Introduction
Non-alcoholic fatty liver disease (NAFLD) includes a
broad spectrum of disorders from NAFL to non-alcoholic
steatohepatitis (NASH) and steatofibrosis. Histologically,
hepatocyte steatosis, hepatocyte ballooning, hepatic inflammation
and fibrosis characterize NASH (1). The majority of patients with NAFL
present no symptoms; however, ~20% of patients with NAFL progress
to NASH, or even cirrhosis, portal hypertension and hepatocellular
carcinoma (HCC) (1). Hepatic
inflammation is associated with the prognosis of patients with
NAFLD. Globally, a total of 40.76% patients with NASH progress to
fibrosis and end stage liver disease (2). Until now, only a limited number of
established medications for NASH are clinically applicable.
Therefore, a better understanding of the underlying mechanisms
leading to NAFLD progression is required, which may in turn improve
the efficacy of NASH treatments. During the progression of
steatosis to NASH, it has been confirmed that hepatocellular injury
and chronic inflammation are the critical mediators (2). This inflammation is associated with
recruitment of macrophages to the liver and the expression of
pro-inflammatory factors, including the chemokine monocyte
chemoattractant protein-1 (MCP-1) and tumor necrotic factor-α
(TNF-α) (3). On the basis of lipid
toxicity, the generation and secretion of MCP-1 by hepatocytes
increases, which in turn interact with C-C chemokine receptor 2
(CCR2) on the surface of macrophages, and mediate the recruitment
and activation of liver macrophages. In addition, increased amounts
of pro-inflammatory and pro-fibrotic factors are released by liver
macrophages. In patients with NASH, the activation of hepatic
macrophages and their pro-inflammatory activity are markers of
disease progression, which affect fatty degeneration, attract
lymphocytes, stimulate angiogenesis and promote liver fibrosis
(3). Macrophages differentiate
into two cellular subtypes: Pro-inflammatory M1 macrophages and
immune-regulatory M2 macrophages. M1 type cells highly express CD86
and CD80, and secrete pro-inflammatory cytokines, including
interleukin (IL)-1β and TNF-α, whereas M2 type cells mainly express
CD206, CD163 and Arginase 1 (Arg1) and secrete factors such as IL-4
and IL-10 (4). MCP-1 inhibition
reduces the infiltration of M1 macrophages and prevents the M2 type
transformation to the M1 type, interrupting NASH progression
(5,6).
Bone morphogenetic protein-9 (BMP-9), also termed
growth differentiation factor-2, belongs to the TGF-β superfamily
and was first cloned from a fetal mouse liver cDNA library
(7). The precursor of human BMP-9
is comprised of 429 amino acids with a molecular weight of ~47 kDa.
Following post-transcriptional modification, the immature precursor
is divided into a pro-region and a mature region (13 kDa). However,
both dimers of the mature regions and BMP-9 pro-region complexes
have the same biological functions after secretion (8). BMP-9 is predominantly produced by the
liver and constitutively circulates at relevant physiological
levels in the bloodstream of healthy individuals (9). After BMP-9 binding to the type II
receptor or the type I receptor on the cell surface, a
receptor-complex is formed and the SMAD family member 1 (Smad1)
signaling pathway is activated. Phosphorylated Smad1 binds to Smad4
and this complex translocates into the cell nucleus, which
regulates the expression of BMP-9 target genes (10). Emerging evidence has indicated that
BMP-9 participates in various physiologic processes, including bone
formation, glucose homeostasis, iron homeostasis and angiogenesis
(11–14). Pathologically, BMP-9 takes part in
the occurrence and development of various types of tumors (10) including HCC (15,16).
Recently, BMP-9 was found to mediate lipid metabolism and the
expression of chemokines (17,18).
In endothelial cells, BMP-9 mediated the expression of MCP-1
(17,18).
It has been previously reported that BMP-9 enhances
liver fibrogenesis (19). Kim
et al (20) further
demonstrated that MB109, a recombinant BMP-9 derivative, could
induce the hepatic expression of fatty acid synthetase in obese
mice and reduced the content of lipid droplets, as well as the
serum level of alanine aminotransferase (ALT) and total
cholesterol. Although BMP-9 has been shown to ameliorate NAFLD in a
high-fat diet model (20), there
is no data regarding the role of BMP-9 in the methionine- and
choline-deficient (MCD)-diet model of NASH. Therefore, the aim of
the present study was to clarify the contribution of BMP-9 to liver
disease in mice fed a MCD diet. This model has been widely accepted
as the classic model to study the underlying mechanisms of NASH. In
the present study, it was demonstrated that adenoviral gene
transfer of BMP-9 via the tail vein elevated BMP-9 levels in the
liver, and promoted the progression of NASH by inducing the
secretion of inflammatory factors and M1 macrophage
infiltration.
