Introduction
Compression, blunt or transection injuries caused by
continuous compression of the peripheral nerve axons damage the
normal structure of nerve axons (1).
During axonal recovery and regeneration, fibroblasts secrete large
amounts of collagen, resulting in the formation of perineural scars
(2). Scars tissue may form an
intraneural barrier, which hinders the regeneration of nerve axons
and may induce tissue adhesion, inhibiting the neural blood supply
and resulting in neural ischemia (3). The aim of the present study was to
determine a method to improve the prevention of perineural scarring
and scarring of surrounding tissues due to facial nerve injuries
following parotidectomy surgeries. This novel method may improve
postoperative nerve functional recovery.
Chitosan is a type of natural polymeric biological
polysaccharide with higher biodegradability and biocompatibility
compared with a number of other scar prevention materials
(including, human amniotic membrane and Seprafilm) (4,5);
chitosan can be automatically degraded into glucosamine in
vivo and absorbed by humans (6).
Additionally, its mechanical properties (including, tensile
strength and compressive strength) make chitosan an ideal
extracellular matrix material (7).
Hyaluronate is a vital component of the extracellular matrix, which
is widely expressed in animals (8).
Hyaluronate has previously been used in many in vivo studies
due to its availability, non-toxic biodegradability and because it
did not trigger immunological rejection (2,9). To the
best of our knowledge, there is currently no experimental study
that has investigated the perineural scar prevention of facial
nerves. The aim of the present study was to investigate the effect
of chitosan combined with hyaluronate on the formation of
perineural scars and nerve functional recovery in a model of facial
nerve injury.
Materials and methods
Animals and surgical methods
Experimental animals
A total of 40 adult (12 months old) New Zealand
white female rabbits (weight, 2.5–3.0 kg) were included in the
current study. The rabbits were supplied by the Laboratory Animal
Centre of Chinese PLA General Hospital (Beijing, China) and
maintained under controlled conditions: 1 atmosphere, 20–25°C, 12 h
light/dark cycle and humidity of 40–60%. The rabbits were given
access to food and water ad libitum. Rabbits were randomized
into four groups (n=10/group): A (chitosan), B (chitosan +
hyaluronate), C (hyaluronate) and D (control). Anesthesia
procedures, painless surgeries and euthanasia procedures were
approved by the ethics committee of the Chinese People's Liberation
Army General Hospital (Beijing, China). Rabbits were treated
according to the requirements of the local animal ethics
commission.
Preparation of chitosan conduit
The chitosan conduits (Beijing Yierkang
Bioengineering Development Center, Beijing, China) were disinfected
with 60Co (inner diameter, 1.8 mm; tube wall thickness,
0.05 mm) and immersed into normal saline for 10 min at room
temperature prior to surgery. The chitosan conduits were cut into
sections (length, 1 or 0.5 cm; circumference, 0.5 cm) and split
longitudinally. Chitosan conduits (1 cm length) were used to cover
upper and lower buccal branches of the facial nerve. Chitosan
conduits (length, 0.5 cm) were also used to cover cervical and
zygomatic branches of the facial nerve.
Surgical methods
Rabbits were anesthetized via intramuscular
injections (50 mg/kg ketamine + 5 mg/kg xylazine hydrochloride) and
immobilized in a lateral position with the right side of their
faces shaved. The buccal branch of the facial nerve was exposed by
a 4-cm-long incision between the tragus and the lower margin of the
mandible. The facial nerve trunk, upper and lower buccal branches
and cervical and zygomatic branches were fully exposed and
separated from the basement membrane. Complete resection of the
superficial lobe and major resection of the deep lobe of the
parotid gland were conducted and the residual tissue was sutured
using 4-0 sutures.
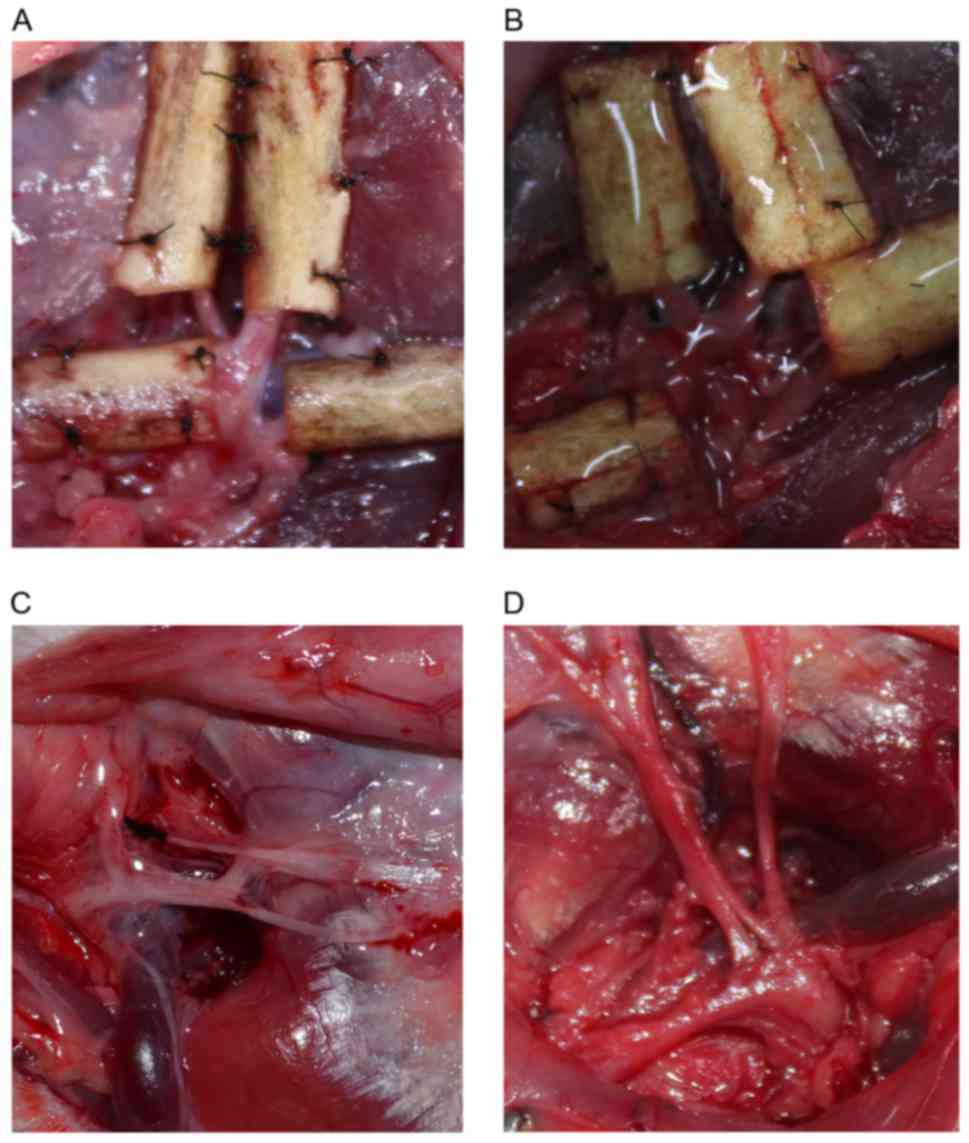
In Group A, the facial nerves were covered by
chitosan conduits (Fig. 1). In Group
B, the nerves were covered by chitosan conduits and then evenly
coated with hyaluronate on the surface (0.2 ml; 15 mg/ml; Shanghai
Medical Instruments Co., Ltd., Shanghai, China). In Group C, the
surfaces of the nerves were evenly coated with 0.2 ml hyaluronate.
