Introduction
Immune checkpoint inhibitors (ICI) targeting
programmed cell death-1 (PD-1) have been developed as cancer
immunotherapy agents (1,2). Given that PD-1 is an inhibitory
immunogenic molecule, the ability of ICI to enhance the immune
system allows it to eliminate cancer cells (1,2).
Patients treated with nivolumab often expect longer-term survival
than would be obtained with conventional chemotherapies, and
overall survival curves have been seen to flatten in some clinical
trials (3-5).
However, extended administration of nivolumab raises concerns of
immune-related adverse events (irAEs) and can create financial
issues (6,7). Therefore, in some patients, nivolumab
may be discontinued for reasons other than disease progression.
In some reports, long-lasting responses were
observed in patients even after discontinuation of nivolumab
treatment and no further anti-cancer treatment (8-10).
Although the mechanisms of long-lasting response are not fully
understood, prolonged binding of nivolumab on T cells is one
possible explanation (11,12). Some groups have indeed reported
prolonged nivolumab binding on T cells after the last nivolumab
infusion, which has stimulated study of the kinetics of nivolumab
binding after discontinuation of treatment (11,12).
However, a relationship between nivolumab binding at relapse and
the efficacy of nivolumab re-challenge has not been reported.
Here, we monitored PD-1 occupancy on T cells of five
patients who discontinued nivolumab treatment for reasons other
than tumor progression and determined the relationship between the
level of nivolumab binding at relapse and the efficacy of
additional nivolumab therapy.
Materials and methods
Patients and sample collections
Between May 2019 and June 2020, peripheral blood
samples were collected from patients at Kobe University Hospital
who had discontinued nivolumab administration after long-term use.
Samples were collected in heparinized tubes. Peripheral blood
mononuclear cells (PBMCs) then were isolated by density gradient
centrifugation using Ficoll-Paque Plus (GE Healthcare, UK) and
SepMate-50 tubes (STEMCELL Technologies, Canada), according to the
manufacturer's instructions.
Flow cytometric analysis for PD-1
receptor occupancy
To detect nivolumab (a human IgG4 monoclonal
antibody) binding to PD-1 molecules on circulating CD3+ T cells,
PBMCs were incubated (4°C, 20 min) with a saturating concentration
(20 µg/ml) of either unlabeled human IgG4 (isotype control) or
nivolumab, washed extensively, and then co-stained with anti-human
CD3-APC (Biolegend, USA) and murine anti-human IgG4 biotin
(Invitrogen, USA) plus BV421 streptavidin (BD Biosciences, USA).
PD-1 binding was determined as the ratio of the percent of CD3+ T
cells stained with anti-human IgG4 after in vitro saturation
with isotype control antibody (indicating in vivo binding)
to that observed after nivolumab saturation (showing total
available binding sites) (11).
The flow cytometry gating strategy for analysis of occupancy rate
is shown in Figs. S1 and S2.
Results
Patient characteristics
Five patients who discontinued nivolumab treatment
for reasons other than tumor progression were investigated
(Table I). Patient characteristics
are described in Table I. One
patient had completed a year of adjuvant nivolumab following
surgery. The other four patients with recurrent disease had been
treated with nivolumab for 52-104 weeks, but decided to discontinue
treatment due to the stable state of their disease and concern over
the development of irAEs. All patients underwent computed
tomography scans every 3-4 months to monitor tumor growth, during
which time no further cancer treatments were done.
 | Table IPatient characteristics. |
Table I
Patient characteristics.
