|
1
|
Loop FD, Lytle BW, Cosgrove DM, Mahfood S,
McHenry MC, Goormastic M, Stewart RW, Golding LA and Taylor PC: J
Maxwell Chamberlain memorial paper. Sternal wound complications
after isolated coronary artery bypass grafting: Early and late
mortality, morbidity, and cost of care. Ann Thorac Surg.
49:179–186; discussion 186-7. 1990.PubMed/NCBI View Article : Google Scholar
|
|
2
|
Lepelletier D, Perron S, Bizouarn P,
Caillon J, Drugeon H, Michaud JL and Duveau D: Surgical-site
infection after cardiac surgery: Incidence, microbiology, and risk
factors. Infect Control Hosp Epidemiol. 26:466–472. 2005.PubMed/NCBI View
Article : Google Scholar
|
|
3
|
Saadatian-Elahi M, Teyssou R and Vanhems
P: Staphylococcus aureus, the major pathogen in orthopaedic
and cardiac surgical site infections: A literature review. Int J
Surg. 6:238–245. 2008.PubMed/NCBI View Article : Google Scholar
|
|
4
|
Abboud CS, Wey SB and Baltar VT: Risk
factors for mediastinitis after cardiac surgery. Ann Thorac Surg.
77:676–683. 2004.PubMed/NCBI View Article : Google Scholar
|
|
5
|
Grossi EA, Culliford AT, Krieger KH, Kloth
D, Press R, Baumann FG and Spencer FC: A survey of 77 major
infectious complications of median sternotomy: A review of 7,949
consecutive operative procedures. Ann Thorac Surg. 40:214–223.
1985.PubMed/NCBI View Article : Google Scholar
|
|
6
|
Filsoufi F, Castillo JG, Rahmanian PB,
Broumand SR, Silvay G, Carpentier A and Adams DH: Epidemiology of
deep sternal wound infection in cardiac surgery. J Cardiothorac
Vasc Anesth. 23:488–494. 2009.PubMed/NCBI View Article : Google Scholar
|
|
7
|
Verhoeven PO, Gagnaire J, Botelho-Nevers
E, Grattard F, Carricajo A, Lucht F, Pozzetto B and Berthelot P:
Detection and clinical relevance of Staphylococcus aureus
nasal carriage: An update. Expert Rev Anti Infect Ther. 12:75–89.
2014.PubMed/NCBI View Article : Google Scholar
|
|
8
|
Gagnaire J, Verhoeven PO, Grattard F,
Rigaill J, Lucht F, Pozzetto B, Berthelot P and Botelho-Nevers E:
Epidemiology and clinical relevance of Staphylococcus aureus
intestinal carriage: A systematic review and meta-analysis. Expert
Rev Anti Infect Ther. 15:767–785. 2017.PubMed/NCBI View Article : Google Scholar
|
|
9
|
Katayanagi T: Nasal methicillin-resistant
S aureus is a major risk for mediastinitis in pediatric
cardiac surgery. Ann Thorac Cardiovasc Surg. 21:37–44.
2015.PubMed/NCBI View Article : Google Scholar
|
|
10
|
van Rijen M, Bonten M, Wenzel R and
Kluytmans J: Mupirocin ointment for preventing Staphylococcus
aureus infections in nasal carriers. Cochrane Database Syst
Rev. 4(CD006216)2008.PubMed/NCBI View Article : Google Scholar
|
|
11
|
Langenberg JCM, Kluytmans JAJW, Mulder
PGH, Romme J, Ho GH and Van Der Laan L: Peri-Operative nasal
eradication therapy prevents staphylococcus aureus surgical
site infections in aortoiliac surgery. Surg Infect (Larchmt).
