Introduction
Biliary mucinous cystic neoplasms (BMCNs) are rare
tumors accounting for <5% of all cystic lesions of the
intrahepatic and extrahepatic biliary tree (1). BMCNs are strongly associated with
female sex and present in their fourth and fifth decade of life
(1). These mucus secreting or, less
commonly, serous epithelium cystic lesions have been also referred
to as ‘biliary cystadenoma’ and ‘biliary cystadenocarcinoma’
(2). In 2010, the World Health
Organization (WHO) categorized them into non-invasive BMCNs with
low-, intermediate-, or high-grade intraepithelial neoplasia and
BMCNs with an invasive component (2,3).
Although, up to 85% of BMCNs are intrahepatic, primary BMCNs of
extrahepatic biliary tract have also been described (4,5).
Surgical resection with negative margins is the treatment of
choice, and its extent is dictated by the localization of the
lesion, as such it may include hepatectomy or extended hepatectomy
with Roux-en-Y reconstruction or resection of extrahepatic biliary
tree, while regional lymphadenectomy is not widely recommended
(6,7).
We herein present a rare case of a primary
extrahepatic BMCN in a middle-aged female patient who presented
with mild jaundice and underwent pancreaticoduodenectomy as a
therapeutic strategy.
Case report
A 55-year-old female patient presented to our
department with a history of right upper quadrant (RUQ) pain
associated with jaundice and weight loss. She did not report any
signs or symptoms of acute cholangitis. Her physical examination
was notable for a mild pain on palpation in the RUQ and for a
remarkable scleral icterus. On auscultation, bowel sounds were
normal, with no sign of bowel obstruction. Laboratory evaluation
revealed hyperbilirubinemia, with a serum total bilirubin of 9.4
mg/dl, alkaline phosphatase (ALP) of 250 U/l, γ-glutamyltransferase
(γGT) of 200 U/l and aspartate transaminase (AST) and alanine
transaminase (ALT) of 50 and 40 U/l, respectively. Moreover,
regarding tumor markers, only a mild elevation of CA 19-9 (103
kU/l) was detected. Her past medical history was unremarkable. The
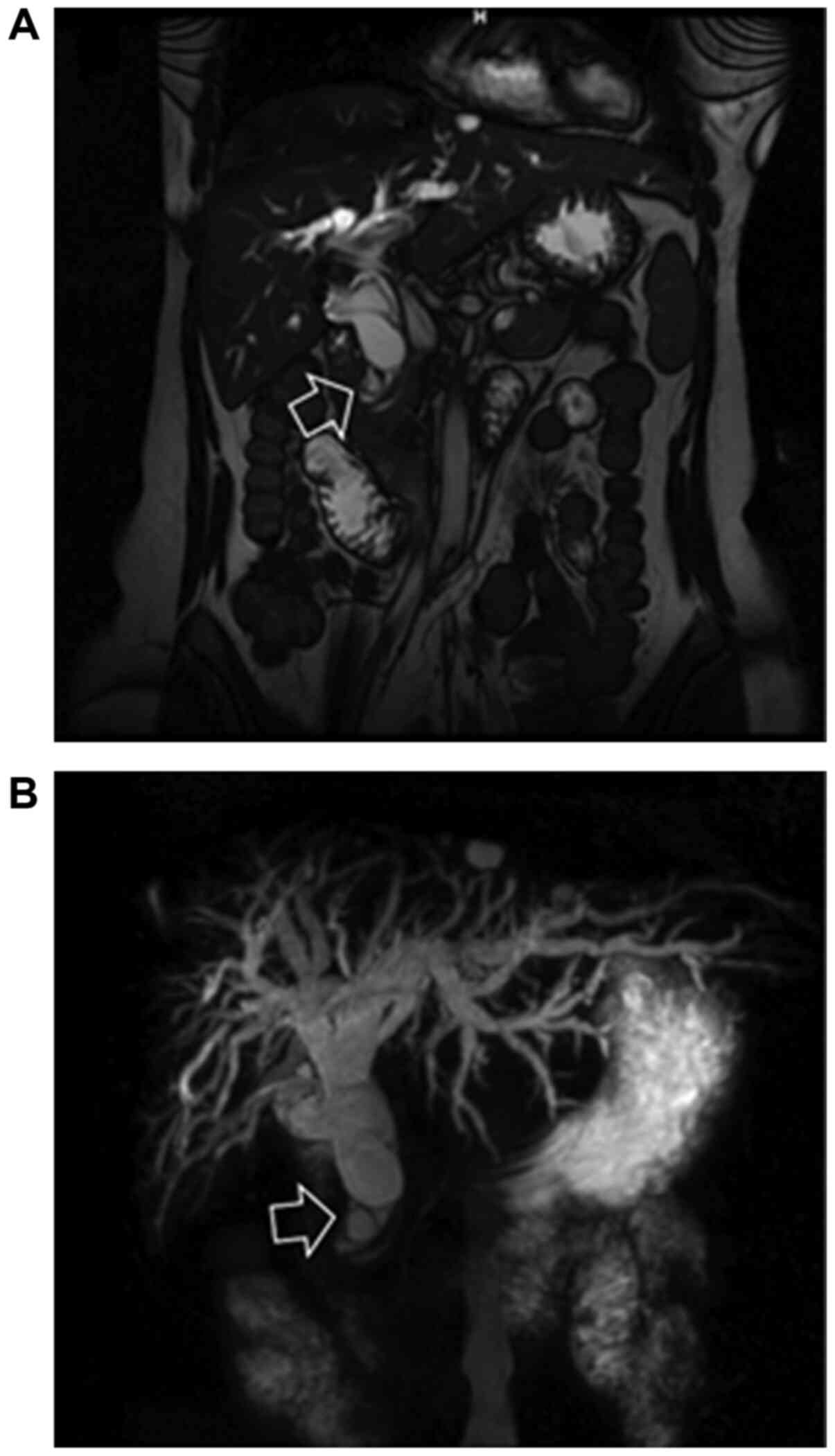
patient underwent magnetic resonance imaging scan (MRI/MRCP), which
