Introduction
Phyllodes tumor (PT) is a rare breast tumor; more
specifically, its diagnosis reaches 0.3 to 1% of all breast tumors
(1). This tumor consists of an
uncommon complex group of fibroepithelial lesions with leaf-like
architecture and increased stromal cellularity (2). The first reference to PT of the
breast (PTB) dates back to the 1800s when Muller was the first
person to report it. It was initially named ‘cystosarcoma
phyllodes’ and was described as a rapidly growing tumor with a
cystic lobulated section (3).
Since then, a lot of names were given by the scientific community
and a lot of controversies and disputes took place to properly
classify this type of tumor. The World Health Organization (WHO)
and its international histological classification group in 2003
recommended that this anomaly should be named ‘phyllodes tumor’ and
that it can be classified into 3 categories: malignant, borderline,
and benign (1). The controversy
and disputes over the years, the evolution, and later the
settlement on the terminology, characteristics, and identification
of this tumor type signifies how rare it is and the difficulty in
its precise diagnosis.
According to the latest (2019) WHO edition of breast
tumours the criteria for diagnosing and grading this rare form of
tumor consist of stromal cellularity, stromal atypia, presence of
stromal overgrowth which is defined as the absence of epithelial
elements containing stroma only in 1 low power field, well defined
or permeative borders, mitotic count, and presence of heterologous
elements (4). The distinction
between benign and borderline PT from malignant PT is important
since benign and borderline PT may recur or metastasize less
frequently while malignant PT show higher rates of recurrence and
hematogenous metastasis (5).
Benign PT shares some common characteristics if compared to
cellular fibroadenoma while malignant PT can be mistaken for
spindle cell metaplastic breast carcinoma or primary breast
sarcoma. Making a distinction can often be problematic and
inconsistent when performing a core biopsy (2). The presence of a bland epithelial
component helps in the differential diagnosis of stromal sarcomas.
It is worth mentioning that based on the reporting of findings for
these tumors, they tend to be benign with borderline malignancy.
Malignant PTs are less commonly reported (6).
Due to its rarity, the method of diagnosis for the
PT has a very low accuracy rate. Attempting to diagnose it
preoperatively has proven uncertain and inefficient and therefore,
it led scientists and professionals to attempt treating and
diagnosing it using various surgical techniques. One of the most
important prognostic features of this form of tumor is the high
local recurrence (LR) rate which reaches up to 40% for the various
histological types of these phyllodes breast tumors. In its
Malignant PT may show an aggressive clinical behavior with rapid
growth and potential for hematogenous or lymphatic metastasis. From
various data gathered by specialists throughout the years, it is
safe to say that PT tends to metastasize in the lungs, bones, and
soft tissue via blood. Lymph node metastasis is extremely rare with
its overall metastasis rate via both blood and lymph nodes being
~4%. It is important to mention that malignant and borderline
metastasis rates are higher than benign ones, for ~30% of its
occurrences (1,7,8).
After performing a core biopsy, some cellular fibroepithelial
lesions might be extracted from the patient by open or
vacuum-assisted excision although surgical excision is the
preferred method for removal (2).
Materials and methods
To find the most recent studies for this systematic
review, a calculated decision was made to utilize the biggest and
most reliable Web Databases in the world of medicine and research.
These databases were PubMed, PubMed Central, Cochrane Library,
Embase, Web of Science, UpToDate, and Google Scholar. A literature
search with citations and specific keywords while using the
advanced search option was performed in every database in order to
narrow down and provide accurate results. The year range of the
studies that were considered to be relevant was 1995 to the
present.
The following keywords were used: phyllodes tumor,
phyllodes tumor, phyllode tumor, phyllode tumor, phyllodes tumor,
phyllodes tumor, breast phyllodes, breast phyllodes, phyllodes
radiotherapy, phyllodes radiotherapy, phyllodes radiation,
phyllodes radiation, cystosarcoma phyllodes, cystosarcoma
phyllodes, phyllodes tumor breast, phyllodes tumor breast,
phyllodes malignant, phyllodes borderline, phyllodes benign,
phyllodes malignant, phyllodes borderline, phyllodes benign. These
keywords were combined with the following Boolean Operators: ‘OR’,
‘AND’ and the wildcard symbol ‘*’.
The advanced search was narrowed down to look for
results in only the titles of the studies. Because of the small
number of results returned from the queries performed to all of the
databases and due to the specificity of the studies required, all
main articles that matched the criteria were also scanned manually
by the authors for more references to studies that could be
included in the review. Moreover, all research material gathered
had to be conducted ethically following the World Medical
Association Declaration of Helsinki, and any studies not conforming
to these principles were not included in the initial result
set.
