Introduction
Rheumatoid arthritis (RA) is one of the most common
inflammatory autoimmune diseases in the world, and is mainly
characterized by synovitis and joint destruction, which ultimately
leads to disability. Approximately 1% of the worldwide population
suffers from RA (1). The exact
mechanism underlying RA pathogenesis remains unclear; however,
accumulating evidence has suggested that genetic and environmental
factors may be associated with the development of RA.
The pro-inflammatory cytokines IL-1β and IL-18 serve
vital roles in bone resorption and cartilage destruction in RA
(2). The NOD-, LRR- and pyrin
domain-containing protein 3 (NLRP3), which is a member of the nod
like receptor (NLR) family, contains a nucleotide-binding domain
(NOD), and is predominantly expressed in peripheral blood
leukocytes (3,4). In response to a variety of signals,
including pathogens and danger signals, NLRP3 rapidly forms NLRP3
inflammasome combined with the apoptosis-associated speck-like
protein (ASC) and the caspase-1 protease (5). As a result, the NLRP3 inflammasome
promotes ASC polymerization and activation of caspase-1, which in
turn induces the secretion of pro-inflammatory cytokines such as
IL-1β and IL-18, eventually leading to pyroptosis (6,7).
Previous evidence has also suggested that mutations in theNLRP3
gene maybe associated with the excessive release of IL-1β (8). Polymorphisms in the NLRP3 gene have
been associated with some common diseases such as type-1 diabetes,
inflammatory bowel disease and gout (9-11).
Furthermore, studies have demonstrated that mutations inNLRP3 may
be involved in the development of RA in different populations
(12-15).
In addition, Choulaki et al (16) revealed that NLRP3 was upregulated in
peripheral blood cells derived from patients with RA, thus
suggesting that NLRP3 could serve a crucial role in RA. However, to
the best of our knowledge, the association of NLRP3 polymorphisms
with susceptibility to RA in Chinese Han patients, and the
expression levels of NLRP3, ASC and caspase-1 in peripheral blood
mononuclear cells (PBMCs) and neutrophils have not yet been
investigated. Therefore, the current study aimed to investigate the
association between two common NLRP3 single-nucleotide
polymorphisms (SNPs) and RA in a case-control study. In addition,
the effect of these SNPs on NLRP3 expression was also evaluated.
Therefore, the NLRP3 mRNA expression levels were determined in
PBMCs and neutrophils from RA and healthy individuals.
Materials and methods
Patients
A total of 934 individuals were recruited from the
Second Hospital of Anhui Medical University, Anhui Province, China,
between August 2016 and March 2018. The main characteristics of the
patients included were shown in Table
I. Among them, 402 were diagnosed with RA and classified
according to the American Rheumatism Association 1987 revised
criteria (17). The inclusion
criteria for patients with RA were as follows: i) Definite
diagnosis of RA; ii) treated only with conventional
disease-modifying antirheumatic drugs such asmethotrexate or/and
leflunomide. The patients suffering from other
inflammatory/autoimmune diseases or cancer were excluded from the
present study. A total of 532 healthy individuals were included.
Exclusion criteria included if patients exhibited a different
inflammatory/autoimmune disease or cancer or had a family history
of RA. Blood samples from 532 age-, sex-, and residential
area-matched healthy subjects, who underwent a health check-up,
were collected. During this period, the expression of NLRP3, ASC
and caspase-1 were determined in 49 randomly selected RA cases,
including 32 active and 17 inactive patients and in 30 healthy
control individuals.
 | Table IThe basic characteristics of the 934
study cases. |
Table I
The basic characteristics of the 934
study cases.
| Characteristic | RA group (N=402) | Healthy control (N
=532) | P-value |
|---|
| Age (years), Mean ±
SD | 58.28±10.119 | 50.17±14.862 | >0.05 |
| Sex (n) | | | >0.05 |
|
Male | 79 | 128 | |
|
Female | 323 | 404 | |
| Disease duration,
(years), Mean ± SD | 13±0.8 | - | - |
| RF (n=402) | | | - |
|
Positive, n
(%) | 353 (87.8) | - | |
|
Negative, n
(%) | 49 (12.2) | - | |
| A-CCP (n=402) | | | - |
|
Positive, n
(%) | 369 (91.8) | - | |
|
Negative, n
(%) | 33 (8.2) | - | |
All clinical characteristics, including rheumatoid
factor (RF), anti-cyclic citrullinated peptide antibodies (A-CCP),
C-reactive protein (CRP), erythrocyte sedimentation rate (ESR),
disease activity score of 28 joint counts (DAS28) (18). Sex, age and disease duration were
recorded in detail. In patients with RA, DAS28 values of ≤2.6 and
>2.6 were considered to indicate inactive and active RA disease
(19). The current study protocol
was approved by the Ethics Committee of the Second Affiliated
Hospital of Anhui Medical University, and all experiments were
carried out in accordance with the declaration of Helsinki.
Finally, informed consent was obtained from all study participants
or their families if the patients were considered incapable of
providing consent.
