Introduction
Cluster of differentiation 146 (CD146) is a cell
adhesion molecule (CAM) which belongs to the immunoglobulin
superfamily (IgSF) (1). Human CD146
has previously been designated several synonyms, including MUC18
(1,2), A32 antigen (3,4),
S-Endo-1 (5), melanoma CAM (MCAM or
Mel-CAM) (4,6,7),
metastasis CAM (MET-CAM) (8) and
hemopoietic CAM (HEMCAM) (9). The
avian homolog of CD146 has been named gicerin (10). CD146 was originally identified as a
marker for melanoma (MCAM), due to its overexpression in metastatic
lesions and advanced primary tumors, yet not in benign lesions
(1,3,4).
Increasing amounts of evidence have demonstrated that CD146 is
overexpressed in a variety of carcinomas, in addition to melanomas
(11–14). As a result of this characteristic,
CD146 has attracted attention and is considered to be a potential
marker for tumor diagnosis, prognosis and treatment. The majority
of studies support the theory that CD146 promotes tumor growth,
angiogenesis and metastasis (15),
therefore, CD146 is a promising target for tumor therapy (16,17).
CD146 is a 113-kDa integral membrane glycoprotein,
whose sequence of amino acids consists of a signal peptide, an
extracellular fragment structure of five immunoglobulin-like
domains (V-V-C2-C2-C2), a transmembrane region and a short
cytoplasmic tail (2,18). The Protein and Peptide
Pharmaceutical Laboratory, Chinese Academy of Sciences-University
of Tokyo, Tokyo, raised an array of mouse antibodies (mAbs) against
CD146, among which AA4 recognizes the epitope located at the second
IgC2 domain (19). AA4 is able to
specifically detect CD146 in tumor specimens from various organs,
including breast tumors (14).
CD146 overexpression has been revealed in ovarian cancer and may be
a marker for poor prognosis in ovarian cancer patients (11). Thus, CD146 Abs may be a useful
marker in the detection of gynecological malignancies. However,
CD146 expression and detection in two other types of gynecological
cancer, cervical and endometrial cancer, has not been
investigated.
This study aimed to evaluate the distribution of
CD146 in cervical and endometrial cancer; the diagnostic use of
CD146 Abs in cervical and endometrial cancer was evaluated by
calculating the correlation between clinical pathological
parameters and the extent of immunohistochemical CD146 expression
in tumor tissues.
Materials and methods
Antibody and reagents
The anti-CD146 monoclonal antibody AA4 was generated
in the Protein and Peptide Pharmaceutical Laboratory (Chinese
Academy of Sciences-University of Tokyo Joint Laboratory of
Structural Virology and Immunology, Beijing, China). A
CD31-specific antibody was purchased from Abcam (Cambridge, MA,
USA). Biotin-conjugated secondary antibodies (goat anti-rabbit or
-mouse) and HRP-conjugated streptavidin were purchased from Dianova
(Rodeo, CA, USA). Goat anti-rabbit Alexa Fluor® 488 and
goat anti-mouse Alexa Fluor® 555 were purchased from
Invitrogen (San Diego, CA, USA). DAPI was purchased from Roche
(Indianapolis, IN, USA). Normal goat serum and a
3,3′-diaminobenzidine (DAB) staining kit were purchased from
ZSGB-BIO (China).
Ethics statement
Informed consent was obtained from all participants
in this study. All procedures have been approved by the Ethics
Committee of Capital Medical University Affiliated Beijing Anzhen
Hospital, Institute of Beijing Heart, Lung and Blood Vessel
Diseases and Institute of Biophysics, Chinese Academy of
Sciences.
Clinical sampling
Malignant specimens were obtained from patients with
gynecological cancer, including cervical carcinoma and endometrial
carcinoma, by surgical excision, in Anzhen Hospital (Beijing,
China) and the Fifth Affiliated Hospital of Zhengzhou University
(Zhengzhou, Henan, China). Normal uterine cervical tissue and
normal endometrium were collected by hysterectomy in non-cancer
patients with multiple uterine leiomyomas or adenomyosis,
respectively. None of the patients had received preoperative
chemotherapy, radiotherapy or hormone therapy or suffered with
malignant tumors, other than the gynecological cancer examined in
this investigation.
