Introduction
Metamizole sodium (dipyrone) is a pyrazoline-derived
non-steroidal anti-inflammatory drug (NSAID) and non-opioid
analgesic. Despite its low inhibitory effect on the enzyme
cyclooxygenase, as well as its low anti-inflammatory effect, it has
a marked analgesic effect (1). The
analgesic properties of dipyrone contribute to its effects in
afferent fibers, the spinal cord and periaqueductal gray matter. It
also has an anti-pyretic and anti-spasmodic effect in vivo
(1).
Of note, dipyrone is easily soluble in water.
Therefore, its pharmaceutical application is simple, e.g.
preparation of an injectable solution. When administered orally,
dipyrone is non-enzymatically and rapidly converted to its active
metabolite, 4-methylamino-antipyrine (4-MAA), in the acidic
contained in the stomach. It is then absorbed through the
gastrointestinal tract. When administered intravenously, it
is converted to 4-MAA in the peripheral blood (1).
Numerous studies have discussed whether the
analgesic effects of NSAIDs are tolerable, similar to opioid
tolerance. Apart from its frequent use in clinical practice, it is
generally accepted that the anti-nociceptive effects of NSAIDs lose
their efficacy. Based on this consensus, dipyrone is also preferred
as a prototype for NSAIDs in studies (1), demonstrating that tolerance to NSAIDs
may be developed.
The use of dipyrone has been banned in the USA and
certain European countries for allegedly causing agranulocytosis in
the bone marrow and fluid/electrolyte imbalance (2). However, in numerous countries, it is
still frequently prescribed in neurosurgery clinics (3) or is administered systemically in
emergency departments (4). Long-term
use of dipyrone loses efficacy to analgesic effects; this has been
identified in the last few years as an important problem (1). Significant resistance, including the
requirement to increase the dosage and thus the adverse effects,
arise over long-term use.
In the literature, the side effects and/or adverse
events associated with dipyrone have been described as follows: a)
Blood disorders, including shock and agranulocytosis, leukopenia
and thrombocytopenia; b) high fever, chills, sore throat and
difficulty swallowing; and c) inflammatory lesions in the mouth,
nose, throat, genital and anal regions. However, its effects on
intervertebral disc tissue cells, including nucleus pulposus (NP)
or annulus fibrosus (AF) cells, have not been indicated in studies
with high evidential value.
No veins, lymph or nerves are present in
intervertebral disc tissue, just as in cartilage tissue. Instead,
disc tissue is fed by synovial fluid. Since the outer layer of the
synovial tissue is thicker, the drugs first diffuse from the
synovial tissue to the synovial fluid. Subsequently, a second
diffusion occurs from the synovial fluid to the disc tissue.
Certain studies have indicated that drugs containing the pyrazole
moiety, including dipyrone, pass into the synovial fluid of model
rats with complete Freund's adjuvant-induced chronic arthritis
(5).
Certain drugs may accumulate in numerous tissues of
the body, including the synovial fluid compartments and the
intervertebral disc tissue (6,7). As a
result of developments in pharmaceutical technology and
regenerative medicine, the toxicity of drugs at the molecular level
and the repair of the damaged tissues continue to be the subject of
numerous studies. In such studies, apart from the drug's effect on
the cell viability and proliferation, changes in the gene
expression levels of certain proteins or specific biomarkers within
the anabolic and/or catabolic pathways in tissues have also been
investigated 6,7). However, to the best of our knowledge, no
previous study has examined whether dipyrone damages
non-degenerate, intact intervertebral disc tissue at the
pharmaco-molecular level with high evidential value.
The present study investigated the effect of
dipyrone on AF/NP cells. Primary cultures obtained from intact
AF/NP tissues were used, and dipyrone was administered to these
cultures for 20 days. The cell viability and proliferation of AF/NP
cells and toxicity of dipyrone were analyzed in vitro. In
addition, the gene expression levels of chondroadherin (CHAD),
cartilage oligo matrix protein (COMP), matrix metalloproteinase 7
(MMP-7), MMP-13 and MMP-19, as well as interleukin-1β (IL-1β) were
examined using reverse transcription-quantitative polymerase chain
reaction (RT-qPCR). No apoptotic death was observed in the
dipyrone-treated AF/NP cell cultures. However, the cell
proliferation was inhibited and the cells lost their specific
morphology. In addition, changes in gene expression were observed
in parallel with the changes in cell morphology.
Materials and methods
Study design
Analyses were repeated three times in total to
minimize any experimental errors. The resection of the
intervertebral disc tissues was performed by the same surgeons.
While the cell cultures from primary human intervertebral disc
tissue were established by the same researchers, the molecular
analyses performed after the drug administration to the cultures
were also performed by the same researchers. Researchers who
performed the analyses did not know which drug was applied to which
cell culture group, or which freshly prepared culture medium was
applied to which cell culture group. While researchers performed
the analyses, they were blinded to the experimental group
identities.
Primary cell cultures of human intervertebral disc
tissue were established from surgically resected tissues.
Subsequently, all analyses were performed using cell samples from a
non-drug-administered control group and drug-administered groups.
The data obtained were then statistically evaluated.
Materials and reagents
Disposable cell culture materials were purchased
from Biosorfa (Zhongguan, China; cat. no. SCD-11-035).
FG-Microplate 96-well plates (cat. no. 4346906), fetal bovine serum
(FBS; cat. no. 10500064), L-glutamine (cat. no. 25030024),
penicillin-streptomycin 10,000 U/ml (cat. no. 15140122) and
amphotericin B (250 UG/ml, cat. no. 12183018) were obtained from
Thermo Fisher Scientific, Inc. (Waltham, MA, USA).
The pharmacological agent containing dipyrone used
in the experiments was Novalgin Ampul in the form of 0.5 g/ml
ampoules. It was procured from Sanofi S.A. (Paris, France). The
commercial kit used to examine the cell viability and proliferation
to analyze toxicity was the Vybrant MTT cell proliferation assay
(cat. no. V13154; Thermo Fisher Scientific, Inc.). The ELISA with
which spectrophotometric analysis was performed was the Mindray MR
96A, PRC (Georgia Tech, Atlanta, GA, USA).
A PureLink™ RNA Mini kit (cat. no. 15290018; Thermo
Fisher Scientific, Inc.) was used for RNA isolation, and a
high-capacity complementary (c)DNA RT kit (cat. no. 4368814; Thermo
Fisher Scientific, Inc.) was used to obtain cDNA. The following
assays were also purchased from Thermo Fisher Scientific, Inc., to
determine the mRNA expression of various genes in all experimental
groups: TaqMan® gene expression assays (cat. no.