revealed an ~2 cm lesion located in the distal common bile duct,
resulting in an excessive upstream extrahepatic and intrahepatic
dilation (Fig. 1). Endoscopic
retrograde cholangiopancreatography (ERCP) confirmed dilatation of
the biliary tree and a large filling defect of distal CBD, while a
notable amount of mucus was shown within the CBD. Given the origin
of the cystic lesion at the very distal CBD and the uncertainty
about the malignant potential of the lesion, our hospital's
multidisciplinary tumor board suggested radical surgical
treatment.
Accordingly, the patient underwent
pylorus-preserving pancreatoduodenectomy. The patient's
postoperative course was complicated by a small intrabdominal
abscess near the pancreaticojejunostomy, which was successfully
treated with computed tomography (CT)-guided aspiration and
intravenous administration of antibiotics. The rest of her
postoperative course was uneventful and she was discharged on 15th
postoperative day. Twenty-four months postoperatively, the patient
remains disease-free in excellent clinical condition.
Histopathological examination of the resected
specimen revealed the presence of a cystic neoplasm consisting of
mucin producing columnar epithelium, accompanied by ovarian-type
stromal elements. Minor dysplastic foci were observed throughout
the neoplastic epithelium. Abundant apical mucin was evident both
through Hematoxylin and eosin (H&E) and Alcian blue
histochemical staining, and the neoplastic cyst-lining epithelial
cells were diffusely positive for MUC5AC (Fig. 2). More specifically, for MUC5AC
immunochemistry we used Thermo Fisher Scientific antibody (REF
M5-145-P) with a dilution of 1/150 in room temperature. Duration of
primary antibody incubation is 30 min (no linker) and the slides
were scanned on D-Sight 200 fluo (A. Menarini Diagnostics). A
hypercellular spindle-cell stromal component, exhibiting variable
degrees of fibrosis accompanied the overlying epithelium without
any histopathological elements indicating invasive growth. Stromal
cells exhibited immunoreactivity for estrogen and progesterone
receptors. Multiple calcifications along with bilirubin debris and
agglomerates of basophilic microorganisms were also observed.
