Introduction
Non-invasive coronary computed tomography
angiography (CCTA) detects significant (≥50%) lumen reduction
associated with coronary artery disease (CAD) (1). In particular, high sensitivity and
negative predictive value (NPV) of ≥95% highlight the diagnostic
technique since its introduction into the clinical practice two
decades ago (2). Of note, clinical
limitation of CCTA is associated with the presence of extensive
coronary calcification, which may lead to false-positive findings;
thus, current guidelines consider CCTA inappropriate in high-risk
populations (3). Those patients
may benefit from the complex approach combining CCTA and myocardial
CT perfusion (CT-MPI) examination to reduce the number of patients
undergoing invasive coronary angiography due to a false-positive
non-invasive approach (4).
In the past, adenosine and dipyridamole were used as
standard pharmacologic stress agents inducing vasodilatation during
CT-MPI (5). However, their use was
associated with frequent adverse events (mild events with higher
frequency: Flushes, chest pain, dyspnea, dizziness and nausea;
serious events with lower frequency: Bronchospasm, atrioventricular
block, and peripheral vasodilation) in ≤80% of patients (6,7).
Therefore clinicians have begun to use regadenoson (selective
A2A receptor agonist) (8) that is associated with improved safety
and tolerability profile when compared with adenosine
(non-selective A1, A2A, A2B and
A3 receptor agonist) (9). Another major advantage of regadenoson
over adenosine and/or dipyridamole is that it is administered as a
single bolus (0.4 mg) whereas adenosine (10) and dipyridamole (11) must be administered as
weight-adjusted infusions. Despite the advantages of regadenoson
over adenosine, clinicians should be aware of potential side
effects. Even though the majority of adverse effects are short,
benign, and spontaneously terminate, they rarely may also graduate
to more serious events (e.g., symptomatic myocardial ischemia,
infarction, atrioventricular block, asystole and/or seizures)
(12). Regadenoson had been
approved by the Food and Drug Administration in 2008 as the next
stress agent for CT-MPI examination (13,14)
whereas the approval in the Slovak Republic came over a decade
later in 2019. The present study presents first experiences from
the East-Slovak Institute of Cardiovascular Diseases with the
administration of regadenoson (with direct comparison to adenosine)
for myocardial perfusion scans.
Materials and methods
The present study retrospectively analyzed 46
patients (Table I) with varying
degrees of coronary artery disease, from nonspecific chest pain to
patients after stent implantation following coronary bypass surgery
to confirm/exclude myocardial perfusion defects.
 | Table IPatient demographic data with relevant
medical history. |
Table I
Patient demographic data with relevant
medical history.
| Population | Adenosine | Regadenoson | P-value |
|---|
| Number of
patients | 15 | 31 | |
| Age | 63.87±10.27
(F72.25±8.84/M60.81±9.26) | 64.74±9.9
(F69.66±8.91/M62.72±9.75) | 0.7825 |
| Sex | 4F/11M | 9F/22M | |
| BMI | 31.66±5.33
(F30.65±4.75/M32.02±5.70) | 29.49±5.46
(F30.87±6.34/M28.91±5.11) | 0.2097 |
| History | | | |
|
CAD | 80.00%
(F-75%/M-81.81%) | 83.87%
(F-77.77%/M-86.36%) | 0.7520 |
|
Myocardial
infarction | 26.66%
(F-0.0%/M-36.36%) | 48.38%
(F-22.22%/M-59.09%) | 0.1679 |
|
PTCA without
stent | 40%
(F-75%/M-27.27%) | 25.81%
(F-44.44%/M-18.18%) | 0.6147 |
|
PTCA with
stent | 26.66%
(F-0.0%/M-36.36%) | 45.16%
(F-11.11%/M-59.09%) | 0.9152 |
|
Bypass | 6.66%
(F-0.0%/M-9.09%) | 9.67%
(F-0.0%/M-13.64%) | 0.3829 |
| Cardiovascular risk
factors | | | |
|
DM | 33.33%
(F50%/M27.27%) | 32.25%
(F11.11%/M40.90%) | 0.9435 |
|
DLP | 80%
(F75%/M81.81%) | 83.87%
(F88.88%/M81.81%) | 0.7520 |
|
HT | 100%
(F100%/M100%) | 90.32%
(F88.88%/M90.90%) | 0.2178 |
|
FH | 53.33%
(F75%/M45.45%) | 48.38%
(F44.44%/M50%) | 0.7596 |
|
S | 40%
(F25%/M45.45%) | 35.48%
(F11.11%/M45.45%) | 0.7723 |
A stress-rest protocol was used in all patients. Of
the total patient sample, 32 were men and 14 were women in the age
categories between 43 and 84 years. Two types of stress-inducing
drugs were administered to the patients: Adenosine (Adenocor) or
reganedoson (Rapiscan). Adenocor was administered to 15 while
Rapiscan was administered to 31 patients.
The East-Slovak Institute of Cardiovascular Diseases
has the latest CT Somatom Force device (Siemens Healthcare GmbH).
