Introduction
Oral carcinoma, which falls in the head and neck
cancer category, represents one of the six most common types of
cancer worldwide (1). Oral tongue
squamous cell carcinoma (OTSCC) is the most common type of oral
cancer, and the incidence of OTSCC has increased by 1.9% annually
between 1975 and 2007, particularly among young adults (2). In the United States, an estimated
16,100 novel cases of OTSCC and 2,290 OTSCC-related fatalities are
expected in 2014 (3). Even with
the combination of surgery, chemotherapy and radiation, the overall
five-year survival rate of OTSCC is only 50–60% (2). Thus, the identification of novel
biomarkers is critical to OTSCC diagnosis and targeted
treatment.
Autophagy is a bulk degradation process in which
cytosolic misfolded proteins and damaged organelles are sequestered
into autophagosomes and degraded by lysosomes to maintain organelle
function and protein quality (4).
Increased autophagy is a primary response to cellular stress that
is an attempt to survive unfavourable conditions, such as nutrient
depletion or hypoxia (5–7). Notably, autophagy is also involved in
an array of biological and pathophysiological conditions, including
tumourigenesis, immunity and embryonic development (8). Beclin-1 is the first identified
mammalian autophagy gene (8).
Previous studies have demonstrated that Beclin-1 is a
haploinsufficient tumour suppressor; early embryonic lethality is
observed in mice with biallelic loss of Beclin-1, and an increased
rate of malignant tumours is observed in Beclin1+/− mice
(9,10). Decreased Beclin-1 protein
expression was confirmed in a series of human tumours, including
hepatocellular carcinoma, ovarian carcinoma and laryngeal squamous
cell carcinoma (11–13). By contrast, other studies have
demonstrated that increased Beclin-1 expression is more frequently
detected in colorectal carcinoma, gastric carcinoma, cutaneous
squamous cell carcinoma and pancreatic ductal adenocarcinoma
compared with the matched non-cancerous tissue of the same patient
(14–18), which suggests that the function of
Beclin-1 in tumourigenesis may vary among different tumour types
(19,20). Furthermore, whether Beclin-1
possesses autophagy-independent functions during tumourigenesis is
now under investigation (5,21).
OTSCC is a type of solid tumour; thus, OTSCC cancer
cells often face nutrient deprivation and hypoxia, which leads to
metabolic stress (2). Therefore,
it was hypothesised that Beclin-1 is involved in the development
and progression of OTSCC. The present study aimed to investigate
Beclin-1 expression and its significance in OTSCC.
Materials and methods
Tissue specimens and patients
For reverse transcription-quantitiative polymerase
chain reaction (RT-qPCR) and western blot analysis, 14 OTSCC
tissues and matched adjacent non-cancerous tongue tissues (at a
distance >2 cm from the tumour) were collected from patients who
underwent half-tongue resection between May and July 2010. In
addition, 133 paraffin-embedded samples of OTSCC specimens were
collected between January 2000 and December 2002 for
immunohistochemical assay. All tissue samples were collected prior
to chemotherapy or radiotherapy and were histologically and
clinically diagnosed at the Third Affiliated Hospital of Kunming
Medical University (Kunming, China). The tumour stage of each
patient was classified according to the 2010 AJCC staging system
(22). The median follow-up time
of patients whose tissues were subjected to an immunohistochemical
assay was 67 months at the time of analysis and ranged from 12 to
124 months. This study was approved by the Ethics Committee of the
Third Affiliated Hospital of Kunming Medical University. The
samples were collected after receiving informed consent from the
patients.
RT-qPCR
The mRNA of OTSCC (NTEC1, TCA8113, TSCCA, SCC-9,
SCC-25 and CAL-27 cells) and matched adjacent noncancerous tissues
was purified using TRIzol Reagent (Invitrogen, Thermo Fisher
Scientific, Inc., Waltham, MA, USA), and 2 µg of each sample
was reverse transcribed using a TIAN Script kit (Invitrogen, Thermo
Fisher Scientific, Inc.). The following primers were used: Sense:
5′-GGTGTCTCTCGCAGATTCATC-3′ and antisense:
5′-TCAGTCTTCGGCTGAGGTTCT-3′ for Beclin-1; and sense:
5′-TGTTGCCATCAATGACCCCTT-3′ and antisense 5′-CTCCACGACGTACTCAGCG-3′
for glyceraldehyde 3-phosphate dehydrogenase (GAPDH), which was
used as an endogenous control. All reactions were run in triplicate
in three independent experiments. All primers were synthesized by
Invitrogen, Thermo Fisher Scientific, Inc. PCR reactions were
performed on a PTC-200 PCR system (Bio-Rad Laboratories, Hercules,
CA, USA) using the following cyclical procedure: 10 min at
94°C, followed by 45 cycles of 15 sec at 94°C, 30 sec
at 54°C, 30 sec at 72°C, and a final cycle at
72°C for 10 min. For OTSCC cells, RT-qPCR and data
collection were performed using an ABI PRISM 7900 HT sequence
detection system (Applied Biosystems, Thermo Fisher Scientific,
Inc.).
Western blot analysis
Cells (NTEC1, TCA8113, TSCCA, SCC-9, SCC-25 and
CAL-27 cells, and patients paired tissue cells) were lysed with 1X
sodium dodecyl sulphate (SDS) sample buffer (62.5 mmol/l Tris-HCl,
2% SDS, 10% glycerol and 5% 2-mercaptoethanol). The protein
concentration was determined using a bicinchoninic acid protein
assay. A total of 25 µg protein was separated
electrophoretically in 9% SDS-polyacrylamide gel electrophoresis,
transferred to polyvinylidene fluoride membranes and incubated
sequentially with primary rabbit monoclonal anti-Beclin-1 (cat. no.
2026-1; 1:4,000, Epitomics Inc., Burlingame, CA, USA), mouse
monoclonal anti-LC3 (cat. no. AM1800a; 1:500, Abgent, San Diego,
CA, USA), mouse monoclonal anti-p62/SQSTM1 (cat. no. sc-28359;
1:1,000, Santa Cruz Biotechnologies Inc., Santa Cruz, CA, USA), for
2 h at room temperature. After washing with TBS-T (Bio Basic Inc.,
Markham, ON, Canada), the membrane was incubated with a goat
anti-mouse IgG (cat. no. 31430; 1:4,000) and goat-anti-rabbit IgG
(cat. no. 31460; 1:3,000) secondary antibodies (Thermo Fisher
Scientific, Inc. The membrane was washed and protein was detected
using enhanced chemiluminescence reagent (Cell Signaling
Technology, Beverly, MA, USA) and XAR film (Eastman Kodak Company,
Rochester, NY, USA) according to the manufacturer's instructions.
