Introduction
Caesarean section, whose prevalence worldwide has
increased significantly in recent years, particularly when
medically indicated, is a life-saving procedure. In numerous cases,
however, it can lead to unexpected short-term or long-term
complications of varying frequency and severity, and can
significantly increase maternal and neonatal morbidity and
mortality (1). A rare complication
of low transverse caesarean section is bladder flap hematoma, which
is the result of bleeding of the uterine closure. The localization
of the haematoma is usually between the bladder and the lower
uterine segment. On more rare occasions, the haematoma may extend
under the uterine serosa along the broad ligaments to the
retroperitoneal space. The formation of bladder flap haematoma is
more frequent during the conventional method of caesarean section,
which is characterised by the closure of the visceral peritoneum
compared to the Misgav Ladach or Stark method, in which no suturing
of the vesicouterine fold to the uterine serosa is required
(2).
The present study describes a case which emphasises
the significant challenges in the management of patients with
post-caesarean bladder flap haematoma. At the same time, it is
highlighted that, despite its rarity, the association of
hydroureteronephrosis and post-caesarean bladder flap hematoma
without closure of the visceral peritoneum is necessary to be
included in the differential diagnosis of a puerperant presenting
signs of intra-abdominal infection in the immediate post-operative
period, even when this is not accompanied by hemodynamic
instability. Furthermore, it is underlined that early diagnosis and
appropriate treatment can reduce maternal morbidity and mortality
significantly.
Case report
A primiparous pregnant woman, 19 years of age, with
inadequate prenatal care and a free personal medical history, at
the 40th gestational week, underwent an emergency caesarean
section. The patient visited the Gynaecology Outpatient Clinic of
the Hospital of Trikala for the first time and had inadequate
prenatal care. She did not provide any previous tests that may have
been performed during the pregnancy. She also reported that she had
not undergone either a first trimester ultrasound nor 2nd level
ultrasound. She had not performed a doppler or specific blood tests
as a glucose challenge test. A foetal biometry during the
ultrasound performed at the Gynaecology-Obstetrics Outpatient
Clinic of the Hospital of Trikala revealed that the estimated
foetal weight (EFW) was below the 10th percentile and also revealed
that the patient had oligohydramnios. The cardiotocography was
non-reassuring and revealed a pattern of chronic hypoxia. The
aforementioned findings were suggestive of possible foetal growth
restriction. The pregnant woman was not in labour and she did not
have ruptured membranes. A vaginal culture collected from the
patient was negative for group B Streptococcus. The pregnant
woman had no fever pre-operatively. Indications for performing the
caesarean section were signs of chronic foetal hypoxia
(oligohydramnios, non-reassuring cardiotocography pattern) combined
with the low Bishop Score of the pregnant woman and the assessed
foetal growth restriction. Intraoperatively, after suturing the
Kerr incision of the uterus and following the careful haemostasis
in the area of the vesicouterine pouch, the vesicouterine fold was
not re-sutured. The estimated intraoperative blood loss from the
caesarean section was ~500 cc. A healthy male neonate with a body
weight of 2,450 g was successfully born. There was no puncture or
incision of the uterine artery during the caesarean section. After
suturing the uterine incision and before the abdominal wall was
closed, a careful overview was made for any bleeding from the Kerr
incision, and no active bleeding was found. On post-operative day
3, the puerperant developed fever up to 38.2˚C and atypical
abdominal pain. Characteristically, continuous severe pain was
reported by the patient, localized mainly in the right renal
region. Fever and pain were accompanied by a marked increase in the
levels of inflammatory markers (white blood cell count,
17.2x103/ml; neutrophil value, 76.4%; C-reactive
protein, 23 mg/dl; erythrocyte sedimentation rate, 95 mm/h). The
haemodynamic status of the puerperant was stable (haematocrit,
35.6%; haemoglobin, 11.7 mg/dl). The results of coagulation tests,
urinalysis and renal function tests were within normal range. A
blood culture was performed as part of the fever evaluation, which
yielded negative results.
