Introduction
Psoriasis is an autoimmune disease with chronic
course, having relapse and remission periods and a variable
European country prevalence from 1.3 to 11.4% (1-3).
Psoriasis may be associated with human
immunodeficiency virus (HIV) infection, but the prevalence of the
viral infection does not differ significantly from that of the
general population. Although it is not a characteristic
presentation of the acquired immunodeficiency syndrome (AIDS), the
evolution of psoriasis can be more severe in patients with HIV
(4-6).
HIV infection can be a triggering factor for
psoriasis development and a first sign of infection in genetically
predisposed patients having the CW*0602 haplotype
(7). In these patients, psoriasis
lesions could improve once immune reconstruction has taken place
after antiretroviral therapy, reaching even spontaneous remission.
That being said, some guttate and vulgar forms of psoriasis can
worsen in the advanced stages of AIDS (4).
The pathogenesis of associating psoriasis to
HIV-infected patients is paradoxical and is explained by the
imbalance between immune cellular components. T lymphocytes have
the main purpose of mediating the excessive inflammatory response
that takes place in psoriasis, while HIV infection is characterized
by T-lymphocyte depletion (a state which renders the body
susceptible to various opportunistic infections) (8). The cytokine profile of the two
diseases is also different, psoriasis having a Th1 pattern
[interleukin-2 (IL2), interferon-γ (INF-γ), tumor necrosis factor-α
(TNF-α)], while HIV infection has a Th2 pattern (IL-2, IL-5, IL-10)
(9-11).
Psoriasis biological therapies which target
lymphocyte Th1 contribute to the severity of HIV infection
progression, while antiretroviral therapy has the capacity to
improve psoriatic lesions. However, some case reports have revealed
that antiretroviral therapy initiation in severe immune-suppressed
patients, especially when T-lymphocyte CD4+ levels are
below 50 cells/mm3, could be associated with a temporary
exacerbation of psoriasis, within the immune reconstruction
inflammatory syndrome (12).
Available therapies for HIV-associated psoriasis are
classified into 3 categories, producing results that vary from
complete remission to lack of any response. Local therapy uses tar
products, emollients, salicylic acid, corticosteroids and
retinoids. Ultraviolet (UV) phototherapy is controversial. Systemic
therapy is based on acitretin, methotrexate (MTX) and cyclosporine,
anti-TNF-α biologic therapy. MTX is rarely used in HIV patients due
to its immune-modulating effect, renal toxicity or the folate
metabolism (13-16).
Previous studies have revealed that the purpose of
Th17 lymphocytes in natural and adaptive immunity in skin and
mucous membranes, is their involvement in the pathogenesis of
autoimmune, neoplastic and infectious processes at this level. Th17
lymphocytes are a Th-lymphocyte subset, which produce cytokines
that act on epithelial cells, thus becoming a target for research
in patients with both psoriasis and HIV infection, in the hopes of
finding new therapies (13-15).
Case report
The case of a 34-year-old male, unqualified
construction worker from a rural environment with a primary school
education level, is presented, who addressed the ‘Sf. Cuvioasa
Parascheva’ Clinical Hospital of Infectious Diseases (Galati,
Romania) for the evaluation, monitoring and treatment of his recent
HIV infection. For over 10 years the patient has been the partner
of a positive HIV patient, with whom the patient has two
seropositive HIV children, systematically breaching the safe sex
measures. His last HIV testing, two years ago, was negative. The
patient was a chronic smoker (23 pack-years) and alcohol consumer
(4 units/day). A total of 18 years ago, the patient suffered
multiple trauma involving cranial-cerebral injuries and coma, being
hospitalized for over a month. A total of 7 years prior to the HIV
diagnosis (when the patient was 28), the patient received the
clinical diagnosis of psoriasis and followed various topical
treatments. The family history is negative for psoriasis and the
patient suffers from low self-image with poor quality of life due
to the appearance and discomfort of the psoriatic lesions.