The membranes were then stripped and probed with an anti-GAPDH
mouse monoclonal antibody (1:3,000, Santa Cruz Biotechnology, Inc.,
Dallas, TX, USA) to confirm equal loading of the samples. The
western blot bands were scanned and were analyzed using the
Quantity One 4.6.7 program (Bio-Rad Laboratories).
Immunohistochemistry assay
In brief, paraffin-embedded OTSCC specimens were cut
into 4-µm sections and incubated at 65°C for 30 min.
The sections were washed with xylene and rehydrated. Sections were
submerged for 2 min into an EDTA buffer at 95°C and 90 kPa
for antigen retrieval and treated with 3% hydrogen peroxide in
methanol, followed by incubation with 1% rabbit serum albumin
(Zhongshan Golden Bridge Biotechnology, Co., Ltd.). The specimens
were incubated overnight at 4°C with anti-Beclin-1 (1:200,
Epitomics Inc.). For the negative control, the primary antibody was
replaced with the non-immune rabbit IgG (Zhongshan Golden Bridge
Biotechnology, Co., Ltd.). of the same isotype. Immunohistochemical
staining to determine the expression of Beclin-1 revealed diffuse,
fine, granular cytoplasmic staining under an XSZ-H microscope
(Chongqing Optical & Electrical Instrument Co., Ltd.,
Chongqing, China). The proportion of cells expressing Beclin-1 was
scored as follows: 0, no expression; 1, 0–25%; 2, 26–50%; and 3,
>50%. The intensity of cell staining was scored as either 0 (no
expression), 1 (yellow) or 2 (brown). The intensity score and
proportion score were added to yield the total score, which was
divided into no/low expression (0 to 2) or high expression (3 to
5).
Cell lines and cell culture
The NTEC1 normal tongue epithelial cell line was
established by culturing normal tongue squamous epithelium from a
healthy patient in keratinocyte/serum-free medium (Invitrogen,
Thermo Fisher Scientific, Inc.). This cell line was a gift from
Professor Musheng Zeng (Sun Yat-sen University Cancer Centre,
Guangzhou, China). CAL-27, SCC-25 and SCC-9 OTSCC cell lines were
purchased from the American Type Culture Collection (Manassas, VA,
USA) and Tca8113 and TSCCA cells were obtained from the Committee
of the Type Culture Collection of the Chinese Academy of Sciences
(Shanghai, China). With the exception of CAL-27, which was cultured
in Dulbecco's modified Eagle's medium (Thermo Scientific, Inc.)
supplemented with 10% foetal bovine serum (FBS, Thermo Fisher
Scientific, Inc.), all cell lines were cultured in RPMI-1640
(Thermo Scientific, Inc.) supplemented with 5% FBS. All cells were
cultured in penicillin (100 U/ml) and streptomycin (100 U/ml) at
37°C in a humidified 5% CO2 incubator.
Plasmids and transfection
For the Beclin-1 expression plasmid, the full-length
coding region of Beclin-1 cDNA was amplified by RT-qPCR, and the
digested and purified PCR products were directly cloned into a
lentivirus vehicle sinhcmv-mcs (r)-pre-cppt-IG (a gift from
Professor Erik Zheng, Sun Yat-sen University Cancer Centre). The
same method was used to construct a full-length LC3 expression
plasmid using a pEGF vector (Invitrogen, Thermo Fisher Scientific,
Inc.) to generate pEGF-C2-LC3. The primer sequences of the
full-length coding region were as follows: Sense:
5′-CGCGGATCCATGGAAGGGTCTAAGACGT-3′ and antisense:
5′-CGGAATTCTCATTTGTTATAAAATTGTGAfor Beclin-1′; and sense:
5′-GAAGATCTTCATGCCCTCAGACCGGCC-3′ and antisense:
5′-CGGAATTCTCAGAAGCCGAAGGTTTCCT-3′ for LC3. All plasmids expressed
enhanced green fluorescent protein (GFP) and were verified by
sequencing. For the Beclin-1 overexpression plasmid, stably
transfected cell lines were generated by lentivirus infection and
selected using flow cytometry according to the manufacturer's
instructions. The LC3 expression plasmid was transfected into OTSCC
cell lines (TCA8113 and TSCCA) using Lipofectamine 2000
(Invitrogen, Thermo Fisher Scientific, Inc.) according to the
manufacturer's instructions.
MTT assay
The cell growth and viability of the stable OTSCC
cell lines (TCA8113 and TSCCA cells) were assessed by using an MTT
assay. Approximately 3,000 cells/well were seeded in a 96-well
plate for 6 duplicate wells with different drug concentrations. The
MTT assay was performed on days 1–5. After incubation, 20 µl
of 5 mg/ml MTT (Sigma-Aldrich, St. Louis, MO, USA) was added to
each well, followed by incubation for 4 h. After discarding the
medium carefully, formazan crystals were dissolved in 150 µl
dimethyl sulfoxide. The optical density was measured with a
microplate spectrophotometer (Bio-Rad Laboratories) at 490 nm.
Absorbance values were normalised to the percentage survival. Each
experiment was performed in triplicate.
GFP LC3 puncta analysis
For analysis of GFP LC3 puncta in cells
overexpressing Beclin-1 and control cells, the cells were observed
under a fluorescence microscope (×400) and representative cells
were selected and photographed. The number of GFP-LC3 puncta per
cell was quantified, and presented as the mean ± standard error of
the mean from 50 randomly selected cells.
Colony formation assay
Cells (200/well; TCA8113 and TSCCA) were counted and
plated in triplicate in six-well plates and were cultured with
RPMI-1640 culture medium for ~10 days until the majority of the
colonies had expanded to >50 cells. The plates were triple
washed with cold phosphate-buffered saline, fixed in pre-chilled
methanol for 10 min, and dyed with 0.5% crystal violet for 5 min at
room temperature. After washing to remove excess stain, the plates
were photographed. Images were analysed using Image J 1.42 software
(National Institutes of Health, Bethesda, MD, USA), according to
the manufacturer's instructions. At least three independent
experiments were performed for each assay.
