1. Introduction
Angiopoietin-like proteins are a group of seven
proteins whose structure is comparable to that of angiopoietins;
however, they do not bind to Tie2 or Tie1 receptors (1). Angiopoietin-like proteins are present
in the majority of the mammals' reign, apart from angiopoietin-like
protein 5, which is exclusively human. Angiopoietin-like protein 8,
also known as betatrophin, is another form of angiopoietin-like
protein, characterized by N-terminal domains similar to
angiopoietin-like protein 3, without a C-terminal fibrinogen-like
domain (2).
Angiopoietin-like protein 1, or angioarrestin, is an
inhibitor of vascular endothelial growth factor (VEGF), which has
been demonstrated to block the STAT3 pathway and, consequently,
angiogenesis in hepatocellular carcinoma (3). Angiopoietin-like protein 2 activates
nuclear factor-κB (NF-κB) and plays a role in inflammatory
diseases, reactive oxygen species production and carcinogenesis
(4-6).
Angiopoietin-like protein 3 inhibits lipoprotein lipase (LPL),
similar to a angiopoietin-like protein 4 (ANGPTL4), and together
with angiopoietin-like protein 8, they are involved in lipid
metabolism. Moreover, both angiopoietin-like proteins 3 and 8 are
more highly expressed in hepatocellular carcinoma (7).
Angiopoietin-like protein 5 and angiopoietin-like
protein 7 play a role in the expansion of hematopoietic stem cells
and lung cancer. While angiopoietin-like protein 7 appears to be
associated with the inhibition of cancer, increased levels of
angiopoietin-like protein 5 have been shown to be associated with
the poor survival of patients with non-small cell lung cancer
(8).
Angiopoietin-like protein 6 is expressed in
keratinocytes and the liver. This protein binds to ERK1 and ERK2,
regulating epidermal proliferation. It is involved in psoriasis and
appears to interact with E-cadherin as a poor prognostic factor in
colon cancer (9).
The present review discusses the role of ANGPTL4 in
podocypopathies. For this purpose, a search was performed on the
Medline, Embase, Cochrane Central Register of Controlled Trials
(CENTRAL), Ovid and google scholar databases to identify relevant
articles. A search was made for articles in the English language.
The following key words were used: Angiopoietin-like protein OR
angiopoietin-like protein 4 OR ANGPTL OR ANGPLT4; proteinuria OR
nephrotic syndrome OR minimal change disease OR mcd OR focal and
segmental glomerulosclerosis (FSGS) OR focal and segmental
glomerulosclerosis OR podocytopathies; Animal studies OR in
vitro OR human studies.
2. Angiopoietin-like protein 4
ANGPLT4 is also known as peroxisome
proliferator-activated receptor-γ (peroxisome
proliferator-activated receptor-γ) angiopoietin-related or
Fasting-induced adipose factor, and its gene is located in
chromosome 19p13.3. This protein has a molecular weight of 45-65
kDa and is composed of 406 amino acids, including four cysteines
responsible of sulfide linkages, three N-terminal glycosylation
sites and a fibrinogen-like C-terminal domain. Following cleavage,
the N-terminal fragment spreads around as an oligomeric protein,
while C-terminal protein as a monomer.
ANGPLT4 is produced by several tissues, including
the liver, blood plasma, placenta, small intestine, heart and
adipose tissue, induced by both glucocorticoid and nuclear hormone
receptors via a peroxisome proliferator-activated
receptor-γ-response element located in the human ANGPLT4 gene
(10). The function of ANGPLT4 is
tissue-dependent; thus, it may be involved in the regulation of
vascular permeability, angiogenesis, tumor metastasis and
ischemia-reperfusion injury (11).
ANGPLT4 interacts with β1 and β5-integrin of the
renal extracellular matrix, modifying the podocyte cytoskeleton
(12,13). The inflammatory response associated
with ANGPLT4 overexpression can lead to the development of
podocytopathies and nephrotic syndrome, while lower glomerular
levels of this protein have been shown to be associated with a
reduced apoptotic rate of podocytes (14), improving their repair processes
(15). However, the intravenous
administration of recombinant ANGPLT4 has been found to reduce
proteinuria in rat models of nephrotic syndrome due to membranous
nephropathy and diabetic kidney disease (15).
Two forms of ANGPLT4 are known on the basis of their
sialylation state: Hyposialylated ANGPLT4, which has a
high-isoelectric point (high-pI), while normal sialylated ANGPLT4
has a neutral isoelectric point (neutral-pI) (16). The second isoform is the most
secreted, particularly by bone and muscle, in response to
hypertriglyceridemia (17) and,
unlike the hyposialylated ANGPLT4, neutral-pI ANGPLT4 may also
reduce proteinuria by binding β5 integrin, as has been demonstrated
in an experimental model (16).
Previous studies have indicated that neutral-pI ANGPLT4 is secreted
in podocytopathies and other glomerulonephritis, while high-pI
ANGPLT4 is upregulated in minimal change disease (MCD) (16,17).
Furthermore, ANGPLT4 can increase reactive oxygen species
production, as it spurs NADPH oxidase 1(18) and increases the levels of
pro-inflammatory interleukins (such as interleukin-6), the
O2-/H2O2 ratio and the
synthesis of serum amyloid A protein (10).
According to the study by Clement et al
(15), normal sialylated
angiopoietin-like protein 4 can protect the glomerular endothelium,
while the hyposialylated form may be a cause of injury in MCD, as
the glomerular secretion of ANGPLT4 can influence the glomerular
basement membrane charge, modifying its diaphragm power and
increasing protein loss (16). The
expression of ANGPLT4 is also increased in renal cancer cells and
metastatic disease, although its role in tumor progression remains
unclear (19,20).
