Introduction
Myocardial ischemia, which is caused by an imbalance
between the myocardial oxygen supply and myocardial oxygen
requirement, can induce arrhythmia, cardiac dysfunction, myocardial
infarction and sudden death (1).
Although there are a number of novel drugs available for the
treatment and prevention of myocardial ischemia, the mortality and
morbidity continue to increase (2). It was previously reported that
apoptosis may be an important step in the pathogenesis of
myocardial injury, and exploring anti-apoptotic drugs may provide
novel therapeutic opportunities for the treatment of myocardial
ischemia (3).
Traditional Chinese medicine (TCM) has been used to
treat cardiovascular diseases for more than 1,000 years with
significant efficacy and minimal side effects (4). Among the herbs used in TCM, Radix
Salvia miltiorrhiza (SM) and Lignum Dalbergia
odorifera (DO) have been widely used in clinical and basic
laboratory studies for the prevention and treatment of
cardiovascular diseases, including in China (5-10).
SM, known as Danshen in Chinese, has been used to treat
cardiovascular diseases, including coronary heart disease,
hyperlipidemia and cerebrovascular diseases (11). DO, known as Jiangxiang in Chinese,
has been used to treat ischemia, necrosis, swelling, blood
disorders and rheumatic pain (12). A number well-known Chinese
medicines for treating cardiovascular disease contain SM and DO,
including Guanxin II, Guanxin Danshen capsules, Xiangdan injection
and Qishen Yiqi pills. The effect of the combination of SM-DO has
been shown to be efficacious in clinical use (13,14); however, there are few studies
regarding their action and the underlying mechanisms responsible.
In our previous experiment, the cardioprotective effects of SM and
DO were evaluated in a rat myocardial ischemia-reperfusion model.
The results indicated that combined treatment with SM and DO had
significant cardioprotective effects, and that the combination of
SM with DO volatile oil (DOO) (SM 5 g/kg/day, DOO 0.5 ml/kg/day)
was significantly more effective than SM, DO or DOO alone (15). However, the effects of SM-DOO in
chronic myocardial ischemia have yet to be reported.
The aim of the present study was to investigate the
cardio-protective effect and potential mechanisms of SM-DOO in a
pig model of chronic myocardial ischemia. The major chemical
components of SM and DOO were also determined using
high-performance liquid chromatography (HPLC) and gas
chromatography coupled with mass spectrometry (GC-MS),
respectively.
Materials and methods
Materials and reagents
SM extract was purchased from Xi'an Honson
Biotechnology Co., Ltd. (Xi'an, China; batch no. 161025). The major
components were hydrophilic salvanolic acid and hydrophobic
tanshinones, as evaluated by HPLC analysis. DOO was purchased from
Jishui Jinhai Natural Perfume Oil Technology Co., Ltd. (Jiangxi,
China; batch no. XC20160918) and the major components were
evaluated by GC-MS. Standards for danshensu, rosmarinic acid,
salvianolic acid B, salvianolic acid A, protocatechuic acid,
protocatechuic aldehyde, dihydrotanshinone I, cryptotanshinone,
tanshinone IIA and tanshinon IIA silate
sodium were purchased from Shanghai ANPEL Laboratory Technologies,
Inc. (Shanghai, China; batch no. Q2880010). Acetonitrile was
purchased from Thermo Fisher Scientific, Inc. (Waltham, MA, USA).
All other reagents were analysis grade.
Deionized water was prepared using a Milli-Q water
purification system (EMD Millipore, Bedford, MA, USA).
2,3,5-triphenyltetrazolium chloride (TTC) was purchased from
Sigma-Aldrich (Merck KGaA, Darmstadt, Germany). Pig creatine
kinase-MB (CK-MB), cardiac troponin I (cTnI) and myoglobin (Myo)
ELISA kits were bought from Xitang Biology Technology Company
(Shanghai, China). Lactate dehydrogenase (LDH), alanine
aminotransferase (ALT) and aspartate aminotransferase (AST) test
kits were purchased from Nanjing Jiancheng Bioengineering Institute
(Nanjing, China). All primary antibodies, including Bcl-2
associated X (Bax; cat. no. 2772), Bcl-2 (cat. no. 2870), Akt (cat.
no. 9272), phosphorylated (p)-Akt (cat. no. 9271), glycogen
synthase kinase (GSK)-3β (cat. no. 9315), p-GSK-3β (cat. no. 9336)
and β-actin (cat. no. 4970), were purchased from Cell Signaling
Technologies, Inc. (Danvers, MA, USA). The secondary antibody
(anti-rabbit IgG-B; cat. no. sc-53804) was purchased from Santa
Cruz Biotechnology, Inc. (Dallas, TX, USA).
Herbal extraction
SM was dried at 50°C and ground into powder (<1
mm). SM (150 g) was soaked in 8-fold the volume of water for 30 min
at room temperature and extracted for 3 h (1.5 h/reflux), followed
by reflux extraction with 75% ethanol. The filtrates were combined,
concentrated under reduced pressure and freeze-dried. DOO was
isolated by steam distillation for 5 h, with a yield of 0.5% DOO,
which was stored at 4°C.
Preparation of standard solutions
Primary standard solutions of the 10 components were
prepared by dissolving the solid standards in methanol. Working
mixed standard solutions (40 μg/ml) were prepared by mixing
and diluting the stock solution with methanol. The mixed standard
solution was filtered through a 0.22-μm membrane before HPLC
analysis.
Preparation of herb solutions
SM was dried at a temperature of 50°C and ground
into powder. Subsequently, 0.25 g SM was soaked in 8-fold the
volume of water for 30 min at room temperature and extracted for 4
h, followed by ultrasound-assisted extraction for 30 min with 80%
methanol. The suspension was filtered, concentrated and diluted to
a 50-ml volume with methanol. The solution was filtered through a
0.22-μm membrane prior to HPLC analysis.
An aliquot of 200 μl DOO was diluted in 20 ml
of ethyl acetate and dried over anhydrous sodium sulfate. The
supernatant was filtered through a 0.22-μm membrane prior to
GC-MS analysis.
Chromatographic conditions
HPLC analysis was performed using an Agilent 1260
HPLC system (Agilent Technologies, Santa Clara, CA, USA) and
chromatographic separation was accomplished using an Agilent TC-C18
column (4.6×250 mm, 5 μm). The column temperature was set at
30°C with a 20-μl injection volume. The mobile phase
consisted of 0.2% formic acid (v/v) in water (A) and acetonitrile
(B). The gradient program used was as follows: 10% B to 30% B (0-15
min), 30% B to 32% B (15-40 min), 32% B to 55% B (40-55 min), 55% B
to 67% B (55-65 min), 67% B to 72% B (65-75 min), 72% B to 85% B
(75-85 min) and 100% B (85-100 min). The flow rate was set at 0.8
ml/min throughout the analysis, and UV detection was set at 270
nm.
The components of DOO were analyzed using an Agilent
7890A gas chromatograph coupled with an Agilent 5975C mass
selective detector (Agilent Technologies). Chromatographic
separation was performed using an HP-5MS capillary column (30 m ×
0.25 mm × 0.25 μm film thickness, Agilent Technologies). The
split ratio was 15:1, and the injection volume was set to 2
μl. The inlet and ion source temperatures were set to 260°C
and 230°C, respectively. The helium flow rate was set to 1.0
ml/min. The oven temperature was initially 60°C, followed by a
1.5°C/min increase to 105°C for 10 min, then a 1°C/min increase to
115°C for 10 min, a 2.5°C/min increase to 160°C for 5 min and
finally to 260°C at a heating rate of 20°C/min. MS was used in full
scan mode with the acquisition range set to 30-800 m/z. GC-MS
post-run analysis was performed, and the main components were
identified using the library of the National Institute of Standards
and Technology (NIST) (16). The
peak area normalization method was used to establish the relative
content of each substance in the sample.
Animals and experimental protocol
A total of 18 male Yorkshire pigs (25-30 kg) were
purchased from the Institute of Experiment Animals at the Fuwai
Hospital Experimental Animal Center (Beijing, China) and kept in an
animal room at 25±1°C with 55±5% humidity. The Animal Welfare and
Ethics Committee of Fuwai Hospital, Chinese Academy of Medical
Sciences approved all experiments [approval no. 0072-1-27-HX (F)].
After one week of acclimation, the pigs were randomized into 3
groups as follows: i) Sham group (n=6), oral administration of
regular diet and sham-operated without ameroid constrictor
implantation; ii) Model group (n=6), oral administration of regular
diet; iii) SM-DOO group (n=6), oral administration of regular diet
with 1 g/kg/day SM and 0.1 ml/kg/day DOO. The dosages of SM and DOO
were determined based on our previous studies, and adjusted for
pigs according to a previously published method (15,17). Pigs were provided free access to
water and were fed twice a day. All animals were observed during
feeding to ensure the entire portion of food was consumed.
At 4 weeks after the dietary modification,
pentobarbital sodium (25 mg/kg) was administered intramuscularly
(i.m.) to induce anesthesia. Animals were intubated, ventilated
with oxygen at 1.5-2 l/min and anesthetized with 3% isoflurane. The
pigs were right lateral decubitus, and a small thoracotomy was
performed in intercostal segments 3 and 4 by sterile techniques. An
ameroid constrictor (Research Instruments NW, Inc., Lebanon, OR,
USA) with a 2.5-mm internal diameter was implanted around the left
anterior descending artery (LAD). The ameroid constrictor was
designed to achieve myocardial ischemia by inducing progressive
coronary artery stenosis with a progression similar to that
observed in humans. The pericardium was closed using a 6-0
polypropylene suture (Ethicon, Inc., Somerville, NJ, USA) and the
chest was sutured closed. After the surgery, penicillin (6,400,000
U/day, i.m.) was administered to all pigs to prevent infection.
After 8 weeks, echocardiography, X-ray coronary
angiography and hemodynamics analysis were performed. All surgical
protocols were designed to minimize the suffering of the pigs. A
schematic presentation of the study protocol is shown in Fig. 1.
