Introduction
Cannabinoids have been implicated in physiological
and pathological conditions including inflammation, immunity,
analgesia, neoplasia and others (1). These associations have increased the
interest in cannabinoids in recent years. The effect of
cannabinoids in colorectal cancer (CRC) has been demonstrated in
in vitro experiments and animal models, which indicate the
antiproliferative, apoptotic and antimetastatic actions of
cannabinoid agonists (2–5). In accordance with these observations,
the levels of the major endogenous cannabinoids have been
identified to be 2- to 3-fold higher in CRC than in the neighboring
normal mucosa (5).
Antineoplastic effects are mediated by the
activation of cannabinoid type I (CB1), type 2 (CB2) or a
non-cannabinoid receptor-mediated mechanism (6). Among the receptors, the mechanism of
tumor cell apoptosis has been rigorously investi gated by several
research groups who have studied the CB1 receptor (2–5). CB1
is abundantly expressed in the brain and in numerous peripheral
neurons (7). It is also found not
only in normal colonic epithelium, smooth muscle and the submucosal
myenteric plexus (8), but also in
several colon cancer cell lines (6). Expression levels of CB1 receptors are
downregulated in cancer compared with adjacent normal mucosa
(3). Loss or inhibition of the CB1
receptor has been demonstrated to accelerate intestinal adenoma
growth, whereas activation of the CB1 receptor attenuated
intestinal tumor growth by inducing cell death via downregulation
of the anti-apoptotic factor, survivin, in a genetic model of CRC
progression (3). CRC patients who
are either homo- or heterozygous for the 1359 G/A CB1 receptor
polymorphism exhibit a shorter survival time compared with G/G
wild-type patients, although the post-transcriptional mechanism has
not yet been delineated (9).
The evidence mentioned thus far suggests that the
endogenous cannabinoid system is able to regulate cancer
progression and affect disease progression and outcomes. Although
there have been a small number of studies concerning the prognostic
role of the CB1 receptor in human tissues (10–12),
the results were discrepant and CB1 expression of CRC has only been
addressed in a single study (13).
We hypothesize that increased CB1 receptor expression may be
associated with decreased disease severity and more favorable
clinical outcomes. Therefore, the aim of the present study was to
investigate the correlation between disease severity/clinical
outcomes and the expression level of the CB1 receptor.
Materials and methods
Patients
Between January, 2004 and December, 2007, a total of
544 consecutive patients with CRC who underwent surgery at Seoul
St. Mary’s Hospital, Seoul, Korea, were enrolled. Patients who had
surgery-related mortality (n=10) were excluded from this study;
therefore, the clinical data of 534 patients were analyzed. The
patients were followed up after surgery at regular 3- to 6-month
intervals during the first year and then at 6-month intervals
thereafter. Abdominal computed tomography was performed annually
for the first 3 years and colonoscopy was performed every 1–3 years
for evaluation of recurrence. The follow-up time for patients who
did not survive was defined as the duration between the dates of
surgery and mortality. The Institutional Review Board at Seoul St.
Mary’s Hospital approved the handling of tissue samples and the
patient data in the present study. Written informed consent was
obtained from the patients and patient anonymity was preserved
throughout this study.
The mean patient age was 62.8 years (standard
deviation, 11.7) and 328 of the patients (61.4%) were male. The
tumor location was the right colon in 150 (28.1%) patients, the
left colon in 178 patients (33.3%) and the rectum in 206 patients
(38.6%). The numbers of patients with disease stages I, II, III and
IV were 78 (14.6%), 162 (30.3%), 206 (38.6%) and 88 (16.5%),
respectively, according to the American Joint Committee on Cancer
tumor node metastasis (TNM) system (14). The tumor grade was well/moderately
differentiated in 494 (92.5%) patients and poorly differentiated in
40 (7.5%) patients, by the World Health Organization tumor
classifcation system (15). R0
resection was administered to 478 (89.5%) patients, and 97 (18.2%)
patients received adjuvant chemotherapy. The median follow-up time
was 42 months (range, 2–80). All data regarding the follow-up
studies were evaluated on the basis of information available as of
October, 2010.