| Patient | Age, years | Sex | Cancer type | Prior treatment | Reason for
nivolumab treatment
(stage) | Dosing duration of
nivolumab
(times) | Liver
functionc (AST/ALT
U/ml) | Creatinine
clearancec
(Cockcroft- Gault, ml/min) | irAEd (Grade) |
Recurrencee (number, site, size) |
|---|
| Patient 1 | 71 | Male | Melanoma | Surgery | Adjuvant setting
(Stage II) | 52 weeks (22) | 25/23 | 63.3 | None | - |
| Patient 2 | 75 | Male | Laryngeal cancer |
Chemoradiotherapya after surgery | Recurrence (Stage
IV) | 100 weeks (49) | 23/16 | 25.2 | Dermatitis (G1) | - |
| Patient 3 | 72 | Female | Cancer of unknown
primary in the head and neck |
Chemoradiotherapya after surgery | Recurrence (Stage
IV) | 98 weeks (47) | 23/9 | 24.5 | None | - |
| Patient 4 | 70 | Male | Oropharyngeal
cancer |
Chemoradiotherapya after surgery | Recurrence (Stage
IV) | 58 weeks (28) | 20/16 | 51.5 | Dermatitis (G1)
Thyroiditis (G2) | 1, Left adrenal
grant, 15.6-mm |
| Patient 5 | 68 | Male | Cancer of unknown
primary in the mediastinal lymph node |
Chemotherapyb | Metastasis (Stage
IV) | 104 weeks (50) | 26/30 | 66.1 | Thyroiditis (G2) | 1, Right hilar lymph
node, 25.1-mm |
Monitoring occupancy of nivolumab on
PD-1 of CD3 T cells after discontinuation
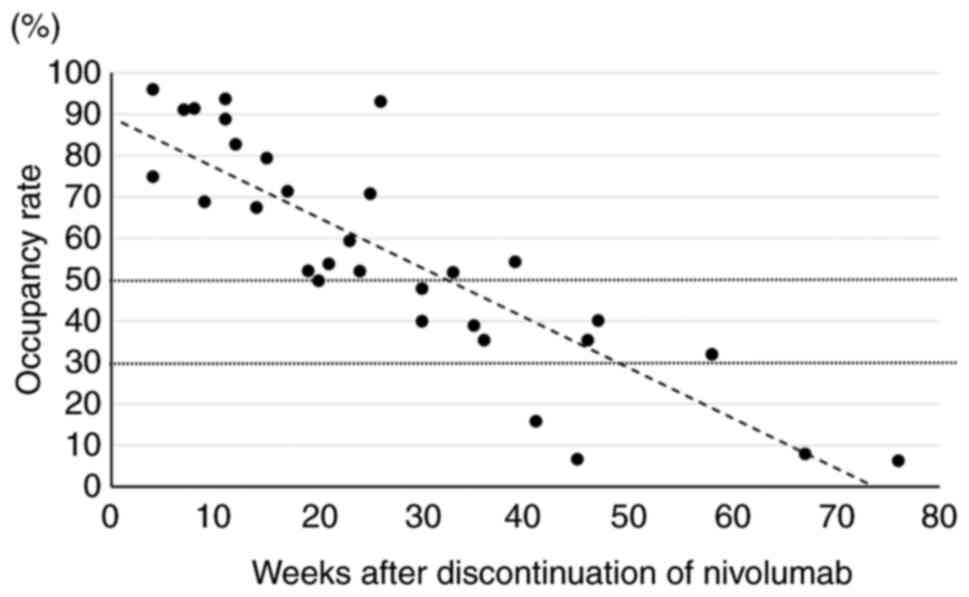
We monitored the binding of nivolumab to T cells by
flow cytometric analysis at 32 different times (6.4
points/patient). Linear regression analysis indicated that it took
32.4 and 48.9 weeks to decrease occupancies by 50 and 70%,
respectively (Fig. 1). The
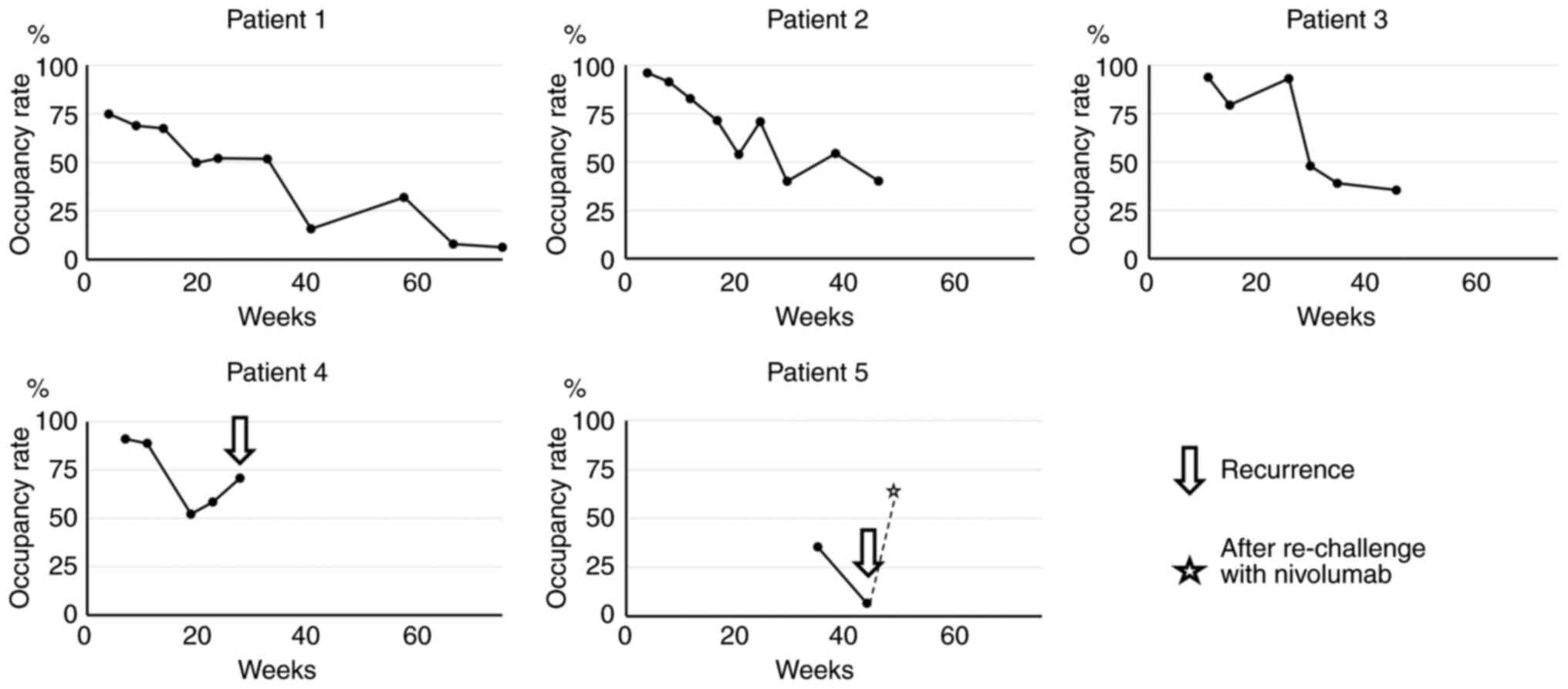
individual ratios for each patient are shown in Fig. 2.
Relationship between PD-1 occupancy at
relapse and efficacy of retreatment
Patients 4 and 5 had disease recurrence 28 and 45
weeks after their last nivolumab infusion, respectively, at which
time treatment was re-initiated. Nivolumab binding at recurrence
