Introduction
Osteosarcoma is a high-grade bone malignancy and
represents the most common primary bone cancer in children and
adolescents (1). Osteosarcoma
tumors are characterized by highly proliferating and invasive
spindle cells of mesenchymal origin, with immature osteoid matrix
deposition. The current standard management strategy for this
disease involves surgical resection of all clinically-detectable
lesions and systemic pre- and postoperative multidrug chemotherapy.
Depending on the clinical guidelines followed by each country or
region, these chemotherapeutic regimens usually combine high-dose
methotrexate with doxorubicin and cisplatin, or etoposide in
addition to ifosfamide (2,3). Despite incorporation of these
multimodality therapy approaches, 30-40% of osteosarcoma patients
still develop local recurrences or distant metastases, becoming an
exceptionally challenging disease with elevated mortality rates
(4). Alarmingly, while 5-year
survival rates of up to 70% are achieved in high-income countries,
prognosis in low- and middle-income countries (LMICs) is
significantly poorer, with reported survival rates as low as 45%
(5). In a context of economic
inequalities and resource-constrained health-care systems, these
disparities are linked to limited access to adequate treatment and
high rates of diagnostic delays, leading to late stage cancer
diagnosis and poor survival (6,7).
Considering that in the last few decades advances in osteosarcoma
management and survival rates have reached a discouraging plateau,
there is a critical need to identify novel therapeutic tools for
osteosarcoma.
Drug repurposing in oncology comprises the
identification and use of already-approved drugs with a
non-oncology primary use for cancer treatment (8). This strategy arises as an attractive
alternative to de novo drug development, offering
considerable advantages, such as an already proven safety profile,
which in consequence can facilitate clinical evaluation, low
production costs and widespread availability (9,10).
Following this rationale, during the past years our group has
explored and characterized the use of hemostatic drug desmopressin
(1-deamino-8-D-arginin vasopressin; dDAVP) as an adjuvant agent in
cancer treatment. dDAVP has been used as a blood-saving agent for
nearly 50 years in patients with bleeding disorders or undergoing
complex surgeries characterized by large blood loss (11). This compound is a 1st generation
synthetic analog of the vasopressin hormone (AVP) and acts as a
selective agonist for the vasopressin membrane receptor type 2
(AVPR2) expressed in microvascular endothelium (12) and several transformed tissues,
including breast (13-15),
prostate (16), lung (17) and colorectal cancer (18,19).
Agonistic stimulation of vascular AVPR2 is associated with a cyclic
adenosine monophosphate (cAMP)-mediated acute release of several
hemostatic factors into the bloodstream, including factor VIII,
tissue-type plasminogen activator and von Willebrand factor (VWF).
VWF is a multifaceted blood glycoprotein involved in different
biological processes such as coagulation, vascular normalization,
cancer cell apoptosis and metastatic resistance (20-22).
Preclinical studies by our research group and others using breast,
colorectal, and lung cancer models reported that activation of
tumor AVPR2 by dDAVP triggers antiproliferative signaling
mechanisms after cAMP/cAMP-dependent protein kinase (PKA) axis
activation, resulting in cell cycle arrest and decreased cell
survival and growth (14,16-18,23-25).
Cytostatic activity showed to be AVPR2-dependent as dDAVP effects
on malignant cells were completely reverted after AVPR2
phamacological blockade or siRNA-mediated receptor depletion was
performed (16,23,24).
dDAVP administration to animals bearing human or murine carcinomas
was also capable of reducing tumor vascularization, and such
angiostatic effects were associated to proteolytic production of
antiangiogenic protein angiostatin (ANG) (26). Interestingly, several preclinical
animal studies, as well as veterinary trials, showed that
administration of dDAVP at clinically relevant doses has a profound
antimetastatic activity, impairing dissemination and progression of
residual metastatic cells and showing benefits in terms of distant
recurrences after tumor resection and overall survival (14,18,27-31).
Taking into account its potential anticancer properties as well as
its validated and safe hemostatic activity, a phase II
dose-escalation trial was conducted exploring dDAVP use as an
adjuvant therapy during breast cancer surgical excision
(NCT01606072). A perioperative treatment using two 1 µg/kg i.v.
doses was associated to reduced intraoperative bleeding, increased
plasmatic VWF and a postsurgical drop of circulating tumor cells
(15). In a second phase I/II
clinical trial, safety and symptom control were assessed in rectal
cancer patients with bleeding. As a result, after 4 days of
treatment initiation, complete hemostatic control and reduction of
tumor vascular perfusion were achieved in the vast majority of
patients (32). Despite dDAVP
deployed interesting and promising anticancer activity as a
repurposed agent in a variety of experimental and clinical
settings, its potential therapeutic benefits in osteosarcoma were
never evaluated.
As previously mentioned, osteosarcoma is fatal for
about one-third of the patients worldwide and effective therapeutic
options are rather limited, especially for advanced or refractory
disease. In order to improve patient's chances of survival there is
an urgent need for developing novel cost-effective therapeutic
strategies. In view of this scenario, our present work sought to
study the anticancer activity of repurposed hemostatic drug dDAVP
on human osteosarcoma experimental models. Apart from exploring
direct in vitro cytostatic effects of the compound, our
study aimed to explore AVPR2 target expression in osteosarcoma
xenografts as well as human tissue samples, and to evaluate the
impact of sustained dDAVP administration in osteosarcoma tumor
progression.
Materials and methods
Drugs and compounds
dDAVP was obtained from Romikin S.A. following GMP
standards. Peptide purity was 98-99% as assessed by MS-HPLC.
Peptide sequence: Mpr-Tyr-Phe-Gln-Asn-Cys-Pro-DArg-Gly-NH2
(disulfide bridge between Mpr-Cys). In order to achieve work
concentrations, dDAVP was diluted in phosphate buffered saline
(PBS) as vehicle. PDE3/4 inhibitor rolipram (ROL) was purchased
from Sigma-Aldrich; Merck KGaA. Control groups were treated with
PBS as vehicle.
Tumor cell lines and culture
conditions
MG-63 (ATCC® CRL-1427™) and U-2OS
(ATCC® HTB-96™) human osteosarcoma cell lines were
obtained from the American Type Culture Collection. Human breast
MCF-7 (ATCC® HTB-22™) and MDA-MB-231 (ATCC®
HTB-26™) or lung H-125 (ATCC® CRL-5801™) cancer cell
lines were used as controls for in vitro or in vivo
AVPR2 expression and were also acquired from the American Type
Culture Collection. Tumor cell lines were grown in Dulbecco's
modified Eagle's medium (DMEM, Thermo Fisher Scientific Inc.) plus
10% fetal bovine serum (FBS, Natocor), 2 mM glutamine and 80 µg/ml
gentamycin in monolayer culture, at 37˚C in a humidified atmosphere
of 5% CO2. Cells were harvested using a trypsin/EDTA
solution (Thermo Fisher Scientific Inc.) diluted in PBS and
routinely tested for mycoplasma.
In vitro studies AVPR2 expression
analysis in osteosarcoma cells
Total RNA of MG-63 and U-2 OS cells was purified
from 1x106 cells using the EasyPure®
(TransGen) RNA kit following the manufacturer's protocol. RNA was
reverse-transcribed with SuperScript III first-Strand Synthesis
System (Thermo Fisher Scientific Inc.). The following forward and
reverse primers were used: For AVPR2 5'-CTGGCCAAGGACACTTCATC-3' and
5'-GAAGGCAGCTGAGCTTC-3', for hypoxanthine phosphoribosyl
transferase 1 (HPRT1), 5'-AACGTCTTGCTCGAGATGTG-3' and
5'-GCTTTGATGTAATCCAGCAGG-3'. Quantitative real time polymerase
chain reaction (RT-qPCR) was performed using the SYBR Green PCR
Master Mix (Thermo Fisher Scientific Inc.) and StepOne Real-Time
PCR System (Applied Biosystems; Thermo Fisher Scientific Inc.).
Thermal cycling conditions were 48˚C for 30 min, 95˚C for 10 min,
40 cycles of 95˚C for 15 sec followed by 60˚C for 60 sec. Each
sample was analysed in triplicate and mean cycle threshold values
(Ct) were used for further analysis. Ct values were normalized for
HPRT1 expression levels. The AVPR2 expression in MCF-7 cells
(positive control) was considered as ‘1’. Relative quantification
values were calculated as 2-∆∆Ct.
Osteosarcoma cell growth and
cytotoxicity studies
Antiproliferative activity against rapidly growing
tumor cells was determined using 72-h cell growth assays and
crystal violet staining. 2.5x103 MG-63 or U-2 OS cells
in 200 µl were plated in 96-well flat bottom plates in complete
DMEM, allowed to attach, and 24 h later treated with dDAVP (0.1, 1
or 10 µM) or PBS for 72 h. By the end of the experiment, cells were
briefly fixed with methanol, stained with 0.5% crystal violet
solution, washed and dried overnight. After addition of
ethanol/acetic acid 3:1 solution on crystal violet-dyed cultures,
absorbance was measured at 595 nm. The optical density of
PBS-treated control cells was taken as 100% of cell growth. Lack of
direct cytotoxicity of dDAVP (1 µM for 24 h) on MG-63
semi-confluent monolayers was performed using the trypan blue dye
exclusion assay as previously described (16).
