Introduction
Gastrointestinal stromal tumors (GISTs) arise from
the interstitial cells of Cajal and are the most frequently
occurring mesenchymal tumors of the gastrointestinal tract
(1). The majority of GISTs (~90%)
exhibit constitutively activating KIT mutations, while ~5%
show mutations in another tyrosine kinase receptor gene,
platelet-derived growth factor receptor α. In addition to the
abnormal activation of tyrosine kinase receptors observed in a
majority of GISTs, a previous study revealed succinate
dehydrogenase mutations to perform a critical role in the induction
of aberrant DNA methylation in pediatric GISTs (2). These findings indicate that genetic and
epigenetic dysregulation are causally associated with the
pathogenesis of GISTs.
MicroRNAs (miRNAs/miRs) are small noncoding RNAs
that perform critical roles in physiological and pathological
settings (3). Dysregulation of miRNAs
is commonly observed in malignancies, and numerous miRNAs are
thought to act as oncogenes or tumor suppressors (4,5). We
previously screened miRNAs to identify epigenetically silenced
miRNA genes in GIST cells, and revealed that miR-34a and miR-335
are silenced in association with CpG island methylation in GISTs
(6). In addition, functional analyses
suggested that miR-34a and miR-335 act as tumor suppressors in
GISTs and that the two genes are frequently methylated in primary
GIST specimens. In addition, we observed that elevated expression
of miR-196a is clearly associated with aggressiveness and poor
prognosis of GISTs, which is indicative of its oncogenicity
(7). These results highlight the
critical impact of miRNA dysregulation in the pathogenesis of
GISTs.
Distant metastasis is a critical event that prevents
complete cure of malignant tumors. The process of tumor metastasis
involves several steps: Detachment of cells from the primary tumor;
tissue invasion by the tumor cells; intravasation, arrest and
extravasation of the cells; and proliferation of the cells at
metastatic sites (8). It is well
known that a subset of miRNAs perform key roles in cancer
metastasis. For instance, miR-10b is strongly expressed in
metastatic breast cancer cells and promotes cell migration and
invasion by suppressing HOXD10, which results in increased
expression of a pro-metastatic gene, RHOC (9). miR-21 is also reportedly oncogenic and
targets genes that suppress invasion and metastasis (10). On the other hand, members of the
miR-200 family suppress metastasis by downregulating ZEB1, a
negative modulator of E-cadherin (11). However, dysregulation of these miRNAs
has not been reported in GISTs, and the mechanism underlying GIST
metastasis is not fully understood. The present study therefore
aimed to identify miRNAs involved in GIST metastasis. By analyzing
miRNA expression profiles in a series of primary GISTs, it was
determined that the downregulation of miR-186 is associated with
metastatic recurrence and poor prognosis, which suggests that a
loss of miR-186 could potentially act to drive GIST metastasis.
Materials and methods
Tissue samples
A total of 32 fresh frozen GIST specimens were
obtained from Sapporo Medical University Hospital (Sapporo, Japan)
and Osaka University Hospital (Osaka, Japan) as described
previously (7). In addition,
formalin-fixed paraffin-embedded tissue sections from 100 GIST
specimens were obtained from Niigata University Hospital (Niigata,
Japan), as described previously (7).
Informed consent was obtained from all patients prior to the
collection of the specimens, and the present study was approved by
the institutional review board. Risk grade was assessed based on
tumor size and mitotic activity, according to the risk
classification system proposed by Fletcher et al (12). Total RNA was extracted using TRIzol
reagent (Thermo Fisher Scientific, Inc., Waltham, MA, USA).
Cell line and transfection
GIST-T1 cells were cultured as described previously
(13). Cells (3×106) were
transfected with 100 pmol mirVana miRNA inhibitor (Thermo Fisher
Scientific, Inc., Waltham, MA, USA) or 100 pmol mirVana miRNA
inhibitor Negative Control (Thermo Fisher Scientific, Inc.) using a
Cell Line Nucleofector kit V (Lonza Group, Ltd., Basel,
Switzerland) and a Nucleofector I electroporation device (Lonza
Group, Ltd.) according to the manufacturer's protocol.
miRNA expression analysis
miRNA expression profiles were analyzed using the
miRNA microarray data obtained in our previous study (7). The Gene Expression Omnibus accession
number for the microarray data is GSE31741. Expression of selected
miRNAs was examined using TaqMan microRNA assays (Thermo Fisher
Scientific, Inc.). DNase treatment was performed prior to the
reverse transcription quantitative polymerase chain reaction
(RT-qPCR), which was performed in a 7500HT Fast Real-Time PCR
System (Thermo Fisher Scientific, Inc.) according to the
manufacture's protocol, using primers supplied from the
manufacturer (Thermo Fisher Scientific, Inc.). SDS v1.4 software
(Thermo Fisher Scientific, Inc.) was used for comparative ∆Cq
analysis (14). U6 snRNA (RNU6B;
Thermo Fisher Scientific, Inc.) was used as an endogenous control.
Experiments were performed in triplicate.
Cell viability assay
GIST-T1 cells were transfected with miRNA inhibitor
or negative control as described above, and seeded into a 96-well
plate to a density of 1×105 cells per well. Cell
viabilities were examined every 24 h for 96 h using a Cell Counting
kit-8 (Dojindo Molecular Technologies, Inc., Tokyo, Japan)
according to the manufacturer's protocol.
Wound healing assays
GIST-T1 cells were transfected with the miRNA
inhibitor or a negative control as described above. Subsequently,
cells were suspended in 500 µl of Dulbecco's Modified Eagle's
Medium (Sigma-Aldrich; Merck KGaA, Darmstadt, Germany) supplemented
with 10% fetal bovine serum, and 70 µl aliquots of cell suspension
were added to the wells of Culture-Insert 2 plates (Ibidi, Munich,
Germany). Subsequent to an incubation for 24 h at 37°C, the culture
inserts were removed, and migration was assessed subsequent to
incubation for an additional 16 h at 37°C. Cell images were
captured using an IX81 light microscope system (Olympus, Tokyo,
Japan) and wound area was measured using ImageJ software version
1.47 (National Institutes of Health, Bethesda, Maryland, USA).
