Introduction
Tumour size (TSize) has long been used as a variable
of prognostic significance and is employed universally in staging
systems for all solid tumours (1).
With the evolution of surgical techniques, boundaries continue to
be pushed and the prediction of which patients will definitively
benefit from resection has never been so important. Accordingly,
there is an increased emphasis on improving staging systems that
incorporate variables of the greatest prognostic significance. In
pancreatic ductal adenocarcinoma (PDAC), primary tumour
characteristics are known to be the most important determinants of
outcome (2).
Tumour volume (TVol) has been investigated as a
marker of prognosis in lung cancer (3), prostate cancer (4), renal cell carcinoma (5), tongue cancer (6), peri-ampullary malignancy (7) and osteosarcoma (8). When compared with existing staging
variables, TVol has been shown to enhance outcome prediction
significantly, above and beyond single dimensions such as TSize
(3–6,8). This is
logical, given that solid tumours are three-dimensional structures
and one dimension, whilst generally associated with outcome, may
not accurately reflect the primary tumour burden of the
disease.
Despite the investigation of a number of solid organ
tumour types, PDAC TVol has not been examined and compared with
TSize specifically with regard to perioperative variables and
outcome. Using a retrospective analysis of the prospective
institutional database for the Royal North Shore Hospital (St.
Leonards, NSW, Australia), we hypothesised that TVol would
significantly predict outcome better that TSize alone, following
pancreatoduodenectomy (PD) for pancreatic head PDAC.
Materials and methods
Study approval
Approval was granted from the Northern Sydney Area
Health Service Human Research Ethics Committee prior to study
commencement.
Patients
Pancreatic resection data from the Royal North Shore
Hospital Campus of Sydney University was prospectively collated
over the period of April 2004 to November 2010. A total of 198 PD's
were performed during this period for a number of indications.
Cases not involving PDAC as the primary indication for resection
were excluded. In order to calculate TVol, only cases where
histopathology reports included three measured tumour dimensions
were included. Following exclusion of non-PDAC cases and those with
inadequate pathology data, 103 cases of were available for
analysis.
Demographic data was obtained in addition to
American Society of Anaesthesiologists (ASA) grading. Perioperative
clinical data included surgical time, intraoperative blood loss,
perioperative blood transfusion requirements, hospital stay (days),
complications (and complication grade), in hospital and 90 day
mortality. Histopathological data included three tumour dimensions,
margin (R) status, evidence of neurovascular invasion and the
number of lymph nodes resected (including the number positive for
disease). Clinical follow up at three-month intervals (up to a
year), six-month intervals (up to two years) and annually
thereafter, enabled collation of survival data.
Collation of three tumour dimensions enabled
analysis of primary TSize (defined by the maximum tumour
dimension), mean TSize (the mean of three tumour dimensions) and
TVol. TVol was calculated according to the formula for an ellipse
using the radius (r) of three reported tumour dimensions as
follows: 4/3π(r1×r2×r3) (5,7,8). For the
purposes of sub-group analysis, patients were dichotomised into
high and low TVol groups (based on TVol above and below the overall
median TVol, respectively). This was repeated for high and low
TSize (greatest tumour dimension) to enable a comparison between
TVol and TSize.
Statistical analysis
Univariate and multivariate logistic regression was
used to identify TVol associations with outcome. χ2
tests, Fisher's exact tests and Mann-Whitney U tests were used to
compare variables between high and low TVol groups where
appropriate. Survival data was assessed between these two groups
with Kaplan-Meier curves and a log-rank test. P<0.05 was
considered to indicate a statistically significant difference. All
statistical analyses were performed using Stata/IC12 (StataCorp LP,
College Station, TX, USA).
Results
In total 103 patients underwent PD for PDAC and had
three reported macroscopic tumour dimensions available for
analysis. Within this cohort, the median age was 67 years (range,
34–83 years) and 55% of patients were male (57 males vs. 46
females). The median ASA grading was 2 (range, 1–4).
Table I shows a
summary of selective clinicopathological indices for all patients.
Tables II and III present univariate and multivariate
regression analysis data using mortality as the dependent variable
of interest.
 | Table I.Clinicopathological data for all cases
(n=103). |
Table I.
