Introduction
The aberrant activation of the phosphatidylinositol
3-kinase (PI3K) signaling pathway is an essential component of
cellular processes that are critical for malignant tumor
development, such as growth, proliferation and invasion (1,2).
The small molecule inhibitors, including PI3K itself and associated
pathway proteins, have been investigated as potential targets for
new anticancer drugs (3).
Puquitinib mesylate (XC-302) is a novel multiple-target agent that
has been developed independently by Xinchang Pharmacy Corp.
(Zhejiang Medicine Co., Ltd., Zhejiang, China). The ability to
immediately suppress the activity of PI3K (subtype IA,
IC50 against PI3K isoforms: p110α=766.6 nM, p110β=699.4
nM, p110δ=2.8 nM and p110γ=89.7 nM) in vitro has been
reported in a preclinical study. It also can apparently inhibit the
protein kinase B (AKT) phosphorylation mediated by epidermal growth
factor receptor, the activity of receptor tyrosine kinase (kinase
insert domain receptor and platelet-derived growth factor receptor
β) and the formation of the vascular endothelial cells in the
lumen. Preliminary studies have reported that XC-302 has clear
antitumor efficacy in xenograft nude mice and in vitro,
including cells of colon cancer, lung cancer and lymphoma (all with
the IC50 in a range of 0.5–2.0 µM). In addition,
XC-302 shows low toxicity in toxicological experiments. It is also
rapid to absorb and has a high-level absolute bioavailability,
which have been indicated by the preclinical pharmacokinetics
tests. The phase I clinical trials also exhibit notable safety,
tolerability and efficiency of XC-302 in advanced solid tumors and
hematological malignancies (data are unpublished information from
Xinchang Pharmacy Corp.).
Epidemiology studies show that nasopharyngeal
carcinoma (NPC) is a type of familiar head and neck cancer in
Southern China and Southeast Asia (4). Currently, irradiation alone or
chemotherapy combined with radiotherapy is the major treatment on
the basis of the disease stage (5). Due to the marked breakthroughs in
diagnosis and treatment (such as intensity-modulated radiation
therapy), the majority of early-stage patients could be cured
(6). Even in patients with
locally advanced stage disease, the 5-year local control rate is
more than 90% (7). However, there
remain a portion of locally advanced and numerous metastasis NPC
patients who fail to achieve long-term disease control and succumb
from the disease when it begins to progress out of control. One of
the reasons for the poor prognosis may be treatment resistant
(8). Therefore, evolving novel
antitumor drugs research and development is a notable prospect for
oncotherapy. Preclinical studies demonstrated that the
PI3K/mechanistic target of rapamycin (mTOR) signaling pathway is
commonly activated in numerous cancers and inhibition of this
pathway could increase radiosensitivity, including NPC (9,10),
suggesting that the PI3K/mTOR pathway may be a promising target in
NPC (11). A previous study has
shown that BEZ235, a dual PI3K/mTOR inhibitor, has a therapeutic
potential and can reverse resistance to cisplatin in NPC (10). Another study reported that
GSK2126458 and PKI-587, which are also dual PI3K/mTOR inhibitors,
suppress tumor progression and increase radiosensitivity in NPC
(9).
The feasibility of medicines in anticancer
treatments is assessed by their capacity to induce cell death
(12). Three major modalities of
cell death have been defined, including apoptosis (type I),
autophagy (type II), which has been regarded as 'programmed cell
death', and necrosis (type III), which has been considered as
accidental and unregulated (13).
There are limited studies that have observed that autophagy can be
induced by drugs in NPC, including drugs targeted for the
PI3K/AKT/mTOR pathway (14,15). As a consequence, XC-302 may not
exhibit an antitumor effect by inducing autophagy in NPC cells. In
addition, we hypothesize that the present study could provide an
initial basis of XC-302 for subsequent clinical application.
Materials and methods
Cell cultures and reagents
The human NPC cell line, CNE-2 (poorly
differentiated), was supplied from State Key Laboratory of Oncology
(Sun Yat-sen University Cancer Center, Guangzhou, China). The cell
lines were maintained in RPMI-1640 with 10% fetal bovine serum
(FBS). Cells in the logarithmic phase were used in the experiments.
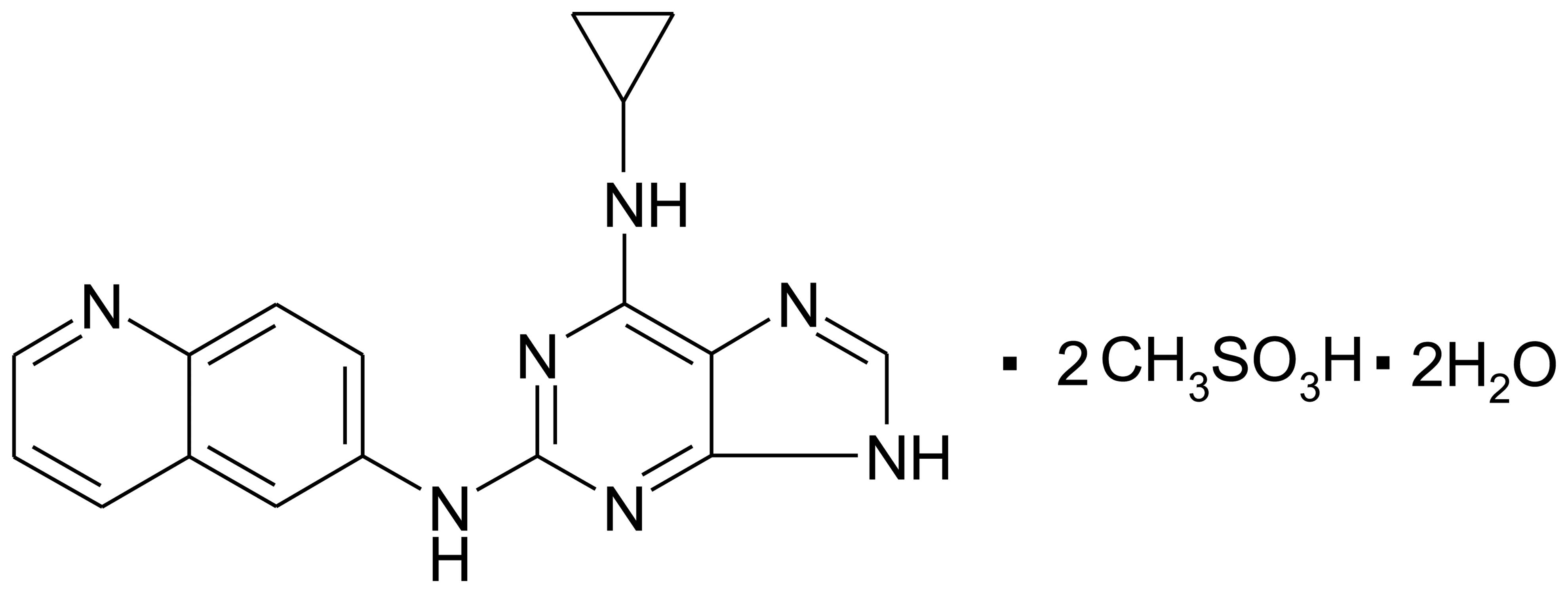
The puquitinib mesylate (XC-302; chemical structure shown in
Fig. 1) was obtained from
Xinchang Pharmacy Corp. and dissolved in dimethyl sulfoxide (DMSO;
Sigma-Aldrich, St. Louis, MO, USA) at a storage concentration of 40
mM.
