Introduction
Severe acute pancreatitis (SAP) is a severe systemic
disease that can lead to local and systemic life-threatening
complications. Cognitive impairments induced by SAP, otherwise
known as pancreatic encephalopathy (PE), are severe complications
that significantly contribute to the increased mortality rate of
patients with SAP (1). The
mortality rate of patients with SAP accompanied with PE may reach
67–100% (2). Improvement of
SAP-induced cognitive impairments is important in order to decrease
mortality associated with SAP. Diagnoses of SAP-induced cognitive
impairments are challenging, as they predominantly depend upon the
exclusion of all other underlying conditions that exhibit similar
symptoms (1). The exact etiology
of PE and the functional brain area affected by PE remain unknown,
and, to the best of our knowledge, there have been no previous
studies that have investigated effective therapeutic strategies for
the treatment of SAP-induced cognitive impairments.
During the development of SAP, inflammatory
mediators have a critical role in SAP-associated pathogenesis,
which not only aggravate pancreatic injury, but also contribute to
the subsequent systemic inflammatory response syndrome and multiple
organ dysfunction syndrome (3).
The pathological sequelae of SAP are regulated by inflammatory
mediators, including proinflammatory cytokines, such as tumor
necrosis factor (TNF)-α and interleukin (IL)-1β; anti-inflammatory
cytokines, such as IL-10 and IL-13; and numerous endogenous
regulators, such as heme oxygenase 1 and its by-product, carbon
monoxide (4,5). It has been well established that
neuroinflammation significantly contributes to brain damage, during
which astrocytes and microglia are activated and proinflammatory
cytokines are released, including IL-1β, TNF-α and cytokine
receptors, from endothelial cells and immune cells (6). Development of a neuroprotective drug
with anti-inflammatory properties may represent a potential
therapeutic strategy for the treatment of patients with PE.
Berberine is an isoquinoline alkaloid that is
extractable from the Chinese herb, Coptis rhizome, and has been
widely used as a traditional drug in China. Coptis rhizome exhibits
numerous biological effects, including anti-inflammatory,
anti-oxidative, anti-bacterial and anti-apoptotic effects, and is
able to scavenge free radicals (7,8).
Studies have revealed that berberine exhibits neuroprotective
effects on spatial memory impairment when administered to rat
models of Parkinson's disease (9)
and diabetes (10). Recently, it
has been reported that treatment with berberine may have
therapeutic effects against status epilepticus and spontaneous
recurrent seizures in intrahippocampal kainate models of epilepsy,
as well as exerting neuroprotective effects, primarily via
suppression of oxidative stress and neuroinflammation, and
potentially via suppression of apoptosis (11). However, to the best of our
knowledge, the effect of berberine on SAP-induced cognitive
impairments in rats has not yet been investigated. The present
study hypothesized that berberine may attenuate SAP-induced
cognitive deficits. Furthermore, the present study aimed to
determine the underlying mechanisms of PE.
Materials and methods
Animals
The present study was approved by the Institutional
Animal Experimental Ethics Committee of Sichuan University
(Chengdu, China). Adult male Wistar rats (n=128; age, 3 months old;
body weight, 200–300 g) were purchased from the Experimental Animal
Centre of West China, Centre of Medical Sciences of Sichuan
University (Chengdu, China) and were used in the present study.
Animals were housed in cages under a 12-h light/dark cycle, with
free access to food and water. The temperature of the cages were
maintained at 21–25°C with 50–60% humidity. To reduce the potential
influences of sex differences (12) and transportation (13) on cognitive assessment, only male
rats were used in the present study, which were transferred from
the rearing room into the behavioral testing room at least 30 min
prior to the initiation of each experiment.
Experimental design
Rats were randomly divided into four groups (n=32
per group): Sham group, Sham + berberine group, SAP group and SAP +
berberine group. The SAP model was induced via two intraperitoneal
injections of 3 g/kg L-arginine (dissolved in normal saline, 1:5,
w/v; Sigma-Aldrich; Merck KGaA, Darmstadt, Germany) at an interval
of 1 h (14), whereas rats in the
sham groups received equivalent volumes of a saline vehicle.
Following the second injection of L-arginine, 100 mg/kg berberine
(15) (dissolved in 1 ml normal
saline/200 g body weight; Sigma-Aldrich; Merck KGaA) was
administered immediately and then once a day for 6 consecutive
days. A total of 48 h after the 2nd injection of L-arginine was
administered, disease severity of SAP was assessed. A total of 7
days post-SAP induction, the survival rates of rats were calculated
and behavioral tests were subsequently performed. Furthermore,
surviving rats were sacrificed and hippocampal tissues were
isolated for subsequent biochemical analysis.
Assessment of SAP disease
severity
A total of 48 h post-SAP induction, rats were
sacrificed via i.p. injection of 2% sodium pentobarbital (100
mg/kg; Sigma-Aldrich; Merck KGaA) and pancreatic tissues were
removed and subsequently fixed in 10% neutral buffer formaldehyde
at room temperature for 24 h. Subsequently, tissues were embedded
in paraffin and sectioned. The tissue sections (1 mm3)
were then stained using hematoxylin and eosin, and were observed
under light microscopy. Histological alterations were assessed
using a previously established histopathological scoring system
(16) with slight modifications:
For each pathological section, ten visual fields were randomly
selected, visualized under a high-power microscope (magnification,
×100) and then blindly scored by a pathologist. The overall score
was presented as the sum of severity of inflammation, extension of
inflammation (none, 0; slight, 1; moderate, 2; and severe, 3) and
fat/acinar necrosis (none, 0; basal 1/3 damaged, 1; basal 2/3
damaged, 2; only surface epithelium intact, 3; and transmural, 4).
In addition, disease severity of SAP was also assessed by measuring
the levels of serum amylase. Blood samples were centrifuged at 3000
× g at 4°C for 10 min and serum amylase was subsequently determined
by routine colorimetric methods using a commercial kit (cat. no.
C016; Nanjing Jiancheng Bioengineering Institute, Nanjing, China)
and expressed as U/L.
Locomotor activity assessment
To investigate locomotor activity, which may affect
the results of cognitive assessment, an automated rotarod (cat. no.
47750; Ugo Basile SRL, Gemonio, Italy) was used to ensure locomotor
activity of rats was completely recovered following the induction
of SAP. Locomotor activity assessment was conducted twice, with an
accelerating rotational speed of 0.2 rotations/sec (from 4–40 rpm),
including two consecutive training trials and one testing trial.