Clinicopathological data for all cases
(n=103).
| Variable | Value |
|---|
| Median age (range),
years | 66 (34–83) |
| Gender, n (%) |
|
| Male | 57 (55.3) |
|
Female | 46 (44.7) |
| Median ASA grade
(range) | 2 (1–4) |
| Surgical
timea, min | 432.9±39.7 |
| Vascular resection,
% | 52.4 |
| Intraoperative blood
lossa, ml | 660.3±63.7 |
| Perioperative
transfusion, % | 22.0 |
| Complications, % | 34.6 |
| Hospital stay,
daysa | 15.8±1.3 |
| TSizea,b,
mm | 38.5±3.4 |
| Mean
TSizea,c, mm | 30.1±1.1 |
| Tumour
volumea,
cm3 | 19.7±1.9 |
| Histological
graded, n (%) |
|
| Well | 4 (3.9) |
|
Moderate | 68 (66.0) |
| Poor | 27 (26.2) |
|
Undifferentiated | 3 (2.9) |
| Neural invasion,
% | 73.8 |
| Vascular invasion,
% | 67.9 |
| Positive margin,
% | 34.9 |
| Lymph node
yielda | 19±1.7 |
| Lymph node-positive,
% | 70.8 |
| Overall 2-year
survival, % | 34.1 |
 | Table II.Univariate analysis of
clinicopathological variable associations with mortality. |
Table II.
Univariate analysis of
clinicopathological variable associations with mortality.
| Variable | OR | 95% CI | P-value |
|---|
| Age | 1.02 | 0.98–1.07 | 0.302 |
| ASA | 1.20 | 0.72–2.00 | 0.488 |
| Surgical time | 0.99 | 0.99–1.00 | 0.619 |
| Vascular
resection | 1.64 | 0.75–3.59 | 0.212 |
| Intraoperative blood
loss | 1.00 | 0.99–1.00 | 0.159 |
| Perioperative
transfusion | 4.18 | 1.42–12.37 | 0.010 |
| Complications | 0.81 | 0.36–1.83 | 0.613 |
| Hospital stay | 0.99 | 0.94–1.05 | 0.785 |
| Tumour size | 1.01 | 0.99–1.04 | 0.300 |
| Tumour volume | 1.00 | 0.99–1.00 | 0.478 |
| Histological
grade | 1.58 | 0.80–3.11 | 0.183 |
| Neural invasion | 4.90 | 1.84–13.03 | 0.001 |
| Vascular
invasion | 3.38 | 1.41–8.09 | 0.006 |
| Positive margin | 1.94 | 0.84–4.45 | 0.120 |
| Lymph
node-positive | 2.15 | 0.90–5.11 | 0.083 |
 | Table III.Multivariate analysis of
clinicopathological variable associations with mortality (using a
univariate P-value of <0.1 for model inclusion). |
Table III.
Multivariate analysis of
clinicopathological variable associations with mortality (using a
univariate P-value of <0.1 for model inclusion).
| Variable | OR | 95% CI | P-value |
|---|
| Perioperative
transfusion | 2.98 | 0.95–9.35 | 0.061 |
| Tumour size | 0.99 | 0.96–1.04 | 0.950 |
| Tumour volume | 1.00 | 0.99–1.01 | 0.586 |
| Neural invasion | 3.94 | 1.36–11.40 | 0.011 |
| Vascular
invasion | 2.23 | 0.79–6.30 | 0.132 |
| Lymph
node-positive | 1.24 | 0.44–3.53 | 0.680 |
Univariate analysis identified perioperative blood
transfusion, and neural and vascular invasion to be significantly
associated with post-resection mortality. When included in a
multivariate regression model, neural invasion remained as the only
variable significantly associated with mortality [odds ratio, 3.94;
95% confidence interval (CI), 1.36–11.40; P=0.011].
Pairwise analyses showed significant correlations
between TSize and the variables of mean TSize (coeff., 0.87;
P<0.001) and TVol (coeff., 0.73; P<0.001). Further analysis
with an emphasis on TSize and TVol revealed a modest increase in
the variability accounted for by the regression model when
including TVol (without TVol, 14.5%; P=0.002; vs. with TVol, 15.7%;
P=0.001). When specifically comparing TVol with TSize (by
exchanging them in the regression analysis), TVol marginally
improved the prediction of mortality (14.7%, P=0.001 vs. 14.9%,
P=0.001). Additionally, linear regression analysis demonstrated a
significant negative correlation between the pancreatic neck margin
and TVol (P=0.007).
Table IV compares
outcome variables between high and low TVol cases. When compared
with low TVol, high TVol cases involved longer surgical times
(P<0.001), a greater requirement for vascular resection
(P=0.007) and higher intraoperative blood losses (P=0.007).
 | Table IV.Comparison between high and low TVol
groups. |
Table IV.
