|
1
|
Benjamin EJ, Muntner P, Alonso A,
Bittencourt MS, Callaway CW, Carson AP, Chamberlain AM, Chang AR,
Cheng S, Das SR, et al: Heart disease and stroke statistics-2019
update: A report from the American heart association. Circulation.
139:e56–e528. 2019. View Article : Google Scholar
|
|
2
|
GBD 2017 Disease, Injury Incidence and
Prevalence Collaborators: Global, regional, and national incidence,
prevalence, and years lived with disability for 354 diseases and
injuries for 195 countries and territories, 1990–2017: A systematic
analysis for the global burden of disease study 2017. Lancet.
392:1789–1858. 2018. View Article : Google Scholar
|
|
3
|
Chen X and Wang K: The fate of medications
evaluated for ischemic stroke pharmacotherapy over the period
1995–2015. Acta Pharm Sin B. 6:522–530. 2016. View Article : Google Scholar
|
|
4
|
Zhang JJ and Liu X: Aspirin plus
dipyridamole has the highest surface under the cumulative ranking
curves (SUCRA) values in terms of mortality, intracranial
hemorrhage, and adverse event rate among 7 drug therapies in the
treatment of cerebral infarction. Medicine (Baltimore).
97:e01232018. View Article : Google Scholar
|
|
5
|
Yusuf S, Joseph P, Dans A, Gao P, Teo K,
Xavier D, López-Jaramillo P, Yusoff K, Santoso A, Gamra H, et al:
Polypill with or without aspirin in persons without cardiovascular
disease. N Engl J Med. 384:216–228. 2021. View Article : Google Scholar
|
|
6
|
Ibraheem M and Goldstein LB: Polypill
trials for stroke prevention-main results, critical appraisal, and
implications for US population. Curr Neurol Neurosci Rep.
20:102020. View Article : Google Scholar
|
|
7
|
Abdoulaye IA and Guo YJ: A Review of
recent advances in neuroprotective potential of 3-N-butylphthalide
and its derivatives. Biomed Res Int. 2016:50123412016. View Article : Google Scholar
|
|
8
|
Wang S, Ma F, Huang L, Zhang Y and Peng Y,
Xing C, Feng Y, Wang X and Peng Y: Dl-3-n-butylphthalide (NBP): A
promising therapeutic agent for ischemic stroke. CNS Neurol Disord
Drug Targets. 17:338–347. 2018. View Article : Google Scholar
|
|
9
|
Edaravone Acute Infarction Study Group, :
Effect of a novel free radical scavenger, edaravone (MCI-186), on
acute brain infarction. Randomized, placebo-controlled,
double-blind study at multicenters. Cerebrovasc Dis. 15:222–229.
2003. View Article : Google Scholar
|
|
10
|
Enomoto M, Endo A, Yatsushige H, Fushimi K
and Otomo Y: Clinical effects of early edaravone use in acute
ischemic stroke patients treated by endovascular reperfusion
therapy. Stroke. 50:652–658. 2019. View Article : Google Scholar
|
|
11
|
Kern R, Nagayama M, Toyoda K, Steiner T,
Hennerici MG and Shinohara Y: Comparison of the European and
Japanese guidelines for the management of ischemic stroke.
Cerebrovasc Dis. 35:402–418. 2013. View Article : Google Scholar
|
|
12
|
Chen C, Li M, Lin L, Chen S, Chen Y and
Hong L: Clinical effects and safety of edaravone in treatment of
acute ischaemic stroke: A meta-analysis of randomized controlled
trials. J Clin Pharm Ther. 46:907–917. 2021. View Article : Google Scholar
|
|
13
|
Hua K, Sheng X, Li TT, Wang LN, Zhang YH,
Huang ZJ and Ji H: The edaravone and 3-n-butylphthalide
ring-opening derivative 10b effectively attenuates cerebral
ischemia injury in rats. Acta Pharmacol Sin. 36:917–927. 2015.
View Article : Google Scholar
|
|
14
|
Sheng X, Hua K, Yang C, Wang X, Ji H, Xu
J, Huang Z and Zhang Y: Novel hybrids of 3-n-butylphthalide and
edaravone: Design, synthesis and evaluations as potential
anti-ischemic stroke agents. Bioorg Med Chem Lett. 25:3535–3540.