This is a third generation dual source CT. The critical features of
this CT device for successful performance of myocardial perfusion
scan are: i) Scan parameters: 2x96x0.6-mm collimation resulting in
a 105-mm z-axis coverage by shuttle mode, ii) rotation time ≤250
msec, iii) temporal resolution ≤66 msec, iv) spatial resolution
0.24 mm, v) tube voltage 70-80 kV with automated exposure control
(300 mAs/rotation at 80 kV as reference), vi) 3.0-mm-thick slices
reconstructed with 2.0-mm overlap and vii) maximum speed of 73
cm/sec with Turbo Flash.
All subjects were kindly asked to refrain from
caffeine-containing drinks for 12 h and nicotine (may act as a
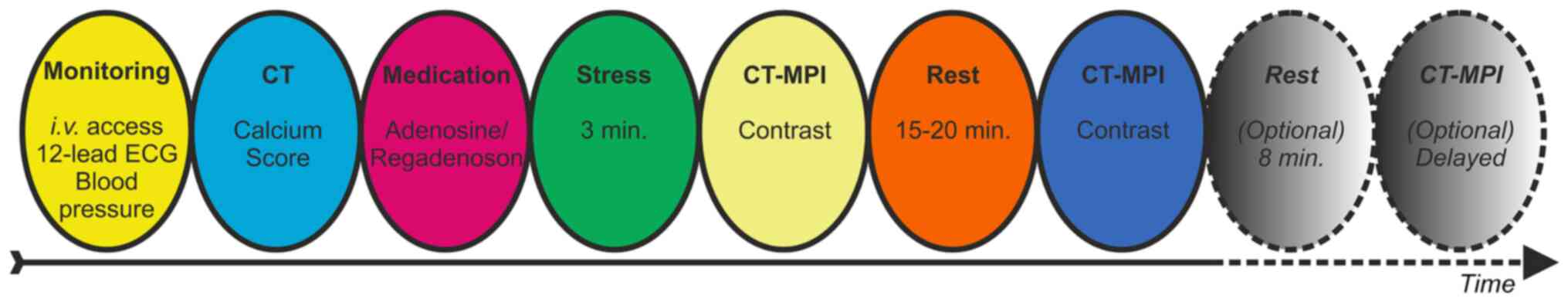
vasodilators) for 3 h prior the scan (15). The stress-rest protocol is shown in
Fig. 1. The cardiac rhythm was
continuously monitored, and the blood pressure was measured at
regular intervals. Briefly, stress protocol (hyperemia) was induced
by i) intravenous adenosine (140 µg/kg/min) over 3 min or ii)
intravenous regadenoson (single bolus of 0.4 mg). The standard
contrast injection protocol was a 50 ml in load phase and 50 ml in
rest phase contrast bolus at 5.5 ml/s (iopromide; Ultravist; Bayer
AG; 370 mg/ml), followed by 40 ml saline. The CT-MPI scan started 4
sec after contrast injection, using alternating table positions
(shuttle mode) for complete myocardial coverage. Cardiac shuttle
mode scan at CT SOMATOM Force is a dual source prospective ECG
triggered sequence with shuttle move of the table. The 10.5 cm
range is scanned in two slabs where each slab is scanned in
separated R-R intervals (usually in systolic phase). Speed of the
table is dynamic and is dependent on heart rate. Speed at start and
end position is slower to avoid movement artifacts. Since each R-R
interval is scanned in shuttle mode, the approximate table speed in
patient with heart rate 60 beats/min is >50 mm/sec. The data set
consisted of 10-15 CT data samples over 30 sec.
The rest protocol was performed 15-20 min after the
first CT-MPI and included both the second CT-MPI and CCTA using
prospective electrocardiogram-triggered axial or high-pitch spiral
scans. Sublingual nitroglycerin was administered before CCTA and
intravenous β1-blockers were given if the heart rate was >75
beats per min (BPM). Images were reconstructed with a medium-smooth
kernel, 0.6-mm slice thickness and 0.4 mm increments.
All CT scans were examined by two experienced
radiologists blinded to clinical history using syngo. CT Myocardial
Perfusion (Siemens Healthcare GmbH), a widely used CTP
post-processing software. Quality of the image was evaluated by a
4-point scale (Likert). Low quality CT-MPI images were omitted from
the analysis. Discordant findings were reconciled during a
consensus read. For qualitative analysis dynamic stress CT
perfusion study was interpreted visually in conjunction with
delayed enhancement CT viability scan. A myocardial segment was
considered as showing reversible ischemia when hypoperfusion lasted
>6 heart beats under adenosine/regadenoson stress without
delayed enhancement on viability scans. Homogeneously perfused
myocardium during adenosine/regadenoson stress that did not show
delayed enhancement on viability studies was classified as normal
(16).
Coronary stenosis were classified based on the
Coronary Artery Disease Reporting and Data System (17). CT-MPI maps were compared
side-by-side with the CTA images. The coronary anatomy based on the
CTA scan was used to locate myocardial perfusion defects to the
respective coronary artery. Based on the CCTA and CT-MPI scans, the
presence of hemodynamically relevant CADs were determined (CT-MPI
findings were superior to CCTA). The most severely affected
coronary branch determined per-territory disease
classification.