Inclusion and exclusion criteria
Exclusion criteria
Due to the subject of this review and the fact that
there is still much to learn about it, the result set of the
combined searches was not massive. To further narrow down the
results and make it a subset of studies that were of interest, any
studies that did not measure any LR even if there weren't any, were
excluded. Also, any studies that did at least consider mastectomy
as an option, even if mastectomy wasn't performed eventually, were
removed from the result set. If the studies remaining did not
involve any malignant PTs they were also excluded along with every
study that did not reference radiotherapy as a consideration and,
if radiotherapy wasn't a consideration, the existence of a valid
reason as to why it was not preferred. If a study did not contain
any detailed information on the number of LRs after a specific
treatment, for example ‘10 patients having local occurrence after
they underwent a mastectomy and 20 patients having local occurrence
after they underwent local excision, it was also excluded from the
set.
Inclusion criteria
Furthermore, all studies should also specify a mean
or median age. The age range should have been between 20 and 55
years. There should also be a reference to the method of treatment
for the PT whether it was a breast-conserving surgery (BCS) or a
mastectomy. There should also be at least some patients in the
study with LR in order to review the rate at which the tumors
reappeared locally. A distinction between malignant and benign or
borderline PTs of the breast (PBT) with the actual amount of
patients in each category should also be present in the study so
the reviewers could better understand and identify why the
researchers in these studies concluded to specific treatments and
practices. A reference to follow-ups, even if the patients chose
not to have any was also one factor to deem a study eligible for
reviewing.
Data extraction
Two authors separately reviewed the 10 remaining
studies after the inclusion and exclusion criteria were applied to
the result set. The number of participants, the mean or median age,
the number of patients with benign, borderline, or malignant
tumors, the number of patients that underwent BCS or mastectomy,
any patients that were exposed to radiotherapy, the follow-up
period in months or any patients that had LR of the tumor were the
main extraction items from the data. If a specific study allowed
it, the authors also extracted the number of patients that had an
LR after a BCS, or an LR after mastectomy. The preferred method for
operating on LRs and whether it was partial/local mastectomy or
local/wide excision was also extracted. If there was any history of
fibroadenoma before the appearance of a PT it was deemed as
important information and was also recorded.
The findings of the two authors were then compared
to each other and in every scenario where there was a dispute on
the data that were extracted, a joint review of the study would
take place, and if there were still any discrepancies between the
reviewers a group discussion would occur to resolve it. Some data
were still discordant after the joint effort of the authors and
could not be extracted from certain studies even after the
reviewing took place. Due to that, all authors agreed to mark the
data for these studies as ‘N/A’ based on the context of the
uncertain information. For the detailed table of extracted data
please refer to Table I. The study
data have also been registered with the National Institute for
Health Research's PROSPERO database on the 21st of February 2021
(ID: CRD42021230914).
 | Table I.Extracted data from final result set
of studies. |
Table I.
Extracted data from final result set
of studies.
| Study name, year | Population | Mean age (years) | BN/BL | MLG | BCS | MT | RT | FLW MD | LR | LR after BCS | LR after MT | BCS after LR | MT after LR | History (FA) | (Refs.) |
|---|
| Barrio et al,
2007 | 293 | 41.7 | 203 | 90 | 245 | 48 | 0 | 94.8 | 35 | 31 | 4 | 21 | 10 | 109 | (16) |
| Chen et al,
2005 | 172 | 50.0 | 143 | 29 | 126 | 46 | 2 | 71.2 | 19 | 19 | 0 | 14 | 5 | 22 | (11) |
| Cheng et al,
2006 | 182 | 37.0 | 151 | 31 | 132 | 50 | 3 | 60.5 | 20 | 20 | 0 | 17 | 3 | N/A | (13) |
| Fajdić et al,
2007 | 36 | 56.0 | 30 | 6 | 29 | 7 | 0 | 98.5 | 3 | 3 | 0 | 3 | 0 | N/A | (17) |
| Fou et al,
2006 | 27 | 51.0 | 0 | 27 | 18 | 9 | 0 | 52.0 | 4 | 4 | 0 | 0 | 4 | N/A | (14) |
| Jang et al,
2012 | 164 | 43.0 | 124 | 40 | 148 | 16 | 3 | 33.6 | 31 | 28 | 3 | N/A | N/A | N/A | (18) |
| Kapiris et
al, 2001 | 48 | 47.0 | 0 | 48 | 24 | 24 | 10 | 108.0 | 21 | 10 | 11 | 14 | N/A | N/A | (10) |
| Moffat et
al, 1995 | 32 | 52.0 | 27 | 5 | 20 | 12 | 0 | 135.0 | 6 | 6 | 0 | 2 | 4 | N/A | (9) |
| Roa et al,
2006 | 47 | 42.5 | 37 | 10 | 30 | 17 | 3 | 97.3 | 9 | 8 | 1 | N/A | N/A | N/A | (12) |
| Taira et al,
2007 | 45 | 45.0 | 36 | 9 | 42 | 3 | 0 | 101.0 | 6 | 6 | 0 | 6 | 0 | 3 | (15) |
Statistical analysis
Review Manager (RevMan) v5.3, a tool developed by
Cochrane to support the preparation and maintenance of systematic
reviews, was used for this systematic review. It was run in
Non-Cochrane mode. The tool allowed the authors to pool together
all the different data that were extracted from the 10 different
studies manually and provide a combined result. The outcomes of LR
for both BCS patients and patients that underwent mastectomy were
fed into the software as dichotomous values and were analyzed as
odd ratios (ORs). The analysis was performed using the
Mantel-Haenszel method and by utilizing a fixed effect analysis
model. The confidence intervals were set to 95%. RevMan also
assessed the statistical heterogeneity by using the I2
index. The intervals for I2 were set as follows:
I2 <25% was considered to represent low
heterogeneity, I2 >25% but also I2 <75%
was considered to represent moderate heterogeneity, and
I2 >75% was considered to represent high
heterogeneity. Figs. 1 and
2 have been directly extracted
from RevMan and represent forest plots visually indicating the
statistical significance of the meta-analysis of the data the
authors extracted from the selected studies.
