Introduction
Colorectal cancer (CRC) is one of the most prevalent
and fatal types of disease worldwide (1). Although significant progress has been
made in diagnostic techniques, chemotherapy and surgery, ~70–80% of
patients with CRC will experience recurrence or metastasis,
resulting from the dormancy and spread of chemotherapy-resistant
cells and the majority of patients with metastatic CRC (mCRC) will
succumb to the disease eventually (2,3). However,
the mechanisms of chemoresistance in CRC have not been fully
clarified.
Current evidence reveals that the complexity of the
tumor microenvironment (TME) serves a critical role in altering the
biological behavior of cancer cells, including resistance to
conventional chemotherapy (4). TME is
a dynamic and complicated system that consists of cancer-associated
fibroblasts, endothelial cells and immune cells, and exhibits high
levels of cytokines, growth factors and hormones (5,6).
Previously, numerous studies indicated that a small number of cells
and components may release transforming growth factor-β1 (TGF-β),
and TGF-β results in an alteration in chemosensitivity in
certain situations in the TME (4,7–14).
TGF-β signaling pathways are considered necessary
for cancer progression (7). The main
types of TGF-β, TGF-β1, TGF-β2 and TGF-β3, regulate cancer cell
proliferation, migration, differentiation, apoptosis and
chemosensitivity in TME (15). Of the
three ligands, TGF-β1 is the most extensively studied isoform
(16). TGF-β1 gives rise to drug
resistance via the promotion of EMT, cancer stem cell-like
properties, participating in crosstalk with interleukin 6,
regulating DNA mismatch repair system and inducing cell cycle
arrest and autophagy in several cancers (8–14). By
contrast, blocking the TGF-β1 pathway may enhance the efficacy of
chemotherapy under certain circumstances (13). These data have ensured that TGF-β1 is
one of the most important types of components that affect
chemoresistance in TME.
In previous decades, due to the use of standard
chemotherapy containing oxaliplatin (LOH), the response rates,
progression-free and overall survival have been significantly
improved in patients with CRC (17,18). At
present, combinations of chemotherapy containing LOH continue to
exhibit powerful efficacy in the treatment of CRC (19). However, the alteration in sensitivity
of CRC cells to LOH under the administration of TGF-β1 has not been
previously demonstrated.
Thus, the aims of the present study were to assess
whether TGF-β1 contributes to LOH chemosensitivity in cultured CRC
cell lines, and to explore the mechanisms by which TGF-β1 is
responsible for these effects.
Materials and methods
Cell culture and reagents
The human CRC HCT-116, CL187 and SW620 cell lines
were all purchased from the ATCC (American Type Culture
Collection). HCT-116 cells were cultured in McCoy's 5A medium
(Sigma-Aldrich; Merck KGaA, Darmstadt, Germany). CL187 cells were
cultured in high glucose Dulbecco's Modified Eagle Medium (Gibco;
Thermo Fisher Scientific, Inc., Waltham, MA, USA) and SW620 cells
were cultured in Leibovitz-15 (Gibco; Thermo Fisher Scientific,
Inc.). The cell lines were cultured with 10% heat-inactivated fetal
bovine serum (Gibco; Thermo Fisher Scientific, Inc.), 50 U/ml
penicillin and 50 µg/ml streptomycin at 37°C supplied with 5%
CO2. Human recombinant TGF-β1 (rh TGF-β1) was purchased
from PeproTech, Inc. (Rocky Hill, NJ, USA); LOH was obtained from
HengRui Therapeutics, Inc., (Princeton, NJ, USA). LOH was dissolved
with 5% glucose at 10 mM prior to dilution to the indicated
concentrations with culture medium prior to use. RhTGF-β1 was
diluted according to the manufacturer's protocol.
Cell viability and proliferation
assays
Cell viability was measured by MTT assay. CRC cells
were plated at a density of 3×103 per well in 96-well
plates. RhTGF-β1 was added at the final concentrations of 0, 3 or 5
ng/ml, or 0–20 ng/ml after 24 h. At 72 h subsequent to rhTGF-β1
treatment, CRC cells were then exposed to increasing doses of LOH
for an additional 72 h, to detect LOH resistance. Then, 4 or 7 days
subsequent to plating, 0.5 mg/ml MTT solution was added to the
medium for 4 h incubation at 37°C, and then 100 µl dimethyl
sulfoxide was added to each well. The absorbance at 570 nm was
determined with a scanning multi-well spectrophotometer (Tecan US,
Inc., Morrisville, NC, USA). Each assay was performed in
triplicate.
Western blot analysis
HCT-116 cells were treated with rhTGF-β1 at a
gradient of concentrations [1, 3, 5, 10 and 20 ng/ml],
simultaneously, a mock and TGF-β1 antibody (Santa Cruz
Biotechnology, Inc., Dallas, TX, USA) served as controls. Western
blot analysis was performed as described previously (20). Cells were harvested at 3 days
subsequent to treatment and lysed in a radioimmunoprecipitation
assay (RIPA) lysis buffer (Beyotime Institute of Biotechnology,
Shanghai, China) containing phenylmethylsulfonyl fluoride and
leupeptin for 30 min at room temperature (RT). The soluble protein
concentration was determined by bicinchoninic acid (BCA) protein
assay (Boster, Wuhan, China). Protein (80 µg) was electrophoresed
in SDS-PAGE and transferred to polyvinylidene fluoride membranes
(EMD Millipore, Billerica, MA, USA). Primary monoclonal antibody to
E-cadherin (catalog no. 20874-1-AP; dilution, 1:1,000; ProteinTech
Group, Inc., Chicago, IL, USA), N-cadherin (catalog no. 610920;
dilution, 1:1,000; BD Transduction Laboratories, New Jersey, USA),
Snail (catalog no. #3895; dilution, 1:1,000; Cell Signaling
Technology, Massachusetts, USA) and GAPDH (catalog no. G8795;
dilution, 1:10,000; Sigma-Aldrich; Merck KGaA) were incubated with
polyvinylidene fluoride membranes overnight at 4°C. Binding of the
primary antibody was detected by horse anti-mouse immunoglobulin
(catalog no. 7076; dilution, 1:2,000; Cell Signaling Technology,
Inc., Danvers, MA, USA) or goat anti-rabbit immunoglobulin (catalog
no. 7077; dilution, 1:2,000; Cell Signaling Technology, Inc.)
conjugated to horseradish peroxidase, which was incubated for 1 h
at room temperature. Electrochemiluminescent reagents were used to
test the signals, according to the manufacturer's instructions
(TransGen Biotech, Inc. Beijing, China). ImageJ software (version
Java 1.6.0_20; National Institutes of Health, Bethesda, MD, USA)
was used to analyze the gray value of each band.