19:510–515. 2018.PubMed/NCBI View Article : Google Scholar
|
|
12
|
Bode LG, Kluytmans JA, Wertheim HF,
Bogaers D, Vandenbroucke-Grauls CM, Roosendaal R, Troelstra A, Box
AT, Voss A, van der Tweel I, et al: Preventing surgical-site
infections in nasal carriers of Staphylococcus aureus. N
Engl J Med. 362:9–17. 2010.PubMed/NCBI View Article : Google Scholar
|
|
13
|
Konvalinka A, Errett L and Fong IW: Impact
of treating Staphylococcus aureus nasal carriers on wound
infections in cardiac surgery. J Hosp Infect. 64:162–168.
2006.PubMed/NCBI View Article : Google Scholar
|
|
14
|
Lemaignen A, Armand-Lefevre L, Birgand G,
Mabileau G, Lolom I, Ghodbane W, Dilly MP, Nataf P and Lucet JC:
Thirteen-year experience with universal Staphylococcus
aureus nasal decolonization prior to cardiac surgery: A
quasi-experimental study. J Hosp Infect. 100:322–328.
2018.PubMed/NCBI View Article : Google Scholar
|
|
15
|
Sakr A, Brégeon F, Rolain JM and Blin O:
Staphylococcus aureus nasal decolonization strategies: A
review. Expert Rev Anti Infect Ther. 17:327–340. 2019.PubMed/NCBI View Article : Google Scholar
|
|
16
|
Liu Z, Norman G, Iheozor-Ejiofor Z, Wong
JK, Crosbie EJ and Wilson P: Nasal decontamination for the
prevention of surgical site infection in Staphylococcus
aureus carriers. Cochrane Database Syst Rev.
5(CD012462)2017.PubMed/NCBI View Article : Google Scholar
|
|
17
|
Schweizer M, Perencevich E, McDanel J,
Carson J, Formanek M, Hafner J, Braun B and Herwaldt L:
Effectiveness of a bundled intervention of decolonization and
prophylaxis to decrease Gram positive surgical site infections
after cardiac or orthopedic surgery: Systematic review and
meta-analysis. BMJ. 346(f2743)2013.PubMed/NCBI View Article : Google Scholar
|
|
18
|
