|
1
|
Satirapoj B and Adler SG: Prevalence and
management of diabetic nephropathy in western countries. Kidney Dis
(Basel). 1:61–70. 2015.PubMed/NCBI View Article : Google Scholar
|
|
2
|
Zhang L, Long J, Jiang W, Shi Y, He X,
Zhou Z, Li Y, Yeung RO, Wang J, Matsushita K, et al: Trends in
chronic kidney disease in China. N Engl J Med. 375:905–906.
2016.PubMed/NCBI View Article : Google Scholar
|
|
3
|
Cho NH, Shaw JE, Karuranga S, Huang Y, da
Rocha Fernandes JD, Ohlrogge AW and Malanda B: IDF diabetes atlas:
Global estimates of diabetes prevalence for 2017 and projections
for 2045. Diabetes Res Clin Pract. 138:271–281. 2018.PubMed/NCBI View Article : Google Scholar
|
|
4
|
Luk AOY, Hui EMT, Sin MC, Yeung CY, Chow
WS, Ho AYY, Hung HF, Kan E, Ng CM, So WY, et al: Declining trends
of cardiovascular-renal complications and mortality in type 2
diabetes: The Hong Kong diabetes database. Diabetes Care.
40:928–935. 2017.PubMed/NCBI View Article : Google Scholar
|
|
5
|
Schmidt MI, Duncan BB, Sharrett AR,
Lindberg G, Savage PJ, Offenbacher S, Azambuja MI, Tracy RP and
Heiss G: Markers of inflammation and prediction of diabetes
mellitus in adults (Atherosclerosis Risk in Communities study): A
cohort study. Lancet. 353:1649–1652. 1999.PubMed/NCBI View Article : Google Scholar
|
|
6
|
Rayego-Mateos S, Morgado-Pascual JL,
Opazo-Ríos L, Guerrero-Hue M, García-Caballero C, Vázquez-Carballo
C, Mas S, Sanz AB, Herencia C, Mezzano S, et al: Pathogenic
pathways and therapeutic approaches targeting inflammation in
diabetic nephropathy. Int J Mol Sci. 21(3798)2020.PubMed/NCBI View Article : Google Scholar
|
|
7
|
Gamboa JL, Pretorius M, Todd-Tzanetos DR,
Luther JM, Yu C, Ikizler TA and Brown NJ: Comparative effects of
angiotensin-converting enzyme inhibition and angiotensin-receptor
blockade on inflammation during hemodialysis. J Am Soc Nephrol.
23:334–342. 2012.PubMed/NCBI View Article : Google Scholar
|
|
8
|
Perkovic V, Jardine MJ, Neal B, Bompoint
S, Heerspink HJL, Charytan DM, Edwards R, Agarwal R, Bakris G, Bull
S, et al: Canagliflozin and renal outcomes in type 2 diabetes and
nephropathy. N Engl J Med. 380:2295–2306. 2019.PubMed/NCBI View Article : Google Scholar
|
|
9
|
Lupsa BC and Inzucchi SE: Use of SGLT2
inhibitors in type 2 diabetes: Weighing the risks and benefits.
Diabetologia. 61:2118–2125. 2018.PubMed/NCBI View Article : Google Scholar
|
|
10
|
GBD Chronic Kidney Disease Collaboration.
Global, regional, and national burden of chronic kidney disease,
1990-2017: A systematic analysis for the global burden of disease
study 2017. Lancet. 395:709–733. 2020.PubMed/NCBI View Article : Google Scholar
|
|
11
|
Zhao JX, Deng DQ and Li Q: Identification
of Chinese medicine diseases related to diabetic nephropathy. J
Nanjing Univ Traditional Chin Med. 288-289:2005.
|
|
12
|
Huang YR, Wei QX, Wan YG, Sun W, Mao ZM,
Chen HL, Meng XJ, Shi XM, Tu Y and Zhu Q: Ureic clearance granule,
alleviates renal dysfunction and tubulointerstitial fibrosis by
promoting extracellular matrix degradation in renal failure rats,
compared with enalapril. J Ethnopharmacol. 155:1541–1552.
2014.PubMed/NCBI View Article : Google Scholar
|
|
13
|
Disease SPGoTCAGotCMftToC: The clinical
application guide of chinese patent medicine in the treatment of
chronic kidney disease stage 3-5 (Non Dialysis) (2020 Version).
Chin J Integrated Traditional and Western Medicine. 41:261–272.