ANGPLT4 and lipid metabolism
The oligomerization of ANGPLT4 reduces the activity
of LPL in uptaking free fatty acids (FFAs) in muscle cells and
adipose tissue, causing hypertriglyceridemia, as demonstrated in
experimental models with high-pI titers of angiopoietin-like
protein (17). Oligomerization
stabilizes ANGPLT4 following cleavage (12,21)
and the N-terminal interaction with lipoprotein lipase is
transient; however, it causes the permanent inactivity of this
enzyme, inducing its conversion from a dimeric to monomeric
inactive form. Some mutations of ANGPLT4, as those regarding Cys76
and Cys80, reduce the inhibitory effects of ANGPLT4 on LPL
(22). This protein carries out
its role in lipid metabolism by inhibiting the fasting signal in
the hypothalamus cortex, where it is expressed (12). Furthermore, some genetic mimicry of
ANGPTL4 appear to be related to a reduced risk of developing
coronary heart disease in patients with diabetes (23). It is known that free fatty acids
increase ANGPLT4 through the activation of peroxisome
proliferator-activated receptor (peroxisome proliferator-activated
receptor), in particular in the case of a high FFA/albumin ratio,
as occurs in proteinuric diseases such as MCD, characterized by the
selective urinary loss of albumin and in analbuminemic experimental
models. Moreover, according to the study by Clement et al
(21), the transgenic expression
of adipose aP2-ANGPLT4 gene increases serum ANGPLT4, but does not
affect proteinuria, differently from the selective overexpression
of podocyte NPHS2-ANGPLT4, which induces proteinuria and the loss
of glomerular basement membrane charge, reflecting the different
roles of the isoforms of ANGPLT4. Leptin appears to be directly or
indirectly implicated with angiopoietin-like protein regulation, as
it can inhibit ANGPLT4 mRNA transcription (10). Moreover, it has been demonstrated
that ANGPLT4 overexpression is related to inflammation and hypoxia,
particularly in adipose tissue, causing chronic inflammation and
macrophage infiltration in white adipose tissue (24).
ANGPLT4 and MCD
MCD is a podocytopathy, representing the most
frequent cause of nephrotic syndrome in children and one of the
most frequent in adults. It is characterized by selective
proteinuria (often without hematuria), hypertension and edema
(25). The typical histological
lesions are visible with electron microscopy, which reveals the
effacement and fusion of podocyte foot processes in the absence of
electron-dense deposits. In 1974, Shalhoub (26) suggested that T-lymphocytes play a
primary role in the pathogenesis of MCD and further studies
confirmed an association between MCD and atopy or an increased
number of the T-helper 2 (Th2) cell subset (27,28).
The disease is usually cortico-sensitive, with a remission rate of
up to 90% of cases, unlike other podocytopathies, such as FSGS, in
which complete remission is achieved in 30-40% of patients
(29-31).
In 2004, Reiser et al (32) demonstrated that lipopolysaccharide
(LPS) upregulates B7-1 (CD80), increasing proteinuria and in 2016,
Liu (33) proposed the existence
of an association between B7-1 and the modified charge of
glomerular basement membrane induced by ANGPLT4, although this is
not yet completely clear. A previous study using a child
population, demonstrated that ANGPTL4 worsens the nephrotic
syndrome, with a reduction of podocin and actin on podocyte foots
(34). Similarly, recombinant
ANGPTL4 animal models or treatment that reduced it, as reported in
a review of 2014, seemed to be related with an improvement in the
nephrotic syndrome (35). Similar
results were found in another animal study at 21 weeks of follow-up
(36). The observation of murine
models of MCD, such as puromycin aminonucleoside-affected
glomeruli, has revealed a deficiency in heparan sulfate
proteoglycans compared to healthy glomeruli (37).
ANGPLT4 appears to induce the effacement of podocyte
foot processes by activating signals at the podocyte-glomerular
basement membrane interface binding αvβ5 integrin (38); consistently, ANGPLT4 is poorly
expressed in normal glomeruli, although it is overexpressed in
mouse models of MCD, both locally as confirmed by the in
situ hybridization of capillary loop, and in serum and urine
(24,39).
In particular, in puromycin aminonucleoside-affected
glomeruli, there is a glucocorticoid sensitive overexpression of
high-pI ANGPLT4. This isoform is present at a higher concentration
in the case of MCD relapses and it is not detectable during disease
remission, membranous nephropathy and FSGS (16). Furthermore, increased serum levels
of high-pI angiopoietin-like protein have been found in patients
with MCD (17). The administration
of N-acetylmannosamine (ManNAc), which converts high-pI ANGPLT4 to
neutral-pI ANGPLT4, has been demonstrated to lead to a reduction in
albuminuria of 40% (39).
According to Davin (40), the hyposialylated form is a
mediator of proteinuria in MCD, through its binding to glomerular
basement membrane and endothelial cells: Specifically, in
glomeruli, it binds to endothelial alpha V beta5 integrin (at the
very least) and modifies putative-podocyte feedback loops to reduce
proteinuria. Furthermore, increased serum levels of high-pI
angiopoietin-like protein have been found in patients with MCD
(40).
In addition, according to the study by Li et
al (41), urinary ANGPLT4 may
represent an earlier biomarker of podocyte injury in a rat model of
damage induced by adriamycin. Another study found that ANGPLT4
glomerular expression and urinary excretion exhibited the same
trend, associated with the early stage proteinuria (42). Proteinuria then continued to
increase despite the decrease in ANGPLT4 levels. Glomerular ANGPLT4
upregulation appeared significantly earlier than the changes in
desmin and synaptopodin in rats with damage induced by adriamycin,
suggesting that adriamycin and glomerular ANGPLT4 may result in
foot process effacement and cytoskeletal damage. When rats with
damage induced by adriamycin received tacrolimus administration, it
resulted in preventing desmin enhanced expression and reversing the
reduction in synaptopodin. Moreover, the immunosuppressive effects
of tacrolimus significantly reduced angiopoietin-like protein 4
glomerular countenance and urinary release (43).
In another study on an animal model of
cisplatin-induced acute kidney injury, increased levels of mRNA and
neutral ANGPLT4 were observed in proximal tubules, probably
associated with lipoprotein lipase damage (44).
Glucocorticoid therapy appears to reduce
proteinuria, as well as serum ANGPLT4 levels within 6 days;
however, it remains unclear whether it is a direct impact on
ANGPLT4 expression, or whether this relation is subject to a
reduction of nephrotic syndrome manifestations (proteinuria and
hypoalbuminemia), which act as a stimulus for the renal synthesis
of ANGPLT4(26).