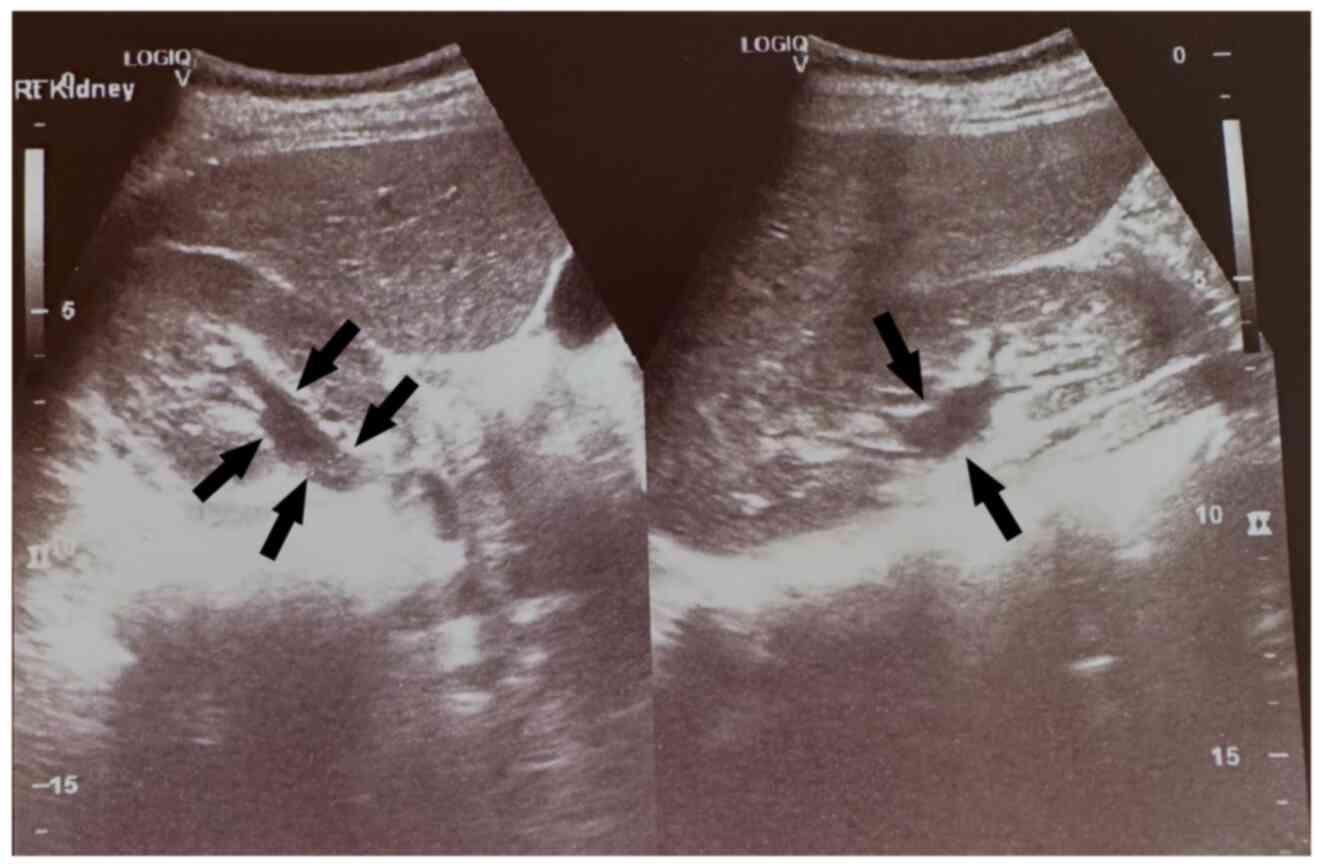
During the diagnostic evaluation of possible
intra-abdominal infection by transvaginal ultrasound, extensive
fluid collection with solid components in the vesicouterine pouch
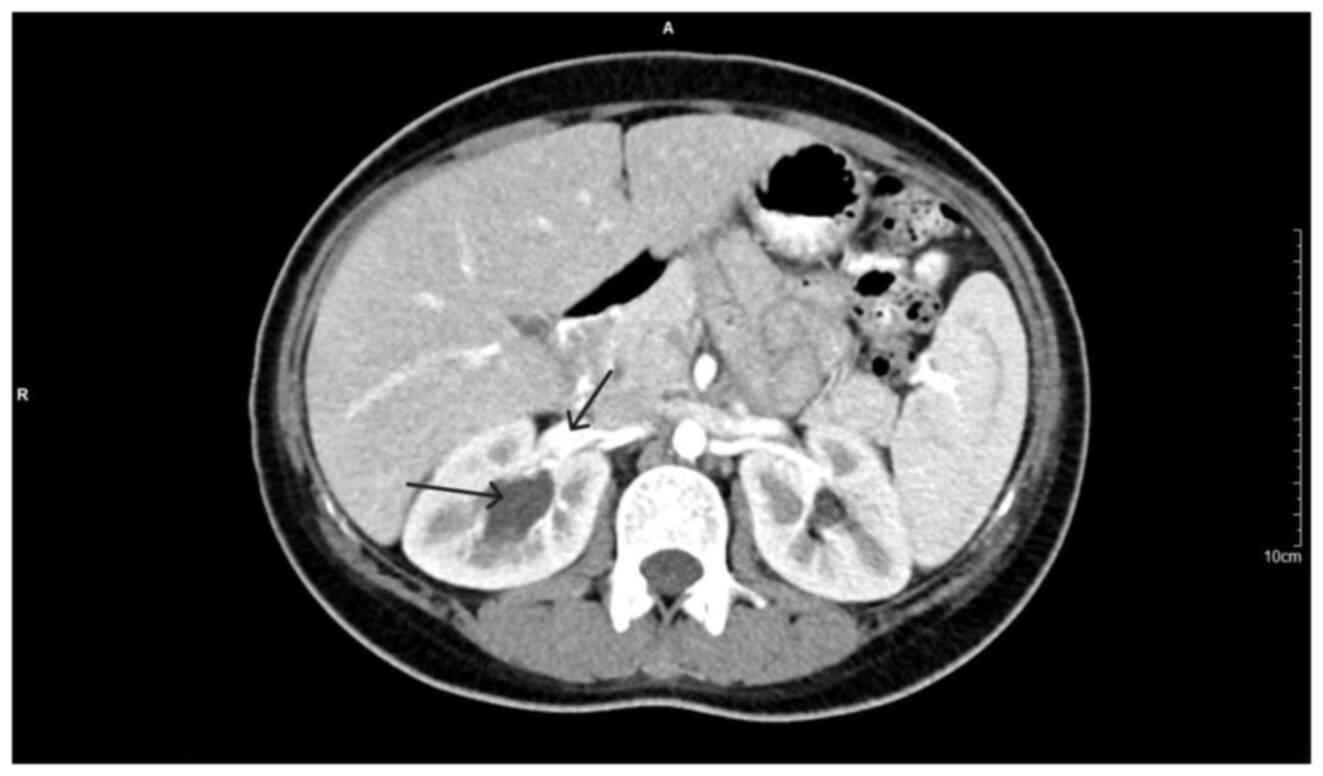
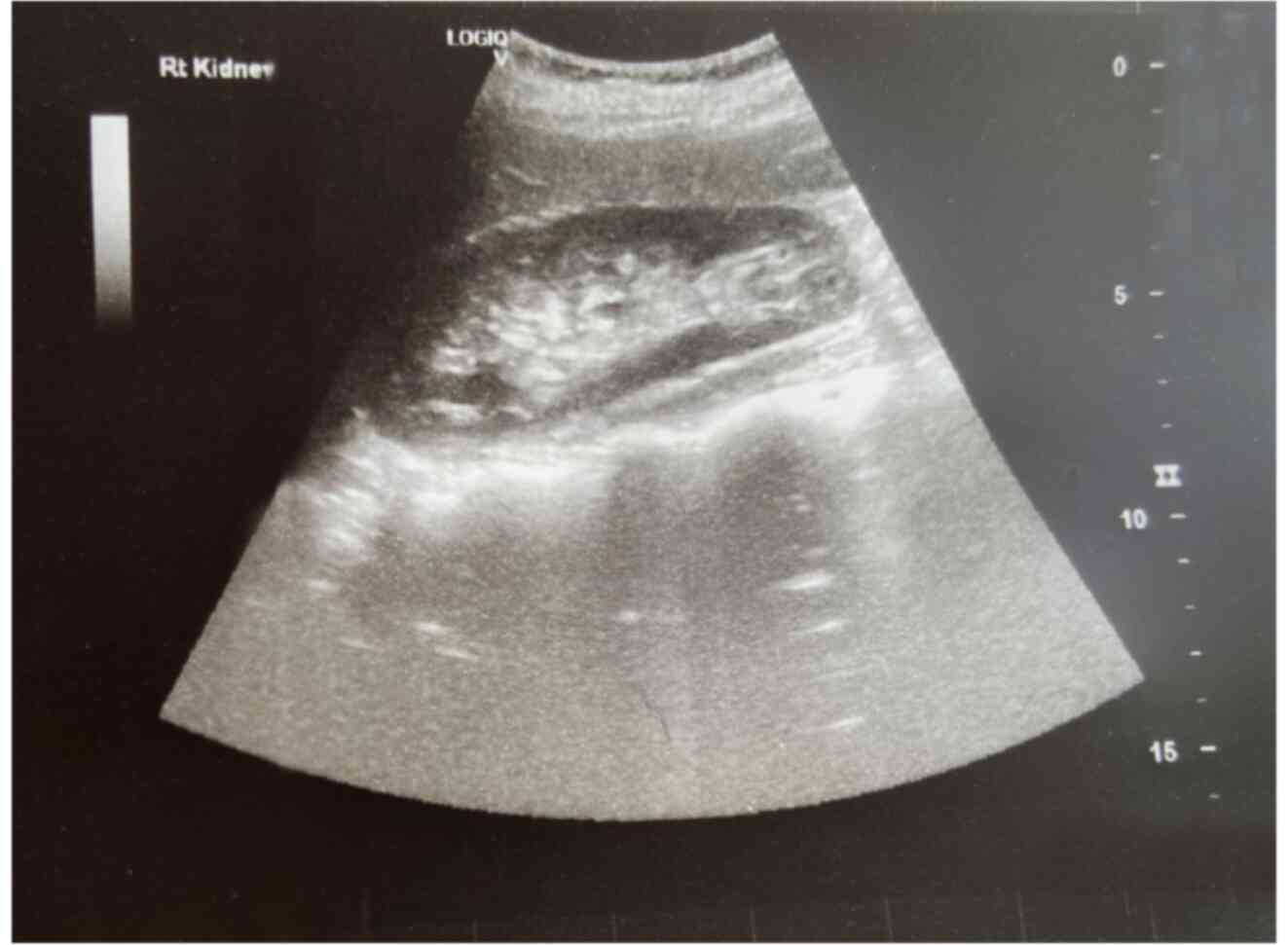