Granulation tissue formation was evident in various areas of the
tumor. The neoplasm was signed out as an intraductal mucinous
cystic neoplasm of the extra hepatic biliary tract, with low-grade
dysplasia.
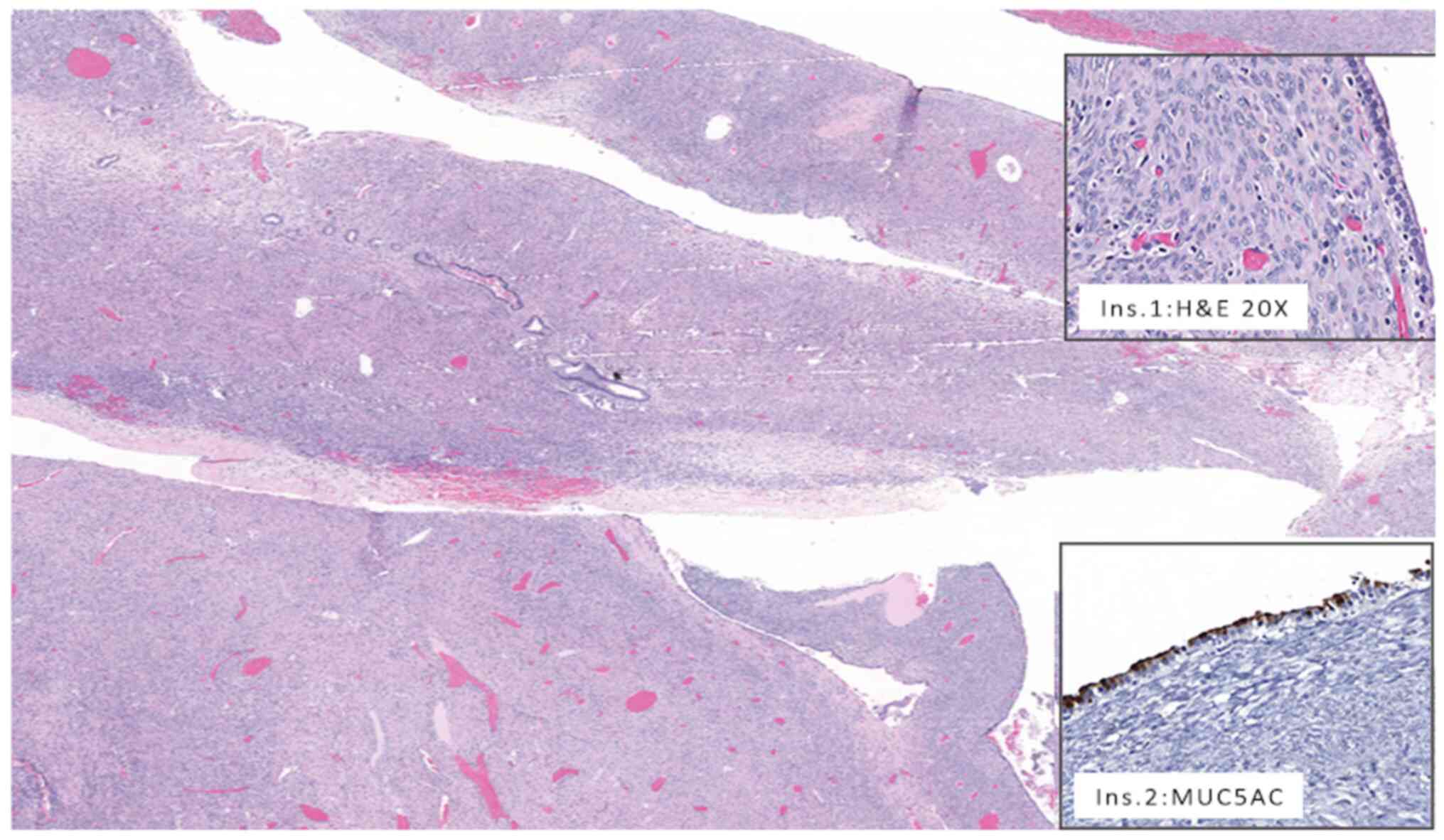 | Figure 2Histopathological evaluation of the
patient. The neoplasm consisted of multiple cystic formations of
various sizes accompanied by underlying hypercellular ovarian type
stroma (Η&Ε; magnification, x10). Inset 1 (Η&Ε;
magnification, x20). highlights that the neoplastic epithelium
consisted of bland, cuboidal, columnar cells, which only
occasionally exhibited minimum, low-grade dysplastic changes with
disruption of normal basal cellular orientation. Inset 2 shows that
MUC5AC was strongly and diffusely positive in epithelial cells
(magnification, x20). Ins, inset; MUC5AC, mucin 5AC, oligomeric
mucus/gel-forming. |
Discussion
BMCNs of the intrahepatic and extrahepatic biliary
tree, formerly known as bile duct/biliary cystadenoma and biliary
cystadenocarcinoma, represent an extremely rare entity,
characterized by the presence of ovarian-type stroma (3,8).
Besides their more common localization in the intrahepatic biliary
tree, they can also develop in the extrahepatic biliary tract
(9,10). According to current literature,
BMCNs represent less than 5% of non-parasitic hepatic cystic
lesions and so far, only few case reports of these rare lesions
have been published (11,12). In 85-95% of cases, patients
diagnosed with BMCNs are middle-aged women commonly asymptomatic or
presenting with non-specific symptoms and signs, thus, the clinical
diagnosis is highly incredibly challenging (11,13,14).
Interestingly, a case report of a young woman with intrahepatic
BMCN with extrahepatic growth has also been published (10). This fact indicates the potential
relationship of this entity with female-sex. The differential