Soft-agar anchorage-independent growth
assay
For the bottom layer, six-well plates were coated
with a 0.6% agar in medium supplemented with 20% FBS. For the top
layer, 5,000 cells were prepared in 0.3% agar with 10% FBS and
seeded in triplicate. The plates were then incubated at 37°C
in a humidified 5% CO2 incubator for two weeks until
colonies had formed. Each experiment was repeated at least three
times. Colonies were photographed (final magnification ×200) under
a phase-contrast microscope, and colonies >50 mm in diameter
were counted under a light microscope.
Statistical analysis
All statistical analyses were performed using SPSS
16.0 statistical software package (SPSS Inc., Chicago, IL, USA).
The χ2 test for proportions was used to analyse
the correlation between Beclin-1 expression and the
clinicopathologic features of OTSCC. Survival curves were plotted
using the Kaplan-Meier method and compared using the log-rank test.
P<0.05 was considered to indicate a statistically significant
difference.
Results
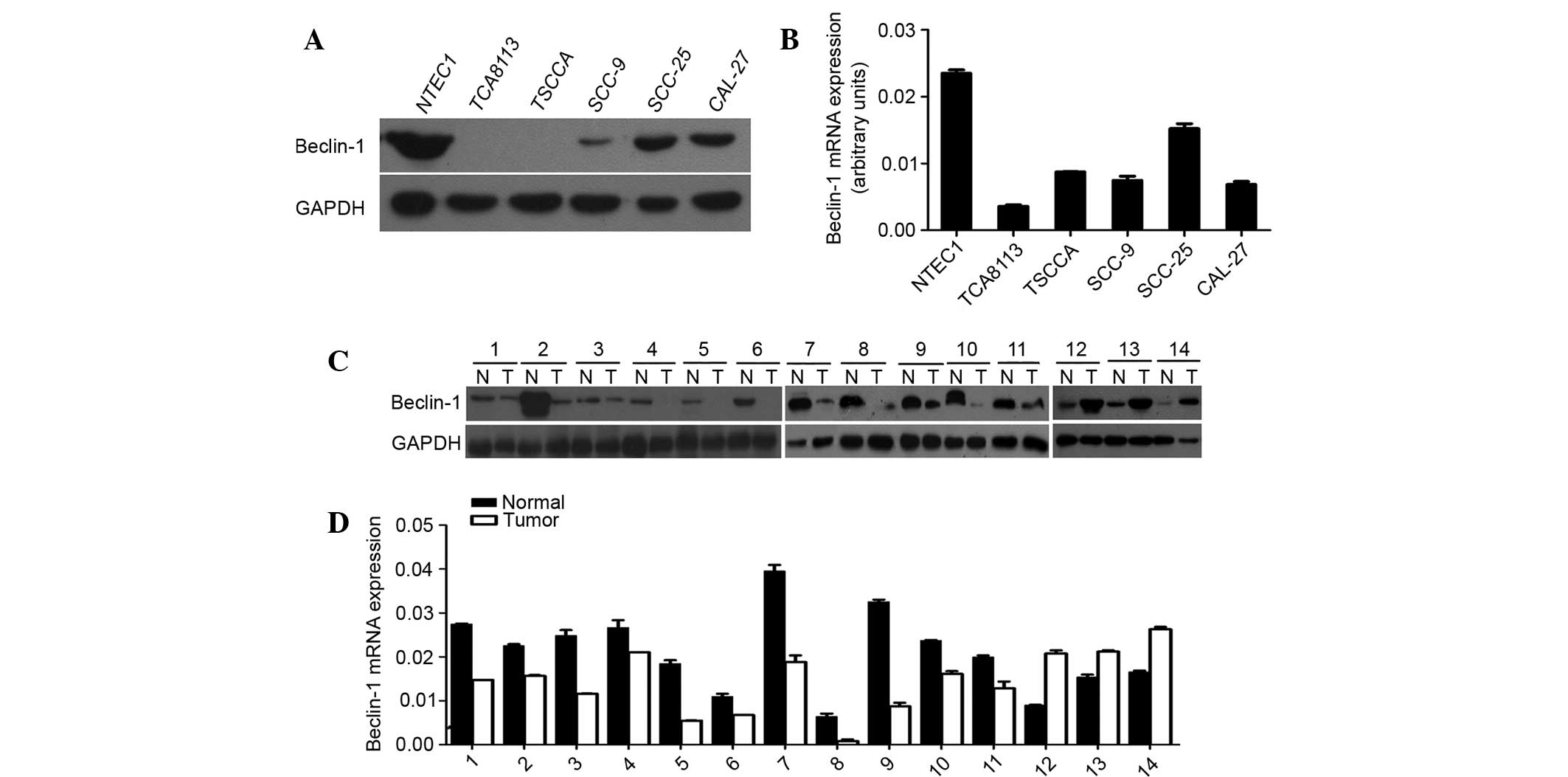
Decreased expression of Beclin-1 in fresh
OTSCC tissues and cell lines
The mRNA and protein expression of Beclin-1 were
decreased in 78.6% of OTSCC tissues and cell lines relative to the
matched adjacent noncancerous tissues and the NTEC1 normal tongue
epithelial cell line, respectively (Fig. 1).
