Introduction
Breast cancer is the most common cancer among women
and the second most common cancer worldwide (1). It has been estimated that there were
1.7 million new cases and 521,900 deaths due to the disease in
2012; this corresponds to 25% of all new cancer cases and 15% of
cancer deaths among women, respectively (2). Family history, environment and stress
are all somehow implicated in the development of breast cancer
(3). The 5-year survival of women
with breast cancer is highly dependent on tumor stage: that of
women with stage 0 or I is 98% and those of stages II and III are
85 and 60%, respectively (4).
However, the 5-year survival of stage IV is only 20% (4). Early detection of breast cancer can
provide increased treatment options as well as improved conditions
for treatment or surgery.
Diagnostic techniques including mammography,
magnetic resonance imaging, ultrasound, computerized tomography,
positron emission tomography and biopsy have been used for
detecting breast cancer (5). These
strategies are expensive, time-consuming and cannot cope with large
numbers of patients at the same time. Cancer screening using serum
biomarkers would be an ideal diagnostic technique since cancer
could be detected by routine health examination. Moreover, such
screening could increase the rate of detection of early stage
cancer and eventually lead to increased survival.
CA15-3 is a soluble form of MUC1, a transmembrane
protein that possesses variable numbers of tandem repeats of
peptides modified by glycosylation, and the most extensively
studied serum biomarker for breast cancer (6). The current system for detecting serum
CA15-3 is a sandwich enzyme-linked immunosorbent assay (ELISA)
using two types of monoclonal anti-CA15-3 antibodies (115D8:
capture antibody; DF3: detection antibody) (7,8).
Attempts to use ELISA systems in the screening of breast cancer
over the past three decades have indicated that the serum CA15-3
level is not suitable for early detection of breast cancer since
its level rarely increases in patients with early or localized
breast cancer (7). CA15-3 remains
useful for monitoring the effects of treatment in patients with
metastatic breast cancer (9).
Currently, the American Society of Clinical Oncology does not
recommend use of CA15-3 for screening, diagnosis, staging, or
routine surveillance of breast cancer (10).
Changes in glycosylation are a hallmark of cancer
progression. Numerous studies suggest that aberrant glycosylation
is a sensitive indicator of carcinogenesis (11). Cancer-related changes in
glycosylation are thought to involve altered expression of
glycosyltransferase and chaperone genes, and mislocalization of
glycosyltransferases (11). Most
analyses of glycosylation have involved highly purified
glycoproteins and expensive procedures such as mass spectrometry,
capillary electrophoresis and high-performance liquid
chromatography. These are not suitable for routine examination
although they provide detailed glycosylation profiles.
Since CA15-3 is a heavily glycosylated protein
(12), glycosylation changes have
great potential for reflecting carcinogenesis, and previous studies
have indeed pointed to glycosylation changes of CA15-3 in breast
cancer (13). Antibody-lectin
sandwich assays have been suggested as platforms for examining
glycosylation in non-purified serum samples (14). In such assays, the antibody against
the target glycoprotein immobilized on 96-well plates captures the
serum glycoprotein, and glycosylation of the glycoprotein is
detected with a lectin (15). There
is some evidence that antibody-lectin sandwich assays can be used
for cancer screening (16,17). However, the capture antibody is also
glycosylated and this can interfere with detection of the target
glycosylation signal. Also, glycoproteins contained in blocking
agents can inhibit the target signal.
In the present study, we developed an
antibody-lectin sandwich assay for detecting glycosylation of
CA15-3 in non-purified serum samples that was designed to overcome
these technical issues. Our results indicated that this strategy is
useful for screening early or localized breast cancer.
Materials and methods
Ethical approval
This study was carried out with the approval of the
Ewha Womans University Mokdong Hospital Institutional Review Board
(Seoul, Korea) and was conducted in accordance with the Declaration
of Helsinki. Serum samples of patients were collected after
obtaining written informed consents.
Specimens
Samples were collected in a prospective and
consecutive manner. Sera from women diagnosed with benign breast
disease (n=47) and breast cancer stages 0 (n=6), I (n=48), IIA
(n=36), IIB (n=12) and III (n=26) were collected from November 2015
to January 2017 at the Breast and Thyroid Cancer Center of Ewha
Womans University Cancer Center for Women. The mean age of the
benign group was 40, and those of breast cancer stage 0, I, IIA,
IIB and III were 49, 51, 50, 55 and 54, respectively. The age range
of the benign group was 19–74, and those of breast cancer stage 0,
I, IIA, IIB and III were 25–76, 29–78, 29–75, 33–83 and 36–78,
respectively. The breast cancer stage was determined according to
the tumor-node-metastasis (TNM) staging system. Serum samples were
collected before surgery or treatment. Each serum sample was
centrifuged at 12,000 × g for 10 min, aliquoted and stored at −80°C
until use, and a vial set was used within a few days after
thawing.
Investigation of the effects of
oxidation of the coating antibody and blocking agent
Immunoplates (96-wells) (Greiner Bio-One,
Kremsmünster, Austria) were coated with mouse anti-CA15-3
monoclonal antibody (100 ng/well; vol. 100 µl; cat. no. 10-C03E;
Fitzgerald Industries International, Acton, MA, USA) or regular
fetal bovine serum (FBS; vol. 100 µl; GenDEPOT, Barker, TX, USA) at
4°C for 16 h. The anti-CA15-3 monoclonal antibody and FBS were
prepared in phosphate-buffered saline (PBS) at 1 µg/ml and 10%
(v/v), respectively. The coated wells were reacted with 320 µl
oxidation buffer [50 mM sodium acetate (Duksan Pure Chemicals, Co.,
Ltd., Ansan, Korea), 50 mM sodium metaperiodate (Sigma-Aldrich;
Merck, St. Louis, MO, USA) pH 4.0] for 1 h at room temperature.
Control wells were reacted with Tris-buffered saline (TBS)
containing 1% Tween-20 (TBS-T) instead of oxidation buffer. The
plates were blocked with TBS-T for 3 h at room temperature
(reaction vol. 320 µl). Twelve types of biotinylated lectin were
prepared in TBS-T at final concentrations of 1 µg/ml and incubated
on the plates for 1 h at room temperature (reaction vol. 100 µl).
All the lectins were purchased from Vector Laboratories, Inc.
(Burlingame, CA, USA). Lectins bound to the coated antibody or FBS
were detected with poly-horseradish peroxidase (HRP)-conjugated
streptavidin (Pierce; Thermo Fisher Scientific, Inc., Waltham, MA,
USA; 1/10,000 dilution; reaction vol. 100 µl). The plates were
washed three to five times using TBS-T between reactions. Color
reactions were developed with o-phenylenediamine
(Sigma-Aldrich; Merck) and measured at 492 nm.
Antibody-lectin sandwich assay for the
detection of the glycosylation of CA15-3
Immunoplates (96 wells) were coated with mouse
anti-CA15-3 monoclonal antibody (100 ng/well, vol. 100 µl) in PBS
for 16 h at 4°C, then blocked with 10% FBS in TBS-T (320 µl) for 3
h at room temperature. The coating antibody and FBS were oxidized
using the oxidation buffer (320 µl) aforementioned to block lectin
binding. The wells were further blocked with 1% oxidized bovine
serum albumin (oBSA) in TBS-T for 2 h at room temperature (reaction
vol. 320 µl). oBSA was prepared as previously described (18). BSA was dissolved at a final
concentration of 5% in the oxidation buffer, maintained at 4°C for
2 h and dialyzed against TBS-T for 2 days to remove the sodium
metaperiodate. Sera were diluted 1/3,000 or 1/4,000 using 1% oBSA
in TBS-T and reacted in the wells for 2 h at 37°C (reaction vol.
100 µl). Biotinylated lectins were prepared at a concentration of 1
µg/ml in TBS-T and reacted in the wells for 1 h at room temperature
(reaction vol. 100 µl). Thereafter lectin bound to the CA15-3
glycan was detected with poly-HRP-conjugated streptavidin (reaction
vol. 100 µl). Color was developed as aforementioned. The plates
were washed three to five times using TBS-T between reactions, and
seven washes were carried out prior to the color reaction.
A mirror plate, the coating antibody reaction which
was omitted, was prepared, to check the non-specific reaction of
the serum. The reaction of the mirror plate included blocking,
oxidation, serum reaction, lectin reaction and streptavidin
reaction steps. The values of the anti-CA15-3-ConA sandwich assays
were calculated as follows: optical density of the full series of
reactions-optical density of the mirror plate reaction.