In Group D, the nerves were exposed and did not receive
treatments.
Following the establishment of the model, the tissue
was sutured and a rubber drainage strip was indwelled. The wound
was disinfected for 3 days using iodophor (once/day) and penicillin
was injected intramuscularly for 3 days (0.06 g/kg, twice/day). The
drainage strips were indwelled for 2–3 days until no exudation was
observed. Rabbits were euthanized intravenously with pentobarbital
sodium at the dose of 100 mg/kg 12 weeks after surgery.
Postoperative examination
Vibrissae motion evaluation
At 24 h and 2, 4, 6, 8, 10 and 12 weeks after
surgery, the vibrissae motion on the surgical side was compared
with that of the contralateral side. Motion was scored using the
following criteria: 0, no motion with vibrissae hanging down; 1,
minor movement; 2, inadequate movement; 3, adequate movement, but
weaker compared the contralateral side; 4, normal movement,
identical to the contralateral side (10,11).
Scar adhesion analysis
At 4 and 12 weeks after surgery, the incision was
open again under anesthesia. According to the classification
standard by Petersen, the force of separating the skin from muscles
and fascia from nerves was graded as follows: i) Separation was not
required or only blunt dissection was required; ii) hard blunt
separation was required; and iii) sharp separation was required
(10).
Electrophysiological evaluation
Under general anesthesia at 4 and 12 weeks after
surgery, the former incision site was opened and the facial nerve
trunk and branches were exposed. Two stimulating electrodes were
placed on the trunk, while the recording electrode was inserted
into the orbicularis oris. The amplitude and latency of the
orbicularis oris, and the distance between two electrodes was
measured. The nerve conduction velocity (NCV) of the branches was
calculated using the following formula: v = (d1 - d2)/(t1 - t2),
where d1 - d2 was the distance between the two electrodes and t1 -
t2 was the spike latency of the orbicularis oris excited by two
stimulating electrodes.
Histological staining
Following the electrophysiological examinations, the
chitosan conduits or nerve samples were removed from 5 rabbits for
each time point (postoperative weeks 4 and 12), the conduits were
then divided into ~4 sections and fixed in paraffin or epoxy.
i) Extraneural scar examination
One of the middle sections was fixed in 10%
formaldehyde for 24 h at 4°C, embedded in paraffin, sliced into
5-µm-thick sections and subjected to Masson staining for 24 h at
4°C to assess the status of extraneural scar hyperplasia and the
amount of type I and III collagen fibers. The sections were
observed using a light microscopy with a magnification of ×200.
Four visual fields were observed to measure the average collagen
thickness of extraneural scars.
The other middle section was fixed directly at 4°C
in 2.5% glutaric acid for 24 h and 1% osmic acid for 2 h, sliced
into semi-thin (2-µm-thick) sections, dehydrated in an ascending
series of acetone and embedded in epoxy resin at 4°C for 10 min.
Harris hematoxylin staining was conducted at 4°C for 10 min and
tissues were observed under a transmission electron microscopy
(TEM) at a magnification of ×3,000. The average thickness of
collagen in the epineurium and conduit were measured in six optical
fields per section.
ii) Axon morphometric analysis
The epoxy-embedded sections were sliced into
semi-thin (2-µm-thick) sections and the number of myelinated fibers
was measured under an inverted microscope in six random optical
fields per section. The sections were also sliced into ultrathin
(50-nm-thick) sections. The thickness of the myelin sheath, and the
number and diameter of myelinated fibers were observed in six
optical fields per section.
Conduit analysis
At 12 weeks after surgery, implanted chitosan
conduits were removed, fixed in 2.5% glutaric acid for 24 h at 4°C,
allowed to dry out and adhered to a metal plate with conductive
tapes. Next, the samples were introduced into the chamber of the
sputter coater and coated with a very thin film of gold. The
surface and cross section of the conduits were investigated prior
to and 12 weeks after implantation under a scanning electron
microscope (SEM) at a magnification of ×500.
Statistical analysis
Statistical analysis was performed using SPSS 19.0
(IBM Corp., Armonk, NY, USA). Data are presented as the mean ±
standard deviation. Analysis of variance was used to compare
differences among groups followed by the Student-Newman-Keuls test.
P<0.05 was considered to indicate a statistically significant
difference.
Results
Vibrissae motion is similar among the
four groups
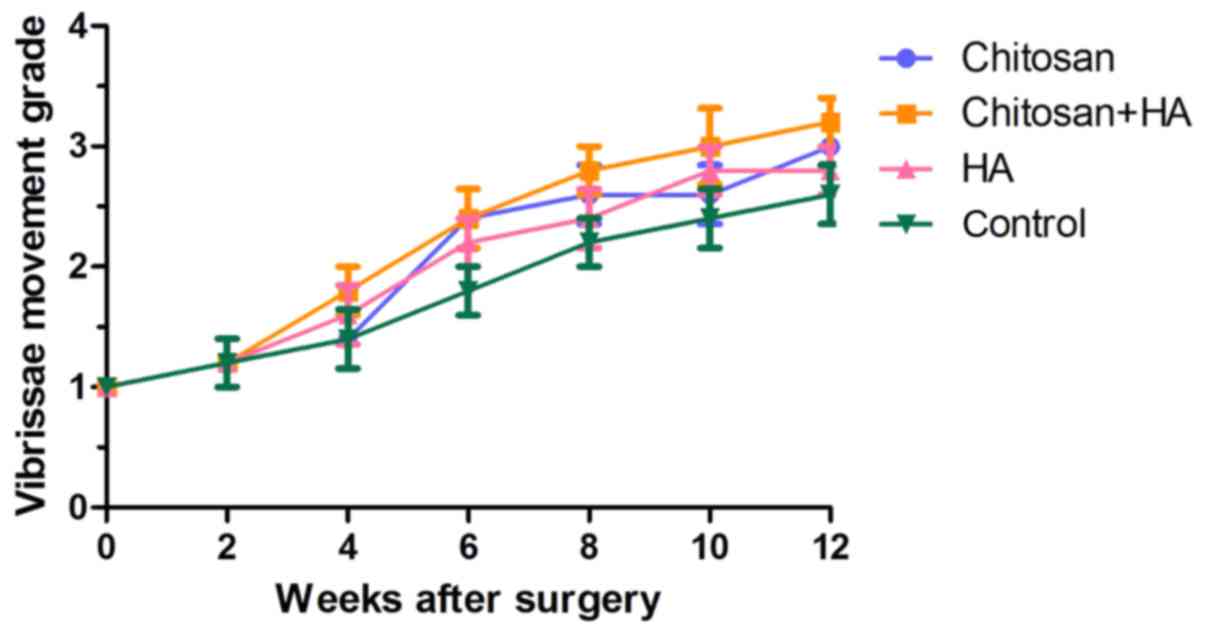
No significant differences in vibrissae motion were
identified between 24 h and 2 weeks post-surgery in any group
(Fig. 2). At week 4, scores were
higher in Groups B and C compared with Groups A and D, but no
statistical differences were identified. From week 6, vibrissae
motion was markedly improved in all groups. Group D had the lowest
scores, however no significant differences were identified.