along the uterine incision was found (Fig. 1). In addition, ultrasound of the
urinary tract revealed moderate pelvicalyceal system dilatation on
the right kidney and the ipsilateral proximal ureter without the
presence of urolithiasis (Fig. 2). A
previous renal ultrasound performed at 35th gestational week and
provided by the patient did not reveal any abnormal imaging
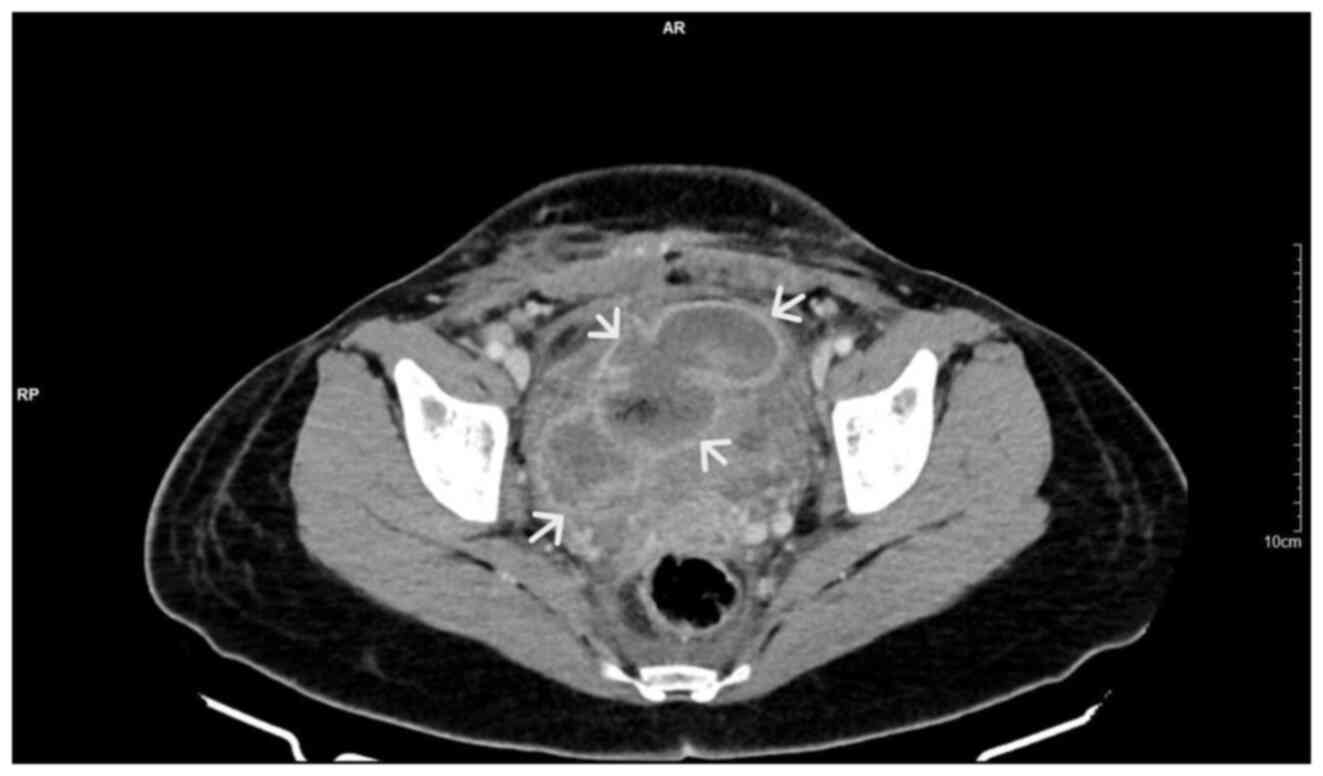
findings. The computed tomography scan confirmed the findings of
the ultrasound. In the area of the vesicouterine pouch, an
encapsulated fluid collection was found resembling a haematoma,
with dimensions of 110x55 mm and with extensive retroperitoneal
extension in the right parametrium (Fig.
