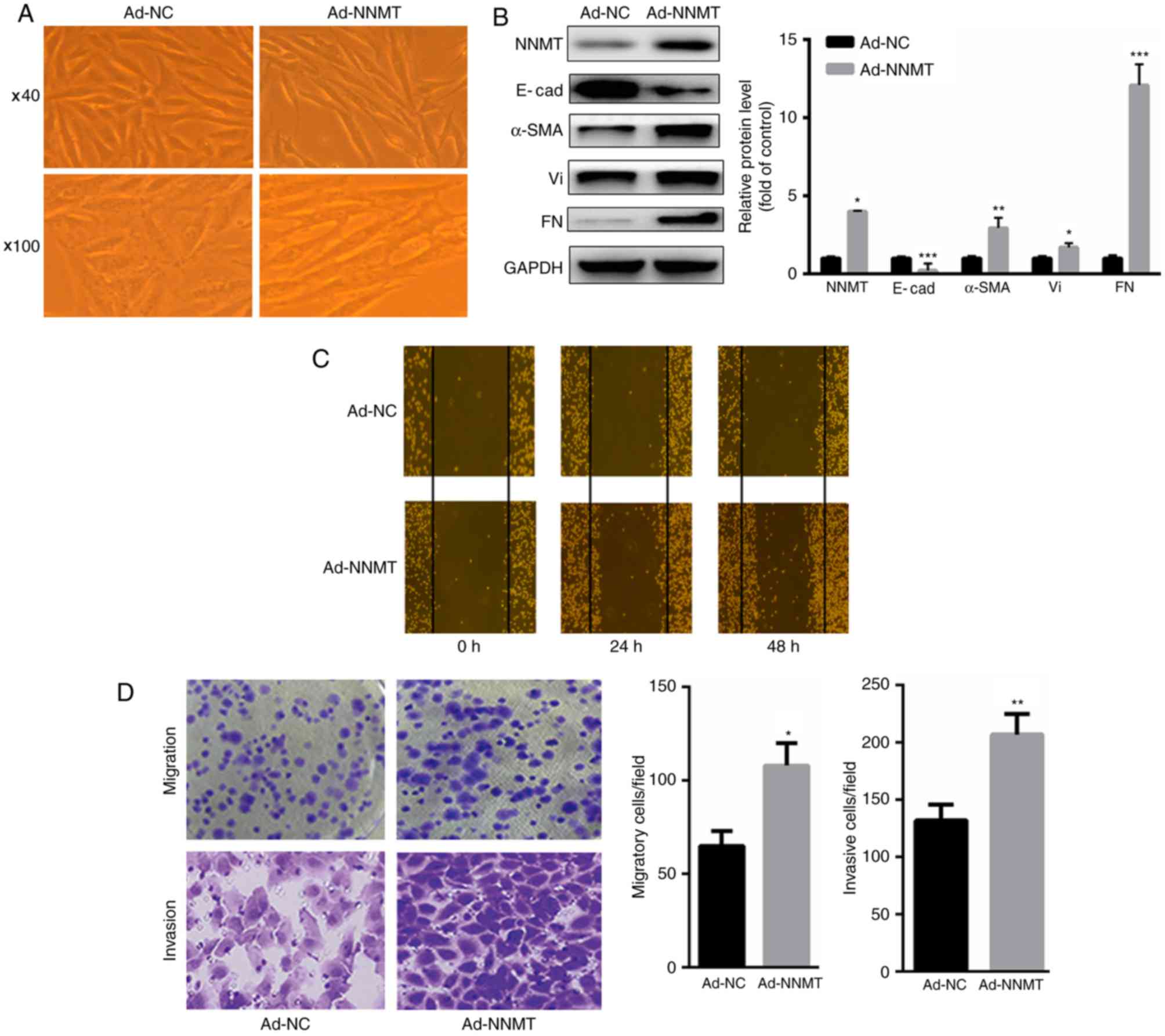 | Figure 2.NNMT promotes EMT in BGC-823 cells.