Immunohistochemistry
This assay was conducted according to classically
established methods (14). Briefly,
tissue sections were fixed with formalin and embedded with
paraffin. Tissue sections were then cut (5 μm) and stained with
hematoxylin and eosin (H&E) solution. Following
deparaffinization, tissue sections were stained with a CD146- or
CD31-specific antibody, then with biotin-conjugated secondary
antibodies (1:1000), followed by HRP-conjugated streptavidin
(Dianova). The sections were counterstained with hematoxylin to
visualize the nuclei.
Double-staining immunohistofluorescence
analysis
Sections (5 μm) were fixed in 4% paraformaldehyde
(pH 7.4) for 15 min at room temperature. Following the general
procedure, which included permeabilization and blocking, the slides
were co-incubated with antibodies for CD146 (mAb) and CD31 (rAb,
rabbit Ab) overnight at 4°C. After washing with PBS three times,
the slides were incubated with a mixture of the two secondary
antibodies (anti-rabbit Alexa Fluor® 488 and anti-mouse
Alexa Fluor® 555) in the dark for 1 h. The nuclei were
stained with DAPI. Fluorescent images were acquired using a
confocal microscope (FV1000, Olympus, Tokyo, Japan).
Statistical analysis
Statistical analysis was conducted using SPSS
software. The significant differences between the groups and the
association between CD146 expression and different
clinicopathological parameters were evaluated using the Chi-square
test or Fisher’s exact test. P<0.05 was considered to indicate a
statistically significant difference.
Results
Classification of cervical cancer
specimens into categories
The collected specimens were divided into normal
tissue and cancerous tissue groups. The mean age of the patients
with normal and cancerous uterine cervical tissue was 44.12±10.61
and 48.25±9.86 years, respectively. The cervical samples consisted
of 16 normal (control) and 256 malignant specimens (Table I). Cervical cancer is a malignant
neoplasm originating from cells in the cervix uteri and consists of
two histological subtypes. The majority of cervical cancer types
are squamous cell carcinomas, arising in the squamous epithelial
cells that line the cervix. Adenocarcinomas, arising in glandular
epithelial cells, are the second most common type of cervical
cancer (20). Cancer rarely occurs
in other types of cells in the cervix. In this study, 241 of the
cancer samples had the squamous carcinoma subtype and only 15
samples had the adenocarcinoma subtype. Cervical cancer tissue was
further classified into categories following the review of existing
patient medical records. With regard to the histological grade, 46
cases were grade 1 (G1), with a high differentiation phenotype, 154
tumors were moderately differentiated (grade 2, G2) and 56 tumors
had a poorly differentiated phenotype (grade 3, G3). According to
the International Federation of Gynecology and Obstetrics (FIGO)
systems, 226 patients were in the early stages (I–II) and 30
patients were in the advanced stages (III–IV) of the disease
(Table II).
 | Table IDistribution of CD146 in normal and
cancerous tissues from the cervix and endometrium. |
Table I
Distribution of CD146 in normal and
cancerous tissues from the cervix and endometrium.
| Variable |
CD146+ |
CD146− | Total | χ2 | P-value | PPV | NPV | Sensitivity | Specificity |
|---|
| Cervical samples | | | | 11.900 | <0.01 | 100 | 10.00 | 43.75 | 100 |
| Cancer | 112a | 144b | 256 | | | | | | |
| Normal | 0c | 16d | 16 | | | | | | |
| Endometrial
samples | | | | 5.345 | <0.05 | 89.39 | 28.21 | 67.81 | 61.11 |
| Cancer | 59a | 28b | 87 | | | | | | |
| Normal | 7c | 11d | 18 | | | | | | |
 | Table IICorrelation of CD146 expression with
clinicopathological parameters in cervical carcinoma. |
Table II
Correlation of CD146 expression with
clinicopathological parameters in cervical carcinoma.
