Introduction
Median raphe cyst is a rare benign lesion located in
the median raphe and is thought to be derived from the urethral
mucosa or urethral gland (Littre’s gland). It appears commonly in
children or adolescents. The normal urethral mucosa and the
epithelial cells of the median raphe cyst usually lack melanocytes
and/or melanin pigment. However, albeit extremely rare, the
presence of melanin pigment and/or melanocytes in median raphe
cyst, namely pigmented median raphe cyst, has been reported,
although the pathogenesis of melanocytic colonization in this tumor
has not been clarified (1–5). Herein, we report the sixth case of
pigmented median raphe cyst and discuss the possible mechanisms of
melanocytic colonization in this tumor. Written informed consent
was obtained from the patient.
Case report
Case presentation
A 48-year-old male presented with a nodule on the
ventral aspect of the penis, which had been recognized since
childhood. Physical examination revealed that the nodule was
slightly elevated with a smooth surface, skin-colored, elastic,
soft and measured 10×3.5 mm2, on the median raphe of the
penis. Surgical resection of the nodule was performed under the
clinical diagnosis of median raphe cyst.
Immunohistochemistry
The formalin-fixed, paraffin-embedded tissue blocks
of the resected specimen were sectioned (3 μm thick),
deparaffinized and rehydrated. Each section was stained with
hematoxylin and eosin and then used for immunostaining.
Immunohistochemical analyses were performed using an autostainer
(Benchmark XT system; Ventana Medical Systems, Inc., Tucson, AZ,
USA) according to the manufacturer’s instructions. The following
primary antibodies were used: Mouse monoclonal antibodies against
α-smooth muscle actin (alphasm-1; Novocastra Laboratories, Ltd.,
Newcastle upon Tyne, UK), endothelin-1 (TR.ET.48.5; Sigma-Aldrich,
St. Louis, Missouri, USA), gross cystic disease fluid protein-15
(GCDFP-15; 23A3; Novocastra Laboratories, Ltd.), HMB-45 (HMB-45;
Novocastra Laboratories, Ltd.), Melan-A (A103; Novocastra
Laboratories, Ltd.) and stem cell factor (G-3; Santa Cruz
Biotechnology, Inc., Santa Cruz, CA, USA); and a rabbit polyclonal
antibody against S-100 protein (Nichirei Biosciences Inc., Tokyo,
