Introduction
Chronic prostatitis has a high incidence; its
prevalence rate has been reported to be 9%, similar to that of
ischemic heart disease or diabetes (1). It is estimated that the global
incidence is 9–14% (2). According
to the Classification Criteria of the United States National
Institutes of Health (NIH) (3),
prostatitis syndromes are divided into 4 categories: type I is
acute bacterial prostatitis, type II is chronic bacterial
prostatitis, type III is chronic non-bacterial prostatitis/chronic
pelvic pain syndrome (CNP/CPPS) and type IV is asymptomatic
inflammatory prostatitis. CNP/CPPS may also be divided into
inflammatory [IIIA, white blood cell (WBC) >10/high power field
(HPF) in expressed prostatic secretion (EPS)] and non-inflammatory
(IIIB, WBC ≤10/HPF in EPS) categories (4). CPPS is the most common form of
chronic prostatitis, a frequently occurring disease in males with
an unknown etiological mechanism, complex clinical symptoms,
specific anatomical position and clinically recurrent attacks.
Antibiotics, particularly quinolones, affect the
cytokine activity of the immune response, specifically by
regulating the expression of IL-6 and IL-8 and decreasing the
cytokine levels in the prostate fluid of chronic prostatitis
patients. Antibiotics also have analgesic effects, which have been
reported to alleviate the pain symptoms of chronic prostatitis
(5–9). However, there have been contrary
studies (10) in which antibiotics
were not observed to be the preferred therapy. In patients treated
with antibiotics, it was observed that the patient-perceived
symptom improvement rate, symptom score improvement rate and
prostate fluid routine WBC reduction rate were not statistically
significantly improved compared with those of the control group. In
particular, the associated pain, which was not treated
satisfactorily for a long period, caused the patients to lose
confidence and even led to suicidal thoughts.
At present there is no definitively effective
treatment and numerous patients experience various degrees of
sexual dysfunction, neuropsychiatric symptoms, fatigue, insomnia
and mood disorders, and semen quality is seriously affected in
certain patients. The condition is a cause of infertility and
seriously affects the quality of life and work. Currently,
treatments such as Western or Chinese medicine and physical therapy
do not have good efficacy and if patients discontinue their
medication for a few days, the symptoms may return to their
original status, without signs of improvement. Certain patients
even consider that the symptoms are aggravated by medication. We
propose that the reasons for the above lie in the fact that the
therapy is unable to clear the accumulation of inflammatory
metabolites from the prostatic tube, acini and interstitial region.
Long-term blockage, hardening and tension in the local gland duct
is likely to generate a variety of symptoms and since these factors
are not readily relieved by drug therapy or the autologous system,
the treatment is invalid. It has been suggested that treatment
should eliminate these factors, as in the Western therapy theory,
of ‘operating on an ulcer to clean a toxin’. Only in this way may
the treatment provide instant results.
In order to improve the treatment of CPPS, we
combined the prostatic anatomy of Western medicine with Chinese
acupuncture principles and techniques, to design a one-finger
manipulation method for clearing the blockage. This may eliminate
the deposits of inflammatory metabolic products from the prostate,
in a similar manner to Western incision methods, improve the local
metabolism and circulation, rapidly eliminate inflammatory products
and improve the symptoms. The clinical application of this approach
achieved stable curative effects and satisfactory results.