(A) Overexpression of NNMT led to significant morphological changes
in BGC-823 cells, which acquired an elongated and spindle-shaped
phenotype (magnification, ×40 and ×100). (B) Upregulation of NNMT
significantly increased the expression of α-SMA, Vi and FN, but
decreased the expression levels of E-cad. (C) Upregulation of NNMT
significantly increased the migration of BGC-823 cells at 24 and 48
h, as assessed using a wound healing assay. (D) Overexpression of
NNMT significantly increased the migratory and invasive ability of
BGC-823 cells. *P<0.05, **P<0.01 and ***P<0.001 vs. Ad-NC.
NNMT, nicotinamide N-methyltransferase; EMT, epithelial-mesenchymal
transition; Vi, vimentin; FN, fibronectin; E-cad,
E-cadherin/epithelial cadherin; α-SMA, α-smooth muscle actin; Ad,
adenovirus; NC, control. |
NNMT increases the expression level of
TGF-β1 in BGC-823 cells
Since TGF-β1 serves a key function in EMT, the
present study investigated whether NNMT may increase the expression
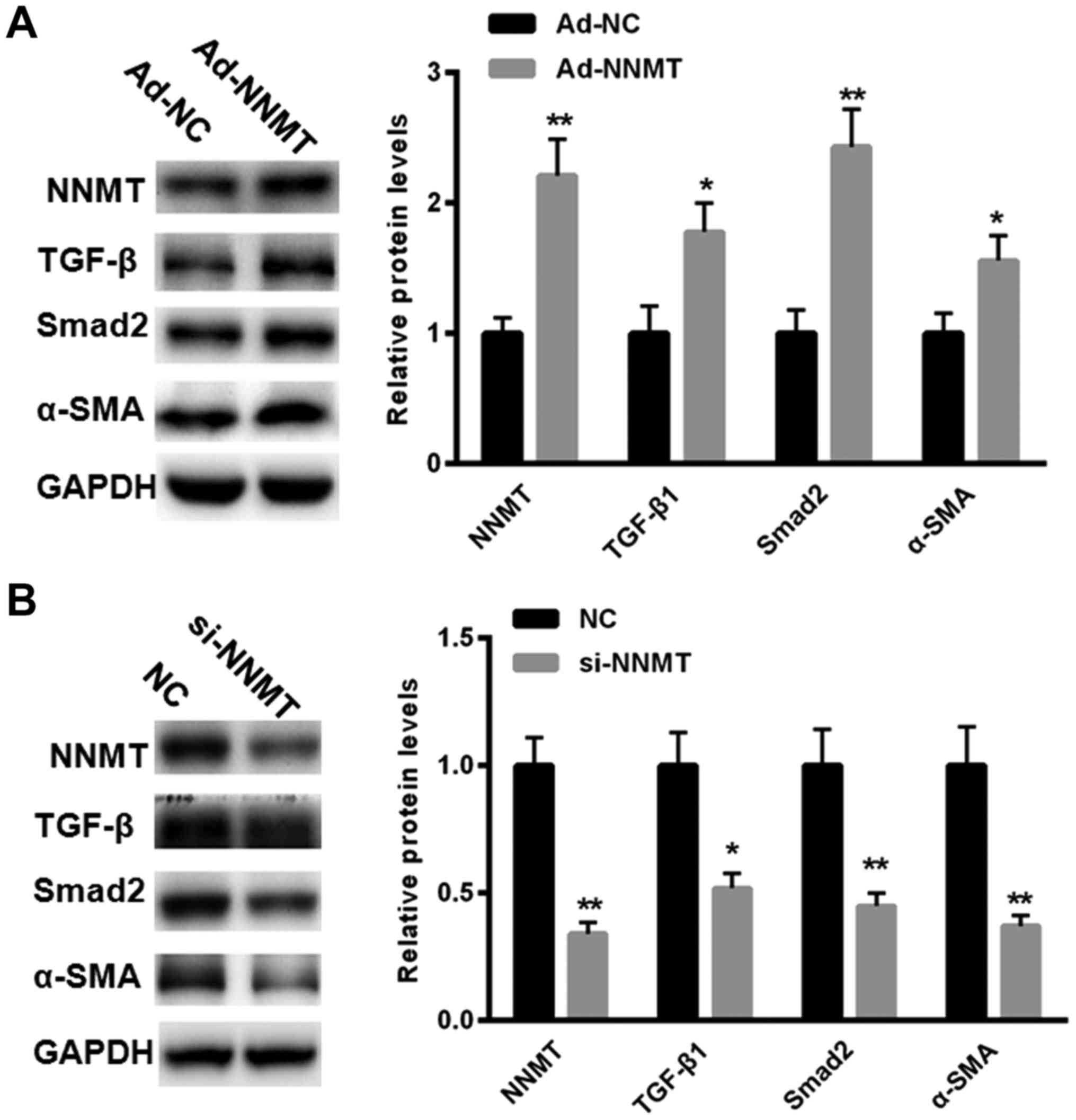
levels of TGF-β1 in BGC-823 cells. The results demonstrated that
overexpression of NNMT (achieved using Ad-NNMT) increased the
expression of TGF-β1 in BGC-823 cells, as assessed using western
blot analysis (Fig. 3A).
Additionally, treatment with Ad-NNMT increased the expression of
Smad2 and α-SMA in the BGC-823 cells compared with treatment with