Materials and methods
Adenoviruses
Adenoviruses Ad-BMP-9-HA(c) and Adnull were
commercially purchased from SinoGenoMax Co., Ltd.
Animal model
Specific pathogen free C57BL/6 mice (male, 6 weeks,
18–20 g) were used in the present study. Mice were maintained in a
standard 12-h light/dark cycle environment with a constant
temperature (22±2°C) and humidity (40–60%) and free access to chow
and water. The ingredients comprising the MCD are listed in
Table SI. A total of 48 mice were
divided into four groups: Control, MCD, MCD+Ad-BMP-9-HA(c) and
MCD+Adnull group (n=12/group). Six mice in each group were fed
their assigned diet for 2 weeks and an additional 6 mice in each
group were fed their assigned diet for 4 weeks. In the control
group, mice were fed a chow diet and in the MCD groups, mice were
fed the MCD diet. In the MCD+adenovirus groups, mice received
1×109 plaque forming unit (PFU) of adenovirus vectors
via the tail vein once a week for 4 weeks. Animals were sacrificed
24 h after the end of their 2 and 4 weeks diet periods,
respectively. Mouse cardiac blood samples were taken to measure ALT
and aspartate transaminase (AST) levels. Liver tissues were fixed
in 4% paraformaldehyde at room temperature for >24 h or frozen
for subsequent staining experiments. The remaining liver tissues
were frozen at −80°C and subsequently used for reverse
transcription-quantitative (RT-qPCR).
All animal experiments were approved by the Animal
Care and Use Committee at Tongji Medical College, Huazhong
University of Science and Technology and in full compliance with
Hubei Province Laboratory Animal Care Guidelines for the use of
animals in research (21).
ALT, AST and liver triglyceride (TG)
content measurement
The serum levels of ALT/AST and the liver TG content
were determined using commercially available reagents (ALT:C009-2,
AST:C0010-2 and TG:A110-1; Nanjing Jiancheng Bioengineering
Institute) according to the manufacturer's instructions.
Histology and immunohistochemistry
(IHC)
Mouse liver tissues were fixed in 4%
paraformaldehyde at room temperature for >24 h, and embedded in
paraffin. For hematoxylin-eosin (H&E) staining, liver sections
(4 µm) were dewaxed, stained with hematoxylin for 5 min and
differentiated with 1% hydrochloric acid alcohol for 5–10 sec, then
stained with eosin and followed by dehydration. For Sirius red
staining, dewaxed liver sections were stained with Sirius red stain
for 1 h and Mayer hematoxylin stain for 10 min. For Oil red O
staining, frozen liver sections (8 µm) were fixed in 4%
paraformaldehyde for 10 min and washed with deionized water, then
stained with Oil Red O working solution (Sigma-Aldrich) for 10 min
at room temperature and washed in deionized water, and finally
stained with hematoxylin. IHC staining was performed as previously
described (15). Briefly, the
sections were deparaffinized in xylene, rehydrated in graded
ethanol and washed in distilled water. Antigen retrieval was
performed with microwave in EDTA buffer (1 mM, pH 8.0) at 100°C for
15 min. The slides were immersed in 3% H2O2
for 30 min at room temperature and then washed with PBS three
times. Then, Dako peroxidase blocking reagent (Agilent
Technologies, Inc.) was used to block the endogenous peroxidase at
room temperature for 15 min. Slides were incubated with primary
antibodies including F4/80 (1:200; cat. no. 27044-1-AP; ProteinTech
Group, Inc.), inducible nitric oxide synthase (iNOS; 1:200; cat.
no. 18985-1-AP; ProteinTech Group, Inc.), CD206 (1:100; cat. no.
18704-1-AP; ProteinTech Group, Inc.) and α-smooth muscle actin
(α-SMA; 1:200; cat. no. 14395-1-AP; ProteinTech Group, Inc.) at 4°C
overnight. On the following day, the slides were warmed to the room
temperature and washed with PBS three times before being incubated
with HRP-conjugated Affinipure Goat Anti-Rabbit IgG(H+L) secondary
antibodies (1:200; cat. no. SA00001-2;, ProteinTech Group, Inc.) at
room temperature for 1 h. The immune-reactivity were visualized
with a Dako REAL EnVision Detection System, Peroxidase/DAB+ kit
(cat. no. K5007, Agilent Technologies, Inc.). Then the slides were
counterstained with hematoxylin at room temperature for 5 min. All
staining images of H&E, Sirius red, Oil red O and IHC were
acquired on a routine light microscope.
For semi-quantitative analysis of the iNOS
immunostaining, positively stained cells presenting maximal
immune-positivity were counted using a light microscope in four
fields in each section at ×40 magnification and analyzed using
ImageJ software version 1.8.0 (National Institute of Health). The
numbers of positively stained macrophages were statistically
compared in the 4 groups.
