Introduction
Esophageal cancer is an aggressive disease that
typically metastasizes to the lymph nodes, lungs and liver
(1), while its metastasis to the eyes
is extremely rare. Breast and lung cancers are the source of the
majority of malignant intraocular metastatic tumors (2). To date, several cases of esophageal
carcinoma with intraocular metastasis have been reported (3–5), although
these were all adenocarcinomas and spread to the choroid but not
the iris. Previous studies indicated that while metastatic lesions
mainly invade the posterior uvea, and in particular the choroid, a
small portion may arise in the iris, ciliary body or retina
(6,7).
This is often considered to be due to the particular anatomical
structure: The posterior aspect of the uvea (choroid) has very rich
blood supply but the iris has few arteries, therefore the tumor
cells easily arrive and seed into the choroid through short
posterior ciliary artery. The choroidal blood supply is abundant,
and characterized by large lumen with a small volume of blood
imported and exported; metastatic cancer cells are easily able to
seed here (8). In the present report,
a rare case of a patient presenting with right eye lesion due to
metastasis of esophageal squamous cell carcinoma is discussed.
Furthermore, the present report identifies the potential diagnoses
and treatment of this type of tumor. Written informed consent was
obtained from the patient.
Case report
A 64-year-old male, with a history of esophageal
squamous cell cancer diagnosed 13 months previously, which was
treated by total esophagectomy (stage IIa, pT3N0M0) and
postoperative radiotherapy and chemotherapy, sought treatment for a
two-week history of a progressively distending pain in the right
eye with associated blurred vision.
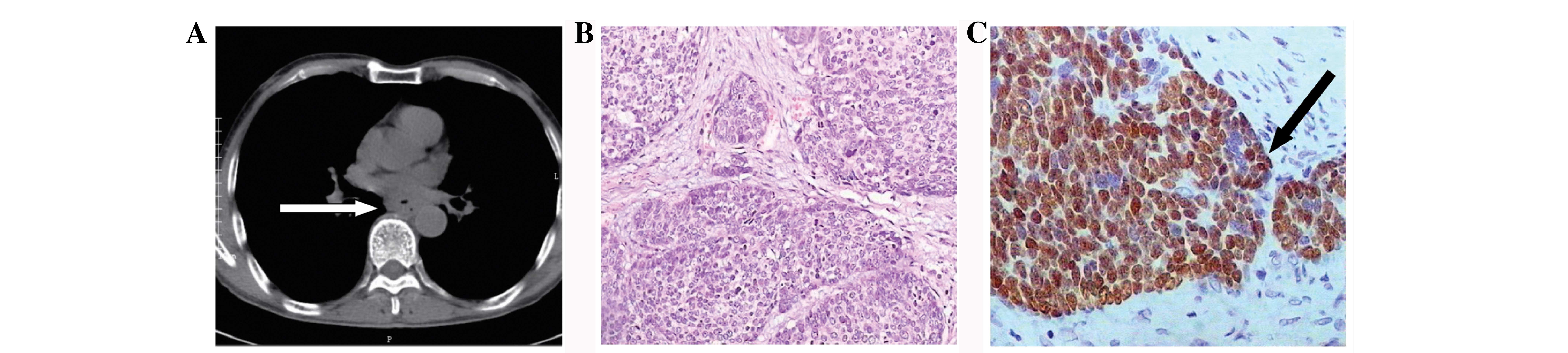
The patient's original computed tomography (CT)
(Fig. 1A) and postoperative pathology
results (Fig. 1B) revealed a
lower-differentiation squamous cell carcinoma. The specimen stained
positive for immunohistochemical (IHC) markers for P63 (Fig. 1C). Additional medical history included
hypertension and gastric stromal tumor (low risk). However, the
patient had no previously known ophthalmic diseases.
Ophthalmic examination was subsequently conducted.