Ad-NC group (Fig. 3A). In the present
study, the effects of downregulating the expression of NNMT using
siRNAs were assessed. The results demonstrated that treatment with
si-NNMT significantly inhibited the expression of TGF-β1, Smad2 and
α-SMA compared with that in the NC group in the BGC-823 cells
(Fig. 3B). These results suggest that
NNMT may upregulate the expression of TGF-β1, therefore promoting
EMT.
TGF-β1-induced EMT is partially
reversed in response to treatment with si-NNMT
In order to further validate the effects of NNMT in
EMT, BGC-823 cells were treated with si-NNMT, with or without
TGF-β1. As presented in Fig. 4A,
treatment with TGF-β1 significantly increased the expression of
Smad2, vimentin, fibronectin and α-SMA, but decreased the
expression of E-cadherin in the BGC-823 cells. However, treatment
with si-NNMT decreased the expression levels of Smad2, fibronectin
and α-SMA (Fig. 4A). Combined
treatment with si-NNMT and TGF-β1 significantly increased the
expression levels of Smad2, α-SMA and fibronectin but decreased the
expression levels of E-cadherin compared with that in the si-NNMT
group (Fig. 4A). Furthermore,
TGF-β1-mediated cell morphological changes were partially
eliminated by the silencing of NNMT (Fig.
4B). These results demonstrate that NNMT induces EMT partially
by mediating TGF-β1 signaling.