Cell immunofluorescence staining
HCT-116 cells were seeded on 8-well chamber slides
(BD-falcon; BD Biosciences, Franklin Lakes, NJ, USA) at
~1×104 per well. A Treatment of rhTGF-β1 at the
increasing concentrations of 0, 1, 3, 5, 10 and 20 ng/ml were given
for 72 h after the cells were adherent. TGF-β1 antibody-treated
cells were used as a control. The cells were washed with Dulbecco's
phosphate-buffered saline (D-PBS) 3 times and then fixed in 4%
paraformaldehyde for 15 min at RT. Then, 1% Triton 100 in D-PBS
buffer was allowed to permeate the cells at RT for 30 min.
Subsequent to washing 3 times, the cells were blocked with 5%
normal goat serum (Vector Laboratories, Inc., Burlingame, CA, USA)
in 1% bovine serum albumin (BSA)/D-PBS buffer at RT for 1 h, and
then incubation with the primary antibodies rabbit anti-E-cadherin
(catalog no. 20874-1-AP; dilution, 1:1,000, ProteinTech Group,
Inc.) and mouse anti-N-cadherin (catalog no. 610920; dilution,
1:1,000, BD Transduction Laboratories) overnight at 4°C. Subsequent
to the 3 washes, the cells were incubated with the Alexa Fluor 594
(catalog no. A-11012; Invitrogen; Thermo Fisher Scientific, Inc.)
and FITC-labeled secondary antibody (catalog no. bs-0926G-FITC;
Bioss, Beijing, China) for 1 h at RT, respectively. Finally, nuclei
were stained with Prolong Gold Antifade reagent with DAPI (catalog
no. P-36931; Invitrogen; Thermo Fisher Scientific, Inc.). Images of
the stained cells were captured with a fluorescent microscope
(Olympus Corporation, Tokyo, Japan) at equal exposure time.
Flow cytometric analyses for
apoptosis
A total of 5×104 cells per well were
plated in 6-well plates. Then, 24 h after plating, the cells were
treated for 3 days with rhTGF-β1 at doses of 0, 3 and 5 ng/ml, in
addition to LOH treatment at increasing concentrations from 0 to 30
µM for 3 days. Apoptotic cell death was detected using an Annexin
V-fluorescein isothiocyanate/propidium iodide (FITC/PI) double
staining kit (Dojindo Molecular Technologies, Kumamoto, Japan)
according to the manufacturer's protocol. The cells were washed
twice with PBS and re-suspended cells in 1X Annexin-V binding
buffer at a concentration of 1×106 cells/ml. Annexin
V-FITC and PI were added separately to 5 µl cell suspensions and
incubated for 30 min in the dark. The samples were analyzed by
FACScan flow cytometer (BD Biosciences, San Jose, CA, USA). Data
were analyzed by using Flow Jo software (version 7.6,
Treestar).
Alkaline comet assay
The preparation samples for comet assays (Trevigen,
Gaithersburg, MD, USA) were the same as the aforementioned Annexin
V-FITC/PI double staining. Cells were combined with molten LM
Agarose and 50 µl agarose/cells was immediately spread over a
CometSlide™. The slides were cooled at 4°C in the dark for 10 min
and then the slides were immersed in Lysis Solution overnight at
4°C. Subsequent to lysis, the cells were subjected to unwinding,
electrophoresis and drying and staining with SYBR-Green I (Dingguo
Biotechnology Co., Beijing, China). Subsequently, the cells were
observed using fluorescent microscopy (Olympus Corporation). One
hundred cells were analyzed for each group using Comet Score
software (version 1.5, TriTek Solutions, Inc. Rancho Santa
Margarita, CA, USA). The tail moment and the amount of DNA in the
tail were manually scored by an examiner blinded to the treatment
group. Experiments were repeated in triplicate.
Statistical analysis
Data were analyzed using JMP version 11.0 software
(SAS Institute Co., Ltd., Shanghai, China). Data were described and
statistically tested if they were normally distributed. Data are
shown as the mean ± standard error of the mean or standard
deviation from at least three independent experiments. The
chemoresistance induced by TGF-β1 were compared and analyzed by
one-way analysis of variance. Other data were performed with
un-paired Student's t-test and nonparametric Wilcoxon test to
evaluate differences among the experimental groups. P<0.05 was
considered to indicate a statistically significant difference.
