Introduction
Recent advances in the biology of non-small cell
lung cancer (NSCLC) have identified driver mutations that can
predict response to the therapy. This molecularly targeted therapy
has dramatically improved results for patients whose tumors harbor
somatically activated oncogenes, such as epidermal growth factor
receptor (EGFR), anaplastic lymphoma receptor tyrosine
kinase (ALK), ret proto-oncogene (RET) or ROS
proto-oncogene 1 (ROS1) (1–3). Although
EGFR mutations and ALK, RET and ROS1
translocations are predominantly detected in lung adenocarcinomas
from never-smokers and light smokers, these associations are not
absolute; thus, clinical profile must not be used to exclude
patients from molecular testing for specific alterations (4).
Activating rearrangements of ALK gene are
detectable in 1.9–6.8% of NSCLC cases (5–9). In these
tumors, a fusion gene involving echinoderm microtubule associated
protein-like 4 (EML4) and ALK (EML4-ALK)
encodes a chimeric protein with constitutive tyrosine kinase
activity that confers transformation potential and responsiveness
to specific targeted inhibitors (5).
Whereas the fused ALK gene region remains constant (exon
20), different EML4 exons can be affected, generating
several variants; other ALK fusion partners have also been
reported (10,11). In patients with ALK-positive
NSCLC, the use of crizotinib, an oral ATP-competitive selective
inhibitor of the ALK tyrosine kinase, along with a new
generation of ALK tyrosine kinase inhibitors (alectinib and
ceritinib), has demonstrated superiority over standard chemotherapy
(3,4).
Fluorescence in situ hybridization (FISH),
bright-field dual-color chromogenic in situ hybridization
(12), immunohistochemistry (IHC)
(7,12)
and reverse transcriptase-polymerase chain reaction (13) are available methods for the detection
of ALK rearrangements. ALK FISH has been recognized
as the most sensitive method (9).
Recently, the FDA has approved the Ventana ALK (D5F3) CDx Assay
(Roche, Tucson, AZ, USA) to identify patients for crizotinib
therapy. Ultrasensitive IHC assays may obviate FISH confirmation in
positive IHC cases; however, the likelihood of false negative IHC
results demands FISH testing, at least in some situations (7,8,12). Currently, the only approved FISH assay
for the detection of ALK positivity, as a companion
diagnostic tool for crizotinib-based treatment eligibility, is the
Vysis ALK Break Apart FISH Probe Kit (Abbott Molecular, Des
Plaines, IL, USA).
In the current study, we describe our experience of
FISH ALK rearrangement detection in 2,045 routine diagnostic
samples in the public health care system of Galicia (Spain). This
report is of particular interest for comparative purposes due to
Galicia's isolation in North-Western Spain and its specific
cultural characteristics, which may contribute to the emergence of
genetic diversity (14).
Materials and methods
Patients and samples
A total of 2,045 unselected samples of NSCLC from
patients in 9 hospitals of the Galician public health care system
(Spain), collected between October 2010 and July 2015, were
investigated. Samples were received as buffered formalin-fixed,
paraffin-embedded tissue biopsies, cell blocks and cytological
smears. In the referral center (Clinical University Hospital,
Santiago de Compostela, Spain), pathologists verified the adequacy
of the samples and reviewed the diagnosis according to the World
Health Organization criteria (1). For
all patients, medical records were reviewed, and written informed
consent obtained. The Independent Ethics Committee of Galicia
(Galician Healthcare Service; SERGAS) approved the study protocol,
which was conducted in accordance with the Declaration of Helsinki
and applicable Spanish laws.
ALK FISH analysis
The ALK genetic status of each patient was
evaluated by FISH in representative tumor areas, with an LSI
ALK dual-color, break-apart rearrangement probe (Vysis
ALK Break Apart FISH Probe Kit, Abbott Molecular Inc.),
following the manufacturer's protocol. In each case, 50
non-overlapping nuclei were examined by fluorescence microscope
(BX51; Olympus Corporation, Barcelona, Spain). The kit included red
(3′) and green (5′) break-apart probes. ALK was determined
to be not rearranged when the two signals were adjacent or fused
(appearing yellow under an Orange/Green V2 filter) or when there
was a single green signal. ALK was considered positive
(rearranged) when ≥1 set of red and green signals were ≥2 signal
diameters apart, or when a single red signal was present. A sample
was considered negative for ALK if <5 cells out of 50
(<10%), and positive when >25 cells out of 50 (>50%),
exhibited split ALK 5′ and 3′ probe signals or isolated 3′
signals. With borderline results, when the number of positive cells
was 5–25 (10–50%), a second reader evaluated the slide: First and
second cell count readings were added together and a percentage out
of 100 cells was calculated. If the positive cell percentage was
≥15%, the sample was considered positive.