diagnosis of BMCNs includes hydatid cysts, simple benign liver
cysts, liver abscess and mucinous cystic neoplasms with associated
invasive carcinoma (11).
Furthermore, similarly with our case, Pattarapuntakul et al
(10) described a young woman
presented with mild jaundice and impaired liver function in
biochemical laboratory tests. Both our case and case published by
Pattarapuntakul et al (10)
underwent an MRI/MRCP and ERCP, while our case did not have an
endoscopic ultrasound. Our patient underwent a Whipple procedure,
and in contrast, surgical team decide to perform a left
hepatectomy, because the tumor was intrahepatic with an
extrahepatic growth. To our knowledge, our case is one of the few
totally extrahepatic BMCNs, which treated with a pylorus-preserving
Whipple procedure.
In 2000 the classification by WHO included the terms
bile duct cystadenoma and cystadenocarcinoma, defined as cystic
tumors, that were characterized only by mucus-secreting or, less
commonly, serous epithelium (8).
Moreover, ovarian-type stroma was not a mandatory criterion for
histological diagnosis of these kind of lesions (2,8). With
regards to the current classification by WHO (2010), BMCNs are
defined as epithelial cystic lesions associated with ovarian-type
mesenchymal stroma (3). They are
divided into non-invasive and invasive BMCNs, whilst non-invasive
lesions are further classified into three histological subtypes
according to the grade of epithelial atypia: Low-, intermediate-
and high-grade intraepithelial neoplasia (3,15).
Although, intrahepatic or extrahepatic BMCNs with invasive
component are characterized as malignant tumors, the presence of
cell atypia in the histological evaluation of BMCN suggests also
significant malignant characteristics (15). On the other hand, non-invasive BMCNs
with anaplastic cell morphology are defined as neoplasms with
high-grade intraepithelial neoplasia (3).