Apoptosis
Apoptotic cells were detected by terminal
deoxynucleotidyl transferase dUTP nick end labeling (TUNEL). First,
1x104 MG-63 cells were plated on 24-well flat bottom
plates and allowed to attach overnight. After 24-h starvation,
cells were treated for 48 h with dDAVP (1 µM) in complete medium.
After incubation, cells were fixed in 4% paraformaldehyde (PFA) in
PBS. DNA strand breaks were labeled with digoxigenin-dUTP using
DeadEnd™ Fluorometric TUNEL System according to the manufacturer's
protocol (Promega Corp.). Slides were mounted with DAPI-containing
mounting medium Vectashield™ (Vector Laboratories Inc.) and
visualized using a Cytation-Gen5 Cell Imaging Multi-Mode Reader
(Biotek Instruments Inc.). A total of 10 images per experimental
condition were acquired for analysis. The percentage of apoptotic
cells in MG-63 cultures was calculated as (number of TUNEL-positive
cells/total cells) x100. Apoptosis in MG-63 cultures was confirmed
using cytotoxic agent cisplatin (10 µM) as a positive control.
Mitotic index of osteosarcoma cells in
vitro
Osteosarcoma cell cultures were analyzed for mitotic
index calculation after 48-h treatment with dDAVP (1 µM), using the
same starvation, PFA-fixation and DAPI-staining protocol as in
previously described apoptosis assay. Ten images per experimental
group were used for quantification. Mitotic figures in all 4 basic
stages of mitosis (prophase, metaphase, anaphase and telophase)
were counted using a high-power field magnification (HPF) of
400-fold magnification (x400) and the percentage of mitotic cells
was obtained after quantification of total cell number per HPF.
Assessment of cAMP levels
Activation of canonical adenylate cyclase/cAMP/PKA
axis after dDAVP-mediated AVPR2 stimulation was preliminary
assessed by measuring intracellular cAMP levels in MG-63 cells.
Semi-confluent osteosarcoma cultures were exposed to dDAVP (1 µM)
or PBS for 1 h and cAMP was quantified using a competitive
enzymatic immunoassay cAMP EIA Kit (Cayman Chemical Co.) following
the steps detailed by the supplier.
Osteosarcoma cell chemotaxis
Tumor cell migration was assessed using the
Transwell® migration assay. After overnight starvation,
2.5x104 MG-63 cells were seeded into 8 µm pore inserts
in 24-well plates (JetBiofil) in serum-free growth medium. The
lower chamber was filled with DMEM containing 10% FBS, which was
used as a chemoattractant. After 24-h incubation with dDAVP (0.1, 1
or 10 µM) cells in the upper surface of the membranes were gently
removed with cotton swabs. Cells that migrated to the lower surface
were fixed with PFA and stained with 0.5% crystal violet. Migrated
cells in five randomly selected x400 HPF were counted and
normalized to control.
In vivo osteosarcoma xenograft
progression Animals
Outbred athymic female N:NIH(S)-nu mice aged 8 weeks
with a weight of approximately 20 g, were purchased from the UNLP
Animal Facility (National University of La Plata, School of
Veterinary Sciences, Buenos Aires, Argentina), and housed at 5 mice
per cage in our animal house facility at the National University of
Quilmes. Food and water were provided ad libitum and general
health status of the animals was monitored daily.
Tumor progression
To generate human osteosarcoma xenografts, a 150
µl-suspension containing 5x106 MG-63 cells in 1:0.5
volume ratio mixture of DMEM and Matrigel® (Becton,
Dickinson and Company) was injected subcutaneously in athymic mice.
Tumors were measured periodically with a calliper and tumor volume
was calculated by the formula: 0.52 x width2 x length.
Animal weight and tumor growth rates were also assessed along the
protocol. Four days after cell inoculation and once all tumors were
detectable by palpation, administration of dDAVP began, using a 12
µg/kg i.v. dose, 3 times per week during 4 weeks. Animal dosing was
determined by dose extrapolation using the ‘dose by factor’ method
based on allometric scaling, following the United States Food and
Drug Administration guidelines (33). A clinically validated dDAVP dose of
1 µg/kg i.v. was taken as the reference dose (15,30-32)
and multiplied by 12.3 for human to mice conversion (33). Mice equivalent dose was rounded down
from 12.3 to 12 µg/kg i.v. to facilitate drug preparation and
administration. When lesions reached volumes >300
mm3, and signs of tumor necrosis and skin infiltration
were observed in the majority of tumors, animals were euthanized by
cervical dislocation. Tumors were removed, weighted, fixed with 10%
formalin and processed for hematoxylin and eosin (H&E) or
Masson trichrome staining in order to explore tumor histology.
Hematological and blood biochemical
analysis
On the final day of the tumor progression protocol,
after 1 h of dDAVP administration and before euthanasia, animals
were anesthetized using intraperitoneal ketamine at 100 mg/kg in
combination with 10 mg/kg xylazine, and EDTA-anticoagulated
whole-blood samples from each of the experimental subjects were
collected for further hematological and biochemical analysis.
Hematocrite, red and white blood cell and platelet count,
cholesterol, total protein, direct bilirubin, creatinine and
albumin levels, as well as aspartate aminotransferase and alanine
aminotransferase activity were assessed.
Immunohistochemical staining for AVPR2
in osteosarcoma xenografts or human samples
MG-63 osteosarcoma tumor samples were fixed in 10%
formalin, embedded in paraffin, and tissue sections of 4 µm were
cut and placed on silane coated slides for anti-AVPR2
immunohistochemistry (IHC) staining. Sections were microwaved for
antigen retrieval in 0.01 M sodium citrate buffer (pH 6.0) during
20 min, and later incubated with 3% hydrogen peroxide for 10 min to
block endogenous peroxidase. Immunostaining was performed using an
anti-AVPR2 primary polyclonal rabbit antibody (V5514; 1:100
dilution, Sigma-Aldrich; Merck KGaA) at room temperature for 1 h.
For visualizing immunoreactivity, a 15-min incubation using Super
Sensitive™ One-Step Polymer-HRP IHC Detection System (Bio-genex)
was conducted. Finally, sections were counterstained with
hematoxylin. MCF-7 and MDA-MB-231 breast cancer xenografts were
generated in athymic nude mice by a subcutaneous injection of a 300
µl suspension containing 5x106 cancer cells in a 1:1
volume ratio mixture of DMEM and Matrigel®, as reported
(25,34,35).
After 45 days of tumor progression, tumors were resected and
processed as previously described, and were used as positive
controls for in vivo AVPR2 expression. For expression
analysis of targeted receptor in human tumor samples,
formalin-fixed paraffin-embedded chemotherapy-naïve conventional
osteosarcoma biopsy specimens were processed for IHC after
diagnosis confirmation by the pathological anatomy service from the
Edgardo Rebagliati Martins National Hospital. Additionally,
histological characteristics of different osteosarcoma subtypes
were assessed using hematoxylin and eosin (plus alcian blue) or
Masson's trichrome (plus aniline blue) staining.
Statistical analysis
All statistical analyses were performed using the
PRISM 6 (GraphPad Software Inc.) or Compusyn software (Combosyn
Inc., New Jersey, United States). To compare differences between 2
experimental groups, two-tailed Mann Whitney or t-tests were used
for non-parametric or normal distribution of data, respectively. In
case of more than 2 experimental groups, ANOVA analysis with
Tukey's multiple comparisons post-test was used. Kruskal-Wallis
analysis with Dunn's multiple comparisons post-test was used in
case of non-parametric distribution of data. In drug combination
studies synergy was determined when combination index (CI) was
<1. The number of mitotic or apoptotic cells was expressed as
percentage of positive cells/total number of cells counted in each
specific condition (±95% confidence limits), and analysed by the
χ2 test. In tumor progression protocols, growth rates
represent the slopes of the linear regressions of the tumor volumes
over time. Differences were considered statistically significant at
a level of P<0.05. Data were presented as mean ± standard
deviation (SD) or standard error of mean (SEM). Data were derived
from at least two or three independent experiments, unless stated
otherwise.
