Introduction
Primary percutaneous coronary intervention (PCI) is,
at present, the most commonly used management strategy for acute
myocardial infarction (AMI) with ST-segment elevations. However, a
significant number of patients receiving PCI fail to achieve
complete and sustained myocardial reperfusion and therefore remain
at risk of developing large infarcts (1). The in-hospital mortality of patients
with AMI undergoing PCI is between 4 and 7% (2). The poor outcome amongst these
patients has been attributed to the effects of the restoration of
blood flow to previously ischemic tissue (3). Increases in knowledge have revealed
that the common pathophysiological scenario, myocardial ischemia
reperfusion injury, including ischemia/reperfusion (I/R) and
hypoxia/reoxygenation (H/R) forms of injury, results in depressed
myocardial function and harmful morphological alterations, which
may lead to heart failure (4).
Additionally, it may clinically manifest with myocardial necrosis,
cardiac arrhythmia, myocardial stunning and microvascular
dysfunction (5). Previous studies
have identified apoptosis as a significant mechanism underlying
cell death during I/R injury in cultured cardiac myocytes (6,7), and
that the inhibition of this apoptosis is able to prevent I/R injury
(8).
Green tea, a beverage consumed worldwide, has been
suggested to possess significant health-promoting effects, while
polyphenol (−)-epigallocatechin-3-gallate (EGCG), the predominant
catechin from tea, has been reported to exert a variety of
beneficial cardiovascular effects by influencing the activity of
receptor and signal transduction kinases (9). In addition, the consumption of green
tea by humans has been hypothesized to be associated with a lower
incidence of coronary artery disease (10). A previous study identified that
in vivo treatment with EGCG reduced I/R injury by inhibiting
the nuclear factor-κB and activator protein 1 pathways in rat
hearts (11). In addition,
Townsend et al (12)
reported that EGCG reduced signal transducers and activators of
transcription-1 phosphorylation and protected cardiac myocytes
against I/R-induced apoptotic cell death in isolated rat hearts.
Furthermore, administration of EGCG in vitro was observed to
prevent apoptosis of cardiomyocytes by regulating pro-apoptotic and
anti-apoptotic proteins, including B cell lymphoma-2 (Bcl-2) and
Bcl-2-associated X protein, and by simultaneously regulating
caspase-3 in isolated rat hearts (13). EGCG has been suggested to inhibit
cardiac myocyte apoptosis by preventing telomere shortening and
telomere repeat-binding factor 2 loss (14). Therefore, EGCG may function as an
effective anti-apoptotic agent.
Several previous studies have focused on evaluating
the interactions of catechin with metal ions. Catechin interacts
with metal ions, particularly transitional metal ions, which lead
to alterations in the bioactivity of catechin (15,16).
Zinc has been reported to be an essential biometal, which has
various pleiotropic roles in biological systems (17). In reference to cell survival, zinc
has been demonstrated to exhibit anti-apoptotic effects, acting
either as an inorganic ion or as a key cofactor of various organic
molecules. Previous studies have suggested that the
cardioprotective effects of zinc against I/R injury are dependent
on its ability to activate phosphatidylinositol-3-kinase (PI3K)/Akt
signaling (18,19). It has been demonstrated that the
activation of PI3K/Akt results in the growth and survival of
cardiac myocytes. In addition, zinc-induced ErbB2 protein
expression provides a clue, indicating that ErbB2 may act upstream
of Akt activation and be essential in preventing reperfusion injury
(18). These results have
significance with regard to the preventive effects of zinc on
cardiomyocytes against H/R-induced apoptosis.
Preliminary investigations led to the development of
the process of ischemic preconditioning, which is a
cardioprotective method against the development of irreversible
damage following I/R, and demonstrates that I/R injury may be
attenuated (20). The prophylactic
use of pharmacological agents mimicking the effects of ischemic
preconditioning may represent an effective strategy for reducing
the extent of myocardial damage resulting from I/R or H/R. The
PI3K/Akt pathway has been reported to be essential for
cardioprotection in response to ischemic preconditioning (21). In a previous study, the
anti-apoptotic effects of EGCG were observed in cardiomyocytes
(12); however, it was reported
that EGCG attenuated the I/R-induced phosphorylation of Akt in
human umbilical vein endothelial cells (22). Thus, the role of EGCG and zinc in
preconditioning and toxicity in H9c2 cells and its underlying
mechanism of action are beginning to be elucidated. In the present
study, the effectiveness of EGCG with exogenous zinc at an
optimized concentration in terms of biological activity at
ameliorating H/R injury was investigated using H9c2 cells in
vitro. The biochemical mechanism underlying the
cardio-protective effects was investigated by examining alterations
in the expression levels of phosphorylated (p)-Akt and cleaved
caspase-3 activity in the H9c2 cell model of H/R, in addition to
the effects of EGCG and zinc on cell viability following H/R
injury.
Materials and methods
Chemicals
Purified EGCG (>98%), zinc chloride, Dulbecco’s
modified Eagle’s medium (DMEM) and fetal bovine serum (FBS) were
purchased from Sigma-Aldrich (St. Louis, MO, USA). Human H9c2 cells
were purchased from the Shanghai Institute of Cell Biology, Chinese
Academy of Sciences (Shanghai, China). Western blotting was
performed using specific antibodies against p-Akt and cleaved
caspase-3 (Santa Cruz Biotechnology, Inc., Santa Cruz, CA, USA).
All other chemicals were of extra-pure or analytical grade unless
otherwise specified.
Treatment of H9c2 cells
H9c2 cells were maintained in DMEM supplemented with
10% FBS, 2% l-glutamine, 10% sodium bicarbonate, 10% sodium
pyruvate, 5% Hepes, 1% penicillin/streptomycin and 1% gentamycin
(Sangon Biotech Co., Ltd., Shanghai, China) in an incubator (37°C,
95% air + 5% CO2). The cells were cultured for 1–2 days
under these normal conditions, until they reached 90% confluence
prior to anoxic treatment. EGCG (0, 5, 10, 15 and 20 µM) and
Zn2+ (0, 5, 10, 15 and 20 µM) were added to the
myocytes 30 min prior to reoxygenation. Hypoxic stress was
implemented by incubating cultured H9c2 cells in serum- and
glucose-free DMEM. The culture dish was placed in an airtight
incubator at 37°C under an atmosphere of 95% N2 and 5%
CO2 for 3 h followed by reoxygenation for 1 h in normal
(37°C, 95% air + 5% CO2) conditions with 10% FBS-DMEM.
EGCG and Zn2+ at various concentrations were added 30
min prior to the reoxygenation. Myocytes not exposed to H/R served
as normoxic controls. At the end of the H/R treatment, myocytes
were examined for viability and apoptosis by Hoechst 33258
(Beyotime Institute of Biotechnology, Haimen, China) staining and
western blot analysis.
MTT assays
MTT assays were performed in order to determine the
effects of EGCG and Zn2+ on the growth of H9c2 cells.