The myocardial blood flow (MBF; ml/100 ml/min)
per-coronary artery territory was calculated from maximum slope of
the fit model curve normalized to the peak arterial enhancement as
follow: A region of interest (corresponding to 0.5 cm3
of subendocardial myocardium) was sampled onto the MBF polar maps
for each vessel territory (either in the area of suspected ischemia
or centrally within territories without suspected ischemia). The
reference MBF was defined as the 75th percentile of the
automatically generated global endocardial MBF representing a
robust measure of normal MBF in a specific patient/examination
relatively unaffected by territorial ischemia or artifacts
(18). Relative MBF was calculated
(per vessel territory) as the absolute MBF divided by the reference
MBF.
Statistical analysis was conducted with the MedCalc
Version 12.5.00 (MedCalc Software Ltd.) software. Selected
demographic data with relevant medical history (see Table I), MBF, calcium score and BPM
values were expressed as mean ± standard deviation and compared
(between adenosine and regadenoson group) with the unpaired t-test
or non-parametric Kruskal-Wallis test. For correlation analysis
(BMI correlation with MBF or BPM increase), the Spearman's rho
coefficient was calculated. P<0.05 was considered to indicate a
statistically significant difference.
Results
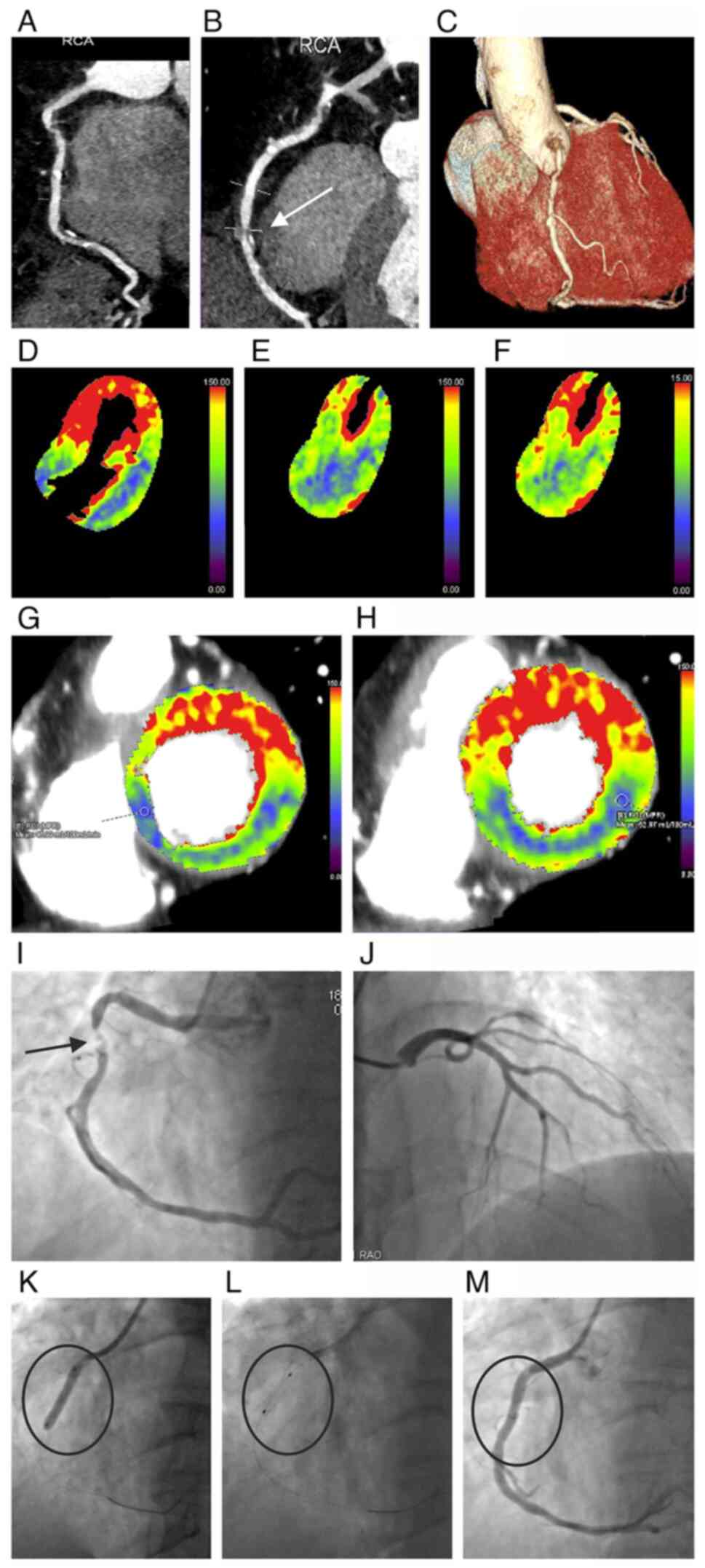
A reliable perfusion examination could be performed
in all patients (Fig. 2) Of note,
33 mild adverse effects were observed in patients treated with
adenosine (shortness of breath, chest discomfort, nausea,
palpitations, hypotension and bradycardia) and 12 in patients
treated with regadenoson (shortness of breath, chest discomfort,
palpitations and bradycardia) (Table
II). No severe adverse effects were observed. In 13 patients
from adenosine group and 13 patients from regadenoson group,
moderate to severe regional myocardial perfusion disorders were
present, with MBF <75 ml/100 ml/min, of which three and eight
patients had confirmed myocardial-scar necrosis after MI,
respectively. Of note, no perfusion disorders or MBF values >75
ml/100 ml/min. were found in two and 18 patients from adenosine and
regadenoson group, respectively.