Statistical analysis
Statistical analysis was conducted with SPSS version
19.0 (IBM SPSS, Armonk, NY, USA). The association between
ALK mutation status and clinicopathological features was
calculated using Pearson's χ2 test or Fisher's exact
test. P<0.05 was considered to indicated a statistically
significant difference.
Results
ALK assessment
The 2,045 samples of NSCLC included 1,686 (82.4%)
tissue biopsies, 306 (15%) cell block samples and 53 (2.6%)
cytological smears. Among the total samples examined, 1,866 (91.2%)
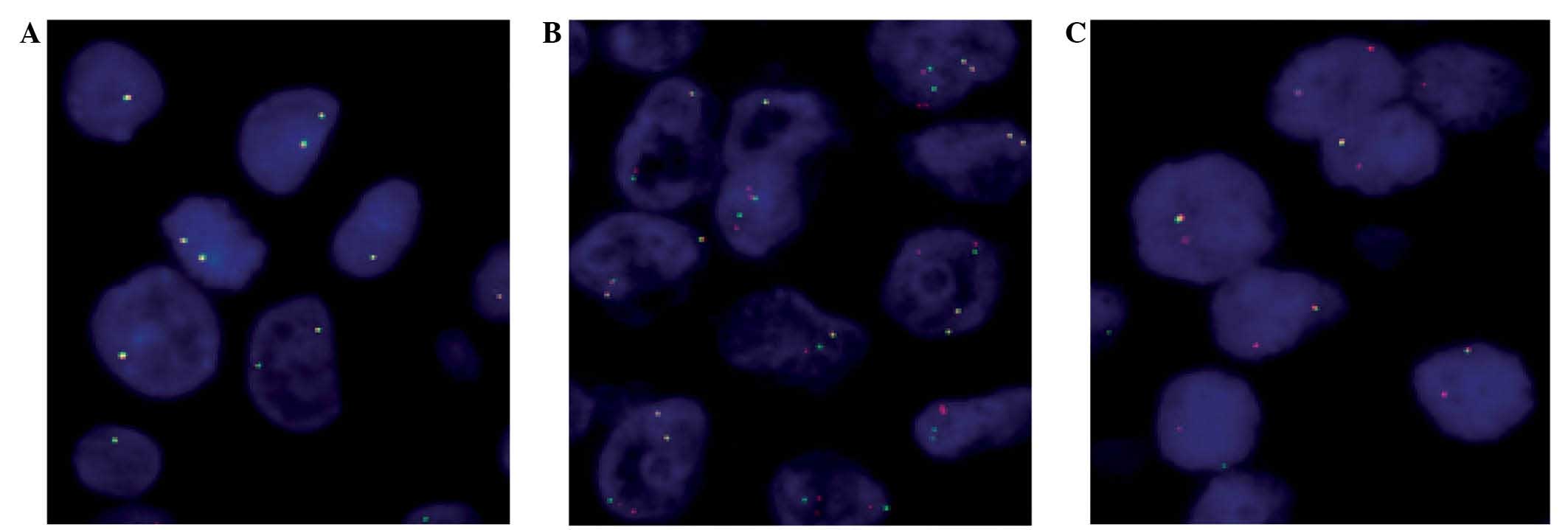
could be tested by FISH (Fig. 1).
Specifically, 1,566 (92.9%) tissue biopsies, 256 (83.7%) cell
blocks and 46 (86.8%) cytological smears could be assessed. In the
remaining 179 (8.8%) samples, the FISH result was not obtained
owing to insufficient/non-representative tumor material (n=143;
79.9%) or to assay failure (n=36; 20.1%) due to pre-analytical
factors (poor fixation, decalcification treatment, etc.). The rate
of successful evaluation was not significantly higher in
histological samples compared with cytological samples (92.9% vs.
84.1%). Additionally, no differences were found between cell blocks
and cytological smears (83.7% vs. 86.8%).