Results
In vitro treatment with dDAVP inhibits
tumor cell growth in AVPR2-expressing osteosarcoma and is
associated with elevated cAMP levels
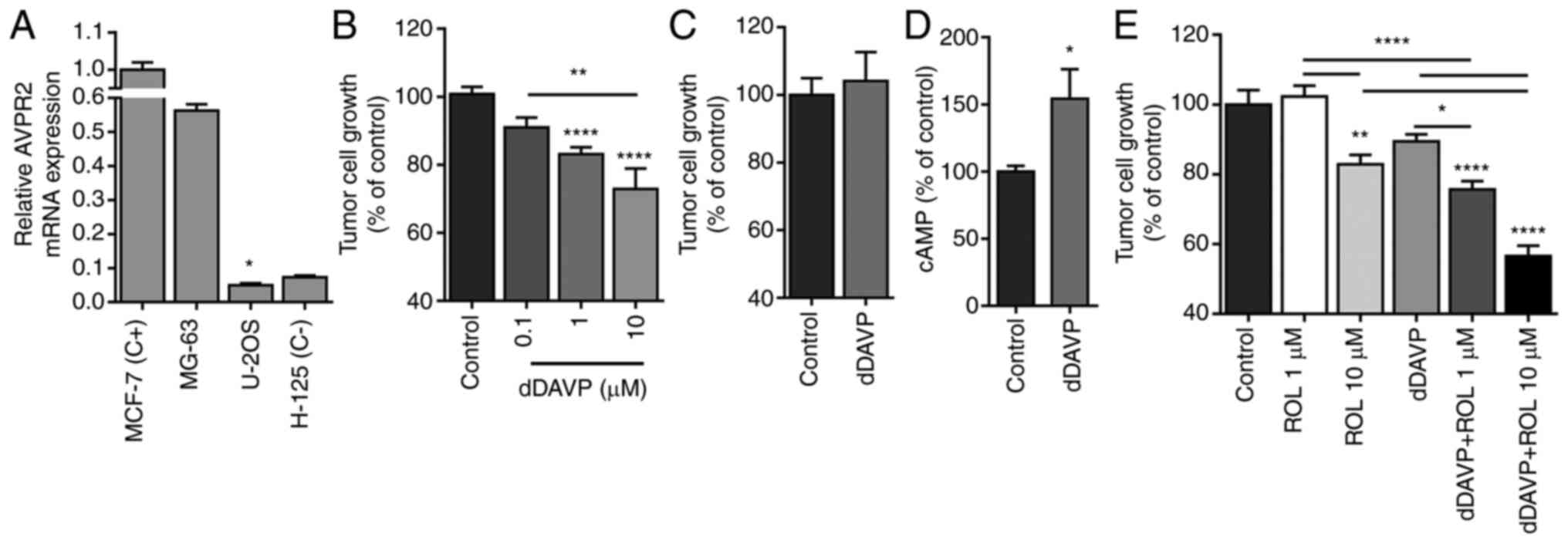
First, AVPR2 expression was assessed in MG-63 and
U-2 OS human osteosarcoma cells. RT-qPCR analysis showed comparable
AVPR2 expression levels between MG-63 and MCF-7 cells (positive
control). In contrast, AVPR2 gene expression in U-2 OS was almost
undetectable (Fig. 1A). In
accordance with these results, exposure of MG-63 semiconfluent
monolayers to dDAVP (0.1-10 µM), but not of AVPR2-negative U-2 OS
cultures, resulted in a significant dose-dependent inhibitory
effect over cell growth (Fig. 1B
and C). Given that direct
antiproliferative activity of dDAVP on tumor cells seems to be
mediated by cAMP/PKA signalling-related pathways (19,23),
we assessed intracellular cAMP levels in MG-63 cultures after dDAVP
treatment. As a result, a 54% increase in cAMP intracellular
concentration was observed after dDAVP treatment in osteosarcoma
cells. Both in normal and malignant cells, elevated intracellular
cAMP levels are rapidly restored by efflux and/or decomposition
through different multidrug-resistance proteins and
phosphodiesterases, respectively. We, therefore, evaluated the
effect of phosphodiesterase inhibition using rolipram in
combination with cAMP-elevating agent dDAVP. Osteosarcoma cells
were incubated with dDAVP (1 µM) plus effective (10 µM) or
sub-optimal (1 µM) concentrations of rolipram, obtaining
synergistic growth inhibitory effects in both tested drug
combinations (Fig. 1E).
Cytostatic activity of dDAVP in
osteosarcoma cells is associated with mitosis inhibition, increased
apoptosis and antimigratory effects
In order to gain further insights into dDAVP
anti-osteosarcoma effects, we preliminarily explored compound's
capacity to modulate other key events in osteosarcoma tumor biology
such as mitosis, apoptosis and migration. As shown in Fig. 2, a 48-h treatment with dDAVP reduced
the percentage of MG-63 cells undergoing mitosis by nearly 70% in
contrast to vehicle-treated cells. In equivalent experimental
conditions, dDAVP at 1 µM caused a 3.4-fold increase in the number
of osteosarcoma apoptotic cells, as evaluated by DNA fragmentation
labeling (Fig. 2A and B, respectively). Furthermore,
Transwell chemotaxis assays demonstrated a significant
decrease in the migratory capacity of osteosarcoma cells upon
overnight incubation with tested compound (Fig. 2C). Lack of short-term cytotoxicity
of dDAVP on osteosarcoma cells was confirmed using the trypan blue
dye exclusion assay (Fig. 2D).
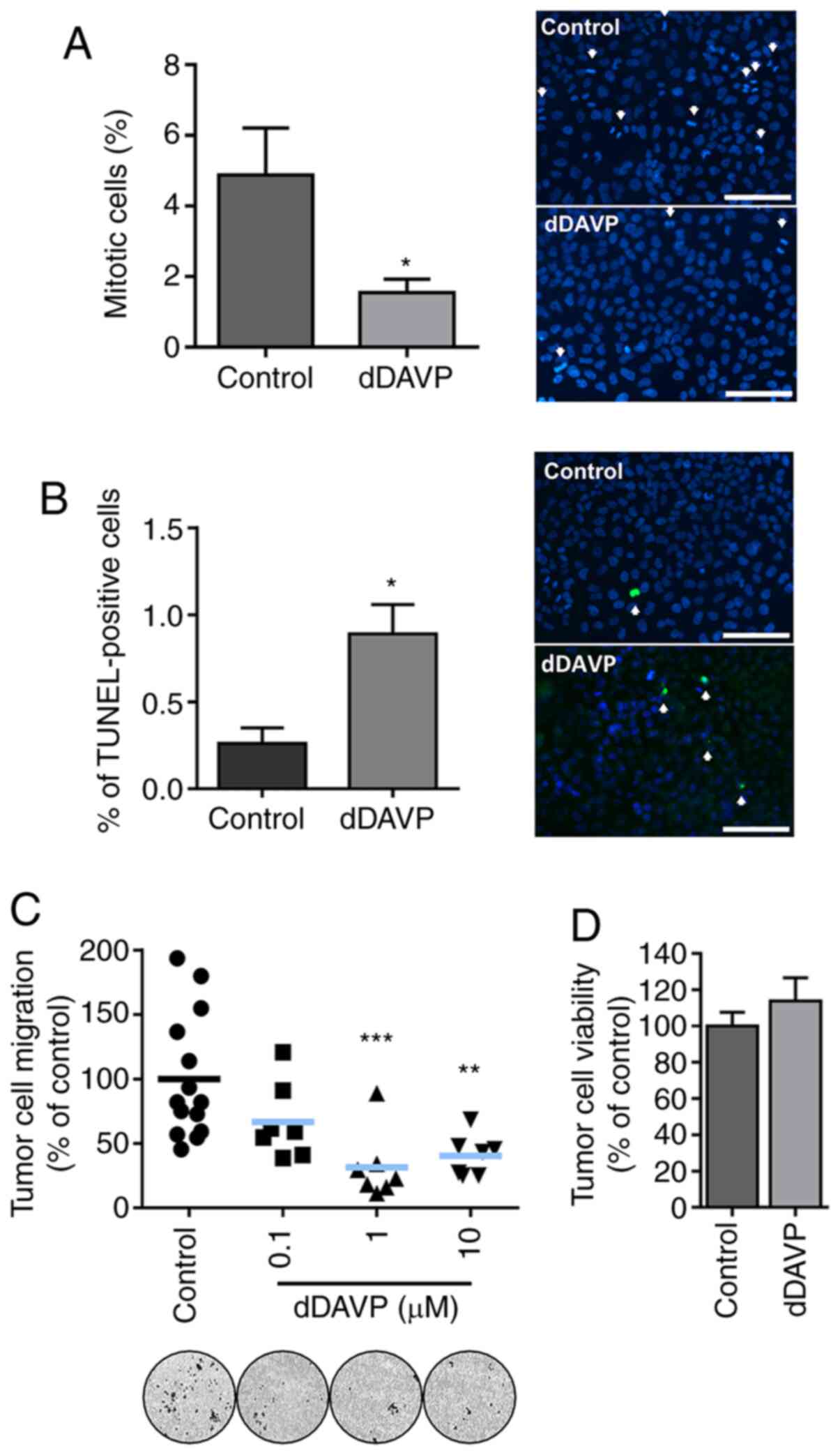 | Figure 2Direct cytostatic effects of dDAVP on
osteosarcoma cells are associated to reduced mitosis, increased
apoptosis and impaired tumor cell chemotaxis. (A) Reduction of
cellular mitotic index on MG-63 cell cultures after a 48 h
treatment with dDAVP (1 µM). Quantification of mitosis (left)
expressed as % of mitotic cells/total cells. Magnification, x400.