Ma N, Cameron A, Tivey D, Grae N, Roberts
S and Morris A: Systematic review of a patient care bundle in
reducing staphylococcal infections in cardiac and orthopaedic
surgery. ANZ J Surg. 87:239–246. 2017.PubMed/NCBI View Article : Google Scholar
|
|
19
|
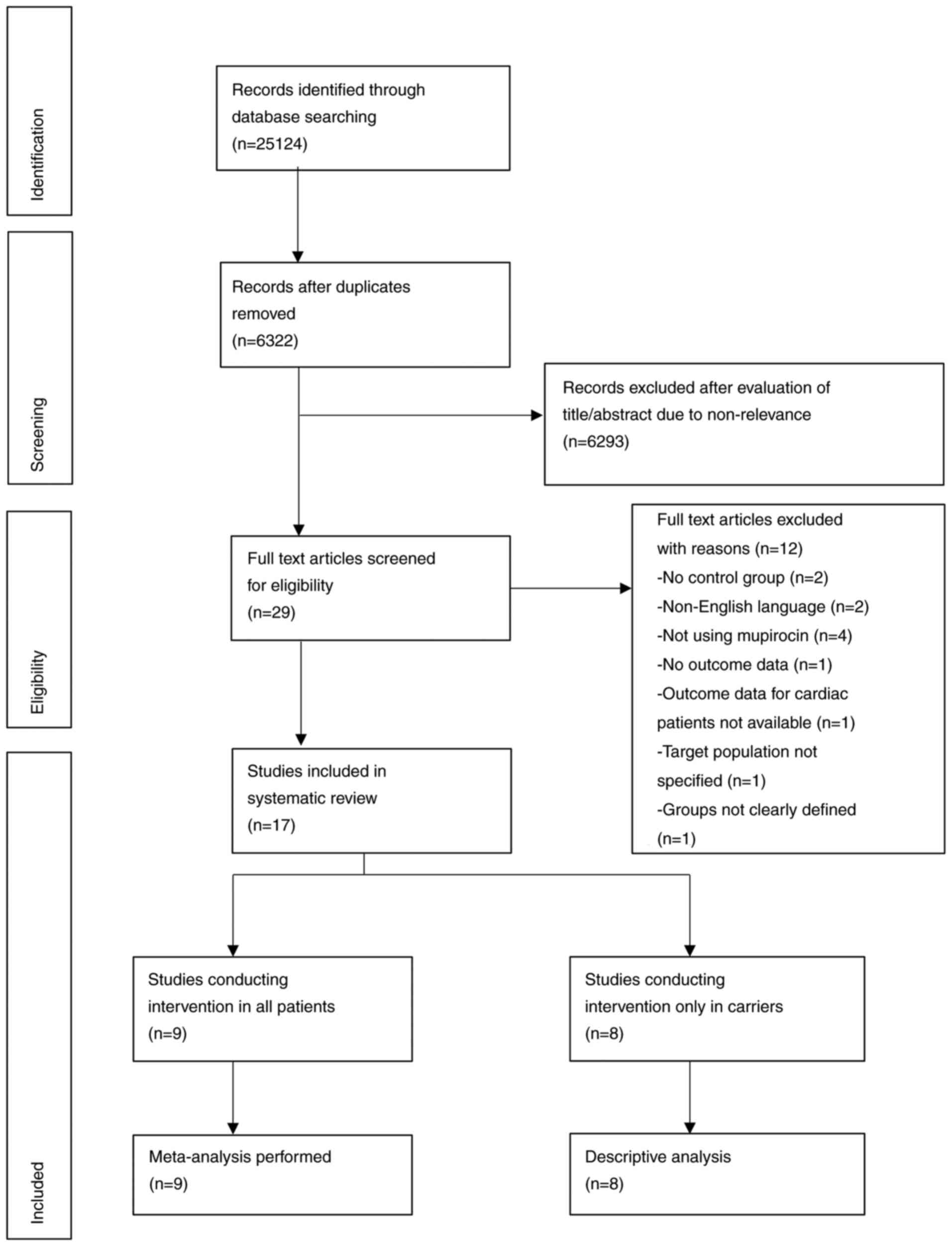
Moher D, Liberati A, Tetzlaff J, Altman DG
and PRISMA Group: Preferred reporting items for systematic reviews
and meta-analyses: The PRISMA statement. BMJ.
339(b2535)2009.PubMed/NCBI View Article : Google Scholar
|
|
20
|
Higgins JPT, Thomas J, Chandler J,
Cumpston M, Li T, Page MJ and Welch VA: Cochrane Handbook for
Systematic Reviews of Interventions. Version 6.1 (updated September
2020). Cochrane, 2020. Available from www.training.cochrane.org/handbook.
|
|
21
|
Kim SY, Park JE, Lee YJ, Seo HJ, Sheen SS,
Hahn S, Jang BH and Son HJ: Testing a tool for assessing the risk
of bias for nonrandomized studies showed moderate reliability and
promising validity. J Clin Epidemiol. 66:408–414. 2013.PubMed/NCBI View Article : Google Scholar
|
|
22
|
Wallace BC, Schmid CH, Lau J and
Trikalinos TA: Meta-analyst: Software for meta-analysis of binary,
continuous and diagnostic data. BMC Med Res Methodol.
9(80)2009.PubMed/NCBI View Article : Google Scholar
|
|
23
|
Usry GH, Johnson L, Weems JJ Jr and
Blackhurst D: Process improvement plan for the reduction of sternal
surgical site infections among patients undergoing coronary artery
bypass graft surgery. Am J Infect Control. 30:434–436.
2002.PubMed/NCBI View Article : Google Scholar
|
|
24
|
Cimochowski GE, Harostock MD, Brown R,
Bernardi M, Alonzo N and Coyle K: Intranasal mupirocin reduces
sternal wound infection after open heart surgery in diabetics and
nondiabetics. Ann Thorac Surg. 71:1572–1578; discussion 1578-9.
