Introduction
Colorectal cancer (CRC) is one of the most frequent
causes of cancer-related deaths worldwide (1). Its carcinogenesis is a multistep
process and the molecular mechanisms of its development and
metastasis remain elusive (2).
Although some improvements have been made in early diagnosis and
systemic therapies, only ~50% of patients with CRC survive for at
≥5 years following diagnosis (3).
Chemotherapeutic drugs can significantly inhibit the progression of
CRC, but drug resistance remains a major cause of failure in
chemotherapy regimens (4,5).
Chaperone-mediated autophagy (CMA) is a highly
selective form of autophagy for cellular quality control (6). During CMA, the heat shock cognate
protein 70 (HSC70) chaperone carries target proteins endowed with a
certain KFERQ-like motif to the lysosome-associated membrane
protein 2A (LAMP2A), which then translocates them into lysosomes
for degradation (6,7). LAMP2A is the best criterion to
determine whether protein degradation occurs via CMA (8). CMA is activated in multiple types of
cancers such as breast (9,10), colorectal (11), gastric (12) and liver (13) cancer which demonstrates that LAMP2A
overexpression contributes to tumor growth and metastasis. In
addition, CMA is reported to be associated with the resistance to
anticancer therapy (11,14).
Phospholipase D (PLD) is an enzyme that catalyzes
the hydrolysis of phosphatidylcholine, the most abundant
phospholipid in eukaryotic cell membranes, to produce phosphatidic
acid (PA) and choline (15). PA is
the second messenger that can be metabolized to other lipid
metabolites, such as lyso-PA and diacylglycerol (16). A total of two mammalian isoforms of
PLD have been described; PLD1 and PLD2, which are almost ubiquitous
and share ~50% homology (17,18).
PLD2 overexpression increases proliferation, adhesion, invasion and
metastasis in a wide variety of cancers including gastric,
colorectal, renal, stomach, lung and breast cancers (16,19–22).
In addition, it has been reported that PLD2 is associated with
multidrug resistance in human cancer cells (23).
To obtain insights into the mechanism of 5-FU
resistance in CRC cells, the present study constructed
5-FU-resistant HCT116 and DLD-1 cells from parental HCT116 and
DLD-1 cell lines. It demonstrated that HCT116- R/DLD-1-R cells
exhibited a drastic elevation of LAMP2A and this resulted in
enhanced PLD2 expression through the activation of the NF-κB-p65
pathway. Accordingly, loss or gain of function of LAMP2A in 5-FU
resistant CRC cells rendered them sensitive or resistant to 5-FU,
respectively.
Materials and methods
Cell culture and reagents
HCT-116, DLD-1 and NCM460 cell lines were obtained
from Professor Miyagi Yohei (Clinical Research Institute, Kanagawa
Cancer Center, Yokohama, Japan). The cell lines were cultured as
monolayers in RPMI-1640 medium (Thermo Fisher Scientific, Inc.)
supplemented with 10% fetal bovine serum (FBS; Thermo Fisher
Scientific, Inc.) with 100 U/ml penicillin and 100 µg/ml
streptomycin at 37°C in a humidified atmosphere containing 5%
CO2. All cells were harvested by centrifugation (1,500 ×
g for 10 min at 4°C) and rinsed with phosphate-buffered saline
(PBS). Anti-LAMP2A (cat. no. ab18528) and anti-PLD2 (cat. no.
ab78907) antibodies were purchased from Abcam. NF-κB Pathway
Sampler kit (cat. no. 9936T) was purchased from Cell Signaling
Technology, Inc. Anti-cluster of differentiation
(CD)147/extracellular matrix metalloproteinase inducer (EMMPRIN;
cat. no. SC-21746) antibody was purchased from Santa Cruz
Biotechnology, Inc. Anti-lung resistance-related protein 1 (LRP1;
cat. no. ab92544), anti-P-glycoprotein 1 (PGP)/multidrug resistance
(MDR; cat. no. ab242104), anti-glutathione S-transferase π (GST-π;
cat. no. ab138491), anti-MutL homologue 1 (MLH1; cat. no. ab92312),
Anti-F-box and WD40 domain protein 7 (FBXW7) antibody (cat. no.
ab12292) and anti-multidrug resistance-associated protein 1 (MRP1;
cat. no. ab233383) antibodies were purchased from Abcam. Anti-Bcl-2
(cat. no. 15071) and anti-BAX (cat. no. 14796) antibodies were
purchased from Cell Signaling Technology, Inc.
LysoTracker-LysoGreen was purchased from Nanjing KeyGen Biotech
Co., Ltd. (cat. no. KGMP006-2). Pyrrolidine dithiocarbamate (PDTC;
cat. no. P8765.) and chloroquine (CQ; cat. no. C6628.) were
purchased from Sigma-Aldrich (Merck KGaA) and 5-fluorouracil (5-FU)
was purchased from Shanghai Xudong Haipu Pharmaceutical Co., Ltd.
Oxaliplatin (OXA) was purchased from Nanjing Pharmaceutical
Factory, Co. Ltd.
Cell viability assay
Cell viability was measured using the MTT assay. CRC
and 5-FU-resistant CRC cells were seeded in triplicate in 96-well
plates at 6,000 cells/well and incubated at 37°C for 24 h in
RPMI-1640 medium supplemented with 10% FBS. Subsequently, the cells
were treated with the indicated doses of 5-FU (10 mM), OXA (10 mM),
or FOX (5-FU: 10 mM + OXA: 10 mM) for 96 h at 37°C. The same volume
of dimethyl sulfoxide (DMSO) was used as the negative control.
Following this, 25 µl MTT solution (5 mg/ml) was added to each well
for 4 h at 37°C, then the cell culture supernatants were carefully
removed and 200 µl DMSO was added to dissolve the purple formazan.
Finally, the optical density was measured at a wavelength of 570 nm
using a microplate reader (Model 550; Bio-Rad Laboratories,
Inc.).
Cell migration and invasion
assays
For the migration assay, 2×105 cells were
resuspended in serum-free RPMI-1640 and seeded in the
Matrigel-coated insert (BD Biosciences) insert on the top portion
of the chamber (BD Biosciences). The lower compartment of the
chamber contained 10% FBS as a chemoattractant. After incubation
for 24 h, cells on the membrane were scrubbed, washed with PBS,
fixed in 100% methanol for 10 min at room temperature and stained
with 10% Giemsa dye for 10–15 min at room temperature. For the
invasive assay, the procedures were the same as above with a
control-membrane insert (BD Biosciences). A total of five random
fields were selected to count and images were captured under an
inverted fluorescence microscope (×10 magnification; Nikon
Corporation).
Quantification of apoptosis by flow
cytometry
Flow cytometry was performed with 7-aminoactinomycin
and phycoerythrin labeled Annexin V (BD Pharmingen; BD Biosciences)
to detect phosphatidylserine externalization as an endpoint
indicator of apoptosis. Cell apoptosis was detected by staining
with Annexin V-PE/7AAD (KeyGen Biotech Co., Ltd.; cat. no. KGA214)
according to the manufacturer's instructions. Apoptotic rate was
calculated by the percentage of early + late apoptotic cells. After
washing with PBS and centrifuging twice (both 1,000 × g, 5 min),
cells were resuspended in Annexin-V binding buffer. They were
stained with Annexin V-PE/7AAD and incubated for another 15 min at
room temperature in a dark room. Cell samples were analyzed by flow
cytometry (FACScan; BD Biosciences) to acquire the apoptotic
fractions. Apoptotic fractions were investigated by Cell Quest 3.0
software (BD Biosciences).
