Introduction
Cholangiocellular carcinoma (CCC) is an epithelial
cell malignancy arising from various locations within the biliary
tree, which is classified as intrahepatic, perihilar and distal
cholangiocarcinoma based on anatomical location (1). CCC accounts for 3% of gastrointestinal
tumors worldwide and is the second most common primary liver cancer
(2). Even with greatly improved
diagnosis and treatment technologies in the past 30 years, the
5-year survival rate including patients with radical surgical
resection, the only means for cure, remain at <5% (3). High recurrence risks and poor
prognoses in CCC patients have been a major challenge to medical
workers (4). Therefore, it is
necessary to identify a tumor marker for predicting therapeutic
response, recurrence and the survival of CCC, and developing
targeted therapy to improve patient prognosis.
HOX genes are an evolutionarily conserved
family of genes that encode a class of important transcription
factors which function in various developmental processes (5). In addition to their role in
embryogenesis, HOX genes are expressed in adult cells where
they regulate the expression of genes involved in cell
proliferation as well as cell-cell and cell-extracellular matrix
interactions (6). As one of such
homeobox genes, the overexpression of HOXD10 has been demonstrated
to maintain a quiescent, differentiated phenotype in endothelial
cells by suppressing the expression of genes involved in remodeling
the extracellular matrix and cell migration (7). In breast cancer cell lines, HOXD10
induces cell phenotypic reversion from highly invasive tumor cells
to a non-malignant state in a three-dimensional culture model
(8).
Overexpression or loss of HOXD10 is involved in
tumorigenesis characterized as an oncogene or tumor-suppressor
because of its importance in cancer cell survival, proliferation,
invasion and migration in several malignancies, including breast,
gastric, hepatocellular, ovarian, malignant glioma, head and neck,
bladder, and colorectal cancer (9–16).
However, the role of HOXD10 in CCC malignant progression remains
elusive. Therefore, we investigated whether HOXD10 plays a role in
the development and progression of CCC.
Materials and methods
Patients and clinicopathological
data
Concurrent clinical and pathological data were
retrospectively collected from 87 patients who underwent surgical
resection of pathologically confirmed CCC between March 3, 2008 and
December 20, 2013 at the First Affiliated Hospital of Xi'an
Jiaotong University and the Tangdu Hospital (Shaanxi, China).
Demographic data and pathological results were collected for each
patient. The study was approved by the ethics committees of the
above hospitals in March 2008. The patients provided signed
informed consent. The follow up of patients was conducted through
phone calls until death or the study deadline date of December 20,
2013. Additionally, 30 cases of para-carcinoma tissue were included
as controls. Histopathological diagnosis was performed by the
Department of Pathology of each Institution. Clinicopathological
staging was determined by the TNM classification of the 7th edition
American Joint Committee on Cancer (AJCC) for intrahepatic,
perihilar and distal cholangiocarcinoma, respectively (17). Tissue samples were fixed in 4%
formalin immediately after removal for immunohistochemical (IHC)
staining.
Immunohistochemical analysis
Fixed tumor samples were processed conventionally
for paraffin-embedded tumor slides. The slides were subjected to
antigen retrieval and the endogenous peroxidase activity was
blocked with 3% hydrogen peroxide for 10 min. The sections were
incubated with 1% bovine serum albumin to decrease non-specific
staining and reduce endogenous peroxidase activity. For IHC
staining, the sections were incubated with antibodies against
HOXD10 (1:800; Abgent Corporation, San Diego, CA, USA) and RHOC
(1:200; Abcam, Cambridge, MA, USA). PBS was used to replace the
primary antibody as a negative control. After being washed with
PBS, the slides were incubated with biotinylated secondary antibody
followed by conjugated horseradish peroxidase (HRP)-labeled
streptavidin (Dako, Glostrup, Denmark) and then washed with PBS.
The slides were then incubated with diaminobenzidine (DAB; Sigma,
St. Louis, MO, USA) as the chromogen, followed by counterstaining
with diluted Harris's hematoxylin (Sigma). After staining, five
high-power fields (×400) were randomly selected in each slide, and
the average proportion of positive cells in each field was counted.
The immunoreactivity score of each section was based on the
proportion of immunopositive cells (0, <10%; 1, ≥10 to <25%;
2, ≥25 to <50%; 3, ≥50 to <75% and 4, ≥75%) x their intensity
of staining (0, no positivity; 1, weak; 2, moderate and 3, strong)
and was divided into 4 levels, 0 (negative), 1–4 (weak), 5–8
(moderate) and 9–12 (strong). The final immunoreaction score was
defined as the sum of the two parameters (extension and intensity),
and the samples were grouped as negative (0), weak (1–2),
moderate (3) and strong (4–6)
staining. For statistical purposes, only the final immunoreaction
scores of moderate and strong were considered positive, and the
other final scores negative.
Cell culture and transfection with
lentiviral-mediated overexpression of HOXD10 vectors
The RBE cell line was purchased from the Shanghai
Institute for Biological Sciences (Shanghai, China). The HCCC-9810
cell line was obtained from the Wuhan Boster Biological Engineering
Corporation (Wuhan, China). The cells were maintained in RPMI-1640
medium containing 10% fetal bovine serum (FBS) and were routinely
cultivated in a humidified incubator at 37°C with 5%
CO2.
A lentivirus encoding the complete human HOXD10/GFP
open reading frame (lentivirus-GFP-HOXD10) and a control negative
lentivirus encoding a green fluorescent protein (GFP) open reading
frame (lentivirus-GFP) were constructed by Genechem Biotechnology
Inc., Ltd. (Shanghai, China). The HOXD10 coding sequence was
amplified from human genomic DNA by PCR using the primers: sense,
5′-GAGGATCCCCGGGTACCGGTCGCCACCATGTCCTTTCCCAACAG CTC-3′ and
antisense, 5′-TCCTTGTAGTCCATACCAGAA AACGTGAGGTTGGC-3′. The
amplified HOXD10 gene was cloned into GV358 mammalian
expressing vector, and transferred into the lentiviral vector,
Ubi-MCS-3FLAG-SV40-EGFP-IRES-puromycin, using in vitro
recombination, to generate the recombinant lentiviral expression
vector, LV-HOXD10. The empty lentiviral vector LV-GFP was also
packaged in the same manner and used as a negative control. The
expression of GFP was examined under a fluorescence microscope, and
the intensity of green fluorescence indicated the transduction
efficiency. The two CCC cells were transfected with high titer
(2×108 TU/ml) lentivirus-HOXD10 and negative control
lentivirus expression vector particles (all with a MOI of 30
transfection concentration) according to the manufacturer's
instructions. Stable HOXD10 overexpression and negative lentiviral
transfectants were obtained by continuous treatment with 2
µg/ml puromycin in transfected RBE and HCCC-9810 cell
lines.
Reverse transcription-PCR (RT-PCR)
Total RNA was extracted from the cultured cells
using the TRIzol reagent (Invitrogen-Life Technologies). Oligo
(dT)-primed RNA (1 µg) was reverse-transcribed with reverse
transcriptase (Takara Biotechnology Co., Ltd., Dalian, China)
according to the manufacturer's instructions. The primers (Sangon
Biotech, Shanghai, China) used to detect the expression of HOXD10,
MMP2, MMP9, MMP14 and GAPDH (internal control) were: HOXD10 sense,
5′-GACATGGGGACCTATGGAATGC-3′ and antisense,
5′-TGGTGGTTCACTTCTCTTTTGG-3′; MMP2 sense, 5′-CTTCTTCCCTCGCAAGCC-3′
and anti-sense, 5′-ATGGATTCGAGAAAACCG-3′; MMP9 sense,
5′-ACGCAGACATCGTCATCC-3′ and antisense, 5′-AACCGAGTTGAACCACG-3′;
MMP14 sense, 5′-TCCATCAACACTGCCTACGA-3′ and antisense,
5′-TGAATGACCCTCTGGGAGAC-3′; and GAPDH sense,
5′-AGGTCCACCACTGACACGTT-3′ and antisense,
5′-GCCTCAAGATCATCAGCAAT-3′.