SNP selection and genotyping
The SNPs rs4612666 and rs10754558 were selected due
to their involvement in other diseases, including gastric cancer
(20), type 1diabetes (9), inflammatory bowel disease (10) and primary gouty arthritis (11). The genomic DNA was isolated from 1
ml of peripheral blood using the AxyPrep DNA Purification kit
(Axygen; Corning, Inc). The primers designed were as follows:
rs4612666 forward-5'-TGGAGTTTCAGTTCTGCAAG-3' and reverse
5'-ATGGACAAGGAAGCACCCG-3'; rs10754558 forward
5'-TTGAGCCTTCTTGGTAGGAGTGG-3' and reverse
5'-GAATAGAAAGATAGCGGGAATG-3'. The PCR amplification in Sanger
sequencing was performed in a 30 µl volume solution which contained
15 µl 2x Green Master Mix, 0.5 µl genomic DNA, 0.75 µl of each
primer and 13 µl Nuclease-Free Water. The conditions of PCR were as
follows: Initial denaturation at 95˚C for 5 min, followed by 35
cycles at 95˚C for 15 sec, with annealing at 50˚C for 30 sec and
extension at 72˚C for 30 sec, followed by a final extension at 72˚C
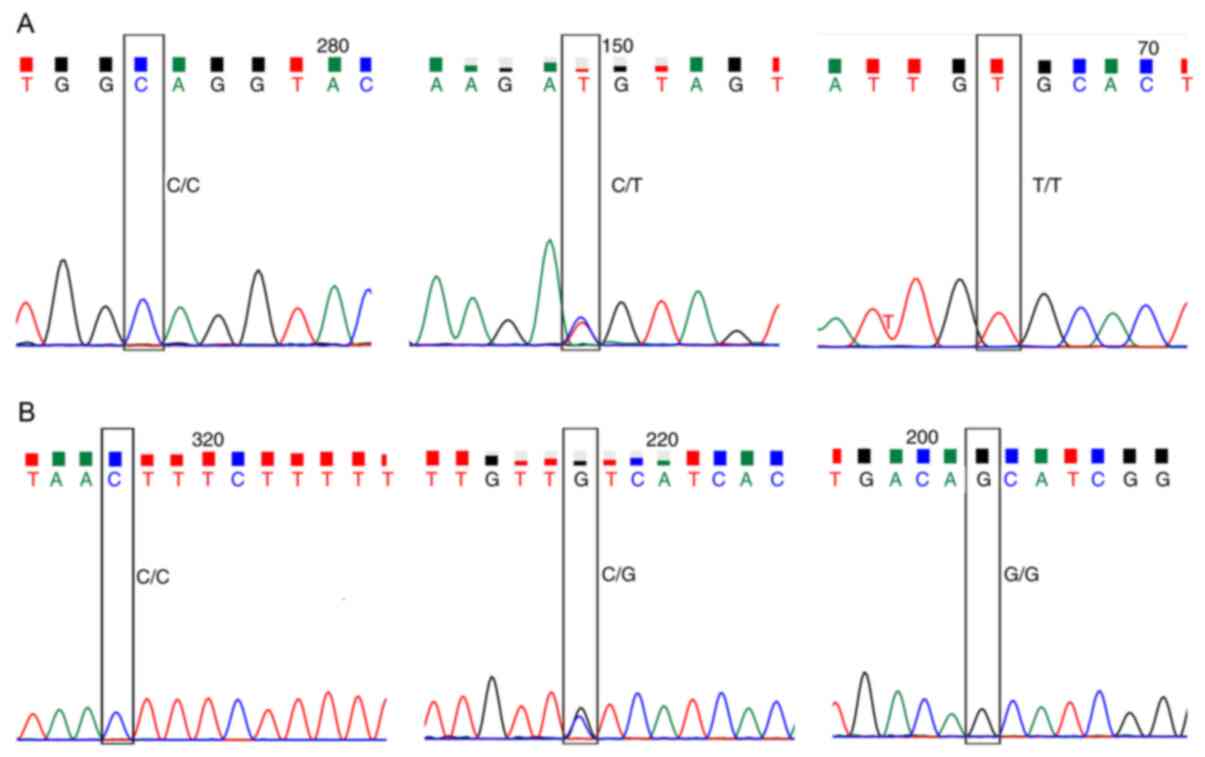
for 10 min with 1 cycle. The genotyping of NLRP3 rs4612666 and
rs10754558 was conducted using direct sequencing. The results were
analyzed with chromas software (version2.6; Technelysium Pty Ltd)
to identify possible mutations. The results are presented in
Fig. 1.
Reverse transcription-quantitative PCR
(RT-qPCR)
PBMCs and neutrophils of 49 patients with RA and 30
healthy controls were separated using density-gradient
centrifugation (Beijing Solarbio Science & Technology Co.,
Ltd.) that was performed at 400 x g for 20 min at 20˚C and at 500 x
g for 35 min at 20˚C, respectively. Total RNA was extracted from
PBMCs and neutrophils using Trizol® reagent (Invitrogen;
Thermo Fisher Scientific, Inc.). Subsequently, RNA was reverse
transcribed into complementary (c)DNA using the Prime Script RT
reagent kit (Takara Biotechnology Co., Ltd.) according to the
manufacturer's protocol. The specific primer sequences are
presented in Table II. RT-PCR was
carried out in a 20 µl reaction volume comprising of 1.6 µl primers
(0.8 µl forward primer and reverse primer), 2 µl cDNA, 0.4 µl ROX
Reference dye II, 6 µld H2O and 10 µl SYBR Premix Ex
Taq™II. The conditions of PCR were as follows: Initial denaturation
at 95˚C for 15 min, 94˚C for 30 sec, 59˚C for 60 sec, 72˚C for 1
min then 40 cycles and a final extension at 72˚C for 7 min. All the
samples were amplified at the same site on ABI 7500 real-time
polymerase chain reaction system (Applied Biosystems; Thermo Fisher
Scientific, Inc). The expression levels of NLRP3, ASC and caspase-1
were calculated using the 2-ΔΔCq method (21).
 | Table IIPrimers used for reverse-transcription
quantitative PCR. |
Table II
Primers used for reverse-transcription
quantitative PCR.
| Genes | Primer sequence |
|---|
| β-actin | |
|
Forward |
5'-TGGCACCCAGCACAATGAA-3' |
|
Reverse |
5'-CTAAGTCATAGTCCGCCTAGAAGCA-3' |
| NLRP3 | |
|
Forward |
5'-CTCTAGCTGTTCCTGAGGCTG-3' |
|
Reverse |
5'-TTAGGCTTCGGTCCACACAG-3' |
| ASC | |
|
Forward |
5'-TCCTCAGTCGGCAGCCAAG-3' |
|
Reverse |
5'-CCTTCCCGTACAGAGCATCC-3' |
| Caspase-1 | |
|
Forward |
5'-GCCTGTTCCTGTGATGTGGA-3' |
|
Reverse |
5'-CTTCACTTCCTGCCCACAGA-3' |
Statistical analysis
Statistical analyses were performed using SPSS 10.0
software (SPSS Inc.). An exact χ2 test was applied to
assess Hardy-Weinberg equilibrium (HWE). A χ2 test or a
Fisher exact test was used to compare genotype and allele
frequencies between patients and controls. The association between
NLRP3 SNPs, rs4612666 and rs10754558 and RA were assessed by odds
ratio and 95% confidence intervals using logistic regression
analyses. Dominant and recessive models were also used for
statistical analysis, including the dominant model (for isolated
SNPs: Homozygote rare + heterozygote vs. homozygote common) and
recessive mode (for isolated SNPs: Homozygote rare vs. heterozygote
+ homozygote common). A non-parametric Kruskal-Wallis test was
performed to compare the expression of NLRP3, ASC, and caspase-1
between groups. Furthermore, Spearman's correlation analysis was
applied to analyze correlations between NLRP3 expression and
clinical data. P<0.05 was considered to indicate a statistically
significant difference.
