Introduction
Pancreatic cancer is an aggressive and lethal
disease with a poor prognosis, representing the fourth leading
cause of cancer-associated mortality worldwide (1). The overall prognosis of pancreatic
cancer has remained unchanged even though advances have been made
in surgical techniques and adjuvant treatment regimens (2). The biological features of pancreatic
cancer and the hypoxic environments surrounding cancer cells often
lead to resistance to radiotherapy and chemotherapy (3). The tumor microenvironment has an active
role in the progression of pancreatic cancer, and targeting the
components of this microenvironment may denote a novel therapeutic
strategy (4). Pancreatic cancer is
characterized by an abundant desmoplastic/stromal reaction. It is
reported that pancreatic stellate cells (PSCs) are responsible for
the development of the desmoplastic reaction (5). As one of the most important types of
stromal cell in the microenvironment of pancreatic cancer cells,
PSCs have become notable (6,7).
Normally, PSCs are in their quiescent state,
characterized by abundant vitamin A stored in lipid droplets in the
cytoplasm (8). In response to
pancreatic injury or pancreatic inflammation, PSCs are activated,
transforming from quiescent phenotypes into myofibroblast-like
cells that express the cytoskeletal protein α-smooth muscle actin
(α-SMA), and synthesize excessive amounts of extracellular matrix
(ECM) proteins leading to fibrosis (9,10). The
interaction between pancreatic cancer cells and PSCs is the focus
of an increasing number of studies. There is accumulating evidence
that PSCs have an important role in the progression of pancreatic
fibrosis in chronic pancreatitis, as well as in pancreatic cancer
(11–13). PSCs interact with pancreatic cancer
cells to create a fibrotic and hypoxic microenvironment, which
promotes the initiation, development of and resistance to
chemoradiation therapy. However, the specific role of PSCs in
pancreatic cancer is currently unclear, and the association between
PSCs and pancreatic cancer cells is under discussion. The present
study was performed in order to explore the effect of PSCs on the
viability of pancreatic cancer cells, and to elucidate the
potential molecular mechanisms underlying the interaction between
PSCs and pancreatic cancer cells.
Materials and methods
Cell culture
The PANC-1 and MIA-PaCa-2 human pancreatic cancer
cell lines (American Type Culture Collection, Manassas, VA, USA)
were grown at 37°C in Dulbeccos modified Eagles medium (DMEM)
supplemented with high glucose, 1.5 g/l sodium bicarbonate, 100
U/ml penicillin, 100 mg/ml streptomycin (Invitrogen; Thermo Fisher
Scientific, Inc., Waltham, MA, USA) and 10% fetal calf serum (FCS;
HyClone; GE Healthcare, Logan, UT, USA). AsPC-1 cells (American
Type Culture Collection) were maintained in RPMI-1640 (Invitrogen;
Thermo Fisher Scientific, Inc.) supplemented with 10% FCS,
penicillin (100 U/ml) and streptomycin (100 mg/ml). Cells were
maintained in a 5% CO2 humidified incubator at 37°C.