Gene expression microarray
analysis
GIST-T1 cells were transfected with the miRNA
inhibitor or a negative control as described above, and total RNA
was extracted 48 h after transfection. One-color microarray-based
gene expression array analysis was then carried out according to
the manufacturer's protocol (Agilent Technologies, Inc., Santa
Clara, CA, USA). Briefly, 100 ng of total RNA was amplified and
labeled using a Low-input Quick Amp Labeling kit One-color (Agilent
Technologies, Inc.). The synthesized cRNA was subsequently
hybridized to a SurePrint G3 Human GE microarray v2 (G4851; Agilent
Technologies, Inc.). The microarray experiments were performed in
duplicate, and data were analyzed using GeneSpring GX version 13
(Agilent Technologies, Inc.). The Gene Expression Omnibus accession
number for the microarray data is GSE85613.
Statistical analysis
Quantitative variables were analyzed using a
Student's t-test or one-way analysis of variance. Categorical
values were compared using Fisher's exact test. Logistic regression
analysis was used to assess the correlation between
clinicopathological factors and gene expression. Survival was
analyzed using a Cox's regression model; the log-rank test was used
for two-group comparisons. All data were analyzed using EZR version
1.32 (15).
Results
Identification of miRNAs associated
with GIST metastasis
To identify miRNAs associated with GIST metastasis,
the present study first analyzed miRNA microarray data previously
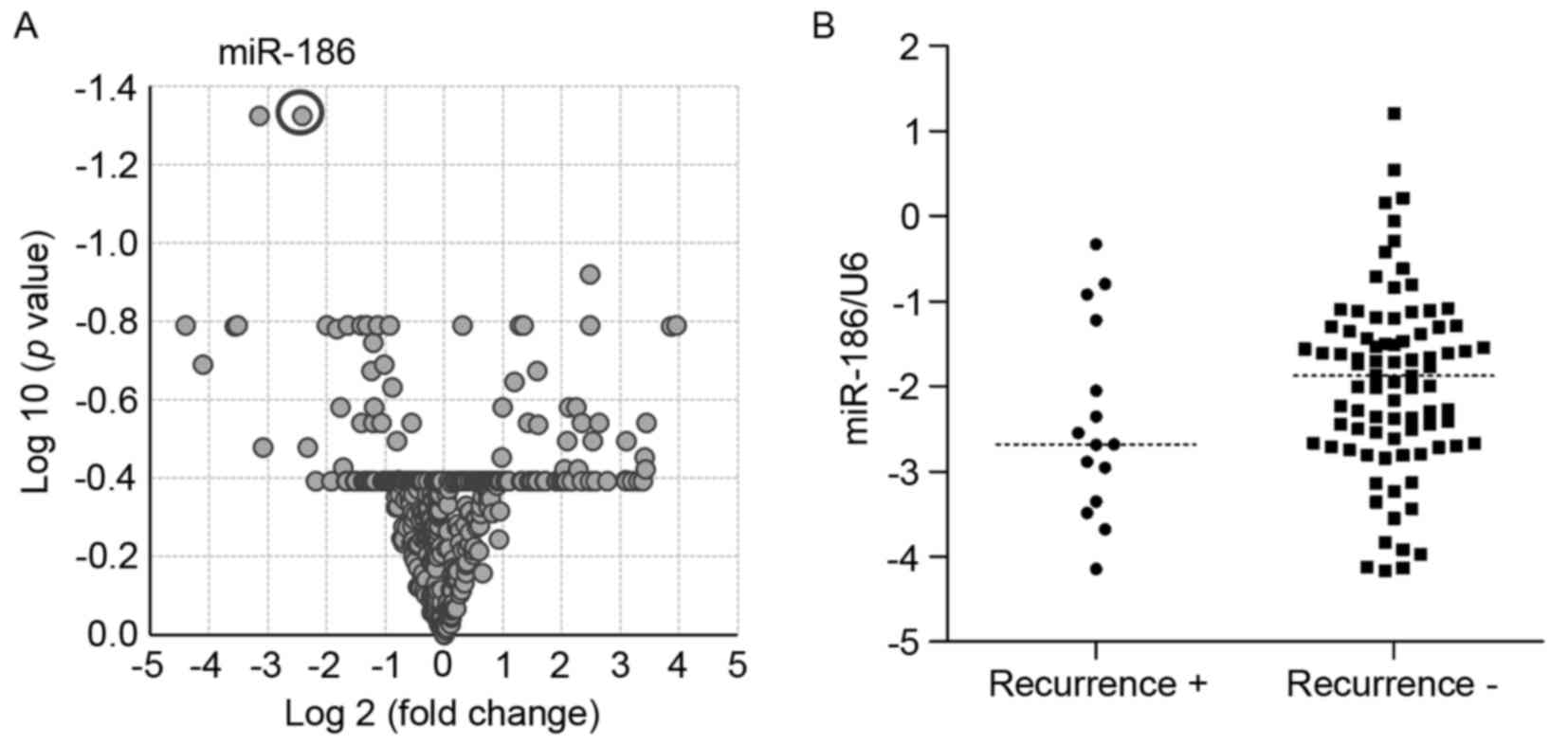
obtained from 32 primary GIST specimens (7). Volcano plot analysis revealed that
levels of miR-186 and miR-99a expression differed between tumors
with or without metastatic recurrence (P<0.05, >2-fold)
(Fig. 1A, Table I). The present study then validated
the microarray results using RT-qPCR with an independent cohort of
primary GISTs. Since the preliminary analysis suggested that
expression of miR-99a was not associated with metastatic recurrence
and poor prognosis in GISTs, miR-186 was selected for additional
studies (data not shown). RT-qPCR analysis of the new cohort of
GIST specimens (n=100) demonstrated that levels of miR-186
expression tended to be lower in GISTs with metastatic recurrence
compared with those without recurrence, although the difference was
not observed to be statistically significant (Fig. 1B).
 | Table I.miRNAs associated with metastatic
recurrence in GIST. |
Table I.
miRNAs associated with metastatic
recurrence in GIST.