Japan).
Histopathological and immunohistochemical
results
Histopathological analysis revealed that a
unilocular cyst was present under the squamous epithelium. The cyst
wall was covered by two to several layers of uniform cuboidal to
urothelial cells without nuclear atypia. Decapitation secretion and
mucinous and ciliated cells were not observed. In addition, no
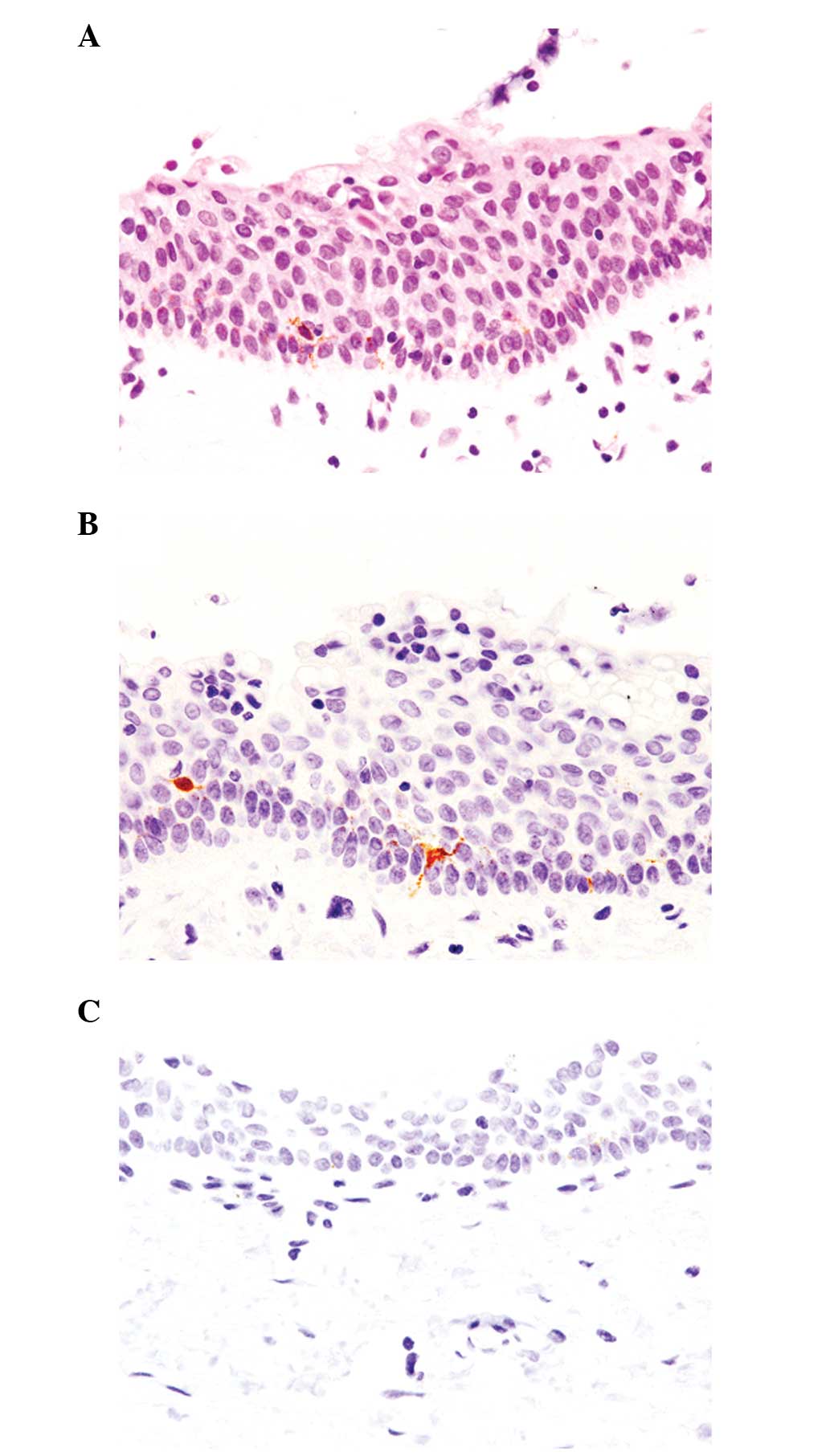
mitotic figures were present. The unusual observation was the
presence of dendritic melanocytes among the epithelial cells
(Fig. 1A).
Immunohistochemical analyses showed that these
dendritic melanocytes were positive for Melan-A and S-100 protein
(Fig. 1B), but negative for HMB-45.
GCDFP-15 was negative in the epithelial cells and α-smooth muscle
actin-positive myoepithelial cells were not present. Moreover, stem
cell factor and endothelin-1 were not expressed in the epithelial
cells (Fig. 1C).
According to these histopathological and
immunohistochemical results, an ultimate diagnosis of pigmented
median raphe cyst was determined.
Discussion
The cyst wall of the median raphe cyst is lined by
cuboidal to columnar cells, transitional (urothelial) cells,
stratified squamous cells or a mixture of these (4). The presence of mucous and ciliated
cells and decapitation secretion have also been previously reported
(5). Albeit rare, the presence of
melanin pigment and/or melanocytes in median raphe cyst, namely
pigmented median raphe cyst, has been documented (4). Previously, Nishida et al
summarized the clinicopathological features of pigmented median
raphe cyst (4). According to the
analyses, the incidence of this variant is 2.1% and no
clinicopathological differences have been identified between the
pigmented and conventional cysts, with the exception of the
presence or absence of melanin pigment and/or melanocytes (4).
It is well-known that non-neoplastic melanocytes are
rarely found in various benign and malignant non-melanocytic tumors
of the various sites, a phenomenon known as ‘colonization’
(6–10). The urethral mucosa is normally
devoid of melanocytes and the mechanism by which melanocytes and/or
melanin pigment appear in median raphe cyst remains unclear.