ANGPLT4 and other podocytopathies
Both in humans and experimental models, there is no
modification in the expression of ANGPLT4 mRNA in collapsing type
FSGS, in contrast to what occurs in MCD (36). Clement et al reported a
significant upregulation of ANGPLT4 in experimental MCD as opposed
to FSGS, and anti-Thy1.1 (mesangial proliferative)
glomerulonephritis (MsPGN) (15).
Conversely, urinary ANGPLT4 is overexpressed in FSGS
during relapses and appears to be associated with proteinuria in
relapsing FSGS and other glomerulopathies, excluding MCD (45). Furthermore, serum ANGPLT4 levels
appear to be reduced in association with LPS podocyte injury,
whereas urinary and glomerular ANGPLT4 levels appear to be
increased. No changes have been found in mesangial cells (46). In in vitro experiments, LPL
and puromycin aminonucleoside-induced injury caused minimal change
disease. This can explain the similar ANGPLT4 evolution (45).
When comparing patients with MCD, FSGS and
membranous nephropathy, elevated circulating levels of high-pI and
oligomeric neutral-pI ANGPLT4 have been detected only in relapsing
MCD (24). Furthermore, the
hyposialylated form is not upregulated in membranous syndrome or
other glomerulopathies.
Soluble urokinase-type plasminogen
activator receptor: A potential confounding factor in FSGS
MCD and FSGS are often considered as two faces of
the same disease. Of note, similar mechanisms are present in these
conditions, including ANGPLT4 involvement through the soluble
urokinase-type plasminogen activator receptor (suPAR). Its
pathogenetic role in FSGS is currently a topic of debate among
scientists (47). Soluble
urokinase-type plasminogen activator receptor is a
glycosylphosphatidylinositol-anchored membrane glycoprotein,
composed of three homologue domains termed DI, DII and DIII, and
found in an insoluble form of 35-60 kDa or a soluble form 20-50
kDa, with different molecular masses depending on the site of
glycosylation. Its secretion increases in an inflammatory status
and its serum levels are associated with chronic kidney disease and
a decline in the glomerular filtration rate (48-50).
It is found in FSGS at high serum levels during disease flare,
while lower levels are associated with remission of the disease.
Apart from its role in the regulation of chemotaxis, suPAR can
interact with α3β1 and αvβ3 integrins which have both a structural
role binding vitronectin molecules and podocyte actin-based
cytoskeleton to the glomerular basement membrane, and a role in
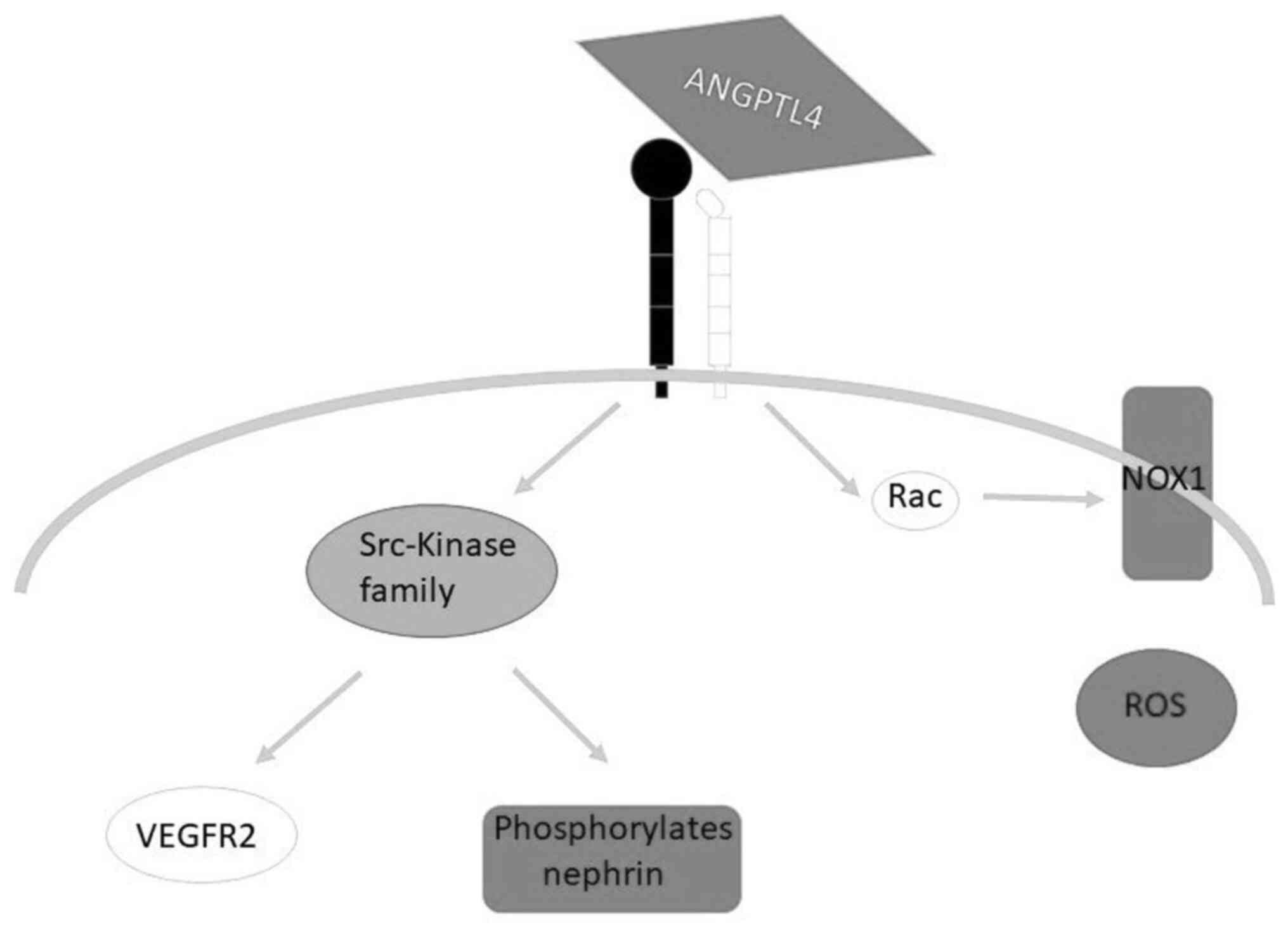
intracellular signaling. suPAR is able to induce
vitronectin-dependent αvβ3-integrin activation, thus modulating the
Rac1 pathway and increasing the production of contractile fibers in
cultured podocytes and murine models, determining foot process
effacement. Conversely, β1 integrin can modulate the Src-kinase
family that phosphorylates nephrin and, consequently, regulates
actin polymerization, and β5 can regulate laminin and fibronectin
distribution (51) (Fig. 1).