Results
TGF-β1 promotes chemoresistance to LOH
in CRC cells
To examine whether CRC cells exhibit chemoresistance
to LOH subsequent to treatment with TGF-β1, the effect of LOH on
TGF-β1 treatment in all three cell lines was examined using an MTT
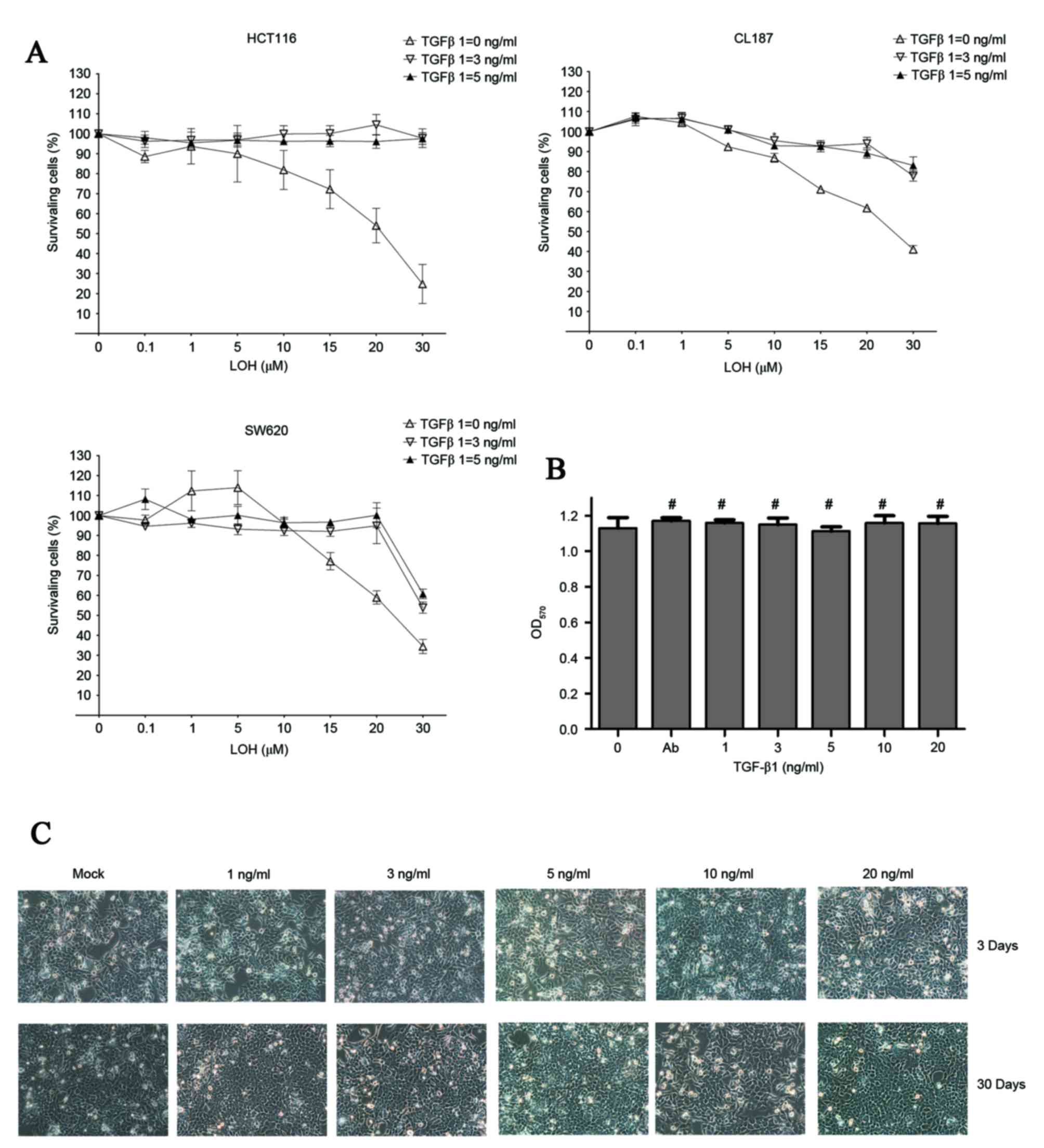
assay. As is evident in Fig. 1A,
along with the increasing concentration of LOH, CRC cells showed
different levels of accumulative effects of death. By contrast, CRC
cells that were pretreated with TGF-β1 demonstrated significant
levels of resistance to LOH even at the highest dose of 50 µM LOH.
However, no differences in viability were observed between groups
treated with 5 ng/ml TGF-1 plus a serial concentration of LOH and 3
ng/ml TGF-1 plus a serial concentration of LOH. These results
strongly support the initial hypothesis. These data indicate that
the change in chemosensitivity to LOH of the HCT-116 cell line was
the most significant among the three CRC cell lines. For the
purposes of explaining the reasons for TGF-β1-treated CRC cells
exhibiting chemoresistance to LOH, the colon cancer cell line
HCT-116 was selected as the subject for the subsequent
experiments.
No obvious morphological or changes in
viability in TGF-β1-treated HCT-116 cells
Morphological observations and viability tests of
TGF-β1-treated HCT-116 cells were performed. Following treatment
with TGF-β1 for three days, cells with EMT phenotype (characterized
by elongated morphology) were not observed, even after the 30 days
of TGF-β1 treatment (Fig. 1B).
Additionally, cell viability was tested using MTT assays. Similar
results were revealed in that there were no significant differences
among each group with the TGF-β1 concentration from 0 to 20 ng/ml
observed (Fig. 1C). In conclusion,
the data in Fig. 1B and C indicate
that TGF-β1 does not significantly affect the morphological changes
and changes to the viability of HCT-116 cells. Therefore,
TGF-β1-induced chemoresistance is not associated with cell
viability and cell proliferation.