One test was performed prior to SAP induction (the baseline
latency) and the other was performed on the 7th day prior to
cognitive assessment. A blinded observer recorded the average time
spent on the bar, which was considered to represent the latency to
fall from the rod, with a 10 min interval between each trial in one
test.
Fear conditioning test (FCT)
On the next day following locomotor activity
assessment, FCT was performed using a dedicated conditioning
chamber (cat. no. 46000; Ugo Basile SRL) as previously described
(13) with modifications,
including training, context testing and cued testing. During the
training period in FCT, rats were placed in the conditioning
chamber and were permitted to explore the training environment for
5 min. Following this, an auditory cue (2500 Hz, 75 dB) was
presented for 2.5 sec as a conditioned stimulus (CS) that
co-terminated with a 0.5 mA electric foot shock, which represented
an unconditioned stimulus (US) during the last 2 sec of the
auditory cue. Following a 57.5 sec inter-trial interval, the
pairing of the auditory cue and the foot shock (CS-US) was again
administered and repeated a further 15 times. A total of 24 h
post-CS-US testing, all rats were placed back in the same chamber
to investigate long-term memory. During the context test, which
investigates hippocampus-dependent memory, rats were permitted to
freely explore the chamber for 10 min in the absence of CS and US
stimulation. Following this, the cued test was performed to
determine hippocampus-independent memory functioning, in which rats
were placed in a novel context environment with altered olfactory
cues and lighting, as well as the attachment of patterned contexts
on the walls and floor, received an auditory cue (2500 Hz, 75 dB),
10 times at 57.5 sec time intervals, without the foot shock.
Cognitive deficit was investigated via determination of the
percentage of time spent completely immobilized except for
respiration, which was automatically recorded by a digital
video-tracking system.
Blood brain barrier (BBB)
permeability
A total of 48 h post-SAP induction, 3 ml/kg 2% Evans
blue (EB) dye in PBS was administrated into the tail vein to
evaluate the integrity of the BBB. A total of 1 h
post-administration, rats were sacrificed via i.p. injection of 2%
sodium pentobarbital (100 mg/kg) and perfused through the left
heart ventricle with PBS until the outflow from the right auricle
was colorless. Following this, brain tissues were harvested and
homogenized in formamide solution buffer and then centrifuged at
10,000 × g for 20 min at 4°C. The extracted supernatant was
investigated at a wavelength of 655 nm using a spectrophotometer
based on external standards in the same solvent as the control, and
data are expressed as ng/mg of total brain tissue.
ELISA
Following cognitive assessment, rats were sacrificed
via i.p. injection of 2% sodium pentobarbital (100 mg/kg). The
brains of each group were harvested and hippocampal tissues were
isolated, which were subsequently snap-frozen in liquid nitrogen
and stored at −80°C prior to further experimentation. Levels of
TNF-α (cat. no. CSB-E11987r; Cusabio Biotech Co. Ltd., Wuhan,
China) and IL-1β (cat. no. CSB-E08055r, Cusabio Biotech Co. Ltd.,
Wuhan, China) were determined by ELISA in accordance with the
manufacturer's protocols. Briefly, the stored brain tissues were
homogenized in normal saline using a sonicator (120 times; 1 time
for 0.8 sec, then 1 sec with 2 sec intervals) at room temperature,
and the supernatants were subsequently harvested and centrifuged at
3000 × g for 15 min at 4°C. The supernatant was subsequently
collected and incubated with biotinylated antibodies (included in
the ELISA kits) for 30 min at 37°C. Subsequently, the supernatant
was incubated with streptavidin-horseradish peroxidase solution for
1 h at 37°C and the protein concentrations were subsequently
quantified using the Bradford protein assay (cat. no. P0010;
Beyotime Institute of Biotechnology, Haimen, China). Following
incubation with supplied chromogen solution and stop solution,
protein concentrations were determined at an absorbance of 450 nm.
Levels of TNF-α and IL-1β were calculated using a standard curve
and expressed as pg/ml.
Western blotting
Following cognitive assessment, rats were sacrificed
via i.p. injection of 2% sodium pentobarbital (100 mg/kg).
Hippocampal tissues were harvested following cognitive assessments
to investigate the protein expression levels of anti-cleaved
caspase-3 (1:500; cat. no. 9661; Cell Signaling Technology, Inc.,
Danvers, MA, USA), anti-receptor-interacting protein kinase (RIP)1
(1:750; cat. no. ab106393; Abcam, Cambridge, UK) and anti-RIP3
(1:750; cat. no. ab62344; Abcam) via western blotting. Briefly, the
frozen hippocampal tissue samples were homogenized in cell lysis
buffer (Cell Signaling Technology, Inc.) The samples were then
centrifuged at 3000 × g for 15 min at 4°C, the supernatant was
collected and total protein concentrations of the supernatants were
determined using a Bradford protein assay (P0010, Beyotime
Institute of Biotechnology). Equal amounts of protein (0.1 mg/µl)
extracts were heated, denatured and separated by electrophoresis on
a NuPAGE 8–15% Bis-Tris gel (Invitrogen; Thermo Fisher Scientific,
Inc., Waltham, MA, USA) and subsequently transferred to
polyvinylidene difluoride membranes. Following blocking using 5%
non-fat dry milk for 90 min at room temperature, these membranes
were probed with primary antibodies overnight at 4°C and then
incubated with horseradish peroxidase-conjugated secondary
antibodies (1:5,000; cat. no. 7076; Cell Signaling Technology,
Inc.) for 1 h at room temperature. β-actin (1:1,000; cat. no. 8457;
Cell Signaling Technology, Inc.) was used as an internal
housekeeping protein. Proteins were visualized using an enhanced
chemiluminescence detection kit (cat. no. sc-2048; Santa Cruz
Biotechnology, Inc., Dallas, TX, USA) and densitometric analysis
was performed using ImageJ software (version 1.52; National
Institutes of Health, Bethesda, MD, USA).
Statistical analysis
Data are presented as the means ± standard error of
the mean of three repeated experiments, and were analyzed using
SPSS software (version 22.0; IBM Corp., Armonk, NY, USA). One-way
analysis of variance followed by the Bonferroni test was used to
analyze the differences among the groups. Survival rates were
analyzed using the Kaplan-Meier method and subsequently compared
using the log-rank test. P<0.05 was considered to indicate a
statistically significant difference.