Results
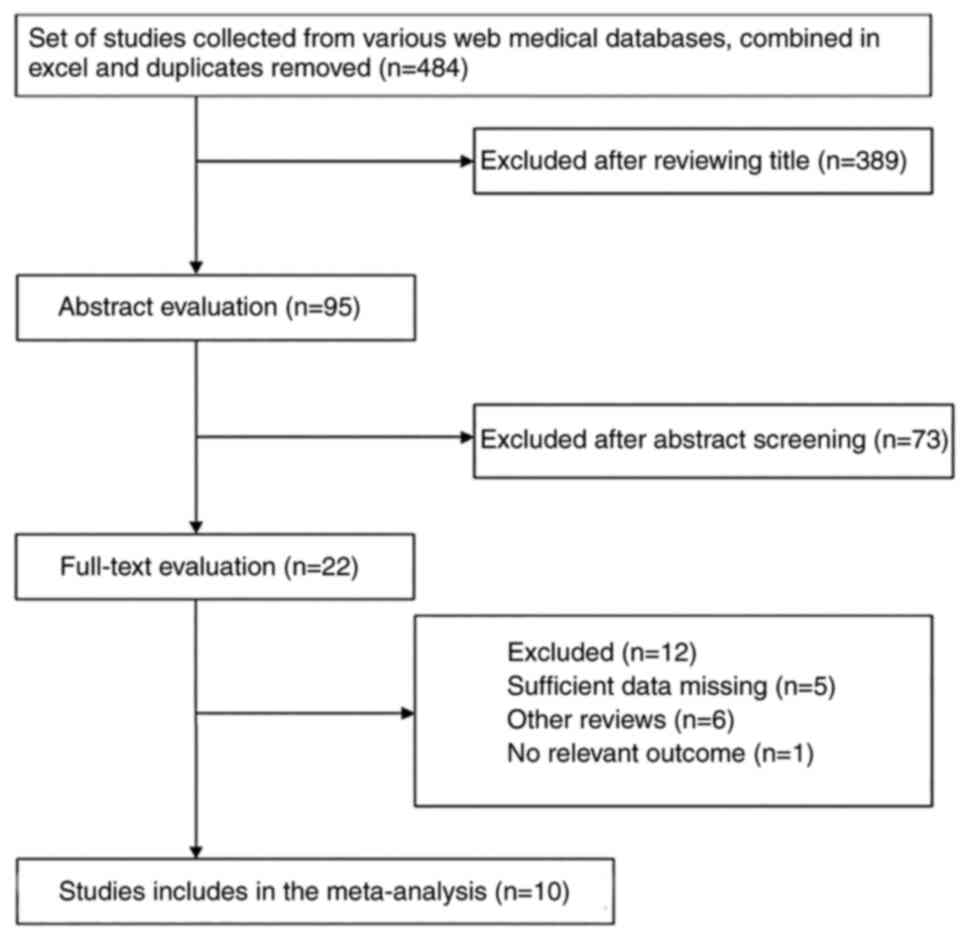
Study selection process
484 studies were initially identified after
searching all medical web databases the authors utilized and all
duplicates from the result sets of these databases were removed.
Filtering for a year range while performing the search in these
databases helped the authors avoid the manual labor required to
distinguish recent and older studies. The authors were only
interested in studies that were performed over the last 25 years.