 | Table IIFrequency and severity of side effects
of studied agents. |
Table II
Frequency and severity of side effects
of studied agents.
| Symptom | Adenosine | Regadenoson | Severity |
|---|
| Shortness of
breath | 9 | 3 | Mild/Mild |
| Chest discomfort | 14 | 4 | Mild/Mild |
| Vertigo | 0 | 0 | |
| Nausea | 2 | 0 | Mild |
| Palpitations | 6 | 4 | Mild/Mild |
| Headache | 0 | 0 | |
| Hypotension | 1 | 0 | Mild |
| Bradycardia | 1 | 1 | Mild/Mild |
| Hypertension | 0 | 0 | |
| AV block | 0 | 0 | |
| Cardiac arrest | 0 | 0 | |
Following CCTA, invasive coronary angiography was
performed in nine patients with stent implantation (Fig. 2). Of note, no patient was assessed
as false positive in the adenosine group whereas in two patients
from the regadenoson group the invasive coronarography was
performed and stents were not implanted.
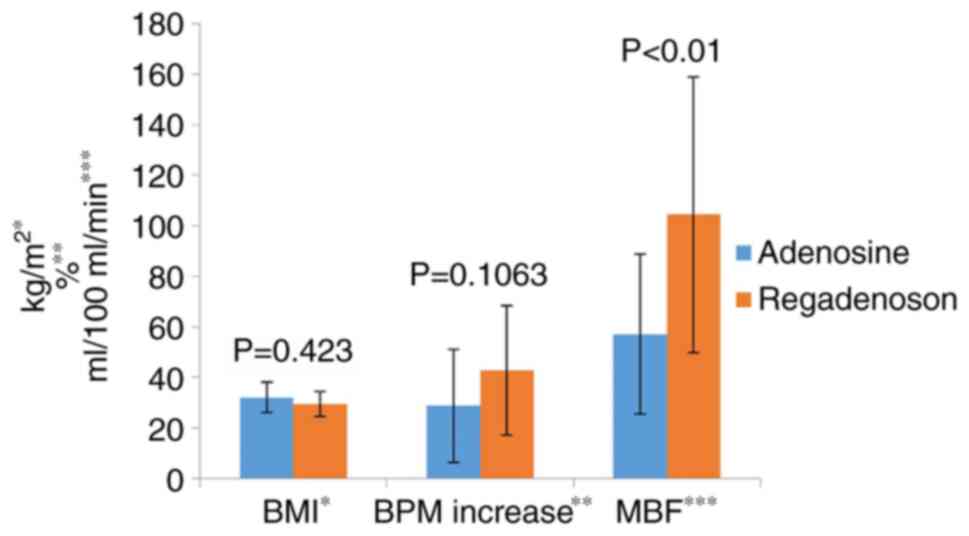
The two studied agents were able to significantly
increase the heart rate following infusion (Table III). Administration of adenosine
led to an increase from 71.53±24.5 to 83.71±18.48 BPM while
administration of regadenoson led to an increase from 62.42±11.91
to 93.83±32.1 BPM. Although regadenoson induced slightly higher BPM
increase (compared with adenosine) in studied group of patients,
the difference was not significant (P=0.1063; Fig. 3). On the other hand, the difference
in MBF increase between regadenoson (104.43±54.52) and adenosine
(57.08±31.67) was significant (P<0.01).
 | Table IIIPerfusion data, dynamic parameters
and indicated procedures following CT perfusion examination. |
Table III
Perfusion data, dynamic parameters
and indicated procedures following CT perfusion examination.
