Introduction
Subtotal resection (STR) of the highly aggressive
primary brain tumor glioblastoma multiforme (GBM) has been shown to
significantly decrease the progression-free (PFS) and overall
survival (OS) compared to gross total resection (GTR) (1). Various GBM trials have confirmed that
an extent of resection (EOR) of 78% improves patients' outcome
(2). Survival rates further
increased when EOR rates of 96–100% can be achieved. This is true
not only for newly diagnosed GBM but also for recurrent GBM
(3,4). In the latter, a cutoff of 80% EOR
improved patients' outcome in the second line setting. However,
even after repeated multimodal treatment, median survival is
limited to approximately 20 months, which emphasizes the need for
new treatment options (5).
Tumor Treating Fields (TTFields) are a local,
non-invasive modality adjunct to first or second line therapy,
which are delivered through transducer arrays placed on the shaved
scalp and generated by a portable device. TTFields are alternating
electric fields of intermediate frequency (100–300 kHz, 200 kHz for
GBM) and low intensity (1–3 V/cm), which interfere with processes
of mitosis to stop or slow down cell division and eventually induce
cell death (6). The phase III trial
EF-14 demonstrated that adding TTFields to standard chemotherapy
significantly improved PFS and OS in patients with newly diagnosed
GBM by 2.7 and 4.9 months, respectively (7). The compliance of the therapy is of
importance as a post-hoc analysis of the EF-14 study revealed that
higher compliance was associated with longer PFS and OS (8). The OS benefit of TTFields was
independent of gender, O-6-methylguanine-DNA methyltransferase
(MGMT) methylation status, age, region, performance status (KPS)
and EOR (8) defined by MRI criteria
as well as tumor progression.
Although complete radiological response (CR) was
seen occasionally in the subgroup analysis of the EF-14 trial, no
details, however, have been reported in literature about the
clinical course of patients with residual tumors under TTFields
treatment.
We report on three patients who showed complete
radiologic response after subtotal resection of GBM under
multimodal treatment including TTFields.
Case report
GBM patient characteristics following
STR treatment in 2015 and 2016
Between 2015 and 2016, 27 patients received STR at
our institution. Of the 27 STR-patients, 4 were treated with
TTFields in addition to chemotherapy. Here, STR was defined as any
residual contrast enhancing lesion. Three out of those 4 patients
(75%; 3/4) displayed a CR, defined as no detectable contrast
enhancement in the follow up after initial STR, while one patient
remained radiologically stable for over 10 months before
progression, which was treated by re-irradiation. Seventeen of the
23 patients without TTFields treatment developed early recurrence
within 2 to 4 months while being on first-line standard therapy.
Two patients were lost to follow up. One patient stayed
radiologically stable for 8 months but then suffered from recurrent
seizures, accompanied by a declining general condition and died
after a short time in palliative care. One patient has remained
stable for 10 months to-date. Only two of 23 patients who had not
received TTFields had a CR in contrast enhancement after 6 and 15
months (8.7%; 2/23).
All tumors were histologically assessed and graded
on formaline fixed and paraffin embedded tissue sections by an
experienced neuropathologist according to the 2016 criteria of the
World Health Organisation. The IDH status was examined by
immunohistochemistry using the antibody against IDH1 R132H and
completed by a sequence analysis of IDH1 and IDH2 gene.
For determination of extent of resection, tumor
progression as well as radiological responses to therapies RANO
criteria were applied (9), which
include diverse MRI criteria and clinical data as well. Observation
period was closed in March 2018.
This study was carried out in accordance with the
recommendations of the Declaration of Helsinky, in accordance with
which all three presented subjects gave written informed consent
for their data to be published.
Clinical course of patient one
Patient one (female, 54 years, KPS 80%) presented
with recurrent speech impairment. A CT scan revealed a left
frontotemporal lesion with perifocal edema. MRI revealed an
irregular contrast enhancing tumor highly susceptible for GBM,
located in the frontal operculum and in close contact to the
caudate nucleus and anterior crus of the internal capsule with
moderate compression of the lateral ventricle and midline shift.
