Introduction
Nasopharyngeal carcinoma (NPC) is a head and neck
cancer with low survival rate and a fairly high incidence in its
endemic region (1). The reported
incidence of NPC in China is relatively higher than that in other
parts of the world, with an incidence of 3.26/100,000. The
incidence of NPC in males is 4.51/100,000, which is 2.32 times
higher than that in females, and the mortality rate in China is
1.77/100,000 (2,3). The incidence of NPC in China is also
regional; the incidence of NPC in the southern region is as high as
50/100,000 (4). At present, the main
treatment for NPC is radiotherapy, chemotherapy, and their
combination. However, the survival rate after treatment tends to
decrease with the development of the disease. The 10-year overall
survival rates for stages I, II, III and IV are 100, 87.1, 75.5 and
55.6%, respectively (5,6). The main causes of poor prognosis in NPC
patients are local treatment failure and distant metastasis
(7). Therefore, finding prognostic
factors for NPC is more conducive compared to timely optimal
treatment in improving the disease outcome.
MicroRNA, a small single stranded RNA molecule, has
been widely studied. Some microRNAs have been found to be related
to the development and disease in the process of life (8). The effect of microRNAs on NPC has also
been studied. Cheng et al (9)
have shown that the low expression of miR-122 can inhibit the
proliferation of NPC cells and promote their apoptosis. Chen et
al (10) have shown that
miR-203a-3p inhibits the growth and metastasis of NPC tumors. In
recent years, studies on miR-34a have been reported and have shown
that miR-34a can inhibit the proliferation and metastasis of oral
squamous carcinoma cells (11).
However, whether miR-34a expression is also associated with NPC has
not been clarified yet.
Ki67 is a marker used to evaluate cell proliferation
and is highly expressed in malignant cells. However, Ki67 is often
undetectable in normal cells. Therefore, it is often used to
predict the progression of cancer (12). It has been reported that Ki67 can be
used as an independent prognostic indicator of NPC, and its
increase is associated with poor prognosis (13). However, there are few studies on the
relationship between the clinicopathological features of NPC and
Ki67.
In the present study, we investigated the expression
levels of miR-34a and Ki67 in NPC, and explored their relationship
with clinicopathological features and prognosis, to provide a
reference for clinical use.
Patients and methods
Clinical data of patients
A prospective study was performed on cancer tissues
of 56 NPC patients who underwent needle biopsy from March 2011 to
December 2013 in Xiangyang No. 1 People's Hospital (Xiangyang,
China). These tissues were selected as the study group, while the
adjacent tissues (~2 cm away from the lesion) comprised the control
group. There were 41 males and 15 females with an average age of
52.44±13.75 years. The clinical staging criteria were based on the
NPC Diagnostic Criteria (14), as
set out by the Cancer Staging Guide of the American Joint Committee
on Cancer in 2010. The study was approved by the Medical Ethics
Committee of Xiangyang No. 1 People's Hospital (no. JS2011HHHC012)
and all the patients were informed and signed an informed consent
form.
Inclusion and exclusion criteria
Inclusion criteria: Patients diagnosed with NPC by
imaging and pathology; patients that hadn't undergone radiotherapy
and chemotherapy before the needle biopsy; patients without distant
metastasis; patients with complete clinical data; patients that
could be followed up by telephone. Exclusion criteria: Patients
with other otorhinolaryngological diseases; patients with other
malignant tumors; patients with severe cardio-cerebrovascular
disease; patients with severe inflammation; pregnant or lactating
women.
Main instruments and reagents
PCR instrument (ABI 7500; Applied Biosystems; Thermo
Fisher Scientific, Inc.), Ultraviolet spectrophotometer
(6135000041; Eppendorf, Inc.), total RNA extraction EasyPure miRNA
kit (ER601-01; Beijing Transgen Biotech Co., Ltd.), reverse
transcription and PCR kit TransScript miRNA First-Strand cDNA
Synthesis SuperMix (AT351-01; Beijing Transgen Biotech Co., Ltd.).
TransStart® Tip Green qPCR SuperMix (+Dye II) (AQ142-21;
Beijing Transgen Biotech Co., Ltd.). All primers were designed and
synthesized by Shanghai Shenggong Biological Co., Ltd. (Table I).
 | Table I.Primer sequences. |
Table I.
Primer sequences.