Western blot analysis
Equal amounts of protein sample from the RBE and
HCCC-9810 cells were separated by SDS-PAGE and then transferred to
polyvinylidene difluoride (PVDF) membranes (Millipore, Bedford, MA,
USA). The membranes were blocked and then probed with a primary
antibody against HOXD10 (1:300; Abgent Corporation), RHOC, MMP2 and
MMP9 (all at 1:1,000) and MMP14 (1:2,000), (all from Abcam), AKT,
ERK1/2, p-AKT, p-ERK1/2 (all at 1:500; Wanleibio Co., Ltd., China)
and β-actin (1:5,000; Santa Cruz Biotechnology, Inc., Santa Cruz,
CA, USA). After being washed, the membranes were incubated with
HRP-conjugated goat anti-mouse/rabbit IgG (Santa Cruz
Biotechnology, Inc.) and detected using the enhanced
chemiluminescence (ECL) detection kit from Pierce (Rockford, IL,
USA).
Cell viability assay
Cell viability was assessed using a MTT assay
according to the manufacturer's instructions. The absorbance at 490
nm was detected using a microplate reader (Bio-Rad, Hercules, CA,
USA). A growth curve was prepared according to the absorbance
values at 490 nm. The results reflect the average of three
replicates under the same conditions.
Colony formation assay
Non-transfected and transfected RBE and HCCC-9810
cells (200 cells/dish) were seeded in 60-mm culture dishes. After
14 days of culture, the adherent cells were washed twice with PBS
and fixed with 4% paraformaldehyde for 30 min at room temperature.
The colonies were stained with Giemsa solution for 15 min, washed
with water and air-dried. The number of colonies was counted using
a light microscope. The experiments were performed in
triplicate.
Analysis of the cell cycle distribution
and apoptosis
The effect of HOXD10 overexpression on cell cycle
progression was determined using flow cytometry following propidium
iodide (PI) staining. Briefly, the cells were harvested and fixed
in 70% ethanol at 4°C overnight. For the analysis, 1 ml of freshly
prepared PBS staining solution (50 µg/ml PI and 100
µg/ml RNase A) was added to the cells. Following incubation
for 1 h in the dark at room temperature, the cells were analyzed
using flow cytometry (FACSCalibur; BD Biosciences, Franklin Lakes,
NJ, USA). The proportion of DNA in different phases was analyzed
using dedicated software (BD Biosciences). Quantification of
apoptosis was determined by analyzing the percentages of apoptotic
cells. The cells were stained using an Annexin V-APC/7-AAD
apoptosis detection kit (KGA1023–1026; Nanjing KeyGen Biotech. Co.,
Ltd.) according to the manufacturer's instructions and were
analyzed by flow cytometry using a Beckman Coulter flow
cytometer.
Cell invasion assay
Cell invasion was assessed using 6.5-mm Transwell
chambers with a pore size of 8 µm (Corning, NY, USA). The
Transwell upper chambers were pre-coated with 50 µg/chamber
of a solubilized basement membrane in the form of Matrigel (BD
Biosciences). RPMI-1640/10% FBS was added to the bottom chamber.
CCC cells (3×104/chamber) were seeded in
serum-containing media in the upper well of the Transwell chambers.
The cells were incubated for 48 h, and those that did not invade
through the pores were removed with a cotton swab. The invasive
cells in the lower chamber (below the filter surface) were fixed in
70% ethanol, stained with 0.1 mg/ml crystal violet solution, and
counted under a microscope (×20 magnification). Individual
experiments had triplicate inserts, and five randomly selected
fields were counted per insert.
Statistical analysis
Data were analysed using SPSS software version 18.0
(SPSS Inc., Chicago, IL, USA). The data are presented as the mean ±
SD. The data were analyzed using the χ2 test and the
Student's t-test. The Kaplan-Meier test was used for univariate
survival analysis. The Cox proportional hazard model was used for
multivariate analysis and for determining the 95% confidence
intervals. Differences with P<0.05 were considered to indicate a
statistically significant result.
Results
Low HOXD10 and high RHOC expression in
poorly-differentiated CCC tissues and the association with a poor
outcome in CCC patients
To determine the role of HOXD10 in CCC, we evaluated
HOXD10 expression in tumor or para-carcinoma tissue from patients
with CCC by using IHC. The positive expression rate of HOXD10 in
well-differentiated cancerous tissues (25/28, 89.3%) was not
significantly different compared to that of the adjacent
para-carcinoma tissues (27/30, 90%) (P>0.05). However, the
HOXD10-positive expression rate in well-differentiated cancerous
tissues (25/28, 89.3%) was significantly higher than that of the
poorly-differentiated cancerous tissues (4/21, 19%) (P<0.001).
Furthermore, HOXD10 expression was progressively reduced with
increasing degrees of malignancy (Fig.
1A and Table I,
P<0.001).
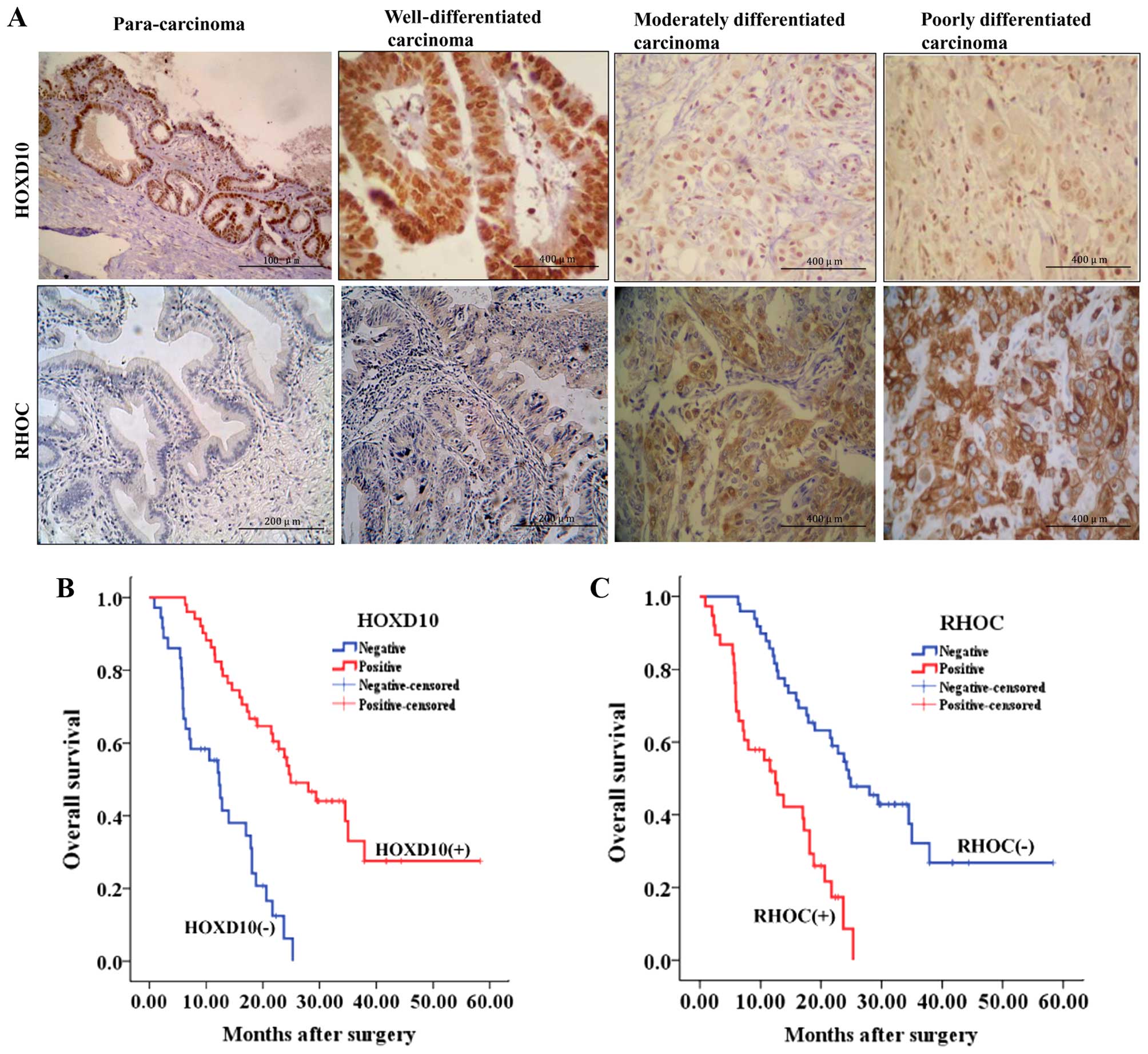 | Figure 1Decreased HOXD10 and increased RHOC
expression in CCC and the negative association of the dysregulated
expressions with prognosis. (A) Immunohistochemical stainings for