Sandwich ELISA for the detection of
CA15-3
Immunoplates (96 wells) were coated with mouse
anti-CA15-3 monoclonal antibody (50 ng/well) and blocked with 5%
skim milk at room temperate for 3 h. Skim milk was prepared in
phosphate-buffered saline (PBS) containing 0.05% Tween-20 (PBS-T).
Then the plates were reacted with serum samples (1:100 dilution
ratio) prepared in 0.5% skim milk in PBS-T at 37°C for 2 h. The
captured CA15-3 was detected using rabbit anti-MUC1 polyclonal
antibody (1:3,000 dilution ratio; reaction: 37°C for 1 h; Sino
Biological, Inc., Beijing, China; cat. no. 12123-T24), together
with HRP-conjugated anti-rabbit IgG polyclonal antibody (1:5,000
dilution ratio; reaction: 37°C for 40 min, Bethyl Laboratories,
Inc., Montgomery, TX, USA; cat. no. A120-100P). The antibodies used
to detect CA15-3 were prepared in 0.5% skim milk in PBST-T. The
plates were washed three to five times using PBS-T between
reactions. Color reactions were developed with
o-phenylenediamine and measured at 492 nm.
Immunoprecipitation of serum
CA15-3
The serum sample was diluted 1:10 with PBS and
reacted with rabbit anti-MUC1 polyclonal antibody (Sino Biological,
Inc.; cat. no. 12123-T24) coupled with protein A agarose beads
(Sigma-Aldrich; Merck) for 16 h at 4°C. The protein A agarose beads
were mixed with 5% BSA in PBS to block non-specific reactions. The
protein A agarose beads were then washed three times with PBS-T by
centrifugation at 12,000 x g for 10 min, and the immunoprecipitates
were collected by centrifugation as aforementioned and analyzed by
western or lectin blotting.
Western blotting for CA15-3
Immunoprecipitates were diluted 1:10, fractionated
on 12.5% polyacrylamide gels, and transferred onto polyvinylidene
difluoride membranes (EMD Millipore, Burlington, MA, USA), and the
membranes were blocked with 5% skim milk (Bioworld Technology,
Inc., St. Louis Park, MN, USA) in TBS-T. CA15-3 on the
polyvinylidene difluoride membranes was detected using rabbit
anti-MUC1 polyclonal antibody (1:1,000 dilution ratio), together
with HRP-conjugated anti-rabbit IgG (1:5,000). CA15-3 and
anti-CA15-3 antibody bands were visualized on X-ray film (Kodak,
USA) using an enhanced chemiluminescence kit (AbClon, Seoul,
Korea).
Lectin blotting for detecting CA15-3
glycosylation
Immunoprecipitates were diluted 1:100, fractionated
and transferred onto polyvinylidene difluoride membranes as
aforementioned. The membranes were blocked with 5% oBSA in TBS-T
for 4 h at room temperature with shaking overnight. The
mannosylated N-glycosylation of CA15-3 was detected with
biotinylated ConA (1 µg/ml), followed by poly-HRP-conjugated
streptavidin (1:10,000). The bands were visualized as previously
described. ConA and streptavidin were prepared in 0.5% oBSA in
TBS-T.
Statistical analysis
Kruskal-Wallis or Mann-Whitney U test was used to
evaluate differences in the glycosylation level of CA15-3 between
groups, and P<0.05 was considered significant. P-values,
receiver operating characteristic (ROC) curves and area under the
curve (AUC) values were obtained using GraphPad prism version 5.01
(GraphPad Software, Inc., La Jolla, CA, USA), and sensitivity and
specificity were determined from the ROC curves: cut-offs were
selected to maximize the sum of the sensitivity and specificity.
Specificity = number of true negatives × 100/number of true
negatives + number of false positives. Sensitivity = number of true
positives × 100/number of true positives + number of false
negatives. Correlation between the mannosylated
N-glycosylation level of CA15-3 and age was analyzed by the
GraphPad prism program, and the correlation was presented as
Pearson r, correlation coefficient. Statistical power values (1-β
error) were calculated using the G*Power 3.1 program.
Results
Effects of oxidation of the coating
antibody and blocking agent
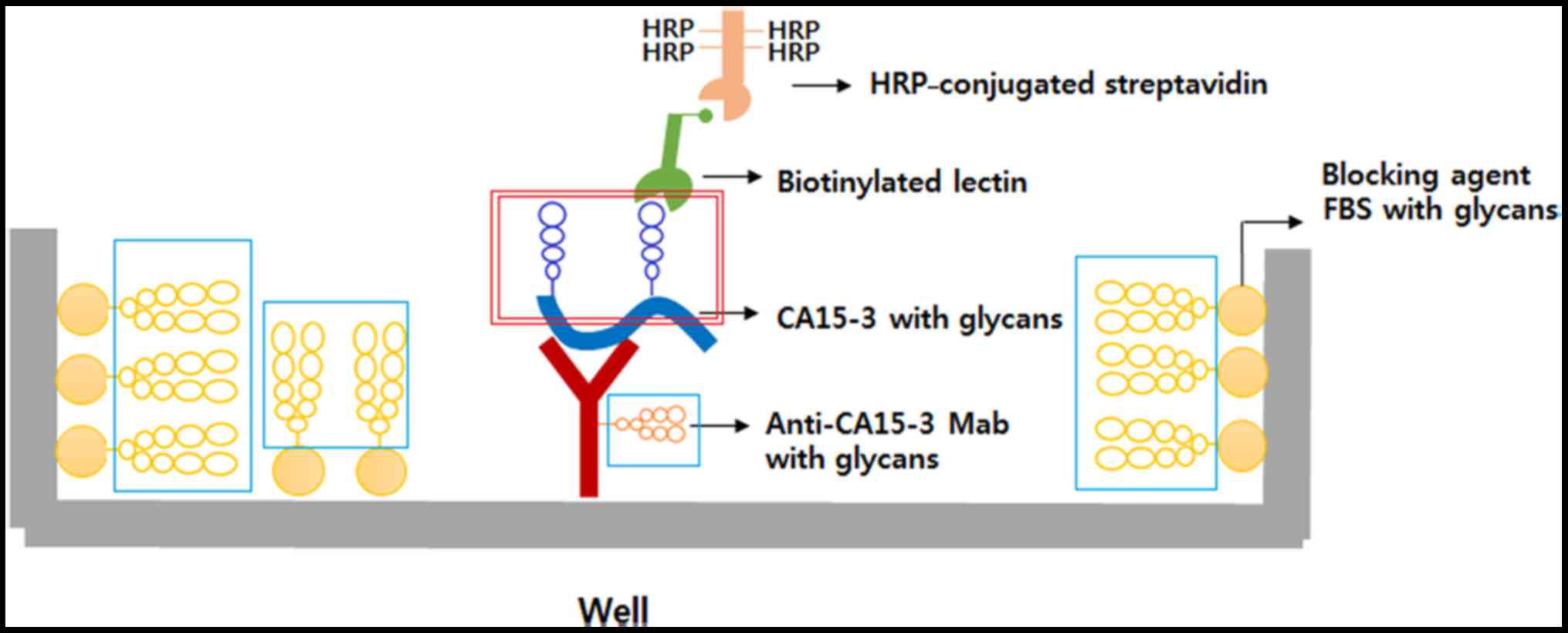
Fig. 1 is a
schematic diagram of the antibody-lectin sandwich assay for
detecting glycosylation of serum CA15-3. The basic purpose of the
system is to detect specific reactions between glycosyl groups of
CA15-3 and the lectin (red box). Both the anti-CA15-3 monoclonal
antibody used as a coating antibody and the normal FBS used as a
blocking agent contain large amounts of glycosyl groups (blue box).
Therefore, a reaction between the glycans of the coating antibody,
FBS and the lectin (blue box) have to be blocked prior to the
reaction between glycans of CA15-3 and the lectin (red box).
Twelve types of lectin were used to investigate the
lectin-binding properties of the coating antibody and FBS. The
binding-specificities of lectins for the glycan structures are
shown in Table I. FBS was found to
react strongly with Concanavalin A (ConA), Sambucus nigra
lectin (SNA), Ricinus communis agglutinin I (RCA I),
Maackia amurensis lectin II (MAA) and jacalin (Fig. 2A) while the immobilized anti-CA15-3
monoclonal antibody was found to react strongly with ConA, SNA, RCA
I, Aleuria aurantia lectin (AAL), Lens culinaris
agglutinin (LCA), Aspergillus oryzae lectin (AOL) and
jacalin (Fig. 2B). Oxidation of the
coating antibody and FBS with sodium metaperiodate caused a
significant reduction in reactivity with the lectins. However,
oxidation did not completely block the reactions of the coating
antibody and FBS with SNA, MAA and jacalin (red boxes in Fig. 2). Therefore, these three lectins
were omitted from subsequent lectin screens.