Furthermore, nephrin expression is reduced with the
increased expression of ANGPTL4 following treatment with palmitic
acid, perhaps mediated by the AMP activated protein
kinase/phosphor-acetyl-coA carboxylase pathway (52).
ANGPTL4 and peroxisome
proliferator-activated receptors
Peroxisome proliferator-activated receptors are
steroid/thyroid nuclear hormone receptors involved in metabolic
homeostasis and distinct in three forms: Peroxisome
proliferator-activated receptor α (NR1C1), peroxisome
proliferator-activated receptor γ (NR1C3) and peroxisome
proliferator-activated receptors β/δ (NR1C2). Their activation can,
in turn, reduce hypertriglyceridemia (peroxisome
proliferator-activated receptor α), serum glucose in type 2
diabetes, independent of the insulin-glucose effect (peroxisome
proliferator-activated receptor γ), or provide benefit to
steatohepatitis in metabolic syndrome, as well as reducing the
regulation of the molecule NF-κB (peroxisome proliferator-activated
receptors β/δ) (53). Peroxisome
proliferator-activated receptor γ expression is low in the
glomerular basement membrane, whereas it increases after damage.
Peroxisome proliferator-activated receptors α and γ are also
ANGPTL4 and leptin targets (10,53).
ANGPTL4 mRNA expression is lower in heterozygous
peroxisome proliferator-activated receptor γ-mutant mice than in
non-mutant mice; conversely, the leptin level is higher (49). In embryonic mouse fibroblast NIH
3t3 cells, ANGPTL4 mRNA expression is low prior to the
administration of pioglitazone, although its expression multiplies
2 h after treatment (54). On the
contrary, Lu et al demonstrated that paeoniflorin restores
podocyte features and upregulates peroxisome proliferator-activated
receptor γ expression, decreasing ANGPTL4 levels in the kidney, in
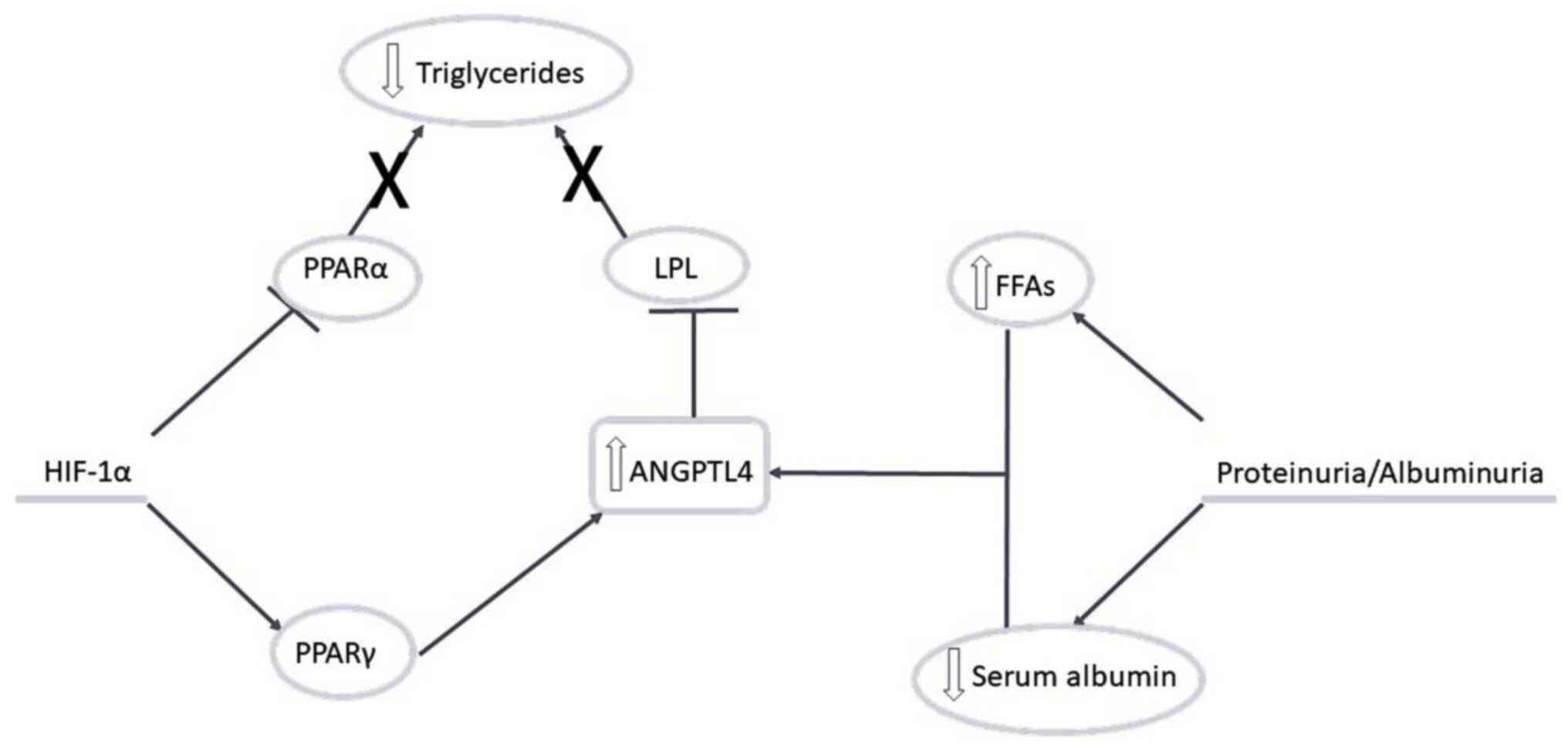
an experimental model of nephrotic syndrome (55). In a model of puromycin
aminonucleoside nephropathy, Yang (51) demonstrated that the early
administration of peroxisome proliferator-activated receptor
agonist reduced overall sclerosis and decreased ANGPTL4 expression
(Fig. 2).