2001.PubMed/NCBI View Article : Google Scholar
|
|
25
|
Coskun D and Aytac J: Decrease in
Staphylococcus aureus surgical site infections following
cardiovascular surgery. J Hosp Infect. 60:287–289. 2005.
|
|
26
|
Martorell C, Engelman R, Corl A and Brown
RB: Surgical site infections in cardiac surgery: An 11-year
perspective. Am J Infect Control. 32:63–68. 2004.PubMed/NCBI View Article : Google Scholar
|
|
27
|
Thompson P and Houston S: Decreasing
methicillin-resistant Staphylococcus aureus surgical site
infections with chlorhexidine and mupirocin. Am J Infect Control.
41:629–633. 2013.PubMed/NCBI View Article : Google Scholar
|
|
28
|
Walsh EE, Greene L and Kirshner R:
Sustained reduction in methicillin-resistant Staphylococcus
aureus wound infections after cardiothoracic surgery. Arch
Intern Med. 171:68–73. 2011.PubMed/NCBI View Article : Google Scholar
|
|
29
|
Kohler P, Sommerstein R, Schönrath F,
Ajdler-Schäffler E, Anagnostopoulos A, Tschirky S, Falk V, Kuster
SP and Sax H: Effect of perioperative mupirocin and antiseptic body
wash on infection rate and causative pathogens in patients
undergoing cardiac surgery. Am J Infect Control. 43:e33–e38.
2015.PubMed/NCBI View Article : Google Scholar
|
|
30
|
Nicholson MR and Huesman LA: Controlling
the usage of intranasal mupirocin does impact the rate of
Staphylococcus aureus deep sternal wound infections in
cardiac surgery patients. Am J Infect Control. 34:44–48.
2006.PubMed/NCBI View Article : Google Scholar
|
|
31
|
Shrestha NK, Banbury MK, Weber M, Cwynar
RE, Lober C, Procop GW, Karafa MT and Gordon SM: Safety of targeted
perioperative mupirocin treatment for preventing infections after
cardiac surgery. Ann Thorac Surg. 81:2183–2188. 2006.PubMed/NCBI View Article : Google Scholar
|
|
32
|
Jog S, Cunningham R, Cooper S, Wallis M,
Marchbank A, Vasco-Knight P and Jenks PJ: Impact of preoperative
screening for meticillin-resistant Staphylococcus aureus by
real-time polymerase chain reaction in patients undergoing cardiac
surgery. J Hosp Infect. 69:124–130. 2008.PubMed/NCBI View Article : Google Scholar
|
|
33
|
Schweizer ML, Chiang HY, Septimus E, Moody
J, Braun B, Hafner J, Ward MA, Hickok J, Perencevich EN, Diekema
DJ, et al: Association of a bundled intervention with surgical site
infections among patients undergoing cardiac, hip, or knee surgery.
JAMA. 313:2162–2171. 2015.PubMed/NCBI View Article : Google Scholar
|
|
34
|
Saraswat MK, Magruder JT, Crawford TC,
Gardner JM, Duquaine D, Sussman MS, Maragakis LL and Whitman GJ:
Preoperative staphylococcus aureus screening and targeted
decolonization in cardiac surgery. Ann Thorac Surg. 104:1349–1356.
2017.PubMed/NCBI View Article : Google Scholar
|
|
35
|
Nicolas R, Carricajo A, Morel J, Rigaill
J, Grattard F, Guezzou S, Audoux E, Campisi S, Favre JP, Berthelot
P, et al: Evaluation of effectiveness and compliance with the
mupirocin nasal ointment part of Staphylococcus aureus
decolonization in real life using UPLC-MS/MS mupirocin
quantification. J Antimicrob Chemother. 75:1623–1630.
