Introduction
Acute pancreatitis (AP) is an inflammatory condition
that is characterized by the autodigestion, edema, bleeding and
even necrosis of pancreatic tissues (1). Over the past number of decades, AP
has been observed to be one of the most prevalent gastrointestinal
conditions leading to hospitalization in China, USA and Japan
(1-3).
Furthermore, AP incurs considerable financial burden on the
patients and healthcare system, with costs of >$2 billion
attributed to it annually in the USA alone (4). Despite developments in the diagnosis
(including laboratory tests, electrocardiography and chest
radiography) and treatment (including early fluid resuscitation,
antibiotics and nutritional support) strategies of AP (1,2,5),
rates of morbidity and mortality from AP remain high, with the
morbidity of ~60,000 and mortality of ~50,000 in the USA alone in
2021 (6,7). In addition, local or systemic
complications, such as pancreatic abscess and acute respiratory
failure, adversely affect the quality of life of patients with AP
(1-3,5).
Due to these remaining obstacles in the management of AP, exploring
potential novel biomarkers for ameliorating this condition is of
importance.
Cell division cycle 42 (CDC42) has the capacity to
modulate several biological processes, including cytoskeleton
organization, membrane trafficking, cell migration and adhesion
(8,9). Of note, a number of studies have
previously reported that CDC42 can inhibit systemic inflammation by
regulating the activity of macrophages and T cells (10-13).
It has been suggested that CDC42 can promote M2 macrophage
polarization to suppress inflammation (12,13).
In addition, CDC42 has been found to inhibit the differentiation of
T helper (Th)17 cells whilst promoting that of Th2 cells and
regulatory T cells (Tregs), in turn suppressing inflammation
(10,11). Previous studies have also reported
that CDC42 can regulate the pathophysiology of AP (14,15).
Based on these previous findings aforementioned, it was speculated
that CDC42 may serve as a potential prognostic biomarker for AP.
However, this concept remains poorly understood.
Therefore, the aim of the present study was to
explore the possible association between CDC42 expression and the
disease characteristics of AP and inflammation, in addition to its
predictive value for mortality risk in patients with AP.
Materials and methods
Subjects
Between January 2018 and May 2021, a total of 149
patients with AP (aged 23-77, male:female ratio, 3.8:2) in the
Affiliated Nanhua Hospital, University of South China Hunan, China
were consecutively enrolled into the present study. The enrollment
criteria were as follows: i) Confirmed as AP according to the 2016
Revised Atlanta Classification for Acute Pancreatitis (16); ii) aged >18 years; iii)
enrollment within 24 h of diagnosis; and iv) ability to provide
informed consent and provide a peripheral blood (PB) sample. The
exclusion criteria were as follows: i) Diagnosed with pancreatic
cancer or other hepatobiliary malignancies; ii) accompanied with
autoimmune diseases or hematological malignancies; iii) received
radiotherapy or chemotherapy within 180 days; and iv) being
pregnant or lactating.
Within the same time period, 50 age- and sex-matched
healthy individuals (aged 35-65, male:female ratio, 3:2) were also
enrolled into the present study as healthy controls (HCs). The
health status of HCs was checked when they came to the Affiliated
Nanhua Hospital, University of South China Hunan, China for
physical examination. The recruitment criteria for HCs were as
follows: i) No history of pancreatitis; ii) no history of
hepatobiliary diseases; iii) no history of malignant diseases; and
iv) normal biochemical indices.
The present study was approved by the Institutional
Review Board of the Affiliated Nanhua Hospital, University of South
China (approval no. 2017-136) and written informed consent was
obtained from all subjects or their guardians.
Collection of data
Demographic and clinical characteristics of patients
with AP were recorded following physical examination. AP severity
was classified in accordance with the 2016 Revised Atlanta
Classification for Acute Pancreatitis (16), which included mild AP (MAP),
moderate-severe AP (MSAP) and severe AP (SAP). The Ranson's, Acute
Pathologic and Chronic Health Evaluation II (APACHE II) (17) and Sequential Organ Failure
Assessment (SOFA) (18) scores of
the patients with AP were also evaluated ordinally within 24 h from
hospitalization. All patients with AP were closely followed up
until either they succumb to the disease in hospital or are
discharged from the hospital, where in-hospital mortality was
recorded. Age and sex of all individuals in the HC group were
recorded following health examination.
Collection of blood samples
PB (10 ml) from all individuals was collected by
venipuncture within 24 h from admission or enrollment. Following
collection, half of the blood samples were kept at room temperature
(37˚C) for >0.5 h and then centrifuged at 4˚C, 1,170 x g for 10
min to separate the serum and the supernatant was collected by
discarding the pellet. The serum was used immediately for cytokine
determination. PB mononuclear cells (PBMCs) were isolated
immediately from the other half of the PB sample using Ficoll-Paque
density gradient centrifugation. Briefly, PB sample diluted with
phosphate buffered saline (PBS) was gently layered over an equal
volume of Ficoll-Paque PLUS (cat. no. 17144002; Cytiva) in a Falcon
tube and centrifuged for 20 min at 400 x g (20˚C). Then four layers
formed, each containing different cell types. The second white
layer which contained PBMCs was gently removed using a Pasteur
pipette and added to PBS to wash off any remaining platelets.
Reverse transcription-quantitative PCR
(RT-qPCR)
RT-qPCR was performed to quantitatively measure the
expression of CDC42 in the PBMCs. Briefly, total RNA was extracted
using a QIAamp RNA Blood Mini kit (Qiagen China Co., Ltd.) and
reverse-transcribed using PrimeScript™ RT reagent kit (Perfect Real
Time; Takara Biotechnology Co., Ltd.). The reverse transcription
was performed at 42˚C for 15 min. qPCR was performed using
SYBR® Premix DimerEraser™ (Takara Biotechnology Co.,
Ltd.). The reactions of qPCR were incubated in 96-well optical
plates (95˚C, 5 min), followed by 30 cycles (94˚C for 30 sec, 55˚C
for 1 min and 72˚C for 1 min). The specific primers used for qPCR
were as follows: CDC42 forward, 5'-GCCCGTGACCTGAAGGCTGTCA-3' and
reverse, 5'-TGCTTTTAGTATGATGCCGACACCA-3'. GAPDH was used as an
internal control: forward, 5'-AAGGTGAAGGTCGGAGTCA-3' and reverse,
5'-GGAAGATGGTGATGGGATTT-3' (19).
