Introduction
Hepatocellular carcinoma (HCC) is one of the most
commonly diagnosed types of cancer worldwide (1). While there are specific differences in
its etiology associated with different regional effects for
example, in western countries, alcoholic hepatitis is the main
reason for HCC. However, in China, a large number of HCC cases
arise as a consequence of Hepatitis B virus (HBV) infection
(2). HCC is a complicated disease and
represents a significant cause of morbidity and mortality in China
(2,3).
Previous advances in treatment methods for HCC have
improved the clinical outcomes of patients with HCC. Liver
transplantation, curative surgical resection, percutaneous ethanol
injection and radiofrequency ablation are considered curative
treatments, while transarterial treatments, including transarterial
chemoembolization (TACE) in particular, are currently recognized as
treatments that may prolong survival time (3).
TACE has been suggested to treat Barcelona Clinic
Liver Cancer (BCLC) B- or C-stage HCC through 2 potential methods
(4). Firstly, arterial embolization
may stop blood supply to the HCC tissue and inhibit tumor growth
until neovascularization occurs (5).
Secondly, the controlled release of chemotherapeutic agents allows
the delivery of a stable concentration of drug to the lesions, and
decreases the severity of systemic side effects (6). However, a previous study demonstrated
that TACE may trigger cancer angiogenesis by upregulating the
expression of certain cytokines and growth factors, including basic
fibroblast growth factor (bFGF), vascular endothelial growth factor
(VEGF) and hypoxia-inducible factor 1α (7) Furthermore, additional studies have
demonstrated that the expression levels of these cytokines and
growth factors were markedly decreased in patients treated with
surgery alone compared with those that underwent pre-surgical TACE
(8).
Sorafenib is an orally-administered small molecule
drug (9) that inhibits multiple
protein kinases, including VEGF receptors 2 and 3 and
Platelet-derived growth factor (PDGF) receptor B (9), which are involved in tumor angiogenesis,
and the family of Raf kinases, which facilitates the proliferation
of cancer cells (10). Sorafenib is
globally accepted and widely used as the first-line treatment for
advanced-stage HCC (11). However,
the effects of treatment with sorafenib alone on overall survival
(OS) have not been satisfactory in patients with advanced HCC
(12).
Novel therapies are urgently required in order to
improve the OS of patients with advanced HCC. At present, sorafenib
is the only approved systemic drug for patients with advanced-stage
disease (BCLC C-stage) (13). TACE is
suggested as the primary treatment method for BCLC B-stage HCC in
the BCLC guidelines (14). Physicians
have demonstrated that TACE was also effective for patients with
BCLC C-stage HCC with vascular invasion or metastases (14,15).
Furthermore, previous data have indicated that combined therapy,
including sorafenib combined with TACE, may achieve significant
improvements in the treatment of advanced HCC compared with single
TACE treatment (16).
At present, clinical studies generally use the
modified Response Evaluation Criteria In Solid Tumors (mRECIST) to
evaluate the effect of sorafenib and TACE treatment on HCC
(17). However, hemodynamic digital
subtraction angiography (DSA) images and the structure of the
vascular network, which reflect the hemodynamic features of liver
cancer, have been proposed as priority concerns by interventional
radiology physicians for analyzing the effects of treatments
including TACE prior and subsequent to initiation of treatment
(18). To the best of our knowledge,
few studies have been performed investigating the arterial
characteristics of HCC following treatment with sorafenib combined
with TACE. Therefore, the aim of the present study was to compare
the changes in the tumor vasculature of HCC following the use of
TACE alone compared with its use in combination with sorafenib. The
results of the present study may provide insight into this
combination treatment method as a therapy for advanced HCC.
Patients and methods
In the present study, 20 patients (5 females and 15
males; median age 51 years, age range, 37–74 years) with
HBV-associated HCC admitted to Zhongshan Hospital Affiliated to
Xiamen University (Xiamen, China) our hospital between January 2011
and August 2016 were reviewed. All patients exhibited advanced HCC
according to the BCLC staging system (BCLC C-stage) (19), confirmed by abdominal enhanced
computed tomography (CT) or magnetic resonance imaging (MRI). None
of the patients had been previously treated for HCC. A total of 10
patients were included in the TACE combined with sorafenib
treatment (TS) group. All of these patients were initially treated
with TACE, followed by treatment with sorafenib (200 mg orally;
Bayer AG, Leverkusen, Germany) at a dose of 400 mg twice daily, for
1 week. After 6 weeks, the patients in the TS group were treated
with a second session of TACE. The first angiography was performed
prior to each session of TACE and prior to sorafenib treatment; the
angiography was then repeated during the second session of TACE and
following sorafenib treatment. The remaining 10 patients were
treated with TACE only, with at least two sessions of TACE. The
data from the first TACE session were then compared with those from
the second TACE session using the angiography data collected. The
angiography was performed following each TACE session in the
TACE-only group, then the first angiography was compared with the
second angiography.
In the present study, grade ≤3 hepatic artery
branches were defined as microvascular vessels. The patient
inclusion criteria are summarized in Table I and exclusion criteria are described
in Table II. The baseline
information of patients is summarized in Table III. The present study was approved
by the Ethics Committee of Zhongshan Hospital Affiliated to Xiamen
University (Xiamen, China). Patients provided written informed
consent to participate prior to treatment, and for publication.
TACE was performed according to a standardized approach.
 | Table I.Patient inclusion criteria. |
Table I.
Patient inclusion criteria.
| Criteria | Cut-off |
|---|
| BCLC grade | C |
| Liver function | Child-Pugh class A
or B (39) |
| Total bilirubin,
µmol/l | <34.2
(3.4–17.1) |
| Alanine
transaminase level, U | <100 (7–40) |
| Aspartate
aminotransferase level, U | <90 (13–35) |
| Prothrombin time
activity, sec | <22 (9–13) |
| Serum creatinine
level, µmol/l | 1.5-fold the normal
value (53–97) |
| Neutrophil count,
/l | 4-10×109
(4–10) |
| Hemoglobin level,
g/l | ≥90 (115–150) |
|
Cardiopulmonary | NA |
| Cerebral
function | NA |
| Estimated life
expectancy, weeks | >12 |
 | Table II.Patients exclusion criteria. |
Table II.
Patients exclusion criteria.
| Criteria | Cut-off |
|---|
| Tumor volume/total
liver volume, % | >70 |
| Portal vein
patency | Main portal
vein/right branch of portal vein completely obstructed |
| Previous treatment
(surgical resection, ablation or TAI) | Yes |
 | Table III.Comparison of the baseline
information between the TS and TACE groups. |
Table III.