Scale bar, 100 µm. Representative images (right) of cell cultures
under DAPI nuclear staining evidencing mitotic bodies. (B)
Percentage (%) of TUNEL-positive cells relative to total cell count
after DAPI-stained nuclei quantification (left). Representative
images of MG-63 apoptotic cells after 48 h exposure to dDAVP (1 µM)
(right). Magnification, x400. Scale bar, 100 µm. Arrows indicate
mitotic bodies or TUNEL-positive apoptotic cells, respectively. (C)
dDAVP impact on MG-63 cell migration after a 16 h treatment as
assessed by Transwell migration assays. Representative
images of migrated osteosarcoma cells on the bottom of the inserts
(bottom, left to right, control and increasing concentrations of
dDAVP). Magnification, x100. (D) 24 h viability assay using
semiconfluent MG-63 cell monolayers exposed to dDAVP. Data
presented as mean ± SEM. *P<0.05,
**P<0.01 and ***P<0.001 vs. control
group. Contingency χ2 test was used in (A) and (B).
dDAVP, Desmopressin. |
Sustained dDAVP treatment impairs
osteosarcoma xenograft growth in athymic mice
In order to explore potential therapeutic activity
on in vivo osteosarcoma growth, the effect of dDAVP
treatment was evaluated in MG-63 xenograft-bearing athymic nude
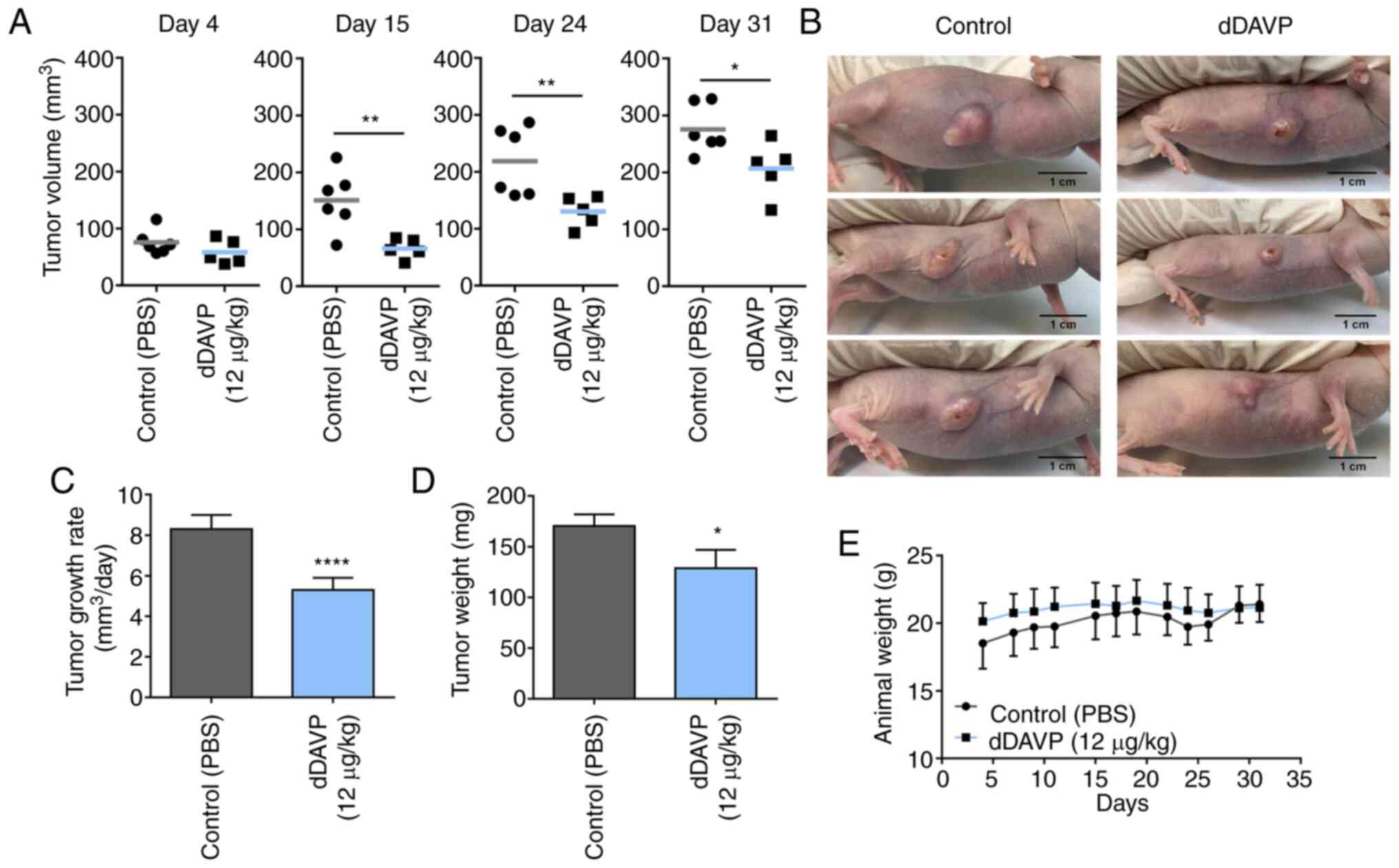
mice (Fig. 3). Sustained
intravenous administration of dDAVP (12 µg/kg) caused a significant
decrease in tumor volume over time (Fig. 3A), resulting in a tumor growth rate
inhibition of 34% in comparison to control group (Fig. 3C). Impact of dDAVP treatment on
final tumor burden was confirmed after observing a 25% reduction in
resected tumor weight (Fig. 3D).
Interestingly, despite observed significant differences regarding
disease progression between groups, at the end of the protocol the
majority of experimental subjects displayed necrotic and ulcerated
lesions with erratic and jagged tumor growth patterns (Figs. 3B and S1A and B). dDAVP treatment had no impact on the
general health status of treated animals as assessed by body weight
(Fig. 3D), and blood biochemical
and hematological studies. As observed in Table I, nearly all biochemical and
hematological parameters remain unaltered after 1 month of drug
administration. In consistency with the compound well characterized
hemostatic action, a significant 13% drop in the mean platelet
count was observed in animals receiving dDAVP.
 | Table IBiochemical and hematological
parameters assessed in EDTA-anticoagulated whole-blood from MG-63
xenograft-bearing athymic nude mice under dDAVP treatment. |
Table I
Biochemical and hematological
parameters assessed in EDTA-anticoagulated whole-blood from MG-63
xenograft-bearing athymic nude mice under dDAVP treatment.
| | Treatment
group |
|---|
| Parameter | Control (saline,
mean ± SD) | dDAVP (1 µg
kg-1, mean ± SD) |
|---|
| Weight
(g)a | 21.4±1.3 | 21.1±1.7 |
| Hematocrit (%) | 38.7±1.8 | 38.0±2.3 |
| RBC (106
ml-1) | 75.6±4.3 | 71.3±3.9 |
| WBC (103
ml-1) | 2.9±1.0 | 3.0±0.2 |
| Platelets
(106 ml-1) | 10.9±0.8 |
9.5±0.5b |
| Cholesterol (mg
dl-1) | 81.2±13.5 | 86.8±13.2 |
| Total protein (g
dl-1) | 4.2±0.4 | 4.3±0.5 |
| Direct bilirrubin
(mg dl-1) | 0.02±0.01 | 0.01±0.0 |
| Creatinine (mg
ml-1) | 0.13±0.04 | 0.14±0.04 |
| AST/GOT (IU
l-1) | 135.7±16.3 | 157.2±47.8 |
| ALT (IU
l-1) | 40.2±11.5 | 38.8±9.3 |
| Plasmatic albumin
(g dl-1) | 2.5±0.2 | 2.5±0.4 |
AVPR2 expression in osteosarcoma
xenografts and human biopsies
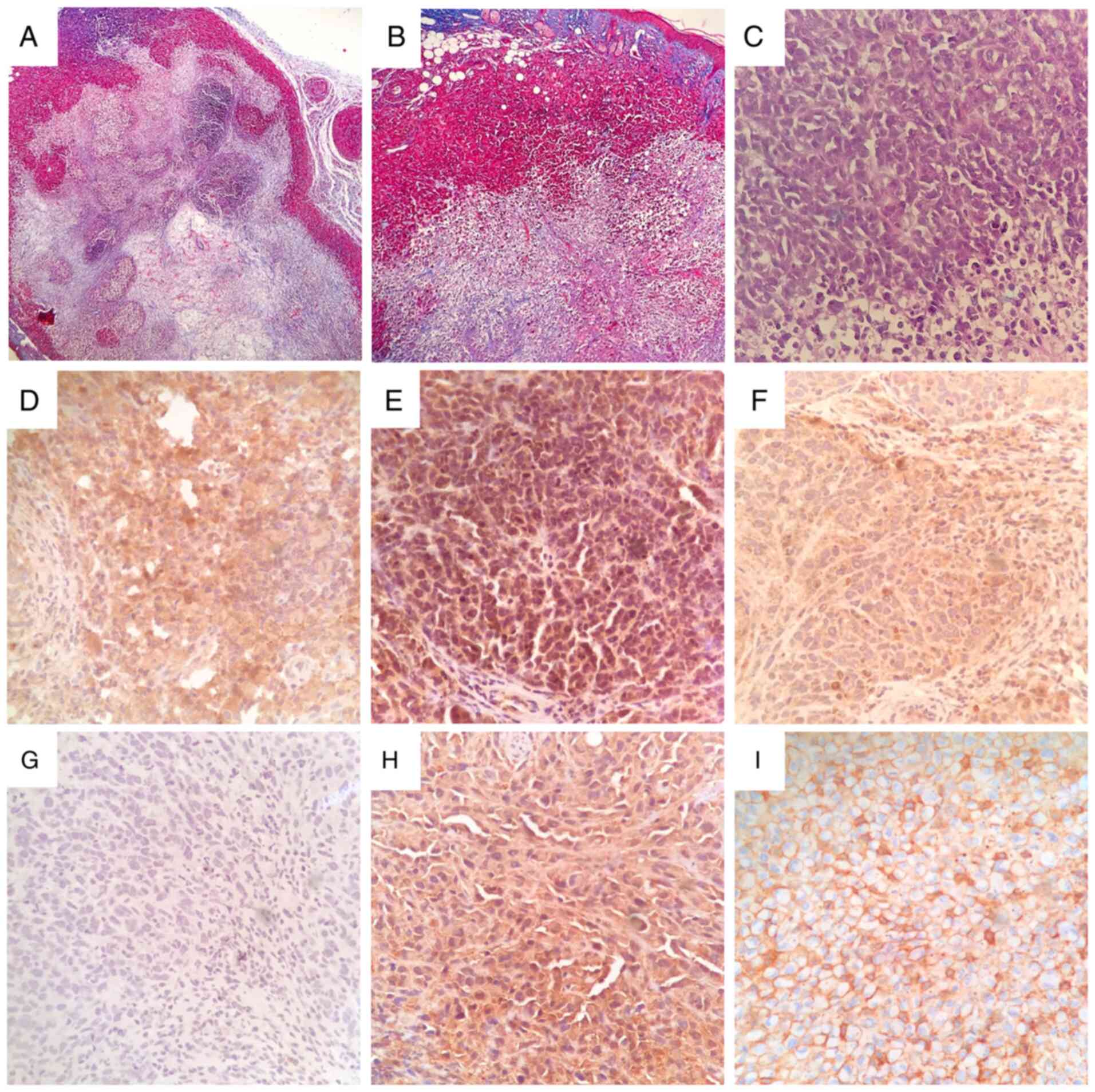