4331182), CHAD TaqMan gene expression assays (cat. no. 4331182),
COMP TaqMan gene expression assays (cat. no. 4331182), MMP-7 TaqMan
gene expression assays (cat. no. 4331182), MMP-13 TaqMan gene
expression assays (cat. no. 4331182), MMP-19 TaqMan gene expression
assays (cat. no. 4331182), IL-1β TaqMan gene expression assays
(cat. no. 4331182), internal control genes (housekeeping
genes-β-actin) and Taqman Fast Advanced MMix 5ml (cat. no.
4444557).
Case selection criteria
Patients with a pyrazoline allergy, certain
metabolic diseases (e.g., hepatic porphyria), congenital
glucose-6-phosphate-dehydrogenase deficiency, blood dysregulation,
hypersensitivity or intolerance to drugs containing pharmacological
agents, including metamizole, isopropyl aminophenazone,
propyphenazone, phenazone and phenylbutazone, were excluded from
the study. If the tissues of these patients had been included in
the study, it would not have been possible to determine whether the
results on cytotoxicity or changes in cell morphology were due to
dipyrone or to cell cultures obtained from the tissues of these
patients. Similarly, the tissues of patients with a history of
alcohol consumption or those using cyclosporine in the last three
weeks were not included in the study, as the toxicity of dipyrone
in these cases may have been affected by adverse drug synergism
with alcohol or cyclosporine, which may accumulate in tissues. This
may have adversely affected the results of the study.
Resection of the tissues via surgery
and preparation of the primary cell cultures
Non-degenerate healthy disc material (intact NP and
AF tissue) was obtained as surplus surgical material from 3 male
(age range, 25–31 years; mean age, 28) and 3 female patients (age
range, 29–30 years; median age, 29.33 years). Subsequently, human
primary intervertebral disc cell cultures were established
individually according to standard protocols (6,7).
Physical and neurological examinations were performed on patients
referred to the emergency department with the complaint of spinal
trauma. Direct radiography, spinal-computed tomography scan and
magnetic resonance imaging examinations were performed for possible
spinal trauma localization. After these examinations, surgical
intervention was planned in patients with spinal instability,
traumatic intervertebral disc herniation and spinal cord
compression.
All patients were placed in the prone position under
endotracheal general anesthesia. Surgical field antisepsis was
provided with 10% povidone-iodine solution and the area was covered
in a sterile drape. After the skin was perforated with a median
incision, paravertebral muscles were dissected subperiosteally.
Neural decompression, traumatic disc excision and subsequent
stabilization with the transpedicular screw-rod system were
performed (6,7).
Under aseptic conditions at 4°C, disc and
granulation tissues were transferred to the laboratory in a culture
medium [Dulbecco's modified Eagle's medium (DMEM; Gibco; Thermo
Fisher Scientific, Inc., Waltham, MA, USA) supplemented with 1%
penicillin-streptomycin, 15% FBS and 1% L-glutamine]. Tissue
samples were irrigated with a 0.9% isotonic sodium chloride
solution in the laminar flow cabinet and clarified from the red
blood cells. Next, tissues were dissected into 0.4 cm3
pieces, washed in Hank's balanced salt solution and transferred to
Falcon tubes. A total of 0.375 mg Collagenase type II enzyme
(Gibco; Thermo Fisher Scientific, Inc.) dissolved in complete
medium was added to each tube and the samples were incubated with
5% CO2 at 37°C overnight. Next, the samples were
centrifuged at 161 × g for 10 min at 37°C The cell pellets obtained
were re-suspended by adding cell culture medium, transferred to T75
flasks and incubated to obtain primary cell cultures. Cells were
counted in the presence of Trypan blue. Later, they were
transferred to 96-well plates at 1.6×104 cells/well for
MTT analysis, to 24-well plates at 4.3×104 cells/well
for inverted microscopy and petri dishes at 5.1×106
cells/dish for acridine orange (AO)/propidium iodide (PI) analysis
and for RNA isolation. They were then incubated for 24 h in an
incubator with a humidified atmosphere containing 5% CO2
at 37°C. After the incubation period, dipyrone was administered to
the cell cultures.
Application of dipyrone to the
cultures
The major stock solution was freshly prepared as 0.5
g/ml of dipyrone in DMEM in a flow cabinet. Subsequently, the major
stock solutions were subjected to color coding, which enabled
researchers to be blinded to the analyses. Dipyrone was applied to
human primary NP/AF cell cultures at the final concentration of 250
µM. In another experiment, dipyrone was applied to the cultures at
concentrations of 1, 50, 100, 250, 500 and 1,000 µM.
Cell proliferation was previously reported to stop
completely in cultures where dipyrone at concentrations of
>250–300 µM was applied (8).
Therefore, dipyrone was applied at concentrations allowing for
proliferation. Group I was prepared to resemble control group
cells. The cells in this group were composed of cells obtained from
healthy non-degenerated tissues [intact (i) AF/NP]. No drugs were
administered to the cells in Group I. The cells forming the study
group were Group II, in which human primary iAF/NP culture cells
were cultivated with dipyrone at a concentration of 250 µM for 20
days.
Inverted/fluorescence microscopy
analysis
Cell morphology and confluency were observed using
an inverted light microscope (Olympus CKX41; Olympus, Tokyo,
Japan). Microphotographs of cell organization were obtained and
analyzed during the confocal/contrast phase prior to and after
dipyrone applications by Olympus Cell Soft Imaging System software
(Olympus Corporation; version, Cell^A5.1). For further analysis of
cell organization and characterization, cultures were stained with
Giemsa (GS500; Sigma-Aldrich; Merck KGaA, Germany) and examined. A
fluorescent microscope (DM 2500; Leica Microsystems, Wetzlar,
Germany) was used for AO/PI analysis. Photomicrographs of the cells
were obtained prior to and during dipyrone applications, and the
images were evaluated using Cytovision Capture Station imaging
software (version 7.0; Genetix; Leica Microsystems).
Analysis of cell viability, toxicity
and proliferation by MTT assay
Viable cells digested the tetrazolium rings of MTT
with their active mitochondrial dehydrogenase enzymes to generate
formazan crystals. Unlike viable cells, dead cells did not form
these formazan crystals (6,7). The density of the resulting formazan
crystals was detected with a spectrophotometer. Viability tests
were performed using a commercial MTT kit. MTT analyses of iAF/NP
cell viability and proliferation were performed, and the toxicity
of dipyrone was determined. MTT analyses were performed at 0 h, 10
days and 20 days.
