|
1
|
Crépy L, Monchau F, Chai F, Raoul G,
Hivart P, Hildebrand HF, Martin P and Joly N: Evaluation of a
bio-based hydrophobic cellulose laurate film as biomaterial-study
on biodegradation and cytocompatibility. J Biomed Mater Res B Appl
Biomater. 100:1000–1008. 2012. View Article : Google Scholar : PubMed/NCBI
|
|
2
|
Lavoine N, Desloges I, Dufresne A and Bras
J: Microfibrillated cellulose-its barrier properties and
applications in cellulosic materials: A review. Carbohydr Polym.
90:735–764. 2012. View Article : Google Scholar : PubMed/NCBI
|
|
3
|
Spencer PC, Schmidt B, Samtleben W, Bosch
T and Gurland HJ: Ex vivo model of hemodialysis membrane
biocompatibility. Trans Am Soc Artif Intern Organs. 31:495–498.
1985.PubMed/NCBI
|
|
4
|
Gissinger D and Stamm A: A comparative
study of cross-linked carboxymethylcellulose as tablet
disintegrant. Pharm Ind. 42:189–192. 1980.
|
|
5
|
Franz G: Polysaccharides in pharmacy. Adv
Polymer Sci. 76:1–30. 1986. View Article : Google Scholar
|
|
6
|
Ito H, Shibata T, Miyamoto T, Noishiki Y
and Inagaki H: Formation of polyelectrolyte complexes between
cellulose derivatives and their blood compatibility. J Appl Polym
Sci. 31:2491–2500. 1986. View Article : Google Scholar
|
|
7
|
Matasuzaki K, Yamamoto I, Sato T and
Oshima R: Synthesis of water-soluble branched polysaccharides and
their antitumor activity, 1. Branched polysaccharides from
cellulose acetate. Macromol Chem Phys. 186:449–456. 1985.
View Article : Google Scholar
|
|
8
|
Lee CG, Da Silva CA, Lee JY, Hartl D and
Elias JA: Chitin regulation of immune responses: An old molecule
with new roles. Curr Opin Immunol. 20:684–689. 2008. View Article : Google Scholar : PubMed/NCBI
|
|
9
|
Hirano S: Chitin biotechnology
applications. Biotechnol Annu Rev. 2:237–258. 1996. View Article : Google Scholar : PubMed/NCBI
|
|
10
|
Mu X, Yu H, Zhang C, Chen X, Cheng Z, Bai
R, Wu X, Yu Q, Wu C and Diao Y: Nano-porous nitrocellulose liquid
bandage modulates cell and cytokine response and accelerates
cutaneous wound healing in a mouse model. Carbohydr Polym.
136:618–629. 2016. View Article : Google Scholar : PubMed/NCBI
|
|
11
|
Fricain JC, Granja PL, Barbosa MA, de Jéso
B, Barthe N and Baquey C: Cellulose phosphates as biomaterials. In
vivo biocompatibility studies. Biomaterials. 23:971–980. 2002.
View Article : Google Scholar : PubMed/NCBI
|
|
12
|
Martson M, Viljanto J, Hurme T, Laippala P
and Saukko P: Is cellulose sponge degradable or stable as
implantation material? An in vivo subcutaneous study in the rat.
Biomaterials. 20:1989–1995. 1999. View Article : Google Scholar : PubMed/NCBI
|
|
13
|
Petkewich R: Liquid bandages. Chem Eng
News. 86:612008. View Article : Google Scholar
|
|
14
|
Choi SJ, Lee JH, Lee YH, Hwang DY and Kim
HD: Synthesis and properties of polyurethane-urea-based liquid
bandage materials. J Appl Polym Sci. 121:3516–3524. 2011.
View Article : Google Scholar
|
|
15
|
Shepler TR and Seiff SR: Use of isobutyl
cyanoacrylate tissue adhesive to stabilize external eyelid weights
in temporary treatment of facial palsies. Ophthalmic Plast Reconstr
Surg. 17:169–173. 2001. View Article : Google Scholar : PubMed/NCBI
|
|
16
|
Taravella MJ and Chang CD: 2-Octyl
cyanoacrylate medical adhesive in treatment of a corneal
perforation. Cornea. 20:220–221. 2001. View Article : Google Scholar : PubMed/NCBI
|
|
17
|
Suhr MA, Günther M and Springer IN: Ptosis
relief after botox injection using dermabond. Plast Reconstr Surg.