Comparison of the baseline
information between the TS and TACE groups.
| Parameters | TS group | TACE group |
|---|
| Sex,
male/female | 8/2 | 7/3 |
| Average age,
years | 55 | 50 |
| BCLC grade | C | C |
| Prothrombin time
activity, sec | 13.9
(12.7–16.2) | 14.9
(13.2–16.6) |
| Total bilirubin,
µmmol/l | 16.3
(8.6–32.8) | 16.9
(7.9–29.0) |
| Hemoglobin,
g/l | 127.0
(106.0–177.0) | 124.0
(104.0–140.0) |
| Alanine
transaminase, U | 78.2
(38.0–95.5) | 72.4
(54.3–89.2) |
| Aspartate
aminotransferase, U | 57.1
(25.0–84.0) | 60.1
(33.0–83.8) |
The TACE procedure was performed. Firstly, a
catheter was implanted into the celiac artery using the Seldinger
technique, and then a hepatic angiography was performed via a
common femoral approach using a 4 Fr angiographic catheter (Terumo
Medical Co., Tokyo, Japan). Subsequent to locating the lesion by
selective arteriography using a 2.0–2.7 Fr microcatheter (Terumo
Medical Co.), an emulsion consisting of lipiodol (Guerbet, Roissy,
France), epirubicin (Pfizer, Inc., New York, NY, USA) and
oxaliplatin (Jiangsu Aosaikang Pharmaceutical Industry Ltd., Co.,
Nanjing, China) was infused via the feeding arteries.
The angiography was then performed to observe the
tumor and to identify all the feeding arteries of the tumor. The
nonionic contrast iopromide (Bayer AG) was injected into each
hepatic artery at 5 ml/sec using an automated power injector. The
duration of the arterial injection was 11 sec. Subsequently, the
diameters of the branches of the celiac trunk, including the
hepatic and proper hepatic arteries, hepatic arterial branches,
splenic, gastroduodenal and left gastric arteries and the
microvessels within tumors, were evaluated and analyzed. The tumor
lesions in all 20 patients were supplied with nutrients and
connected via the proper hepatic arteries and their branches, but
not the left gastric, splenic or gastroduodenal arteries.
Therefore, in the present study, the proper hepatic arteries and
their branches were considered tumor-associated arteries, while the
left gastric, splenic and gastroduodenal arteries were considered
non-tumor-associated arteries. The diameters of the portal vein and
its branches were evaluated using a contrast-enhanced liver CT
scan. Then, the differences in the tumor-associated and
non-tumor-associated arteries between pre- and post-sorafenib
treatment analyses in the TS group were compared, as were the
differences in the arteries between the measurements taken
following the first and second TACE sessions in the TACE group. The
DSA images were analyzed by 2 radiologists (Zhongshan Hospital
Affiliated to Xiamen University) who were blind to the type of
treatment administered, according to the following method: The
angiography images were saved in the Artis workplace of the DSA
system (Artis zee biplane, Siemens AG, Munich, Germany). With this
workplace, the radiologists used the Postproc software included in
the DSA system to measure the diameter of vessels; prior to
measurement, radiologists calibrated the distance using the width
of the 4 Fr angiographic catheter as a reference. Microvascular
vessels were defined as ≤grade 3 branches of hepatic arteries and
these microvascular vessels were able to be detected by DSA.
Statistical analysis
The data are presented as the mean ± standard
deviation, and differences were compared using paired Student's
t-tests. P<0.05 was considered to indicate a statistically
significant difference. Analysis was performed using SPSS software
(version 19.0; IBM Corp., Armonk, NY, USA) and GraphPad Prism
software (version 5.01; GraphPad Software, Inc., La Jolla, CA,
USA).
Results
TACE combined with sorafenib decreases
the diameters of tumor-associated arteries
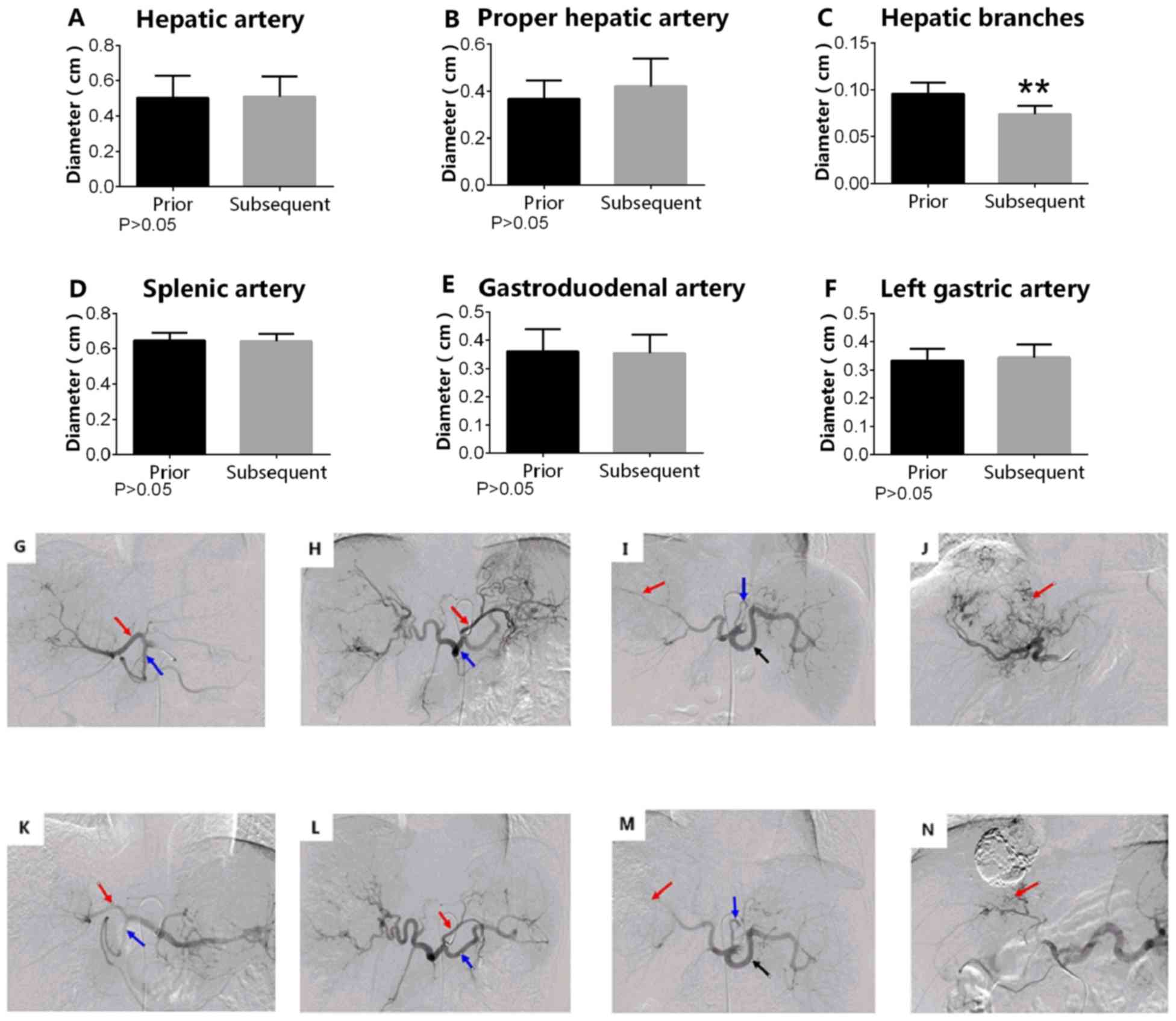
In the TS group, the diameters of tumor-associated
arteries prior to sorafenib administration were significantly
increased compared with those measured following sorafenib
treatment, including the diameters of the hepatic artery
(0.218±0.0423 vs. 0.158±0.0321 cm; P<0.05), the proper hepatic
artery (0.350±0.042 vs. 0.314±0.040 cm; P<0.05) and the hepatic
artery branches (0.218±0.042 vs. 0.158±0.032 cm, P<0.05;
Fig. 1).