After reviewing the titles of the result set, 389 studies were
excluded with 95 studies remaining for abstract evaluation. After
the abstract screening of these 95 studies, 73 studies were removed
from the result set either because of a lack of information
presented or their comparison with other elements that were
irrelevant to this review. The remainder of this result set were 22
studies which the authors then closely evaluated by performing a
full-text analysis, ensuring all the relevant parameters of
interest were measured and sufficient details were present in each
study. From this result set, 5 studies were missing important data
such as referencing appropriate data for LR on patients after they
underwent mastectomy or any other BCS or the outcome wasn't clear
for one of the two groups the authors were interested in, for
example there was a reference to local occurrence on patients that
had a mastectomy but not any other form of surgery-like local
excision. 6 studies were also excluded because they were systematic
reviews and 1 was excluded because it had no relevant outcome for
the purpose of this study. The outcome of the study selection
process was 10 studies (9–18). The literature review can be seen in
Fig. 3.
Population characteristics
From these 10 studies, the total amount of
participants was 1,046. The lowest mean age of the studies was 37
years of age and the highest was 56. A total of 751 patients had
benign or borderline PT. A total of 295 patients had a malignant
PT. Then, 232 underwent mastectomy as a therapeutic approach while
814 were treated with any other BCS-like local or wide excision.
For 21 patients radiotherapy was also offered as part of the
treatment. The follow-up means in months varied, with the lowest
being 33.6 months and the highest being 135 months. 154 of these
patients that underwent a mastectomy, local or wide excision, and
radiotherapy had an LR of the tumor. 19 had LR after mastectomy was
performed while 135 had LR after other BCS operations. 134 patients
had a history of fibroadenoma before being diagnosed with PT. Of
all the patients who developed LR, 26 had a mastectomy to treat the
LR, and 77 had milder surgery such as local or wide excision.
Table II presents the baseline
characteristics of the studies the authors included.
 | Table II.Baseline characteristics of studies
included. |
Table II.
Baseline characteristics of studies
included.
| First author
(Refs.) | Country (year) | Population | Mastectomy | BCS | RT | Mean age
(years) | Mean follow-up
(months) |
|---|
| Moffat CJC
(9) | England (1995) | 32 | 12 | 20 | N/A | 52.0 | 135.0 |
| Kapiris I (10) | England (2001) | 48 | 24 | 24 | 10 | 47.0 | 108.0 |
| Chen WH (11) | Taiwan (2005) | 172 | 46 | 126 | 2 | 50.0 | 71.2 |
| Roa JC (12) | Chile (2006) | 47 | 17 | 30 | 3 | 42.5 | 97.3 |
| Cheng SP (13) | Taiwan (2006) | 182 | 50 | 132 | 3 | 37.0 | 60.5 |
| Fou A (14) | USA (2006) | 27 | 9 | 18 | N/A | 51.0 | 52.0 |
| Taira N (15) | Japan (2007) | 45 | 3 | 42 | N/A | 45.0 | 101.0 |
| Barrio AV (16) | USA (2007) | 293 | 48 | 245 | N/A | 41.7 | 94.8 |
| Fadjic J (17) | Croatia and Germany
(2007) | 36 | 7 | 29 | N/A | 56.0 | 98.5 |
| Jang JH (18) | Korea (2012) | 164 | 16 | 148 | 3 | 43.0 | 33.6 |
Meta-analysis
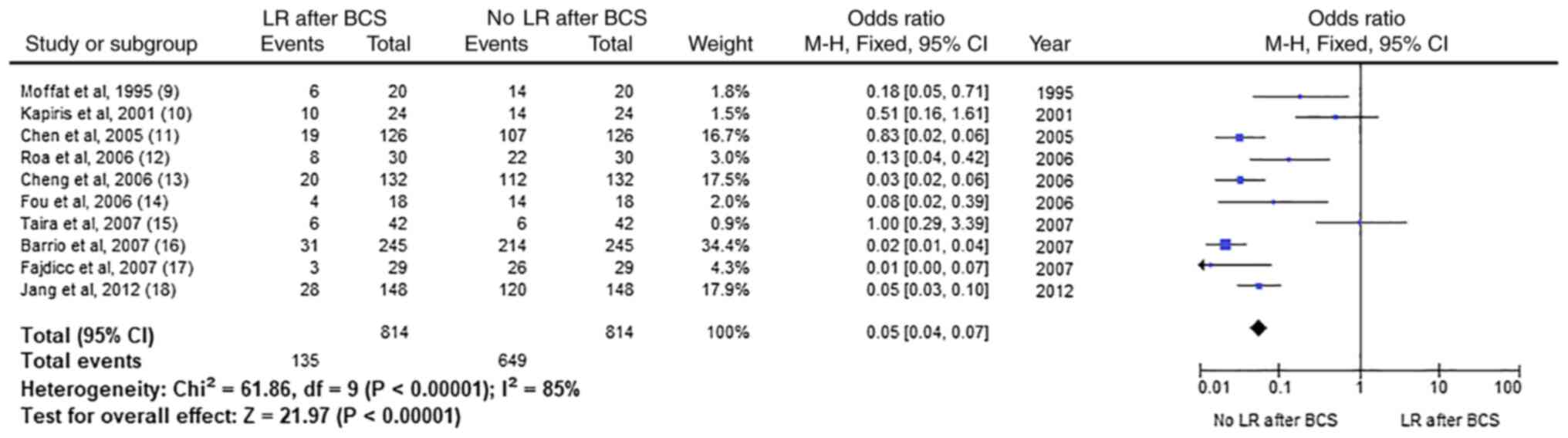
LR in patients after any BCS
The final result set data consisted of 10 studies
with 1046 participants. In Fig. 1
which can be seen further below, analytical data on the odds ratio,
heterogeneity, and the likelihood of LR after a BCS are being
demonstrated. The odds ratio for LR after a BCS is 0.05 with 0.04
and 0.07 confidence intervals (CIs). The heterogeneity of the
results is at 85% which, as stated earlier is considered high.