Subjects and methods
Clinical data
Between January 2008 and March 2012, 721 cases of
CPPS, comprising male outpatients from the Department of
Reproductive Medicine, Zhejiang Provincial Hospital of Integrated
Chinese and Western Medicine (Hangzhou, China), including 307
unmarried and 414 married patients, were treated and observed. All
the patients had a sexual history and the course of the condition
was 5–183 months, with an average of 28.3 months. The patients all
received antibiotics, α receptor blockers, antiphlogistic
analgesics and drugs, which were ineffective. Therefore, patients
were treated with manipulation. The oldest patient was 63 years
old, the youngest was 17 years old, and the average age was 32.6
years old. The symptoms were as follows: 320 cases of perineal
pain, 291 of perianal pain, 340 of lower abdomen and groin area
aches, 298 of penile pain, 251 of double inner thigh pain, 293 of
urinary frequency, 233 of more-frequent nocturia, 121 of urine
bifurcation, 302 of delayed urination, 293 of neurasthenia, 353 of
sleep disorders, 387 of sexual dysfunction, 373 of memory decline,
391 of fatigue, 149 of testicular pain, 187 of lumbosacral pain,
118 of suprapubic pain, 194 of urinary pain or burning sensations,
43 of ejaculatory pain, 238 of incomplete urination, 238 of wet
scrotum and 229 of increased dreams. The rectal digital examination
results were as follows: 453 cases of unsmoothly surfaced prostate,
463 of texture hardening, 393 of swelling and 565 of nodosity. In
the prostate fluid routine examination, the leukocyte counts were
>3–40/HPF, the lecithin corpuscle density was reduced and the
EPS bacterial culture results of all cases (Meares-Stamey two-cup
method) (3) were negative,
consistent with the diagnostic standard of NIH-CPPS. Ultrasound
examination prior to the treatment showed inhomogeneous echo or
calcification; no echo area around the prostate peripheral area; or
no clear echo from the prostate film. The present study was
conducted in accordance with the Declaration of Helsinki and with
approval from the Ethics Committee of Zhejiang Provincial Hospital
of Integrated Chinese and Western Medicine. Written informed
consent was obtained from all participants.
The patients were divided into two groups according
to the EPS routine examination results: group IIIA (inflammatory
group), 440 cases (EPS WBC >10/HPF) and group IIIB
(non-inflammatory group), 281 cases (EPS WBC ≤10/HPF). The average
ages were 32.2 and 32.8 years and the average durations were 28.2
and 28.5 months in groups IIIA and IIIB, respectively. According to
the chronic prostatitis symptom index (NIH-CPSI) scoring method
(11), the scores in the two
groups were 26.79 and 24.59, respectively, with no significant
difference between them (P>0.05).
Treatment methods
The treatment method was based on the prostate
massage method (12). By combining
traditional Chinese medicine acupuncture principles and techniques.
we designed the prostate manipulation method, detailed as follows:
i) The physician must understand traditional Chinese medical theory
and knowledge and have mastered the basic skills and techniques of
massage, particularly one-finger manipulation massage (13–18).
ii) The patient first evacuated their bowels by defecation, then
the physician pulled back the foreskin of the patient’s penis to
completely expose the urethra and sterilized disposable film gloves
were used to cover the whole scrotum and penis and accept the
prostatic discharge. The patient adopted a knee-chest position
while kneeling down on a couch with the arms on the sides of the
head and the waist angled straight downward. The angle between the
lumbar and thigh was 75–85° and the anus formed an angle of ∼45°
with the couch surface. iii) The physician wore sterilized medical
disposable latex gloves or disposable PE gloves and stood upright
to the right (left), parallel to the patient. PPI-iodine was used
for the disinfection of the anus and surrounding area. After
lubricating the left (right)-hand finger with a disinfected medical
cotton ball or vaseline paraffin oil, the physician then lubricated
the patient’s anus with paraffin oil cotton or vaseline, using
gentle massage to facilitate acceptance by the patient. The right
(left)-hand finger gently contacted the patients’ external anal
aperture and was inserted into the rectum along the rectal tube,
until it touched the prostate. iv) Through digital rectal
examination, the prostate size, texture, presence of nodules,
tenderness, swelling, elasticity and degree of smoothness were
evaluated (19). v) When
performing one-finger manipulation, the central sulcus was set as
the center line, and standard manipulation techniques from right
(left) to left (right), such as pointing, rolling, rubbing and
pushing, were used. The massaging procedure was carried out in
segmental order, with each section treated 3–4 times. The pressure
applied was flexible, and varied in power and strength according to
the lesion texture. The strength and technique applied were
selected according to the observed status of the patient. For
instance, if the finger pulp was able to touch the end section of
the prostate, then the hook-push method was applied. In certain
patients, the hooking-push of the prostate was carried out along