| Genes | Upstream primers | Downstream
primers |
|---|
| miR-34a |
5′-CTAGCTAGCTTGCTGTCCGCTTGATACTGG-3′ |
5′-GGAAGATCTCCCCGATCTGGTCACCGA-3′ |
| Ki67 |
5′-AAACCCCACCAAGTAAAACA-3′ |
5′-CCAAGGCAAGCTCAGGAC-3′ |
| GAPDH |
5′-AAAGAAGCTCAACTACATGG-3′ |
5′-TGCAAAGAATGCGTCCCAGAG-3′ |
| U6 |
5′-CTCGCTTCGGCAGCACA-3′ |
5′-AACGCTTCACGAATTTGCGT-3′ |
RT-qPCR detection method
Tissue (3 mm) stored at −80°C was ground in liquid
nitrogen. Total RNA from tissue suspension was extracted in strict
accordance with the manufacturer's instructions of total RNA
extraction kit. The purity and concentration of RNA were detected
using ultraviolet spectrophotometer and agarose gel
electrophoresis. Total RNA was then reversely transcribed using the
TransScript® miRNA RT Enzyme Mix and 2X TS miRNA
Reaction Mix (AT351-01; Beijing Transgen Biotech Co., Ltd.). After
shaking, total RNA was insulated at 30°C for 5 min and then
incubated at 42°C for 50 min in strict accordance with the
manufacturer's instructions. Next, PCR amplification was carried
out in a 20-µl reaction volume containing 1 µl of cDNA, 0.4 µl of
each upstream and downstream primers, 10 µl of 2X
TransStart® Tip Green qPCR SuperMix and 0.4 µl of
Passive Reference Dye (50X), to a final volume made up by
ddH2O. PCR conditions were as follows: Pre-denaturation
at 94°C for 30 sec, denaturation at 94°C for 5 sec, and annealing
and extension at 60°C for 30 sec, for a total of 40 cycles. Each
sample was tested in 3 repeat wells, and the experiment was carried
out 3 times. U6 and GAPDH were used as internal reference for
miR-34a and Ki67, respectively, and the 2−∆∆Cq method
(15) was used to analyze the
data.
Follow up
Fifty-six patients were followed up by telephone and
visit. Follow-up was conducted every 3 months for 1–2 years after
operation, and then at each 6 months for 2–5 years after operation.
The follow-up period was 5 years and the deadline was December
2018. All patients were followed up, with an average time of 51
months. The overall survival time was from the first day of the
operation to the last follow-up or death.
Outcome measures
The expression levels of miR-34a and Ki67 in the
study and the control group were compared, and the 5-year survival
of the patients was recorded. At 5 years, the patients were divided
into two groups: The survival group and the deceased group.
Multivariate COX regression was used to analyze the relevant
factors and Pearson's correlation analysis was used to analyze the
correlation between miR-34a and Ki67 in NPC tissues.
The optimal cut-off values of miR-34a- and
Ki67-associated mortality in NPC were analyzed by receiver
operating characteristic (ROC) curves. The best cut-off values of
miR-34a and Ki67 were divided into high- and low-expression groups
to observe the 5-year mortality and to draw Kaplan-Meier survival
curves.
Statistical analysis
SPSS 20.0 medical statistical analysis software (IBM
Corp.) was used for the statistical analysis of the collected data,
and GraphPad Prism 7 (GraphPad Software, Inc.) for plotting the
figures. Enumeration data were expressed as rate (%) and tested by
Chi-square test. Measurement data were expressed as the mean ±
standard deviation (means ± SD). All measurement data followed a
normal distribution. Independent samples t-test was used for their
comparison between two groups. The 5-year survival was analyzed by
Kaplan-Meier survival analysis. The ability of miR-34a and Ki67 to
diagnose NPC-associated mortality was analyzed by log-rank test and
was evaluated by ROC curves analysis. Multiple factor Cox
regression test was used for multivariate analysis of survival.
Pearson's correlation analysis was used for analyzing the
correlation between miR-34a and Ki67 expression in NPC tissues.
P<0.05 was considered to indicate a statistically significant
difference.
Results
Expression of miR-34a and Ki67 in the
study and control groups
By comparing the expression levels of miR-34a and
Ki67 between the two groups, it was found that the relative
expression of miR-34a in the study group was significantly lower
than that in the control group, and there was a significant
difference between the two groups (P<0.05). The relative
expression of Ki67 in the study group was significantly higher than
that in the control group (P<0.05) (Table II).
 | Table II.Expression levels of miR-34a and Ki67
in the study and control groups. |
Table II.
Expression levels of miR-34a and Ki67
in the study and control groups.
| Index | Study group
(n=56) | Control group
(n=56) | t value | P-value |
|---|
| miR-34a | 4.285±0.208 | 5.147±0.257 | 19.510 | <0.001 |
| Ki67 | 8.673±0.435 | 6.947±0.237 | 26.073 | <0.001 |
Association of miR-34a, Ki67 and
clinicopathological features in patients with NPC
By analyzing the expression levels of miR-34a and
Ki67, it was found that the expression of miR-34a was significantly
associated with bone metastasis and TNM staging (P<0.05). The
expression of Ki67 in NPC was significantly associated with
lymphatic metastasis and TNM staging (P<0.05) (Table III).
 | Table III.Association of miR-34a and Ki67 with
the clinicopathological features in patients with NPC. |
Table III.
Association of miR-34a and Ki67 with
the clinicopathological features in patients with NPC.