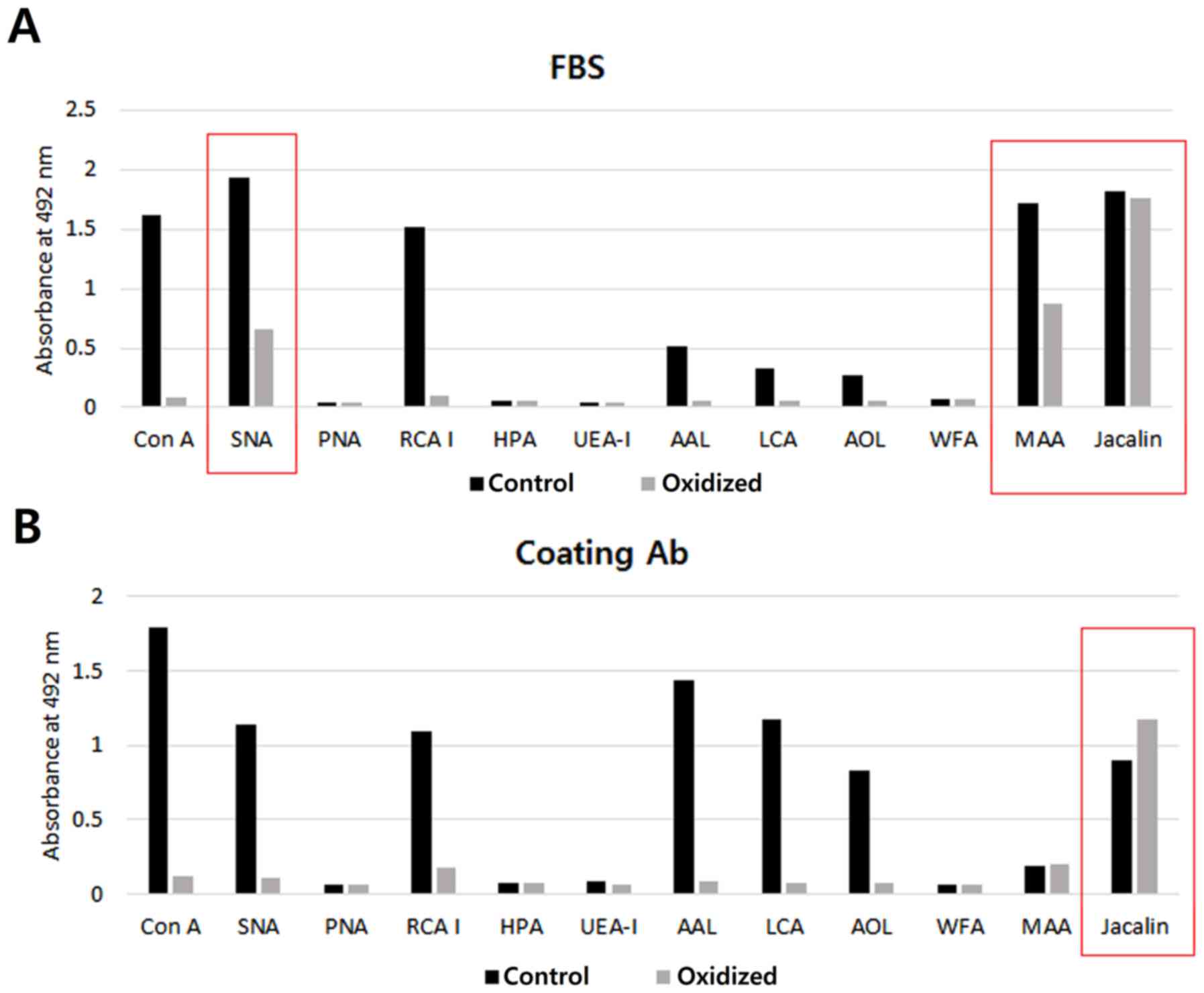 | Figure 2.The effect of oxidation on the
coating antibody and blocking agent. Immunoplates (96 wells) were
coated with (A) FBS or (B) the anti-CA15-3 monoclonal antibody and
incubated with oxidation buffer (oxidation) or TBS-T (control).
Twelve types of lectins were used. ConA, Concanavalin A; SNA,
Sambucus nigra lectin; PNA, Peanut agglutinin; RCA I,
Ricinus communis agglutinin I; HPA, Helix pomatia
agglutinin; UEA-I, Ulex europaeus agglutinin I; AAL,
Aleuria aurantia lectin; LCA, Lens culinaris
agglutinin; AOL, Aspergillus oryzae lectin; WFA, Wisteria
floribunda lectin; MAA, Maackia amurensis lectin II. |
 | Table I.Binding properties of lectins used in
this study. The binding-specificities of lectins were referred from
a previous report (15). |
Table I.
Binding properties of lectins used in
this study. The binding-specificities of lectins were referred from
a previous report (15).
| Abbreviation | Full name | Specificity | Type of glycan
linkage |
|---|
| ConA | Concanavalin A | α-linked mannose
high mannose type glycans | N-linked |
| SNA | Sambucus
nigra lectin | Sialic acid
attached to galactose in α-2,6 linkage | N- and
O-linked |
| PNA | Peanut
agglutinin | Galactose attached
to N-acetylgalactosamine in β-1,3 linkage | O-linked |
| RCA I | Ricinus
communis agglutinin I | Galactose attached
to N-acetylglucosamine in β-1,4 linkage | N-linked |
| HPA | Helix
pomatia agglutinin |
N-acetylgalactosamine | O-linked |
| UEA-I | Ulex
europaeus agglutinin I | α-linked
fucose | N- and
O-linked |
| AAL | Aleuria
aurantia lectin | Fucose linked (α
−1,6) to N-acetylglucosamine or fucose linked (α −1,3) to
N-acetyllactosamine | N- and
O-linked |
| LCA | Lens
culinaris agglutinin | α-linked mannose
α-linked fucose attached to the N-acetylchitobiose portion
markedly enhances affinity | N-linked |
| AOL | Aspergillus
oryzae lectin | α1,6-linked
fucose | N-linked |
| WFA | Wisteria
floribunda Lectin | Carbohydrate
structures terminating in N-acetylgalactosamine linked α or
β to the 3 or 6 position of galactose | NA |
| MAA | Maackia
amurensis lectin II | Sialic acid
attached to galactose in α-2,3 linkage | N- and
O-linked |
| Jacalin | Jackfruit
(Artocarpus heterophyllus) | Galactose attached
to N-acetylgalactosamine in β-1,3 linkage/mono- or
disialylated form of O-glycan | O-linked |
Selection of a lectin for detecting
glycosylation of CA15-3
Fig. 3A reveals the
results of a full series of sandwich assays using 9 different
lectins. The signal produced with ConA was considerably higher than
those produced with the other lectins. There were no reactions when
human serum or ConA reactions were omitted (Fig. 3B), confirming that the reaction was
specific for glycosylation of CA15-3. ConA has been revealed to
recognize mannosylated N-glycans (19). Hence our results indicate that the
mannosylated N-glycans of CA15-3 are the most effective
targets for the antibody-lectin sandwich assay.