Cells were plated in 96-well tissue culture plates and treated with
varying doses of EGCG (0, 5, 10, 15 and 20 µM) or
Zn2+ (0, 5, 10, 15 and 20 µM) for 6, 12 and 24 h
at 37°C in an atmosphere containing 5% CO2 and 95% air.
Following completion of the treatment, cells were washed with
phosphate-buffered saline (PBS; Beyotime Institute of
Biotechnology) and 50 µl MTT (5 mg/ml; Sigma-Aldrich) was
added. The cells were subsequently incubated for 4 h at 37°C to
allow for the formation of formazan precipitate, which was
dissolved in dimethyl sulfoxide (Sigma-Aldrich). The absorbance at
490 nm in each well was then measured with a Multiskan Ascent ELISA
reader (Thermo Fisher Scientific, Waltham, MA, USA). The cell
viability was defined relative to that of the untreated control
cells as follows: Cell viability = absorbance of treated
sample/absorbance of control.
The results of the aforementioned experiments
revealed that the optimal concentrations of EGCG and
Zn2+ were 10 µM and 5 µM, respectively.
Subsequently, these optimal concentrations of EGCG and
Zn2+ were added to three groups of H9c2 cells (group I,
10 µM EGCG; group II, 5 µM Zn2+ and group
III, 10 µM EGCG + 5 µM Zn2+) in order to
investigate their toxicity. The treated cells were incubated for 24
h at 37°C and their viability was determined by MTT assays.
Morphological analysis of H9c2 cells
adhering to the plate
H9c2 cells were equally seeded at a density of
2×105 cells/well in six-well plates (20 × 20 mm) for 24
h and were subsequently randomly divided into five groups (A, B, C,
D and E). Group A (H/R group) was exposed to 3-h simulated anoxia
followed by 1-h re-oxygenation. In group B, EGCG was added at a
dose of 10 µM prior to 3-h simulated anoxia followed by 1-h
reoxygenation. In group C, Zn2+ was added at a dose of 5
µM prior to hypoxia treatment. In group D, EGCG was added at
a dose of 10 µM with 5 µM Zn2+ prior to
hypoxia treatment. In group E, the PI3K inhibitor LY294002 [0.5
µM/0.57 µM/0.97 µM (PI3Kα/δ/β) Sigma-Aldrich]
was added with EGCG and Zn2+ simultaneously. Cells
without treatment were considered as the controls. Subsequent to
treatment, microscopic images of H9c2 cells adhering to the plate
were captured using an inverted microscope at a magnification of
x200 (CKX41SF; Olympus Corp., Tokyo, Japan).
Hoechst 33258 staining
Cells of groups A–E were washed twice in cold PBS
and fixed in 4% formaldehyde (Sangon Biotech Co., Ltd.) at 4°C for
10 min. Subsequently, the fixed cells were washed and labeled with
Hoechst 33258 (5 µg/ml) at room temperature in the dark for
10 min. The cells were then observed and imaged using a
fluorescence inverted microscope (Eclipse TE2000-S; Nikon Corp.,
Tokyo, Japan) with excitation at 350 nm and emission at 460 nm.
Western blot analysis of protein
expression
H9c2 cells were seeded in 100-mm cell culture dishes
at a density of 2×106 cells/well and incubated according
to the aforementioned time-temperature protocol. Cells were lysed
in a whole cell extract buffer (Sigma-Aldrich). Protein
concentration was determined using a Bicinchoninic Acid Protein
Assay kit, according to the manufacturer’s instructions (Beyotime
Institute of Biotechnology). Protein samples of the whole cell
lysate were mixed with an equal volume of 5X SDS sample buffer
(Beyotime Institute of Biotechnology), boiled for 5 min and then
separated by 8–15% SDS-PAGE (Beyotime Institute of Biotechnology).
Following electrophoresis (Mini-PROTEAN 3 cell; Bio-Rad
Laboratories, Inc., Hercules, CA, USA), the proteins were
transferred to nitrocellulose membranes (Beyotime Institute of
Biotechnology). The membranes were blocked in 5% non-fat dried milk
for 1 h, rinsed and incubated with the following antibodies: Mouse
monoclonal anti-p-Akt (cat. no. 2920) and rabbit monoclonal cleaved
caspase-3 (cat. no. 9664) in PBS containing 0.1% Tween-20 (PBS-T)
overnight at 4°C. The primary antibodies were removed by washing
the membranes three times in PBS-T, which were then incubated for 1
h with horseradish peroxidase-conjugated goat anti-rabbit (cat. no.
7074) and horse anti-mouse (cat. no. 7076) immunoglobulin G
secondary antibodies (Cell Signaling Technology, Inc., Danvers, MA,
USA). Following three washes with PBS-T, immunopositive bands were
visualized using chemiluminescent reagent (Beyotime Institute of
Biotechnology) and exposed to X-ray film (Thermo Fisher
Scientific).
Statistical analysis
Data were expressed as the mean ± standard
deviation. Statistical differences were analyzed using a one-way
analysis of variance followed by the least significant difference
test, to determine significant differences within groups. P<0.05
was considered to indicate a statistically significant difference
in all calculations. Statistical analyses were performed using
SPSS, version 17.0 (SPSS, Inc., Chicago, IL, USA).