3). In addition, the typical dilatation of the right
pelvicalyceal system and the ipsilateral proximal ureter was
observed (Fig. 4). No arteriogram or
venogram was performed as this diagnostic test was not available at
the authors' hospital.
For the treatment of the intra-abdominal infection,
it was initially decided to intravenously administer a double
antibiotic treatment of tigecycline 100 mg/12 h (this antibiotic is
effective in complicated intra-abdominal infections) (3) and tazobactam-piperacillin 4 g/8 h, as a
broad-spectrum antibiotic. However, as there was no improvement in
the patient's clinical condition and taking into consideration the
high levels of inflammatory markers of revealed by the blood test
results, it was decided to perform a laparotomy on 10th
post-operative day following the caesarean section.
Intraoperatively, a large bladder flap hematoma was found with
retroperitoneal extension to the right parametrium. There were no
macroscopic findings consistent with an abscess. A sample of the
hematoma was collected for a culture test, which was negative.
Drainage of the haematoma was performed, washing away the area with
normal saline (0.9%,). A careful overview of the integrity of the
incision on the uterine wall and thorough haemostasis were also
made. Suction drainages were placed in the vesicouterine pouch and
in the pouch of Douglas.
During the immediate post-operative period,
remission of the fever and a gradual improvement in the levels of
inflammation markers were observed (white blood cell count,
8x103/ml; neutrophil value, 68.2%; C-reactive protein,
3.1 mg/dl; erythrocyte sedimentation rate, 15 mm/h). The patient
was discharged from the clinic on the 5th post-operative day
following the re-operation, and underwent a consultation for
re-examination at the gynaecology Outpatient Clinic of Trikala. At
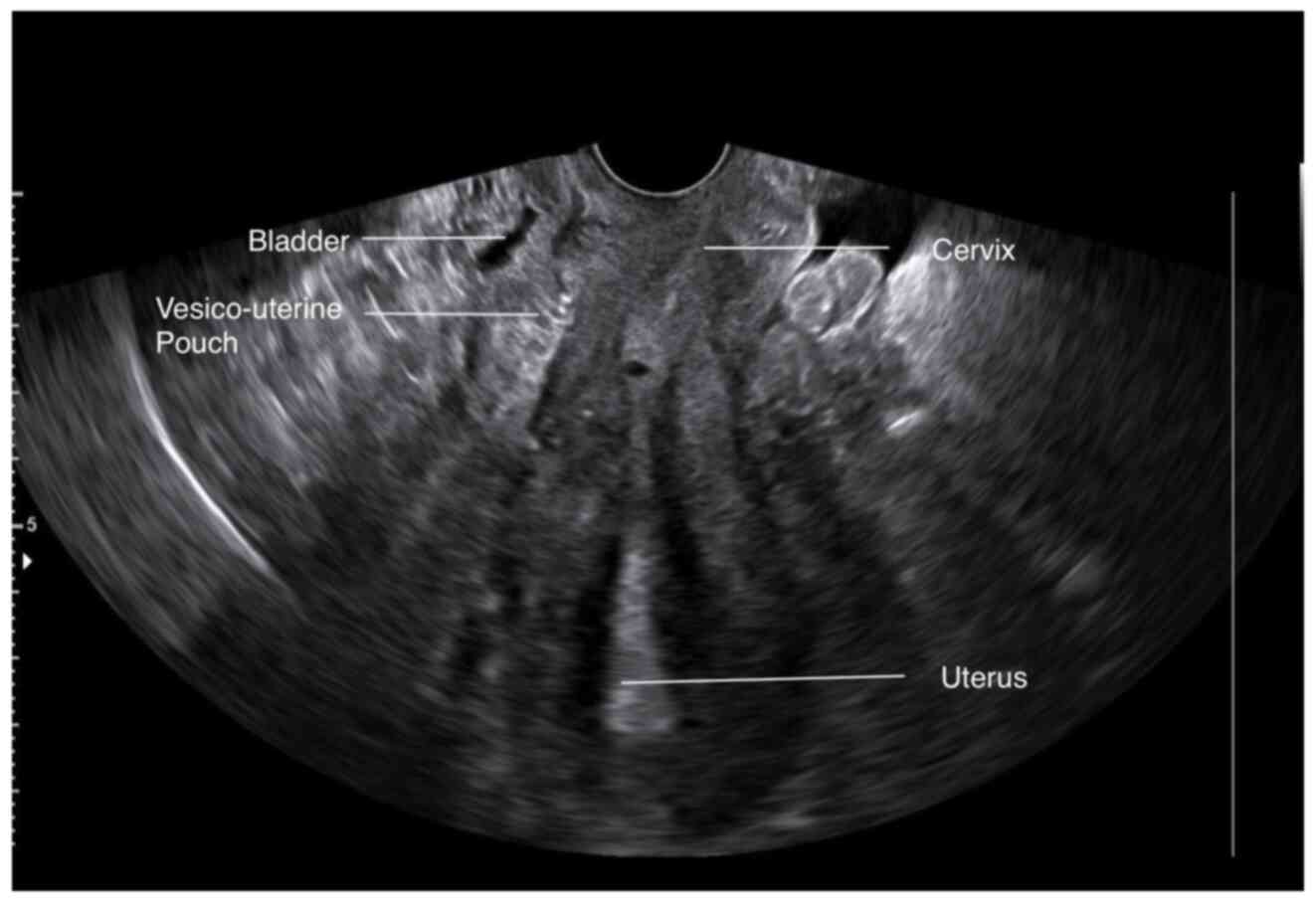
20 days after the re-operation, an ultrasound of the patient
revealed that the bladder flap hematoma had been completely
absorbed (Fig. 5). The complete
repair of the dilatation of the right pelvicalyceal system and the
ipsilateral ureter was also observed (Fig. 6). Τhe patient was provided with a
thorough consultation about the difficulties that may arise during
the next caesarean section and the fact that a general surgeon or a
gynaecologic oncologist may be required.
Discussion
The clinical diagnosis of post-caesarean section
bladder flap haematoma is relatively difficult. The haemodynamic
instability of the puerperant with signs of hypovolemia (decrease
in haemoglobin levels, tachycardia, oliguria) and/or signs of