Based on the CI and the p-value in the figure it is fair to say
that the result is statistically significant and that LR is not
very common for patients that were treated for PBT with BCS.
It is also noteworthy that cases of benign or
borderline PT tend to be treated with BCS-like local or wide
excision and since they are not as aggressive as the malignant ones
their LR is expected to be low. The overall percentage of LR in
patients treated with BCS is 16.58% which was estimated after
finding the percentage that corresponds to the 135 LR events for
the total of 814 patients that were treated with any form of
BCS.
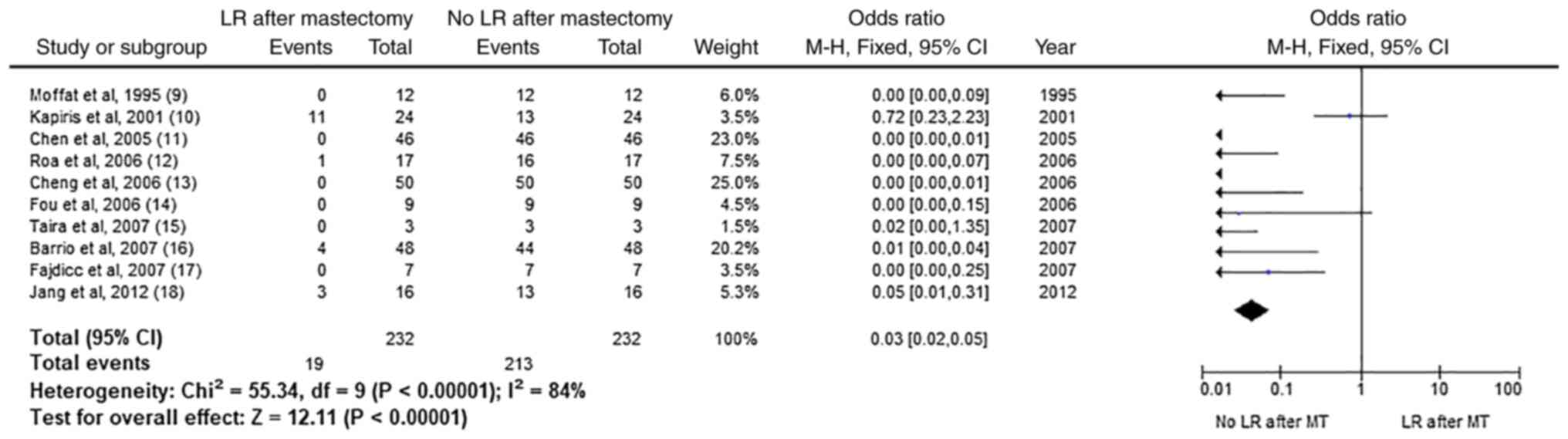
LR in patients after mastectomy
On the following forest plot (Fig. 2), analytical data on the odds
ratio, heterogeneity, and the likelihood of LR after a mastectomy
can be observed. The heterogeneity, at 84% is at par with the LR
after a BCS and is considered high. The odds ratio is at 0.03 with
0.02 and 0.05 CIs. The LR on patients that were treated with
mastectomy for PBT is not common as concluded from the P-value
which signifies that the result is statistically significant.
Now contrary to benign and borderline tumors being
treated with BCS treatments, mastectomy is preferred in malignant
PTs due to their potentially aggressive behavior. One could argue
that since the treatment is harsher and a lot more tissue is being
removed, maybe it is more effective as well. Based on the results,
the percentage that corresponds to the 19 patients with LR from the
232 patients that underwent a mastectomy in total is 8.19%.