Correlation between Beclin-1 expression
and the clinicopathological features and prognosis of patients with
OTSCC
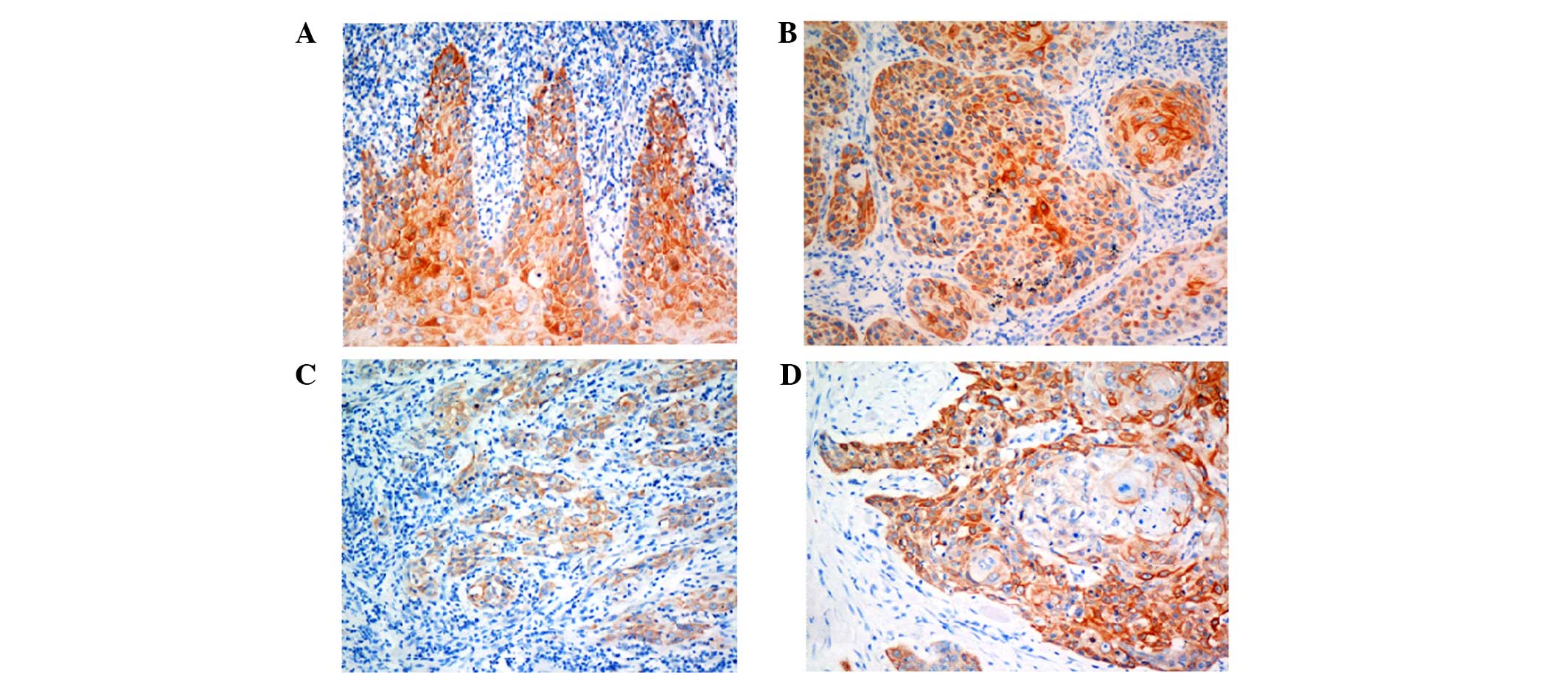
To further verify the expression of Beclin-1, an
immunohistochemical assay was performed on 133 OTSCC specimens. As
shown in Fig. 2, Beclin-1 protein
was expressed in the cytoplasm. The decrease in Beclin-1 expression
was closely correlated with poor differentiation, lymph node
metastasis, and advanced clinical tumour-node-metastasis (TNM)
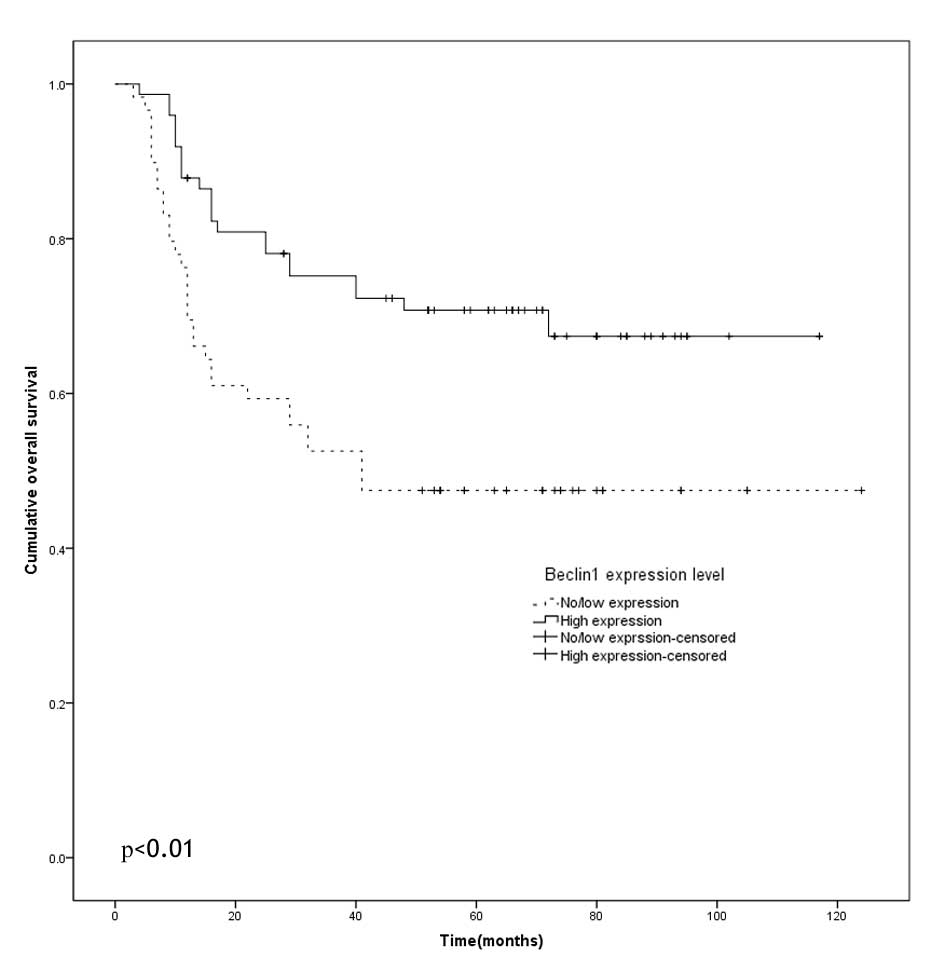
stage of OTSCC (Table I). Notably,
the five-year overall survival rate in the patients with no or low
Beclin-1 expression was 47.5%, significantly shorter than that of
the patients with high Beclin-1 expression (70.8%) (Fig. 3, P<0.01).
 | Table ICorrelation between Beclin-1
expression and clinicopathological features of the patients with
OTSCC. |
Table I
Correlation between Beclin-1
expression and clinicopathological features of the patients with
OTSCC.
