Introduction
Ovarian epithelial carcinoma is one of the most
common gynecological cancers (1).
Once clinical symptoms are apparent, patients have developed mid-
to late-stage ovarian cancer, at which point aggressive treatments
may yield more favorable results than conservative ones. Surgery
remains the primary treatment for stage III ovarian cancer and
allows removal of gross disease. Following surgery, intravenous
(IV) or intraperitoneal (IP) chemotherapy extends the survival time
of patients and is associated with superior results for recurrent
ovarian cancer relative to other treatment modes. In addition to IV
and IP chemotherapy, other treatment regimens, including oral
chemotherapy, hormones and gonadotrophin-releasing hormone
antagonists, exert certain positive effects (2). More recently, biologic therapy for
ovarian cancer has become an area of focus and may be attempted in
clinical treatment (3).
Patients treated with IP paclitaxel/cisplatin
chemotherapy have been observed to live significantly longer lives
than those treated with IV paclitaxel/cisplatin chemotherapy, which
indicates that IP administration is the optimal route for ovarian
cancer treatment (4).
Paclitaxel/carboplatin chemotherapy is more suitable for patients
with a poor performance status than for patients with a good
performance status. However, the outcome of chemotherapy for
elderly patients with advanced disease and a poor performance
status has not been reported. Chemotherapy is also contraindicated
for patients with Eastern Cooperative Oncology Group (ECOG)
performance statuses of 3 or 4.
The combination of bevacizumab with
carboplatin/paclitaxel is associated with significantly longer
disease-free survival than carboplatin/paclitaxel alone. However,
no significant difference has been observed between bevacizumab
plus carboplatin/paclitaxel and carboplatin/paclitaxel in terms of
overall survival rate (5). Thus,
bevacizumab does not appear to confer any survival advantage, and
the National Comprehensive Cancer Network panel does not recommend
its use. Bevacizumab may be used as a maintenance drug subsequent
to chemotherapy; however, clinical studies have indicated that it
results in numerous many side effects. Therefore, clinicians should
consider the advantages and disadvantages of bevacizumab prior to
prescribing the drug to patients.
Case report
An 82-year-old female, who presented with abdominal
distension, abdominal pain, a slight sense of fullness subsequent
to eating and increased urination frequency every day for two
months was diagnosed with ovarian cancer in May 2004. The attending
gynecologist performed a hysterectomy, a bilateral
salpingo-oophorectomy and an omentectomy, and removed all evidence
of gross disease. Diffuse metastatic involvement of the omentum and
diaphragmatic metastasis were observed. Pathological assessment
showed stage IIIC epithelial ovarian cancer. From June 2004 to
January 2005, the patient received six cycles of conventional
treatment in combination with IV paclitaxel (Bristol-Myers Squibb
Co., Princeton, New Jersey, USA) and cisplatin (Qilu Pharmaceutical
Co., Ltd, Jinan, China). Following surgery and chemotherapy, the
patient’s cancer antigen-125 (CA-125) levels declined to 7.3 U/ml.
The patient’s abdominal distension and pain, and the sense of
fullness subsequent to eating were alleviated, while the urination
frequency was reduced. Furthermore, the patient’s appetite improved
significantly.
In 2007, the patient developed abdominal distension
and gradually deteriorated, and was admitted to The First
Affiliated Hospital, The Fourth Military Medical University of the
PLA (Xi’an, China) on May 8, 2007. Physical examination and
laboratory analyses revealed dry and moist rales in both lungs,
shifting dullness in the abdomen and a CA-125 level of 1,030 U/ml.
Computed tomography (CT) scans (Model 5124069-5; GE Healthcare Co.