114:262–263. 2004. View Article : Google Scholar : PubMed/NCBI
|
|
18
|
Osaki TH, Osaki MH, Belfort R Jr, Osaki T,
Sant'anna AE and Haraguchi DK: Management of progressive myopathic
blepharoptosis with daily application of octyl-2-cyanoacrylate
liquid bandage. Ophthalmic Plast Reconstr Surg. 25:264–266. 2009.
View Article : Google Scholar : PubMed/NCBI
|
|
19
|
Osaki TH, Osaki MH and Osaki TH: Temporary
management of involutional entropion with octyl-2-cyanoacrylate
liquid bandage application. Arq Bras Oftalmol. 73:120–124. 2010.
View Article : Google Scholar : PubMed/NCBI
|
|
20
|
Song SH, Kim JE, Lee YJ, Kwak MH, Sung GY,
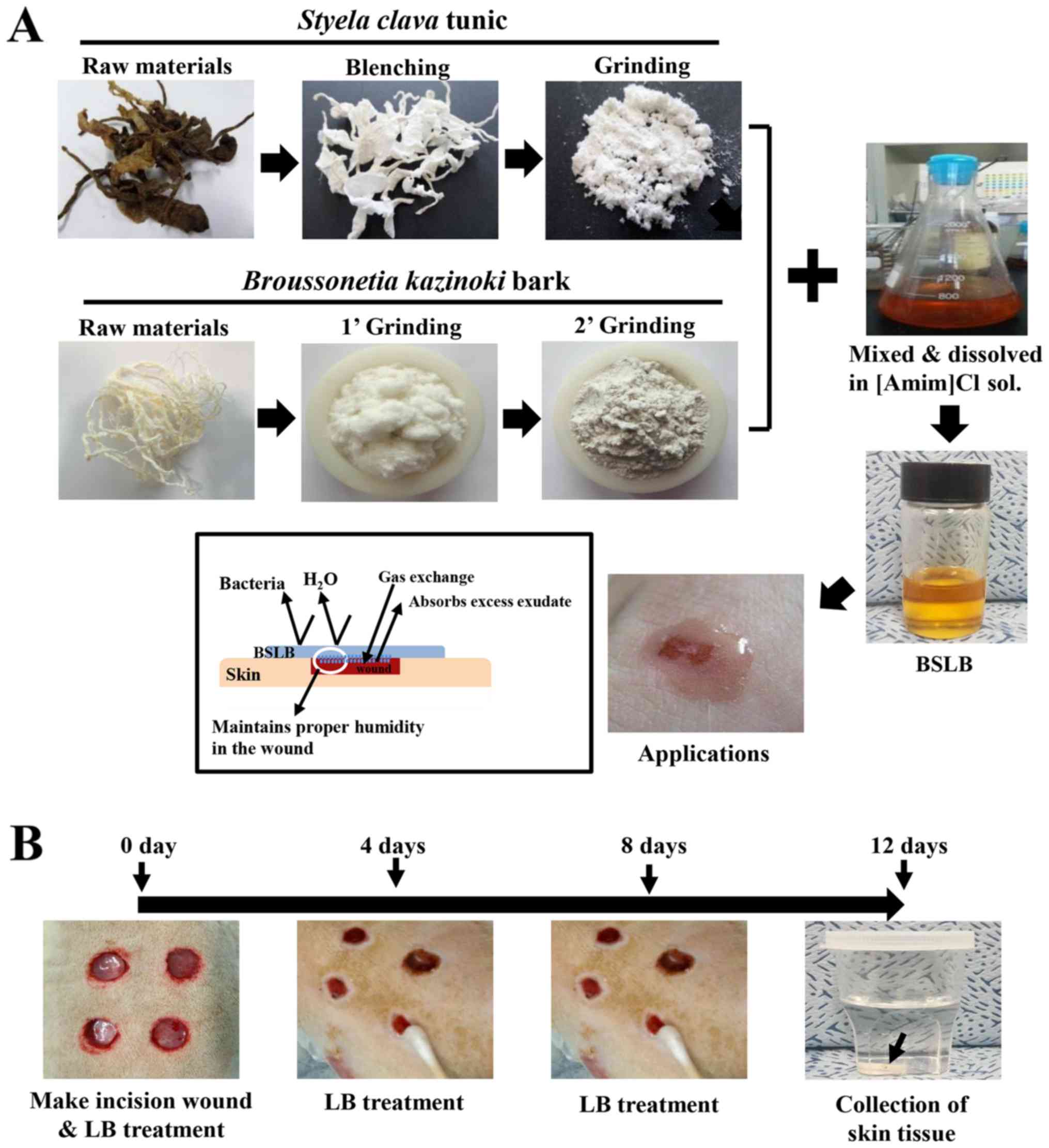
Kwon SH, Son HJ, Lee HS, Jung YJ and Hwang DY: Cellulose film
regenerated from Styela clava tunics have biodegradability,
toxicity and biocompatibility in the skin of SD rats. J Mater Sci
Mater Med. 25:1519–1530. 2014. View Article : Google Scholar : PubMed/NCBI
|
|
21
|
Hwang DY, Chae KR, Kang TS, Hwang JH, Lim
CH, Kang HK, Goo JS, Lee MR, Lim HJ, Min SH, et al: Alterations in
behavior, amyloid beta-42, caspase-3, and Cox-2 in mutant PS2
transgenic mouse model of Alzheimer's disease. FASEB J. 16:805–813.