the longitudinal axis, by compressing and sliding forward and
backward, which was more conducive to prostate drainage. In the
central sulcus, the finger pulp applied point-pressure and
linear-pressure from the distal to proximal points, with the same
method repeated on the other side. If necessary, the physician
supported the lower back and abdominal parts of the patient with
the left (right) hand to adjust the patients’ posture if pain was
experienced, while observing the patient’s behavior and expression
and talking with the patient to relieve his pain. When the patient
felt an effusion, repeated pushing and pressing once or twice was
used and the patient was asked to kneel straight. The physician
used their left (right) hand to squeeze, pinch, rub and press
homeopathically forward from the penis and scrotum root, which
forced the overflowing prostatic secretions to flow into the film
glove. These secretions were then sent for testing. If the drainage
method was used, photographic images of the secretions were
captured to enable changes in the quantity and properties of the
prostate discharge during the whole process of manipulation to be
observed. vi) Following the manipulation, clockwise
(counterclockwise) point-pushing with the finger pulp was used to
treat prostate nodules, stiffness, swelling, tenderness and
induction points, for the facilitation of improved discharge of the
local gland duct sediment, while paying attention to the patient’s
response. When necessary, the left (right) hand performed
corresponding matching massage in the lower abdomen and perineal
areas while the right (left) finger manipulated. For example,
two-finger manipulation: the exterior and interior fingers
corresponded to each other, separated by related tissues in the
abdomen and perineum, while they pushed; palm-finger manipulation:
using the exterior part of the palm, the finger was pushed around,
setting the palm center to the settling point, with the hand
pushing around this center; fist-finger manipulation: the finger
pulp pointed at the corresponding glands or sensitive points, then
the fist was used to move the body forwards and backwards. During
the use of these methods, sustainable clamping pressure was applied
to the tissues to strengthen the discharge capacity of the
continuous secretion. vii) Finally, the physician slowly withdrew
the finger, stopping for 3–5 sec when it was removed from the anus.
viii) During the entire drainage therapy, attention was paid to the
patient’s tolerance and care was taken to apply moderate strength,
a stable force and safe methods, and to avoid injury to the
rectum.
Observation indices
The manipulation was performed once every 3 days and
during the treatment, tobacco, alcohol and spicy food were
prohibited and only moderate sexual activity was recommended.
Treatment periods were set as 30 days and at the end of each
treatment period, follow-up was performed to assess the NIH-CPSI
score (11) and carry out routine
EPS examination. After 3 periods, the therapeutic effects were
evaluated. Prior to and following the treatment, routine prostate,
liver function, blood, urine, electrocardiogram and adverse
reactions were evaluated.
Efficacy standard
The EPSRt WBC count scoring criteria used in the two
groups was as follows: 0 points, WBC count <10/HPF; 1 point,
10–20/HPF; 2 points, 20–50/HPF; 3 points, >50/HPF. The efficacy
criteria were: significantly effective, NIH-CPSI score reduced by
≥10 points compared with that before treatment and EPS WBC count
score reduced by ≥2 points compared with normal or that before
treatment; effective, NIH-CPSI score reduced by ≥5 points compared
with that before treatment and EPS WBC count score reduced by ≥1
point compared with that before treatment; invalid, NIH-CPSI score
reduced by <5 compared with that before treatment or EPS WBC
count score reduced by <1 compared with that before
treatment.
Statistical analysis
SPSS 15.0 software was used to carry out the
statistical analysis and the measurement data were expressed as the
mean ± SD. Comparisons of NIH-CPSI score and WBC count score in
EPSRt used the paired t-test and the rank-sum test was used for
comparisons between the two groups. P<0.05 was considered to
indicate a statistically significant result.
Results
Treatment results
Following three treatment periods, the effectiveness
rate in the IIIA group was 72.3%, with an efficiency of 15.9%,
while those of the IIIB group were 71.8 and 16.3%, respectively.
Through statistical analysis, the effects in the two groups were
not significantly different (P>0.05). The NIH-CPSI and EPSRt WBC
count scores before and after treatment are shown in Table I. Following each treatment, all
NIH-CPSI scores of the two groups were significantly improved
(P<0.01; P<0.05). The group IIIA WBC count score was reduced
in the first and third course, although no clear changes were
observed following the second course (Table I). Following the treatment,
ultrasound examination revealed that the prostate inhomogeneous
echo, film anechoic and anechoic regions surrounding the prostate
had disappeared in 306 cases.
 | Table IComparison of the NIH-CPSI and EPSRt
WBC count scores of the two groups (mean ± S). |
Table I
Comparison of the NIH-CPSI and EPSRt
WBC count scores of the two groups (mean ± S).