TGF-β1 induces EMT in HCT-116
cells
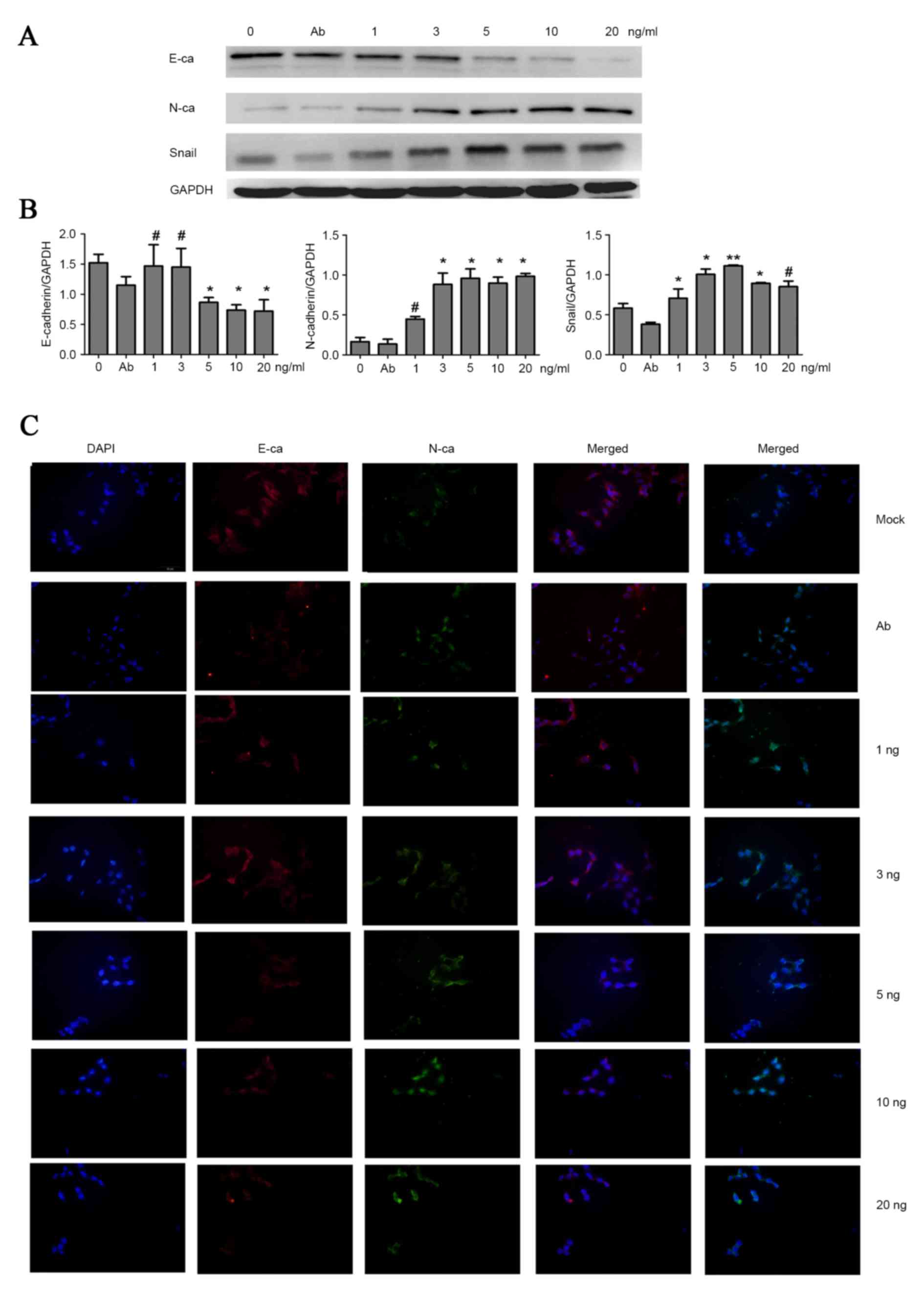
To detect the EMT phenotype, cell immunofluorescent
staining and western blot analyses were performed to examine the
expression of indicators associated with EMT. It was demonstrated
that with the increasing concentration of TGF-β1, HCT-116
upregulated the mesenchymal marker of neural cadherin (N-cadherin),
and downregulated the epithelial marker epithelial cadherin
(E-cadherin), despite the lack of typical morphology of EMT
observed under the microscope. Concurrently, the level of
transcription factor zinc finger protein SNAI1 (Snail), associated
with EMT, also increased (Fig. 2A and
B). Additionally, immunofluorescent staining was performed to
evaluate EMT. Consistent with the result of western blot analyses,
Fig. 2C shows that treating cells
with 3 and 5 ng/ml TGF-β1 was a feasible method to inducing EMT.
However, the EMT assays suggested that no significantly higher
levels of N-cadherin and Snail, and lower levels of E-cadherin
expression were observed among cells treated by 3–20 ng/ml TGF-β1.
These data demonstrate that TGF-β1-induced EMT remains present in
colon cancer HCT-116 cells. Therefore, the attenuation of the