Human PSCs were isolated as previously described
(14). The protocols used in the
present study were approved by the Ethics Committee of the
Affiliated Hospital of Qingdao University, and conducted in full
accordance with ethical principles. All patients gave informed
consent to use excess pathological specimens for research and human
pancreatic cancer tissues were collected with written informed
consent from patients prior to participation in the study. The
resected pancreatic tissues from patients who had undergone surgery
for pancreatic cancer were digested with a mixture of collagenase
P, pronase and DNase in Geys balanced salt solution (Sigma-Aldrich,
Merck KGaA, Darmstadt, Germany). The suspension of cells was
centrifuged in a 28.7% Nycodenz gradient at 1,400 × g for 23 min at
room temperature. Stellate cells separated into a hazy band just
above the interface of the Nycodenz solution and the aqueous
buffer. This band was harvested, and the cells were washed and
resuspended in Iscove's modified Dulbecco's medium (Invitrogen;
Thermo Fisher Scientific, Inc.) containing 10% FBS (Hyclone; GE
Healthcare, Life Sciences, Logan, UT, USA), 4 mmol/l glutamine
(Life Technologies; Thermo Fisher Scientific, Inc.) and antibiotics
(Invitrogen; Thermo Fisher Scientific, Inc.). The cultured PSCs
were used with their second-fourth passages. The expression of
glial fibrillary acidic protein (GFAP) and α-SMA was examined by
immunofluorescent staining. Briefly, PSCs were incubated without
serum for 24 h at 37°C and fixed in 4% paraformaldehyde for 30 min
at room temperature. Following blocking with 1% normal bovine serum
albumin (Sigma-Aldrich, Merck KGaA, Darmstadt, Germany) for 1 h at
room temperature, cells were incubated with mouse anti α-SMA
antibody (Sigma-Aldrich, Merck KGaA; catalog number: A5228) or
anti-GFAP antibody (Abcam; catalog number: ab7260) at 1:400
dilution overnight at 4°C. Following washing with PBS, PSCs cells
were incubated with anti-rabbit Alexa 488Yconjugated IgG at 1:100
dilution (Abcam; catalog number: ab150077) and Alexa 555Y labeled
anti-mouse IgG antibody (Abcam; catalog number: AB_2563179) at
1:100 dilution for 1 h at 4°C and washed again with PBS, and then
samples were analyzed for fluorescence under a confocal laser
scanning microscope (Nikon A1/C1, Tokyo, Japan). For the negative
control, the primary antibody was replaced with 2% bovine serum
albumin or polyclonal rabbit IgG at 1:200 dilution (Abcam; catalog
number: ab6721).
Co-culture of pancreatic cancer cells
and PSCs
Pancreatic cancer cells were seeded at a density of
2×105 cells/well into 6-well culture plates (BD
Biosciences, Franklin Lakes, NJ, USA). Human PSCs were seeded at
4×105 cells/culture insert into culture inserts with 1.0
µm pores (BD Biosciences). The subsequent day, the culture inserts
seeded with PSCs were placed into the 6-well plates containing
pancreatic cancer cells, and incubation was continued for ≤3 days
at 37°C.
Cellular viability assay
PANC-1, MIA-PaCa-2 and AsPC-1 pancreatic cancer cell
lines in the exponential phase of growth were seeded into a 96-well
tissue culture plate with (1×104)/well and incubated for
24 h at 37°C. The cells were co-cultured with medium alone (control
group) or PSCs or SB525334, an inhibitor for TGF-beta1 receptor,
(Abmole Bioscience Inc., Huston, TX, USA; Catalog number: M2108)
for 12, 24 and 48 h for evaluation. Cell viability was determined
using an MTT assay, according to the manufacturer's protocol (kit
CGD1, Sigma-Aldrich,). Briefly, cells were grown in media
supplements with 10% FBS, harvested using trypsin (Thermo Fisher
Scientific, Inc.; Catalog number: 25200056) and counted using
Trypan blue and a hemocytometer. Cells were then serially diluted
in a clear cell culture plate and incubated for 3 h with MTT
reagent at 37°C. Following this incubation, cells were treated with
MTT solvent for 15 min at room temperature and measured with
spectrophotometer (SKU: S500, Parco Scientific Company, USA).
Absorbance was measured at OD=590 nm.
Cellular invasion analysis
A cellular migration assay was performed using
modified Boyden Chambers consisting of Transwell pre-coated
Matrigel membrane filter inserts with 8 µm pores in 24-well tissue
culture plates (BD Biosciences). Briefly, PSCs were seeded at
5×104 cells/well into the plates. Media supplemented
with 10% FCS in the lower chamber served as the chemoattractant.
The following day, pancreatic cancer cells were seeded at
2×105 cells/insert into the culture inserts (8 µm pores)
and placed on the 24-well plate containing human PSCs or SB525334.
After a 24-h incubation at 37°C, the stained cells were counted by
inverted microscopy. Briefly, cells were removed from the upper
surface of the membranes with a cotton swab, and cells that
migrated to the lower surface were stained with 0.2% (w/v) crystal
violet in 2% ethanol for 15 min at room temperature and were washed
with water. Dried membranes were cut out and mounted on glass
slides in immersion oil. At least 10 random high-power fields from
each of triplicate membranes were counted for each experimental
condition at ×200 magnification. Each experiment was performed in
triplicate.