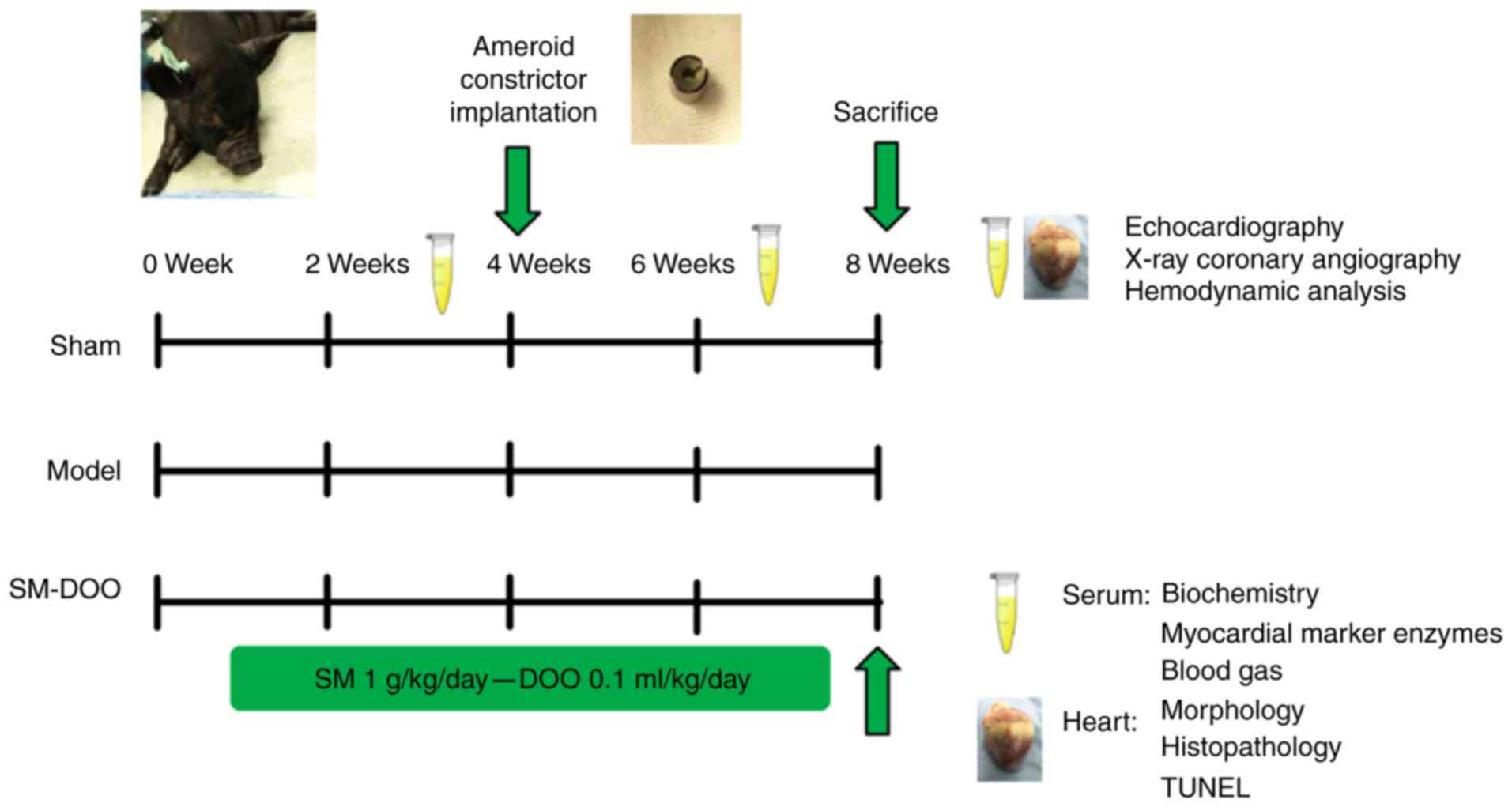 | Figure 1Schematic presentation of the study
protocol. Pigs were randomly divided into 3 groups: Sham, Model and
SM-DOO (n=6). The SM-DOO group received SM (1 g/kg/day) and DOO
(0.1 ml/kg/day) orally for 8 weeks. At 4 weeks, an ameroid
constrictor was placed around the left anterior descending coronary
artery in the Model and SM-DOO groups. At weeks 2, 4 and 8,
biochemical markers, myocardial marker enzymes and blood gas
constituents were measured in the serum. After 8 weeks,
echocardiography, X-ray coronary angiography and hemodynamic
analysis were performed. Myocardial tissue underwent morphological,
histopathological, apoptosis and western blot analysis to evaluate
the cardioprotective effects and underlying mechanisms of SM-DOO.
SM, Radix Salvia miltiorrhiza; DOO, Lignum Dalbergia
odorifera volatile oil; TUNEL, terminal deoxynucleotidyl
transferase-mediated dUTP nick end-labeling. |
Measurement of myocardial injury
markers
Blood samples were collected in heparinized tubes,
allowed to clot for 30 min and centrifuged at 2,285 × g at 4°C for
15 min. Myocardial injury markers, including CK-MB, LDH, ALT, AST,
cTnI and Myo, were measured using assay kits or pig-specific ELISA
kits according to the manufacturers' protocols.
Blood gas analysis
At weeks 2, 6 and 8, pH, PO2 and
PCO2 were measured in arterial blood samples taken from
the femoral artery (500-700 μl) using pre-heparinized
syringes (1,000 IU/ml) and analyzed using an i-STAT 1 blood gas
system (Abbott Laboratories, Chicago, IL, USA).
Echocardiography
Echocardiography was performed at the end of the
study using a Vivid 9 machine (GE Vingmed Ultrasound AS, Horten,
Norway). Left ventricular end-diastolic diameter (LVEDd), left
ventricular end-systolic diameter (LVEDs), end-diastolic volume
(EDV), end-systolic volume (ESV), ejection fraction (EF) and
fractional shortening (FS) were recorded to assess cardiac
function. The FS value was calculated based on the following
equation: FS (%) = [(LVEDd-LVEDs)/LVEDd] × 100%. Images were stored
and analyzed using Echopac software (GE Vingmed Ultrasound AS).
X-ray coronary angiography
X-ray coronary angiography (GE Medical Systems,
Milwaukee, WI, USA) with iopromide (Juste SAQF, Madrid, Spain) was
performed on all experimental animals to verify the occlusion of
the LAD and assess collateral vessel filling at the end of the
experiment. The grade of collateral filling was scored using a
standard 4-point scale as follows (18): 0 = no collateral filling; 1 =
minimal collateral filling; 2 = moderate collateral filling, but
less than the contralateral or ipsilateral non-infarct coronary
artery; 3 = normal collateral filling compared with the
contralateral or ipsilateral non-infarct coronary artery.
Hemodynamic monitoring
The heart rate (HR), mean arterial blood pressure
(MAP), left ventricular systolic pressure (LVSP), left ventricular
end-diastolic pressure (LVEDP), left ventricular maximum upstroke
velocity (+dp/dtmax) and left ventricular maximum
descent velocity (−dp/dtmax) were recorded using a
pressure transducer (Millar Instruments, Houston, TX, USA)
connected to an anesthesia monitor (Philips, Eindhoven,
Netherlands).
Morphometric and histopathological
examination
Animals were sacrificed by intravenous injection
with potassium chloride after the imaging study, and their hearts
were explanted. Hearts were serially sliced and incubated with 2%
TTC for 20 min at 37°C. An Image-Pro Plus image system (Media
Cybernetics, Bethesda, MD, USA) was used to analyze the infarct
(white) and non-infarct (red) areas. The percentage of myocardial
infarct was calculated as infarct area divided by total area.
The left ventricle was harvested, fixed in 4%
paraformaldehyde, embedded in paraffin and sectioned. Sections were
stained with hematoxylin and eosin (H&E) for histological
examination. The pathology of heart sections was investigated using
a light microscope, and photomicrographs were captured.
Measurement of myocardial apoptosis
Myocardial apoptosis was measured using an In-Situ
Cell Death Detection kit (Wanlei Bio, Shenyang, China) according to
the manufacturer's protocol. Myocardial slices were subjected to
terminal deoxynucleotidyl transferase-mediated dUTP nick
end-labeling (TUNEL) staining combined with a DAPI (Sigma-Aldrich;
Merck KGaA) counterstain. Images were obtained under a fluorescence
microscope at ×400 magnification (Nikon Corporation, Tokyo, Japan),
to confirm the successful labeling of apoptotic cells and nuclei.
The percentage of TUNEL-positive cells was calculated as the number
of apoptotic cells divided by the total number of nuclei × 100.
Western blotting analysis
Myocardial tissues were homogenized in RIPA buffer
containing 1% PMSF and 1% protease inhibitor cocktail (Nanjing
Jiancheng Bioengineering Institute), and the supernatant was
harvested by concentration (18,447 x g at 4°C for 10 min). The
protein concentration was determined based on the BCA method using
a Protein Quantitative Analysis kit (Nanjing Jiancheng
Bioengineering Institute). The lysates were separated by 10%
SDS-PAGE. Following separation, the proteins were transferred onto
polyvinyl difluoride membranes, blocked for 1 h at 37°C with 5%
non-fat dried milk, washed 3 times with Tween in Tris-buffered
saline, and incubated with primary antibodies against Bax, Bcl-2,
Akt, p-Akt, GSK-3β, p-GSK-3β and β-actin (dilution, 1:1,000)
overnight at 4°C. Subsequent to washing 3 times as described above,
the membranes were incubated with secondary antibodies (dilution,
1:5,000) at 37°C for 1 h. Immunoreactive bands were detected using
the enhanced chemiluminescence method and semi-quantified using
ImageJ Software version 1.47 (National Institutes of Health,
Bethesda, MD, USA).
Statistical analysis
Statistical analysis was conducted using GraphPad
Prism version 6.02 (GraphPad Software, Inc., La Jolla, CA, USA).
All data are presented as the mean ± standard deviation. One-way
analysis of variance with Tukey's multiple comparison post-hoc test
was performed to analyze the data. P<0.05 was considered to
represent a statistically significant difference.
Results
Evaluation of the chronic myocardial
ischemia model and effect of SM-DOO on collateral vessel
filling
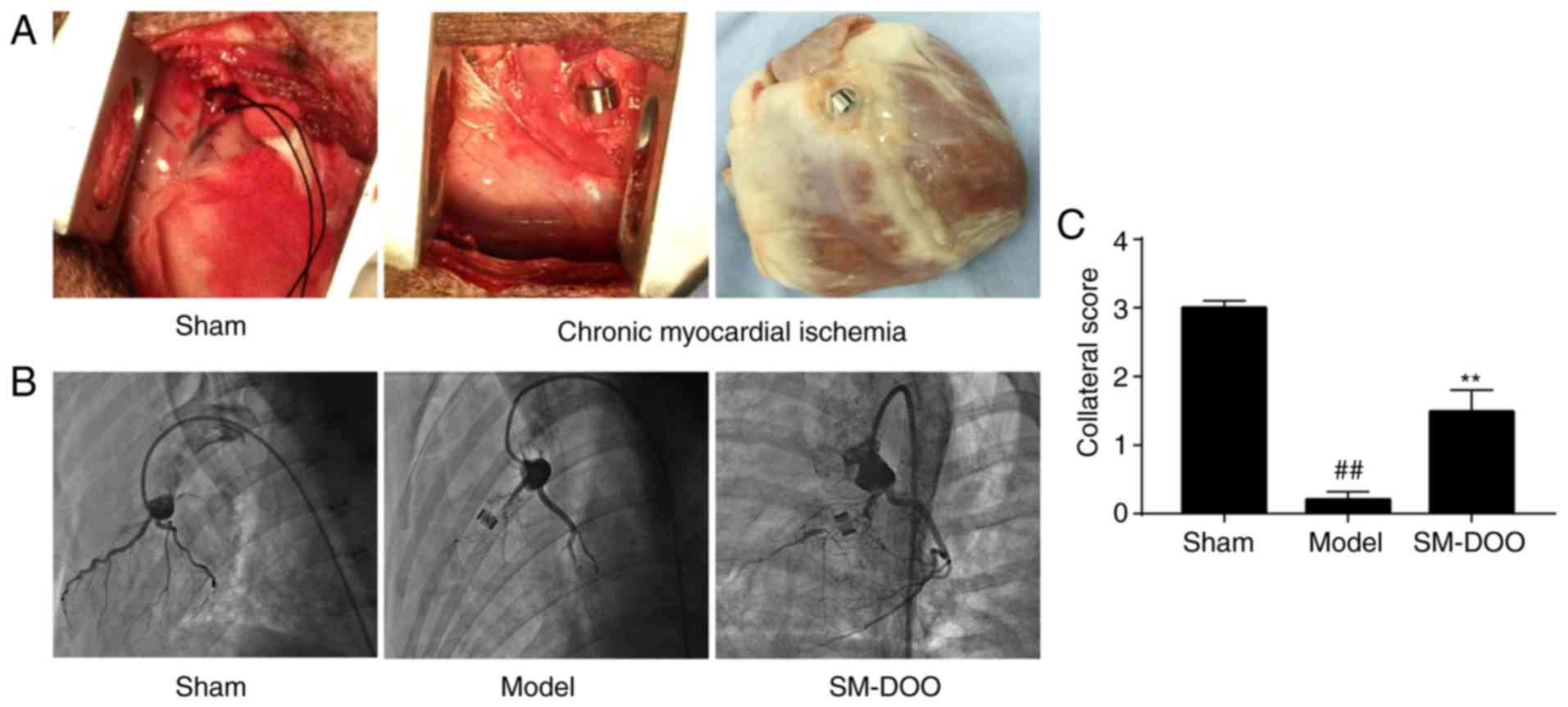
The ameroid constrictor was used to induce coronary
closure. Coronary angiography indicated that the rate of coronary
stenosis reached 98-100% 4 weeks after ameroid constrictor
implantation, indicating that chronic myocardial ischemia was
stably established. As shown in Fig.
