1. Introducing paediatric virology
Over the past three decades, scientific advances in
the field of clinical virology and molecular medicine have led to
significant changes in clinical practice regarding the management
and treatment of neonates and children with viral infections. These
advances have highlighted the role of paediatric virology as a new
unique challenging scientific area, where paediatric professionals
of the 21st century will require enhanced state-of-the-art
education. The new challenges related to the rapidly evolving world
of paediatric viral infections include new emerging infections
(e.g., SARS-CoV-2, Zika virus), re-emerging infections (e.g., Ebola
virus), opportunistic infections in immunocompromised patients
(e.g., CMV), the development of new and improved antivirals and
vaccines, antimicrobial resistance and the development of improved
diagnostic tests. In most countries, children with viral infections
are usually managed by general paediatricians or paediatric
infectious disease (PID) subspecialists assisted by microbiologists
or clinical virologists. Recently, paediatric virology was proposed
as a separate candidate for paediatric subspecialisation (1), while different educational pathways on
paediatric virology were presented by Mammas et al (2). The aim of the present article was to
review current practices in the UK giving examples of the existing
educational platforms and training options in paediatric virology,
which currently are offered to paediatric trainees wanting to
pursue a career in paediatric virology.
2. Subspecialty training in paediatric
infectious diseases and immunology
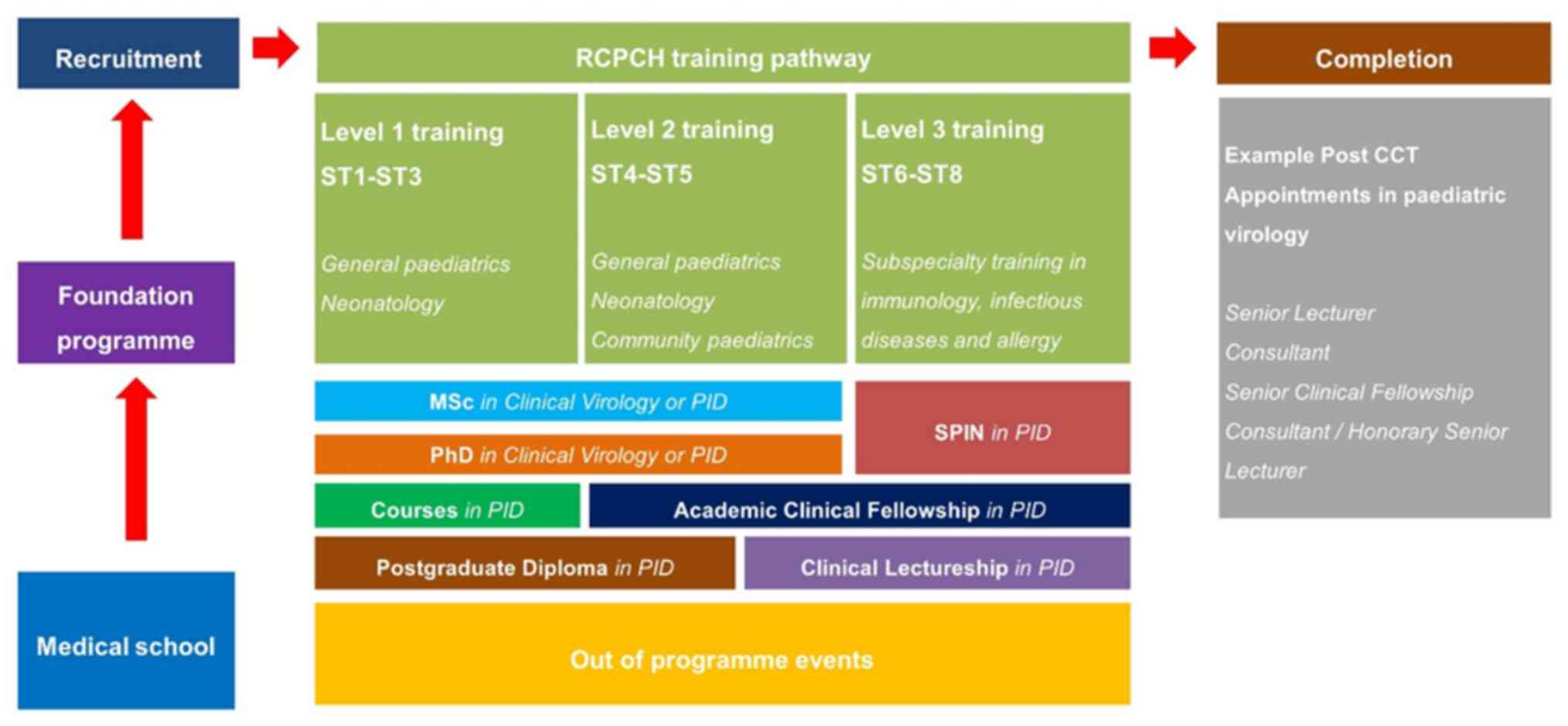
Training to become a consultant paediatrician in the
UK, currently, takes 8 years - specialty training (ST) years
1-8(3). To become a subspecialist
in paediatric infectious diseases - it is currently not possible to
become a subspecialist in paediatric virology alone - a trainee
must usually apply to enter the subspecialty training programme
(‘grid training’) in ST5 or ST6 to start in ST6 or ST7(4). Trainees, therefore, undertake 2 or 3
years of subspecialty training and ultimately will enter the
Specialist Register with the General Medical Council (GMC) as a
consultant paediatrician with a subspecialty interest in infectious
diseases. For those who do not wish to become subspecialists but
wish to develop further skills in a particular subspecialty there
is the opportunity to undertake a specialist interest (SPIN) module
(5). SPIN modules allow trainees to
undertake additional training and gain experience in a specific
area of paediatrics. The curriculum for the paediatric infectious
diseases SPIN module is currently under review. At present neither
PID Grid training nor the PID SPIN module allow for training in
paediatric virology as a separate subspecialty (Fig. 1).