CDC42 expression was calculated using the 2-ΔΔCq method
(20).
ELISA
The levels of CRP in the serum of patients with AP
and HCs were measured using a Human C-Reactive Protein ELISA kit
(cat. no. CYT298; Merck KGaA). The levels of TNF-α and IL-6 in the
serum of patients with AP were measured using a Human TNF-α
Quantikine ELISA kit (cat. no. DTA00C; R&D Systems, Inc.) and
Human IL-6 ELISA kit (cat. no. LS-F29154; LifeSpan BioSciences,
Inc.). All processes were performed according to the manufacturers'
protocols.
Statistical analysis
Statistical analysis was performed using the SPSS
26.0 software (IBM Corp.) and figures were plotted using GraphPad
Prism 7.01 software (GraphPad Software, Inc.). Continuous data were
displayed with mean ± standard deviation (SD) and median with
interquartile range (IQR) as appropriate. Categorical data were
displayed as numbers (percentage). Differences in demographics,
clinical features and biochemical indexes among subjects were
assessed using unpaired Student's t-test, χ2 test,
Mann-Whitney U test, Kruskal-Wallis test and one-way analysis of
variance. Multiple comparisons were performed by Dunn post hoc test
with Bonferroni correction. Correlation between CDC42 expression
and the level of inflammatory cytokines or disease assessment
indicators were evaluated using the Spearman's rank correlation
test. Receiver operating characteristic (ROC) curve analysis was
used to investigate the efficacy of CDC42 expression for the
evaluation of AP severity. Univariate logistic regression analysis
was used to assess factors associated with in-hospital mortality,
then all potential factors were included in the multivariate
logistic regression analysis with step forward method by SPSS 26.0
software (IBM Corp.). P<0.05 was considered to indicate a
statistically significant difference.
Results
Characteristics of HCs and patients
with AP
The group of patients with AP consisted of 51
(34.2%) women and 98 (65.8%) men with a mean age of 52.5±13.9
years. The 50 HCs consisted of 20 (40.0%) women and 30 (60.0%) men
with a mean age of 51.7±9.4 years (Table I). Furthermore, the median CRP
level in patients with AP [55.1 (31.7-91.3)] was significantly
higher compared with that in HCs [3.2 (1.2-4.6); P<0.001;
Table I]. In terms of the
Ranson's, APACHE II and SOFA scores, patients in the SAP groups
scored the highest, followed by the MSAP and the MAP groups (all
P<0.001). However, no differences in age or sex could be
identified between the AP and HC groups (Table I). Regarding the Ranson's, APACHE
II and SOFA scores in patients with AP, they were found to be 2.0
(1.0-3.0), 7.0 (4.0-11.0) and 2.0 (1.0-4.0), respectively. The
in-hospital mortality incidence was 12 (8.1%) in patients with AP
(Table I).
 | Table ICharacteristics of HCs and patients
with AP. |
Table I
Characteristics of HCs and patients
with AP.
| Items | HCs (n=50) | Patients with AP
(n=149) | Statistic
(t/χ2/Z) | P-value | MAP (n=78) | MSAP (n=47) | SAP (n=24) | Statistic
(F/χ2/H) | P-value |
|---|
| Age (years), mean ±
SD | 51.7±9.4 | 52.5±13.9 | -0.487 | 0.627 | 53.5±12.5 | 50.2±15.1 | 53.8±15.6 | 0.946 | 0.391 |
| Sex, N (%) | | | 0.543 | 0.461 | | | | 0.729 | 0.694 |
|
Female | 20 (40.0) | 51 (34.2) | | | 26 (33.3) | 15 (31.9) | 10 (41.7) | | |
|
Male | 30 (60.0) | 98 (65.8) | | | 52 (66.7) | 32 (68.1) | 14 (58.3) | | |
| CRP (mg/l), median
(IQR) | 3.2 (1.2-4.6) | 55.1
(31.7-91.3) | -10.546 | <0.001 | 39.2
(20.9-57.3) | 71.5
(55.2-120.8) | 91.4
(50.0-188.4) | 43.314 | <0.001 |
| Etiology, N
(%) | | | - | - | | | | 11.349 | 0.078 |
|
BAP | - | 73 (49.0) | | | 32 (41.0) | 25 (53.2) | 16 (66.7) | | |
|
HTGAP | - | 49 (32.9) | | | 31 (39.7) | 13 (27.7) | 5 (20.8) | | |
|
AAP | - | 10 (6.7) | | | 3 (3.8) | 6 (12.8) | 1 (4.2) | | |
|
Others | - | 17 (11.4) | | | 12 (15.4) | 3 (6.4) | 2 (8.3) | | |
| Ranson's score,
mean ± SD | - | 2.0 (1.0-3.0) | - | - | 1.0 (1.0-1.0) | 3.0 (2.0-4.0) | 3.5 (3.0-5.0) | 112.684 | <0.001 |
| APACHE II score,
mean ± SD | - | 7.0 (4.0-11.0) | - | - | 5.0 (3.0-7.0) | 11.0
(8.0-16.0) | 11.5
(7.0-20.8) | 69.920 | <0.001 |
| SOFA score, mean ±
SD | - | 2.0 (1.0-4.0) | - | - | 1.0 (1.0-1.0) | 3.0 (2.0-4.0) | 5.5 (4.0-7.0) | 95.265 | <0.001 |
| TNF-α (pg/ml),
median (IQR) | - | 67.5
(39.4-108.2) | - | - | 54.2
(28.1-79.5) | 98.6
(60.1-141.7) | 92.6
(59.8-197.5) | 33.028 | <0.001 |
| IL-6 (pg/ml),
median (IQR) | - | 39.2
(22.5-62.9) | - | - | 25.6
(14.8-43.1) | 52.4
(34.9-76.0) | 52.1
(28.7-112.9) | 31.366 | <0.001 |
| Treatment, N
(%) | | | - | - | | | | 33.556 | <0.001 |
|
Conservative
therapy | - | 121 (81.2) | | | 73 (93.6) | 37 (78.7) | 11 (45.8) | | |
|
Laparotomy | - | 15 (10.1) | | | 0 (0.0) | 6 (12.8) | 9 (37.5) | | |
|
Percutaneous
drainage | - | 13 (8.7) | | | 5 (6.4) | 4 (8.5) | 4 (16.7) | | |
| In-hospital
mortality, No. (%) | - | 12 (8.1) | - | - | 0 (0.0) | 5 (10.6) | 7 (29.2) | 21.703 | <0.001 |
Patients with AP were further classified into those
with MAP (n=78), MSAP (n=47) and SAP (n=24) according to the 2016
Revised Atlanta Classification for Acute Pancreatitis (16). Comparative analysis revealed no
difference in age, sex and etiology among patients with MAP, MSAP
and SAP, whilst significant differences were identified in other
characteristics (all P<0.001; Table
I). Furthermore, the incidence of in-hospital mortality was the
highest in patients with SAP (29.2%), followed by patients with
MSAP (10.6%) and was the lowest in patients with MAP (0.0%;
P<0.001; Table I).