Histological assessment of rapidly growing MG-63
tumors revealed large necrotic foci with evident loose fibrous and
reticular connective tissue deposition (Fig. 4A and B), and scattered areas of high cellularity
showing typical spindle/fibroblastoid cell morphology (Fig. 4C). Large necrotic areas were found
in all tumors, and could in part explain the jagged growth patterns
and irregular progression of tumors observed in all experimental
subjects. In vivo confirmation of therapeutic target AVPR2
expression in MG-63 xenografts was conducted using IHC.
Osteosarcoma tissue displayed a diffuse membrane and cytoplasmatic
distribution of AVPR2 throughout the tumor, with variable staining
intensity (Fig. 4D, E and F).
Human MDA-MB-231 and MCF-7 breast cancer xenografts were used as
positive controls for AVPR2 expression (Fig. 4H and I) (13).
It is worth noting that, in contrast to the membranous staining
pattern observed in typically rounded and epithelial MCF-7 cells,
AVPR2 expression pattern in spindle-shaped MDA-MB-231 cells was
much more similar to that observed in MG-63 mesenchymal tumors.
AVPR2 presence was also evaluated in 6 chemotherapy-naive human
conventional osteosarcoma biopsies belonging to different
histological subtypes, as depicted in Fig. 5A-F. After IHC assessment, 66% (4/6)
of osteosarcoma samples displayed immunoreactivity, showing mild
(Fig. 5K; #16-34538), moderate
(Fig. 5I and L; #14-2289 and #16-40077) and strong
(Fig. 5J; #16-17130) staining
intensities. Osteosarcoma samples #16-24375 and #16-10997 (Fig. 5G and H) showed no immunoreactivity against
AVPR2.
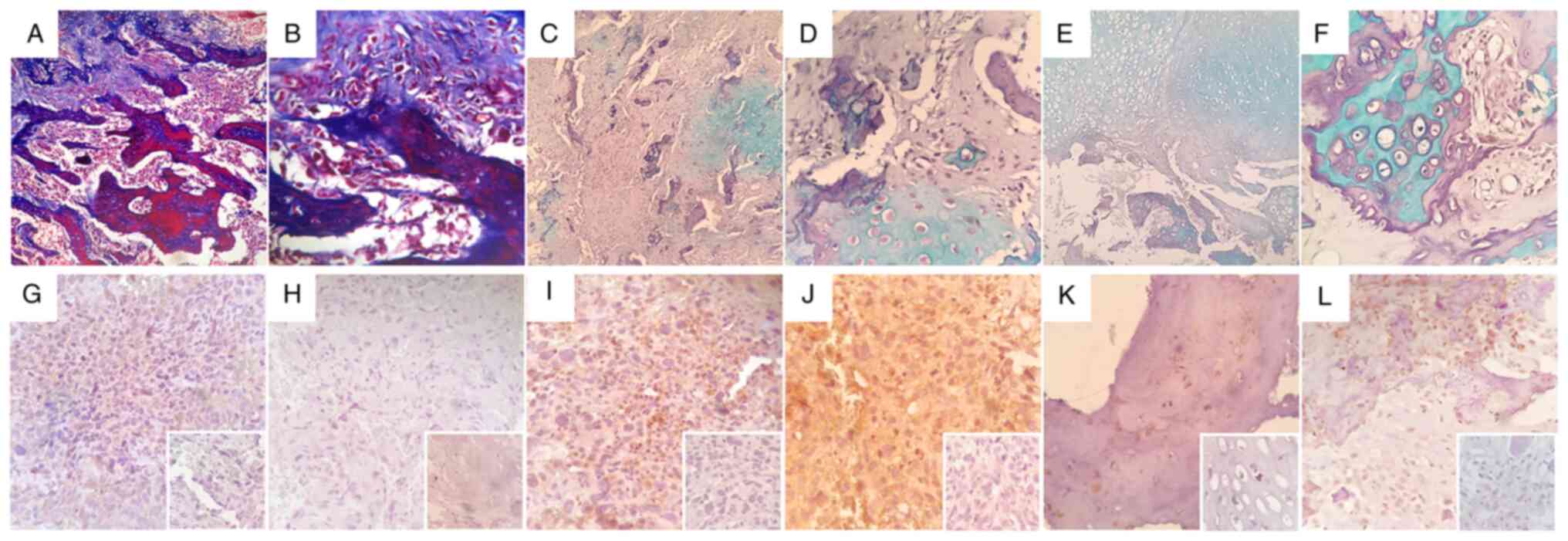 | Figure 5Immunohistochemical detection of
AVPR2 in human osteosarcoma samples. Histochemical assessment
revealing predominant osteoid extra-cellular matrix (A and B, x100
and x400 magnification, respectively), mixed osteoid/chondroid
areas (C and D, x100 and x400 magnification, respectively) or
predominant chondroid matrix (E and F, x100 and x400 magnification,
respectively) in different human conventional osteosarcoma samples;
(A and B) Sample #16-10997 with Masson's trichrome staining plus
aniline blue, (C and D) samples #16-40077 and (E and F) #16-34538
stained with hematoxylin and eosin plus alcian blue. (G-L)
Representative microphotographs of human osteosarcoma samples after
anti-AVPR2 immunohistochemistry detection. Human osteosarcoma
samples (G) #16-24375, (H) #16-10997, (I) #14-2289, (J) #16-17130,
(K) #16-34538 and (L) #16-40077 are presented. Inset: Incubation
with primary antibody was omitted. All insets are x400
magnification. AVPR2, vasopressin membrane receptor type 2. |
Discussion
In the present study, we report for the first time
the anti-osteosarcoma activity of repurposed hemostatic drug dDAVP.
Using the AVPR2-expressing MG-63 model, we showed that, in
accordance with previously reported preclinical studies (14,16-18,23-25),
in vitro dDAVP treatment reduced osteosarcoma cell growth
and chemotaxis, and cytostatic activity was related to increased
cAMP intracellular levels upon AVPR2 stimulation. Furthermore,
inhibition of cAMP-degrading phosphodiesterases by addition of
rolipram enhanced the antiproliferative effects of dDAVP in
osteosarcoma cells. Different anticancer properties of cAMP
elevating compounds, as well as cAMP synthetic derivatives, have
been reported in the past, postulating the adenylate
cyclase/cAMP/PKA signalling axis as a tumor suppressor system
(36-39).