| miRNA | P-value | Corrected
P-value | Fold change |
|---|
| hsa-miR-186 |
1.01×10−4 | 0.047 | −5.33 |
| hsa-miR-99a |
6.67×10−5 | 0.047 | −8.89 |
| hsa-miR-299-3p |
3.85×10−5 | 0.120 | 5.61 |
| hsa-miR-320d |
9.17×10−4 | 0.162 | 2.44 |
| hsa-miR-23b |
2.76×10−3 | 0.162 | −3.12 |
| hsa-miR-145* |
2.30×10−3 | 0.162 | −2.48 |
| hsa-miR-34b |
2.37×10−3 | 0.162 | 5.58 |
| hsa-miR-144 |
1.81×10−3 | 0.162 | 15.53 |
| hsa-miR-30c |
1.54×10−3 | 0.162 | −1.91 |
| hsa-miR-647 |
2.40×10−3 | 0.162 | 1.25 |
| hsa-miR-30e |
1.15×10−3 | 0.162 | −2.19 |
| hsa-miR-27b |
2.55×10−3 | 0.162 | −2.64 |
| hsa-miR-204 |
1.62×10−3 | 0.162 | −21.18 |
| hsa-miR-30e* |
1.94×10−3 | 0.162 | −4.00 |
| hsa-miR-10a |
2.63×10−3 | 0.162 | −11.49 |
| hsa-miR-320c |
1.73×10−3 | 0.162 | 2.54 |
|
hsa-miR-199b-5p |
3.00×10−3 | 0.163 | −11.79 |
| hsa-miR-431 |
3.12×10−3 | 0.163 | 14.61 |
| hsa-miR-148a |
3.36×10−3 | 0.166 | −3.54 |
| hsa-miR-34a |
3.84×10−3 | 0.180 | −2.30 |
The association between clinicopathological features
and levels of miR-186 expression in the validation cohort is
summarized in Table II. The mean
levels of miR-186 expression were not associated with age, gender,
tumor location or risk classifications of the primary GISTs
(Table II). However, logistic
regression analysis revealed that low levels of miR-186 expression
were associated with an elevated risk of metastatic recurrence
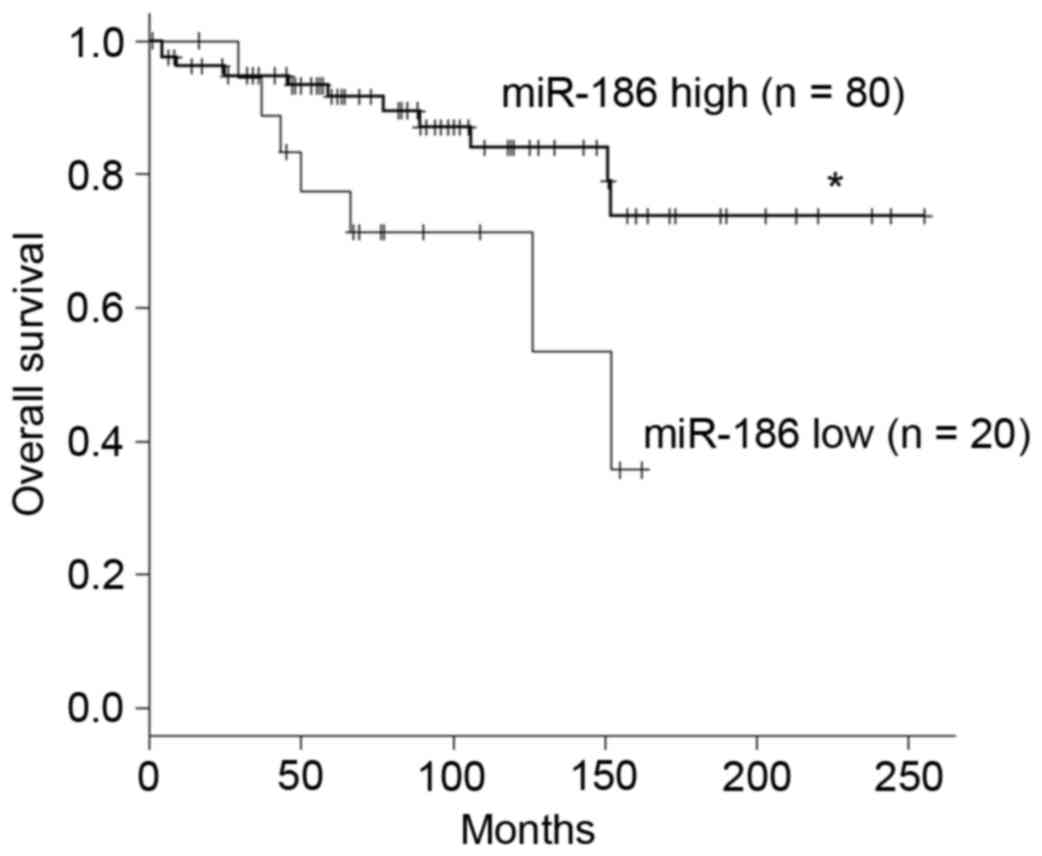
(Table III). In addition, Cox's
hazard analysis revealed that the hazard ratio was highest for
patients with downregulated miR-186 expression when a cutoff value
of miR186/U6 ≤0.143 was employed (Table
IV). Kaplan-Meyer analysis demonstrated that lower expression
of miR-186 is associated with poorer overall survival among
patients with GIST (Fig. 2).
 | Table II.Correlation between miR-186
expression and the clinicopathological features of GISTs. |
Table II.
Correlation between miR-186
expression and the clinicopathological features of GISTs.
| Clinicopathological
feature | n | miR-186/U6 (mean ±
95% CI) | P-value |
|---|
| Age, years |
|
|
|
|
>65 | 44 | 0.30±0.21 | 0.34 |
|
≤65 | 56 | 0.36±0.38 |
|
| Gender |
|
|
|
|
Male | 44 | 0.39±0.32 | 0.07 |
|
Female | 56 | 0.28±0.31 |
|
| Tumor location |
|
|
|
|
Stomach | 84 | 0.31±0.30 | 0.17 |
|
Intestine | 8 | 0.28±0.37 |
|
|
Colon | 3 | 0.44±0.29 |
|
|
Esophagus | 5 | 0.62±0.50 |
|
| Risk
classificationa |
|
|
|
| Very
low | 1 | 0.31 | 0.95 |
|
Low | 45 | 0.33±0.23 |
|
|
Intermediate | 25 | 0.37±0.34 |
|
|
High | 26 | 0.32±0.43 |
|
| Metastatic
recurrence |
|
|
|
| + | 15 | 0.25±0.22 | 0.32 |
| − | 85 | 0.34±0.33 |
|
 | Table III.miR-186 expression is associated with
metastatic recurrence risk in GIST patients. |
Table III.
miR-186 expression is associated with
metastatic recurrence risk in GIST patients.
| Features | OR (95% CI) | P-value | Adjusted OR (95%
CI) | P-value |
|---|
| Tumor location |
|
|
|
|
|
Stomach | 1 |
|
|
|
| Other
(intestine, esophagus, colon) | 0.78
(0.16–3.85) |
0.76 | 3.12
(0.47–20.9)a |
0.24 |
| Risk
classification |
|
|
|
|
| Low or
intermediate risk | 1 |
|
|
|
| High
risk | 12.8
(3.59–45.8) | <0.001 | 13.4
(3.47–51.7)b | <0.001 |
| miR-186/U6 |
|
|
|
|
|
>0.172 | 1 |
|
|
|
|
≤0.172 | 4.04
(1.30–12.6) | <0.05 | 3.84
(1.02–14.4)c | <0.05 |
 | Table IV.miR-186 expression is associated with
poor clinical outcome in GIST patients. |
Table IV.