Cell transfection
The short hairpin (sh)RNA and LAMP2A expression
plasmids were designed, constructed and purified by Shanghai
GenePharma Co., Ltd. The shRNA and LAMP2A expression plasmids were
transfected using Attractene Transfection Reagent (Qiagen GmbH) in
accordance with the manufacturer's instructions. Cells cultured in
6-well plates were transfected with 1.2 ug/well shRNA or LAMP2A
expression plasmids. At 24 h after transfection, the cells were
collected to extract RNA and total protein for subsequent
experimentation.
RNA extraction
Total RNA was extracted from cultivated cells using
TRIzol® reagent (Thermo Fisher Scientific, Inc.) in
accordance with the manufacturer's protocols. RNA purification was
performed using the RNeasy Mini kit (Qiagen GmbH) according to the
manufacturer's instructions.
Reverse transcription-quantitative
(RT-q) PCR
Total RNA was extracted from CRC cells
(1×106) using the Qiagen RNeasy Mini kit (Qiagen GmbH),
according to the manufacturer's protocols. Total RNA was subjected
to cDNA synthesis using avian myeloblastosis virus reverse
transcriptase and random primer (Takara Bio, Inc.). General- and
RT-qPCR amplification was performed using TaKaRa Hot Start Taq
Polymerase (Takara Bio, Inc.) and SYBR Premix Ex Taq TM II kit
(Takara Bio, Inc.), respectively, all according to the
manufacturer's protocols. All experiments were performed three
times. mRNA expression analysis was performed using SYBR Green
Master Mix (Life Technologies; Thermo Fisher Scientific, Inc.) on a
LightCycler 96 Detection system (Roche Diagnostics) using β-actin
for normalization. The cycling parameters were: 95°C for 5 min,
followed by 59 cycles at 95°C for 30 sec, annealing at 55°C for 30
sec and extension at 72°C for 30 sec. Expression levels were
normalized to endogenous controls and relative quantification
(2−ΔΔCq) was used for fold-change calculation (24). Using GenBank, oligonucleotide
primers were designed as follows: LAMP2A: Forward primer:
5′-GCCGTTCTCACACTGCTCTA-3′; reverse primer:
5′-CCGCTATGGGCACAAGGAA-3′. PLD2: Forward primer:
5′-CCACAAACAGGGGTGGTGTT-3′; reverse primer:
5′-GAATGGCCTGGATGGAGTTG-3′; β-actin: Forward primer:
5′-GGTGGCTTTTAGGATGGCAAG-3′; reverse primer:
5′-ACTGGAACGGTGAAGGTGACAG-3′.
Western blot analysis
Cells were lysed in SDS cell lysis buffer containing
50 mM Tris (pH, 8.1) and 1% SDS, supplemented with protease
inhibitors (Roche Diagnostics) for 30 min on ice. The homogenates
were centrifuged at 18,000 × g for 10 min at 4°C. Supernatants were
collected, and the protein concentration was determined by
Bradford's assay (Bio-Rad Laboratories, Inc.); 30 µg protein was
loaded for analysis. The proteins were separated via 12% SDS-PAGE
and electrotransferred onto a PVDF (polyvinylidene fluoride)
membrane, which was then blocked overnight in 5% skimmed milk in
Tris-buffered saline with Tween-20 (TBST, 10 mM Tris-HCl, 150 mM
NaCl, 0.1% Tween-20) at 4°C. For immunoblotting, the membrane was
incubated with primary antibody (all 1:1,000) for 2 h at room
temperature (20°C) as follows: LAMP2A, PLD2, NF-κB, Bcl-2, BAX,
MRP1, PGP, CD147, FBXW7, MLH1, LRP1 and GSTπ. Then, it was
incubated with anti-rabbit or anti-mouse IgG antibodies conjugated
to horseradish peroxidase (Dako; Agilent Technologies, Inc.) at a
dilution of 1:5,000 for 2 h at room temperature. The bands were
visualized using ECL-Plus detection reagents (Santa Cruz
Biotechnology, Inc.). The densitometric quantification was
performed with β-actin (1:1,000; Santa Cruz Biotechnology, Inc.;
cat. no. sc-47778) control using - ImageJ software (ImageJ 1.52a;
National Institutes of Health).
Co-immunoprecipitation
CRC cells (1×107) were seeded onto 100 mm
plates and allowed to attach overnight at 37°C. The cells were then
washed twice with PBS and lysed in lysis buffer (1% Triton X-100,
50 mM Tris-HCl pH 7.4, 150 mM NaCl, 10 mM EDTA, 100 mM NaF, 1 mM
Na3VO4, 1 mM phenylmethylsulfonyl fluoride
and 2 µg/ml aprotinin) on ice. Co-immunoprecipitation was performed
using 200 µg lysates with 4 µl of rabbit anti- NF-κB or control IgG
mixed with protein G agarose beads (GE Healthcare Bio-Sciences).
The final mixture was gently agitated overnight at 4°C. Following
this, the beads were centrifuged for 1 min at 13,000 × g at 4°C and
washed four times with lysis buffer for 1 min. Finally, 40 µl
sampling buffer (Beyotime Institute of Biotechnology) was added,
boiled at 95°C for 5 min and subjected to western blot analysis. A
total of 30 µg protein was loaded for analysis. The proteins were
separated via 10% SDS-PAGE and transferred onto a PVDF membrane,
which was then blocked overnight in 5% skimmed milk in TBST (10 mM
Tris-HCl, 150 mM NaCl, 0.1% Tween-20) at 4°C. For immunoblotting,
the membrane was incubated with primary antibodies (all 1:1,000)
for 2 h at room temperature (20°C) as follows: LAMP2A, PLD2, NF-κB,
MRP1, PGP, CD147, FBXW7, MLH1, LRP1 and GSTπ. Then, it was
incubated with anti-rabbit or anti-mouse IgG antibodies conjugated
to horseradish peroxidase (Dako; Agilent Technologies, Inc.) at a
dilution of 1:5,000 for 2 h at room temperature. The bands were
visualized using ECL-Plus detection reagents (Santa Cruz
Biotechnology, Inc.). The densitometric quantification was
performed with β-actin (1:1,000; Santa Cruz Biotechnology, Inc.;
cat. no. sc-47778) control using ImageJ software (version 1.52a;
National Institutes of Health).
Statistical analysis
All statistical analyses were performed by SPSS
v24.0 (IBM Corp.) with the Student's t-test (two tailed) and by
one-way analysis of variance with Tukey's post hoc test for
multiple groups. The results are representative of three different
experiments and data are expressed as mean ± standard deviation.
P<0.05 was considered to indicate a statistically significant
difference.
Results
Establishment of 5-FU-resistant human
CRC cell line
To obtain 5-FU-resistant cells, CRC cells were first
selected using increasing concentrations of 5-FU on parental
HCT-116/DLD-1 cells. They were then intermittently treated with
large doses of 5-FU. Cells that acquired 5-FU resistance were
identified by cell survival assay and showed increased expression
of drug resistance proteins, CD147/EMMPRIN (25); LRP1 (26); PGP/MDR (26); GST-π (27); MLH1 (28,29);
MRP1 (26); FBXW7 (30), as verified by western blotting. They
were labeled as HCT116-R or DLD-1-R cells (Fig. 1A-D). HCT116-R or DLD-1-R cells
increased in size and the nuclei were irregular. Some cells had
multiple, enlarged lysosomes. The proliferation rate of HCT116-R or
DLD-1-R cells was similar to the parental cells, but the doubling
time was prolonged in vitro (Fig. 1A and B). Co-resistance to other
chemotherapy drugs such as OXA were also observed in HCT116-R or
DLD-1-R cells (Fig. 1E).