was 70.8 and 6.6%, respectively (Fig.
2). The flow cytometry plots for patients 4 and 5 are shown in
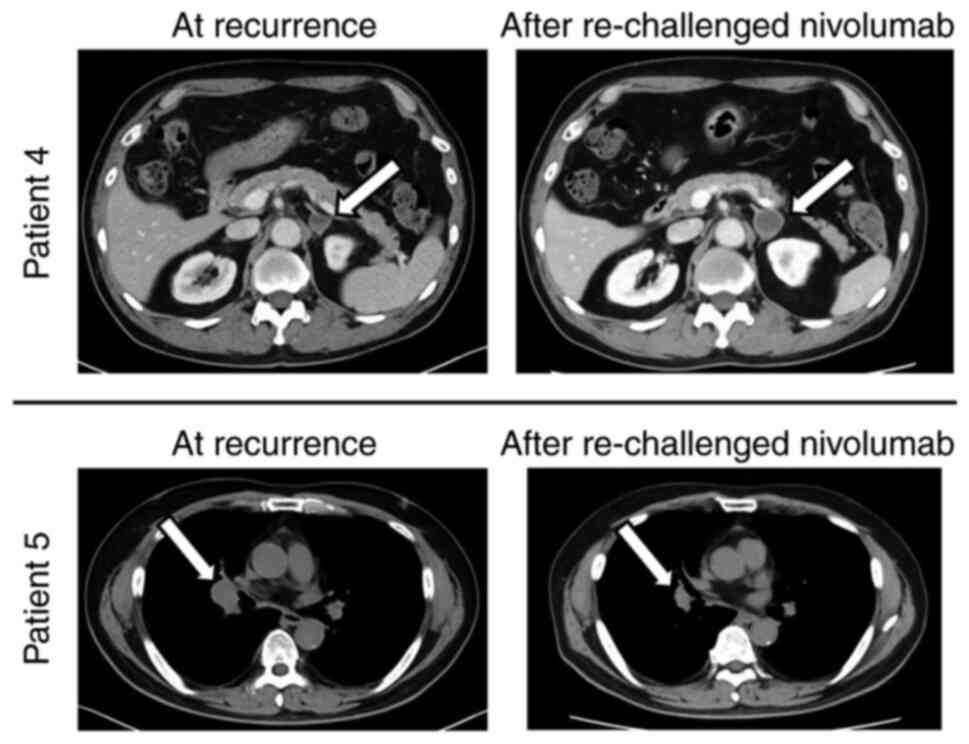
Supplemental Fig. 2. Only
treatment of the patient with 6.6% binding was efficacious
(Fig. 3). Occupancy in Patient 5
at 4 weeks after re-administration was 68.3% (Fig. 2).
Discussion
The optimal duration of treatment with nivolumab
remains unknown. In a largely community-based phase IIIb/IV study,
CheckMate 153(13), the effects of
either one-year or continuous treatment were evaluated. An
important result was that continuing nivolumab beyond one year
improved outcomes (13). On the
other hand, the financial burden and irAE occurrence on long-term
use of nivolumab should be considered. We note that therapy with
another anti-PD-1 antibody, pembrolizumab, was ended after 2 years
in most clinical trials (14,15).
Nivolumab discontinuation is one strategy that should be considered
for patients with prolonged stable disease due to long-term use of
nivolumab. Further studies about discontinuation of ICI are ongoing
(16).
A few previous studies have examined the binding of
nivolumab to PD-1 on T cells after nivolumab discontinuation
(11,12). As in our study, Osa et al
investigated nivolumab binding on T cells in lung cancer patients
and reported that prolonged binding (more than 20 weeks) was
maintained (12). Consistent with
these reports, several studies have demonstrated prolonged
remission in patients after the discontinuation of nivolumab
therapy (8,17,18).
Accordingly, a correlation may be present between long-term PD-1
occupancy and a prolonged treatment effect (9). In our study, two patients experienced
disease recurrence after discontinuation of nivolumab. Patient 4
relapsed 28 weeks after discontinuation, at which point occupancy
was 70.8%. This case might therefore suggest that relapse is not