Results
Clinical characteristics of the study
population
The clinical and baseline characteristics of
patients and controls (n=934) are summarized in Table I. The RA and control groups were
matched based on age and sex (P>0.05).
Prevalence of NLRP3 alleles and
genotypes in patients with RA and controls
The rs4612666 and rs10754558 SNPs were in HWE in
controls (P=0.930 and 0.086, respectively), the details are
presented in Table III. As
presented in Table IV, regarding
the NLRP3 rs4612666 polymorphism, individuals carrying the C allele
exhibited a significantly increased risk for RA (OR=1.204; 95%
CI=1.002-1.447; P=0.047). A statistical significance was also
revealed in the dominant model (CC + CT vs. TT:OR=1.549; 95%
CI=1.120-2.144; P=0.008), but not in the recessive model (CC vs. CT
+ TT: OR=1.119; 95% CI=0.834-1.501; P=0.454). Furthermore,
significant differences in NLRP3 rs10754558 genotype distribution
was observed between RA and control individuals, while the G allele
was positively correlated with RA risk compared with the C allele
(OR=1.515; 95% CI 1.250-1.835; P<0.001). Additionally,
significant differences were obtained in the dominant model (GG +
GC vs. CC: OR=2.000; 95% CI=1.529-2.616; P<0.001), whereas no
discrepancy was observed in the recessive model (GG vs. CC + GC:
OR=1.244; 95% CI=0.839-1.845; P=0.277). The logistic regression
analyses demonstrated the rs4612666 and rs10754558 loci were
independent risk factors for the development of RA.
 | Table IIIPrimary information of two nucleotide
polymorphisms of NLRP3. |
Table III
Primary information of two nucleotide
polymorphisms of NLRP3.
| | MAF | |
|---|
| SNP | Alleles | Patients | Control | P-value for HWE in
controls |
|---|
| rs4612666 | C/T | 0.450 | 0.392 | 0.930 |
| rs10754558 | G/C | 0.403 | 0.308 | 0.086 |
 | Table IVAllele and genotype frequencies of
rs4612666 and rs10754558 in patients with RA and healthy
controls. |
Table IV
Allele and genotype frequencies of
rs4612666 and rs10754558 in patients with RA and healthy
controls.
| SNP and
genotype | RA (n=402) n
(%) | Controls (n=532) n
(%) | χ2 | OR (95% CI) | P-values |
|---|
| rs4612666 | | | | | |
|
CC | 110 (27.36) | 134 (25.19) | 7.057 | N/A | 0.029 |
|
CT | 222 (55.22) | 267 (50.19) | | | |
|
TT | 70 (17.41) | 131 (24.62) | | | |
|
C | 442 (54.98) | 535 (60.78) | 3.929 | 1.204
(1.002-1.447) | 0.047 |
|
T | 362 (45.02) | 529 (39.22) | | Reference | |
| Dominant model | | | | | |
|
CC + CT | 332 (82.6) | 401 (75.4) | 7.050 | 1.549
(1.120-2.144) | 0.008 |
|
TT | 70 (17.4) | 131 (24.6) | | Reference | |
| Recessive
model | | | | | |
|
CC | 110 (27.4) | 134 (25.2) | 0.561 | 1.119
(0.834-1.501) | 0.454 |
|
CT + TT | 292 (72.6) | 398 (74.8) | | Reference | |
| rs10754558 | | | | | |
|
GG | 54 (13.43) | 59 (11.09) | 34.879 | N/A | P<0.001 |
|
GC | 216 (53.73) | 210 (39.47) | | | |
|
CC | 132 (32.83) | 263 (49.44) | | | |
|
G | 324 (40.30) | 328 (30.83) | 18.081 | 1.515
(1.250-1.835) | P<0.001 |
|
C | 480 (59.70) | 736 (69.17) | | Reference | |
| Dominant model | | | | | |
|
GG + GC | 270 (67.2) | 269 (50.6) | 25.854 | 2.000
(1.529-2.616) | P<0.001 |
|
CC | 132 (32.8) | 263 (49.4) | | Reference | |
| Recessive
model | | | | | |
|
GG | 54 (13.4) | 59 (11.1) | 1.182 | 1.244
(0.839-1.845) | 0.277 |
|
CC + GC | 348 (86.6) | 473 (88.9) | | Reference | |
| rs4612666 | | | | | P<0.001 |
|
CC | 110 (27.36) | 134 (25.19) | 73.341 | Reference | |
|
CT | 222 (55.22) | 267 (50.19) | | | |
|
TT | 70 (17.41) | 131 (24.62) | | | |
| rs10754558 | | | | | P<0.001 |
|
GG | 54 (13.43) | 59 (11.09) | 83.916 | Reference | |
|
GC | 216 (53.73) | 210 (39.47) | | | |
|
CC | 132 (32.83) | 263 (49.44) | | | |
Association between NLRP3 mRNA
expression and SNPs in PBMCs and neutrophils from patients with
RA
No significant differences were observed between the
rs4612666 and rs10754558 genotypes and NLRP3 mRNA expression in
PBMCs and neutrophils (P>0.05; Table
V).
 | Table VNLRP3 mRNA expression of
PBMCs/neutrophils indifferent genotypes of rs4612666 and rs10754558
in patients with RA. |
Table V
NLRP3 mRNA expression of
PBMCs/neutrophils indifferent genotypes of rs4612666 and rs10754558
in patients with RA.