Tissue microarray generation
Tissue microarrays were constructed from archival
formalin-fixed, paraffin-embedded carcinoma samples obtained from
primary CRC specimens using a manual tissue arrayer (Quick-Ray
Manual Tissue Microarrayer; Unitma Co., Ltd.; Seoul, Korea). For
each sample, two areas rich in viable tumor cells (>80%) in the
invasive front and in the tumor center were identified by light
microscopic examination of hematoxylin and eosin-stained sections,
and were marked for use in the tissue microarrays. Tissue cylinders
with a diameter of 2 mm were punched from the previously marked
tumor area of each block (the donor block) and inserted into a
recipient paraffin block, resulting in a 6×10 array.
Immunohistochemical staining
Immunohistochemistry for CB1 was performed on
paraffin-embedded tissue sections of the tissue microarrays.
Immunohistochemical reactions were conducted using a Polink-2 HRP
Plus Broad detection system (Golden Bridge International; Mukilteo,
WA, USA) according to the manufacturer’s instructions. Briefly, the
tissue sections were deparaffinized and quenched with 3% hydrogen
peroxide in methanol for 10 min. Antigen retrieval was then
conducted using 0.01 mol/l citrate buffer (pH 6.0) by heating the
sample in a microwave pressure cooker for 20 min. The sections were
incubated with rabbit polyclonal CB1 antibody (1:50; Cat. No.
23703; Abcam; Cambridge, UK) (10,13) at
room temperature for 30 min, followed by incubation with Broad
Antibody Enhancer for 10 min and then with Polymer-HRP for 10 min
(Golden Bridge International, Inc., Mukilteo, WA, USA). The
peroxidase reaction was developed using 3′3-diaminobenzidine
tetrahydrochloride as the chromogen. Negative controls included
substitution of the primary antibodies with normal rabbit IgG of
the same concentration as the primary antibodies.
Scoring of immunohistochemistry
Each preserved specimen was examined by a
pathologist (C.K.J.) who was blind to the clinical status of the
patients. The immunoreactive area for CB1 was scored as 0 (0%), 1
(<33%), 2 (33–66%) or 3 (>66%), as discussed previously by
Michalski et al(11). Using
a simple median split, i.e., <3 or =3, immunoreactivity of CB1
expression was categorized as low or high under light microscopy.
When the pathologist had scored all the samples, these were
repeatedly measured using the same procedure, but without accessing
any previous data. Cases with different scores were then evaluated
once more, also without knowledge of the previous results. The
final scores were then entered into the database for analysis by
another investigator (J.M.P.).
Statistical analysis
Continuous data are presented as the mean ± standard
deviation (SD), and categorical data are presented as quantities
and proportions. To evaluate the difference between the groups of
patients according to the immunoreactivity of CB1 receptor
expression, the χ2 test was used for categorical data,
and the two-sample independent t-test was used for continuous
variables. Cumulative survival curves for patients according to CB1
immunoreactivity were determined by the Kaplan-Meier method, and
differences between the groups were compared using the log-rank
test. Univariate and multivariate analyses were performed with the
Cox proportional hazard regression model to determine factors
related to overall survival. All statistical analyses were
performed using Statistical Analysis Software (SAS; SAS Institute;
Cary, NC, USA). P<0.05 was considered to indicate a
statistically significant difference.
