Article
Open Access
Association between αβ and γδ T‑cell subsets and clinicopathological characteristics in patients with breast cancer
- Authors:
- Meng Zhang
- Xueling Lu
- Changran Wei
- Xiangqi Li
-
View Affiliations / Copyright
Affiliations:
First Clinical College, Shandong University of Traditional Chinese Medicine, Jinan, Shandong 250355, P.R. China, Department of Nuclear Medicine, Tai'an City Central Hospital, Tai'an, Shandong 271000, P.R. China, Department of Breast Surgery, The Second Affiliated Hospital of Shandong First Medical University, Tai'an, Shandong 271000, P.R. China
-
Article Number:
325
|
Published online on:
October 5, 2020
https://doi.org/10.3892/ol.2020.12188
- Expand metrics +
Metrics:
Total
Views: 0
(Spandidos Publications: | PMC Statistics:
)
Metrics:
Total PDF Downloads: 0
(Spandidos Publications: | PMC Statistics:
)
This article is mentioned in:
Abstract
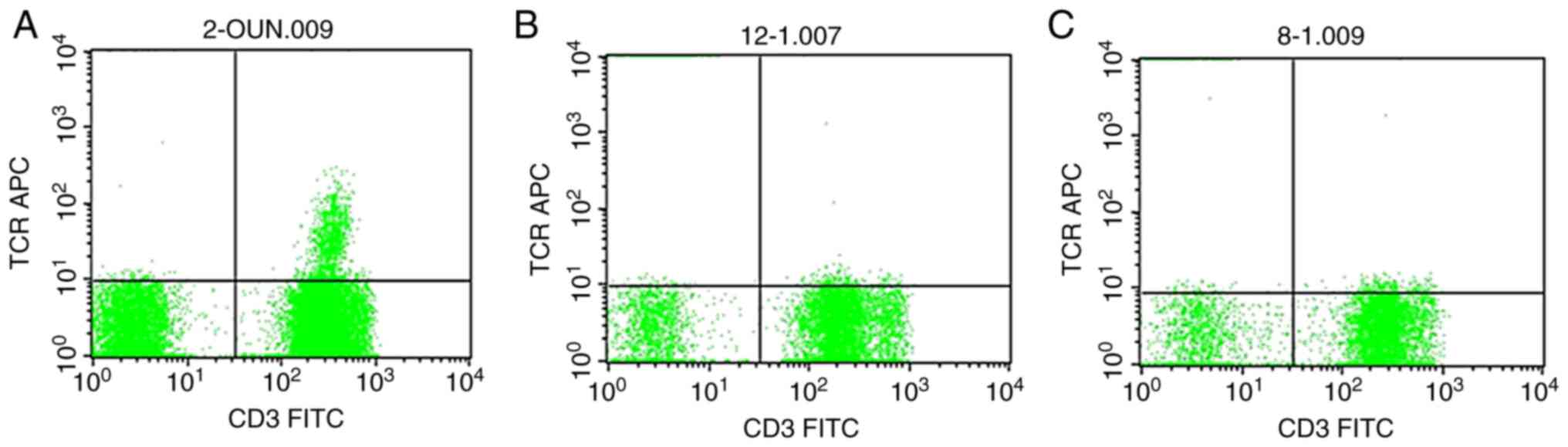
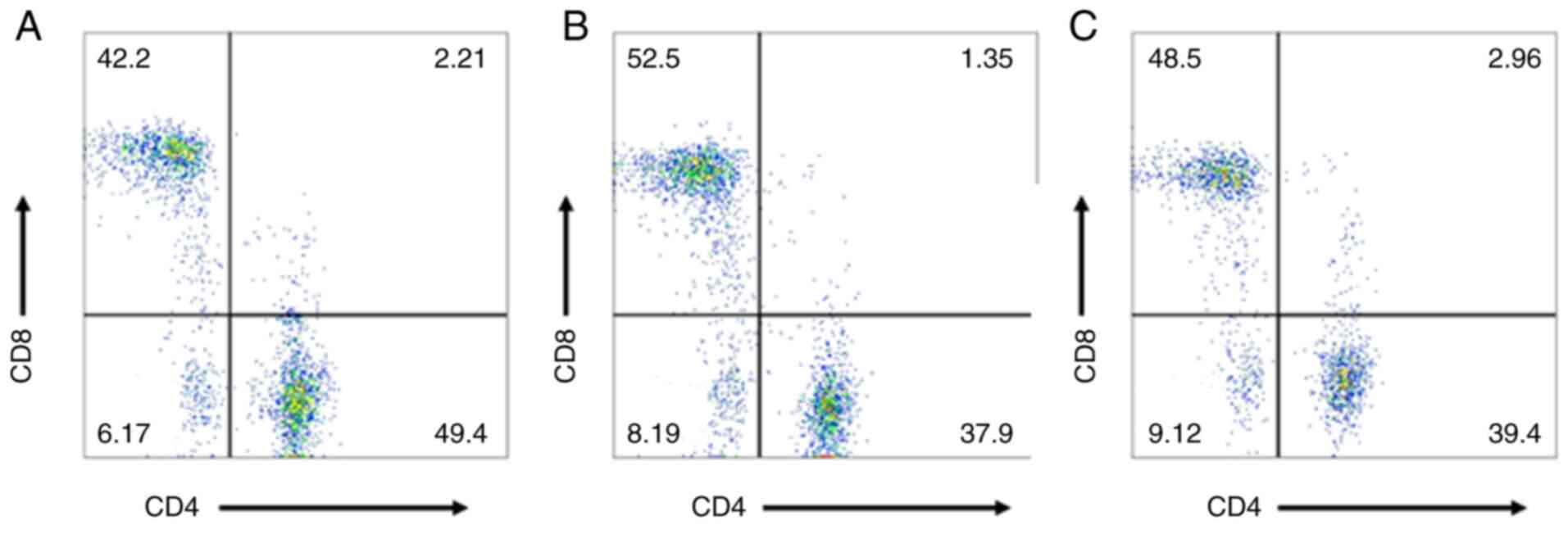
The aim of the present study was to discuss the effect of surgery on the T‑lymphocyte subsets of patients with breast cancer (BC) and investigate the association between peripheral blood αβ and γδ T‑cell counts and the clinicopathological characteristics of BC. The CD3+, CD4+, CD8+ and γδ T‑cell subsets in the peripheral blood of healthy volunteers and Patients with BC before and after surgery were determined using flow cytometry. The association between αβ and γδ T‑cell counts in the peripheral blood and clinicopathological characteristics was analyzed by comparing the differences in the αβ and γδ T‑cell counts in the peripheral blood of Patients with BC before and after surgery with those of healthy volunteers and combining with clinicopathological data. The CD3+, CD4+ and γδ T‑cell counts in the peripheral blood of Patients with BC were lower compared with those in healthy volunteers (P=0.0077, 0.0116 and 0.0003, respectively), whereas the number of CD8+ cells was higher (P=0.0241). The CD3+, CD4+ and γδ T‑cell