| MBF | Adenosine | Regadenoson |
|---|
|
ml/100
ml/min | 57.08±31.67 | 104.43±54.52 |
|
Calcium
Score | 1,323±1610 | 933±906 |
| Heart rate
(BPM) | | |
|
Baseline | 71.53±24.5 | 62.42±11.91 |
|
Stress | 83.71±18.48 | 93.83±32.1 |
|
Rest | 61.54±10.65 | 65.46±13.91 |
|
Base to
Stress increase (%) | 21.50±28.27 | 50.33±38.49 |
| Indicated
procedure | | |
|
PTCA without
stent | 0.00%
(F-0.00%/M-0.00%) | 6.45%
(F-11.11%/M-4.54%) |
|
PTCA with
stent | 26.66%
(F-0.00%/M-36.36%) | 29.03%
(F-44.44%/M-22.72%) |
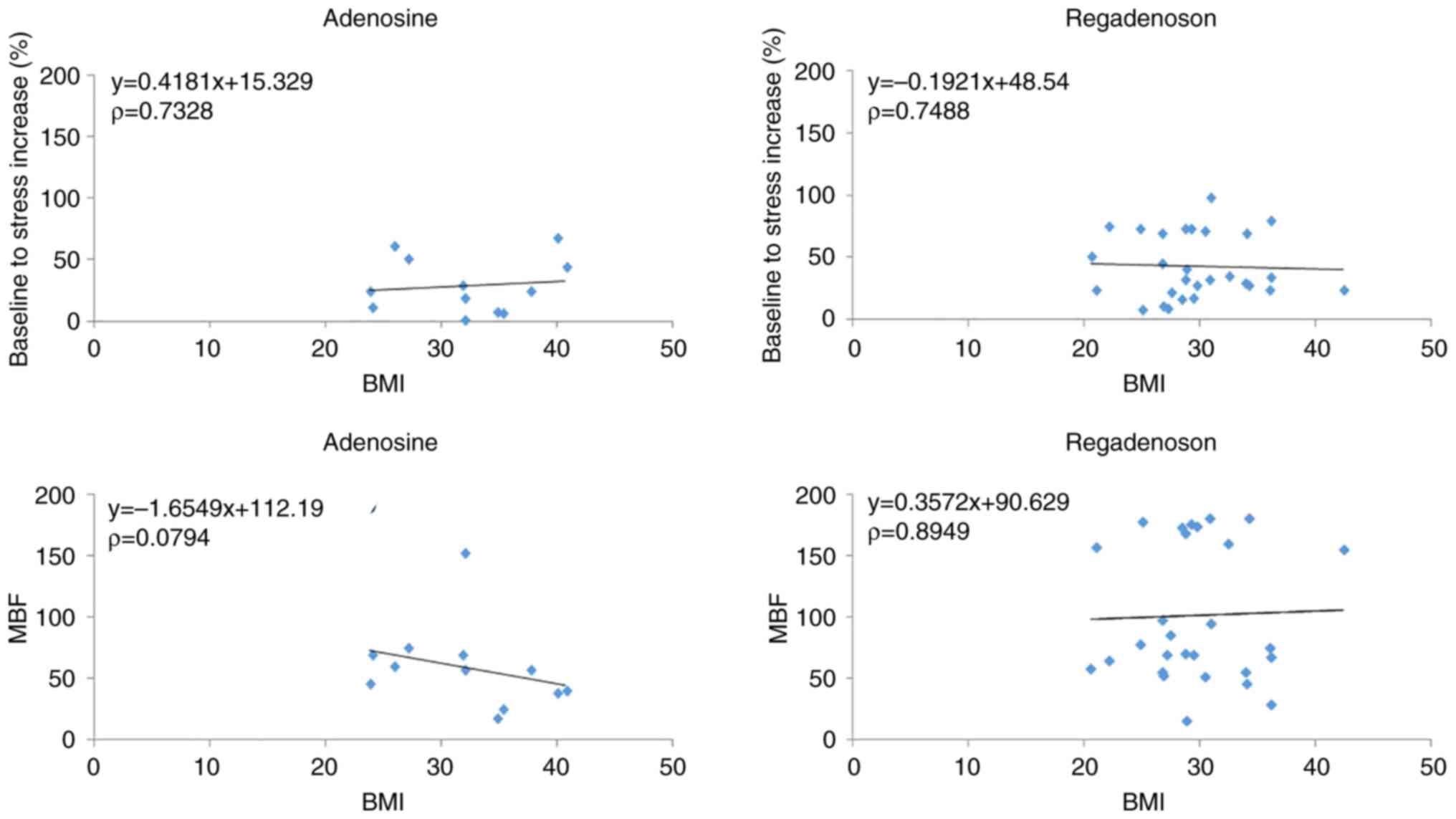
The analysis revealed no correlation (Fig. 4) between BPM increase (%) and BMI
of patients subjected to adenosine- or regadenoson-induced stress
CT-MPI.
Discussion
The analysis of clinical myocardial perfusion CT
examinations in the present study revealed that regadenoson is
comparable to adenosine in detecting myocardial perfusion defects.
Clinically important, the selective A2A receptor agonist
regadenoson elicited an increase in MBF comparable to adenosine
and/or dipyridamole (11) (of
note, adenosine and dipyridamole doses were adapted to patient
weight), while the flow response to regadenoson appeared to be
largely independent of patient size, despite being administered as
a bolus (fixed dose of 0.4 mg) (19). The equal bolus dose may
theoretically result to a bodyweight-dependent attenuation of the
effect. However, as shown previously (19) the present study also did not
observe a clinically relevant relationship between dose and BMI of
the patient. Published data confirms that the bolus of 0.4 mg
sufficiently saturates A2A receptors independent on the
BMI of the patient (19). Notably,
the MBF increase was significantly higher following regadenoson
compared with dipyridamole (11)
or adenosine (observed also in the present study) which may result
either from different application technique (bolus compared with
infusion) or by more efficient stimulation of the sympathetic
nervous system via the A2A receptor (20).