miR-186 expression is associated with
poor clinical outcome in GIST patients.
|
| Outcome |
|
|
|
|
|
|---|
|
|
|
|
|
|
|
|
|---|
| miR-186/U6 | Mortality | Survival | Total | HR (95% CI) | P-value | Adjusted
HRa (95% CI) | P-value |
|---|
| >0.143 | 11 | 69 | 80 |
|
|
|
|
| ≤0.143 | 7 | 13 | 20 | 2.89
(1.12–7.49) | <0.05 | 2.73
(1.04–7.16) | <0.05 |
Functional analysis of miR-186 in
GIST-T1 cells
The association between low miR-186 expression and
malignant characteristics of GISTs suggests that miR-186 may act as
a tumor suppressor in these tumors. The present study therefore
investigated the function of miR-186 in GIST cells. RT-qPCR
revealed that GIST-T1 cells strongly express miR-186
(miR-186/U6=7.34). The present study therefore transiently
transfected GIST-T1 cells with an inhibitor of miR-186 or a
negative control and assessed their effects on cell viability and
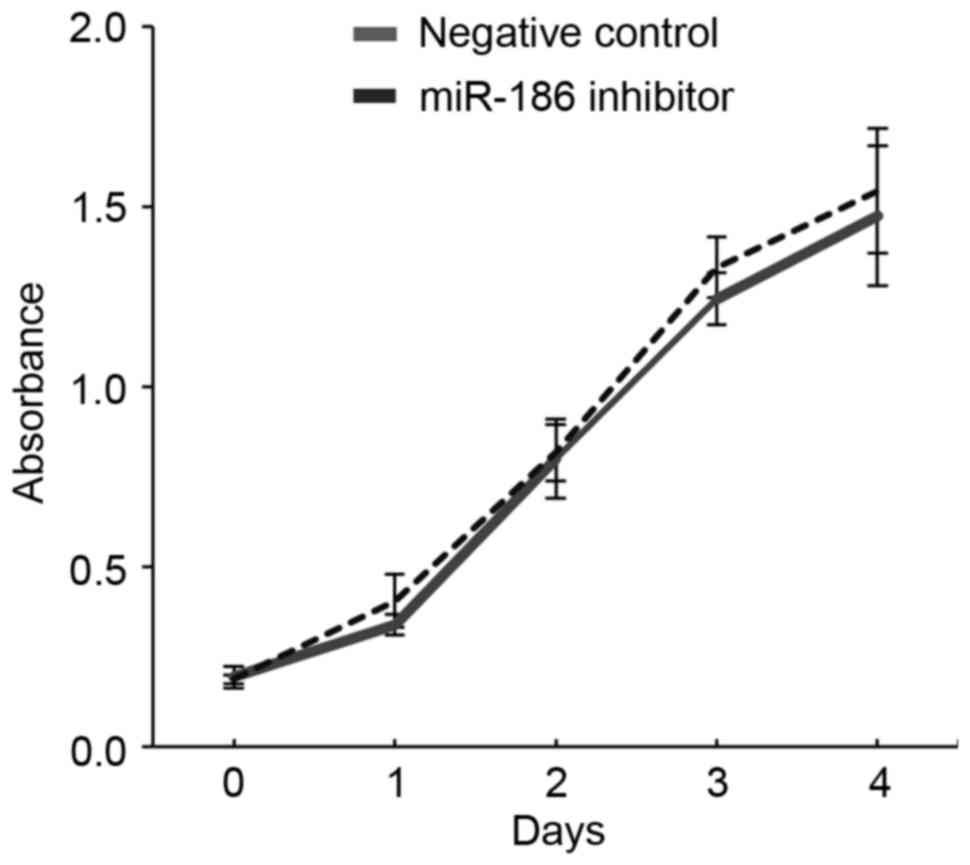
migration. It was revealed that inhibiting miR-186 in GIST-T1 cells
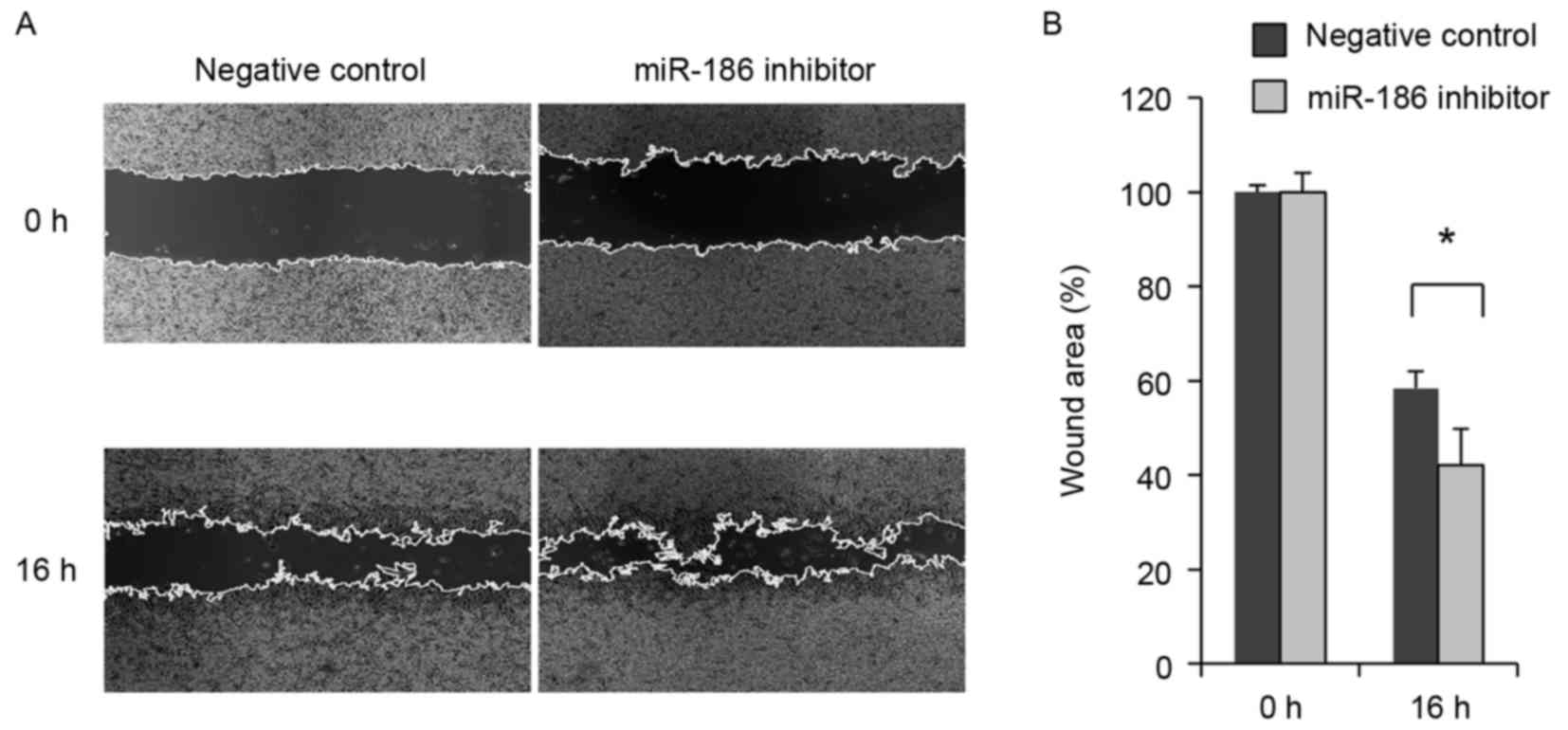
did not affect cellular proliferation (Fig. 3). By contrast, wound healing assays
revealed that inhibiting miR-186 promoted GIST-T1 cell migration
(Fig. 4).