Scarring is greatest in control
rabbits 12 weeks after surgery
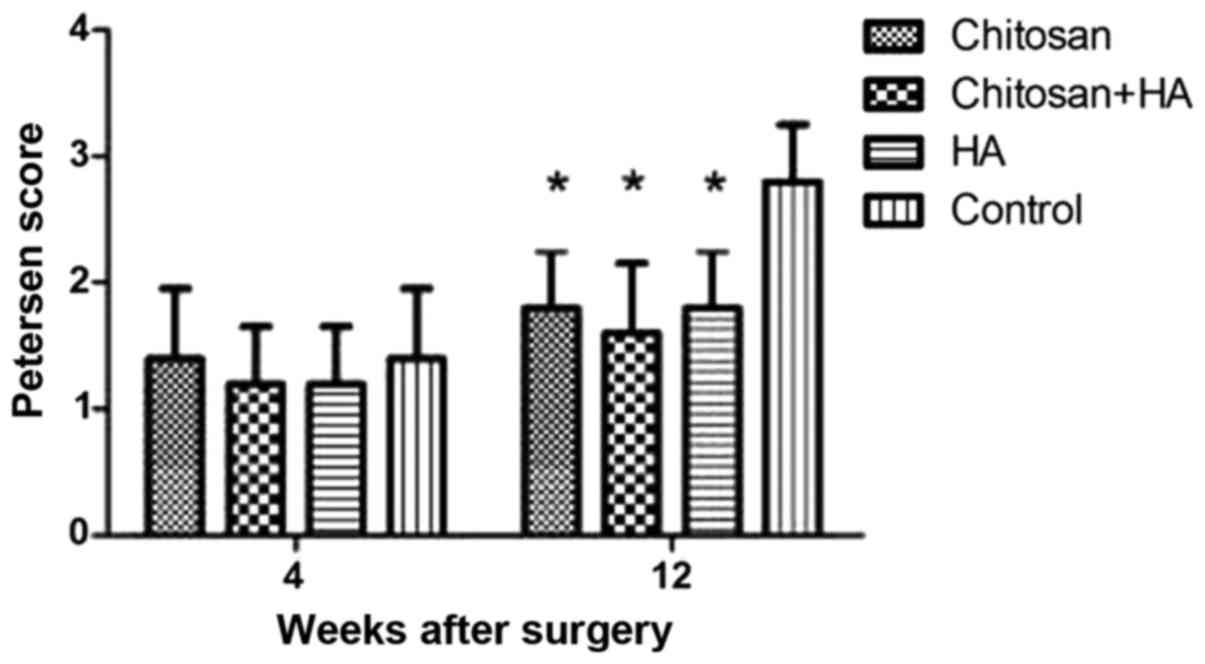
At week 4, the nerves had only mildly adhered to the
surrounding tissue in all groups and were easy to separate
(Fig. 3). No significant differences
were identified between the groups at week 4, although Groups B and
C had the lowest scores according to the Petersen classification
system. At week 12 after surgery, Group D adhered to the
surrounding tissue significantly more compared with the other
groups (P<0.05). No significant differences were identified
among the experimental groups.
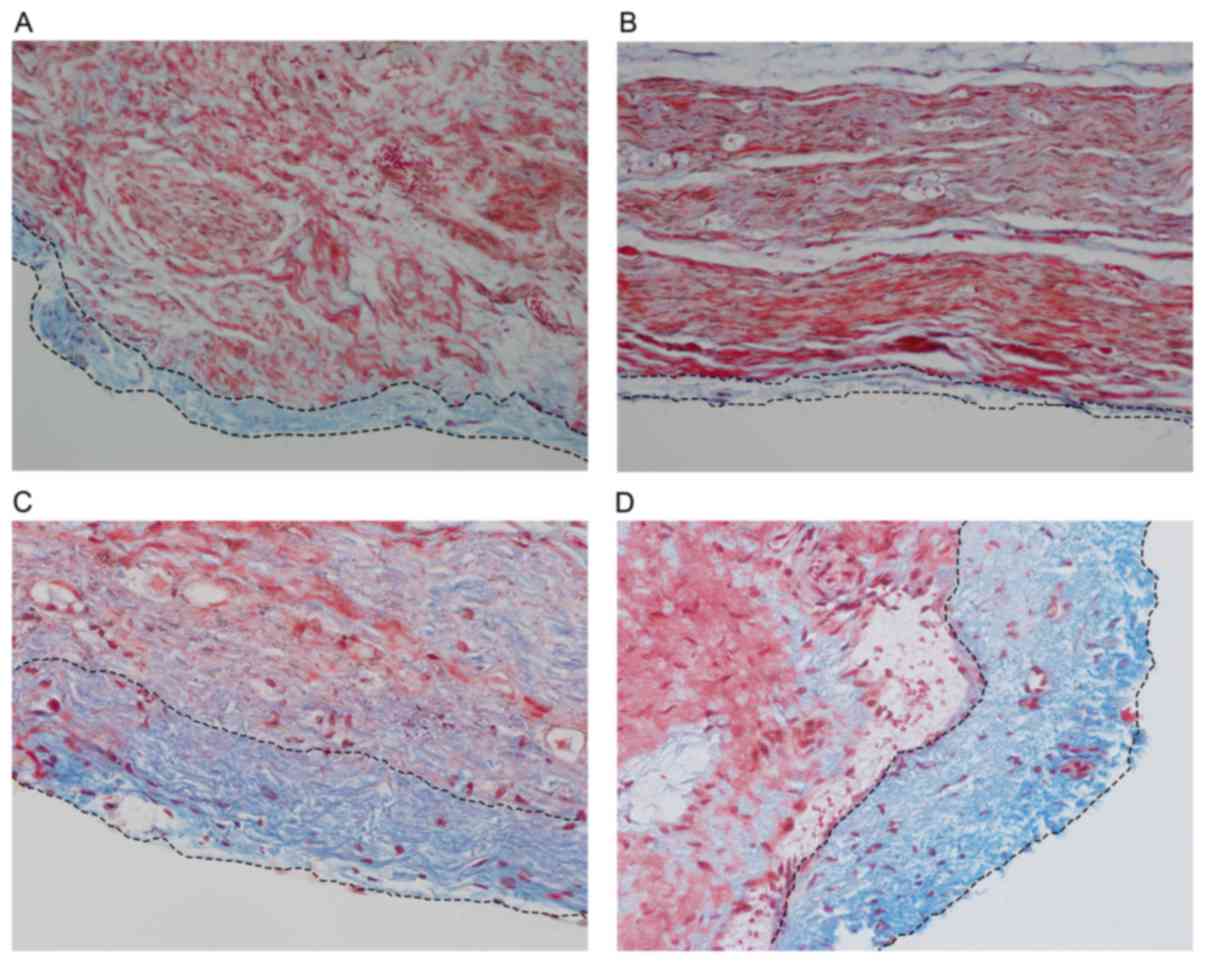
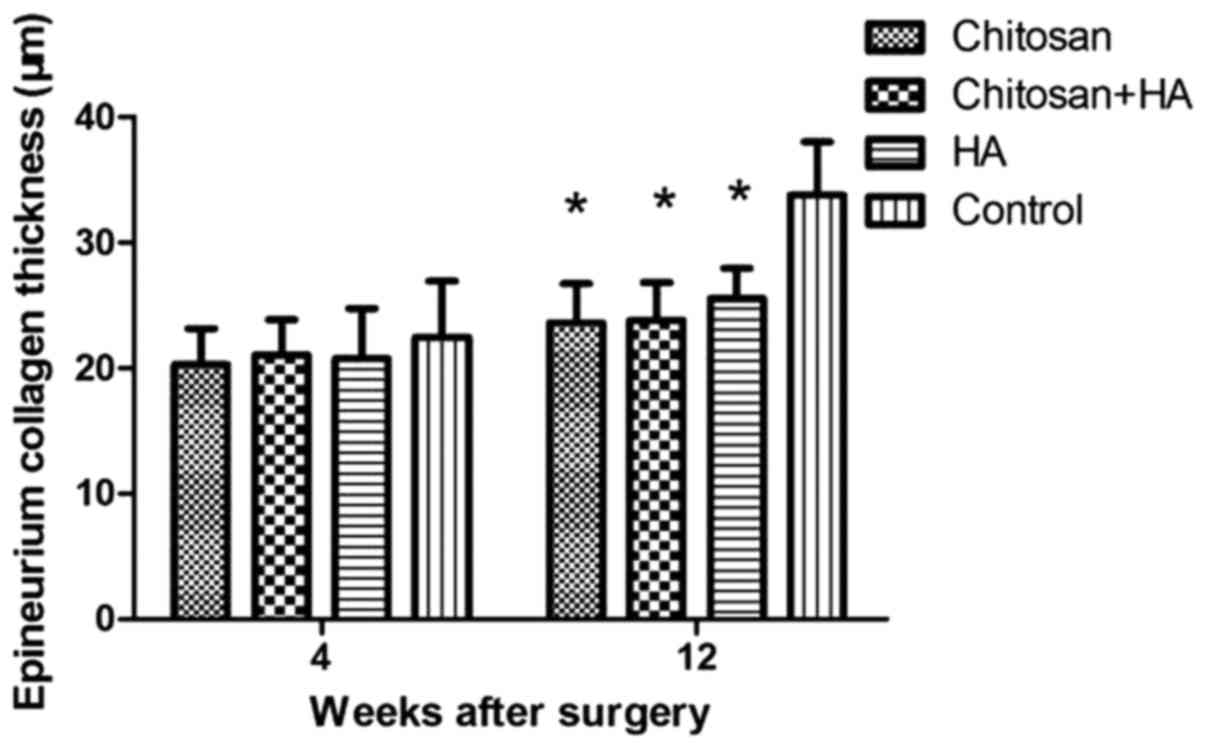
Epineuria are thicker in control
rabbits 12 weeks after surgery
At week 4, the epineurium was thicker in Group D
compared with the treatment groups. However, no significant