Moreover, PDE4, a key enzyme involved in cAMP hydrolysis and
degradation, is highly expressed in human mandibular osteosarcoma,
and its pharmacological inhibition resulted in decreased cell
survival, highlighting the role of cAMP in osteosarcoma cell
proliferation (40). With the aim
of gaining knowledge on AVPR2-related signaling pathways in
osteosarcoma, and considering that cAMP is involved in a myriad of
biological processes implicated in malignant cell growth
regulation, further studies on both canonical and non-canonical
AVPR2/cAMP effectors such as PKA, exchange proteins activated by
cAMP 1 and 2 (Epac1 and 2) and the mitogen-activated protein kinase
(MAPK) on osteosarcoma cells are mandatory (41).
dDAVP antitumor activity was confirmed in
vivo on human osteosarcoma xenografts growing in
immunocompromised mice. Sustained intravenous administration of the
compound using clinically relevant equivalent doses reduced MG-63
tumor growth without clear signs of toxicity, confirming its known
profile of good tolerability and safety (11). Although growth inhibition by dDAVP
in MG-63 cells was related to increased apoptosis, impaired
migration and mitotic arrest, other potential and unexplored
AVPR2-mediated mechanisms could be playing a role in the in
vivo anti-osteosarcoma activity of the compound. It was
previously reported that dDAVP is capable of blocking
tumor-associated angiogenesis by favoring the production of
angiostatin (ANG), an endogenous angiogenesis inhibitor
specifically produced by malignant tissue. ANG overproduction
resulted from breast cancer cell-mediated proteolysis of
plasminogen as a result of AVPR2-mediated increased urokinase and
metalloproteinase activity (26,42).
As a result, ANG triggers apoptosis and reduces cell growth and
chemotaxis in both malignant and vascular cells (43,44).
Taking into account dDAVP antiangiogenic mechanisms in other tumor
types as well as the key role that angiogenesis has in osteosarcoma
biology, impact of dDAVP on pro- and antiangiogenic factor
production by osteosarcoma cells should be assessed in the
future.
As mentioned in the introduction, 20% of
osteosarcoma patients present clinically detectable metastasis at
diagnosis, and nearly 90% of them have lung lesions as the sole
site of metastasis (5,7). Interestingly, dDAVP has also proven to
be a highly antimetastatic compound, being capable of impairing
both experimental and spontaneous metastatic colonization of the
lungs and drastically decreasing local and distant spread after
surgical manipulation of aggressive tumors (14,18,28,29).
Besides its direct cytostatic and angiostatic effects, which depend
on AVPR2 expression by tumor tissue, dDAVP antimetastatic activity
was also associated to vascular release of VWF, a complex
glycoprotein capable of inducing apoptosis in disseminated tumor
cells (20-22).
Given that metastatic osteosarcoma management remains highly
challenging, further exploration of dDAVP effects on osteosarcoma
dissemination and distant organ colonization is both interesting
and necessary.
AVPR2 expression was confirmed in experimental
osteosarcoma tumors as well as in two thirds of human osteosarcoma
biopsy specimens, as evaluated by IHC. All assessed biopsies belong
to untreated patients diagnosed with conventional osteosarcoma of
different histological subtypes. Although the number of clinical
samples was rather limited, AVPR2 expression in osteosarcoma tumors
appeared to be higher than that previously reported for breast
carcinoma tumors (66 vs. 33%, respectively) (15). As new osteosarcoma cases are
currently being incorporated, comparison of AVPR2 expression
between primary and metastatic lesions or between pre- and
post-chemotherapy, as well as correlation between AVPR2 expression
and disease progression will be assessed in future studies.
Regardless of the chosen chemotherapy regimen,
resection of both primary and secondary osteosarcoma remains
critical for obtaining remission and improving patient survival.
Osteosarcoma removal using amputation or limb salvage techniques
involves complex and time-consuming surgical procedures often
associated to high-volume blood loss and perioperative transfusion
requirements. As observed in many types of cancer, evidence suggest
a strong link between perisurgical transfusion, immunosuppression
and worse prognosis in patients undergoing resection of
osteosarcoma or other bone sarcomas (45,46).
Moreover, surgical manipulation of the tumor could favor
dissemination and growth of residual cells by inducing local and
systemic inflammatory responses, increased production of
proangiogenic factors and suppression of antimetastatic immunity
(47,48). As reviewed by Pantziarka and Bouche,
as a consequence of these multiple prorecurrence mechanisms
associated with tumor resection, osteosarcoma is associated with
alarmingly high recurrence rates in comparison to other cancer
types, showing distant recurrence rates after curative intent
surgery of nearly 50% (49). In
this setting, perioperative administration of dDAVP during
osteosarcoma removal could provide several therapeutic benefits.
First, compound reduces intraoperative bleeding after releasing VWF
and other hemostatic factors from vascular endothelium, reducing
the need of perisurgical blood transfusion. On the other hand,
dDAVP could limit osteosarcoma recurrence after surgery by
impairing the survival and outgrowth of disseminated tumor cells
(50,51). In order to evaluate if perioperative
dDAVP (administered immediately prior to surgery and during the
early postoperative period) could help to antagonize deleterious
mechanisms triggered by surgery, drug should be tested using
experimental models of incomplete surgical resection of
osteosarcoma tumors, especially in syngeneic and immunocompetent
animal models (52,53). Apart from evaluating time to local
recurrence or metastatic progression to lungs, modulation of
signaling pathways involved in cancer cell growth and angiogenesis
should also be assessed in the postsurgical and premetastatic
niches. Furthermore, given its low-associated toxicity and low
production costs, dDAVP could be used as a safe and affordable
perioperative therapy without increasing the risk of surgical
complications or perisurgical costs.
It is important to note that osteosarcomas are known
to promote a hypercoagulation state in certain patients. There is
some evidence indicating that human osteosarcoma cells such as
MG-63 can induce platelet aggregation activity by interacting with
platelet membrane glycoproteins Ib/IX and IIb/IIIa even in
VWF-deficient plasma (54).
However, the evidence for high VWF levels induced by dDAVP as a
risk factor for venous thromboembolism is weak and perioperative
use of the compound appears safe. In this regard, dDAVP
administration also produces a rapid release of tissue-type
plasminogen activator, with consequent activation of fibrinolysis
and shortening of euglobulin lysis time. dDAVP has few hemostatic
side effects but caution in small children and elderly people is
recommended, due to the risk of fluid retention and hyponatremia
(11).
Drug repurposing stands as an interesting approach
in oncology, not only for overwhelmed health-care systems or
developing countries with restrained economies, but also for rare
and aggressive diseases with limited therapeutic alternatives
(8-10).
As observed in many diseases, prognosis of osteosarcoma patients is
significantly worse in LMICs, mainly due to inadequate access to
diagnostic and therapeutic resources, including surgery and
radio-chemotherapy (5-7).
In this setting, repurposing of blood-saving agent dDAVP for
osteosarcoma treatment is highly promising due to its
widely-characterized clinical use, potential antitumor activity,
low treatment-associated toxicity and production costs. Compound
could be administered as a co-adjuvant agent concomitantly with
chemotherapy or during complex osteosarcoma removal procedures in a
perioperative manner.
Supplementary Material
(A) Mean and (B) individual mouse
tumor volumes measured over time from day 4 after osteosarcoma cell
inoculation in athymic mice. Results are expressed as mean ± SEM.
****P<0.0001. dDAVP, desmopressin.
Acknowledgements
The authors would like to acknowledge the
participation of Dr Berenice Freile (Alexander Fleming Institute,
Buenos Aires, Argentina) and Dr Alejandra Scursoni (Hospital ‘Dr
Isidoro Iriarte’, Buenos Aires, Argentina) for their involvement in
histological processing and analysis, and Dr Guillermo Chantada,
(Pediatric Hospital ‘Prof. Dr Juan P. Garrahan’, Buenos Aires,
Argentina) for critical reading and reviewing of the manuscript.
MG-63 and U-2 OS cell lines were kindly provided by Dr Ignacio E.
León (Laboratory of Metal based Drugs, National University of La
Plata, Buenos Aires, Argentina) and Dr Vanesa Gottifredi (Cell
Cycle and Genomic Stability Lab, Leloir Institute Foundation,
Buenos Aires, Argentina), respectively.
Funding
Funding: The current study was supported by the National Agency
for the Promotion of Science and Technology (ANPCYT; Argentina;
grant no. PICT2017/2056), the National Institute of Cancer (grant
no. INC2018/2020) and the National University of Quilmes Research
Program grant (grant no. PUNQ1297/19).
Availability of data and materials
The datasets used and/or analyzed during the current
study are available from the corresponding author on reasonable
request.
Authors' contributions
NTS performed formal analysis, conducted the
experiments, assessed the authenticity of raw data, contributed to
the methodology and validation of the current study. LMS performed
formal analysis, data curation, conducted the experiments, assessed
the authenticity of raw data, contributed to the methodology of the
current study and wrote the manuscript. BB contributed to the
methodology and validation of the current study and reviewed and
edited the manuscript. LV contributed to the methodology and
validation of the current study and reviewed and edited the
manuscript. GVR performed formal analysis and data curation. JG
conceptualized the study, performed formal analysis, acquired
funding, contributed to the methodology and validation of the
current study, was involved in project administration, validation
and visualization and wrote, reviewed and edited the manuscript.
DFA conceptualized the study, acquired funding, was involved in
project administration, reviewed and edited the manuscript and
supervised the study. All authors read and approved the final
manuscript.
Ethics approval and consent to
participate
Clinical tumor samples were used for histological
studies. Approval for the project was obtained from the Ethics
Committee of the Edgardo Rebagliati Martins National Hospital.