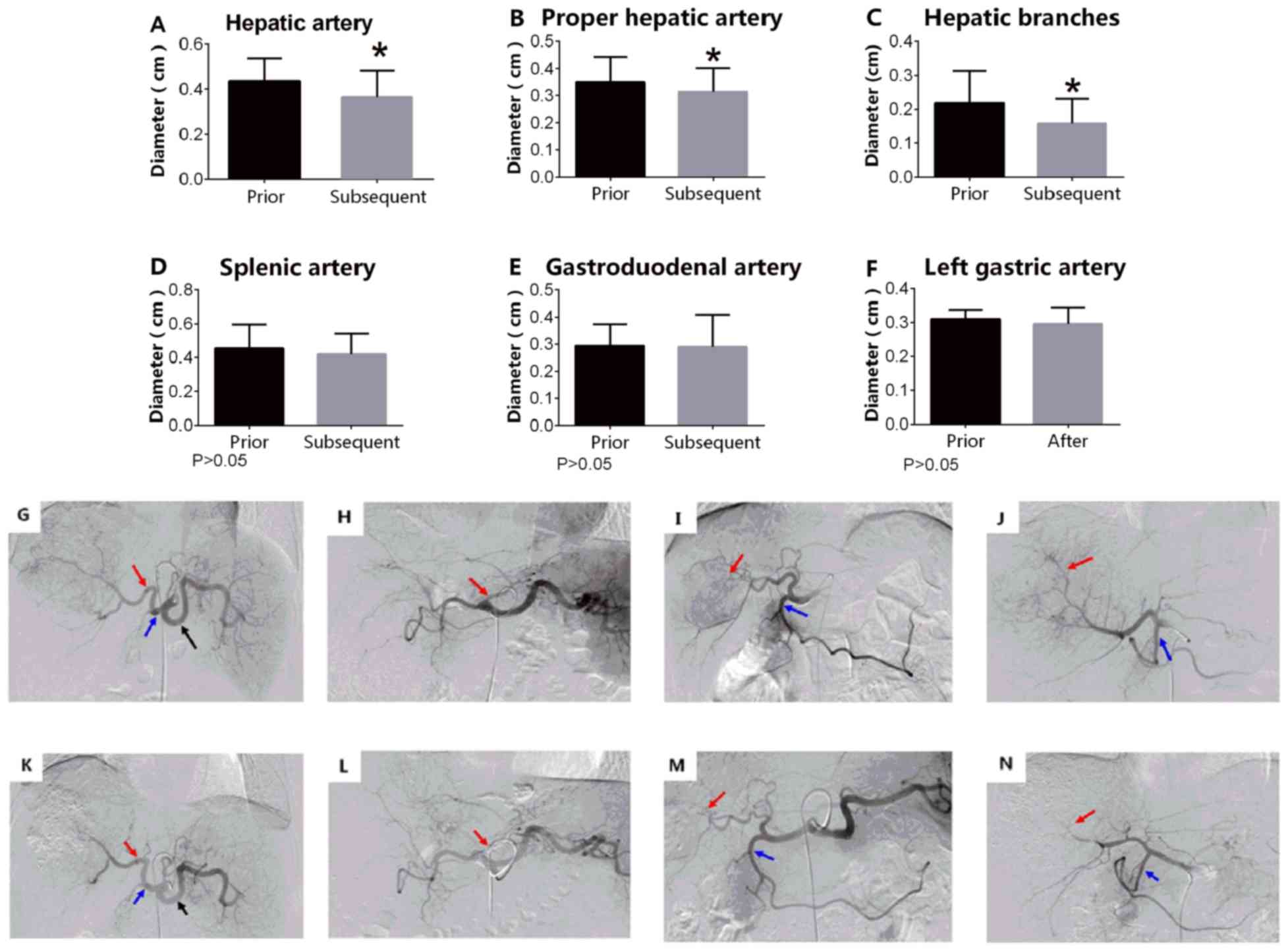 | Figure 1.TACE combined with sorafenib. TS
significantly reduced the diameter of tumor-associated arteries,
including the (A) hepatic artery, (B) proper hepatic artery and (C)
hepatic branches. *P<0.05. TS did not change the diameter of the
non-tumor associated arteries, including the (D) splenic artery,
(E) gastroduodenal artery and (F) left gastric artery. P>0.05.
G, K, H, L, I, M, J and N represent the same patient prior and
subsequent to adminstration of sorafenib respectively. G, H, I and
J are images collected in the first TACE procedure; K, L, M and N
are images collected in the second TACE procedure. (G) Arrow from
left to right indicates the proper hepatic, hepatic and splenic
arteries. (H) Arrow indicates left gastric artery. (I) Arrow from
left to right indicates the hepatic artery branches and
gastroduodenal artery. (J) Arrow from left to right indicates the
hepatic artery branches and gastroduodenal artery. (K) Arrow from
left to right indicates the proper hepatic, hepatic and splenic
arteries. (L) Arrow indicates left gastric artery. (M) Arrow from
left to right indicates the hepatic artery branches and
gastroduodenal artery. (N) Arrow from left to right indicates
hepatic artery branches and gastroduodenal artery. TACE,
transarterial chemoembolization; TS group, TACE combined with
sorafenib. The magnification for all images in Figure 1 is 1:4. |
TACE combined with sorafenib does not
decrease the diameters of non-tumor-associated arteries
In the TS group, the diameters of the
non-tumor-associated arteries prior to the administration of
sorafenib were not significantly different compared with those
measured following sorafenib treatment, including the diameters of
the splenic artery (0.454±0.063 vs. 0.418±0.055 cm; P>0.05), the
gastroduodenal artery (0.294±0.036 vs. 0.29±0.053 cm; P>0.05)
and the left gastric artery (0.310±0.012 vs. 0.296±0.022 cm;
P>0.05; Fig. 1).