Results
Viability of H9c2 cells in the presence
of EGCG and Zn2+
To analyze cell survival, cells were cultured with
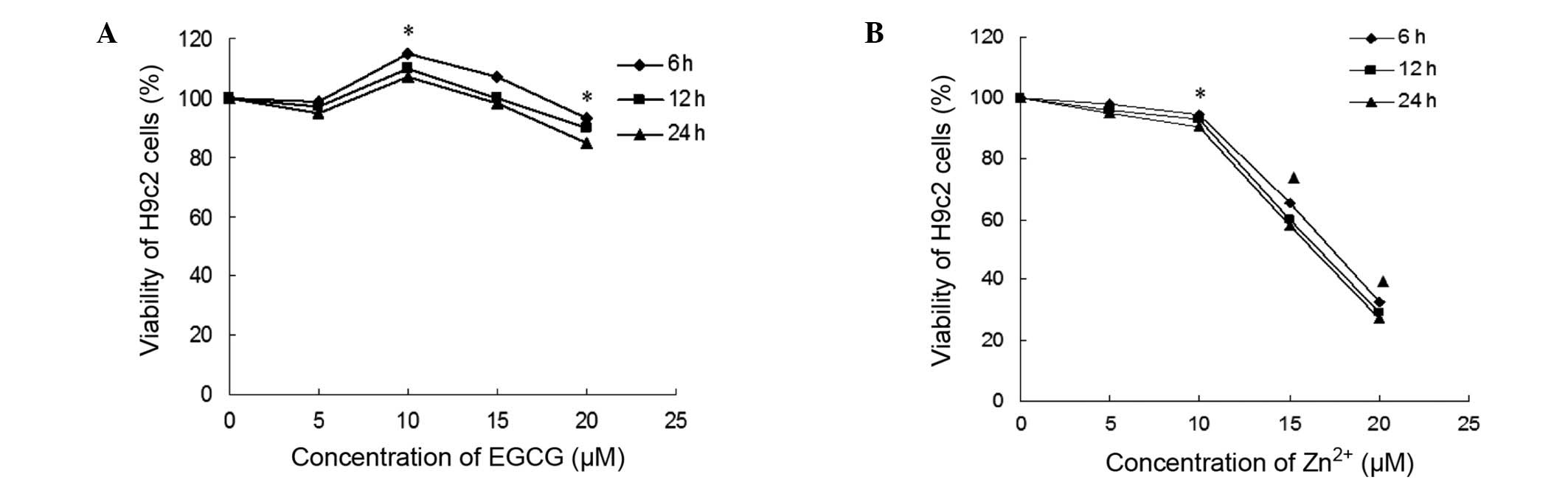
various concentrations of EGCG and Zn2+. As presented in
Fig. 1, treatment with low
concentrations of EGCG (<5 µM) and Zn2+
(<10 µM) resulted in no significant alterations in H9c2
cell growth. Treatment with 10 µM EGCG significantly
increased the viability of H9c2 cells compared with that of the
control group. By contrast, treatment with high concentrations of
EGCG (>20 µM) resulted in a significant loss of cell
viability. Zn2+ administration at concentrations of 0–5
µM resulted in no significant alterations in H9c2 cell
growth. However, treatment with high concentrations (>10
µM) of Zn2+ resulted in a significant loss of
cell viability, with a sharp reduction at concentrations of 15–20
µM. Therefore, the optimal concentrations were proposed to
be 10 µM for EGCG and 5 µM for Zn2+.
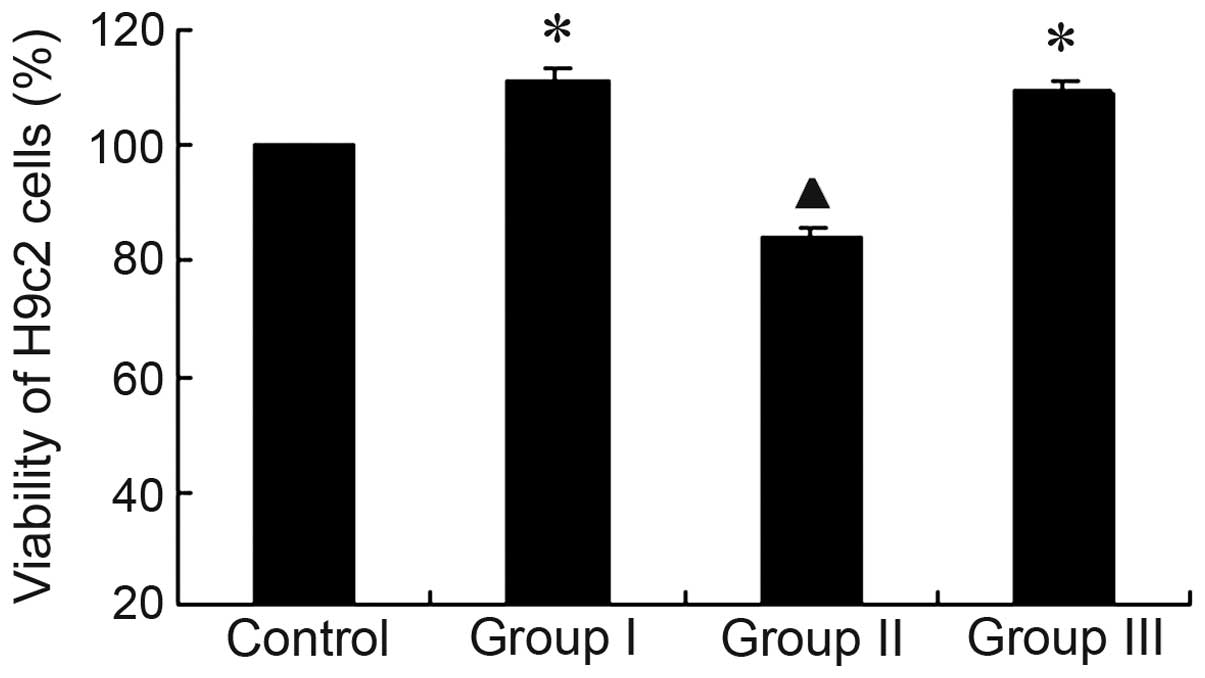
Subsequently, the identified optimal concentrations
of EGCG (10 µM) and Zn2+ (5 µM) were added
to three groups of H9c2 cells (group I, 10 µM EGCG; group
II, 5 µM Zn2+; and group III, 10 µM EGCG +
5 µM Zn2+) in order to investigate their
toxicity. As demonstrated in Fig.
2, no significant alterations in toxicity were observed in
group III when compared with group I.