Upon initial clinical examination, when the patient
was diagnosed as being HIV-positive, his general health status was
favorable, the patient was afebrile with a body mass index (BMI) of
21,2 kg/m2 and blood pressure of 150/100 mmHg, with
rhythmic heartbeats and no additional heart sounds; the lung sounds
were normal, as was the neurologic examination. Mucosal examination
revealed candidiasis lesions. Onychomycosis and squamous scalp
lesions were also identified, and the skin examination revealed
disseminated vulgar psoriasis lesions. Laboratory data revealed an
CD4+ T-lymphocyte number of 466 cells/mm3, a
ribonucleic acid (RNA)-HIV viral load of 146,000 copies/ml, with
negative serologic examination for hepatitis B virus (HBV),
hepatitis C virus (HCV), cytomegalovirus (CMV), toxoplasma and
syphilis. The remaining hematological and biochemical
investigations were in the normal ranges, while no significant
lesions were found on the thoracic X-ray.
The patient received antiretroviral treatment with
Triumeq (dolutegravir + lamivudine + abacavir), registering a
favorable viral response with complete viral suppression after 12
weeks. The treatment was well tolerated, but the pre-existent
psoriatic lesions treated with topical medication became more
extended and accentuated the inflammatory response with a Psoriasis
Area and Severity Index (PASI) score of 21,2. The patient then
received systemic treatment with MTX as 15 mg/week, for 12 weeks,
with major improvement of lesions and partial remission. Under
strict biologic monitoring, MTX treatment was continued with the
same dosage for a year, but the lesions reappeared, coinciding with
a three-fold increase in alanine aminotransferase (ALT) levels. The
laboratory changes during MTX treatment (from May 2019 to September
2020) are highlighted in Table I,
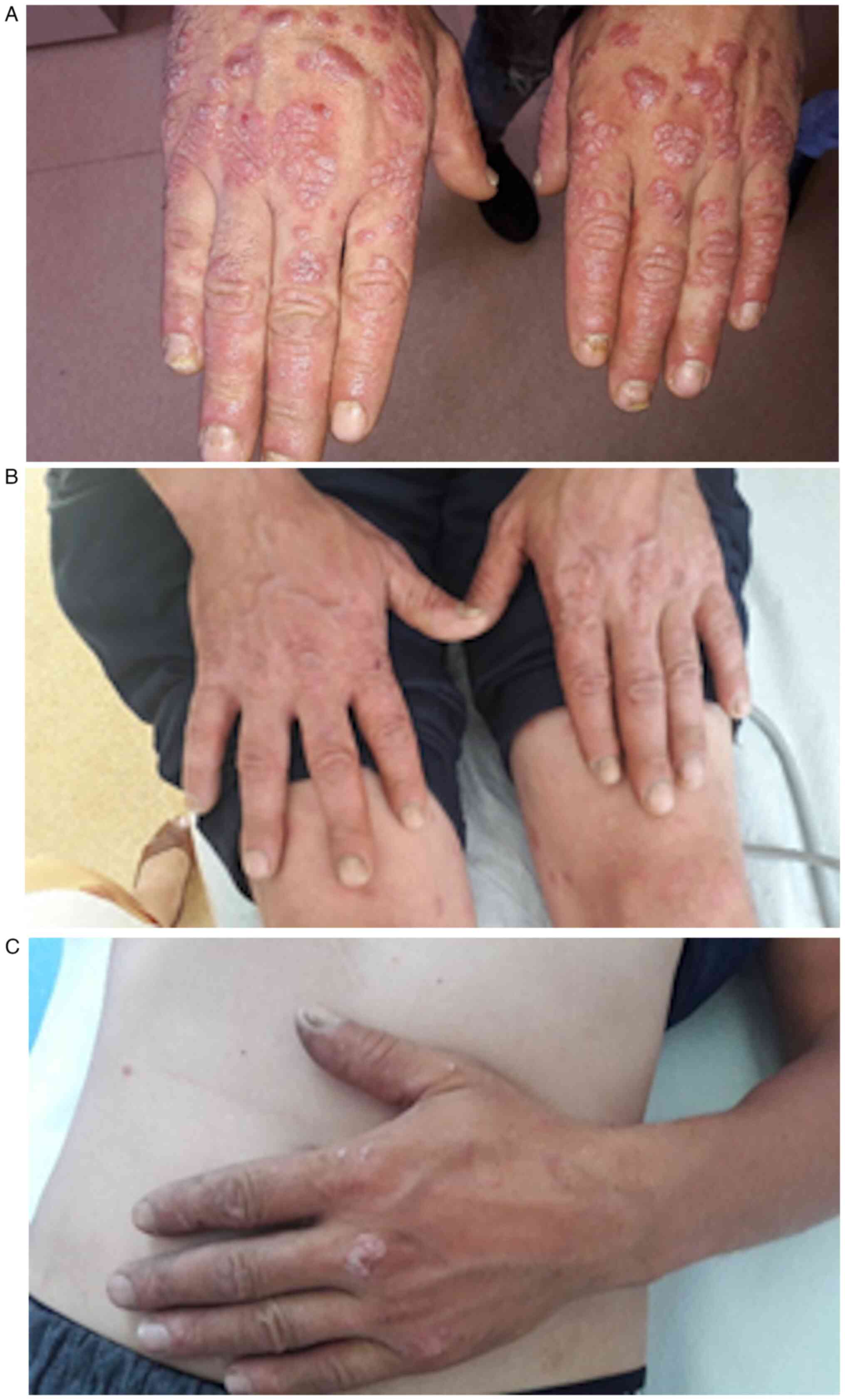
along with the evolution of hand skin lesions in Fig. 1.
 | Table IBiologic outcome in an HIV-positive
patient suffering from psoriasis, under MTX treatment. |
Table I