| A, PBMCs | | | |
|---|
| Genotype | Number | M (P25,P75) | P-value |
| rs4612666 | | | 0.811 |
|
CC | 12 | 0.980
(0.665,1.320) | |
|
CT | 26 | 0.930
(0.790,1.115) | |
|
TT | 11 | 0.855
(0.773,1.240) | |
| rs10754558 | | | 0.077 |
|
GG | 9 | 1.180
(0.870,1.260) | |
|
CG | 21 | 0.830
(0.720,1.130) | |
|
CC | 19 | 0.930
(0.825,1.183) | |
| B, Neutrophils | | | |
| Genotype | Number | M (P25,P75) | P-value |
| rs4612666 | | | 0.187 |
|
CC | 12 | 1.260
(0.945,1.573) | |
|
CT | 26 | 0.945
(0.795,1.280) | |
|
TT | 11 | 0.950
(0.785,1.510) | |
| rs10754558 | | | 0.424 |
|
GG | 9 | 1.070
(0.950,2.350) | |
|
CG | 21 | 1.000
(0.820,1.335) | |
|
CC | 19 | 0.850
(0.740,1.430) | |
NLRP3, ASC and caspase-1 mRNA
expression in PBMCs and neutrophils from patients with RA and
healthy controls
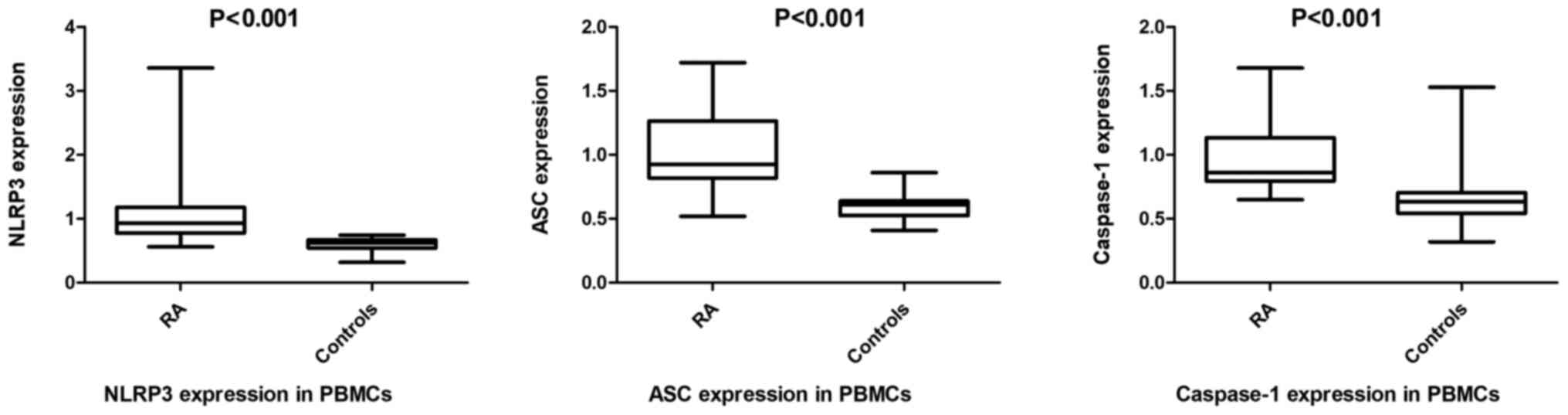
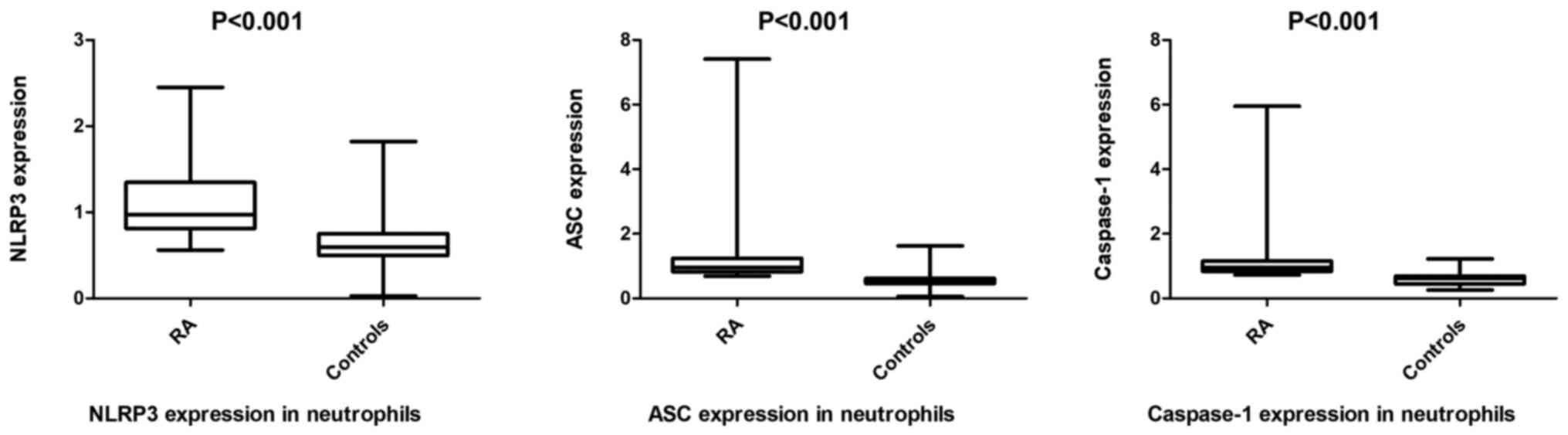
As presented in Figs.