Cell proliferation assay
In brief, tumor cells (3×103/100
µl/well) were plated in 96-well plates and incubated for 24
h. Culture medium containing gradient concentrations of XC-302
(16–0.125 µM) were added to each well, and 0.1% DMSO was set
as the negative control. MTT (5.0 mg/l; 20 µl) was added
after the cells were incubated for 68 h, followed by the addition
of 150 µl DMSO into each well to dissolve the dark blue
crystals. The absorbance (A) was measured at wavelengths of 570 and
630 nm, respectively (Model-550; Bio-Rad, Hercules, CA, USA).
Finally, the cell viability value was calculated using the
following formula: (Asample -
Ablank)/(Acontrol - Ablank) ×
100%. All the experiments were executed independently at least
three times in triplicate.
Monodansylcadaverine (MDC) staining
The MDC assay was used to label preliminary
autophagosomes (16). Cells grown
on 6-well plates were treated with XC-302 (0.5–8 µM) for 24
h, incubated with 0.05 mM MDC for 30 min at 37°C and washed with
phosphate-buffered saline (PBS). Fluorescence images were captured
by an Olympus IX71 fluorescence microscope (Olympus, Center Valley,
PA, USA).
Transmission electron microscopy
(TEM)
The presence of autophagosomes in TEM is the
standard for detecting autophagy. Cells grown on 6-well plates were
treated with XC-302 (4 µM) and 24 h later were trypsinized
and washed with PBS prior to fixing in fixative buffer.
Subsequently, cells were collected by centrifugation at 500 × g for
10 min, suspended and incubated for 2 h in 2.5% glutaraldehyde.
Following fixation, cell samples were treated with 2% osmium
tetroxide in 0.1 M sodium cacodylate buffer, dehydrated through a
graded series of acetone and embedded in resin. Finally, the
samples were sliced into 65-nm sections, which were processed for
TEM (Hitachi electron microscope H-600; Hitachi, Ltd., Toyko,
Japan).
Transfection of green fluorescent protein
(GFP)-light chain 3 (LC3) expression vector
The GFP-LC3 expression vector was generously
provided by Professor X.F. Zhu (State Key Laboratory of Oncology).
Following transfection of the GFP-LC3 expression vector with
Lipofectamine 2000 (Invitrogen) for 24 h, following the
manufacturer's protocol, cells were divided into groups based as
follows: i) Negative control with 0.1% DMSO (4 µM); ii)
XC-302 (4 and 8 µM); iii) 3-MA (5 mM); and iv) 3-MA (5 mM) +
XC-302 (4 and 8 µM). Following the indicated treatment, the
localization of GFP was directly observed with a laser scanning
confocal microscope.
Western blot analysis
Following treatment of various concentrations of
XC-302 for different times, the total protein from the CNE-2 cells
was obtained by lysing in cell lysis buffer (Cell Signaling
Technology, Beverly, MA, USA). The proteins were resolved by sodium
dodecyl sulfate-polyacrylamide gel electrophoresis and transferred
to a polyvinylidene fluoride membrane. The membranes were
subsequently blocked with skimmed milk (5%) and incubated overnight
at 4°C with the following antibodies: Total AKT (1:1,000, #9916,
rabbit anti-human), mTOR, phospho-AKT (S473; 1:2,000, #9916, rabbit
anti-human), phospho-mTOR (1:1,000, #5536, rabbit anti-human), LC3
(1:1,000, #4599, rabbit anti-human), beclin 1 (1:1,000, #3495,
rabbit anti-human), p62 (1:1,000, #8025, rabbit anti-human) and
glyceraldehyde 3-phosphate dehydrogenase (GAPDH; 1:3,000, #5174,
rabbit anti-human), which were purchased from Cell Signaling
Technology. The samples were incubated with a secondary antibody
(1:4,000, #9916, anti-rabbit IgG; CST) for 1 h at room temperature
and the labeled proteins were detected using chemiluminescence
reagent and automatic X-ray film. Equal loading GAPDH was assessed
as the internal control for western blot analysis.
Downregulation of gene expression by
small interfering RNA (siRNA)
The specific siRNA oligomers against beclin 1
(forward, 5′-CAGTTTGGCACAATCAATAtt-3′) and si-control (forward,
5′-UUCUCCGAACGUGUCACGUtt-3′) were purchased from the Gene
Technology Co. (Shanghai, China). The CNE-2 cells were transfected
with si-beclin 1 and Lipofectamine 2000 (Invitrogen, Thermo Fisher
Scientific, Waltham, MA, USA) according to the manufacturer's
protocol. After incubation for 12 h, the transient transfected
CNE-2 were used for the following experiments.
Colony formation assay
The cells were grown for 24 h and subsequently
treated for 6 h as follows: Groups without intervention of siRNA,
i) negative control; ii) XC-302 (4 µM); iii) 3-MA (5 mM);
and iv) 3-MA (5 mM) + XC-302 (4 µM); and groups with
silencing of siRNA, i) si-control; ii) si-control cells with XC-302
(4 µM); iii) si-beclin 1; and iv) si-beclin 1 cells with
XC-302 (4 µM). The cells were trypsinized and subsequently
seeded in 6-well culture plates (500/well) for 2 weeks. The cells
were washed and fixed with ice-cold methanol for 10 min, followed
by the addition of 0.5% crystal violet solution for 10 min to
observe the colony formation.