HOXD10 and RHOC expression. The positive HOXD10 staining was
primarily localized in the nucleus, while the positive RHOC
staining was localized in the cytoplasm. The HOXD10 stainings are
strong, strong, moderate and weak in para-carcinoma (×100), well-
(×400), moderately- (×400) and poorly-differentiated carcinoma
(×400), respectively, while the RHOC stainings are weak, weak,
moderate and strong in para-carcinoma (×200), well- (×200),
moderately- (×400) and poorly-differentiated carcinoma (×400),
respectively. (B) Kaplan-Meier plots of the overall survival rate
of CCC patients based on nuclear HOXD10-positive or -negative
expression. (C) Kaplan-Meier plots of the overall survival rate of
CCC patients based on RHOC-positive or -negative expression. CCC,
cholangiocellular carcinoma. |
 | Table ICorrelations between HOXD10
expression and the clinicopathological characteristics of CCC
patients. |
Table I
Correlations between HOXD10
expression and the clinicopathological characteristics of CCC
patients.
|
Parameters/categories | No. of cases
(n) | HOXD10
|
|---|
| No. of positive
cases (%) | χ2 | P-value |
|---|
| Age | | | | |
| <70 | 66 | 38 (57.6) | 0.123 | 0.726 |
| ≥70 | 21 | 13 (61.9) | | |
| Gender | | | | |
| Male | 46 | 26 (56.5) | 0.177 | 0.674 |
| Female | 41 | 25 (61.0) | | |
| Histological
grade | | | | |
| G1 | 28 | 25 (89.3) | 24.420 | <0.001a |
| G2 | 38 | 22 (57.9) | | |
| G3 | 21 | 4 (19.0) | | |
| TNM stage | | | | |
| I-II | 77 | 46 (59.7) | 0.346 | 0.556 |
| III-IV | 10 | 5 (50.0) | | |
| Lymph node
metastasis | | | | |
| Negative | 60 | 39 (65.0) | 3.244 | 0.072 |
| Positive | 27 | 12 (44.4) | | |
| CA-199 | | | | |
| <35 | 39 | 27 (69.2) | 3.281 | 0.070 |
| ≥35 | 48 | 24 (50.0) | | |
| Venous/lymphatic
invasion | | | | |
| Negative | 44 | 24 (54.5) | 0.610 | 0.435 |
| Positive | 43 | 27 (62.8) | | |
| Perineural
invasion | | | | |
| Negative | 45 | 29 (64.4) | 1.303 | 0.254 |
| Positive | 42 | 22 (52.4) | | |
| Tumor location | | | | |
| Intrahepatic | 8 | 3 (37.5) | 1.749 | 0.417 |
| Perihilar | 21 | 12 (57.1) | | |
| Distal | 58 | 36 (62.1) | | |
We assessed the correlation between the expression
of HOXD10 and the histopathological parameters in CCC patients. As
shown in Table I, the positive
expression of HOXD10 was significantly associated with histologic
grade (P<0.001). However, HOXD10 expression was not correlated
with gender, age, TNM stage, CA19–9 level, venous/lymphatic
invasion, tumor location or lymph node metastasis (P>0.05). The
results of the Kaplan-Meier analysis for overall survival based on
HOXD10 expression are shown in Table
II (P<0.001). The prognosis for patients with a positive
HOXD10 expression was significantly better than that for patients
with a negative HOXD10 expression (Fig.
1B).
 | Table IIUnivariate analyses showing the
overall survival rate of CCC patients. |
Table II
Univariate analyses showing the
overall survival rate of CCC patients.
|
Parameters/categories | No. of cases
(n) | Mean survival time
in months (95% CI) | P-value |
|---|
| Age | | | |
| <70 | 66 | 18.1
(13.0–23.2) | 0.352 |
| ≥70 | 21 | 23.7
(13.7–33.7) | |
| Gender | | | |
| Male | 46 | 19.0
(13.8–24.1) | 0.393 |
| Female | 41 | 17.2
(8.3–26.1) | |
| Histological
grade | | | |
| G1 | 28 | 35.0
(27.9–42.1) | <0.001a |
| G2 | 38 | 13.8
(11.6–16.0) | |
| G3 | 21 | 10.6
(0.1–21.1) | |
| TNM stage | | | |
| I-II | 77 | 20.6
(15.5–25.7) | 0.007a |
| III-IV | 10 | 12.1
(9.1–15.1) | |
| Lymph node
metastasis | | | |
| Negative | 60 | 23.8
(17.7–29.9) | 0.005a |
| Positive | 27 | 14.6
(7.5–21.7) | |
| CA-199 | | | |
| <35 | 39 | 22.8
(16.5–29.1) | 0.100 |
| ≥35 | 48 | 16.3
(11.9–20.7) | |
| Venous/lymphatic
invasion | | | |
| Negative | 44 | 19.0
(12.5–25.5) | 0.822 |
| Positive | 43 | 18.8
(12.2–25.4) | |
| Perineural
invasion | | | |
| Negative | 45 | 18.1
(10.8–25.4) | 0.586 |
| Positive | 42 | 18.8
(13.5–24.1) | |
| HOXD10 | | | |
| Negative | 36 | 12.5
(8.3–16.7) | <0.001a |
| Positive | 51 | 24.2
(19.8–28.6) | |
| RHOC | | | |
| Negative | 49 | 23.8
(17.8–29.8) | <0.001a |
| Positive | 38 | 13.8
(5.2–22.4) | |
RHOC, a member of the Rho family GTPases, is
involved at multiple stages of tumorigenesis and progression, and
is HOXD10-dependent in breast and gastric cancer cell lines
(18–22). To analyze the role of HOXD10 in CCC,
we investigated the RHOC protein expression using the same set of
CCC samples. The IHC analysis revealed tumors with lower HOXD10
levels also exhibited a higher RHOC expression (Fig. 1A), showing a direct negative
association between HOXD10 and RHOC expression (Table III, P<0.001). Moreover, the
results of the Kaplan-Meier analysis for overall survival based on
RHOC expression are shown in Table
II (P<0.001). The patients with a negative RHOC expression
had a longer survival than those with a positive RHOC expression
(Fig. 1C).
 | Table IIICorrelation between HOXD10 and RHOC
expression in CCC patients. |
Table III
Correlation between HOXD10 and RHOC
expression in CCC patients.