TACE alone does not cause a decrease
in diameter of the tumor-associated arteries, with the exception of
the hepatic artery branches
In the TACE group, the diameters of the
tumor-associated arteries following the first session were not
significantly different compared with those following the second
session of TACE, including the diameters of the hepatic artery
(0.521±0.0272 vs. 0.502±0.0329 cm; P>0.05) and the proper
hepatic artery (0.450±0.037 vs. 0.407±0.0419 cm; P>0.05).
However, the diameters of the hepatic artery branches were
significantly decreased subsequent to the second session of TACE
compared with the measurements taken following the first session of
TACE (0.110±0.010 vs. 0.087±0.003 cm; P<0.05; Fig. 2).
TACE alone does not decrease the diameters of
non-tumor- associated arteries. In the TACE group, the diameters of
non-tumor-associated arteries following the first session of TACE
were not significantly different compared with those measured
following the second session of TACE, including the diameters of
the left gastric artery (0.300±0.018 vs. 0.301±0.021 cm;
P>0.05), the gastroduodenal artery (0.352±0.020 vs. 0.338±0.021
cm; P>0.05) and the splenic artery (0.602±0.026 vs. 0.61±0.028
cm; P>0.05; Fig. 2).
TACE combined with sorafenib and TACE
alone significantly decrease the number of tumor microvascular
vessels
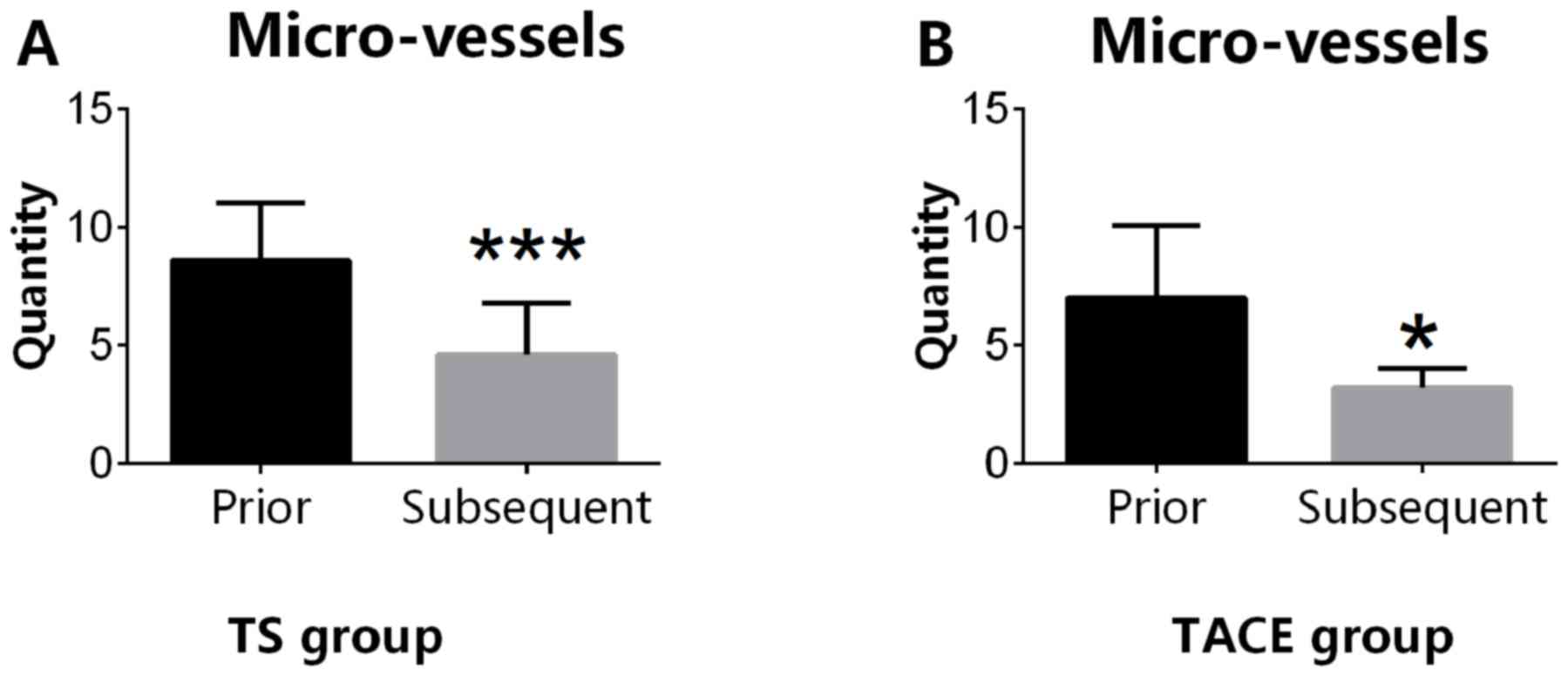
In the TS group, the number of tumor microvessels
prior to the administration of sorafenib was significantly
increased compared with the number following the sorafenib
treatment (8.60±1.07 vs. 4.6±0.980 cm; P<0.05). In the
TACE-alone group, the number of microvessels within the tumor
following the first session of TACE was also significantly
increased compared with that measured following the second session
of TACE (6.00±0.745 vs. 3.80±1.14 cm; P<0.05; Fig. 3).