| Clinicopathological
features | n | miR-34a (n=56) | t value | P-value | Ki67 (n=56) | t value | P-value |
|---|
| Age (years) |
|
|
0.302 | 0.764 |
|
0.196 | 0.846 |
|
<50 | 27 | 4.804±0.212 |
|
| 8.037±0.368 |
|
|
| ≥50 | 29 | 4.787±0.209 |
|
| 8.018±0.359 |
|
|
| Sex |
|
|
0.462 | 0.646 |
|
0.662 | 0.511 |
| Male | 41 | 4.675±0.221 |
|
| 7.856±0.372 |
|
|
|
Female | 15 | 4.706±0.226 |
|
| 7.784±0.326 |
|
|
| Smoking history |
|
|
1.627 | 0.110 |
|
0.063 | 0.950 |
| Yes | 25 | 4.497±0.217 |
|
| 8.022±0.418 |
|
|
| No | 31 | 4.616±0.224 |
|
| 8.015±0.415 |
|
|
| Differentiation |
|
|
0.898 | 0.373 |
|
0.171 | 0.866 |
|
Undifferentiated | 14 | 4.772±0.236 |
|
| 7.982±0.387 |
|
|
| Low and
moderately differentiated | 42 | 4.844±0.267 |
|
| 8.003±0.403 |
|
|
| Bone
metastasis |
|
|
9.020 | <0.001 |
|
0.069 | 0.945 |
|
Yes | 19 | 4.334±0.202 |
|
| 8.029±0.417 |
|
|
| No | 37 | 4.947±0.258 |
|
| 8.021±0.408 |
|
|
| Lymphatic
metastasis |
|
|
0.708 | 0.482 |
|
8.951 | <0.001 |
|
Yes | 18 | 4.578±0.225 |
|
| 7.847±0.384 |
|
|
| No | 38 | 4.624±0.228 |
|
| 6.984±0.313 |
|
|
| Local invasion of
tumor |
|
|
0.725 | 0.472 |
|
0.926 | 0.359 |
|
Yes | 24 | 4.734±0.243 |
|
| 7.815±0.357 |
|
|
| No | 32 | 4.782±0.247 |
|
| 7.729±0.334 |
|
|
| TNM staging |
|
| 10.110 | <0.001 |
| 20.535 | <0.001 |
| Stage
I–II | 33 | 4.884±0.236 |
|
| 6.324±0.305 |
|
|
| Stage
III–IV | 23 | 4.263±0.211 |
|
| 8.293±0.413 |
|
|
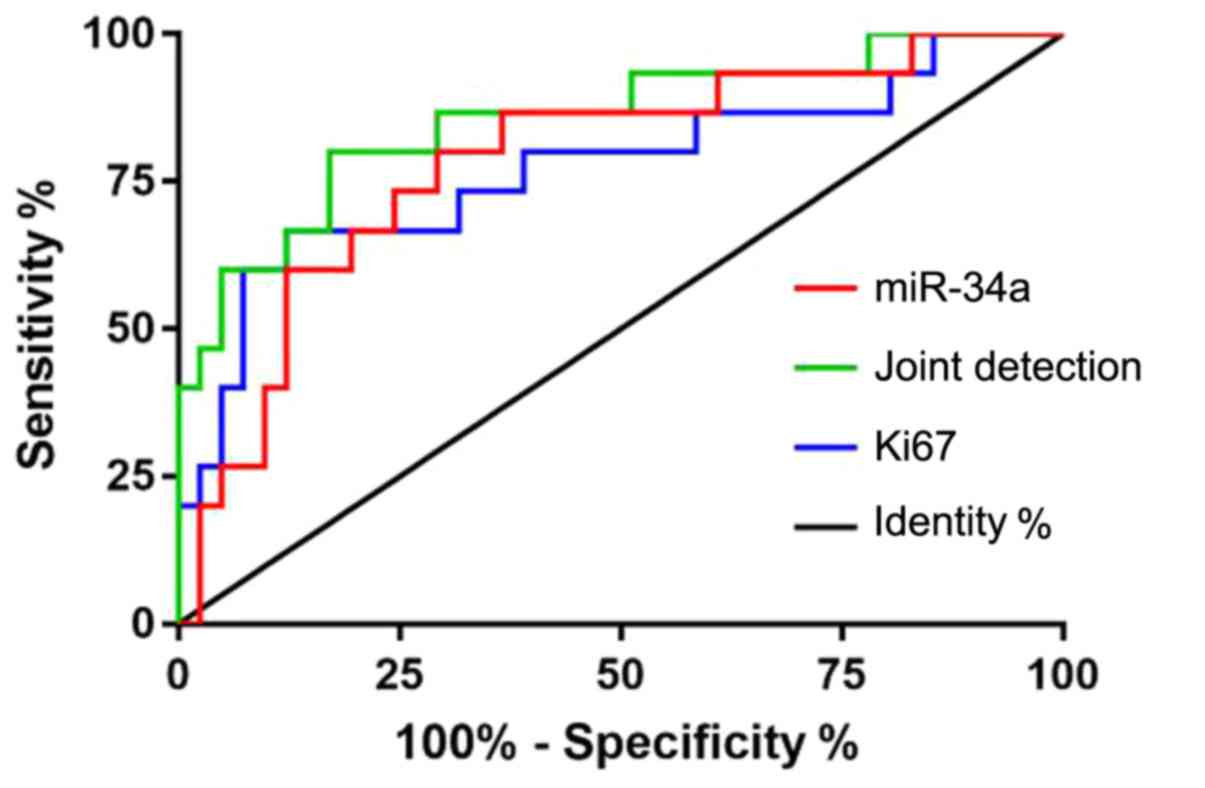
Diagnostic value of miR-34a and Ki67
in NPC-associated mortality
Patients were divided into survival group and
deceased group according to their survival. ROC curves were drawn
for the expression levels of miR-34a and Ki67 in both groups to
analyze the diagnostic value of the two indexes in NPC. The area
under curve (AUC) for miR-34a was 0.785, the 95% CI was
0.649–0.922, the specificity was 68.29%, the sensitivity was
80.00%, and the cut-off value was 4.680. The AUC of Ki67 was 0.772,
the 95% CI was 0.616–0.929, the specificity was 87.80%, the
sensitivity was 60.00%, and the cut-off value was 8.073. The AUC of
the joint detection was 0.855, the 95% CI was 0.734–0.977, the
specificity was 82.93%, the sensitivity was 73.33%, and the cut-off
value was 0.271 (Table IV and
Fig. 1).
 | Table IV.Diagnostic value of miR-34a, Ki67,
and their combination in NPC-associated mortality. |
Table IV.