CDC42 in HCs and patients with AP
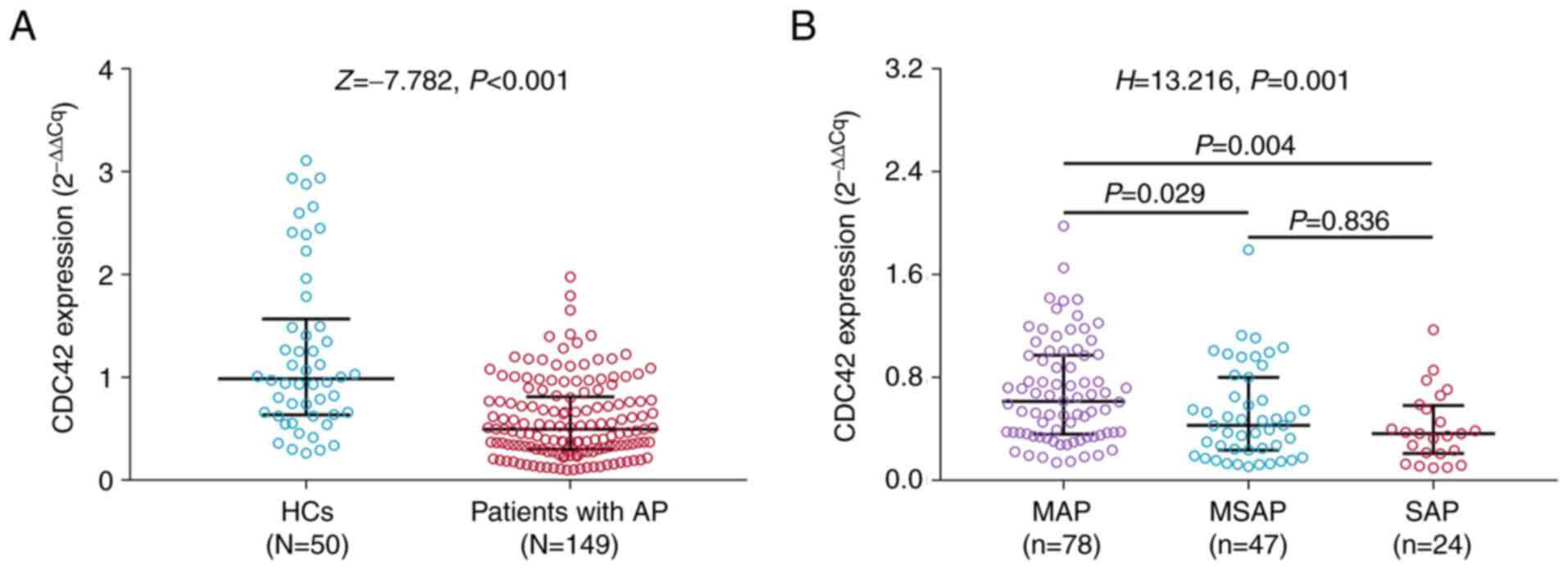
The levels of CDC42 expression was significantly
lower in patients with AP [0.495 (0.302-0.811)] compared with those
in the HC group [0.985 (0.635-1.569); P<0.001; Fig. 1A)]. Furthermore, CDC42 expression
was declined in patients with MSAP [0.429 (0.236-0.801)] compared
with patients with MAP [0.614 (0.359-0.974)] (P=0.029); moreover,
CDC42 expression was decreased in patients with SAP [0.364
(0.210-0.582)] compared with patients with MAP [0.614
(0.359-0.974)] (P=0.004); while no difference in CDC42 expression
was found between patients with MSAP and patients with SAP
(P=0.836; Fig. 1B). However, no
changes in CDC42 expression could be observed among patients with
AP of different etiologies (P=0.292; Fig. S1).