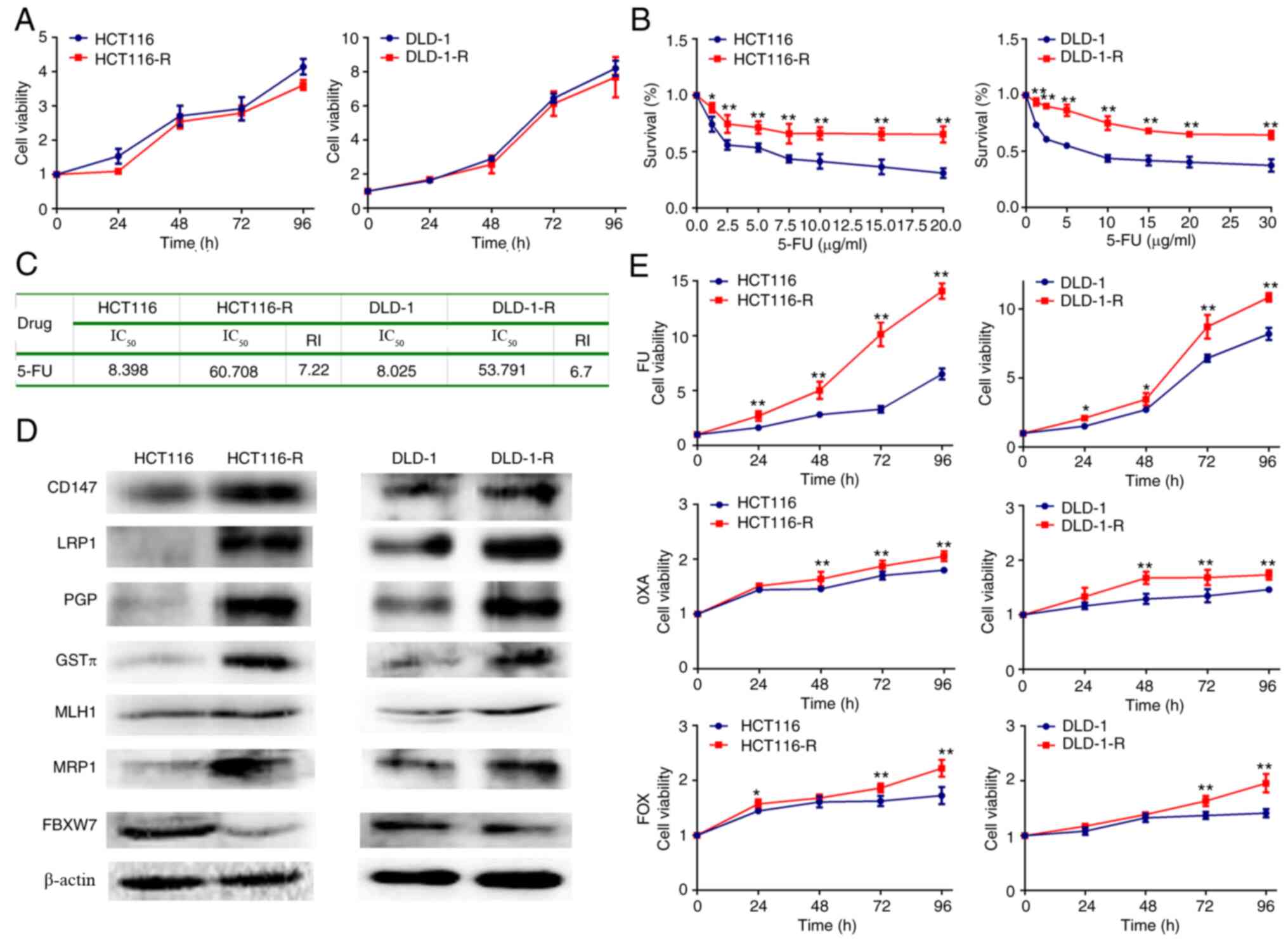 | Figure 1.Generation and characterization of
5-FU-resistant cells from HCT116 and DLD-1 cells. (A) Cell
proliferation curve of HCT116/DLD-1 and HCT116-R/DLD-1-R cells. (B)
Cell survival curve of HCT116/DLD-1 and HCT116-R/DLD-1-R cells. (C)
RI and IC50 of 5-FU in HCT116/DLD-1 and HCT116-R/DLD-1-R
cells. (D) Protein expression of chemoresistance-related genes by
western blotting. (E) Cell proliferation curve of HCT116/DLD-1 and
HCT116-R/DLD-1-R cells after chemotherapy drug treatment. The data
represent the mean ± standard deviation from three independent
experiments. *P<0.05. **P<0.01. 5-FU, 5-fluorouracil; R,
resistance; RI, resistance index; IC50, inhibitory
concentration; 5-FU, 10 mM; 5-FU; OXA, 10 mM oxaliplatin; FOX, 10
mM 5-FU + 10 mM oxaliplatin; CD, cluster of differentiation; LRP1,
lung resistance-related protein 1; PGP, P-glycoprotein 1; GSTπ,
glutathione S-transferase π; MLH1, MutL homologue 1; MRP1;
multidrug resistance-associated protein 1; FBXW7, F-box and WD40
domain protein 7. |
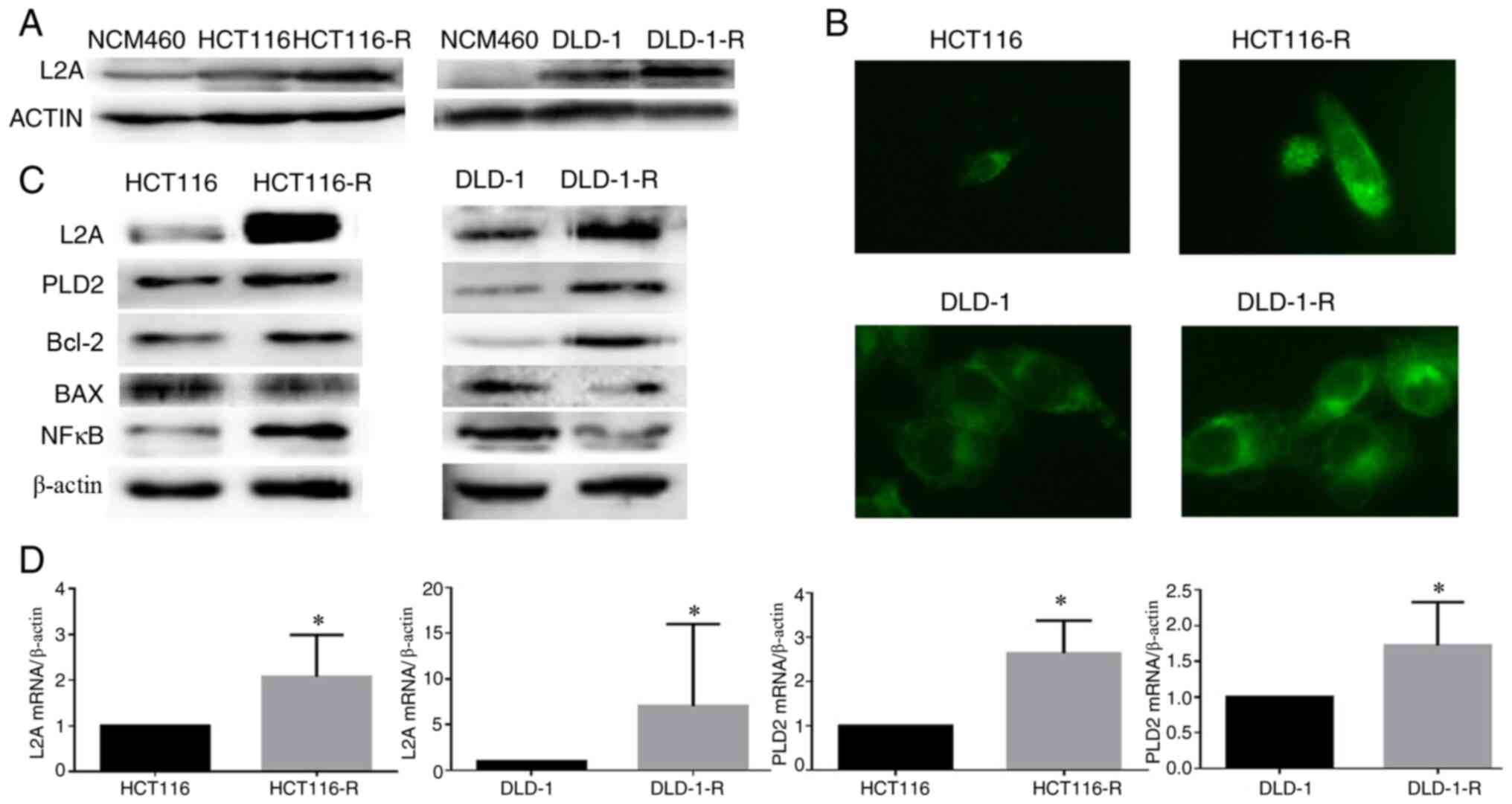
LAMP2A is highly expressed in human
CRC cell lines
Compared to parental cells, a significant elevation
of LAMP2A was found in HCT116-R/DLD-1-R cells. However, the
expression of LAMP2A was minimal in their corresponding normal
colonic epithelial cells, NCM460 (Fig.