Apoptosis assay
The apoptosis of MIA-PaCa-2 and AsPC-1 pancreatic
cancer cells, with or without human PSCs, was induced by
gemcitabine and detected by flow cytometry using an Annexin
V-fluorescein isothiocyanate (FITC) Apoptosis Detection kit
(Nanjing KeyGen Biotech, Co., Ltd., Nanjing, China) according to
the manufacturer's protocol. Briefly, the cells were harvested and
stained with propidium iodide (PI) and Annexin V-FITC. The
apoptosis rate was assayed using a FACSCalibur flow cytometer (BD
Biosciences and Beckman-Coulter, Inc., San Jose, CA, USA) at a
488-nm wavelength.
In vivo experiments
BALB/c female nude mice at the age of 6–8 weeks
(weighing, 18–22 g) were used. BALB/c mice were purchased from the
Center of Experimental Animals, Affiliated Hospital of Medical
College, Qingdao University, and maintained in a pathogen-free
facility at room temperature. Mice had free access to food and
water and were kept in a 12 h light/dark cycle. Female BALB/c nude
mice were divided into the following groups: MIA-PaCa-2 alone as
the control group; co-transplantation of MIA-PaCa-2 and PSCs group;
co-transplantation of MIA-PaCa-2, PSCs and SB525334 group.
MIA-PaCa-2 (1×105) and PSCs (5×104) or
SB525334 were suspended in 100 µl PBS, and then subcutaneously
co-transplanted with PSCs (5×104) into the right flank
of the mice. In total, 10 mice were used in each group, and the
number of mice used in the experiment is 30. Tumor sizes and body
weight were measured every week by external caliper, and the
average tumor volumes were calculated as (length ×
weight2). A total of 2.5 weeks subsequent to
implantation, mice were humanely euthanized with 3% pentobarbital
sodium (Sigma-Aldrich, Merck KGaA, Darmstadt, Germany) and tumors
were harvested. All protocols were approved by the Animal Ethics
Committee of the Affiliated Hospital of Medical College, Qingdao
University.
Statistical analysis
Results are presented as the mean ± standard
deviation of triplicate cultures, and statistical differences were
assessed using the Student's t-test or two-way analysis of
variance. P<0.05 was considered to indicate a statistically
significant difference. Data were analyzed using SPSS version 16.0
(SPSS, Chicago, IL, USA).
Results
Isolation and identification of
PSCs
PSCs from human pancreatic cancer tissues were