2 and 3, the mRNA expression of
NLRP3, ASC and caspase-1 were upregulated in PBMCs [0.93
(0.78-1.18) vs. 0.62 (0.54-0.67); 0.93 (0.82-1.27) vs. 0.61
(0.53-0.64); 0.86 (0.80-1.14) vs. 0.64 (0.54-0.71), respectively]
and neutrophils [0.97 (0.81-1.35) vs. 0.60 (0.50, 0.75); 0.95
(0.83-1.24) vs. 0.52 (0.47-0.62); 0.95 (0.84-1.16) vs. 0.62
(0.45-0.69), respectively] of patients with RA compared with
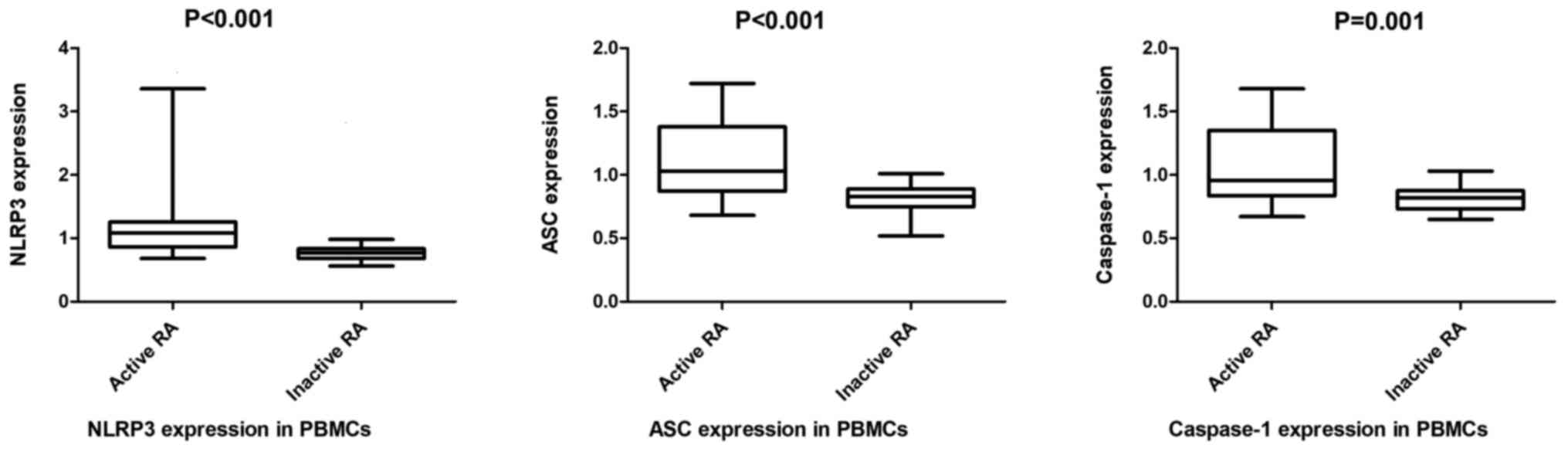
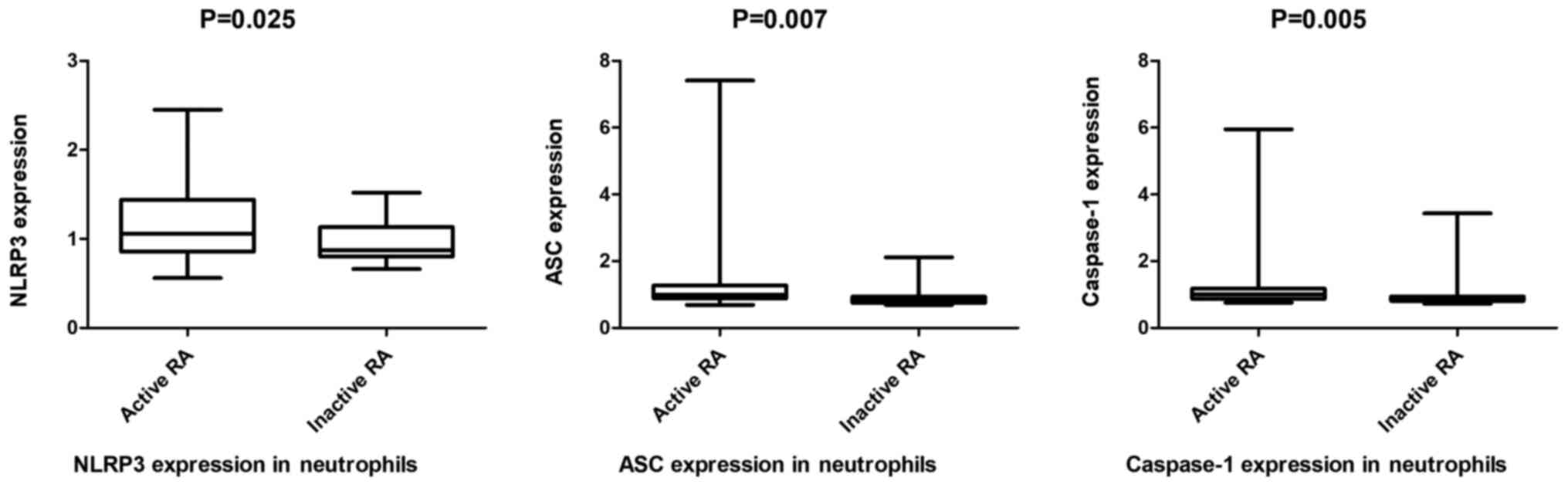
healthy individuals (all P<0.001. Furthermore, the NLRP3, ASC
and caspase-1 mRNA levels in PBMCs [1.09 (0.86-1.26) vs. 0.78
(0.68-0.86); 1.03 (0.87-1.38) vs. 0.83 (0.75-0.89); 0.96
(0.84-1.35) vs. 0.82 (0.73-0.88)] and neutrophils [1.12
(0.94-1.47)] vs. 0.87 (0.80-1.14); 0.99 (0.88-1.28) vs. 0.84
(0.75-0.94); 1.00 (0.87-1.18) vs. 0.87 (0.81-0.95)] from patients
with active RA were significantly increased compared with those
with inactive RA (all P<0.05; Figs.
4 and 5).
Correlation between the expression of
NLRP3 and clinical data
The basic clinical and laboratory parameters are
listed in Table VI. As presented
in Table VII, the NLRP3
expression in PBMCs and neutrophils were significantly correlated
with ESR, CRP and DAS28 (P<0.05). No correlation was observed
between the expression of NLRP3 and RF, A-CCP and disease course
(P>0.05).
 | Table VIThe basic clinical and laboratory
parameters of 49 patients with RA. |
Table VI
The basic clinical and laboratory
parameters of 49 patients with RA.
| Parameter | RA group
(n=49) | Healthy control
(n=30) |
|---|
| Age (years), mean ±
SD | 44.6±13.2 | 45.17±14.86 |
| Sex | | |
|
Male | 10 | 8 |
|
Female | 39 | 22 |
| Disease duration,
years, M (P25, P75) | 4.6 (1.2,18.1) | - |
| ESR (mm/h), mean ±
SD | 38.90±27.50 | - |
| CRP (mg/l), M (P25,
P75) | 13.0
(4.18,32.0) | - |
| DAS28, mean ±
SD | 4.13±1.80 | - |
| RF (IU/ml), M (P25,
P75) | 112.50
(54.18,277.7) | - |
| A-CCP (RU/ml), mean
± SD | 549.69±302.10 | - |
 | Table VIICorrelations between the expression
of NLRP3 at mRNA levels of PBMCs/neutrophils and clinical data. |
Table VII
Correlations between the expression
of NLRP3 at mRNA levels of PBMCs/neutrophils and clinical data.