| HOXD10
expression | RHOC expression
| χ2 | P-value |
|---|
| Positive | Negative |
|---|
| Positive | 6 | 45 | 51.026 | <0.001a |
| Negative | 32 | 4 | | |
To obtain a more precise estimate regarding patient
prognosis, the Cox proportional hazard regression model was
applied. The results confirmed that a positive HOXD10 expression
was an independent prognostic factor for CCC patients, and a
positive HOXD10 expression may contribute to the reduced mortality
rate following surgery by 65.9% (HR=0.341, Table IV).
 | Table IVMultivariate analysis of the overall
survival rate of CCC patients. |
Table IV
Multivariate analysis of the overall
survival rate of CCC patients.
|
Parameters/categories | HR (95% CI) | P-value |
|---|
| HOXD10
expression | | |
| Negative | 0.341
(0.139–0.838) | 0.019a |
| Positive | | |
| RHOC
expression | | |
| Negative | 1.744
(0.691–4.402) | 0.239 |
| Positive | | |
| TNM stage | | |
| I-II | 2.923
(1.210–7.064) | 0.017a |
| III-IV | | |
| Lymph node
metastasis | | |
| Negative | 1.311
(0.713–2.411) | 0.383 |
| Positive | | |
| Histological
grade | | |
| G1–G2 | 1.215
(0.646–2.284) | 0.545 |
| G3 | | |
HOXD10 mRNA and protein expression is
effectively induced by lentiviral-mediated overexpression of HOXD10
in RBE and HCCC-9810 cell lines
Since HOXD10 protein expression was downregulated in
CCC tissues and associated with poor outcome of CCC patients, the
function of HOXD10 was determined using a lentivirus-mediated
HOXD10 overexpression vector in the RBE and HCCC-9810CCC cell lines
that had low endogenous HOXD10 mRNA and protein expression levels
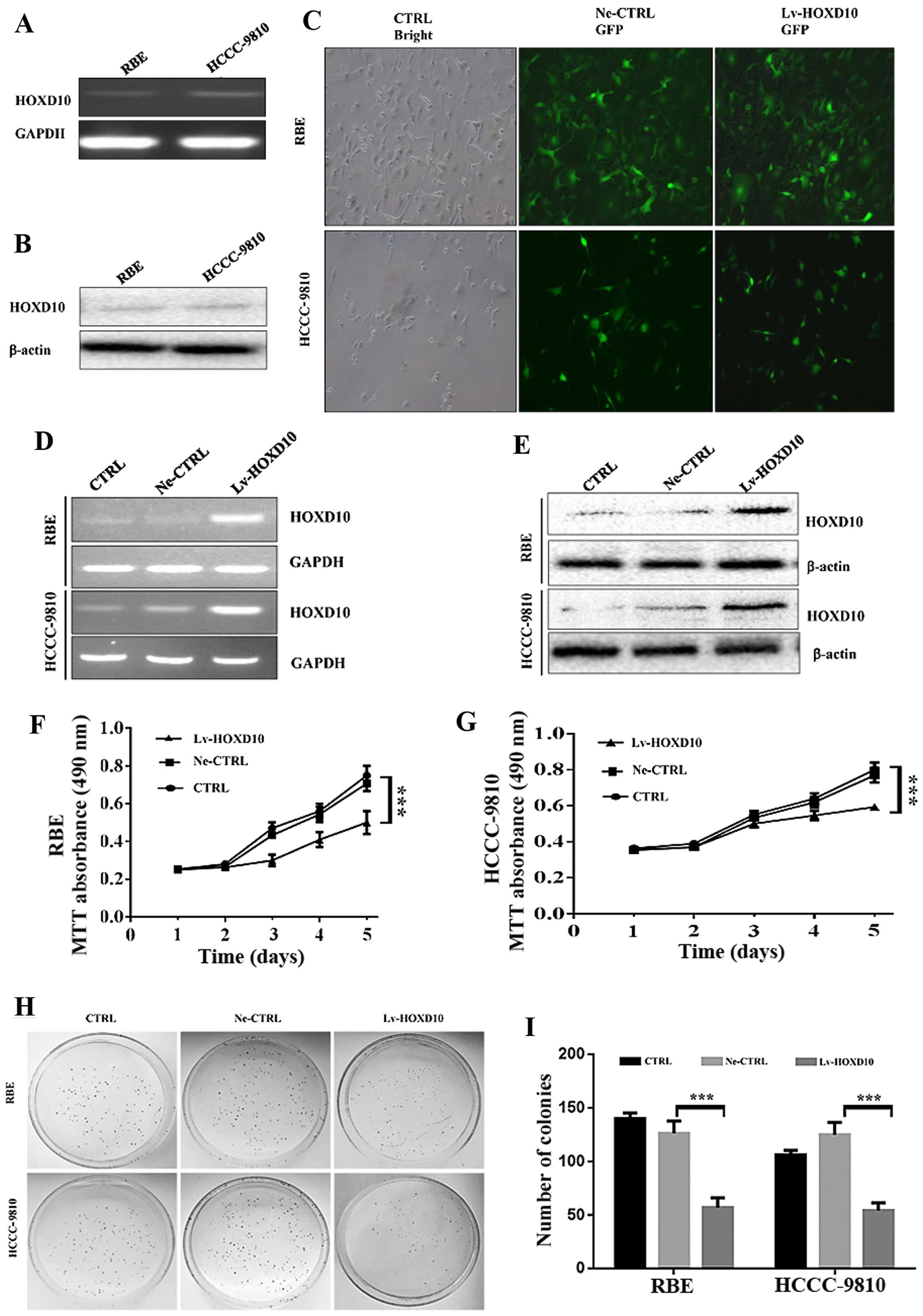
(Fig. 2A and B). To observe the
lentiviral transfection efficiency in RBE and HCCC-9810 cells, GFP
expression was examined using fluorescent microscopy 4 days after
infection (Fig. 2C). The efficiency
of lentiviral transfection in RBE and HCCC-9810 cells was ≥95% on
the 4th day or later at the MOI of 30.
Five days after transfection, the HOXD10 mRNA and
protein expressions in RBE and HCCC-9810 cells were analyzed using
RT-PCR and western blotting, respectively. The levels of HOXD10
mRNA and protein in RBE and HCCC-9810 cells transfected with
recombinant lentivirus HOXD10 were significantly increased,
compared with cells transfected with negative lentivirus HOXD10 and
the blank control cells (Fig. 2D and
E). These results indicated that a lentivirus-mediated
overexpression vector effectively and specifically induced HOXD10
overexpression in RBE and HCCC-9810 cells.
Establishment of RBE and HCCC-9810 cells
stably overexpressing HOXD10
In preliminary studies, adequate selection pressure
was maintained with 2 µg/ml of puromycin. The expression of
GFP and HOXD10 was observed. After the cells were frozen in liquid
nitrogen for 6 months and revived monthly, GFP expression was
observed in >95% of the lentivirus-transfected RBE and HCCC-9810
cells treated with 2 µg/ml of puromycin. PCR and western
blotting showed the stable overexpresion of HOXD10 mRNA and
protein, respectively, in the same cells. These results showed that
the stably transfected RBE and HCCC-9810 cell lines were
successfully established with lentivirus and that the
overexpression of HOXD10 lasted ≥6 months. The stably transfected
RBE and HCCC-9810 cell lines were defined as lentiviral-HOXD10
(Lv-HOXD10) cells and negative lentiviral-HOXD10 (Ne-CTRL) control
cells, respectively, and used in subsequent experiments.