2002. View Article : Google Scholar : PubMed/NCBI
|
|
22
|
Eaglstein WH: Moist wound healing with
occlusive dressings: A clinical focus. Dermatol Surg. 27:175–181.
2001. View Article : Google Scholar : PubMed/NCBI
|
|
23
|
Nissen NN and DiPietro LA: Angiogenic
mediators in healing wounds. angiogenesis in Health and Disease.
Gabor MR: Marcel Dekker Inc.; New York: pp. 417–427. 2000
|
|
24
|
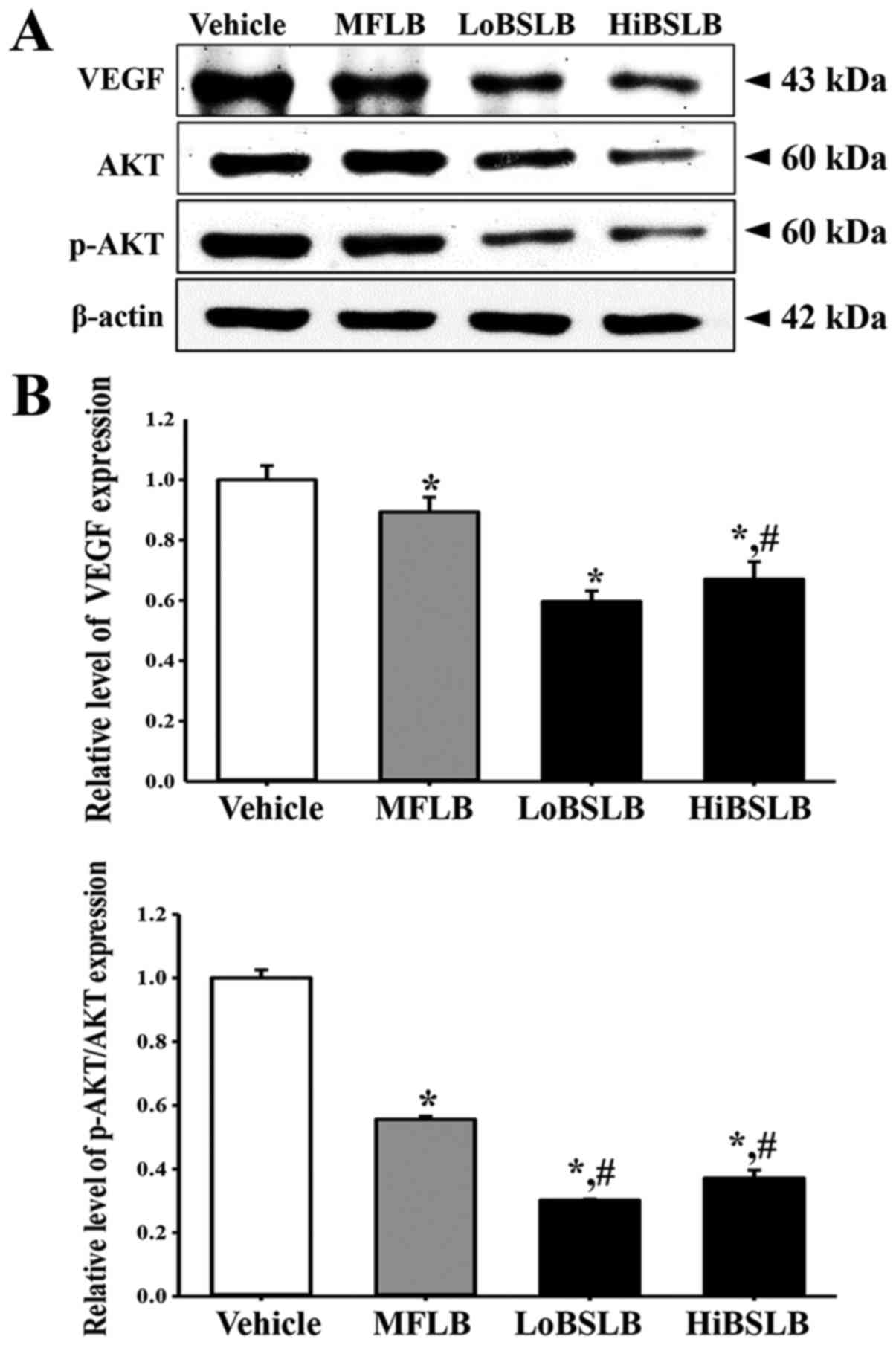
Ferrara N: Vascular endothelial growth
factor and the regulation of angiogenesis. Recent Prog Horm Res.
55:15–36. 2000.PubMed/NCBI
|
|
25
|
Ferrara N: Role of vascular endothelial
growth factor in regulation of physiological angiogenesis. Am J
Physiol Cell Physiol. 208:C1358–C1366. 2001. View Article : Google Scholar
|
|
26
|
Taub PJ, Silver L and Weinberg H: Plastic
surgical perspectives on vascular endothelial growth factor as gene
therapy for angiogenesis. Plast Reconstr Surg. 105:1034–1042. 2000.
View Article : Google Scholar : PubMed/NCBI
|
|
27
|
Gerber HP, McMurtrey A, Kowalski J, Yan M,
Keyt BA, Dixit V and Ferrara N: Vascular endothelial growth factor
regulates endothelial cell survival through the
phosphatidylinositol 3′-kinase/Akt signal transduction pathway.