counts and the CD4+/CD8+ ratio after surgery were significantly higher compared with those before surgery (P=0.0109, 0.0031, 0.0165 and 0.018, respectively). There was no significant difference between the number of CD8+ cells before and after surgery (P=0.0053), but the number of CD8+ cells was higher in healthy volunteers compared with that in Patients with BC (P<0.05). Moreover, the CD3+ cell number was higher in patients with TNM stage II/III compared with those with TNM stage I disease (P=0.187 and 0.022, respectively), and the peripheral blood CD4+/CD8+ ratio and number of γδ T cells were lower in stage III compared with stage I Patients with BC (P=0.0065 and 0.0176, respectively). Histological grading demonstrated that the CD4+/CD8+ ratio and number of γδ T cells in patients with stage III BC were lower compared with those with stage I BC (P=0.02 and 0.0128, respectively). The γδ T‑cell count in patients with luminal A and B subtypes was significantly higher compared with that in patients with basal‑like subtype (P=0.004 and 0.0104, respectively). The CD3+, CD4+ and γδ T‑cell counts were significantly lower in patients with lymph node (LN) metastasis compared with those without LN metastasis, and the CD8+ cell number was lower in patients without LN metastasis compared with that in patients with >10 LN metastases (P=0.0086, 0.0000 and 0.00468, respectively). The CD8+ cell count in patients without LN metastasis was lower compared with that in patients with 4‑9 and >10 LN metastases (P=0.0435 and 0.0283, respectively). Surgery affects the T‑lymphocyte subpopulations in patients with BC, and αβ and γδ T‑cell counts may increase following mastectomy. Therefore, measurement of peripheral blood lymphocyte subsets is crucial for understanding the immune function status of Patients with BC with differences in TNM stage, histological grade, cell subtypes and LN metastases, and may provide a basis for the application of T‑cell subsets in the comprehensive treatment of BC.