2A). In addition, HCT116-R/DLD-1-R cells had multiple, enlarged
lysosomes when examined by LysoTracker staining (Fig. 2B). Meanwhile, enhanced PLD2 and
Bcl-2 protein expression was found in HCT116-R/DLD-1-R cells
(Fig. 2C). The same results were
observed in the mRNA levels of LAMP2A and PLD2 by a RT-qPCR
(Fig. 2D).
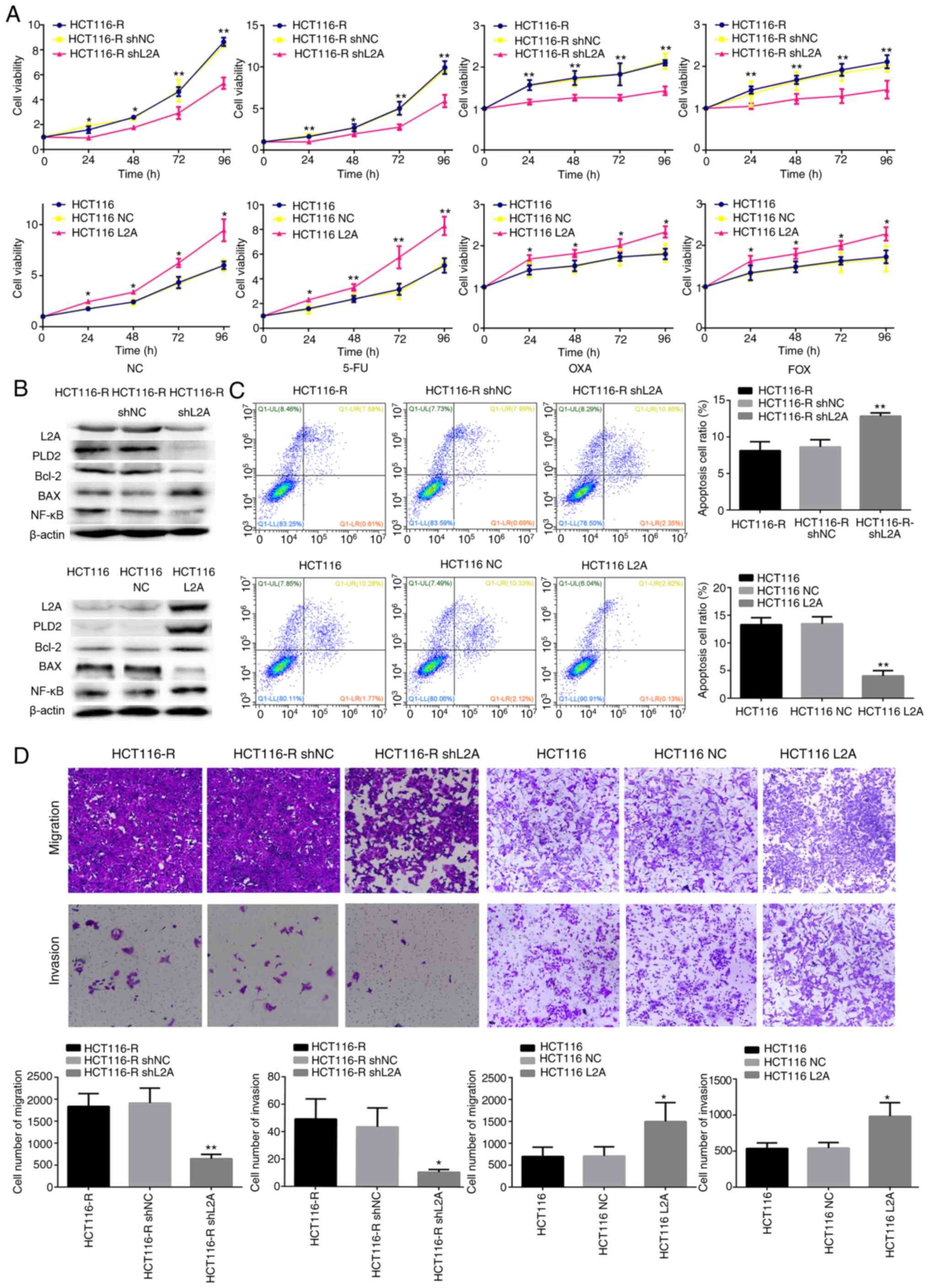
Effect of LAMP2A expression on the
sensitivity to 5-FU in human CRC cell lines
Excessive LAMP2A expression is one of the major
features of HCT116-R/DLD-1-R cells. It was hypothesized that the
silence or overexpression LAMP2A expression in HCT116-R/DLD-1-R
cells would affect the sensitivity to 5-FU. LAMP2A expression was
decreased in HCT116-R/DLD-1-R cells by transfection with shLAMP2A
plasmid, which resulted in decreased cell growth rate and increased
5-FU-mediated cell death (Figs. 3A and
B; 4A and B). Conversely, when
LAMP2A expression was increased in HCT116/DLD-1 cells by
transfection with the LAMP2A overexpression plasmid, markedly
increased cell growth rate and decreased 5-FU-mediated cell death
was observed (Figs. 3A and B and
4A and B). The same results were
observed following treatment with OXA and FOX (Figs. 3A and 4A). In addition, the knockdown of LAMP2A
in HCT116-R/DLD-1-R cells or overexpression of LAMP2A in
HCT116/DLD-1 cells was associated with decreased or increased
expression of Bcl-2. The expression of Bax was opposite (Figs. 3B and 4B). Migration and invasion were lower in
cells with knockdown of LAMP2A, but apoptosis was higher. Adverse
results were found in cells overexpression of LAMP2A (Figs. 3C and D and 4C and D). Therefore, it was confirmed that
HCT116-R/DLD-1-R cells can regain sensitivity to 5-FU if LAMP2A
expression is reduced.