Results
Immunohistochemical evaluation of CB1
expression
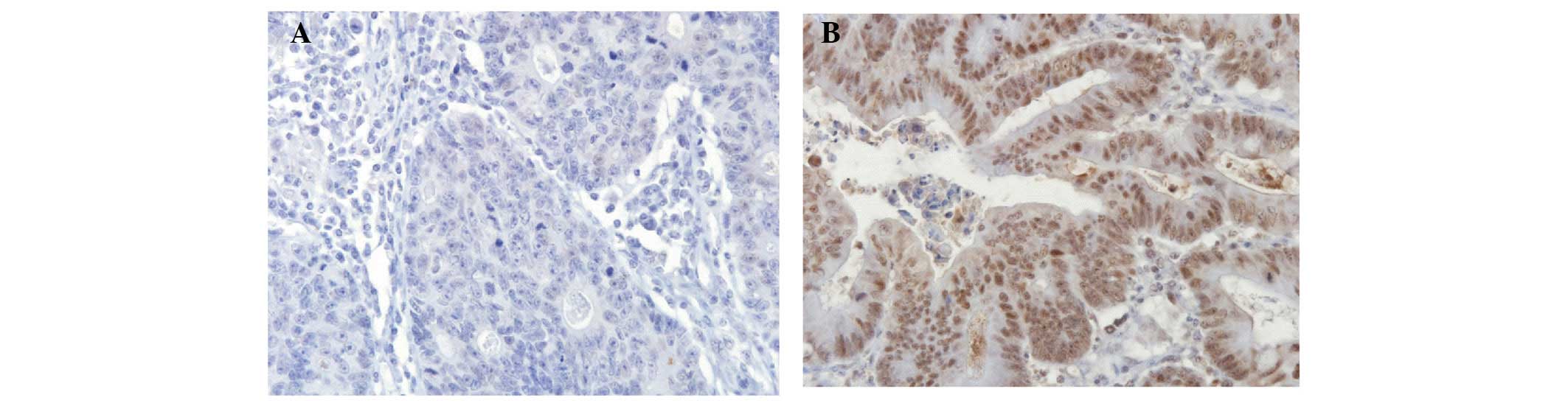
Tumor cells with positive cytoplasmic staining for
CB1 are illustrated in Fig. 1.
Positive immunoreactivity for the CB1 receptor was observed in 409
patients (76.6%). The area of immunoreactive tumor cells was zero
in 125 patients (23.4%), <33% in 24 patients (4.5%), 33–66% in
114 patients (21.3%) and >66% in 271 patients (50.7%). The
proportion of low expression was significantly higher in stage IV
than in stage I/II or III cancer (P<0.01 for both; Fig. 2). The expression level of the CB1
receptor at the invasive front was similar to that in the specimens
from the tumor center (P=NS).
Association of CB1 expression with
clinicopathological findings
The correlations between CB1 receptor expression and
the clinicopathological characteristics are summarized in Table I. No significant differences were
observed in age, gender, tumor size, histological differentiation,
primary tumor site, depth of invasion and lymph node metastasis
between high and low CB1 receptor expression in the immunostaining
results. However, distant metastasis was significantly higher in
the patients with low CB1 receptor expression compared with those
classified as having high expression (P= 0.003). Accordingly, the
frequency was shown to be different in stage IV cancer
(P=0.023).
 | Table ICharacteristics of the tumor tissue
samples with high and low expression of the cannabinoid type I
(CB1) receptor. |
Table I
Characteristics of the tumor tissue
samples with high and low expression of the cannabinoid type I
(CB1) receptor.
| Expression of the CB1
receptor
| |
|---|
| Categories | Low (n=263) (%) | High (n=271) (%) | P-value |
|---|
| Mean age ± SD
(years) | 62.3±11.7 | 63.3±11.7 | 0.319 |
| Gender | | | |
| Male | 163 (62.0) | 165 (60.9) | 0.796 |
| Female | 100 (38.0) | 106 (39.1) | |
| Tumor size | 5.0±1.8 | 5.4±2.4 | 0.168 |
| Histological
differentiationa | | | |
| Differentiated | 245 (93.2) | 249 (91.9) | 0.576 |
|
Undifferentiated | 18 (6.8) | 22 (8.1) | |
| Tumor site | | | |
| Right | 71 (27.0) | 79 (29.2) | 0.157 |
| Left | 80 (30.4) | 98 (36.2) | |
| Rectum | 112 (42.6) | 94 (34.7) | |
| Depth of
invasion | | | 0.888 |
| T1 | 7 (2.7) | 8 (3.0) | |
| T2 | 32 (12.2) | 39 (14.4) | |
| T3 | 167 (63.5) | 167 (61.6) | |
| T4 | 57 (21.7) | 57 (21.0) | |
| Lymph node
metastasis | | | |
| N0 | 119 (45.2) | 137 (50.6) | 0.112 |
| N1 | 67 (25.5) | 76 (28.0) | |
| N2 | 77 (29.3) | 58 (21.4) | |
| Distant
metastasis | | | |
| M0 | 207 (78.7) | 239 (88.2) | 0.003 |
| M1 | 56 (21.3) | 32 (11.8) | |
| TNM stage | | | 0.023 |
| I | 36 (13.7) | 42 (15.5) | |
| II | 71 (27.0) | 91 (33.6) | |
| III | 100 (38.0) | 106 (39.1) | |
| IV | 56 (21.3) | 32 (11.8) | |
As the frequency of distant metastasis was different
between the group with high and low CB1 receptor expression, we
compared the clinicopathological characteristics in stage IV cancer
(Table II). No significant
differences were observed in age, gender, histological
differentiation, tumor site and follow-up interval between high and
low CB1 receptor expression. Additionally, no significant
difference was observed in the number of R0 resections performed in
patients with high and low CB1 receptor expression; 18 (56.3%) and
29 (51.8%), respectively (P=0.686).