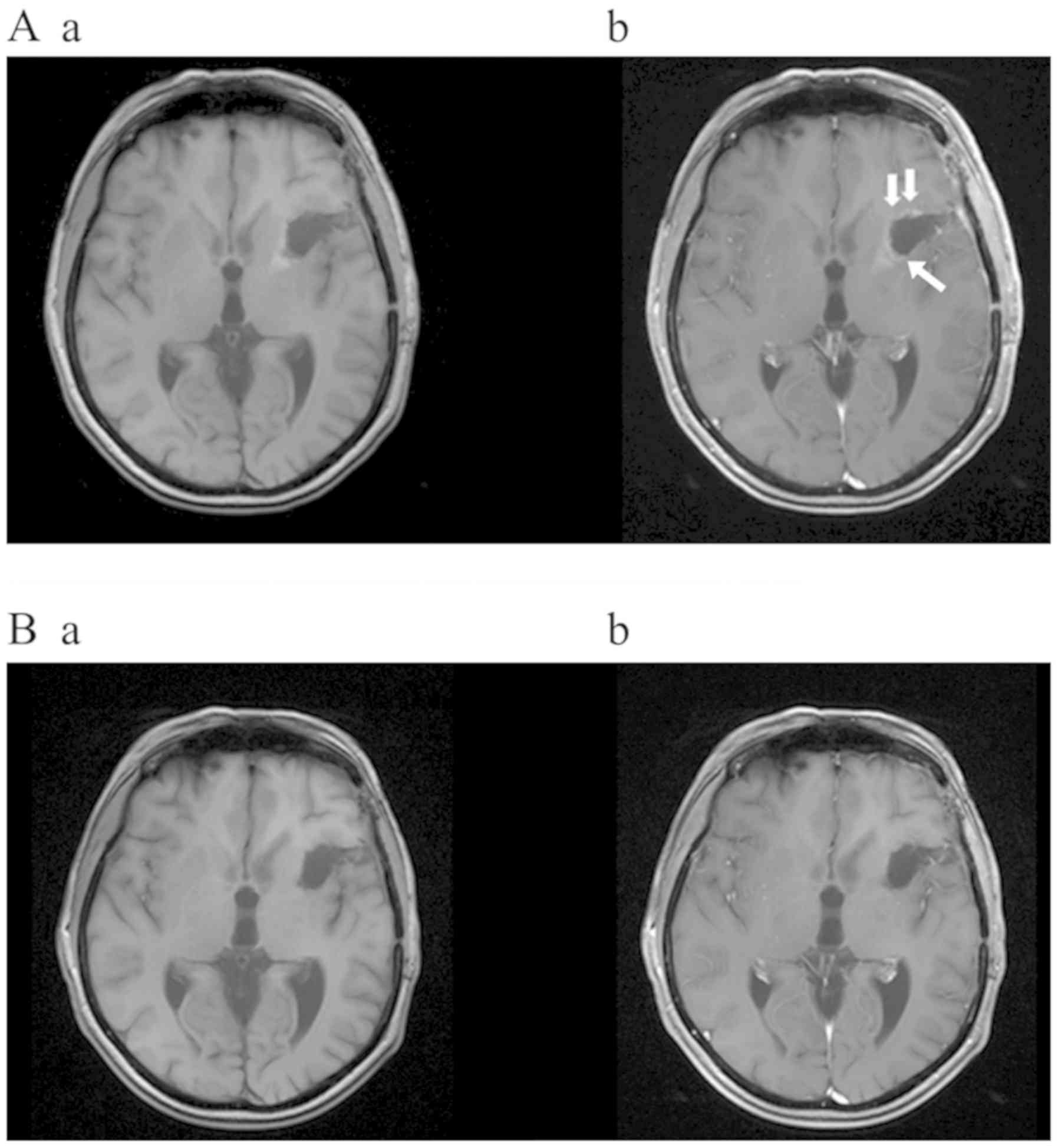
After 5-ALA- and ultrasound-guided resection, the early
postoperative MRI showed remaining tumor tissue in the rostral and
dorsolateral marginal zones of the resection cavity, confirming a
STR (Fig. 1A). Apart from a slight
dysphasia, no neurological abnormalities were recorded after
surgery. The histological diagnosis confirmed GBM WHO Grade IV,
with methylated MGMT promoter, IDH1/2 wild-type and sustained
nuclear expression of ATRX. Concomitant radiochemotherapy was
administered (53.4 Gy/Temozolomide (TMZ) with 75 mg/m2
daily). A follow-up MRI at 3 months postoperatively and at 2 weeks
after radiation termination showed a new contrast enhancement at
the rostral margin of the left ventricle in an area initially
suspected as non-contrast enhancing tumor. This new contrast
enhancement was interpreted as pseudoprogression, while the
postoperative residual tumor was defined as stable. The adjuvant
chemotherapy with TMZ according to the Stupp protocol (10) was initiated 4 weeks after termination
of radiochemotherapy. Application of TTFields was started at the
same time. The patient was in a good general condition during the
first cycle of TMZ, but suffered from persisting speech impairment.