associated with a lack of nivolumab. It may instead be due to tumor
cells developing resistance to the drug or to changes in the
relationship between the cancer and its microenvironment, including
immune cells and alterations in genes encoding components of the
antigen processing and/or presentation apparatus (e.g., class I
MHC, β2-microglobulin) (19,20).
In this case, re-administration of nivolumab was not effective. In
contrast, patient 5 relapsed 45 weeks after the last dose,
displaying only 6.6% occupancy. In such cases, re-administration of
nivolumab to increase the level of binding may be a useful
strategy. In fact, occupancy quickly increased up to 68.3% at 4
weeks after re-administration.
In addition to occupancy, a number of other factors
have been identified as being associated with the effectiveness of
nivolumab. One group reported a relationship between metastatic
sites and their numbers and the efficacy of ICI in patients with
advanced non-small cell lung cancer (21). In their report, patients with brain
metastases had shorter overall survival than those without, and a
greater number of involved metastatic organs was related with a
poorer response to ICIs. In our study, the two patients with
recurrence both had a single site of recurrence (Patient 4, adrenal
grand; and Patient 5, lymph node), and the relationship between the
number of metastases and the effect is not clear. Further studies
are needed to reveal other factors.
Some studies have investigated ICI re-challenge in
cancer patients. One group reported an objective response rate on
nivolumab re-challenge of 2.9% and disease control rate of 42.9%
(20). Regarding pembrolizumab,
another PD-1 antibody, a second group reported outcomes in patients
who completed 2 years of pembrolizumab treatment: among 21 patients
who underwent re-challenge after recurrence, 11 (52.4%) had an
objective response (22).