For semi-quantitative analysis of F4/80, α-SMA
immunostaining and Sirius red staining, the percentage of
positively stained areas were counted in four fields under a
microscope at ×20 magnification and analyzed using ImageJ software
version 1.8.0 (National Institute of Health). The percentage area
of positive staining was statistically compared in the 4
groups.
The histological scoring of the liver lesions was
evaluated with NAFLD activity score (NAS). The NAS scores for
steatosis were 0–3, for lobular inflammation were 0–3 and for
ballooning were 0–2; therefore the scores ranged from 0 to 8
(22,23).
RNA isolation, cDNA synthesis and
RT-qPCR
Total RNA from cells and liver tissue samples was
isolated using TRIzol® Reagent (Takara Biotechnology
Co., Ltd.) and reverse transcribed into cDNA using a PrimeScript™
RTase kit (Takara Biotechnology Co., Ltd.) according to the
manufacturer's protocol (37°C for 15 min, 85°C for 5 sec, then
cooled to 8°C). RT-qPCR was conducted using the SYBR Green PCR
Master Mix (Takara Biotechnology Co., Ltd.). Primer sequences are
listed in Table I. cDNA samples
were amplified in duplicate using LightCycler 480 Software version
1.5.0 (Roche Diagnostics GmbH). The RT-qPCR thermocycling
conditions were as follows: 95°C for 10 min, followed by 40 cycles
of 95°C for 15 sec and 60°C for 1 min. Fluorescence data of the
target genes were analyzed using the 2−ΔΔCq method
(24) for relative quantification
using β-actin as a control.
 | Table I.Primer sequences for reverse
transcription-quantitative PCR. |
Table I.
Primer sequences for reverse
transcription-quantitative PCR.
| Primer | Forward
(5′-3′) | Reverse
(5′-3′) |
|---|
| β-actin |
GGCTGTATTCCCCTCCATCG |
CCAGTTGGTAACAATGCCATGT |
| BMP-9 |
CAGAACTGGGAACAAGCATCC |
GCCGCTGAGGTTTAGGCTG |
| CCR2 |
ATCCACGGCATACTATCAACATC |
CAAGGCTCACCATCATCGTAG |
| Collagen Ia1 |
GCTCCTCTTAGGGGCCACT |
CCACGTCTCACCATTGGGG |
| TGF-β1 |
CTCCCGTGGCTTCTAGTGC |
GCCTTAGTTTGGACAGGATCTG |
| α-SMA |
GTCCCAGACATCAGGGAGTAA |
TCGGATACTTCAGCGTCAGGA |
| MMP-2 |
CAAGTTCCCCGGCGATGTC |
TTCTGGTCAAGGTCACCTGTC |
| MMP-9 |
CTGGACAGCCAGACACTAAAG |
CTCGCGGCAAGTCTTCAGAG |
| CTGF |
GGGCCTCTTCTGCGATTTC |
ATCCAGGCAAGTGCATTGGTA |
| MCP-1 |
ATCCACGGCATACTATCAACATC |
CAAGGCTCACCATCATCGTAG |
| TNF-α |
CCCTCACACTCAGATCATCTTCT |
GCTACGACGTGGGCTACAG |
| IL-10 |
GCTCTTACTGACTGGCATGAG |
CGCAGCTCTAGGAGCATGTG |
| PAI-1 |
TTCAGCCCTTGCTTGCCTC |
ACACTTTTACTCCGAAGTCGGT |
| F4/80 |
TGACTCACCTTGTGGTCCTAA |
CTTCCCAGAATCCAGTCTTTCC |
| iNOS |
GTTCTCAGCCCAACAATACAAGA |
GTGGACGGGTCGATGTCAC |
| IL-1β |
GCAACTGTTCCTGAACTCAACT |
ATCTTTTGGGGTCCGTCAACT |
| IL-6 |
TAGTCCTTCCTACCCCAATTTCC |
TTGGTCCTTAGCCACTCCTTC |
| IL-12 |
TGGTTTGCCATCGTTTTGCTG |
ACAGGTGAGGTTCACTGTTTCT |
| IL-17 |
TCAGCGTGTCCAAACACTGAG |
CGCCAAGGGAGTTAAAGACTT |
Protein extraction and western blot
assay
Total protein samples were extracted by treating
liver tissues with RIPA lysis buffer and protease inhibitor
cocktail tablets. Proteins were denatured at 100°C for 10 min, then
were stored at −20°C or used for western blot assay immediately.