It is also possible to undertake training in adult
medicine and subspecialise as a medical virologist (6). It is then possible to advise on the
diagnosis and management of viral infections in children although
not work as a paediatrician unless training in paediatrics is also
undertaken.
3. Doctorate, Masters, Postgraduate diploma
and Short courses
Another pathway to gain knowledge and experience in
paediatric viral infections is to undertake a higher degree,
diploma or short course on the topic. There are a number of
Doctorate (e.g., PhD or MD) or Masters (e.g., MSc) programmes run
by various institutions in the UK which paediatric trainees can
apply for. Examples of UK institutions that regularly fund Doctoral
or Masters students include the Wellcome Trust (https://wellcome.ac.uk/), the Medical Research Council
(MRC) (https://mrc.ukri.org/) and the National
Institute for Health Research (NIHR) (https://www.nihr.ac.uk/). Each of these allows
applications on many topics of medical research including viral
infections in children which can be undertaken in the UK or abroad.
Occasionally there are specific calls on topics related to
infections in children. Most UK universities also have regular or
ad hoc Doctorate or Masters posts than can be applied to.
The University of Oxford's postgraduate diploma in
paediatric infectious diseases (PgDip PID) (7) and MSc in paediatric infectious
diseases (8) are well-established
UK courses for paediatricians and other specialists with an
interest in paediatric infectious diseases. The PgDip PID covers a
wide range of topics including viral infections, such as congenital
infections, viral exanthem, respiratory viruses and HIV. The PENTA
Tr@inforPedHIV course (9) is undertaken as part of the diploma.
The MSc is open to students who have completed the PgDip PID and
can be undertaken on any topic of paediatric infection including
viral infections.
In addition, there are many short courses available
across the UK on platforms including face-to-face, online with or
without tutoring and massive online open courses (MOOC) on
paediatric infections including virology (Table I).
 | Table IExample of short courses available
across the UK on platforms including face-to-face, online with or
without tutoring and MOOC on paediatric infections including
virology. |
Table I
Example of short courses available
across the UK on platforms including face-to-face, online with or
without tutoring and MOOC on paediatric infections including
virology.
| Course title | Course provider | Type of course |
|---|
| Virology: Fundamental
Laboratory Techniques and Practices | Public Health
England | Face to face |
| COVID-19: Tackling
the Novel Coronavirus | London School of
Hygiene and Tropical Medicine | MOOC |
| Ebola in context:
Understanding transmission, Response and Control | London School of
Hygiene and Tropical medicine | Free online
course |
| Infectious diseases
and host defence | Imperial College
London | Face to face and
online |
| Hazards in Travel
Health | Liverpool School of
Tropical Medicine | Online course |
| Preventing the Zika
Virus: Understanding and Controlling the Aedes Mosquito | FutureLearn | MOOC |
| Maternal
Infections | Oxford Maternal and
Perinatal Health Institute (OMPHI) | Free online
course |
4. Other training pathways
It is possible to train in paediatric infectious
diseases outside the UK, either undertaking time out of programme
from the UK paediatrics training programme or training abroad and
then applying to enter the UK training programme or applying
directly for a consultant post. For those taking time out of the
programme for clinical training, this is often done as a clinical
fellowship (commonly 1-2 years). In theory, this can be done in any
country; however, Canada and Australia are common places for UK
paediatricians to go to due to their well-established paediatric
infectious diseases training programmes and the relative ease with
which UK doctors can obtain medical registration, work visas, etc.
(e.g., compared with the USA where USMLE exams need to be completed
prior to being able to work there). The time out of the programme
has to be approved by the appropriate UK authorities (e.g., local
paediatric deanery).