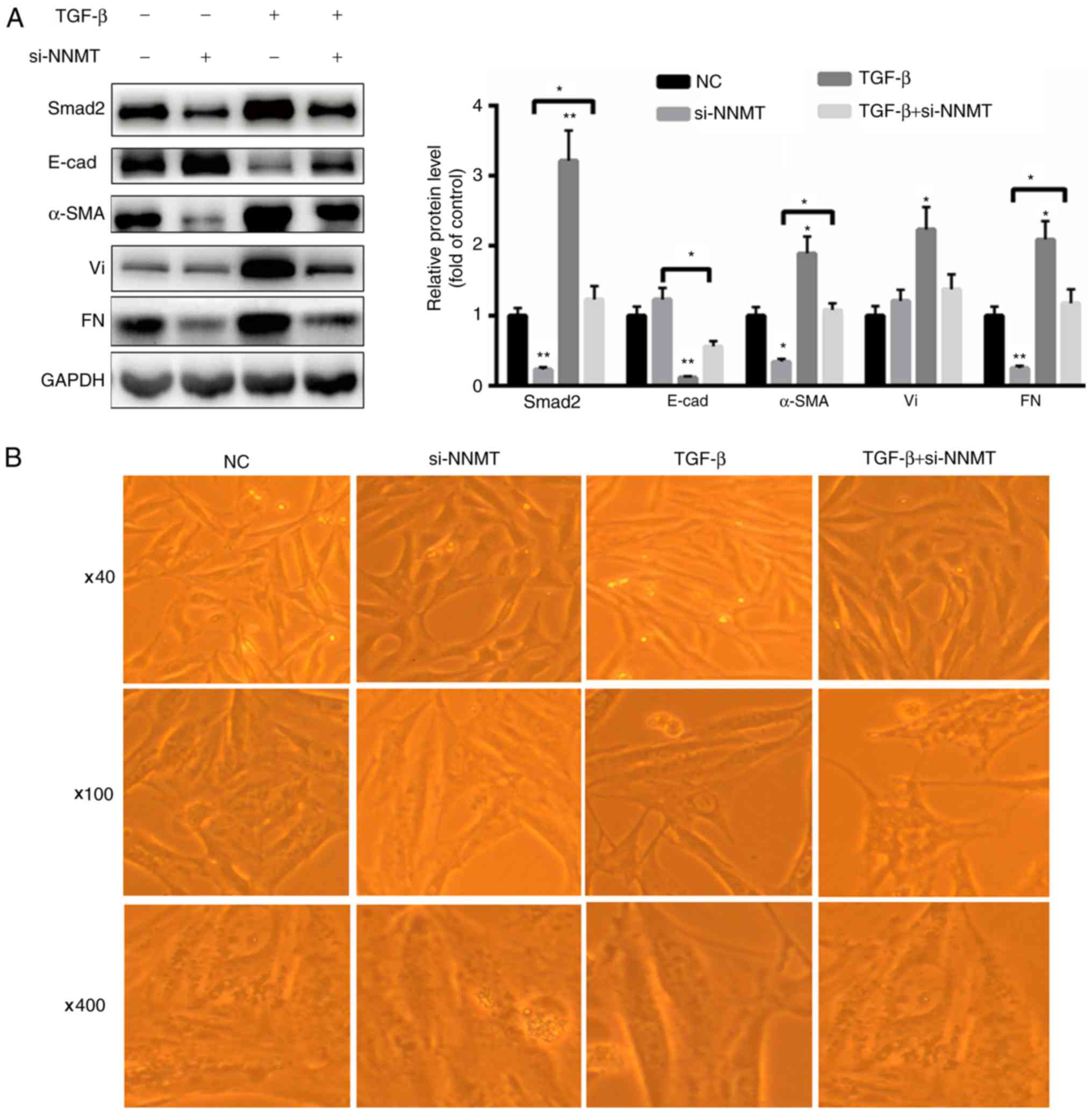 | Figure 4.TGF-β1-mediated EMT is partially
reversed by silencing of NNMT in BGC-823 cells. (A) TGF-β1
significantly increased the expression of Smad2 and α-SMA.
Treatment with si-NNMT partially reversed the changes in the
expression of EMT markers, which were induced in response to
treatment with TGF-β1. (B) Silencing of NNMT partially reversed
TGF-β1-mediated cellular morphological changes (magnification, ×40,
×100 and ×400). *P<0.05 and **P<0.01 vs. control. NNMT,
nicotinamide N-methyltransferase; TGF, transforming growth factor;
Smad, mothers against decapentaplegic homolog; Vi, vimentin; FN,
fibronectin; E-cad, E-cadherin/epithelial cadherin; α-SMA, α-smooth
muscle actin; Ad, adenovirus; NC, control; si, siRNA/small
interfering RNA. |
Discussion
NNMT catalyzes the methylation of nicotinamide and
pyridine, therefore regulating the metabolism of drugs and other
xenobiotics (21). The abnormal
expression of NNMT has been widely identified in several types of
tumor (22,23). It has been demonstrated that NNMT is
involved in the malignant migration of tumor cells and that it may
be used as a potential biomarker for predicting tumor invasion
(24,25). In the present study, it was
demonstrated that the expression of NNMT was significantly
increased in gastric cancer cell lines compared with that in normal
control cell lines. However, the precise molecular mechanism
underlying the NNMT-mediated progression of gastric cancer remains
unclear.