Proteins were separated by 10% SDS-PAGE Gel (Beyotime, P0012A) and
then transferred to polyvinylidene difluoride (PVDF) membranes (EMD
Millipore). The membranes with proteins were blocked with 8%
skimmed milk at room temperature for 1 h and incubated with BMP9
primary antibodies (1:2,000, AF-3209, R&D Systems) at 4°C
overnight. Then, the membranes were incubated with secondary
antibody of Rabbit anti Goat IgG (H L) labeled with HRP (1:2,000,
ANT021s, Antgene Biotechnology Co., Ltd.) for 1 h at room
temperature. Then immunoreactive protein bands were visualized with
chemiluminescence (ECL) kit (P0018S; Beyotime Institute of
Biotechnology).
Statistical analysis
The quantitative data were presented as the mean ±
standard deviation and presented graphically as the mean ± standard
error of the mean. Comparisons between two groups were performed
with Student's t-test. Comparisons between multiple groups were
performed using one-way analysis of variance and Tukey's multiple
comparisons test. P<0.05 was considered to indicate a
statistically significant comparison.
Results
BMP-9 mRNA expression is significantly
induced in the liver tissues of NASH model mice
NASH is histologically diagnosed with hepatocyte
steatosis, hepatocyte ballooning and hepatic inflammation (22). In the present study, an MCD-induced
NASH model was successfully established, being characterized with
hepatocyte steatosis, hepatocyte ballooning and hepatic
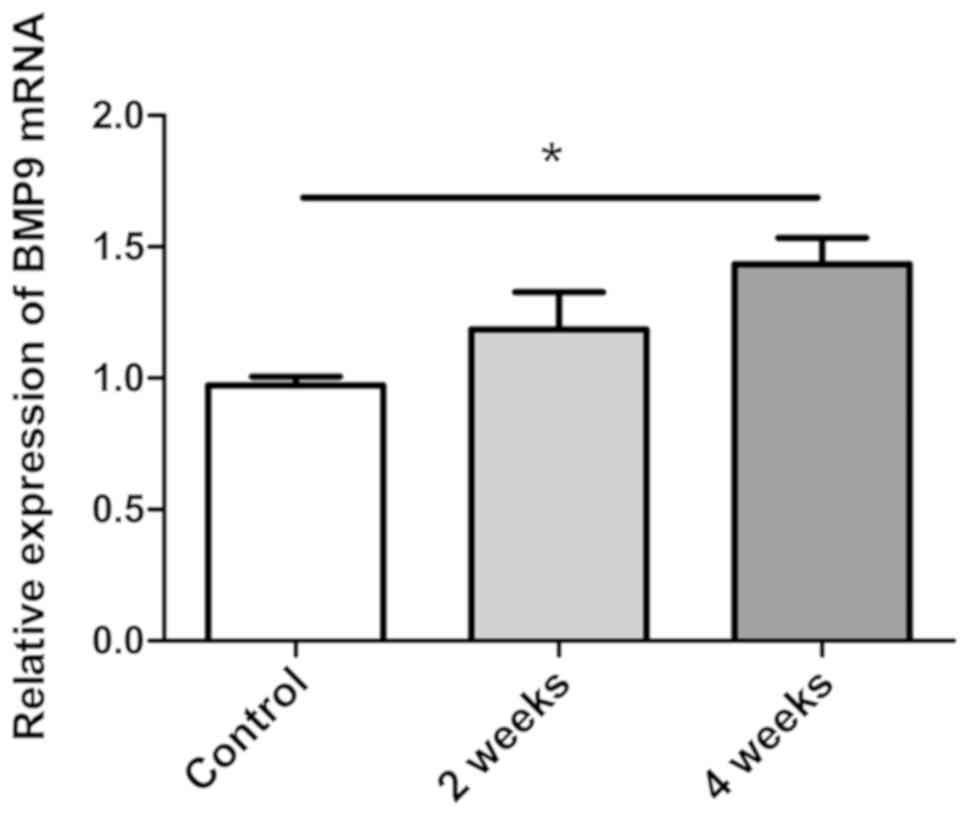
inflammation in mouse livers. Through RT-qPCR analysis, BMP-9 mRNA
levels were measured in the livers of NASH mice (induced by MCD
diet). BMP-9 was revealed to be significantly upregulated in
MCD-induced NASH mice following 4 weeks when compared with the
control mice (P<0.05; Fig. 1).
This upregulation of BMP-9 expression in the NASH model indicated
that BMP-9 may serve a role in the progression of NASH.
Adenovirus mediated-BMP-9
overexpression in the liver aggravates MCD-induced NASH in
mice
BMP-9 tagged with HA at the C-terminus
[Ad-BMP-9-HA(c)] with or without (Adnull) adenovirus under the
transcriptional control of the cytomegalovirus promoter was used
for infection experiments in mice. At 2 weeks, BMP-9 mRNA
expression was increased in BMP-9 overexpressing mice, and the mRNA
and protein expression levels of BMP-9 were confirmed in the liver
tissues of C57BL/6 mice after tail vein injection of
1×109 PFU Ad-BMP-9-HA(c) once a week for 4 weeks
(Figs. 2A, and 3A and B).