Annexin V-FITC/propidium iodide (PI)
double staining
Briefly, the CNE-2 cells were treated with different
concentrations of XC-302 (4 and 8 µM) and/or 5 mM
3-methyladenine (3-MA, M9281; Sigma-Aldrich) for 24 h. Following
collection, the cells were stained with Annexin V-FITC and PI. The
apoptotic cells were estimated using a Beckman-Gallios flow
cytometer (Beckman-Gallios, Miami, FL, USA).
Statistical analysis
Whole data are exhibited as mean ± standard error of
the mean of more than two independent experiments in each group.
The variances between each group were calculated by Student's
t-test and P<0.05 was considered to indicate a statistically
significant difference.
Results
XC-302 inhibits the proliferation of
CNE-2 cells by inducing autophagy and apoptosis
To assess the effects of XC-302 on NPC cell
proliferation in vitro, CNE-2 cells were treated with XC-302
at different concentrations for 72 h and subsequently evaluated by
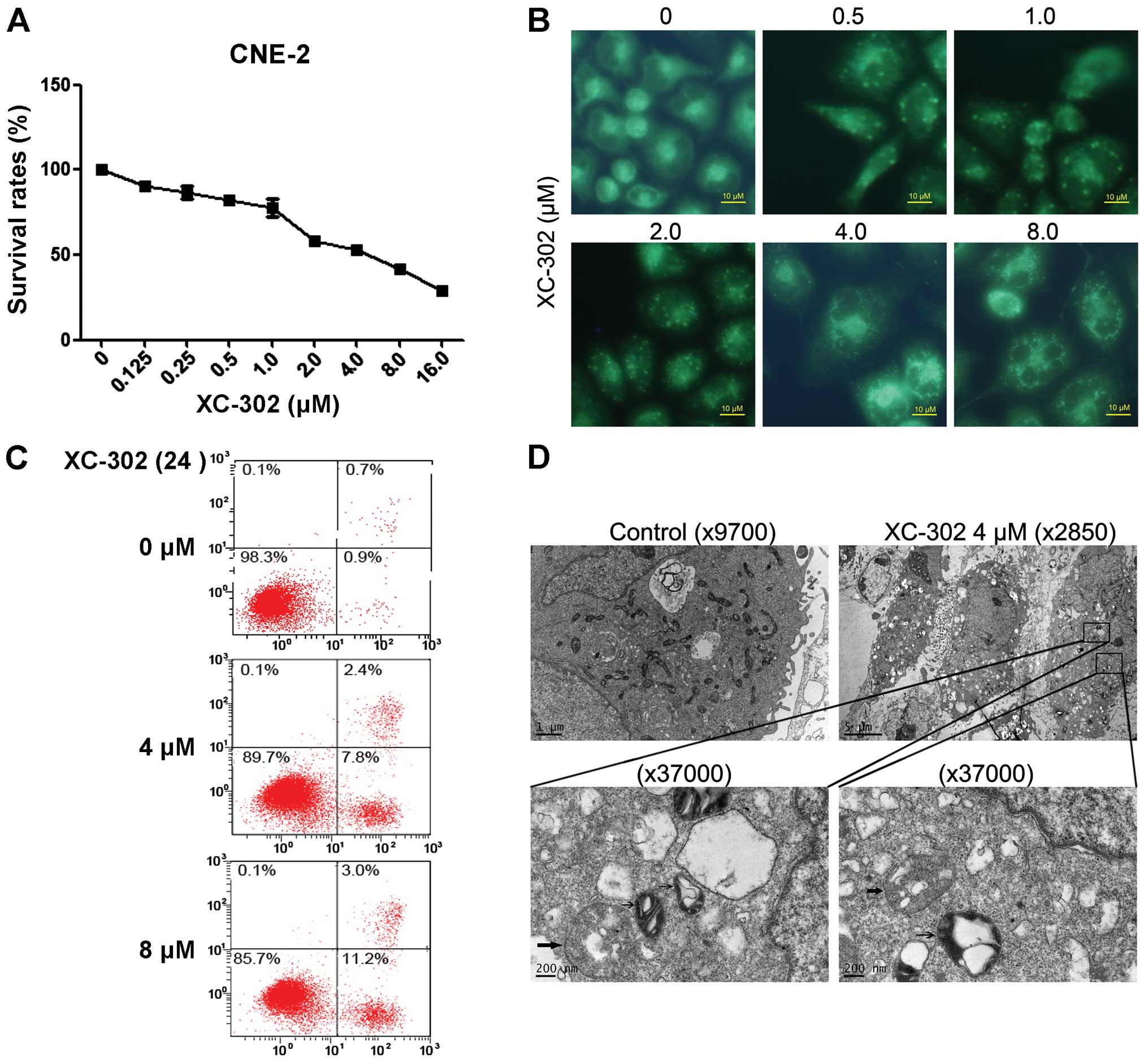
the MTT assays. Exposure to XC-302 showed a dose-dependent
inhibition of cell viability. MDC is known as a specific marker of
autophagic vacuoles (Fig. 2A).
XC-302-treated CNE-2 cells resulted in fluorescence intensity
enhanced with the increasing dose of the drug (Fig. 2B). In addition to autophagy,
XC-302 treatment also induced apoptosis in the CNE-2 cells. The
Annexin V-FITC/PI double staining showed that cells treated with
XC-302 increased the percentage of apoptosis up to 14.2% (Fig. 2C). The TEM was adopted to further
examine the autophagosomes of XC-302-treated cells. Compared with
the control cells, XC-302 treatment not only resulted in a rapid
increase of autophagosomes (thick arrow), but also induced the
formation of autolysosomes (thin arrow) in a portion of CNE-2 cells
(Fig. 2D).
XC-302 inhibits the activation of the
PI3K/AKT pathway during the process of autophagy in CNE-2
cells
Microtubule-associated protein 1 LC3 is a specific
marker for autophagy. It is converted from the inactive form,
LC3-I, to a cleaved form (LC3-II) during autophagy, and the LC3-II
protein has been frequently used for autophagy detection. In the
present study, the changes of the markers in autophagy were
analyzed by western blotting analysis. The LC3-II protein levels
were markedly increased by XC-302 treatment. The beclin 1 level was
augmented and as a degradation product, the expression of p62 was
decreased (Fig. 3A and B).