Several theories have been described about the
presence of ovarian-type mesenchymal stroma in liver and
extrahepatic biliary tract (16,17).
It is known that during embryogenesis, the location of gonads,
normally, is under the diaphragm and dorsally to the liver,
extrahepatic biliary tree and pancreatic tail (16,17).
Additionally, the morphology of embryonic peritoneum in this
specific location is characterized by activated cells that might
reveal an evidence of relationship between gonads and developing
liver, biliary tree and pancreas (16). These ectopic ovarian deposits might
develop the tumors known as BMCNs by stimulating the proliferation
of adjacent biliary or pancreatic ducts (18).
While differentiating BMCNs from other entities is
very demanding, selecting the appropriate preoperative imaging
studies in order to diagnose them is a challenging process.
Preoperative imaging assessment usually includes Ultrasonography
(US), CT and magnetic resonance imaging (MRI) (19). BMCNs are usually characterized by
specific radiological features on CT and MRI, such as the presence
of a multi-loculated and well-defined cyst, internal septations,
thick capsulated cystic wall and less commonly a solid papillary
component (20,21). An associated significant upstream
ductal dilation can be identified secondary to bile flow
obstruction by the tumor, as in our case. Preoperative ERCP and
percutaneous transhepatic cholangiopancreatography (PTC) are useful
in demonstrating the communication between BMCNs and biliary tract,
while intra-operative cholangiography might also be a useful
modality in diagnosing extra-hepatic BMCNs (22,23).
Radiological findings such as irregular and thickened cystic wall,
papillary projections, hypervascular mural solid nodules and
calcifications suggest an increased suspicion of an invasive BMCN
(23). However, preoperative
imaging modalities cannot effectively distinguish benign from
malignant BMCNs (15).
As BMCNs have a malignant potential and their
preoperative differentiation from invasive BMCNs is extremely
difficult, thus, the most efficient curative treatment of choice
for all patients diagnosed with BMCNs and who are surgical
candidates, is radical surgical resection (24). Negative margins are recommended but
wide resections are not mandatory. Due to high recurrence rate,
these lesions should be treated regardless of their invasiveness
(25). As such, even a low-grade
non-invasive BMCN should be treated with complete surgical
resection (15). Enucleation with
negative margins is a valid alternative option for large lesions
which are located to the central liver segments and are associated
with important structures such as big vessels or large bile ducts
(7). Other more conservative
approaches like marsupialization, internal Roux en Y drainage,
aspiration and sclerosing agents application are associated with
high rates of complications (6,7).
Finally, liver transplantation has been described for unresectable
cases including recurrent or giant tumors (26,27).
Only few cases of patients with BMCNs who were
treated with chemoradiotherapy, have been described (15,24).
In 2009, Vanags et al (18)
reported the beneficial impact of systemic 5-fluoruracil-based
chemotherapy in a patient diagnosed with recurrent and metastatic
disease 41 months after the surgical resection of an invasive BMCN.
In another case, as the patient was not candidate for major
hepatectomy, hepatic arterial infusion of cisplatin was used
(28). The outcome of this
therapeutic option was a remarkable reduction of the tumor's size
from 12 cm to 2cm (28). In
addition, in a case series conducted by Läuffer et al
(24), three patients received
chemoradiation as the primary treatment and their 5-year overall
survival rate was approximately 35%.
As BMCNs are very uncommon tumors and only few
studies describing these lesions have been published, it is very
difficult to establish their prognosis. However, it seems to depend
both on the presence or absence of invasion and the margin
resection status. Moreover, Zen et al (29) reported that 24 patients with
non-invasive BMCN, who were surgically treated, had a median
overall survival rate of 47 months. They also described that an
incomplete resection of the lesion lead to a significantly high
recurrence rate (29). Almost 20%
of patients with non-invasive BMCNs who had a R1 resection or no
surgical treatment at all, can develop malignant transformation of
the tumor (20). In terms of
prognosis of invasive BMCNs, they have considerably better
prognosis after R0 resection compared with other primary malignant
hepatic lesions, such as hepatocellular carcinoma (HCC) and
cholangiocarcinoma (13,15,24).