isolated by the aforementioned enzymatic digestion-gradient
centrifugation method. Attached cells exhibited an activated
phenotype, characterized by a myofibroblast-like appearance and a
shortening of double time. Under cytoimmunochemistry examination,
the PSC markers α-SMA and GFAP were overexpressed in the cytoplasm
of the PSCs.
In vitro proliferation assay
The AsPC-1, PANC-1 and MIA-PaCa-2 (1×105)
pancreatic cancer cell lines and PSCs (5×104) were
seeded into the upper and lower chambers, respectively. The cells
were then co-cultured for 72 h. Subsequently, an MTT assay was
performed to determine the number of pancreatic cancer cells in the
upper chamber, and the results were expressed as the absorbance at
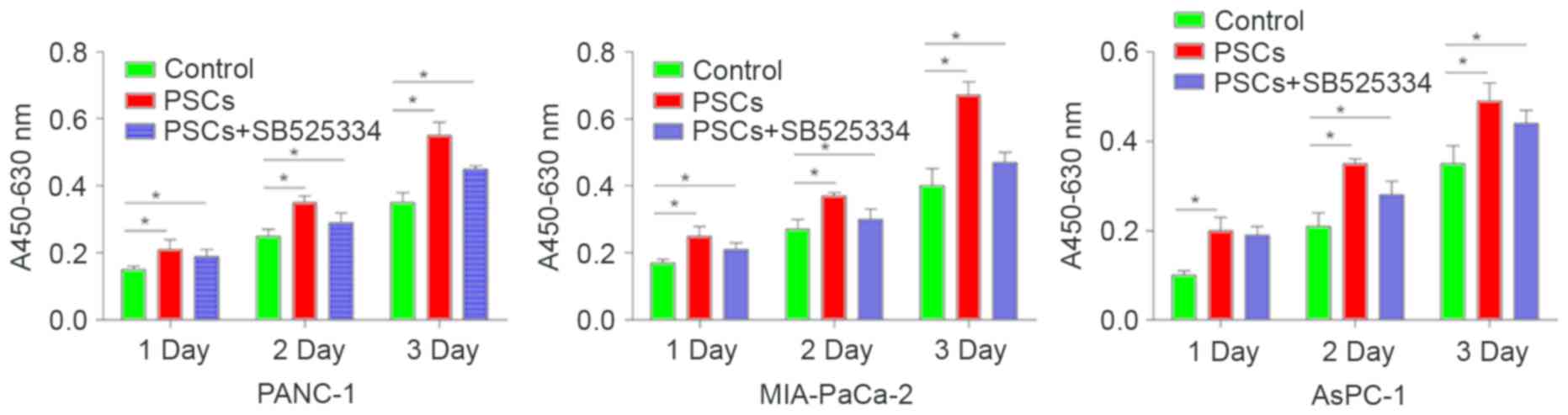
490 nm in a spectrophotometer. The MTT assay revealed that,
subsequent to a 72-h co-culture with PSCs, the viability of cancer
cells significantly increased, compared with those in the control
group without co-culture (P<0.05). The effect of PSCs on the
viability of AsPC-1 was significantly higher compared with the
control (140.13±12.50% vs. 104.21±8.9%; P=0.014). However, the
proliferation of pancreatic cancer cells promoted by PSCs was
partially blocked by the transforming growth factor-β (TGF-β)
inhibitor, SB525334 (125.71±11.30% vs. 140.13±12.50%; P=0.036;
Fig. 1). The viability of PANC-1 in
control, PSCs and SB525334 group was 65.06±10.9, 137.13±11.30 and
99.78±13.11% respectively (P=0.017). The viability of MIA-PaCa-2 in
control, PSCs and SB525334 group was 87.26±11.1, 165.73±15.35 and
95.18±11.09% (P=0.008), demonstrating that PANC-1 and MIA-PaCa-2
also exhibited similar results. These findings demonstrated that
PSCs promoted the viability of pancreatic cancer cells, and the
effects may be partially inhibited by SB525334.
Cells migration analysis
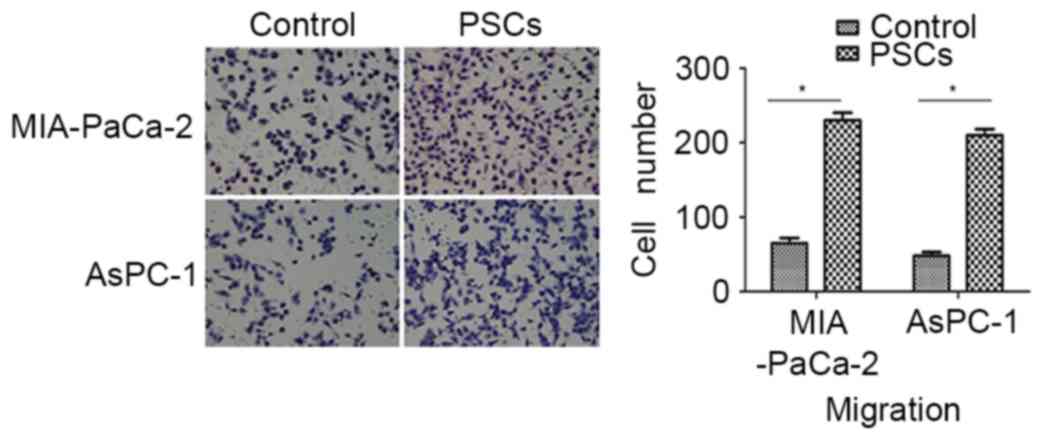
A Matrigel invasion assay was performed to evaluate
the effect of PSCs on the invasion ability of pancreatic cancer
cells. With the presence of PSCs in the lower chambers, the
invasion capacity of AsPC-1 cells was prone to increase as compared
with the control (437.50±21.61%; P<0.001). A significant
increase in the migration of MIA-PaCa-2 cells was also induced in
the presence of PSCs, as compared with the control (353.85±19.16%;
P=0.013; Fig. 2).