ALK rearrangement
ALK rearrangements were identified in 82 (4%)
out of 2,045 tumor samples: 65 (79.3%) tissue biopsies, 15 (18.3%)
cell blocks and 2 (2.4%) cytological smears (Table I). The mean percentage of
ALK-positive cells was 52% (range, 15–92%). A typical
translocation pattern was observed in 62 (75.6%) cases, and the
remaining cases (24.4%) exhibited a split pattern (Fig. 1).
 | Table I.Clinical and pathological features of
patients positive and negative for ALK rearrangement. |
Table I.
Clinical and pathological features of
patients positive and negative for ALK rearrangement.
| Variable | All cases | ALK-negative
cases | ALK-positive
cases | P-value |
|---|
| Total, n
(%a) | 2,045 | 1,784 (87.2) | 82 (4.0) |
|
| Age, years |
|
|
| <0.001 |
|
Range | 25–94 | 31–94 | 25–83 |
|
|
Median | 64.0 | 64.4 | 58.0 |
|
| Gender, n
(%b) |
|
|
| <0.001 |
|
Male | 1,420 (69.4) | 1,262 (70.7) | 31
(37.8) |
|
|
Female | 605
(29.6) | 507
(28.4) | 49
(59.8) |
|
|
Unknown | 20
(1.0) | 15
(0.8) | 2
(2.4) |
|
| Histology, n
(%b) |
|
|
| 0.017 |
|
Adenocarcinoma | 1,559 (76.2) | 1,352 (75.8) | 72
(87.8) |
|
|
Squamous cell carcinoma | 263
(12.9) | 239
(13.4) | 1
(1.2) |
|
| Large
cell neuroendocrine carcinoma | 21
(1.0) | 18
(1.0) | 2
(2.4) |
|
|
Adenosquamous carcinoma | 17
(0.8) | 16
(0.9) | 0
(0.0) |
|
| Not
otherwise specified | 185
(9.0) | 159
(8.9) | 7
(8.5) |
|
| Smoking history, n
(%b) |
|
|
| <0.001 |
|
Ex-smoker | 783
(38.3) | 688
(38.6) | 20
(24.4) |
|
|
Smoker | 761
(37.2) | 661
(37.0) | 23
(28.0) |
|
|
Non-smoker | 372
(18.2) | 312
(17.5) | 34
(41.5) |
|
|
Unknown | 129
(6.3) | 123
(6.9) | 5
(6.1) |
|
| Stage, n
(%b) |
|
|
| <0.001 |
| T1
(T1a+T1b) | 36
(1.8) | 34
(1.9) | 1
(1.2) |
|
| T2 | 39
(1.9) | 38
(2.1) | 1
(1.2) |
|
| T3 | 126
(6.2) | 117
(6.6) | 3
(3.7) |
|
| T4 | 883
(43.2) | 780
(43.7) | 47
(57.3) |
|
|
Unknown | 961
(47.0) | 815
(45.7) | 30
(36.6) |
|
Clinicopathological findings
The clinicopathological features of the 2,045 NSCLC
patients are summarized in Table I.
The majority were male (69.4%) and ex-smokers (38.3%) or current