differences were identified. At week 12, the thickness of the
epineurium in Group D was significantly greater compared with the
treatment groups (P<0.01; Figs. 4
and 5).
Axon morphology analysis
H&E staining and TEM analyses were performed to
observe the morphology of the nerve fibers. The number and diameter
of nerve fibers and the myelin sheath thickness were quantified
using the images from the TEM analysis.
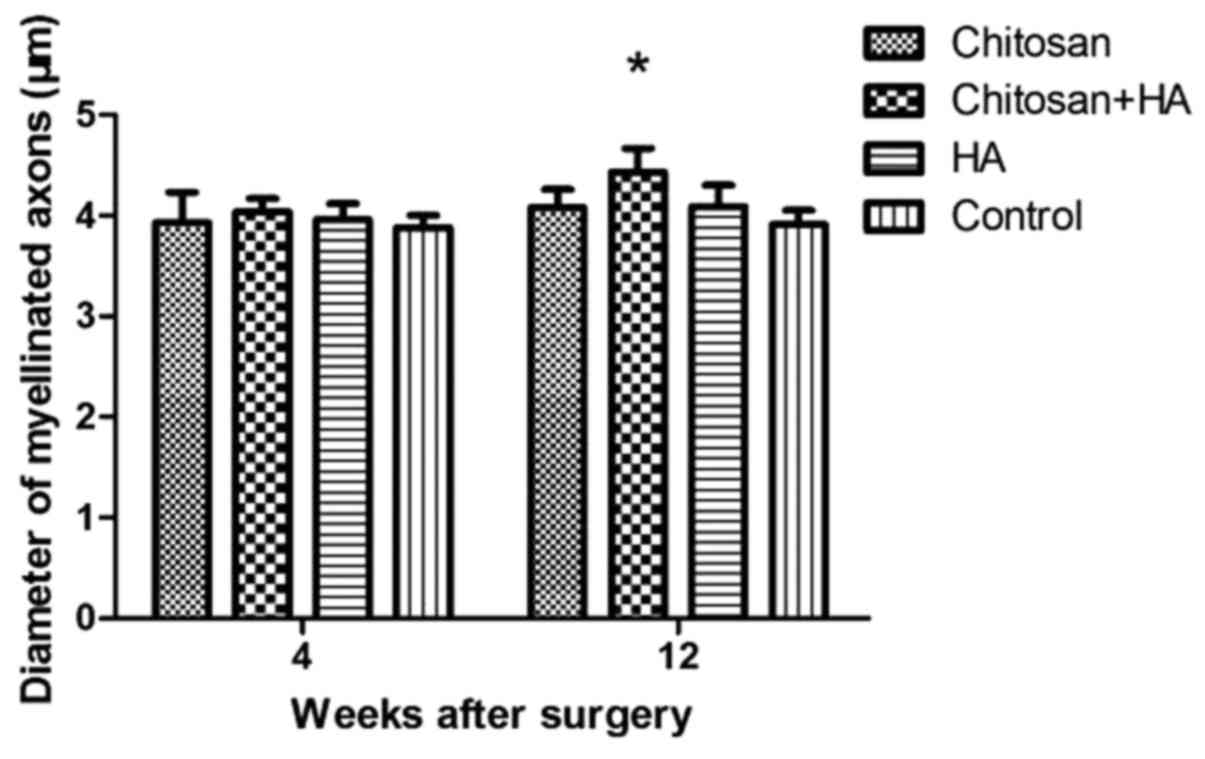
Myelinated nerve fiber diameter is
larger with chitosan and hyaluronate treatment
At 4 weeks, no significant differences in the mean
diameter of myelinated nerve fibers were observed between the
groups. However, at 12 weeks post-surgery, the mean diameter of
myelinated nerve fibers in Group B was significantly larger
compared with Group D (P<0.05; Fig.