EMT is an important process in carcinogenesis since
it increases the invasive ability of cancer cells (26,27). As a
result of EMT, epithelial-derived tumor cells lose their features
and obtain mesenchymal-like characteristics (28,29), and
tumor cells invade the surrounding tissue and break through the
capillary into the circulatory system, leading to distant
metastasis (30). During EMT, the
expression level of molecular markers for epithelial cells,
including E-cadherin, are decreased, but the expression of
molecular markers of mesenchymal cells, including vimentin,
neuronal cadherin and α-SMA, are increased (31,32).
In the present study, the function of NNMT in the
EMT-mediated changes in gastric cancer cells was evaluated. The
results demonstrated that that upregulation of NNMT led to
morphological changes in BGC-823 cells, which acquired a
spindle-shaped phenotype, suggesting that NNMT may promote EMT in
cancer cells. To further investigate how NNMT regulated EMT, the
effects of NNMT on the TGF-β1 signaling pathway were investigated.
The results revealed that the overexpression of NNMT (achieved
using Ad-NNMT) induced the expression of TGF-β1 in gastric cancer
cells. Additionally, TGF-β1-induced EMT was partially reversed by
the silencing of NNMT, as demonstrated by the morphological changes
observed under light microscopy and the changes in the expression
of EMT markers detected using western blot analysis. These results
indicated that NNMT promoted EMT in gastric cancer cells mainly by
upregulating TGF-β1 expression. It has been demonstrated that
NNMT-mediated methylation is an important conjugation reaction in
the biotransformation of a number of drugs and xenobiotics,
including pyridine and other structurally-associated compounds
(18). The epigenetic silencing of
TGF-β1 genes is associated with the development of pituitary
adenoma (33). In the present study,
it was hypothesized that NNMT-mediated changes in DNA methylation
may be involved in TGF-β-induced EMT in gastric cancer cells. A
previous study demonstrated that the phosphoinositide
3-kinase/protein kinase B signaling pathway exerts a critical
function in the NNMT-mediated invasion of renal carcinoma cells
(34). It has been revealed that NNMT
increased the resistance to 5-fluorouracil partially through
suppressing the signal-regulating kinase 1/p38 mitogen-activated
protein kinase signaling pathway in colorectal cancer cells
(17). Therefore, additional
signaling pathways may be involved in the NNMT-mediated migration
and invasion of gastric cancer cells and further studies are
required to confirm these conclusions.
The results of the present study demonstrated that
the overexpression of NNMT increased the expression of TGF-β1 in
gastric cancer cells, suggesting that NNMT may activate the
TGF-β1/Smad signaling, which in turn promotes EMT. These results
suggest that NNMT may be associated with the occurrence and
development of gastric tumors. Future studies investigating the
clinical and pathological characteristics of NNMT may provide novel
predictive markers for the pathological classification and
prognosis of cancer.
References
|
1
|
Zhao Z, Yin Z and Zhao Q: Red and
processed meat consumption and gastric cancer risk: A systematic
review and meta-analysis. Oncotarget. 8:30563–30575. 2017.
View Article : Google Scholar : PubMed/NCBI
|
|
2
|
Yuan X, Meng Y, Li P, Ge N, Kong F, Yang
L, Björkholm M, Zhao S and Xu D: The association between the TERT
rs2736100 AC genotype and reduced risk of upper tract urothelial
carcinomas in a Han Chinese population. Oncotarget. 7:31972–31979.