Furthermore, another group reported the results of pembrolizumab
re-treatment in patients with melanoma who relapsed 6 months after
completing 1 year of adjuvant pembrolizumab therapy. Although only
9 patients were evaluable, one achieved a complete response and
three patients were categorized with stable disease by re-challenge
(23). These reports suggest that
re-challenge might even benefit those patients with a history of
disease progression after ICI therapy. Nevertheless, it remains
unclear which patients will benefit from re-challenge. Research
into the relationship between occupancy and efficacy may aid the
identification of candidates for re-administration.
Our study has some limitations. First, it was a
small case series and only two patients received re-administration
of nivolumab. Clarifying the relationship between efficacy of
re-administration and occupancy rate will require prospective
confirmation in larger studies. Second, compared with the serum
half-life of nivolumab, occupancy is maintained for an extended
period. However, the mechanism underlying the long-term residual
binding of nivolumab on T cells is still unclear. Furthermore,
factors influencing the fluctuation of binding rate are also
unclear. Although two of five patients had reduced renal function
in our study, there was no clear difference in the trend in
occupancy between these patients and those with normal renal
function. Further research into the pharmacokinetics of this agent
is required. Third, in patients 4 and 5, because the period between
the date of registration and recurrence was short, only five and
two measurements were made, respectively. These numbers may be
insufficient to clarify the precise trends. We also do not have
data on occupancy during nivolumab treatment in all patients. To
improve the accuracy of the trend, measurement at additional points
would be necessary. Finally, although we believe this measurement
method for occupancy is sufficient to show a trend, degree of
measurement error will be present, owing to the complicated and
multi-process nature of FACS.
In conclusion, nivolumab occupied PD-1 on T cells
for an extended period. Re-challenge with nivolumab may provide a
good response in patients with lowered occupancy.
Supplementary Material
Representative example of the flow
cytometry gating strategy used to analyze of occupancy rate.
Samples were stained with antibodies and analyzed using flow
cytometry using the gating strategy shown. Occupancy rate was
estimated as the percent of CD3+ T cells stained with
anti-human IgG4 after in vitro saturation with isotype
control antibody (indicating in vivo binding; A) to that
observed after nivolumab saturation; B) showing total available
binding sites.
Flow cytometry plots for patients 4
and 5. The gating strategy is described in Fig. S1.
Acknowledgements
Not applicable.
Funding
Funding: This research was supported by the Kinki Promotion
Network for Clinical Oncology (grant no. 201704).
Availability of data and materials
The datasets used and/or analyzed during the current
study are available from the corresponding author on reasonable
request.
Authors' contributions
TN and YF conceived and designed the study,
collected, analyzed and interpreted the data and drafted and wrote
the article. HS and YN collected and interpreted the data. YI, MT
and NK collected and interpreted the data, and were involved in
patient management. HM supervised the project, interpretated the
data and reviewed and revised the manuscript. All authors read and
approved the final version of the article. TN and YF confirm the
authenticity of all the raw data.
Ethics approval and consent to
participate
The present investigation was approved by the Kobe
University Hospital Ethics Committee (approval no. 180152) and was
conducted in accordance with the Declaration of Helsinki.
Patient consent for publication
All patients provided written informed consent for
this investigation and publication of their data.
Competing interests
Hironobu Minami has received research grants and
honoraria from Bristol-Myers Squibb and Chugai Pharmaceutical.
Naomi Kiyota has received research grants from Bristol-Myers
Squibb. The other authors declare that they have no competing
interests.
References
|
1
|
Pardoll DM: The blockade of immune
checkpoints in cancer immunotherapy. Nat Rev Cancer. 12:252–264.
2012.PubMed/NCBI View
Article : Google Scholar
|
|
2
|
Topalian SL, Drake CG and Pardoll DM:
Immune checkpoint blockade: A common denominator approach to cancer
therapy. Cancer Cell. 27:450–461. 2015.PubMed/NCBI View Article : Google Scholar
|
|
3
|
Topalian SL, Hodi FS, Brahmer JR,
Gettinger SN, Smith DC, McDermott DF, Powderly JD, Sosman JA,
Atkins MB, Leming PD, et al: Five-year survival and correlates
among patients with advanced melanoma, renal cell carcinoma, or
non-small cell lung cancer treated with nivolumab. JAMA Oncol.