2, coronary angiography revealed LAD stenosis with no evidence
of collateral vessel filling in the Model group (0.20±0.11);
however, collateral filling was observed in the SM-DOO group
(1.49±0.31). Collateral scores were significantly increased by the
administration of SM-DOO compared with the Model group
(P<0.01).
Effect of SM-DOO on myocardial injury
markers
As presented in Fig.
3, no differences were observed in CK-MB, LDH, ALT, AST, cTnI
and Myo between the 3 groups at week 2. CK-MB, LDH, ALT, AST, cTnI
and Myo levels in the Model group were higher compared with the
Sham group at weeks 6 and 8. In the Model group, at week 8, the
expression of myocardial injury markers was higher compared with at
week 6. Conversely, CK-MB, LDH, ALT, AST, cTnI and Myo were
significantly decreased in the SM-DOO group compared with the Model
group (P<0.05 or P<0.01), demonstrating that SM-DOO
ameliorated injury in chronic myocardial ischemia.
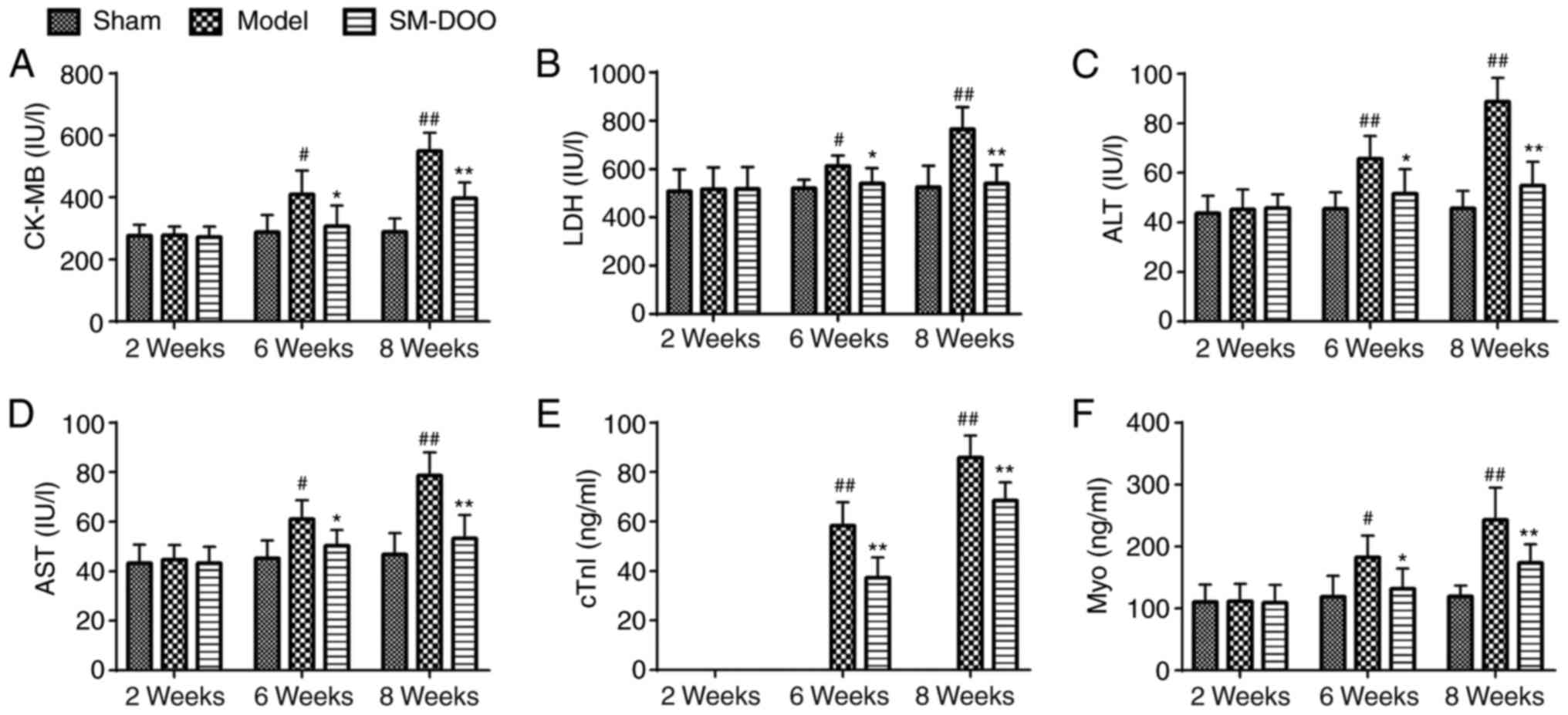 | Figure 3Effects of SM-DOO on myocardial
injury markers at weeks 2, 6 and 8 in pigs with chronic myocardial
ischemia, including (A) CK-MB, (B) LDH, (C) ALT, (D) AST, (E) cTnI
and (F) Myo. All values are presented as the mean ± standard
deviation. #P<0.05 and ##P<0.01 vs.
Sham group; *P<0.05 and **P<0.01 vs.
Model group. SM, Radix Salvia miltiorrhiza; DOO, Lignum
Dalbergiae odoriferae volatile oil; CK-MB, Pig creatine
kinase-MB; LDH, lactate dehydrogenase; ALT, alanine
aminotransferase; AST, aspartate aminotransferase; cTnI, cardiac
troponin I; Myo, myoglobin. |
Effect of SM-DOO on myocardial oxygen
consumption
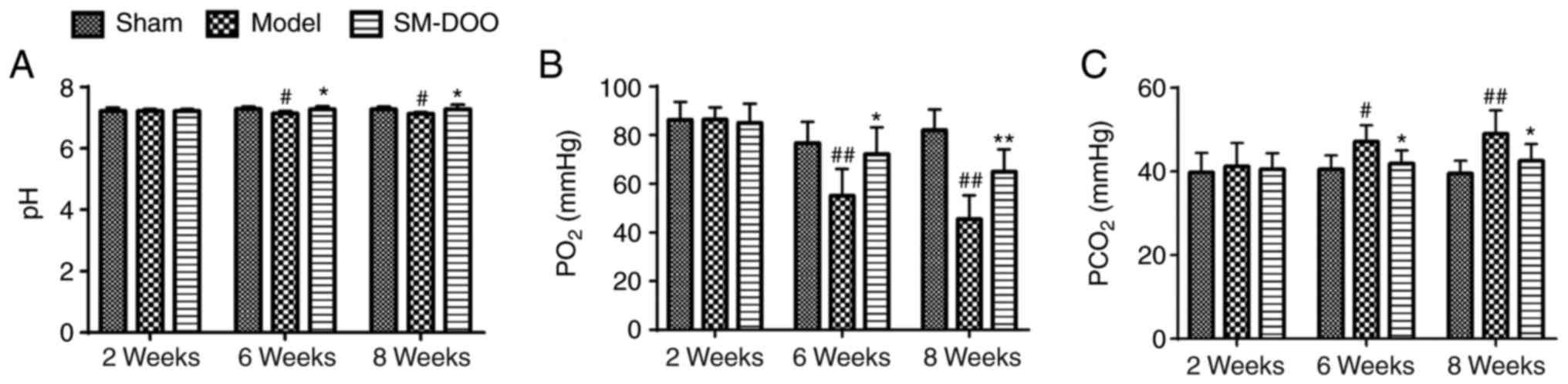
To investigate whether the cardioprotective effects
of SM-DOO were mediated by affecting myocardial oxygen consumption,
blood gas was quantified. As presented in Fig. 4, pH, PO2 and
PCO2 were the same in all 3 groups prior to the
induction of chronic myocardial ischemia. By weeks 6 and 8, the
arterial pH and PO2 were markedly lower, while the
PCO2 was higher in the Model group than that in the Sham
group (47.13±3.91 vs. 40.57±3.29 mmHg at week 6; 49.05±5.56 vs.
39.46±3.10 mmHg at week 8). Thus, compared with the Model group,
SM-DOO markedly ameliorated the effects on pH, PO2 and
PCO2 induced by myocardial ischemia.
Effects of SM-DOO on left ventricular
function
To assess the cardioprotective effects of SM-DOO,
left ventricular function was examined. Compared with the Sham
group, the mitral and apical levels in the Model group were
reduced, the papillary muscle was thinned, and the left ventricular
anterior wall moments were weakened (Table I). Additionally, in the Model
group, the echocardiography parameters of LVEDd, LVEDs, EDV and ESV
were significantly increased, while EF and FS were markedly reduced
(P<0.01 or P<0.05). The results indicated that the left
ventricular function in the Model group was markedly altered.
Conversely, the effects on the left ventricular anterior wall
thickness and moments were ameliorated in the SM-DOO group; the
levels of LVEDd, LVEDs, EDV and ESV were significantly reduced,
whereas EF and FS were increased following treatment with SM-DOO
(62.5±4.848% for EF, P<0.05; 44.5±8.526% for FS; P<0.01;
Fig. 5).