infection (pelvic pain, fever, leukocytosis) could be clinical
conditions and laboratory findings that support the formation of
bladder flap hematoma, but they are non-specific (4). Similarly, in the patient described
herein, despite the formation of a large bladder flap hematoma, the
hemodynamic status was stable. The decrease in haemoglobin levels
between the initial pre-operative blood tests and those of the
third post-operative day was 1.4 mg/dl. In addition, it was
uncommon that the formation of an encapsulated hematoma in the
vesicouterine pouch occurred after performing a caesarean section
without the closure of the visceral peritoneum. In similar cases,
the blood loss leaks into the peritoneal cavity, resulting in the
formation of a haemoperitoneum, rather than the formation of a
bladder flap haematoma. Furthermore, notable is the fact that the
lateral extension of the haematoma into the retroperitoneal space
of the right parametrium caused the extrinsic compression of the
right ureter, resulting in ipsilateral hydroureteronephrosis. To
date, at least to the best of our knowledge, there is no report
available in the worldwide literature that associates
hydroureteronephrosis with the formation of post-caesarean section
bladder flap hematoma.
In contrast to clinical conditions and laboratory
findings, the diagnosis of bladder flap haematoma is greatly
assisted by imaging. Upon an ultrasound, a non-specific solid mass
or a mass with solid and cystic components, the size of which
varies and may exceed 10 cm (as in the case in the present study),
is usually detected between the posterior bladder wall and the
anterior wall of the lower uterine segment. However, in any case,
the differentiation between a haematoma and an infected hematoma or
abscess may be difficult (5).
Computed tomography is the method of choice for the imaging of
severe post-operative intra-abdominal complications following
caesarean section, such as intra-abdominal haematomas, abscesses,
bladder flap haematomas, uterine dehiscence-rupture and pelvic
thrombophlebitis (6). The role of
magnetic resonance imaging is limited to those cases where it is
necessary to clarify ultrasound and computed tomography findings,
or when there is a strong contraindication to the use of contrast
media (7). However, regardless of
the imaging method used, it is considered that knowledge of the
normal post-operative pelvic anatomy is essential to assist in the
optimal timely diagnosis and appropriate management of the
complication, in order to avoid unnecessary surgical interventions
and adjunctive treatments (8).