Effect of HOXD10 upregulation on RBE and
HCCC-9810 cell growth and proliferation
The viability of the transfected cell lines was
detected using an MTT assay (Fig. 2F
and G). The sustainable HOXD10 overexpression markedly
inhibited the viability of RBE and HCCC-9810 cells in a
time-dependent manner. The percentage of viable cells in the RBE
and HCCC-9810 cells with Lv-HOXD10 significantly decreased compared
with the Ne-CTRL and the blank control (CTRL) cells
(P<0.001).
Furthermore, the colony formation analysis revealed
that stably enhancing HOXD10 significantly decreased the number of
colonies of RBE and HCCC-9810 cells compared with the Ne-CTRL and
CTRL groups (Fig. 2H and I,
P=0.001). These results suggested that HOXD10 may play a
vital-suppressive role in CCC cell growth and proliferation.
G1/S progression arrest and apoptosis
promotion of RBE and HCCC-9810 cells induced by upregulation of
HOXD10 expression
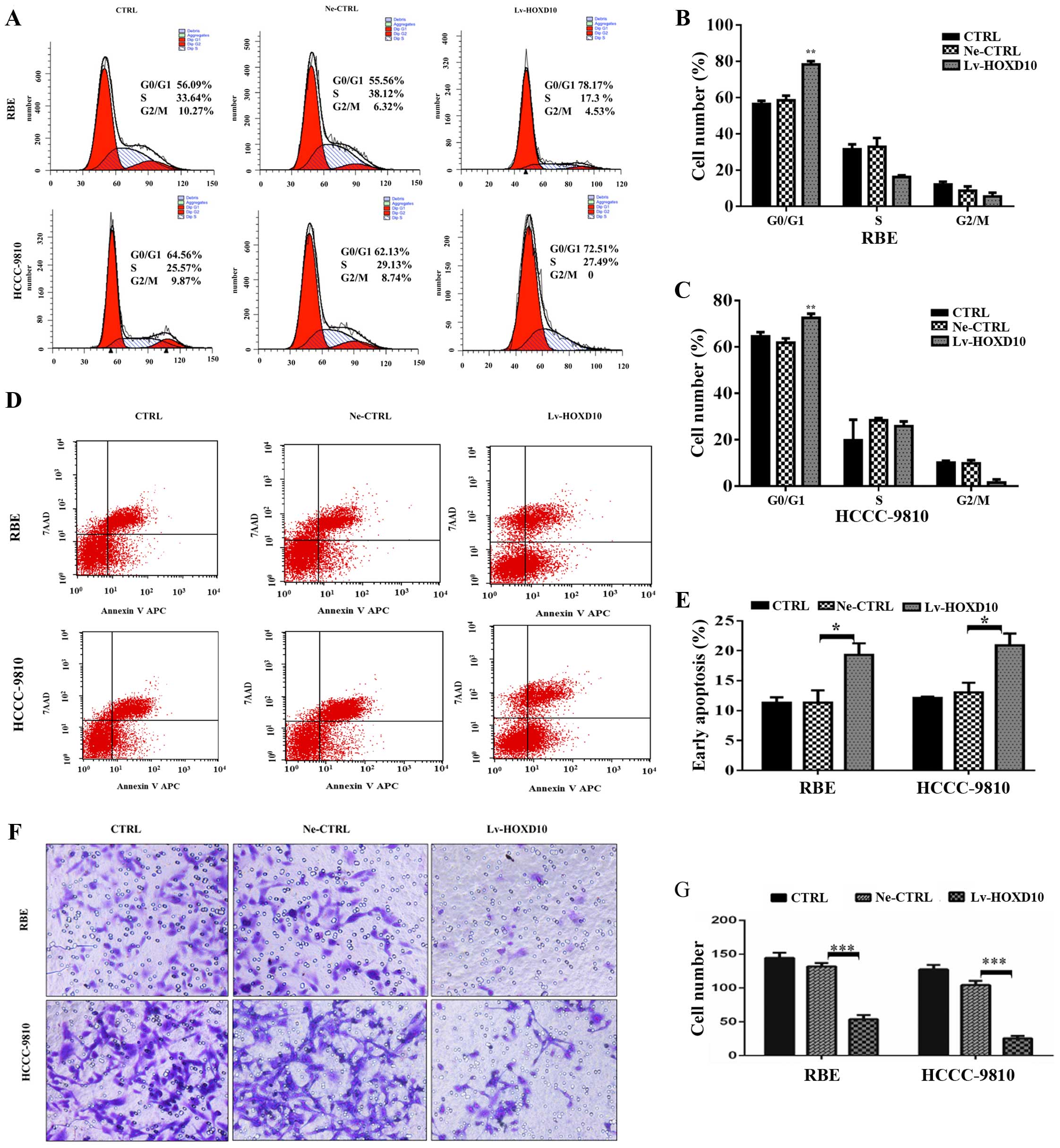
The effect of overexpression of HOXD10 on cell cycle
progression was examined via PI staining followed by FACS analysis.
As shown in Fig. 3A–C, cells
overexpressing HOXD10 accumulated in the G1 phase compared with the
control cells and showed a corresponding decrease in cell numbers
in the S and G2/M phase. Additionally, the percentages of early
cell apoptosis (right lower quadrant) were markedly increased in
the two CCC cell lines after transfection with HOXD10 lentivirus
(Fig. 3D and E, P<0.05). These
results indicated that stable HOXD10 overexpression inhibited RBE
and HCCC-9810 cell proliferation by inducing G1/S phase arrest and
apoptosis.
Effect of HOXD10 overexpression on
invasive potential of RBE and HCCC-9810 cells
The clinical spread of CCC is characterized by
expansion and invasive growth along the lymphangion or perineurium
or direct invasion into the liver. HOXD10 has been shown to mediate
the invasion of breast, gastric, malignant glioma, ovarian, bladder
and hepatocellular cancer (12–15,18,19).