2015. View Article : Google Scholar
|
|
15
|
Zhao Y, Yang J, Li C, Zhou G, Wan H, Ding
Z, Wan H and Zhou H: Role of the neurovascular unit in the process
of cerebral ischemic injury. Pharmacol Res. 160:1051032020.
View Article : Google Scholar
|
|
16
|
Wang L, Xiong X, Zhang L and Shen J:
Neurovascular unit: A critical role in ischemic stroke. CNS
Neurosci Ther. 27:7–16. 2021. View Article : Google Scholar
|
|
17
|
Boltze J, Aronowski JA, Badaut J,
Buckwalter MS, Caleo M, Chopp M, Dave KR, Didwischus N, Dijkhuizen
RM, Doeppner TR, et al: New mechanistic insights, novel treatment
paradigms, and clinical progress in cerebrovascular diseases. Front
Aging Neurosci. 13:6237512021. View Article : Google Scholar
|
|
18
|
National Research Council (US) Committee
for the Update of the Guide for the Care and Use of Laboratory
Animals, . Guide for the Care and Use of Laboratory Animals. 8th
edition. National Academies Press; Washington, DC: 2011
|
|
19
|
Feng L, Sharma A, Niu F, Huang Y, Lafuente
JV, Muresanu DF, Ozkizilcik A, Tian ZR and Sharma HS:
TiO2-nanowired delivery of DL-3-n-butylphthalide
(DL-NBP) attenuates blood-brain barrier disruption, brain edema
formation, and neuronal damages following concussive head injury.
Mol Neurobiol. 55:350–358. 2018. View Article : Google Scholar
|
|
20
|
Alzoubi KH, Shatnawi A, Al-Qudah MA and
Alfaqih MA: Edaravone prevents memory impairment in an animal model
of post-traumatic distress. Behav Pharmacol. 30:201–207. 2019.
View Article : Google Scholar
|
|
21
|
Bederson JB, Pitts LH, Tsuji M, Nishimura
MC, Davis RL and Bartkowski H: Rat middle cerebral artery
occlusion: Evaluation of the model and development of a neurologic