| Characteristic | N | Beclin-1 expression
| χ2 | P-value |
|---|
| No/low (%) | High (%) |
|---|
| Gender | | | | 0.170 | 0.680 |
| Male | 74 | 34 (45.9) | 40 (54.1) | | |
| Female | 59 | 25 (42.4) | 34 (57.6) | | |
| Age (years) | | | | 2.844 | 0.092 |
| <50 | 50 | 17 (34.0) | 33 (66.0) | | |
| ≥50 | 83 | 42 (50.6) | 41 (49.4) | | |
| Clinical T
phase | | | | 2.425 | 0.119 |
| T1-2 | 117 | 49 (41.9) | 68 (58.1) | | |
| T3-4 | 16 | 10 (62.5) | 6 (37.5) | | |
| Clinical N
phase | | | | 10.035 | 0.002 |
| N0 | 99 | 36 (36.4) | 63 (63.6) | | |
| N1-2 | 34 | 23 (67.6) | 11 (32.4) | | |
| cTNM stage | | | | 8.718 | 0.003 |
| I–II | 92 | 33 (35.9) | 59 (64.1) | | |
| III–IV | 41 | 26 (63.4) | 15 (36.6) | | |
| Histological
differentiation | | | | 9.950 | 0.002 |
| Well | 97 | 35 (36.1) | 62 (63.9) | | |
| Moderately or
poorly | 36 | 24 (66.7) | 12 (33.3) | | |
| Recurrence | | | | 0.847 | 0.357 |
| Yes | 44 | 22 (50.0) | 22 (50.0) | | |
| No | 89 | 37 (41.6) | 52 (58.4) | | |
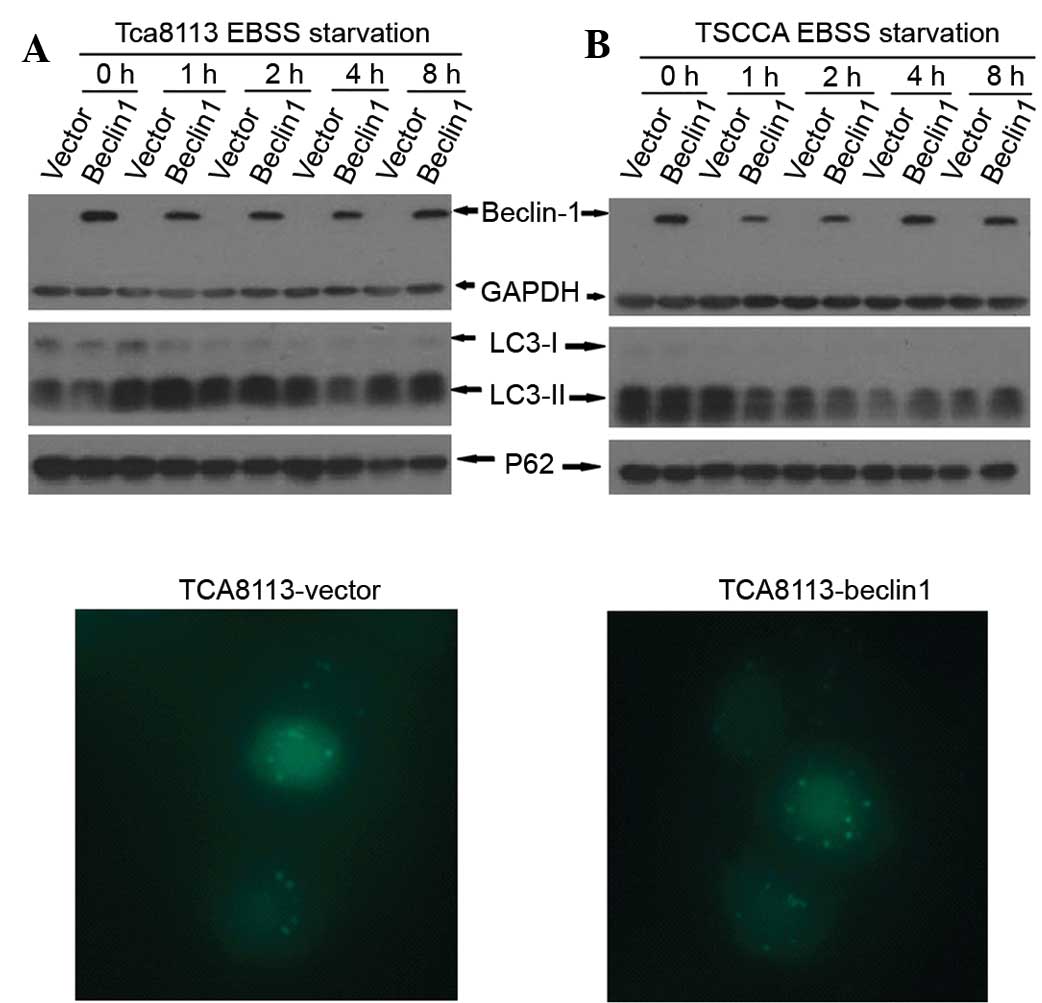
Beclin-1 overexpression did not affect
the level of autophagy but did inhibit cell proliferation
Beclin-1 is a pivotal gene in the process of
autophagy. Therefore, the influence of Beclin-1 overexpression on
autophagy upon starvation of OTSCC cells was investigated. As
normal culture medium contains serum which may influence autophagy
level, the cells were cultured in Earle's balanced salts (EBSS) to
observe autophagy level. No significant difference in the
expression levels of LC3-II and p62 was identified between the
Beclin-1 overexpression cell line and the vehicle cell line
subjected to starvation by culturing in EBSS for 1, 2, 4 or 8 h.