2016.PubMed/NCBI
|
|
3
|
Jia S, Qu T, Wang X, Feng M, Yang Y, Feng
X, Ma R, Li W, Hu Y, Feng Y, et al: KIAA1199 promotes migration and
invasion by Wnt/beta-catenin pathway and MMPs mediated EMT
progression and serves as a poor prognosis marker in gastric
cancer. PLoS One. 12:e01750582017. View Article : Google Scholar : PubMed/NCBI
|
|
4
|
Wang G, Fu Y, Liu G, Ye Y and Zhang X:
miR-218 inhibits proliferation, migration, and EMT of gastric
cancer cells by targeting WASF3. Oncol Res. 25:355–364. 2017.
View Article : Google Scholar : PubMed/NCBI
|
|
5
|
Xiang J, Fu X, Ran W and Wang Z: Grhl2
reduces invasion and migration through inhibition of TGFβ-induced
EMT in gastric cancer. Oncogenesis. 6:e2842017. View Article : Google Scholar : PubMed/NCBI
|
|
6
|
Xu J, Liu D, Niu H, Zhu G, Xu Y, Ye D, Li
J and Zhang Q: Resveratrol reverses Doxorubicin resistance by
inhibiting epithelial-mesenchymal transition (EMT) through
modulating PTEN/Akt signaling pathway in gastric cancer. J Exp Clin
Cancer Res. 36:192017. View Article : Google Scholar : PubMed/NCBI
|
|
7
|
Yang Y, Zhang J, Yan Y, Cai H, Li M, Sun
K, Wang J, Liu X, Wang J and Duan X: Low expression of Rap1GAP is
associated with epithelial-mesenchymal transition (EMT) and poor
prognosis in gastric cancer. Oncotarget. 8:8057–8068.
2017.PubMed/NCBI
|
|
8
|
Carino A, Graziosi L, D'Amore C, Cipriani
S, Marchianò S, Marino E, Zampella A, Rende M, Mosci P, Distrutti
E, et al: The bile acid receptor GPBAR1 (TGR5) is expressed in
human gastric cancers and promotes epithelial-mesenchymal
transition in gastric cancer cell lines. Oncotarget. 7:61021–61035.
2016. View Article : Google Scholar : PubMed/NCBI
|
|
9
|
Zhu XJ, Lin YJ, Chen W, Wang YH, Qiu LQ,
Cai CX, Xiong Q, Chen F, Chen LH, Zhou Q and Li JH: Physiological
study on association between nicotinamide N-methyltransferase gene
polymorphisms and hyperlipidemia. Biomed Res Int. 2016:75219422016.
View Article : Google Scholar : PubMed/NCBI
|
|
10
|
Li JH, Chen W, Zhu XJ, Lin YJ, Qiu LQ, Cai
CX, Wang YH, Xiong Q, Chen F and Chen LH: Associations of
nicotinamide N-methyltransferase gene single nucleotide
polymorphisms with sport performance and relative maximal oxygen
uptake. J Sports Sci. 35:2185–2190. 2017. View Article : Google Scholar : PubMed/NCBI
|
|
11
|
Chen C, Wang X, Huang X, Yong H, Shen J,
Tang Q, Zhu J, Ni J and Feng Z: Nicotinamide N-methyltransferase: A
potential biomarker for worse prognosis in gastric carcinoma. Am J
Cancer Res. 6:649–663. 2016.PubMed/NCBI
|
|
12
|
Fedorowicz A, Mateuszuk Ł, Kopec G, Skórka
T, Kutryb-Zając B, Zakrzewska A, Walczak M, Jakubowski A, Łomnicka
M, Słomińska E and Chlopicki S: Activation of the nicotinamide
N-methyltransferase (NNMT)-1-methylnicotinamide (MNA) pathway in
pulmonary hypertension. Respir Res. 17:1082016. View Article : Google Scholar : PubMed/NCBI
|
|
13
|
Sazci G, Sazci B, Sazci A and Idrisoglu
HA: Association of nicotinamide-N-methyltransferase gene rs694539
variant with epilepsy. Mol Neurobiol. 53:4197–4200. 2016.