EGCG + Zn2+ treatment prevents
morphological variations of H9c2 cells following H/R injury
Morphological variations of H9c2 cells treated with
EGCG, Zn2+ and EGCG + Zn2+ with and without
LY294002 were observed through an inverted microscope. As indicated
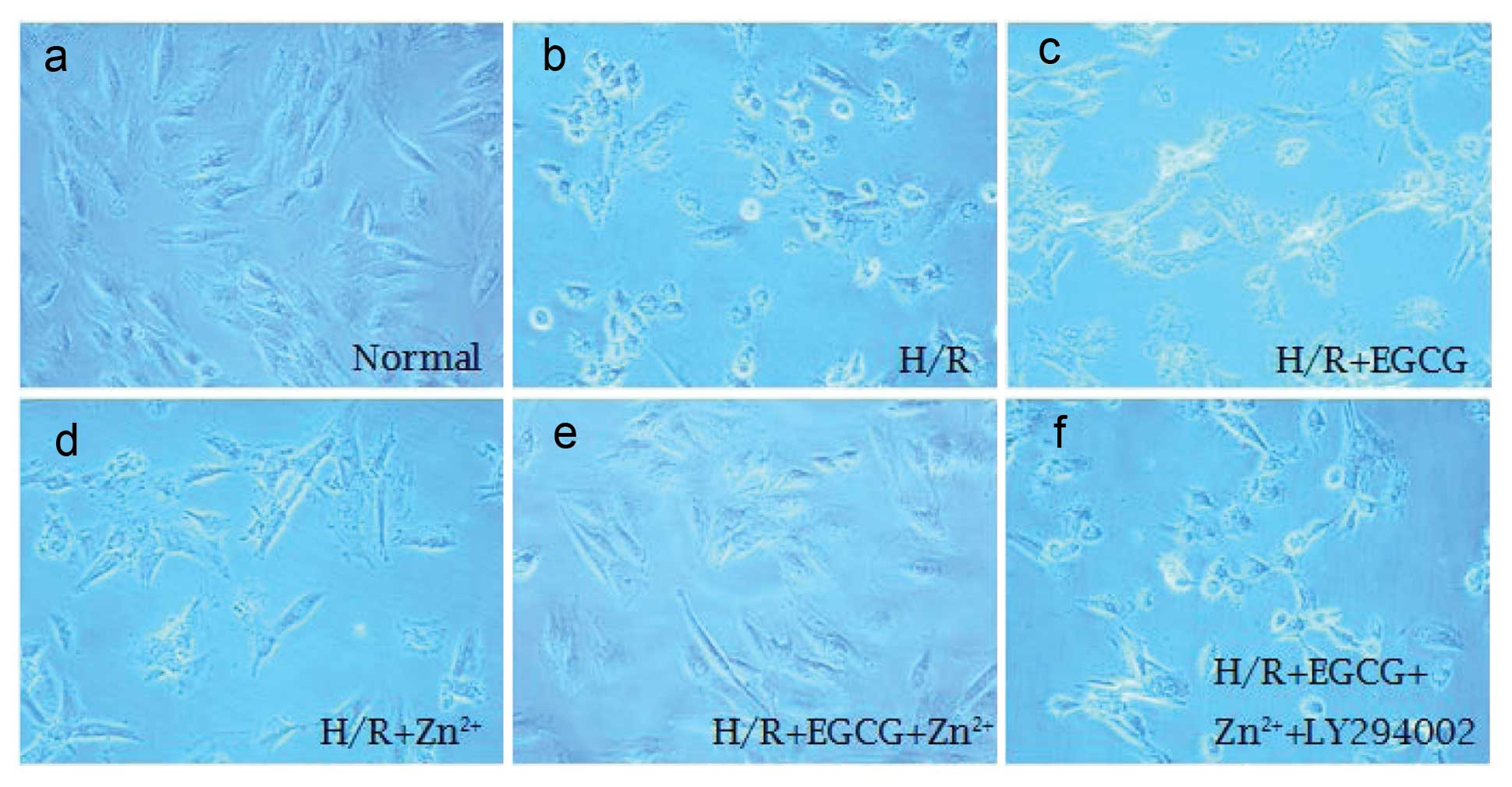
in Fig. 3, normal H9c2 cells
adhered to the plate uniformly, with a filamentous shape (Fig. 3a). When exposed to H/R injury, H9c2
cells appeared to exhibit morphological variations, becoming round
or irregular in shape, which indicated the cytotoxic capacity of
H/R injury (Fig. 3b). Following
pretreatment with Zn2+, the extent of cell damage was
attenuated (Fig. 3d). When exposed
to the mixture of EGCG and Zn2+, H9c2 cells exhibited no
significant morphological variations, as compared with the other
groups, with the majority of cells remaining a normal shape
following H/R injury (Fig. 3e). No
significant differences were observed in cell morphology between
the H/R group and the cells treated with EGCG alone (Fig. 3c) or the PI3K inhibitor LY294002
(Fig. 3f).
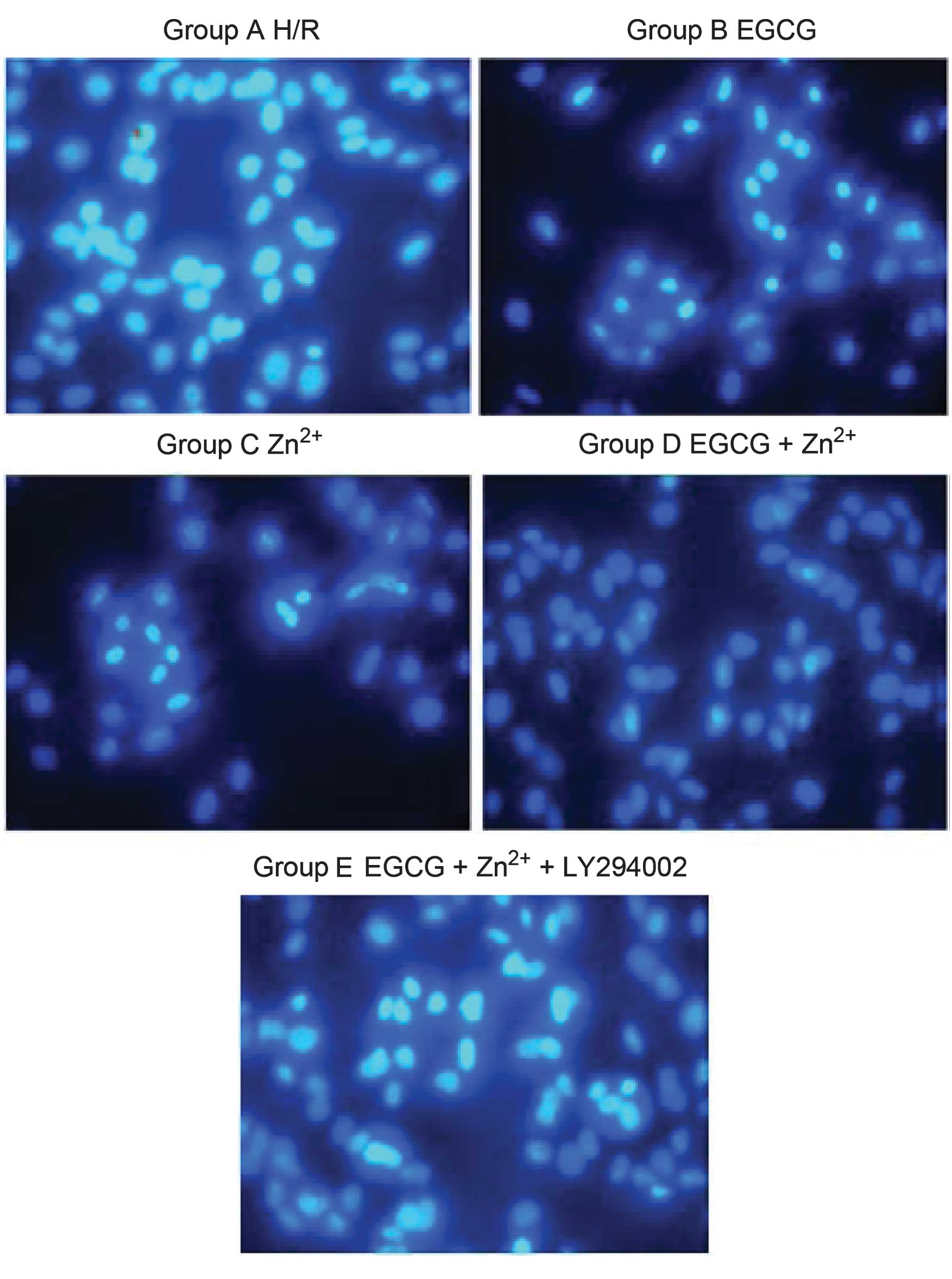
The Hoechst 33258 dye was able to diffuse through
the intact membranes of H9c2 cells and stain their DNA, thus
assessing the levels of apoptotic cell death. Apoptosis was