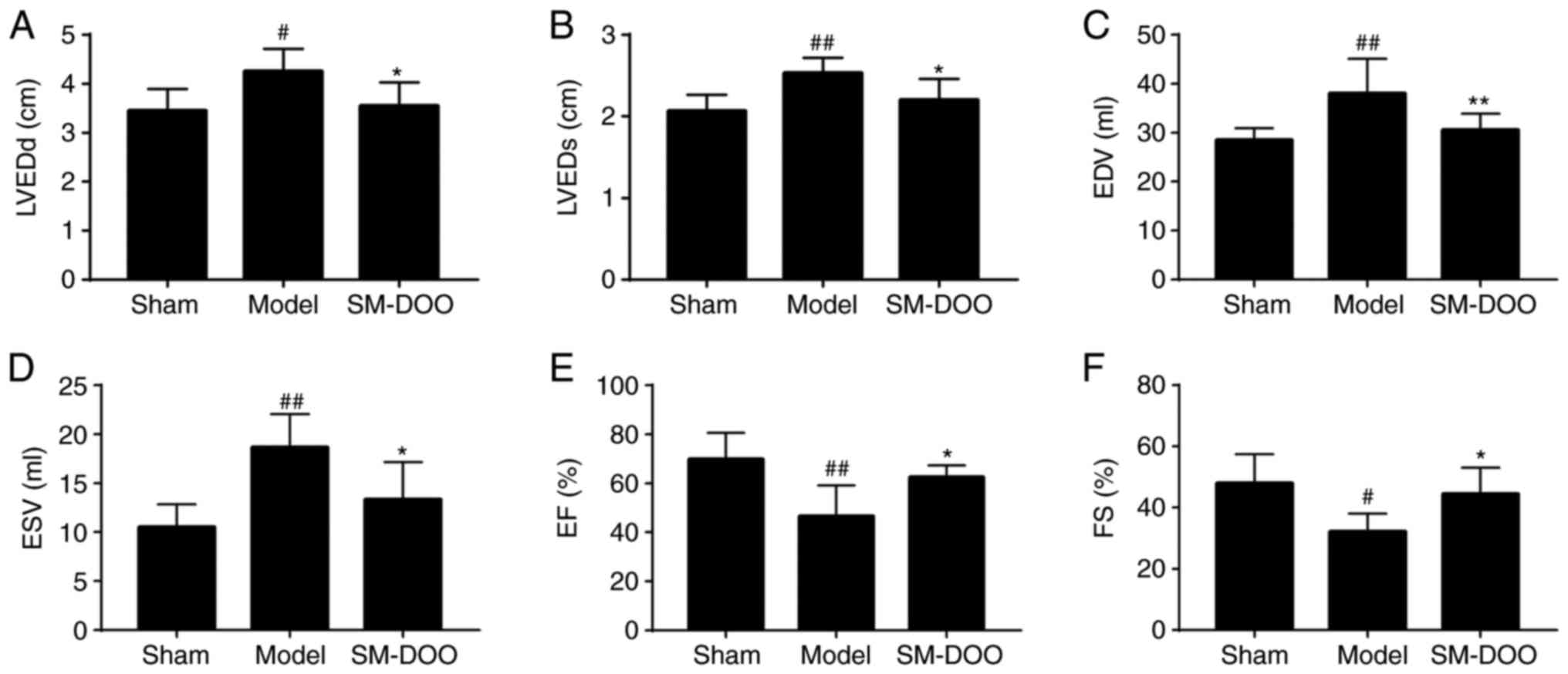 | Figure 5Effects of SM-DOO on left ventricular
function after chronic myocardial ischemia, including (A) LVEDd,
(B) LVEDs, (C) EDV, (D) ESV, (E) EF and (F) FS. All values are
presented as the mean ± standard deviation. #P<0.05
and ##P<0.01 vs. Sham group; *P<0.05
and **P<0.01 vs. Model group. LVEDd, left ventricular
end-diastolic diameter; LVEDs, left ventricular end-systolic
diameter; EDV, end-diastolic volume; ESV, end-systolic volume; EF,
ejection fraction; FS, fractional shortening. |
 | Table IMovement of the left ventricular
anterior wall at the mitral level, papillary muscle level and
apical level. |
Table I
Movement of the left ventricular
anterior wall at the mitral level, papillary muscle level and
apical level.
| Group | Mitral level
| Papillary muscle
level
| Apical level
|
|---|
| End-systolic | End-diastolic | End-systolic | End-diastolic | End-systolic | End-diastolic |
|---|
| Sham | 1.067±0.121 | 0.773±0.103 | 1.100±0.141 | 0.750±0.084 | 1.100±0.126 | 0.700±0.063 |
| Model | 0.800±0.063b | 0.550±0.055b | 0.850±0.138a | 0.583±0.075b | 0.767±0.103b | 0.533±0.052b |
| SM-DOO | 0.950±0.105c | 0.683±0.075c | 1.067±0.105c | 0.717±0.075c | 0.950±0.085c | 0.667±0.103c |
Effects of SM-DOO on hemodynamic
factors
As shown in Fig.
6, the hemodynamic parameters indicated that the left
ventricular function of the Model group was significantly decreased
compared with the Sham group. In the SM-DOO group, HR, LVEDP and
−dp/dtmax were markedly reduced (P<0.05 or 0.01),
whereas MAP, LVSP and +dp/dtmax were significantly
increased, compared with the Model group (102.176±22.203 vs.
67.079±16.378 mmHg for MAP; 115.522±21.528 vs. 83.206±9.189 mmHg
for LVSP; and 2,017.917±548.228 vs. 1,244.587±284.314 mmHg/sec for
+dp/dtmax; P<0.05).
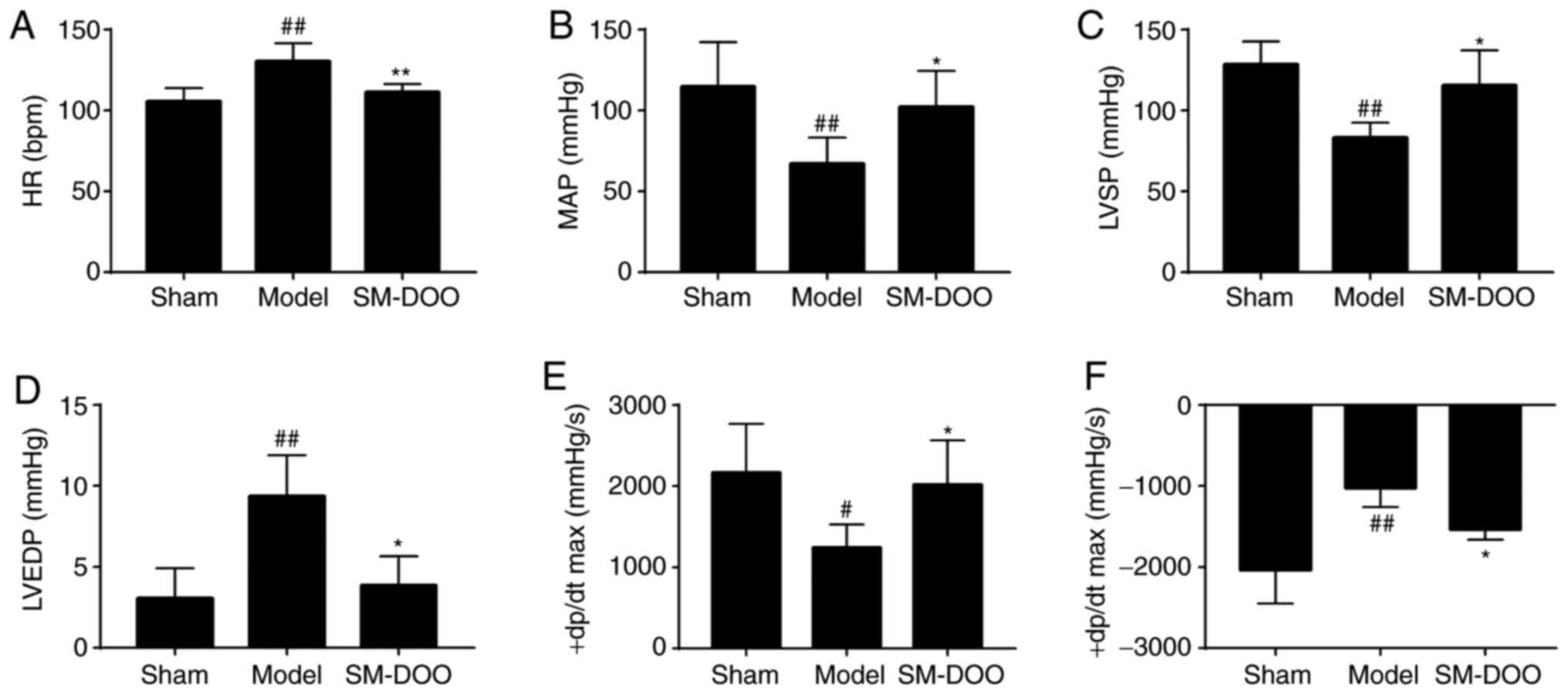 | Figure 6Effects of SM-DOO on hemodynamics.
The (A) HR, (B) MAP, (C) LVSP, (D) LVEDP, (E) +dp/dtmax
and (F) −dp/dtmax levels in each group were determined.
All values are presented as the mean ± SD. #P<0.05
and ##P<0.01 vs. Sham group, *P<0.05
and **P<0.01 vs. Model group. SM, Radix Salvia
miltiorrhiza; DOO, Lignum Dalbergia odorifera volatile
oil; HR, heart rate; MAP, mean arterial blood pressure; LVSP, left
ventricular systolic pressure; LVEDP, left ventricular
end-diastolic pressure; +dp/dtmax, left ventricular
maximum upstroke velocity; −dp/dtmax, left ventricular
maximum descent velocity. |
Effects of SM-DOO on myocardial
damage
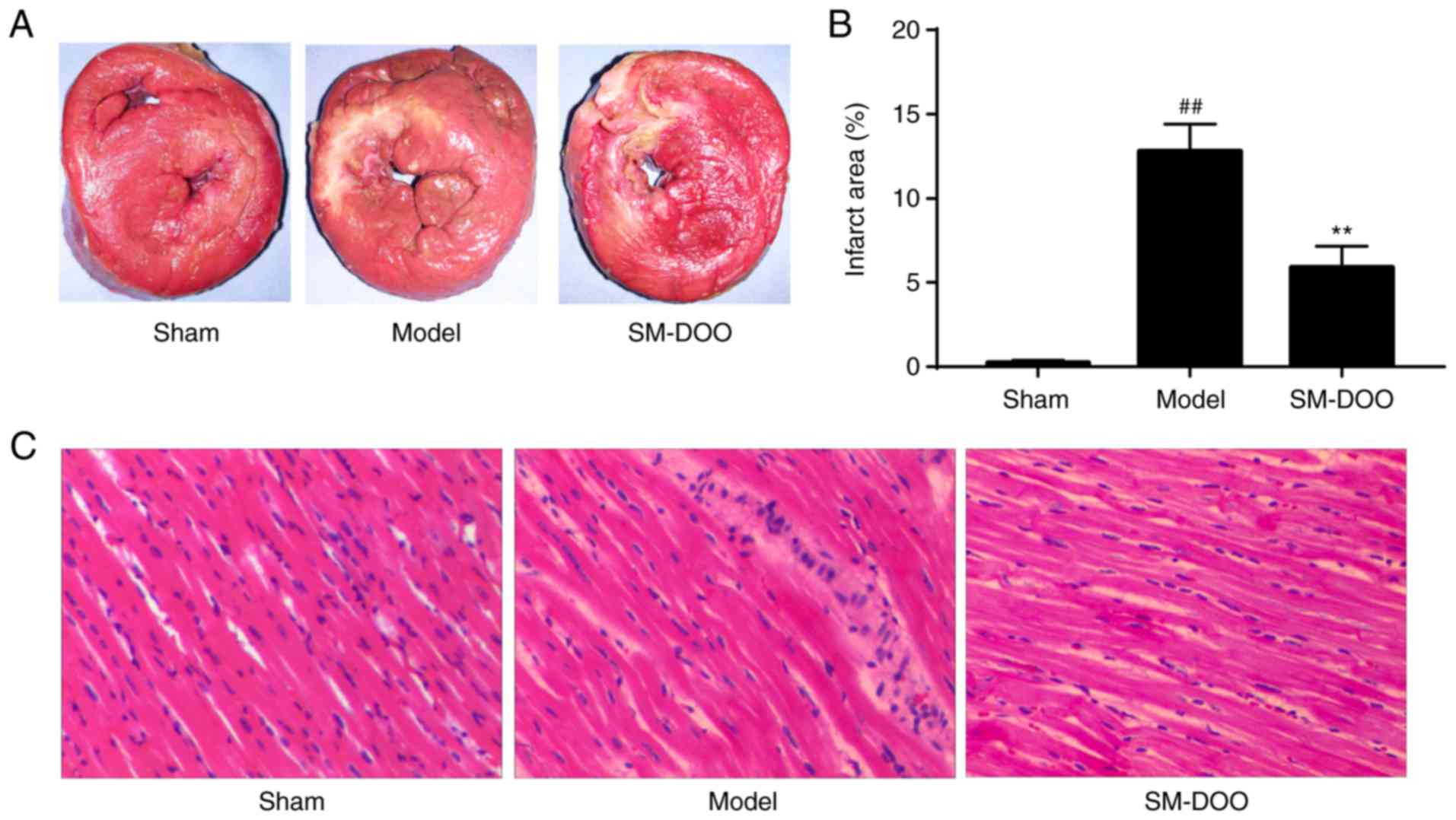
After the pigs were sacrificed, hearts were
collected for morphometric and histopathological analysis. Cardiac
sections were stained with TTC to compare the infarct size between
the 3 groups. As shown in Fig.