examination. Stroke. 17:472–476. 1986. View Article : Google Scholar
|
|
22
|
Middeldorp J and Hol EM: GFAP in health
and disease. Prog Neurobiol. 93:421–443. 2011. View Article : Google Scholar
|
|
23
|
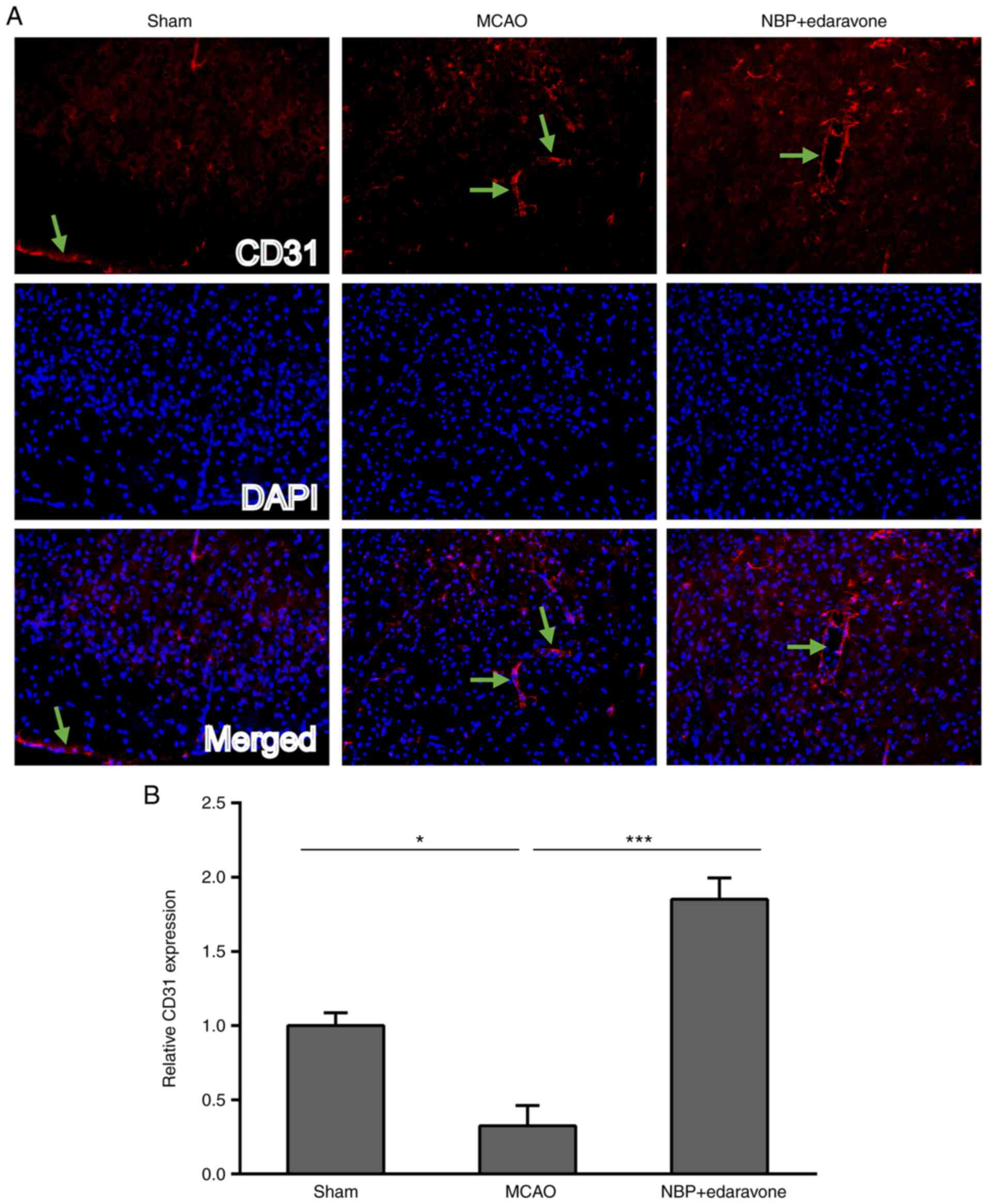
Lertkiatmongkol P, Liao D, Mei H, Hu Y and
Newman PJ: Endothelial functions of platelet/endothelial cell
adhesion molecule-1 (CD31). Curr Opin Hematol. 23:253–259. 2016.
View Article : Google Scholar
|
|
24
|
Chang Q and Wang XL: Effects of chiral
3-n-butylphthalide on apoptosis induced by transient focal cerebral
ischemia in rats. Acta Pharmacol Sin. 24:796–804. 2003.
|
|
25
|
Li J, Li Y, Ogle M, Zhou X, Song M, Yu SP
and Wei L: DL-3-n-butylphthalide prevents neuronal cell death after
focal cerebral ischemia in mice via the JNK pathway. Brain Res.
1359:216–226. 2010. View Article : Google Scholar
|
|
26
|
Zhao Y, Liu D, Li J, Zhang X and Wang X:
L-NBP, a multiple growth factor activator, attenuates ischemic
neuronal impairments possibly through promoting neuritogenesis.
Neurochem Int. 124:94–105. 2019. View Article : Google Scholar
|
|
27
|
Zhao Q, Zhang C, Wang X, Chen L, Ji H and
Zhang Y: (S)-ZJM-289, a nitric oxide-releasing derivative of
3-n-butylphthalide, protects against ischemic neuronal injury by
attenuating mitochondrial dysfunction and associated cell death.
Neurochem Int. 60:134–144. 2012. View Article : Google Scholar
|
|
28
|
Cabezas JA, Bustamante A, Giannini N,
Pecharroman E, Katsanos AH, Tsivgoulis G, Rozanski M, Audebert H,
Mondello S, Llombart V and Montaner J: Discriminative value of
glial fibrillar acidic protein (GFAP) as a diagnostic tool in acute
stroke. Individual patient data meta-analysis. J Investig Med.