Biologic outcome in an HIV-positive
patient suffering from psoriasis, under MTX treatment.
| Timeline | February 2019 | May 2019 | September 2019 | September 2020 |
|---|
| Hb (g/dl) | 15.2 | 15.4 | 14.5 | 15.5 |
| WBC
(cells/mm3) | 8,110 | 6,310 | 9,600 | 11,000 |
| ALT (UI/l) | 24.2 | 31 | 24.6 | 96.3 |
| AST (UI/l) | 22 | 28.2 | 26.4 | 66.8 |
| Creatinine
(mg/dl) | 0.82 | 0.79 | 0.74 | 0.75 |
| T-lymphocyte CD4
(cells/mm3) | 466 | 581 | 450 | 500 |
| ARN-HIV
(copies/ml) | 146,000 | Undetectable | Undetectable | Undetectable |
| TRIUMEQ | √ | √ | √ | √ |
| MTX | | √ | √ | √ |
| PASI (%) | 21.2 | 19 | 17 | 16.2 |
Discussion
MTX is an immune suppressive drug frequently used in
autoimmune and inflammatory dermatological diseases (17,18).
Current treatment guidelines recommend MTX as
first-line systemic treatment in any form of psoriasis which cannot
be controlled by topical therapy, which significantly affects the
quality of life of the patient and fulfills one of the following
conditions: is extensive (PASI >10%); is localized, but is
associated with significant functional deterioration; or
phototherapy cannot be used, is inefficient or has led to a fast
relapse. Concerning severity scores after MTX use for 12-24 weeks,
randomized prospective studies conducted on large cohorts of
patients suffering from psoriasis, proved to have similar efficacy
as biological therapies with adalimumab, briakinumab, infliximab,
but also as with cyclosporine (17).
MTX use in HIV patients is associated with a high
risk for opportunistic infections. Medical literature data has
reported a case of toxic encephalopathy which improved after
cessation of MTX (19). In another
study, 2 out of the 4 patients treated with MTX suffered from
pneumocystis pneumonia, although they received prophylaxis for
opportunistic infections prior to starting treatment (19). Having associated infections with
HBV, HCV or latent tuberculosis are absolute contraindications for
MTX use (19,20), but in our case the serologic markers
of the patients for these infections were negative.