Thus, we examined whether HOXD10 was involved in the invasion of
RBE and HCCC-9810 cells. A Matrigel invasion Transwell assay was
conducted to confirm the effect of HOXD10 on the invasive
properties of cholangiocarcinoma cell lines. As expected, stable
overexpression of HOXD10 significantly decreased the invasive
potential of both the RBE and HCCC-9810 cell lines (Fig. 3F and G, P<0.001), suggesting that
HOXD10 was associated with the metastatic capacity of CCC. These
results elucidated the aforementioned correlation of lower HOXD10
expression with poor prognosis of CCC patients. Furthermore, the
effects of upregulated HOXD10 on the expression of tumor invasion
compared to the regulators were examined using RT-PCR and western
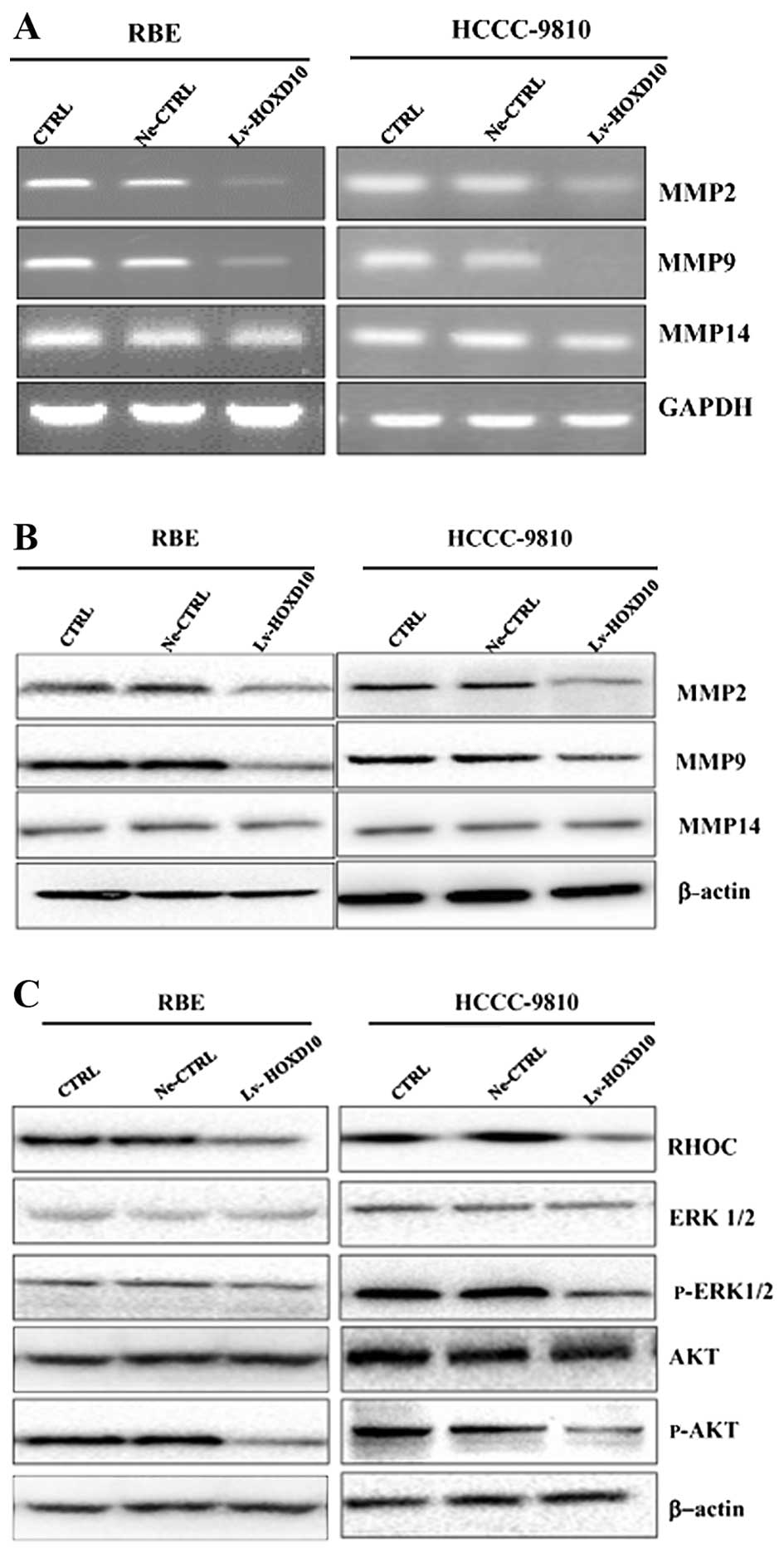
blot analysis. As shown in Fig. 4A and
B, the mRNA and protein expression of MMP2 and MMP9 was
significantly inhibited in the Lv-HOXD10 group compared with the
Ne-CTRL and CTRL group, while no significant change was observed in
the expression of MMP14. These results suggested that
overexpression of HOXD10 inhibited the invasion of CCC cells,
possibly partly by disturbing the expression of MMP2 and MMP9.
Involvement of RHOC/AKT and MAPK pathways
in tumor-suppresive effect of HOXD10
Upregulated expression of HOXD10 resulted in the
decreased expression of tumor metastatic-associated gene,
RHOC. Since we observed a significant correlation between
HOXD10 and RHOC expression and CCC patient prognosis, it was
suggested that HOXD10 may inhibit CCC cell growth and metastasis by
reducing RHOC signaling. As shown in Fig. 4C, the RHOC protein levels were
markedly reduced in the Lv-HOXD10 group. As RHOC promotes tumor
metastasis in distinct carcinomas by stimulating the activity of a
series of kinases including PI3K/AKT and mitogen-activated protein
kinase (MAPK) in prostate, head and neck, as well as gastric and
breast cancers, we investigated the AKT and ERK phosphorylation
states in the two CCC cell lines (18,19,22–24).
As expected, the upregulated expression of HOXD10 led to AKT and
ERK dephosphorylation, showing that the PI3K/AKT and MAPK pathways
were significantly inactivated (Fig.
4C). These results suggested that RHOC was a key negative
mediator of HOXD10-dependent CCC development and progression and
that the PI3K/AKT and MAPK pathways were involved in this
process.
Discussion
CCC is a highly lethal cancer due to lack of early
detection, resistance to chemoradiotherapy and high propensity to
invade locally and distantly (25).
Current therapeutic approaches for highly invasive
cholangiocarcinoma are not very effective (26). The low overall survival rate of CCC
has led investigators to investigate the mechanisms involved in the
characteristic development and progression of CCC to identify
effective therapeutic methods.
In the present study, IHC staining for HOXD10 was
performed in a large cohort of CCC patients with complete
clinicopathological and follow-up data. Our results clearly showed
that the positive rate of HOXD10 protein decreased gradually with
the increase of histological grade in CCC patients, which suggests
HOXD10 is involved in the malignant progression of CCC. These
results are consistent with those of previous studies in gastric,
ovarian and hepatocellular carcinoma (11,13,27,28).
In the univariate analysis of the present study, we found that the
prognosis for patients with a positive HOXD10 protein expression
was better than that of patients with a negative HOXD10 protein
expression. Furthermore, a positive expression of HOXD10 was an
independent predictor for longer survival in CCC patients as
evidenced by the Kaplan-Meier curves and multivariable Cox
proportional hazards regression analysis. Therefore, HOXD10 is a
potential therapeutic target for CCC treatment and may also be used
as a potential prognostic marker for CCC patients.
To evaluate the biological significance of HOXD10 in
CCC pathogenesis, we employed a lentiviral-mediated HOXD10
overexpression vector to effectively and sustainably increase
HOXD10 expression in the RBE and HCCC-9810 cholangiocarcinoma cell
lines. We found that ectopic overexpression of HOXD10 significantly
inhibited RBE and HCCC-9810 cell proliferation, which can be partly
attributed to the induction of a G1-phase cell cycle arrest and
increased apoptosis in vitro, suggesting that HOXD10 plays
an important suppressive role in CCC cells. Additionally, the
overexpression of HOXD10 markedly inhibited the cell invasion
potential of cholangiocarcinoma cells, at least partly, by
downregulating the expression of invasive factors MMP2 and MMP9,
but not that of MMP14. Thus, more studies are needed to determine
the precise molecular mechanisms by which HOXD10 overexpression
inhibits invasion in RBE and HCCC-9810 cell lines.
The results of the present study provide evidence
for the tumor-suppressive properties of HOXD10 in CCC cell lines.
However, the underlying mechanisms of HOXD10 in the malignant
progression of cholangiocarcinoma, particularly the downstream
signaling pathways, remain unclear. RHOC belongs to RHO family
proteins, which regulate extracellular stimuli-mediated signaling
pathways that control numerous intracellular processes, including
actin cytoskeletal organization, gene expression, invasion and cell
cycle progression (22,29–31).
RHOC has been characterized as an oncogenic kinase that promotes
cancer cell proliferation, invasion and migration (32–34).
High levels of RHOC activity are associated with metastatic lesions
and a poor clinical outcome (35,36).
RHOC has been identified as a downstream major effector of HOXD10
in breast and gastric cancer cells (18,19).
In the present study, the IHC analysis of CCC samples showed that a
lower HOXD10 expression was directly associated with a higher
expression of RHOC. Additionally, western blot analysis indicated
that the overexpression of HOXD10 significantly downregulated RHOC
expression in RBE and HCCC-9810 cell lines. Since AKT and MAPK
(ERK) kinases are known to be involved in RHOC downstream signaling
pathways, we determined AKT and ERK1/2 activities and found that
HOXD10/RHOC expression affected AKT and ERK1/2 phosphorylation,
suggesting that these signaling pathways are involved in the
development of HOXD10-dependent cholangiocarcinoma (15,23,24).