Comparison between high and low TVol
groups.
| Variable | Low TVol | High TVol | P-value |
|---|
| Number of
patients | 5 | 53 |
|
| Median age (range),
years | 68 (46–83) | 65.5 (34–82) | 0.077 |
| ASA grade | 2.0 (1–4) | 2.0 (1–3) | 0.469 |
| Median surgical
time (range), min | 390 (290–620) | 430 (290–720) | <0.001 |
| Vascular resection,
n (%) | 20 (39.2) | 34 (65.4) | 0.007 |
| Median
intraoperative blood loss (range), ml | 500 (90–2400) | 745 (250–2360) | 0.007 |
| Perioperative
transfusion, n (%) | 8 (15.7) | 15 (28.9) | 0.085 |
| Complications, n
(%) | 16 (31.4) | 20 (38.5) | 0.537 |
| Median hospital
stay (range), days | 13 (7–36) | 13 (9–41) | 0.573 |
| Median tumour size
(range), mm | 30 (15–45) | 45 (27–100) | <0.001 |
| Median tumour
volume (range), cm3 | 5.37
(0.6–11.8) | 20.9
(11.5–138.2) | <0.001 |
| Histological grade,
n (%) |
|
|
|
|
Well | 2 (3.9) | 3 (5.8) | 0.280 |
|
Moderate | 33 (64.7) | 35 (67.3) |
|
|
Poor | 16 (31.4) | 11 (2.1) |
|
|
Undifferentiated | 3 (5.8) |
|
|
| Neural invasion, n
(%) | 36 (70.6) | 40 (76.9) | 0.306 |
| Vascular invasion,
n (%) | 32 (62.8) | 38 (73.1) | 0.181 |
| Positive margin, n
(%) | 18 (35.3) | 18 (34.6) | 0.553 |
| Median lymph node
yield (range), n | 17 (4–65) | 17.5 (6–43) | 0.436 |
| Median lymph
node-positive (range), n | 37 (72.6) | 36 (69.2) | 0.439 |
| 2-year survival,
% | 41.2 | 26.9 | 0.068 |
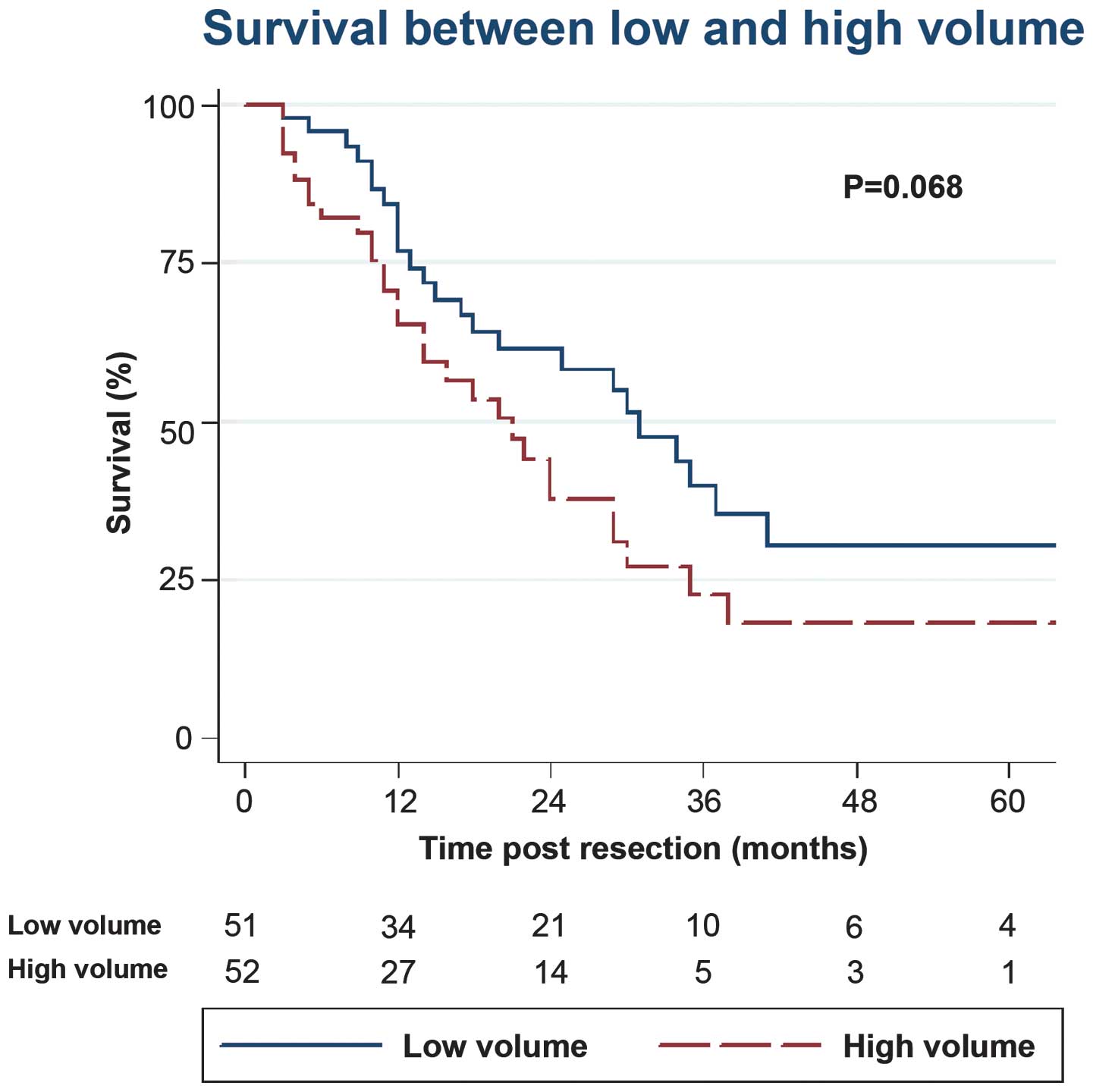
The two-year survival rate was 41.2% in the low TVol
group compared with 26.9% in the high TVol group. Fig. 1 displays Kaplan-Meier survival curves
between the groups [hazards ratio (HR), 1.65; 95% CI, 0.96–2.84;
P=0.068). This compares with TSize, which when divided into groups
above and below the median, did not approach a significant
difference (HR, 1.44; 95% CI, 0.84–2.47; P=0.182).
Discussion
It is well known that TSize impacts directly on
clinical outcome in a multitude of cancer types, including PDAC
(2), and it is a logical assumption
to suggest that this would generally hold true of TVol. In keeping
with this, the present analysis showed that TSize and TVol are
negatively associated with survival. The real issue under
contention, however, is that of the superiority of TVol to existing
prognostic variables, such as TSize, which has never truly been
tested in PDAC.
In 1993, Sellner and Machacek (7) reported their analysis of a cohort of
patients with mixed periampullary cancer, in a study that grouped