LR BCS vs. mastectomy
In both measurements, it was identified that LR was
not common. Both forest plots had 95% CI, a low OR, and a very low
p-value which made the results statistically significant and of
high heterogeneity. It is interesting to notice though that the
percentage of individuals having an LR after BCS was higher at
16.58% than the percentage of individuals having LR after
mastectomy at 8.19%. Is it due to the bigger amount of patients
undergoing BCS that a noticeable higher rate of LR persists? Or is
it because BCS techniques are milder than a mastectomy? The
important result to mind here is that LR is not as common in
patients who were treated with local excision, wider excision, or
mastectomy. Also, a higher LR rate occurs for patients treated with
any form of BCS when compared to individuals who underwent a
mastectomy.
Discussion
There is still much to discover about PT. Not a lot
of extensive studies exist on the subject and due to its very rare
occurrence and the minimal amount of data existing to date; it is
unlikely that at this point a solid treatment process can be
followed as the gold standard. Numerous scientists attempted to
perform retrospective studies on the matter but their findings did
not suggest a conclusive result in terms of disease-free survival
or overall survival rates after treating this rare neoplasm. We
strongly consider that breast cancer management should be a part of
gynecological care. Worldwide more and more gynecologists are being
specialized in breast cancer management since it can be diagnosed
in women of a younger age who want to preserve the possibility of a
future pregnancy.
Keeping this in mind, professionals in the field
currently take all necessary measures to ensure treatment of this
tumor will allow for greater life expectancy, the well-being of
patients, and the ability to have a pregnancy even after being
treated. Therefore, most physicians tend to remove the tumor via
surgery along with the extraction of 1 cm or more of surrounding
healthy breast tissue to ensure the tumor won't recur. This process
is also known as wide excision. Lumpectomy and mastectomy can also
occur in situations where the tumor is proven large in size,
malignant and aggressive (19).
Breast imaging, clinical examination, and needle biopsy are most
commonly used as the procedures a patient should undergo for a
tumor to be evaluated since mammography and ultrasound are
inconclusive when it comes to biopsy, due to the tumor's
resemblance to benign fibroadenomas. Because of this
characteristic, PT might recur after their initial extraction. And
due to their irresponsiveness to other breast cancer treatments
such as chemotherapy, drugs, or hormone therapy, PTs are being
treated similarly to sarcomas. Another reason they are being
treated as such is that they arise from stromal elements in the
breast (20,21). Radiotherapy is the standard for
treating sarcomas and a lymph node sampling on a percentage of the
patients that underwent this treatment backs up this theory
(20).
Based on one of the largest retrospective systematic
reviews to date on the matter, which was performed by Gnerlich
et al, scientists still face a limitation when attempting to
report and rely on their findings since most authorities monitoring
the prognosis, diagnosis, and outcomes of PT tend to focus on
collecting data for malignant cases only, making it hard to
cross-reference rates and outcomes since, as reported earlier in
this study, a malignant PT is extremely rare in its occurrence
(20).
Even more so, when scientists attempt to conclude
the recurrence of this rare tumor by utilizing results that in some
instances tend to be inconclusive or different from other studies
that were performed on the same matter. There are also some
limitations, such as the lack of follow-up data from patients that
were treated for malignant PT. Or the lack of accurate data kept by
the institutions treating the patients due to the nature of the
staff that maintains the registry and since in some cases they do
not have the knowledge or skill set to understand the difference
between malignant, borderline, and benign tumors from just a
surgical pathology report. Or even the lack of data on the
recurrence and location of recurrence of the tumor itself (20).
Despite these facts though, in most studies on this
subject, some common factors lead to the utilization of
radiotherapy, as mentioned earlier, as a method for additional
treatment after extraction. Factors such as the size of the tumor,
its malignancy, the age of the patient, the date of the diagnosis,
and the sampling of the node are taken into consideration. Various
studies attempted to compare results for patients that were
diagnosed with PT and were treated with an alternative therapeutic
method. Some patients underwent a mastectomy, others underwent
lumpectomy or wide excision. Mastectomy was mostly used on women of
older age and/or patients with larger tumors. The survival rate for
women who underwent mastectomy was lower than for women who were
treated with wide excision (21)
but that is due to the more aggressive and malignant nature of the
tumor. All studies signify though, that when radiotherapy is
utilized as a part of the treatment in malignant PT with a high
risk of post-treatment LR (20,22–24)
the patients have a higher survival rate based on follow-ups and
monitoring.
It is also noteworthy that there isn't any
significant difference when utilizing radiotherapy as a treatment
option between patients with a low and high risk of recurrence
(20) and this is due to, again,
the lack of collected data on the marginal width of the tumor. The
systematic review by Gnerlich et al (20) indicates that although the
common consensus is to perform radiotherapy for patients with a
tumor width of at least 1 cm, there are cases where patients with
less than 1 cm width underwent radiotherapy.