| Variable | CD146
| Total | χ2 | P-value | Correlation
coefficient |
|---|
| Positive, n
(%) | Negative, n
(%) |
|---|
| Age (years) | | | | 2.435 | 0.119 | –0.098 |
| <48 | 52 (39) | 81 (61) | 133 | | | |
| ≥48 | 60 (49) | 63 (51) | 123 | | | |
| Histological
grade | | | | 1.830 | 0.401 | 0.080 |
| G1 | 24 (52) | 22 (48) | 46 | | | |
| G2 | 66 (43) | 88 (57) | 154 | | | |
| G3 | 22 (39) | 34 (61) | 56 | | | |
| FIGO stage | | | | 0.002 | 0.961 | 0.003 |
| I–II | 99 (44) | 127 (56) | 226 | | | |
| III–IV | 13 (43) | 17 (57) | 30 | | | |
| Histological tumor
type | | | | 12.393a | <0.001 | 0.220 |
|
Squamouscarcinoma | 112 (46) | 129 (54) | 241 | | | |
|
Adenocarcinoma | 0 (0) | 15 (100) | 15 | | | |
Classification of endometrial cancer
specimens into categories
The mean age of the patients with normal and
cancerous endometrial tissue were 33.12±10.56 and 54.69±9.43 years,
respectively. Endometrial samples consisted of 18 normal (control)
and 87 malignant specimens (Table
I). The majority of endometrial cancer types are
adenocarcinomas, originating from epithelial cells that line the
endometrium and form the endometrial glands. There are numerous
microscopic subtypes of endometrial carcinomas, including the
common endometrioid type, the more aggressive papillary serous
carcinoma and clear cell endometrial carcinomas (21). Eighty samples were endometrioid
adenocarcinomas (EECs) and 7 samples were non-endometrioid
adenocarcinomas (NEECs), which included 5 squamous endometrial
carcinomas, 1 papillary serous endometrial carcinoma and 1
adeno-squamous endometrial carcinoma. FIGO grading showed that 30
samples were well-differentiated (G1) and 57 samples had moderate
(G2) or no (G3) differentiation (Table
III).
 | Table IIICorrelation of CD146 expression with
clinicopathological parameters in endometrial carcinoma. |
Table III
Correlation of CD146 expression with
clinicopathological parameters in endometrial carcinoma.
| Variable | CD146
| Total | χ2 | P-value | Correlation
coefficient |
|---|
| Positive, n
(%) | Negative, n
(%) |
|---|
| Age (years) | | | | 0.284 | 0.594 | 0.057 |
| <55 | 31 (71) | 13 (30) | 44 | | | |
| ≥55 | 28 (65) | 15 (35) | 43 | | | |
| Histological
grade | | | | 4.400a | <0.05 | –0.225 |
| G1 | 16 (53) | 14 (47) | 30 | | | |
| G2–G3 | 43 (75) | 14 (25) | 57 | | | |
| FIGO stage | | | | 0.202 | 0.653 | –0.048 |
| I–II | 46 (67) | 23 (33) | 69 | | | |
| III–IV | 13 (72) | 5 (28) | 18 | | | |
| Depth of myometrial
infiltration | | | | 5.036a | <0.05 | –0.241 |
| 0 or <0.5 | 27 (57) | 20 (43) | 47 | | | |
| >0.5 | 32 (80) | 8 (20) | 40 | | | |
| Histological tumor
type | | | | 1.117 | 0.290 | –0.113 |
| Endometrioid
adenocarcinoma | 53 (66) | 27 (34) | 80 | | | |
| Non-endometrioid
adenocarcinoma | 6 (86) | 1 (14) | 7 | | | |
CD146 is highly expressed in cervical and
endometrial cancer
To investigate the expression of CD146 in cervical
and endometrial cancer, we conducted immunohistochemical assays
with AA4 mAb on all the collected specimens, which consisted of 377
samples of normal and cancerous tissue. As summarized in Table I, CD146 was detected in a large
number of cancer samples. The number of true positives (Table I) in cervical and endometrial cancer
was 112 and 59, respectively. The number of false negatives
(Table I) in the cancerous cervical
and endometrial tissue was 144 and 28, respectively. By contrast,
CD146 was only detected in a limited number of normal samples. The
number of false positives (Table I)
in normal cervical and endometrial tissue was 0 and 7,
respectively. The number of true negatives (Table I) in normal cervical and endometrial
tissue was 16 and 11, respectively. Using the equation described in
the legend of Table I, the positive
predictive value (PPV), negative predictive value (NPV),
sensitivity and specificity of CD146 expression for cervical cancer
detection were calculated as 100 (112/112), 10.00 (16/160), 43.75
(112/256) and 100% (16/16), respectively. For the detection of
endometrial cancer based on CD146 expression, PPV, NPV, sensitivity
and specificity were 89.4 (59/66), 28.2 (11/39), 67.8 (59/87) and
61.1% (11/18), respectively.