2021.
|
|
14
|
Zheng Y, Cai GY, He LQ, Lin HL, Cheng XH,
Wang NS, Jian GH, Liu XS, Liu YN, Ni ZH, et al: Efficacy and safety
of niaoduqing particles for delaying moderate-to-severe renal
dysfunction: A randomized, double-blind, placebo-controlled,
multicenter clinical study. Chin Med J (Engl). 130:2402–2409.
2017.PubMed/NCBI View Article : Google Scholar
|
|
15
|
Wang YX, Yu GQ, Su XY, Chen J and Zhuang
YZ: The ameliorating effect of uremic clearance granule played on
micro-inflammatory state for patients in early and mild stage of
chronic renal insufficiency. Chin J Int Trad Western Nephrol.
17:1050–1052. 2016.
|
|
16
|
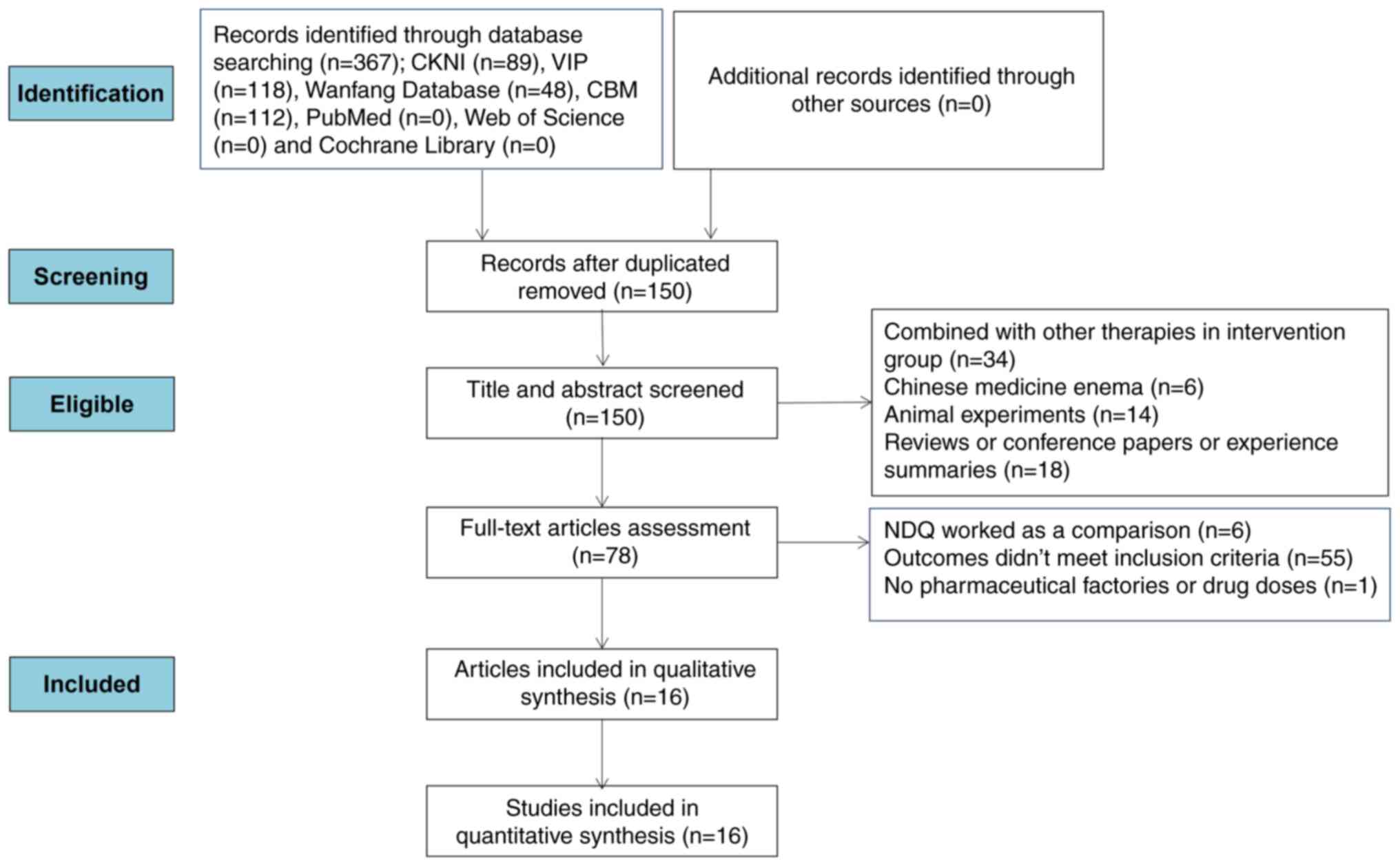
Moher D, Liberati A, Tetzlaff J and Altman
DG: Preferred reporting items for systematic reviews and
meta-analyses: The PRISMA statement. BMJ. 339(b2535)2009.PubMed/NCBI View Article : Google Scholar
|
|
17
|
The MCGoCDA: Expert consensus of
prevention and treatment of diabetic kidney disease (2014 version).