| Expression | CRP | ESR | RF | A-CCP | DAS28 | Course |
|---|
| NLRP3 mRNA
(PBMCs) | | | | | | |
|
ρ-value | 0.501 | 0.494 | 0.206 | 1.000 | 0.498 | -0.103 |
|
P-value | <0.001 | <0.001 | 0.159 | 0.999 | <0.001 | 0.485 |
| NLRP3 mRNA
(neutrophils) | | | | | | |
|
ρ-value | 0.372 | 0.416 | 0.068 | 0.057 | 0.007 | 0.378 |
|
P-value | 0.008 | 0.003 | 0.641 | 0.696 | 0.007 | 0.378 |
Discussion
RA is an autoimmune disease that is characterized by
chronic inflammation and joint pain (22). Abundant evidence has shown that
inflammasome is activated by its ligands, resulting in
abnormalities of the immune system (23). Currently, it is widely considered
that the inflammasomes, especially the NLRP3/ASC/caspase-1 pathway,
are involved in the pathogenesis of several diseases, including RA
(24). It is widely accepted that
the NLRP3 inflammasome is highly expressed in monocytes and
macrophages in response to inflammatory stimuli (12,15,16,24,25). A
number of studies on gout, ischemia reperfusion injury and renal
tubule injury have demonstrated that the mRNA expression of the
NLRP3 inflammasome were upregulated; therefore, NLRP3 is thought to
exert a vital role in the pathogenesis of these diseases (26-28).
A number of studies have also demonstrated that NLRP3 is
upregulated in RA and have further suggested that NLRP3
inflammasome may serve an essential role in RA pathogenesis
(13,15,16,24,25).
It has been previously reported that mutations in the NLRP3 gene
serve an indispensable role in a number of diseases, and previous
studies have suggested that polymorphisms may affect gene
expression (9-11,20).
An increasing number of studies have shown RA
symptoms may be improved following suppression of the NLRP3 pathway
that might suggest the NLRP3 pathway serves an important role in
the severity of RA (29,30). It has also been proposed that NLRP3
may be a promising therapeutic target in autoimmune diseases,
including RA (31). The
aforementioned studies indicated that the NLRP3 signaling pathway
could serve a major role in the pathogenesis of RA and provided a
therapeutic approach for its treatment.
Only a few studies have been conducted in PBMCs and
neutrophils. Taken together, the results of the present study
suggested that SNPs in the NLRP3 inflammasome, and NLRP3 expression
maybe involved in the pathogenesis of RA. Therefore, to the best of
our knowledge, the current case-control study was the first to
reveal the association between NLRP3 rs4612666 and rs10754558 SNPs
and RA susceptibility in Chinese Han population. The expression of
NLRP3, ASC and caspase-1 in PBMCs and neutrophils were compared
between RA cases and controls.
In agreement with previous reports, the current
study identified a significant association between the variant
genotypes rs4612666 and rs10754558, and RA risk in Chinese Han
individuals. Furthermore, the C and the G allele of the rs4612666
and rs10754558 SNPs, respectively, were highly associated with RA,
indicating an increased susceptibility to RA. Logistic regression
analysis further indicated that the NLRP3 rs10754558 and rs4612666
SNPs were considered to be independent prognostic factors for RA.
However, the study failed to reveal any correlation between the
rs4612666 and rs10754558 mutations and the NLRP3 mRNA expression
levels in both PBMCs and neutrophils from patients with RA. This
may be due to other susceptible polymorphisms in the NLRP3 gene,
which may affect its expression.
When NLRP3 expression was compared between patients
with RA and healthy individuals, NLRP3 was only revealed to be
upregulated in PBMCs and neutrophils from patients with RA. In
addition, the mRNA levels of other components of the NLRP3 pathway
such as ASC and caspase-1 were also upregulated in both cell types.
When the mRNA levels were compared between patients with active and
inactive RA, ASC and caspase-1 levels were increased in patients
with active RA compared with those in patients in remission in both
cell types. These findings were consistent with previous reports
(13,15,16,24,25),
further supporting the importance of the NLRP3/ASC/caspase-1
pathway. Furthermore, a positive correlation between NLRP3 mRNA
expression and DAS28/CRP/ESR was also observed in patients with RA,
suggesting that the NLRP3 inflammasome maybe closely associated
with RA activity. It was suggested that DAS28, CRP and ESR in
patients with RA could be decreased by inhibiting the NLRP3
pathway, which was mainly based on the results of previously
published articles that demonstrated that RA symptoms might be
improved following inhibition of the NLRP3 pathway (29,30).
However, further research would be required to confirm the
association of the severity of RA and the NLRP3 pathway.
Nevertheless, no clear association was observed between NLRP3
expression and autoantibody levels, including RF and A-CCP. Overall
the aforementioned findings indicated that the expression of the
NLRP3 inflammasome-related genes (NLRP3, ASC and caspase-1) in
PBMCs may serve a critical role and be associated with RA
pathogenesis and disease activity.
To the best of our knowledge, the current study was
the first to demonstrate that the NLRP3 polymorphisms (rs4612666
and rs10754558) were associated with susceptibility to RA in
Chinese Han population by investigating the expression of NLRP3
inflammasome in PBMCs and neutrophils from patients with RA and
healthy controls. However, the present study has some limitations
that should be addressed in future research. Firstly, the selection
bias was unavoidable as this was a case-control study. Secondly,
the sample size was not large enough, which might be underpowered
to detect a weak association, Thirdly, unknown factors, which were
not investigated, could be also involved in theNLRP3/ASC/caspase-1
pathway. The aforementioned limitations could explain the
relatively small OR value indicated in the NLRP3 rs10754558 C
allele and the P value of ~0.05. Additionally, only two
polymorphisms (rs4612666 and rs10754558) were investigated.