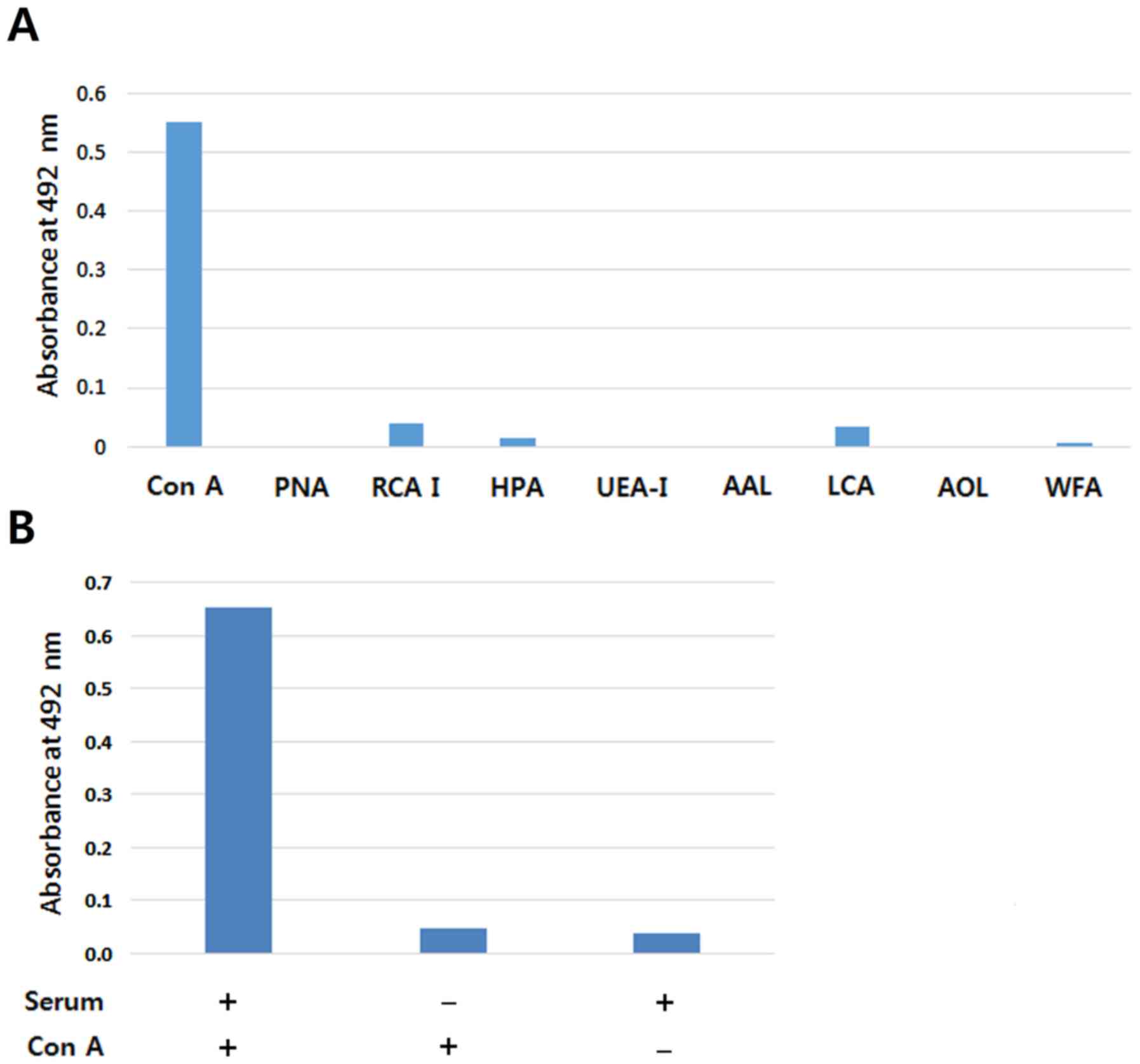 | Figure 3.Screening of lectins suitable for
detecting serum CA15-3, and the reaction specificity of the
antibody-lectin sandwich assay. (A) Antibody-lectin sandwich assays
were conducted with the 9 lectins. A mixture of sera of breast
cancer stage III (n=24) was used to screen the lectins. (B)
Specificity of the anti-CA15-3 antibody-Con A sandwich assay. The
value of human serum reaction-omitted condition or Con A
reaction-omitted condition was compared with that of a full series
reaction. ConA, Concanavalin A; PNA, Peanut agglutinin; RCA I,
Ricinus communis agglutinin I; HPA, Helix pomatia
agglutinin; UEA-I, Ulex europaeus agglutinin I; AAL,
Aleuria aurantia lectin; LCA, Lens culinaris
agglutinin; AOL, Aspergillus oryzae lectin; WFA, Wisteria
floribunda lectin. |
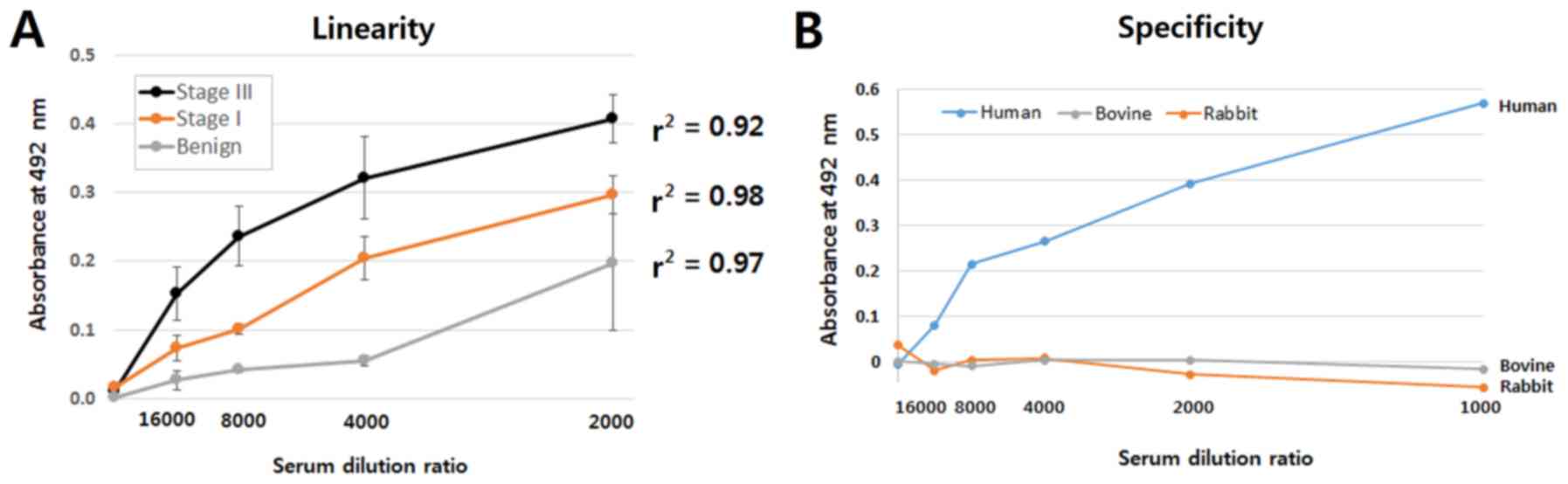
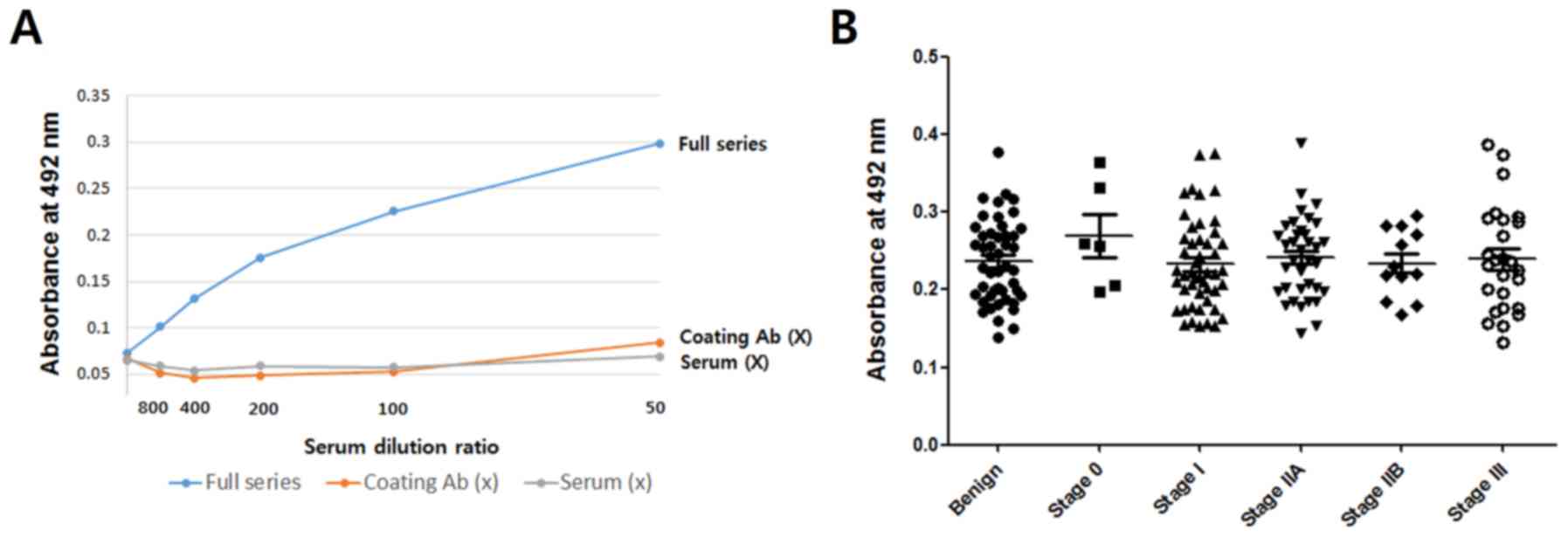
Linearity of the antibody-lectin
sandwich assay
Three serum samples each were selected from benign,
stage I and stage III cancers, respectively, to investigate
linearity as a function of serum dilution. These serum samples were
chosen to yield low, medium and high values of the sandwich assay,
respectively. As shown in Fig. 4A,
the r2 values of all three groups appeared to be high
(r2 >0.9). No signal was found when rabbit or bovine
serum was used (Fig. 4B),
indicating that the sandwich assay is specific for human
CA15-3.