CD146 expression levels are positively
correlated with the histological subtypes of cervical cancer
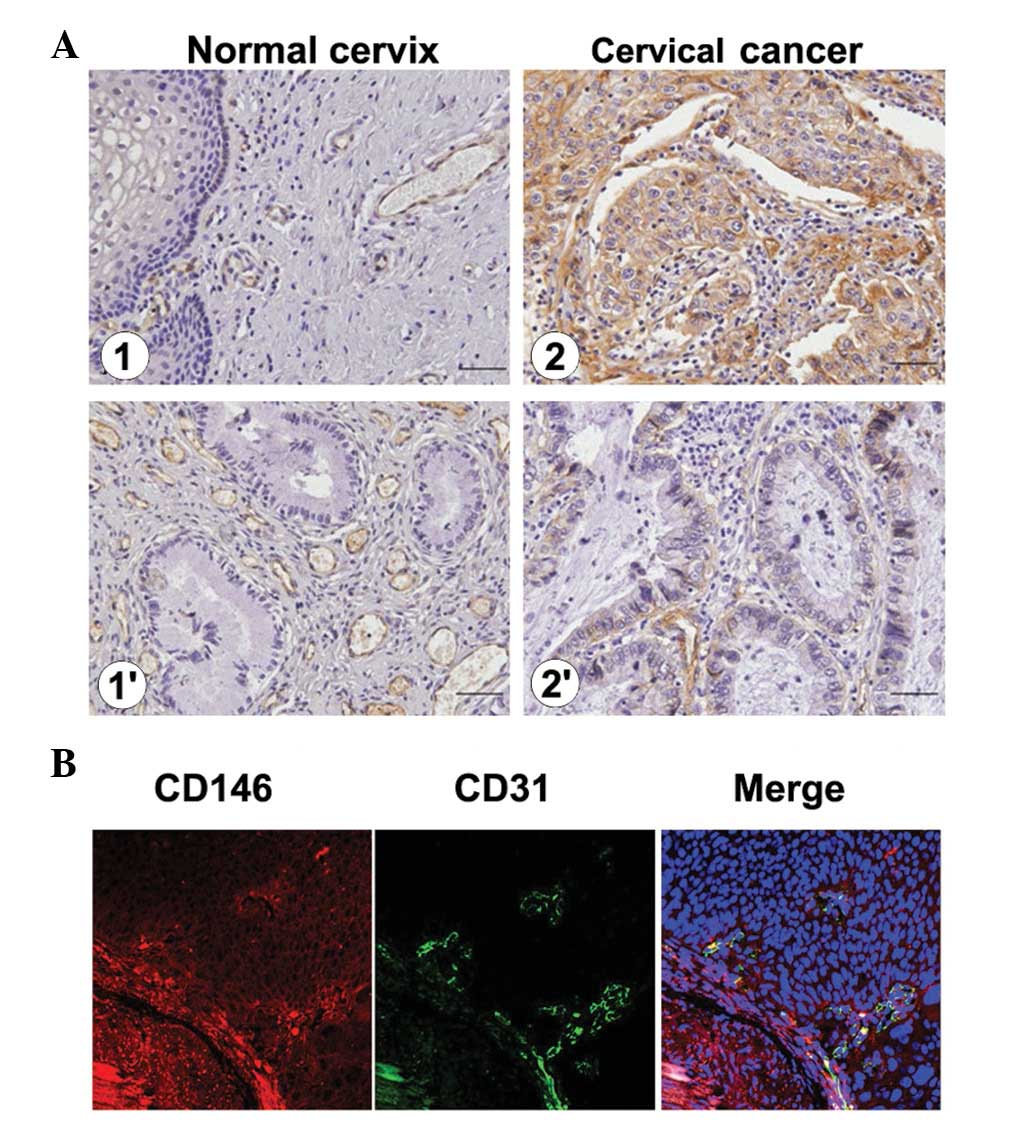
Immunohistochemical assays showed that CD146
expression did not occur in normal cervical squamous epithelium and
mucosal glands. In cervical carcinomas, CD146 was detected mainly
in the membranes and cytoplasm of squamous tumor and vascular
endothelial cells (Fig. 1A). This
was consistent with the localization data from fluorescent
immunohistochemistical assays, as shown in Fig. 1B, in which the tumor cells with
CD146+ expression were labeled with CD146 mAb AA4 and
the vascular endothelial cells with CD146+ expression
were confirmed with an endothelial marker for CD31. The overlapping
yellow regions are indicative of the co-localization of CD31 and
CD146 in vascular cells. These data demonstrated that CD146 was
localized in tumor cells and vascular endothelial cells in cervical
carcinomas.