Correlation between CDC42 and each of
the disease assessment indicators tested in patients with AP
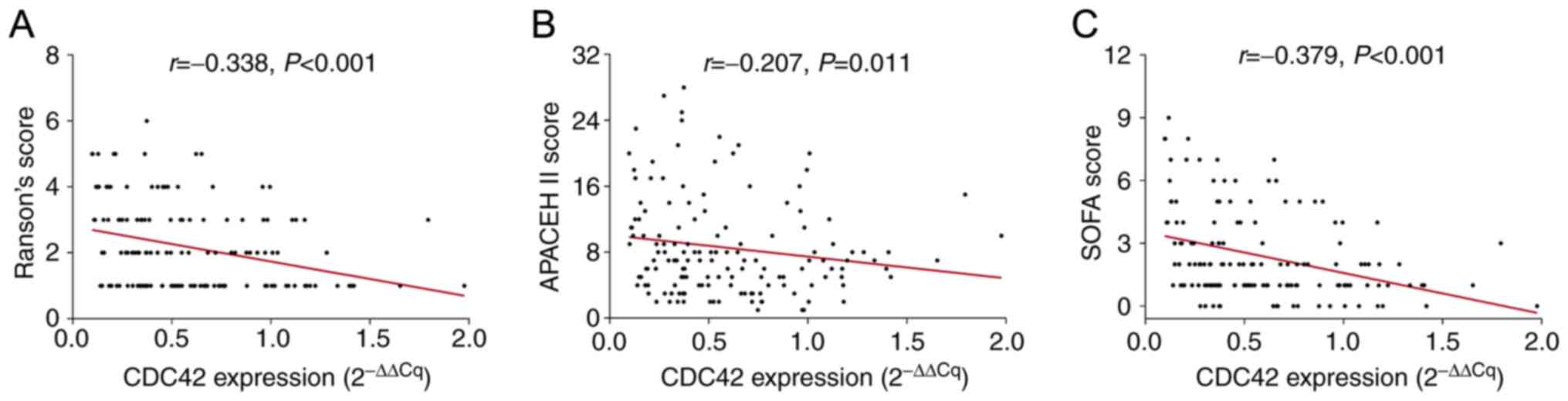
The Ranson's, APACHE II and SOFA scores were
recorded in each patient with AP, which revealed that CDC42 was
negatively correlated with the Ranson's (r=-0.338; P<0.001),
APACHE II (r=-0.207; P=0.011) and SOFA (r=-0.379; P<0.001)
scores (Fig. 2A-C).
Correlation between CDC42 and each of
the inflammatory indices in patients with AP
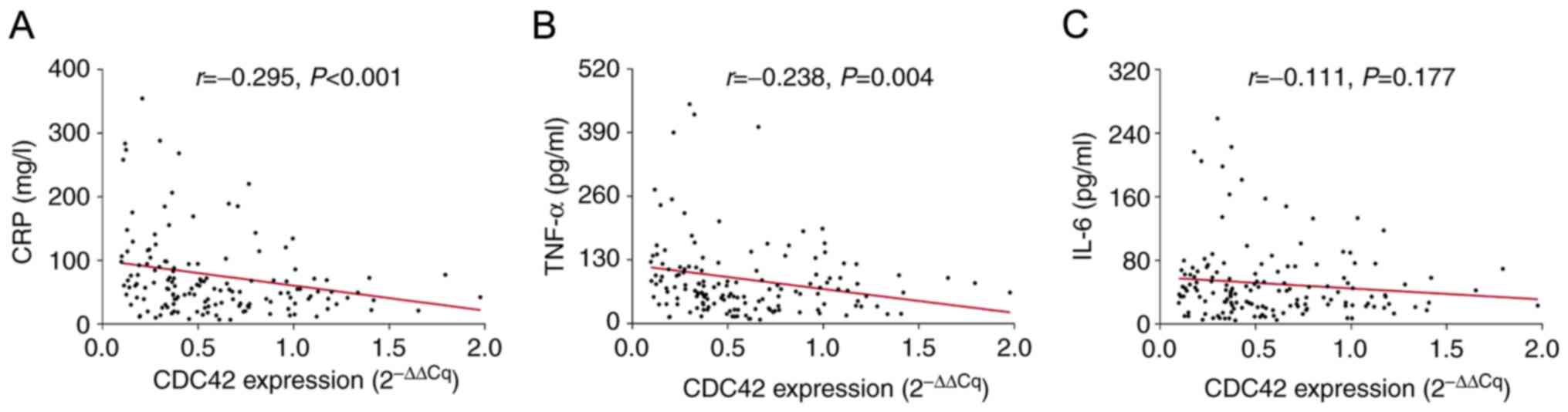
The levels of CRP, TNF-α and IL-6 were measured
using ELISA to evaluate the degree of inflammation in patients with
AP, which revealed that CDC42 was negatively correlated with CRP
(r=-0.295; P<0.001) and TNF-α (r=-0.238; P=0.004; Fig. 3A and B). However, no correlation could be found
between CDC42 expression and IL-6 levels (r=-0.111; P=0.177;
Fig. 3C).