Due to leukocytopenia, the third cycle of TMZ was delayed for a
month while TTFields therapy was applied continuously. Speech
impairment improved, and the next follow-up MRI 4 months after
surgery indicated reduced contrast enhancement of the
pseudoprogression as well as the residual tumor. After termination
of 6 cycles of TMZ, the patient continued with TTFields treatment
at a median compliance rate of 92% [range: 88–96%]. The MRI at five
months after TTFields start did not show any contrast enhancement
indicating a CR according to the RANO criteria (9) in both regions, residual tumor and
pseudoprogression as well. The patient's status remained stable for
7 months (Fig. 1B) before multifocal
tumor recurrence occurred. Since resection was not feasible, the
patient was treated with re-irradiation and further 6 cycles of
TMZ. TTFields was discontinued due to patient's decision at 12
months after initiation for 23 days. Afterwards, the patient
resumed TTFields treatment, which is still ongoing for 24 months in
total. The patient presents a mild decline of neurological
functions due to slow but ongoing tumor growth.
Clinical course of patient two
Patient two (female, 46 years, KPS 90%) displayed a
right-sided hemiparesis. Her MRI revealed a left parietal lesion
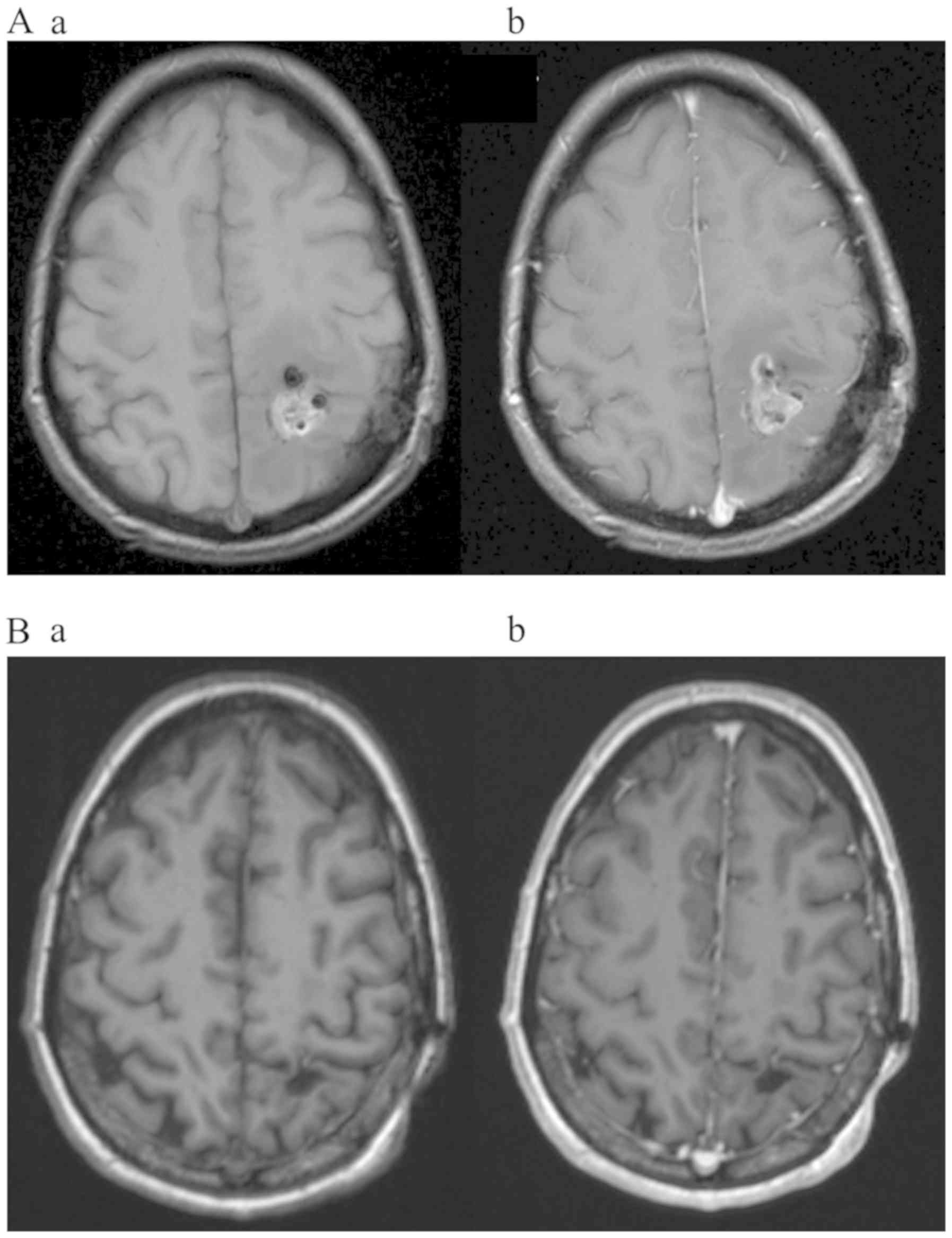
infiltrating the post-central gyrus. After STR contrast enhancement
was still discernible at the resection margins 24 h after surgery
(Fig. 2A). Histopathology confirmed
GBM (methylated MGMT promoter, IDH1/2 WT, sustained nuclear
expression of ATRX). Postoperative irradiation up to 61.2 Gy
administered with concomitant daily TMZ (75 mg/m2) was
well tolerated. Six cycles of adjuvant TMZ therapy were