7A, the mean infarct size in the Model group was larger than
that in the SM-DOO group. The infarct size was significantly
decreased in the SM-DOO group (5.91±1.25%) compared with the Model
group (12.93±1.68%; P<0.01; Fig.
7B). Thus, SM-DOO treatment reduced the myocardial infarct size
after chronic myocardial ischemia.
As presented in Fig.
7C, the myocardium was H&E stained for histological
examination. Myocardial tissues in the Sham group exhibited no
abnormalities. As expected, chronic myocardial ischemia induced
evident injury to the myocardial structure, including chronic
inflammatory cells, edema in the myocardial fibers and ruptured
myocardial fibers in the Model group. Myocardial alterations
following chronic myocardial ischemia, in particular, disruption to
the myocardial fibers, were significantly ameliorated by
SM-DOO.
Effects of SM-DOO on myocardial apoptosis
and Bax and Bcl-2 expression
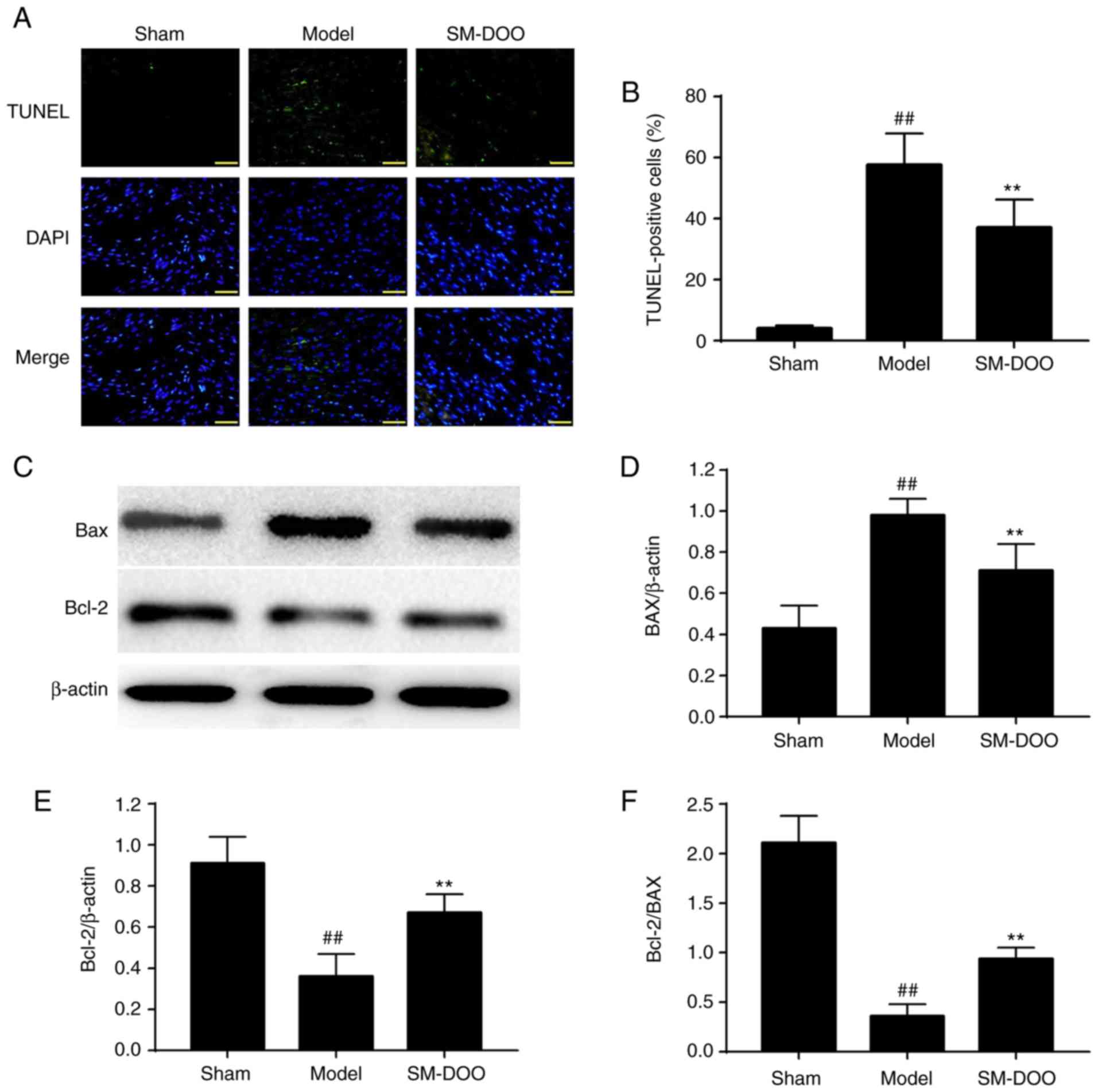
As shown in Fig.
8A, more apoptotic cells were observed in the Model group
compared with the Sham group. The percentage of TUNEL-positive
cells was significantly lower in the SM-DOO group (19.78±2.51%)
compared with the Model group (28.20±5.33%), as shown in Fig. 8B (P<0.01). To further examine
the potential mechanisms of the anti-apoptotic effect of SM-DOO,
the expression of Bax and Bcl-2 was determined. As shown in
Fig. 8C, D and E, the expression
of Bax was significantly increased and Bcl-2 was significantly
decreased in the Model group. In addition, the Bcl-2/Bax ratio was
significantly decreased in the Model group (Fig. 8F; P<0.01). Thus, treatment with
SM-DOO ameliorated the effects of chronic myocardial ischemia on
apoptosis.
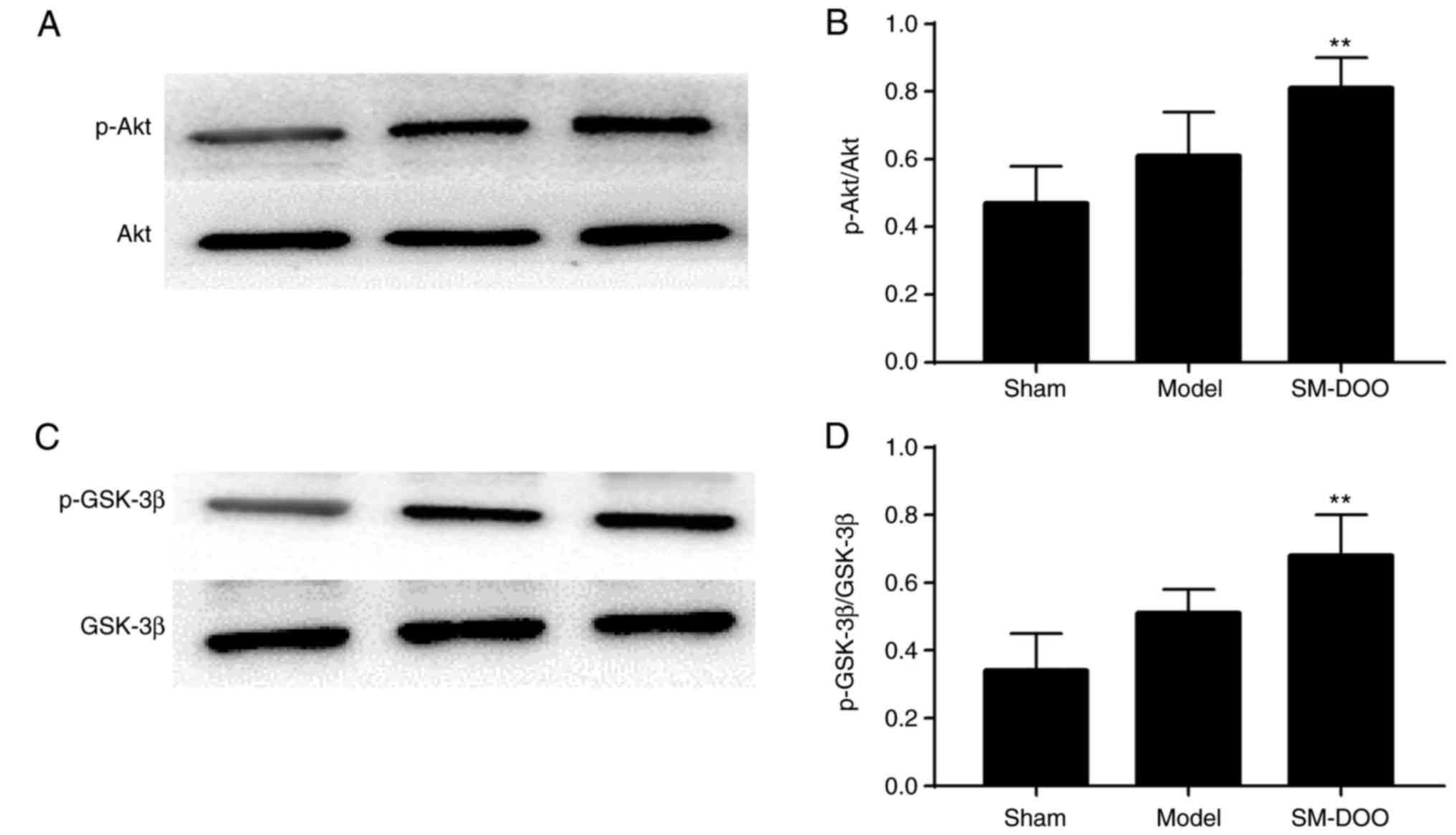
Effect of SM-DOO on Akt and GSK-3β
activation
To investigate the signaling pathways involved in
the cardioprotective effects of SM-DOO, the expression of Akt,
p-Akt, GSK-3β and p-GSK-3β was determined. As shown in Fig. 9, compared with the Sham group, the
expression of p-Akt and p-GSK-3β was slightly increased, while Akt
and GSK-3β levels were not altered in the Model group. Compared
with the Model group, the SM-DOO group had significantly higher
levels of p-Akt/Akt and p-GSK-3β/ GSK-3β (P<0.01), indicating
that SM-DOO administration markedly increased p-Akt and p-GSK-3β
levels.