To the best of our knowledge, there is no specific,
established treatment protocol for the management of bladder flap
haematoma available in the current literature. Conservative
management with administration of broad-spectrum antibiotics may be
the first treatment choice, particularly in patients who are
haemodynamically stable. A re-laparotomy to drain the haematoma may
be used in those cases where blood loss is severe or when the
formation of the haematoma is accompanied by clinical signs of
intra-abdominal infection that do not respond to appropriate
antibiotic treatment (2). In a
previous study, the rate of re-laparotomy following caesarean
section was estimated at 1.04%, with a high maternal mortality rate
that reached 11.4% (9). The main
indication for re-operation was intra-abdominal bleeding (41.7%).
This was followed by haematomas and intra-abdominal infections with
rates of 29.2 and 7.7%, respectively. Re-laparotomy for the
treatment of bladder flap haematoma was not reported (9). In a recent study, active bleeding was
the cause of ~78% of re-operations in puerperants who underwent
caesarean section. Placenta previa and an emergency caesarean
section, particularly when performed during the second stage of
labour, have been found to be the main risk factors for
re-laparotomy following caesarean section (10). In the present study, as the patient
had no risk factors for haemorrhage, the bladder flap hematoma was
treated by laparotomy due to the non-responsiveness of the patient
to antibiotic treatment (persistent fever and continued increase in
inflammation markers). Laparoscopy was not available at the
authors' hospital.
Laparoscopic surgery in well-organised and
experienced centres is currently an excellent minimally invasive
and safe treatment option for the drainage of the bladder flap
haematoma and the management of other pelvic haematomas and
abscesses. It is considered that laparoscopy for the management of
bladder flap haematoma is easier and has higher success rates in
those cases where no visceral peritoneal closure has been performed
(2). In addition, percutaneous
aspiration or surgical transvaginal evacuation may be an
alternative conservative treatment option for the management of
small pelvic haematomas. Hysterectomy may be considered in cases of
sepsis with severe uterine necrosis and irreversible endometritis
with formation of extensive multiple abscesses (4,11).
Finally, it is useful to emphasise that despite the
widespread use of caesarean section in recent decades, there is no
consensus available to date on the optimal surgical technique to be
used to minimise complications of the operation, at least to the
best of our knowledge. The intraoperative thorough control of
haemostasis and post-operative universal antibiotic administration
constitute the basis of prophylactic measures to prevent
post-operative haemorrhagic complications following caesarean
section (4). In addition, the
non-closure of the visceral peritoneum after suturing the uterine
incision allowing the vesicouterine pouch to communicate with the
peritoneal cavity may be a recommendation to avoid formation of
bladder flap hematoma (12).
Furthermore, eschewing superficial incising and dissecting the
peritoneal lining to separate the urinary bladder from the lower
uterine segment before uterine incision, which results in the
avoidance of bladder flap formation, may currently be a weak
recommendation to prevent bladder flap haematoma and reduce
maternal morbidity after performing a caesarean section (12).
In conclusion, post-caesarean section bladder flap
haematoma without suturing the visceral peritoneum is a rare
postpartum complication. The extensive lateral extension of the
haematoma into the retroperitoneal space of the parametrium and its
association with hydroureteronephrosis due to extrinsic compression
of the distal ureter is a unique case report in the international
literature. Despite its rarity, the bladder flap hematoma should be
included in the differential diagnosis of puerperant presenting
signs of intra-abdominal infection, with or without hemodynamic
instability, in the immediate post-operative period following a
caesarean section, with the aim of reducing maternal morbidity and
mortality.
Acknowledgements
The authors would like to thank the doctors from the
Radiology Department and the doctors from the Anaesthesiology
Department of the General Hospital in Trikala (Greece) for their
important assistance in the patient's management.
Funding
Funding: No funding was received.
Availability of data and materials
The data used in the current study are available
from the corresponding author upon reasonable request.
Authors' contributions
All authors (ET, AT, EK, IP, VG, EEG and IT)
participated in the preparation of the manuscript and in the final
approval of the manuscript. ET and AT participated in the
conception and design of the study, in the writing of the
manuscript and in final approval of the manuscript. EK and IP were
involved in the conception and design of the study, in the
provision of study materials (such as blood tests, culture test,
imaging) or patient data, in data collection and aggregation, data
analysis and interpretation, and in the final approval of the
manuscript. VG and EEG were involved in the provision of study
materials (such as blood tests, culture test, imaging) or patient
data, patient care, data collection and aggregation, data analysis
and interpretation, and in the final approval of the manuscript. IT
was involved in the conception and design of the study, in
administrative support, in the provision of study materials (such
as blood tests, culture test, imaging) or patient data, in patient
care, in data collection and analysis, in manuscript writing, and
in the final approval of the manuscript. EK and IP confirm the
authenticity of the raw data. All authors have read and approved
the final manuscript.