Results
Berberine attenuates the severity of
SAP and improves survival in SAP rats
It has been reported that repeated injections with
high doses of L-arginine may induce AP in rodents with
well-defined, gradually progressive pancreatic necrosis (14). In the present study, L-arginine was
used to induce SAP, and disease severity was assessed by
investigating alterations in pancreatic histopathology and serum
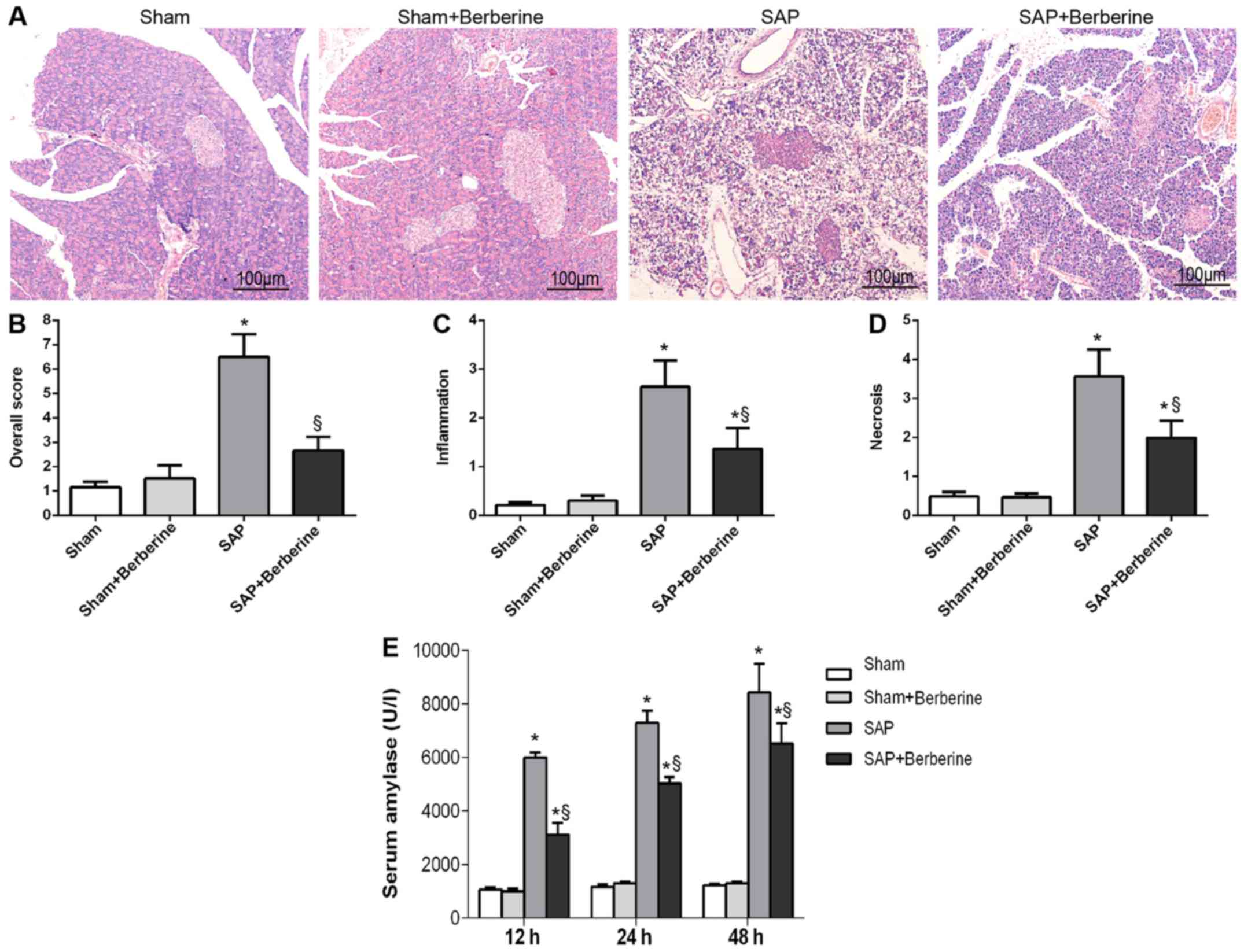
amylase levels. Following treatment with L-arginine for a total of
48 h, all typical features of SAP, including significant isolation
of pancreatic lobes, marked inflammatory cell infiltration,
hemorrhaging and acinar cell necrosis, were observed in the SAP
group (Fig. 1A). Following
treatment with berberine, pancreatic morphology was markedly
attenuated in the SAP + berberine group compared with the SAP group
(Fig. 1A). These pancreatic
morphological alterations at 48 h were reflected by the pancreatic
histopathological scores (Fig.
1B-D). Pancreatic tissues obtained from the SAP + berberine
group exhibited a significantly decreased overall histopathological
score compared with the SAP group (mean score, 2.66 vs. 6.49;
P<0.05; Fig. 1B), and
significantly decreased neutrophil infiltration and acinar necrosis
scores compared with the SAP group (Fig. 1C and D). As presented in Fig. 1E, serum amylase levels were
significantly increased in the SAP group compared with the Sham
group, and significantly decreased in the SAP + berberine group
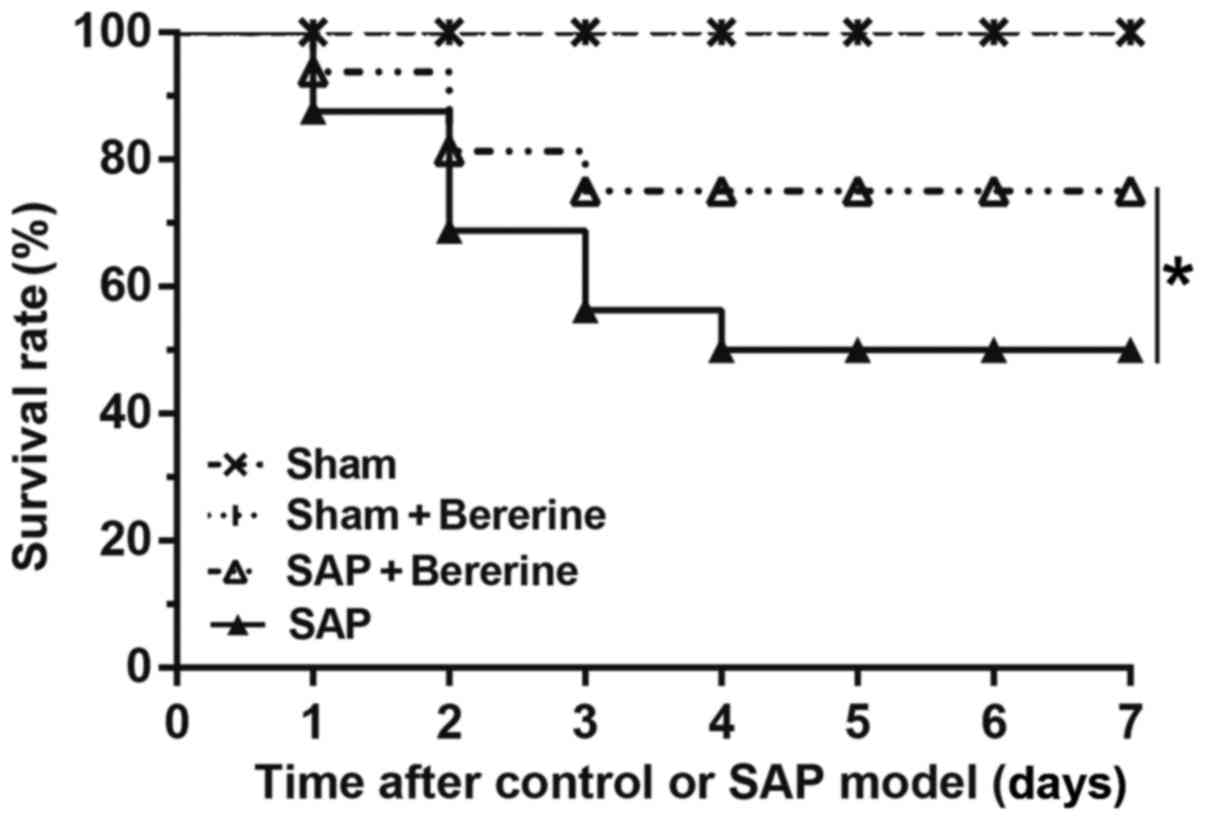
compared with the SAP group. In the present study, the survival
rate of rats in the SAP group over the 7 day time period was
investigated, and the results revealed that the survival rate of
rats with SAP was ~50%, which was consistent with the findings of a
previous study (17). Following
repeated treatment with berberine, there was a significant increase