Apoptosis assay
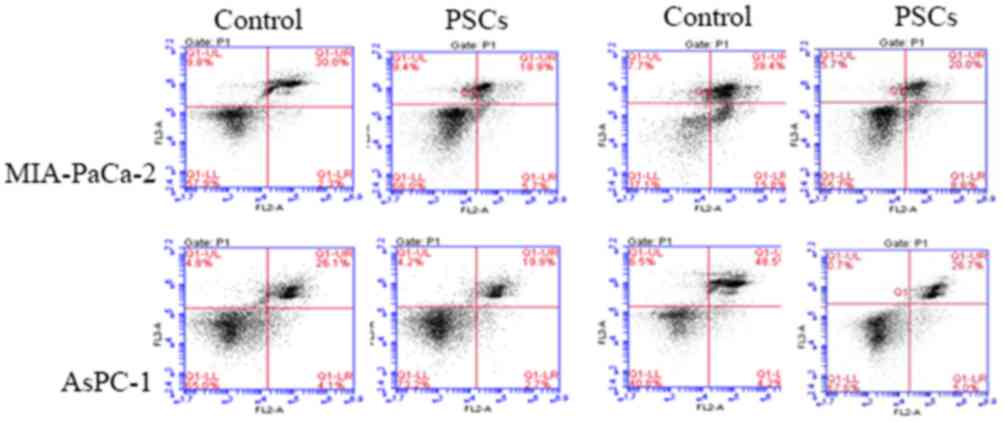
The percentage of apoptotic cells in the two groups
was increased with the extension of the intervention time, and the
percentage of apoptotic cells was significantly different
(P<0.05). The percentage of apoptotic cells for AsPC-1 in the
PSCs group was decreased compared with that in control group at 48
h subsequent to intervention (32.7±6.1% vs. 55.3±9.1%; P=0.027;
Fig. 3). The percentage of apoptotic
cells for MIA-PaCa-2 cells in PSCs group and in control group was
39.6±7.3% vs. 68.3±8.7% (P=0.013), a similar result being observed
for MIA-PaCa-2 cells.
In vivo experiments
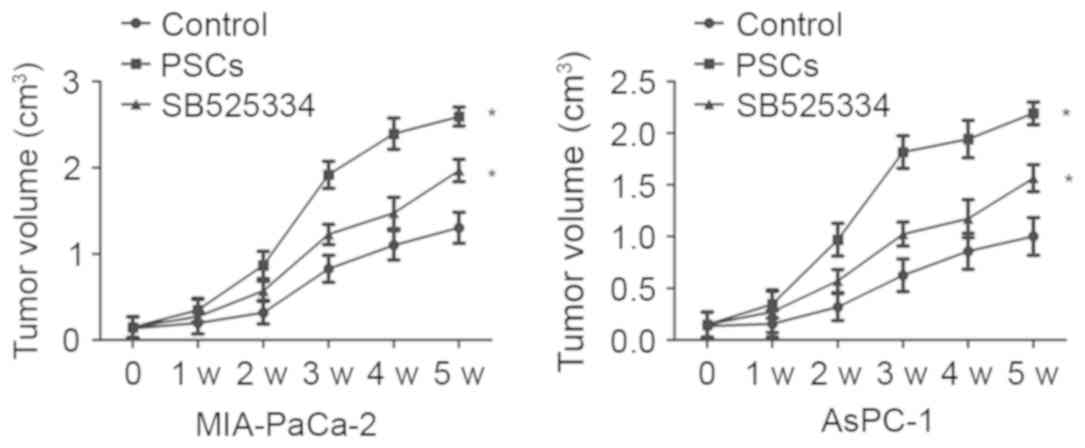
To evaluate the effects of PSCs on in vivo
tumor growth, MIA-PaCa-2 cells and PSCs or SB525334 were
co-transplanted into nude mice. The results demonstrated that PSCs
significantly enhanced the growth of MIA-PaCa-2 cells compared with
the control group (P=0.003). Mice bearing MIA-PaCa-2 cells and PSCs
exhibited an increase in the rate of tumor growth compared with
MIA-PaCA-2 cells alone, whereas SB525334 delayed the tumor
progression induced by PSCs. The tumor volumes in the control group
and co-transplantion group differed significantly at 3, 4 and 5
weeks subsequent to implantation (the P-values were 0.02, 0.013 and
0.007 respectively). In total, 5 weeks subsequent to implantation,
the mean tumor volume changed to 1,374.6±195.8 mm3 from
109.0±14.7 mm3 in the control group, compared with in
the mice with co-transplanted MIA-PaCa-2 cells and PSCs
(2,548.6±142.9 mm3) or with co-transplanted MIA-PaCa-2
cells and SB525334 (2,015.7±202.3 mm3; Fig. 4). Body weight was not significantly
different among the three groups.