5:1411–1420. 2019.PubMed/NCBI View Article : Google Scholar
|
|
4
|
Hodi FS, Chiarion-Sileni V, Gonzalez R,
Grob JJ, Rutkowski P, Cowey CL, Lao CD, Schadendorf D, Wagstaff J,
Dummer R, et al: Nivolumab plus ipilimumab or nivolumab alone
versus ipilimumab alone in advanced melanoma (CheckMate 067):
4-year outcomes of a multicentre, randomised, phase 3 trial. Lancet
Oncol. 19:1480–1492. 2018.PubMed/NCBI View Article : Google Scholar
|
|
5
|
Quinn C, Garrison LP, Pownell AK, Atkins
MB, de Pouvourville G, Harrington K, Ascierto PA, McEwan P, Wagner
S, Borrill J and Wu E: Current challenges for assessing the
long-term clinical benefit of cancer immunotherapy: A
multi-stakeholder perspective. J Immunother Cancer.
8(e000648)2020.PubMed/NCBI View Article : Google Scholar
|
|
6
|
Postow MA, Sidlow R and Hellmann MD:
Immune-related adverse events associated with immune checkpoint
blockade. N Engl J Med. 378:158–168. 2018.PubMed/NCBI View Article : Google Scholar
|
|
7
|
Brahmer JR, Lacchetti C, Schneider BJ,
Atkins MB, Brassil KJ, Caterino JM, Chau I, Ernstoff MS, Gardner
JM, Ginex P, et al: Management of immune-related adverse events in
patients treated with immune checkpoint inhibitor therapy: American
Society of clinical oncology clinical practice guideline. J Clin
Oncol. 36:1714–1768. 2018.PubMed/NCBI View Article : Google Scholar
|
|
8
|
Takagi T, Yoshida K, Kobayashi H, Kondo T,
Iizuka J, Okumi M, Ishida H, Fukuda H, Ishihara H and Tanabe K:
Durable response after discontinuation of nivolumab therapy in
patients with metastatic renal cell carcinoma. Jpn J Clin Oncol.
48:860–863. 2018.PubMed/NCBI View Article : Google Scholar
|
|
9
|
Yatsuda Y, Hirose S, Ito Y, Onoda T,
Sugiyama Y, Nagafuchi M, Suzuki H, Niisato Y, Tange Y, Ikeda T, et
al: A Durable response after the discontinuation of nivolumab in an
advanced gastric cancer patient. Intern Med. 60:1011–1017.
2021.PubMed/NCBI View Article : Google Scholar
|
|
10
|
Kimura H, Araya T, Yoneda T, Shirasaki H,
Kurokawa K, Sakai T, Koba H, Tambo Y, Nishikawa S, Sone T and
Kasahara K: Long-lasting responses after discontinuation of
nivolumab treatment for reasons other than tumor progression in
patients with previously treated, advanced non-small cell lung
cancer. Cancer Commun (Lond). 39(78)2019.PubMed/NCBI View Article : Google Scholar
|
|
11
|
Brahmer JR, Drake CG, Wollner I, Powderly
JD, Picus J, Sharfman WH, Stankevich E, Pons A, Salay TM, McMiller
TL, et al: Phase I study of single-agent anti-programmed death-1
(MDX-1106) in refractory solid tumors: Safety, clinical activity,
pharmacodynamics, and immunologic correlates. J Clin Oncol.
28:3167–3175. 2010.PubMed/NCBI View Article : Google Scholar
|
|
12
|
Osa A, Uenami T, Koyama S, Fujimoto K,
Okuzaki D, Takimoto T, Hirata H, Yano Y, Yokota S, Kinehara Y, et
al: Clinical implications of monitoring nivolumab immunokinetics in
non-small cell lung cancer patients. JCI insight.