Best-corrected visual acuity was 20/400 in the right eye and 20/25
in the left eye. Intraocular pressures, extraocular motility,
confrontation fields, external exam and slit-lamp examination of the
left eye were all normal. The right eye exhibited blepharospasm,
conjunctival hyperemia, corneal slight edema and high intraocular
pressure (25 mmHg). Slit-lamp examination of the right eye
identified a gray, irregular and vascularized neoplasm on the
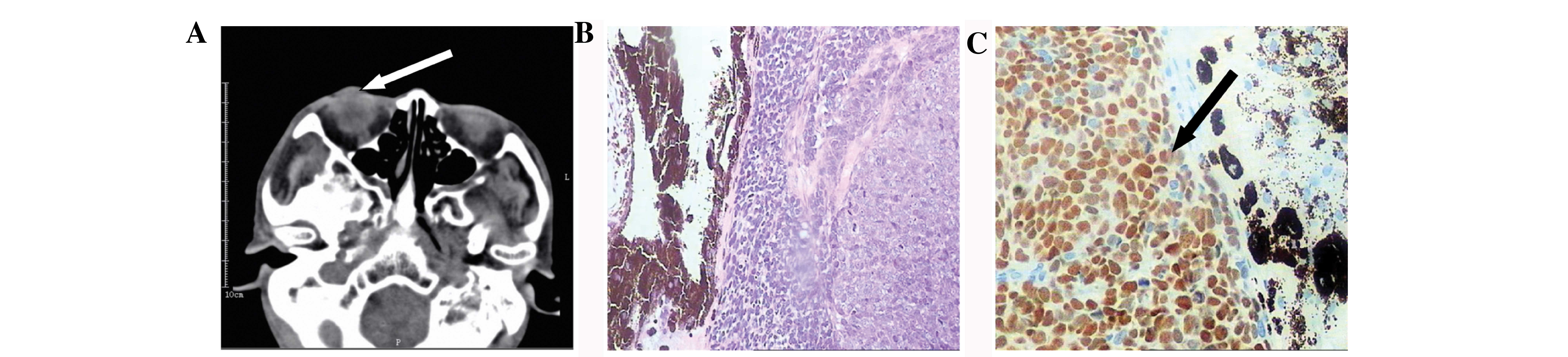
temporal side of the iris. CT examination (Fig. 2A) and ophthalmic ultrasound verified
the neoplasm in the right eye. The patient underwent ophthalmectomy
of the right side. Postoperative pathology revealed the tumor to be
0.7×0.5×0.3 cm in size and confirmed the diagnosis of a metastatic
iris neoplasm of esophageal squamous cell cancer origin (Fig. 2B and C). Subsequently, adjuvant
radiation with a total dose of 40 Gy was administered, but the
patient refused postoperative chemotherapy.
Discussion
Ocular metastases of malignant gastrointestinal
tumors are rare and have a poor prognosis of just 13 months median
survival following diagnosis. Furthermore, iris metastases comprise
<8% of all ocular metastases reported within the literature
(9). The most common primary sites of
ocular metastasis are breast cancer in females and lung cancer in
males. In addition, sarcomas and melanomas may also metastasize to
the eye (10). For esophageal
carcinoma, only two cases of iris metastases have been reported in
the last 20 years, one of which was adenocarcinoma (11) and the other was moderately
differentiated squamous cell carcinoma (12). To the best of our knowledge, the
present report was therefore only the second reported case of
esophageal squamous cell carcinoma metastasis to the iris.
Iris metastasis has a variety of clinical
manifestations, including decreased vision, ophthalmodynia,
diplopia, proptosis and periorbital swelling (13). The present patient sought medical
advice once the blurred vision had almost caused blindness, and a
cataract was suspected.
This rare case highlights a number of important
considerations. In clinical work, particular attention should be
paid to the ocular lesions of patients with a history of cancer.
Furthermore, it is necessary to perform comprehensive and serious
systemic and specialist examinations in order to avoid
misdiagnosis.
The diagnosis of ocular metastasis is often
difficult. Ophthalmic examination with slit-lamp biomicroscopy and
indirect ophthalmoscopy are important diagnostic tools for use upon
initial examination. Furthermore, ocular ultrasound, CT, magnetic
resonance imaging and positron emission tomography (PET)/CT
examination are used as powerful diagnostic tools. In particular,
PET/CT scans may aid the identification of benign or malignant
lesions and indicate the potential primary site. However a clear
history of a systemic malignancy is still the most significant
factor. Biopsy and immunohistochemical staining may be used for the
final diagnosis, to characterize the neoplasm and determine the
primary site, particularly in certain rare, poorly-differentiated
cases (14).