6).
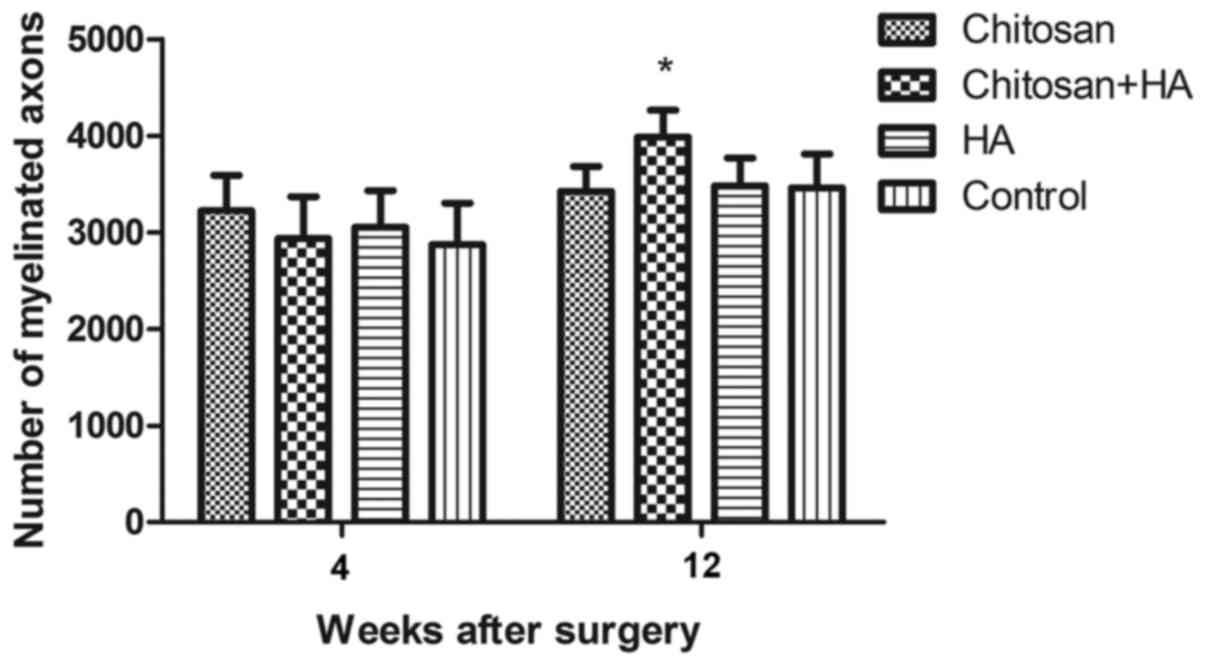
Myelinated nerve fiber numbers are
greater with chitosan and hyaluronate treatment
At 4 weeks following surgery, no significant
differences in the number of myelinated nerve fibers were
identified between the groups. However, the number of myelinated
nerve fibers in Group B was significantly greater compared with
Group D at week 12 (P<0.05; Fig.
7).
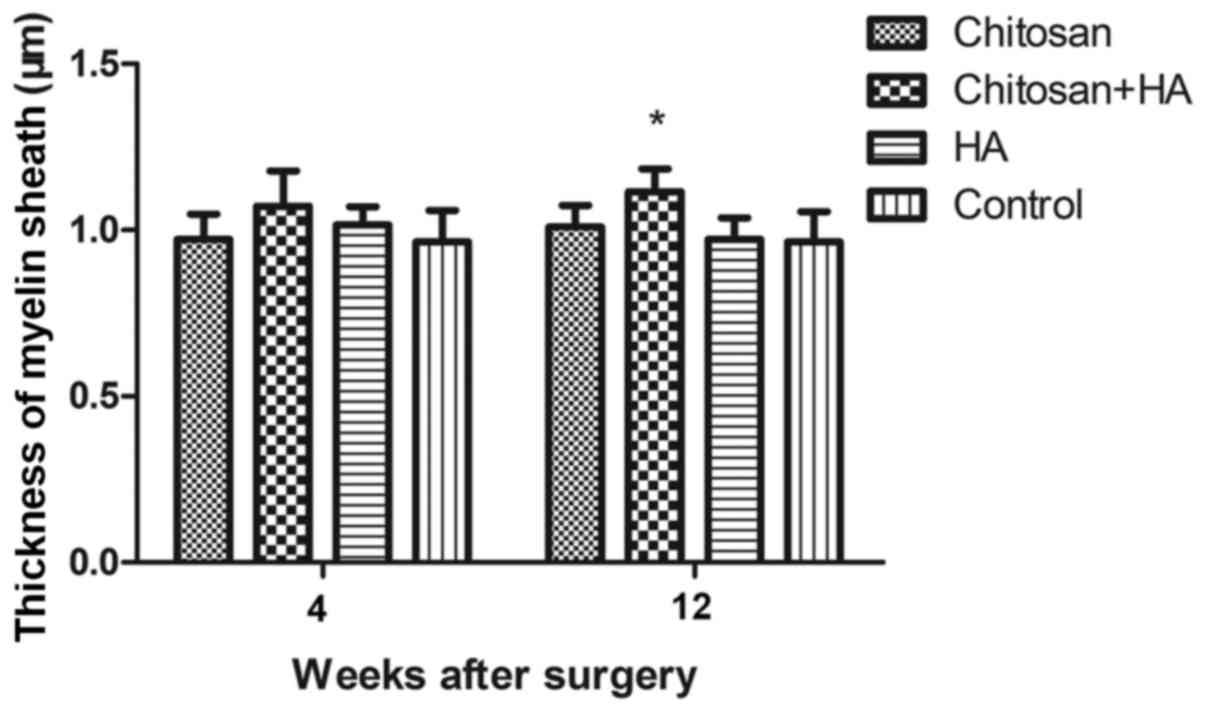
Myelin sheath thickness increases with
chitosan and hyaluronate treatment
At 4 weeks following surgery, no significant
differences in myelin sheath thickness were identified between the
groups. However, the myelin sheath thickness in Group B was
significantly increased compared with Group D at week 12
(P<0.05; Fig. 8).
Conduit analysis
Prior to and at 12 week after surgery, the surface
and cross section of the chitosan conduits were observed using SEM.