Previously, a few hypotheses with regard to melanocytic
colonization in non-melanocytic lesions have been proposed. For
example, it has been suggested that the presence of melanocytes may
be presented as heterotopic cell rests resulting from aberrant
melanocytic migration during the embryonic period (4). It has also been hypothesized that the
epithelial cells may produce factors that simulate the
proliferation and differentiation of melanocytes, such as stem cell
factor and endothelin-1 (11).
Satomura et al reported a case of pigmented squamous cell
carcinoma of the hard palate. The authors clearly demonstrated stem
cell factor and endothelin-1 expression in the neoplastic squamous
cells, which may have led to the development of melanocytic
colonization in squamous cell carcinoma (11).
The current case report is the first to analyze the
immunohistochemical expression of stem cell factor and endothelin-1
in median raphe cyst. It was revealed that the epithelial cells of
the median raphe cyst showed negative immunoreactivity for these
markers. Therefore, colonization of melanocytes in median raphe
cyst is not associated with the production of stem cell factor and
endothelin-1 by the epithelial cells of the cyst. In addition,
aberrant migration of melanocytes may contribute to the development
of this rare lesion. In conclusion, this report is the first to
analyze the immunohistochemical expression of melanocytic
proliferation and differentiation factors, and demonstrate that
they are not involved in the pigmentation of median raphe cyst.
Therefore, aberrant migration of melanocytes may contribute to the
development of this rare lesion. Further analysis is required to
clarify the pathogenesis of pigmented median raphe cyst.
References
|
1
|
Fetissof F, Lorette G, Dubois MP, Philippe
A, Tharanne MJ and Jobard P: Endocrine cells in median raphe cyst
of the penis. Pathol Res Pract. 180:644–646. 1985. View Article : Google Scholar
|
|
2
|
Hitti IF, Vuletin JC and Rapuano J: Giant
median raphe cyst of the penis with diffuse melanosis of its
epithelial lining. Urol Int. 44:121–124. 1989. View Article : Google Scholar : PubMed/NCBI
|
|
3
|
Urahashi J, Hara H, Yamaguchi Z and
Morishima T: Pigmented median raphe cysts of the penis. Acta Derm
Venereol. 80:297–298. 2000. View Article : Google Scholar : PubMed/NCBI
|
|
4
|
Nishida H, Kashima K, Daa T, et al:
Pigmented median raphe cyst of the penis. J Cutan Pathol.
39:808–810. 2012. View Article : Google Scholar : PubMed/NCBI
|
|
5
|
Shao IH, Chen TD, Shao HT and Chen HW:
Male median raphe cysts: serial retrospective analysis and
histopathological classification. Diagn Pathol. 7:1212012.
View Article : Google Scholar : PubMed/NCBI
|
|
6
|
Ishida M, Kagotani A, Yoshida K and Okabe
H: Pigmented cervical intraepithelial neoplasia. Int J Gynecol
Pathol. 32:146–147. 2013. View Article : Google Scholar : PubMed/NCBI
|
|
7
|
Ishida M, Hotta M, Kushima R and Okabe H:
A case of porocarcinoma arising in pigmented hidroacanthoma simplex
with multiple lymph node, liver and bone metastases. J Cutan
Pathol. 38:227–231. 2011. View Article : Google Scholar : PubMed/NCBI
|
|
8
|
Ishida M, Yoshida K, Kagotani A, et al:
Pigmented Paget’s disease: a diagnostic pitfall. Diagn Cytopathol.
2013.(In press).
|
|
9
|
Ishida M and Okabe H: Pigmented anal gland
adenocarcinoma with pagetoid spread. J Cutan Pathol. 40:428–430.
2013. View Article : Google Scholar : PubMed/NCBI
|
|
10
|
Ishida M, Koshinuma S, Oue K, Higo T,
Yamamoto G and Okabe H: Pigmented keratocystic odontogenic tumor: a
case report with review of the literature. Mol Clin Oncol.
1:430–432. 2013.
|
|
11
|
Satomura K, Tokuyama R, Yamasaki Y, et al:
Possible involvement of stem cell factor and endothelin-1 in the
emergence of pigmented squamous cell carcinoma in oral mucosa. J
Oral Pathol Med. 36:621–624. 2007. View Article : Google Scholar : PubMed/NCBI
|