confirmed by observing specific morphological alterations,
including reduction in cell volume and nuclear chromatin
condensation. Subsequent to staining, the H/R group was uniformly
stained with a significant fluorescent signal, and demonstrated
clear apoptotic morphology since the cells were condensed and
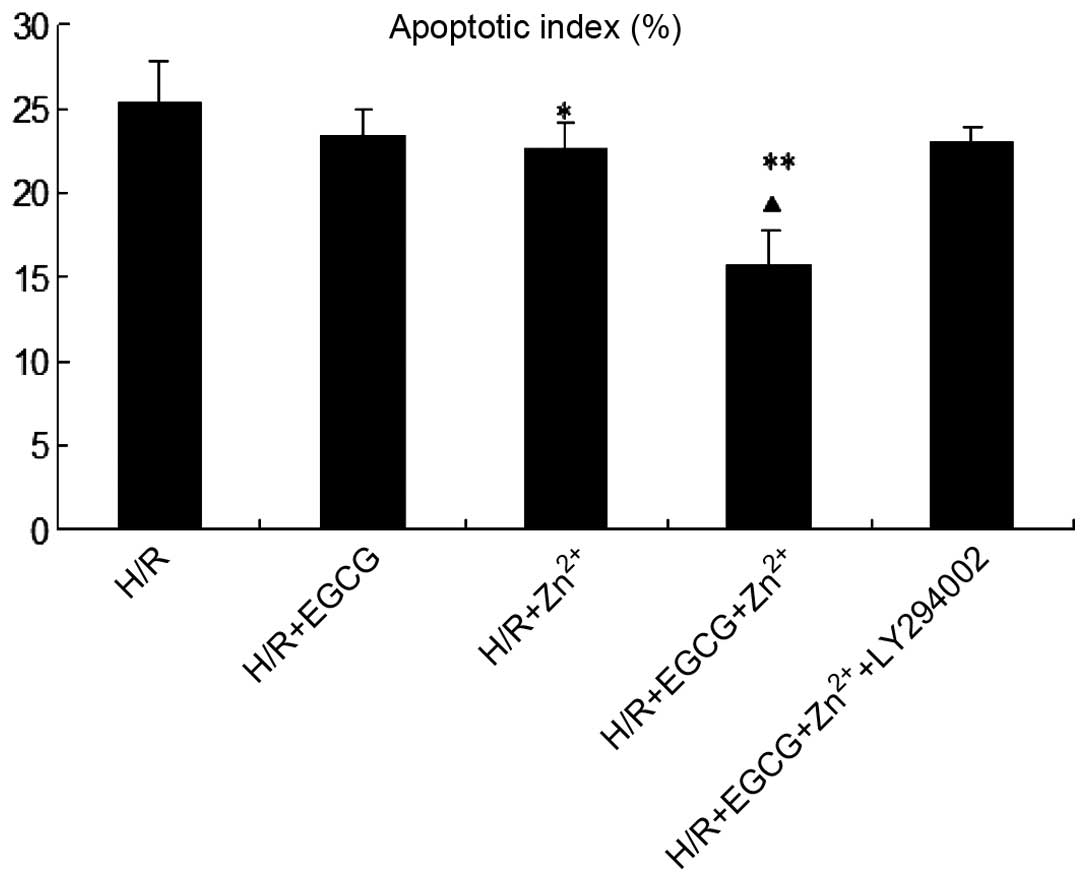
contained fragmented chromatin in their nuclei (Fig. 4). To investigate whether EGCG and
Zn2+ were cardio-protective, the number of apoptotic
cells was determined and expressed as a percentage of the apoptotic
index. The apoptotic index of H9c2 cells was determined as the
percentage of apoptotic cells over the total number of cells
counted, and a minimum of 500 cells were counted in each experiment
(Fig. 5). Treatment with EGCG +
Zn2+ significantly reduced the apototic index compared
with that of the H/R group (P<0.01) and the H/R +
Zn2+ group (P<0.01).
EGCG + Zn2+ treatment
significantly reduces cleaved caspase-3 expression and enhances
p-Akt expression in H9c2 cells
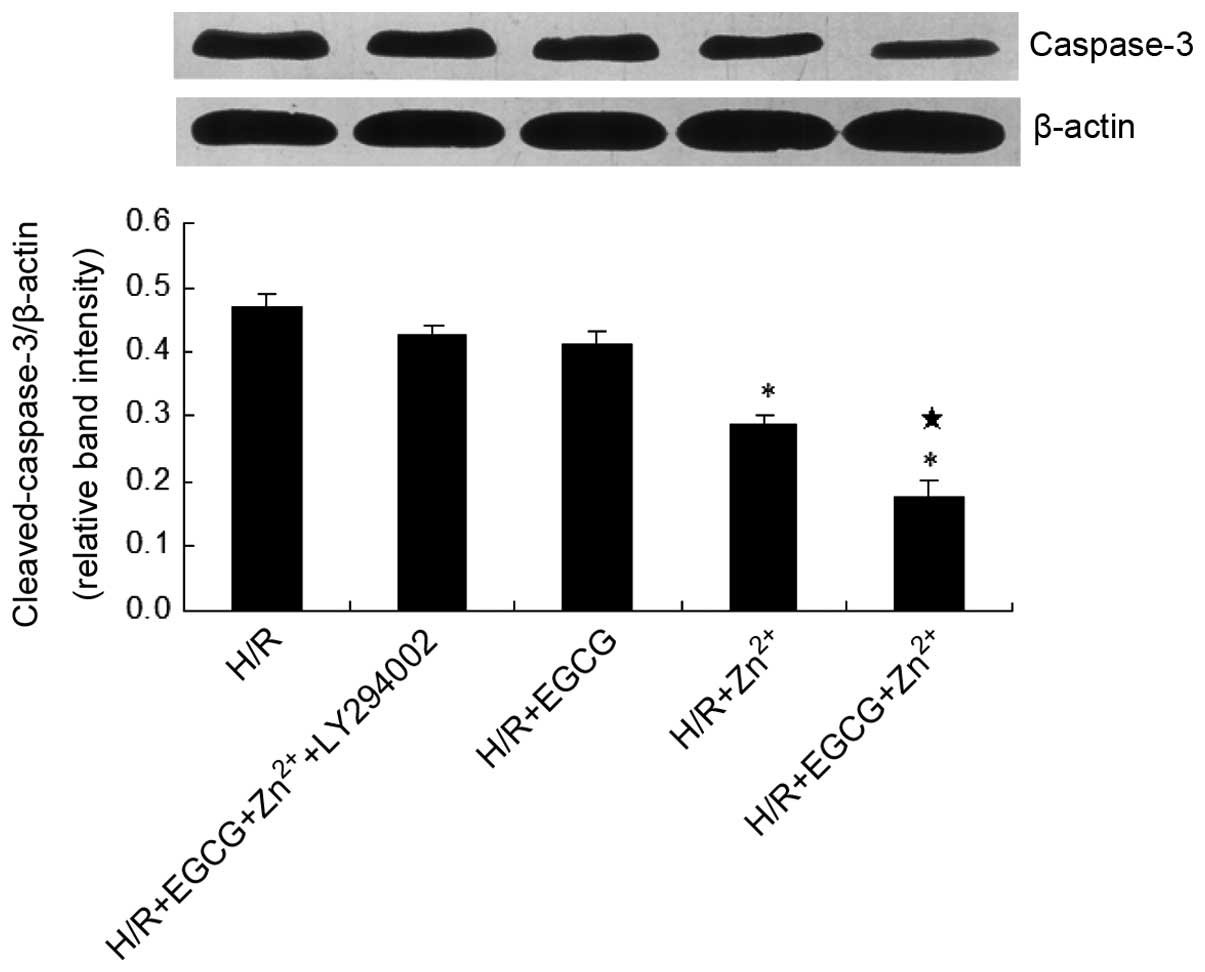
To explore the potential signaling pathways
contributing to the anti-apoptotic functions of EGCG and
Zn2+, the expression of cleaved caspase-3 was examined.