At week 12, chitosan conduits had partially been degraded and
absorbed; also, diameters of the chitosan conduits pores had
increased and the conduits had been partially absorbed into the
nerves (Fig. 9). At week 12 after
surgery, chitosan conduits were revealed to be compatible with the
rabbits as they were partially absorbed and no regional
inflammatory rejection occurred.
Neuralelectrophysiological
measurement
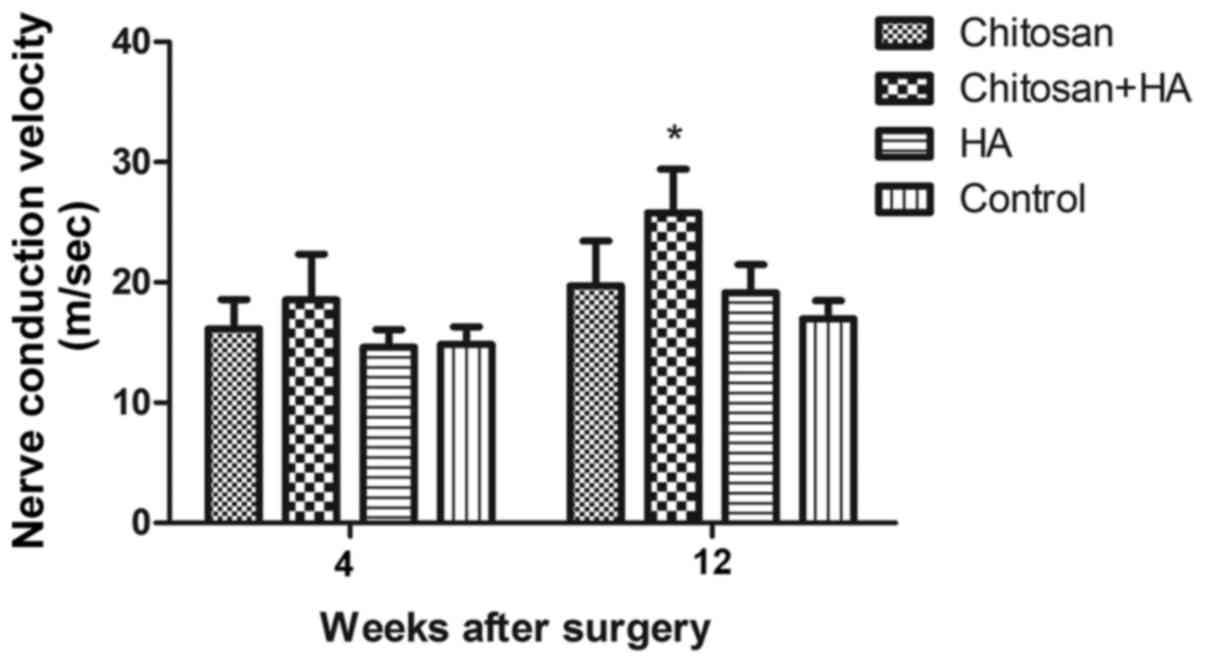
NCV was measured by electrophysiological assessment;
at week 4 post-surgery, no significant differences in NCV were
identified between the groups. At week 12, NCV in Group B was
significantly faster compared with Group D (P<0.05; Fig. 10).
Discussion
Severe injury to peripheral nerves causes
extraneural scarring, which increases the adhesion of nerves to
surrounding tissues (12). The
adhesion of peripheral nerves to surrounding tissues can lead to
compressive edema within nerve bundles, fibrotic changes and
tethering; fibrotic changes can interfere with blood flow to the
nerve and tethering can be harmful when stretching the extremities
(13). Therefore, extraneural
scarring has an impact on the functional recovery of peripheral
nerves.
Several studies have demonstrated that using a
variety of physical barriers or pharmaceutical interventions can
promote peripheral nerve regeneration and functional recovery
(2,5,9,14–16).
Peripheral nerve scar formation is associated with damage to the
blood-nerve barrier structure and function and fibroblast
activation, as well as extracellular matrix and cytokine imbalance
conversion regulation disorders (17,18).
Thus, reducing the number of activated fibroblasts,
downregulating α-smooth muscle actin, reducing transforming growth
factor (TGF)-β1 and TGF-β2, increasing TGF-β3 and increasing the
activity of collagenase have been used to inhibit the generation of
peripheral nerve scars (19). A
number of reagents have been demonstrated to reduce peripheral
nerve scar production and promote the recovery of neurological
function, including upregulating TGF-β inhibitors
mannose-6-phosphate, tissue plasminogen activator, chondroitinase,
interleukin-10, adrenocorticotropic hormone, hyaluronate, human
amniotic fluid, placenta suspension and heparin sulfate
glycosaminoglycan (9,20–24).
However, to the best of our knowledge, no studies have investigated
perineural scar prevention of the facial nerve.
Facial nerve injury following parotid gland surgery
or injury often requires surgical exposure of the facial nerve
(25). In the present study, damage
to the facial nerve and surrounding tissue with the potential to
cause facial nerve peripheral scarring and affect the restoration
of facial nerve function was inflicted. Such damage often leads to
different degrees of facial paralysis, affecting the patient's
physical and mental health (25). In
revision surgery for recurrent parotid gland tumors, adhesion of
the facial nerve to the surrounding tissue increases the difficulty
of the surgery and makes protecting the facial nerve more
challenging (26). It has been
reported that the incidence of permanent facial paralysis in the
first parotid gland surgery was 0–3.9%, however this could rise to
11.3–29.0% in revision surgery (27–29).
Chitosan is a natural polysaccharide macromolecule,
which can inhibit the growth of fibroblasts and prevent tissue
adhesion (2,30). The compatibility and hydrophilicity
of chitosan are improved following carboxymethylation, making it
suitable for implantation in vivo (2). High-degree deacetylation of chitosan
can inhibit the contraction of collagen-producing fibroblasts,
which may serve an important role in alleviating scar formation
(31). As a natural substance in
vivo, hyaluronate is biodegradable and serves as a neurolytic
agent to reduce scarring (2,32).
In the present study, chitosan conduits combined
with hyaluronate was selected to investigate improvements in neural
regeneration during nerve repair. The potential preventive effects
of chitosan, hyaluronate or a combination on extraneural scarring
and adhesion were evaluated using a rat facial nerve injury model.
A total of 4 weeks after surgery, no scarring was identified in the
nerves or surrounding tissues of the three experimental groups,
with infrequent adherence of muscle and nerve tissues. Nerve
membrane collagen thickness was lower in the treatment groups
compared with the control, however this difference was not
statistically significant. Furthermore, the Petersen scores of
Groups B and C were lower compared with Group D. Scar adhesion
formation was markedly improved at week 12 compared with week 4 in
all groups. The Petersen score of Group D was significantly higher
and the collagen in the external scar tissue was thicker compared
with the other three groups.
It was hypothesized that the scar tissue began to
form and wrap around the nerves of Group C and D at week 4.