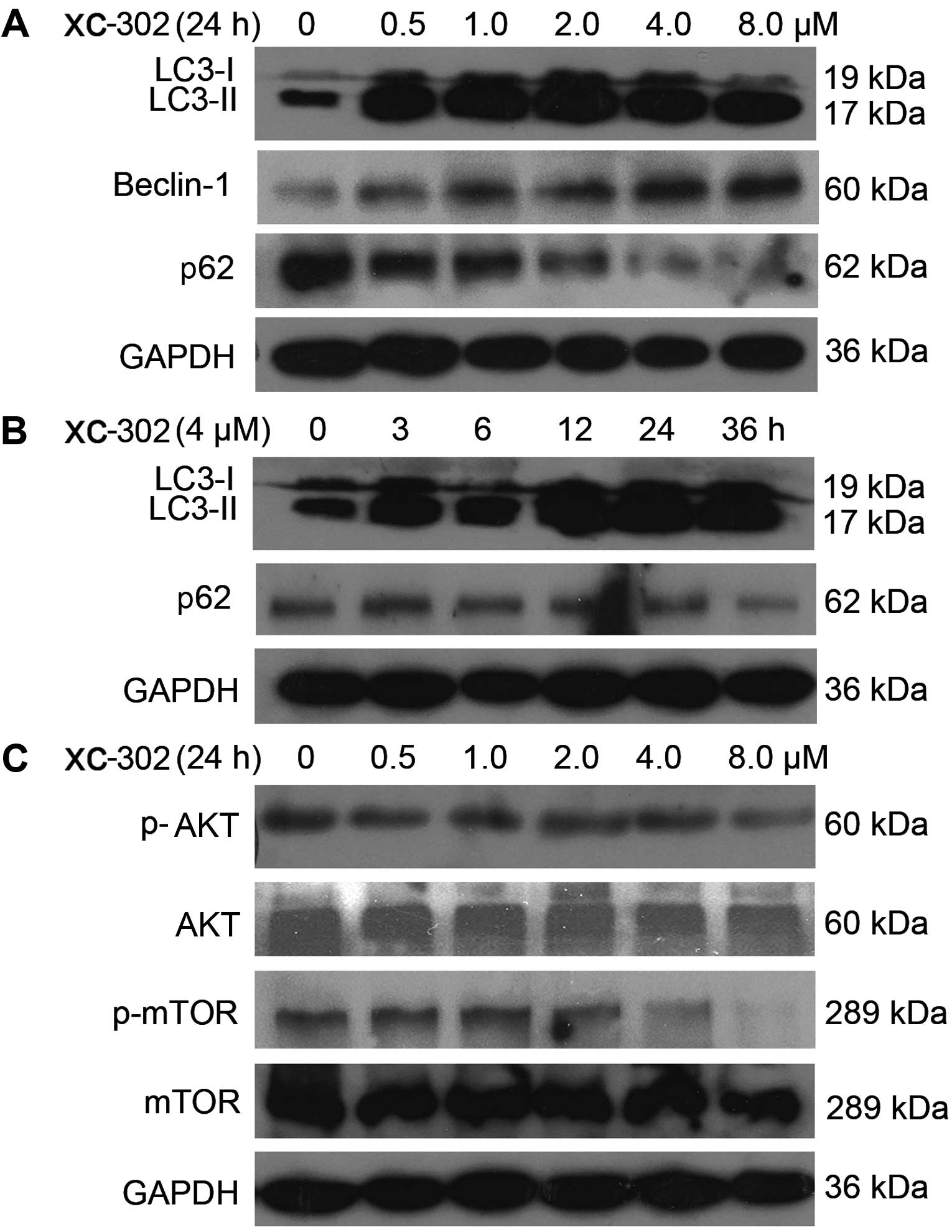 | Figure 3Western blot analysis was performed
for autophagy- and phospha-tidylinositol 3-kinase (PI3K)
pathway-related markers. (A) The cells were treated with XC-302
(8.0–0.5 µM) for 24 h. Cell lysates were prepared, and an
immunoblot was performed using antibodies against LC3-I, LC3-II,
beclin 1 and p62. (B) The effects of 4 µM XC-302 incubation
on the protein expression of LC3-I, LC3-II and p62 in CNE-2 cells
at 0, 3, 6, 12, 24 and 36 h. (C) Cells were treated with different
concentrations of XC-302 for 24 h. The immunoblot was conducted and
probed with anti-AKT, anti-p-AKT, anti-mTOR and anti-p-mTOR. LC,
light chain; AKT, protein kinase B; mTOR, mechanistic target of
rapamycin. |
Subsequently, whether the downstream targets of PI3K
could be inhibited by XC-302 was examined in the CNE-2 cell line.
As shown in Fig. 3C, following
exposure to XC-302 for 24 h, although the levels of AKT and mTOR
did not exhibit significant changes, the phosphorylation levels of
AKT and mTOR protein were attenuated when treated by XC-302 in a
dose-dependent manner.