Milwaukee, WI, USA) revealed an infection in the right upper lobe
of the right lung, left-sided pleural effusion, sclerotic lesions
in the apex of the right lung and the lower lobe of the left lung
and a little ascites. Hypodense lesions in the right lobe of the
liver and spleen and enlarged retroperitoneal lymph nodes were
considered metastatic. Pelvic CT scans showed postoperative
agenesis of the uterus and ovaries, as well as soft tissue shadows
at the junction between the rectum and sigmoid colon, and in front
of the intestine. The condition of the patient gradually
deteriorated; she was immobile, with an ECOG performance status of
4 and further chemotherapy was not considered. Instead, doses of 50
mg etoposide (Jiangsu Hengrui Medicine Co., Ltd. Lianyungang,
China) and 40 mg megestrol acetate (Bristol-Myers Squibb Co.) were
administered orally once daily. On May 12, 3.6 mg goserelin acetate
(AstraZeneca UK Limited, Cheshire, UK) implant was injected
subcutaneously.
The patient’s condition continued to decline with
the development of severe abdominal distension, breathing
difficulties and an inability to eat on 15 May. Ultrasound (iU33;
Philips Ultrasound, Bothell, WA, USA) showed massive ascites and
left pleural effusion, and the patient appeared to be in a critical
condition. Treatment with etoposide and megestrol acetate was
discontinued and parenteral nutrition was provided. The patient
underwent thoracentesis and abdominocentesis, during which 1,000 ml
clear yellow ascitic fluid was extracted, and 300 mg carboplatin
(Qilu Pharmaceutical Co., Ltd) was injected intraperitoneally into
the abdominal cavity on May 19. The patient’s condition did not
improve, and 1,500 ml clear yellow ascite fluid was removed on May
21. The condition of the patient remained poor until May 27, at
which time, an IV infusion of 200 mg bevacizumab
(Avastin®, Genentech, Inc., South San Francisco, CA,
USA) was administered. Written informed consent was obtained from
the patient. Thoracentesis was performed again when the patient
complained of breathing difficulties, and 1,500 ml clear yellow
pleural fluid was extracted on May 31.
From June 1, 2007, a gradual improvement was
observed in the patient’s condition. Dyspnea, abdominal distension
and abdominal pain were significantly reduced, the patient had a
significant improvement in appetite and urine and feces had