Detection of SM and DOO components by
chromatography
By comparing the retention times of mixed standard
solutions with SM (Fig. 10A), 8
components were identified as danshensu, rosmarinic acid,
salvianolic acid B, salvianolic acid A, tanshinone IIA
silate sodium, dihydrotanshinone I, cryptotanshinone and tanshinone
IIA by chromatography (Fig. 10B). The main components of SM
were salvianolic acid B (18.67%), crypto-tanshinone (11.83%) and
tanshinone IIA (10.55%). A total of 9 chemical
components of DOO were detected by GC-MS and identified by NIST
Database retrieval, as shown in Table II. The major components of DOO
were nerolidol (22.52%), caryophyllene oxide (12.70%), α-santalol
(9.01%) and β-farnesene (5.16%). The total ion current (TIC) of DOO
is given in Fig. 10C.
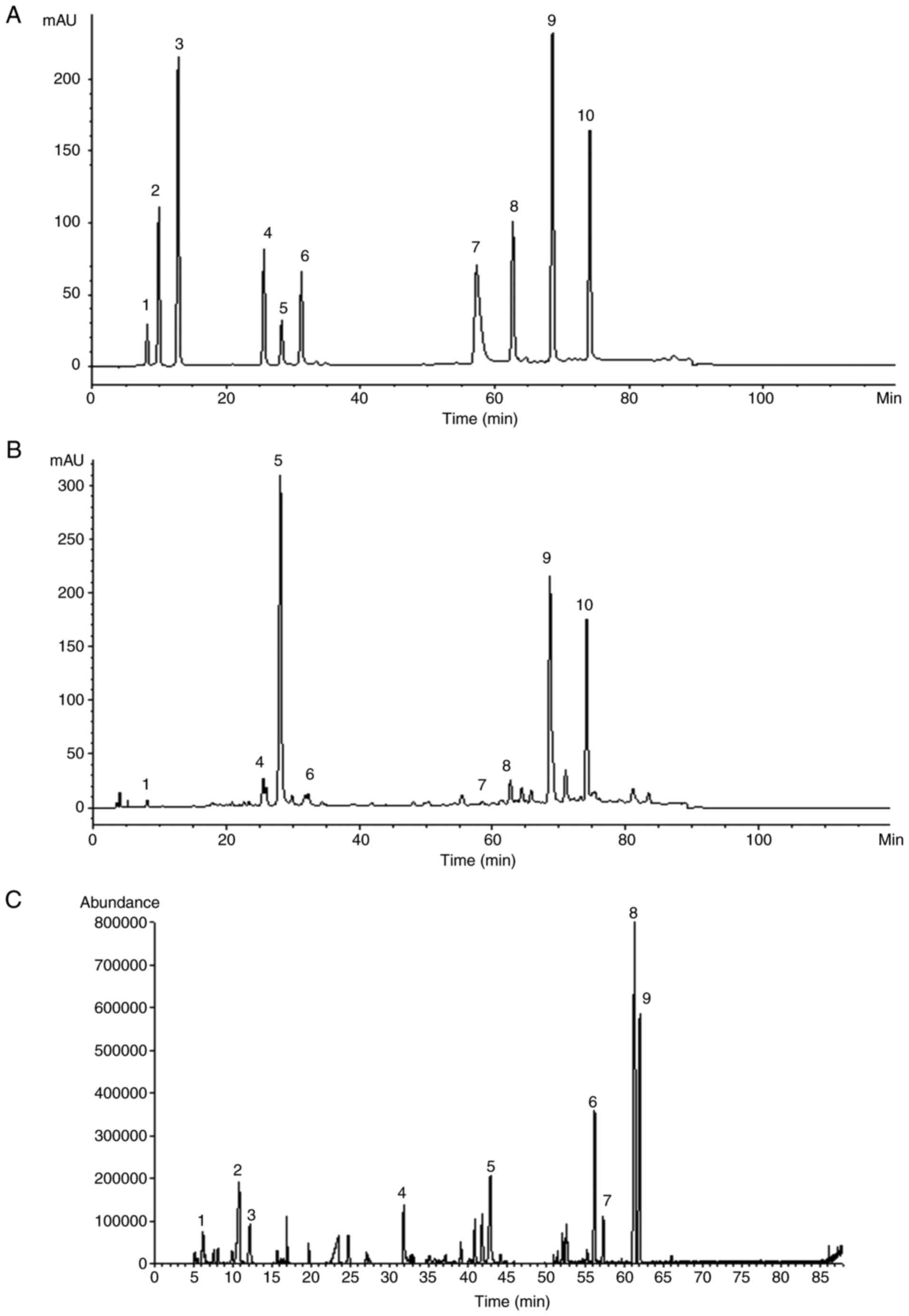 | Figure 10Representative chromatograms of the
identified components in (A) mixed standard solutions of SM and (B)
the SM extract, including 1. danshensu, 2. protocatechuic acid, 3.
protocatechuic aldehyde, 4. rosmarinic acid, 5. salvianolic acid B,
6. salvianolic acid A, 7. tanshinone IIA silate sodium, 8.
dihydrotanshinone I, 9. cryptotanshinone and 10. tanshinone
IIA. (C) Total ion chromatogram of DOO, as determined by
gas chromatography coupled with mass spectrometry. SM, Radix
Salvia miltiorrhiza; DOO, Lignum Dalbergia odorifera
volatile oil. |
 | Table IIComponents of Lignum Dalbergia
odorifera volatile oil as determined by gas chromatography
coupled with mass spectrometry. |
Table II
Components of Lignum Dalbergia
odorifera volatile oil as determined by gas chromatography
coupled with mass spectrometry.
| No. | Compound name | Fomula | Retention time
(min) | Relative mass
fraction (%) |
|---|
| 1 | Pinene |
C10H16 | 6.216 | 1.89 |
| 2 | Terpinolene |
C10H16 | 10.841 | 4.71 |
| 3 | Eucalyptol |
C10H18O | 12.216 | 2.38 |
| 4 | Eugenol |
C10H12O2 | 31.883 | 3.49 |
| 5 | β-Farnesene C | 15H24 | 42.945 | 5.16 |
| 6 | α-santalol C | 15H24O | 56.260 | 9.01 |
| 7 | α-Farnesene C | 15H24 | 57.368 | 2.63 |
| 8 | Nerolidol |
C15H26O | 61.348 | 22.52 |
| 9 | Caryophyllene
oxide |
C15H24O | 62.001 | 12.70 |
Discussion
Myocardial ischemia has become one of the most
common cardiovascular diseases, and it is difficult to treat in the
clinic. The beneficial effects of SM-DOO in the prevention and
treatment of heart disease have been demonstrated. However, little
has been reported regarding the potential cardioprotective effects
of SM-DOO in chronic myocardial ischemia. To address this problem,
a clinically relevant animal model was used in the present study to
evaluate the cardioprotective effects of SM-DOO in chronic
myocardial ischemia.
Small animal models have been extensively used in
cardiovascular research (19-21). However, they bear only a partial
resemblance to humans, which may not translate to clinical trials
(22). Pig models are widely used
to research cardiovascular disease because of the similarities
between pig and human hearts, such as cardiac anatomy and function,
hemodynamics, coronary circulation, drug dosing, pharmacokinetics
and a lack of preexisting collateral circulation (23). An ameroid constrictor is a
stainless steel jacket with a casein bar in its central lumen.
Dehydrated casein has a tendency to absorb fluid and swell, thus
gradually leading to the chronic myocardial ischemia by obstructing
the coronary artery (24-27). In the present study, an X-ray
coronary angiography demonstrated that the chronic myocardial
ischemia model was stably established.
CK-MB, LDH, Myo and cTnI levels are considered to be
important indicators of myocardial damage, and are significantly
increased by blockage of the LAD (28-32). In addition, AST and ALT have
previously been used to diagnose coronary heart disease (33,34). The elimination and release of
myocardial injury markers occurred at different times, suggesting
that the combined analysis of myocardial injury markers may provide
more precise information to influence therapeutic decisions
(35). Thus, sensitive myocardial
injury markers, including CK-MB, LDH, ALT, AST, cTnI and Myo, were
measured to determine whether SM-DOO alleviated the degree of
myocardial ischemia. As expected, SM-DOO significantly reduced
changes in these markers, demonstrating an amelioration of
myocardial injury. Furthermore, the echocardiographic (LVEDd,
LVEDs, EDV, ESV, EF and FS) and hemodynamic (MAP, HR, LVSP, LVEDP,
+dp/dtmax and −dp/dtmax) parameters suggested
that SM-DOO had a beneficial effect on preventing the impairment of
cardiac function. In addition, LAD occlusion leads to myocardial
injury and metabolic acidosis, decreasing the levels of
PO2 and increasing PCO2 (29,36). In the present study, SM-DOO
significantly prevented these changes, ameliorating myocardial
oxygen consumption. Severe myocardial ischemia is associated with
microstructural abnormalities in the myocardium (37). Pre-treatment with SM-DOO decreased
the infarct size and reduced the extent of myocardial damage,
supporting that conclusion that SM-DOO provided cardioprotective
effects.
The results of the present study have determined
that SM-DOO has a cardioprotective effect against chronic
myocardial ischemia. Next, the potential mechanisms of these
effects were explored. Apoptosis plays an important role in cardiac
injury and has become a focus of research (38). The expression of several
apoptosis-related genes is altered in ischemic tissue, including
Bax and Bcl-2, which play important roles in apoptosis (39). The Bcl-2 family members are key
regulators of physiological and pathological apoptosis, including
cell death promoters such as Bax and Bcl-2 associated agonist of
cell death, and cell death inhibitors such as Bcl-2, Bcl-X and
Mcl-1 (40). Changes in the
Bcl-2/Bax ratio leads to the induction of apoptotic cell death
(41). In the present study, the
anti-apoptotic effects of SM-DOO may be mediated by inhibiting the
upregulation of Bax and downregulation of Bcl-2. This finding is
consistent with the results of the TUNEL assay. These results
suggest that SM-DOO may exert its cardioprotective effect against
myocardial injury following chronic myocardial ischemia by
preventing apoptosis.
The PI3K/Akt pathway is particularly important in
mediating myocardial cell survival. Studies have shown that
activation of the PI3K/Akt signaling pathway is essential for
anti-apoptotic and cardioprotective effects (42,43). GSK-3 is a serine/threonine kinase
with versatile cellular functions in the heart, including in gene
expression, hypertrophy and apoptosis (44). GSK-3β is active in cardiomyocytes
unstimulated by ischemia and ischemia/reperfusion, and sensitizes
cells to death-promoting insults, which may be an underlying
mechanism of cardioprotection (45). Akt phosphorylates and subsequently
inactivates GSK-3β, which contributes to the attenuation of
myocardial injury (46). To
investigate the involvement of the PI3K/Akt signaling pathway on
the cardio-protective effects of SM-DOO treatment, the expression
of Akt and GSK-3β was determined using western blotting. As shown
in the results, pretreatment with SM-DOO significantly increased
the relative p-Akt and p-GSK-3β levels compared with the Model
group. These findings suggest that the PI3K/Akt/GSK-3β signaling
pathway may be involved in the cardioprotective effects of SM-DOO
in a chronic myocardial ischemia model. However, further studies
utilizing an inhibitor of PI3K/Akt are required to validate the
involvement of this pathway.