More precisely, the 5-year survival rate of surgically treated
patients with malignant BMCNs ranges from 65 to 70%, while the
5-year survival rate of HCC and cholangiocarcinoma is around 40 and
22%, respectively (15).
Interestingly, BMCNs have better prognosis in comparison to
intraductal papillary mucinous neoplasms (IPMN) after surgical
resection (15,30). Kubota et al (30) reported that the 5-year survival rate
was 100% in patients with BMCNs after R0 resection, while in
patients with biliary IPMN was 84%. A periodical postoperative
follow-up with the already known imaging modalities, is mandatory,
in order to prevent recurrence of BMCNs, especially in invasive
BMCNs (31).
In conclusion, BMCNs are very rare entities, located
in intrahepatic and extrahepatic biliary tree characterized by a
very challenging preoperative diagnosis, as their clinical,
biochemical and radiological features are not specific. Surgical
resection with negative margins is the treatment of choice for both
non-invasive and invasive BMCNs. Finally, due to malignant
potential of these lesions and the high rates of recurrence, a
meticulous postoperative surveillance is recommended.
Acknowledgements
Not applicable.
Funding
No funding was received.
Availability of data and materials
The datasets used and/or analyzed during the current
study are available from the corresponding author on reasonable
request.
Authors' contributions
AP, AM and DS conceived the idea and designed the
study. NM, VN, SK and VD acquired, analyzed and interpreted the
data. AP and DS drafted and revised the manuscript. AM and DS
confirmed the authenticity of all the raw data. All authors read
and approved the final manuscript.
Ethics approval and consent to
participate
Not applicable.
Patient consent for publication
Written informed consent was obtained from the
patient for publication of this case report and any accompanying
images.
Competing interests
The authors declare that they have no competing
interests.
References
|
1
|
Dixon E, Sutherland FR, Mitchell P,
McKinnon G and Nayak V: Cystadenomas of the liver: A spectrum of
disease. Can J Surg. 44:371–376. 2001.PubMed/NCBI
|
|
2
|
Rodriguez RM, Barrio M, Parker ML, Saeed
O, Sherman S and Ceppa EP: Mucinous cystic neoplasms of the liver:
Presence of biliary communication. J Surg Case Rep.
2019(rjz364)2019.PubMed/NCBI View Article : Google Scholar
|
|
3
|
Tsui WMS, Adsay NV, Crawford JM, Hurban R
and Kloppel G WA: Mucinous cystic neoplasms of the liver. In: WHO
Classification of Tumours of the Digestive System. 4th
edition.Bosman FT, Carneiro F, Hruban RH and Theise ND, (eds).
International Agency for Research on Cancer, Lyon, pp236-238,
2010.
|
|
4
|
Metussin A, Telisinghe P, Kok K and Chong
V: Extrahepatic biliary cystadenoma: A rare cause of biliary
obstruction. Oman Med J. 30:66–68. 2015.PubMed/NCBI View Article : Google Scholar
|
|
5
|
Albores-Saavedra J, Córdova-Ramón JC,
Chablé-Montero F, Dorantes-Heredia R and Henson DE: Cystadenomas of
the liver and extrahepatic bile ducts: Morphologic and
immunohistochemical characterization of the biliary and intestinal
variants. Ann Diagn Pathol. 19:124–129. 2015.PubMed/NCBI View Article : Google Scholar
|
|
6
|
Thomas KT, Welch D, Trueblood A, Sulur P,
Wise P, Gorden DL, Chari RS, Wright JK Jr, Washington K and Pinson
CW: Effective treatment of biliary cystadenoma. Ann Surg.