Chin J Diab Mellitus. 6:792–801. 2014.
|
|
18
|
The MCGoCDA: Chinese clinical practice
guideline of diabetic kidney disease. Chin J Diab Mellitus.
11:15–28. 2019.
|
|
19
|
Tong GY and Zhu DL: Interpretation of
clinical practice guidelines and expert consensuses for the
evaluation and management of diabetic kidney disease at home and
abroad. Chin J Pract Int Med. 37:211–216. 2017.
|
|
20
|
Mogensen CE, Schmitz A and Christensen CK:
Comparative renal pathophysiology relevant to IDDM and NIDDM
patients. Diabetes Metab Rev. 4:453–483. 1988.PubMed/NCBI View Article : Google Scholar
|
|
21
|
Deyno S, Eneyew K, Seyfe S, Tuyiringire N,
Peter EL, Muluye RA, Tolo CU and Ogwang PE: Efficacy and safety of
cinnamon in type 2 diabetes mellitus and pre-diabetes patients: A
meta-analysis and meta-regression. Diabetes Res Clin Pract.
156(107815)2019.PubMed/NCBI View Article : Google Scholar
|
|
22
|
Liang Y: Clinical effIcacy of compound
alpha ketoacid combined with Niaoduqing granules in treatment of
patients with stage IV diabetic kidney disease. Med Diet Health.
19:66–67. 2021.
|
|
23
|
Zhang HY, Zhang HX, Xiao Y and Feng XZ:
Effects of Niaoduqing granules on renal function and serum hs-CRP
levels in DN patients with chronic renal insufficiency. Shand Med
J. 51:77–78. 2011.
|
|
24
|
Zhang C, Wang ML, Ma H, Xia XB and Ma J:
The effects of Niaoduqing granules on micro-inflammatory state and
vascular endothelial growth factor in aged patients with diabetic
nephropathy. Chin J Diff Compl Cases. 13:697–699, 703. 2014.
|
|
25
|
He YM and Ding XQ: Clinical research of
Niaoduqing granules on inflammation factors in patients with early
and middle diabetic nephropathy. Pharmacol Clin Chin Mat Med.
31:160–162. 2015.
|
|
26
|
He YH: Effect of niaoduqing granules
combined with valsartan on kidney function, inflammatory factors
and immune function in patients with early diabetic nephropathy.
New Chin Med. 53:60–63. 2021.
|
|
27
|
Yang SX and Chen BP: Changes of Niaoduqing
granules on IL-6 levels in treatment of early renal failure of type
2 diabetic nephropathy. Chi Comm Doct. 12(161)2010.
|
|
28
|
Wu P: Effects of Niaoduqing granules
combined with Valsartan on kidney function in patients of early
diabetic nephropathy. Chron Pathematol J. 22:474–475+478. 2021.
|
|
29
|
Li XY: Changes of renal function and serum
hs-CRP levels in diabetes patients with chronic renal insufficiency
before and after taking Niaoduqing particle. Chin J Pract Med.
42:41–42. 2015.
|
|
30
|
Liu B and Yang SL: Effect of niaoduqing
combined with insulin detemir on inflammation, oxidative stress and
curative effect in patients with diabetic nephropathy. Diab New
World. 23:13–17. 2020.
|
|
31
|
Li Q, Cao M, Li K and Li J: Observation on
the effect of niaoduqing granules combined with irbesartan in the
treatment of early diabetic nephropathy. Med Innov China. 18:16–20.
2021.
|
|
32
|
Chen X, Luo HY, Gao J and Qi C: Clinical
efficacy of insulin degludec and insulin aspart combined with
Niaoduqing in treatment of patients with early diabetic
nephropathy. Chin J Integrated Trad West Med Int Crit Care.
28:404–408. 2021.
|
|
33
|
Zheng N, An Z and Liu HG: Effects of
combination of Niaoduqing granules and artificial kidney on blood
lipid metabolism inflammatory response and cellular immune function
in patients with diabetic nephropathy undergoing maintenance
hemodialysis. Mod J Int Trad Chin West Med. 28:2208–2211. 2019.
|
|
34
|
Wang B: Effect of Atorvastatin and
Niaoduqing in diabetic nephropathy patients with maintenance
hemodialysis and influence of micro inflammatory. J Med Forum.