As indicated in Fig. 6, treatment
of H9c2 cells with Zn2+ in the presence or absence of
EGCG reduced the expression levels of cleaved caspase-3 when
compared with those of the H/R group. Furthermore, the EGCG +
Zn2+ group reduced the enhancement in the expression
levels of active caspase-3 following simulated H/R, compared with
those following Zn2+ treatment alone. By contrast, with
the addition of the PI3K inhibitor LY294002, the EGCG +
Zn2+ group exhibited no significant differences in
caspase-3 expression levels compared with those of the H/R group.
Thus, the anti-apoptotic effects of EGCG + Zn2+ may
occur as a result of reduced processing and activation of the
downstream effector caspase-3 in H9c2 cells exposed to H/R, thus
leading to a cardioprotective effect.
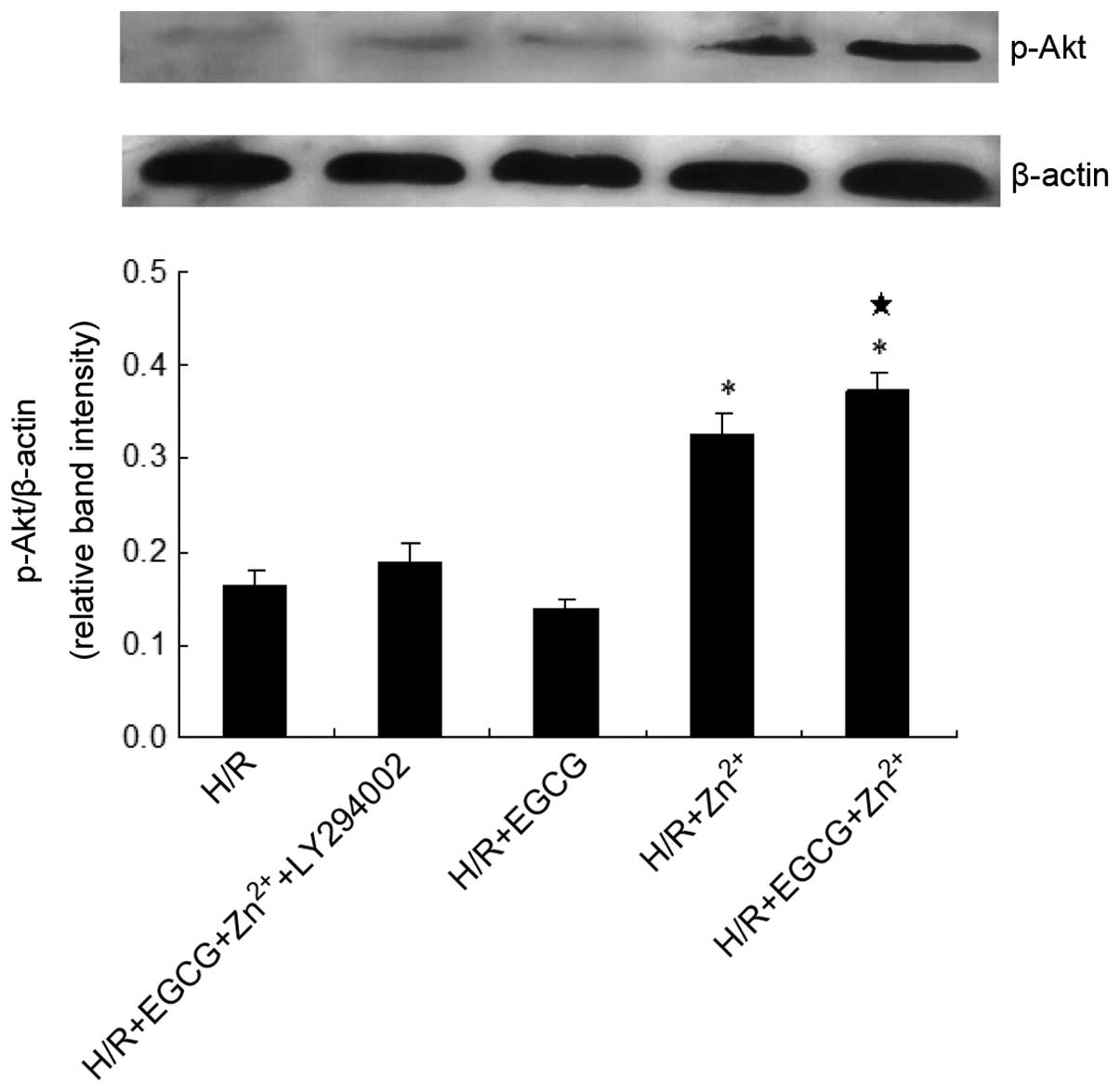
Protein expression levels of of p-Akt were measured
in order to determine whether EGCG and Zn2+ were able to
inhibit apoptosis by regulation of the expression of p-Akt via the
PI3K/Akt pathway. The results indicated that treatment with 10
µM EGCG + 5 µM Zn2+ significantly
increased the expression levels of p-Akt protein compared with
those of the H/R group. When treated with Zn2+ alone,
the expression levels of p-Akt were also increased (Fig. 7). The efficacy of the PI3K
inhibitor LY294002 was confirmed through the observed reduction in
p-Akt. When H9c2 cells were pre-incubated with this inhibitor, the
expression levels of p-Akt were significantly reduced compared with
those in the H/R + EGCG + Zn2+ group (P<0.05).
Therefore, these data suggested that the apoptotic effects of EGCG
+ Zn2+ on hypoxic stress-induced apoptosis of
cardiomyocytes were mediated, at least in part, through PI3K/Akt
signaling.