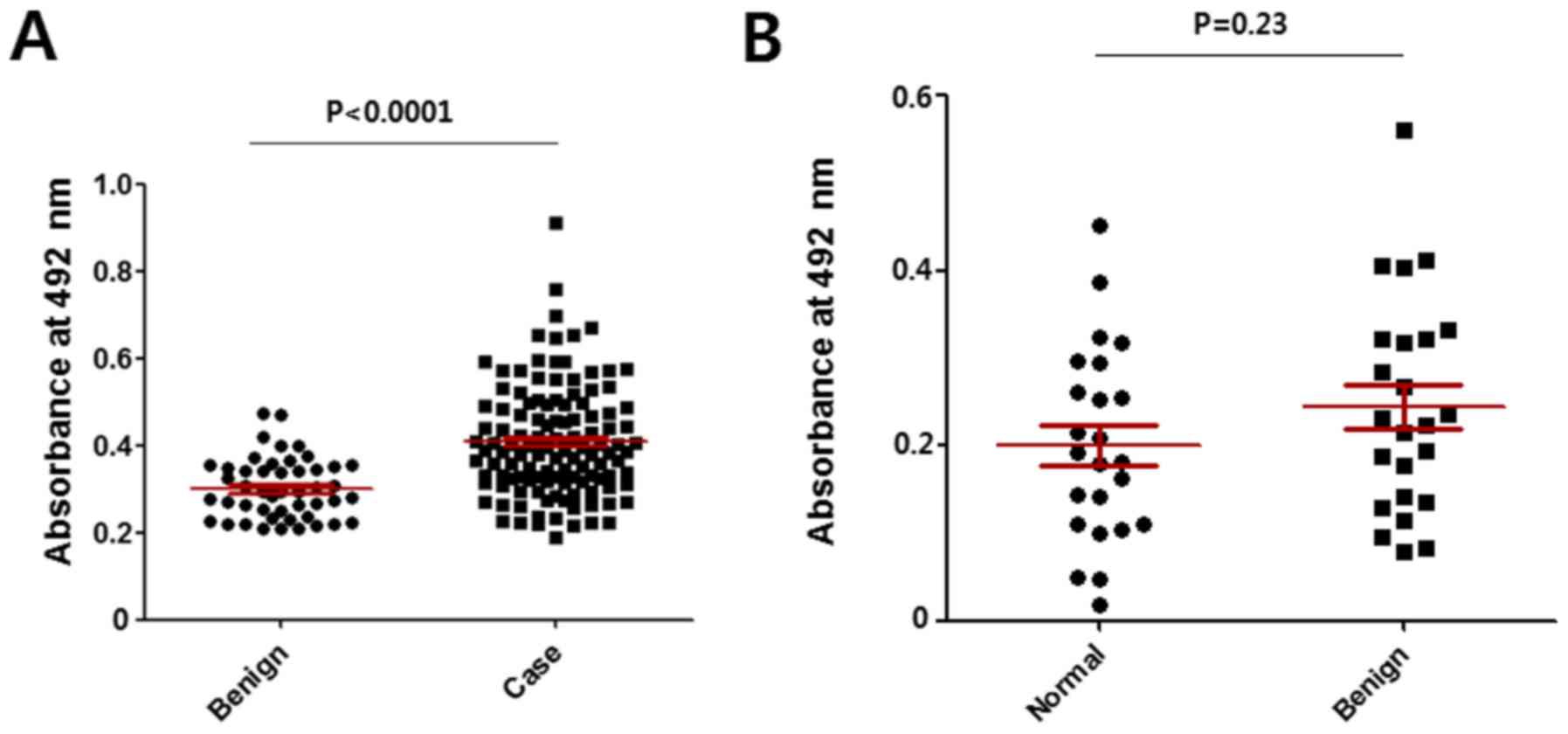
Comparison of the results for the
different cancer groups
The N-glycan levels of CA15-3 in benign
breast disease and breast cancer (cases) were assessed with the
anti-CA15-3 antibody-ConA sandwich assay. As shown in Fig. 5A, markedly higher values were found
in the breast cancers. There was no difference between the normal
and benign group in the mannosylated N-glycan level of
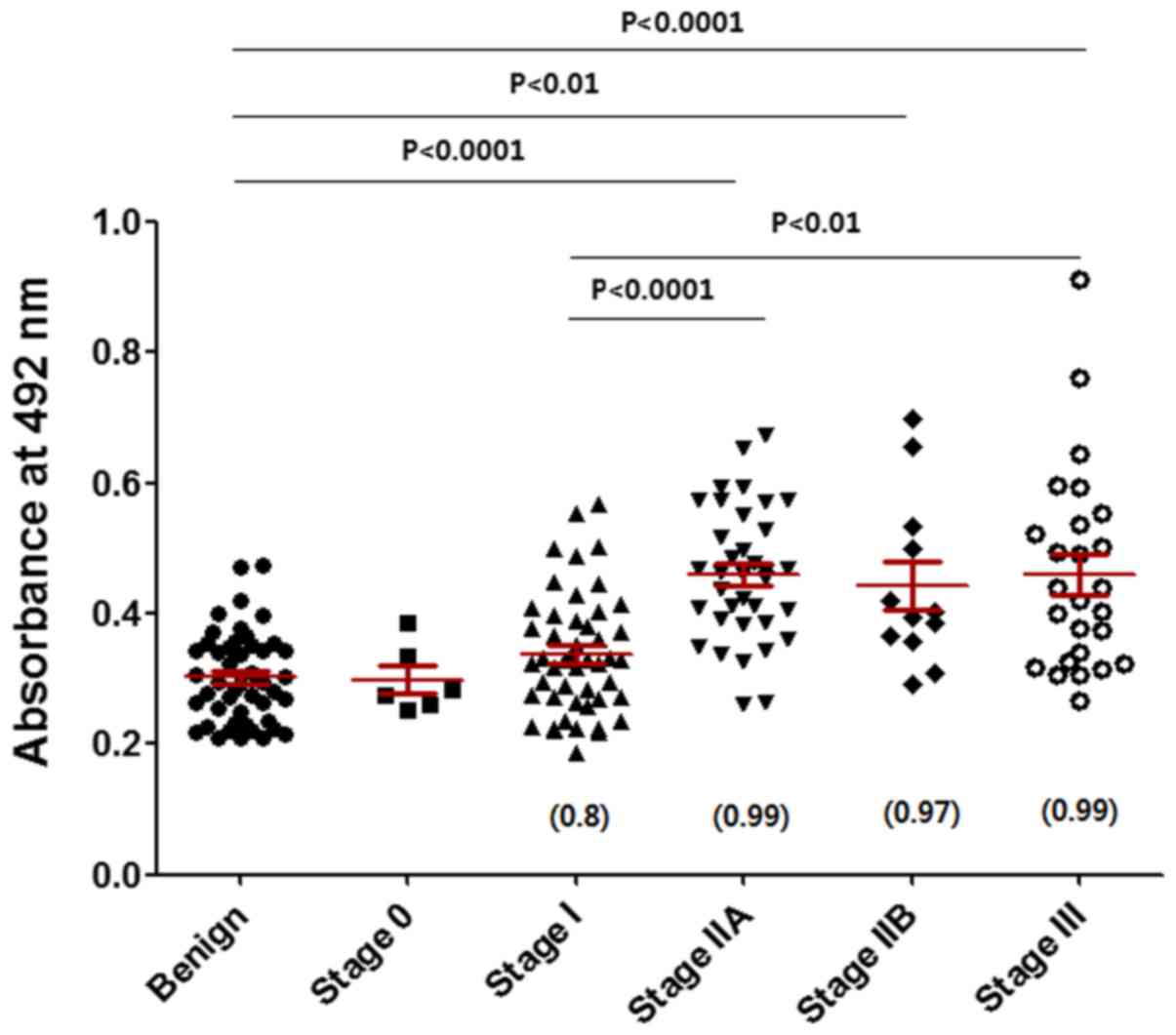
CA15-3 (Fig. 5B). The level of
CA15-3 appeared to increase with increasing stage of breast cancer
(Fig. 6). Mean age of the benign
group was 40, and those of breast cancer stage 0, I, IIA, IIB and
III were 49, 51, 50, 55 and 54, respectively. No correlation was
found between age and the mannosylated N-glycan level of
CA15-3 in each group (Table II).