38:34–35+38. 2017.
|
|
35
|
Gong LN: Clinical efficacy of compound
Niaoduqing particles and irbesartan in patients with stage Ⅳ
diabetic nephropathy. J Front Med. 115–116. 2013.
|
|
36
|
Tong CC, Chen HC, Cong ZY, Wang W, Li Q,
Zhao XJ and Zheng Y: Effects of Dapagliflozin combined with
Niaoduqing granules in the treatment of diabetic nephropathy.
Modern Journal of Integrated Traditional Chinese and Western
Medicine. 31:3310–3314. 2022.
|
|
37
|
Yu H, Liang CD, Hu XH and Yu Y: Effects of
Niaoduqing granules on oxidative/antioxidant balance and serum
LncRNA KCNQ1OT1 and LncRNA Malat1 in the adjuvant treatment of
early diabetic nephropathy. Lab Med Clin. 19:3334–3338. 2022.
|
|
38
|
Ciani O, Manyara A and Taylor RS: Need for
better reporting of trials with surrogate endpoints:
SPIRIT|CONSORT-SURROGATE extensions. J Epidemiol Community Health.
76:769–770. 2022.PubMed/NCBI View Article : Google Scholar
|
|
39
|
Pepys MB and Hirschfield GM: C-reactive
protein: A critical update. J Clin Invest. 111:1805–1812.
2003.PubMed/NCBI View Article : Google Scholar
|
|
40
|
Sinha SK, Nicholas SB, Sung JH, Correa A,
Rajavashisth TB, Norris KC and Lee JE: hs-CRP is associated with
incident diabetic nephropathy: Findings from the Jackson heart
study. Diabetes Care. 42:2083–2089. 2019.PubMed/NCBI View Article : Google Scholar
|
|
41
|
Balamir I, Ates I, Topcuoglu C and Turhan
T: Association of endocan, ischemia-modified albumin, and hsCRP
levels with endothelial dysfunction in type 2 diabetes mellitus.
Angiology. 69:609–616. 2018.PubMed/NCBI View Article : Google Scholar
|
|
42
|
Zhang L, Shen ZY, Wang K, Li W, Shi JM,
Osoro EK, Ullah N, Zhou Y and Ji SR: C-reactive protein exacerbates
epithelial-mesenchymal transition through Wnt/β-catenin and ERK
signaling in streptozocin-induced diabetic nephropathy. FASEB J.
33:6551–6563. 2019.
|
|
43
|
Navarro JF and Mora-Fernández C: The role
of TNF-alpha in diabetic nephropathy: Pathogenic and therapeutic
implications. Cytokine Growth Factor Rev. 17:441–450.
2006.PubMed/NCBI View Article : Google Scholar
|
|
44
|
Niewczas MA, Gohda T, Skupien J, Smiles
AM, Walker WH, Rosetti F, Cullere X, Eckfeldt JH, Doria A, Mayadas
TN, et al: Circulating TNF receptors 1 and 2 predict ESRD in type 2
diabetes. J Am Soc Nephrol. 23:507–515. 2012.PubMed/NCBI View Article : Google Scholar
|
|
45
|
Lee BT, Ahmed FA, Hamm LL, Teran FJ, Chen
CS, Liu Y, Shah K, Rifai N, Batuman V, Simon EE, et al: Association
of C-reactive protein, tumor necrosis factor-alpha, and
interleukin-6 with chronic kidney disease. BMC Nephrol.
16(77)2015.PubMed/NCBI View Article : Google Scholar
|
|
46
|
Fathy SA, Mohamed MR, Ali M, El-Helaly AE
and Alattar AT: Influence of IL-6, IL-10, IFN-γ and TNF-α genetic
variants on susceptibility to diabetic kidney disease in type 2
diabetes mellitus patients. Biomarkers. 24:43–55. 2019.PubMed/NCBI View Article : Google Scholar
|
|
47
|
Kalantarinia K, Awad AS and Siragy HM:
Urinary and renal interstitial concentrations of TNF-alpha increase
prior to the rise in albuminuria in diabetic rats. Kidney Int.