The medical literature has few data concerning the
efficacy of systemic therapies in HIV-positive patients suffering
from psoriasis, most recommendations exerting caution in their use.
However, the American Academy of Dermatology collected data on the
use of TNF-α inhibitors (etanercept, adalimumab and infliximab) in
HIV-positive patients suffering from psoriatic arthritis who did
not respond to the combination treatment with MTX and cyclosporine,
adherent to the antiretroviral therapy with encouraging results
(20,21). Ustekinumab is a p40-IL 12/23
inhibitor that was used for refractory forms of HIV-associated
psoriasis, without registering any adverse effects in the first
months of treatment (20,22).
Concerning certolizumab, a TNF-α inhibitor and an
approved biologic drug for plaque psoriasis and for psoriatic
arthritis, this is an agent that could be used as systemic
treatment in HIV-positive patients suffering from psoriasis, having
an undetectable viral load and under highly active antiretroviral
therapy (HAART) (23,24). Risankizumab and guselkumab are both
biologicals approved for targeting the p19 subunit of IL-23
(IL23/p19 inhibitors), used in moderate to severe plaque psoriasis.
The advantage of using these two drugs would be an improved safety
profile (as compared with TNF-α inhibitors) (23,25).
Although guselkumab is reported to be safe and effective in
HIV-positive patients suffering from psoriasis, on condition of
close monitoring, there remains insufficient data for guselkumab
and risankizumab use in these particular patients. These three
agents could have positive effects on the T-lymphocyte
CD4+ counts and on the viral load (17,23,25).
The case features were as follows: i) In spite of
repeated unprotected sexual contact, the patient suffering from
psoriasis was not infected with HIV for a long time, suggesting a
strong immune response with a particular genetic determinism; ii)
psoriasis was diagnosed prior to HIV and its onset was at a young
age, corresponding most probably to type I psoriasis; iii) the
genetic profile CW*0602 remained uninvestigated, having
no family links to other cases of psoriasis; iv) the evolution of
psoriasis could be favored by external factors including alcohol,
smoking, excessive sun exposure, hygiene deficit, which were not
corrected during therapy; v) antiretroviral treatment was followed
by immune recovery and complete viral suppression; vi) psoriasis
exacerbation after the first weeks of efficient antiviral treatment
could correspond to a rare paradoxical inflammatory syndrome of
immune reconstruction; vii) topical therapy resistance and
controversies regarding the efficacy and safety of phototherapy in
the HIV-positive patient justified the decision of using MTX as
first-line systemic treatment; viii) MTX use in the patient with
antiviral therapy-controlled HIV infection, was well tolerated and
efficient, with a partial remission of psoriasis lesions in the
first 12 weeks; and ix) re-emergence of lesions after one year of
continuation of MTX could be explained by the development of
treatment resistance, making it necessary to apply or associate
other therapeutic options.
In conclusion, in the context of HIV infection,
progression of psoriasis may be an expression of specific viral
pathogenic immune deficiency, but also of inflammatory processes
which accompany immune reconstruction after antiretroviral therapy.
MTX use for severe psoriasis treatment was an efficient and safe
solution for dermatological lesion control in the HIV-infected
patient, but the benefits were limited to only one year. Biological
therapies are the future options for psoriasis treatment after MTX
failure, but they require rigorous monitoring for adverse effects,
CD4+ lymphocytes and viral levels.
Acknowledgements
Not applicable.
Funding
Funding: The present study was supported by ‘Dunarea de Jos’
University of Galati.
Availability of data and materials
The datasets used and/or analyzed during the current
study are available from the corresponding author on reasonable
request.