Another common characteristic between studies is the
indication of decreased rates in LR for patients who underwent
radiotherapy in comparison to patients that underwent surgery for
removal alone. Similarly, patients that underwent mastectomy
instead of any other BCS had a decreased rate of LR. That is why,
as observed by the studies the authors investigated, mastectomy was
preferable as a second treatment option. Moreover, the period for
any LR if any, increased. This led to the conclusion that patients,
who were exposed to radiotherapy or underwent a mastectomy, or were
treated with both to remove any borderline or malignant PTB had a
higher survival rate. This is because their follow-up exams did not
suggest any local occurrence of the tumor after extraction
(23).
Based on this and other studies' findings, surgical
excision and radiotherapy tend to be the preferred methods of
treating PT. The authors concluded that standard common practices
for other more common malignancies helped in the treatment and
survival rates of patients suffering from a PT. Because of this
tumor's unpredictable behavior though and due to the lack of excess
data to this date, the scientific community still has a way to go
in order to advance in an improved understanding of this rare form
of cancer and identify the appropriate treatment practices
physicians should adapt to help minimize LR and improve the
disease-free and overall survival rates.
Acknowledgements
Not applicable.
Funding
Funding: No funding was received.
Availability of data and materials
The data of the present study was registered with
PROSPERO (https://www.crd.york.ac.uk/prospero/display_record.php?RecordID=230914,
accession no. CRD42021230914). The datasets used and/or analyzed
during the current study are available from the corresponding
author on reasonable request.
Authors' contributions
IB participated in the conceptualization, designed
methodology, analyzed data and wrote and prepared original draft.
AK designed the methodology, analyzed data, wrote and prepared the
original draft. DD and NK analyzed data. SMG designed methodology,
analyzed data and prepared original draft. KS designed methodology
and prepared original draft. CD and SK designed Methodology and
interpretation of data. IB and AK confirm the authenticity of all
the raw data. All authors have read and approved the final
manuscript.
Ethics approval and consent to
participate
The authors hereby declare that the research
material presented in the present study has been conducted
ethically in accordance with the World Medical Association
declaration of Helsinki.
Patient consent for publication
Not applicable.
Competing interests
The authors declare that they have no competing
interest.
References
|
1
|
Zhou ZR, Wang CC, Yang ZZ, Yu XL and Guo
XM: Phyllodes tumors of the breast: Diagnosis, treatment and
prognostic factors related to recurrence. J Thorac Dis.
8:3361–3368. 2016. View Article : Google Scholar : PubMed/NCBI
|
|
2
|
Tan BY, Acs G, Apple SK, Badve S,
Bleiweiss IJ, Brogi E, Calvo JP, Dabbs DJ, Ellis IO, Eusebi V, et
al: Phyllodes tumours of the breast: A consensus review.
Histopathology. 68:5–21. 2016. View Article : Google Scholar : PubMed/NCBI
|
|
3
|
Muller J: About the fine structure and the
forms of pathological tumors. Reimer; Berlin, Germany: pp. 54–57.
1938, (In German).
|
|
4
|
World Health Organization (WHO), . Breast
tumors. WHO classification of tumors. 2. 5th edition. International
Agency for Research on Cancer; Lyon: 2019
|
|
5
|
Kokkali S, Stravodimou A, Duran-Moreno J,
Koufopoulos N, Voutsadakis IA and Digklia A: Chemotherapy and
targeted treatments of breast sarcoma by histologic subtype. Expert
Rev Anticancer Ther. 21:591–604. 2021. View Article : Google Scholar : PubMed/NCBI
|
|
6
|
Bernstein L, Deapen D and Ross KR: The
descriptive epidemiology of malignant cystosarcoma phyllodes tumors
of the breast. Cancer. 71:3020–3024. 1993. View Article : Google Scholar : PubMed/NCBI
|
|
7
|
Khosravi-Shahi P: Management of non
metastatic phyllodes tumors of the breast: Review of the
literature. Surg Oncol. 20:e143–e148. 2011. View Article : Google Scholar : PubMed/NCBI
|
|
8
|
Chaney AW, Pollack A, McNeese MD, Zagars
GK, Pisters PW, Pollock RE and Hunt KK: Primary treatment of
cystosarcoma phyllodes of the breast. Cancer. 89:1502–1511. 2000.
View Article : Google Scholar : PubMed/NCBI
|
|
9
|
Moffat CJ, Pinder SE, Dixon AR, Elston CW,
Blamey RW and Ellis IO: Phyllodes tumours of the breast: A
clinicopathological review of thirty-two cases. Histopathology.