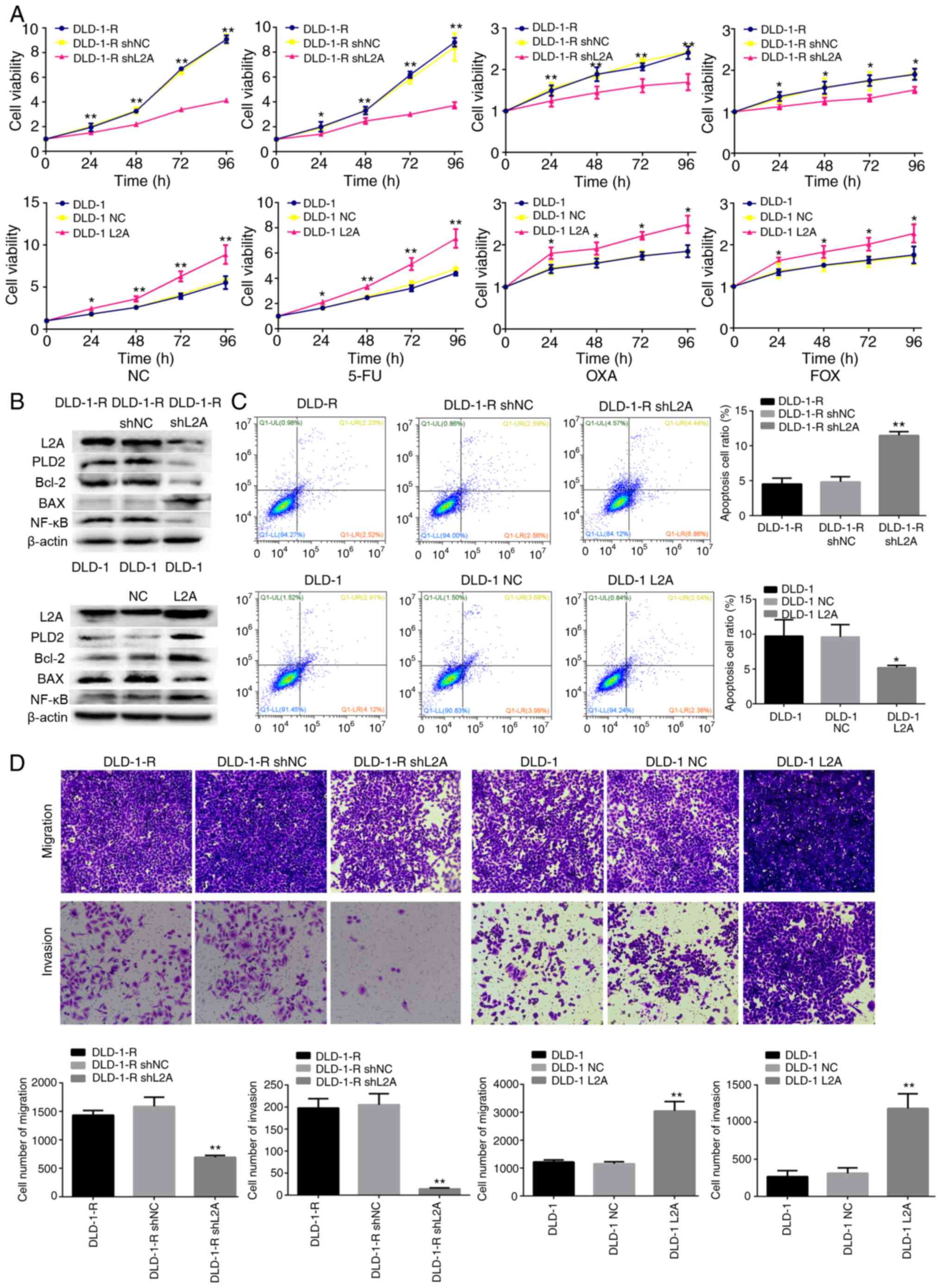 | Figure 4.Effect of LAMP2A expression on the
sensitivity to 5-FU in human CRC cell line. (A) Cellular viability
of different drug treatments in shLAMP2A-modified DLD-1-R or
LAMP2A-modified DLD-1 cells. (B) Expression of associated proteins
was visualized by western blotting in shLAMP2A-modified DLD-1-R
cells or in LAMP2A-modified DLD-1 cells. (C) Apoptosis and (D)
migration and invasion in shLAMP2A-modified DLD-1-R cells or in
LAMP2A-modified DLD-1 cells (×10 magnification). The data represent
the mean ± standard deviation from three independent experiments.
*P<0.05, **P<0.01. LAMP2A, lysosome-associated membrane
protein 2A; 5-FU, 5-fluorouracil; CRC, colorectal cancer; sh, short
hairpin; R, resistance; NC, negative control; 5-FU, 10 mM; 5-FU;
OXA, 10 mM oxaliplatin; FOX, 10 mM 5-FU + 10 mM oxaliplatin; PLD2,
phospholipase D2. |
High expression of LAMP2A enhances
PLD2 expression and 5-FU chemoresistance through the activation of
the NF-κB pathway
Knockdown of LAMP2A in HCT116-R/DLD-1-R cells or
overexpression of LAMP2A in HCT116/DLD-1 cells was associated with
decreased or increased expression of PLD2 and NF-κB, respectively.
It was hypothesized whether high expression of LAMP2A enhanced PLD2
expression through activation of NF-κB pathway. Therefore,
HCT116-R/DLD-1-R cells were treated with CQ or PDTC to inhibit the
lysosomal or NF-κB pathways. When HCT116/DLD-1 and HCT116-R/DLD-1-R
cells were treated with CQ (50 mM) and harvested at specific time
points (0, 2, 4, 6, 8 and 10 h), it was identified that PLD2 first
decreased and then increased (Fig.
5A). The lowest level was observed at 4 h. Next, HCT116/DLD-1
and HCT116-R/DLD-1-R cells were treated with CQ (50 mM) for 4 h and
a clear and significant reduction of PLD2 was observed compared
with non-treated cells in the western blot analysis (Fig. 5B and C). Notably, similar results
were obtained with PDTC (10 mM, 2 h; Fig. 5B and C). Co-immunoprecipitation
experiments further confirmed the interaction of NF-κB with PLD2
(Fig. 5D). In addition, some
drug-resistance proteins (CD147, GST3 and MLH1) were observed to be
associated with NF-κB by co-immunoprecipitation experiments
(Fig. 5D).