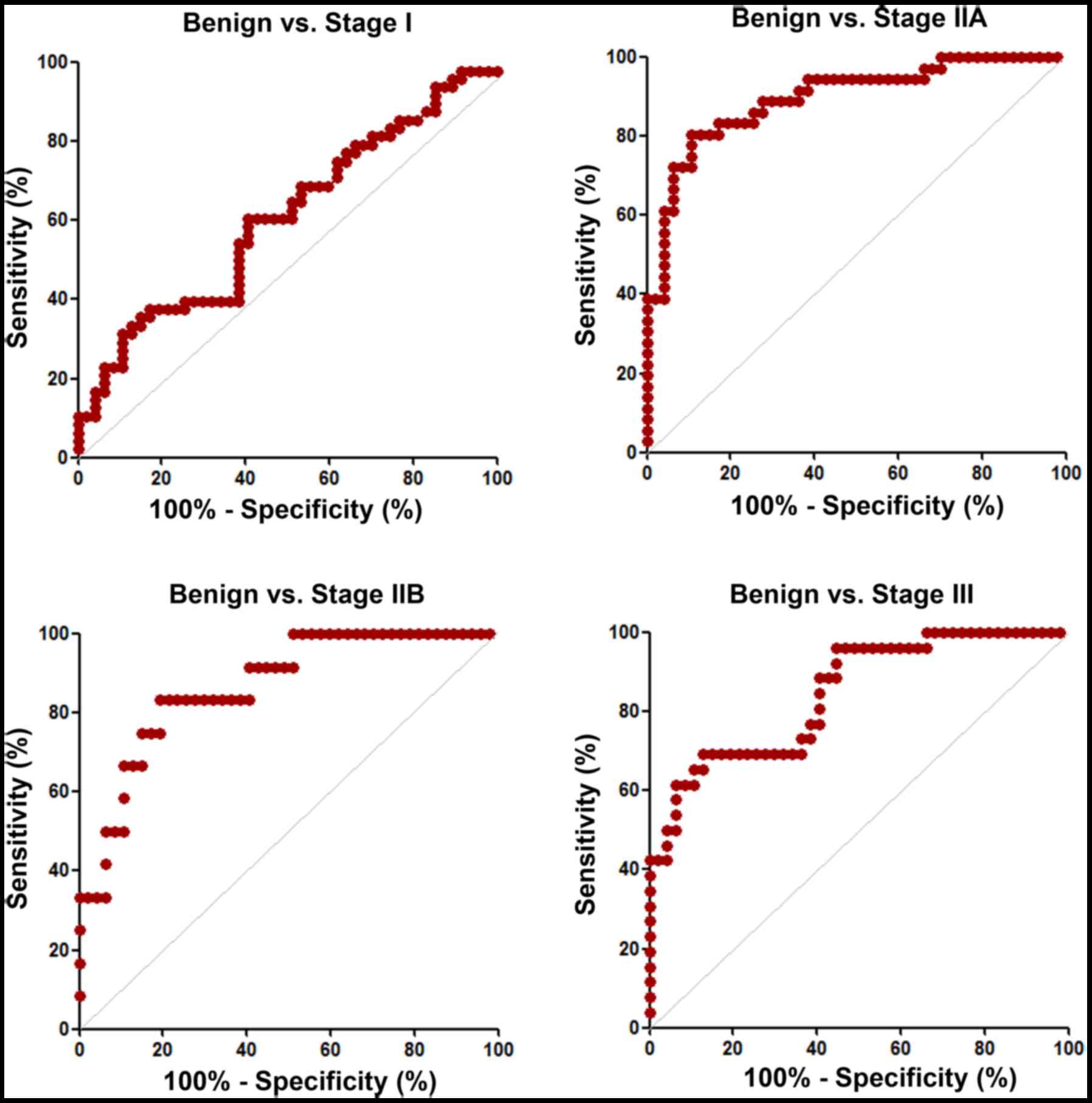
Fig. 7 reveals the ROC curves
obtained from Fig. 6. Sensitivity,
specificity and AUC values in discriminating breast cancer stage I,
IIA, IIB or III from benign disease were calculated from three
independent assays. The specificity, sensitivity and AUC values
were found to be higher when discriminating stage IIA, IIB and III
from benign (Table III).
 | Table II.Correlation between mannosylated
N-glycan levels of CA15-3 and age in each group. |
Table II.
Correlation between mannosylated
N-glycan levels of CA15-3 and age in each group.
|
| Benign (n=47) | Stage 0 (n=6) | Stage I (n=48) | Stage IIA
(n=36) | Stage IIB
(n=12) | Stage III
(n=26) |
|---|
| Range of age | 19–74 | 25–76 | 29–78 | 29–75 | 33–83 | 36–78 |
| Mean age | 40 | 49 | 51 | 50 | 55 | 54 |
| Pearson, r | −0.09 | −0.38 | −0.12 | 0.22 | 0.02 | −0.23 |
 | Table III.Sensitivity, specificity and AUC
values when discriminating stage I, IIA, IIB or III from benign.
Three independent assays were carried out and sensitivity,
specificity and AUC values were calculated from the assays. |
Table III.
Sensitivity, specificity and AUC
values when discriminating stage I, IIA, IIB or III from benign.
Three independent assays were carried out and sensitivity,
specificity and AUC values were calculated from the assays.
|
| Sensitivity | Specificity | AUC |
|---|
| Benign vs. stage
I | 63±30 | 69±23 | 0.64±0.05 |
| Benign vs. stage
IIA | 77±4 | 75±15 | 0.78±0.12 |
| Benign vs. stage
IIB | 69±17 | 86±12 | 0.79±0.07 |
| Benign vs. stage
III | 80±10 | 65±20 | 0.75±0.08 |
No differences were found between the groups in a
sandwich ELISA using two different anti-CA15-3 antibodies rather
than the CA15-3 antibody-ConA combination (Fig. 8). The trend in the CA15-3 level
between groups in the sandwich ELISA was similar to that reported
previously (7). This result
indicates that the increased response of the cancer samples in the
antibody-lectin sandwich assay is due to increased
N-glycosylation of CA15-3 rather than to an increased
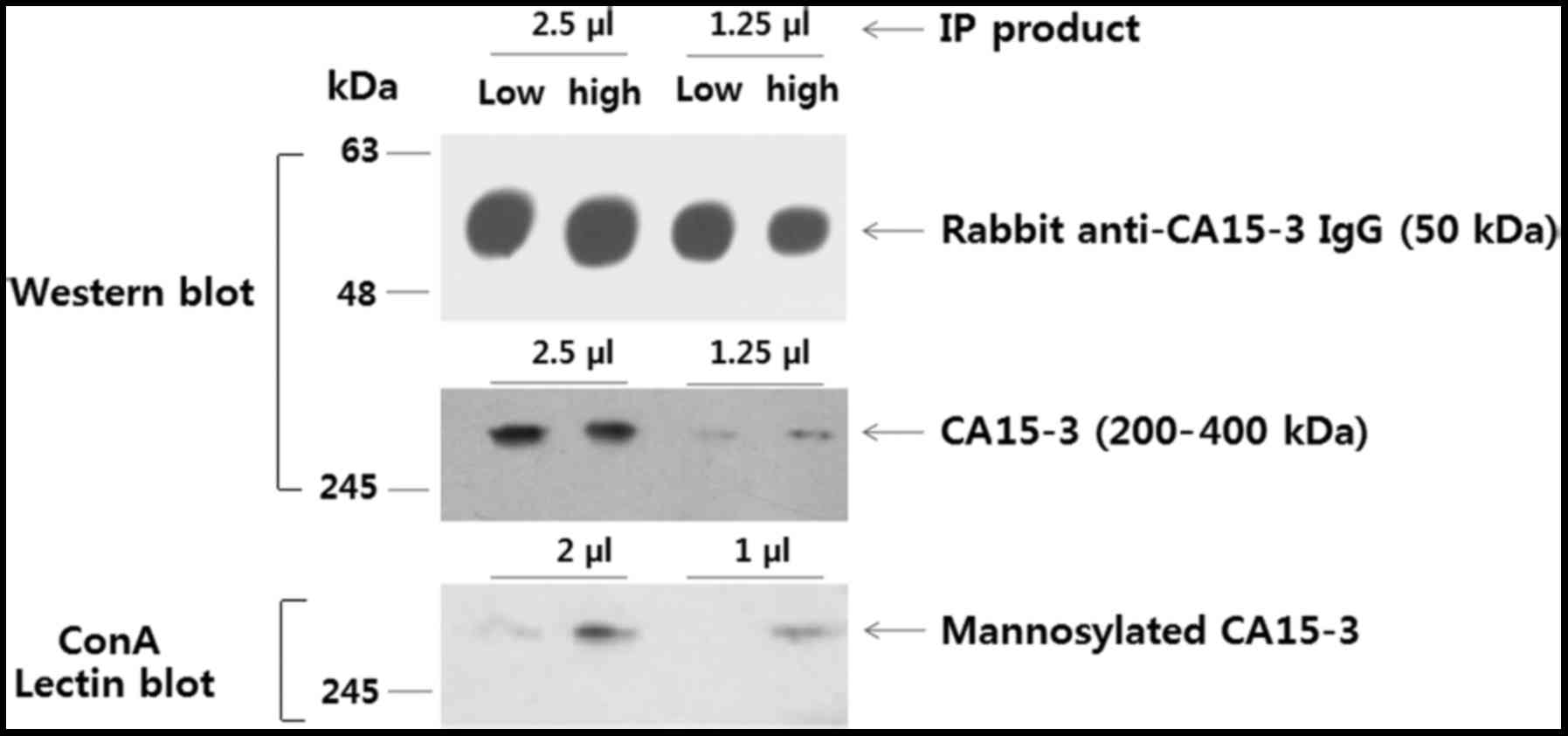
concentration of CA15-3. This inference was confirmed by a Western
blot detecting CA15-3 and a ConA blot detecting N-glycans on
CA15-3 (Fig. 9). In summary, our
results indicated that the anti-CA15-3 antibody-ConA sandwich assay
could be valuable for screening early breast cancers.