together patients with lower common bile duct cancer, cancer of the
ampulla of Vater and 49 patients with carcinoma of the pancreatic
head. By using three dimensions to calculate TVol, as in the
present study, the study demonstrated a negative association
between survival time and TVol. This finding was reinforced by the
present study and stands as the only other report of associations
between clinical outcome and TVol in pancreatic cancer. Further
discussion of the study by Sellner and Machacek (7) is limited by the fact that the three
aforementioned and distinct malignancies were grouped for the
purposes of further analysis. Given that these diseases are now
known to harbour a specific natural history, and convey a differing
prognosis, further information regarding PDAC TVol in isolation was
unable to be deduced. Furthermore, no comparison with TSize was
undertaken.
Despite previous studies showing significant
correlations between outcome and TVol in a number of solid tumours
(3–8),
the present analysis failed to demonstrate the same degree of
prognostic value beyond simple TSize. This is difficult to
reconcile in the absence of previous studies with a specific focus
on and adequate analysis of PDAC. It may be that the
three-dimensional tumour burden (as calculated in the present
study) does not convey the same prognostic value as it does in
other malignancies.
Although previous studies have reported prognostic
associations with TVol, it should also be noted that there exists
disagreement in the literature, with prostate cancer being a good
example. While the study of Chun et al (4) previously concluded that prostate TVol
predicts prognosis, other studies have failed to find any
correlation with outcome (9,10). In a study of almost 900 men with
localised prostate cancer and TVol data, Porten et al
(9) conclude that ‘there is no
evidence that TVol is an independent predictor of prostate cancer
outcome’. Additionally, Wolters et al found that although a
computer-assisted determination of prostate TVol did correlate with
existing markers of prognosis, volume itself failed to be a
significant independent predictor of outcome following multivariate
analysis (10). These findings are
similar to those of the present study of post-resection PDAC
outcome, whereby associations between existing prognostic markers
(e.g., neural invasion) and TVol were observed (data not shown),
but TVol was not shown to be an independent predictor of
mortality.