PI3K/AKT/MAPK pathways have been found to play a
vital role in cholangiocarcinoma (37–39).
Okada et al reported that rapamycin, an inhibitor of the
PI3K/AKT/mTOR pathway, effectively inhibited the growth of
cholangiocarcinoma cell lines with a decreased AKT expression
significantly in a dose-dependent manner (40). Sorafenib, a specific inhibitor of
the Ras-Raf-Mek-Erk pathway, was administered in patients with
advanced biliary cancers in a phase II clinical study. The median
progression-free and overall survival with sorafenib were not
inferior to those reported with cytotoxic chemotherapy regimens in
biliary cancer patients (41). The
aforementioned studies revealed the potential value of targeting
the AKT/MAPK (ERK) pathway in CCC treatment. The results of this
study provide a further molecular basis for this role.
Although the functions of tumor suppression of
HOXD10 have been evaluated, the results of previous studies have
also indicated that HOXD10 has complicated roles in certain cell
type tumors. For example, the expression levels of HOXD10 were
higher in oral squamous cell carcinoma samples compared to those in
normal oral mucosa (16).
Overexpression of HOXD10 decreased cell invasion but increased
proliferation, adhesion and migration in HNSCC cell lines (16). In addition, it was reported that
HOXD10 is not involved in the inhibition of the tumor growth of
primary breast cancer but markedly suppresses the formation of lung
metastases in a mouse mammary tumor model (42). Thus, whether HOXD10 is
anti-tumorigenic or pro-tumorigenic depends on the cell context and
the type of stimulus (7). In the
present study, downregulation or loss of HOXD10 may contribute to
CCC malignant progression. However, the precise mechanism of
dysregulation of HOXD10 in CCC is not clear. In gastric carcinoma,
the downregulation or loss of HOXD10 expression occurs due to
promoter methylation (11). By
contrast, HOXD10 was negatively regulated by miR-10b via a specific
target site within the 3′UTR of HOXD10 at the post-transcriptional
level in breast cancer (18). Other
regulation mechanisms of HOXD10 include the possible role of long
non-coding RNAs such as HOX transcript antisense RNA (HOTAIR) and
histone modification (7,43). However, the underlying mechanism of
HOXD10 downregulation in CCC remains to be investigated.
In conclusion, HOXD10 plays an inhibitory role in
CCC development and progression possibly via the RHOC/AKT/MAPK
(ERK) pathways, suggesting that HOXD10 is a potential target for
treating CCC.
Acknowledgments
This study was supported by the National Natural
Science Foundation of China (no. 81172026).
References
|
1
|
Lazaridis KN and Gores GJ:
Cholangiocarcinoma. Gastroenterology. 128:1655–1667. 2005.
View Article : Google Scholar : PubMed/NCBI
|
|
2
|
Mosconi S, Beretta GD, Labianca R, Zampino
MG, Gatta G and Heinemann V: Cholangiocarcinoma. Crit Rev Oncol
Hematol. 69:259–270. 2009. View Article : Google Scholar
|
|
3
|
Razumilava N and Gores GJ:
Cholangiocarcinoma. Lancet. 383:2168–2179. 2014. View Article : Google Scholar : PubMed/NCBI
|
|
4
|
Cardinale V, Semeraro R, Torrice A, Gatto
M, Napoli C, Bragazzi MC, Gentile R and Alvaro D: Intra-hepatic and
extra-hepatic cholangiocarcinoma: New insight into epidemiology and
risk factors. World J Gastrointest Oncol. 2:407–416. 2010.
View Article : Google Scholar : PubMed/NCBI
|
|
5
|
Cillo C: HOX genes in human cancers.
Invasion Metastasis. 14:38–49. 1994–1995.
|
|
6
|
Quinonez SC and Innis JW: Human HOX gene
disorders. Mol Genet Metab. 111:4–15. 2014. View Article : Google Scholar
|
|
7
|
Shah N and Sukumar S: The Hox genes and
their roles in oncogenesis. Nat Rev Cancer. 10:361–371. 2010.
View Article : Google Scholar : PubMed/NCBI
|
|
8
|
Carrio M, Arderiu G, Myers C and Boudreau
NJ: Homeobox D10 induces phenotypic reversion of breast tumor cells
in a three-dimensional culture model. Cancer Res. 65:7177–7185.
2005. View Article : Google Scholar : PubMed/NCBI
|
|
9
|
Wang YF, Li Z, Zhao XH, Zuo XM, Zhang Y,
Xiao YH, Li J and Peng ZH: MicroRNA-10b is upregulated and has an
invasive role in colorectal cancer through enhanced Rhoc
expression. Oncol Rep. 33:1275–1283. 2015.PubMed/NCBI
|
|
10
|
Vardhini NV, Rao PJ, Murthy PB and
Sudhakar G: HOXD10 expression in human breast cancer. Tumour Biol.
35:10855–10860. 2014. View Article : Google Scholar : PubMed/NCBI
|
|
11
|
Wang L, Chen S, Xue M, Zhong J, Wang X,
Gan L, Lam EK, Liu X, Zhang J, Zhou T, et al: Homeobox D10 gene, a
candidate tumor suppressor, is downregulated through promoter
hypermethylation and associated with gastric carcinogenesis. Mol
Med. 18:389–400. 2012.
|
|
12
|
Li Q, Ding C, Chen C, Zhang Z, Xiao H, Xie
F, Lei L, Chen Y, Mao B, Jiang M, et al: miR-224 promotion of cell
migration and invasion by targeting homeobox D 10 gene in human
hepatocellular carcinoma. J Gastroenterol Hepatol. 29:835–842.
2014. View Article : Google Scholar
|
|
13
|
Nakayama I, Shibazaki M, Yashima-Abo A,
Miura F, Sugiyama T, Masuda T and Maesawa C: Loss of HOXD10
expression induced by upregulation of miR-10b accelerates the
migration and invasion activities of ovarian cancer cells. Int J
Oncol. 43:63–71. 2013.PubMed/NCBI
|
|
14
|
Sasayama T, Nishihara M, Kondoh T, Hosoda
K and Kohmura E: MicroRNA-10b is overexpressed in malignant glioma
and associated with tumor invasive factors, uPAR and RhoC. Int J
Cancer. 125:1407–1413. 2009. View Article : Google Scholar : PubMed/NCBI
|
|
15
|
Xiao H, Li H, Yu G, Xiao W, Hu J, Tang K,
Zeng J, He W, Zeng G, Ye Z, et al: MicroRNA-10b promotes migration
and invasion through KLF4 and HOXD10 in human bladder cancer. Oncol
Rep. 31:1832–1838. 2014.PubMed/NCBI
|
|
16
|
Hakami F, Darda L, Stafford P, Woll P,
Lambert DW and Hunter KD: The roles of HOXD10 in the development
and progression of head and neck squamous cell carcinoma (HNSCC).
Br J Cancer. 111:807–816. 2014. View Article : Google Scholar : PubMed/NCBI
|
|
17
|
Edge SBBD; Compton CC, Fritz AG, Greene FL
and Trotti A: AJCC Cancer Staging Manual. 7th edition. Springer;
New York: pp. 60–62. pp. 66–71. 2010
|
|
18
|
Ma L, Teruya-Feldstein J and Weinberg RA:
Tumour invasion and metastasis initiated by microRNA-10b in breast
cancer. Nature. 449:682–688. 2007. View Article : Google Scholar : PubMed/NCBI
|
|
19
|
Liu Z, Zhu J, Cao H, Ren H and Fang X:
miR-10b promotes cell invasion through RhoC-AKT signaling pathway
by targeting HOXD10 in gastric cancer. Int J Oncol. 40:1553–1560.