Diagnostic value of miR-34a, Ki67,
and their combination in NPC-associated mortality.
| Index | AUC | 95% CI | Specificity
(%) | Sensitivity
(%) | Youden index
(%) | Cut-off |
|---|
| miR-34a | 0.785 | 0.649–0.922 | 68.29 | 80.00 | 48.29 | <4.680 |
| Ki67 | 0.772 | 0.616–0.929 | 87.80 | 60.00 | 47.80 | >8.073 |
| Joint
detection | 0.855 | 0.734–0.977 | 82.93 | 73.33 | 52.68 | >0.271 |
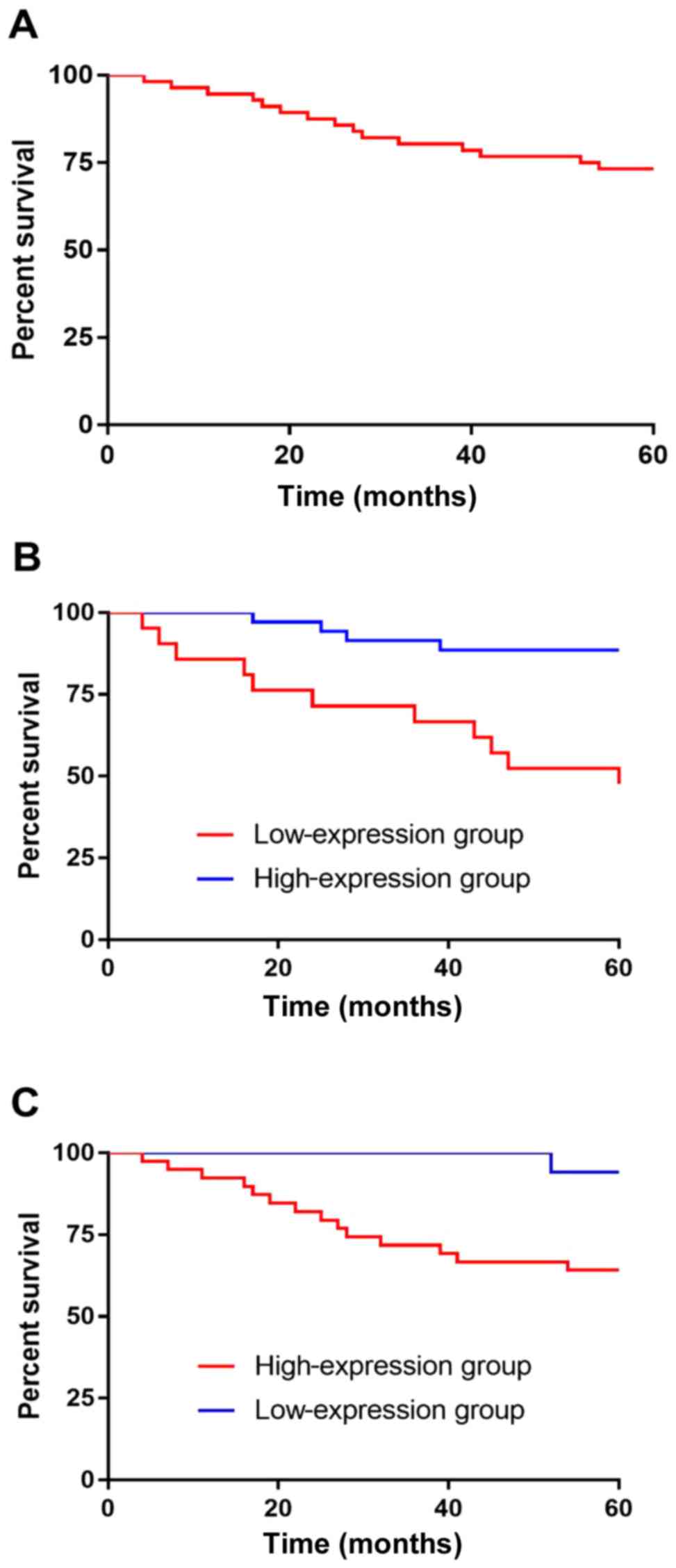
Relationship of the expression levels
of miR-34a and Ki67 with the 5-year survival of patients
According to the 5-year survival analysis of
patients, 56 cases were followed up and no case was lost. All
patients were followed up; 15 patients died and 41 survived within
5 years, and the survival rate was 73.21%. According to the median
value of miR-34a and Ki67 expression levels, the patients were
divided into high- and low-expression groups. The Kaplan-Meier
survival analysis revealed that the survival rate of patients with
low expression of miR-34a was significantly lower than that of
patients with high miR-34a expression, and there was significant
difference between the two groups (P<0.001). According to the
observation of Ki67 expression in two groups of patients, it was
found that the survival of patients with high expression of Ki67
was significantly lower than that of patients with low expression,
and there was a significant difference between the two groups
(P=0.022) (Fig. 2).
Univariate analysis of patient
survival
The clinical data of patients in the survival and
deceased group were collected and analyzed by univariate analysis.