Heterogeneity in the literature is further
compounded by the various methods employed to calculate TVol; thus
making comparisons between studies, even if focussed on the same
tumour type, difficult. In the present study, the single centre
pathology unit that was involved prospectively measured three
tumour dimensions at the time of formal histopathological
assessment. These values were collated retrospectively and the TVol
was calculated using the formula for the volume of an ellipse. This
method has successfully been applied to osteosarcoma (8) and nephrectomy specimens for renal cell
carcinoma (5). In a subset of renal
cell carcinoma patients, Jorns et al (5) showed that the risk of mortality was
significantly higher in patients with an ellipsoidal TVol above the
median compared with simple TSize above the median. Although not
proving to be significant, a similar trend was observed in the
present analysis of PDAC (Fig. 1) and
suggests that the additional tumour dimensions can be useful in
translating the true tumour burden, as it relates to mortality
outcome.
A variety of methods have been reported in the
literature to assess TVol and may explain certain disparities in
the results between studies. Simple cuboidal (7) and ellipsoidal (5,7,8) volume calculations based on macroscopic
tumour dimensions have been supplemented by computer-assisted
morphometric assessments, (10)
magnetic resonance imaging volumetric reconstructions (6) and whole-body metabolic positron emission
tomography volume imaging (3). The
use of such imaging modalities to assess TVol and associations with
outcome is an increasing trend that may ultimately lead to specific
changes in management. Possessing the capacity to accurately
predict who may or may not benefit from aggressive surgical
intervention based on relatively simple indices, such as in
vivo TVol, is an attractive proposition (2).
The method of calculating TVol would also
theoretically benefit from inclusion of a correction factor based
on the individual patient's body composition. It could be assumed
that a 5-cm tumour in a 50-kg female represents a significantly
larger tumour burden when compared to the same absolute TSize in a
100-kg male. A simple method to normalise TVol for organ size has
been employed previously in thyroid surgery and relies only on a
simple calculation of body surface area (11). Minimal data regarding body composition
(e.g., height and weight) was not available for the present
analysis, but should be borne in mind for future studies. Although
the resected pancreatic head dimensions and weight were available,
these variables reflect more on the technical resection, rather
than the patient's size.
Beyond independent TVol associations with mortality
outcome, this study has revealed additional findings of
significance. Univariate analysis showed that neural and vascular
invasion were associated with a worse outcome, as was perioperative
transfusion. These concepts have been highlighted previously
(2) and the finding of neural
invasion as an independent predictor of mortality following
multivariate analysis supports its use as a prognostic and reported
variable of significance.
It was also found that a higher TVol was associated
with a closer pancreatic neck margin and a higher rate of formal
vascular resection in the present study. In keeping with this, and
as expected, a higher TVol is also correlated with longer surgical
times and larger intraoperative blood losses. A longer surgery,
vascular resection, closer pancreatic neck margins, higher
intraoperative blood losses and perioperative transfusion are all
known to be independently negative prognostic variables (2,12–14). Multivariate analysis was therefore
employed in the present study in an effort to control for the
effect of these confounding factors on outcome when considering
TVol and mortality in isolation.
A drawback of the present study was the absence of
additional data regarding outcome and therapy. Knowledge of local
recurrence, development of distant metastases, and the use of
neo-adjuvant and adjuvant therapy would have been ideal in an
attempt to control for all factors that affect outcome. This data
was not available for the present analysis. It is also unknown if
TVol more precisely predicts for recurrence, as opposed to
mortality due to disease for instance.
In conclusion, the ability to accurately predict the
true tumour burden and the impact this may have on the natural
history of an individual patient's outcome is now more poignant
than ever. Clinicians now work in a translational environment, and
an individual patient's tumour genotype and phenotype are
increasingly dictating management. Formal assessment of TVol
represents additional information regarding tumour phenotype that
should not be ignored, and in time, may be shown to be clearly
superior to simple TSize, which is so highly emphasised in today's
staging systems. The next challenge lies in identifying the best
method to employ to extract this valuable prognostic
information.