 | Table IIClinicopathological characteristics
of patients with stage IV colorectal cancer in relation to
expression of cannabinoid type I (CB1) receptor
immunoreactivity. |
Table II
Clinicopathological characteristics
of patients with stage IV colorectal cancer in relation to
expression of cannabinoid type I (CB1) receptor
immunoreactivity.
| Expression of the
CB1 receptor
| |
|---|
| Categories | Low (n=56) (%) | High (n=32)
(%) | P-value |
|---|
| Mean age ± SD
(years) | 59.1±11.9 | 61.5±9.3 | 0.293 |
| Gender | | | |
| Male | 34 (60.7) | 20 (62.5) | 0.869 |
| Female | 22 (39.3) | 12 (37.5) | |
| Histological
differentiationa | | | 0.210 |
|
Differentiated | 48 (85.7) | 24 (75.0) | |
|
Undifferentiated | 8 (14.3) | 8 (25.0) | |
| Tumor site | | | 0.187 |
| Right | 20 (35.7) | 8 (25.0) | |
| Left | 17 (30.4) | 16 (50.0) | |
| Rectum | 19 (33.9) | 8 (25.0) | |
| Adjuvant
chemotherapy | 18 (32.1) | 7 (21.9) | 0.304 |
| R0 resection | 29 (51.8) | 18 (56.3) | 0.686 |
| Follow-up
(months)b | 22.5 (15–40.3) | 17 (8.3–32.3) | 0.134 |
Survival according to cancer stage
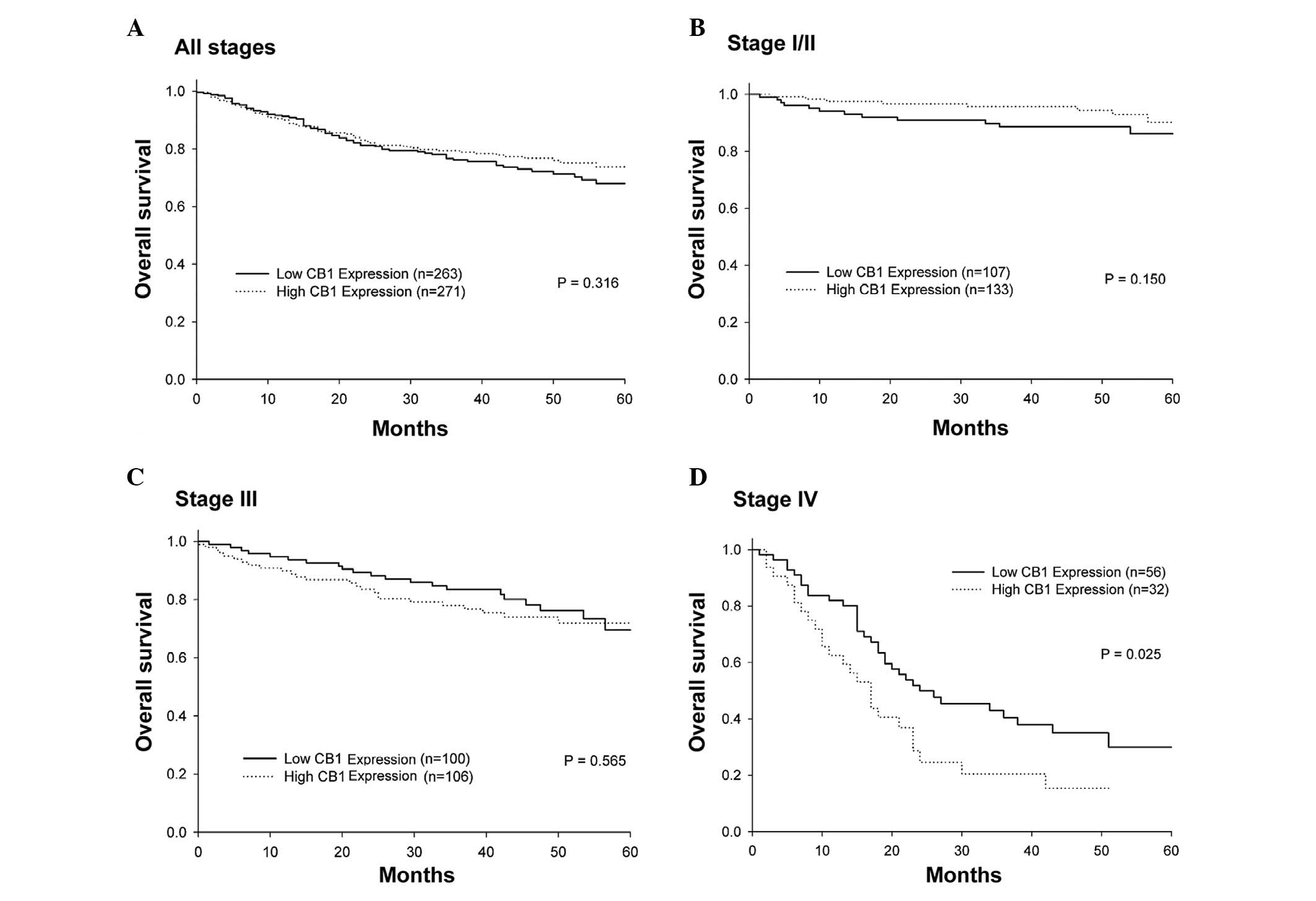
The Kaplan-Meier analysis of the data for a total of
534 patients revealed that the overall survival between the
patients with high vs. low CB1 receptor expression in tumors was
not significantly different (Fig.
3A) (log-rank test; P=0.316). In stage I/II and III cancers,
the overall survival of patients with high vs. low CB1 receptor
expression was not significantly different (Fig. 3B and C). The patients with high CB1
receptor expression in tumors had poorer outcomes than the patients
with low expression (Fig. 3D). The