in the survival rate of rats in the SAP + berberine group compared
with the SAP group (75 vs. 50%; Fig.
2; P<0.05).
Berberine attenuates cognitive
deficits in SAP rats
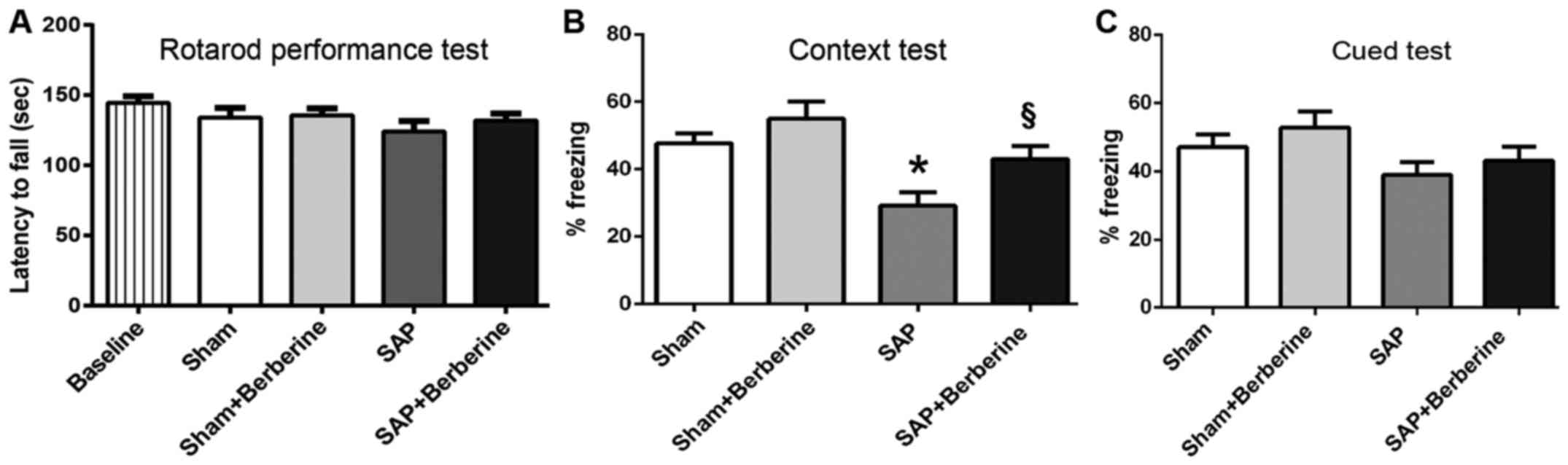
To ensure that the locomotor activity of rats was
completely recovered following SAP, an automated rotarod was used
to investigate the locomotor activity of rats, which may have
affected the results of cognitive assessment. Compared with the
baseline locomotor activity, there was no significant difference
among all groups prior to cognitive assessment (P>0.05; Fig. 3A). The clinical presentation of
cognitive impairments induced by SAP is not specific, and is
characterized by functional disabilities and long-term cognitive
impairment (2). In the present
study, FCTs were performed to investigate SAP-induced cognitive
impairments. The FCT is one of the most reliable and widely used
behavioral paradigms used to assess associative fear learning and
memory in rodents (13,18), which predominantly includes context
and cued FCTs. Context fear conditioning requires the presentation
of complex associations of stimuli and an aversive stimulus, which
is processed by the hippocampus. Therefore, context FCT is used to
investigate hippocampus-dependent memory, whereas cued FCT is
performed to investigate hippocampus-independent memory. The
results revealed that the freezing time exhibited by rats in the
SAP group during the context test was significantly decreased
compared with the Sham group, thus suggesting that SAP may induce
hippocampus-dependent long-term memory deficits, whereas this
effect was significantly attenuated following treatment with
berberine (Fig. 3B). In addition,
there were no significant differences in the freezing times
exhibited by rats in all four groups during the cued test (Fig. 3C), which suggested that the
hippocampus-independent memory of rats was not affected by SAP.