The culture media containing dipyrone was discarded
from the wells and 100 ml MTT solution (12 mM; prepared by adding 1
ml sterile PBS to 5 mg MTT) was added to each well. Cultures were
incubated at 37°C for 2 h under the exclusion of light. The
solution was discarded prior to the addition of DMSO, which was
added to stop the reaction. Following this, wells were incubated at
37°C for an additional 10 min, prior to photometric analysis of the
absorbance at a wavelength of 540 nm. The viability of the control
group was assumed to be 100% (6,7).
AO/PI staining
To determine cell viability and confirm the results
of the MTT assay, the nucleic acid-binding dyes AO and PI were
used. AO stained all nucleated cells, whether alive or dead,
generating green fluorescence. PI penetrated only dead cells with
poor membrane integrity and stained nucleated cells to generate red
fluorescence. When stained with AO and PI, all live nucleated cells
exhibited green fluorescence and all dead nucleated cells displayed
red fluorescence (6,7). To prepare the AO/PI stain, 4 mg AO
(dissolved in 2 ml 99% ethanol), 10 g sodium EDTA, 4 mg PI and 50
ml FBS were mixed well. Sterile distilled water was added to reach
a final volume of 200 ml (6,7,9).
Real-time PCR analysis of CHAD, COMP,
MMP-7, MMP-13, MMP-19 and IL-1β expression
Total RNA was extracted from cultured primary iAF/NP
cells using the PureLink™ RNA Mini kit. The quantity of RNA was
measured and 50 ng RNA was reverse-transcribed using a
high-capacity cDNA RT kit to obtain cDNA using a thermal cycler.
For synthesis of cDNA, 10 µl 10X RT buffer, 4 µl 25X dNTP, 10 µl
10X random primers, 5 µl 50 U/µl reverse transcriptase, 51 µl
nuclease-free water and 20 µl RNA were mixed well and held at 25°C
for 10 min. They were then maintained at 37°C for 2 h. To determine
gene expression profiles, all genes were amplified using TaqMan
gene expression assays for CHAD, β-actin (ACTβ), COMP, MMP-7,
MMP-13, MMP-19 and IL-1β. qPCR was performed on an Applied
Biosystems 7300/7500 real-time PCR system (Thermo Fisher
Scientific, Inc.). The reaction mixture consisted of 1 µl TaqMan
gene expression assay (probes and primers), 10 µl TaqMan gene
expression master mix, 4 µl cDNA template and UltraPure
DNase/RNase-free distilled water for each gene in MicroAmp fast
optical 96-well reaction plates. The thermocycling conditions were
as follows: A holding stage for 2 min at 50°C, a second holding
stage for 10 min at 95°C and a 40 cycles of 15 sec at 95°C and 1
min at 60°C. The steps were performed only once. As a result of the
qPCR experiment, the relative quantity (RQ) values of each sample
were obtained using the 7500 Fast-SDS program V.2.3 (Thermo Fisher
Scientific, Inc.). ACTβ was used as an endogenous control to
normalize the targeted gene expression. For obtaining comparative
results, a reference (calibrator) sample (Group 1, 0 h) was used,
and RQ values were calculated using the 2∆∆Cq method
(6,7,9).
Statistical analyses
Minitab 16 Statistical Software was used to evaluate
the data. Analysis of variance (ANOVA) was used to calculate the
difference between the mean values of the data obtained. After the
ANOVA test, Tukey's honestly significant difference test was used
to determine which groups were different from each other or whether
all groups were different from each other. Values are expressed as
the mean ± standard deviation. In the statistical analyses, a 95%
confidence interval was assumed and differences with an alpha value
of <0.05 were considered to be statistically significant.
Results
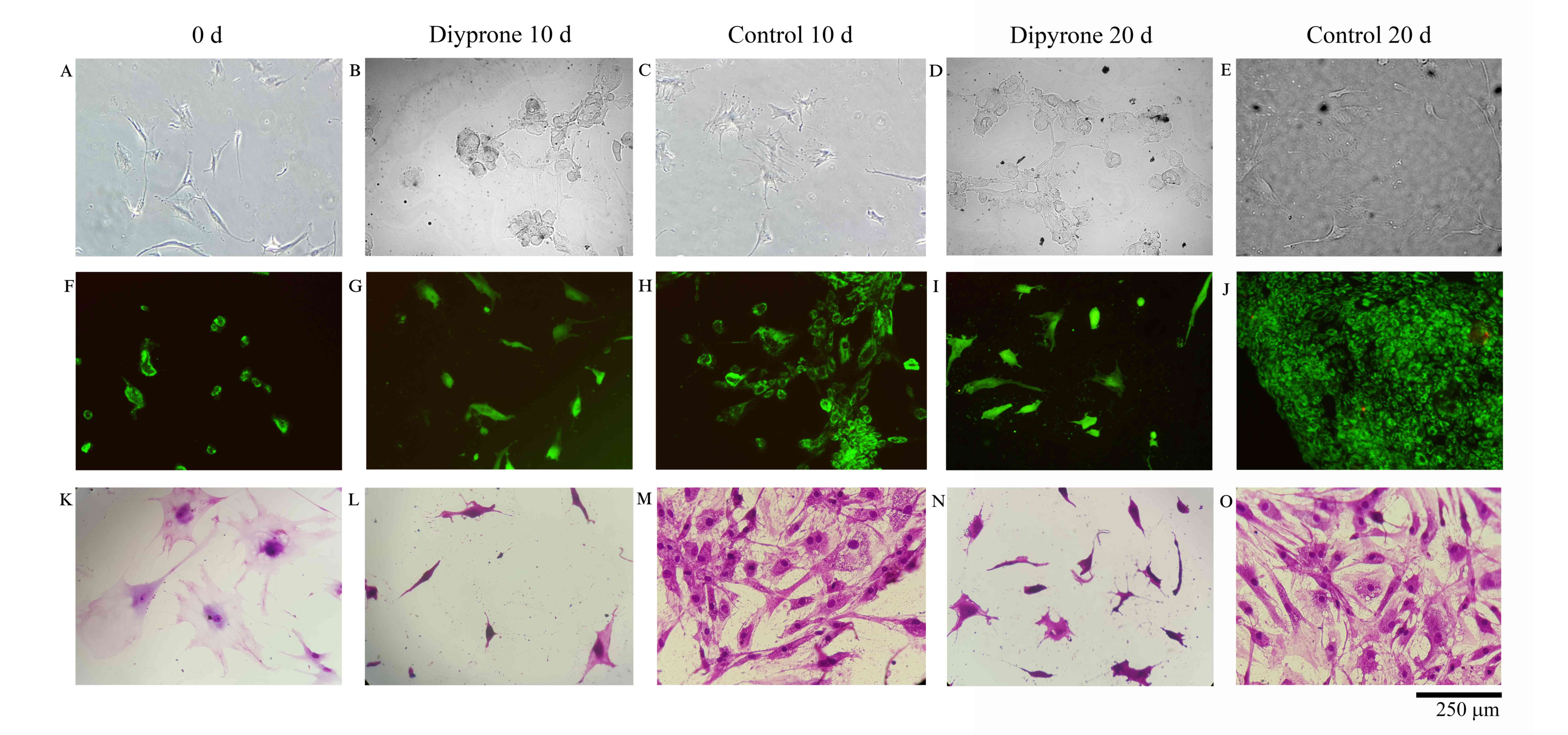
Evaluation of AO/PI staining
The formation of the extracellular matrix structure
was significantly decreased in the dipyrone-treated samples
compared with that in the control group. When the dipyrone-treated
cells of the intervertebral disc tissue were examined, they were
observed to have lost their morphology and become rounder in shape,
an indicator of cytotoxicity. Thus, cell proliferation in the
cultures treated with dipyrone was decreased. However, no acute
cell death was observed on AO/PI staining (Fig. 1).