A common point between ANGPTL4 and peroxisome
proliferator-activated receptors is hypoxia. ANGPTL4 has a
hypoxia-inducible factor (HIF)-1α-dependent mechanism.
Hypoxia-inducible factor is a heterodimeric transcription factor
with angiogenic activity. The Α-subunit is oxygen-sensitive and
contains proline residues (residues 402 and 564). Following the
hydroxylation of these residues, von Hippel-Lindau tumor suppressor
protein binds HIF-1α for degradation. If oxygenation is <5%,
HIF-1α binds to HIF-1β. It has been observed that the reduction of
HIF-1α expression decreases ANGPTL4 mRNA expression. Conversely,
peroxisome proliferator-activated receptors β/δ, in synergy with
HIF-1α, upregulate ANGPTL4 mRNA expression (56,57).
Peroxisome proliferator-activated receptor γ
agonists improve glomerulosclerosis in rat models administered
puromycin aminonucleoside, reducing the expression of peroxisome
proliferator-activated receptor γ and restoring the negative
effects on glomeruli. In vivo, peroxisome
proliferator-activated receptor γ agonists increase VEGF expression
and reduce ANGPTL4 expression.
3. New treatments
In 2011, Clement et al (21) fed NPHS-ANGPTL4 transgenic rats
ManNAc, to examine its efficacy on a model of MCD. The
administration of ManNAc resulted in an increased sialylation of
ANGPTL4 and a main reduction of albuminuria of ~40.6% (21).
Salvianolic acid A is a hydrosoluble substance
effective against peroxidative damage in the retina and kidneys. In
addition to low doses of prednisone, it has been demonstrated to
reduce proteinuria and high levels of triglycerides, increase serum
albumin more than steroids alone, as well as prevent the
deterioration of kidney function and even revert foot processes
fusion. In the same study, the authors demonstrated that
salvianolic acid A increased the levels of synaptopodin and desmin
in vivo, as well as in vitro, affecting the
RhoA-pathway and peroxisome proliferator-activated receptor γ
expression (58).
In the same year, Liu and He (59) demonstrated that the intraperitoneal
administration of epigallocatechin-3-gallate in mice ameliorated
sclerosis and decreased proteinuria and ANGPTL4 expression in renal
tissue by suppressing the HIF1α/ANGPTL4 pathway.
In 2016, new therapeutic agents were proposed, such
as recombinant mutated human ANGPTL4, which was demonstrated to
significantly ameliorate proteinuria without hypertrigliceridemia,
or Bis-T-23(60). This small
molecule has been investigated in several murine models of
proteinuric kidney diseases and stimulates actin-dependent dynamin
oligomerization and actin polymerization, reducing or even
preventing proteinuria (11,49).
4. Conclusion and future perspectives
It remains unclear whether FSGS and MCD are
different diseases or different manifestations of the same
pathology; however, MCD may represent an early form of FSGS. CD80
lymphocytes and soluble urokinase-type plasminogen activator
receptor, despite both being elevated in FSGS and MCD, have
different profiles of expression in each of these
podocytopathies.
The role of ANGPTL4 in podocytopathies is
increasingly recognized, and may be adopted as an early predictor
of MCD; however, high levels of this protein in other diseases and
its impact on lipid metabolism make this hypothesis unlikely.
The high-pI ANGPTL4/neutral-pI ANGPTL4 ratio in
serum and urine or between the two isoforms of ANGPTL4 and soluble
urokinase-type plasminogen activator receptor should be further
studied, in order to identify a marker that allows for the
differential diagnosis between early FSGS and MCD. This may also
lead to the development of appropriate therapeutic protocols, in
particular in younger patients or those who are not eligible for a
kidney biopsy.
Acknowledgements
Not applicable.
Funding
Funding: No funding was received.
Availability of data and materials
Not applicable.
Authors' contributions
VCa and FGV conceptualized the study. FZ and VCe
were involved in the search for relevant literature. FZ and VCa and
RS were involved in the writing and preparation of the original
draft of the manuscript. VCa and DS were involved in the analysis
of the studies identified in the literature for inclusion in the
review. FGV and FZ and RS were involved in the writing, reviewing
and editing of the manuscript. VCe and FGV were involved in the
processing of images. DS supervised the study. All authors have
read and agreed to the published version of the manuscript. Data
authentication is not applicable.
Ethics approval and consent to
participate
Not applicable.
Patient consent for publication
Not applicable.
Competing interests
The authors declare that they have no competing
interests.
References
|
1
|
Kadomatsu T, Tabata M and Oike Y:
Angiopoietin-like proteins: Emerging targets for treatment of
obesity and related metabolic diseases. FEBS J. 278:559–564.
2011.PubMed/NCBI View Article : Google Scholar
|
|
2
|
Endo M: The roles of ANGPTL families in
cancer progression. J UOEH. 41:317–325. 2019.PubMed/NCBI View Article : Google Scholar
|
|
3
|
Yan Q, Jiang L, Liu M, Yu D, Zhang Y, Li
Y, Fang S, Li Y, Zhu YH, Yuan YF and Guan XY: ANGPTL1 interacts
with integrin α1β1 to suppress HCC angiogenesis and metastasis by
inhibiting JAK2/STAT3 signaling. Cancer Res. 77:5831–5845.
2017.PubMed/NCBI View Article : Google Scholar
|
|
4
|
Tabata M, Kadomatsu T, Fukuhara S, Miyata
K, Ito Y, Endo M, Urano T, Zhu HJ, Tsukano H, Tazume H, et al:
Angiopoietin-like protein 2 promotes chronic adipose tissue
inflammation and obesity-related systemic insulin resistance. Cell
Metab. 10:178–188. 2009.PubMed/NCBI View Article : Google Scholar
|
|
5
|
Aoi J, Endo M, Kadomatsu T, Miyata K,
Ogata A, Horiguchi H, Odagiri H, Masuda T, Fukushima S, Jinnin M,
et al: Angiopoietin-like protein 2 accelerates carcinogenesis by
activating chronic inflammation and oxidative stress. Mol Cancer
Res. 12:239–249. 2014.PubMed/NCBI View Article : Google Scholar
|
|
6
|
Aoi J, Endo M, Kadomatsu T, Miyata K,
Nakano M, Horiguchi H, Ogata A, Odagiri H, Yano M, Araki K, et al:
Angiopoietin-like protein 2 is an important facilitator of
inflammatory carcinogenesis and metastasis. Cancer Res.