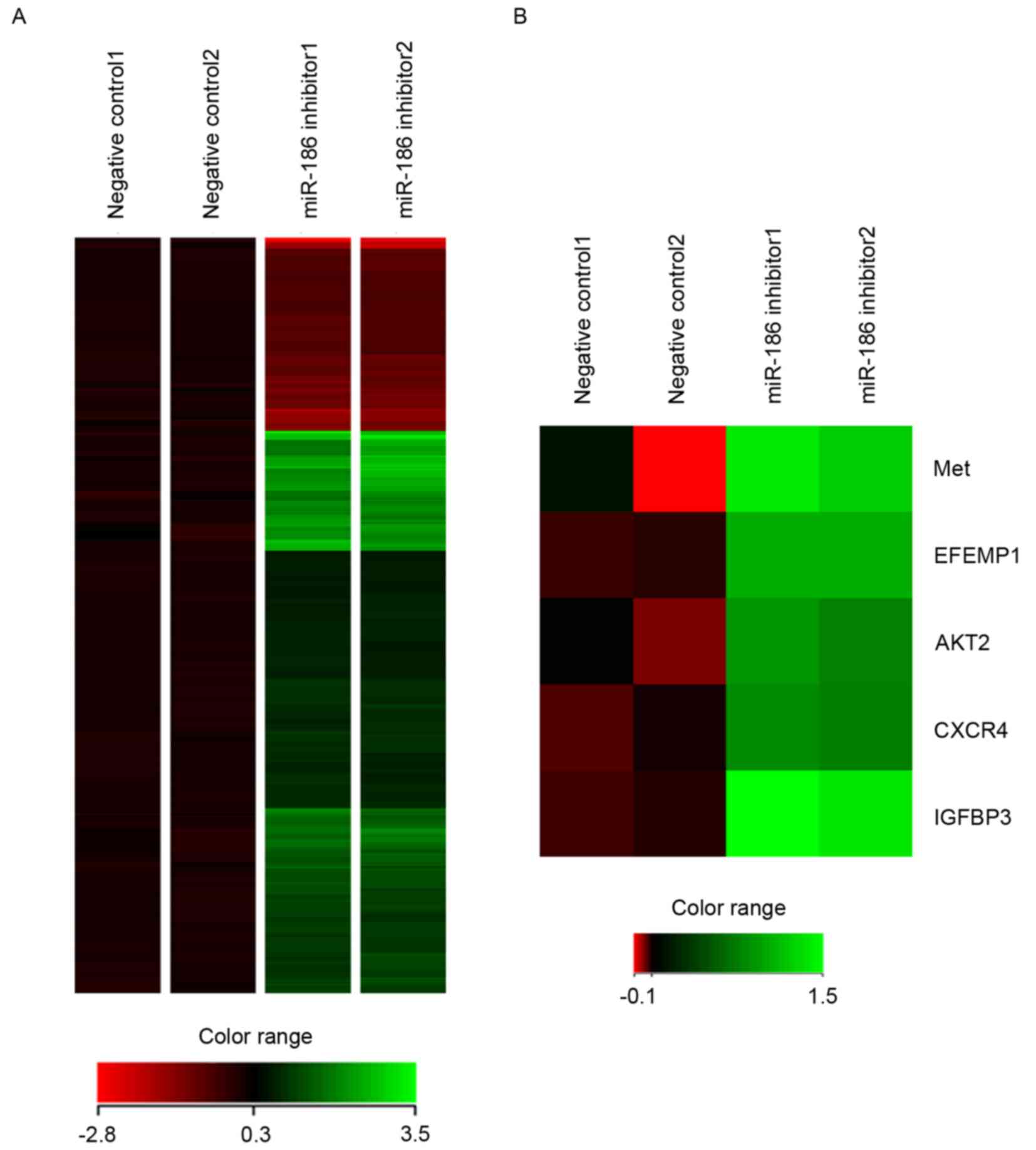
To identify downstream targets of miR-186 in GIST
cells, gene expression microarray analysis was conducted in GIST-T1
cells transfected with the miR-186 inhibitor or negative control.
It was revealed that 253 probe sets (corresponding to 229 unique
genes) were upregulated and 87 probe sets (corresponding to 66
unique genes) were downregulated by the miR-186 inhibitor in
GIST-T1 cells (Fig. 5A). Among them,
it was noted that several genes were implicated in cancer
metastasis, including MET (hepatocyte growth factor
receptor), EFEMP1 (epidermal growth factor-containing
fibulin-like extracellular matrix protein 1), AKT serine/threonine
kinase 2, CXCR4 (CXC chemokine receptor 4) and IGFBP3
(insulin-like growth factor-binding protein 3), were all
upregulated by inhibition of miR-186 (Fig. 5B).