The results showed that there was no significant difference in age,
sex and smoking history between the two groups (P>0.05).
However, there were significant differences in differentiation
degree, bone metastasis, lymphatic metastasis, local invasion of
tumor, TNM staging, miR-34a and Ki67 between the two groups
(P<0.05) (Table V).
 | Table V.Univariate analysis. |
Table V.
Univariate analysis.
| Factors | Survival group
(n=41) | Deceased group
(n=15) | t/χ2
value | P-value |
|---|
| Age (years) |
|
|
0.020 | 0.889 |
|
<50 | 20 (48.78) | 7
(46.67) |
|
|
|
≥50 | 21 (51.22) | 8
(53.33) |
|
|
| Sex |
|
|
0.448 | 0.503 |
|
Male | 31 (75.61) | 10 (66.67) |
|
|
|
Female | 10 (24.39) | 5
(33.33) |
|
|
| Smoking
history |
|
|
0.034 | 0.854 |
|
Yes | 18 (43.90) | 7
(46.67) |
|
|
| No | 23 (56.10) | 8
(53.33) |
|
|
|
Differentiation |
|
|
5.130 | 0.024 |
|
Undifferentiated | 7
(17.07) | 7
(46.67) |
|
|
| Low and
moderately differentiated | 34 (82.93) | 8
(53.33) |
|
|
| Bone
metastasis |
|
|
6.212 | 0.013 |
|
Yes | 10 (24.39) | 9
(60.00) |
|
|
| No | 31 (75.61) | 6
(40.00) |
|
|
| Lymphatic
metastasis |
|
|
2.574 | 0.040 |
|
Yes | 10 (24.39) | 8
(53.33) |
|
|
| No | 31 (75.61) | 7
(46.67) |
|
|
| Local invasion of
tumor |
|
|
4.743 | 0.029 |
|
Yes | 14 (34.15) | 10 (66.67) |
|
|
| No | 27 (65.85) | 5
(33.33) |
|
|
| TNM staging |
|
| 17.598 | <0.001 |
| Stage
I–II | 31 (75.61) | 2
(13.33) |
|
|
| Stage
III–IV | 10 (24.39) | 13 (86.67) |
|
|
| miR-34a | 4.942±0.247 | 4.221±0.212 | 10.022 | <0.001 |
| Ki67 | 7.643±0.352 | 8.547±0.427 |
8.034 | <0.001 |
Multivariate analysis of patient
survival
Indices that differed from univariate analysis were
incorporated into assignments (Table
VI). The results of multivariate Cox regression analysis showed
that the degree of differentiation, bone metastasis, lymphatic
metastasis and local invasion of tumor were not independent factors
for the survival of the patients. TNM staging (OR: 2.561, 95% CI:
0.182–8.598), miR-34a (OR: 0.011, 95% CI: 0.005–0.681) and Ki67
(OR: 0.016, 95% CI: 0.002–2.278) were independent factors in NPC
patients (Table VII).
 | Table VI.Assignments. |
Table VI.
Assignments.
| Factors | Assignment |
|---|
| Degree of
differentiation | Undifferentiated=1,
Lowly and moderately differentiated=0 |
| Bone
metastasis | Yes=1, No=0 |
| Lymphatic
metastasis | Yes=1, No=0 |
| Local invasion of
tumor | Yes=1, No=0 |
| TNM staging | Stage III+IV=1,
Stage I+II=0 |
| miR-34a | Data belong to
continuous variables using raw data analysis |
| Ki67 | Data belong to
continuous variables using raw data analysis |
| Survival time | Data belong to
continuous variables using raw data analysis |
| Survival
status | Death=1,
Survival=0 |
 | Table VII.Multivariate analysis. |
Table VII.
Multivariate analysis.
|
|
|
|
|
|
| Exp(B) 95% CI |
|---|
|
|
|
|
|
|
|
|
|---|
| Factors | B | S.E. | Wals | Sig. | Exp (B) | Lower limit | Upper limit |
|---|
| TNM staging | −7.925 | 3.848 | 4.242 | 0.039 | 2.561 | 0.182 | 8.598 |
| miR-34a | −13.839 | 5.838 | 5.620 | 0.018 | 0.011 | 0.005 | 0.681 |
| Ki67 | 4.262 | 2.140 | 3.966 | 0.030 | 0.016 | 0.002 | 2.278 |
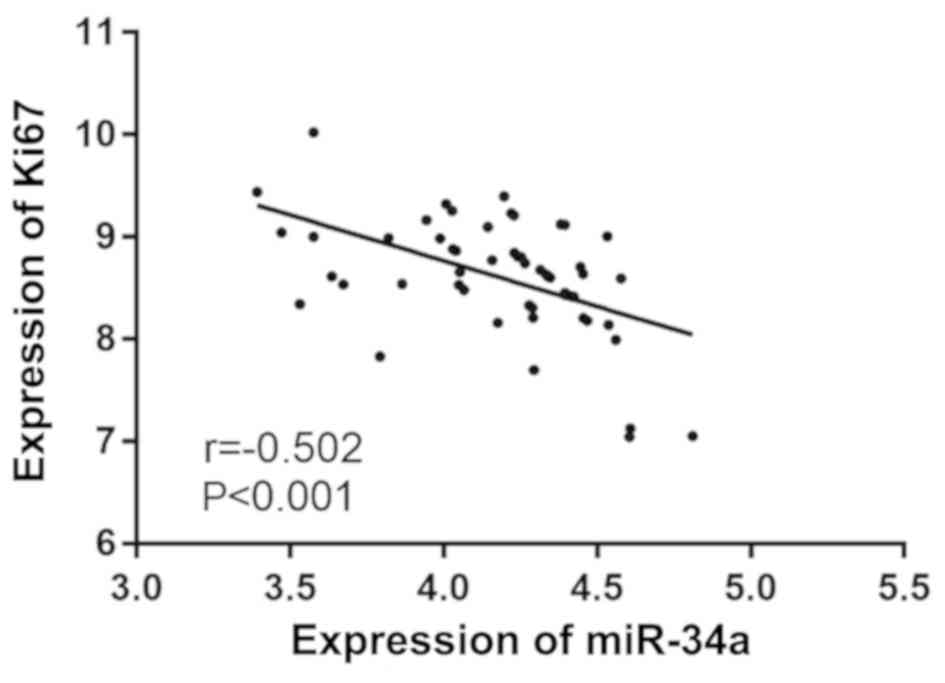
Correlation analysis of miR-34a and
Ki67 expression levels in NPC
There was a negative correlation between the
expression levels of miR-34a and Ki67 in NPC tissues, as predicted
by Pearson's correlation analysis. The expression of Ki67 was found
to decrease with the increase of miR-3a expression (r=−0.502,
P<0.001) (Fig. 3).