administered concomitantly with TTFields, which were applied for 14
months at compliance rate of above 90%. Four months after
initiating TMZ + TTFields, MRI revealed a CR of the residual tumor
(Fig. 2B). After a follow-up period
of 16 months, MRI did not show any signs of tumor recurrence.
Clinical course of patient three
Patient three (male, 44 years, KPS 100%) presented
with seizures. The MRI showed a right frontal lesion involving
parts of the corpus callosum. The FET-PET scan revealed a maximal
tumor-to-background ratio (TBR) in the right anterior middle
frontal gyrus. Early postoperative MRI showed residual tumor tissue
at the margins of the resection cavity. Histopathology confirmed
anaplastic astrocytoma WHO grade III. Subsequent irradiation
therapy was administered up to 61.2 Gy with concomitant daily TMZ
(75 mg/m2). After 4 cycles of adjuvant TMZ, a follow-up
MRI revealed a progression of the contrast enhancing lesion at the
inferior margin of the resection cavity and the corpus callosum,
which was identified as a true tumor recurrence by a FET-PET scan.
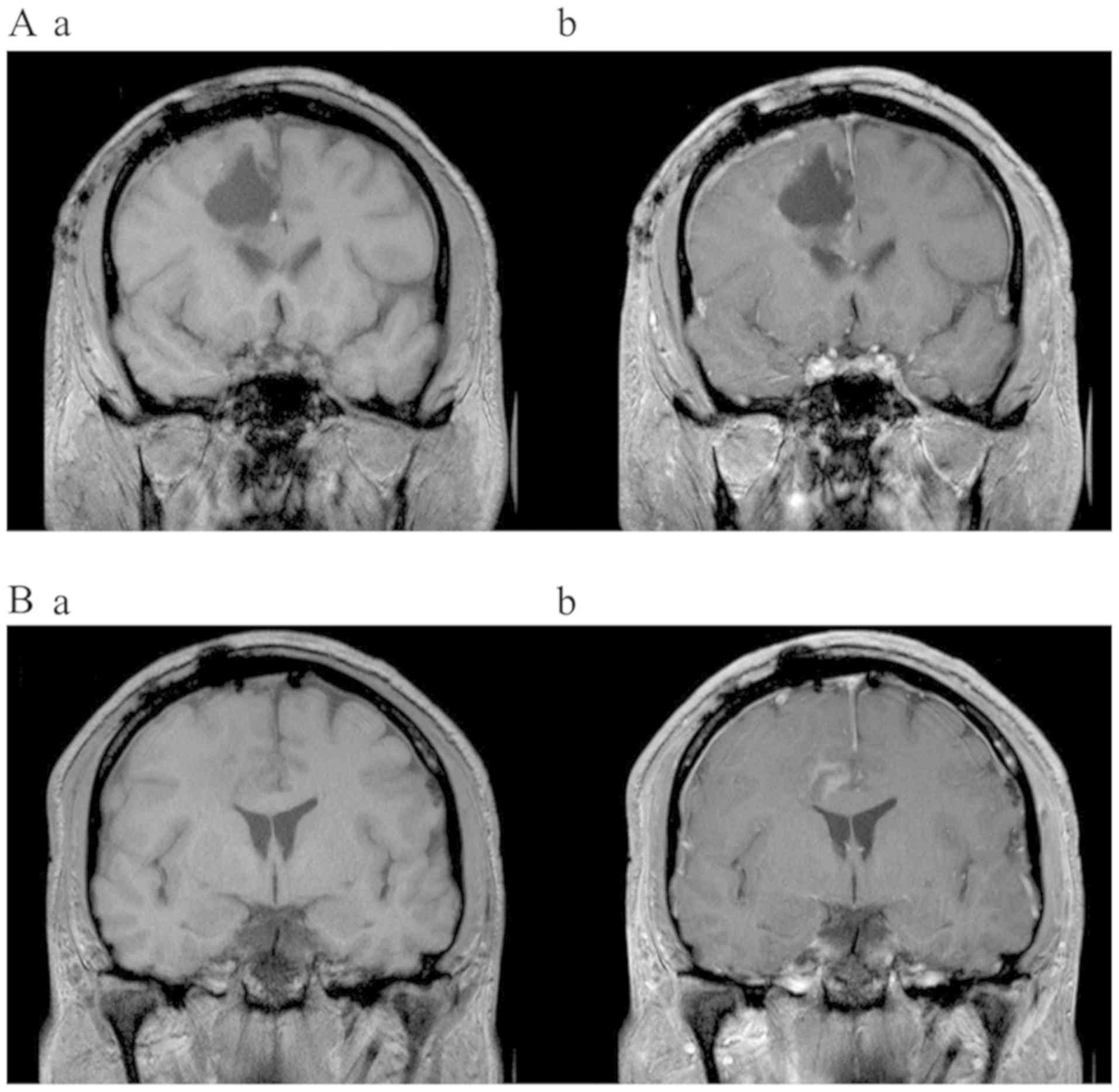
After repeated surgery, the early postoperative MRI presented a
contrast enhancing tumor residue at the inferior margin of the
resection cavity (Fig. 3A),
extending into the genu of the corpus callosum (Fig. 3B) due to the subtotal resection.
Histopathological workup revealed GBM WHO grade IV (methylated MGMT
promoter, IDH1 R132H mutation). Due to the presence of methylated
MGMT-promoter, TMZ therapy was resumed for another 6 cycles. In
addition, TTFields treatment was initiated at cycle 4. During the
first period of the TTFields treatment, the patient started at a
compliance rate of ~75%. Interestingly, 6 months after surgery, the