Discussion
Numerous miRNAs are reportedly implicated in
tumorigenesis, acting as oncogenes or tumor suppressors (4,5). The
present study revealed that low levels of miR-186 expression were
associated with metastatic recurrence and a worse outcome in
patients with GISTs. Functional analysis revealed that inhibiting
miR-186 in GIST cells promotes cell migration and upregulates a set
of genes involved in cancer metastasis, which supports our
hypothesis that the downregulation of miR-186 is, at least in part,
associated with metastatic recurrence of GISTs.
Studies have revealed suggested that miR-186 acts as
a tumor suppressor in lung adenocarcinoma (16), esophageal squamous cell carcinoma
(17), hepatocellular carcinoma (HCC)
(18) and bladder cancer (19). In lung adenocarcinoma, downregulated
expression of miR-186 is associated with poor survival, whilst
overexpression of miR-186 inhibits cellular proliferation by
inducing G1-S cell cycle arrest (16). miR-186 also reportedly inhibits the
migration and invasion of non-small cell lung cancer (NSCLC) cells
by targeting the pituitary tumor transforming gene (20). Another study has reported that miR-186
suppresses the growth and metastasis of NSCLC cells by targeting
Rho-associated protein kinase 1 (21). In bladder cancer, miR-186 suppresses
cellular proliferation and invasion by targeting nucleosomal
binding protein 1 (also termed high mobility group nucleosome
binding domain 5) (19). miR-186 is
also downregulated in several HCC cell lines, where it suppresses
cell migration, invasion and proliferation by targeting
Yes-associated protein 1 (18). The
introduction of miR-186 into ovarian cancer cells downregulates
Twist1, which leads to induction of mesenchymal-to-epithelial
transition, G1 cell cycle arrest and apoptosis (22). By contrast, miR-186 is reportedly
overexpressed in pancreatic ductal adenocarcinoma and is associated
with a poor prognosis (23). These
results clearly suggest that altered expression of miR-186 affects
tumor growth, invasion and metastasis in various cancers, although
its function may differ among malignancies of different
origins.
Microarray analysis in the present study revealed
that inhibiting miR-186 in GIST cells upregulated a set of genes
implicated in cancer metastasis. IGFBP3 interacts with insulin-like
growth factor (IGF), which antagonizes IGF1 activities or,
conversely, stabilizes tumorigenic potential (24). An association between high IGFBP3
expression and distant metastasis has been reported in oral
squamous cell carcinoma (25),
colorectal cancer (26) and
pancreatic endocrine neoplasms (27).
IGF signaling has also been implicated in GIST. IGF1 receptor is
reportedly overexpressed in all GIST cases, and higher levels of
IGF1 and IGF2 expression are positively associated with malignant
clinicopathological characteristics, including larger tumor size,
higher mitotic count, higher risk and metastasis (28). However, functional analysis of IGFBP3
in GIST cells yielded complicated results. Loss of IGFBP3 from
GIST882 cells, where IGFBP3 is abundantly expressed, suppressed
cell viability, whereas overexpression of IGFBP3 in GIST-T1 cells,
where IGFBP3 is not endogenously expressed, had a cytotoxic effect
(29). Although these results suggest
that IGFBP3 has dual opposing effects on GIST cell viability, its
effects on GIST recurrence and metastasis remains to be
clarified.
It is known that hepatocyte growth factor receptor
(c-Met)/phosphatidylinositol 3-kinase (PI3K)/protein kinase B (Akt)
signaling performs a pivotal role in promoting
epithelial-mesenchymal transition (EMT), and miRNAs reportedly
affect the process. For instance, miR-206 inhibits hepatocyte
growth factor-induced EMT by directly targeting c-Met and
suppressing its downstream PI3K/Akt/mechanistic target of rapamycin
signaling pathway (30). In gastric
cancer, miR-338-3p directly targets ZEB2 and metastasis-associated
in colon cancer-1 (MACC1), which results in repression of
MACC1/Met/Akt signaling and EMT (31). By contrast, miR-93 activates
Met/PI3K/Akt activity in HCC by directly inhibiting phosphatase and
tensin homolog and cyclin dependent kinase inhibitor 1A (32). Taken together with these observations,
our results suggest that miR-186 may regulate GIST metastasis by
modulating Met/Akt signaling. CXCR4 is a receptor for chemokine CXC
ligand 12 (also termed stromal cell-derived factor 1), and their
binding leads to the activation of several key signal pathways that
promote cancer growth and metastasis (33). Elevated expression of CXCR4, for
example, has been observed in breast (34) and colorectal cancer (35), and head and neck squamous cell
carcinoma (HNSCC) (36). Activation
of CXCR4 in estrogen receptor-positive breast cancer cells drives a
metastatic and endocrine therapy-resistant phenotype by increasing
MAPK signaling (34). Overexpression
of CXCR4 is associated with lymph node metastasis and poor
disease-free survival in colorectal cancer (35). In addition, high CXCR4 expression is
associated with distant metastasis in HNSCC (36). Notably, one recent study demonstrated
that deletion of exon 11 codons 557–558 from KIT is
associated with GIST liver metastasis (37). Mechanistically, KIT exon 11
557–558 deletion upregulates CXCR4 through increased binding of ETS
variant 1 to the CXCR4 promoter. This in turn leads to
increased GIST cell motility and liver metastasis. EFEMP1 is member
of the fibulin family of extracellular matrix proteins, and its
overexpression correlates with lymph node metastasis in ovarian
cancer (38). EFEMP1 has also been
demonstrated to promote migration, invasion and metastasis in
osteosarcoma, and upregulation of EFEMP1 is an indicator of poor
prognosis (39). Upregulation of
CXCR4 and EFEMP1 through miR-186 inhibition in
GIST-T1 cells suggests that downregulation of miR-186 is associated
with an increased risk of metastatic recurrence in GIST.
In summary, the present study revealed that low
miR-186 expression is associated with metastatic recurrence and a
poor prognosis in patients with GIST. Downregulation of miR-186 may
promote GIST metastasis by inducing expression of
metastasis-associated genes. miR-186 may thus be a useful biomarker
for predicting recurrence and assessing prognosis in patients with
GIST, and could potentially be an effective therapeutic agent with
which to treat malignant GISTs.
Acknowledgements
The authors would like to thank Ms. Mutsumi Toyota
and Ms. Tomo Hatahira for technical assistance and Dr William F.
Goldman for editing the manuscript. The present study was supported
in part by ‘Grants-in-Aid for Young Investigators (B)’ from Japan
Society for the Promotion of Science (grant no. JSPS KAKENHI
16K19352) and Grant-in-Aid for Scientific Research (B) from Japan
Society for the Promotion of Science (grant no. JSPS KAKENHI
15H04299).