2012.PubMed/NCBI
|
|
20
|
Zhao ZH, Tian Y, Yang JP, Zhou J and Chen
KS: RhoC, vascular endothelial growth factor and microvascular
density in esophageal squamous cell carcinoma. World J
Gastroenterol. 21:905–912. 2015.PubMed/NCBI
|
|
21
|
Gou WF, Zhao Y, Lu H, Yang XF, Xiu YL,
Zhao S, Liu JM, Zhu ZT, Sun HZ, Liu YP, et al: The role of RhoC in
epithelial-to-mesenchymal transition of ovarian carcinoma cells.
BMC Cancer. 14:4772014. View Article : Google Scholar : PubMed/NCBI
|
|
22
|
Iiizumi M, Bandyopadhyay S, Pai SK, Watabe
M, Hirota S, Hosobe S, Tsukada T, Miura K, Saito K, Furuta E, et
al: RhoC promotes metastasis via activation of the Pyk2 pathway in
prostate cancer. Cancer Res. 68:7613–7620. 2008. View Article : Google Scholar : PubMed/NCBI
|
|
23
|
Bu Q, Tang HM, Tan J, Hu X and Wang DW:
Expression of RhoC and ROCK-1 and their effects on MAPK and Akt
proteins in prostate carcinoma. Zhonghua Zhong Liu Za Zhi.
33:202–206. 2011.In Chinese. PubMed/NCBI
|
|
24
|
Islam M, Datta J, Lang JC and Teknos TN:
Downregulation of RhoC by microRNA-138 results in de-activation of
FAK, Src and Erk1/2 signaling pathway in head and neck squamous
cell carcinoma. Oral Oncol. 50:448–456. 2014. View Article : Google Scholar : PubMed/NCBI
|
|
25
|
Mathema VB and Na-Bangchang K: Current
insights on cholangiocarcinoma research: A brief review. Asian Pac
J Cancer Prev. 16:1307–1313. 2015. View Article : Google Scholar : PubMed/NCBI
|
|
26
|
Ulahannan SV, Rahma OE, Duffy AG,
Makarova-Rusher OV, Kurtoglu M, Liewehr DJ, Steinberg SM and Greten
TF: Identification of active chemotherapy regimens in advanced
biliary tract carcinoma: A review of chemotherapy trials in the
past two decades. Hepat Oncol. 2:39–50. 2015. View Article : Google Scholar : PubMed/NCBI
|
|
27
|
Liao CG, Kong LM, Zhou P, Yang XL, Huang
JG, Zhang HL and Lu N: miR-10b is overexpressed in hepatocellular
carcinoma and promotes cell proliferation, migration and invasion
through RhoC, uPAR and MMPs. J Transl Med. 12:2342014. View Article : Google Scholar : PubMed/NCBI
|
|
28
|
Redline RW, Hudock P, MacFee M and
Patterson P: Expression of AbdB-type homeobox genes in human
tumors. Lab Invest. 71:663–670. 1994.PubMed/NCBI
|
|
29
|
Ruth MC, Xu Y, Maxwell IH, Ahn NG, Norris
DA and Shellman YG: RhoC promotes human melanoma invasion in a
PI3K/Akt-dependent pathway. J Invest Dermatol. 126:862–868. 2006.
View Article : Google Scholar : PubMed/NCBI
|
|
30
|
Ridley AJ: RhoA, RhoB and RhoC have
different roles in cancer cell migration. J Microsc. 251:242–249.
2013. View Article : Google Scholar : PubMed/NCBI
|
|
31
|
Oxford G and Theodorescu D: Ras
superfamily monomeric G proteins in carcinoma cell motility. Cancer
Lett. 189:117–128. 2003. View Article : Google Scholar
|
|
32
|
Karlsson R, Pedersen ED, Wang Z and
Brakebusch C: Rho GTPase function in tumorigenesis. Biochim Biophys
Acta. 1796:91–98. 2009.PubMed/NCBI
|
|
33
|
Tumur Z, Katebzadeh S, Guerra C, Bhushan
L, Alkam T and Henson BS: RhoC mediates epidermal growth
factor-stimulated migration and invasion in head and neck squamous
cell carcinoma. Neoplasia. 17:141–151. 2015. View Article : Google Scholar : PubMed/NCBI
|
|
34
|
Chen R, Cheng Y, Zhang Y, Li Z and Geng L:
RhoC mediates invasion and migration of CaSki cells through the
Rho-associated serine-threonine protein kinase 1 signaling pathway.
Int J Gynecol Cancer. 24:184–191. 2014. View Article : Google Scholar : PubMed/NCBI
|
|
35
|
Bellovin DI, Simpson KJ, Danilov T,
Maynard E, Rimm DL, Oettgen P and Mercurio AM: Reciprocal
regulation of RhoA and RhoC characterizes the EMT and identifies
RhoC as a prognostic marker of colon carcinoma. Oncogene.
25:6959–6967. 2006. View Article : Google Scholar : PubMed/NCBI
|
|
36
|
Wang W, Yang LY, Yang ZL, Peng JX and Yang
JQ: Elevated expression of autocrine motility factor receptor
correlates with overexpression of RhoC and indicates poor prognosis
in hepato-cellular carcinoma. Dig Dis Sci. 52:770–775. 2007.
View Article : Google Scholar : PubMed/NCBI
|
|
37
|
Maemura K, Natsugoe S and Takao S:
Molecular mechanism of cholangiocarcinoma carcinogenesis. J
Hepatobiliary Pancreat Sci. 21:754–760. 2014. View Article : Google Scholar : PubMed/NCBI
|
|
38
|
Dokduang H, Juntana S, Techasen A, Namwat
N, Yongvanit P, Khuntikeo N, Riggins GJ and Loilome W: Survey of
activated kinase proteins reveals potential targets for
cholangiocarcinoma treatment. Tumour Biol. 34:3519–3528. 2013.
View Article : Google Scholar : PubMed/NCBI
|
|
39
|
Leelawat K, Udomchaiprasertkul W, Narong S
and Leelawat S: Induction of MKP-1 prevents the cytotoxic effects
of PI3K inhibition in hilar cholangiocarcinoma cells. J Cancer Res
Clin Oncol. 136:1537–1544. 2010. View Article : Google Scholar : PubMed/NCBI
|
|
40
|
Okada T, Sawada T and Kubota K: Rapamycin
inhibits growth of cholangiocarcinoma cells.
Hepatogastroenterology. 56:6–10. 2009.PubMed/NCBI
|
|
41
|
El-Khoueiry AB, Rankin CJ, Ben-Josef E,
Lenz HJ, Gold PJ, Hamilton RD, Govindarajan R, Eng C and Blanke CD:
SWOG 0514: A phase II study of sorafenib in patients with
unresectable or metastatic gallbladder carcinoma and
cholangiocarcinoma. Invest New Drugs. 30:1646–1651. 2012.
View Article : Google Scholar :
|
|
42
|
Ma L, Reinhardt F, Pan E, Soutschek J,
Bhat B, Marcusson EG, Teruya-Feldstein J, Bell GW and Weinberg RA:
Therapeutic silencing of miR-10b inhibits metastasis in a mouse
mammary tumor model. Nat Biotechnol. 28:341–347. 2010. View Article : Google Scholar : PubMed/NCBI
|
|
43
|
Zhang H, Cai K, Wang J, Wang X, Cheng K,
Shi F, Jiang L, Zhang Y and Dou J: miR-7, inhibited indirectly by
lincRNA HOTAIR, directly inhibits SETDB1 and reverses the EMT of
breast cancer stem cells by downregulating the STAT3 pathway. Stem
Cells. 32:2858–2868. 2014. View Article : Google Scholar : PubMed/NCBI
|