Autophagy inhibitor 3-MA reduces cell
death induced by XC-302 in the CNE-2 cells
3-MA is a known specific inhibitor of autophagy,
which is frequently used to detect the role of autophagy under
various treatments. Thus, the effects of 3-MA was investigated on
the apoptosis, autophagy, proliferation and clone formation of
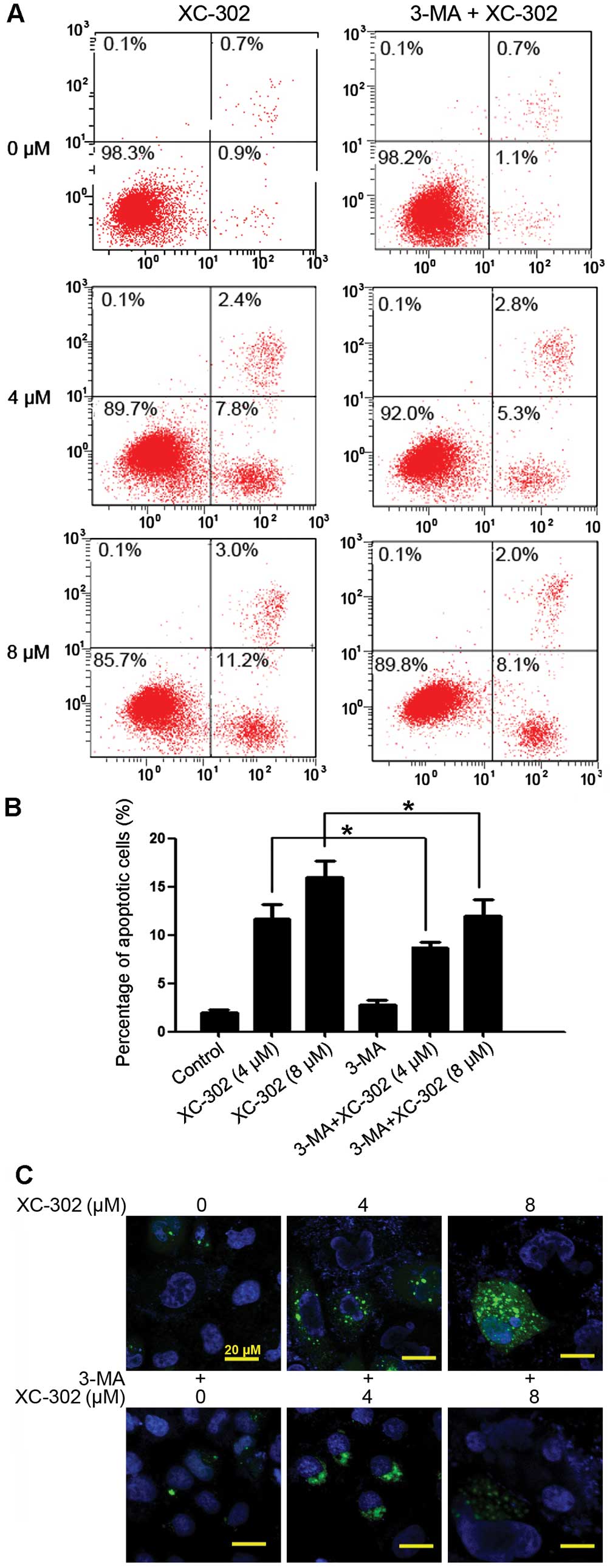
XC-302-treated CNE-2 cells. The apoptosis rate of cells were
markedly decreased in cells co-treated with various concentrations
of XC-302 and 3-MA, compared with those treated with XC-302 alone
(P<0.05) (Fig. 4A and B). To
detect the formation of autophagosomes specifically, cells were
transfected with the GFP-LC3 plasmid transiently. Following
treatment with XC-302, cells showed increased LC3 punctures
compared with the control in a dose-dependent manner (Fig. 4C), visualized by fluorescence
microscopy. In addition, there was a significant degradation of
green fluorescence in XC-302 (8 µM) and 3-MA co-treated
cells. These results corroborate the observation that XC-302
induced autophagy, as well as 3-MA decreased the accumulation of
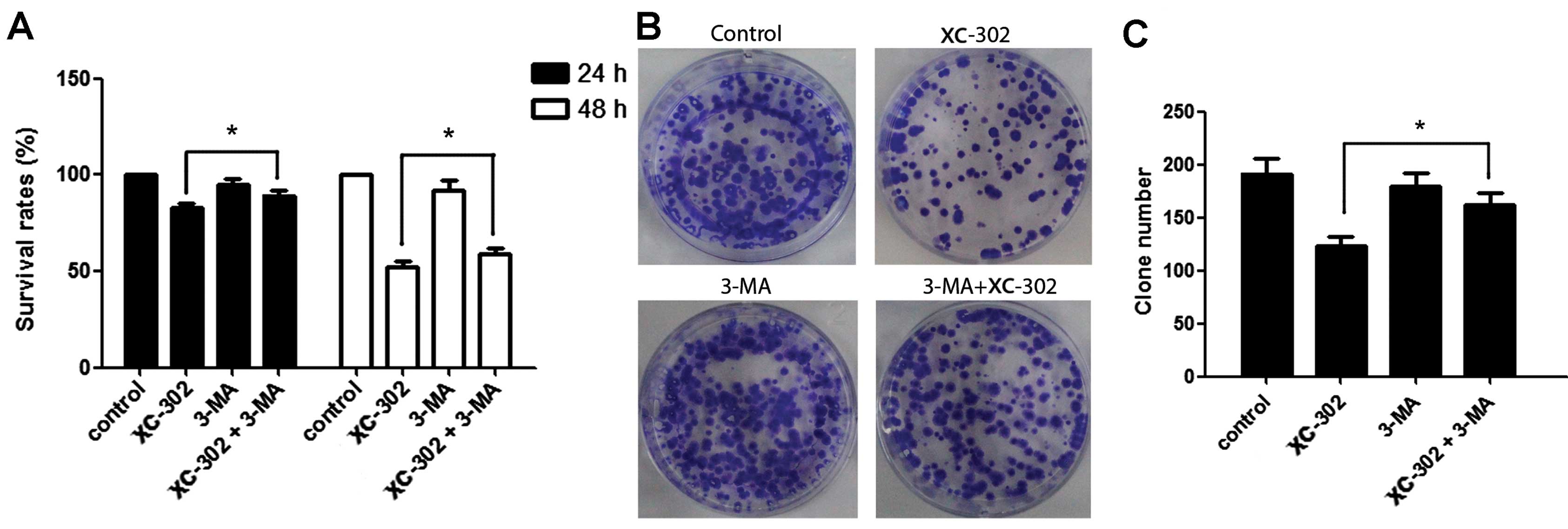
autophagosomes, in XC-302-exposed CNE-2 cells. The proliferation of
the CNE-2 cells was inhibited by XC-302 and could be reversed by
exposure to 3-MA after 24 or 48 h, as revealed by the MTT assay
(P<0.05) (Fig. 5A).
Subsequently, clone formation assays were used to further ensure
that 3-MA reduced the sensitivity of the cells to XC-302. The group
combining 5 mM 3-MA with 4 µM XC-302 formed more colonies
compared with the individual use of XC-302 (P<0.05) (Fig. 5B and C). These results clearly
reveal that autophagy contributes to XC-302-induced cell death in
CNE-2 cells.