Previously it was demonstrated that regadenoson
increased blood flow >2.5-fold lasting 2-3 min, thus the effect
is brief and easily tolerated (21). The study also demonstrated that the
maximal coronary hyperemia induced by regadenoson appeared to be
similar in magnitude to that induced by adenosine or dipyridamole.
In another study, the MBF response to regadenoson was noninvasively
measured using 15O-water and PET in healthy subjects. Notably, the
work revealed a flow reserve of 2.97±0.16 that did not
significantly change following caffeine application (22). Similarly, 82Rb myocardial perfusion
PET examination revealed a flow response of 2.9 in the
regadenoson-treated group (11).
The flow response also appeared to be somewhat independent of the
patient's body size.
Moreover, studies have demonstrated a lower
incidence of side effects and patient's discomfort due to the
receptor subtype selectivity of the agent (11,23),
thus regadenoson can safely be administered as a fixed bolus
regardless of age, gender, BMI and diabetes (24). Although, individuals <65 years
of age and women had increased occurrence of side effects and
benefit from aminophylline (bronchodilatator theophylline and
ethylenediamine 2:1) administration (25). Hence, further important parameters
associated with side effects present with sex and age. Women
demonstrate a higher median BPM associated with a significantly
higher rate of side effects compared with men (26). Regarding the frequency of side
effects, the present study was consistent with previously published
work (21) where the presence of
adverse events like chest pain, tachycardia, and hypotension was
similar to those reported in the present study. Although occurrence
of first-degree atrioventricular block were already noted upon
regadenoson administration no significant heart rhythm disturbances
were observed. These observations provided a rationale for a wider
use of regadenoson, which is currently being explored; for example,
in patients with asthma and obstructive airway disease, thus with
dipyridamole and/or adenosine contraindication (27). However, a single-center
retrospective cohort study reveals that the use of adenosine was
associated with a lower occurrence of adverse effects and lower
rate of rescue agent use (28).
From this point of view, adenosine still presents a cost saving
opportunity in direct comparison with regadenoson.
Although the present study did not provide entirely
novel information, it should be seen as a further clinical evidence
for a more wider use of regadenoson over adenosine (in particular
due to a lower occurrence of adverse effects and administration
management). Nevertheless, it is necessary to consider three main
limitations of this single-center study. First, presented data are
summarized based on an observational retrospective analysis. The
present study only compared two groups of patients with myocardial
perfusion CT images who were administered either regadenoson or
adenosine. Based on the current retrospective analysis, it is also
impossible to control other potential interfering factors. From
this point of view, a more complex prospective randomized study
would be more appropriate albeit expensive and time-consuming.
Second, the blood flow response to adenosine and regadenoson should
be compared in healthy volunteers to exclude/reduce potentially
interfering factors. Finally, the limited number of patients
included in the present study was the third main limitation of the
investigation. Nevertheless, in is considered that the present data
reflect a realistic single-center clinical situation where the
agents will be routinely administered for myocardial perfusion
examination.
Acknowledgements
The authors would like to thank Professor Ladislav
Mirossay (Department of Pharmacology, Faculty of Medicine, P. J.
Šafárik University, Košice, Slovakia) for critically reading the
manuscript and for his useful comments.
Funding
Funding: No funding was received.
Availability of data and materials
The datasets used and/or analyzed during the current
study are available from the corresponding author on reasonable
request.
Authors' contributions
MS and PG designed the present study. CG, PM, MH and
RK performed the clinical part of the study. LU and PG analyzed
data. PG wrote the first draft of the manuscript. CG and LU confirm
the authenticity of all the raw data. All authors read and approved
the final manuscript.
Ethics approval and consent to
participate
The present study was approved by the Ethics
Committee of East-Slovak Institute of Cardiovascular Diseases, Inc.
(June 10 2022; approval no. A3062022).
Patient consent for publication
Not applicable.
Competing interests
The authors declare that they have no competing
interests.
References
|
1
|
Yang L, Zhou T, Zhang R, Xu L, Peng Z,
Ding J, Wang S, Li M and Sun G: Meta-analysis: Diagnostic accuracy
of coronary CT angiography with prospective ECG gating based on
step-and-shoot, Flash and volume modes for detection of coronary
artery disease. Eur Radiol. 24:2345–2352. 2014.PubMed/NCBI View Article : Google Scholar
|
|
2
|
American College of Cardiology Foundation
Task Force on Expert Consensus Documents. Mark DB, Berman DS,
Budoff MJ, Carr JJ, Gerber TC, Hecht HS, Hlatky MA, Hodgson JM,
Lauer MS, et al: ACCF/ACR/AHA/NASCI/SAIP/SCAI/SCCT 2010 expert
consensus document on coronary computed tomographic angiography: A
report of the American College of cardiology foundation task force
on expert consensus documents. Circulation. 121:2509–2543.