Discussion
NPC is a common malignant tumor in South China and
Southeast Asia (16). The specific
etiology of NPC is still unclear, however, it has been reported
that NPC is related to EBV virus infection, and methylation of the
parkin gene may also promote tumors of NPC (17,18).
Although NPC patients are sensitive to radiotherapy, the prognosis
of NPC patients is still poor due to recurrence and distant
metastasis (19). Therefore, finding
biomarkers that affect the prognosis of NPC is of great
significance to improve the prognosis and survival rate of the
patients.
In recent years, there has been a series of studies
on microRNAs in NPC. In the study of Sanchez Calle et al
(20), a series of biological assays
were carried out on NPC cell line in vitro and in
vivo, and it was found that miR-130a-3p was downregulated in
both NPC tissue and cell line. This result is similar to the result
of the present study, that the expression of miR-34a in cancer
tissue samples is lower than that in adjacent tissues. Huang et
al (21) found that miR-34a
inhibited epithelial mesenchymal transformation, invasion and
migration of NPC cells induced by TGF-β through directly targeting
Smad4. However, the relationship between miR-34a and
clinicopathological features and prognosis of NPC has rarely been
reported. Therefore, in the present study, the relationship between
miR-34a and the clinicopathological features of the patients was
further studied and it was found that the expression of miR-34a is
significantly associated with bone metastasis and TNM staging.
Ki67, used for the evaluation or as a prognostic indicator of
breast cancer, gastrointestinal pancreatic neuroendocrine tumo, and
other cancers, has been extensively studied in recent years
(22,23). In the present study, it was found
that Ki67 expression in cancer tissues is significantly higher than
that in adjacent tissues. The relationship between Ki67 and
clinicopathological features revealed that the expression of Ki67
is significantly associated with lymphatic metastasis and TNM
staging. Guan et al (24)
detected the expression of Ki67 protein in 90 pairs of NPC and
distant normal tissue by immunohistochemical method, and found that
the expression of Ki67 in tumor was higher than that in normal
tissue, which is similar to our results.
The 5-year survival of patients in this study was
followed up. Of the total 56 patients, 15 patients died within 5
years, 41 patients survived, and the survival rate was 73.21%.
Patients were divided according to their survival, and the
diagnostic value of miR-34a and Ki67 was analyzed by ROC curve
analysis. The AUC of miR-34a was 0.785, when the cut-off value was
<4.680, and the optimum specificity and sensitivity were 68.29
and 80.00%, respectively. The AUC for Ki67 was 0.772, the optimum
specificity and sensitivity were 87.80 and 60.00%, respectively,
when the cut-off value was >8.073. These results suggest that
miR-34a and Ki67 may be used as predictors of NPC-associated
mortality. At the same time, the sensitivity and specificity of the
two indexes were significantly different from each other. Through
the joint detection of the two indicators, it was found that the
area under the joint detection curve was 0.855, and the best
specificity and sensitivity were 82.93 and 73.33%, respectively,
when the cut-off value was >0.271. These results suggest that
the deficiency of the two can be overcome by joint detection.
Patients were divided into high- and low-expression groups
according to the median values of the two groups, and the
Kaplan-Meier survival curves that were drawn. The 5-year survival
of patients with low expression of miR-34a was significantly lower
than that of patients with high miR-34a expression, and the 5-year
survival of patients with high expression of Ki67 was significantly
lower than that of patients with low Ki67 expression.
Zhao et al (25), reported on the 3-year overall
survival and the high and low Ki67 expression in 45 patients with
NPC. The results revealed that the survival rate of patients with
high expression of Ki67 was lower, which is similar to our results.