Discussion
The incidence of pancreatic cancer is gradually
increasing and the mortality rate has not reduced significantly
(1). The pathogenesis of pancreatic
cancer has primarily focused on the molecular biology of the tumor
cells (15). Previously, it has been
reported that the initiation, growth and progression of cancer is
associated with intricate crosstalk between the tumor and stroma
(16). The interaction between
pancreatic cancer cells and the surrounding microenvironment, which
consists of ECM proteins, growth factors and constituent non-tumor
cells, remains largely ignored (17).
In 2004, PSCs were revealed to produce the ECM proteins and were
the principal source of collagen in the fibrotic matrix, which
comprised the pancreatic tumor stroma (18). Additionally, the presence of activated
PSCs in surrounding human pancreatic intraepithelial neoplastic
lesions (Pan-INs) demonstrated that they may function during the
early stages of cancer development (10). Therefore, the interaction between
pancreatic cancer cells and PSCs is receiving increasing
attention.
The present study isolated, identified and cultured
human PSCs. The role of PSCs in stimulating pancreatic cancer cell
migration, invasion and resistance to chemotherapy was determined.
The findings of the present study may be summarized as follows:
Activated PSCs are present in pancreatic cancer tissues; PSCs
promote the viability of pancreatic cancer cells; the viability
induced by PSCs may be blocked by SB525334, an inhibitor of TGF-β;
PSCs increase the invasive ability of pancreatic cancer cells; PSCs
decrease the degree of apoptosis induced by gemcitabine, indicating
that PSCs have an important role in the resistance of pancreatic
cancer cells to gemcitabine; co-injection of pancreatic cancer
cells with PSCs in an orthotopic model resulted in increased tumor
volume.
TGF-β1 is a pleiotropic cytokine that controls
cellular proliferation, differentiation, adhesion, migration,
apoptosis and the epithelial-mesenchymal transition (19). TGF-β1 also has a vital role in the
interaction between cellular and non-cellular components of the
tumor microenvironment (20). It has
previously been demonstrated that TGF-β1 promotes the activation
and proliferation of PSCs, as well as the epithelial-mesenchymal
transition of pancreatic cancer cells (21,22).
SB525334 is a selective inhibitor of TGF-β1 (23). In the present study, SB525334
partially blocked the increased proliferation and the invasive
ability of pancreatic cancer cells induced by PSCs. Additionally,
SB525334 reduced the resistance of pancreatic cancer cells to
gemcitabine caused by PSCs.
In the present study, the association between
pancreatic cancer cells and PSCs has been determined. However, the
mechanism by which PSCs regulate the proliferation and apoptosis of
pancreatic cancer cells remains unclear. In particular, signaling
pathways involved in genetic alterations during the process of PSC
activation must be characterized. The origin of activated PSCs
arising from the existing pool of quiescent PSCs or from
mesenchymal stem cells remains controversial (24,25). An
improved understanding of the pathophysiology of pancreatic cancer
is possible following the resolution of current challenges in the
field. PSCs are a potential novel therapeutic target, which may
improve the outcome of pancreatic cancer.
Acknowledgements
Not applicable.
Funding
The present study was supported by the National
Natural Science Foundation of China (grant nos. 81802888; and
81572314) and the Key Research and Development Project of Shandong
Province (grant no. 2018GSF118088).
Availability of data and materials
The datasets used and analyzed for the present study
are available from the corresponding author upon reasonable
request.