Berberine attenuates SAP-induced
increases in BBB permeability and inflammatory responses
BBB breakdown has been revealed to represent an
important factor associated with the development of
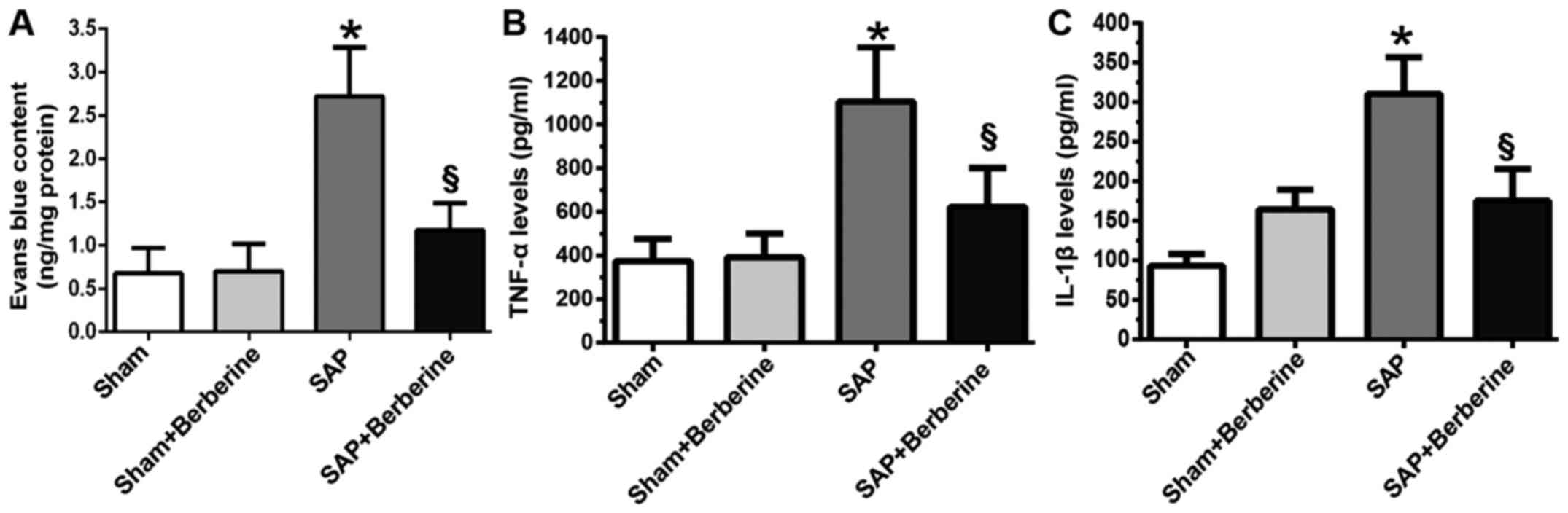
sepsis-associated cognitive impairment (19). The permeability of the BBB was
investigated via determination of EB content in rat brain tissues.
A total of 48 h post-induction of SAP, the rats in the SAP group
exhibited significantly increased levels of extravasation of EB
into brain tissues compared with the Sham group; however the
extravasation of EB was significantly decreased in the SAP +
berberine group compared with the SAP group (Fig. 4A).
Levels of TNF-α and IL-1β proinflammatory cytokines
in rat hippocampal tissues during the development of SAP were
investigated via ELISA analyses. The results revealed that levels
of TNF-α and IL-1β were significantly increased in the brain
tissues of rats in the SAP group compared with rats in the Sham
group. Therefore, the results suggested that treatment with
berberine attenuates elevated levels of IL-1β and TNF-α in rat
hippocampal tissues (Fig. 4B and
C).
Berberine attenuates increased levels
of proteins associated with neuronal apoptosis and necroptosis in
the hippocampal tissues of SAP rats
It has been well established that neuronal apoptosis
and necroptosis represent crucial factors associated with the
development of neurodegeneration during brain dysfunction (20,21).
To further investigate the hippocampus-dependent memory impairment
exhibited by rats in the SAP group, as demonstrated by the
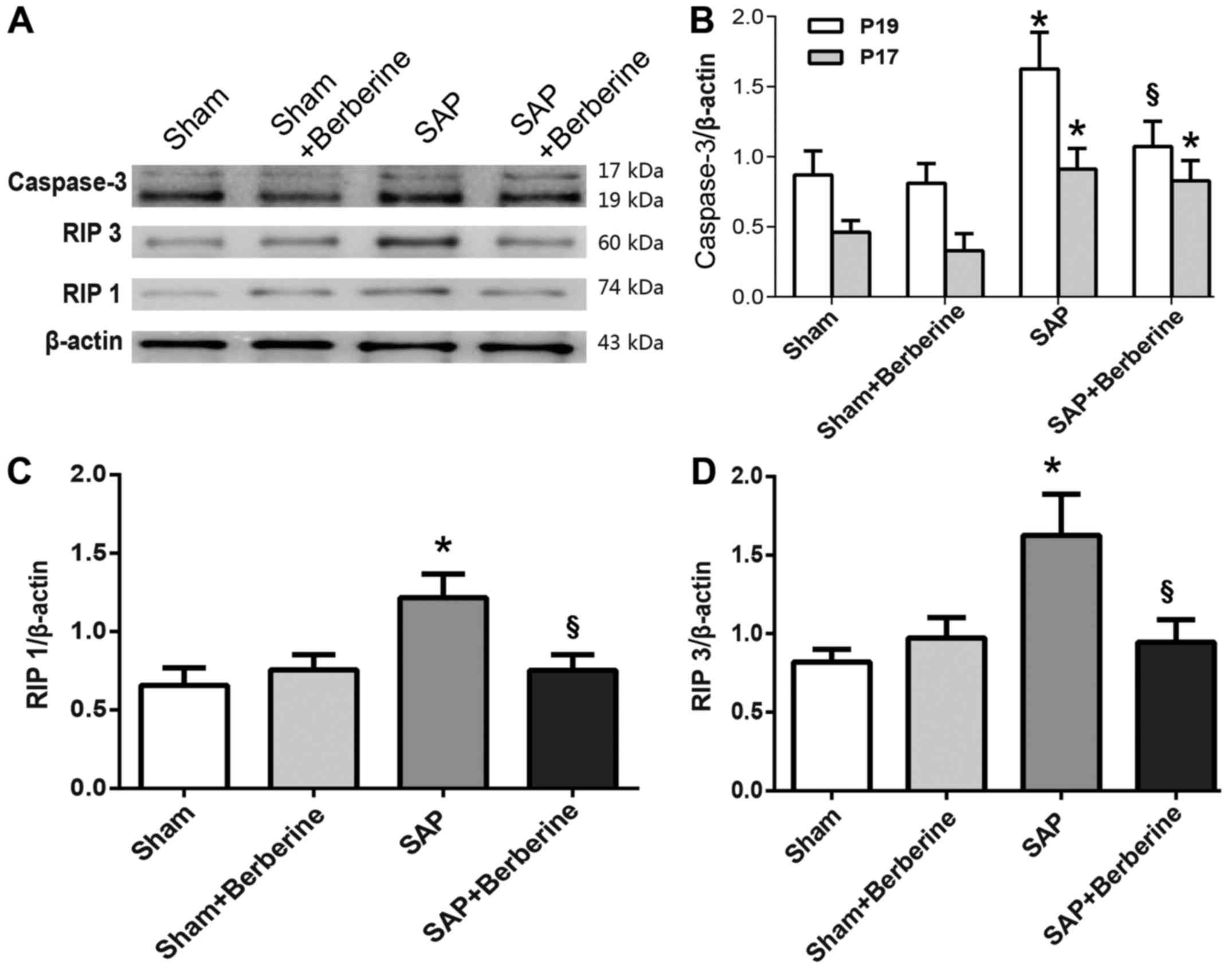
aforementioned FCT, western blotting was performed to determine the
expression levels of proteins associated with apoptosis and
necroptosis in hippocampal tissues (Fig. 5A). The results demonstrated that
the protein expression levels of caspase-3, an inducing apoptosis
effector, were significantly increased in the hippocampal tissues
of SAP rats compared with rats belonging to the Sham group;
however, this effect was significantly attenuated following
treatment with berberine (Fig.