smokers (37.2%). At diagnosis, the vast majority were in advanced
stage (43.2% at stage IV). The predominant histological type was
adenocarcinoma (76.2%). Significant associations between ALK
rearrangement and younger age (P<0.001; Mann-Whitney U test),
female gender (P<0.001; Pearson's χ2 test),
non-smoking history (P<0.001; likelihood ratio test), stage IV
at diagnosis (P<0.001; likelihood ratio test) and the
adenocarcinoma histological type (P=0.046; likelihood ratio test)
were found. Other ALK-positive tumor types were large cell
neuroendocrine carcinomas (n=2), squamous carcinoma (n=1) and not
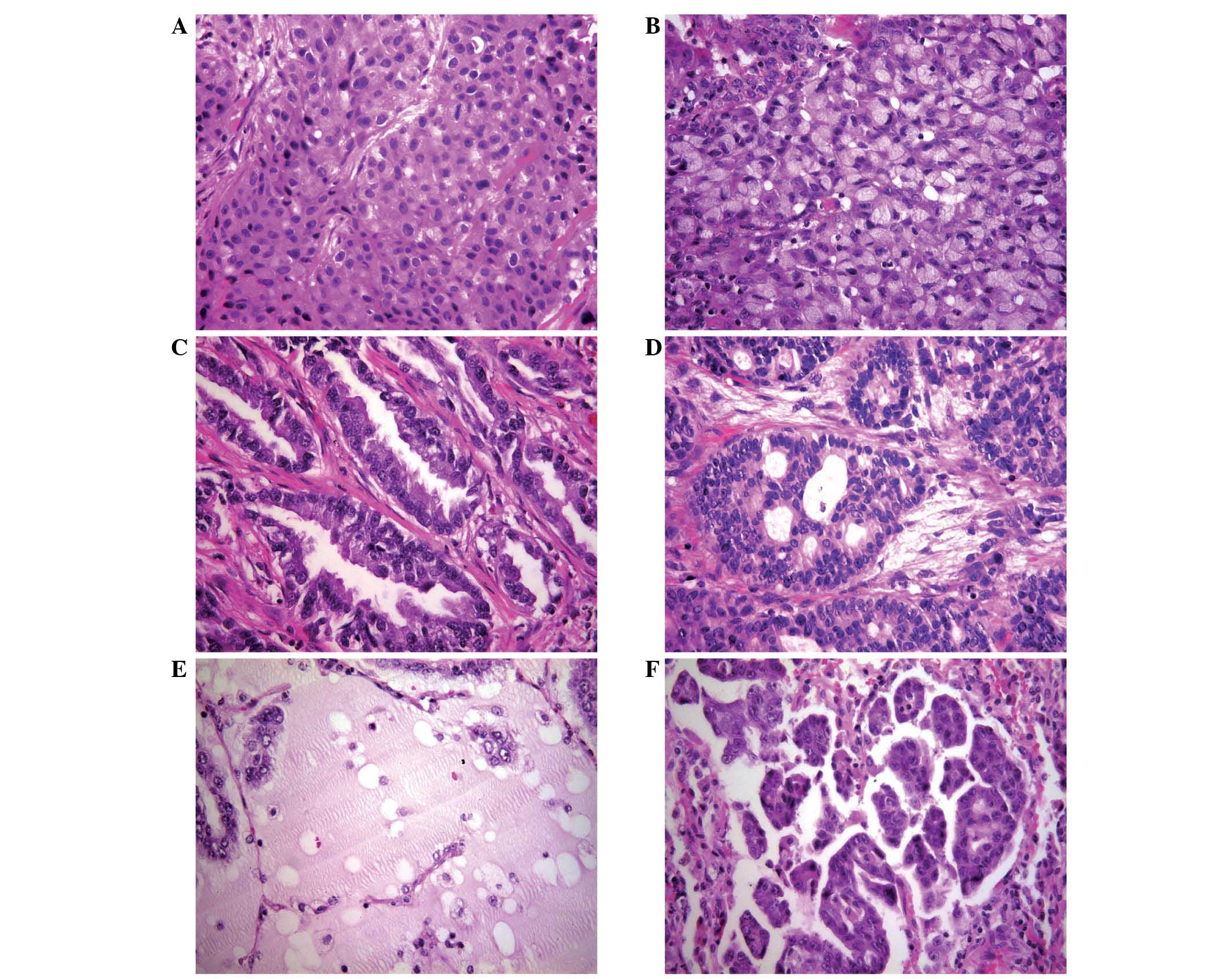
otherwise specified carcinomas (n=7). ALK-positive
adenocarcinomas (n=72) exhibited a predominantly solid pattern of
growth in 45.8% of cases, with cellular features of signet ring
cell carcinoma in 36.4% (n=12) of these (Table II and Fig.
2). No simultaneous EGFR mutations were detected in any
cases.
 | Table II.Adenocarcinoma growth patterns of
ALK gene rearrangement-positive patients (n=72). |
Table II.
Adenocarcinoma growth patterns of
ALK gene rearrangement-positive patients (n=72).
| Pattern of
growth | Cases, n |
|---|
| Solid
adenocarcinoma NOS | 19 |
| Solid with signet
ring cells | 12 |
| Acinar
adenocarcinoma NOS | 13 |
| Cribriform
adenocarcinoma | 2 |
| Colloid
adenocarcinoma | 4 |
| Mixed
adenocarcinomaa | 5 |
| Adenocarcinoma
NOS | 8 |
| Unknown | 9 |
Discussion
To the best of our knowledge, this is the largest
study on ALK rearrangements in unselected NSCLC patients in
a Spanish Caucasian population. It is also the first study in
Galicia, North-Western Spain, and is particularly interesting as
the adequacy and histology of all samples were reviewed in a single
institution by the same pathologists using the same criteria.
Although Galicia is relatively isolated, the current results
confirm the low frequency of ALK rearrangements (4%) in
unselected Caucasian NSCLC patients, which is marginally higher
than values from other areas of Spain (3%) (6), and within the range of 1.9–6.8% reported
in the literature (5,7–9).