Correlation between CDC42 expression
and mortality risk in patients with AP
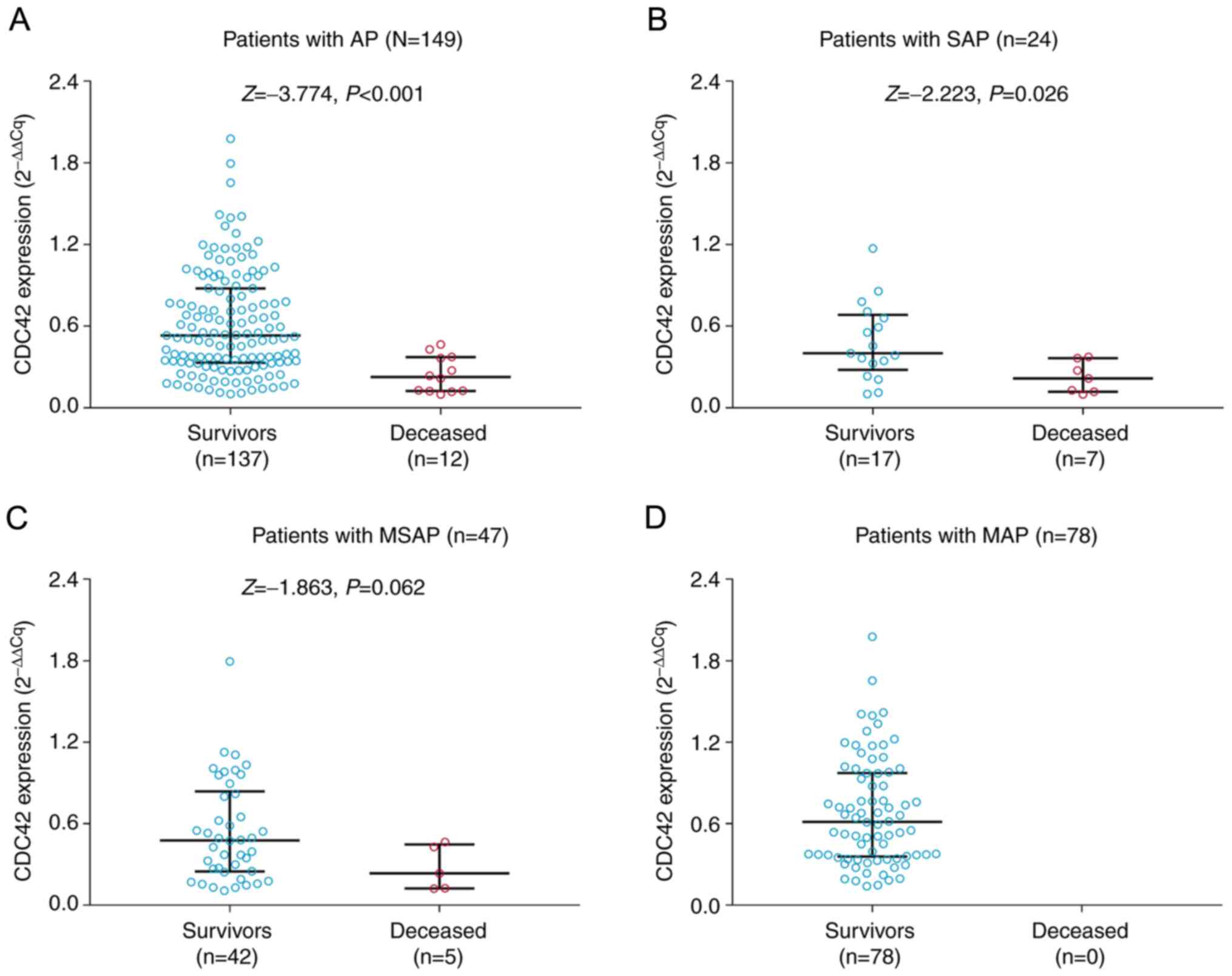
CDC42 expression was found to be significantly
decreased in patients who succumbed to AP [median (IQR): 0.226
(0.124-0.372)] compared with that in survivors of AP [median (IQR),
0.531 (0.332-0.878); P<0.001; Fig.
4A]. Furthermore, subgroup analysis was performed in patients
with SAP, MSAP and MAP. CDC42 expression was significantly reduced
in patients who succumbed to SAP [median (IQR), 0.216
(0.118-0.364)] compared with that in survivors of SAP [median
(IQR), 0.400 (0.279-0.684); P=0.026; Fig. 4B). However, no change in CDC42
expression was observed between patients who succumbed to MSAP and
survivors of MSAP (P=0.062; Fig.
4C). In addition, since there were no in-hospital deaths among
patients with MAP, it was not possible to compare CDC42 expression
between MAP survivors and those who succumbed to MAP (Fig. 4D). Multivariate logistic regression
model analysis revealed that higher CDC42 expression was
independently associated with reduced mortality in patients with AP
[odds ratio, 0.002; 95% confidence interval (CI), 0.001-0.274;
P=0.013; Table S1].
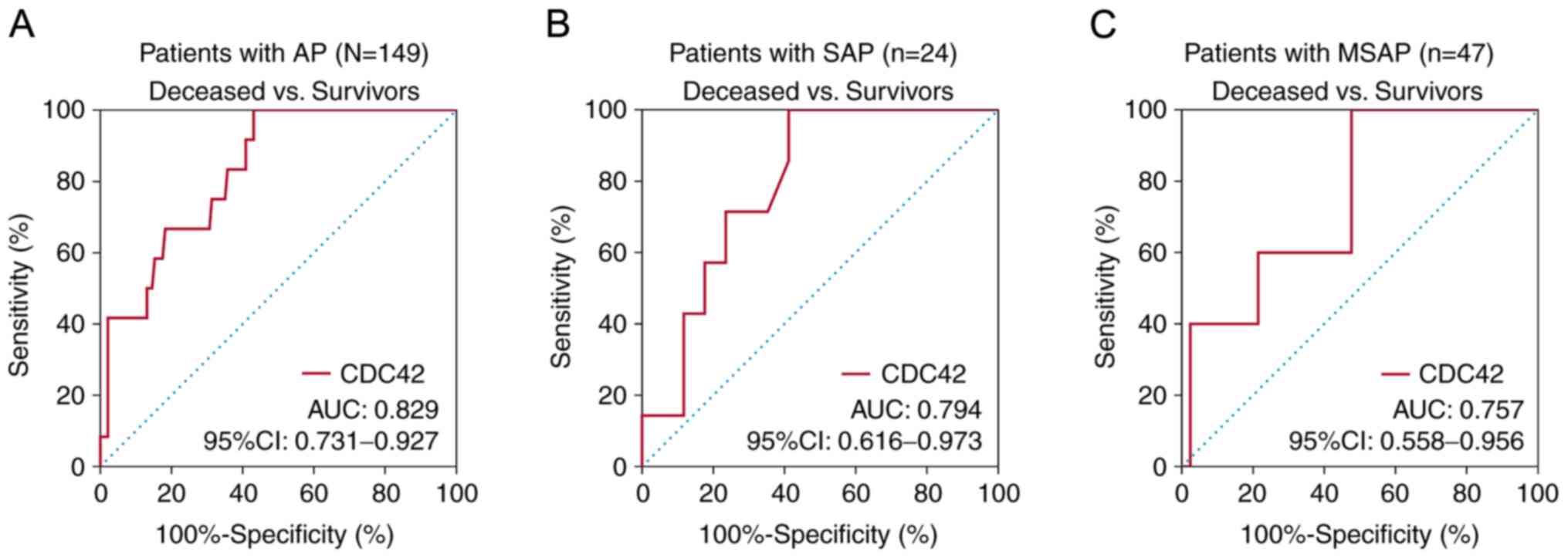
Subsequent receiver operating characteristic
analysis found that CDC42 had good potential in predicting
mortality from AP, with area under the curve (AUC) of 0.829 and a
95% confidence interval (CI) of 0.731-0.927 (Fig. 5A). In addition, CDC42 had certain
potential in predicting mortality from SAP and MSAP, with AUC (95%
CI) of 0.794 (0.616-0.973) and 0.757 (0.558-0.956), respectively
(Fig. 5B and C). In terms of the prognostic value of
Ranson's score (Fig. S2A), APACHE
II score (Fig. S2B) and SOFA
score (Fig. S2C) in patients with
AP, they also had potential in predicting mortality from AP, with
AUC (95% CI) of 0.941 (0.898-0.985), 0.843 (0.722-0.965) and 0.931
(0.882-0.981), respectively.