2010.PubMed/NCBI View Article : Google Scholar
|
|
3
|
Taylor AJ, Cerqueira M, Hodgson JM, Mark
D, Min J, O'Gara P and Rubin GD: American College of Cardiology
Foundation Appropriate Use Criteria Task Force; Society of
Cardiovascular Computed Tomography; American College of Radiology
et al. ACCF/SCCT/ACR/AHA/ASE/ASNC/NASCI/SCAI/SCMR 2010
appropriate use criteria for cardiac computed tomography. a report
of the American College of cardiology foundation appropriate use
criteria task force, the society of cardiovascular computed
tomography, the American college of radiology, the American heart
association, the American society of echocardiography, the American
Society of nuclear cardiology, the North American Society for
cardiovascular imaging, the society for cardiovascular angiography
and interventions, and the society for cardiovascular magnetic
resonance. Circulation. 122:e525–e555. 2010.PubMed/NCBI View Article : Google Scholar
|
|
4
|
Bamberg F, Becker A, Schwarz F, Marcus RP,
Greif M, von Ziegler F, Blankstein R, Hoffmann U, Sommer WH,
Hoffmann VS, et al: Detection of hemodynamically significant
coronary artery stenosis: Incremental diagnostic value of dynamic
CT-based myocardial perfusion imaging. Radiology. 260:689–698.
2011.PubMed/NCBI View Article : Google Scholar
|
|
5
|
Botvinick EH: Current methods of
pharmacologic stress testing and the potential advantages of new
agents. J Nucl Med Technol. 37:14–25. 2009.PubMed/NCBI View Article : Google Scholar
|
|
6
|
Lette J, Tatum JL, Fraser S, Miller DD,
Waters DD, Heller G, Stanton EB, Bom HS, Leppo J and Nattel S:
Safety of dipyridamole testing in 73,806 patients- the multicenter
dipyridamole safety study. J Nucl Cardiol. 2:3–17. 1995.PubMed/NCBI View Article : Google Scholar
|
|
7
|
Cerqueira MD, Verani MS, Schwaiger M, Heo
J and Iskandrian AS: Safety profile of adenosine stress perfusion
imaging-Results from the adenoscan-multicenter-trial-registry. J Am
Coll Cardiol. 23:384–389. 1994.PubMed/NCBI View Article : Google Scholar
|
|
8
|
Cerqueira MD: The future of pharmacologic
stress: Selective A2A adenosine receptor agonists. Am J Cardiol.
94:33D–42D. 2004.PubMed/NCBI View Article : Google Scholar
|
|
9
|
Hasko G, Linden J, Cronstein B and Pacher
P: Adenosine receptors: Therapeutic aspects for inflammatory and
immune diseases. Nat Rev Drug Discov. 7:759–770. 2008.PubMed/NCBI View
Article : Google Scholar
|
|
10
|
Iskandrian AE, Bateman TM, Belardinelli L,
Blackburn B, Cerqueira MD, Hendel RC, Lieu H, Mahmarian JJ, Olmsted
A, Underwood SR, et al: Adenosine versus regadenoson comparative
evaluation in myocardial perfusion imaging: Results of the ADVANCE
phase 3 multicenter international trial. J Nucl Cardiol.
14:645–658. 2007.PubMed/NCBI View Article : Google Scholar
|
|
11
|
Goudarzi B, Fukushima K, Bravo P, Merrill
J and Bengel FM: Comparison of the myocardial blood flow response
to regadenoson and dipyridamole: A quantitative analysis in
patients referred for clinical 82Rb myocardial perfusion PET. Eur J
Nucl Med Mol Imaging. 38:1908–1916. 2011.PubMed/NCBI View Article : Google Scholar
|
|
12
|
Andrikopoulou E and Hage FG: Adverse
effects associated with regadenoson myocardial perfusion imaging. J
Nucl Cardiol. 25:1724–1731. 2018.PubMed/NCBI View Article : Google Scholar
|
|
13
|
Al Jaroudi W and Iskandrian AE:
Regadenoson: A new myocardial stress agent. J Am Coll Cardiol.
54:1123–1130. 2009.PubMed/NCBI View Article : Google Scholar
|
|
14
|
Johnson SG and Peters S: Advances in
pharmacologic stress agents: Focus on regadenoson. J Nucl Med
Technol. 38:163–171. 2010.PubMed/NCBI View Article : Google Scholar
|
|
15
|
Nous FMA, Geisler T, Kruk MBP, Alkadhi H,
Kitagawa K, Vliegenthart R, Hell MM, Hausleiter J, Nguyen PK, Budde
RPJ, et al: Dynamic myocardial perfusion CT for the detection of
hemodynamically significant coronary artery disease. JACC
Cardiovasc Imaging. 15:75–87. 2022.PubMed/NCBI View Article : Google Scholar
|
|
16
|
Bastarrika G, Ramos-Duran L, Rosenblum MA,
Kang DK, Rowe GW and Schoepf UJ: Adenosine-stress dynamic
myocardial CT perfusion imaging: Initial clinical experience.