68:1379–1385. 2020. View Article : Google Scholar
|
|
29
|
Li H, Zhang N, Sun G and Ding S:
Inhibition of the group I mGluRs reduces acute brain damage and
improves long-term histological outcomes after
photothrombosis-induced ischaemia. ASN Neuro. 5:195–207. 2013.
View Article : Google Scholar
|
|
30
|
Li H, Zhang N, Lin HY, Yu Y, Cai QY, Ma L
and Ding S: Histological, cellular and behavioral assessments of
stroke outcomes after photothrombosis-induced ischemia in adult
mice. BMC Neurosci. 15:582014. View Article : Google Scholar
|
|
31
|
Choudhury GR and Ding S: Reactive
astrocytes and therapeutic potential in focal ischemic stroke.
Neurobiol Dis. 85:234–244. 2016. View Article : Google Scholar
|
|
32
|
Mestriner RG, Saur L, Bagatini PB,
Baptista PP, Vaz SP, Ferreira K, Machado SA, Xavier LL and Netto
CA: Astrocyte morphology after ischemic and hemorrhagic
experimental stroke has no influence on the different recovery
patterns. Behav Brain Res. 278:257–261. 2015. View Article : Google Scholar
|
|
33
|
Liu P, Zhang R, Liu D, Wang J, Yuan C,
Zhao X, Li Y, Ji X, Chi T and Zou L: Time-course investigation of
blood-brain barrier permeability and tight junction protein changes
in a rat model of permanent focal ischemia. J Physiol Sci.
68:121–127. 2018. View Article : Google Scholar
|
|
34
|
Liu G and Geng J: Glial fibrillary acidic
protein as a prognostic marker of acute ischemic stroke. Hum Exp
Toxicol. 37:1048–1053. 2018. View Article : Google Scholar
|
|
35
|
Fahrig T: Changes in the solubility of
glial fibrillary acidic protein after ischemic brain damage in the
mouse. J Neurochem. 63:1796–1801. 1994. View Article : Google Scholar
|
|
36
|
Cheung WM, Wang CK, Kuo JS and Lin TN:
Changes in the level of glial fibrillary acidic protein (GFAP)
after mild and severe focal cerebral ischemia. Chin J Physiol.
42:227–235. 1999.
|
|
37
|
He F, Dai R, Zhou X, Li X, Song X, Yan H,
Meng Q, Yang C and Lin Q: Protective effect of 4-methoxy benzyl
alcohol on the neurovascular unit after cerebral ischemia
reperfusion injury. Biomed Pharmacother. 118:1092602019. View Article : Google Scholar
|
|
38
|
Pang XB, Xie XM, Wang HY and Wang BQ:
Protective effect of mailuoning injection on cerebral
ischemia/reperfusion injury in rats and its mechanism. Zhongguo
Zhong Yao Za Zhi. 39:721–725. 2014.(In Chinese).
|
|
39
|
Zhou PT, Wang LP, Qu MJ, Shen H, Zheng HR,
Deng LD, Ma YY, Wang YY, Wang YT, Tang YH, et al:
Dl-3-N-butylphthalide promotes angiogenesis and upregulates sonic
hedgehog expression after cerebral ischemia in rats. CNS Neurosci
Ther. 25:748–758. 2019. View Article : Google Scholar
|
|
40
|
Ye ZY, Xing HY, Wang B, Liu M and Lv PY:
DL-3-n-butylphthalide protects the blood-brain barrier against
ischemia/hypoxia injury via upregulation of tight junction
proteins. Chin Med J (Engl). 132:1344–1353. 2019. View Article : Google Scholar
|
|
41
|
Chong ZZ and Feng YP:
dl-3-n-butylphthalide attenuates reperfusion-induced blood-brain
barrier damage after focal cerebral ischemia in rats. Zhongguo Yao
Li Xue Bao. 20:696–700. 1999.
|
|
42
|
Zhao H, Yun W, Zhang Q, Cai X, Li X, Hui
G, Zhou X and Ni J: Mobilization of circulating endothelial
progenitor cells by dl-3-n-butylphthalide in acute ischemic stroke
patients. J Stroke Cerebrovasc Dis. 25:752–760. 2016. View Article : Google Scholar
|
|
43
|
DeLisser HM, Newman PJ and Albelda SM:
Molecular and functional aspects of PECAM-1/CD31. Immunol Today.