To date, the treatments for ocular metastasis
available include radiation, laser, chemotherapy, anti-vascular
endothelial growth factor and eye enucleation (10). More than half of patients exhibit
another metastatsis at the time the ocular lesion is detected
(2), therefore treatment is typically
non-curative. Taking into account the severe eyeball pain of the
patient and the inability to restore vision, eyeball enucleation
and adjuvant radiation was selected in the present case.
A notable contrast was also identified: The
pathological results demonstrated that the cellular differentiation
degree of the ocular metastatic lesion was worse than that of the
primary tumor site. It was suggested that this may be attributed to
the metastatic lesion originating from residual cancer stem cells
following multiple treatments, which have a worse phenotype and
exhibit drug-resistance subsequent to relapse. This highlighted the
importance of targeting cancer stem cell therapy in the future.
References
|
1
|
Kato H and Nakajima M: Treatments for
esophageal cancer: A review. Gen Thorac Cardiovasc Surg.
61:330–335. 2013. View Article : Google Scholar : PubMed/NCBI
|
|
2
|
Shields CL, Shields JA, Gross NE, Schwartz
GP and Lally SE: Survey of 520 eyes with uveal metastases.
Ophthalmology. 104:1265–1276. 1997. View Article : Google Scholar : PubMed/NCBI
|
|
3
|
Knezevic J, Radovanovic N, Simic A, Bobić
Radovanović A, Latković Z, Micev M and Pesko P: Isolated choroidal
metastasis from primary adenocarcinoma of the distal esophagus: A
case report. Dis Esophagus. 16:41–43. 2003. View Article : Google Scholar : PubMed/NCBI
|
|
4
|
Buskens CJ, Tan HS, Hulscher JB, de Smet
MD and van Lanschot JJ: Adenocarcinoma of the esophagus with
choroidal metastasis. Dis Esophagus. 14:70–72. 2001. View Article : Google Scholar : PubMed/NCBI
|
|
5
|
Parikh HK, Deshpande RK, Swaroop DV and
Desai PB: Choroidal metastasis from primary adenocarcinoma of the
esophagus - a case report. Indian J Cancer. 29:210–214.
1992.PubMed/NCBI
|
|
6
|
d'Abbadie I, Arriagada R, Spielmann M and
Lê MG: Choroid metastases: Clinical features and treatments in 123
patients. Cancer. 98:1232–1238. 2003. View Article : Google Scholar : PubMed/NCBI
|
|
7
|
Kim CY, Ha CW and Lee SC: Vitreous and
retinal metastasis from gastric cancer. Eur J Ophthalmol.
20:615–617. 2010.PubMed/NCBI
|
|
8
|
Albert DM, Zimmermann AW Jr and Zeidman I:
Tumor metastasis to the eye. 3. The fate of circulating tumor cells
to the eye. Am J Ophthalmol. 63:733–738. 1967. View Article : Google Scholar : PubMed/NCBI
|
|
9
|
Shields JA, Shields CL, Kiratli H and de
Potter P: Metastatic tumors to the iris in 40 patients. Am J
Ophthalmol. 119:422–430. 1995. View Article : Google Scholar : PubMed/NCBI
|
|
10
|
Giuliari GP and Sadaka A: Uveal metastatic
disease: Current and new treatment options (review). Oncol Rep.
27:603–607. 2012.PubMed/NCBI
|
|
11
|
Lee WB, Sy HM, Filip DJ and Grossniklaus
HE: Metastatic esophageal adenocarcinoma presenting in the iris. Am
J Ophthalmol. 144:477–479. 2007. View Article : Google Scholar : PubMed/NCBI
|
|
12
|
Ichiki Y, Morita M, Yano K, Sugio K,
Yasumoto K and Hirose N: Iris metastasis of esophageal cancer. Ann
Thorac Surg. 79:1782–1784. 2005. View Article : Google Scholar : PubMed/NCBI
|
|
13
|
Freedman MI and Folk JC: Metastatic tumors
to the eye and orbit. Patient survival and clinical
characteristics. Arch Ophthalmol. 105:1215–1219. 1987. View Article : Google Scholar : PubMed/NCBI
|
|
14
|
Kanthan GL, Jayamohan J, Yip D and Conway
RM: Management of metastatic carcinoma of the uveal tract: An
evidence-based analysis. Clin Experiment Ophthalmol. 35:553–565.
2007. View Article : Google Scholar : PubMed/NCBI
|