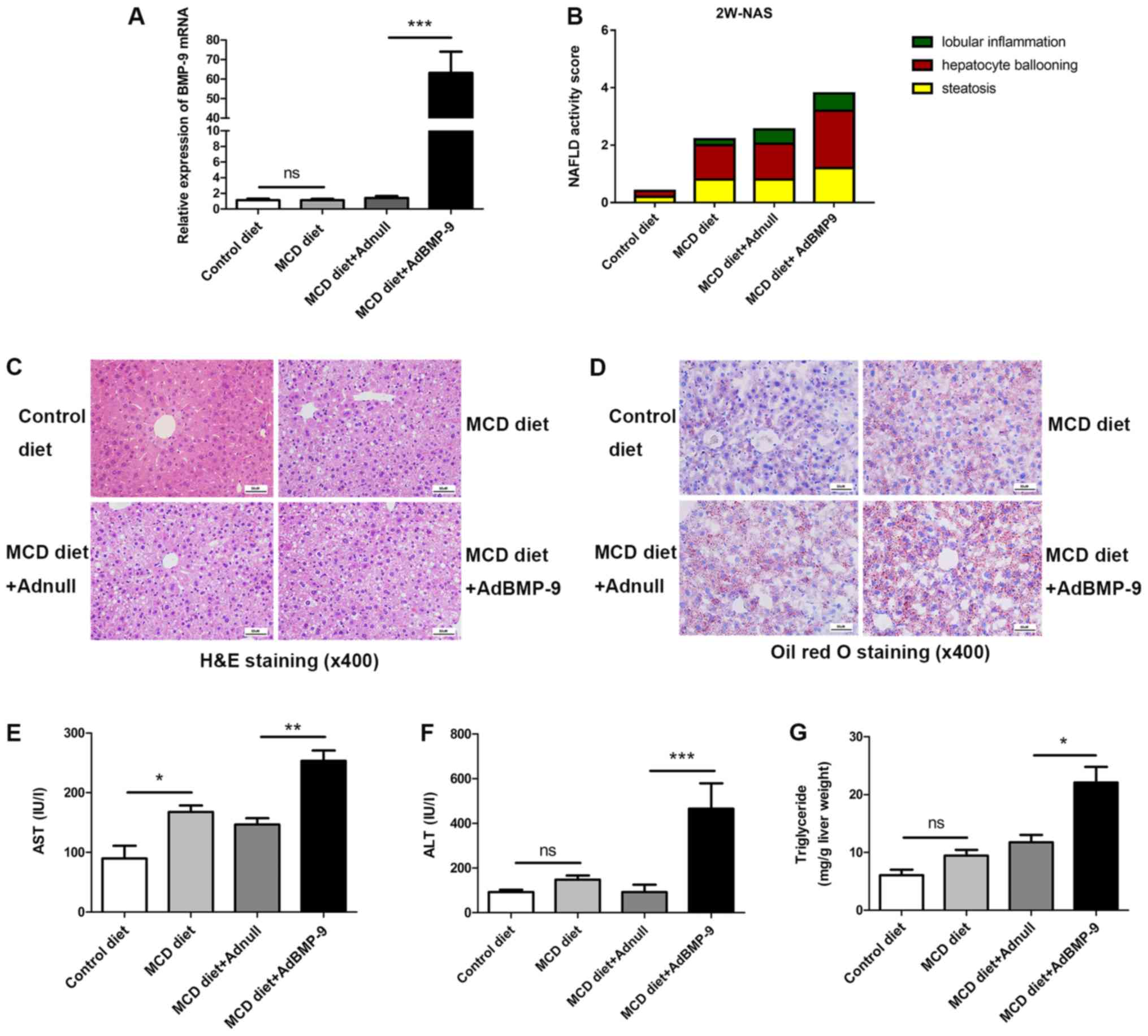 | Figure 2.Effect of BMP-9 overexpression on
liver histology, serum ALT, serum AST and liver triglyceride levels
in mice fed the MCD diet for 2 weeks. BMP-9 overexpressing and wild
type mice, both with a C57BL/6 genetic background, were fed either
the control diet or the MCD diet for 2 weeks. (A) Bar graphs
presenting the results of the quantitative analysis of the mRNA
expression of BMP-9 in the liver tissues of the 4 groups. (B) The
NAS for the 4 different groups. (C) Representative photomicrographs
of H&E-stained and (D) Oil Red-stained liver tissues for the 4
groups (magnification, ×400). (E) Bar graphs presenting the results
of the quantitative analysis of serum AST, (F) serum ALT and (G)
liver triglyceride levels in the 4 groups. *P<0.05, **P<0.01
and ***P<0.001, as indicated. Data are expressed as the mean ±
standard error of the mean (n=6 mice in each group). NAFLD,
non-alcoholic fatty liver disease; NAS, NAFLD activity score;
BMP-9, bone morphogenetic protein-9; MCD, methionine- and
choline-deficient diet; ALT, alanine aminotransferase; AST,
aspartate transaminase; ns, not significant; H&E, hematoxylin
and eosin. |
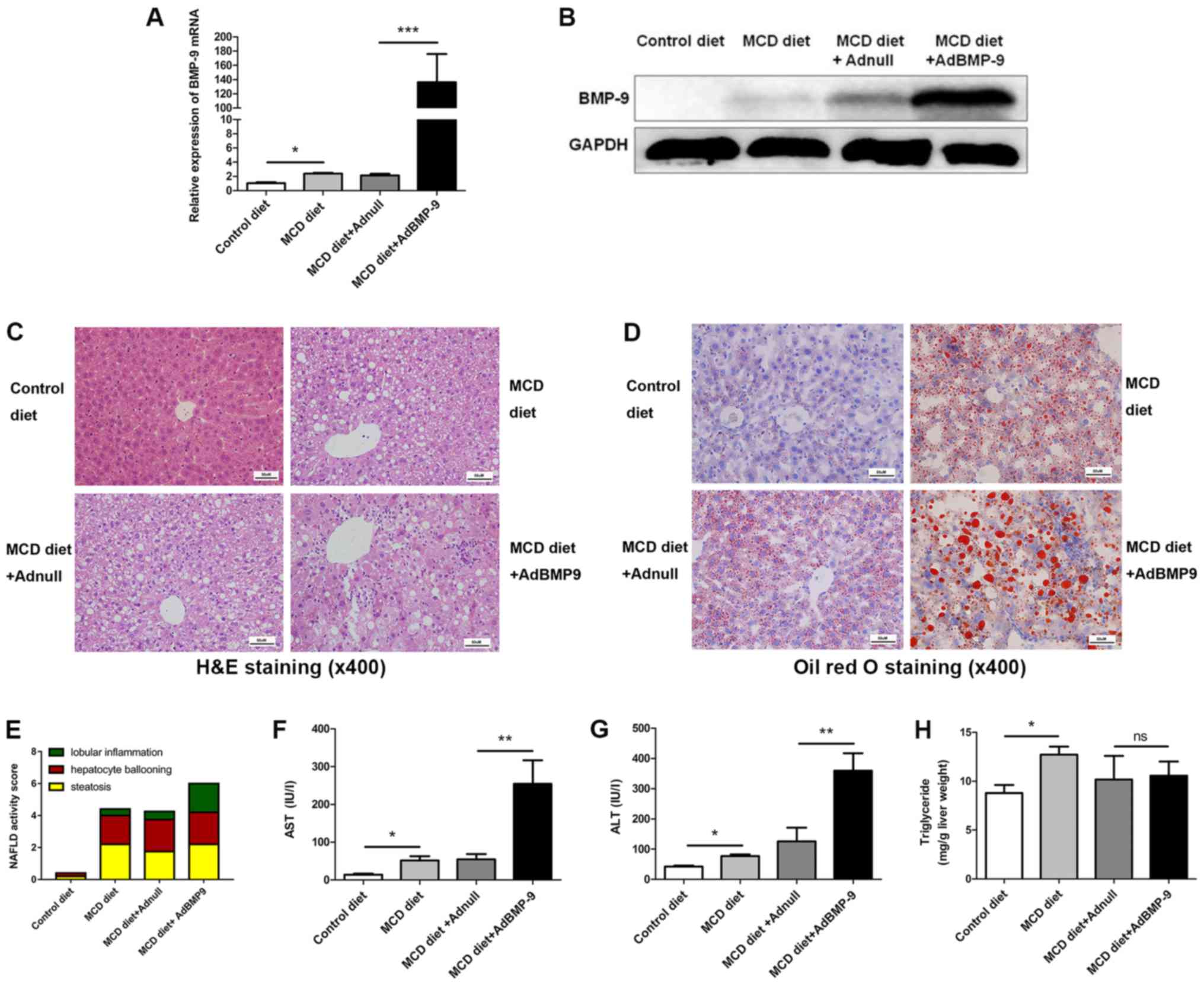 | Figure 3.Effect of BMP-9 overexpression on
liver histology, serum ALT, serum AST and liver triglyceride levels
in mice fed the MCD diet for 4 weeks. BMP-9 overexpressing and wild
type mice, both with a C57BL/6 genetic background, were fed either