TACE combined with sorafenib and
TACE-alone treatments do not affect the diameters of the portal
vein and its branches
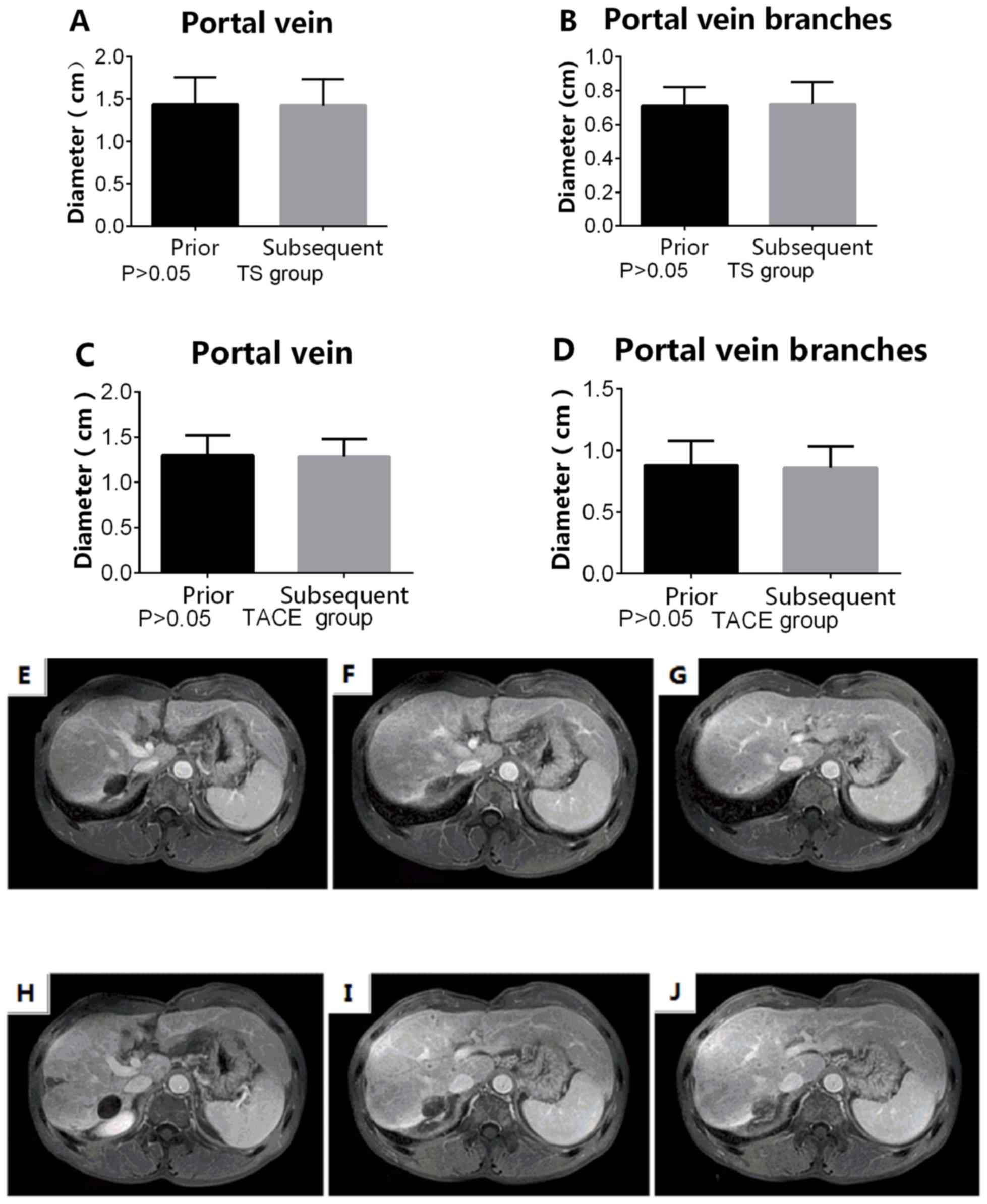
In the TS group, the diameters of the portal vein
and its branches prior to sorafenib treatment were not
significantly different compared with those measured following
sorafenib treatment (portal vein, 1.44±0.146 vs. 1.426±0.138 cm;
portal vein branches, 0.710±0.0491 vs. 0.718±0.0591 cm; both
P>0.05). In the TACE group, the diameters of the portal vein and
its branches following the first session of TACE were not
significantly different compared with those measured following the
second session of TACE (portal vein, 1.304±0.069 vs. 1.289±0.060
cm; portal vein branches, 0.879±0.063 vs. 0.859±0.055 cm; both
P>0.05; Fig. 4).
TACE combined with sorafenib
significantly reduces the diameters of tumor-associated arteries
and the number of tumor microvascular vessels compared with those
in the TACE-only group
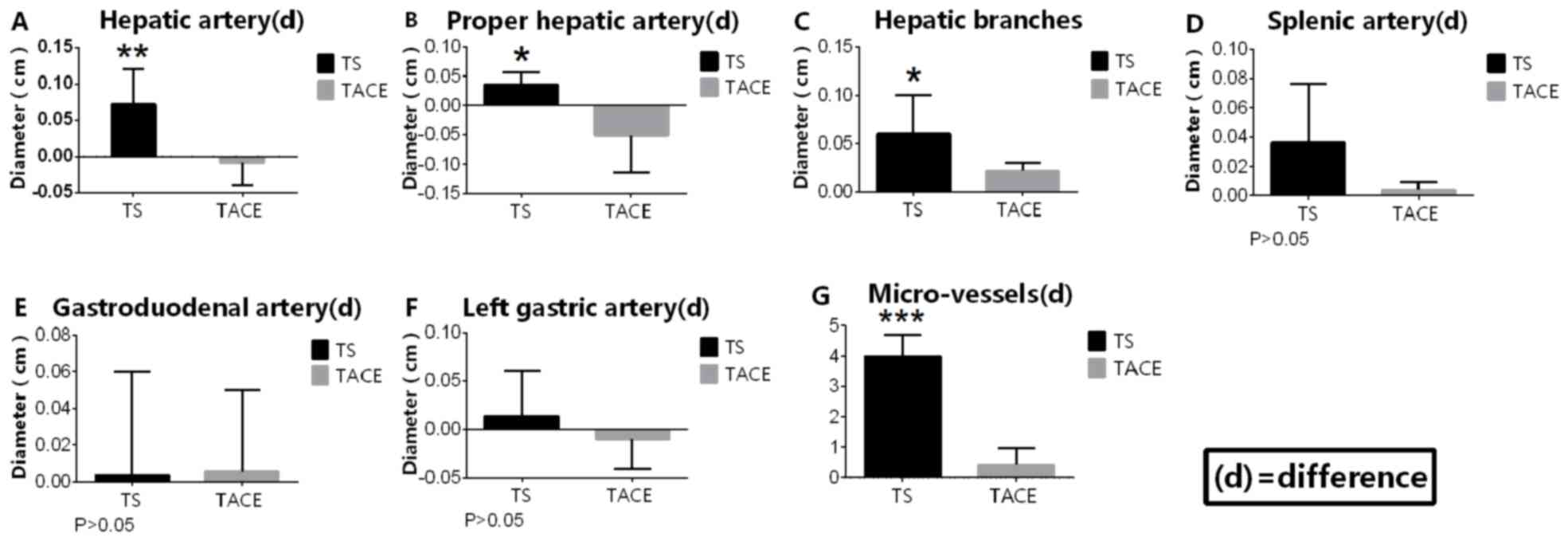
The difference in the diameters of tumor-associated
arteries, including the hepatic and the proper hepatic arteries and
the hepatic artery branches, between pre-sorafenib and
post-sorafenib measurements in the TS group was significantly
increased compared with the difference in the diameters measured
following the first and the second TACE sessions in the TACE-only
group. Concurrently, the number of microvascular vessels following
the second session in the TACE-only group was significantly
increased compared with that in the TS group (0.400±0.927 vs.