In another study, the high expression of Ki67 was considered to be
beneficial to anti-radiation, leading to local recurrence and
distant metastasis, which would result in poor prognosis (26). By analyzing the patients'
clinicopathologic features, it was also found, in the present
study, that the patients in stages I and II have lower expression
of Ki67 and higher expression of miR-34a compared with those in
stage III and IV. Thus, the proportion of patients in the early
stage with low expression of Ki67 and high expression of miR-34a
was higher, and their survival condition was better. Multivariate
Cox regression analysis was also performed and it was found that
TNM staging, miR-34a and Ki67 were independent factors for
NCP-associated mortality, indicating that TNM staging, miR-34a and
Ki67 could be used as clinical indexes to evaluate the prognosis of
NPC patients. In addition, the correlation of miR-34a and Ki67 in
NPC was detected by Pearson's correlation analysis, and it was
found that there is a negative correlation between miR-34a and Ki67
expression levels, which suggests that there might be a close
relationship between miR-34a and Ki67, although this was not
explored in depth.
Although the relationship among miR-34a, Ki67,
clinical pathology and prognosis of NPC was determined, there are
still some deficiencies. Therefore further studies are
required.
In conclusion, the expression of miR-34a is
associated with bone metastasis and TNM staging, the expression of
Ki67 is associated with lymphatic metastasis and TNM staging, and
there is a negative correlation between miR-34a and Ki67 expression
levels. miR-34a and Ki67 can be used as predictors of
NPC-associated mortality. miR-34a, Ki67 and TNM staging are
associated with prognosis.
Acknowledgements
Not applicable.
Funding
No funding was received.
Availability of data and materials
The datasets used and/or analyzed during the present
study are available from the corresponding author on reasonable
request.
Authors' contributions
LW and CS performed PCR. YZ contributed to the
analysis of the observation indexes. CS was responsible for the
statistical analysis of the data. LW wrote the manuscript. All
authors read and approved the final manuscript.
Ethics approval and consent to
participate
The study was approved by the Ethics Committee of
Xiangyang No. 1 People's Hospital (Xiangyang, China). Patients who
participated in this research had complete clinical data. Signed
informed consents were obtained from the patients and/or
guardians.
Patient consent for publication
Not applicable.
Competing interests
The authors declare that they have no competing
interests.
References
|
1
|
Paul P, Deka H, Malakar AK, Halder B and
Chakraborty S: Nasopharyngeal carcinoma: Understanding its
molecular biology at a fine scale. Eur J Cancer Prev. 27:33–41.
2018. View Article : Google Scholar : PubMed/NCBI
|
|
2
|
Fu ZT, Guo XL, Zhang SW, Zeng HM, Sun KX,
Chen WQ and He J: Incidence and mortality of nasopharyngeal
carcinoma in China, 2014. Zhonghua Zhong Liu Za Zhi. 40:566–571.
2018.(In Chinese). PubMed/NCBI
|
|
3
|
Kong L, Li X, Wang H, He G and Tang A:
Calycosin inhibits nasopharyngeal carcinoma cells by influencing
EWSAT1 expression to regulate the TRAF6-related pathways. Biomed
Pharmacother. 106:342–348. 2018. View Article : Google Scholar : PubMed/NCBI
|
|
4
|
Huang WB, Chan JYW and Liu DL: Human
papillomavirus and World Health Organization type III
nasopharyngeal carcinoma: Multicenter study from an endemic area in
Southern China. Cancer. 124:530–536. 2018. View Article : Google Scholar : PubMed/NCBI
|
|
5
|
Fangzheng W, Chuner J, Lei W, Weijun C,
Min X, Quanquan S, Tongxin L, Aizawa R, Sakamoto M and Zhenfu F:
Outcome and long-term efficacy of four facio-cervical fields
conformal radiotherapy for nasopharyngeal carcinoma. Oncotarget.
8:39756–39765. 2017. View Article : Google Scholar : PubMed/NCBI
|
|
6
|
Wu LR, Liu YT, Jiang N, Fan YX, Wen J,
Huang SF, Guo WJ, Bian XH, Wang FJ, Li F, et al: Ten-year survival
outcomes for patients with nasopharyngeal carcinoma receiving
intensity-modulated radiotherapy: An analysis of 614 patients from
a single center. Oral Oncol. 69:26–32. 2017. View Article : Google Scholar : PubMed/NCBI
|
|
7
|
Zhou Y, Xia L, Lin J, Wang H, Oyang L, Tan
S, Tian Y, Su M, Wang H, Cao D, et al: Exosomes in nasopharyngeal
carcinoma. J Cancer. 9:767–777. 2018. View Article : Google Scholar : PubMed/NCBI
|
|
8
|
Witwer KW and Halushka MK: Toward the
promise of microRNAs - Enhancing reproducibility and rigor in
microRNA research. RNA Biol. 13:1103–1116. 2016. View Article : Google Scholar : PubMed/NCBI
|
|
9
|
Cheng C, Xiaohua W, Ning J, Dan Z,
Chengyun Y, Lijun Z, Li Y, Shengfu H, Hong J and He X: MiR-122
exerts anti-proliferative and apoptotic effects on nasopharyngeal
carcinoma cells via the PI3K/AKT signaling pathway. Cell Mol Biol.
64:21–25. 2018. View Article : Google Scholar : PubMed/NCBI
|
|
10
|
Chen L, Gao H, Liang J, Qiao J, Duan J,
Shi H, Zhen T, Li H, Zhang F, Zhu Z, et al: miR-203a-3p promotes
colorectal cancer proliferation and migration by targeting PDE4D.