Therefore, further clinical and genetic studies on the NLRP3
pathway are required to elaborate the association between NLRP3 and
RA.
In summary, the present study revealed a significant
association between NLRP3 rs4612666 and rs10754558 SNPs and the
risk of RA in a Chinese population. Furthermore, increased
expressions of the NLRP3 inflammasome were detected in PBMCs and
neutrophils from patients with RA. These findings provide a novel
genetic mechanism that maybe involved in the activation of the
NLRP3 inflammasome pathway and may be used as an effective
treatment for RA.
Acknowledgements
Not applicable.
Funding
Funding: The current study was supported by The Scientific
Research Project for Academic and Technical Leaders, Anhui, China
(grant no. 2017H143) and The Linkage Projects of Public Welfare
Technology Application Research, Anhui, China (grant no.
1704f0804024).
Availability of data and materials
The datasets used and/or analyzed during the current
study are available from the corresponding author on reasonable
request.
Authors' contributions
LQ conceived and designed the experiment(s). LC
performed the experiments, contributed to the analysis and drafted
the manuscript. XL and DL helped to conduct the experiment(s), CL
analyzed the results. All authors read and approved the final
manuscript.
Ethics approval and consent to
participate
The Ethical Committee of the second Affiliated
Hospital of Anhui Medical University (Hefei, China) approved the
study protocol. All experiments were performed in accordance with
relevant guidelines and regulations of the Declaration of Helsinki.
Informed consent was obtained from all the participants or their
families if the patients were incapable of giving consent.
Patient consent for publication
Not applicable.
Competing interests
The authors declare that they have no competing
interests.
References
|
1
|
Sangha O: Epidemiology of rheumatic
disease. Rheumatology (Oxford). 39 (Suppl 2):S3–S12.
2000.PubMed/NCBI View Article : Google Scholar
|
|
2
|
Joosten LA, Helsen MM, Saxne T, van De Loo
FA, Heinegard D and van Den Berg WB: IL-1 alpha beta blockade
prevents cartilage and bone destruction in murine type II
collagen-induced arthritis, whereas TNF-alpha blockade only
ameliorates joint inflammation. J Immunol. 163:5049–5055.
1999.PubMed/NCBI
|
|
3
|
Haneklaus M, O'Neill LA and Coll RC:
Modulatory mechanisms controlling the NLRP3 inflammasome in
inflammation: Recent developments. Curr Opin Immunol. 25:40–45.
2013.PubMed/NCBI View Article : Google Scholar
|
|
4
|
Bauernfeind F, Rieger A, Schildberg FA,
Knolle PA, Schmid-Burgk JL and Hornung V: NLRP3 inflammasome
activity is negatively controlled by miR-223. J Immunol.
189:4175–4181. 2012.PubMed/NCBI View Article : Google Scholar
|
|
5
|
Zhong Z, Sanchez-Lopez E and Karin M:
Autophagy, NLRP3 inflammasome and autoinflammatory/immune diseases.
Clin Exp Rheumatol. 34 (4 Suppl 98):S12–S16. 2016.PubMed/NCBI
|
|
6
|
Jo EK, Kim JK, Shin DM and Sasakawa C:
Molecular mechanisms regulating NLRP3 inflammasome activation. Cell
Mol Immunol. 13:148–159. 2016.PubMed/NCBI View Article : Google Scholar
|
|
7
|
Martinon F, Mayor A and Tschopp J: The
inflammasomes: Guardians of the body. Annu Rev Immunol. 27:229–265.
2009.PubMed/NCBI View Article : Google Scholar
|
|
8
|
Verma D, Lerm M, Blomgran Julinder R,
Eriksson P, Söderkvist P and Särndahl E: Gene polymorphisms in the
NALP3 inflammasome are associated with interleukin-1 production and
severe inflammation: Relation to common inflammatory diseases?
Arthritis Rheum. 58:888–894. 2008.PubMed/NCBI View Article : Google Scholar
|
|
9
|
Pontillo A, Brandao L, Guimaraes R, Segat
L, Araujo J and Crovella S: Two SNPs in NLRP3 gene are involved in
the predisposition to type-1 diabetes and celiac disease in a
pediatric population from northeast Brazil. Autoimmunity.
43:583–589. 2010.PubMed/NCBI View Article : Google Scholar
|
|
10
|
Bank S, Julsgaard M, Abed OK, Burisch J,
Broder Brodersen J, Pedersen NK, Gouliaev A, Ajan R, Nytoft
Rasmussen D, Honore Grauslund C, et al: Polymorphisms in the NFkB,
TNF-alpha, IL-1beta, and IL-18 pathways are associated with
response to anti-TNF therapy in Danish patients with inflammatory
bowel disease. Aliment Pharmacol Ther. 49:890–903. 2019.PubMed/NCBI View Article : Google Scholar
|
|
11
|
Zhang QB, Qing YF, He YL, Xie WG and Zhou
JG: Association of NLRP3 polymorphisms with susceptibility to
primary gouty arthritis in a Chinese Han population. Clin
Rheumatol. 37:235–244. 2018.PubMed/NCBI View Article : Google Scholar
|
|
12
|
Kastbom A, Verma D, Eriksson P, Skogh T,
Wingren G and Söderkvist P: Genetic variation in proteins of the
cryopyrin inflammasome influences susceptibility and severity of
rheumatoid arthritis (the Swedish TIRA project). Rheumatology
(Oxford). 47:415–417. 2008.PubMed/NCBI View Article : Google Scholar
|
|
13
|
Mathews RJ, Robinson JI, Battellino M,
Wong C and Taylor JC: Biologics in Rheumatoid Arthritis Genetics
and Genomics Study Syndicate (BRAGGSS). Eyre S, Churchman SM,
Wilson AG, Isaacs JD, et al: Evidence of NLRP3-inflammasome
activation in rheumatoid arthritis (RA); genetic variants within
the NLRP3-inflammasome complex in relation to susceptibility to RA
and response to anti-TNF treatment. Ann Rheum Dis. 73:1202–1210.
2014.PubMed/NCBI View Article : Google Scholar
|
|
14
|
Ben Hamad M, Cornelis F, Marzouk S,
Chabchoub G, Bahloul Z, Rebai A, Fakhfakh F, Ayadi H,
Petit-Teixeira E and Maalej A: Association study of CARD8 (p.C10X)
and NLRP3 (p.Q705K) variants with rheumatoid arthritis in French
and Tunisian populations. Int J Immunogenet. 39:131–136.