71:7502–7512. 2011.PubMed/NCBI View Article : Google Scholar
|
|
7
|
Arca M, Minicocci I and Maranghi M: The
angiopoietin-like protein 3: A hepatokine with expanding role in
metabolism. Curr Opin Lipidol. 24:313–320. 2013.PubMed/NCBI View Article : Google Scholar
|
|
8
|
Wang L, Geng T, Guo X, Liu J, Zhang P,
Yang D, Li J, Yu S and Sun Y: Co-expression of immunoglobulin-like
transcript 4 and angiopoietin-like proteins in human non-small cell
lung cancer. Mol Med Rep. 11:2789–2796. 2015.PubMed/NCBI View Article : Google Scholar
|
|
9
|
Marchiò S, Soster M, Cardaci S, Muratore
A, Bartolini A, Barone V, Ribero D, Monti M, Bovino P, Sun J, et
al: A complex of α6 integrin and E-cadherin drives liver metastasis
of colorectal cancer cells through hepatic angiopoietin-like 6.
EMBO Mol Med. 4:1156–1175. 2012.PubMed/NCBI View Article : Google Scholar
|
|
10
|
Yoon JC, Chickering TW, Rosen ED, Dussault
B, Qin Y, Soukas A, Friedman JM, Holmes WE and Spiegelman BM:
Peroxisome proliferator-activated receptor gamma target gene
encoding a novel angiopoietin-related protein associated with
adipose differentiation. Mol Cell Biol. 20:5343–5349.
2000.PubMed/NCBI View Article : Google Scholar
|
|
11
|
Guo L, Li SY, Ji FY, Zhao YF, Zhong Y, Lv
XJ, Wu XL and Qian GS: Role of Angptl4 in vascular permeability and
inflammation. Inflamm Res. 63:13–22. 2014.PubMed/NCBI View Article : Google Scholar
|
|
12
|
Zhu P, Goh YY, Chin HFA, Kersten S and Tan
NS: Angiopoietin-like 4: A decade of research. Biosci Rep.
32:211–219. 2012.PubMed/NCBI View Article : Google Scholar
|
|
13
|
Peng L, Ma J, Cui R, Chen X, Wei SY, Wei
QJ and Li B: The calcineurin inhibitor tacrolimus reduces
proteinuria in membranous nephropathy accompanied by a decrease in
angiopoietin-like-4. PLoS One. 9(e106164)2014.PubMed/NCBI View Article : Google Scholar
|
|
14
|
Chugh SS, Clement LC and Macé C: New
insights into human minimal change disease: Lessons from animal
models. Am J Kidney Dis. 59:284–292. 2012.PubMed/NCBI View Article : Google Scholar
|
|
15
|
Clement LC, Macé C, Avila-Casado C, Joles
JA, Kersten S and Chugh SS: Circulating angiopoietin-like 4 links
proteinuria with hypertriglyceridemia in nephrotic syndrome. Nat
Med. 20:37–46. 2014.PubMed/NCBI View
Article : Google Scholar
|
|
16
|
Zhu P, Tan MJ, Huang RL, Tan CK, Chong HC,
Pal M, Lam CRI, Boukamp P, Pan JY, Tan SH, et al: Angiopoietin-like
4 protein elevates the prosurvival intracellular O2(-):H2O2 ratio
and confers anoikis resistance to tumors. Cancer Cell. 19:401–415.
2011.PubMed/NCBI View Article : Google Scholar
|
|
17
|
Zhang T, Niu X, Liao L, Cho EA and Yang H:
The contributions of HIF-target genes to tumor growth in RCC. PLoS
One. 8(e80544)2013.PubMed/NCBI View Article : Google Scholar
|
|
18
|
Dong D, Jia L, Zhou Y, Ren L, Li J and
Zhang J: Serum level of ANGPTL4 as a potential biomarker in renal
cell carcinoma. Urol Oncol. 35:279–285. 2017.PubMed/NCBI View Article : Google Scholar
|
|
19
|
Ge H, Yang G, Yu X, Pourbahrami T and Li
C: Oligomerization state-dependent hyperlipidemic effect of
angiopoietin-like protein 4. J Lipid Res. 45:2071–2079.
2004.PubMed/NCBI View Article : Google Scholar
|
|
20
|
Yin W, Romeo S, Chang S, Grishin NV, Hobbs
HH and Cohen JC: Genetic variation in ANGPTL4 provides insights
into protein processing and function. J Biol Chem. 284:13213–13222.
2009.PubMed/NCBI View Article : Google Scholar
|
|
21
|
Clement LC, Avila-Casado C, Macé C, Soria
E, Bakker WW, Kersten S and Chugh SS: Podocyte-secreted
angiopoietin-like-4 mediates proteinuria in
glucocorticoid-sensitive nephrotic syndrome. Nat Med. 17:117–122.
2011.PubMed/NCBI View
Article : Google Scholar
|
|
22
|
La Paglia L, Listì A, Caruso S, Amodeo V,
Passiglia F, Bazan V and Fanale D: Potential role of ANGPTL4 in the
cross talk between metabolism and cancer through PPAR signaling
pathway. PPAR Res. 2017(8187235)2017.PubMed/NCBI View Article : Google Scholar
|
|
23
|
Wang Q, Oliver-Williams C, Raitakari OT,
Viikari J, Lehtimäki T, Kähönen M, Järvelin MR, Salomaa V, Perola
M, Danesh J, et al: Metabolic profiling of angiopoietin-like
protein 3 and 4 inhibition: A drug-target Mendelian randomization
analysis. Eur Heart J. 42:1160–1169. 2021.PubMed/NCBI View Article : Google Scholar
|
|
24
|
Kubo H, Kitajima Y, Kai K, Nakamura J,
Miyake S, Yanagihara K, Morito K, Tanaka T, Shida M and Noshiro H:
Regulation and clinical significance of the hypoxia-induced
expression of ANGPTL4 in gastric cancer. Oncol Lett. 11:1026–1034.