Written informed consent was obtained from all patients or their
parents prior to the samples' examination. All animal protocols
were carried out in accordance with the Guide for the Care and Use
of Laboratory Animals as adopted by the U.S. National Institutes of
Health (NIH Publications No. 8023, revised 1978) and were approved
by our institutional Animal Care Committee UNQ-CICUAL (Resolution
CD CyT No. 075/14); Protocol code: 011-15. Results were reported
following the ARRIVE guidelines.
Patient consent for publication
Not applicable.
Competing interests
The authors declare that they have no competing
interests.
References
|
1
|
Mirabello L, Troisi RJ and Savage SA:
International osteosarcoma incidence patterns in children and
adolescents, middle ages and elderly persons. Int J Cancer.
125:229–234. 2009.PubMed/NCBI View Article : Google Scholar
|
|
2
|
Durfee RA, Mohammed M and Luu HH: Review
of osteosarcoma and current management. Rheumatol Ther. 3:221–243.
2016.PubMed/NCBI View Article : Google Scholar
|
|
3
|
Marec-Berard P, Laurence V, Occean BV,
Ray-Coquard I, Linassier C, Corradini N, Collard O, Chaigneau L,
Cupissol D, Kerbrat P, et al: Methotrexate-Etoposide-ifosfamide
compared with doxorubicin-cisplatin-ifosfamide chemotherapy in
osteosarcoma treatment, patients aged 18-25 years. J Adolesc Young
Adult Oncol. 9:172–182. 2020.PubMed/NCBI View Article : Google Scholar
|
|
4
|
Meazza C and Scanagatta P: Metastatic
osteosarcoma: A challenging multidisciplinary treatment. Expert Rev
Anticancer Ther. 16:543–556. 2016.PubMed/NCBI View Article : Google Scholar
|
|
5
|
Moreno F, Cacciavillano W, Cipolla M,
Coirini M, Streitenberger P, Lopez Marti J, Palladino M, Morici M,
Onoratelli M, Drago G, et al: Childhood osteosarcoma: Incidence and
survival in argentina. report from the national pediatric cancer
registry, ROHA network 2000-2013. Pediatr Blood Cancer 64 2017.
|
|
6
|
Revon-Riviere G, Banavali S, Heississen L,
Gomez Garcia W, Abdolkarimi B, Vaithilingum M, Li CK, Leung PC,
Malik P, Pasquier E, et al: Metronomic chemotherapy for children in
low- and middle-income countries: Survey of current practices and
opinions of pediatric oncologists. J Glob Oncol. 5:1–8.
2019.PubMed/NCBI View Article : Google Scholar
|
|
7
|
Gyawali B, Bouche G, Crisp N and André N:
Challenges and opportunities for cancer clinical trials in low- and
middle-income countries. Nature Cancer. 1:142–145. 2020.
|
|
8
|
Bertolini F, Sukhatme VP and Bouche G:
Drug repurposing in oncology-patient and health systems
opportunities. Nat Rev Clin Oncol. 12:732–742. 2015.PubMed/NCBI View Article : Google Scholar
|
|
9
|
Pushpakom S, Iorio F, Eyers PA, Escott KJ,
Hopper S, Wells A, Doig A, Guilliams T, Latimer J, McNamee C, et
al: Drug repurposing: Progress, challenges and recommendations. Nat
Rev Drug Discov. 18:41–58. 2019.PubMed/NCBI View Article : Google Scholar
|
|
10
|
Pantziarka P and Andre N: Editorial: Drug
repurposing. Front Med (Lausanne). 6(154)2019.PubMed/NCBI View Article : Google Scholar
|
|
11
|
Svensson PJ, Bergqvist PB, Juul KV and
Berntorp E: Desmopressin in treatment of haematological disorders
and in prevention of surgical bleeding. Blood Rev. 28:95–102.
2014.PubMed/NCBI View Article : Google Scholar
|
|
12
|
Kaufmann JE, Oksche A, Wollheim CB,
Gunther G, Rosenthal W and Vischer UM: Vasopressin-induced von
Willebrand factor secretion from endothelial cells involves V2
receptors and cAMP. J Clin Invest. 106:107–116. 2000.PubMed/NCBI View
Article : Google Scholar
|
|
13
|
Garona J, Pifano M, Pastrian MB, Gomez DE,
Ripoll GV and Alonso DF: Addition of vasopressin synthetic analogue
[V(4)Q(5)]dDAVP to standard chemotherapy enhances tumour growth
inhibition and impairs metastatic spread in aggressive breast
tumour models. Clin Exp Metastasis. 33:589–600. 2016.PubMed/NCBI View Article : Google Scholar
|
|
14
|
Garona J, Pifano M, Scursoni AM, Gomez DE,
Alonso DF and Ripoll GV: Insight into the effect of the vasopressin
analog desmopressin on lung colonization by mammary carcinoma cells
in BALB/c mice. Anticancer Res. 34:4761–4765. 2014.PubMed/NCBI
|
|
15
|
Weinberg RS, Grecco MO, Ferro GS,
Seigelshifer DJ, Perroni NV, Terrier FJ, Sánchez-Luceros A, Maronna
E, Sánchez-Marull R, Frahm I, et al: A phase II dose-escalation
trial of perioperative desmopressin (1-desamino-8-d-arginine
vasopressin) in breast cancer patients. Springerplus.
4(428)2015.PubMed/NCBI View Article : Google Scholar
|
|
16
|
Pifano M, Garona J, Capobianco CS,
Gonzalez N, Alonso DF and Ripoll GV: Peptide agonists of
vasopressin V2 receptor reduce expression of neuroendocrine markers
and tumor growth in human lung and prostate tumor cells. Front
Oncol. 7(11)2017.PubMed/NCBI View Article : Google Scholar
|
|
17
|
Pifano M, Garona J, Sobol NT, Alberto M,
Alonso DF and Ripoll GV: Search of vasopressin analogs with
antiproliferative activity on small-cell lung cancer: Drug design
based on two different approaches. Future Med Chem. 10:879–894.
2018.PubMed/NCBI View Article : Google Scholar
|
|
18
|
Ripoll GV, Garona J, Hermo GA, Gomez DE
and Alonso DF: Effects of the synthetic vasopressin analog
desmopressin in a mouse model of colon cancer. Anticancer Res.
30:5049–5054. 2010.PubMed/NCBI
|
|
19
|
Garona J, Sobol NT, Pifano M, Segatori VI,
Gomez DE, Ripoll GV and Alonso DF: Preclinical efficacy of [V4
Q5]dDAVP, a second generation vasopressin analog, on metastatic
spread and tumor-associated angiogenesis in colorectal cancer.
Cancer Res Treat. 51:438–450. 2019.PubMed/NCBI View Article : Google Scholar
|
|
20
|
Terraube V, Pendu R, Baruch D, Gebbink MF,
Meyer D, Lenting PJ and Denis CV: Increased metastatic potential of
tumor cells in von Willebrand factor-deficient mice. J Thromb
Haemost. 4:519–526. 2006.PubMed/NCBI View Article : Google Scholar
|
|
21
|
Mochizuki S, Soejima K, Shimoda M, Abe H,
Sasaki A, Okano HJ, Okano H and Okada Y: Effect of ADAM28 on
carcinoma cell metastasis by cleavage of von Willebrand factor. J
Natl Cancer Inst. 104:906–922. 2012.PubMed/NCBI View Article : Google Scholar
|
|
22
|
Gragnano F, Sperlongano S, Golia E, Natale
F, Bianchi R, Crisci M, Fimiani F, Pariggiano I, Diana V, Carbone
A, et al: The role of von willebrand factor in vascular
inflammation: From pathogenesis to targeted therapy. Mediators
Inflamm. 2017(5620314)2017.PubMed/NCBI View Article : Google Scholar
|
|
23
|
Keegan BP, Akerman BL, Pequeux C and North
WG: Provasopressin expression by breast cancer cells: Implications
for growth and novel treatment strategies. Breast Cancer Res Treat.
95:265–277. 2006.PubMed/NCBI View Article : Google Scholar
|
|
24
|
Garona J, Pifano M, Orlando UD, Pastrian
MB, Iannucci NB, Ortega HH, Podesta EJ, Gomez DE, Ripoll GV and
Alonso DF: The novel desmopressin analogue [V4Q5]dDAVP inhibits
angiogenesis, tumour growth and metastases in vasopressin type 2
receptor-expressing breast cancer models. Int J Oncol.
46:2335–2345. 2015.PubMed/NCBI View Article : Google Scholar
|
|
25
|
Sasaki H, Klotz LH, Sugar LM, Kiss A and
Venkateswaran V: A combination of desmopressin and docetaxel
inhibit cell proliferation and invasion mediated by urokinase-type
plasminogen activator (uPA) in human prostate cancer cells. Biochem
Biophys Res Commun. 464:848–854. 2015.PubMed/NCBI View Article : Google Scholar
|
|
26
|
Ripoll GV, Garona J, Pifano M, Farina HG,
Gomez DE and Alonso DF: Reduction of tumor angiogenesis induced by
desmopressin in a breast cancer model. Breast Cancer Res Treat.