241:769–775. 2005.PubMed/NCBI View Article : Google Scholar
|
|
7
|
Fragulidis GP, Vezakis AI, Konstantinidis
CG, Chondrogiannis KK, Primetis ES, Kondi-Pafiti A and Polydorou
AA: Diagnostic and therapeutic challenges of intrahepatic biliary
cystadenoma and cystadenocarcinoma: A report of 10 cases and review
of the literature. Int Surg. 100:1212–1219. 2015.PubMed/NCBI View Article : Google Scholar
|
|
8
|
Teng XD, Hamilton SR and Aaltonen LA
(eds.): World Health Organization Classification of Tumours.
Pathology and Genetics of Tumours of the Digestive System. IARC
Press, Lyon, 2000. Zhonghua Bing Li Xue Za Zhi. 34:544–546.
2005.(In Chinese).
|
|
9
|
Anand S, Chandrasekar S, Raja K and
Pottakkat B: Mucinous cystic neoplasm of the liver with biliary
communication: An exception to the current classification. BMJ Case
Rep. 12:10–12. 2019.PubMed/NCBI View Article : Google Scholar
|
|
10
|
Pattarapuntakul T, Ovartlarnporn B and
Sottisuporn J: Mucinous cystic neoplasm of the liver with
extrahepatic growth presenting with ascending cholangitis diagnosed
by endoscopic ultrasound features: A case report. J Med Case Rep.
12(33)2018.PubMed/NCBI View Article : Google Scholar
|
|
11
|
Walt AJ: Cysts and benign tumors of the
liver. Surg Clin North Am. 57:449–464. 1977.PubMed/NCBI View Article : Google Scholar
|
|
12
|
Tholomier C, Wang Y, Aleynikova O,
Vanounou T and Pelletier JS: Biliary mucinous cystic neoplasm
mimicking a hydatid cyst: A case report and literature review. BMC
Gastroenterol. 19(103)2019.PubMed/NCBI View Article : Google Scholar
|
|
13
|
Emre A, Serin KR, Ozden I, Tekant Y, Bilge
O, Alper A, Güllüoğlu M and Güven K: Intrahepatic biliary cystic
neoplasms: Surgical results of 9 patients and literature review.
World J Gastroenterol. 17:361–365. 2011.PubMed/NCBI View Article : Google Scholar
|
|
14
|
Davies W, Weiland L, Batts K and Nagorney
DM: Intrahepatic biliary cystadenomas with and without mesenchymal
stroma. HPB. 1:141–146. 1999.
|
|
15
|
Simo KA, McKillop IH, Ahrens WA, Martinie
JB, Iannitti DA and Sindram D: Invasive biliary mucinous cystic
neoplasm: A review. HPB (Oxford). 14:725–740. 2012.PubMed/NCBI View Article : Google Scholar
|
|
16
|
Erdogan D, Kloek J, Lamers WH, Offerhaus
GJA, Busch ORC, Gouma DJ and Van Gulik TM: Mucinous cystadenomas in
liver: Management and origin. Dig Surg. 27:19–23. 2010.PubMed/NCBI View Article : Google Scholar
|
|
17
|
Zamboni G, Scarpa A, Bogina G, Iacono C,
Bassi C, Talamini G, Sessa F, Capella C, Solcia E, Rickaert F, et
al: Mucinous cystic tumors of the pancreas: Clinicopathological
features, prognosis, and relationship to other mucinous cystic
tumors. Am J Surg Pathol. 23:410–422. 1999.PubMed/NCBI View Article : Google Scholar
|
|
18
|
Vanags A, Pavars M, Prieditis P, Strumfa
I, Irmejs A and Gardovskis J: Biliary cystic tumours with
mesenchymal stroma. Acta Chir Latv. 9:95–99. 2010.
|
|
19
|
Mortelé KJ and Ros PR: Cystic focal liver
lesions in the adult: Differential CT and MR imaging features.