5B). RIP1 and RIP3 are the predominant inducers of neuronal
necroptosis (22). In comparison
with the Sham group, SAP-induced rats exhibited significantly
increased expression levels of RIP1 and RIP3 in hippocampal
tissues. Notably, rats in the SAP + berberine group exhibited
significantly decreased expression levels of RIP1 and RIP3 in
hippocampal tissues compared with the SAP group (Fig. 5C and D).
Discussion
The present study investigated the effects of
berberine on cognitive impairments in a rat model of SAP. Berberine
was demonstrated to significantly attenuate cognitive deficits
induced by SAP. The protective effect of berberine may be
associated with suppression of inflammation and necroptosis in the
hippocampal tissues of rats with SAP. To the best of our knowledge,
the present study is the first to investigate the protective
effects of berberine on cognitive impairments using a SAP rat
model.
Clinical presentations of cognitive impairments
associated with SAP are variable among patients and diagnoses are
challenging (2). In addition, the
functional brain area affected by SAP has not been accurately
identified. Following investigations of hippocampus-dependent and
hippocampus-independent memory via context and cued testing,
respectively, the results revealed that the hippocampus, an
important brain region for learning and memory, was affected during
SAP. Although berberine may affect other areas of the brain
(9), the results of the present
study suggested that treatment with berberine may protect
hippocampal tissues from damage in rats with SAP.
Previous clinical and experimental studies have
demonstrated that inflammatory cytokines are involved in the
pathogenesis of cognitive impairments (23,24).
Systemic manifestations of SAP are regulated by numerous pro- and
anti-inflammatory cytokines (25,26).
During inflammatory responses, numerous type 2 anti-inflammatory
cytokines, such as IL-10 and IL-13, may inhibit the production of
TNF-α and IL-1β (25).
Furthermore, numerous endogenous regulators of IL-1, such as IL-1
Ra and IL-1 RII, may downregulate neuroinflammatory responses
(26), which may subsequently
attenuate cognitive impairment associated with SAP. In the present
study, the results demonstrated that levels of TNF-α and IL-1β
proinflammatory cytokines were significantly increased in the
hippocampal tissue of rats suffering from SAP. It has been reported
that the toll-like receptor (TLR)4-mediated nuclear factor (NF)-κB
signaling pathway is a potential important mediator in the
development of SAP (27,28). In the present study, treatment with
berberine attenuated hippocampal TNF-α expression levels in rats
suffering from SAP and exerted neuroprotective effects; these
findings suggested that the effects of berberine may be mediated by
the TLR4-mediated NF-κB signaling pathway in SAP model. Increased
proinflammatory cytokines that cross the BBB and enter
cerebrospinal fluid and interstitial fluid spaces of the brain may
directly interact with the central nervous system (CNS) and affect
its function. Tight junctions associated with the BBB have
important roles in the maintenance of a stable cerebral
microenvironment via regulation of the movement of molecules in and
out of the brain (29). In the
present study, BBB permeability was investigated using a large
molecule, EB, which could be excluded by the BBB under certain
physiological conditions. The results demonstrated that the
concentration of EB in the brain of rats with SAP was significantly
increased compared with the Sham group. Numerous studies have
revealed that dysfunction of the BBB may lead to brain edema,
destruction of the cerebral microenvironment and subsequent brain
damage (19,30). Consequently, BBB dysfunction has
been proposed to represent an important factor associated with the
development of PE (19,20,30).
In the present study, decreased levels of EB extravasation
suggested that berberine has a protective effect against BBB
dysfunction.
Inflammation is an important factor involved in
sepsis-associated encephalopathy, which is strongly associated with
neuronal apoptosis (20,31). Another form of programmed cell
death, necroptosis (32), which is
strongly associated with inflammation, shares common morphological
features with apoptosis and is tightly regulated by kinases, such
as RIP1 and RIP3 (33). Numerous
studies have demonstrated that necroptosis is a common feature of
neuronal death in a number of CNS diseases, such as
neurodegenerative diseases (34,35)
and traumatic brain injury (36).
Therefore, the present study aimed to identify whether necroptosis
was involved in SAP-induced cognitive impairments. Following the
determination of the expression levels of important kinases
associated with necroptosis (RIP1 and RIP3) in hippocampal tissues
via western blotting, the results demonstrated that the expression
levels of RIP1 and RIP3 were significantly increased in the
hippocampal tissues of SAP rats and were significantly attenuated
following treatment with berberine. The results demonstrated that
the protective effects of berberine may be associated with
attenuation of necroptosis.
There were two limitations of the present study.
Firstly, only surviving rats were subjected to neurocognitive
testing and biochemical analyses, which may have introduced
survival bias into the study. Secondly, SAP model only induced by
L-arginine, which may generate choice bias, so, the results of the
present study should be further investigated using alternative AP
models, such as AP models induced by L-ornithine, bile acids and
hyperlipidemia (37).
In conclusion, the results of the present study
revealed that SAP induces neuroinflammation, BBB breakdown, and
elevated levels of proteins associated with apoptosis and
necroptosis, which may result in the development of
hippocampus-dependent cognitive impairments and eventual mortality.
Furthermore, the results revealed that berberine may protect the
integrity of the BBB, decrease levels of brain inflammation,
attenuate necroptosis and cognitive deficits, and reduce the 7-day
mortality rate in SAP rats. In addition, it was revealed that
necroptosis was involved in neurodegeneration associated with the
development of SAP. The results of the present study suggested that
berberine may represent a novel therapeutic strategy for the
treatment of cognitive impairments induced by SAP.