The number of GFP-LC3 puncta was also counted in at least 50 cells
after transient transfection of pEGF-C2-LC3, and no significant
difference was observed between the cells overexpressing Beclin-1
and the vehicle group (12.66±0.32 vs. 11.98±0.34; P=0.7996)
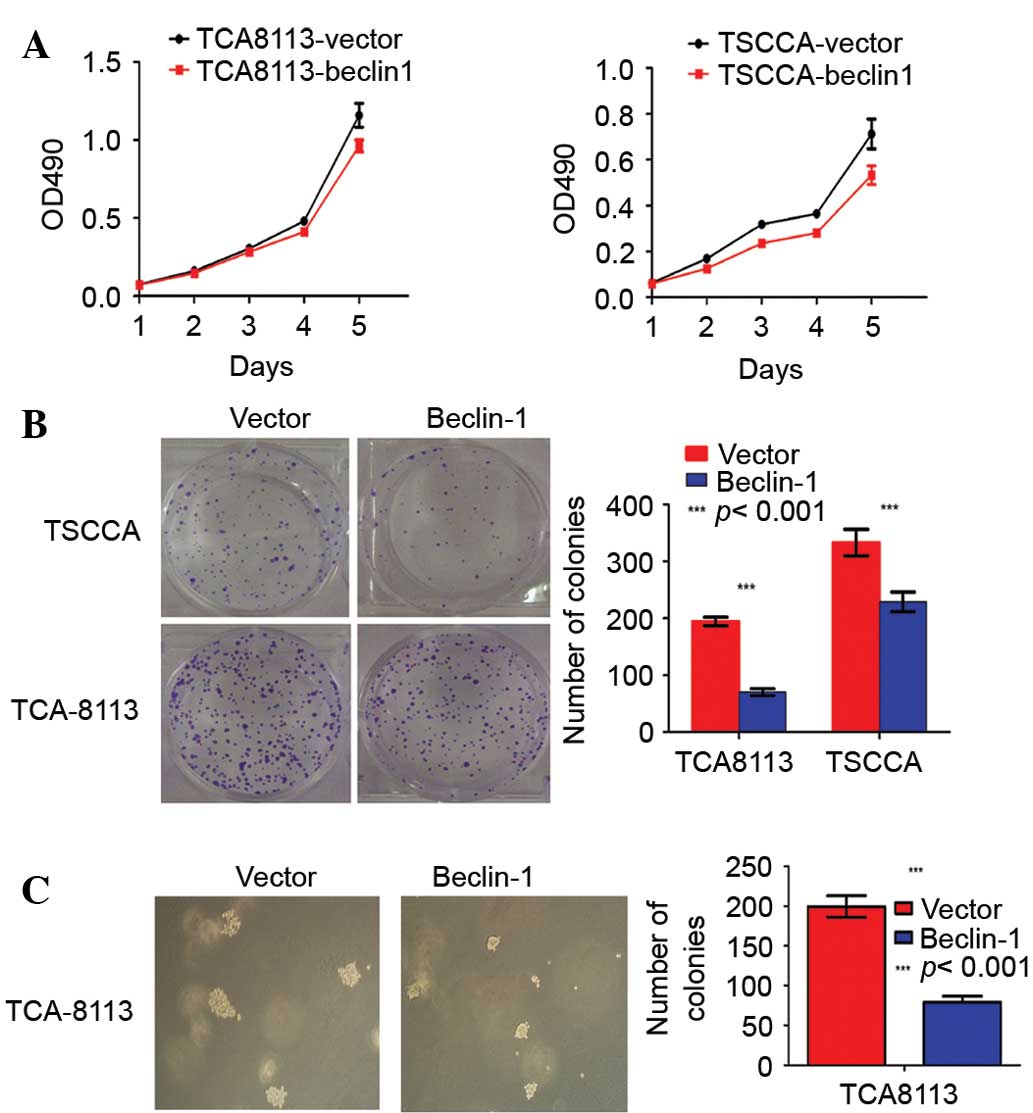
(Fig. 4). To determine whether
Beclin-1 inhibited OTSCC cell proliferation, an MTT assay was
performed, and the results suggested that Beclin-1 overexpression
significantly inhibited the proliferation of OTSCC cell lines
(Fig. 5A).
Beclin-1 inhibits the transformation of
OTSCC cells lines
To further investigate whether Beclin-1 can inhibit
the transformation of OTSCC cells, colony formation and soft-agar
anchorage-independent growth assays were performed. In total, 200
cells were plated in triplicate wells of six-well plates. After 10
days of culture, the number of colonies formed by
Beclin-1-expressing cells was significantly lower than that formed
by negative-control cells or vehicle-control groups (Fig. 5B). Furthermore, Beclin-1-expressing
cells formed significantly smaller and fewer colonies compared with
the vector cells in the soft-agar assay (Fig. 5C).
Discussion
In the present study, Beclin-1 expression was
decreased in 78.6% OTSCC tissues when compared with matched
adjacent non-cancerous tissues, which implied that Beclin-1 may be
important in carcinogenesis, consistent with other findings
(12,13,15–18,23,24).
Similarly, it was observed that the mRNA and protein levels of
Beclin-1 in a normal tongue squamous cell line were higher than
those of OTSCC cell lines. Although Beclin-1 is an important
autophagy gene, in the present study, Beclin-1 overexpression did
not significantly change the autophagy level of OTSCC cells upon
starvation. As shown for Atg6 in yeast, Beclin-1 may exhibit a
non-autophagic role in specific cell types and environmental
contexts (5,25). For this reason, MTT, colony
formation, and soft-agar anchorage-independent growth assays were
conducted. These assays demonstrated that Beclin-1 overexpression
significantly inhibits the proliferation and clonogenicity of OTSCC
cells. Similarly, Koneri et al (26) reported that knockdown of Beclin-1
in a colon cancer cell line resulted in growth inhibition. In
addition, Liang et al (9)
also reported that Beclin-1 expression in the MCF-7 human breast
carcinoma cell line significantly inhibited clonogenicity in
vitro and tumourigenesis in nude mice. These results
demonstrate that Beclin-1 can inhibit tumourigenesis by
non-autophagic methods (7,27). In the present study, decreased
Beclin-1 expression by immunohistochemistry was associated with
poor differentiation, lymph node metastasis, and advanced clinical
TNM stage of OTSCC, indicating that Beclin-1 may be involved in the
tumourigenesis and progression, consistent with the results of
several studies (8,13,15,18,27–29).
Accordingly, increased Beclin-1 expression was associated with the
absence of lymphatic invasion and a low rate of distant metastasis
in pancreatic ductal adenocarcinoma or laryngeal squamous cell
carcinoma (11,18), reduced cell proliferation in glioma
(30), and reduced invasiveness
and metastasis of oesophageal squamous cell carcinoma (31). However, the autophagy-related genes
are also known to exhibit conflicting roles in tumourigenesis
(7,25,32).
Consistent with this dual role, certain studies reports have
demonstrated that the increased expression of Beclin-1 is
correlated with poor differentiation of ovarian carcinoma (8) and endometrial adenocarcinomas
(33). Similarly, the prognostic
relevance of Beclin-1 expression has been discussed in various
malignancies, but the results are controversial (8–15,18,28,31,33–35).