For patients who were <48 years old, 39% (52/133)
of samples had CD146+ staining, whereas, for patients
who were ≥48 years old, a higher number of cases were
CD146+ and had a staining rate of 49% (60/123). There
was no significant difference between the cervical cancer and
normal cervical samples in the two parameters of clinical FIGO
stage (I–II and III–IV stages) and histological grade (G1–G3). By
contrast, as shown in Table II, the
AA4+ reaction rate is significantly higher in squamous
cervical carcinoma (112/241, 46.5%) than in cervical adenocarcinoma
(0/15, 0%). This indicates that CD146 presence was a potential
predictive marker (P=0.000) for discrimination of the two
histological subtypes of cervical carcinoma, namely that a cervical
carcinoma with higher CD146 expression levels was more likely to be
the squamous carcinoma subtype than the adenocarcinoma subtype.
CD146 expression levels are positively
correlated with histological grade and the depth of the myometrial
invasion in endometrial cancer
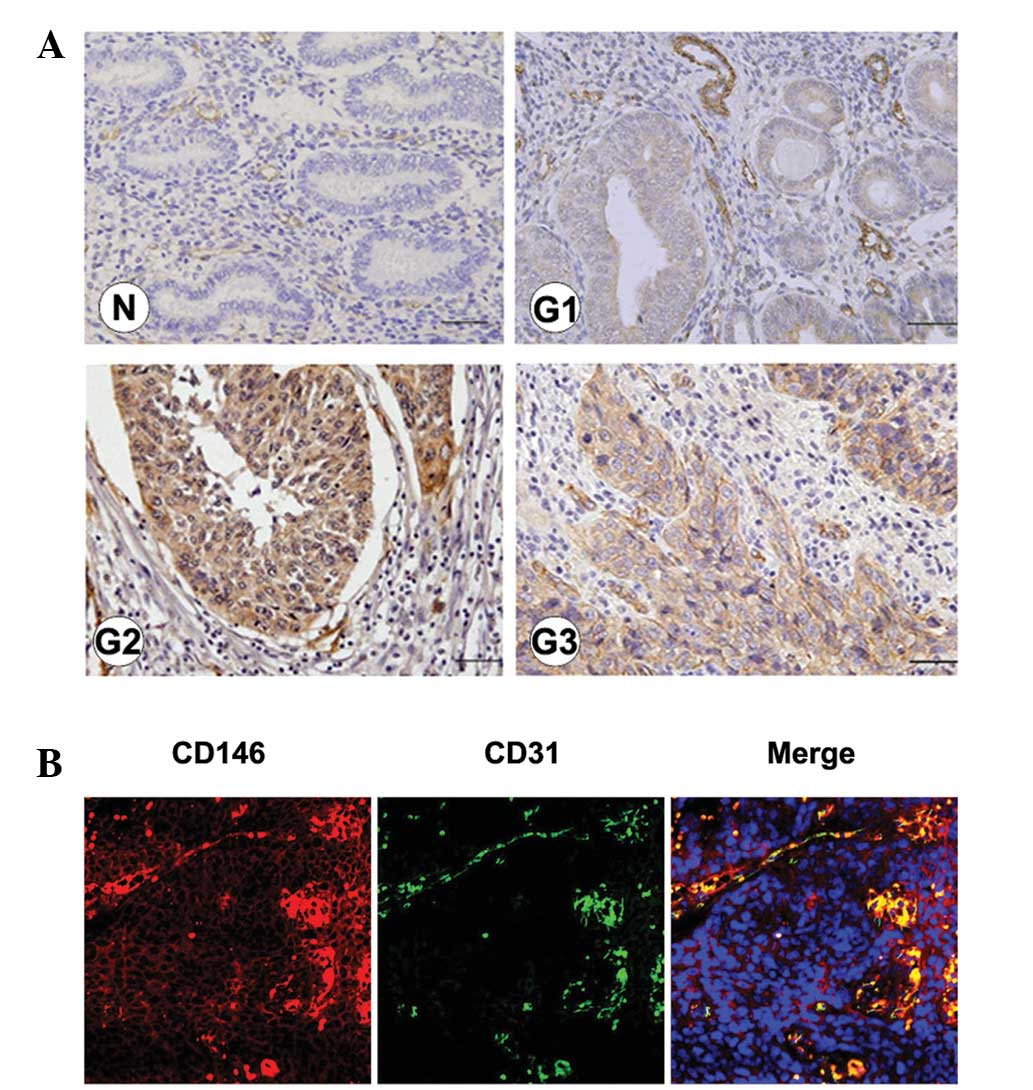
In normal endometrium samples, CD146 was detected in
vascular endothelial cells and also in glands during the
hyperplasia period. In endometrial cancer samples, CD146 was
detected in the majority of tumor cells, in addition to vascular
endothelial cells (Fig. 2A). The
CD146 localization in vascular endothelial cells was further
confirmed using fluorescent immunohistochemistry. Similar to the
results in Fig. 1B, the
co-localization of CD31 and CD146 in the endothelial cells of tumor
blood vessels was observed in endometrial cancer (Fig. 2B).