| Group | Period | Pain | Urine symptoms | Life quality | Total score | WBC count score |
|---|
| IIIA (n=40) | Before | 10.53±3.31 | 7.56±2.29 | 9.35±2.87 | 26.79±8.31 | 2.56±0.87 |
| 1 | 7.38±4.02a | 5.96±2.74a | 7.82±3.21a | 21.79±7.39a | 1.79±0.73a |
| 2 | 6.10±4.36a | 4.48±2.35a | 6.49±3.31a | 17.98±7.89a | 1.51±0.83 |
| 3 | 3.83±1.59a | 2.19±1.12a | 3.23±1.37a | 9.13±3.79a | 1.03±1.11b |
| IIIB (n=281) | Before | 9.93±3.12 | 6.96±2.37 | 8.93±3.25 | 24.99±8.73 | |
| 1 | 7.04±2.13a |
4.93±1.39ad |
6.83±2.23ad |
19.73±5.69ac | |
| 2 | 5.77±2.27a |
3.39±1.41ad |
5.39±2.14ac |
14.91±6.15ac | |
| 3 |
2.19±0.93ac | 1.93±1.11a | 2.91±1.31a |
7.53±3.21ac | |
During treatment, 493 cases experienced a small
amount of abdominal perineal pleasure, while in the first 3–5
manipulations, 247 cases appeared to suffer from increased
flatulence or defecation frequency, 35 had small amounts of blood
in their urine, 25 ejaculated a brown liquid and 95 had thick
byssine urine. The remaining patients had no serious adverse
reactions. The liver and kidney function, blood, urine and
electrocardiogram had no abnormal changes.
Discussion
In 1998, the International Prostatitis Collaborative
Network Conference confirmed the chronic prostatitis syndrome
classification standard and the NIH-CPSI scoring system presented
by the NIH in 1995 (3), which are
the current gold standard evaluation methods for the diagnosis and
treatment of chronic prostatitis.
Chronic prostatitis (CP)/CPPS comprises a group of
pelvic pain symptoms and voiding syndromes which are difficult to
define and cause anxiety (19).
The potential factors which may cause prostate congestion, such as
frequent sexual intercourse, masturbation, alcohol, spicy food,
cold and extended pressure to the perineum, possibly induce CPPS or
exacerbate the symptoms. However the exact etiology and
pathogenesis of CPPS are extremely complex, including urine reflux
(chemical prostatitis), autonomic dysfunction, immune-related
disorders, bacterial infection and other factors (20–23).
Treatments also vary greatly, particularly empirical clinical
therapies, and in certain patients are not effective (24). Treatments using α receptor
blockers, antibiotics, plant preparations, anti-inflammatory drugs
and antidepressants are commonly used, but have no definite effect.
Certain studies have reported that treatment with α receptor
blockers significantly mitigated the difficult to treat symptoms
which cause damage to the lower urinary tract, but had no clear
effects on pelvic pain and other symptoms. In the cases where α
blockers or antibiotic treatments were ineffective, i.e. refractory
CP/CPPS, a single drug therapy was unable to produce a satisfactory
curative effect, even if administered for an adequate period
(24). It has been suggested that,
even for newly diagnosed cases, α receptor blockers may have no
positive effect. For refractory CP/CPPS, orally administered α
receptor blockers or antibiotics have been reported to have similar
effects to a placebo (24,25). Terasaki et al proposed the
intrapelvic venous congestion (IVC) etiology of prostate pain and
designated it IVCS (26).
Therefore, the treatment of this disease remains
controversial. The most feasible treatment scheme is: i) direct
relief of pain symptoms; ii) diagnostic follow-up; and iii) pilot
etiological therapy (27).
In traditional Chinese medicine, this condition
belongs to the categories of muddy semen, consumptive micturition
disorders, lumbago due to deficiency of the kidney and other
fields. Long-term disease often leads to deficiency of the kidney
and difficulty in recovering. Anatomically, the prostate is located
at an interchange position of Ren, Du and Chong and is the center
of Qi and blood circulation. Prostatitic swelling, nodule formation
and fibrosis cause blockage of the meridian or even stagnation, as
observed from the principle of veins and arteries and causes
feelings of discomfort such as swelling and pain.