chemotherapeutic effects of LOH on HCT-116 cells may be due to
TGF-β1-induced EMT.
TGF-β1 attenuates LOH-induced DNA
damage and apoptotic death in HCT-116 cells
Platinum compounds exert their anticancer effects
usually through DNA damage. LOH may induce single- and
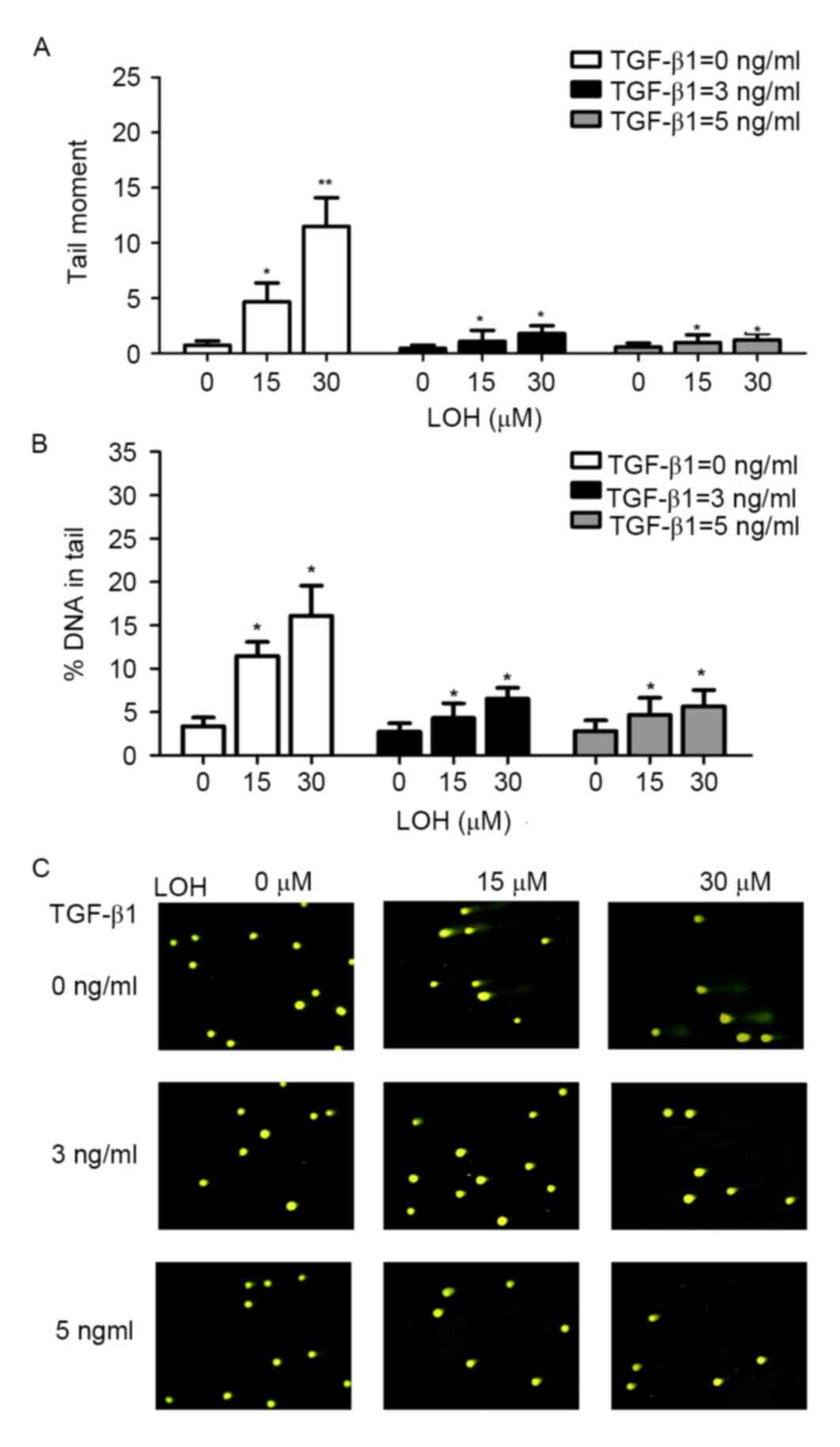
double-stranded DNA breaks. Therefore, alkaline comet assays were
performed to explore the levels of DNA damage in TGF-β1-induced
chemoresistance to LOH. The cells were treated with TGF-β1 and LOH
as aforementioned. Representative images of comet tails for each
group are shown in Fig. 3C. The
percentage of total DNA of cells found in the tail which reflects
migrating DNA fragments from the nucleoid is shown in Fig. 3B. In addition, tail moment is an
additional method used to measure the level of DNA damage, which
combine the amount of DNA in the tail with the distance of
migration (Fig. 3A). These collective
data indicate that TGF-β1 induces HCT-116 cells to resist LOH
through the attenuation of DNA damage. As DNA damage usually leads
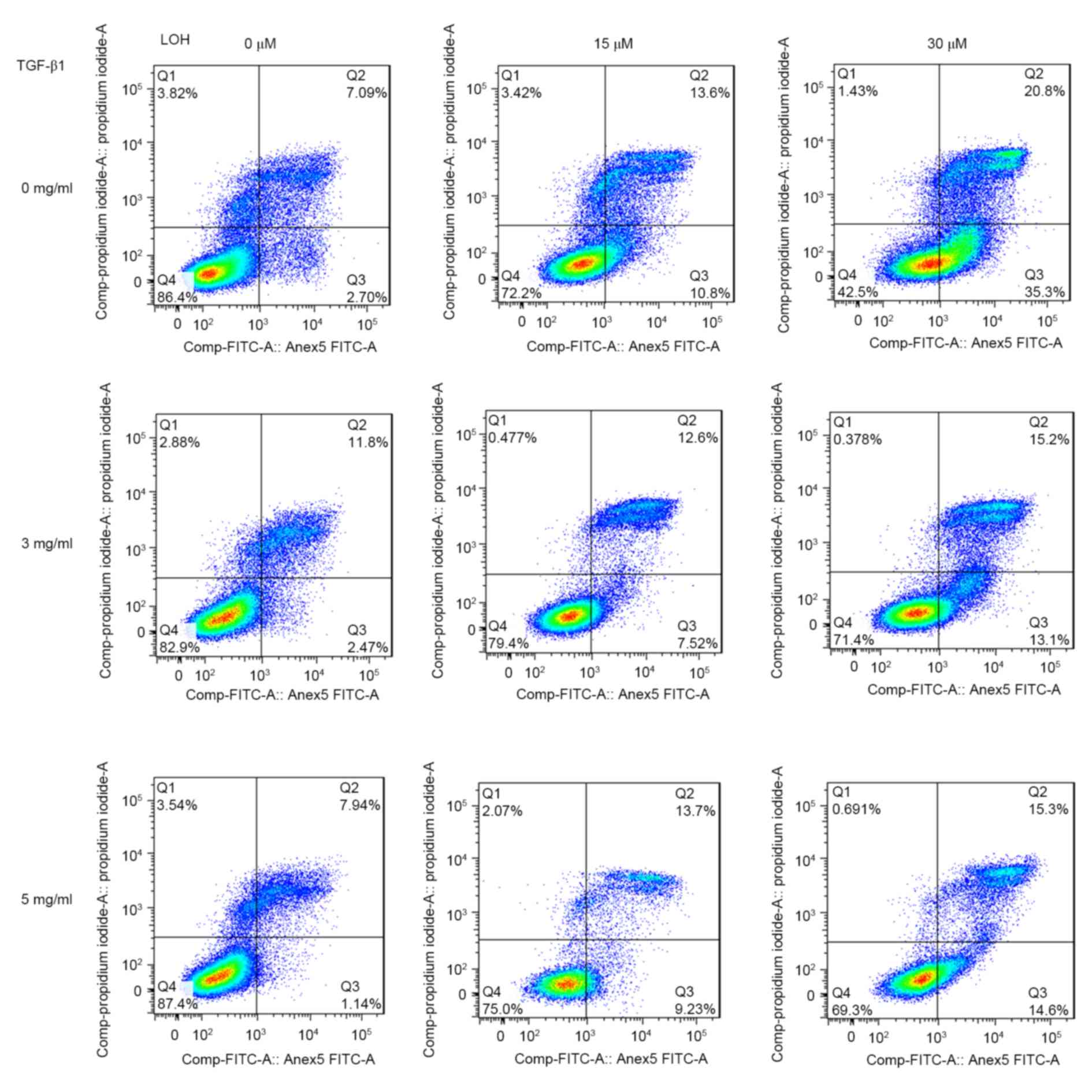
to the induction of apoptosis, the effects of TGF-β1 on apoptosis
induced by LOH in HCT-116 cells were additionally characterized.