Immunohistochemistry results showed that no
statistically significant differences in CD146 expression existed
between the two groups for endometrial cancer samples from patients
<55 years old (70%) or ≥55 years old (65%). Furthermore, no
significant difference in CD146+ expression was
identified between cancer samples with different FIGO stages (P=
0.653). CD146+ staining occured in 67% (46/69) of cases
in cancer samples with an early clinical stage (I–II phase),
compared with 72% (13/18) in cancer samples with an advanced
clinical stage (III–IV phase). For the histological subtypes of
endometrial cancer, CD146 expression was detected in EEC and NEEC
in 66% (53/80) and 86% (6/7) of samples, respectively, indicating
that there is no significant difference in CD146 expression between
the two subtypes of endometrial cancer (P=0.290).
By contrast, CD146+ samples showed
significant differences in the histological grade and the depth of
myometrial infiltration parameters. CD146+ cases
occured at a significantly higher rate (P= 0.036) in poorly
differentiated histological grades (G2–G3) of endometrial cancer
(43/57, 75%) than in the highly differentiated grade (G1) of
endometrial cancer (16/30, 53%). Similarly, the depth of myometrial
infiltration indicated that CD146+ samples were
significantly more frequent in the lesions with deep (>0.5)
myometrial infiltration (32/40, 80%), compared with the lesions
without or with shallow (0 or <0.5) myometrial infiltration
(27/47, 57%), as evaluated by statistical analysis (P=0.025).
Discussion
In this study, we demonstrated that the specificity,
sensitivity and PPV of AA4 (a mAb for CD146) is suitable for use in
the detection of cervical cancer and endometrial cancer. Results
showed that CD146 expression levels were higher in cervical and
endometrial cancer tissues compared with their corresponding normal
tissues. Notably, CD146 expression was positively and significantly
correlated with various subtypes of cervical cancer, as higher
expression levels were detected in the squamous carcinoma subtype
than in the adenocarcinoma subtype (Table II). The significant correlation
which was identified between CD146 expression and the histological
classification or the depth of myometrial invasion indicates that
CD146 may be involved in the onset and development of endometrial
cancer (Table III). This hypothesis
was further strengthened by an immunohistofluorescent assay, where
the broad expression of CD146 in the cellular membrane of malignant
cancer was confirmed. Furthermore, in accordance with previous
studies (22,23), immunohistofluorescence data in this
study showed that CD146 was present in the majority of cancer blood
vessels (Figs. 1 and 2), suggesting that CD146 may be actively
implicated in the dissemination and metastasis of cervical cancer
and endometrial cancer via the vascular system.
Gynecological malignant cancer, including cervical
cancer, endometrial carcinoma and ovarian cancer, is
life-threatening to females (24).
The incidence of cervical cancer is higher than endometrial and
ovarian cancer (20) and the
mortality rate of ovarian cancer is the highest among these three
types of cancer (25). Therefore,
effective screening methods and potential therapeutic targets have
been pursued in this field. At present, the clinically used
biomarkers for detection of gynecological malignancies principally
include squamous cell carcinoma antigen (SCC), carcinoembryonic
antigen (CEA) and sugar antigens CA125, CA199 and CA153 (26–29).
However, the sensitivity and specificity are not
satisfactory for the accuracy of predictive detection for
gynecological malignancies (26).
Therefore, seeking more reliable biomarkers is likely to aid the
successful detection of tumors in the early stages of the disease
and also for determining an effective therapeutic approach. Our
findings of CD146 overexpression in cervical and endometrial
cancer, plus the ability of AA4 to detect CD146 with high
sensitivity and specificity, provides insight for further
development of CD146 mAbs in the detection of malignant
gynecological cancer. It also implies that a combined treatment
strategy of anti-CD146 immunotherapy with other traditional chemo-
or radiotherapy treatments may be a promising anticancer
technique.