hazard ratio (HR) was 1.782 with a 95% confidence interval (CI) of
1.049–2.988 (P=0.033).
Factors affecting overall survival
The multivariate analysis of factors related to
overall survival in stage IV is shown in Table III. A Cox proportional hazards
regression analysis indicated that a high CB1 expression level,
along with incomplete resection of the tumor and undifferentiated
pathology was an independent variable associated with a poorer
disease outcome in stage IV cancer (HR, 1.805; 95% CI, 1.042–3.094;
P= 0.035).
 | Table IIIMultivariate analysis of tumor
variables and overall survival in stage IV cancer (n=88). |
Table III
Multivariate analysis of tumor
variables and overall survival in stage IV cancer (n=88).
| Variable | HR (95% CI) | P-value |
|---|
| Age | 1.000
(0.974–1.021) | 0.7803 |
| Expression of CB1
receptor (≥66 vs. <66%) | 1.805
(1.042–3.094) | 0.0353 |
| Resection (R1/R2
vs. R0) | 4.506
(1.933–13.152) | 0.0002 |
| Chemotherapy (no
vs. yes) | 2.000
(0.761–6.213) | 0.1653 |
| Differentiation
(undifferentiated vs. differentiated) | 2.755
(1.449–4.987) | 0.0027 |
Discussion
The function of the CB1 receptor underlying the
pathophysiology and outcome of CRCs has not been clearly
delineated. In this study, we demonstrated that CB1 receptor
expression is correlated with distant metastasis, but not with
tumor invasion and lymph node metastasis, in CRC. In terms of the
patient outcome, high CB1 receptor expression is correlated with
poor survival in stage IV CRC, and is an independent prognostic
factor even after adjusting for covariates. However, high CB1
receptor expression was not associated with the clinical outcomes
in stage I/II and III CRC.