4.00±0.927 vessels respectively; P<0.05). However, the
difference in the diameters of non-tumor-associated arteries,
including the left gastric, splenic and gastroduodenal arteries,
between pre-sorafenib and post-sorafenib measurements in the TS
group was not significantly different compared with the difference
between the measurements taken following the first and second TACE
sessions in the TACE-only group (Fig.
5).
Discussion
The results of the present study demonstrated that
TACE combined with sorafenib significantly decreased the diameter
of tumor-associated hepatic arteries and their branches, notably
following the oral administration of sorafenib, while TACE alone
did not alter the diameter of the tumor-associated arteries
(20). Furthermore, the number of
microvascular vessels in the tumor, as detected by hepatic
arteriography, was markedly decreased following combination
treatment with sorafenib and TACE. Compared with the first
angiography, TACE alone also significantly decreased the number of
microvascular vessels within the HCC tumor tissues (21). TACE combined with sorafenib
significantly reduced the diameter of tumor-associated arteries and
tumor microvascular vessels when compared with TACE alone.
Previous studies have indicated that VEGF expression
in patients with HCC is associated with radiological features
(21,22). Previous data have also indicated that
the degree of enhancement in hepatic arteriography in HCC was
closely associated with the pro-angiogenic cytokine level, and that
VEGF contributed to the development of dense vascular networks in
cancer lesions (23,24). In the present study, following
combinatorial therapy with TACE and sorafenib, the number of tumor
microvascular vessels was significantly decreased. Previous studies
have also demonstrated that tumor-associated hepatic arterial
perfusion parameters were additionally decreased following
sorafenib treatment (25). Therefore,
we hypothesized that sorafenib combined with TACE, compared with
TACE alone, may reduce the serum levels of VEGF and bFGF in
patients with liver cancer, and inhibit angiogenesis by reducing
the production of pro-angiogenic factors, by preventing them from
binding to their receptors or by blocking their actions.
Previous data have demonstrated that the level of
VEGF facilitated the formation of arteries with larger diameters,
which provides increased blood supply to cancer lesions (26). In addition, the present study
demonstrated that the diameter of tumor-associated arteries in
patients with HCC treated with TACE combined with sorafenib was
significantly reduced, and that the microvascular density of HCC
tumor tissues was markedly decreased, compared with those in
patients treated with TACE only (27). We hypothesize that sorafenib inhibited
the upregulation of TACE-induced pro-angiogenic cytokines,
including VEGF or PDGF, which are critical during the development
of cancer; furthermore, pro-angiogenic cytokines including VEGF
serve a key role in stimulating angiogenesis and endothelial cell
proliferation. However, the absence of quantified data on these
growth factors is a limitation of the present study. In addition,
this was a retrospective observational study and HCC biopsies were
not routinely performed; diagnoses were usually made according to
the results of enhanced CT or MRI-T1 and -T2 diffusion-weighted
imaging scans. The absence of HCC biopsy data is an additional
limitation of the present study.
Parenchymal arterialization, sinusoidal
capillarization and the development of unpaired arteries are among
the multiple steps involved in HCC carcinogenesis (28). Ultimately, the blood supply of HCC
shifts from the portal vein to the hepatic artery. A total of
>95% of the blood supply in HCC originates from the hepatic
artery, while the non-tumor liver region obtains 80% of its blood
supply from the portal vein (29).
Previous studies have demonstrated that when contrast agent was
infused via the hepatic artery, the intratumoral contrast
concentrations were increased 10-fold compared with those following
infusion through the portal vein, and also indicated that the
tissue concentration of contrast agents within the tumor was >40
times increased compared with of the surrounding normal liver
tissue (30,31). In the present study, it was revealed
that TACE combined with sorafenib and TACE alone did not decrease
the diameters of the portal vein or its branches. A previous study
also revealed that during hepatocarcinogenesis the majority of
hepatocellular nodules exhibit a deterioration of arterial blood
flow rate and pressure prior to the loss of portal blood flow
(32). Subsequently, as a result of a
marked increase in neo-vascularized arteries, with the assistance
of increased pro-angiogenic cytokine secretion, arterial blood flow
becomes dominant (33).
Recent advances in imaging have enabled clinicians
to evaluate the hemodynamics of hepatocellular lesions, in
particular dysplastic nodules or HCC, using CT or MRI hepatic
arteriography and CT or MRI during arterial portography (34). As a tumor with a typically good blood
supply, HCC exhibits hyper-enhancement on DSA in the majority of
cases; more specifically, it demonstrates marked hyper-enhancement
during the arterial phase, with such enhancement gradually
decreasing during the venous phase and disappearing during the
delayed phase (35). To the best of
our knowledge, few studies have been performed to investigate the
hemodynamic characteristics of HCC treated with sorafenib. In
addition, the hemodynamic changes following combination treatment
with sorafenib and TACE have not been well-evaluated
radiologically. The present study compared the diameter of
different hepatic arteries in patients treated sorafenib combined
with TACE or TACE alone (36).
Previously, the response of HCC to treatment has been primarily
evaluated using the mRECIST criteria. However, the staining of DSA
images and the structure of the vascular network prior to and
following interventional therapy are priority concerns for
interventional radiologists. In the present retrospective study,
DSA provided a useful evaluation tool for assessing the response of
HCC to combination treatment with TACE and sorafenib (37,38).
In conclusion, TACE and sorafenib are used
individually in the treatment of HCC at different stages, and the
two treatments have an anti-angiogenic effect, with sorafenib
exhibiting broader effects due to its capacity for tyrosine kinase
inhibition. The results of the present study indicated improved
hepatic hemodynamic outcomes when TACE and sorafenib were used in
combination for the treatment of advanced-stage HCC, compared with
TACE alone.
Acknowledgements
The authors would like to thank Dr Xinhua Zhou for
aiding with data analysis.
Funding
This work was supported by the Project of National
Natural Science Foundation of China (no. 81371698).
Availability of data and materials
The datasets used or analysed during the current
study are available from the corresponding author on reasonable
request.
Authors' contributions
YFZ, HZ, HP, QL, XZ, WW, YL, MZ and JW collected and
analyzed the data. YLZ, LC and JZ designed the research and wrote
the manuscript. All authors contributed toward data analysis,
drafting and revising the paper and agree to be accountable for all
aspects of the work.