Authors' contributions
SL, YL and YZ designed the experiments, contributed
to the analysis and interpretation of data, and wrote the initial
draft of the manuscript. SC and BS performed the experiments. DC
and DW revised the paper, assisted with the experiments and
supervised the experimental work. All authors approved the final
manuscript.
Ethics approval and consent to
participate
Tissue samples were collected once ethical approval
was obtained from the Ethics Committee of the Affiliated Hospital
of Qingdao University. In all cases written informed consent was
obtained.
Patient consent for publication
Not applicable.
Competing interests
The authors declare that they have no competing
interests.
References
|
1
|
Siegel RL, Miller KD and Jemal A: Cancer
Statistics, 2017. CA Cancer J Clin. 67:7–30. 2017. View Article : Google Scholar : PubMed/NCBI
|
|
2
|
Dai MH, Liu SL, Chen NG, Zhang TP, You L,
Q Zhang F, Chou TC, Szalay AA, Fong Y and Zhao YP: Oncolytic
vaccinia virus in combination with radiation shows synergistic
antitumor efficacy in pancreatic cancer. Cancer Lett. 344:282–290.
2014. View Article : Google Scholar : PubMed/NCBI
|
|
3
|
Hidalgo M: Pancreatic cancer. N Engl J
Med. 362:1605–1617. 2010. View Article : Google Scholar : PubMed/NCBI
|
|
4
|
Li X, Ma Q, Xu Q, Duan W, Lei J and Wu E:
Targeting the cancer-stroma interaction: A potential approach for
pancreatic cancer treatment. Curr Pharm Des. 18:2404–2415. 2012.
View Article : Google Scholar : PubMed/NCBI
|
|
5
|
Vonlaufen A, Phillips PA, Xu Z, Goldstein
D, Pirola RC, Wilson JS and Apte MV: Pancreatic stellate cells and
pancreatic cancer cells: An unholy alliance. Cancer Res.
68:7707–7710. 2008. View Article : Google Scholar : PubMed/NCBI
|
|
6
|
McCarroll JA, Naim S, Sharbeen G, Russia
N, Lee J, Kavallaris M, Goldstein D and Phillips PA: Role of
pancreatic stellate cells in chemoresistance in pancreatic cancer.
Front Physiol. 5:1412104.
|
|
7
|
Hata T, Kawamoto K, Eguchi H, Kamada Y,
Takamatsu S, Maekawa T, Nagaoka S, Yamada D, Iwagami Y, Asaoka T,
et al: Fatty acid-mediated stromal reprogramming of pancreatic
stellate cells induces inflammation and fibrosis that fuels
pancreatic cancer. Pancreas. 46:1259–1266. 2017. View Article : Google Scholar : PubMed/NCBI
|
|
8
|
Pang TCY, Wilson JS and Apte MV:
Pancreatic stellate cells: What's new? Curr Opin Gastroenterol.
33:366–373. 2017. View Article : Google Scholar : PubMed/NCBI
|
|
9
|
Apte MV and Wilson JS: Dangerous liaisons:
Pancreatic stellate cells and pancreatic cancer cells. J
Gastroenterol Hepatol. 27 Suppl 2:S69–S74. 2012. View Article : Google Scholar
|
|
10
|
Apte MV, Wilson JS, Lugea A and Pandol SJ:
A starring role for stellate cells in the pancreatic cancer
microenvironment. Gastroenterology. 144:1210–1219. 2013. View Article : Google Scholar : PubMed/NCBI
|
|
11
|
Masamune A and Shimosegawa T: Signal
transduction in pancreatic stellate cells. J Gastroenterol.
44:249–260. 2009. View Article : Google Scholar : PubMed/NCBI
|
|
12
|
Omary MB, Lugea A, Lowe AW and Pandol SJ:
The pancreatic stellate cell: A star on the rise in pancreatic
diseases. J Clin Invest. 117:150–159. 2007. View Article : Google Scholar
|
|
13
|
Masamune A, Watanabe T, Kikuta K and
Shimosegawa T: Roles of pancreatic stellate cells in pancreatic
inflammation and fibrosis. Clin Gastroenterol Hepatol. 7:(11
Suppl). S48–S54. 2009. View Article : Google Scholar : PubMed/NCBI
|
|
14
|
Masamune A, Kikuta K, Watanabe T, Satoh K,
Hirota M, Hamada S and Shimosegawa T: Fibrinogen induces cytokine
and collagen production in pancreatic stellate cells. Gut.