142:9–18. 2013.PubMed/NCBI View Article : Google Scholar
|
|
27
|
Ripoll GV, Farina HG, Yoshiji H, Gomez DE
and Alonso DF: Desmopressin reduces melanoma lung metastasis in
transgenic mice overexpressing tissue inhibitor of
metalloproteinases-1. In Vivo. 20:881–885. 2006.PubMed/NCBI
|
|
28
|
Alonso DF, Skilton G, Farias EF, Bal de
Kier Joffe E and Gomez DE: Antimetastatic effect of desmopressin in
a mouse mammary tumor model. Breast Cancer Res Treat. 57:271–275.
1999.PubMed/NCBI View Article : Google Scholar
|
|
29
|
Giron S, Tejera AM, Ripoll GV, Gomez DE
and Alonso DF: Desmopressin inhibits lung and lymph node metastasis
in a mouse mammary carcinoma model of surgical manipulation. J Surg
Oncol. 81:38–44. 2002.PubMed/NCBI View Article : Google Scholar
|
|
30
|
Hermo GA, Torres P, Ripoll GV, Scursoni
AM, Gomez DE, Alonso DF and Gobello C: Perioperative desmopressin
prolongs survival in surgically treated bitches with mammary gland
tumours: A pilot study. Vet J. 178:103–108. 2008.PubMed/NCBI View Article : Google Scholar
|
|
31
|
Hermo GA, Turic E, Angelico D, Scursoni
AM, Gomez DE, Gobello C and Alonso DF: Effect of adjuvant
perioperative desmopressin in locally advanced canine mammary
carcinoma and its relation to histologic grade. J Am Anim Hosp
Assoc. 47:21–27. 2011.PubMed/NCBI View Article : Google Scholar
|
|
32
|
Iseas S, Roca EL, O'Connor JM, Eleta M,
Sanchez-Luceros A, Di Leo D, Tinelli M, Fara ML, Spitzer E, Demarco
IA, et al: Administration of the vasopressin analog desmopressin
for the management of bleeding in rectal cancer patients: Results
of a phase I/II trial. Invest New Drugs. 38:1580–1587.
2020.PubMed/NCBI View Article : Google Scholar
|
|
33
|
Nair AB and Jacob S: A simple practice
guide for dose conversion between animals and human. J Basic Clin
Pharm. 7:27–31. 2016.PubMed/NCBI View Article : Google Scholar
|
|
34
|
Ray G, Banerjee S, Saxena NK, Campbell DR,
Van Veldhuizen P and Banerjee SK: Stimulation of MCF-7 tumor
progression in athymic nude mice by 17beta-estradiol induces
WISP-2/CCN5 expression in xenografts: A novel signaling molecule in
hormonal carcinogenesis. Oncol Rep. 13:445–448. 2005.PubMed/NCBI
|
|
35
|
Pastrian MB, Guzman F, Garona J, Pifano M,
Ripoll GV, Cascone O, Ciccia GN, Albericio F, Gómez DE, Alonso DF
and Iannucci NB: Structure-activity relationship of
1-desamino-8-D-arginine vasopressin as an antiproliferative agent
on human vasopressin V2 receptor-expressing cancer cells. Mol Med
Rep. 9:2568–2572. 2014.PubMed/NCBI View Article : Google Scholar
|
|
36
|
Carie AE and Sebti SM: A chemical biology
approach identifies a beta-2 adrenergic receptor agonist that
causes human tumor regression by blocking the Raf-1/Mek-1/Erk1/2
pathway. Oncogene. 26:3777–3788. 2007.PubMed/NCBI View Article : Google Scholar
|
|
37
|
Insel PA, Zhang L, Murray F, Yokouchi H
and Zambon AC: Cyclic AMP is both a pro-apoptotic and
anti-apoptotic second messenger. Acta Physiol (Oxf). 204:277–287.
2012.PubMed/NCBI View Article : Google Scholar
|
|
38
|
Naviglio S, Di Gesto D, Romano M,
Sorrentino A, Illiano F, Sorvillo L, Abbruzzese A, Marra M,
Caraglia M, Chiosi E, et al: Leptin enhances growth inhibition by
cAMP elevating agents through apoptosis of MDA-MB-231 breast cancer
cells. Cancer Biol Ther. 8:1183–1190. 2009.PubMed/NCBI View Article : Google Scholar
|
|
39
|
Castoria G, Migliaccio A, D'Amato L, Di
Stasio R, Ciociola A, Lombardi M, Bilancio A, Di Domenico M, de
Falco A and Auricchio F: Integrating signals between cAMP and MAPK
pathways in breast cancer. Front Biosci. 13:1318–1327.
2008.PubMed/NCBI View
Article : Google Scholar
|
|
40
|
Narita M, Murata T, Shimizu K, Sugiyama T,
Nakagawa T, Manganiello VC and Tagawa T: Phosphodiesterase 4 in
osteoblastic osteosarcoma cells as a potential target for growth
inhibition. Anticancer Drugs. 14:377–381. 2003.PubMed/NCBI View Article : Google Scholar
|
|
41
|
Fajardo AM, Piazza GA and Tinsley HN: The
role of cyclic nucleotide signaling pathways in cancer: Targets for
prevention and treatment. Cancers (Basel). 6:436–458.
2014.PubMed/NCBI View Article : Google Scholar
|
|
42
|
Ripoll G, Iannucci N, Giron S, Cascone O,
Gomez D and Alonso D: Angiostatic activity of
1-Deamino-8-D-Arginine vasopressin and novel peptide analogues in
breast cancer cells. Cancer Res. 68(295)2008.
|
|
43
|
Sakurai T and Kudo M: Signaling pathways
governing tumor angiogenesis. Oncology. 81 (Suppl 1):S24–S29.
2011.PubMed/NCBI View Article : Google Scholar
|
|
44
|
Westphal JR, Van't Hullenaar R,
Geurts-Moespot A, Sweep FC, Verheijen JH, Bussemakers MM, Askaa J,
Clemmensen I, Eggermont AA, Ruiter DJ and De Waal RM: Angiostatin
generation by human tumor cell lines: Involvement of plasminogen
activators. Int J Cancer. 86:760–767. 2000.PubMed/NCBI View Article : Google Scholar
|
|
45
|
Chesi R, Cazzola A, Bacci G, Borghi B,
Balladelli A and Urso G: Effect of perioperative transfusions on
survival in osteosarcoma treated by multimodal therapy. Cancer.
64:1727–1737. 1989.PubMed/NCBI View Article : Google Scholar
|
|
46
|
Park JH, Hong SH and Jang WY: Restrictive
allogeneic blood transfusion strategy in patients with extremity
bone sarcomas. Medicine (Baltimore). 98(e18482)2019.PubMed/NCBI View Article : Google Scholar
|
|
47
|
Horowitz M, Neeman E, Sharon E and
Ben-Eliyahu S: Exploiting the critical perioperative period to
improve long-term cancer outcomes. Nat Rev Clin Oncol. 12:213–226.
2015.PubMed/NCBI View Article : Google Scholar
|
|
48
|
Garona J and Alonso DF: Perioperative
biology in primary breast cancer: Selective targeting of
vasopressin type 2 receptor using desmopressin as a novel
therapeutic approach. Breast Cancer Res Treat. 158:597–599.
2016.PubMed/NCBI View Article : Google Scholar
|
|
49
|
Pantziarka P and Bouche G: Perioperative
therapies-using repurposed drugs to improve cancer surgery
outcomes. Cancer J. 25:100–105. 2019.PubMed/NCBI View Article : Google Scholar
|
|
50
|
Garona J, Sobol NT and Alonso DF: Impact
of Perioperative blood transfusion on survival among women with
breast cancer: Potential benefits of blood-saving agent
desmopressin use during surgery. Am J Ther. 25:e569–e570.
2018.PubMed/NCBI View Article : Google Scholar
|
|
51
|
Garona J, Sobol NT, Solerno LM and Alonso
DF: Potential use of desmopressin during hepatic resection for
colorectal liver metastases. J Surg Res. 237:1–2. 2019.PubMed/NCBI View Article : Google Scholar
|
|
52
|
Gottardo MF, Capobianco CS, Sidabra JE,
Garona J, Perera Y, Perea SE, Alonso DF and Farina HG: Preclinical
efficacy of CIGB-300, an anti-CK2 peptide, on breast cancer
metastasic colonization. Sci Rep. 10(14689)2020.PubMed/NCBI View Article : Google Scholar
|
|
53
|
Guijarro MV, Ghivizzani SC and Gibbs CP:
Animal models in osteosarcoma. Front Oncol. 4(189)2014.PubMed/NCBI View Article : Google Scholar
|
|
54
|
Clezardin P, Drouin J, Morel-Kopp MC,
Hanss M, Kehrel B, Serre CM, Kaplan C and Delmas PD: Role of
platelet membrane glycoproteins Ib/IX and IIb/IIIa, and of platelet
alpha-granule proteins in platelet aggregation induced by human
osteosarcoma cells. Cancer Res. 53:4695–4700. 1993.PubMed/NCBI
|