Cell viability, toxicity and
proliferation
Microscopic analysis indicated reduced proliferation
in dipyrone-treated cultures. These results were confirmed by MTT
analysis. In the drug-treated groups, cell viability and
proliferation were decreased by almost half compared with those in
the untreated control group. These results were statistically
significant (P<0.05; Table
I).
 | Table I.Grouping of Tukey test data after
ANOVA performed in 95% confidence interval between control and
dipyrone groups. |
Table I.
Grouping of Tukey test data after
ANOVA performed in 95% confidence interval between control and
dipyrone groups.
| A, MTT viability
assay (ANOVA) |
|---|
|
|---|
| Group | DF | Adj SS | Adj MS | F-value | P-value |
|---|
| Incubation times
(h) | 1 | 0.088621 | 0.088621 | 231.08 | <0.001 |
| Non-treated with
dipyrone | 1 | 0.001860 | 0.001860 | 4.85 | 0.036 |
| Dose | 1 | 0.053464 | 0.053464 | 139.41 | <0.001 |
|
| B, MTT viability
assay (Tukey's honestly significant differences test) |
|
| Group/incubation
time | N | Mean ± standard
deviation |
Grouping |
|
| Control group 20
days | 8 | 0.4120±0.034 | A |
| Control group 10
days | 8 | 0.3150±0.008 | B |
| Dipyrone 10
days | 8 | 0.2915±0.013 | B |
| Dipyrone 20
days | 8 | 0.2250±0.011 | C |
Interpretation of RT-qPCR
analysis
The expression of all genes analyzed by RT-qPCR was
assumed as 100% (RQ=1) on day 0. In the untreated control group,
the expression of CHAD on the tenth day increased by ~3.2-fold and
IL-1β expression increased by ~3.4-fold. The gene expression of
MMP-19 exhibited an increase with RQ=1.7. COMP expression in the
control group did not change (RQ=1.0), but MMP-13 (RQ=0.4) and
MMP-7 (RQ=0.1) expression decreased (P<0.05). In the control
group, on day 20, the expression of CHAD had increased by 4.3-fold
and the gene expression of IL-1β increased by 7.03-fold
(P<0.05). The expression of MMP-13 (RQ=0.1) and MMP-7 (RQ=0.1)
decreased, while the expression of COMP (RQ=1.3) and MMP-19
(RQ=1.5) exhibited a slight increase (P<0.05). In the
dipyrone-treated cultures, gene expression stopped in a manner
consistent with the morphologically observed senescence (data not
shown). In the dipyrone-treated group, although, internal control
β-actin gene expression was persistent no expression of the analyte
genes was detected after 20 days. The cells did not die through
apoptosis or any other mechanism but became senescent after
dipyrone application. This result demonstrated the complete halt of
cell proliferation.
Discussion
Dipyrone is a 4-MAA derivative that is commonly used
as an NSAID in certain European countries, South America, South
Africa and the Middle East due to its analgesic and anti-pyretic
effects. Particularly in the practice of neurosurgery, studies
exist on the use of this drug for the following purposes: a) In
post-operative pain control, b) in the treatment of cerebral
vasospasm after subarachnoid hemorrhage, c) as a neuroprotective in
ischemic cerebrovascular occlusions and d) as a local anesthetic in
awake craniotomies (10–12).
Different results have been reported in toxicology
studies performed with dipyrone. A statistically significant weight
loss has been indicated, particularly in female rats, but no
changes in the mean lifespan, blood parameters or tumor development
have been indicated (13). In
addition, mild hemosiderosis, an increase in reticulocyte count and
increase in Heinz body formation have been reported in live mammals
exposed to high doses of dipyrone for 6 months (14). In a similar study, a case of aplastic
anemia due to dipyrone use for 12 months was reported (15). Even though numerous adverse effects
of the drug have been reported in the literature, its effects on
intervertebral disc tissue cells, including NP or AF cells, have
not been examined. Therefore, the present study aimed to
investigate the positive or negative effects of dipyrone on intact
intervertebral disc tissue cells at the pharmaco-molecular
level.
Most cytotoxicity studies used experimental setups
involving tissues of living mammalian subjects (16,17).
However, the results obtained with animal tissues may be different
from those obtained with human tissue due to differences in
sensitivity (18). In numerous
studies where animal tissues were not used, commercial cell lines
were used (19,20). However, in systems such as cell
lines, one type of cell is used, and in such commercial cell lines,
no complex coordination mechanisms with the microenvironment
involving other tumor-associated cells are present. As a result,
the in vitro test results may not resemble in vivo
conditions and may become even more controversial, since the cell
does not interact with factors such as the extracellular matrix. In
addition, since the genetic structure of the cells in the cell line
would have been modified, they would not carry the genotypic and/or
phenotypic characteristics that they have in the human body
(21). Therefore, the present study
did not use any commercial cell lines or cells isolated from animal
tissues. The study was performed on primary cell cultures isolated
from intact human intervertebral disc tissues. This may be one of
the aspects in which the results of the present study are
superior.