58:550–559. 2009. View Article : Google Scholar : PubMed/NCBI
|
|
15
|
Ohnishi H, Miyata T, Yasuda H, Satoh Y,
Hanatsuka K, Kita H, Ohashi A, Tamada K, Makita N, Iiri T, et al:
Distinct roles of Smad2-, Smad3-, and ERK-dependent pathways in
transforming growth factor-beta1 regulation of pancreatic stellate
cellular functions. J Biol Chem. 279:8873–8878. 2004. View Article : Google Scholar : PubMed/NCBI
|
|
16
|
Mazzocca A, Fransvea E, Dituri F, Lupo L,
Antonaci S and Giannelli G: Down-regulation of connective tissue
growth factor by inhibition of transforming growth factor beta
blocks the tumor-stroma cross-talk and tumor progression in
hepatocellular carcinoma. Hepatology. 51:523–534. 2010. View Article : Google Scholar : PubMed/NCBI
|
|
17
|
Dunér S, Lopatko Lindman J, Ansari D,
Gundewar C and Andersson R: Pancreatic cancer: The role of
pancreatic stellate cells in tumor progression. Pancreatology.
10:673–681. 2010. View Article : Google Scholar : PubMed/NCBI
|
|
18
|
Apte MV, Park S, Phillips PA, Santucci N,
Goldstein D, Kumar RK, Ramm GA, Buchler M, Friess H, McCarroll JA,
et al: Desmoplastic reaction in pancreatic cancer: Role of
pancreatic stellate cells. Pancreas. 29:179–187. 2004. View Article : Google Scholar : PubMed/NCBI
|
|
19
|
Gupta DK, Singh N and Sahu DK: TGF-β
mediated crosstalk between malignant hepatocyte and tumor
microenvironment in hepatocellular carcinoma. Cancer Growth
Metastasis. 7:1–8. 2014. View Article : Google Scholar : PubMed/NCBI
|
|
20
|
Liu FL, Mo EP, Yang L, Du J, Wang HS,
Zhang H, Kurihara H, Xu J and Cai SH: Autophagy is involved in
TGF-β1-induced protective mechanisms and formation of
cancer-associated fibroblasts phenotype in tumor microenvironment.
Oncotarget. 7:4122–4141. 2016.PubMed/NCBI
|
|
21
|
Gao X, Cao Y, Yang W, Duan C, Aronson JF,
Rastellini C, Chao C, Hellmich MR and Ko TC: BMP2 inhibits
TGF-β-induced pancreatic stellate cell activation and extracellular
matrix formation. Am J Physiol Gastrointest Liver Physiol.
304:G804–G813. 2013. View Article : Google Scholar : PubMed/NCBI
|
|
22
|
Kikuta K, Masamune A, Watanabe T, Ariga H,
Itoh H, Hamada S, Satoh K, Egawa S, Unno M and Shimosegawa T:
Pancreatic stellate cells promote epithelial-mesenchymal transition
in pancreatic cancer cells. Biochem Biophys Res Commun.
403:380–384. 2010. View Article : Google Scholar : PubMed/NCBI
|
|
23
|
Guan S, Xu W, Han F, Gu W, Song L, Ye W,
Liu Q and Guo X: Ginsenoside Rg1 attenuates cigarette smoke-induced
pulmonary epithelial-mesenchymal transition via inhibition of the
TGF-β1/Smad pathway. Biomed Res Int. 2017:71714042017. View Article : Google Scholar : PubMed/NCBI
|
|
24
|
Tian L, Lu Z and Miao Y: Primary cultures
for pancreatic stellate cells (PSCs). Methods Mol Biol.
1882:149–155. 2019. View Article : Google Scholar : PubMed/NCBI
|
|
25
|
Kawakubo K, Ohnishi S, Fujita H, Kuwatani
M, Onishi R, Masamune A, Takeda H and Sakamoto N: Effect of fetal
membrane-derived mesenchymal stem cell transplantation in rats with
acute and chronic pancreatitis. Pancreas. 45:707–713. 2016.
View Article : Google Scholar : PubMed/NCBI
|