Radiographics. 21:895–910. 2001.PubMed/NCBI View Article : Google Scholar
|
|
20
|
Soares KC, Arnaoutakis DJ, Kamel I, Anders
R, Adams RB, Bauer TW and Pawlik TM: Cystic neoplasms of the liver:
Biliary cystadenoma and cystadenocarcinoma. J Am Coll Surg.
218:119–128. 2014.PubMed/NCBI View Article : Google Scholar
|
|
21
|
Kim JY, Kim SH, Eun HW, Lee MW, Lee JY,
Han JK and Choi BI: Differentiation between biliary cystic
neoplasms and simple cysts of the liver: Accuracy of CT. Am J
Roentgenol. 195:1142–1148. 2010.PubMed/NCBI View Article : Google Scholar
|
|
22
|
Borhani AA, Wiant A and Heller MT: Cystic
hepatic lesions: A review and an algorithmic approach. Am J
Roentgenol. 203:1192–1204. 2014.PubMed/NCBI View Article : Google Scholar
|
|
23
|
Marrone G, Maggiore G, Carollo V, Sonzogni
A and Luca A: Biliary cystadenoma with bile duct communication
depicted on liver-specific contrast agent-enhanced MRI in a child.
Pediatr Radiol. 41:121–124. 2011.PubMed/NCBI View Article : Google Scholar
|
|
24
|
Läuffer JM, Baer HU, Maurer CA, Stoupis C,
Zimmerman A and Büchler MW: Biliary cystadenocarcinoma of the
liver: The need for complete resection. Eur J Cancer. 34:1845–1851.
1998.PubMed/NCBI View Article : Google Scholar
|
|
25
|
Ohtsuka M, Shimizu H, Kato A, Yoshitomi H,
Furukawa K, Tsuyuguchi T, Sakai Y, Yokosuka O and Miyazaki M:
Intraductal papillary neoplasms of the bile duct. Int J Hepatol.
2014(459091)2014.PubMed/NCBI View Article : Google Scholar
|
|
26
|
Grubor NM, Colovic RB, Atkinson HD and
Micev MT: Giant biliary mucinous cystadenoma of the liver. Ann
Hepatol. 12:979–983. 2013.PubMed/NCBI
|
|
27
|
Limongelli P, Pai M, Damrah O, Lauretta A,
Atijosan O, Habib N and Jiao LR: Cystic tumors of the biliary
tract: A complete excision is crucial. Int Surg. 94:136–140.
2009.PubMed/NCBI
|
|
28
|
Hazanaki K, Yoshizawa K and Mori H:
Hepatic arterial infusion chemotherapy of cisplatin for biliary
cystadenoma. Hepatogastrenterology. 46:462–464. 1999.PubMed/NCBI
|
|
29
|
Zen Y, Pedica F, Patcha VR, Capelli P,
Zamboni G, Casaril A, Quaglia A, Nakanuma Y, Heaton N and Portmann
B: Mucinous cystic neoplasms of the liver: A clinicopathological
study and comparison with intraductal papillary neoplasms of the
bile duct. Mod Pathol. 24:1079–1089. 2011.PubMed/NCBI View Article : Google Scholar
|
|
30
|
Kubota K, Nakanuma Y, Kondo F, Hachiya H,
Miyazaki M, Nagino M, Yamamoto M, Isayama H, Tabata M, Kinoshita H,
et al: Clinicopathological features and prognosis of
mucin-producing bile duct tumor and mucinous cystic tumor of the
liver: A multi-institutional study by the Japan Biliary
Association. J Hepatobiliary Pancreat Sci. 21:176–185.
2014.PubMed/NCBI View
Article : Google Scholar
|
|
31
|
Ratti FA, Ferla F, Paganelli M, Cipriani
FA, Aldrighetti LA and Ferla G: Biliary cystadenoma: Short-and
long-term outcome after radical hepatic resection. Updates Surg.
64:13–18. 2012.PubMed/NCBI View Article : Google Scholar
|