returned to normal. The patient was upright and mobile. Bevacizumab
was administered by IV infusion at a dosage of 400 mg every two
weeks from June 9, followed by a dosage of 200 mg every two weeks
from the end of November. On June 10, 2007, ultrasound showed that
the massive left-side pleural effusion had disappeared. On June 29,
2007, a CT scan showed that the ascites, and the liver, spleen and
pelvic lesions had disappeared. The patient’s CA-125 level was
31.17 U/ml on July 3, 2007, and 300 mg IP carboplatin was
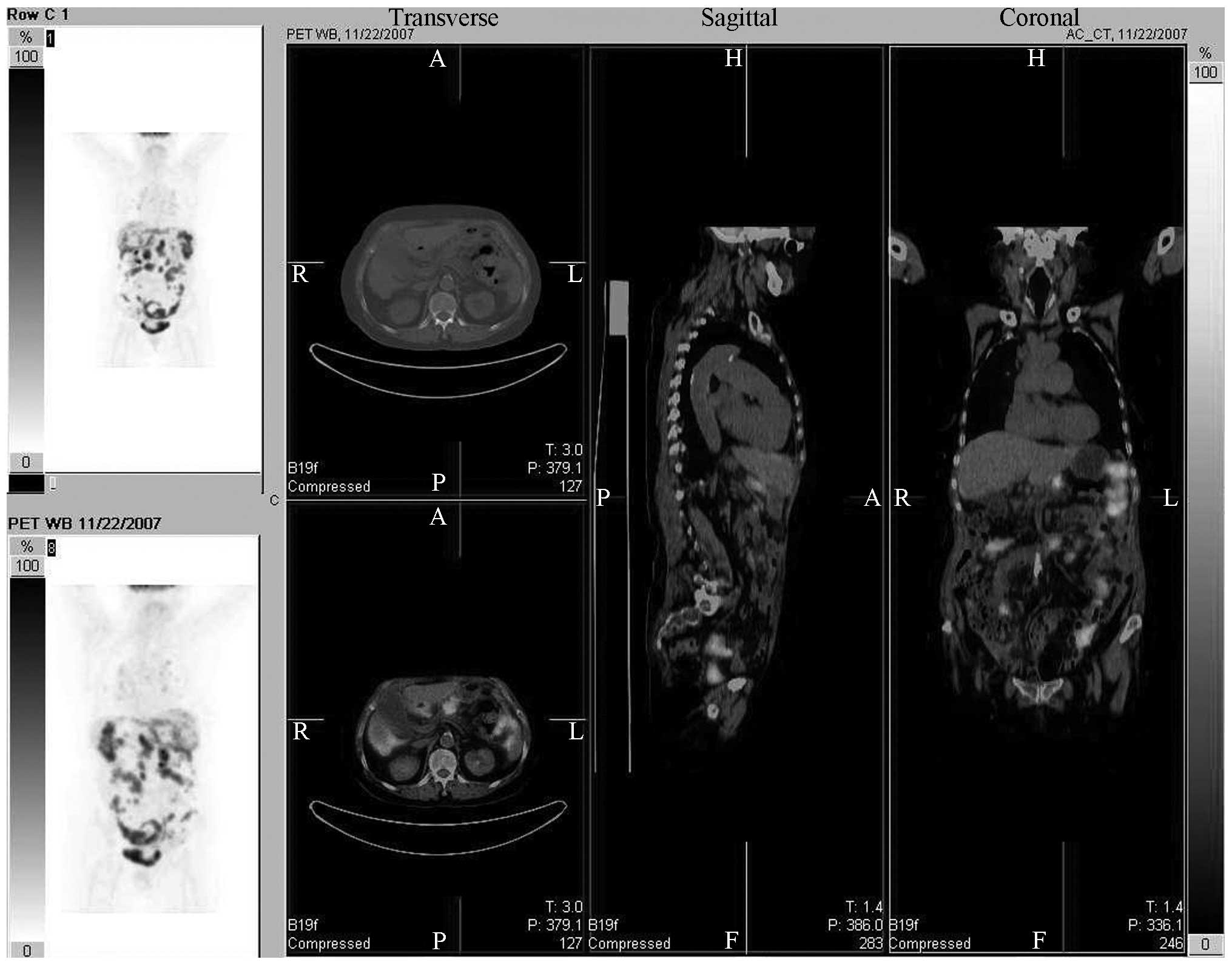
administered on November 4, 2007. Positron emission tomography-CT
scans (Biograph™ TruePoint™ PET•CT; Siemens
Medical Solutions USA, Inc., Knoxville, TN, USA) showed widespread
metastases in the patient’s body on November 22, 2007 (Fig. 1). IP carboplatin was administered
several times. The patient exhibited disease-free survival until
July 2009 when disease progression was observed, followed by
disease recurrence in August 2009. The patient died of multiple
organ failure in September 2009.
Discussion
Following ovarian cancer surgery, the patient
exhibited disease-free survival for several years until the cancer
recurred and a CT scan revealed widespread intra-abdominal
metastases. The patient had concomitant diseases and developed
massive ascites and pleural effusion. Treatment included IP
chemotherapy and oral etoposide. These treatments were ineffective
and the condition of the patient deteriorated further. To the best
of our knowledge, no similar clinical case has been reported, and
palliative care remains the recommended treatment for such cases
(2,6).
Ascites disappear rapidly with bevacizumab treatment
(7–9). In the present case study, massive
effusion in the thoracic and abdominal cavity disappeared within a
short time-frame subsequent to bevacizumab administration, thereby
providing a basis for the next treatment. Bevacizumab was
administered by IV infusion every two weeks and IP carboplatin was
administered intermittently until the death of the patient. The
patient was likely to have died earlier if pleural effusion had not
been rapidly controlled; by contrast, the patient experienced
disease-free survival for 25 months and treatment was associated
with favorable results. Thus, bevacizumab may be concluded to play
a key role in disease control.