the control diet or the MCD diet for 4 weeks. (A) Bar graphs
presenting the results of the quantitative analysis of the mRNA
expression of BMP-9 in the liver tissues of the 4 groups. (B)
Western blotting of the protein expression of BMP-9 in the liver
tissues of the 4 groups. (C) Representative photomicrographs of
H&E-stained and (D) Oil Red-stained liver tissues for the 4
groups (magnification, ×400). (E) The NAS for the 4 different
groups. (F) Bar graphs presenting the results of the quantitative
analysis of serum AST, (G) serum ALT and (H) liver triglyceride
levels in the 4 groups. *P<0.05, **P<0.01 and ***P<0.001,
as indicated. Data are expressed as the mean ± standard error of
the mean (n=6 mice in each group). NAFLD, non-alcoholic fatty liver
disease; NAS, NAFLD activity score; BMP-9, bone morphogenetic
protein-9; MCD, methionine- and choline-deficient diet; ALT,
alanine aminotransferase; AST, aspartate transaminase; ns, not
significant; H&E, hematoxylin and eosin. |
H&E and Oil red-stained slides were examined by
a pathologist. Mice fed the MCD diet developed panacinar
macrovesicular hepatic steatosis. Compared with the control, in the
MCD and MCD+Adnull groups at 2 weeks, the mouse livers with BMP-9
overexpression exhibited enhanced hepatocyte ballooning, focal
inflammatory cell infiltration and bullous steatosis (Fig. 2B-D), which were further intensified
at 4 weeks (Fig. 3C-E).