Certain studies have provided evidence that dipyrone
applied at low doses was not toxic but had a cytoprotective effect.
Pompeia et al (8) evaluated
the effect of dipyrone on the viability in human leukocyte cell
lines upon the following apoptotic treatments: Arachidonic acid
(AA), cycloheximide (CHX), tumor necrosis factor (TNF) and
ultraviolet (UV) irradiation. They investigated different
dose-dependent effects of dipyrone. First, they reported that it
was cytotoxic and caused apoptosis at high concentrations (beyond
300 µM). Furthermore, they indicated that it was cytoprotective at
lower concentrations (37.5–300 µM) and that it delayed the loss of
membrane integrity generated by AA (100–200 µM), UV irradiation and
the cytotoxicity of CHX (25–50 µM). They did not identify any
effect of dipyrone on TNF-induced cytotoxicity (250 ng/ml). They
emphasized that the cytoprotective effect of dipyrone was
associated with a decrease in DNA fragmentation when assessed by
electrophoresis and flow cytometry of genomic DNA. They also
underscored that the cytoprotective effect on leukocyte apoptosis
occurred at concentrations that are common for the major active
metabolite of the drug (8).
Arkhipchuk et al (22)
applied dipyrone and acetylsalicylic acid drugs to different
systematic groups formed from plants, invertebrates and
vertebrates. They evaluated the toxicity, cytotoxicity and
genotoxicity of the drugs on those different systematic groups.
When the pharmaceutical substances were administered to live
mammalian cells, they were applied at a dose resembling the
IC50, which was half of the concentration of the
substance known to be inhibitory. They reported that dipyrone had
acute toxic effects when applied at a concentration of 6.25%. After
30–360 min of exposure of the respective organism to the drug, the
nucleolar size in plant and animal cells (i.e., the transcription
activity of the ribosomal genes) changed. Furthermore, they also
indicated that dipyrone gave rise to nucleolar structural damage in
90% of hydra cells at as early as 30 min of exposure (22). CHAD, a continuously expressed
NP-specific marker, is known to be linked with the development of
the spinal cord and dorsal column (6,7,9). COMP is the most well-known marker
amongst the degradation markers. Increased levels of this marker
are thought to indicate the progression of osteoarthritis and aging
of the tissues. COMP, a non-aggrecan and non-collagenous marker,
indicates degradation of cartilage. However, studies have indicated
that COMP also occurs in bones, ligaments, tendons and in the
vascular smooth muscles. However, COMP expression was not
identified in NP or AF cells. The utility of COMP as a marker has
also been investigated in molecular studies regarding lumbosacral
spine disc space narrowing, intervertebral disc tissue and lower
back symptoms (23–26).
MMPs, the enzymes responsible for the destruction of
extracellular matrix proteins and organogenesis, the process of
growth and normal tissue regeneration, have essential functions in
maintaining physiological incidents in the organism. They perform
these functions through a balance between MMP activity and specific
endogenous tissue inhibitors. The shift of this balance to MMP
activity leads to matrix destruction and pathophysiological events
(27). While MMP synthesis and
activity is low in healthy tissues, its level increases in numerous
pathological and/or adverse conditions, including inflammatory
diseases, tumor progression and metastasis; this increase causes
tissue destruction (28).
Since 1991, MMPs in the intervertebral disc cells
have been known to cause degeneration of healthy intact disc tissue
(29). As is known, large collagen
types are present in NP and AF tissues. The structure of these
collagens and their association with each other have a vital role
in the mechanical function of the disc. These collagen molecules
may only be degraded by specific enzymes, primarily MMPs. MMPs are
the major enzymes in the catabolism of collagen molecules and
differ regarding their substrate specificity. MMPs degrade all
known matrix components (29).
Degenerated discs are more vascular than normal discs, and vascular
structures are known to produce MMPs. Although immunohistochemistry
provides limited information, when considering the ratio of disc
cells to vascular cells, most MMPs are produced by disc cells. The
high MMP levels in the herniated discs indicate that the MMPs are
naturally responsible for the repair of disc herniation (29).
Yurube et al (30) investigated the degeneration of
intervertebral disc tissue in rats, which were used as experimental
live mammals. They reported that MMP-7 and MMP-13 are catabolic
genes associated with the degeneration of disc tissue. MMP-13,
classified into the group of collagenases, is an enzyme with the
ability to break down intact interstitial collagen molecules
(31). MMP-7, also known as
matrilin, is capable of degrading non-collagenase proteins,
including proteoglycans and MMP-3. MMP-7 is able to break down the
intermolecular network between collagen fibrils, as it breaks down
denatured collagen molecules (32).
MMP-19, which is known to hydrolyze certain basal
membrane proteins, is also referred to as RASI-1 (33). The human MMP-19 gene encodes a
protein that has a role in normal physiological processes,
including embryonic development, reproduction and tissue
remodeling, as well as in the degradation of extracellular matrix
in processes associated with various diseases, e.g. arthritis and
metastasis. The encoded protein is secreted as an inactive
proprotein that is activated upon cleavage by extracellular
proteases (34).
In their study regarding MMP-19, Gruber et al
(35) reported that no previous
studies had assessed the effects of MMP-19 on the extracellular
matrix components of the disc, and that MMPs degrade the
extracellular matrix components of the disc. They indicated that in
other tissue types, MMP-19 was implicated in the proteolysis of
insulin-like growth factor (IGF) binding protein-3, thus exposing
this protein to make it available to influence cell behavior. They
also reported that MMP-19 inhibited capillary-like formation and
thus has a role in the avascular nature of the disc. They examined
normal discs obtained from subjects aged 0–10 years (n=6) and disc
samples obtained from control donors or surgical patients (n=20;
mean age, 40.2 years) for immunolocalization of MMP-19. They
classified the discs as Thompson grade I (n=6), II (n=5), III
(n=8), IV (n=5) and V (n=1) and analyzed them. The results
indicated that MMP-19 was uniformly localized in the outer AF
structure of discs from young subjects; however, MMP-19
localization was rarely observed in outer and inner AF cells in
discs from adult donors and surgical patients. In addition, the
highest expression of MMP-19 was observed in discs from younger
subjects, while it was low in disks from older subjects or
degenerating discs. They concluded that MMP-19 regulates
IGF-mediated proliferation in tissues other than discs and that
aging or degenerating discs may contribute to an age-associated
decreases in disc cell numbers (35).