Ethics approval and consent to
participate
The present study was approved by the Ethics
Committee of Zhongshan Hospital Xiamen University. Patients
provided written informed consent prior to treatment.
Consent for publication
Patients provided written informed consent for
publication.
Competing interests
The authors declare that they have no competing
interests.
References
|
1
|
Elserag HB and Rudolph KL: Hepatocellular
carcinoma: Epidemiology and molecular carcinogenesis.
Gastroenterology. 132:2557–2576. 2007. View Article : Google Scholar : PubMed/NCBI
|
|
2
|
Wang JS, Huang T, Su J, Liang F, Wei Z,
Liang Y, Luo H, Kuang SY, Qian GS, Sun G, et al: Hepatocellular
carcinoma and aflatoxin exposure in Zhuqing Village, Fusui County,
People's Republic of China. Cancer Epidemiol Biomarkers Prev.
10:143–146. 2001.PubMed/NCBI
|
|
3
|
Alloatti A, Testero SA and Uttaro AD:
Chemical evaluation of fatty acid desaturases as drug targets in
Trypanosoma cruzi. Int J Parasitol. 39:985–993. 2009. View Article : Google Scholar : PubMed/NCBI
|
|
4
|
Burrel M, Reig M, Forner A, Barrufet M, de
Lope CR, Tremosini S, Ayuso C, Llovet JM, Real MI and Bruix J:
Survival of patients with hepatocellular carcinoma treated by
transarterial chemoembolisation (TACE) using drug eluting beads.
Implications for clinical practice and trial design. J Hepatol.
56:1330–1335. 2012. View Article : Google Scholar : PubMed/NCBI
|
|
5
|
Boas FE, Kamaya A, Do B, Desser TS,
Beaulieu CF, Vasanawala SS, Hwang GL and Sze DY: Classification of
hypervascular liver lesions based on hepatic artery and portal vein
blood supply coefficients calculated from triphasic CT scans. J
Digit Imaging. 28:213–223. 2015. View Article : Google Scholar : PubMed/NCBI
|
|
6
|
Brade AM, Ng S, Brierley J, Kim J,
Dinniwell R, Ringash J, Wong RR, Cho C, Knox J and Dawson LA: Phase
1 trial of sorafenib and stereotactic body radiation therapy for
hepatocellular carcinoma. Int J Radiat Oncol Biol Phys. 94:580–587.
2016. View Article : Google Scholar : PubMed/NCBI
|
|
7
|
Brock TJ, Browse J and Watts JL: Genetic
regulation of unsaturated fatty acid composition in C. elegans.
PLoS Genet. 2:e1082006. View Article : Google Scholar : PubMed/NCBI
|
|
8
|
Jia ZZ, Jiang GM and Feng YL: Serum
HIF-1alpha and VEGF levels pre- and post-TACE in patients with
primary liver cancer. Chin Med Sci J. 26:158–162. 2011. View Article : Google Scholar : PubMed/NCBI
|
|
9
|
Chen J, Zhang WJ, Guo Z, Wang HB, Wang DD,
Zhou JJ and Chen QW: pH-responsive iron manganese silicate
nanoparticles as T1-T2* dual-modal imaging probes for tumor
diagnosis. ACS Appl Mater Interfaces. 7:5373–5383. 2015. View Article : Google Scholar : PubMed/NCBI
|
|
10
|
Das S, Ladell DS, Podgrabinska S,
Ponomarev V, Nagi C, Fallon JT and Skobe M: Vascular endothelial
growth factor-C induces lymphangitic carcinomatosis, an extremely
aggressive form of lung metastases. Cancer Res. 70:1814–1824. 2010.
View Article : Google Scholar : PubMed/NCBI
|
|
11
|
Di Costanzo GG, Tortora R, Morisco F,
Addario L, Guarino M, Cordone G, Falco L and Caporaso N: Impact of
diabetes on outcomes of sorafenib therapy for hepatocellular
carcinoma. Target Oncol. 12:61–67. 2017. View Article : Google Scholar : PubMed/NCBI
|
|
12
|
Enoch HG, Catalá A and Strittmatter P:
Mechanism of rat liver microsomal stearyl-CoA desaturase. Studies
of the substrate specificity, enzyme-substrate interactions, and
the function of lipid. J Biol Che. 251:5095–5103. 1976.
|
|
13
|
Funami Y, Okuyama K, Koide Y, Kouzu T,
Kinoshita H, Shimada Y and Isono K: Anatomical analysis of small
bronchial arteries in front of the trachea by 3D-CT and digital
subtraction angiography: Implications for esophageal cancer
surgery. Nihon Geka Gakkai Zasshi. 96:207–212. 1995.(In Japanese).
PubMed/NCBI
|
|
14
|
Kim BK, Kim SU, Park JY, Kim DY, Ahn SH,
Park MS, Kim EH, Seong J, Lee DY and Han KH: Applicability of BCLC
stage for prognostic stratification in comparison with other
staging systems: single centre experience from long-term clinical
outcomes of 1717 treatment-naïve patients with hepatocellular
carcinoma. Liver Int. 32:1120–1127. 2012. View Article : Google Scholar : PubMed/NCBI
|
|
15
|
Han K and Kim JH: Transarterial
chemoembolization in hepatocellular carcinoma treatment: Barcelona
clinic liver cancer staging system. World J Gastroenterol.
21:10327–10335. 2015. View Article : Google Scholar : PubMed/NCBI
|
|
16
|
Iavarone M, Cabibbo G, Piscaglia F,
Zavaglia C, Grieco A, Villa E, Cammà C and Colombo M: SOFIA
(SOraFenib Italian Assessment) study group: Field-practice study of
sorafenib therapy for hepatocellular carcinoma: A prospective
multicenter study in Italy. Hepatology. 54:2055–2063. 2011.
View Article : Google Scholar : PubMed/NCBI
|
|
17
|
Park JW, Koh YH, Kim HB, Kim HY, An S,
Choi JI, Woo SM and Nam BH: Phase II study of concurrent
transarterial chemoembolization and sorafenib in patients with
unresectable hepatocellular carcinoma. J Hepatol. 56:1336–1342.