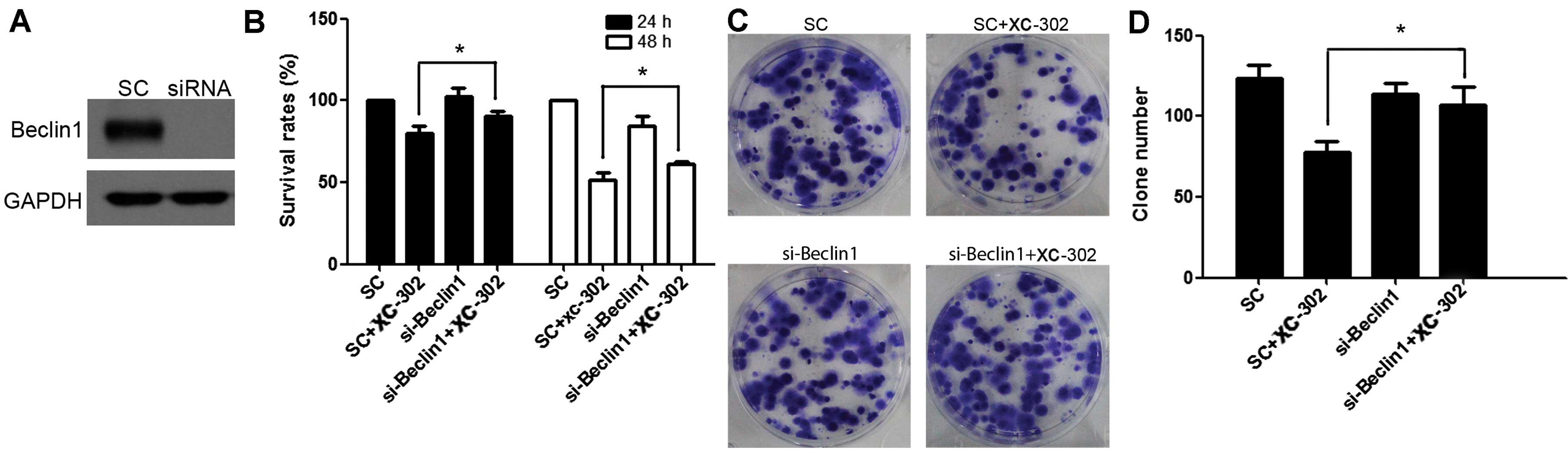
Knockdown of beclin 1 accelerates
proliferation and clone formation of CNE-2 cell line treated by
XC-302
Beclin 1 is a critical regulator of autophagy, which
can specifically suppress the autophagy pathway by knockdown of it.
The beclin 1 gene was further knocked down using siRNA and the
efficiency of the knockdown was confirmed by western blotting
(Fig. 6A). Using the MTT assay,
similar to the effect of 3-MA, the knockdown of beclin 1 resulted
in a higher vital rate following exposure to XC-302 (P<0.05)
(Fig. 6B). Additionally, clone
formation is markedly increased in beclin 1 knockdown cells
compared with the scramble control cells following the treatment of
XC-302 (Fig. 6C and D). Taken
together, these results revealed that the inhibition of autophagy
by beclin 1 knockdown promoted proliferation and clone formation of
CNE-2 cells that were exposed to XC-302.
Discussion
The PI3K/AKT/mTOR signaling pathway has a crucial
role in the tumorigenesis of human cancers, including NPC (17,18), which is extremely attractive for
targeted, molecular drug therapies. The NPC cell lines and tissues
also overexpressed phosphorylated AKT (19-21). The two well-studied PI3K
inhibitors are wortmannin and LY294002 (22). However, due to toxic responses,
and poor pharmacological properties, their application has been
primarily restricted. As a novel multiple target point inhibitor,
including PI3K, which was developed independently, XC-302 exhibited
promising inhibition of NPC cell proliferation, and not only
induced apoptotic cell death but also autophagy in the present
study.
As well as apoptosis, autophagy is a type of
programmed cell death that is mediated by activation of the
autophagy-related gene proteins. When autophagy is induced, the
characteristic structure change is the formation of acidic
vesicular organelles with double-membrane structures engulfing bulk
cytoplasmic organelles. Numerous antitumor agents have been
reported to induce autophagy (23). The results of the present study
showed the autophagosome accumulations in the CNE-2 cells and
MDC-positive stain following exposure to XC-302. LC3-II, beclin 1
and p62 are the reliable biomarkers of autophagy (24). As shown by western blotting
analysis, XC-302 augmented LC3-II and beclin 1 levels, and
downregulated p62 in the CNE-2 cells. Currently, increasing studies
have suggested that the PI3K/AKT pathway has a vital role in the
regulation of autophagy (25–27). The consequences of protein
expression are the hypothesis that the inhibition of the
PI3K/AKT/mTOR pathway is involved in XC-302 induced autophagy. In
the present study, XC-302 caused autophagy in the CNE-2 cell line,
which was activated when PI3K/AKT/mTOR was inhibited. In
particular, 3-MA suppressed the XC-302-induced accumulation of
autophagosomes. As opposed to triggering the type I PI3K by XC-302,
3-MA inhibits autophagy in mammalian cells through inhibiting class
III PI3K (28,29), which may explain the diverse
effects of XC-302 and 3-MA in autophagy. XC-302 treatment also
triggered apoptosis, as evidenced by Annexin V-PI double
staining.
However, whether autophagy represents a survival
mechanism or contributes to cell death remains controversial
(30). The present study has
defined the role of XC-302-mediated autophagy in CNE-2 cell
functions. Inhibition of autophagy by 3-MA could markedly suppress
XC-302-induced cell death. Consistent with this, the present
findings were further strengthened by transduction of specific
target siRNAs to block autophagy, and knockdown of beclin 1 in
combination with XC-302 markedly accelerated proliferation and
clone formation of the CNE-2 cell line compared to using XC-302
alone. Taken together, these results propose that autophagy
provided a survival disadvantage for these NPC cells.