Over the last two decades, it has been reported that
cytokines are produced by NP cells in the intervertebral disc
structure, mainly chondrocytes, histiocytes and fibroblasts
(36). IL-1β has been reported to
have a role in disc metabolism and to be the predominant
proinflammatory cytokine of the disc. The ability of IL-1β to
convert chondrocytes from featuring anabolic activity to catabolic
activity has been indicated (36).
In this manner, it causes degradation and increases angiogenetic
factors to facilitate angiogenesis. IL-1β increases proteoglycan
release and destructive enzymes (36). In addition, IL-1β stimulates the
release of pain mediators, including prostaglandin-E2, from
intervertebral disc cells. IL-1α has been reported to enhance the
synthesis of MMPs and nitric oxide, as well as directly increase
catabolism of disc proteoglycans, providing a basis for
degeneration. IL-1β has been reported to have a role in disc
metabolism and is the predominant proinflammatory cytokine of the
disc (36).
A recent study reported that IL-1β caused apoptosis
of AF cells and had negative effects on intervertebral disc tissue
cells (37). Rats were used as live
mammals in the study, and IL-1β induction was reported to
significantly reduce chondroitin sulfate glycosyltransferases-1/2/3
at the mRNA level in NP cells (37).
In addition, inflammatory cytokines including IL-1β stimulated
mRNA-194 and mRNA-515, targeted CHSY-1/2/3 mRNA and significantly
degraded translation and downstream chondroitin sulfate
accumulation in the mechanism of intervertebral disc degeneration
(38).
Therefore, proliferation and cytotoxicity analysis
were performed in the present study with the cell cultures of the
non-degenerate, intact intervertebral disc tissue after drug
administration. In addition, the levels of CHAD, COMP, MMP-7,
MMP-13, MMP-19 and IL-1β were examined and compared between the
non-drug-treated control groups and the dipyrone-treated groups.
This was to determine whether the cells isolated from the
non-degenerated intact intervertebral disc tissue were inclined to
degenerate after application of the active pharmacological agent
dipyrone.
The present study investigated whether dipyrone had
any cytotoxic effect on intact intervertebral disc tissue cells.
This situation was comparatively investigated in the untreated and
dipyrone-treated cultures. No acute cell death was observed, even
when a deterioration of the cell morphology was observed in the
dipyrone-treated samples during the experiments. However, a
suppression of cell proliferation was observed. Whether this was
associated with a poorly developing microenvironment was examined
by comparing the gene expression of CHAD and COMP with that of
MMP-19. CHAD and COMP proteins secreted from AF/NP cells constitute
the extracellular matrix and contribute to the formation of a
healthy microenvironment in the intervertebral disc tissue
(6,7,39). COMP is also important in cross-linking, along with other
extracellular matrix elements. MMP-19 is an enzyme that cleaves
COMP. IL-1β is an inflammatory cytokine that was increased during
the degeneration of intervertebral disc tissue cells. The increase
in IL-1β expression causes an increase in MMP-7 and MMP-13.
Therefore, the gene expression of MMP-7 and MMP-13, along with that
of IL-1β, was investigated to determine whether the degenerated
cell morphology may be indicative of degeneration.
In the present study, all the genes in the control
group and the β-actin gene (which was used as an internal control)
in the dipyrone-treated cultures, continued to be expressed.
Dipyrone-treated cultures were only obtained from 6 patients, which
serves as a limitation of the current study. Although analyses were
repeated to eliminate this limitation, gene expression in the
cultures were significantly low, which did not allow for their
detection via respective assays. Furthermore, the number of
patients could not be augmented due to the following reasons:
Difficulty in obtaining intact tissue from patients, a low number
of patients with spinal trauma from whom intact IVD tissue could be
extracted and difficulty in obtaining Ethics Committee approval and
written consent forms.
In the present study, cell proliferation in the
drug-treated group decreased compared with that in the untreated
control group. This indicated that the dipyrone agent had an
inhibitory effect on the intervertebral disc tissue cells (P≤0.05).
In addition, no gene expression, as was the case compared with the
untreated group at the same incubation time, was observed on the
tenth and twentieth day in the dipyrone-treated experimental
groups. The cells did not die through apoptosis or any other
mechanism but became senescent after dipyrone application; their
proliferation was suppressed and stopped. A clearer result may
therefore be drawn similar study on a larger number of
patients.
The most important limitation of the present study
was the fact that dipyrone is a prodrug and thus does not affect
the enzyme cyclooxygenase in vitro. Therefore, investigation
of the gene expression in living mammal subjects with an in
vivo experimental design or in the human body is of significant
importance. An in vivo study using an animal model is
required to immunohistochemically evaluate the expression of MMP
and proteins associated with apoptotic pathways.
Although no cell death was observed in the analyses
of AF/NP cells obtained from intact tissue on the twentieth day,
suppressed proliferation was present and the gene expression was
suppressed. For this reason, dipyrone, which is frequently used by
clinicians as an analgesic, anti-pyretic and anti-spasmodic, should
be applied with caution, since it may slow down the healing
process.
Acknowledgements
Not applicable.
Funding
No funding was received.
Availability of data and materials
The data and materials generated/analyzed in the
present study are available from the corresponding author on
reasonable request.
Authors' contributions
FA conceived and designed the current study, wrote
the manuscript, acquired patient data, analyzed and interpreted the
data, performed ELISA and performed microscopic evaluation. DS
analyzed and interpreted the data, prepared the human primary cell
culture and performed PCR analysis. IY and NuK prepared the human
primary cell culture, performed inverted light microscopy, analyzed
PCR results and prepared/stored dipyrone. HO, IY and NuK performed
statistical analysis and wrote the manuscript. ATS, YEK, NeK and YA
selected the patients who met the inclusion criteria and performed
statistical analyses. FSA, NuK, NeK, YA, TC and OA diagnosed and
performed patient, and removed tissue for laboratory analysis. OA,
HO, NuKa, DYS, IY, YEK and FSA prepared the manuscript and
critically revised it for important intellectual content. All
authors have read and approved the final version of the
manuscript.
Ethics approval and informed consent
The present study was approved by the ethics
committee of the Istanbul Medipol University School of Medicine
(Istanbul, Turkey). Written informed consent was obtained from all
subjects.