2012. View Article : Google Scholar : PubMed/NCBI
|
|
18
|
Igal RA: Roles of stearoylCoA desaturase-1
in the regulation of cancer cell growth, survival and
tumorigenesis. Cancers (Basel). 3:2462–2477. 2011. View Article : Google Scholar : PubMed/NCBI
|
|
19
|
Llovet JM, Brã C and Bruix J: Prognosis of
hepatocellular carcinoma: The BCLC staging classification. Semin
Liver Dis. 19:329–338. 1999. View Article : Google Scholar : PubMed/NCBI
|
|
20
|
Wang ZL: Research on the security and
clinical curative effect of TACE combined with sorafenib in the
treatment of hepatocellular carcinoma in the middle and late
period. China Foreign Med Treat. 1:126–127. 2016.
|
|
21
|
Chung YH, Han G, Yoon JH, Yang J, Wang J,
Shao GL, Kim BI, Lee TY and Chao Y: Interim analysis of START:
Study in Asia of the combination of TACE (transcatheter arterial
chemoembolization) with sorafenib in patients with hepatocellular
carcinoma trial. Int J Cancer. 132:2448–2458. 2013. View Article : Google Scholar : PubMed/NCBI
|
|
22
|
Li X, Feng GS, Zheng CS, Zhuo CK and Liu
X: Expression of plasma vascular endothelial growth factor in
patients with hepatocellular carcinoma and effect of transcatheter
arterial chemoembolization therapy on plasma vascular endothelial
growth factor level. World J Gastroenterol. 10:2878–2882. 2004.
View Article : Google Scholar : PubMed/NCBI
|
|
23
|
Yamaguchi R, Yano H, Iemura A, Ogasawara
S, Haramaki M and Kojiro M: Expression of vascular endothelial
growth factor in human hepatocellular carcinoma. Hepatology.
28:68–77. 1998. View Article : Google Scholar : PubMed/NCBI
|
|
24
|
Poon RT, Lau CP, Ho JW, Yu WC, Fan ST and
Wong J: Tissue factor expression correlates with tumor angiogenesis
and invasiveness in human hepatocellular carcinoma. Clin Cancer
Res. 9:5339–5345. 2003.PubMed/NCBI
|
|
25
|
Maio MD, Daniele B and Perrone F: Targeted
therapies: Role of sorafenib in HCC patients with compromised liver
function. Nat Rev Clin Oncol. 6:505–506. 2009. View Article : Google Scholar : PubMed/NCBI
|
|
26
|
Wilhelm SM, Adnane L, Newell P, Villanueva
A, Llovet JM and Lynch M: Preclinical overview of sorafenib, a
multikinase inhibitor that targets both Raf and VEGF and PDGF
receptor tyrosine kinase signaling. Mol Cancer Ther. 7:3129–3140.
2008. View Article : Google Scholar : PubMed/NCBI
|
|
27
|
Zhang L, Hu P, Chen X and Bie P:
Transarterial chemoembolization (TACE) plus sorafenib versus TACE
for intermediate or advanced stage hepatocellular carcinoma: A
meta-analysis. PLoS One. 9:e1003052014. View Article : Google Scholar : PubMed/NCBI
|
|
28
|
Ooka Y, Kanai F, Okabe S, Ueda T,
Shimofusa R, Ogasawara S, Chiba T, Sato Y, Yoshikawa M and Yokosuka
O: Gadoxetic acid-enhanced MRI compared with CT during angiography
in the diagnosis of hepatocellular carcinoma. Magn Reson Imaging.
31:748–754. 2013. View Article : Google Scholar : PubMed/NCBI
|
|
29
|
Rossi S, Garbagnati F, Lencioni R,
Allgaier HP, Marchianò A, Fornari F, Quaretti P, Tolla GD, Ambrosi
C, Mazzaferro V, et al: Percutaneous radio-frequency thermal
ablation of nonresectable hepatocellular carcinoma after occlusion
of tumor blood supply. Radiology. 217:119–126. 2000. View Article : Google Scholar : PubMed/NCBI
|
|
30
|
Numata K, Tanaka K, Kiba T, Saito S,
Isozaki T, Hara K, Morimoto M, Sekihara H, Yonezawa H and Kubota T:
Using contrast-enhanced sonography to assess the effectiveness of
transcatheter arterial embolization for hepatocellular carcinoma.
AJR Am J Roentgenol. 176:1199–1205. 2001. View Article : Google Scholar : PubMed/NCBI
|
|
31
|
Koito K, Namieno T, Ichimura T, Hirokawa
N, Syonai T, Hareyama M, Katsuramaki T, Hirata K and Nishi M: Power
Doppler sonography: Evaluation of hepatocellular carcinoma after
treatment with transarterial embolization or percutaneous ethanol
injection therapy. AJR Am J Roentgenol. 174:337–341. 2000.
View Article : Google Scholar : PubMed/NCBI
|
|
32
|
Breedis C and Young G: The blood supply of
neoplasms in the liver. Am J Pathol. 30:969–977. 1954.PubMed/NCBI
|
|
33
|
Yamasaki T, Kurokawa F, Shirahashi H,
Kusano N, Hironaka K and Okita K: Percutaneous radiofrequency
ablation therapy for patients with hepatocellular carcinoma during
occlusion of hepatic blood flow. Comparison with standard
percutaneous radiofrequency ablation therapy. Cancer. 95:2353–2360.
2002. View Article : Google Scholar : PubMed/NCBI
|
|
34
|
Burrel M, Llovet JM, Ayuso C, Iglesias C,
Sala M, Miquel R, Caralt T, Ayuso JR, Solé M, Sanchez M, et al: MRI
angiography is superior to helical CT for detection of HCC prior to
liver transplantation: An explant correlation. Hepatology.
38:1034–1042. 2003. View Article : Google Scholar : PubMed/NCBI
|
|
35
|
Kudo M: Imaging blood flow characteristics
of hepatocellular carcinoma. Oncology. 62 Suppl 1:S48–S56. 2002.
View Article : Google Scholar
|
|
36
|
Woo HY, Heo J, Yoon KT, Kim GH, Kang DH,
Song GA and Cho M: Clinical course of sorafenib treatment in
patients with hepatocellular carcinoma. Scand J Gastroenterol.
47:809–819. 2012. View Article : Google Scholar : PubMed/NCBI
|
|
37
|
Tsurusaki M and Murakami T: Surgical and
locoregional therapy of HCC: TACE. Liver Cancer. 4:165–175. 2015.
View Article : Google Scholar : PubMed/NCBI
|
|
38
|
Wan X, Zhai X, Yan Z, Yang P, Li J, Wu D,
Wang K, Xia Y and Shen F: Retrospective analysis of transarterial
chemoembolization and sorafenib in Chinese patients with
unresectable and recurrent hepatocellular carcinoma. Oncotarget.
7:83806–83816. 2016. View Article : Google Scholar : PubMed/NCBI
|
|
39
|
Pressiani T, Boni C, Rimassa L, Labianca
R, Fagiuoli S, Salvagni S, Ferrari D, Cortesi E, Porta C,
Mucciarini C, et al: Sorafenib in patients with Child-Pugh class A
and B advanced hepatocellular carcinoma: A prospective feasibility
analysis. Ann Oncol. 24:406–411. 2013. View Article : Google Scholar : PubMed/NCBI
|