Bevacizumab in combination with paclitaxel and
carboplatin improves the progression-free survival of patients with
ovarian cancer; however, it does not increase their overall
survival time. Furthermore, the use of the drug in maintenance
therapy subsequent to chemotherapy does not appear to increase
overall survival (5). Other
studies have indicated that bevacizumab does not increase overall
survival in any cancer type, despite its ability to prolong
progression-free survival (10–12).
Thus, it was concluded that no overall survival benefit may be
derived from bevacizumab. However, chemotherapy is contraindicated
for patients with massive ascites, massive pleural effusions,
breathing difficulties and poor performance status. Continuing
chemotherapy in such cases may aggravate the patient’s condition
and possibly lead to death. In the present case study, the
patient’s ascites and pleural effusion disappeared following
administration of bevacizumab, and a significant improvement in
performance status was observed. IP chemotherapy combined with
bevacizumab also led to extended disease-free survival. Thus, the
role of bevacizumab in prolonging survival in patients with ovarian
cancer warrants further study. The pulmonary artery systolic
pressure of the patient rose continually until her death; such
increases in arterial pressure may be associated with the use of
bevacizumab.
Chemotherapy regimens for platinum-sensitive
relapsed ovarian cancer include monotherapy with agents such as
cisplatin and carboplatin, as well as combination therapies,
including paclitaxel plus carboplatin, carboplatin plus gemcitabine
and cisplatin plus gemcitabine (13–16).
Other regimens may also be effective, including monotherapy with
paclitaxel, docetaxel, cyclophosphamide, ifosfamide, oxaliplatin,
melphalan, irinotecan, capecitabine, pemetrexed and etoposide, and
hormone therapy with tamoxifen, anastrozole, letrozole, leuprorelin
acetate and megestrol acetate (16–18).
In the present case study, the patient received goserelin acetate
implant, etoposide and megestrol acetate; however, these treatments
were not efficacious. IP carboplatin was beneficial until the
patient was no longer able to tolerate the treatment. Carboplatin
was prescribed as it has a lower impact on the kidney than other
drugs. This treatment strategy had a favorable outcome for the
patient.
Bevacizumab rapidly eliminated the massive ascites
and pleural effusion and achieved an effect that was not able to be
attained with other treatments. Bevacizumab appears to be an
effective means of controlling late-stage relapse and refractory
ovarian cancer. Future clinical studies are required to confirm the
effectiveness of the drug.
References
|
1
|
Jemal A, Siegel R, Xu J and Ward E: Cancer
statistics, 2010. CA Cancer J Clin. 60:277–300. 2010. View Article : Google Scholar
|
|
2
|
Morgan RJ Jr, Alvarez RD, Armstrong DK, et
al: Epithelial Ovarian Cancer Clinical Practice Guidelines in
Oncology. J Natl Compr Canc Netw. 9:82–113. 2011.
|
|
3
|
Willmott LJ and Fruehauf JP: Targeted
therapy in ovarian cancer. J Oncol. 2010:7404722010. View Article : Google Scholar : PubMed/NCBI
|
|
4
|
Armstrong DK, Bundy B, Wenzel L, et al;
Gynecologic Oncology Group. Intraperitoneal cisplatin and
paclitaxel in ovarian cancer. N Engl J Med. 354:34–43. 2006.
View Article : Google Scholar : PubMed/NCBI
|
|
5
|
Burger RA, Brady MF, Bookman MA, et al:
Phase III trial of bevacizumab (BEV) in the primary treatment of
advanced epithelial ovarian cancer (EOC), primary peritoneal cancer
(PPC), or fallopian tube cancer (FTC): a Gynecologic Oncology Group
study. J Clin Oncol (ASCO Meeting Abstracts). 28:LBA12010.
|
|
6
|
Barbera L, Elit L, Krzyzanowska M, Saskin
R and Bierman AS: End of life care for women with gynecologic
cancers. Gynecol Oncol. 118:196–201. 2010. View Article : Google Scholar : PubMed/NCBI
|
|
7
|
Numnum TM, Rocconi RP, Whitworth J and
Barnes MN: The use of bevacizumab to palliate symptomatic ascites
in patients with refractory ovarian carcinoma. Gynecol Oncol.