Abbreviations:
|
CD146
|
cluster of differentiation 146
|
|
mAb
|
mouse antibody
|
|
CAM
|
cell adhesion molecule
|
|
MET-CAM
|
metastasis CAM
|
|
HEMCAM
|
hemopoietic CAM
|
|
V set
|
variable region
|
|
C-2 set
|
constant region
|
|
IgSF
|
immunoglobulin superfamily
|
|
PPV
|
positive predictive value
|
|
NPV
|
negative predictive value
|
|
FIGO
|
International Federation of Gynecology
and Obstetrics systems
|
|
EECs
|
endometrioid adenocarcinomas
|
|
NEECs
|
non-endometrioid adenocarcinomas
|
Acknowledgements
This study was supported by grants
from The National Science and Technology Major Project
(2012ZX10002009-016) and The National Natural Science Foundation of
China (91029732/81272409).
References
|
1
|
Lehmann JM, Holzmann B, Breitbart EW,
Schmiegelow P, Riethmüller G and Johnson JP: Discrimination between
benign and malignant cells of melanocytic lineage by two novel
antigens, a glycoprotein with a molecular weight of 113,000 and a
protein with a molecular weight of 76,000. Cancer Res. 47:841–845.
1987.
|
|
2
|
Lehmann JM, Riethmüller G and Johnson JP:
MUC18, a marker of tumor progression in human melanoma, shows
sequence similarity to the neural cell adhesion molecules of the
immunoglobulin superfamily. Proc Natl Acad Sci USA. 86:9891–9895.
1989. View Article : Google Scholar
|
|
3
|
Shih IM, Elder DE, Speicher D, Johnson JP
and Herlyn M: Isolation and functional characterization of the A32
melanoma-associated antigen. Cancer Res. 54:2514–2520.
1994.PubMed/NCBI
|
|
4
|
Shih IM, Elder DE, Hsu MY and Herlyn M:
Regulation of Mel-CAM/MUC18 expression on melanocytes of different
stages of tumor progression by normal keratinocytes. Am J Pathol.
145:837–845. 1994.PubMed/NCBI
|
|
5
|
Bardin N, Francès V, Lesaule G,
Horschowski N, George F and Sampol J: Identification of the S-Endo
1 endothelial-associated antigen. Biochem Biophys Res Commun.
218:210–216. 1996. View Article : Google Scholar : PubMed/NCBI
|
|
6
|
Rummel MM, Sers C and Johnson JP: Phorbol
ester and cyclic AMP-mediated regulation of the melanoma-associated
cell adhesion molecule MUC18/MCAM. Cancer Res. 56:2218–2223.
1996.PubMed/NCBI
|
|
7
|
Xie S, Luca M, Huang S, et al: Expression
of MCAM/MUC18 by human melanoma cells leads to increased tumor
growth and metastasis. Cancer Res. 57:2295–2303. 1997.PubMed/NCBI
|
|
8
|
Wu GJ, Wu MW, Wang C and Liu Y: Enforced
expression of METCAM/MUC18 increases tumorigenesis of human
prostate cancer LNCaP cells in nude mice. J Urol. 185:1504–1512.
2011. View Article : Google Scholar : PubMed/NCBI
|
|
9
|
Vainio O, Dunon D, Aïssi F, Dangy JP,
McNagny KM and Imhof BA: HEMCAM, an adhesion molecule expressed by
c-kit+ hemopoietic progenitors. J Cell Biol. 135:1655–1668.
1996.PubMed/NCBI
|
|
10
|
Taira E, Takaha N, Taniura H, Kim CH and
Miki N: Molecular cloning and functional expression of gicerin, a
novel cell adhesion molecule that binds to neurite outgrowth
factor. Neuron. 12:861–872. 1994. View Article : Google Scholar : PubMed/NCBI
|
|
11
|
Aldovini D, Demichelis F, Doglioni C, et
al: M-CAM expression as marker of poor prognosis in epithelial
ovarian cancer. Int J Cancer. 119:1920–1926. 2006. View Article : Google Scholar : PubMed/NCBI
|
|
12
|
Feng G, Fang F, Liu C, Zhang F, Huang H
and Pu C: CD146 gene expression in clear cell renal cell carcinoma:
a potential marker for prediction of early recurrence after
nephrectomy. Int Urol Nephrol. 44:1663–1669. 2012. View Article : Google Scholar : PubMed/NCBI
|
|
13
|
Liu WF, Ji SR, Sun JJ, et al: CD146
Expression Correlates with Epithelial-Mesenchymal Transition
Markers and a Poor Prognosis in Gastric Cancer. Int J Mol Sci.