Ethics approval and consent to
participate
The present study was conducted according to the
guidelines of the Declaration of Helsinki. Written informed consent
was obtained from the patient.
Patient consent for publication
Written informed consent was obtained from the
patient for publication of her data and any related images in the
present case report.
Competing interests
The authors declare that they have no competing
interests.
References
|
1
|
Sandall J, Tribe RM, Avery L, Mola G,
Visser GH, Homer CS, Gibbons D, Kelly NM, Kennedy HP, Kidanto H, et
al: Short-term and long-term effects of caesarean section on the
health of women and children. Lancet. 392:1349–1357.
2018.PubMed/NCBI View Article : Google Scholar
|
|
2
|
Malvasi A, Tinelli A, Tinelli R, Rahimi S,
Resta L and Tinelli FG: The post-cesarean section symptomatic
bladder flap hematoma: A modern reappraisal. J Matern Fetal
Neonatal Med. 20:709–714. 2007.PubMed/NCBI View Article : Google Scholar
|
|
3
|
Yaghoubi S, Zekiy AO, Krutova M, Gholami
M, Kouhsari E, Sholeh M, Ghafouri Z and Maleki F: Tigecycline
antibacterial activity, clinical effectiveness, and mechanisms and
epidemiology of resistance: narrative review. Eur J Clin Microbiol
Infect Dis. 41:1003–1022. 2022.PubMed/NCBI View Article : Google Scholar
|
|
4
|
Lata K, Davis AA, Panwar A, Kriplani I and
Kriplani A: Laparoscopic management of post-cesarean uterovesical
abscess: A new approach to an old problem. J Obstet Gynaecol India.
71:313–317. 2021.PubMed/NCBI View Article : Google Scholar
|
|
5
|
Baker ME, Bowie JD and Killam AP:
Sonography of post-cesarean-section bladder-flap hematoma. AJR Am J
Roentgenol. 144:757–759. 1985.PubMed/NCBI View Article : Google Scholar
|
|
6
|
Sierra A, Burrel M, Sebastia C, Radosevic
A, Barrufet M, Albela S, Buñesch L, Domingo MA, Salvador R and Real
I: Utility of multidetector CT in severe postpartum hemorrhage.
Radiographics. 32:1463–1481. 2012.PubMed/NCBI View Article : Google Scholar
|
|
7
|
Lee NK, Kim S, Lee JW, Sol YL, Kim CW,
Hyun Sung K, Jang HJ and Suh DS: Postpartum hemorrhage: Clinical
and radiologic aspects. Eur J Radiol. 74:50–59. 2010.PubMed/NCBI View Article : Google Scholar
|
|
8
|
Gui B, Danza FM, Valentini AL, Laino ME,
Caruso A, Carducci B, Rodolfino E, Devicienti E and Bonomo L:
Multidetector CT appearance of the pelvis after cesarean delivery:
Normal and abnormal acute findings. Diagn Interv Radiol.
22:534–541. 2016.PubMed/NCBI View Article : Google Scholar
|
|
9
|
Raagab AE, Mesbah YH, Brakat RI, Zayed AA
and Alsaammani MA: Re-laparotomy after cesarean section: Risk,
indications and management options. Med Arch. 68:41–43.
2014.PubMed/NCBI View Article : Google Scholar
|
|
10
|
Weissmann-Brenner A, Barzilay E, Meyer R,
Levin G, Harmatz D, Alakeli A, Domniz N and Yoles I: Relaparotomy
post-cesarean delivery: Characteristics and risk factors. Arch
Gynecol Obstet. 304:1427–1432. 2021.PubMed/NCBI View Article : Google Scholar
|
|
11
|
Tinelli A, Malvasi A and Vittori G:
Laparoscopic treatment of post-cesarean section bladder flap
hematoma: A feasible and safe approach. Minim Invasive Ther Allied
Technol. 18:356–360. 2009.PubMed/NCBI View Article : Google Scholar
|
|
12
|
Sentilhes L, Schmitz T, Madar H,
Bouchghoul H, Fuchs F, Garabédian C, Korb D, Nouette-Gaulain K,
Pécheux O, Sananès N, et al: The cesarean procedure: Guidelines for
clinical practice from the French college of obstetricians and
gynecologists. Gynecol Obstet Fertil Senol. 51:7–34.
2023.PubMed/NCBI View Article : Google Scholar : (In French).
|