Notably, the promoted effect of apoptosis due to
XC-302 treatment was reversed when autophagy was suppressed by 3-MA
in the CNE-2 cells. In NPC, the associations of apoptosis with
autophagy in response to PI3Ks inhibition remain unknown. The
present results demonstrate that autophagy, as well as apoptosis,
participate commonly in the death of CNE-2 cells induced by XC-302,
and furthermore, autophagy may serve as a significant role in the
process of apoptotic cell death. The mechanisms connecting
autophagy with apoptosis are not entirely clear, and studies have
generated inconsistent results. However, B-cell lymphoma-2 (Bcl-2)
has been defined as a central regulator of autophagic and apoptotic
signaling pathways (31–34). Beclin 1 was discovered by a yeast
two-hybrid system as a binding partner of Bcl-2 (Bcl-2-beclin 1
complex) (31). Recent
discoveries have suggested that certain apoptotic proteins modulate
autophagy (35). In the present
study, the phenomenon of mitochondrial swelling was observed when
cells were exposed to XC-302. Tolkovsky et al (36) considered that the cytochrome
c released by injured mitochondria could activate autophagy
and apoptosis when the permeability of mitochondria was altered,
which prompted the membrane potential. Therefore, it is possible
that the mitochondria switches the cellular program from one to
another.
In conclusion, to the best of our knowledge, this is
the first study to report that XC-302 may induce autophagy, which
promotes the program of CNE-2 cell death probably by inhibition of
the PI3K/AKT/mTOR signaling pathway. Thus, XC-302 may be a
potential novel candidate for treating human NPC, and enhancing
autophagy is a new way to strengthen the effects of antitumor
therapies. Furthermore, XC-302 also promoted apoptosis in CNE-2
cells, which could be reversed when autophagy was suppressed. While
autophagy has been served as a possible therapeutic target in NPC
treated with XC-302, the exact effects and association between
autophagy and apoptosis remain unclear. More studies are required
in the future to elucidate the associations.
References
|
1
|
Cantley LC: The phosphoinositide 3-kinase
pathway. Science. 296:1655–1657. 2002. View Article : Google Scholar : PubMed/NCBI
|
|
2
|
Luo J, Manning BD and Cantley LC:
Targeting the PI3K-Akt pathway in human cancer: Rationale and
promise. Cancer Cell. 4:257–262. 2003. View Article : Google Scholar : PubMed/NCBI
|
|
3
|
Courtney KD, Corcoran RB and Engelman JA:
The PI3K pathway as drug target in human cancer. J Clin Oncol.
28:1075–1083. 2010. View Article : Google Scholar : PubMed/NCBI
|
|
4
|
Chang ET and Adami HO: The enigmatic
epidemiology of nasopharyngeal carcinoma. Cancer Epidemiol
Biomarkers Prev. 15:1765–1777. 2006. View Article : Google Scholar : PubMed/NCBI
|
|
5
|
Spratt DE and Lee N: Current and emerging
treatment options for nasopharyngeal carcinoma. Onco Targets Ther.
5:297–308. 2012.PubMed/NCBI
|
|
6
|
Lin S, Pan J, Han L, Guo Q, Hu C, Zong J,
Zhang X and Lu JJ: Update report of nasopharyngeal carcinoma
treated with reduced-volume intensity-modulated radiation therapy
and hypothesis of the optimal margin. Radiother Oncol. 110:385–389.
2014. View Article : Google Scholar : PubMed/NCBI
|
|
7
|
Xiao WW, Huang SM, Han F, Wu SX, Lu LX,
Lin CG, Deng XW, Lu TX, Cui NJ and Zhao C: Local control, survival,
and late toxicities of locally advanced nasopharyngeal carcinoma
treated by simultaneous modulated accelerated radiotherapy combined
with cisplatin concurrent chemotherapy: Long-term results of a
phase 2 study. Cancer. 117:1874–1883. 2011. View Article : Google Scholar : PubMed/NCBI
|
|
8
|
Gupta AK1, McKenna WG, Weber CN, Feldman
MD, Goldsmith JD, Mick R, Machtay M, Rosenthal DI, Bakanauskas VJ,
Cerniglia GJ, et al: Local recurrence in head and neck cancer:
relationship to radiation resistance and signal transduction. Clin
Cancer Res. 8:885–892. 2002.PubMed/NCBI
|
|
9
|
Liu T, Sun Q, Li Q, Yang H, Zhang Y, Wang
R, Lin X, Xiao D, Yuan Y, Chen L, et al: Dual PI3K/mTOR inhibitors,
GSK2126458 and PKI-587, suppress tumor progression and increase
radio-sensitivity in nasopharyngeal carcinoma. Mol Cancer Ther.
14:429–439. 2014. View Article : Google Scholar
|
|
10
|
Yang F, Qian XJ, Qin W, Deng R, Wu XQ, Qin
J, Feng GK and Zhu XF: Dual phosphoinositide 3-kinase/mammalian
target of rapamycin inhibitor NVP-BEZ235 has a therapeutic
potential and sensitizes cisplatin in nasopharyngeal carcinoma.
PLoS One. 8:e598792013. View Article : Google Scholar : PubMed/NCBI
|
|
11
|
Liu Y, Chen LH, Yuan YW, Li QS, Sun AM and
Guan J: Activation of AKT is associated with metastasis of
nasopharyngeal carcinoma. Tumour Biol. 33:241–245. 2012. View Article : Google Scholar
|
|
12
|
Hanahan D and Weinberg RA: Hallmarks of
cancer: The next generation. Cell. 144:646–674. 2011. View Article : Google Scholar : PubMed/NCBI
|
|
13
|
Galluzzi L, Vitale I, Abrams JM, Alnemri
ES, Baehrecke EH, Blagosklonny MV, Dawson TM, Dawson VL, El-Deiry
WS, Fulda S, et al: Molecular definitions of cell death
subroutines: Recommendations of the Nomenclature Committee on Cell
Death 2012. Cell Death Differ. 19:107–120. 2012. View Article : Google Scholar :
|
|
14
|
Deng Q, Yu X, Xiao L, Hu Z, Luo X, Tao Y,
Yang L, Liu X, Chen H, Ding Z, et al: Neoalbaconol induces energy
depletion and multiple cell death in cancer cells by targeting
PDK1-PI3-K/Akt signaling pathway. Cell Death Dis. 4:e8042013.
View Article : Google Scholar : PubMed/NCBI
|
|
15
|
Zhao YY, Tian Y, Zhang J, Xu F, Yang YP,
Huang Y, Zhao HY, Zhang JW, Xue C, Lam MH, et al: Effects of an
oral allosteric AKT inhibitor (MK-2206) on human nasopharyngeal
cancer in vitro and in vivo. Drug Des Devel Ther. 8:1827–1837.