Continuative compression may induce degeneration of axons and
myelin sheaths, which may affect the recovery of nerve function
(33). The initial formation of
fibrosis takes 2–3 weeks, but the maturation process may last for 9
months (34,35). At 4 weeks post-surgery, fibrosis had
not been fully completed, so the specimen was able to be isolated
easily. At week 12, however, the fibrosis process appeared to be
complete as the nerves were significantly more difficult to dissect
from the surrounding tissues in Group D compared with the
experimental groups. It was hypothesized that chitosan conduits
effectively prevented neurosurgical scar hyperplasia as it
inhibited the secretion of collagen from activated fibroblasts.
Park et al (2) demonstrated
that a hyaluronic acid-carboxymethylcellulose solution could reduce
the adhesion of nerves to surrounding tissues and prevent the
formation of scars. The current study also revealed that
hyaluronate could inhibit scar formation and that a chitosan
conduit in conjunction with hyaluronate may be more efficient.
Ishikawa et al (36)
demonstrated that chitosan conduits could promote nerve
regeneration following sciatic nerve defects.
In the current study, 12 weeks after surgery the
number of myelinated nerve fibers, the thickness of the myelin
sheath and NCV of Groups B were greater compared with Groups C and
D. The myelinated nerve fiber diameter, number of myelinated nerve
fibers, myelin sheath thickness and NCV of Group B were
significantly higher compared with Group D. It was determined that
neural scarring constricted the nerves continuously in Groups A, C
and D, which may have degenerated the axons and myelin sheaths.
Neural scarring may hinder the recovery of neurological function.
These findings further demonstrate that chitosan conduits combined
with hyaluronate may improve facial nerve regeneration and
function.
In summary, chitosan conduits and/or hyaluronate
promote the recovery of postoperative facial nerve function in
rabbits. The main limitation of the present study was the small
sample size used, resulting in a number of non-significant
differences. Future studies involving additional nerves and larger
samples are warranted.
As biocompatible absorbable materials, chitosan
conduits and hyaluronate have several advantages, including a wide
variety of sources and the possibility of mass production. In
addition, the combination of a chitosan conduit and hyaluronate was
more effective in preventing perineural scar production and
promoting facial nerve regeneration and functional recovery
following parotidectomy surgeries.
Acknowledgements
Not applicable.
Funding
The current study was supported by grants from the
National Natural Science Foundation of China (grant no. 81371116)
and Science and Technology Innovation Fund of the Chinese People's
Liberation Army General Hospital (grant no. 16KMM16).
Availability of data and materials
All data generated or analyzed during this study are
included in this published article.
Authors' contributions
HL and WB analyzed the data. HL, HH and XT performed
the animal experiments. WB, RL, WS, YZ and FZ performed the tissue
staining. WW and MH designed the experiments.
Ethics approval and consent to
participate
Animal anesthesia and euthanasia procedures were
approved by the Ethics Committee of the Chinese People's Liberation
Army General Hospital (Beijing, China).
Consent for publication
Not applicable.
Competing interests
The authors declare that they have no competing
interests.
References
|
1
|
Lane JM, Bora FW Jr and Pleasure D:
Neuroma scar formation in rats following peripheral nerve
transection. J Bone Joint Surg Am. 60:197–203. 1978. View Article : Google Scholar : PubMed/NCBI
|
|
2
|
Park JS, Lee JH, Han CS, Chung DW and Kim
GY: Effect of hyaluronic acid-carboxymethyl cellulose solution on
perineural scar formation after sciatic nerve repair in rats. Clin
Orthop Surg. 3:315–324. 2011. View Article : Google Scholar : PubMed/NCBI
|
|
3
|
Dy CJ, Aunins B and Brogan DM: Barriers to
Epineural scarring: Role in treatment of traumatic nerve injury and
chronic compressive neuropathy. J Hand Surg Am. 43:360–367. 2018.
View Article : Google Scholar : PubMed/NCBI
|
|
4
|
Ozgenel GY and Filiz G: Combined
application of human amniotic membrane wrapping and hyaluronic acid
injection in epineurectomised rat sciatic nerve. J Reconstr Surg.
20:153–157. 2004.
|
|
5
|
Magill CK, Tuffaha SH, Yee A, Luciano JP,
Hunter DA, Mackinnon SE and Borschel GH: The short- and long-term
effects of Seprafilm on peripheral nerves: A histological and
functional study. J Reconstr Microsurg. 25:345–354. 2009.
View Article : Google Scholar : PubMed/NCBI
|
|
6
|
Bak M, Gutkowska ON, Wagner E and Gosk J:
The role of chitin and chitosan in peripheral nerve reconstruction.
Polim Med. 47:43–47. 2017. View Article : Google Scholar : PubMed/NCBI
|
|
7
|
Fregnan F, Ciglieri E, Tos P, Crosio A,
Ciardelli G, Ruini F, Tonda-Turo C, Geuna S and Raimondo S:
Chitosan crosslinked flat scaffolds for peripheral nerve
regeneration. Biomed Mater. 11:0450102016. View Article : Google Scholar : PubMed/NCBI
|
|
8
|
Marcuzzo AV, Tofanelli M, Boscolo Nata F,
Gatto A and Tirelli G: Hyaluronate effect on bacterial biofilm in
ENT district infections: A review. APMIS. 125:763–172. 2017.
View Article : Google Scholar : PubMed/NCBI
|
|
9
|
Smit X, van Neck JW, Afoke A and Hovius
SE: Reduction of neural adhesions by biodegradable autocrosslinked
hyaluronic acid gel after injury of peripheral nerves: An
experimental study. J Neurosurg. 101:648–652. 2004. View Article : Google Scholar : PubMed/NCBI
|
|
10
|
Petersen J, Russell L, Andrus K, MacKinnon
M, Silver J and Kliot M: Reduction of extraneural scarring by
ADCON-T/N after surgical intervention. Neurosurgery. 38:976–984.
1996. View Article : Google Scholar : PubMed/NCBI
|
|
11
|
Most SP: Facial nerve recovery in bcl2
overexpression mice after crush injury. Arch Facial Plast Surg.
6:82–87. 2004. View Article : Google Scholar : PubMed/NCBI
|
|
12
|
Shintani K, Uemura T, Takamatsu K, Yokoi
T, Onode E, Okada M and Nakamura H: Protective effect of
biodegradable nerve conduit against peripheral nerve adhesion after
neurolysis. J Neurosurg. 20:1–10. 2017. View Article : Google Scholar
|
|
13
|
Gaudet AD, Popovich PG and Ramer MS:
Wallerian degeneration: Gaining perspective on inflammatory events
after peripheral nerve injury. J Neuroinflammation. 8:1102011.
View Article : Google Scholar : PubMed/NCBI
|
|
14
|
Abe Y, Doi K and Kawai S: An experimental
model of peripheral nerve adhesion in rabbits. Br J Plast Surg.
58:533–540. 2005. View Article : Google Scholar : PubMed/NCBI
|
|
15
|
Xu J, Varitimidis SE, Fisher KJ, Tomaino
MM and Sotereanos DG: The effect of wrapping scarred nerves with
autogenous vein graft to treat recurrent chronic nerve compression.