64:1208–1213. 2003.PubMed/NCBI View Article : Google Scholar
|
|
48
|
Shikano M, Sobajima H, Yoshikawa H, Toba
T, Kushimoto H, Katsumata H, Tomita M and Kawashima S: Usefulness
of a highly sensitive urinary and serum IL-6 assay in patients with
diabetic nephropathy. Nephron. 85:81–85. 2000.PubMed/NCBI View Article : Google Scholar
|
|
49
|
Chang WT, Huang MC, Chung HF, Chiu YF,
Chen PS, Chen FP, Lee CY, Shin SJ, Hwang SJ, Huang YF and Hsu CC:
Interleukin-6 gene polymorphisms correlate with the progression of
nephropathy in Chinese patients with type 2 diabetes: A prospective
cohort study. Diabetes Res Clin Pract. 120:15–23. 2016.PubMed/NCBI View Article : Google Scholar
|
|
50
|
Nakazato Y, Kurane R, Hirose S, Watanabe A
and Shimoyama H: Variability of laboratory parameters is associated
with frailty markers and predicts non-cardiac mortality in
hemodialysis patients. Clin Exp Nephrol. 19:1165–1178.
2015.PubMed/NCBI View Article : Google Scholar
|
|
51
|
Association TMCGoCD: Chinese clinical
practice guideline of diabetic kidney disease. Chin J Diab.
11:2019.
|
|
52
|
Tang S and Yiu WH: Innate immunity in
diabetic kidney disease. Nat Rev Nephrol. 16:206–222.
2020.PubMed/NCBI View Article : Google Scholar
|
|
53
|
Kaysen GA: The microinflammatory state in
uremia: Causes and potential consequences. J Am Soc Nephrol.
12:1549–1557. 2001.PubMed/NCBI View Article : Google Scholar
|
|
54
|
Lytvyn Y, Bjornstad P, van Raalte DH,
Heerspink HL and Cherney DZ: The new biology of diabetic kidney
disease-mechanisms and therapeutic implications. Endocr Rev.
41:202–231. 2020.PubMed/NCBI View Article : Google Scholar
|
|
55
|
Niewczas MA, Pavkov ME, Skupien J, Smiles
A, Md Dom ZI, Wilson JM, Park J, Nair V, Schlafly A, Saulnier PJ,
et al: A signature of circulating inflammatory proteins and
development of end-stage renal disease in diabetes. Nat Med.
25:805–813. 2019.PubMed/NCBI View Article : Google Scholar
|
|
56
|
Donate-Correa J, Ferri CM,
Sánchez-Quintana F, Pérez-Castro A, González-Luis A, Martín-Núñez
E, Mora-Fernández C and Navarro-González JF: Inflammatory cytokines
in diabetic kidney disease: Pathophysiologic and therapeutic
implications. Front Med (Lausanne). 7(628289)2020.PubMed/NCBI View Article : Google Scholar
|
|
57
|
Rayego-Mateos S, Rodrigues-Diez RR,
Fernandez-Fernandez B, Mora-Fernández C, Marchant V, Donate-Correa
J, Navarro-González JF, Ortiz A and Ruiz-Ortega M: Targeting
inflammation to treat diabetic kidney disease: the road to 2030.
Kidney Int. 103:282–296. 2023.PubMed/NCBI View Article : Google Scholar
|
|
58
|
Tan F, Sheng YH and He Y: Effect of uremic
granule on renal anti-inflammatory and antioxidant protection of
diabetic nephropathy rats and on TGF-β1/p38MAPK signaling pathway.
Trad Chin Drug Res Clin Pharmacol. 30:117–122. 2019.
|
|
59
|
Fu B, Shang Z, Song S, Xu Y, Wei L, Li G
and Yang H: Adverse reactions of Niaoduqing granules: A systematic
review and meta-analysis. Phytomedicine. 109(154535)2023.PubMed/NCBI View Article : Google Scholar
|
|
60
|
Zhang J, Li J, Zhang HL, Qu HS, Zhang XZ,
Cheng YQ, Zhang ZM and Huang JQ: Meta-analysis of niaoduqing
granules combined with ACEI/ARB in the treatment of diabetic
nephropathy. World Chin Med. 16:274–283. 2021.
|
|
61
|
Luan W, Yin H and Gu J: Systematic review
on assisted treatment for diabetic nephropathy with niaoduqing
granule. J Liaoning Univ Trad Chin Med. 17:131–135. 2015.
|
|
62
|
Patrick D: Reporting of patient-reported
outcomes in randomized trials: The CONSORT PRO extension. Value
Health. 16:455–456. 2013.PubMed/NCBI View Article : Google Scholar
|