With regard to the pathological mechanism, ‘blood
stasis’ is the basic pathogenesis (28), mainly caused by phlegm, heat and
blood. According to the therapeutic concept of ‘fluency is the
basis’ in traditional Chinese medicine, among the patients who had
experienced no clear effects following long-term treatment, single
finger manipulation was able to apply pressure to soften the
blockage, eliminate the turbidity and cause the sediment to be
secreted. Clearing the gland may accelerate the removal of
pathogenic microorganisms and toxins, comparable to a debridement
and drainage effect, promoting the abrogation of inflammation,
improving gland duct drainage, reducing sympathetic excitability,
relieving urethral smooth muscle resistance and ensuring the
prostate catheter drainage is unobstructed, thereby eliminating
aches and swellings due to the blockage and the multifactoral
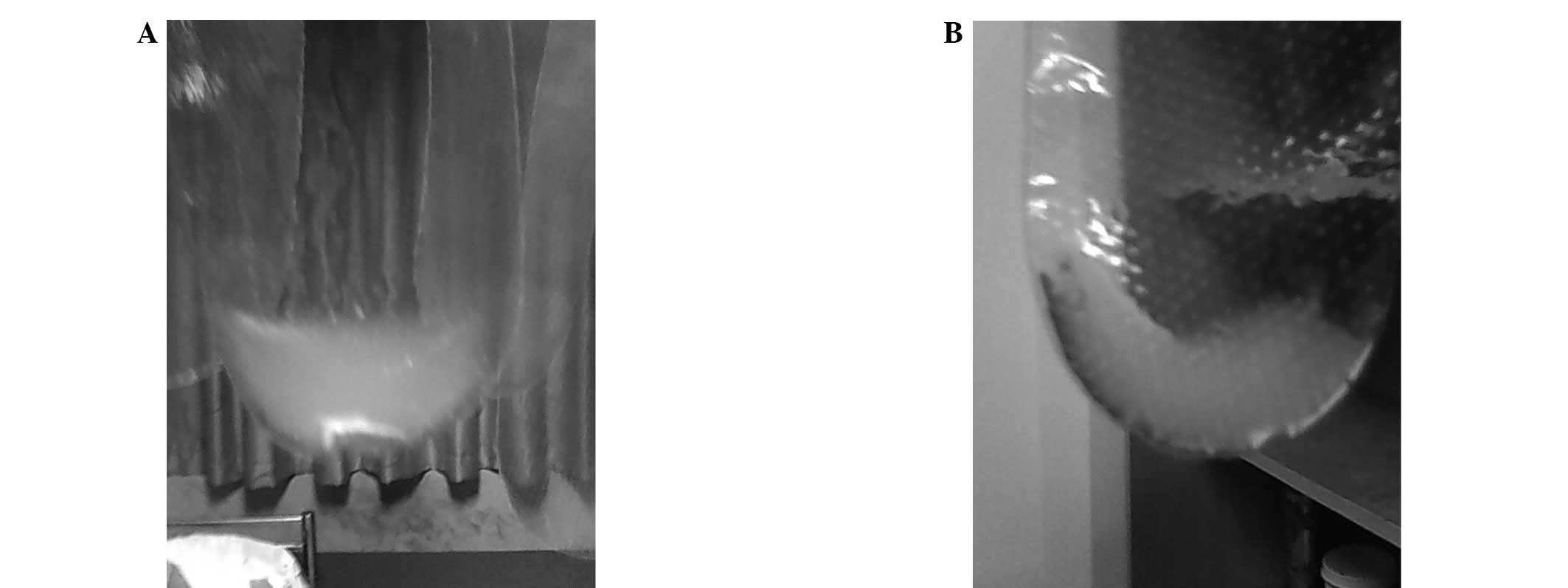
suffering caused by inflammatory lesions. Following the prostatic
massage procedure, the majority of patients discharged a large
amount of sediment, turbid fluid, coagulation and blood, with
yellowish, green, gray and rusty colors (Fig. 1).
Certain patients felt relaxed and their symptoms
immediately disappeared. The discharge was to a certain degree like
thick pus or nasal mucus, with a jelly-like fluid containing a
variety of suspended foreign substances. These substances were
routinely of unknown composition and were difficult to identify.