Am J Cancer Res. 8:2387–2401. 2018.PubMed/NCBI
|
|
11
|
Li YY, Tao YW, Gao S, Li P, Zheng JM,
Zhang SE, Liang J and Zhang Y: Cancer-associated fibroblasts
contribute to oral cancer cells proliferation and metastasis via
exosome-mediated paracrine miR-34a-5p. EBioMedicine. 36:209–220.
2018. View Article : Google Scholar : PubMed/NCBI
|
|
12
|
Yang C, Zhang J, Ding M, Xu K, Li L, Mao L
and Zheng J: Ki67 targeted strategies for cancer therapy. Clin
Transl Oncol. 20:570–575. 2018. View Article : Google Scholar : PubMed/NCBI
|
|
13
|
Zhang J, Liu Y, Deng Y, He J, Lang J and
Fan J: Ki67 and nm23 are potential prognostic markers in patients
with nasopharyngeal carcinoma. Int J Clin Exp Pathol. 9:6350–6356.
2016.
|
|
14
|
Chen Q, Guo Z, Liu S, Quan P, Cao X, Guo
L, Zhang S and Sun X: The cancer incidence and mortality among
children and adolescents during the period of 2010–2014 in Henan
Province, China. Cancer Med. 8:814–823. 2019. View Article : Google Scholar : PubMed/NCBI
|
|
15
|
Livak KJ and Schmittgen TD: Analysis of
relative gene expression data using real-time quantitative PCR and
the 2(-Delta Delta C(T)) method. Methods. 25:402–408. 2001.
View Article : Google Scholar : PubMed/NCBI
|
|
16
|
Wang J, Wang L, Lou GH, Zeng HR, Hu J,
Huang QW, Peng W and Yang XB: Coptidis Rhizoma: A comprehensive
review of its traditional uses, botany, phytochemistry,
pharmacology and toxicology. Pharm Biol. 57:193–225. 2019.
View Article : Google Scholar : PubMed/NCBI
|
|
17
|
DeBord LC, Pathak RR, Villaneuva M, Liu
HC, Harrington DA, Yu W, Lewis MT and Sikora AG: The chick
chorioallantoic membrane (CAM) as a versatile patient-derived
xenograft (PDX) platform for precision medicine and preclinical
research. Am J Cancer Res. 8:1642–1660. 2018.PubMed/NCBI
|
|
18
|
Zhang J, Jia L, Tsang CM and Tsao SW: EBV
infection and glucose metabolism in nasopharyngeal carcinoma. Adv
Exp Med Biol. 1018:75–90. 2017. View Article : Google Scholar : PubMed/NCBI
|
|
19
|
Fangzheng W, Chuner J, Quanquan S, Zhimin
Y, Tongxin L, Jiping L, Sakamoto M, Peng W, Kaiyuan S, Weifeng Q,
et al: Addition of chemotherapy to intensity-modulated radiotherapy
does not improve survival in stage II nasopharyngeal carcinoma
patients. J Cancer. 9:2030–2037. 2018. View Article : Google Scholar : PubMed/NCBI
|
|
20
|
Sanchez Calle A, Kawamura Y, Yamamoto Y,
Takeshita F and Ochiya T: Emerging roles of long non-coding RNA in
cancer. Cancer Sci. 109:2093–2100. 2018. View Article : Google Scholar : PubMed/NCBI
|
|
21
|
Huang G, Du MY, Zhu H, Zhang N, Lu ZW,
Qian LX, Zhang W, Tian X, He X and Yin L: MiRNA-34a reversed
TGF-β-induced epithelial-mesenchymal transition via suppression of
SMAD4 in NPC cells. Biomed Pharmacother. 106:217–224. 2018.
View Article : Google Scholar : PubMed/NCBI
|
|
22
|
Klöppel G and La Rosa S: Ki67 labeling
index: Assessment and prognostic role in gastroenteropancreatic
neuroendocrine neoplasms. Virchows Arch. 472:341–349. 2018.
View Article : Google Scholar : PubMed/NCBI
|
|
23
|
Shan GP, Wang BB, Zheng P, Du FL and Yang
YW: Efficacy and safety of chemotherapy combined with stereotactic
radiotherapy in the treatment of nasopharyngeal carcinoma. Med Sci
Monit. 23:5630–5636. 2017. View Article : Google Scholar : PubMed/NCBI
|
|
24
|
Guan GF, Zhang DJ, Wen LJ, Yu DJ, Zhao Y,
Zhu L, Guo YY and Zheng Y: Prognostic value of TROP2 in human
nasopharyngeal carcinoma. Int J Clin Exp Pathol. 8:10995–11004.
2015.PubMed/NCBI
|
|
25
|
Zhao L, Chen H, Hu B, Zhang H and Lin Q:
Prognostic significance of Ki67 expression and the derived
neutrophil-lymphocyte ratio in nasopharyngeal carcinoma. Cancer
Manag Res. 10:1919–1926. 2018. View Article : Google Scholar : PubMed/NCBI
|
|
26
|
Zhao Y and Shen L, Huang X, Jing D, Huang
D, Fu J, Li Z, Zhang G and Shen L: High expression of Ki-67 acts a
poor prognosis indicator in locally advanced nasopharyngeal
carcinoma. Biochem Biophys Res Commun. 494:390–396. 2017.
View Article : Google Scholar : PubMed/NCBI
|