Discussion
CDC42 has been found to be dysregulated in a number
of inflammatory disorders. For instance, CDC42 expression is
decreased in patients with Crohn's disease compared with that in
the healthy population (21). In
addition, several studies have reported that CDC42 can regulate a
variety of cellular functions in the pancreas, including
glucose-induced insulin secretion and actin cytoskeletal dynamics
(15,22-24).
However, information regarding the potential role of CDC42 in AP is
limited. Therefore, the present study evaluated the expression of
CDC42 in patients with AP and HCs, which revealed that CDC42
expression is decreased in patients with AP compared with that in
HCs. A possible reason for this could be that CDC42 can inhibit
systemic inflammation by promoting M2 macrophage polarization, in
addition to suppressing the differentiation of Th17 cells whilst
enhancing that of Th2 cells and Tregs (11-13).
Since AP is characterized as a systemic inflammatory response
syndrome (25), CDC42 expression
was decreased in patients with AP compared with that in HCs.
The correlation between CDC42 and disease severity
in AP has not been previously reported. To explore this issue,
patients with AP were classified into the MAP, MSAP and SAP
categories according to disease severity. It was subsequently
discovered that CDC42 expression was the lowest in patients with
SAP, followed by patients with MSAP and the highest in patients
with MAP. A possible reason for this may be that organ failure was
associated with in MSAP and SAP (1,26).
Furthermore, CDC42 could prevent multiorgan dysfunction, with
reported effects including the alleviation of intestinal injury
through regulating F-actin cytoskeleton in AP (27-29).
Therefore, CDC42 expression was the lowest in patients with SAP.
Furthermore, the Ranson's, APACHE II and SOFA scores of patients
with AP were evaluated within 24 h from hospitalization, where it
was found that CDC42 expression was negatively correlated with
these scores. A potential explanation for this may be that CDC42
could inhibit inflammation and suppress multiple organ failure
through several pathways such as protein kinase B signaling
(27-29),
which could have led to the decline in the AP assessment scores. In
addition, CDC42 was found to be negatively correlated with
inflammatory indices of patients with AP, which could be explained
by the following: i) CDC42 could restrain the differentiation of
Th1, potentially leading to a subsequent decline in TNF-α levels
(11); and ii) CDC42 could
suppress inflammation by promoting the polarization of M2
macrophages in AP (12,13).
Mortality rates of AP continue to increase,
particularly in patients with SAP (1,30).
Therefore, exploring biomarkers for predicting mortality risk is in
urgent demand to improve the outcome of AP. Currently, the main
methods of predicting mortality risk in AP include bedside index
for severity in acute pancreatitis scoring system and
neutrophil-to-lymphocyte ratio at 48 h, whose measurement
parameters are relatively complicated (31,32).
To identify an accurate and simple approach for predicting
mortality risk, differences in CDC42 expression between patients
who succumbed to AP, SAP and MSAP and those who survived were
evaluated. It was found that lower levels of CDC42 expression
predicted higher mortality risks in all patients with AP, SAP and
MSAP. A potential explanation for this may be that CDC42 could
reduce pancreatic injury by regulating intestinal epithelial cell
cytoskeleton turnover, which could have enhanced survival in
patients with AP (15). Therefore,
data from the present study suggest that CDC42 expression was able
to predict in-hospital mortality from AP. This finding suggested
that CDC42 may serve as a potential predictor of mortality risk for
AP.
The present study had several limitations: i) The
included patients were from a single center, which may have led to
the limited generalizability of the present findings; ii) the role
of CDC42 in the regulatory mechanism of AP should be explored
further to investigate the therapeutic value of CDC42 in AP; iii)
the clinical value of CDC42 in patients with chronic pancreatitis
should be investigated further; iv) RT-qPCR was used for the
quantitative analysis of CDC42 expression in the present study,
whilst the protein expression of CDC42 should be evaluated in the
future studies; v) the levels of TNF-α and IL-6 in the serum from
HCs should be detected in a future study for comparison between
patients with AP and HCs; vi) the number of MSAP and SAP patients
was relatively small, which should be enlarged in the future; and
vii) the correlation of CDC42 expression with disease assessment
and inflammation in patients with AP with different severities
should be explored in a further study.
In conclusion, lower CDC42 expression levels are
were found to be correlated with higher disease susceptibility,
disease severity, inflammation and mortality risk in patients with
AP, suggesting that monitoring CDC42 expression can be used for the
management of AP.