Requirement for Flk-1/KDR activation. J Biol Chem. 273:30336–30343.
1998. View Article : Google Scholar : PubMed/NCBI
|
|
28
|
Abid MR, Guo S, Minami T, Spokes KC, Ueki
K, Skurk C, Walsh K and Aird WC: Vascular endothelial growth factor
activates PI3K/Akt/forkhead signaling in endothelial cells.
Arterioscler Thromb Vasc Biol. 24:294–300. 2004. View Article : Google Scholar : PubMed/NCBI
|
|
29
|
Zheng J, Wen Y, Song Y, Wang K, Chen DB
and Magness RR: Activation of multiple signaling pathways is
critical for fibroblast growth factor 2- and vascular endothelial
growth factor-stimulated ovine fetoplacental endothelial cell
proliferation. Biol Reprod. 78:143–150. 2008. View Article : Google Scholar : PubMed/NCBI
|
|
30
|
Frank S, Hübner G, Breier G, Longaker MT,
Greenhalgh DG and Werner S: Regulation of vascular endothelial
growth factor expression in cultured keratinocytes. Implications
for normal and impaired wound healing. J Biol Chem.
270:12607–12613. 1995. View Article : Google Scholar : PubMed/NCBI
|
|
31
|
Kant V, Gopal A and Kumar D, Bag S, Kurade
NP, Kumar A, Tandan SK and Kumar D: Topically applied substance P
enhanced healing of open excision wound in rats. Eur J Pharmacol.