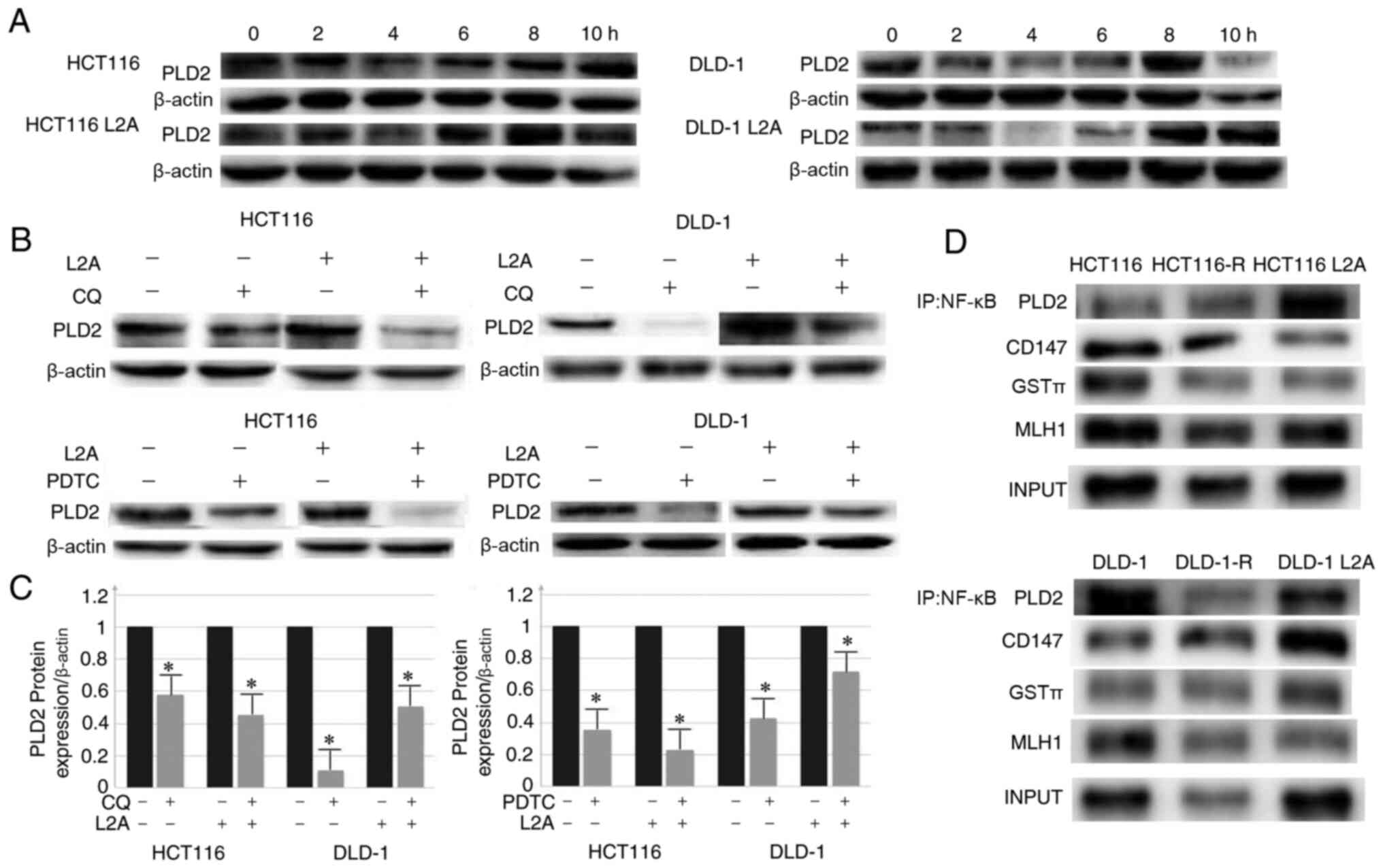 | Figure 5.Inhibition of lysosomal and NF-κB p65
signaling pathways led to proliferation and decrease in expression
level of PLD2 in CRC cell lines. (A) Inhibition of the lysosomal
pathway with CQ (50 mM); PLD2 first declined and then increased
with the lowest point observed at 4 h. (B and C) Inhibition of the
lysosomal pathway (CQ; 50 Mm, 4 h) and NF-κB signaling pathway
(PDTC; 10 mM; 2 h) led to a significant reduction in the expression
level of PLD2 compared with the control group. (D)
Co-immunoprecipitation of NF-κB with PLD2, CD147, GST3, MLH1 in
HCT116/DLD-1, HCT116-R/DLD-1-R and HCT116L2A/DLD-1L2A cells. The
data represent the mean ± standard deviation from three independent
experiments. *P<0.05. PLD2, phospholipase D2; R, resistance;
CRC, colorectal cancer; CQ, clioquinol; PDTC, pyrrolidine
dithiocarbamate; CD, cluster of differentiation; LRP1, lung
resistance-related protein 1; PGP, P-glycoprotein 1; GST,
glutathione S-transferase; MLH1, MutL homologue 1; IP,
immunoprecipitation. |
Discussion
Despite dramatic improvements in CRC diagnosis and
therapeutics in recent years, a significant proportion of patients
still experience recurrence and metastasis due to drug resistance,
which leads to the failure of chemotherapy (4,5,31). To
date, 5-FU remains a commonly used chemotherapeutic drug in cancer
treatment and clinical studies (32). Despite extensive research in recent
years, drug resistance remains a critical limitation to the
clinical application of 5-FU and related chemotherapeutic drugs.
Unfortunately, there few reliable markers available to accurately
predict chemosensitivity in CRC.
Studies on CMA have indicated that the degradation
of intracellular components by the lysosome can be selective
(6). CMA activity is markedly
upregulated in most cancer cell lines and the expression levels of
CMA components, mainly LAMP2A, are elevated in a number of human
tumors (9,33,34).
CMA can degrade anti-proliferative proteins (such as Rho family
GTPase 3) (12), tumor suppressor
proteins (such as phosphoprotein enriched in diabetes) (35), mutant p53 (36) and pro-apoptotic proteins such as
Bcl-2 binding component 3 (37) to
maintain tumor growth. It also can indirectly promote the
production of survivin for the stabilization of myeloid cell
leukemia-1 (38). CMA is also
involved in the mechanism of CRC chemotherapy resistance. A
previous study confirmed that 5-FU undergoes extensive
deacetylation in a variety of CRC cell lines (11). It reduces the ability of histone
acetyltransferase p300 and CBP to bind to chromatin and induces
lysosomal degradation. The lysosomal degradation is achieved
through CMA and inhibition of the degradation of p300 and CBP can
enhance the effects of 5-FU and reverse drug resistance (11). This suggests that the efficacy of
chemotherapy can be increased with anti-CMA therapy administered at
the same time as 5-FU chemotherapy.
The present study constructed and analyzed two
5-FU-resistant cell lines from HCT-116 and DLD-1 cell lines,
providing a tool to investigate the molecular pathways and detailed
mechanisms that are associated with drug resistance in CRC. In the
engineered 5-FU-resistant CRC cell lines, significant elevation of
LAMP2A was identified; this was responsible for loss of function of
LAMP2A in 5-FU-resistant CRC cells or gain of function in deficient
cells, which rendered them sensitive or resistant to 5-FU,
respectively.
Concurrently, a positive association was identified
between LAMP2A and PLD2. PLD2 is one of the two isoforms of PLD in
mammals, which catalyzes the hydrolysis of the diester bond of
phospholipids to generate PA and the free lipid headgroup (39). PLD2 expression is elevated in a
number of human tumors and is highly variable (16,19–22).
In CRC, the expression level of PLD2 was significantly associated
with tumor size and survival of patients, which suggests that PLD2
may be a target for therapy in CRC (40).
The present study verified whether PLD2 variation
exists along with LAMP2A through activation of the NF-κB pathway.
PDTC was used to block the NF-κB pathway and resulted in decreased
PLD2 levels. The relation between PLD2 and NF-κB was demonstrated
by co-immunoprecipitation. PDTC, a metal chelator and antioxidant,
can inhibit the activation of the NF-κB pathway specifically by
suppressing the release of the inhibitory subunit, IκB (41). Cuervo et al (42) identified that IκB can be degraded by
CMA during starvation. The present study found that the decrease of
IκB in the cytoplasm was associated with an increase of LAMP2A
levels. Co-immunoprecipitation experiments further confirmed the
interaction of IκB with Hsc70. IkB was identified as a substrate of
CMA. Therefore, when CMA was high in 5-FU-resistant CRC cell lines,
the IκB level in cytoplasm decreased, resulting in increased NF-κB
activity. Thereafter, the combination forms of PLD2 and NF-κB
increased, which facilitated the grown of CRC cells.
CQ was used to inhibit the lysosomal pathway and it
was observed that the levels of PLD2 declined early on and then
increased. This might because IκB degraded though two pathways; CMA
and proteasome (42). When lysosome
pathway was blocked, the proteasome pathway was activated in
compensation later. PLD contributes to signaling pools of PA and is
under tight regulation by elaborate mechanisms and so may increase
reactivity in cells (15). In
addition, the present study found the interaction of NF-κB with
some drug resistance genes, such as CD147, GST3 and MLH1, through
co-immunoprecipitation. This may be another important piece of
evidence that the NF-κB pathway is associated with drug resistance
in CRC.