cranial MRI displayed a distinct regression of the contrast
enhancement in the corpus callosum. Another 3 months later, no
contrast enhancing tumor residues were discernible, which continued
for 40 months after the second resection and until the end of the
follow-up period (Fig. 3C and
3D). Simultaneously, the patient
reported a high quality of life (QoL) and active participation in
his Martial Arts training sessions as well as travel activities to
foreign countries. Although suffering from psoriasis of the arms,
legs and scalp, being treated with urea-based lotion and
intermittendly with cortisol-based lotion, there were no adverse
events besides mild skin irritation, no seizures or neurological
abnormalities. The patient is working full-time and is permanently
using the TTFields therapy with an average compliance of around 60%
before terminating TTFields application after 37 and 40 months
after STR up to the end of observation period.
Discussion
We present a series of three GBM patients presenting
CR after STR according to the RANO criteria. All of these patients
received adjuvant first line radio-chemotherapy and additional
TTFields treatment. From 2015 to 2016, a total of 27 GBM patients
underwent STR in our hospital. Four GBM patients received STR and
were treated with TTFields. CRs were observed in three of these
four subtotal resected GBM patients. Only 2 out of 23 GBM patients
(8.7%) being treated solely with standard radiochemotherapy after
STR showed complete radiologic responses. This suggests a better
radiologic response after STR by the addition of TTFields
therapy.
The presented patients tolerated the TTFields
treatment well for an average of 25 months and reported a good QoL.