Annexin/PI double staining was used to detect cell apoptosis. As is
evident in Fig. 4, there was a marked
trend that demonstrated that 3 and 5 ng/ml TGF-β1 exerted more
powerful anti-apoptotic effects compared with untreated cells.
Taken together, the data from the present study revealed that the
resistance to LOH subsequent to TGF-β1 treatment on HCT-116 cells
is due to attenuated DNA damage and ensuing anti-apoptotic effects
caused by EMT.
Discussion
Oxaliplatin is widely used as a first-line
chemotherapeutic agent globally in patients with mCRC (21). However, the mechanisms underlying LOH
resistance are modulated by multiple factors, and have not been
fully understood until now.
Extensive data suggest that the TME serves a crucial
role in generating and promoting chemoresistance (4,8,9,22,23). TGF-β is a universal cytokine in the
TME, which may be produced by cancer-associated fibroblasts,
cancer-associated macrophages, mesenchymal stem cells, platelets
and even cancer cells. TGF-β may not only maintain homeostasis in
healthy cells, but also regulate the proliferation, migration,
differentiation, invasion, metastasis and drug resistance of cancer
cells via the Smad and/or non-Smad pathways (7,15,24). A number of studies suggested that
TGF-β resulted in chemoresistance through several mechanisms. Among
the chemoresistant effects caused by TGF-β, EMT was identified most
frequently (8–14,25). EMT
is considered a common process induced by TGF-β1, in which cancer
cells lose epithelial features and acquire a mesenchymal phenotype
with enhanced malignant behaviors such as invasion and metastasis,
and chemoresistance in numerous cancer cell types (26–30).
There are no studies investigating the
chemoresistant effect of TGF-β1-induced EMTs on CRC cells in the
published literature. In the present study, the CRC cell lines used
exhibited chemoresistance to LOH subsequent to TGF-β1 treatment.
EMT, attenuated DNA damage and anti-apoptotic effects were
demonstrated in the detailed experiments using TGF-β1-treated CRC
cells, which may account for the TGF-β1-induced LOH resistance in
CRC. Additionally, it was revealed that the LOH cytotoxicity assay
and the DNA damage and apoptotic assays agreed with the
phenotypical changes of EMT and cells demonstrated significant
changes with the treatment of 3 and 5 ng/ml TGF-β1 compared with
their untreated counterparts in the CRC cell lines. These data
reveal that 3 and 5 ng/ml TGF-β1 are appropriate concentrations for
producing chemoresistance effects in the CRC cell line. In the
present study, CRC cells treated with >5 ng/ml TGF-β1 did not
exhibit significant changes in cell viabilities and EMT phenotypes,
and these results suggested that the subsequent experiments should
be performed with concentrations of TGF-β1 treatment <5 ng/ml.
The final data indicated that CRC cells demonstrated no significant
differences between the groups treated by 3 and 5 ng/ml TGF-β1 in
the MTT, EMT, comet and apoptotic assays.
The promotion of resistance to platinum-based
chemotherapy by EMT has been demonstrated previously (25). However, LOH is a third-generation
platinum compound that varies its mechanisms of resistance from its
former associated platinum compounds. A number of previous studies
revealed that numerous genes, proteins and transcription factors
are involved in sensitivity of oxaliplatin treatment (19,31–36).
Nevertheless, to the best of our knowledge, a small number of
studies have addressed the association between the aforementioned
LOH chemoresistance mechanisms and the biological functions of the
TGF-β1 signaling pathways except for phosphoinositide-3-kinase
(PI3K)/protein kinase B signaling. Additionally, TGF-β in the TME
is a potent, multi-functional cytokine that exerts either
tumor-suppressing or tumor-promoting activities, which depends on
the specific TME, cancer stage, cancer type and chemotherapeutic
agents present (30,37). These data indicate that the mechanisms
underlying TGF-β1-induced chemoresistance to LOH remain
incompletely characterized. Additional studies should focus on the
TGF-β1 pathway associated with LOH resistance. In addition, except
for EMT assays performed in the present study, other methods should
be studied due to the complexity of LOH resistance caused by
TGF-β1, which may include changing of CSC properties, crosstalk
with other cytokines, regulating DNA mismatch repair system,
modulating cell cycle arrest and autophagy.
In conclusion, the present study demonstrated that 3
and 5 ng/ml TGF-β1 induced EMT efficiently, which resulted in the
attenuation of DNA damage and anti-apoptotic effects in CRC cells.
These changes account for LOH resistance. Additional studies should
focus on blocking the TGF-β pathway for re-sensitizing patients
with CRC to LOH.
Acknowledgements
The authors would like to thank Miss Miao Guo and Dr
Yanan Xu (Immunology and Allergy laboratory, The First Affiliated
Hospital of Jinzhou Medical University) for excellent technical
assistance with the flow cytometry-based analysis. The present
study was supported by General Program of the National Natural
Science Foundation of China (grant no., 81472460), The President
Foundation of Jinzhou Medical University and The Leading Project on
Colorectal Cancer of Jinzhou Medical University.