Cannabinoid molecules have been of significance in
the study of potential cancer therapies, as they have demonstrated
potential antitumor effects in cultured cell lines and in animal
models. Previous studies have indicated that the majority of the
effects of exogenous cannabinoids act through the activation of the
CB1 receptor (6). In an endogenous
system, downregulation of CB1 receptor expression was observed in
neoplastic epithelial cells from colon cancer biopsies (16). The mechanism of this finding is
explained by epigenetic silencing of the CB1-encoding gene that
contributes to a loss of its trans cription (3), as is frequently found in the
inactivation of tumor suppressor genes (17). However, the functions of the CB1
receptor gene and the mechanisms underlying the transcriptional
regulation of the CB1 receptor are not clearly delineated. The
present data revealed that CB1 receptor expression is downregulated
as CRC progresses to a highly advanced stage, which is concordant
with our hypothesis. This finding is also supported by a previous
observation by Gustafsson et al that 64% of patients with
stage IV CRC exhibited low immunoreactivity of the CB1 receptor
(13).
Our data demonstrated that high CB1 receptor
expression in CRC confers a poor prognosis for the patient. We had
predicted that high CB1 receptor expression would lead to a better
outcome in patients with CRC; however, the opposite result was
observed. Notably, our observation was similar to that of the study
by Gustafsson et al, in which CRC with a high intensity of
the CB1 receptor was correlated with a shorter survival time than
those with a low CB1 receptor intensity (13). It is difficult to clearly explain
this observation. In general, the prognosis of CRC has been known
to be correlated with the type, density and location of immune
cells within the tumor (18), and
certain studies have indicated that the presence of
tumor-infiltrating lymphocytes within cancer cell nests and the
tumor stroma is related to improved survival (19,20).
CB1 has a pivotal role in modulating the immune response. A
previous study demonstrated that mice in which the CB1-encoding
gene had been knocked out exhibited a stronger inflammatory
response in the colon compared with wild-type mice in response to
treatment with pro-inflammatory agents (21), suggesting an immunomodulatory role
of the CB1 receptor. Therefore, it may be speculated that tumors
with low CB1 expression in the tumor tissue may elicit a low
inflammatory environment. The study by Gustafsson et al
revealed that CRC with low CB1 receptor intensity in the tumor
front presented a higher number of infiltrating lymphocytes than
CRC with high CB1 receptor intensity, with marginal statistical
significance (13). The other
possible explanation for this observation is that a high level of
CB1 receptor expression is able to activate the pro-survival
cellular pathway. CB1 receptors are coupled to a variety of
signaling cascades, including cyclic AMP and activation of the
extracellular signal-related kinase pathway (7), which are able to cause cell
proliferation (22). Furthermore, a
previous study indicated that activation of the CB1 receptor
results in activation of the Akt signaling pathway and that
cannabinoids only induced tumor cell apoptosis when this pathway
was inhibited (23).
Another potential explanation is that CB1 receptor
expression is a compensatory response for the endogenous
cannabinoid level. This implies that a higher degree of endogenous
cannabinoid in tumors favors apoptosis in cancer cells; this
results in better survival and leads to downregulation of CB1
receptor expression in a compensatory way. Regarding this
explanation, the level of endogenous cannabinoid-metabolizing
enzymes, as well as the CB1 receptor, were analyzed in a pancreatic
cancer study; however, this study failed to indicate the
correlation between enzyme function and CB1 receptor level and
patient survival (11). Studies in
CRC to further explain this observation are necessary.
Notably, high CB1 receptor expression in stage IV
CRC is an independent prognostic factor, even following adjustment
for R0 resection, tumor differentiation and chemotherapy. A recent
study indicated that the CB1 receptor antagonist rimonabant was
able to control tumor growth (24).
Therefore, it would be valuable to know whether patients with high
CB1 receptor expression can be treated effectively with this
receptor-blocking agent.