715:345–353. 2013. View Article : Google Scholar : PubMed/NCBI
|
|
32
|
Sun X, Cheng L, Zhu W, Hu C, Jin R, Sun B,
Shi Y, Zhang Y and Cui W: Use of ginsenoside Rg3-loaded electrospun
PLGA fibrous membranes as wound cover induces healing and inhibits
hypertrophic scar formation of the skin. Colloids Surf B
Biointerfaces. 115:61–70. 2014. View Article : Google Scholar : PubMed/NCBI
|
|
33
|
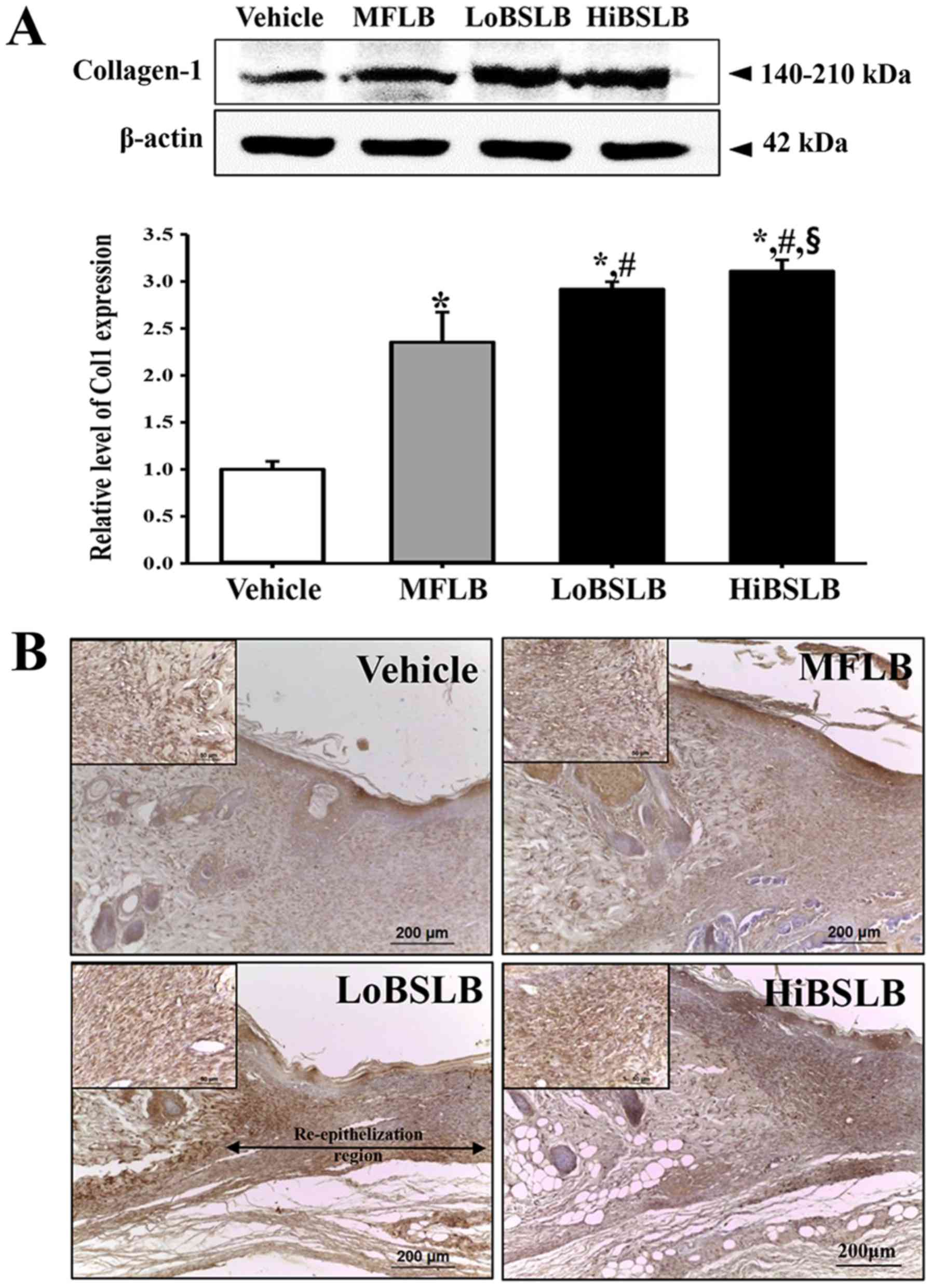
Mian M, Beghè F and Mian E: Collagen as a
pharmacological approach in wound healing. Int J Tissue React. 14
Suppl:S1–S9. 1992.
|
|
34
|
Kwak MH, Go J, Kim JE, Lee YJ, Lee SH, Lee
HS, Son HJ, Jung YJ and Hwang DY: Property and efficacy analysis of
hydrocolloid membrane containing Styela clava tunic on the
wound repair of skin in SD rats. Biomat Res. 17:91–101. 2013.
|