2016.PubMed/NCBI View Article : Google Scholar
|
|
25
|
Vivarelli M, Massella L, Ruggiero B and
Emma F: Minimal change disease. Clin J Am Soc Nephrol. 12:332–345.
2017.PubMed/NCBI View Article : Google Scholar
|
|
26
|
Shalhoub RJ: Pathogenesis of lipoid
nephrosis: A disorder of T-cell function. Lancet. 2:556–560.
1974.PubMed/NCBI View Article : Google Scholar
|
|
27
|
Yokoyama H, Kida H, Tani Y, Abe T,
Tomosugi N, Koshino Y and Hattori N: Immunodynamics of minimal
change nephrotic syndrome in adults T and B lymphocyte subsets and
serum immunoglobulin levels. Clin Exp Immunol. 61:601–607.
1985.PubMed/NCBI
|
|
28
|
Kimata H, Fujimoto M and Furusho K:
Involvement of interleukin (IL)-13, but not IL-4, in spontaneous
IgE and IgG4 production in nephrotic syndrome. Eur J Immunol.
25:1497–1501. 1995.PubMed/NCBI View Article : Google Scholar
|
|
29
|
Kanai T, Shiraishi H, Yamagata T, Ito T,
Odaka J, Saito T, Aoyagi J and Momoi MY: Th2 cells predominate in
idiopathic steroid-sensitive nephrotic syndrome. Clin Exp Nephrol.
14:578–583. 2010.PubMed/NCBI View Article : Google Scholar
|
|
30
|
Nachman PH, Jennette JC and Falk R:
Primary glomerular disease. In: The Kidney. Brenner BM (ed). 8th
edition. Elsevier, Philadelphia, PA, pp987-1066, 2008.
|
|
31
|
Pei Y, Cattran D, Delmore T, Katz A, Lang
A and Rance P: Evidence suggesting under-treatment in adults with
idiopathic focal segmental glomerulosclerosis. Regional
glomerulonephritis registry study. Am J Med. 82:938–944.
1987.PubMed/NCBI View Article : Google Scholar
|
|
32
|
Reiser J, von Gersdorff G, Loos M, Oh J,
Asanuma K, Giardino L, Rastaldi MP, Calvaresi N, Watanabe H,
Schwarz K, et al: Induction of B7-1 in podocytes is associated with
nephrotic syndrome. J Clin Invest. 113:1390–1397. 2004.PubMed/NCBI View
Article : Google Scholar
|
|
33
|
Liu S and Chen J: New insight in
pathogenesis of podocyte disfunction in minimal change disease.
Zhejiang Da Xue Xue Bao Yi Xue Ban. 45:214–218. 2016.PubMed/NCBI View Article : Google Scholar : (In Chinese).
|
|
34
|
Kaneko K, Tsuji S, Kimata T, Kitao T,
Yamanouchi S and Kato S: Pathogenesis of childhood idiopathic
nephrotic syndrome: A paradigm shift from T-cells to podocytes.
World J Pediatr. 11:21–28. 2015.PubMed/NCBI View Article : Google Scholar
|
|
35
|
Chugh SS, Macé C, Clement LC, Del Nogal
Avila M and Marshall CB: Angiopoietin-like 4 based therapeutics for
proteinuria and kidney disease. Front Pharmacol.
5(23)2014.PubMed/NCBI View Article : Google Scholar
|
|
36
|
Li Y, Xu Z, Deng H, Liu M, Lin X, Zhang M,
Li G, Yue S and Gao X: ANGPTL4 promotes nephrotic syndrome by
downregulating podocyte expression of ACTN4 and podocin. Biochem
Biophys Res Commun. 639:176–182. 2023.PubMed/NCBI View Article : Google Scholar
|
|
37
|
McCarthy KJ and Wassenhove-McCarthy DJ:
The glomerular basement membrane as a model system to study the
bioactivity of heparan sulfate glycosaminoglycans. Microsc
Microanal. 18:3–21. 2012.PubMed/NCBI View Article : Google Scholar
|
|
38
|
Jia S, Peng X, Liang L, Zhang Y, Li M,
Zhou Q, Shen X, Wang Y, Wang C, Feng S, et al: The study of
Angptl4-modulated podocyte injury in IgA nephropathy. Front
Physiol. 11(575722)2021.PubMed/NCBI View Article : Google Scholar
|
|
39
|
Zuo Y, He Z, Chen Y and Dai L: Dual role
of ANGPTL4 in inflammation. Inflamm Res. 72:1303–1313.
2023.PubMed/NCBI View Article : Google Scholar
|
|
40
|
Davin JC: The glomerular permeability
factors in idiopathic nephrotic syndrome. Pediatr Nephrol.
31:207–215. 2016.PubMed/NCBI View Article : Google Scholar
|
|
41
|
Li Y, Gong W, Liu J, Chen X, Suo Y, Yang H
and Gao X: Angiopoietin-like protein 4 promotes
hyperlipidemia-induced renal injury by down-regulating the
expression of ACTN4. Biochem Biophys Res Commun. 595:69–75.
2022.PubMed/NCBI View Article : Google Scholar
|
|
42
|
Bertelli R, Bonanni A, Caridi G, Canepa A
and Ghiggeri GM: Molecular and cellular mechanisms for proteinuria
in minimal change disease. Front Med (Lausanne).
5(170)2018.PubMed/NCBI View Article : Google Scholar
|
|
43
|
Li JS, Chen X, Peng L, Wei SY, Zhao SL,
Diao TT, He YX, Liu F, Wei QJ, Zhang QF and Li B:
Angiopoietin-like-4, a potential target of tacrolimus, predicts
earlier podocyte injury in minimal change disease. PLoS One.