15:490–495. 1994. View Article : Google Scholar
|
|
44
|
Abbott NJ, Rönnbäck L and Hansson E:
Astrocyte-endothelial interactions at the blood-brain barrier. Nat
Rev Neurosci. 7:41–53. 2006. View Article : Google Scholar
|
|
45
|
Hu X, Zheng H, Yan T, Pan S, Fang J, Jiang
R and Ma S: Physical exercise induces expression of CD31 and
facilitates neural function recovery in rats with focal cerebral
infarction. Neurol Res. 32:397–402. 2010. View Article : Google Scholar
|
|
46
|
Zhang SJ, Wang RL, Zhao HP, Tao Z, Li JC,
Ju F, Han ZP, Ma QF, Liu P, Ma SB, et al: MEPO promotes
neurogenesis and angiogenesis but suppresses gliogenesis in mice
with acute ischemic stroke. Eur J Pharmacol. 849:1–10. 2019.
View Article : Google Scholar
|
|
47
|
Lin Y, Dong J, Yan T, He X, Zheng X, Liang
H and Sui M: Involuntary, forced and voluntary exercises are
equally capable of inducing hippocampal plasticity and the recovery
of cognitive function after stroke. Neurol Res. 37:893–901. 2015.
View Article : Google Scholar
|
|
48
|
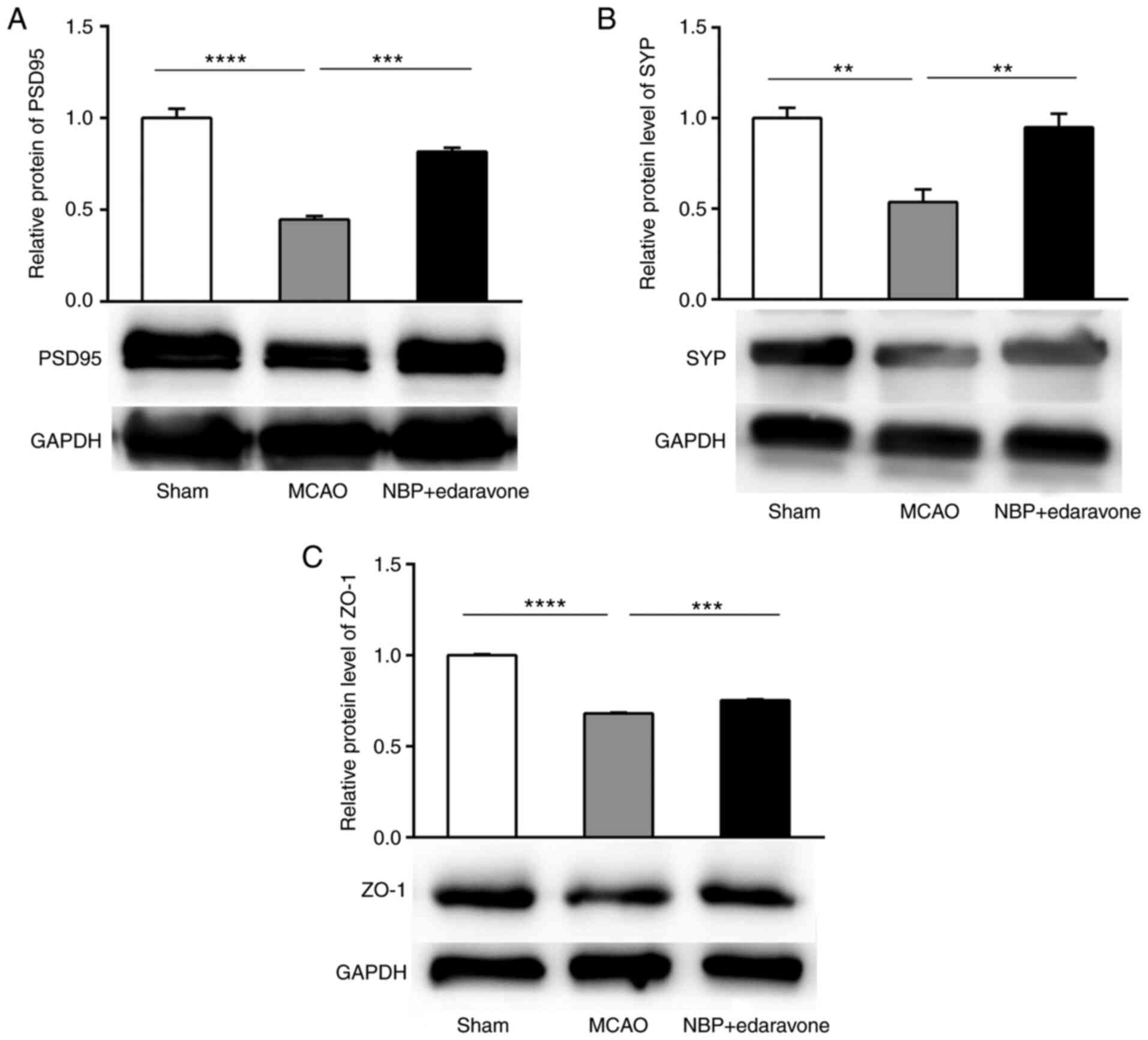
Sell GL, Barrow SL and McAllister AK:
Chapter 1-molecular composition of developing glutamatergic
synapses. Synapse Development and Maturation. Rubenstein J, Rakic
P, Chen B, Kwan KY, Cline HT and Cardin J: Academic Press; London:
pp. 3–32. 2020, View Article : Google Scholar
|
|
49
|
Fanning AS and Anderson JM: Zonula
occludens-1 and −2 are cytosolic scaffolds that regulate the
assembly of cellular junctions. Ann N Y Acad Sci. 1165:113–120.
2009. View Article : Google Scholar
|
|
50
|
Abdullahi W, Tripathi D and Ronaldson PT:
Blood-brain barrier dysfunction in ischemic stroke: Targeting tight
junctions and transporters for vascular protection. Am J Physiol
Cell Physiol. 315:C343–C356. 2018. View Article : Google Scholar
|
|
51
|
Li XF, Zhang XJ, Zhang C, Wang LN, Li YR,
Zhang Y, He TT, Zhu XY, Cui LL and Gao BL: Ulinastatin protects
brain against cerebral ischemia/reperfusion injury through
inhibiting MMP-9 and alleviating loss of ZO-1 and occludin proteins
in mice. Exp Neurol. 302:68–74. 2018. View Article : Google Scholar
|
|
52
|
Hao FL, Han XF, Wang XL, Zhao ZR, Guo AH,
Lu XJ and Zhao XF: The neurovascular protective effect of
alogliptin in murine MCAO model and brain endothelial cells. Biomed
Pharmacother. 109:181–187. 2019. View Article : Google Scholar
|
|
53
|
Kikuchi K, Uchikado H, Miyagi N, Morimoto
Y, Ito T, Tancharoen S, Miura N, Miyata K, Sakamoto R, Kikuchi C,
et al: Beyond neurological disease: New targets for edaravone
(Review). Int J Mol Med. 28:899–906. 2011.