Finally, when all the prostate nodules had been cleared, the
glandular tubes were immediately unobstructed and the sediment was
discharged, inflammation disappeared and the discharged prostate
fluid was clear, similar in appearance to the alcohol (Fig. 2). It appeared to be light blue in
the glass dish. There was no clear discomfort. The symptoms,
including perineal pain, lower abdominal pain, waist and rib
soreness, headaches, dizziness, wet scrotum, increased dreams and
dysphoria, were reduced significantly or even disappeared following
the massage, while mental status and sexual dysfunction also
improved significantly. However, symptoms may recur if the patients
develop an unhealthy lifestyle. Therefore healthy living and
working behavior should be enforced, and repeated, continuous and
regular manipulation should be maintained to eradicate the disease.
Practical observations suggest that CPPS is usually repeated focal
inflammation rather than prostatitis affecting the whole prostate,
where the prostate gland is partially mechanically obstructed and
pressing on the prostatic stroma or prostate surrounding area.
Therefore, the symptoms and prostate palpation findings of the
patients are changeable, and are correlated with life and work
factors.
The results showed that, following each treatment
period, the NIH-CPSI scores for urinary pain and discomfort
symptoms and quality of life in the two groups were improved
significantly (P<0.01), indicating that the prostate massage
improves the clinical symptoms of CPPS. When comparing the EPS WBC
count scores of the IIIA group before and after treatment, the
changes following the 2nd course were not clear, while the scores
following the 1st and the last course were reduced.
In the present study, the total effective rate in
the 721 cases following 3 courses of treatment was 72.1% and the
average obvious effective rate was 16.1%, giving a total effective
rate of 88.2%, which was a satisfactory effect. No serious adverse
reactions occurred in the course of the treatment. During
treatment, it is recommended that attention is paid to diet,
optimistic spirit, moderate work with rest, proper exercise and
sweating, early sleep and a regular sex life (avoiding congestion
and stagnation), which are likely to contribute to the
rehabilitation from this disease.
References
|
1.
|
Roberts RO, Lieber MM, Rhodes T, Girman
CJ, Bostwick DG and Jacobsen SJ: Prevalence of a physician-assigned
diagnosis of prostatitis: the Olmsted County Study of Urinary
Symptoms and Health Status Among Men. Urology. 51:578–584. 1998.
View Article : Google Scholar : PubMed/NCBI
|
|
2.
|
Shoskes DA: Use of antibiotics in chronic
prostatitis syndromes. Can J Urol. 8(Suppl 1): 24–28. 2001.
|
|
3.
|
Na YQ and Sun G: Index Manual of Chinese
Urinary Surgery Disease Diagnosis. People’s Medical Publishing
House; Beijing: pp. 108–109. 2009, (In Chinese).
|
|
4.
|
Nickel JC, Nyberg LM and Hennenfent M:
Research guidelines for chronic prostatitis: consensus report from
the first National Institutes of Health International Prostatis
Collaborative Network. Urology. 54:229–233. 1999. View Article : Google Scholar
|
|
5.
|
Nickel JC, Zadeikis N, Spivey M, et al:
Clinical significance of antimicrobial therapy in chronic
prostatitis associated with non-traditional uropathogens. J Urol.
173:s302005.
|
|
6.
|
Galley HF, Nelson SJ, Dubbels AM and
Webster NR: Effect of ciprofloxacin on the accumulation of
interleukin-6, interleukin-8, and nitrite from a human endothelial
cell model of sepsis. Crit Care Med. 25:1392–1395. 1997. View Article : Google Scholar : PubMed/NCBI
|
|
7.
|
Hochreiter WW, Nadler RB, Koch AE, et al:
Diagnostic value of serial cytokine changes in expressed prostatic
secretions. J Urol. 163(Suppl 4): 242000.
|
|
8.
|
Suaudeau C, Chait A, Cimetiere C and de
Beaurepaire R: Analgesic effects of antibiotics in rats. Pharmacol
Biochem Behav. 46:361–364. 1993. View Article : Google Scholar : PubMed/NCBI
|
|
9.
|
Nickel JC, Downey J, Johnston B and Clark
J; Canadian Prostatitis Research Group: Predictors of patient
response to antibiotic therapy for the chronic prostatitis/chronic
pelvic pain syndrome: a prospective multicenter clinical trial. J
Urol. 165:1593–1544. 2001. View Article : Google Scholar
|
|
10.