2012.PubMed/NCBI View Article : Google Scholar
|
|
15
|
Addobbati C, da Cruz HLA, Adelino JE, Melo
Tavares Ramos AL, Fragoso TS, Domingues A, Branco Pinto Duarte ÂL,
Oliveira RDR, Louzada-Júnior P, Donadi EA, et al: Polymorphisms and
expression of inflammasome genes are associated with the
development and severity of rheumatoid arthritis in Brazilian
patients. Inflamm Res. 67:255–264. 2018.PubMed/NCBI View Article : Google Scholar
|
|
16
|
Choulaki C, Papadaki G, Repa A, Kampouraki
E, Kambas K, Ritis K, Bertsias G, Boumpas DT and Sidiropoulos P:
Enhanced activity of NLRP3 inflammasome in peripheral blood cells
of patients with active rheumatoid arthritis. Arthritis Res Ther.
17(257)2015.PubMed/NCBI View Article : Google Scholar
|
|
17
|
Arnett FC, Edworthy SM, Bloch DA, McShane
DJ, Fries JF, Cooper NS, Healey LA, Kaplan SR, Liang MH, Luthra HS,
et al: The American Rheumatism Association 1987 revised criteria
for the classification of rheumatoid arthritis. Arthritis Rheum.
31:315–324. 1988.PubMed/NCBI View Article : Google Scholar
|
|
18
|
Prevoo ML, van 't Hof MA, Kuper HH, van
Leeuwen MA, van de Putte LB and van Riel PL: Modified disease
activity scores that include twenty-eight-joint counts. Development
and validation in a prospective longitudinal study of patients with
rheumatoid arthritis. Arthritis Rheum. 38:44–48. 1995.PubMed/NCBI View Article : Google Scholar
|
|
19
|
Fransen J, Creemers MC and Van Riel PL:
Remission in rheumatoid arthritis: Agreement of the disease
activity score (DAS28) with the ARA preliminary remission criteria.
Rheumatology (Oxford). 43:1252–1255. 2004.PubMed/NCBI View Article : Google Scholar
|
|
20
|
Castaño-Rodríguez N, Kaakoush NO, Goh KL,
Fock KM and Mitchell HM: The NOD-like receptor signaling pathway in
Helicobacter pylori infection and related gastric cancer: A
case-control study and gene expression analyses. PLoS One.
9(e98899)2014.PubMed/NCBI View Article : Google Scholar
|
|
21
|
Livak KJ and Schmittgen TD: Analysis of
relative gene expression data using real-time quantitative PCR and
the 2(-Delta Delta C(T)) Method. Methods. 25:402–408.
2001.PubMed/NCBI View Article : Google Scholar
|
|
22
|
McInnes IB and Schett G: The pathogenesis
of rheumatoid arthritis. N Engl J Med. 365:2205–2219.
2011.PubMed/NCBI View Article : Google Scholar
|
|
23
|
Muruve DA, Pétrilli V, Zaiss AK, White LR,
Clark SA, Ross PJ, Parks RJ and Tschopp J: The inflammasome
recognizes cytosolic microbial and host DNA and triggers an innate
immune response. Nature. 452:103–107. 2008.PubMed/NCBI View Article : Google Scholar
|
|
24
|
Kim HW, Kwon YJ, Park BW, Song JJ, Park YB
and Park MC: Differential expressions of NOD-like receptors and
their associations with inflammatory responses in rheumatoid
arthritis. Clin Exp Rheumatol. 35:630–637. 2017.PubMed/NCBI
|
|
25
|
Ruscitti P, Cipriani P, Di Benedetto P,
Liakouli V, Berardicurti O, Carubbi F, Ciccia F, Alvaro S, Triolo G
and Giacomelli R: Monocytes from patients with rheumatoid arthritis
and type 2 diabetes mellitus display an increased production of
interleukin (IL)-1β via the nucleotide binding domain and
leucine-rich repeat containing family pyrin 3(NLRP3)-inflammasome
activation: A possible implication for therapeutic decision in
these patients. Clin Exp Immunol. 182:35–44. 2015.PubMed/NCBI View Article : Google Scholar
|
|
26
|
Kim HY, Kim SJ and Lee SM: Activation of
NLRP3 and AIM2 inflammasomes in Kupffer cells in hepatic
ischemia/reperfusion. FEBS J. 282:259–270. 2015.PubMed/NCBI View Article : Google Scholar
|
|
27
|
Martinon F, Pétrilli V, Mayor A, Tardivel
A and Tschopp J: Gout-associated uric acid crystals activate the
NALP3 inflammasome. Nature. 440:237–241. 2006.PubMed/NCBI View Article : Google Scholar
|
|
28
|
Iyer SS, Pulskens WP, Sadler JJ, Butter
LM, Teske GJ, Ulland TK, Eisenbarth SC, Florquin S, Flavell RA,
Leemans JC and Sutterwala FS: Necrotic cells trigger sterile
inflammatory response through the Nlrp3 inflammasome. Proc Natl
Acad Sci USA. 106:20388–20393. 2009.PubMed/NCBI View Article : Google Scholar
|
|
29
|
Fu Q, Gao Y, Zhao H, Wang Z and Wang J:
Galangin protects human rheumatoid arthritis fibroblast-like
synoviocytes via suppression of the NF-κB/NLRP3 pathway. Mol Med
Rep. 18:3619–3624. 2018.PubMed/NCBI View Article : Google Scholar
|
|
30
|
Liu Y, Wei W, Wang Y, Wan C, Bai Y, Sun X,
Ma J and Zheng F: TNF-α/calreticulin dual signaling induced NLRP3
inflammasome activation associated with HuR nucleocytoplasmic
shuttling in rheumatoid arthritis. Inflamm Res. 68:597–611.
2019.PubMed/NCBI View Article : Google Scholar
|
|
31
|
Shen HH, Yang YX, Meng X, Luo XY, Li XM,
Shuai ZW, Ye DQ and Pan HF: NLRP3: A promising therapeutic target
for autoimmune diseases. Autoimmun Rev. 17:694–702. 2018.PubMed/NCBI View Article : Google Scholar
|