2014. View Article : Google Scholar : PubMed/NCBI
|
|
16
|
Munafó DB and Colombo MI: A novel assay to
study autophagy: Regulation of autophagosome vacuole size by amino
acid deprivation. J Cell Sci. 114:3619–3629. 2001.PubMed/NCBI
|
|
17
|
Ma BB, Lui VW, Hui EP, Lau CP, Ho K, Ng
MH, Cheng SH, Tsao SW and Chan AT: The activity of mTOR inhibitor
RAD001 (everolimus) in nasopharyngeal carcinoma and
cisplatin-resistant cell lines. Invest New Drugs. 28:413–420. 2010.
View Article : Google Scholar
|
|
18
|
Ma BB, Lui VW, Hui CW, Lau CP, Wong CH,
Hui EP, Ng MH, Tsao SW, Li Y and Chan AT: Preclinical evaluation of
the AKT inhibitor MK-2206 in nasopharyngeal carcinoma cell lines.
Invest New Drugs. 31:567–575. 2013. View Article : Google Scholar
|
|
19
|
Morrison JA, Gulley ML, Pathmanathan R and
Raab-Traub N: Differential signaling pathways are activated in the
Epstein-Barr virus-associated malignancies nasopharyngeal carcinoma
and Hodgkin lymphoma. Cancer Res. 64:5251–5260. 2004. View Article : Google Scholar : PubMed/NCBI
|
|
20
|
Huang XM, Dai CB, Mou ZL, Wang LJ, Wen WP,
Lin SG, Xu G and Li HB: Overproduction of cyclin D1 is dependent on
activated mTORC1 signal in nasopharyngeal carcinoma: Implication
for therapy. Cancer Lett. 279:47–56. 2009. View Article : Google Scholar : PubMed/NCBI
|
|
21
|
Chen J, Hu CF, Hou JH, Shao Q, Yan LX, Zhu
XF, Zeng YX and Shao JY: Epstein-Barr virus encoded latent membrane
protein 1 regulates mTOR signaling pathway genes which predict poor
prognosis of nasopharyngeal carcinoma. J Transl Med. 8(30)2010.
View Article : Google Scholar
|
|
22
|
Liu P, Cheng H, Roberts TM and Zhao JJ:
Targeting the phosphoinositide 3-kinase pathway in cancer. Nat Rev
Drug Discov. 8:627–644. 2009. View
Article : Google Scholar : PubMed/NCBI
|
|
23
|
Tekirdag KA, Korkmaz G, Ozturk DG, Agami R
and Gozuacik D: MIR181A regulates starvation- and rapamycin-induced
autophagy through targeting of ATG5. Autophagy. 9:374–385. 2013.
View Article : Google Scholar : PubMed/NCBI
|
|
24
|
Mizushima N: Methods for monitoring
autophagy. Int J Biochem Cell Biol. 36:2491–2502. 2004. View Article : Google Scholar : PubMed/NCBI
|
|
25
|
Fujiwara K, Iwado E, Mills GB, Sawaya R,
Kondo S and Kondo Y: Akt inhibitor shows anticancer and
radiosensitizing effects in malignant glioma cells by inducing
autophagy. Int J Oncol. 31:753–760. 2007.PubMed/NCBI
|
|
26
|
Hung JY, Hsu YL, Li CT, Ko YC, Ni WC,
Huang MS and Kuo PL: 6-Shogaol, an active constituent of dietary
ginger, induces autophagy by inhibiting the AKT/mTOR pathway in
human non-small cell lung cancer A549 cells. J Agric Food Chem.
57:9809–9816. 2009. View Article : Google Scholar : PubMed/NCBI
|
|
27
|
Shin SY, Lee KS, Choi YK, Lim HJ, Lee HG,
Lim Y and Lee YH: The antipsychotic agent chlorpromazine induces
autophagic cell death by inhibiting the Akt/mTOR pathway in human
U-87MG glioma cells. Carcinogenesis. 34:2080–2089. 2013. View Article : Google Scholar : PubMed/NCBI
|
|
28
|
Seglen PO and Gordon PB: 3-Methyladenine:
Specific inhibitor of autophagic/lysosomal protein degradation in
isolated rat hepatocytes. Proc Natl Acad Sci USA. 79:1889–1892.
1982. View Article : Google Scholar : PubMed/NCBI
|
|
29
|
Lum JJ, Bauer DE, Kong M, Harris MH, Li C,
Lindsten T and Thompson CB: Growth factor regulation of autophagy
and cell survival in the absence of apoptosis. Cell. 120:237–248.
2005. View Article : Google Scholar : PubMed/NCBI
|
|
30
|
Eisenberg-Lerner A and Kimchi A: The
paradox of autophagy and its implication in cancer etiology and
therapy. Apoptosis. 14:376–391. 2009. View Article : Google Scholar : PubMed/NCBI
|
|
31
|
Pattingre S, Tassa A, Qu X, Garuti R,
Liang XH, Mizushima N, Packer M, Schneider MD and Levine B: Bcl-2
antiapoptotic proteins inhibit Beclin 1-dependent autophagy. Cell.
122:927–939. 2005. View Article : Google Scholar : PubMed/NCBI
|
|
32
|
Levine B, Sinha S and Kroemer G: Bcl-2
family members: Dual regulators of apoptosis and autophagy.
Autophagy. 4:600–606. 2008. View Article : Google Scholar : PubMed/NCBI
|
|
33
|
Chang NC, Nguyen M, Germain M and Shore
GC: Antagonism of Beclin 1-dependent autophagy by BCL-2 at the
endoplasmic reticulum requires NAF-1. EMBO J. 29:606–618. 2010.
View Article : Google Scholar :
|
|
34
|
Marquez RT and Xu L: Bcl-2:Beclin 1
complex: multiple, mechanisms regulating autophagy/apoptosis toggle
switch. Am J Cancer Res. 2:214–221. 2012.PubMed/NCBI
|
|
35
|
Mukhopadhyay S, Panda PK, Sinha N, Das DN
and Bhutia SK: Autophagy and apoptosis: where do they meet?
Apoptosis. 19:555–566. 2014. View Article : Google Scholar : PubMed/NCBI
|
|
36
|
Tolkovsky AM, Xue L, Fletcher GC and
Borutaite V: Mitochondrial disappearance from cells: A clue to the
role of autophagy in programmed cell death and disease? Biochimie.
84:233–240. 2002. View Article : Google Scholar : PubMed/NCBI
|