Discussion
I/R induces multiple modes of cellular injury and
death, and necrosis and apoptosis are suggested to be key
mediators. Necrosis describes pathological death of cells resulting
in irreversible damage, whereas apoptosis is characterized by
ATP-dependent programmed cell death, progressing via signaling
pathways that offer potential targets for therapeutic intervention
(8). Previous studies have
demonstrated that inhibiting caspases limits myocardial injury and
specifically individually inhibiting caspase-3, -8 and -9 limits
the infarct size in animal models (23,24).
Therefore, agents that possess anti-apoptotic activities may
provide therapeutic potential for the attenuation of I/R injury.
The PI3K/Akt pathway is known to be a target of I/R injury and
serves a critical role in cell survival by regulating
caspase-mediated apoptosis. In addition, activation of this
signaling pathway has been reported to have anti-apoptotic effects
in cardiomyocytes and other cell types (25,26).
A previous study demonstrated that the consumption
of tea, particularly green tea, is beneficial for the prevention of
cardiovascular disease (27).
Previous studies have attempted to take advantage of and enhance
the desirable bioactivities of green tea (9,28,29).
Investigations into the pharmaceutical activities of
metal-flavonoid complexes have additionally attracted research
interest. The desirable effects of flavonoids, including anticancer
and antioxidant effects, have been demonstrated to be enhanced by
metals. Kagaya et al (30)
observed that zinc was able to enhance the hepatoprotective effects
of EGCG in isolated rat hepatocytes, and it has also been reported
that exogenous zinc protects cardiomyocytes against H/R-induced
apoptosis by targeting the PI3k/Akt pathway (18). In addition, previous studies have
observed that the pretreatment with EGCG had protective effect on
INS-1 cells against oxidative stress via the enhancement of
anti-apoptosis signaling through increased levels of phosphorylated
PI3K and Akt (31). The effects of
EGCG on PI3K/Akt signaling in myoctyes remain to be fully
elucidated, and little is known about the actions of EGCG +
Zn2+ on H/R-induced H9c2 cell growth and apoptosis and
the associated intracellular signaling pathways.
The results of the present study indicated that
pretreatment with 10 µM EGCG resulted in no significant
effects on apoptosis when compared with the H/R group; however,
Zn2+ treatment reduced the apoptotic index at
concentrations of 5 µM. In addition, the apoptotic index
following treatment with EGCG + Zn2+ was observed to be
significantly reduced compared with that following Zn2+
treatment alone. The signaling pathways involved in this
cardioprotective effect were subsequently evaluated. Furthermore,
no significant alterations in the expression levels of caspase-3
and p-Akt were identified in H9c2 cells with EGCG-treatment alone,
which implied that EGCG did not exhibit an anti-apoptotic effect
through the PI3K-Akt pathway at a concentration of 10 µM.
When treated with Zn2+ alone, an anti-apoptotic effect
was observed through the activation of the p-Akt protein. It was
identified that administration of EGCG + Zn2+
significantly reduced the expression levels of cleaved caspase-3
protein and elevated those of p-Akt protein in H9c2 cells compared
with those in the H/R and Zn2+ treatment groups. An
investigation using the PI3K inhibitor LY294002 was also conducted,
which was used to verify the effect of the PI3K pathway in
myocardial apoptosis. Pretreatment with LY294002 and EGCG +
Zn2+ did not further reduce caspase-3 activity or
increase p-Akt expression following H/R injury.
The results of the current study suggested that the
PI3K/Akt pathway may be the major pathway underlying EGCG +
Zn2+, with regard to the prevention of reperfusion
injury and myocardial apoptosis. Notably, zinc supplementation with
EGCG effectively enhanced the p-Akt levels following H/R, resulting
in increased cell viability. The results suggested that the
interactions between EGCG and zinc may preserve and enhance their
anti-apoptotic effects via the PI3K/Akt pathway. The prophylactic
administration of pharmacological agents mimicking the effects of
ischemic preconditioning are suggested to represent an effective
method of reducing the extent of myocardial damage resulting from
I/R or H/R injury. The current study aimed to evaluate the
anti-apoptotic activity of EGCG + Zn2+, with the
objective of discovering an effective and safe cardioprotective
agent for the prevention and/or treatment of I/R injury. Zinc
acetate was previously approved by the Food and Drug Association in
1997 as a drug for the treatment of Wilson’s disease, which
indicates the clinical safety of zinc supplementation (32). Further understanding of the safety
and efficacy of EGCG + Zn2+ in clinical practice would
be beneficial.
The results of the current study suggest that the
inhibition of I/R injury may provide opportunities to improve the
function and viability of H9c2 cells, through exhibiting an
anti-apoptotic effect. It was demonstrated that when EGCG
interacted with zinc, the cardioprotective activity was
significantly enhanced, as compared with EGCG treatment alone,
potentially via activation of the PI3K/Akt pathway. In conclusion,
EGCG and zinc may represent a potent therapeutic agent for I/R
injury.
Acknowledgments
The current study was supported by a specialized
research fund for the Doctoral program of Higher Education (grant
no. 2011440211006). The authors would like to thank the Laboratory
of Molecular Cardiology of the First Affiliated Hospital of Shantou
University Medical College (Shantou, China) for providing technical
assistance.
References
|
1
|
Cannon RO III: Mechanisms, management and
future directions for reperfusion injury after acute myocardial
infarction. Nat Clin Pract Cardiovasc Med. 2:88–94. 2005.
View Article : Google Scholar : PubMed/NCBI
|
|
2
|
Aversano T, Aversano LT, Passamani E, et
al: Thrombolytic therapy vs. primary percutaneous coronary
intervention for myocardial infarction in patients presenting to
hospitals without on-site cardiac surgery: a randomized controlled
trial. JAMA. 287:1943–1951. 2002. View Article : Google Scholar : PubMed/NCBI
|
|
3
|
Fröhlich GM, Meier P, White SK, Yellon DM
and Hausenloy DJ: Myocardial reperfusion injury: looking beyond
primary PCI. Eur Heart J. 34:1714–1722. 2013. View Article : Google Scholar : PubMed/NCBI
|
|
4
|
Wang GW, Zhou Z, Klein JB and Kang YJ:
Inhibition of hypoxia/reoxygenation-induced apoptosis in
metallothionein-overexpressing cardio-myocytes. Am J Physiol Heart
Circ Physiol. 280:H2292–H2299. 2001.PubMed/NCBI
|
|
5
|
Moens AL, Claeys MJ, Timmermans JP and
Vrints CJ: Myocardial ischemia/reperfusion-injury, a clinical view
on a complex patho-physiological process. Int J Cardiol.
100:179–190. 2005. View Article : Google Scholar : PubMed/NCBI
|
|
6
|
Stephanou A, Brar B, Liao Z, et al:
Distinct initiator caspases are required for the induction of
apoptosis in cardiac myocytes during ischaemia versus reperfusion
injury. Cell Death Differ. 8:434–435. 2001. View Article : Google Scholar : PubMed/NCBI
|
|
7
|
Scarabelli TM, Stephanou A, Pasini E, et
al: Different signaling pathways induce apoptosis in endothelial
cells and cardiac myocytes during ischemia/reperfusion injury. Circ
Res. 90:745–748. 2002. View Article : Google Scholar : PubMed/NCBI
|
|
8
|
Buja LM and Entman ML: Modes of myocardial
cell injury and cell death in ischemic heart disease. Circulation.