At 2 weeks, serum AST levels were significantly
increased in mice when comparing the MCD diet to the control
(167.91±21.35 vs. 89.76±37.11 U/l; P<0.05) and were even higher
in BMP-9 overexpressing mice fed the MCD diet (MCD diet+AdBMP-9 vs.
MCD diet+Adnull (253.69±34.27 vs. 146.52±21.89 U/l; P<0.01;
Fig. 2E). ALT was not increased
with the MCD diet (control vs. MCD diet: 82.58±12.98 vs.
138.06±21.29 U/l; P>0.05); however, a significant increase in
the MCD mice with BMP-9 overexpression was observed (MCD
diet+Adnull vs. MCD diet+AdBMP-9: 113.43±16.08 vs. 465.74.4±54.13
U/l; P<0.001; Fig. 2F). Liver
TG levels were reported to be similar to those of AST (control vs.
MCD diet: 6.05±2.12 vs. 9.47±1.94 mg/g liver; P>0.05; MCD
diet+Adnull vs. MCD diet+AdBMP-9: 11.76±2.52 vs. 22.09±6.01 mg/g
liver; P<0.05; Fig. 2G).
At 4 weeks, serum AST levels were significantly
increased in mice on the MCD diet (control vs. MCD diet; 14.18±2.52
vs. 51.62±11.30 U/l; P<0.05) and were even higher in BMP-9
overexpressing mice fed the MCD diet (MCD diet+Adnull vs. MCD
diet+AdBMP-9; 54.55±13.88 vs. 254.3±62.46 U/l; P<0.01; Fig. 3F). The same was observed for ALT
(control vs. MCD diet; 44.27±3.66 vs. 77.3±5.27 U/l; P<0.05; MCD
diet+Adnull vs. MCD diet+AdBMP-9: 125.4±45.56 vs. 359.8±57.55 U/l;
P<0.01; Fig. 3G). An increase
in liver TG was also observed in MCD mice (control vs. MCD diet:
8.78±0.83 vs. 12.71±0.83 mg/g liver; P<0.05), whereas no
significant differences were observed in BMP-9 overexpression (MCD
diet+Adnull vs. MCD diet+AdBMP-9: 10.18±2.42 vs. 10.57±1.45 mg/g
liver; P>0.05; Fig. 3H).
These results implied that BMP-9 exacerbates
hepatocyte damage and enhances MCD-induced NASH in mice.
BMP-9 overexpression induces
inflammatory gene expression in MCD-induced NASH mice
Since inflammation is a critical factor in the
progression of fatty liver to NASH (25). The present study investigated BMP-9
overexpression-induced enhancement of focal inflammatory cell
infiltration in MCD mice. In addition, the expression of a number
of inflammatory genes was examined. At both 2 and 4 weeks, when
compared with mice administered the MCD diet, the mRNA expression
levels of MCP-1 were increased in the livers of MCD mice (Fig. 4A). BMP-9 overexpression in the
liver further enhanced the increase in MCP-1 mRNA expression at 2
and 4 weeks (P<0.05; Figs. 4A
and 5A). For F4/80, IL-1β and
IL-12, BMP-9 overexpression significantly enhanced mRNA expression
at both time points compared with the MCD diet+Adnull group
(Figs. 4D, F and I, and 5D, F and I). For the mRNA expression
levels of CCR2 and IL-17, no significant differences were observed
for BMP-9 overexpression at both time points (Figs. 4C and J, and Fig. 5C and J). However, there was a
tendency for BMP-9 to reduce IL-10 expression at both time points
when compared with MCD diet+Adnull (Figs. 4H and 5H). Despite the fact that TNF-α mRNA
expression was enhanced at 2 weeks by BMP-9 overexpression, no
significant difference was identified at 4 weeks (Figs. 4B and 5B). By contrast, unlike TNF-α mRNA
expression, iNOS mRNA was significantly increased at 4 weeks with
BMP-9 overexpression but not at 2 weeks (Figs. 4E and 5E).