5. Future perspectives
An in-depth knowledge of paediatric virology is
essential for paediatricians with an interest in infectious
diseases. There are several avenues to obtain training on
paediatric virology although it does not currently exist as a
specific subspecialty in the UK. In light of recent
epidemics/pandemics of viral infections and an increased
understanding of the pathophysiology of viral infections in
children, it remains to be seen whether there will become a need
for paediatric virology to become a new, separate paediatric
subspecialty. The future contribution of the newly founded
Institute of Paediatric Virology in this direction is
essential.
Acknowledgements
This article is published in the context of the
foundation of the Institute of Paediatric Virology (IPV; https://paediatricvirology.org) based on the
island of Euboea (Greece), under the auspices of the World Academy
of Sciences (WAS) and the support of the Department of Clinical
Virology of the University of Crete School of Medicine and the
First Department of Paediatrics of the University of Athens School
of Medicine. We would like to thank all the members of the IPV for
their valuable comments and corrections.
Funding
No funding was received.
Availability of data and materials
Not applicable.
Authors' contributions
All authors (SBD, AMB and AG) contributed to the
conception and design of this manuscript, wrote the original draft,
edited and critically revised the manuscript, read and approved the
final manuscript.
Ethics approval and consent to
participate
Not applicable.
Patient consent for publication
Not applicable.
Competing interests
SBD is a consultant paediatrician and subspecialist
in paediatric infectious diseases and immunology, lectures and
examines on the University of Oxford's PgDip PID and MSc courses,
and is a Member of the Advisory Academic Board (AAB) of the
Institute of Paediatric Virology (IPV). AMB declares that she has
no competing interests. AG is Chair of the Advisory Academic Board
(AAB) of the IPV.
References
|
1
|
Mammas IN, Greenough A, Theodoridou M and
Spandidos DA: Paediatric Virology: A new paediatric subspecialty? A
proposal at the Workshop on Paediatric Virology, Athens, October
10, 2015. Exp Ther Med. 11:3–5. 2016.
|
|
2
|
Mammas IN, Greenough A, Theodoridou M and
Spandidos DA: Educational pathways in Paediatric Virology: Pros and
cons. Exp Ther Med. 18:3260–3262. 2019.
|
|
3
|
Royal College of Paediatrics and Child
Health (RCPCH): Current training pathway. RCPCH, 2020. urihttps://www.rcpch.ac.uk/resources/training-guide#current-training-pathwaysimplehttps://www.rcpch.ac.uk/resources/training-guide#current-training-pathway.
Last Updated September 8, 2020.
|
|
4
|
Royal College of Paediatrics and Child
Health (RCPCH): Sub-specialty training (GRID). RCPCH, 2020.
urihttps://www.rcpch.ac.uk/resources/training-guide#sub-specialty-training-gridsimplehttps://www.rcpch.ac.uk/resources/training-guide#sub-specialty-training-grid.
Last Updated September 8, 2020.
|
|
5
|
Royal College of Paediatrics and Child
Health (RCPCH): Special interests (SPIN) modules. RCPCH, 2020.
urihttps://www.rcpch.ac.uk/resources/training-guide#special-interests-spin-modulessimplehttps://www.rcpch.ac.uk/resources/training-guide#special-interests-spin-modules.
Last Updated September 8, 2020.
|
|
6
|
The Royal College of Pathologists:
Training in Virology. RCPath, 2020. urihttps://www.rcpath.org/discover-pathology/careers-in-pathology/train-to-work-in-pathology/training-in-virology.htmlsimplehttps://www.rcpath.org/discover-pathology/careers-in-pathology/train-to-work-in-pathology/training-in-virology.html.
|
|
7
|
University of Oxford: PGDip in Paediatric
Infectious Diseases. University of Oxford, 2020. urihttps://www.ox.ac.uk/admissions/graduate/courses/pgdip-paediatric-infectious-diseases?wssl=1simplehttps://www.ox.ac.uk/admissions/graduate/courses/pgdip-paediatric-infectious-diseases?wssl=1).
Last Updated September 1, 2020.
|
|
8
|
University of Oxford: MSc in Paediatric
Infectious Diseases. University of Oxford, 2020. urihttps://www.ox.ac.uk/admissions/graduate/courses/msc-paediatric-infectious-diseases?wssl=1simplehttps://www.ox.ac.uk/admissions/graduate/courses/msc-paediatric-infectious-diseases?wssl=1.
Last Updated September 1, 2020.
|
|
9
|
Penta: Training and education. Penta,
2020. urihttps://penta-id.org/education/trainforpedhiv/#:~:text=It%20is%20a%20training%20programme,learning%20with%20interactive%20residential%20coursessimplehttps://penta-id.org/education/trainforpedhiv/#:~:text=It%20is%20a%20training%20programme,learning%20with%20interactive%20residential%20courses.
|