102:425–428. 2006. View Article : Google Scholar : PubMed/NCBI
|
|
8
|
Hamilton CA, Maxwell GL, Chernofsky MR,
Bernstein SA, Farley JH and Rose GS: Intraperitoneal bevacizumab
for the palliation of malignant ascites in refractory ovarian
cancer. Gynecol Oncol. 111:530–532. 2008. View Article : Google Scholar : PubMed/NCBI
|
|
9
|
Woopen H and Sehouli J: Current and future
options in the treatment of malignant ascites in ovarian cancer.
Anticancer Res. 29:3353–3359. 2009.PubMed/NCBI
|
|
10
|
Wright JD, Hagemann A, Rader JS, et al:
Bevacizumab combination therapy in recurrent, platinum-refractory,
epithelial ovarian carcinoma: a retrospective analysis. Cancer.
107:83–89. 2006. View Article : Google Scholar
|
|
11
|
Burger RA, Sill MW, Monk BJ, Greer BE and
Sorosky JI: Phase II trial of bevacizumab in persistent or
recurrent epithelial ovarian cancer or primary peritoneal cancer: a
Gynecologic Oncology Group study. J Clin Oncol. 25:5165–5171. 2007.
View Article : Google Scholar : PubMed/NCBI
|
|
12
|
Cannistra SA, Matulonis UA, Penson RT, et
al: Phase II study of bevacizumab in patients with
platinum-resistant ovarian cancer or peritoneal serous cancer. J
Clin Oncol. 25:5180–5186. 2007. View Article : Google Scholar
|
|
13
|
Strauss HG, Henze A, Teichmann A, et al:
Phase II trial of docetaxel and carboplatin in recurrent
platinum-sensitive ovarian, peritoneal and tubal cancer. Gynecol
Oncol. 104:612–616. 2007. View Article : Google Scholar : PubMed/NCBI
|
|
14
|
Pfisterer J, Plante M, Vergote I, et al;
AGO-OVAR; NCIC CTG; EORTC GCG. Gemcitabine plus carboplatin
compared with carboplatin in patients with platinum-sensitive
recurrent ovarian cancer: an intergroup trial of the AGO-OVAR, the
NCIC CTG, and the EORTC GCG. J Clin Oncol. 24:4699–4707. 2006.
View Article : Google Scholar : PubMed/NCBI
|
|
15
|
Pujade-Lauraine E, Wagner U,
Aavall-Lundqvist E, et al: Pegylated liposomal Doxorubicin and
Carboplatin compared with Paclitaxel and Carboplatin for patients
with platinum-sensitive ovarian cancer in late relapse. J Clin
Oncol. 28:3323–3329. 2010. View Article : Google Scholar : PubMed/NCBI
|
|
16
|
Rose PG, Blessing JA, Mayer AR and
Homesley HD: Prolonged oral etoposide as second- line therapy for
platinum- resistant and platinum-sensitive ovarian carcinoma: a
Gynecologic Oncology Group study. J Clin Oncol. 16:405–410.
1998.PubMed/NCBI
|
|
17
|
Emons G and Schally AV: The use of
luteinizing hormone releasing hormone agonists and antagonists in
gynecological cancers. Hum Reprod. 9:1364–1379. 1994.PubMed/NCBI
|
|
18
|
Wiernik PH, Greenwald ES, Ball H, Young JA
and Vogl S: High-dose megestrol acetate in the treatment of
patients with ovarian cancer who have undergone previous treatment:
Eastern Cooperative Oncology Group Study PD884. Am J Clin Oncol.
21:565–567. 1998. View Article : Google Scholar
|