98:1355–1357. 1998. View Article : Google Scholar : PubMed/NCBI
|
|
9
|
Geleijnse JM, Launer LJ, Hofman A, Pols HA
and Witteman JC: Tea flavonoids may protect against
atherosclerosis: the Rotterdam Study. Arch Intern Med.
159:2170–2174. 1999. View Article : Google Scholar : PubMed/NCBI
|
|
10
|
Sano J, Inami S, Seimiya K, et al: Effects
of green tea intake on the development of coronary artery disease.
Circ J. 68:665–670. 2004. View Article : Google Scholar : PubMed/NCBI
|
|
11
|
Aneja R, Hake PW, Burroughs TJ, et al:
Epigallocatechin, a green tea polyphenol, attenuates myocardial
ischemia reperfusion injury in rats. Mol Med. 10:55–62. 2004.
View Article : Google Scholar : PubMed/NCBI
|
|
12
|
Townsend PA, Scarabelli TM, Pasini E, et
al: Epigallocatechin-3-gallate inhibits STAT-1 activation and
protects cardiac myocytes from ischemia/reperfusion-induced
apoptosis. FASEB J. 18:1621–1623. 2004.PubMed/NCBI
|
|
13
|
Piao CS, Kim DS, Ha KC, et al: The
protective effect of epigallocatechin-3 gallate on
ischemia/reperfusion injury in isolated rat hearts: An ex vivo
approach. Korean J Physiol Pharmacol. 15:259–266. 2011. View Article : Google Scholar : PubMed/NCBI
|
|
14
|
Sheng R, Gu ZL and Xie ML:
Epigallocatechin gallate, the major component of polyphenols in
green tea, inhibits telomere attrition mediated cardiomyocyte
apoptosis in cardiac hypertrophy. Int J Cardiol. 162:199–209. 2013.
View Article : Google Scholar
|
|
15
|
Hayakawa F, Ishizu Y, Hoshino N, et al:
Prooxidative activities of tea catechins in the presence of
Cu2+. Biosci Biotechnol Biochem. 68:1825–1830. 2004.
View Article : Google Scholar : PubMed/NCBI
|
|
16
|
Yu HN, Shen SR and Xiong YK: Cytotoxicity
of epigallo-catechin-3-gallate to LNCaP cells in the presence of
Cu2+. J Zhejiang Univ Sci B. 6:125–131. 2005. View Article : Google Scholar : PubMed/NCBI
|
|
17
|
Chen X, Yu H, Shen S and Yin J: Role of
Zn2+ in epigallocatechin gallate affecting the growth of
PC-3 cells. J Trace Elem Med. 21:125–131. 2007. View Article : Google Scholar
|
|
18
|
Viswanath K, Bodiga S, Balogun V, Zhang A
and Bodiga VL: Cardioprotective effect of zinc requires ErbB2 and
Akt during hypoxia/reoxygenation. Biometals. 24:171–180. 2011.
View Article : Google Scholar
|
|
19
|
Lee S, Chanoit G, McIntosh R, et al:
Molecular mechanism underlying Akt activation in zinc-induced
cardioprotection. Am J Physiol Heart Circ Physiol. 297:H569–H575.
2009. View Article : Google Scholar : PubMed/NCBI
|
|
20
|
Vinten-Johansen J, Zhao ZQ, Jiang R, Zatta
AJ and Dobson GP: Preconditioning and postconditioning: innate
cardioprotection from ischemia-reperfusion injury. J Appl Physiol
(1985). 103:1441–1448. 2007. View Article : Google Scholar
|
|
21
|
Hausenloy DJ and Yellon DM: Survival
kinases in ischemic preconditioning and postconditioning.
Cardiovasc Res. 70:240–253. 2006. View Article : Google Scholar : PubMed/NCBI
|
|
22
|
Zhang T, Yang D, Fan Y, et al:
Epigallocatechin-3-gallate enhances ischemia/reperfusion-induced
apoptosis in human umbilical vein endothelial cells via AKT and
MAPK pathways. Apoptosis. 14:1245–1254. 2009. View Article : Google Scholar : PubMed/NCBI
|
|
23
|
Yaoita H, Ogawa K, Maehara K and Maruyama
Y: Attenuation of ischemia/reperfusion injury in rats by a caspase
inhibitor. Circulation. 97:276–281. 1998. View Article : Google Scholar : PubMed/NCBI
|
|
24
|
Mocanu MM, Baxter GF and Yellon DM:
Caspase inhibition and limitation of myocardial infarct size:
Protection against lethal reperfusion injury. Br J Pharmacol.
130:197–200. 2000. View Article : Google Scholar : PubMed/NCBI
|
|
25
|
Ross R: Atherosclerosis is an inflammatory
disease. Am Heart J. 138:S419–S420. 1999. View Article : Google Scholar : PubMed/NCBI
|
|
26
|
Bayes-Genis A, Conover CA and Schwartz RS:
The insulin-like growth factor axis: a review of atherosclerosis
and restenosis. Circ Res. 86:125–130. 2000. View Article : Google Scholar : PubMed/NCBI
|
|
27
|
Zeng X, Li Q, Zhang M, et al: Green tea
may be benefit to the therapy of atrial fibrillation. J Cell
Biochem. 112:1709–1712. 2011. View Article : Google Scholar : PubMed/NCBI
|
|
28
|
Sesso HD, Gaziano JM, Buring JE and
Hennekens CH: Coffee and tea intake and the risk of myocardial
infarction. Am J Epidemiol. 149:162–167. 1999. View Article : Google Scholar : PubMed/NCBI
|
|
29
|
Cheng TO: Tea is good for the heart. Arch
Intern Med. 160:23972000. View Article : Google Scholar : PubMed/NCBI
|
|
30
|
Kagaya N, Kawase M, Maeda H, Tagawa Y,
Nagashima H, Ohmori H and Yagi K: Enhancing effect of zinc on
hepatoprotectivity of epigallocatechin gallate in isolated rat
hepatocytes. Biol Pharm Bull. 25:1156–1160. 2002. View Article : Google Scholar : PubMed/NCBI
|
|
31
|
Kim MK, Jung HS, Yoon CS, et al: EGCG and
quercetin protected INS-1 cells in oxidative stress via different
mechanisms. Front Biosci (Elite Ed). 2:810–817. 2010. View Article : Google Scholar
|
|
32
|
Brewer GJ, Johnson VD, Dick RD, et al:
Treatment of Wilson’s disease with zinc. XVII: treatment during
pregnancy. Hepatology. 31:364–370. 2000. View Article : Google Scholar : PubMed/NCBI
|