Patient consent for publication
Not applicable
Competing interests
The authors declare that they have no competing
interests.
References
|
1
|
Yilmaz I and Ulugol A: The effect of
nitric oxide synthase inhibitors on the development of analgesic
tolerance to dipyrone in mice. Int J Neurosci. 119:755–764. 2009.
View Article : Google Scholar : PubMed/NCBI
|
|
2
|
Garcia S, Canoniero M, Lopes G and Soriano
AO: Metamizole use among Hispanics in Miami: Report of a survey
conducted in a primary care setting. South Med J. 99:924–926. 2006.
View Article : Google Scholar : PubMed/NCBI
|
|
3
|
Dilmen OK, Akcil EF, Tunali Y, Karabulut
ES, Bahar M, Altindas F, Vehid H and Yentur E: Postoperative
analgesia for supratentorial craniotomy. Clin Neurol Neurosurg.
146:90–95. 2016. View Article : Google Scholar : PubMed/NCBI
|
|
4
|
Claros OR, Silva CH, Consolmagno H, Sakai
AT, Freddy R and Fugita OE: Current practices in the management of
patients with ureteral calculi in the emergency room of a
university hospital. Clinics (Sao Paulo). 67:415–418. 2012.
View Article : Google Scholar : PubMed/NCBI
|
|
5
|
Florentino IF, daSilva DP, Martins JL, da
Silva TS, Santos FC, Tonussi CR, Vasconcelos GA, Vaz BG, Lião LM,
Menegatti R and Costa EA: Pharmacological and toxicological
evaluations of the new pyrazole compound (LQFM-021) as potential
analgesic and anti-inflammatory agents. Inflammopharmacology.
24:265–275. 2016. View Article : Google Scholar : PubMed/NCBI
|
|
6
|
Sirin DY and Karaarslan N: Evaluation of
the effects of pregabalin on chondrocyte proliferation and CHAD,
HIF-1α, and COL2A1 gene expression. Arch Med Sci.
14:1340–1347. 2018. View Article : Google Scholar : PubMed/NCBI
|
|
7
|
Karaarslan N, Yilmaz I, Sirin DY, Ozbek H,
Kaplan N, Kaya YE, Akyuva Y, Gurbuz MS, Oznam K and Ates O: Does
pregabalin used in the treatment of neuropathic pain damage
intervertebral disc tissue? Exp Ther Med. 16:1259–1265.
2018.PubMed/NCBI
|
|
8
|
Pompeia C, Boaventura MF and Curi R:
Antiapoptotic effect of dipyroneon HL-60, Jurkat and Raji cell
lines submitted to UV irradiation, arachidonic acid and
cycloheximide treatments. Int Immunopharmacol. 1:2173–2182. 2001.
View Article : Google Scholar : PubMed/NCBI
|
|
9
|
Akyuva Y, Karaarslan N, Yilmaz I, Ozbek H,
Sirin DY, Gurbuz MS, Kaya YE, Kaplan N and Ates O: How scaffolds,
which are polymeric drug delivery systems allowing controlled
release, can be tested in human primary nucleus pulposus and
annulus fibrosus cell cultures? Merit Res J Med Med Sci. 5:477–487.
2017.
|
|
10
|
Silav G, Ergün H, Dolgun H, Sancak T,
Sargon MF and Egemen N: Dipyrone attenuates cerebral vasospasm
after experimental subarachnoid hemorrhage in rabbits. J Neurosurg
Sci. 61:380–387. 2017.PubMed/NCBI
|
|
11
|
Zhang Y, Wang X, Baranov SV, Zhu S, Huang
Z, Fellows-Mayle W, Jiang J, Day AL, Kristal BS and Friedlander RM:
Dipyrone inhibits neuronal cell death and diminishes
hypoxic/ischemic brain injury. Neurosurgery. 69:942–956. 2011.
View Article : Google Scholar : PubMed/NCBI
|
|
12
|
Grossman R, Ram Z, Perel A, Yusim Y,
Zaslansky R and Berkenstadt H: Control of postoperative pain after
awake craniotomy with local intradermal analgesia and metamizol.
Isr Med Assoc J. 9:380–382. 2007.PubMed/NCBI
|
|
13
|
Donaubauer HH, Kief H, Kramer M, Krief K,
Mayer D and Schütz E: Investigations on the carcinogenicity of
dipyrone in rats. Toxicol App Pharmacol. 81:443–451. 1985.
View Article : Google Scholar
|
|
14
|
Kramer M: Chronic toxicity of pyrazolones:
The problem of nitrosation. Br J Clin Pharmacol. 10 (Suppl
2):S313–S317. 1980. View Article : Google Scholar
|
|
15
|
Maj S and Lis Y: The incidence of
metamizole sodium-induced agranulocytosis Poland. J Int Med Res.
30:488–495. 2002. View Article : Google Scholar : PubMed/NCBI
|
|
16
|
Giorgi M, Aupanun S, Lee HK, Poapolathep
A, Rychshanova R, Vullo C, Faillace V and Laus F: Pharmacokinetic
profiles of the active metamizole metabolites in healthy horses. J
Vet Pharmacol Ther. 40:165–171. 2017. View Article : Google Scholar : PubMed/NCBI
|
|
17
|
Schütter AF, Tünsmeyer J and Kästner SB:
Influence of metamizole on 1) minimal alveolar concentration of
sevoflurane in dogs and 2) on thermal and mechanical nociception in
conscious dogs. Vet Anaesth Analg. 43:215–226. 2016. View Article : Google Scholar : PubMed/NCBI
|
|
18
|
Yaşar Şirin D, Yılmaz İ, İsyar M, Öznam K
and Mahiroğulları M: Does leukocyte-poor or leukocyte-rich
platelet-rich plasma applied with biopolymers have superiority to
conventional platelet-rich plasma applications on chondrocyte
proliferation? Eklem Hastalik Cerrahisi. 28:142–151. 2017.
View Article : Google Scholar : PubMed/NCBI
|
|
19
|
Bundscherer AC, Malsy M, Gruber MA, Graf
BM and Sinner B: Acetaminophen and metamizole induce apoptosis in
HT 29 and SW 480 colon carcinoma cell lines in vitro.