View References
|
1
|
Siegel RL, Miller KD, Fedewa SA, Ahnen DJ,
Meester RG, Barzi A and Jemal A: Colorectal cancer statistics,
2017. CA Cancer J Clin. 67:177–193. 2017. View Article : Google Scholar : PubMed/NCBI
|
|
2
|
Markman JL and Shiao SL: Impact of the
immune system and immunotherapy in colorectal cancer. J
Gastrointest Oncol. 6:208–223. 2015.PubMed/NCBI
|
|
3
|
Riazi Rad FR, Ajdary S, Omranipour R,
Alimohammadian MH and Hassan ZM: Comparative analysis of
CD4+ and CD8+ T cells in tumor tissues, lymph
nodes and the peripheral blood from patients with breast cancer.
Iran Biomed J. 19:35–44. 2015.PubMed/NCBI
|
|
4
|
Xu J, Jiang L, Cao H, Jia Y, Wu S, Jiang C
and Sun T: Predictive value of CD4+/CD8+
ratio in patients with breast cancer receiving recombinant human
thrombopoietin. J Interferon Cytokine Res. 38:213–220. 2018.
View Article : Google Scholar : PubMed/NCBI
|
|
5
|
Lin KR, Pang DM, Jin YB, Hu Q, Pan YM, Cui
JH, Chen XP, Lin YX, Mao XF, Duan HB and Luo W: Circulating
CD8+ T-cell repertoires reveal the biological
characteristics of tumors and clinical responses to chemotherapy in
breast cancer patients. Cancer Immunol Immunother. 67:1743–1752.
2018. View Article : Google Scholar : PubMed/NCBI
|
|
6
|
Janssen N, Fortis SP, Speigl L, Haritos C,
Sotiriadou NN, Sofopoulos M, Arnogiannaki N, Stavropoulos-Giokas C,
Dinou A, Perez S, et al: Peripheral T cell responses to tumour
antigens are associated with molecular, immunogenetic and cellular
features of breast cancer patients. Breast Cancer Res Treat.
161:51–62. 2017. View Article : Google Scholar : PubMed/NCBI
|
|
7
|
Silva-Santos B, Serre K and Norell HK: γδ
T cells in cancer. Nat Rev Immunol. 15:683–691. 2015. View Article : Google Scholar : PubMed/NCBI
|
|
8
|
Kassardjian A, Shintaku PI and Moatamed
NA: Expression of immune checkpoint regulators, cytotoxic T
lymphocyte antigen 4 (CTLA-4) and programmed death-ligand 1
(PD-L1), in female breast carcinomas. PLoS One. 13:e01959582018.
View Article : Google Scholar : PubMed/NCBI
|
|
9
|
Morrow ES, Roseweir A and Edwards J: The
role of gamma delta T lymphocytes in breast cancer: A review.
Transl Res. 203:88–96. 2019. View Article : Google Scholar : PubMed/NCBI
|
|
10
|
Sugie T, Murata-Hirai K, Iwasaki M, Morita
CT, Li W, Okamura H, Minato N, Toi M and Tanaka Y: Zoledronic
acid-induced expansion of γδ T cells from early-stage breast cancer
patients: Effect of IL-18 on helper NK cells. Cancer Immunol
Immunother. 62:677–687. 2013. View Article : Google Scholar : PubMed/NCBI
|
|
11
|
Silva-Santos B, Mensurado S and Coffelt
SB: γδ T cells: Pleiotropic immune effectors with therapeutic
potential in cancer. Nat Rev Cancer. 19:392–404. 2019. View Article : Google Scholar : PubMed/NCBI
|
|
12
|
Kobayashi H and Tanaka Y: γδ T cell
immunotherapy-a review. Pharmaceuticals (Basel). 8:40–61. 2015.
View Article : Google Scholar : PubMed/NCBI
|