Authors' contributions
MA and AAA confirm the authenticity of all the raw
data. MA, AAA, EN, SF, LA and ALT were major contributors in
writing the manuscript, were involved in all the stages of the
study, contributed to the conception and design of the work, as
well as revising it and have also contributed in analyzing the data
for the study. MA, AAA, EN, SF, LA and ALT revised it for important
intellectual content. MA, AAA, EN, SF, LA and ALT approved the
final version to be published. All authors read and approved the
final manuscript and agree to be accountable for all aspects of the
work in ensuring that questions related to the accuracy or
integrity of any part of the work are appropriately investigated
and resolved.
Ethics approval and consent to
participate
Ethics approval was granted by the Ethics Committee
of the ‘Sf. Cuvioasa Parascheva’ Clinical Hospital of Infectious
Diseases (Galati, Romania), with the decision no. 31 from
16.03.2021. The patient also provided written informed consent for
participation in the study.
Patient consent for publication
The patient provided written informed consent for
the publication of any associated data and accompanying figure.
Competing interests
The authors declare that they have no competing
interests.
References
|
1
|
Michalek IM, Loring B and John SM: A
systematic review of worldwide epidemiology of psoriasis. J Eur
Acad Dermatol Venereol. 31:205–212. 2017.PubMed/NCBI View Article : Google Scholar
|
|
2
|
Batani A, Brănișteanu DE, Ilie MA, Boda D,
Ianosi S, Ianosi G and Caruntu C: Assessment of dermal papillary
and microvascular parameters in psoriasis vulgaris using in
vivo reflectance confocal microscopy. Exp Ther Med.
15:1241–1246. 2018.PubMed/NCBI View Article : Google Scholar
|
|
3
|
Caruntu C, Boda D, Căruntu A, Rotaru M,
Baderca F and Zurac S: In vivo imaging techniques for psoriatic
lesions. Rom J Morphol Embryol. 55 (3 Suppl):S1191–S1196.
2014.PubMed/NCBI
|
|
4
|
Dlova NC and Mosam A: Inflammatory
noninfectious dermatoses of HIV. Dermatol Clin. 24439–448.
(VI)2006.PubMed/NCBI View Article : Google Scholar
|
|
5
|
Mamkin I, Mamkin A and Ramanan SV:
HIV-associated psoriasis. Lancet Infect Dis. 7(496)2007.PubMed/NCBI View Article : Google Scholar
|
|
6
|
Jordaan HF: Common skin and mucosal
disorders in HIV/AIDS. S Afr Fam Pract. 50:14–23. 2008.
|
|
7
|
Cedeno-Laurent F, Gómez-Flores M, Mendez
N, Ancer-Rodríguez J, Bryant JL, Gaspari AA and Trujillo JR: New
insights into HIV-1-primary skin disorders. J Int AIDS Soc.
14(5)2011.PubMed/NCBI View Article : Google Scholar
|
|
8
|
Fife DJ, Waller JM, Jeffes EW and Koo JY:
Unraveling the paradoxes of HIV-associated psoriasis: A review of
T-cell subsets and cytokine profiles. Dermatol Online J.
13(4)2007.PubMed/NCBI
|
|
9
|
Friedrich M, Krammig S, Henze M, Döcke WD,
Sterry W and Asadullah K: Flow cytometric characterization of
lesional T cells in psoriasis: Intracellular cytokine and surface
antigen expression indicates an activated, memory/effector type 1
immunophenotype. Arch Dermatol Res. 292:519–521. 2000.PubMed/NCBI View Article : Google Scholar
|
|
10
|
Mallon E and Bunker CB: HIV-associated
psoriasis. AIDS Patient Care STDS. 14:239–246. 2000.PubMed/NCBI View Article : Google Scholar
|
|
11
|
Niculet E, Radaschin DS, Nastase F,
Draganescu M, Baroiu L, Miulescu M, Arbune M and Tatu AL: Influence
of phytochemicals in induced psoriasis (review). Exp Ther Med.