References
|
1
|
AJCC, . Staging Resources. 2013,
http://www.cancerstaging.org/Accessed. July
1–2014
|
|
2
|
Garcea G, Dennison AR, Pattenden CJ, Neal
CP, Sutton CD and Berry DP: Survival following curative resection
for pancreatic ductal adenocarcinoma. A systematic review of the
literature. JOP. 9:99–132. 2008.PubMed/NCBI
|
|
3
|
Oh JR, Seo JH, Chong A, Min JJ, Song HC,
Kim YC and Bom HS: Whole-body metabolic tumour volume of 18F-FDG
PET/CT improves the prediction of prognosis in small cell lung
cancer. Eur J Nucl Med Mol Imaging. 39:925–935. 2012. View Article : Google Scholar : PubMed/NCBI
|
|
4
|
Chun FK, Briganti A, Jeldres C, Gallina A,
Erbersdobler A, Schlomm T, Walz J, Eichelberg C, Salomon G, Haese
A, et al: Tumour volume and high grade tumour volume are the best
predictors of pathologic stage and biochemical recurrence after
radical prostatectomy. Eur J Cancer. 43:536–543. 2007. View Article : Google Scholar : PubMed/NCBI
|
|
5
|
Jorns J, Thiel DD, Lohse CM, Williams A,
Arnold ML, Cheville JC, Leibovich BC and Parker AS:
Three-dimensional tumour volume and cancer-specific survival for
patients undergoing nephrectomy to treat pT1 clear-cell renal cell
carcinoma. BJU Int. 110:956–960. 2012. View Article : Google Scholar : PubMed/NCBI
|
|
6
|
Chew MH, Khoo JBK, Chong VFH, Tai BC, Soo
KC and Lim DT: Significance of tumour volume measurements in tongue
cancer: A novel role in staging. ANZ J Surg. 77:632–637. 2007.
View Article : Google Scholar : PubMed/NCBI
|
|
7
|
Sellner F and Machacek E: The importance
of tumour volume in the prognosis of radically treated
periampullary carcinomas. Eur J Surg. 159:95–100. 1993.PubMed/NCBI
|
|
8
|
Munajat I, Zulmi W, Norazman MZ and Wan
Faisham WI: Tumour volume and lung metastasis in patients with
osteosarcoma. J Orthop Surg (Hong Kong). 16:182–185.
2008.PubMed/NCBI
|
|
9
|
Porten SP, Cooperberg MR and Carroll PR:
The independent value of tumour volume in a contemporary cohort of
men treated with radical prostatectomy for clinically localized
disease. BJU Int. 105:472–475. 2010. View Article : Google Scholar : PubMed/NCBI
|
|
10
|
Wolters T, Roobol MJ, van Leeuwen PJ, van
den Bergh RC, Hoedemaeker RF, van Leenders GJ, Schröder FH and van
der Kwast TH: Should pathologists routinely report prostate tumour
volume? The prognostic value of tumour volume in prostate cancer.
Eur Urol. 57:821–829. 2010. View Article : Google Scholar : PubMed/NCBI
|
|
11
|
Moon HG, Jung EJ, Park ST, Jung TS, Jeong
CY, Ju YT, Lee YJ, Hong SC, Choi SK and Ha WS: Thyrotropin level
and thyroid volume for prediction of hypothyroidism following
hemithyroidectomy in an Asian patient cohort. World J Surg.
32:2503–2508. 2008. View Article : Google Scholar : PubMed/NCBI
|
|
12
|
Chang DK, Johns AL, Merrett ND, Gill AJ,
Colvin EK, Scarlett CJ, Nguyen NQ, Leong RW, Cosman PH, Kelly MI,
et al: Margin clearance and outcome in resected pancreatic cancer.
J Clin Oncol. 27:2855–2862. 2009. View Article : Google Scholar : PubMed/NCBI
|
|
13
|
Fatima J, Schnelldorfer T, Barton J, Wood
CM, Wiste HJ, Smyrk TC, Zhang L, Sarr MG, Nagorney DM and Farnell
MB: Pancreatoduodenectomy for ductal adenocarcinoma: Implications
of positive margin on survival. Arch Surg. 145:167–172. 2010.
View Article : Google Scholar : PubMed/NCBI
|
|
14
|
Fukuda S, Oussoultzoglou E, Bachellier P,
Rosso E, Nakano H, Audet M and Jaeck D: Significance of the depth
of portal vein wall invasion after curative resection for
pancreatic adenocarcinoma. Arch Surg. 142:172–180. 2007. View Article : Google Scholar : PubMed/NCBI
|