In the present study, a positive link between the Beclin-1
expression level and favourable survival was revealed in OTSCC,
which was similar to the results in several other types of cancer,
including gastric carcinoma (14,15),
pancreatic ductal adenocarcinoma (18), intrahepatic cholangiocellular
carcinoma (28), hepatocellular
carcinoma (12), oesophageal
squamous cell carcinoma (31),
colon carcinoma (10), lymphoma
(35), ovarian carcinoma (13), and laryngeal squamous cell
carcinoma (11). By contrast,
several studies have reported that patients with lower Beclin-1
expression exhibit a significant overall survival advantage
compared with those with higher expression in nasopharyngeal
carcinoma (34), ovarian carcinoma
(8) and endometrial adenocarcinoma
(33). These discrepant results
indicate that Beclin-1 maybe perform different functions in
different carcinomas (36), and
the methodological differences in immunohistochemistry evaluation
and the small sample size may represent additional reasons for
these discrepant findings.
In conclusion, the present study demonstrated that
decreased Beclin-1 expression is closely associated with poor
differentiation and advanced TNM stage in OTSCC, and that Beclin-1
overexpression inhibited the proliferation and clonogenic formation
of OTSCC cells. This indicated that Beclin-1 functioned as a tumour
suppressor in OTSCC at least partly by non-autophagic mechanisms.
Beclin-1 expression may therefore represent a favourable prognostic
marker or a novel therapeutic target for OTSCC.
Acknowledgments
The present study was supported by grants from the
National Natural Science Foundation of China (grant nos. 30960444
and 81260402), and Special Foundation of High Levels of Health
Technical Personnel Training in Yunnan Province (grant no.
D-201243).
References
|
1
|
Kapoor V, Paliwal D, Baskar Singh S,
Mohanti BK and Das SN: Deregulation of Beclin 1 in patients with
tobacco-related oral squamous cell carcinoma. Biochem Biophys Res
Commun. 422:764–769. 2012. View Article : Google Scholar : PubMed/NCBI
|
|
2
|
Zhang J, Wen HJ, Guo ZM, Zeng MS, Li MZ,
Jiang YE, He XG and Sun CZ: TRB3 overexpression due to endoplasmic
reticulum stress inhibits AKT kinase activation of tongue squamous
cell carcinoma. Oral Oncol. 47:934–939. 2011. View Article : Google Scholar : PubMed/NCBI
|
|
3
|
Siegel R, Ma J, Zou Z and Jemal A: Cancer
statistics, 2014. CA Cancer J Clin. 64:9–29. 2014. View Article : Google Scholar : PubMed/NCBI
|
|
4
|
Maejima Y, Kyoi S, Zhai P, Liu T, Li H,
Ivessa A, Sciarretta S, Del Re DP, Zablocki DK, Hsu CP, et al: Mst1
inhibits autophagy by promoting the interaction between Beclin1 and
Bcl-2. Nat Med. 19:1478–1488. 2013. View
Article : Google Scholar : PubMed/NCBI
|
|
5
|
Wirawan E, Lippens S, Vanden Berghe T,
Romagnoli A, Fimia GM, Piacentini M and Vandenabeele P: Beclin1: A
role in membrane dynamics and beyond. Autophagy. 8:6–17. 2012.
View Article : Google Scholar
|
|
6
|
Gurkar AU, Chu K, Raj L, Bouley R, Lee SH,
Kim YB, Dunn SE, Mandinova A and Lee SW: Identification of ROCK1
kinase as a critical regulator of Beclin1-mediated autophagy during
metabolic stress. Nat Commun. 4:21892013. View Article : Google Scholar : PubMed/NCBI
|
|
7
|
Shin JY, Hong SH, Kang B, Minai-Tehrani A
and Cho MH: Overexpression of beclin1 induced autophagy and
apoptosis in lungs of K-rasLA1 mice. Lung Cancer. 81:362–370. 2013.
View Article : Google Scholar : PubMed/NCBI
|
|
8
|
Zhao Y, Chen S, Gou WF, Xiao LJ, Takano Y
and Zheng HC: Aberrant Beclin 1 expression is closely linked to
carcinogenesis, differentiation, progression and prognosis of
ovarian epithelial carcinoma. Tumour Biol. 35:1955–1964. 2014.
View Article : Google Scholar
|
|
9
|
Huang L, Wang S, Li SS and Yang XM:
Prognostic significance of Beclin-1 expression in laryngeal
squamous cell carcinoma. Pathol Oncol Res. 19:771–777. 2013.
View Article : Google Scholar : PubMed/NCBI
|
|
10
|
Shi YH, Ding ZB, Zhou J, Qiu SJ and Fan J:
Prognositc significance of Beclin 1-dependent apoptotic activity in
hepatocellular carcinoma. Autophagy. 5:380–382. 2009. View Article : Google Scholar : PubMed/NCBI
|
|
11
|
Lin HX, Qiu HJ, Zeng F, Rao HL, Yang GF,
Kung HF, Zhu XF, Zeng YX, Cai MY and Xie D: Decreased expression of
Beclin 1 correlates closely with Bcl-xL expression and poor
prognosis of ovarian carcinoma. PLoS One. 8:e605162013. View Article : Google Scholar : PubMed/NCBI
|
|
12
|
Yu M, Gou WF, Zhao S, Xiao LJ, Mao XY,
Xing YN, Takahashi H, Takano Y and Zheng HC: Beclin 1 expression is
an independent prognostic factor for gastric carcinomas. Tumour
Biol. 34:1071–1083. 2013. View Article : Google Scholar : PubMed/NCBI
|
|
13
|
Chen YB, Hou JH, Feng XY, Chen S, Zhou ZW,
Zhang XS and Cai MY: Decreased expression of Beclin 1 correlates
with a metastatic phenotypic feature and adverse prognosis of
gastric carcinoma. J Surg Oncol. 105:542–547. 2012. View Article : Google Scholar
|
|
14
|
Ahn CH, Jeong EG, Lee JW, Kim MS, Kim SH,
Kim SS, Yoo NJ and Lee SH: Expression of beclin-1, an
autophagy-related protein, in gastric and colorectal cancers.
APMIS. 115:1344–1349. 2007. View Article : Google Scholar
|
|
15
|
Okura R and Nakamura M: Overexpression of
autophagy-related beclin-1 in cutaneous squamous cell carcinoma
with lymph-node metastasis. Eur J Dermatol. 21:1002–1003.
2011.PubMed/NCBI
|
|
16
|
Kim HS, Lee SH, Do SI, Lim SJ, Park YK and
Kim YW: Clinicopathologic correlation of beclin-1 expression in
pancreatic ductal adenocarcinoma. Pathol Res Pract. 207:247–252.