Anticancer Res. 38:745–751. 2018.PubMed/NCBI
|
|
20
|
Malsy M, Graf B and Bundscherer A: Effects
of metamizole, MAA, and paracetamol on proliferation, apoptosis,
and necrosis in the pancreatic cancer cell lines PaTu 8988 t and
Panc-1. BMC Pharmacol Toxicol. 18:772017. View Article : Google Scholar : PubMed/NCBI
|
|
21
|
Guzelant AY, Isyar M, Yilmaz İ, Sirin DY,
Cakmak S and Mahirogullari M: Are chondrocytes damaged when
rheumatologic inflammation is suppressed? Drug Chem Toxicol.
40:13–23. 2017. View Article : Google Scholar : PubMed/NCBI
|
|
22
|
Arkhipchuk VV, Goncharuk VV, Chernykh VP,
Maloshtan LN and Gritsenko IS: Use of a complex approach for
assessment of metamizole sodium and acetylsalicylic acid toxicity,
genotoxicity and cytotoxicity. J Appl Toxicol. 24:401–407. 2004.
View Article : Google Scholar : PubMed/NCBI
|
|
23
|
Rutges J, Creemers LB, Dhert W, Milz S,
Sakai D, Mochida J, Alini M and Grad S: Variations in gene and
protein expression in human nucleus pulposus in comparison with
annulus fibrosus and cartilage cells: potential associations with
aging and degeneration. Osteoarthritis Cartilage. 18:416–423. 2010.
View Article : Google Scholar : PubMed/NCBI
|
|
24
|
van den Akker GG, Surtel DA, Cremers A,
Richardson SM, Hoyland JA, van Rhijn LW, Voncken JW and Welting TJ:
Novel immortal cell lines support cellular heterogeneity in the
human annulus fibrosus. PLoS One. 11:01444972016. View Article : Google Scholar
|
|
25
|
Zhang YG, Guo X, Sun Z, Jia G, Xu P and
Wang S: Gene expression profiles of disc tissues and peripheral
blood mononuclear cells from patients with degenerative discs. J
Bone Miner Metab. 28:209–219. 2010. View Article : Google Scholar : PubMed/NCBI
|
|
26
|
Goode AP, Marshall SW, Kraus VB, Renner
JB, Stürmer T, Carey TS, Irwin DE and Jordan JM: Association
between serum and urine biomarkers and lumbar spine individual
radiographic features: The johnston county osteoarthritis project.
Osteoarthritis Cartilage. 20:1286–1293. 2012. View Article : Google Scholar : PubMed/NCBI
|
|
27
|
Yilmaz I, Gokay NS, Bircan R, Saracoglu
GV, Dervisoglu S and Gokce A: How different methodologies of
harvesting and analysing the samples affect the test results in
determining joint mediators. Arthritis. 2013:6319592013. View Article : Google Scholar : PubMed/NCBI
|
|
28
|
Gokay NS, Yilmaz I, Komur B, Demiroz AS,
Gokce A, Dervisoglu S and Gokay BV: A Comparison of the effects of
neuronal nitric oxide synthase and inducible nitric oxide synthase
inhibition on cartilage damage. Biomed Res Int. 2016:78573452016.
View Article : Google Scholar : PubMed/NCBI
|
|
29
|
Goupille P, Jayson MI, Valat JP and
Freemont AJ: Matrix metalloproteinases: The clue to intervertebral
disc degeneration? Spine (Phila Pa 1976). 23:1612–1626. 1998.
View Article : Google Scholar : PubMed/NCBI
|
|
30
|
Yurube T, Takada T, Suzuki T, Kakutani K,
Maeno K, Doita M, Kurosaka M and Nishida K: Rat tail static
compression model mimics extracellular matrix metabolic imbalances
of matrix metalloproteinases, aggrecanases, and tissue inhibitors
of metalloproteinases in intervertebral disc degeneration.
Arthritis Res Ther. 14:R512012. View
Article : Google Scholar : PubMed/NCBI
|
|
31
|
Weiler C, Nerlich AG, Zipperer J,
Bachmeier BE and Boos N: 2002 SSE Award Competition in Basic
Science: Expression of major matrix metalloproteinases is
associated with intervertebral disc degradation and resorption. Eur
Spine J. 11:308–320. 2002. View Article : Google Scholar : PubMed/NCBI
|
|
32
|
Roberts S, Caterson B, Menage J, Evans EH,
Jaffray DC and Eisenstein SM: Matrix metalloproteinases and
aggrecanase: Their role in disorders of the human intervertebral
disc. Spine (Phila Pa 1976). 25:3005–3013. 2000. View Article : Google Scholar : PubMed/NCBI
|
|
33
|
Sedlacek R, Mauch S, Kolb B, Schätzlein C,
Eibel H, Peter HH, Schmitt J and Krawinkel U: Matrix
metalloproteinase MMP-19 (RASI-1) is expressed on the surface of
activated peripheral blood mononuclear cells and is detected as an
autoantigen in rheumatoid arthritis. Immunobiology. 198:408–423.
1998. View Article : Google Scholar : PubMed/NCBI
|
|
34
|
NCBI, . Matrix metallopeptidase 19 [Homo
sapiens (human)]. https://www.ncbi.nlm.nih.gov/gene/4327March
3–2018
|
|
35
|
Gruber HE, Ingram JA and Hanley EN Jr:
Immunolocalization of MMP-19 in the human intervertebral disc:
Implications for disc aging and degeneration. Biotech Histochem.
80:157–162. 2005. View Article : Google Scholar : PubMed/NCBI
|
|
36
|
Nishida Y, D'Souza AL, Thonar EJ and
Knudson W: Stimulation of hyaluronan metabolism by
interleukin-1alpha in human articular cartilage. Arthritis Rheum.
43:1315–1326. 2000. View Article : Google Scholar : PubMed/NCBI
|
|
37
|
Hu B, Xu C, Tian Y, Shi C, Zhang Y, Deng
L, Zhou H, Cao P, Chen H and Yuan W: Inflammatory microRNA-194 and
−515 attenuate the biosynthesis of chondroitin sulfate during human
intervertebral disc degeneration. Oncotarget. 8:49303–49317.
2017.PubMed/NCBI
|
|
38
|
Lv FJ, Peng Y, Lim FL, Sun Y, Lv M, Zhou
L, Wang H, Zheng Z, Cheung KMC and Leung VYL: Matrix
metalloproteinase 12 is an indicator of intervertebral disc
degeneration co-expressed with fibrotic markers. Osteoarthritis
Cartilage. 24:1826–1836. 2016. View Article : Google Scholar : PubMed/NCBI
|