Acknowledgements
The authors would like to acknowledge the excellent
technical support provided by members of the Laboratory of
Anesthesia and Critical Care Medicine, West China Hospital of
Sichuan University (Chengdu, China).
Funding
No funding was received.
Availability of data and materials
The datasets and materials used and analyzed during
the current study are available from the corresponding author on
reasonable request.
Authors' contributions
YK, XO and YH designed the study, collected and
analyzed the data, and drafted the manuscript. XO induced the SAP
model and administered treatment. YH performed SAP disease severity
assessment. XL performed locomotor activity assessment and the fear
conditioning test (FCT). CG performed ELISA and western blot
analysis. All authors read and approved the final manuscript.
Ethics approval and consent to
participate
The present study was approved by the Institutional
Animal Experimental Ethics Committee of Sichuan University
(Chengdu, China).
Patient consent for publication
Not applicable.
Competing interests
The authors declare that they have no competing
interests.
References
|
1
|
Estrada RV, Moreno J, Martinez E,
Hernandez MC, Gilsanz G and Gilsanz V: Pancreatic encephalopathy.
Acta Neurol Scand. 59:135–139. 1979. View Article : Google Scholar : PubMed/NCBI
|
|
2
|
Menza MA and Murray GB: Pancreatic
encephalopathy. Biol Psychiatry. 25:781–784. 1989. View Article : Google Scholar : PubMed/NCBI
|
|
3
|
Bhatia M, Wong FL, Cao Y, Lau HY, Huang J,
Puneet P and Chevali L: Pathophysiology of acute pancreatitis.
Pancreatology. 5:132–144. 2005. View Article : Google Scholar : PubMed/NCBI
|
|
4
|
Xiong J, Wang K, Yuan C, Xing R, Ni J, Hu
G, Chen F and Wang X: Luteolin protects mice from severe acute
pancreatitis by exerting HO-1-mediated anti-inflammatory and
antioxidant effects. Int J Mol Med. 39:113–125. 2017. View Article : Google Scholar : PubMed/NCBI
|
|
5
|
Chen P, Sun B, Chen H, Wang G, Pan S, Kong
R, Bai X and Wang S: Effects of carbon monoxide releasing
molecule-liberated CO on severe acute pancreatitis in rats.
Cytokine. 49:15–23. 2010. View Article : Google Scholar : PubMed/NCBI
|
|
6
|
Vezzani A, Aronica E, Mazarati A and
Pittman QJ: Epilepsy and brain inflammation. Exp Neurol. 244:11–21.
2013. View Article : Google Scholar : PubMed/NCBI
|
|
7
|
Yang Y, Wang Q, Xie M, Liu P, Qi X, Liu X
and Li Z: Berberine exerts an anti-inflammatory role in ocular
Behcet's disease. Mol Med Rep. 15:97–102. 2017. View Article : Google Scholar : PubMed/NCBI
|
|
8
|
Huang M, Chen S, Liang Y and Guo Y: The
role of berberine in the multi-target treatment of senile dementia.
Curr Top Med Chem. 16:867–873. 2016. View Article : Google Scholar : PubMed/NCBI
|
|
9
|
Kim M, Cho KH, Shin MS, Lee JM, Cho HS,
Kim CJ, Shin DH and Yang HJ: Berberine prevents nigrostriatal
dopaminergic neuronal loss and suppresses hippocampal apoptosis in
mice with Parkinson's disease. Int J Mol Med. 33:870–878. 2014.
View Article : Google Scholar : PubMed/NCBI
|
|
10
|
Zhou J, Du X, Long M, Zhang Z, Zhou S,
Zhou J and Qian G: Neuroprotective effect of berberine is mediated
by MAPK signaling pathway in experimental diabetic neuropathy in
rats. Eur J Pharmacol. 774:87–94. 2016. View Article : Google Scholar : PubMed/NCBI
|
|
11
|
Sedaghat R, Taab Y, Kiasalari Z,
Afshin-Majd S, Baluchnejadmojarad T and Roghani M: Berberine
ameliorates intrahippocampal kainate-induced status epilepticus and
consequent epileptogenic process in the rat: Underlying mechanisms.
Biomed Pharmacother. 87:200–208. 2017. View Article : Google Scholar : PubMed/NCBI
|
|
12
|
Daviu N, Andero R, Armario A and Nadal R:
Sex differences in the behavioural and
hypothalamic-pituitary-adrenal response to contextual fear
conditioning in rats. Horm Behav. 66:713–723. 2014. View Article : Google Scholar : PubMed/NCBI
|
|
13
|
Shoji H, Takao K, Hattori S and Miyakawa
T: Contextual and cued fear conditioning test using a video
analyzing system in mice. J Vis Exp. e508712014.
|
|
14
|
Zhang CL, Lin ZQ, Luo RJ, Zhang XX, Guo J,
Wu W, Shi N, Deng LH, Chen WW, Zhang XY, et al: Chai-Qin-Cheng-Qi
decoction and carbachol improve intestinal motility by regulating
protein kinase C-mediated Ca2+ release in colonic smooth
muscle cells in rats with acute necrotising pancreatitis. Evid
Based Complement Alternat Med. 2017:58649452017. View Article : Google Scholar : PubMed/NCBI
|
|
15
|
Feng AW, Gao W, Zhou GR, Yu R, Li N, Huang
XL, Li QR and Li JS: Berberine ameliorates COX-2 expression in rat
small intestinal mucosa partially through PPARγ pathway during
acute endotoxemia. Int Immunopharmacol. 12:182–188. 2012.
View Article : Google Scholar : PubMed/NCBI
|
|
16
|
Schmidt J, Rattner DW, Lewandrowski K,
Compton CC, Mandavilli U, Knoefel WT and Warshaw AL: A better model
of acute pancreatitis for evaluating therapy. Ann Surg. 215:44–56.
1992. View Article : Google Scholar : PubMed/NCBI
|
|
17
|
Rau BM, Kruger CM, Hasel C, Oliveira V,
Rubie C, Beger HG and Schilling MK: Effects of immunosuppressive
and immunostimulative treatment on pancreatic injury and mortality
in severe acute experimental pancreatitis. Pancreas. 33:174–183.
2006. View Article : Google Scholar : PubMed/NCBI
|
|
18
|
Fanselow MS and Poulos AM: The
neuroscience of mammalian associative learning. Annu Rev Psychol.