The current study utilized the Food and Drug
Administration (FDA)-approved ALK break-apart FISH method,
with excellent results. The successful evaluation rate difference
between tissue samples and cytological samples was not significant
(92.9% vs. 84.1%); very similar results were obtained using cell
blocks and cytological smears (83.7% vs. 86.8%). Although technical
limitations have been reported in cytological specimens (6), the success rate in the present study was
in line with the literature, which reports the feasibility of
ALK FISH analysis of cytological samples as ranging from
79–97% (15). Cytological smears may
be preferable for FISH assays as they avoid formalin fixation
problems and permit the evaluation of whole nuclei, eliminating
overlapping nuclei and nuclear truncation (16). According to FDA guidelines (12), this FISH analysis is applicable on
histological samples, however, cytological smears could also be
appropriate.
The present study revealed an apparent association
of ALK rearrangement with non-smoking, female gender,
younger age, stage IV and adenocarcinoma. The significant
proportion of ALK-positive non-smokers is consistent with
previous reports (9), but 55.9% of
the current cases were previous or current smokers, which confirms
that smoking is not a reliable criterion on which to predict or
exclude ALK rearrangement. ALK positivity was
determined to be strongly associated with female gender
(P<0.001); however, controversial results have been reported
(6,8).
A marginally, non-significantly higher rate of ALK
positivity in females has been described in a recent meta-analysis
of 6,950 patients (9). The results of
the present study and that of Proietti et al (16) found a younger age to be associated
with ALK rearrangement. We also found ALK positivity
to be associated with stage IV disease; however, analysis of a
greater number of patients in other stages would be desirable to
reach reliable conclusions. Consistently with previous reports
(6,8,9), the
current results found ALK rearrangements to be largely, but
not completely, restricted to adenocarcinomas, specifically solid
or acinar variants or with signet ring cell features. ALK
positivity was also identified in one squamous cell carcinoma and
two large cell neuroendocrine carcinomas.
In conclusion, the present findings indicated that
ALK evaluation by FISH is feasible in tissue and cytological
samples. It was also found that ALK translocation is associated
with a non-smoking history, a younger age, the female gender, stage
IV and the adenocarcinoma histological type. Due to the fact that
ALK rearrangement was detected in various histological tumor types,
the ALK study should not be restricted to adenocarcinomas.
References
|
1
|
Travis WD, Brambilla E, Burke AP, Marx A
and Nicholson AG: Tumours of the lung. Who Classification Of
Tumours Of Lung, Pleura, Thymus And Heart (4th). IARC Press. (Lyon,
France). 9–151. 2015.
|
|
2
|
Kwak EL, Bang YJ, Camidge DR, Shaw AT,
Solomon B, Maki RG, Ou SH, Dezube BJ, Jänne PA, Costa DB, et al:
Anaplastic lymphoma kinase inhibition in non-small-cell lung
cancer. N Engl J Med. 363:1693–1703. 2010. View Article : Google Scholar : PubMed/NCBI
|
|
3
|
Patel JN, Ersek JL and Kim ES: Lung cancer
biomarkers, targeted therapies and clinical assays. Transl Lung
Cancer Res. 4:503–514. 2015.PubMed/NCBI
|
|
4
|
Lindeman NI, Cagle PT, Beasley MB, Chitale
DA, Dacic S, Giaccone G, Jenkins RB, Kwiatkowski DJ, Saldivar JS,
Squire J, et al: Molecular testing guideline for selection of lung
cancer patients for EGFR and ALK tyrosine kinase inhibitors:
Guideline from the College of American pathologists, international
association for the study of lung cancer, and association for
molecular pathology. J Thorac Oncol. 8:823–859. 2013. View Article : Google Scholar : PubMed/NCBI
|
|
5
|
Soda M, Choi YL, Enomoto M, Takada S,
Yamashita Y, Ishikawa S, Fujiwara S, Watanabe H, Kurashina K,
Hatanaka H, et al: Identification of the transforming EML4-ALK
fusion gene in non-small-cell lung cancer. Nature. 448:561–566.
2007. View Article : Google Scholar : PubMed/NCBI
|
|
6
|
Vidal J, Clavé S, de Muga S, González I,
Pijuan L, Gimeno J, Remón J, Reguart N, Viñolas N, Gironés R, et
al: Assessment of ALK status by FISH on 1,000 Spanish non-small
cell lung cancer patients. J Thorac Oncol. 9:1816–1820. 2014.