References
|
1
|
Jemal A, Bray F, Center MM, Ferlay J, Ward
E and Forman D: Global cancer statistics. CA Cancer J Clin.
61:69–90. 2011. View Article : Google Scholar : PubMed/NCBI
|
|
2
|
Zakaria S, Donohue JH, Que FG, Farnell MB,
Schleck CD, Ilstrup DM and Nagorney DM: Hepatic resection for
colorectal metastases: Value for risk scoring systems? Ann Surg.
246:183–191. 2007. View Article : Google Scholar : PubMed/NCBI
|
|
3
|
Nautiyal J, Kanwar SS, Yu Y and Majumdar
AP: Combination of dasatinib and curcumin eliminates
chemo-resistant colon cancer cells. J Mol Signal. 6:72011.
View Article : Google Scholar : PubMed/NCBI
|
|
4
|
Quail DF and Joyce JA: Microenvironmental
regulation of tumor progression and metastasis. Nat Med.
19:1423–1437. 2013. View
Article : Google Scholar : PubMed/NCBI
|
|
5
|
Deep G and Agarwal R: Targeting tumor
microenvironment with silibinin: Promise and potential for a
translational cancer chemopreventive strategy. Curr Cancer Drug
Targets. 13:486–499. 2013. View Article : Google Scholar : PubMed/NCBI
|
|
6
|
Junttila MR and de Sauvage FJ: Influence
of tumour micro-environment heterogeneity on therapeutic response.
Nature. 501:346–354. 2013. View Article : Google Scholar : PubMed/NCBI
|
|
7
|
Pickup M, Novitskiy S and Moses HL: The
roles of TGFβ in the tumour microenvironment. Nat Rev Cancer.
13:788–799. 2013. View
Article : Google Scholar : PubMed/NCBI
|
|
8
|
Asiedu MK, Ingle JN, Behrens MD, Radisky
DC and Knutson KL: TGFbeta/TNF(alpha)-mediated
epithelial-mesenchymal transition generates breast cancer stem
cells with a claudin-low phenotype. Cancer Res. 71:4707–4719. 2011.
View Article : Google Scholar : PubMed/NCBI
|
|
9
|
Fan QM, Jing YY, Yu GF, Kou XR, Ye F, Gao
L, Li R, Zhao QD, Yang Y, Lu ZH and Wei LX: Tumor-associated
macrophages promote cancer stem cell-like properties via
transforming growth factor-beta1-induced epithelial-mesenchymal
transition in hepatocellular carcinoma. Cancer Lett. 352:160–168.
2014. View Article : Google Scholar : PubMed/NCBI
|
|
10
|
Mallini P, Lennard T, Kirby J and Meeson
A: Epithelial-to-mesenchymal transition: What is the impact on
breast cancer stem cells and drug resistance. Cancer Treat Rev.
40:341–348. 2014. View Article : Google Scholar : PubMed/NCBI
|
|
11
|
Yamada D, Kobayashi S, Wada H, Kawamoto K,
Marubashi S, Eguchi H, Ishii H, Nagano H, Doki Y and Mori M: Role
of crosstalk between interleukin-6 and transforming growth
factor-beta 1 in epithelial-mesenchymal transition and
chemoresistance in biliary tract cancer. Eur J Cancer.
49:1725–1740. 2013. View Article : Google Scholar : PubMed/NCBI
|
|
12
|
Yu Y, Wang Y, Ren X, Tsuyada A, Li A, Liu
LJ and Wang SE: Context-dependent bidirectional regulation of the
MutS homolog 2 by transforming growth factor β contributes to
chemoresistance in breast cancer cells. Mol Cancer Res.
8:1633–1642. 2010. View Article : Google Scholar : PubMed/NCBI
|
|
13
|
Tabe Y, Shi YX, Zeng Z, Jin L, Shikami M,
Hatanaka Y, Miida T, Hsu FJ, Andreeff M and Konopleva M:
TGF-β-neutralizing antibody 1D11 enhances cytarabine-induced
apoptosis in AML cells in the bone marrow microenvironment. PLoS
One. 8:e627852013. View Article : Google Scholar : PubMed/NCBI
|
|
14
|
Zhang H, Wu H, Zheng J, Yu P, Xu L, Jiang
P, Gao J, Wang H and Zhang Y: Transforming growth factor β1 signal
is crucial for dedifferentiation of cancer cells to cancer stem
cells in osteosarcoma. Stem Cells. 31:433–446. 2013. View Article : Google Scholar : PubMed/NCBI
|
|
15
|
Ma S, Qu W, Mao L, Zhu Z, Jia L, Zhao L
and Zheng X: Antitumor effects of oncolytic adenovirus armed with
Drosophila melanogaster deoxyribonucleoside kinase in colorectal
cancer. Oncol Rep. 27:1443–1450. 2012.PubMed/NCBI
|
|
16
|
Massague J: How cells read TGF-beta
signals. Nat Rev Mol Cell Biol. 1:169–178. 2000. View Article : Google Scholar : PubMed/NCBI
|
|
17
|
Lievre A, Samalin E, Mitry E, Assenat E,
Boyer-Gestin C, Lepère C, Bachet JB, Portales F, Vaillant JN, Ychou
M and Rougier P: Bevacizumab plus FOLFIRI or FOLFOX in
chemotherapy-refractory patients with metastatic colorectal cancer:
A retrospective study. BMC Cancer. 9:3472009. View Article : Google Scholar : PubMed/NCBI
|
|
18
|
de Gramont A, Figer A, Seymour M, Homerin
M, Hmissi A, Cassidy J, Boni C, Cortes-Funes H, Cervantes A, Freyer
G, et al: Leucovorin and fluorouracil with or without oxaliplatin
as first-line treatment in advanced colorectal cancer. J Clin
Oncol. 18:2938–2947. 2000. View Article : Google Scholar : PubMed/NCBI
|
|
19
|
Seetharam R, Sood A and Goel S:
Oxaliplatin: Pre-clinical perspectives on the mechanisms of action,
response and resistance. Ecancermedicalscience.