Invest Radiol. 45:306–313. 2010.PubMed/NCBI View Article : Google Scholar
|
|
17
|
Cury RC, Abbara S, Achenbach S, Agatston
A, Berman DS, Budoff MJ, Dill KE, Jacobs JE, Maroules CD, Rubin GD,
et al: CAD-RADS: Coronary artery disease-reporting and data system:
An expert consensus document of the society of cardiovascular
computed tomography (SCCT), the American college of radiology (ACR)
and the North American society for cardiovascular imaging (NASCI).
Endorsed by the American College of Cardiology. J Am Coll Radiol.
13:1458–1466 e9. 2016.PubMed/NCBI View Article : Google Scholar
|
|
18
|
Rossi A, Wragg A, Klotz E, Pirro F, Moon
JC, Nieman K and Pugliese F: Dynamic computed tomography myocardial
perfusion imaging: Comparison of clinical analysis methods for the
detection of vessel-specific ischemia. Circ-Cardiovasc Imag.
10(e005505)2017.PubMed/NCBI View Article : Google Scholar
|
|
19
|
Reyes E, Staehr P, Olmsted A, Zeng D,
Blackburn B, Cerqueira MD and Underwood SR: Effect of body mass
index on the efficacy, side effect profile, and plasma
concentration of fixed-dose regadenoson for myocardial perfusion
imaging. J Nucl Cardiol. 18:620–627. 2011.PubMed/NCBI View Article : Google Scholar
|
|
20
|
Dhalla AK, Wong MY, Wang WQ, Biaggioni I
and Belardinelli L: Tachycardia caused by A2A adenosine receptor
agonists is mediated by direct sympathoexcitation in awake rats. J
Pharmacol Exp Ther. 316:695–702. 2006.PubMed/NCBI View Article : Google Scholar
|
|
21
|
Lieu HD, Shryock JC, von Mering GO, Gordi
T, Blackburn B, Olmsted AW, Belardinelli L and Kerensky RA:
Regadenoson, a selective A2A adenosine receptor agonist, causes
dose-dependent increases in coronary blood flow velocity in humans.
J Nucl Cardiol. 14:514–520. 2007.PubMed/NCBI View Article : Google Scholar
|
|
22
|
Namdar M, Koepfli P, Grathwohl R, Siegrist
PT, Klainguti M, Schepis T, Delaloye R, Wyss CA, Fleischmann SP,
Gaemperli O and Kaufmann PA: Caffeine decreases exercise-induced
myocardial flow reserve. J Am Coll Cardiol. 47:405–410.
2006.PubMed/NCBI View Article : Google Scholar
|
|
23
|
Rai M, Ahlberg AW, Marwell J, Chaudhary W,
Savino JA III, Alter EL, Henzlova MJ and Duvall WL: Safety of
vasodilator stress myocardial perfusion imaging in patients with
elevated cardiac biomarkers. J Nucl Cardiol. 24:724–734.
2017.PubMed/NCBI View Article : Google Scholar
|
|
24
|
Cerqueira MD, Nguyen P, Staehr P,
Underwood SR and Iskandrian AE: ADVANCE-MPI Trial Investigators.
Effects of age, gender, obesity, and diabetes on the efficacy and
safety of the selective A2A agonist regadenoson versus adenosine in
myocardial perfusion imaging integrated ADVANCE-MPI trial results.
JACC Cardiovasc Imaging. 1:307–316. 2008.PubMed/NCBI View Article : Google Scholar
|
|
25
|
Rangel MO, Demori RM and Doukky R: Age and
gender as predictors of benefit from aminophylline administration
in patients undergoing regadenoson stress myocardial perfusion
imaging: A substudy of the ASSUAGE trial. Am J Ther. 20:622–629.
2013.PubMed/NCBI View Article : Google Scholar
|
|
26
|
Katsikis A, Kyrozi E, Manira V,
Theodorakos A, Malamitsi J, Tsapaki V, Iakovou I, Voudris V,
Kolovou G and Koutelou M: Gender-related differences in
side-effects and hemodynamic response to regadenoson in patients
undergoing SPECT myocardial perfusion imaging. Eur J Nucl Med Mol
Imaging. 46:2590–2600. 2019.PubMed/NCBI View Article : Google Scholar
|
|
27
|
Golzar Y and Doukky R: Regadenoson use in
patients with chronic obstructive pulmonary disease: The state of
current knowledge. Int J Chronic Obstruct Pulmon Dis. 9:129–137.
2014.PubMed/NCBI View Article : Google Scholar
|
|
28
|
Brink HL, Dickerson JA, Stephens JA and
Pickworth KK: Comparison of the safety of adenosine and regadenoson
in patients undergoing outpatient cardiac stress testing.
Pharmacotherapy. 35:1117–1123. 2015.PubMed/NCBI View Article : Google Scholar
|