3(e59125)2018.PubMed/NCBI View Article : Google Scholar
|
|
13
|
Waterhouse DM, Garon EB, Chandler J,
McCleod M, Hussein M, Jotte R, Horn L, Daniel DB, Keogh G, Creelan
B, et al: Continuous versus 1-year fixed-duration nivolumab in
previously treated advanced non-small-cell lung cancer: CheckMate
153. J Clin Oncol. 38:3863–3873. 2020.PubMed/NCBI View Article : Google Scholar
|
|
14
|
Schachter J, Ribas A, Long GV, Arance A,
Grob JJ, Mortier L, Daud A, Carlino MS, McNeil C, Lotem M, et al:
Pembrolizumab versus ipilimumab for advanced melanoma: Final
overall survival results of a multicentre, randomised, open-label
phase 3 study (KEYNOTE-006). Lancet. 390:1853–1862. 2017.PubMed/NCBI View Article : Google Scholar
|
|
15
|
Danson S, Hook J, Marshall H, Smith A,
Bell S, Rodwell S and Corrie P: Are we over-treating with
checkpoint inhibitors? Br J Cancer. 121:629–630. 2019.PubMed/NCBI View Article : Google Scholar
|
|
16
|
Nomura S, Goto Y, Mizutani T, Kataoka T,
Kawai S, Okuma Y, Murakami H, Tanaka K and Ohe Y: A randomized
phase III study comparing continuation and discontinuation of PD-1
pathway inhibitors for patients with advanced non-small-cell lung
cancer (JCOG1701, SAVE study). Jpn J Clin Oncol. 50:821–825.
2020.PubMed/NCBI View Article : Google Scholar
|
|
17
|
Gauci ML, Lanoy E, Champiat S, Caramella
C, Ammari S, Aspeslagh S, Varga A, Baldini C, Bahleda R, Gazzah A,
et al: Long-term survival in patients responding to Anti-PD-1/PD-L1
therapy and disease outcome upon treatment discontinuation. Clin
Cancer Res. 25:946–956. 2019.PubMed/NCBI View Article : Google Scholar
|
|
18
|
Tachihara M, Negoro S, Inoue T, Tamiya M,
Akazawa Y, Uenami T, Urata Y, Hattori Y, Hata A, Katakami N and
Yokota S: Efficacy of anti-PD-1/PD-L1 antibodies after
discontinuation due to adverse events in non-small cell lung cancer
patients (HANSHIN 0316). BMC Cancer. 18(946)2018.PubMed/NCBI View Article : Google Scholar
|
|
19
|
Shin DS, Zaretsky JM, Escuin-Ordinas H,
Garcia-Diaz A, Hu-Lieskovan S, Kalbasi A, Grasso CS, Hugo W,
Sandoval S, Torrejon DY, et al: Primary Resistance to PD-1 blockade
mediated by JAK1/2 mutations. Cancer Discov. 7:188–201.
2017.PubMed/NCBI View Article : Google Scholar
|
|
20
|
Chen DS and Mellman I: Elements of cancer
immunity and the cancer-immune set point. Nature. 541:321–330.
2017.PubMed/NCBI View Article : Google Scholar
|
|
21
|
Qiao M, Zhou F, Hou L, Li X, Zhao C, Jiang
T, Gao G, Su C, Wu C, Ren S and Zhou C: Efficacy of
immune-checkpoint inhibitors in advanced non-small cell lung cancer
patients with different metastases. Ann Transl Med.
9(34)2021.PubMed/NCBI View Article : Google Scholar
|
|
22
|
Herbst RS, Garon EB, Kim DW, Cho BC,
Gervais R, Perez-Gracia JL, Han JY, Majem M, Forster MD, Monnet I,
et al: Five year survival update from KEYNOTE-010: pembrolizumab
versus docetaxel for previously treated, programmed Death-Ligand
1-positive advanced NSCLC. J Thorac Oncol. 16:1718–1732.
2021.PubMed/NCBI View Article : Google Scholar
|
|
23
|
Eggermont AM, Meshcheryakov A, Atkinson V,
Blank CU, Mandala M, Long GV, Barrow C, Di Giacomo AM, Fisher R,
Sandhu S, et al: Crossover and rechallenge with pembrolizumab in
recurrent patients from the EORTC 1325-MG/Keynote-054 phase III
trial, pembrolizumab versus placebo after complete resection of
high-risk stage III melanoma. Eur J Cancer. 158:156–168.
2021.PubMed/NCBI View Article : Google Scholar
|