View Article : Google Scholar : PubMed/NCBI
|
|
14
|
Sartini D, Muzzonigro G, Milanese G,
Pierella F, Rossi V and Emanuelli M: Identification of nicotinamide
N-methyltransferase as a novel tumor marker for renal clear cell
carcinoma. J Urol. 176:2248–2254. 2006. View Article : Google Scholar : PubMed/NCBI
|
|
15
|
Roessler M, Rollinger W, Palme S, Hagmann
ML, Berndt P, Engel AM, Schneidinger B, Pfeffer M, Andres H, Karl
J, et al: Identification of nicotinamide N-methyltransferase as a
novel serum tumor marker for colorectal cancer. Clin Cancer Res.
11:6550–6557. 2005. View Article : Google Scholar : PubMed/NCBI
|
|
16
|
van Haren MJ, Sastre Toraño J, Sartini D,
Emanuelli M, Parsons RB and Martin NI: A rapid and efficient assay
for the characterization of substrates and inhibitors of
nicotinamide N-methyltransferase. Biochemistry. 55:5307–5315. 2016.
View Article : Google Scholar : PubMed/NCBI
|
|
17
|
Xie X, Liu H, Wang Y, Zhou Y, Yu H, Li G,
Ruan Z, Li F, Wang X and Zhang J: Nicotinamide N-methyltransferase
enhances resistance to 5-fluorouracil in colorectal cancer cells
through inhibition of the ASK1-p38 MAPK pathway. Oncotarget.
7:45837–45848. 2016.PubMed/NCBI
|
|
18
|
Lim BH, Cho BI, Kim YN, Kim JW, Park ST
and Lee CW: Overexpression of nicotinamide N-methyltransferase in
gastric cancer tissues and its potential post-translational
modification. Exp Mol Med. 38:455–465. 2006. View Article : Google Scholar : PubMed/NCBI
|
|
19
|
Guo J, Li M, Meng X, Sui J, Dou L, Tang W,
Huang X, Man Y, Wang S and Li J: MiR-291b-3p induces apoptosis in
liver cell line NCTC1469 by reducing the level of RNA-binding
protein HuR. Cell Physiol Biochem. 33:810–822. 2014. View Article : Google Scholar : PubMed/NCBI
|
|
20
|
Livak KJ and Schmittgen TD: Analysis of
relative gene expression data using real-time quantitative PCR and
the 2(-Delta Delta C(T)) method. Methods. 25:402–408. 2001.
View Article : Google Scholar : PubMed/NCBI
|
|
21
|
Li Q, He MD, Mao L, Wang X, Jiang YL, Li
M, Lu YH, Yu ZP and Zhou Z: Nicotinamide N-methyltransferase
suppression participates in nickel-induced histone H3 Lysine9
dimethylation in BEAS-2B cells. Cell Physiol Biochem. 41:2016–2026.
2017. View Article : Google Scholar : PubMed/NCBI
|
|
22
|
Neelakantan H, Vance V, Wang HL, McHardy
SF and Watowich SJ: Noncoupled fluorescent assay for direct
real-time monitoring of nicotinamide N-methyltransferase activity.
Biochemistry. 56:824–832. 2017. View Article : Google Scholar : PubMed/NCBI
|
|
23
|
Pissios P: Nicotinamide
N-methyltransferase: More than a vitamin B3 clearance enzyme.
Trends Endocrinol Metab. 28:340–353. 2017. View Article : Google Scholar : PubMed/NCBI
|
|
24
|
Hong S, Moreno-Navarrete JM, Wei X,
Kikukawa Y, Tzameli I, Prasad D, Lee Y, Asara JM, Fernandez-Real
JM, Maratos-Flier E and Pissios P: Nicotinamide N-methyltransferase
regulates hepatic nutrient metabolism through Sirt1 protein
stabilization. Nat Med. 21:887–894. 2015. View Article : Google Scholar : PubMed/NCBI
|
|
25
|
Zhou SS, Li D and Zhou Y: Management of
nicotinamide N-methyltransferase overexpression: Inhibit the enzyme
or reduce nicotinamide intake? Diabetologia. 58:2191–2192. 2015.