2011. View Article : Google Scholar : PubMed/NCBI
|
|
17
|
Chen N and Karantza-Wadsworth V: Role and
regulation of autophagy in cancer. Biochim Biophys Acta.
1793:1516–1523. 2009. View Article : Google Scholar : PubMed/NCBI
|
|
18
|
Marino G, Salvador-Montoliu N, Fueyo A,
Knecht E, Mizushima N and López-Otín C: Tissue-specific autophagy
alterations and increased tumorigenesis in mice deficient in
Atg4C/autophagin-3. J Biol Chem. 282:18573–18583. 2007. View Article : Google Scholar : PubMed/NCBI
|
|
19
|
Liu J, Xia H, Kim M, Xu L, Li Y, Zhang L,
Cai Y, Norberg HV, Zhang T, Furuya T, et al: Beclin1 controls the
levels of p53 by regulating the deubiquitination activity of USP10
and USP13. Cell. 147:223–234. 2011. View Article : Google Scholar : PubMed/NCBI
|
|
20
|
Edge SB, Byrd DR, Compton CC, Fritz AG,
Greene FL and Trotti A: AJCC Cancer Staging Manual. 7th edition.
Springer; New York: 2010
|
|
21
|
Huang X, Bai HM, Chen L, Li B and Lu YC:
Reduced expression of LC3B-II and Beclin 1 in glioblastoma
multiforme indicates a down-regulated autophagic capacity that
relates to the progression of astrocytic tumors. J Clin Neurosci.
17:1515–1519. 2010. View Article : Google Scholar : PubMed/NCBI
|
|
22
|
Jiang ZF, Shao LJ, Wang WM, Yan XB and Liu
RY: Decreased expression of Beclin-1 and LC3 in human lung cancer.
Mol Biol Rep. 39:259–267. 2012. View Article : Google Scholar
|
|
23
|
Sun Y, Liu JH, Jin L, Lin SM, Yang Y, Sui
YX and Shi H: Over-expression of the Beclin 1 gene upregulates
chemosensitivity to anti-cancer drugs by enhancing therapy-induced
apoptosis in cervix squamous carcinoma CaSki cells. Cancer Lett.
294:204–210. 2010. View Article : Google Scholar : PubMed/NCBI
|
|
24
|
Koneri K, Goi T, Hirono Y, Katayama K and
Yamaguchi A: Beclin 1 gene inhibits tumor growth in colon cancer
cell lines. Anticancer Res. 27:1453–1457. 2007.PubMed/NCBI
|
|
25
|
Liang XH, Jackson S, Seaman M, Brown K,
Kempkes B, Hibshoosh H and Levine B: Induction of autophagy and
inhibition of tumorigenesis by beclin 1. Nature. 402:672–676. 1999.
View Article : Google Scholar : PubMed/NCBI
|
|
26
|
Won KY, Kim GY, Lim SJ and Kim YW:
Decreased Beclin-1 expression is correlated with the growth of the
primary tumor in patients with squamous cell carcinoma and
adenocarcinoma of the lung. Hum Pathol. 43:62–68. 2012. View Article : Google Scholar
|
|
27
|
Dong LW, Hou YJ, Tan YX, Tang L, Pan YF,
Wang M and Wang HY: Prognostic significance of Beclin 1 in
intrahepatic cholangiocellular carcinoma. Autophagy. 7:1222–1229.
2011. View Article : Google Scholar : PubMed/NCBI
|
|
28
|
Wang ZH, Xu L, Wang Y, Cao MQ, Li L and
Bai T: Clinicopathologic correlations between human papillomavirus
16 infection and Beclin 1 expression in human cervical cancer. Int
J Gynecol Pathol. 30:400–406. 2011. View Article : Google Scholar : PubMed/NCBI
|
|
29
|
Pirtoli L, Cevenini G, Tini P, Vannini M,
Oliveri G, Marsili S, Mourmouras V, Rubino G and Miracco C: The
prognostic role of Beclin 1 protein expression in high-grade
gliomas. Autophagy. 5:930–936. 2009. View Article : Google Scholar : PubMed/NCBI
|
|
30
|
Chen Y, Lu Y, Lu C and Zhang L: Beclin-1
expression is a predictor of clinical outcome in patients with
esophageal squamous cell carcinoma and correlated to
hypoxia-inducible factor (HIF)-1alpha expression. Pathol Oncol Res.
15:487–493. 2009. View Article : Google Scholar : PubMed/NCBI
|
|
31
|
Mathew R, Karantza-Wadsworth V and White
E: Role of autophagy in cancer. Nat Rev Cancer. 7:961–967. 2007.
View Article : Google Scholar : PubMed/NCBI
|
|
32
|
Giatromanolaki A, Koukourakis MI,
Koutsopoulos A, Chloropoulou P, Liberis V and Sivridis E: High
beclin 1 expression defines a poor prognosis in endometrial
adenocarcinomas. Gynecol Oncol. 123:147–151. 2011. View Article : Google Scholar : PubMed/NCBI
|
|
33
|
Wan XB, Fan XJ, Chen MY, Xiang J, Huang
PY, Guo L, Wu XY, Xu J, Long ZJ, Zhao Y, et al: Elevated Beclin 1
expression is correlated with HIF-1 alpha in predicting poor
prognosis of nasopharyngeal carcinoma. Autophagy. 6:395–404. 2010.
View Article : Google Scholar : PubMed/NCBI
|
|
34
|
Koukourakis MI, Giatromanolaki A, Sivridis
E, Pitiakoudis M, Gatter KC and Harris AL: Beclin 1 over- and
underexpression in colorectal cancer: Distinct patterns relate to
prognosis and tumour hypoxia. Br J Cancer. 103:1209–1214. 2010.
View Article : Google Scholar : PubMed/NCBI
|
|
35
|
Huang JJ, Li HR, Huang Y, Jiang WQ, Xu RH,
Huang HQ, Lv Y, Xia ZJ, Zhu XF, Lin TY and Li ZM: Beclin 1
expression: A predictor of prognosis in patients with extranodal
natural killer T-cell lymphoma, nasal type. Autophagy. 6:777–783.
2010. View Article : Google Scholar : PubMed/NCBI
|
|
36
|
Mathew R, Kongara S, Beaudoin B, Karp CM,
Bray K, Degenhardt K, Chen G, Jin S and White E: Autophagy
suppresses tumor progression by limiting chromosomal instability.
Genes Dev. 21:1367–1381. 2007. View Article : Google Scholar : PubMed/NCBI
|