Supplementary Material
Comparison of CDC42 expression levels
in patients with AP of different etiologies. CDC42, cell division
cycle 42; AP, acute pancreatitis; BAP, biliary AP; HTGAP,
hypertriglyceridemia AP; AAP, alcohol-induced AP.
Correlation of Ranson's score, APACHE
II score and SOFA score with mortality of patients with AP. The
ability of (A) Ranson's score, (B) APACHE II score and (C) SOFA
score to predict mortality in patients with AP. AP, acute
pancreatitis; APACHE II, acute Pathologic and Chronic Health
Evaluation II; SOFA, Sequential Organ Failure Assessment; AUC, area
under the curve; CI, confidence interval.
Independent risk factor for mortality
in AP patients by logistic regression model analysis.
Acknowledgements
Not applicable.
Funding
Funding: This study was supported by The Special Funding for the
Construction of Innovative Provinces in Hunan (2021SK4031), The
Scientific Research Project of Hunan Health and Family Planning
Commission (No. A2017015), The Natural Science Foundation of Hunan
Province, China (No. 2016JJ5010), The National Natural Science
Foundation of China (No. 81373465), The Scientific Research Project
of Hunan Health Committee(No. 20201938), The Hengyang Science and
Technology Guide Project (No. 2020jh042880) and The Hengyang
Science and Technology Guide Project (No. 2020jh042914).
Availability of data and materials
The datasets used and/or analyzed during the current
study are available from the corresponding author on reasonable
request.
Authors' contributions
JY and XL conceived and designed the study. XY
contributed to data acquisition of patients. HW contributed to the
PCR and ELISA. LD and NF performed the statistical analysis and
figures plotted. JY performed statistical analysis and critically
revised the manuscript. JY and XL confirm the authenticity of all
the raw data. All authors read and approved the final
manuscript.
Ethics approval and consent to
participate
This study was approved by Institutional Review
Board of the Affiliated Nanhua Hospital, University of South China
(approval no. 2017-136; Hengyang, China). The written informed
consent was obtained from all subjects or their guardians.
Patient consent for publication
Not applicable.
Competing interests
The authors declare that they have no competing
interests.
References
|
1
|
Boxhoorn L, Voermans RP, Bouwense SA,
Bruno MJ, Verdonk RC, Boermeester MA, van Santvoort HC and
Besselink MG: Acute pancreatitis. Lancet. 396:726–734.
2020.PubMed/NCBI View Article : Google Scholar
|
|
2
|
Lee PJ and Papachristou GI: New insights
into acute pancreatitis. Nat Rev Gastroenterol Hepatol. 16:479–496.
2019.PubMed/NCBI View Article : Google Scholar
|
|
3
|
Petrov MS and Yadav D: Global epidemiology
and holistic prevention of pancreatitis. Nat Rev Gastroenterol
Hepatol. 16:175–184. 2019.PubMed/NCBI View Article : Google Scholar
|
|
4
|
Trikudanathan G, Wolbrink DRJ, van
Santvoort HC, Mallery S, Freeman M and Besselink MG: Current
concepts in severe acute and necrotizing pancreatitis: An
evidence-based approach. Gastroenterology. 156:1994–2007 e3.
2019.PubMed/NCBI View Article : Google Scholar
|
|
5
|
Mandalia A, Wamsteker EJ and DiMagno MJ:
Recent advances in understanding and managing acute pancreatitis.
F1000Res 7: F1000 Faculty Rev-959, 2018.
|
|
6
|
Siegel RL, Miller KD, Fuchs HE and Jemal
A: Cancer statistics, 2021. CA Cancer J Clin. 71:7–33.
2021.PubMed/NCBI View Article : Google Scholar
|
|
7
|
Tempero MA, Malafa MP, Al-Hawary M,
Behrman SW, Benson AB, Cardin DB, Chiorean EG, Chung V, Czito B,
Del Chiaro M, et al: Pancreatic adenocarcinoma, version 2.2021,
NCCN clinical practice guidelines in oncology. J Natl Compr Canc
Netw. 19:439–457. 2021.PubMed/NCBI View Article : Google Scholar
|
|
8
|
Pichaud F, Walther RF and Nunes de Almeida
F: Regulation of Cdc42 and its effectors in epithelial
morphogenesis. J Cell Sci. 132(jcs217869)2019.PubMed/NCBI View Article : Google Scholar
|
|
9
|
Liu Y, Dou Y, Yan L, Yang X, He B, Kong L
and Smith W: The role of Rho GTPases' substrates Rac and Cdc42 in
osteoclastogenesis and relevant natural medicinal products study.
Biosci Rep. 40(BSR20200407)2020.PubMed/NCBI View Article : Google Scholar
|
|
10
|
Kalim KW, Yang JQ, Li Y, Meng Y, Zheng Y
and Guo F: Reciprocal regulation of glycolysis-driven Th17
pathogenicity and regulatory T cell stability by Cdc42. J Immunol.
200:2313–2326. 2018.PubMed/NCBI View Article : Google Scholar
|
|
11
|
Guo F: RhoA and Cdc42 in T cells: Are they
targetable for T cell-mediated inflammatory diseases? Precis Clin
Med. 4:56–61. 2021.PubMed/NCBI View Article : Google Scholar
|
|
12
|
Cao J, Zhang C, Jiang GQ, Jin SJ, Wang Q,
Wang AQ and Bai DS: Identification of hepatocellular
carcinoma-related genes associated with macrophage differentiation
based on bioinformatics analyses. Bioengineered. 12:296–309.