Discussion
CA15-3 (MUC1) is an extensively
O-glycosylated and moderately N-glycosylated protein,
and glycosylation is responsible for 50–90% of its total molecular
weight (6). In the present study,
an anti-CA15-3 antibody-ConA sandwich assay system was designed to
detect the N-glycosylation of serum CA15-3. A total of nine lectins
that bind to O-glycans or N-glycans (20), were tested to investigate their
strength binding to captured CA15-3 (Fig. 3A). Unexpectedly, only ConA exhibited
strong reactivity towards CA15-3. This implies that the
accessibilities of the lectins other than ConA are hindered in some
way. Generally, mucin-type glycoproteins and even purified mucin
(21) exhibit a tendency to form
aggregates or gels (22). Moreover,
CA15-3 possesses a self-aggregation domain (23). These properties of mucin-type
glycoproteins are likely to mask the glycans and hinder the access
of lectins. Lectins have poor access to heavily
O-glycosylated serum glycoproteins and their access is
improved by perchloric acid treatment (24). The conformations and sizes of
mucin-type glycoproteins are dependent on factors such as pH and
ionic strength (21). Therefore,
further investigation of the conformational changes of CA15-3 as a
function of physical conditions may extend the utility of
lectins.
The O-glycan profiles of CA15-3 from breast
milk, urine and breast carcinoma cell lines have been investigated
(25–27). The glycan of CA15-3 in culture
supernatants and cell lysates of breast carcinoma cell lines was
found to have a truncated precursor structure (25–28).
On the other hand, little attention has been paid to the
N-glycan profiles of CA15-3 during carcinogenesis. In the
present study, the mannosylated N-glycosylation level of
CA15-3 increased with increasing stage of breast cancer (Fig. 6). A high mannose type of
N-glycan is synthesized early in glycan biosynthesis and the
glycan is then modified by substitution or addition of other sugars
such as sialic acid and galactose (29). Analysis of the N-glycan
profiles of mouse and human sera using total serum glycoprotein
fractions (30) revealed a large
number of high mannose-type glycans containing nine mannoses in the
glycoproteins from both mice and humans with breast cancer.
Therefore, premature termination of the glycosylation pathway is
thought to be a critical indicator of the progression of breast
cancer. We suggest that alterations of the N-glycosylation
of CA15-3 would merit examination in future studies of breast
carcinogenesis.
The current ELISA system for measuring the serum
CA15-3 level (115D8 and DF3 system) allows serum dilutions of
1:50–1:100, whereas our antibody-lectin sandwich assay system
detects serum dilutions exceeding 1:2,000 (Fig. 4A). Therefore, the sensitivity of our
system is significantly higher than that of the current ELISA. This
is because the signal is increased by the abundant glycosylation of
CA15-3. This antibody-lectin sandwich assay system appears to have
great potential for detecting glycosylation levels of serum
glycoproteins in patients with cancers.
Limited success has been achieved to date with
antibody-lectin sandwich systems using clinical samples (16,17).
Glycosylation of the coating antibody and blocking agent tend to
restrict use of lectins (Fig. 2).
Moreover, non-specific reactions of serum proteins are important
consideration. Concurrently, FBS or skim milk, which contain large
amounts of glycoprotein, are much more effective in blocking the
non-specific reactions of human serum protein in immunoassays than
BSA (non-glycosylated protein) (31). The choice of blocking agent is
therefore not straightforward. In the present study, oxidation of
the coating antibody or FBS was not effective in blocking the
binding of SNA, MAA and jacalin, which target sialylation (Fig. 2). Changes in sialylation levels have
been detected in the sera of cancer patients (32) and deserve further study. In
addition, the use of non-glycosylated antibodies and a blocking
agent in antibody-lectin sandwich assays could extend the use of
lectins. One research group has performed antibody-lectin assays
using a Fab fragment of anti-haptoglobin antibody and AAL to detect
fucosylated haptoglobin in the sera of patients with colorectal
cancer (33). Another research team
has suggested that the synthetic blocking agent polymer, polyvinyl
alcohol, is effective in lectin-based assays and avoids the
background signals caused by glycoprotein-based blocking agents
(34).
Limitations of our study are the low number of serum
samples examined, as well as the absence of data on metastatic
breast cancer and changes in glycosylation levels after surgery. We
anticipate that studies with a larger number of samples will extend
the utility of the sandwich assay for measuring the glycosylation
level of CA15-3 in breast cancers and the use of this assay as a
prognostic marker.
Aberrant glycosylation during cancer progression has
been found in several types of serum glycoproteins such as prostate
specific antigen, carcinoma antigen 125, carcinoembryonic antigen
and human chorionic gonadotropin β subunit (14). Since almost 60% of serum proteins
are glycosylated and more than 100 types of lectin are commercially
available (35), the
antibody-lectin sandwich assay platform has great potential for the
early detection of cancers. We believe that the present study
provides a foretaste of a novel and promising type of a
high-throughput cancer screening system.
Acknowledgements
We thank Mei Ling Xu for preparing the samples used
in this study and Julian D. Gross (Oxford University, UK) for
English editing.
Funding
The present study was supported by a grant of the
Korean Health Technology R&D Project, Ministry of Health and
Welfare, Republic of Korea (HI12C0050). URL: https://www.htdream.kr/.
Availability of data and materials
The datasets used during the present study are
available from the corresponding author upon reasonable
request.
Authors' contributions
JWC, HJK, BIM, JWL and HJK conceived and designed
the study. JWC and HJK wrote the paper. BIM and JWL collected
specimens. JWC, HJK and YIJ carried out experiments. HJK is
responsible for the integrity of the work as a whole.
Ethics approval and consent to
participate
The present study was carried out with the approval
of the Ewha Womans University Mokdong Hospital Institutional Review
Board (Seoul, Republic of Korea) and was conducted in accordance
with the Declaration of Helsinki. Serum samples of patients were
collected after obtaining written informed consents.
Consent for publication
Not applicable.
Competing interests
The authors declare that they have no competing
interests.
References
|
1
|
International WCR: Breast cancer
statistics. 16–January. 2015http://www.wcrf.org/int/cancer-facts-figures/data-specific-cancers/breast-cancer-statistics2015.
|
|
2
|
Torre LA, Bray F, Siegel RL, Ferlay J,
Lortet-Tieulent J and Jemal A: Global Cancer Statistics, 2012. Ca
Cancer J Clin. 65:87–108. 2015. View Article : Google Scholar : PubMed/NCBI
|
|
3
|
Dumalaon-Canaria JA, Hutchinson AD,
Prichard I and Wilson C: What causes breast cancer? A systematic
review of causal attributions among breast cancer survivors and how
these compare to expert-endorsed risk factors. Cancer Causes
Control. 25:771–785. 2014. View Article : Google Scholar : PubMed/NCBI
|
|
4
|
Misek DE and Kim EH: Protein biomarkers
for the early detection of breast cancer. Int J Proteomics.
2011:3435822011. View Article : Google Scholar : PubMed/NCBI
|
|
5
|
Chou CP, Peng NJ, Chang TH, Yang TL, Hu C,
Lin HS, Huang JS and Pan HB: Clinical roles of breast 3T MRI, FDG
PET/CT, and breast ultrasound for asymptomatic women with an
abnormal screening mammogram. J Chin Med Assoc. 78:719–725. 2015.