This is in line with the recently published QoL data from the EF-14
study that showed that health-related QoL during TTFields treatment
was not impaired compared to the trial's control arm in all
prespecified parameters, except for the complaint of itchy skin
(11). Applicability, tolerability
and safety have already been shown in several previous studies
(6,7,12,13). In
fact, patient 3 is still actively working in his job as a computer
scientist, more than three years after the first diagnosis of an
anaplastic astrocytoma. All patients participate regularly in
recreational activities. The two female patients reached an average
compliance rate above 90% during the entire treatment period. High
compliance has been associated with better OS and PFS outcomes and
may have contributed to their individual outcome (8). However, even compliance above a
threshold of 50–60% revealed significantly improved overall
survival compared to the control group in a subgroup analysis of
the EF-14 trial (8). Better
compliance rates resulted in a further significant OS increase.
Even though patient 3 has a very active lifestyle, he tolerated
TTFields well enough to reach a compliance of over 60% throughout a
3-year treatment period.
This is even more remarkable as this patient has
been suffering from Psoriasis, which bears the risk of more severe
skin reactions and infections induced by minor skin injury or
irritations, the latter being one major side effect of TTFields.
Prescribing this patient a skin irritating therapy was a matter of
concern in his particular situation. This case shows that this
patient with a skin disorder may well tolerate TTFields treatment
with a good quality of life and no severe skin reactions to the
therapy.
Furthermore, psoriasis, as seen in the third
patient, might additionally be a prognosis-limiting factor. Some
evidence indicates that there may be a negative association between
brain tumors and psoriasis as well as other autoimmune diseases as
chronic rheumatic heart disease, multiple sclerosis, and rheumatoid
arthritis (14,15). Although the third patient accumulated
several positive prognostic factors as his high KPS of 100%,
methylated MGMT, mutated IDH1 and young age (44 years), the fast
progression to a secondary GBM under ongoing TMZ therapy might have
resulted from the confirmed psoriasis in combination with a STR
(16,17). But despite of the clinical course and
the potentially negative prognostic factors, the patient presented
a CR after the second STR which has previously been shown to reduce
PFS and OS even in relapsing GBM (18). The second STR was followed by TMZ
again, but this time accompanied by TTFields, suggesting that
TTFields may have decisively contributed to this favorable clinical
and radiological course.
The CRs of all three patients were seen after 4, 5
and 7 months, which is in line with the observation of a median 5.2
months in the responder patients in the EF-11 trial (19). All three patients had a complete
response and are still alive in spite of their poor prognosis
especially due to the extent of resection, but also their
comorbidity and molecular profiles (20–22).
The observations of this report are supported by the
subgroup analysis of the EF-14 trial. It demonstrated that the
subgroup undergoing STR compared to GTR showed similar OS response
when TTFields were added to their treatment regimen. OS in both
groups exceeded 21 months from randomization (+4.1 months for GTR
patients vs. +6.3 months for STR patients, HR: 0.7 vs. 0.56,
respectively) (7).
In conclusion, adding TTFields to adjuvant
chemotherapy is a valuable treatment option to improve clinical and
radiological outcome after STR in both newly diagnosed and
recurrent GBM. There are limitations due to the small sample size
and the homogenous molecular-pathological profile. Therefore, these
data should be further investigated. However, these observations in
individual cases in clinical practice support the findings of the
clinical trial EF-14. Thus, TTFields therapy can be recommended to
all eligible GBM patients.
Acknowledgements
The authors would like to thank Miss Sandra
Grebsattel (Department of Neurosurgery, Würzburg University
Hospital) for her assistance with patient documentation.
Funding
The current study was funded by the German Research
Foundation (DFG) and the University of Wuerzburg in the funding
program Open Access Publishing.
Availability of data and materials
The datasets used and/or analyzed are available from
the corresponding author on reasonable request.
Authors' contributions
MB, TL, JW and WW reviewed patient clinical history,
reviewed the literature and prepared the manuscript. CH and RIE
reviewed the literature and revised the manuscript. CH contributed
to conception and design of the study. RIE gave advice for data
interpretation. AFK and CMM reviewed patient pathology and the
manuscript. TW and ML reviewed the manuscript and MRI scans. AFK
identified the patient, reviewed patient clinical history,
performed a literature search, and prepared and edited the
manuscript. All authors read and approved the final manuscript.
Ethics approval and consent to
participate
Written informed consent was obtained from all
patients prior to publication.
Patient consent for publication
Patients provided written consent for the
publication of their images and associated data.
Competing interests
Congress participation of the authors AFK and CH was
partially funded by Novocure GmbH. All other authors declare that
they have no competing interests.