References
|
1
|
Joensuu H, Hohenberger P and Corless CL:
Gastrointestinal stromal tumour. Lancet. 382:973–983. 2013.
View Article : Google Scholar : PubMed/NCBI
|
|
2
|
Killian JK, Kim SY, Miettinen M, Smith C,
Merino M, Tsokos M, Quezado M, Smith WI Jr, Jahromi MS, Xekouki P,
et al: Succinate dehydrogenase mutation underlies global epigenomic
divergence in gastrointestinal stromal tumor. Cancer Discov.
3:648–657. 2013. View Article : Google Scholar : PubMed/NCBI
|
|
3
|
Bartel DP: MicroRNAs: Genomics,
biogenesis, mechanism, and function. Cell. 116:281–297. 2004.
View Article : Google Scholar : PubMed/NCBI
|
|
4
|
Croce CM: Causes and consequences of
microRNA dysregulation in cancer. Nat Rev Genet. 10:704–714. 2009.
View Article : Google Scholar : PubMed/NCBI
|
|
5
|
Esquela-Kerscher A and Slack FJ:
Oncomirs-microRNAs with a role in cancer. Nat Rev Cancer.
6:259–269. 2006. View
Article : Google Scholar : PubMed/NCBI
|
|
6
|
Isosaka M, Niinuma T, Nojima M, Kai M,
Yamamoto E, Maruyama R, Nobuoka T, Nishida T, Kanda T, Taguchi T,
et al: A Screen for epigenetically silenced microRNA genes in
gastrointestinal stromal tumors. PLoS One. 10:e01337542015.
View Article : Google Scholar : PubMed/NCBI
|
|
7
|
Niinuma T, Suzuki H, Nojima M, Nosho K,
Yamamoto H, Takamaru H, Yamamoto E, Maruyama R, Nobuoka T, Miyazaki
Y, et al: Upregulation of miR-196a and HOTAIR drive malignant
character in gastrointestinal stromal tumors. Cancer Res.
72:1126–1136. 2012. View Article : Google Scholar : PubMed/NCBI
|
|
8
|
Valastyan S and Weinberg RA: Tumor
metastasis: Molecular insights and evolving paradigms. Cell.
147:275–292. 2011. View Article : Google Scholar : PubMed/NCBI
|
|
9
|
Ma L, Teruya-Feldstein J and Weinberg RA:
Tumour invasion and metastasis initiated by microRNA-10b in breast
cancer. Nature. 449:682–688. 2007. View Article : Google Scholar : PubMed/NCBI
|
|
10
|
Zhu S, Wu H, Wu F, Nie D, Sheng S and Mo
YY: MicroRNA-21 targets tumor suppressor genes in invasion and
metastasis. Cell Res. 18:350–359. 2008. View Article : Google Scholar : PubMed/NCBI
|
|
11
|
Gregory PA, Bert AG, Paterson EL, Barry
SC, Tsykin A, Farshid G, Vadas MA, Khew-Goodall Y and Goodall GJ:
The miR-200 family and miR-205 regulate epithelial to mesenchymal
transition by targeting ZEB1 and SIP1. Nat Cell Biol. 10:593–601.
2008. View
Article : Google Scholar : PubMed/NCBI
|
|
12
|
Fletcher CD, Berman JJ, Corless C,
Gorstein F, Lasota J, Longley BJ, Miettinen M, O'Leary TJ, Remotti
H, Rubin BP, et al: Diagnosis of gastrointestinal stromal tumors: A
consensus approach. Hum Pathol. 33:459–465. 2002. View Article : Google Scholar : PubMed/NCBI
|
|
13
|
Taguchi T, Sonobe H, Toyonaga S, Yamasaki
I, Shuin T, Takano A, Araki K, Akimaru K and Yuri K: Conventional
and molecular cytogenetic characterization of a new human cell
line, GIST-T1, established from gastrointestinal stromal tumor. Lab
Invest. 82:663–665. 2002. View Article : Google Scholar : PubMed/NCBI
|
|
14
|
Livak KJ and Schmittgen TD: Analysis of
relative gene expression data using real-time quantitative PCR and
the 2(-Delta Delta C (T)) Method. Methods. 25:402–408. 2001.
View Article : Google Scholar : PubMed/NCBI
|
|
15
|
http://www.jichi.ac.jp/saitama-sct/SaitamaHP.files/statmedEN.html
|
|
16
|
Cai J, Wu J, Zhang H, Fang L, Huang Y,
Yang Y, Zhu X, Li R and Li M: miR-186 downregulation correlates
with poor survival in lung adenocarcinoma, where it interferes with
cell-cycle regulation. Cancer Res. 73:756–766. 2013. View Article : Google Scholar : PubMed/NCBI
|
|
17
|
He W, Feng J, Zhang Y, Wang Y, Zang W and
Zhao G: microRNA-186 inhibits cell proliferation and induces
apoptosis in human esophageal squamous cell carcinoma by targeting
SKP2. Lab Invest. 96:317–324. 2016. View Article : Google Scholar : PubMed/NCBI
|
|
18
|
Ruan T, He X, Yu J and Hang Z:
MicroRNA-186 targets Yes-associated protein 1 to inhibit Hippo
signaling and tumorigenesis in hepatocellular carcinoma. Oncol
Lett. 11:2941–2945. 2016.PubMed/NCBI
|
|
19
|
Yao K, He L, Gan Y, Zeng Q, Dai Y and Tan
J: MiR-186 suppresses the growth and metastasis of bladder cancer
by targeting NSBP1. Diagn Pathol. 10:1462015. View Article : Google Scholar : PubMed/NCBI
|
|
20
|
Li H, Yin C, Zhang B, Sun Y, Shi L, Liu N,
Liang S, Lu S, Liu Y, Zhang J, et al: PTTG1 promotes migration and
invasion of human non-small cell lung cancer cells and is modulated
by miR-186. Carcinogenesis. 34:2145–2155. 2013. View Article : Google Scholar : PubMed/NCBI
|
|
21
|
Cui G, Cui M, Li Y, Liang Y, Li W, Guo H
and Zhao S: MiR-186 targets ROCK1 to suppress the growth and
metastasis of NSCLC cells. Tumour Biol. 35:8933–8937. 2014.
View Article : Google Scholar : PubMed/NCBI
|
|
22
|
Zhu X, Shen H, Yin X, Long L, Xie C, Liu
Y, Hui L, Lin X, Fang Y, Cao Y, et al: miR-186 regulation of Twist1
and ovarian cancer sensitivity to cisplatin. Oncogene. 35:323–332.