3:1532009.PubMed/NCBI
|
|
20
|
Zhu Z, Mao L, Zhao L, Sun Z, Wang Z, Xu H
and Zheng X: Synergistic therapeutic effect in gastric cancer cells
produced by oncolytic adenovirus encoding Drosophila melanogaster
deoxyribonucleoside kinase. Cancer Biol Ther. 11:874–882. 2011.
View Article : Google Scholar : PubMed/NCBI
|
|
21
|
Cassidy J, Clarke S, Díaz-Rubio E,
Scheithauer W, Figer A, Wong R, Koski S, Rittweger K, Gilberg F and
Saltz L: XELOX vs FOLFOX-4 as first-line therapy for metastatic
colorectal cancer: NO16966 updated results. Br J Cancer. 105:58–64.
2011. View Article : Google Scholar : PubMed/NCBI
|
|
22
|
Rebucci M and Michiels C: Molecular
aspects of cancer cell resistance to chemotherapy. Biochem
Pharmacol. 85:1219–1226. 2013. View Article : Google Scholar : PubMed/NCBI
|
|
23
|
Iseri OD, Kars MD, Arpaci F, Atalay C, Pak
I and Gündüz U: Drug resistant MCF-7 cells exhibit
epithelial-mesenchymal transition gene expression pattern. Biomed
Pharmacother. 65:40–45. 2011. View Article : Google Scholar : PubMed/NCBI
|
|
24
|
Flavell RA, Sanjabi S, Wrzesinski SH and
Licona-Limon P: The polarization of immune cells in the tumour
environment by TGFbeta. Nat Rev Immunol. 10:554–567. 2010.
View Article : Google Scholar : PubMed/NCBI
|
|
25
|
Marchini S, Fruscio R, Clivio L, Beltrame
L, Porcu L, Nerini I Fuso, Cavalieri D, Chiorino G, Cattoretti G,
Mangioni C, et al: Resistance to platinum-based chemotherapy is
associated with epithelial to mesenchymal transition in epithelial
ovarian cancer. Eur J Cancer. 49:520–530. 2013. View Article : Google Scholar : PubMed/NCBI
|
|
26
|
Thiery JP: Epithelial-mesenchymal
transitions in tumour progression. Nat Rev Cancer. 2:442–454. 2002.
View Article : Google Scholar : PubMed/NCBI
|
|
27
|
Thiery JP, Acloque H, Huang RY and Nieto
MA: Epithelial-mesenchymal transitions in development and disease.
Cell. 139:871–890. 2009. View Article : Google Scholar : PubMed/NCBI
|
|
28
|
Bierie B and Moses HL: TGF-beta and
cancer. Cytokine Growth Factor Rev. 17:29–40. 2006. View Article : Google Scholar : PubMed/NCBI
|
|
29
|
Akhurst RJ: TGF beta signaling in health
and disease. Nat Genet. 36:790–792. 2004. View Article : Google Scholar : PubMed/NCBI
|
|
30
|
Wendt MK, Tian M and Schiemann WP:
Deconstructing the mechanisms and consequences of TGF-β-induced EMT
during cancer progression. Cell Tissue Res. 347:85–101. 2012.
View Article : Google Scholar : PubMed/NCBI
|
|
31
|
Aaltonen LA, Peltomäki P, Leach FS,
Sistonen P, Pylkkänen L, Mecklin JP, Järvinen H, Powell SM, Jen J,
Hamilton SR, et al: Clues to the pathogenesis of familial
colorectal cancer. Science. 260:812–816. 1993. View Article : Google Scholar : PubMed/NCBI
|
|
32
|
Gnoni A, Russo A, Silvestris N, Maiello E,
Vacca A, Marech I, Numico G, Paradiso A, Lorusso V and Azzariti A:
Pharmacokinetic and metabolism determinants of fluoropyrimidines
and oxaliplatin activity in treatment of colorectal patients. Curr
Drug Metab. 12:918–931. 2011. View Article : Google Scholar : PubMed/NCBI
|
|
33
|
Kashiwagi E, Izumi H, Yasuniwa Y, Baba R,
Doi Y, Kidani A, Arao T, Nishio K, Naito S and Kohno K: Enhanced
expression of nuclear factor I/B in oxaliplatin-resistant human
cancer cell lines. Cancer Sci. 102:382–386. 2011. View Article : Google Scholar : PubMed/NCBI
|
|
34
|
Kieran D, Woods I, Villunger A, Strasser A
and Prehn JH: Deletion of the BH3-only protein puma protects
motoneurons from ER stress-induced apoptosis and delays motoneuron
loss in ALS mice. Proc Natl Acad Sci USA. 104:pp. 20606–20611.
2007; View Article : Google Scholar : PubMed/NCBI
|
|
35
|
Moser C, Lang SA, Kainz S, Gaumann A,
Fichtner-Feigl S, Koehl GE, Schlitt HJ, Geissler EK and Stoeltzing
O: Blocking heat shock protein-90 inhibits the invasive properties
and hepatic growth of human colon cancer cells and improves the
efficacy of oxaliplatin in p53-deficient colon cancer tumors in
vivo. Mol Cancer Ther. 6:2868–2878. 2007. View Article : Google Scholar : PubMed/NCBI
|
|
36
|
Xiu P, Dong X, Dong X, Xu Z, Zhu H, Liu F,
Wei Z, Zhai B, Kanwar JR, Jiang H, et al: Secretory clusterin
contributes to oxaliplatin resistance by activating Akt pathway in
hepatocellular carcinoma. Cancer Sci. 104:375–382. 2013. View Article : Google Scholar : PubMed/NCBI
|
|
37
|
Gatza CE, Holtzhausen A, Kirkbride KC,
Morton A, Gatza ML, Datto MB and Blobe GC: Type III TGF-β receptor
enhances colon cancer cell migration and anchorage-independent
growth. Neoplasia. 13:758–770. 2011. View Article : Google Scholar : PubMed/NCBI
|