A significant elevation of LAMP2A was found in CRC
cell lines and the increase was even higher in HCT116-R/DLD-1-R
cells. The high expression of LAMP2A promoted proliferation,
invasion and anti-apoptotic function of CRC cells.
In conclusion, upregulated LAMP2A expression might
serve a role in tumorigenesis and growth and may be involved in
drug resistance in CRC. It is a potential biomarker that indicates
the aggressiveness of CRCs and, thus, may be a therapeutic
target.
Acknowledgements
Not applicable.
Funding
The present study was supported by Liaoning
BaiQianWan Talents Program, Award for Liaoning Distinguished
Professor, a Key Scientific and Technological Project of Liaoning
Province (grant no. 2015408001) and National Natural Scientific
Foundation of China (grant nos. 81472544 and 81672700).
Availability of data and materials
The datasets used and/or analyzed are available from
the corresponding author on reasonable request.
Authors' contributions
YX, SZ, XX and LX performed the experiments. YX
analyzed the data and contributed to the manuscript writing. YX and
HCZ designed the experiments and contributed to data analysis. YX
and HCZ were responsible for confirming the authenticity of the
data. All authors read and approved the final manuscript and agree
to be accountable for all aspects of the research in ensuring that
the accuracy or integrity of any part of the work are appropriately
investigated and resolved.
Ethics approval and consent to
participate
Not applicable.
Patient consent for publication
Not applicable.
Competing interests
The authors declare that they have no competing
interests.
Glossary
Abbreviations
Abbreviations:
|
CMA
|
chaperone-mediated autophagy
|
|
CRC
|
colorectal cancer
|
|
5-FU
|
5-fluorouracil
|
|
CQ
|
clioquinol
|
|
PDTC
|
pyrrolidine dithiocarbamate
|
|
OXA
|
oxaliplatin
|
|
DMSO
|
dimethyl sulfoxide
|
|
shRNA
|
short hairpin RNA
|
References
|
1
|
Siegel RL, Miller KD, Goding Sauer A,
Fedewa SA, Butterly LF, Cercek A, Smith RA and Jemal A: Colorectal
cancer statistics, 2020. CA Cancer J Clin. 70:145–164. 2020.
View Article : Google Scholar : PubMed/NCBI
|
|
2
|
Takayama T, Miyanishi K, Hayashi T, Sato Y
and Niitsu Y: Colorectal cancer: Genetics of development and
metastasis. J Gastroenterol. 41:185–192. 2006. View Article : Google Scholar : PubMed/NCBI
|
|
3
|
De Angelis R, Sant M, Coleman MP,
Francisci S, Baili P, Pierannunzio D, Trama A, Visser O, Brenner H,
Ardanaz E, et al: Cancer survival in Europe 1999–2007 by country
and age: Results of EUROCARE-5 - a population-based study. Lancet
Oncol. 15:23–34. 2014. View Article : Google Scholar : PubMed/NCBI
|
|
4
|
Peng SL, Thomas M, Ruszkiewicz A, Hunter
A, Lawrence M and Moore J: Conventional adverse features do not
predict response to adjuvant chemotherapy in stage II colon cancer.
ANZ J Surg. 84:837–841. 2014. View Article : Google Scholar : PubMed/NCBI
|
|
5
|
Prados J, Melguizo C, Ortiz R, Perazzoli
G, Cabeza L, Alvarez PJ, Rodriguez-Serrano F and Aranega A: Colon
cancer therapy: Recent developments in nanomedicine to improve the
efficacy of conventional chemotherapeutic drugs. Anticancer Agents
Med Chem. 13:1204–1216. 2013. View Article : Google Scholar : PubMed/NCBI
|
|
6
|
Kaushik S and Cuervo AM:
Chaperone-mediated autophagy: A unique way to enter the lysosome
world. Trends Cell Biol. 22:407–417. 2012. View Article : Google Scholar : PubMed/NCBI
|
|
7
|
Catarino S, Pereira P and Girão H:
Molecular control of chaperone-mediated autophagy. Essays Biochem.
61:663–674. 2017. View Article : Google Scholar : PubMed/NCBI
|
|
8
|
Kaushik S and Cuervo AM: The coming of age
of chaperone- mediated autophagy. Nat Rev Mol Cell Biol.
19:365–381. 2018. View Article : Google Scholar : PubMed/NCBI
|
|
9
|
Saha T: LAMP2A overexpression in breast
tumors promotes cancer cell survival via chaperone-mediated
autophagy. Autophagy. 8:1643–1656. 2012. View Article : Google Scholar : PubMed/NCBI
|
|
10
|
Zhang Y, Xu YY, Yao CB, Li JT, Zhao XN,
Yang HB, Zhang M, Yin M, Chen J and Lei QY: Acetylation targets
HSD17B4 for degradation via the CMA pathway in response to estrone.
Autophagy. 13:538–553. 2017. View Article : Google Scholar : PubMed/NCBI
|
|
11
|
Du C, Huang D, Peng Y, Yao Y, Zhao Y, Yang
Y, Wang H, Cao L, Zhu WG and Gu J: 5-Fluorouracil targets histone
acetyltransferases p300/CBP in the treatment of colorectal cancer.
Cancer Lett. 400:183–193. 2017. View Article : Google Scholar : PubMed/NCBI
|
|
12
|
Zhou J, Yang J, Fan X, Hu S, Zhou F, Dong
J, Zhang S, Shang Y, Jiang X, Guo H, et al: Chaperone-mediated
autophagy regulates proliferation by targeting RND3 in gastric
cancer. Autophagy. 12:515–528. 2016. View Article : Google Scholar : PubMed/NCBI
|
|
13
|
Ding ZB, Fu XT, Shi YH, Zhou J, Peng YF,
Liu WR, Shi GM, Gao Q, Wang XY, Song K, et al: Lamp2a is required
for tumor growth and promotes tumor recurrence of hepatocellular
carcinoma. Int J Oncol. 49:2367–2376. 2016. View Article : Google Scholar : PubMed/NCBI
|
|
14
|
Dubois A, Furstoss N, Calleja A, erhouni
M, Cluzeau T, Savy C, Marchetti S, Hamouda MA, Boulakirba S, Orange
F, et al: LAMP2 expression dictates azacytidine response and
prognosis in MDS/AML. Leukemia. 33:1501–1513. 2019. View Article : Google Scholar : PubMed/NCBI
|
|
15
|
Selvy PE, Lavieri RR, Lindsley CW and
Brown HA: Phospholipase D: Enzymology, functionality and chemical
modulation. Chem Rev. 111:6064–6119. 2011. View Article : Google Scholar : PubMed/NCBI
|
|
16
|
Foster DA and Xu L: Phospholipase D in
cell proliferation and cancer. Mol Cancer Res. 1:789–800.
2003.PubMed/NCBI
|
|
17
|
Hammond SM, Altshuller YM, Sung TC, Rudge
SA, Rose K, Engebrecht J, Morris AJ and Frohman MA: Human ADP
ribosylation factor-activated phosphatidylcholine-specific
phospholipase D defines a new and highly conserved gene family. J
Biol Chem. 270:29640–29643. 1995. View Article : Google Scholar : PubMed/NCBI
|
|
18
|
Colley WC, Sung TC, Roll R, Jenco J,
Hammond SM, Altshuller Y, Bar-Sagi D, Morris AJ and Frohman MA:
Phospholipase D2, a distinct phospholipase D isoform with novel
regulatory properties that provokes cytoskeletal reorganization.