2016. View Article : Google Scholar : PubMed/NCBI
|
|
23
|
Zhang ZL, Bai ZH, Wang XB, Bai L, Miao F
and Pei HH: miR-186 and 326 predict the prognosis of pancreatic
ductal adenocarcinoma and affect the proliferation and migration of
cancer cells. PLoS One. 10:e01188142015. View Article : Google Scholar : PubMed/NCBI
|
|
24
|
Baxter RC: IGF binding proteins in cancer:
Mechanistic and clinical insights. Nat Rev Cancer. 14:329–341.
2014. View
Article : Google Scholar : PubMed/NCBI
|
|
25
|
Yen YC, Hsiao JR, Jiang SS, Chang JS, Wang
SH, Shen YY, Chen CH, Chang IS, Chang JY and Chen YW: Insulin-like
growth factor-independent insulin-like growth factor binding
protein 3 promotes cell migration and lymph node metastasis of oral
squamous cell carcinoma cells by requirement of integrin b1.
Oncotarget. 6:41837–41855. 2015. View Article : Google Scholar : PubMed/NCBI
|
|
26
|
Georges RB, Adwan H, Hamdi H, Hielscher T,
Linnemann U and Berger MR: The insulin-like growth factor binding
proteins 3 and 7 are associated with colorectal cancer and liver
metastasis. Cancer Biol Ther. 12:69–79. 2011. View Article : Google Scholar : PubMed/NCBI
|
|
27
|
Hansel DE, Rahman A, House M, Ashfaq R,
Berg K, Yeo CJ and Maitra A: Met proto-oncogene and insulin-like
growth factor binding protein 3 overexpression correlates with
metastatic ability in well-differentiated pancreatic endocrine
neoplasms. Clin Cancer Res. 10:6152–6158. 2004. View Article : Google Scholar : PubMed/NCBI
|
|
28
|
Braconi C, Bracci R, Bearzi I, Bianchi F,
Sabato S, Mandolesi A, Belvederesi L, Cascinu S, Valeri N and
Cellerino R: Insulin-like growth factor (IGF) 1 and 2 help to
predict disease outcome in GIST patients. Ann Oncol. 19:1293–1298.
2008. View Article : Google Scholar : PubMed/NCBI
|
|
29
|
Dupart JJ, Trent JC, Lee HY, Hess KR,
Godwin AK, Taguchi T and Zhang W: Insulin-like growth factor
binding protein-3 has dual effects on gastrointestinal stromal
tumor cell viability and sensitivity to the anti-tumor effects of
imatinib mesylate in vitro. Mol Cancer. 8:992009. View Article : Google Scholar : PubMed/NCBI
|
|
30
|
Chen QY, Jiao DM, Wu YQ, Chen J, Wang J,
Tang XL, Mou H, Hu HZ, Song J, Yan J, et al: MiR-206 inhibits
HGF-induced epithelial-mesenchymal transition and angiogenesis in
non-small cell lung cancer via c-Met/PI3k/Akt/mTOR pathway.
Oncotarget. 7:18247–18261. 2016. View Article : Google Scholar : PubMed/NCBI
|
|
31
|
Huang N, Wu Z, Lin L, Zhou M, Wang L, Ma
H, Xia J, Bin J, Liao Y and Liao W: MiR-338-3p inhibits
epithelial-mesenchymal transition in gastric cancer cells by
targeting ZEB2 and MACC1/Met/Akt signaling. Oncotarget.
6:15222–15234. 2015. View Article : Google Scholar : PubMed/NCBI
|
|
32
|
Ohta K, Hoshino H, Wang J, Ono S, Iida Y,
Hata K, Huang SK, Colquhoun S and Hoon DS: MicroRNA-93 activates
c-Met/PI3K/Akt pathway activity in hepatocellular carcinoma by
directly inhibiting PTEN and CDKN1A. Oncotarget. 6:3211–3224. 2015.
View Article : Google Scholar : PubMed/NCBI
|
|
33
|
Guo F, Wang Y, Liu J, Mok SC, Xue F and
Zhang W: CXCL12/CXCR4: A symbiotic bridge linking cancer cells and
their stromal neighbors in oncogenic communication networks.
Oncogene. 35:816–826. 2016. View Article : Google Scholar : PubMed/NCBI
|
|
34
|
Rhodes LV, Short SP, Neel NF, Salvo VA,
Zhu Y, Elliott S, Wei Y, Yu D, Sun M, Muir SE, et al: Cytokine
receptor CXCR4 mediates estrogen-independent tumorigenesis,
metastasis, and resistance to endocrine therapy in human breast
cancer. Cancer Res. 71:603–613. 2011. View Article : Google Scholar : PubMed/NCBI
|
|
35
|
Ottaiano A, Franco R, Talamanca Aiello A,
Liguori G, Tatangelo F, Delrio P, Nasti G, Barletta E, Facchini G,
Daniele B, et al: Overexpression of both CXC chemokine receptor 4
and vascular endothelial growth factor proteins predicts early
distant relapse in stage II–III colorectal cancer patients. Clin
Cancer Res. 12:2795–2803. 2006. View Article : Google Scholar : PubMed/NCBI
|
|
36
|
Katayama A, Ogino T, Bandoh N, Nonaka S
and Harabuchi Y: Expression of CXCR4 and its down-regulation by
IFN-gamma in head and neck squamous cell carcinoma. Clin Cancer
Res. 11:2937–2946. 2005. View Article : Google Scholar : PubMed/NCBI
|
|
37
|
Wang HC, Li TY, Chao YJ, Hou YC, Hsueh YS,
Hsu KH and Shan YS: KIT exon 11 codons 557–558 deletion mutation
promotes liver metastasis through the CXCL12/CXCR4 axis in
gastrointestinal stromal tumors. Clin Cancer Res. 22:3477–3487.
2016. View Article : Google Scholar : PubMed/NCBI
|
|
38
|
Chen J, Wei D, Zhao Y, Liu X and Zhang J:
Overexpression of EFEMP1 correlates with tumor progression and poor
prognosis in human ovarian carcinoma. PLoS One. 8:e787832013.
View Article : Google Scholar : PubMed/NCBI
|
|
39
|
Wang Z, Cao CJ, Huang LL, Ke ZF, Luo CJ,
Lin ZW, Wang F, Zhang YQ and Wang LT: EFEMP1 promotes the migration
and invasion of osteosarcoma via MMP-2 with induction by AEG-1 via
NF-κB signaling pathway. Oncotarget. 6:14191–14208. 2015.
View Article : Google Scholar : PubMed/NCBI
|