Glossary
Abbreviations
Abbreviations:
|
EOR
|
extent of resection
|
|
GBM
|
glioblastoma multiforme
|
|
GTR
|
gross total resection
|
|
IDH
|
isocitrate dehydrogenase
|
|
KPS
|
Karnofsky performance score
|
|
MGMT
|
O6-methylguanine-DNA
methyltransferase
|
|
OS
|
overall survival
|
|
PFS
|
progression-free survival
|
|
QoL
|
quality of life
|
|
STR
|
subtotal resection
|
|
TMZ
|
Temozolomide
|
|
TTFields
|
Tumor Treating Fields
|
|
WT
|
wild-type
|
References
|
1
|
Kreth FW, Thon N, Simon M, Westphal M,
Schackert G, Nikkhah G, Hentschel B, Reifenberger G, Pietsch T,
Weller M, et al: Gross total but not incomplete resection of
glioblastoma prolongs survival in the era of radiochemotherapy. Ann
Oncol. 24:3117–3123. 2013. View Article : Google Scholar : PubMed/NCBI
|
|
2
|
Sanai N, Polley MY, McDermott MW, Parsa AT
and Berger MS: An extent of resection threshold for newly diagnosed
glioblastoma. J Neurosurg. 115:3–8. 2011. View Article : Google Scholar : PubMed/NCBI
|
|
3
|
Lacroix M, Abi-Said D, Fourney DR,
Gokaslan ZL, Shi W, DeMonte F, Lang FF, McCutcheon IE, Hassenbusch
SJ, Holland E, et al: A multivariate analysis of 416 patients with
glioblastoma multiforme: Prognosis, extent of resection, and
survival. J Neurosurg. 95:190–198. 2001. View Article : Google Scholar : PubMed/NCBI
|
|
4
|
Tsitlakidis A, Foroglou N, Venetis CA,
Patsalas I, Hatzisotiriou A and Selviaridis P: Biopsy versus
resection in the management of malignant gliomas: A systematic
review and meta-analysis. J Neurosurg. 112:1020–1032. 2010.
View Article : Google Scholar : PubMed/NCBI
|
|
5
|
Oppenlander ME, Wolf AB, Snyder LA, Bina
R, Wilson JR, Coons SW, Ashby LS, Brachman D, Nakaji P, Porter RW,
et al: An extent of resection threshold for recurrent glioblastoma
and its risk for neurological morbidity. J Neurosurg. 120:846–853.
2014. View Article : Google Scholar : PubMed/NCBI
|
|
6
|
Kirson ED, Dbalý V, Tovarys F, Vymazal J,
Soustiel JF, Itzhaki A, Mordechovich D, Steinberg-Shapira S,
Gurvich Z, Schneidermann R, et al: Alternating electric fields
arrest cell proliferation in animal tumor models and human brain
tumors. Proc Natl Acad Sci USA. 104:10152–10157. 2007. View Article : Google Scholar : PubMed/NCBI
|
|
7
|
Stupp R, Taillibert S, Kanner A, Read W,
Steinberg D, Lhermitte B, Toms S, Idbaih A, Ahluwalia MS, Fink K,
et al: Effect of tumor-treating fields plus maintenance
temozolomide vs. maintenance temozolomide alone on survival in
patients with glioblastoma: A Randomized Clinical Trial. JAMA.
318:2306–2316. 2017. View Article : Google Scholar : PubMed/NCBI
|
|
8
|
Ram Z, Kim CY, Nicholas G and Toms S:
Compliance and treatment duration predict survival in a phase EF-14
trial of tumor treating fields with temozolomide in patients with
newly diagnosed glioblastoma. Neuro Oncol. 19 (Suppl 6):(6): pp.