2020.PubMed/NCBI View Article : Google Scholar
|
|
36
|
Kluytmans JA, Mouton JW, VandenBergh MF,
Manders MJ, Maat AP, Wagenvoort JH, Michel MF and Verbrugh HA:
Reduction of surgical-site infections in cardiothoracic surgery by
elimination of nasal carriage of staphylococcus aureus.
Infect Control Hosp Epidemiol. 17:780–785. 1996.PubMed/NCBI View Article : Google Scholar
|
|
37
|
Gebreselassie HM, Lo Priore E and
Marschall J: Effectiveness of meticillin-resistant
Staphylococcus aureus decolonization in long-term
haemodialysis patients: A systematic review and meta-analysis. J
Hosp Infect. 91:250–256. 2015.PubMed/NCBI View Article : Google Scholar
|
|
38
|
Nair R, Perencevich EN, Blevins AE, Goto
M, Nelson RE and Schweizer ML: Clinical effectiveness of mupirocin
for preventing staphylococcus aureus infections in
nonsurgical settings: A meta-analysis. Clin Infect Dis. 62:618–630.
2016.PubMed/NCBI View Article : Google Scholar
|
|
39
|
Wenzel RP and Edmond MB: Infection
control: The case for horizontal rather than vertical
interventional programs. Int J Infect Dis. 14 (Suppl 4):S3–S5.
2010.PubMed/NCBI View Article : Google Scholar
|
|
40
|
Huang SS, Septimus E, Kleinman K, Moody J,
Hickok J, Avery TR, Lankiewicz J, Gombosev A, Terpstra L, Hartford
F, et al: Targeted versus universal decolonization to prevent ICU
infection. N Engl J Med. 368:2255–2265. 2013.PubMed/NCBI View Article : Google Scholar
|
|
41
|
Dadashi M, Hajikhani B, Darban-Sarokhalil
D, van Belkum A and Goudarzi M: Mupirocin resistance in
Staphylococcus aureus: A systematic review and
meta-analysis. J Glob Antimicrob Resist. 20:238–247.
2020.PubMed/NCBI View Article : Google Scholar
|
|
42
|
Hayden MK, Lolans K, Haffenreffer K, Avery
TR, Kleinman K, Li H, Kaganov RE, Lankiewicz J, Moody J, Septimus
E, et al: Chlorhexidine and mupirocin susceptibility of
methicillin-resistant staphylococcus aureus isolates in the
REDUCE-MRSA trial. J Clin Microbiol. 54:2735–2742. 2016.PubMed/NCBI View Article : Google Scholar
|
|
43
|
Morgan DJ, Diekema DJ, Sepkowitz K and
Perencevich EN: Adverse outcomes associated with contact
precautions: A review of the literature. Am J Infect Control.
37:85–93. 2009.PubMed/NCBI View Article : Google Scholar
|
|
44
|
McConeghy KW, Mikolich DJ and LaPlante KL:
Agents for the decolonization of methicillin-resistant
Staphylococcus aureus. Pharmacotherapy. 29:263–280.
2009.PubMed/NCBI View Article : Google Scholar
|
|
45
|
Webster J and Osborne S: Preoperative
bathing or showering with skin antiseptics to prevent surgical site
infection. Cochrane Database Syst Rev CD004985, 2015.
|
|
46
|
Franco LM, Cota GF, Pinto TS and Ercole
FF: Preoperative bathing of the surgical site with chlorhexidine
for infection prevention: Systematic review with meta-analysis. Am
J Infect Control. 45:343–349. 2017.PubMed/NCBI View Article : Google Scholar
|
|
47
|
Saleh A, Khanna A, Chagin KM, Klika AK,
Johnston D and Barsoum WK: Glycopeptides versus β-lactams for the
prevention of surgical site infections in cardiovascular and
orthopedic surgery: A mata-analysis. Ann Surg. 261:72–80.
2015.PubMed/NCBI View Article : Google Scholar
|