2021.PubMed/NCBI View Article : Google Scholar
|
|
13
|
Zhang B, Zhang J, Xia L, Luo J, Zhang L,
Xu Y, Zhu X and Chen G: Inhibition of CDC42 reduces macrophage
recruitment and suppresses lung tumorigenesis in vivo. J Recept
Signal Transduct Res. 41:504–510. 2021.PubMed/NCBI View Article : Google Scholar
|
|
14
|
Zhen J, Chen W, Liu Y and Zang X: Baicalin
protects against acute pancreatitis involving JNK signaling pathway
via regulating miR-15a. Am J Chin Med. 49:147–161. 2021.PubMed/NCBI View Article : Google Scholar
|
|
15
|
Wang H, Jiang Y, Li H, Wang J, Li C and
Zhang D: Carbachol protects the intestinal barrier in severe acute
pancreatitis by regulating Cdc42/F-actin cytoskeleton. Exp Ther
Med. 20:2828–2837. 2020.PubMed/NCBI View Article : Google Scholar
|
|
16
|
Foster BR, Jensen KK, Bakis G, Shaaban AM
and Coakley FV: Revised Atlanta classification for acute
pancreatitis: A pictorial essay. Radiographics. 36:675–687.
2016.PubMed/NCBI View Article : Google Scholar
|
|
17
|
Knaus WA, Draper EA, Wagner DP and
Zimmerman JE: APACHE II: A severity of disease classification
system. Crit Care Med. 13:818–829. 1985.PubMed/NCBI
|
|
18
|
Vincent JL, Moreno R, Takala J, Willatts
S, De Mendonça A, Bruining H, Reinhart CK, Suter PM and Thijs LG:
The SOFA (sepsis-related organ failure assessment) score to
describe organ dysfunction/failure. On behalf of the working group
on sepsis-related problems of the european society of intensive
care medicine. Intensive Care Med. 22:707–710. 1996.PubMed/NCBI View Article : Google Scholar
|
|
19
|
Sun N, Ye L, Chang T and Li X and Li X:
microRNA-195-Cdc42 axis acts as a prognostic factor of esophageal
squamous cell carcinoma. Int J Clin Exp Pathol. 7:6871–6879.
2014.PubMed/NCBI
|
|
20
|
Livak KJ and Schmittgen TD: Analysis of
relative gene expression data using real-time quantitative PCR and
the 2(-Delta Delta C(T)) method. Methods. 25:402–408.
2001.PubMed/NCBI View Article : Google Scholar
|
|
21
|
Tang WJ, Peng KY, Tang ZF, Wang YH, Xue AJ
and Huang Y: MicroRNA-15a-cell division cycle 42 signaling pathway
in pathogenesis of pediatric inflammatory bowel disease. World J
Gastroenterol. 24:5234–5245. 2018.PubMed/NCBI View Article : Google Scholar
|
|
22
|
Veluthakal R and Thurmond DC: Emerging
roles of small GTPases in islet β-cell function. Cells.
10(1503)2021.PubMed/NCBI View Article : Google Scholar
|
|
23
|
Chundru SA, Harajli A, Hali M, Gleason N,
Gamage S and Kowluru A: RhoG-Rac1 signaling pathway mediates
metabolic dysfunction of the pancreatic beta-cells under chronic
hyperglycemic conditions. Cell Physiol Biochem. 55:180–192.
2021.PubMed/NCBI View Article : Google Scholar
|
|
24
|
He XQ, Wang N, Zhao JJ, Wang D, Wang CJ,
Xie L, Zheng HY, Shi SZ, He J, Zhou J, et al: Specific deletion of
CDC42 in pancreatic beta cells attenuates glucose-induced insulin
expression and secretion in mice. Mol Cell Endocrinol.
518(111004)2020.PubMed/NCBI View Article : Google Scholar
|
|
25
|
Habtezion A, Gukovskaya AS and Pandol SJ:
Acute pancreatitis: A multifaceted set of organelle and cellular
interactions. Gastroenterology. 156:1941–1950. 2019.PubMed/NCBI View Article : Google Scholar
|
|
26
|
Garg PK and Singh VP: Organ failure due to
systemic injury in acute pancreatitis. Gastroenterology.
156:2008–2023. 2019.PubMed/NCBI View Article : Google Scholar
|
|
27
|
Woods B and Lew DJ: Polarity establishment
by Cdc42: Key roles for positive feedback and differential
mobility. Small GTPases. 10:130–137. 2019.PubMed/NCBI View Article : Google Scholar
|
|
28
|
Li Z, Wu J, Zhang X, Ou C, Zhong X, Chen
Y, Lu L, Liu H, Li Y, Liu X, et al: CDC42 promotes vascular
calcification in chronic kidney disease. J Pathol. 249:461–471.
2019.PubMed/NCBI View Article : Google Scholar
|
|
29
|
Li J, Liu Y, Jin Y, Wang R, Wang J, Lu S,
VanBuren V, Dostal DE, Zhang SL and Peng X: Essential role of Cdc42
in cardiomyocyte proliferation and cell-cell adhesion during heart
development. Dev Biol. 421:271–283. 2017.PubMed/NCBI View Article : Google Scholar
|
|
30
|
Leppäniemi A, Tolonen M, Tarasconi A,
Segovia-Lohse H, Gamberini E, Kirkpatrick AW, Ball CG, Parry N,
Sartelli M, Wolbrink D, et al: 2019 WSES guidelines for the
management of severe acute pancreatitis. World J Emerg Surg.
14(27)2019.PubMed/NCBI View Article : Google Scholar
|
|
31
|
Jinno N, Hori Y, Naitoh I, Miyabe K,
Yoshida M, Natsume M, Kato A, Asano G, Sano H and Hayashi K:
Predictive factors for the mortality of acute pancreatitis on
admission. PLoS One. 14(e0221468)2019.PubMed/NCBI View Article : Google Scholar
|
|
32
|
Dancu GM, Popescu A, Sirli R, Danila M,
Bende F, Tarta C and Sporea I: The BISAP score, NLR, CRP, or BUN:
Which marker best predicts the outcome of acute pancreatitis?
Medicine (Baltimore). 100(e28121)2021.PubMed/NCBI View Article : Google Scholar
|