To our knowledge, four studies have investigated the
correlation between CB1 receptor expression and disease outcome in
cancer. Our data was supported by three of these studies, which
demonstrated that high CB1 receptor immunoreactivity was correlated
with a shorter survival time than low immunoreactivity in
pancreatic, prostate and colorectal cancers (10,11,13).
In contrast, disease-free survival in hepatocellular carcinoma was
observed to be lower in patients with low CB1 receptor
immunoreactivity than in those with high immunoreactivity (12). These discrepant results may indicate
different roles of CB1 receptors that are dependent on the type of
cancer.
The observation time and number of mortalities in
our study may not have been sufficient to discern the survival
difference according to the CB1 receptor expression level in stage
I/II or III CRC; therefore, these factors may have caused different
results from a previous study (13). However, we propose that the results
of stage IV cancer portray the true role of CB1, as fatalities
occurred during a relatively short time period. Furthermore, the
multivariate analysis supports the important and independent
association of the CB1 receptor with patient survival. In a
previous study of patients with pancreatic cancer, which has a
poorer prognosis than CRC, a difference in survival was observed
according to the expression level of CB1 (11). Limitations of the present study
include the status of microsatellite instability, the level of
endogenous cannabinoids and the fact that the metabolizing enzymes
of endogenous cannabinoids in tumors were not evaluated. The use of
a large sample size of well-characterized patients with a long
follow-up period may allow for the correlation between CB1
expression and the disease outcomes to be determined.
In conclusion, the present study demonstrated that
high CB1 receptor expression is independently correlated with
decreased survival in stage IV CRC. Future studies investigating
other components of the endogenous cannabinoid system are required
to clarify the exact mechanism and the correlation with endogenous
cannabinoids.
Acknowledgements
This study was supported by the 2010
Research Foundation of the Department of Internal Medicine, The
Catholic University of Korea and by the Korea Research Foundation
(Grant No. 2009-0066500).
References
|
1
|
Di Marzo V: Targeting the endocannabinoid
system: to enhance or reduce? Nat Rev Drug Discov. 7:438–455.
2008.
|
|
2
|
Greenhough A, Patsos HA, Williams AC and
Paraskeva C: The cannabinoid delta(9)-tetrahydrocannabinol inhibits
RAS-MAPK and PI3K-AKT survival signalling and induces BAD-mediated
apoptosis in colorectal cancer cells. Int J Cancer. 121:2172–2180.
2007. View Article : Google Scholar : PubMed/NCBI
|
|
3
|
Wang D, Wang H, Ning W, Backlund MG, Dey
SK and DuBois RN: Loss of cannabinoid receptor 1 accelerates
intestinal tumor growth. Cancer Res. 68:6468–6476. 2008. View Article : Google Scholar : PubMed/NCBI
|
|
4
|
Patsos HA, Hicks DJ, Dobson RR, et al: The
endogenous cannabinoid, anandamide, induces cell death in
colorectal carcinoma cells: a possible role for cyclooxygenase 2.
Gut. 54:1741–1750. 2005. View Article : Google Scholar : PubMed/NCBI
|
|
5
|
Ligresti A, Bisogno T, Matias I, et al:
Possible endocannabinoid control of colorectal cancer growth.
Gastroenterology. 125:677–687. 2003. View Article : Google Scholar : PubMed/NCBI
|
|
6
|
Izzo AA and Camilleri M: Cannabinoids in
intestinal inflammation and cancer. Pharmacol Res. 60:117–125.
2009. View Article : Google Scholar : PubMed/NCBI
|
|
7
|
Howlett AC, Barth F, Bonner TI, et al:
International Union of Pharmacology. XXVII Classification of
cannabinoid receptors. Pharmacol Rev. 54:161–202. 2002. View Article : Google Scholar : PubMed/NCBI
|
|
8
|
Wright K, Rooney N, Feeney M, et al:
Differential expression of cannabinoid receptors in the human
colon: cannabinoids promote epithelial wound healing.
Gastroenterology. 129:437–453. 2005. View Article : Google Scholar : PubMed/NCBI
|
|
9
|
Bedoya F, Rubio JC, Morales-Gutierrez C,
et al: Single nucleotide change in the cannabinoid receptor-1
(CNR1) gene in colorectal cancer outcome. Oncology. 76:435–441.