13:6399–6406. 2012. View Article : Google Scholar : PubMed/NCBI
|
|
14
|
Zeng Q, Li W, Lu D, et al: CD146, an
epithelial-mesenchymal transition inducer, is associated with
triple-negative breast cancer. Proc Natl Acad Sci USA.
109:1127–1132. 2012. View Article : Google Scholar : PubMed/NCBI
|
|
15
|
Ouhtit A, Gaur RL, Abd Elmageed ZY, et al:
Towards understanding the mode of action of the multifaceted cell
adhesion receptor CD146. Biochim Biophys Acta. 1795:130–136.
2009.PubMed/NCBI
|
|
16
|
Bu P, Gao L, Zhuang J, Feng J, Yang D and
Yan X: Anti-CD146 monoclonal antibody AA98 inhibits angiogenesis
via suppression of nuclear factor-kappaB activation. Mol Cancer
Ther. 5:2872–2878. 2006. View Article : Google Scholar : PubMed/NCBI
|
|
17
|
Wellbrock J and Fiedler W: CD146: a new
partner for VEGFR2. Blood. 120:2164–2165. 2012. View Article : Google Scholar : PubMed/NCBI
|
|
18
|
Johnson JP, Rothbächer U and Sers C: The
progression associated antigen MUC18: a unique member of the
immunoglobulin supergene family. Melanoma Res. 3:337–340. 1993.
View Article : Google Scholar : PubMed/NCBI
|
|
19
|
Zhang Y, Zheng C, Zhang J, et al:
Generation and characterization of a panel of monoclonal antibodies
against distinct epitopes of human CD146. Hybridoma (Larchmt).
27:345–352. 2008. View Article : Google Scholar : PubMed/NCBI
|
|
20
|
Mathew A and George PS: Trends in
incidence and mortality rates of squamous cell carcinoma and
adenocarcinoma of cervix - worldwide. Asian Pac J Cancer Prev.
10:645–650. 2009.PubMed/NCBI
|
|
21
|
Prat J: Prognostic parameters of
endometrial carcinoma. Hum Pathol. 35:649–662. 2004. View Article : Google Scholar
|
|
22
|
Kang Y, Wang F, Feng J, et al: Knockdown
of CD146 reduces the migration and proliferation of human
endothelial cells. Cell Res. 16:313–318. 2006. View Article : Google Scholar : PubMed/NCBI
|
|
23
|
Zheng C, Qiu Y, Zeng Q, et al: Endothelial
CD146 is required for in vitro tumor-induced angiogenesis: the role
of a disulfide bond in signaling and dimerization. Int J Biochem
Cell Biol. 41:2163–2172. 2009. View Article : Google Scholar : PubMed/NCBI
|
|
24
|
Jemal A, Bray F, Center MM, Ferlay J, Ward
E and Forman D: Global cancer statistics. CA Cancer J Clin.
61:69–90. 2011. View Article : Google Scholar
|
|
25
|
Nolen BM and Lokshin AE: Protein
biomarkers of ovarian cancer: the forest and the trees. Future
Oncol. 8:55–71. 2012. View Article : Google Scholar : PubMed/NCBI
|
|
26
|
Tanyi JL and Scholler N: Oncology
biomarkers for gynecologic malignancies. Front Biosci (Elite Ed).
4:1097–1110. 2012. View
Article : Google Scholar : PubMed/NCBI
|
|
27
|
Chmura A, Wojcieszek A, Mrochem J, et al:
Usefulness of the SCC, CEA, CYFRA 21.1, and CRP markers for the
diagnosis and monitoring of cervical squamous cell carcinoma.
Ginekol Pol. 80:361–366. 2009.(In Polish).
|
|
28
|
Micke O, Bruns F, Schäfer U, Prott FJ and
Willich N: The impact of squamous cell carcinoma (SCC) antigen in
patients with advanced cancer of uterine cervix treated with
(chemo-)radiotherapy. Anticancer Res. 25:1663–1666. 2005.PubMed/NCBI
|
|
29
|
Jankovic MM and Milutinovic BS: Glycoforms
of CA125 antigen as a possible cancer marker. Cancer Biomark.
4:35–42. 2008.PubMed/NCBI
|