View Article : Google Scholar : PubMed/NCBI
|
|
26
|
Chong Y, Tang D, Gao J, Jiang X, Xu C,
Xiong Q, Huang Y, Wang J, Zhou H, Shi Y and Wang D: Galectin-1
induces invasion and the epithelial-mesenchymal transition in human
gastric cancer cells via non-canonical activation of the hedgehog
signaling pathway. Oncotarget. 7:83611–83626. 2016. View Article : Google Scholar : PubMed/NCBI
|
|
27
|
Chong Y, Tang D, Xiong Q, Jiang X, Xu C,
Huang Y, Wang J, Zhou H, Shi Y, Wu X and Wang D: Galectin-1 from
cancer-associated fibroblasts induces epithelial-mesenchymal
transition through β1 integrin-mediated upregulation of Gli1 in
gastric cancer. J Exp Clin Cancer Res. 35:1752016. View Article : Google Scholar : PubMed/NCBI
|
|
28
|
Cui Y, Wang Y, Li H, Li Q, Yu Y, Xu X, Xu
B and Liu T: Asparaginyl endopeptidase promotes the invasion and
metastasis of gastric cancer through modulating
epithelial-to-mesenchymal transition and analysis of their
phosphorylation signaling pathways. Oncotarget. 7:34356–34370.
2016. View Article : Google Scholar : PubMed/NCBI
|
|
29
|
Dai J, Qian C, Su M, Chen M and Chen J:
Gastrokine-2 suppresses epithelial mesenchymal transition through
PI3K/AKT/GSK3β signaling in gastric cancer. Tumour Biol.
37:12403–12410. 2016. View Article : Google Scholar : PubMed/NCBI
|
|
30
|
Ding WJ, Zhou M, Chen MM and Qu CY: HOXB8
promotes tumor metastasis and the epithelial-mesenchymal transition
via ZEB2 targets in gastric cancer. J Cancer Res Clin Oncol.
143:385–397. 2017. View Article : Google Scholar : PubMed/NCBI
|
|
31
|
Duan F, Jia D, Zhao J, Wu W, Min L, Song
S, Wu H, Wang L, Wang H, Ruan Y and Gu J: Loss of GFAT1 promotes
epithelial-to-mesenchymal transition and predicts unfavorable
prognosis in gastric cancer. Oncotarget. 7:38427–38439. 2016.
View Article : Google Scholar : PubMed/NCBI
|
|
32
|
Fan Y, Wang YF, Su HF, Fang N, Zou C, Li
WF and Fei ZH: Decreased expression of the long noncoding RNA
LINC00261 indicate poor prognosis in gastric cancer and suppress
gastric cancer metastasis by affecting the epithelial-mesenchymal
transition. J Hematol Oncol. 9:572016. View Article : Google Scholar : PubMed/NCBI
|
|
33
|
Ruskyte K, Liutkevicienė R, Vilkeviciute
A, Vaitkiene P, Valiulytė I, Glebauskiene B, Kriauciuniene L and
Zaliuniene D: MMP-14 and TGFβ-1 methylation in pituitary adenomas.
Oncol Lett. 12:3013–3017. 2016. View Article : Google Scholar : PubMed/NCBI
|
|
34
|
Tang SW, Yang TC, Lin WC, Chang WH, Wang
CC, Lai MK and Lin JY: Nicotinamide N-methyltransferase induces
cellular invasion through activating matrix metalloproteinase-2
expression in clear cell renal cell carcinoma cells.
Carcinogenesis. 32:138–145. 2011. View Article : Google Scholar : PubMed/NCBI
|