|
Xu M and Zhang YK: The effect of
antibacterial agents in treatment of chronic nonbacterial
prostatitis. Journal of Clinical Urology. 15:195–196. 2000.(In
Chinese).
|
|
11.
|
Na YQ and Li M: Advanced Course of Urinary
Surgery. People’s Military Medical Press; Beijing: pp. 2932011
|
|
12.
|
Sun ZM and Bao YZ: Improvements of
prostate massage. Chinese Journal of Andrology. 22:25–26. 2008.(In
Chinese).
|
|
13.
|
Bian YQ: One finger manipulation and
massage. Massage Recovery Med. 1:8–10. 2010.(In Chinese).
|
|
14.
|
Kang YX: The research of one finger
manipulation. Lishizhen Medicine and Materia Medica Research.
18:2999–3001. 2007.(In Chinese).
|
|
15.
|
Fu WT: From the summary of experience to
the clinical application. Massage Guide. 21:34–35. 2005.(In
Chinese).
|
|
16.
|
Zhang JH, Sun AD and Zhang ZC: Massage
Strength Skills. 1st edition. Anhui Science and Technology
Publishing House; Hefei: pp. 12–18. 1992, (In Chinese).
|
|
17.
|
Ding JF: Massage Experience. 1st Edition.
Henan Science and Technology Publishing House; Zhengzhou: pp.
269–280. pp. 328–331. pp. 358pp. 388–390. 1994, (In Chinese).
|
|
18.
|
Herb Doctors Qualification Specialist
Committee: Herb Doctor Quality and Skill Examination Guide. Chinese
Herb Medicine Publisher; Beijing: pp. 62–67. 2010, (In
Chinese).
|
|
19.
|
Litwin MS, McNaughton-Collins M, Fowler FJ
Jr, et al Chronic Prostatitis Collaborative Research Network: The
national institutes of health chronic prostatitis symptom index:
development and validation of a new outcome measure. J Urol.
162:369–375. 1999. View Article : Google Scholar
|
|
20.
|
Nadler RB, Koch AE, Calhoun EA, et al:
IL-1beta and TNF-alpha in prostatic secretions are indicators in
the evaluation of men with chronic prostatitis. J Urol.
164:214–218. 2000. View Article : Google Scholar : PubMed/NCBI
|
|
21.
|
He LY: Symptoms of prostatitis. Chinese
Journal of Urology. 21:697–699. 2000.(In Chinese).
|
|
22.
|
Guo YL and Li HJ: Prostatitis. People’s
Military Medical Press; Beijing: pp. 81–122. 2007, (In
Chinese).
|
|
23.
|
Sun ZM and Ding CF: Clinical research of
Xiaoyutonglie decoction on treating chronic pelvic pain syndrome.
Zhejiang Journal of Integrated Traditional Chinese and Western
Medicine. 16:7–9. 2006.(In Chinese).
|
|
24.
|
Krieger JN and Riley DE: Bacteria in the
chronic prostatitis-chronic pelvic pain syndrome: molecular
approaches to critical research questions. J Urol. 167:2574–2583.
2002. View Article : Google Scholar : PubMed/NCBI
|
|
25.
|
Nickel JC, Downey J, Ardern D, Clark J and
Nickel K: Failure of a monotherapy strategy for difficult chronic
prostatitis/chronic pelvic pain syndrome. J Urol. 172:551–554.
2004. View Article : Google Scholar : PubMed/NCBI
|
|
26.
|
Terasaki T, Watanabe H, Saitoh M, Uchida
M, Okamura S and Shimizu K: Magnetic resonance angiography in
prostatodynia. Eur Urol. 27:280–285. 1995.PubMed/NCBI
|
|
27.
|
Zermann DH, Ishigooka M, Doggweiler-Wiygul
R, Schubert J and Schmidt RA: The male chronic pelvic pain
syndrome. World J Urol. 19:173–179. 2001. View Article : Google Scholar : PubMed/NCBI
|
|
28.
|
Sun ZM and Bao YZ: Recognition and
thoughts about CP. Zhejiang Journal of Integrated Traditional
Chinese and Western Medicine. 2:26–27. 2005.(In Chinese).
|