|
|
54
|
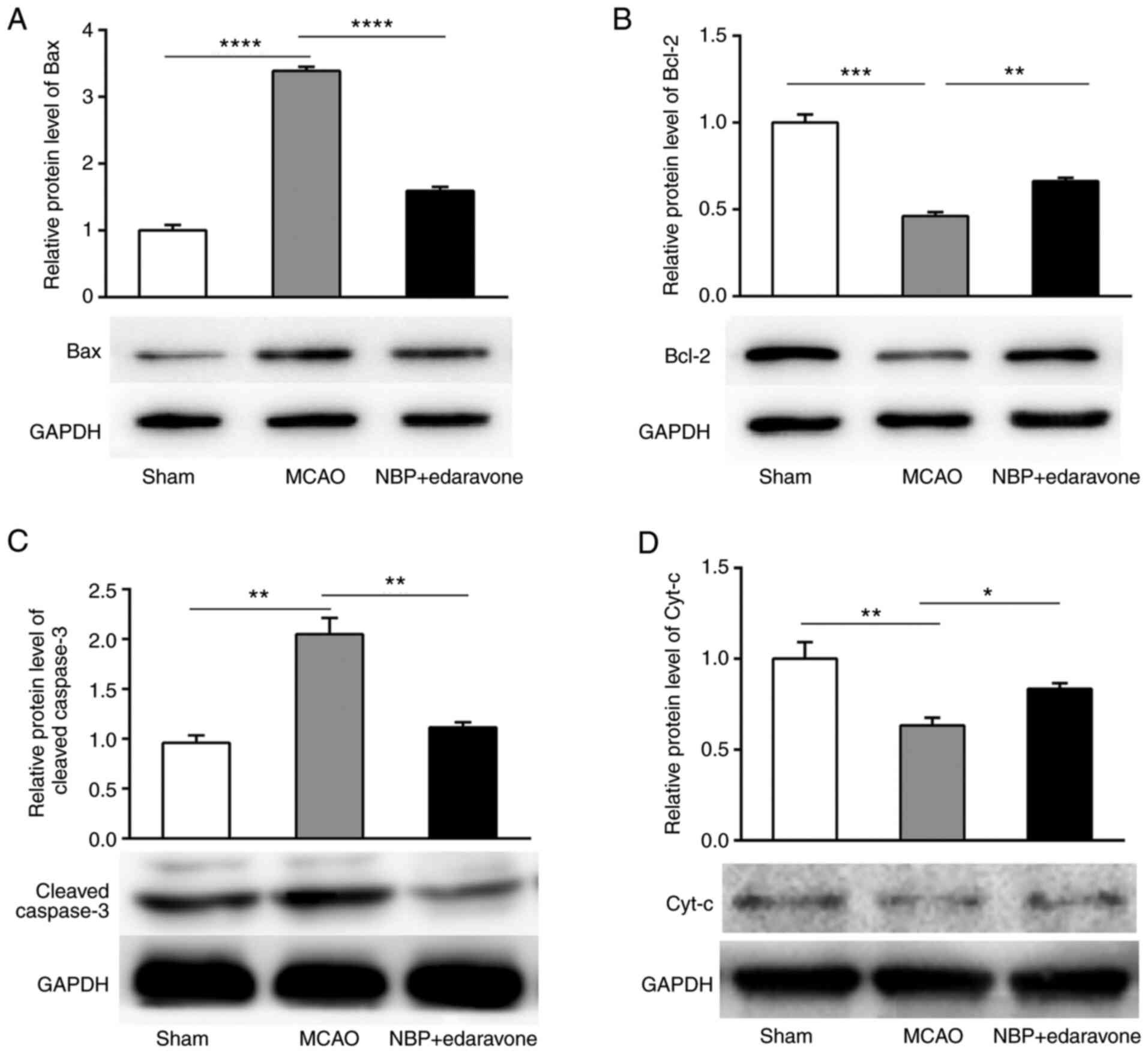
Hai W, Yang Y, Wang YL and Nie YX: The
effect of dl-3n-butylphthalide on the neurons in the hippocampus of
mongolian gerbil and the expression of p-ERK, Bcl-2 and Bax after
global cerebral ischemia and reperfusion damage. Chin J Clinicians
(Electronic Edition). 2015:1157–1162. 2015.(In Chinese).
|
|
55
|
Li C, Mo Z, Lei J, Li H, Fu R, Huang Y,
Luo S and Zhang L: Edaravone attenuates neuronal apoptosis in
hypoxic-ischemic brain damage rat model via suppression of TRAIL
signaling pathway. Int J Biochem Cell Biol. 99:169–177. 2018.
View Article : Google Scholar
|
|
56
|
Zeng Z, Gong X and Hu Z:
L-3-n-butylphthalide attenuates inflammation response and brain
edema in rat intracerebral hemorrhage model. Aging (Albany NY).
12:11768–11780. 2020. View Article : Google Scholar
|