Curr Biol. 7:191–201. 1997. View Article : Google Scholar : PubMed/NCBI
|
|
19
|
Henkels KM, Boivin GP, Dudley ES,
Berberich SJ and Gomez-Cambronero J: Phospholipase D (PLD) drives
cell invasion, tumorgrowth and metastasis in a human breast cancer
xenograph model. Oncogene. 32:5551–5562. 2013. View Article : Google Scholar : PubMed/NCBI
|
|
20
|
Uchida N, Okamura S and Kuwano H:
Phospholipase D activity in human gastric carcinoma. Anticancer
Res. 19:671–675. 1999.PubMed/NCBI
|
|
21
|
Diaz-Aragon R, Ramirez-Ricardo J,
Cortes-Reynosa P, Simoni-Nieves A, Gomez-Quiroz LE and Perez
Salazar E: Role of phospholipase D in migration and invasion
induced by linoleic acid in breast cancer cells. Mol Cell Biochem.
457:119–132. 2019. View Article : Google Scholar : PubMed/NCBI
|
|
22
|
Liu M, Du K, Jiang B and Wu X: High
expression of phospholipaseD2 induced by hypoxia promotes
proliferation of colon cancer cells through activating NF-κ Bp65
signaling pathway. Pathol Oncol Res. 26:281–290. 2018. View Article : Google Scholar : PubMed/NCBI
|
|
23
|
Fiucci G, Czarny M, Lavie Y, Zhao D, Berse
B, Blusztajn JK and Liscovitch M: Changes in phospholipaseD isoform
activity and expression in multidrug-resistant human cancer cells.
Int J Cancer. 85:882–888. 2000. View Article : Google Scholar : PubMed/NCBI
|
|
24
|
Livak KJ and Schmittgen TD: Analysis of
relative gene expression data using real-time quantitative PCR and
the 2(-Delta Delta C(T)) method. Methods. 25:402–408. 2001.
View Article : Google Scholar : PubMed/NCBI
|
|
25
|
Kuang YH, Chen X, Su J, Wu LS, Liao LQ, Li
D, Chen ZS and Kanekura T: RNA interference targeting the CD147
induces apoptosis of multi-drug resistant cancer cells related to
XIAP depletion. Cancer Lett. 276:189–195. 2009. View Article : Google Scholar : PubMed/NCBI
|
|
26
|
Nakayama K, Kanzaki A, Ogawa K, Miyazaki
K, Neamati N and Takebayashi Y: Copper-transporting P-type
adenosine triphosphatase (ATP7B) as a cisplatin based
chemoresistance marker in ovarian carcinoma: Comparative analysis
with expression of MDR1, MRP1, MRP2, LRP and BCRP. Int J Cancer.
101:488–495. 2002. View Article : Google Scholar : PubMed/NCBI
|
|
27
|
Ściskalska M and Milnerowicz H: The role
of GSTπ isoform in the cells signalling and anticancer therapy. Eur
Rev Med Pharmacol Sci. 24:8537–8550. 2020.PubMed/NCBI
|
|
28
|
He J, He J, Min L, He Y, Guan H, Wang J
and Peng X: Extracellular vesicles transmitted miR-31-5p promotes
sorafenib resistance by targeting MLH1 in renal cell carcinoma. Int
J Cancer. 146:1052–1063. 2020. View Article : Google Scholar : PubMed/NCBI
|
|
29
|
Germano G, Lamba S, Rospo G, Barault L,
Magrì A, Maione F, Russo M, Crisafulli G, Bartolini A, Lerda G, et
al: Inactivation of DNA repair triggers neoantigen generation and
impairs tumour growth. Nature. 552:116–120. 2017. View Article : Google Scholar : PubMed/NCBI
|
|
30
|
Xiao G, Li Y, Wang M, Li X, Qin S, Sun X,
Liang R, Zhang B, Du N, Xu C, et al: FBXW7 suppresses
epithelial-mesenchymal transition and chemo-resistance of
non-small-cell lung cancer cells by targeting snai1 for
ubiquitin-dependent degradation. Prolif. 51:e124732018. View Article : Google Scholar
|
|
31
|
Rezasoltani S, Asadzadeh-Aghdaei H,
Nazemalhosseini-Mojarad E, Dabiri H, Ghanbari R and Zali MR: Gut
microbiota, epigenetic modification and colorectal cancer. Iran J
Microbiol. 9:55–63. 2017.PubMed/NCBI
|
|
32
|
Skarkova V, Kralova V, Vitovcova B and
Rudolf E: Selected aspects of chemoresistance mechanisms in
colorectal carcinoma-A focus on epithelial-to-mesenchymal
transition, autophagy, and apoptosis. Cells. 8:2342019. View Article : Google Scholar
|
|
33
|
Kon M, Kiffin R, Koga H, Chapochnick J,
Macian F, Varticovski L and Cuervo AM: Chaperone-mediated autophagy
is required for tumor growth. Sci Transl Med. 3:109ra1172011.
View Article : Google Scholar : PubMed/NCBI
|
|
34
|
Li L, Fang R, Liu B, Shi H, Wang Y, Zhang
W, Zhang X and Ye L: Deacetylation of tumor-suppressor MST1 in
Hippo pathway induces its degradation through HBXIP-elevated HDAC6
in promotion of breast cancer growth. Oncogene. 35:4048–4057. 2016.
View Article : Google Scholar : PubMed/NCBI
|
|
35
|
Quintavalle C, Di Costanzo S, Zanca C,
Tasset I, Fraldi A, Incoronato M, Mirabelli P, Monti M, Ballabio A,
Pucci P, et al: Phosphorylation-regulated degradation of the
tumor-suppressor form of PED by chaperone-mediated autophagy in
lung cancer cells. J Cell. Physiol. 229:1359–1368. 2014.
|
|
36
|
Vakifahmetoglu-Norberg H, Kim M, Xia HG,
Iwanicki MP, Ofengeim D, Coloff JL, Pan L, Ince TA, Kroemer G,
Brugge JS and Yuan J: Chaperone-mediated autophagy degrades mutant
p53. Genes Dev. 27:1718–1730. 2013. View Article : Google Scholar : PubMed/NCBI
|
|
37
|
Xie W, Zhang L, Jiao H, Guan L, Zha J, Li
X, Wu M, Wang Z, Han J and You H: Chaperone-mediated autophagy
prevents apoptosis by degrading BBC3/PUMA. Autophagy. 11:1623–1635.
2015. View Article : Google Scholar : PubMed/NCBI
|
|
38
|
Suzuki J, Nakajima W, Suzuki H, Asano Y
and Tanaka N: Chaperone-mediated autophagy promotes lung cancer
cell survival through selective stabilization of the pro-survival
protein, MCL1. Biochem Biophys Res Commun. 482:1334–1340. 2017.
View Article : Google Scholar : PubMed/NCBI
|
|
39
|
Yao Y, Wang X, Li H, Fan J, Qian X, Li H
and Xu Y: Phospholipase D as a key modulator of cancer progression.
Biol Rev Camb Philos Soc. 95:911–935. 2018. View Article : Google Scholar
|
|
40
|
Saito M, Iwadate M, Higashimoto M, Ono K,
Takebayashi Y and Takenoshita S: Expression of phospholipase D2 in
human colorectal carcinoma. Oncol. Rep. 18:1329–1334. 2017.
|
|
41
|
Li H, Sun Y, Liang J, Fan Y and Zhang XD:
pH-Sensitive pullulan-DOX conjugate nanoparticles for co-loading
PDTC to suppress growth and chemoresistance of hepatocellular
carcinoma. J Mater Chem B. 3:8070–8078. 2015. View Article : Google Scholar : PubMed/NCBI
|
|
42
|
Cuervo AM, Hu W, Lim B and Dice JF:
IkappaB is a substrate for a selective pathway of lysosomal
proteolysis. Mol Biol Cell. 9:1995–2010. 1998. View Article : Google Scholar : PubMed/NCBI
|