56:207–234. 2005. View Article : Google Scholar : PubMed/NCBI
|
|
19
|
Vajtr D, Benada O, Kukacka J, Prusa R,
Houstava L, Toupalik P and Kizek R: Correlation of ultrastructural
changes of endothelial cells and astrocytes occurring during blood
brain barrier damage after traumatic brain injury with biochemical
markers of BBB leakage and inflammatory response. Physiol Res.
58:263–268. 2009.PubMed/NCBI
|
|
20
|
Ning Q, Liu Z, Wang X, Zhang R, Zhang J,
Yang M, Sun H, Han F, Zhao W and Zhang X: Neurodegenerative changes
and neuroapoptosis induced by systemic lipopolysaccharide
administration are reversed by dexmedetomidine treatment in mice.
Neurol Res. 39:357–366. 2017. View Article : Google Scholar : PubMed/NCBI
|
|
21
|
Chavez-Valdez R, Martin LJ, Flock DL and
Northington FJ: Necrostatin-1 attenuates mitochondrial dysfunction
in neurons and astrocytes following neonatal hypoxia-ischemia.
Neuroscience. 219:192–203. 2012. View Article : Google Scholar : PubMed/NCBI
|
|
22
|
Guo Q, Li A, Xia Q, Liu X, Tian B, Mai G,
Huang Z, Chen G, Tang W, Jin X, et al: The role of organ failure
and infection in necrotizing pancreatitis: A prospective study. Ann
Surg. 259:1201–1207. 2014. View Article : Google Scholar : PubMed/NCBI
|
|
23
|
Wichmann MA, Cruickshanks KJ, Carlsson CM,
Chappell R, Fischer ME, Klein BE, Klein R, Tsai MY and Schubert CR:
Long-term systemic inflammation and cognitive impairment in a
population-based cohort. J Am Geriatr Soc. 62:1683–1691. 2014.
View Article : Google Scholar : PubMed/NCBI
|
|
24
|
Calsavara AC, Rodrigues DH, Miranda AS,
Costa PA, Lima CX, Vilela MC, Rachid MA and Teixeira AL: Late
anxiety-like behavior and neuroinflammation in mice subjected to
sublethal polymicrobial sepsis. Neurotox Res. 24:103–108. 2013.
View Article : Google Scholar : PubMed/NCBI
|
|
25
|
Nicoletti F, Mancuso G, Cusumano V, Di
Marco R, Zaccone P, Bendtzen K and Teti G: Prevention of
endotoxin-induced lethality in neonatal mice by interleukin-13. Eur
J Immunol. 27:1580–1583. 1997. View Article : Google Scholar : PubMed/NCBI
|
|
26
|
Dujmovic I, Mangano K, Pekmezovic T,
Quattrocchi C, Mesaros S, Stojsavljevic N, Nicoletti F and Drulovic
J: The analysis of IL-1 beta and its naturally occurring inhibitors
in multiple sclerosis: The elevation of IL-1 receptor antagonist
and IL-1 receptor type II after steroid therapy. J Neuroimmunol.
207:101–106. 2009. View Article : Google Scholar : PubMed/NCBI
|
|
27
|
Li G, Wu XJ, Yang L, He YX, Liu Y, Jin X
and Yuan H: TLR4-mediated NF-κB signaling pathway mediates
HMGB1-induced pancreatic injury in mice with severe acute
pancreatitis. Int J Mol Med. 37:99–107. 2016. View Article : Google Scholar : PubMed/NCBI
|
|
28
|
Li J, Csakai A, Jin J, Zhang F and Yin H:
Therapeutic developments targeting toll-like receptor-4-mediated
neuroinflammation. ChemMedChem. 11:154–165. 2016. View Article : Google Scholar : PubMed/NCBI
|
|
29
|
Kniesel U and Wolburg H: Tight junctions
of the blood-brain barrier. Cell Mol Neurobiol. 20:57–76. 2000.
View Article : Google Scholar : PubMed/NCBI
|
|
30
|
Toklu HZ, Uysal MK, Kabasakal L, Sirvanci
S, Ercan F and Kaya M: The effects of riluzole on neurological,
brain biochemical, and histological changes in early and late term
of sepsis in rats. J Surg Res. 152:238–248. 2009. View Article : Google Scholar : PubMed/NCBI
|
|
31
|
Hotchkiss RS and Nicholson DW: Apoptosis
and caspases regulate death and inflammation in sepsis. Nat Rev
Immunol. 6:813–822. 2006. View
Article : Google Scholar : PubMed/NCBI
|
|
32
|
Linkermann A and Green DR: Necroptosis. N
Engl J Med. 370:455–465. 2014. View Article : Google Scholar : PubMed/NCBI
|
|
33
|
Li J, McQuade T, Siemer AB, Napetschnig J,
Moriwaki K, Hsiao YS, Damko E, Moquin D, Walz T, McDermott A, et
al: The RIP1/RIP3 necrosome forms a functional amyloid signaling
complex required for programmed necrosis. Cell. 150:339–350. 2012.
View Article : Google Scholar : PubMed/NCBI
|
|
34
|
Ito Y, Ofengeim D, Najafov A, Das S,
Saberi S, Li Y, Hitomi J, Zhu H, Chen H, Mayo L, et al: RIPK1
mediates axonal degeneration by promoting inflammation and
necroptosis in ALS. Science. 353:603–608. 2016. View Article : Google Scholar : PubMed/NCBI
|
|
35
|
Ofengeim D, Ito Y, Najafov A, Zhang Y,
Shan B, DeWitt JP, Ye J, Zhang X, Chang A, Vakifahmetoglu-Norberg
H, et al: Activation of necroptosis in multiple sclerosis. Cell
Rep. 10:1836–1849. 2015. View Article : Google Scholar : PubMed/NCBI
|
|
36
|
You Z, Savitz SI, Yang J, Degterev A, Yuan
J, Cuny GD, Moskowitz MA and Whalen MJ: Necrostatin-1 reduces
histopathology and improves functional outcome after controlled
cortical impact in mice. J Cereb Blood Flow Metab. 28:1564–1573.
2008. View Article : Google Scholar : PubMed/NCBI
|
|
37
|
Huang W, Szatmary P, Wan M, Bharucha S,
Awais M, Tang W, Criddle DN, Xia Q and Sutton R: Translational
insights into peroxisome proliferator-activated receptors in
experimental acute pancreatitis. Pancreas. 45:167–178. 2016.
View Article : Google Scholar : PubMed/NCBI
|