20:3421–3424. 2020.PubMed/NCBI View Article : Google Scholar
|
|
12
|
Cheaito MA, Khalifeh M, Jaafar B and Rizk
N: Immune reconstitution inflammatory syndrome presenting as
psoriasis after initiating antiretroviral therapy: A case-report. J
Infect Dis Ther. 6(387)2018.
|
|
13
|
Saketkoo LA and Espinoza LR: Impact of
biologic agents on infectious diseases. Infect Dis Clin North Am.
20:931–961, viii. 2006.PubMed/NCBI View Article : Google Scholar
|
|
14
|
Boda D, Negrei C, Nicolescu F and Badalau
C: Assessment of some oxidative stress parameters in methotrexate
treated psoriasis patients. Farmacia. 62:704–710. 2014.
|
|
15
|
Caruntu C, Boda D, Dumitrascu G,
Constantin C and Neagu M: Proteomics focusing on immune markers in
psoriatic arthritis. Biomark Med. 9:513–528. 2015.PubMed/NCBI View Article : Google Scholar
|
|
16
|
Teh YC, Robinson S, Tan WC, Kwan Z and
Tang MM: Psoriasis patients with human immunodeficiency virus
infection: Data from the malaysian psoriasis registry. Malaysian J
Dermatol. 46:1–10. 2021.
|
|
17
|
Warren RB, Weatherhead SC, Smith CH, Exton
LS, Mohd Mustapa MF, Kirby B and Yesudian PD: British association
of dermatologists' guidelines for the safe and effective
prescribing of methotrexate for skin disease 2016. Br J Dermatol.
175:23–44. 2016.PubMed/NCBI View Article : Google Scholar
|
|
18
|
Ezhilarasan D: Hepatotoxic potentials of
methotrexate: Understanding the possible toxicological molecular
mechanisms. Toxicology. 458(152840)2021.PubMed/NCBI View Article : Google Scholar
|
|
19
|
Kaushik SB and Lebwohl MG: Psoriasis:
Which therapy for which patient: Focus on special populations and
chronic infections. J Am Acad Dermatol. 80:43–53. 2019.PubMed/NCBI View Article : Google Scholar
|
|
20
|
Queirós N and Torres T: HIV-associated
psoriasis. Actas Dermosifiliogr (Engl Ed). 109:303–311.
2018.PubMed/NCBI View Article : Google Scholar : (In English,
Spanish).
|
|
21
|
Gallitano SM, McDermott L, Brar K and
Lowenstein E: Use of tumor necrosis factor (TNF) inhibitors in
patients with HIV/AIDS. J Am Acad Dermatol. 74:974–980.
2016.PubMed/NCBI View Article : Google Scholar
|
|
22
|
Bardazzi F, Magnano M, Campanati A,
Loconsole F, Carpentieri A, Potenza C, Bernardini N, Di Lernia V,
Carrera C, Raone B, et al: Biologic therapies in HIV-infected
patients with psoriasis: An Italian experience. Acta Derm Venereol.
97:989–990. 2017.PubMed/NCBI View Article : Google Scholar
|
|
23
|
Lambert JLW, Segaert S, Ghislain PD,
Hillary T, Nikkels A, Willaert F, Lambert J and Speeckaert R:
Practical recommendations for systemic treatment in psoriasis in
case of coexisting inflammatory, neurologic, infectious or
malignant disorders (BETA-PSO: Belgian evidence-based treatment
advice in psoriasis; part 2). J Eur Acad Dermatol Venereol.
34:1914–1923. 2020.PubMed/NCBI View Article : Google Scholar
|
|
24
|
Esposito M, Carubbi F, Giunta A, Alunno A,
Giacomelli R and Fargnoli MC: Certolizumab pegol for the treatment
of psoriatic arthritis and plaque psoriasis. Expert Rev Clin
Immunol. 16:119–128. 2020.PubMed/NCBI View Article : Google Scholar
|
|
25
|
Yang K, Oak ASW and Elewski BE: Use of
IL-23 inhibitors for the treatment of plaque psoriasis and
psoriatic arthritis: A comprehensive review. Am J Clin Dermatol.
22:173–192. 2021.PubMed/NCBI View Article : Google Scholar
|