J Hand Surg Am. 25:93–103. 2000. View Article : Google Scholar : PubMed/NCBI
|
|
16
|
Albayrak BS, Ismailoglu O, Ilbay K, Yaka
U, Tanriover G, Gorgulu A and Demir N: Doxorubicin for prevention
of epineurial fibrosis in a rat sciatic nerve model: Outcome based
on gross postsurgical, histopathological, and ultrastructural
findings. J Neurosurg Spine. 12:327–333. 2010. View Article : Google Scholar : PubMed/NCBI
|
|
17
|
Ahmed Z, Dent RG, Leadbeater WE, Smith C,
Berry M and Logan A: Matrix metalloproteases: Degradation of the
inhibitory environment of the transected optic nerve and the scar
by regenerating axons. Mol Cell Neurosci. 28:64–78. 2005.
View Article : Google Scholar : PubMed/NCBI
|
|
18
|
Kim JS, Choi IG, Lee BC, Park JB, Kim JH,
Jeong JH, Jeong JH and Seo CH: Neuregulin induces CTGF expression
in hypertrophic scarring fibroblasts. Mol Cell Biochem.
365:181–189. 2012. View Article : Google Scholar : PubMed/NCBI
|
|
19
|
Zou T, Ling C, Xiao Y, Tao X, Ma D, Chen
ZL, Strickland S and Song H: Exogenous tissue plasminogen activator
enhances peripheral nerve regeneration and functional recovery
after injury in mice. J Neuropathol Exp Neurol. 65:78–86. 2006.
View Article : Google Scholar : PubMed/NCBI
|
|
20
|
Ngeow WC, Atkins S, Morgan CR, Metcalfe
AD, Boissonade FM, Loescher AR and Robinson PP: The effect of
Mannose-6-phosphate on recovery after sciatic nerve repair. Brain
Res. 1394:40–48. 2011. View Article : Google Scholar : PubMed/NCBI
|
|
21
|
Neubauer D, Graham JB and Muir D:
Chondroitinase treatment increases the effective length of
acellular nerve grafts. Exp Neurol. 207:163–170. 2007. View Article : Google Scholar : PubMed/NCBI
|
|
22
|
Atik B, Erkutlu I, Tercan M,
Buyukhatipoglu H, Bekerecioglu M and Pence S: The effects of
exogenous melatonin on peripheral nerve regeneration and collagen
formation in rats. J Surg Res. 166:330–336. 2011. View Article : Google Scholar : PubMed/NCBI
|
|
23
|
Atkins S, Loescher AR, Boissonade FM,
Smith KG, Occleston N, O'Kane S, Ferguson MW and Robinson PP:
Interleukin-10 reduces scarring and enhances regeneration at a site
of sciatic nerve repair. J Peripher Nerv Syst. 12:269–276. 2007.
View Article : Google Scholar : PubMed/NCBI
|
|
24
|
Dam-Hieu P, Lacroix C, Said G, Devanz P,
Liu S and Tadie M: Reduction of postoperative perineural adhesions
by Hyaloglide gel: An experimental study in the rat sciatic nerve.
Neurosurgery. 56(2 Suppl): S425–S433. 2005.
|
|
25
|
Glas AS, Vermey A, Hollema H, Robinson PH,
Roodenburg JL, Nap RE and Plukker JT: Surgical treatment of
recurrent pleomorphic adenoma of the parotid gland: A clinical
analysis of 52 patients. Head Neck. 23:311–316. 2001. View Article : Google Scholar : PubMed/NCBI
|
|
26
|
Romano A, Cama A, Corvino R, Graziano P,
Friscia M, Iaconetta G and Califano L: Complications after parotid
gland surgery Our experience. Ann Ital Chir. 88:295–301.
2017.PubMed/NCBI
|
|
27
|
Wittekindt C, Streubel K, Arnold G,
Stennert E and Guntinas-Lichius O: Recurrent pleomorphic adenoma of
the parotid gland: Analysis of 108 consecutive patients. Head Neck.
29:822–828. 2007. View Article : Google Scholar : PubMed/NCBI
|
|
28
|
Liu H, Wen W, Huang H, Liang Y, Tan X, Liu
S, Liu C and Hu M: Recurrent pleomorphic adenoma of the parotid
gland: Intraoperative facial nerve monitoring during parotidectomy.
Otolaryngol Head Neck Surg. 151:87–91. 2014. View Article : Google Scholar : PubMed/NCBI
|
|
29
|
Dell'Aversana Orabona G, Bonavolonta P,
Iaconetta G, Forte R and Califano L: Surgical management of benign
tumors of the parotid gland: Extracapsular dissection versus
superficial parotidectomy-our experience in 232 cases. J Oral
Maxillofac Surg. 71:410–413. 2013. View Article : Google Scholar : PubMed/NCBI
|
|
30
|
Wu XB, Peng CH, Huang F, Kuang J, Yu SL,
Dong YD and Han BS: Preparation and characterization of chitosan
porous microcarriers for hepatocyte culture. Hepatobiliary Pancreat
Dis Int. 10:509–515. 2011. View Article : Google Scholar : PubMed/NCBI
|
|
31
|
Howling GI, Dettmar PW, Goddard PA,
Hampson FC, Dornish M and Wood EJ: The effect of chitin and
chitosan on fibroblast-populated collagen lattice contraction.
Biotechnol Appl Biochem. 36:247–253. 2002. View Article : Google Scholar : PubMed/NCBI
|
|
32
|
Ikeda K, Yamauchi D, Osamura N, Hagiwara N
and Tomita K: Hyaluronic acid prevents peripheral nerve adhesion.
Br J Plast Surg. 56:342–347. 2003. View Article : Google Scholar : PubMed/NCBI
|
|
33
|
Li BH, Yang K and Wang X: Biodegradable
magnesium wire promotes regeneration of compressed sciatic nerves.
Neural Regen Res. 11:2012–2017. 2016. View Article : Google Scholar : PubMed/NCBI
|
|
34
|
Soller EC, Tzeranis DS, Miu K, So PT and
Yannas IV: Common features of optimal collagen scaffolds that
disrupt wound contraction and enhance regeneration both in
peripheral nerves and in skin. Biomaterials. 33:4783–4791. 2012.
View Article : Google Scholar : PubMed/NCBI
|
|
35
|
Demir R, Yayla M, Akpinar E, Cakir M,
Calikoglu C, Ozel L, Ozdemir G and Mercantepe T: Protective effects
of alpha-lipoic acid on experimental sciatic nerve crush injury in
rats: Assessed with functional, molecular and electromicroscopic
analyses. Int J Neurosci. 124:935–943. 2014. View Article : Google Scholar : PubMed/NCBI
|
|
36
|
Ishikawa N, Suzuki Y, Ohta M, Cho H,
Suzuki S, Dezawa M and Ide C: Peripheral nerve regeneration through
the space formed by a chitosan gel sponge. J Biomed Mater Res A.
83:33–40. 2007. View Article : Google Scholar : PubMed/NCBI
|