27:205–218. 1995. View Article : Google Scholar : PubMed/NCBI
|
|
10
|
Kapiris I, Nasiri N, A'Hern R, Healy V and
Gui GP: Outcome and predictive factors of local recurrence and
distant metastases following primary surgical treatment of
high-grade malignant phyllodes tumours of the breast. Eur J Surg
Oncol. 27:723–730. 2001. View Article : Google Scholar : PubMed/NCBI
|
|
11
|
Chen WH, Cheng SP, Tzen CY, Yang TL, Jeng
KS, Liu CL and Liu TP: Surgical treatment of phyllodes tumors of
the breast: Retrospective review of 172 cases. J Surg Oncol.
91:185–194. 2005. View Article : Google Scholar : PubMed/NCBI
|
|
12
|
Roa JC, Tapia O, Carrasco P, Contreras E,
Araya JC, Muñoz S and Roa I: Prognostic factors of phyllodes tumor
of the breast. Pathol Int. 56:309–314. 2006. View Article : Google Scholar : PubMed/NCBI
|
|
13
|
Cheng SP, Chang YC, Liu TP, Lee JJ, Tzen
CY and Liu CL: Phyllodes tumor of the breast: The challenge
persists. World J Surg. 30:1414–1421. 2006. View Article : Google Scholar : PubMed/NCBI
|
|
14
|
Fou A, Schnabel FR, Hamele-Bena D, Wei XJ,
Cheng B, El Tamer M, Klein L and Joseph KA: Long-term outcomes of
malignant phyllodes tumors patients: An institutional experience.
Am J Surg. 192:492–495. 2006. View Article : Google Scholar : PubMed/NCBI
|
|
15
|
Taira N, Takabatake D, Aogi K, Ohsumi S,
Takashima S, Nishimura R and Teramoto N: Phyllodes tumor of the
breast: Stromal overgrowth and histological classification are
useful prognosis-predictive factors for local recurrence in
patients with a positive surgical margin. Jpn J Clin Oncol.
37:730–736. 2007. View Article : Google Scholar : PubMed/NCBI
|
|
16
|
Barrio AV, Clark BD, Goldberg JI, Hoque
LW, Bernik SF, Flynn LW, Susnik B, Giri D, Polo K, Patil S and Van
Zee KJ: Clinicopathologic features and long-term outcomes of 293
phyllodes tumors of the breast. Ann Surg Oncol. 14:2961–2970. 2007.
View Article : Google Scholar : PubMed/NCBI
|
|
17
|
Fajdić J, Gotovac N, Hrgović Z, Kristek J,
Horvat V and Kaufmann M: Phyllodes tumors of the breast diagnostic
and therapeutic dilemmas. Onkologie. 30:113–118. 2007.PubMed/NCBI
|
|
18
|
Jang JH, Choi MY, Lee SK, Kim S, Kim J,
Lee J, Jung SP, Choe JH, Kim JH, Kim JS, et al: Clinicopathologic
risk factors for the local recurrence of phyllodes tumors of the
breast. Ann Surg Oncol. 19:2612–2617. 2012. View Article : Google Scholar : PubMed/NCBI
|
|
19
|
simpleBreastcancer.org;
Treatment of Phyllodes Tumors of the Breast. Breastcancer.org,
Suite 201 Ardmore, PA, 2016. https://www.breastcancer.org/symptoms/types/phyllodes/treatmentSeptember
1–2020
|
|
20
|
Gnerlich JL, Williams RT, Yao K, Jaskowiak
N and Kulkarni SA: Utilization of radiotherapy for malignant
phyllodes tumors: Analysis of the National cancer data base,
1998–2009. Ann Surg Oncol. 21:1222–1230. 2014. View Article : Google Scholar : PubMed/NCBI
|
|
21
|
American Cancer Society, . Phyllodes
Tumors of the Breast. American Cancer Society, Inc.; Atlanta, GA:
2019, https://www.cancer.org/cancer/breast-cancer/non-cancerous-breast-conditions/phyllodes-tumors-of-the-breast.htmlSeptember
1–2020
|
|
22
|
Macdonald OK, Lee CM, Tward JD, Chappel CD
and Gaffney DK: Malignant phyllodes tumor of the female breast:
Association of primary therapy with cause-specific survival from
the Surveillance, Epidemiology, and End Results (SEER) program.
Cancer. 107:2127–2133. 2006. View Article : Google Scholar : PubMed/NCBI
|
|
23
|
Barth RJ Jr, Wells WA, Mitchell SE and
Cole BF: A prospective, multi-institutional study of adjuvant
radiotherapy after resection of malignant phyllodes tumors. Ann
Surg Oncol. 16:2288–2294. 2009. View Article : Google Scholar : PubMed/NCBI
|
|
24
|
Belkacémi Y, Bousquet G, Marsiglia H,
Ray-Coquard I, Magné N, Malard Y, Lacroix M, Gutierrez C, Senkus E,
Christie D, et al: Phyllodes tumor of the breast. Int J Radiat
Oncol Biol Phys. 70:492–500. 2008. View Article : Google Scholar : PubMed/NCBI
|