The chemical composition of SM includes
water-soluble and lipid-soluble components (47,48). Using HPLC analysis, 8 components
of SM were identified by comparing its retention time with the
standards. The main components of SM were salvianolic acid B,
cryptotanshinone and tanshinone IIA. DOO was also
analyzed using the established GC-MS method. The majority of the
components, including pinene, terpinolene, eucalyptol, eugenol,
β-farnesene, α-santalol, α-farnesene, nerolidol and caryophyllene
oxide, were identified by performing a similarity match with the
NIST Database. Studies have demonstrated that various chemical
components of SM, such as danshensu, salvianolic acid B,
salvianolic acid A, rosmarinic acid and tanshinone IIA, have
anti-apoptotic activities (49-52). In addition, recent research
indicates that tanshinone IIA, dihydrotanshinone I, danshensu,
salvianolic acid B and salvianolic acid A play a protective role by
regulating GSK-3β (53-56). However, there are few studies
regarding whether the chemical components of DOO achieve a
protective effect by regulating GSK-3β. We plan to explore the
effects of active chemical constituents of SM-DOO against chronic
myocardial ischemia in the future.
In conclusion, pretreatment with SM-DOO may
ameliorate cardiac injury resulting from chronic myocardial
ischemia. Myocardial injury markers (CK-MB, LDH, ALT, AST, cTnI and
Myo), markers of myocardial oxygen consumption (pH, PO2
and PCO2), metrics of left ventricular function (LVEDd,
LVEDs, EDV, ESV, EF, FS, MAP, HR, LVSP, LVEDP, +dp/dtmax
and −dp/dtmax) and indicators of myocardial tissue
damage (TTC, H&E, TUNEL and western blotting) revealed the
effects of SM-DOO against chronic myocardial ischemia. Furthermore,
the cardioprotective effects of SM-DOO may be partly mediated via
activation of the PI3K/Akt/GSK-3β signaling pathway. The results of
the present study may help to improve our understanding of the
molecular mechanisms underlying the cardioprotective effects of
SM-DOO, and provide a basis for the use of SM-DOO as an effective
drug for the prophylaxis and treatment of chronic myocardial
ischemia.
Funding
The present study was supported by the National
Natural Science Foundation of China (grant nos. 81470174 and
31771265).
Availability of data and materials
All data generated or analyzed during this study are
included in this published article.
Authors' contributions
The present study was performed with collaboration
between all authors. MX, YY and AW defined the research theme and
revised the manuscript critically. RL, JD and FM designed the
methods and experiments, performed the laboratory experiments and
wrote the paper. HB, MNZ, MZ and YL collected and analyzed the
data, and interpreted the results. All authors have read and
approved the final manuscript.
Ethics approval and consent to
participate
The Animal Welfare and Ethics Committee of Fuwai
Hospital, Chinese Academy of Medical Sciences approved all
experiments [approval no. 0072-1-27-HX (F)].
Competing interests
The authors declare that they have no competing
interests.
Acknowledgments
The authors would like to thank Beijing Key
Laboratory of Pre-clinical Research and Evaluation for
Cardiovascular Implant Materials (Fuwai Hospital, Chinese Academy
of Medical Sciences) for providing the experimental animals and
platform.
References
|
1
|
Shimokawa H and Yasuda S: Myocardial
ischemia: Current concepts and future perspectives. J Cardiol.
52:67–78. 2008. View Article : Google Scholar : PubMed/NCBI
|
|
2
|
Lv Y, Liu X, Yan S, Liang X, Yang Y, Dai W
and Zhang W: Metabolomic study of myocardial ischemia and
intervention effects of Compound Danshen Tablets in rats using
ultra-performance liquid chromatography/quadrupole time-of-flight
mass spectrometry. J Pharm Biomed Anal. 52:129–135. 2010.
View Article : Google Scholar : PubMed/NCBI
|
|
3
|
Xu T, Wu X, Chen Q, Zhu S, Liu Y, Pan D,
Chen X and Li D: The anti-apoptotic and cardioprotective effects of
salvianolic acid a on rat cardiomyocytes following
ischemia/reperfusion by DUSP-mediated regulation of the ERK1/2/JNK
pathway. PLoS One. 9:e1022922014. View Article : Google Scholar :
|
|
4
|
JianXin C, Xue X, ZhongFeng L, Kuo G,
FeiLong Z, ZhiHong L, Xian W and HongCai S: Qishen Yiqi Drop Pill
improves cardiac function after myocardial ischemia. Sci Rep.
6:243832016. View Article : Google Scholar : PubMed/NCBI
|
|
5
|
Zhang Y, Shi P, Yao H, Shao Q and Fan X:
Metabolite profiling and pharmacokinetics of herbal compounds
following oral administration of a cardiovascular multi-herb
medicine (Qishen yiqi pills) in rats. Curr Drug Metab. 13:510–523.
2012. View Article : Google Scholar : PubMed/NCBI
|
|
6
|
Wu SD, Wang J, Chen SC, Xu JB, Zheng Q,
Yan YF, Wen TM and Tang YR: Effect of Xiangdan Injection on mRNA
expression of endothelial vasoactive factors of patients with
coronary heart disease and blood stasis. Zhong Xi Yi Jie He Xue
Bao. 2:94–96. 2004.In Chinese. View Article : Google Scholar : PubMed/NCBI
|
|
7
|
Wang SX, Luo K, Liang J, Fan F, Li H,
Zheng JB and Zheng XH: Metabolomics study on the synergistic
interaction between Salvia miltiorrhiza and Lignum dalbergiae
odoriferae used as 'Jun-Shi' herbs in a S. miltiorrhiza recipe. Med
Chem Res. 20:16–22. 2011. View Article : Google Scholar
|
|
8
|
Sugiyama A, Zhu BM, Takahara A, Satoh Y
and Hashimoto K: Cardiac effects of salvia miltiorrhiza/dalbergia
odorifer a mixture, an intravenously applicable Chinese medicine
widely used for patients with ischemic heart disease in China. Circ
J. 66:182–184. 2002. View Article : Google Scholar : PubMed/NCBI
|
|
9
|
Mu F, Duan J, Bian H, Zhai X, Shang P, Lin
R, Zhao M, Hu D, Yin Y, Wen A, et al: Metabonomic strategy for the
evaluation of Chinese medicine salvia miltiorrhiza and dalbergia
odorifera interfering with myocardial ischemia/reperfusion injury
in rats. Rejuvenation Res. 20:263–277. 2017. View Article : Google Scholar : PubMed/NCBI
|
|
10
|
Zheng X, Zhao X, Wang S, Luo K, Wei Y and
Zheng J: Co-administration of Dalbergia odorifera increased
bioavailability of Salvia miltiorrhiza e in rabbits. Am J Chin Med.
35:831–840. 2007. View Article : Google Scholar
|
|
11
|
Zhou L, Zuo Z and Chow MS: Danshen: An
overview of its chemistry, pharmacology, pharmacokinetics, and
clinical use. J Clin Pharmacol. 45:1345–1359. 2005. View Article : Google Scholar : PubMed/NCBI
|
|
12
|
Liu R, Ye M, Guo H, Bi K and Guo DA:
Liquid chromatography/electrospray ionization mass spectrometry for
the characterization of twenty-three flavonoids in the extract of
Dalbergia odorifera. Rapid Commun Mass Spectrom. 19:1557–1565.
2005. View
Article : Google Scholar : PubMed/NCBI
|
|
13
|
Tu J and Song K: Curative effect
observation on Xiangdan injection in the treatment of coronary
artery disease. Chin Med Pharm. 22:110–111. 2011.In Chinese.
|
|
14
|
Qin F and Huang X: Guanxin II for the
management of coronary heart disease. Chin J Integr Med.
15:472–476. 2009. View Article : Google Scholar
|
|
15
|
Mu F, Duan J, Bian H, Yin Y, Zhu Y, Wei G,
Guan Y, Wang Y, Guo C, Wen A, et al: Cardioprotective effects and
mechanism of Radix Salviae miltiorrhizae and Lignum Dalbergiae
odoriferae on rat myocardial ischemia/reperfusion injury. Mol Med
Rep. 16:1759–1770. 2017. View Article : Google Scholar : PubMed/NCBI
|
|
16
|
Krishnamoorthy K and Subramaniam P:
Phytochemical profiling of leaf, stem, and tuber parts of Solena
amplexicaulis (Lam.) Gandhi using GC-MS. Int Sch Res Notices.
2014:5674092014.PubMed/NCBI
|
|
17
|
Huang JH, Huang XZ, Chen ZY, Zheng QS and
Sun RY: Dose conversion among different animals and healthy
volunteers in pharmacological study. Chin J Clin Pharmacol Therap.
9:1069–1072. 2004.
|
|
18
|
Henriques JP, Zijlstra F, van 't Hof AW,
de Boer MJ, Dambrink JH, Gosselink M, Hoorntje JC and Suryapranata
H: Angiographic assessment of reperfusion in acute myocardial
infarction by myocardial blush grade. Circulation. 107:2115–2119.
2003. View Article : Google Scholar : PubMed/NCBI
|
|
19
|
Liu Z, Chen JM, Huang H, Kuznicki M, Zheng
S, Sun W, Quan N, Wang L, Yang H, Guo HM, et al: The protective
effect of trimetazidine on myocardial ischemia/reperfusion injury
through activating AMPK and ERK signaling pathway. Metabolism.
65:122–130. 2016. View Article : Google Scholar : PubMed/NCBI
|
|
20
|
Saito N: Letter by Saito regarding
article, 'Collateral donor artery physiology and the influence of a
chronic total occlusion on fractional flow reserve'. Circ
Cardiovasc Interv. 8:e0027942015. View Article : Google Scholar
|
|
21
|
Zhao HW, Qin F, Liu YX, Huang X and Ren P:
Antiapoptotic mechanisms of Chinese medicine formula,
Guan-Xin-Er-Hao, in the rat ischemic heart. Tohoku J Exp Med.
216:309–316. 2008. View Article : Google Scholar
|
|
22
|
Seok J, Warren HS, Cuenca AG, Mindrinos
MN, Baker HV, Xu W, Richards DR, McDonald-Smith GP, Gao H, Hennessy
L, et al: Genomic responses in mouse models poorly mimic human
inflammatory diseases. Proc Natl Acad Sci USA. 110:3507–3512. 2013.
View Article : Google Scholar : PubMed/NCBI
|
|
23
|
Elmadhun NY, Sabe AA, Robich MP, Chu LM,
Lassaletta AD and Sellke FW: The pig as a valuable model for
testing the effect of resveratrol to prevent cardiovascular
disease. Ann NY Acad Sci. 1290:130–135. 2013. View Article : Google Scholar : PubMed/NCBI
|
|
24
|
Ikonen TS, Pätilä T, Virtanen K, Lommi J,
Lappalainen K, Kankuri E, Krogerus L and Harjula A: Ligation of
ameroid-stenosed coronary artery leads to reproducible myocardial
infarction-a pilot study in a porcine model. J Surg Res.