2009. View Article : Google Scholar : PubMed/NCBI
|
|
10
|
Chung SC, Hammarsten P, Josefsson A, et
al: A high cannabinoid CB(1) receptor immunoreactivity is
associated with disease severity and outcome in prostate cancer.
Eur J Cancer. 45:174–182. 2009. View Article : Google Scholar : PubMed/NCBI
|
|
11
|
Michalski CW, Oti FE, Erkan M, et al:
Cannabinoids in pancreatic cancer: correlation with survival and
pain. Int J Cancer. 122:742–750. 2008. View Article : Google Scholar : PubMed/NCBI
|
|
12
|
Xu X, Liu Y, Huang S, et al:
Overexpression of cannabinoid receptors CB1 and CB2 correlates with
improved prognosis of patients with hepatocellular carcinoma.
Cancer Genet Cytogenet. 171:31–38. 2006. View Article : Google Scholar : PubMed/NCBI
|
|
13
|
Gustafsson SB, Palmqvist R, Henriksson ML,
et al: High tumour cannabinoid CB1 receptor immunoreactivity
negatively impacts disease-specific survival in stage II
microsatellite stable colorectal cancer. PLoS One. 6:e230032011.
View Article : Google Scholar
|
|
14
|
Edge S, Byrd D, Compton C, Fritz A, Greene
F and Trotti A: AJCC Cancer Staging Manual. Springer; New York:
2010
|
|
15
|
Jass JR and Sobin LH: Histological Typing
of Intestinal Tumours WHO International Histological Classification
of Tumours. 2nd edition. Springer-Verlag; Berlin-New York: 1989,
View Article : Google Scholar
|
|
16
|
Cianchi F, Papucci L, Schiavone N, et al:
Cannabinoid receptor activation induces apoptosis through tumor
necrosis factor alpha-mediated ceramide de novo synthesis in colon
cancer cells. Clin Cancer Res. 14:7691–7700. 2008. View Article : Google Scholar
|
|
17
|
Jones PA and Baylin SB: The fundamental
role of epigenetic events in cancer. Nat Rev Genet. 3:415–428.
2002.PubMed/NCBI
|
|
18
|
Galon J, Costes A, Sanchez-Cabo F, et al:
Type, density, and location of immune cells within human colorectal
tumors predict clinical outcome. Science. 313:1960–1964. 2006.
View Article : Google Scholar : PubMed/NCBI
|
|
19
|
Naito Y, Saito K, Shiiba K, et al:
CD8+ T cells infiltrated within cancer cell nests as a
prognostic factor in human colorectal cancer. Cancer Res.
58:3491–3494. 1998.PubMed/NCBI
|
|
20
|
Ropponen KM, Eskelinen MJ, Lipponen PK,
Alhava E and Kosma VM: Prognostic value of tumour-infiltrating
lymphocytes (TILs) in colorectal cancer. J Pathol. 182:318–324.
1997. View Article : Google Scholar : PubMed/NCBI
|
|
21
|
Massa F, Marsicano G, Hermann H, et al:
The endogenous cannabinoid system protects against colonic
inflammation. J Clin Invest. 113:1202–1209. 2004. View Article : Google Scholar : PubMed/NCBI
|
|
22
|
Shaul YD and Seger R: The MEK/ERK cascade:
from signaling specificity to diverse functions. Biochim Biophys
Acta. 1773:1213–1226. 2007. View Article : Google Scholar : PubMed/NCBI
|
|
23
|
Cudaback E, Marrs W, Moeller T and Stella
N: The expression level of CB1 and CB2 receptors determines their
efficacy at inducing apoptosis in astrocytomas. PLoS One.
5:e87022010. View Article : Google Scholar : PubMed/NCBI
|
|
24
|
Malfitano AM, Laezza C, Galgani M, et al:
The CB1 receptor antagonist rimonabant controls cell viability and
ascitic tumour growth in mice. Pharmacol Res. 65:365–371. 2012.
View Article : Google Scholar : PubMed/NCBI
|