vi6–vi7. 2017, https://doi.org/10.1093/neuonc/nox168.022
View Article : Google Scholar
|
|
9
|
Wen PY, Macdonald DR, Reardon DA,
Cloughesy TF, Sorensen AG, Galanis E, Degroot J, Wick W, Gilbert
MR, Lassman AB, et al: Updated response assessment criteria for
high-grade gliomas: Response assessment in neuro-oncology working
group. J Clin Oncol. 28:1963–1972. 2010. View Article : Google Scholar : PubMed/NCBI
|
|
10
|
Stupp R, Mason WP, van den Bent MJ, Weller
M, Fisher B, Taphoorn MJ, Belanger K, Brandes AA, Marosi C, Bogdahn
U, et al: Radiotherapy plus concomitant and adjuvant temozolomide
for glioblastoma. N Engl J Med. 352:987–996. 2005. View Article : Google Scholar : PubMed/NCBI
|
|
11
|
Taphoorn MJB, Dirven L, Kanner AA,
Lavy-Shahaf G, Weinberg U, Taillibert S, Toms SA, Honnorat J, Chen
TC, Sroubek J, et al: Influence of treatment with tumor-treating
fields on health-related quality of life of patients with newly
diagnosed glioblastoma: A secondary analysis of a randomized
clinical trial. JAMA Oncol. 4:495–504. 2018. View Article : Google Scholar : PubMed/NCBI
|
|
12
|
Stupp R, Wong ET, Kanner AA, Steinberg D,
Engelhard H, Heidecke V, Kirson ED, Taillibert S, Liebermann F,
Dbalý V, et al: NovoTTF-100A versus physician's choice chemotherapy
in recurrent glioblastoma: A randomised phase III trial of a novel
treatment modality. Eur J Cancer. 48:2192–2202. 2012. View Article : Google Scholar : PubMed/NCBI
|
|
13
|
Onken J, Staub-Bartelt F, Vajkoczy P and
Misch M: Acceptance and compliance of TTFields treatment among high
grade glioma patients. J Neurooncol. 139:177–184. 2018. View Article : Google Scholar : PubMed/NCBI
|
|
14
|
Hemminki K, Liu X, Försti A, Ji J,
Sundquist J and Sundquist K: Subsequent brain tumors in patients
with autoimmune disease. Neuro Oncol. 15:1142–1150. 2013.
View Article : Google Scholar : PubMed/NCBI
|
|
15
|
Ji J, Shu X, Sundquist K, Sundquist J and
Hemminki K: Cancer risk in hospitalised psoriasis patients: A
follow-up study in Sweden. Br J Cancer. 100:1499–1502. 2009.
View Article : Google Scholar : PubMed/NCBI
|
|
16
|
Wang Y, Li S, Zhang Z, Chen X, You G, Yang
P, Yan W, Bao ZS, Yao K, Wang L, et al: Surgical extent impacts the
value of the established prognosticators in glioblastoma patients:
A prospective translational study in Asia. Head Neck Oncol.
4:802012.
|
|
17
|
Beiko J, Suki D, Hess KR, Fox BD, Cheung
V, Cabral M, Shonka N, Gilbert MR, Sawaya R, Prabhu SS, et al: IDH1
mutant malignant astrocytomas are more amenable to surgical
resection and have a survival benefit associated with maximal
surgical resection. Neuro Oncol. 16:81–91. 2014. View Article : Google Scholar : PubMed/NCBI
|
|
18
|
Bloch O, Han SJ, Cha S, Sun MZ, Aghi MK,
McDermott MW, Berger MS and Parsa AT: Impact of extent of resection
for recurrent glioblastoma on overall survival clinical article. J
Neurosurg. 117:1032–1038. 2012. View Article : Google Scholar : PubMed/NCBI
|
|
19
|
Vymazal J and Wong ET: Response patterns
of recurrent glioblastomas treated with tumor-treating fields.
Semin Oncol. 41 (Suppl 6):S14–S24. 2014. View Article : Google Scholar : PubMed/NCBI
|
|
20
|
Combs SE, Rieken S, Wick W, Abdollahi A,
von Deimling A, Debus J and Hartmann C: Prognostic significance of
IDH-1 and MGMT in patients with glioblastoma: One step forward, and
one step back? Radiat Oncol. 6:1152011. View Article : Google Scholar : PubMed/NCBI
|
|
21
|
Millward CP, Brodbelt AR, Haylock B,
Zakaria R, Baborie A, Crooks D, Husband D, Shenoy A, Wong H and
Jenkinson MD: The impact of MGMT methylation and IDH-1 mutation on
long-term outcome for glioblastoma treated with chemoradiotherapy.
Acta Neurochir (Wien). 158:1943–1953. 2016. View Article : Google Scholar : PubMed/NCBI
|
|
22
|
Yang P, Zhang W, Wang Y, Peng X, Chen B,
Qiu X, Li G, Li S, Wu C, Yao K, et al: IDH mutation and MGMT
promoter methylation in glioblastoma: Results of a prospective
registry. Oncotarget. 6:40896–40906. 2015. View Article : Google Scholar : PubMed/NCBI
|