142:195–201. 2007. View Article : Google Scholar : PubMed/NCBI
|
|
25
|
Caillaud D, Calderon J, Réant P, Lafitte
S, Dos Santos P, Couffinhal T, Roques X and Barandon L:
Echocardiographic analysis with a two-dimensional strain of chronic
myocardial ischemia induced with ameroid constrictor in the pig.
Interact Cardiovasc Thorac Surg. 10:689–693. 2010. View Article : Google Scholar : PubMed/NCBI
|
|
26
|
Tuzun E, Oliveira E, Narin C, Khalil H,
Jimenez-Quevedo P, Perin E and Silva G: Correlation of ischemic
area and coronary flow with ameroid size in a porcine model. J Surg
Res. 164:38–42. 2010. View Article : Google Scholar
|
|
27
|
von Degenfeld G, Raake P, Kupatt C,
Lebherz C, Hinkel R, Gildehaus FJ, Münzing W, Kranz A, Waltenberger
J, Simoes M, et al: Selective pressure-regulated retroinfusion of
fibroblast growth factor-2 into the coronary vein enhances regional
myocardial blood flow and function in pigs with chronic myocardial
ischemia. J Am Coll Cardiol. 42:1120–1128. 2003. View Article : Google Scholar : PubMed/NCBI
|
|
28
|
Eisenman A: Troponin assays for the
diagnosis of myocardial infarction and acute coronary syndrome:
Where do we stand. Expert Rev Cardiovasc Ther. 4:509–514. 2006.
View Article : Google Scholar : PubMed/NCBI
|
|
29
|
Li X, Shao D, Wang G, Jiang T, Wu H, Gu B,
Cao K, Zhang J, Qi L and Chen Y: Effects of different LAD-blocked
sites on the development of acute myocardial infarction and
malignant arrhythmia in a swine model. J Thorac Dis. 6:1271–1277.
2014.PubMed/NCBI
|
|
30
|
Tsaroucha A, Chondrogiannis C, Mani A and
Staikou C: Myocardial involvement during ischemia-induced acute
liver failure in the pig. J Invest Surg. 26:99–104. 2013.
View Article : Google Scholar : PubMed/NCBI
|
|
31
|
Arya DS, Bansal P, Ojha SK, Nandave M,
Mohanty I and Gupta SK: Pyruvate provides cardioprotection in the
experimental model of myocardial ischemic reperfusion injury. Life
Sci. 79:38–44. 2006. View Article : Google Scholar
|
|
32
|
Doganci S, Yildirim V, Bolcal C, Korkusuz
P, Gumusel B, Demirkilic U and Aydin A: Sodium nitrite and
cardioprotective effect in pig regional myocardial
ischemia-reperfusion injury model. Adv Clin Exp Med. 21:713–726.
2012.
|
|
33
|
Elizondo-Montemayor L, Ugalde-Casas PA,
Lam-Franco L, Bustamante-Careaga H, Serrano-González M, Gutiérrez
NG and Martínez U: Association of ALT and the metabolic syndrome
among Mexican children. Obes Res Clin Pract. 8:e79-e872014.
View Article : Google Scholar
|
|
34
|
Xu Q, Higgins T and Cembrowski GS:
Limiting the testing of AST: A diagnostically nonspecific enzyme.
Am J Clin Pathol. 144:423–426. 2015. View Article : Google Scholar : PubMed/NCBI
|
|
35
|
Solymoss BC, Bourassa MG, Fortier A and
Théroux P: Evaluation and risk stratification of acute coronary
syndromes using a low cut-off level of cardiac troponin T, combined
with CK-MB mass determination. Clin Biochem. 37:286–292. 2004.
View Article : Google Scholar : PubMed/NCBI
|
|
36
|
Zhang M, Dong W, Lu S, Yu Y, Liu H, Li G,
Qiang W, Wang L and Lou J: Study on blood-gas changes in the
coronary artery of myocardial ischemia reperfusion injury of
rabbit. J Naval Med College. 1:9–12. 1996.In Chinese.
|
|
37
|
Feng YJ, Chen C, Fallon JT, Lai T, Chen L,
Knibbs DR, Waters DD and Wu AH: Comparison of cardiac troponin I,
creatine kinase-MB, and myoglobin for detection of acute ischemic
myocardial injury in a swine model. Am J Clin Pathol. 110:70–77.
1998. View Article : Google Scholar : PubMed/NCBI
|
|
38
|
Ishihara Y and Shimamoto N: Sulfaphenazole
attenuates myocardial cell apoptosis accompanied with cardiac
ischemia-reperfusion by suppressing the expression of BimEL and
Noxa. J Pharmacol Sci. 119:251–259. 2012. View Article : Google Scholar : PubMed/NCBI
|
|
39
|
Qu D, Han J, Ren H, Yang W, Zhang X, Zheng
Q and Wang D: Cardioprotective effects of Astragalin against
myocardial ischemia/reperfusion injury in isolated rat heart. Oxid
Med Cell Longev. 2016:81946902016. View Article : Google Scholar : PubMed/NCBI
|
|
40
|
Pan H, Li D, Fang F, Chen D, Qi L, Zhang
R, Xu T and Sun H: Salvianolic acid A demonstrates cardioprotective
effects in rat hearts and cardiomyocytes after ischemia/reperfusion
injury. J Cardiovasc Pharmacolm. 58:535–542. 2011. View Article : Google Scholar
|
|
41
|
Zhang Q, Wang G, Yuan W, Wu J, Wang M and
Li C: The effects of phosphodiesterase-5 inhibitor sildenafil
against post-resuscitation myocardial and intestinal
microcirculatory dysfunction by attenuating apoptosis and
regulating microRNAs expression: Essential role of nitric oxide
syntheses signaling. J Transl Med. 13:1772015. View Article : Google Scholar : PubMed/NCBI
|
|
42
|
Wang ZG, Wang Y, Huang Y, Lu Q, Zheng L,
Hu D, Feng WK, Liu YL, Ji KT, Zhang HY, et al: bFGF regulates
autophagy and ubiquitinated protein accumulation induced by
myocardial ischemia/reperfusion via the activation of the
PI3K/Akt/mTOR pathway. Sci Rep. 5:92872015. View Article : Google Scholar : PubMed/NCBI
|
|
43
|
Liu S, Ai Q, Feng K, Li YB and Liu X: The
cardioprotective effect of dihydromyricetin prevents
ischemia-reperfusion-induced apoptosis in vivo and in vitro via the
PI3K/Akt and HIF-1α signaling pathways. Apoptosis. 21:1366–1385.
2016. View Article : Google Scholar : PubMed/NCBI
|
|
44
|
Zhai P, Sciarretta S, Galeotti J, Volpe M
and Sadoshima J: Differential roles of GSK-3β during myocardial
ischemia and ischemia_reperfusion. Circ Res. 109:502–511. 2011.
View Article : Google Scholar : PubMed/NCBI
|
|
45
|
Duan J, Guan Y, Mu F, Guo C, Zhang E, Yin
Y, Wei G, Zhu Y, Cui J, Cao J, et al: Protective effect of butin
against ischemia/reperfusion-induced myocardial injury in diabetic
mice: Involvement of the AMPK/GSK-3β/Nrf2 signaling pathway. Sci
Rep. 7:414912017. View Article : Google Scholar
|
|
46
|
Nagaoka K, Matoba T, Mao Y, Nakano Y,
Ikeda G, Egusa S, Tokutome M, Nagahama R, Nakano K, Sunagawa K, et
al: A new therapeutic modality for acute myocardial infarction:
Nanoparticle-mediated delivery of Pitavastatin induces
cardio-protection from ischemia-reperfusion injury via activation
of PI3K/Akt pathway and anti-inflammation in a rat model. PLoS One.
10:e01324512015. View Article : Google Scholar
|
|
47
|
Liu ZJ, Shi ZL, Tu C, Zhang HZ, Gao D, Li
CY, He Q, Li RS, Guo YM, Niu M, et al: An activity-calibrated
chemical standardization approach for quality evaluation of Salvia
miltiorrhiza Bge. RSC Adv. 7:5331–5339. 2017. View Article : Google Scholar
|
|
48
|
Zhou GJ, Wang W, Xie XM, Qin MJ, Kuai BK
and Zhou TS: Post-harvest induced production of salvianolic acids
and significant promotion of antioxidant properties in roots of
Salvia miltiorrhiza (Danshen). Molecules. 19:7207–7222. 2014.
View Article : Google Scholar : PubMed/NCBI
|
|
49
|
Fan G, Yu J, Asare PF, Wang L, Zhang H,
Zhang B, Zhu Y and Gao X: Danshensu alleviates cardiac
ischaemia/reperfusion injury by inhibiting autophagy and apoptosis
via activation of mTOR signalling. J Cell Mol Med. 20:1908–1919.
2016. View Article : Google Scholar : PubMed/NCBI
|
|
50
|
Jia LQ, Yang GL, Ren L, Chen WN, Feng JY,
Cao Y, Zhang L, Li XT and Lei P: Tanshinone IIA reduces apoptosis
induced by hydrogen peroxide in the human endothelium-derived
EA.hy926 cells. J Ethnopharmacol. 143:100–108. 2012. View Article : Google Scholar : PubMed/NCBI
|
|
51
|
Zhuang P, Zhang Y, Cui G, Bian Y, Zhang M,
Zhang J, Liu Y, Yang X, Isaiah AO, Lin Y, et al: Direct stimulation
of adult neural stem/progenitor cells in vitro and neurogenesis in
vivo by salvianolic acid B. PLoS One. 7:e356362012. View Article : Google Scholar : PubMed/NCBI
|
|
52
|
Li XL, Liu JX, Li P and Zheng YQ:
Protective effect of rosmarinic acid on hypoxia/reoxygenation
injury in cardiomyocytes. Zhongguo Zhong Yao Za Zhi. 39:1897–1901.
2014.In Chinese. PubMed/NCBI
|
|
53
|
Jung SH, Seol HJ, Jeon SJ, Son KH and Lee
JR: Insulin-sensitizing activities of tanshinones, diterpene
compounds of the root of Salvia miltiorrhiza Bunge. Phytomedicine.
16:327–335. 2009. View Article : Google Scholar : PubMed/NCBI
|
|
54
|
Guo C, Yin Y, Duan J, Zhu Y, Yan J, Wei G,
Guan Y, Wu X, Wang Y, Xi M and Wen A: Neuroprotective effect and
underlying mechanism of sodium danshensu [3-(3,4-dihydroxyphenyl)
lactic acid from Radix and Rhizoma Salviae miltiorrhizae = Danshen]
against cerebral ischemia and reperfusion injury in rats.
Phytomedicine. 22:283–289. 2015. View Article : Google Scholar : PubMed/NCBI
|
|
55
|
Gao Q, Hu X, Jiang XJ, Guo MJ, Ji H, Wang
Y and Fan YC: Cardiomyocyte-like cells differentiation from non
β-catenin expression mesenchymal stem cells. Cytotechnology.
66:575–584. 2014. View Article : Google Scholar : PubMed/NCBI
|
|
56
|
Li XL, Fan JP, Liu JX and Liang LN:
Salvianolic acid A protects neonatal cardiomyocytes against
hypoxia/reoxygenation-induced injury by preserving mitochondrial
function and activating Akt/GSK-3beta signals. Chin J Integr Med.
1–8. 2017.
|