10(e0137049)2015.PubMed/NCBI View Article : Google Scholar
|
|
44
|
Li S, Nagothu K, Ranganathan G, Ali SM,
Shank B, Gokden N, Ayyadevara S, Megyesi J, Olivecrona G, Chugh SS,
et al: Reduced kidney lipoprotein lipase and renal tubule
triglyceride accumulation in cisplatin-mediated acute kidney
injury. Am J Physiol Renal Physiol. 303:F437–F448. 2012.PubMed/NCBI View Article : Google Scholar
|
|
45
|
Avila-Casado Mdel C, Perez-Torres I, Auron
A, Soto V, Fortoul TI and Herrera-Acosta J: Proteinuria in rats
induced by serum from patients with collapsing glomerulopathy.
Kidney Int. 66:133–143. 2004.PubMed/NCBI View Article : Google Scholar
|
|
46
|
Shen X, Weng C, Wang Y, Wang C, Feng S, Li
X, Li H, Jiang H, Wang H and Chen J: Lipopolysaccharide-induced
podocyte injury is regulated by calcineurin/NFAT and
TLR4/MyD88/NF-κB signaling pathways through angiopoietin-like
protein 4. Genes Dis. 9:443–455. 2020.PubMed/NCBI View Article : Google Scholar
|
|
47
|
Hayek SS, Sever S, Ko YA, Trachtman H,
Awad M, Wadhwani S, Altintas MM, Wei C, Hotton AL, French AL, et
al: Soluble urokinase receptor and chronic kidney disease. N Engl J
Med. 373:1916–1925. 2015.PubMed/NCBI View Article : Google Scholar
|
|
48
|
Schulz CA, Persson M, Christensson A,
Hindy G, Almgren P, Nilsson PM, Melander O, Engström G and
Orho-Melander M: Soluble urokinase-type plasminogen activator
receptor (suPAR) and impaired kidney function in the
population-based Malmö diet and cancer study. Kidney Int Rep.
2:239–247. 2017.PubMed/NCBI View Article : Google Scholar
|
|
49
|
Siligato R, Cernaro V, Nardi C, De
Gregorio F, Gembillo G, Costantino G, Conti G, Buemi M and Santoro
D: Emerging therapeutic strategies for minimal change disease and
focal and segmental glomerulosclerosis. Expert Opin Investig Drugs.
27:839–879. 2018.PubMed/NCBI View Article : Google Scholar
|
|
50
|
Botta M, Audano M, Sahebkar A, Sirtori CR,
Mitro N and Ruscica M: PPAR agonists and metabolic syndrome: An
established role? Int J Mol Sci. 19(1197)2018.PubMed/NCBI View Article : Google Scholar
|
|
51
|
Yang HC, Ma LJ, Ma J and Fogo AB:
Peroxisome proliferator-activated receptor-gamma agonist is
protective in podocyte injury-associated sclerosis. Kidney Int.
69:1756–1764. 2006.PubMed/NCBI View Article : Google Scholar
|
|
52
|
Qiu W, Huang L, Li Y, Liu Q and Lv Y:
Dysregulation of angiopoietin-like-4 associated with
hyperlipidemia-induced renal injury by AMPK/ACC pathway. Curr Pharm
Des. 29:300–309. 2023.PubMed/NCBI View Article : Google Scholar
|
|
53
|
Kersten S, Mandard S, Tan NS, Escher P,
Metzger D, Chambon P, Gonzalez FJ, Desvergne B and Wahli W:
Characterization of the fasting-induced adipose factor FIAF, a
novel peroxisome proliferator-activated receptor target gene. J
Biol Chem. 275:28488–28493. 2000.PubMed/NCBI View Article : Google Scholar
|
|
54
|
Chen S, McLean S, Carter DE and Leask A:
The gene expression profile induced by Wnt 3a in NIH 3T3
fibroblasts. J Cell Commun Signal. 1:175–183. 2007.PubMed/NCBI View Article : Google Scholar
|
|
55
|
Lu R and Zhou J, Liu B, Liang N, He Y, Bai
L, Zhang P, Zhong Y, Zhou Y and Zhou J: Paeoniflorin ameliorates
adriamycin-induced nephrotic syndrome through the PPARγ/ANGPTL4
pathway in vivo and vitro. Biomed Pharmacother. 96:137–147.
2017.PubMed/NCBI View Article : Google Scholar
|
|
56
|
Xin X, Rodrigues M, Umapathi M,
Kashiwabuchi F, Ma T, Babapoor-Farrokhran S, Wang S, Hu J, Bhutto
I, Welsbie DS, et al: Hypoxic retinal Muller cells promote vascular
permeability by HIF-1-dependent up-regulation of angiopoietin-like
4. Proc Natl Acad Sci USA. 110:E3425–E3434. 2013.PubMed/NCBI View Article : Google Scholar
|
|
57
|
Hu K, Babapoor-Farrokhran S, Rodrigues M,
Deshpande M, Puchner B, Kashiwabuchi F, Hassan SJ, Asnaghi L, Handa
JT, Merbs S, et al: Hypoxia-inducible factor 1 upregulation of both
VEGF and ANGPTL4 is required to promote the angiogenic phenotype in
uveal melanoma. Oncotarget. 7:7816–7828. 2016.PubMed/NCBI View Article : Google Scholar
|
|
58
|
Wang X, Qi D, Fu F, Li X, Liu Y, Ji K, Gao
Z, Kong L, Yu C, Xie H, et al: Therapeutic and antiproteinuric
effects of salvianolic acid A in combined with low-dose prednisone
in minimal change disease rats: Involvement of PPARγ/Angptl4 and
Nrf2/HO-1 pathways. Eur J Pharmacol. 858(172342)2019.PubMed/NCBI View Article : Google Scholar
|
|
59
|
Liu G and He L: Epigallocatechin-3-gallate
attenuates adriamycin-induced focal segmental glomerulosclerosis
via suppression of oxidant stress and apoptosis by targeting
hypoxia-inducible factor-1α/angiopoietin-like 4 pathway.
Pharmacology. 103:303–314. 2019.PubMed/NCBI View Article : Google Scholar
|
|
60
|
Del Nogal-Avila M, Donoro-Blazquez H, Saha
MK, Marshall CB, Clement LC, Macé CE and Chugh SS: Novel
therapeutic approaches for chronic kidney disease due to glomerular
disorders. Am J Physiol Renal Physiol. 311:F63–F65. 2016.PubMed/NCBI View Article : Google Scholar
|