View Article : Google Scholar : PubMed/NCBI
|
|
6
|
Nath S and Mukherjee P: MUC1: A
multifaceted oncoprotein with a key role in cancer progression.
Trends Mol Med. 20:332–342. 2014. View Article : Google Scholar : PubMed/NCBI
|
|
7
|
Duffy MJ, Evoy D and McDermott EW: CA
15-3: Uses and limitation as a biomarker for breast cancer. Clin
Chim Acta. 411:1869–1874. 2010. View Article : Google Scholar : PubMed/NCBI
|
|
8
|
Kufe D, Inghirami G, Abe M, Hayes D,
Justi-Wheeler H and Schlom J: Differential reactivity of a novel
monoclonal antibody (DF3) with human malignant versus benign breast
tumors. Hybridoma. 3:223–232. 1984. View Article : Google Scholar : PubMed/NCBI
|
|
9
|
Duffy MJ, Shering S, Sherry F, McDermott E
and O'Higgins N: CA 15-3: A prognostic marker in breast cancer. Int
J Biol Markers. 15:330–333. 2000. View Article : Google Scholar : PubMed/NCBI
|
|
10
|
Harris L, Fritsche H, Mennel R, Norton L,
Ravdin P, Taube S, Somerfield MR, Hayes DF and Bast RC Jr: American
Society of Clinical Oncology: American society of clinical oncology
2007 update of recommendations for the use of tumor markers in
breast cancer. J Clin Oncol. 25:5287–5312. 2007. View Article : Google Scholar : PubMed/NCBI
|
|
11
|
Munkley J and Elliott DJ: Hallmarks of
glycosylation in cancer. Oncotarget. 7:35478–35489. 2016.
View Article : Google Scholar : PubMed/NCBI
|
|
12
|
Storr SJ, Royle L, Chapman CJ, Hamid UMA,
Robertson JF, Murray A, Dwek RA and Rudd PM: The O-linked
glycosylation of secretory/shed MUC1 from an advanced breast cancer
patient's serum. Glycobiology. 18:456–462. 2008. View Article : Google Scholar : PubMed/NCBI
|
|
13
|
Lavrsen K, Madsen CB, Rasch MG, Woetmann
A, Odum N, Mandel U, Clausen H, Pedersen AE and Wandall HH:
Aberrantly glycosylated MUC1 is expressed on the surface of breast
cancer cells and a target for antibody-dependent cell-mediated
cytotoxicity. Glycoconj J. 30:227–236. 2013. View Article : Google Scholar : PubMed/NCBI
|
|
14
|
Kuzmanov U, Kosanam H and Diamandis EP:
The sweet and sour of serological glycoprotein tumor biomarker
quantification. BMC Med. 11:312013. View Article : Google Scholar : PubMed/NCBI
|
|
15
|
Hashim OH, Jayapalan JJ and Lee CS:
Lectins: An effective tool for screening of potential cancer
biomarkers. Peer J. 5:e37842017. View Article : Google Scholar : PubMed/NCBI
|
|
16
|
Madiyalakan R, Kuzma M, Noujaim AA and
Suresh MR: An antibody-lectin sandwich assay for the determination
of CA125 antigen in ovarian cancer patients. Glycoconj J.
13:513–517. 1996. View Article : Google Scholar : PubMed/NCBI
|
|
17
|
Bamrungphon W, Prempracha N, Bunchu N,
Rangdaeng S, Sandhu T, Srisukho S, Boonla C and Wongkham S: A new
mucin antibody/enzyme-linked lectin-sandwich assay of serum MUC5AC
mucin for the diagnosis of cholangiocarcinoma. Cancer Lett.
247:301–308. 2007. View Article : Google Scholar : PubMed/NCBI
|
|
18
|
Kim HJ and Lee SJ: Antibody-based
enzyme-linked lectin assay (ABELLA) for the sialylated recombinant
human erythropoietin present in culture supernatant. J Pharm Biomed
Anal. 48:716–721. 2008. View Article : Google Scholar : PubMed/NCBI
|
|
19
|
Cummings RD and Etzler ME: Antibodies and
lectins in glycan analysis. 2009.
|
|
20
|
Zhang L, Luo S and Zhang BL: The use of
lectin microarray for assessing glycosylation of therapeutic
proteins. MAbs. 8:524–535. 2016. View Article : Google Scholar : PubMed/NCBI
|
|
21
|
Bansil R and Turner BS: Mucin structure,
aggregation, physiological functions and biomedical applications.
Curr Opin Colloid In. 11:164–170. 2006. View Article : Google Scholar
|
|
22
|
Taylor C, Allen A, Dettmar PW and Pearson
JP: The gel matrix of gastric mucus is maintained by a complex
interplay of transient and nontransient associations.
Biomacromolecules. 4:922–927. 2003. View Article : Google Scholar : PubMed/NCBI
|
|
23
|
Mahanta S, Fessler SP, Park J and Bamdad
C: A minimal fragment of MUC1 mediates growth of cancer cells. PLoS
One. 3:e20542008. View Article : Google Scholar : PubMed/NCBI
|
|
24
|
Lee CS, Taib NAM, Ashrafzadeh A, Fadzli F,
Harun F, Rahmat K, Hoong SM, Abdul-Rahman PS and Hashim OH:
Unmasking heavily o-glycosylated serum proteins using perchloric
acid: Identification of serum proteoglycan 4 and protease c1
inhibitor as molecular indicators for screening of breast cancer.
PLoS One. 11:e1495512016.
|
|
25
|
Bhavanandan VP, Zhu Q, Yamakami K, Dilulio
NA, Nair S, Capon C, Lemoine J and Fournet B: Purification and
characterization of the MUC1 mucin-type glycoprotein, epitectin,
from human urine: Structures of the major oligosaccharide alditols.
Glycoconj J. 15:37–49. 1998. View Article : Google Scholar : PubMed/NCBI
|
|
26
|
Hanisch FG, Stadie TRE, Deutzmann F and
PeterKatalinic J: MUC1 glycoforms in breast cancer - Cell line T47D
as a model for carcinoma-associated alterations of O-glycosylation.
Eur J Biochem. 236:318–327. 1996. View Article : Google Scholar : PubMed/NCBI
|
|
27
|
Brockhausen I, Yang JM, Burchell J,
Whitehouse C and Taylor-papadimitriou J: Mechanisms underlying
aberrant glycosylation of muc1 mucin in breast-cancer cells. Eur J
Biochem. 233:607–617. 1995. View Article : Google Scholar : PubMed/NCBI
|
|
28
|
Hanson RL and Hollingsworth MA: Functional
consequences of differential o-glycosylation of MUC1, MUC4, and
MUC16 (downstream effects on signaling). Biomolecules. 6:E342016.
View Article : Google Scholar : PubMed/NCBI
|
|
29
|
Stanley P: Golgi glycosylation. Cold
Spring Harb Perspect Biol. 3:a0051992011. View Article : Google Scholar : PubMed/NCBI
|
|
30
|
de Leoz ML, Young LJ, An HJ, Kronewitter
SR, Kim J, Miyamoto S, Borowsky AD, Chew HK and Lebrilla CB:
High-mannose glycans are elevated during breast cancer progression.
Mol Cell Proteomics. 10:M1102011. View Article : Google Scholar : PubMed/NCBI
|
|
31
|
Biocompare: Bench tips: tips for reducing
elisa background. http://www.biocompare.com/Bench-Tips/122704-Tips-for-Reducing-ELISA-Background/2012
|
|
32
|
Kirwan A, Utratna M, O'Dwyer ME, Joshi L
and Kilcoyne M: Glycosylation-based serum biomarkers for cancer
diagnostics and prognostics. Biomed Res Int. 2015:4905312015.
View Article : Google Scholar : PubMed/NCBI
|
|
33
|
Takeda Y, Shinzaki S, Okudo K, Moriwaki K,
Murata K and Miyoshi E: Fucosylated haptoglobin is a novel type of
cancer biomarker linked to the prognosis after an operation in
colorectal cancer. Cancer. 118:3036–3043. 2012. View Article : Google Scholar : PubMed/NCBI
|
|
34
|
Thompson R, Creavin A, O'Connell M,
O'Connor B and Clarke P: Optimization of the enzyme-linked lectin
assay for enhanced glycoprotein and glycoconjugate analysis. Anal
Biochem. 413:114–122. 2011. View Article : Google Scholar : PubMed/NCBI
|
|
35
|
Sharon N and Lis H: History of lectins:
From hemagglutinins to biological recognition molecules.
Glycobiology. 14:53R–62R. 2004. View Article : Google Scholar : PubMed/NCBI
|