View Article : Google Scholar : PubMed/NCBI
|
|
7
|
Alì G, Proietti A, Pelliccioni S, Niccoli
C, Lupi C, Sensi E, Giannini R, Borrelli N, Menghi M, Chella A, et
al: ALK rearrangement in a large series of consecutive non-small
cell lung cancers: Comparison between a new immunohistochemical
approach and fluorescence in situ hybridization for the screening
of patients eligible for crizotinib treatment. Arch Pathol Lab Med.
138:1449–1458. 2014. View Article : Google Scholar : PubMed/NCBI
|
|
8
|
Cabillic F, Gros A, Dugay F, Begueret H,
Mesturoux L, Chiforeanu DC, Dufrenot L, Jauffret V, Dachary D,
Corre R, et al: Parallel FISH and immunohistochemical studies of
ALK status in 3,244 non-small-cell lung cancers reveal major
discordances. J Thorac Oncol. 9:295–306. 2014. View Article : Google Scholar : PubMed/NCBI
|
|
9
|
Zhao F, Xu M, Lei H, Zhou Z, Wang L, Li P,
Zhao J and Hu P: Clinicopathological characteristics of patients
with non-small-cell lung cancer who harbor EML4-ALK fusion gene: A
meta-analysis. PLoS One. 10:e01173332015. View Article : Google Scholar : PubMed/NCBI
|
|
10
|
Ou SH, Klempner SJ, Greenbowe JR, Azada M,
Schrock AB, Ali SM, Ross JS, Stephens PJ and Miller VA:
Identification of a novel HIP1-ALK fusion variant in non-small-cell
lung cancer (NSCLC) and discovery of ALK I1171 (I1171N/S) mutations
in two ALK-rearranged NSCLC patients with resistance to Alectinib.
J Thorac Oncol. 9:1821–1825. 2014. View Article : Google Scholar : PubMed/NCBI
|
|
11
|
Iyevleva AG, Raskin GA, Tiurin VI,
Sokolenko AP, Mitiushkina NV, Aleksakhina SN, Garifullina AR,
Strelkova TN, Merkulov VO, Ivantsov AO, et al: Novel ALK fusion
partners in lung cancer. Cancer Lett. 362:116–121. 2015. View Article : Google Scholar : PubMed/NCBI
|
|
12
|
Conde E, Suárez-Gauthier A, Benito A,
Garrido P, García-Campelo R, Biscuola M, Paz-Ares L, Hardisson D,
de Castro J, Camacho MC, et al: Accurate identification of ALK
positive lung carcinoma patients: Novel FDA-cleared automated
fluorescence in situ hybridization scanning system and
ultrasensitive immunohistochemistry. PLoS One. 9:e1072002014.
View Article : Google Scholar : PubMed/NCBI
|
|
13
|
Wang Q, Yang X, He Y, Ma Q, Lin L, Fu P
and Xiao H: Droplet digital PCR for absolute quantification of
EML4-ALK gene rearrangement in lung adenocarcinoma. J Mol Diagn.
17:515–520. 2015. View Article : Google Scholar : PubMed/NCBI
|
|
14
|
Mancikova V, Cruz R, Inglada-Pérez L,
Fernández-Rozadilla C, Landa I, Cameselle-Teijeiro J, Celeiro C,
Pastor S, Velázquez A, Marcos R, et al: Thyroid cancer GWAS
identifies 10q26.12 and 6q14.1 as novel susceptibility loci and
reveals genetic heterogeneity among populations. Int J Cancer.
137:1870–1878. 2015. View Article : Google Scholar : PubMed/NCBI
|
|
15
|
Bozzetti C, Nizzoli R, Tiseo M, Squadrilli
A, Lagrasta C, Buti S, Gasparro D, Zanoni D, Majori M, De Filippo
M, et al: ALK and ROS1 rearrangements tested by fluorescence in
situ hybridization in cytological smears from advanced non-small
cell lung cancer patients. Diagn Cytopathol. 43:941–946. 2015.
View Article : Google Scholar : PubMed/NCBI
|
|
16
|
Proietti A, Alì G, Pelliccioni S, Lupi C,
Sensi E, Boldrini L, Servadio A, Chella A, Ribechini A, Cappuzzo F,
et al: Anaplastic lymphoma kinase gene rearrangements in
cytological samples of non-small cell lung cancer: Comparison with
histological assessment. Cancer Cytopathol. 122:445–1453. 2014.
View Article : Google Scholar : PubMed/NCBI
|