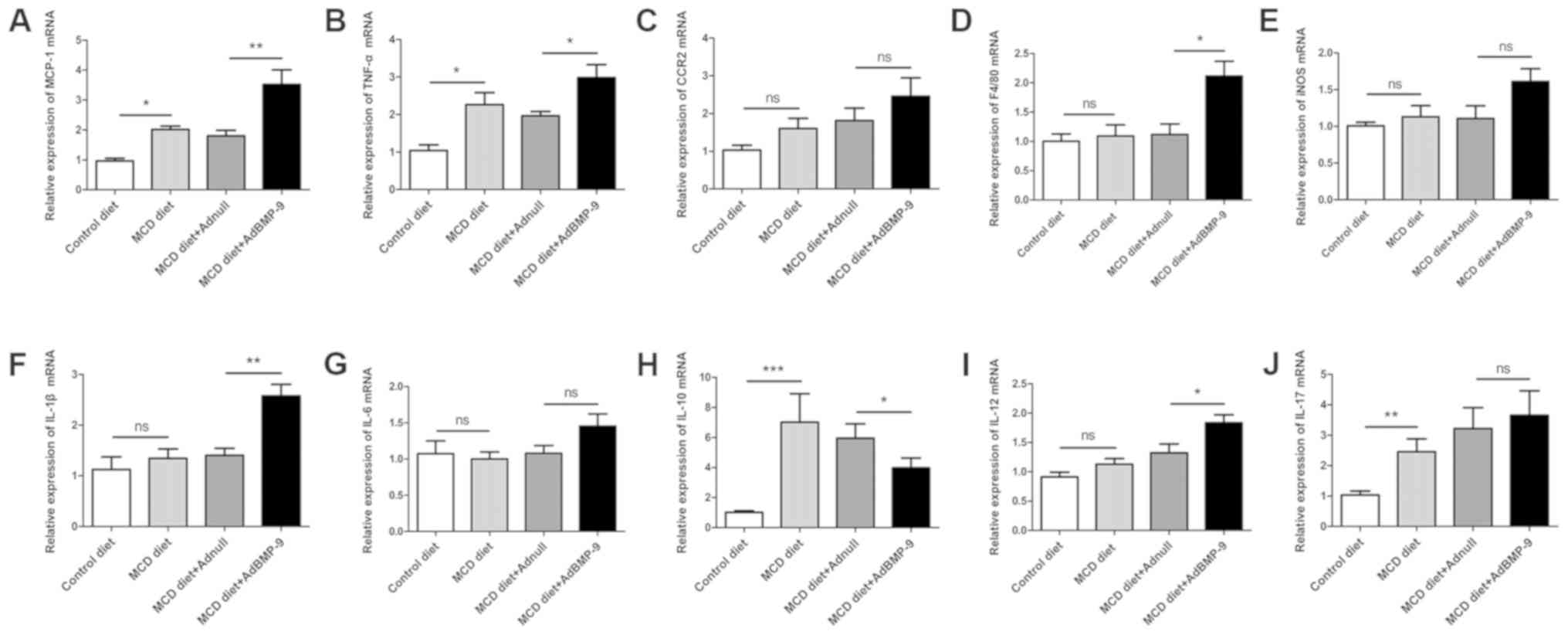 | Figure 4.Effect of BMP-9 overexpression on
hepatic pro-inflammatory gene mRNA levels in mice fed the MCD diet
for 2 weeks. BMP-9 overexpressing and wild type mice were fed
either the control diet or the MCD diet for 2 weeks. (A) Bar graphs
presenting the results of the quantitative analysis of the mRNA
expression of MCP-1, (B) TNF-α, (C) CCR2, (D) F4/80, (E) iNOS, (F)
IL-1β, (G) IL-6, (H) IL-10, (I) IL-12 and (J) IL-17 in the liver
tissues obtained from the 4 groups. *P<0.05, **P<0.01 and
***P<0.001, as indicated. Data are expressed as the mean ±
standard error of the mean (n=6 mice in each group). BMP-9, bone
morphogenetic protein-9; MCD, methionine- and choline- deficient
diet; ns, not significant; MCP-1, monocyte chemoattractant
protein-1; TNF-α, tumor necrotic factor-α; CCR2, C-C chemokine
receptor 2; IL, interleukin; iNOS, inducible nitric oxide
synthase. |
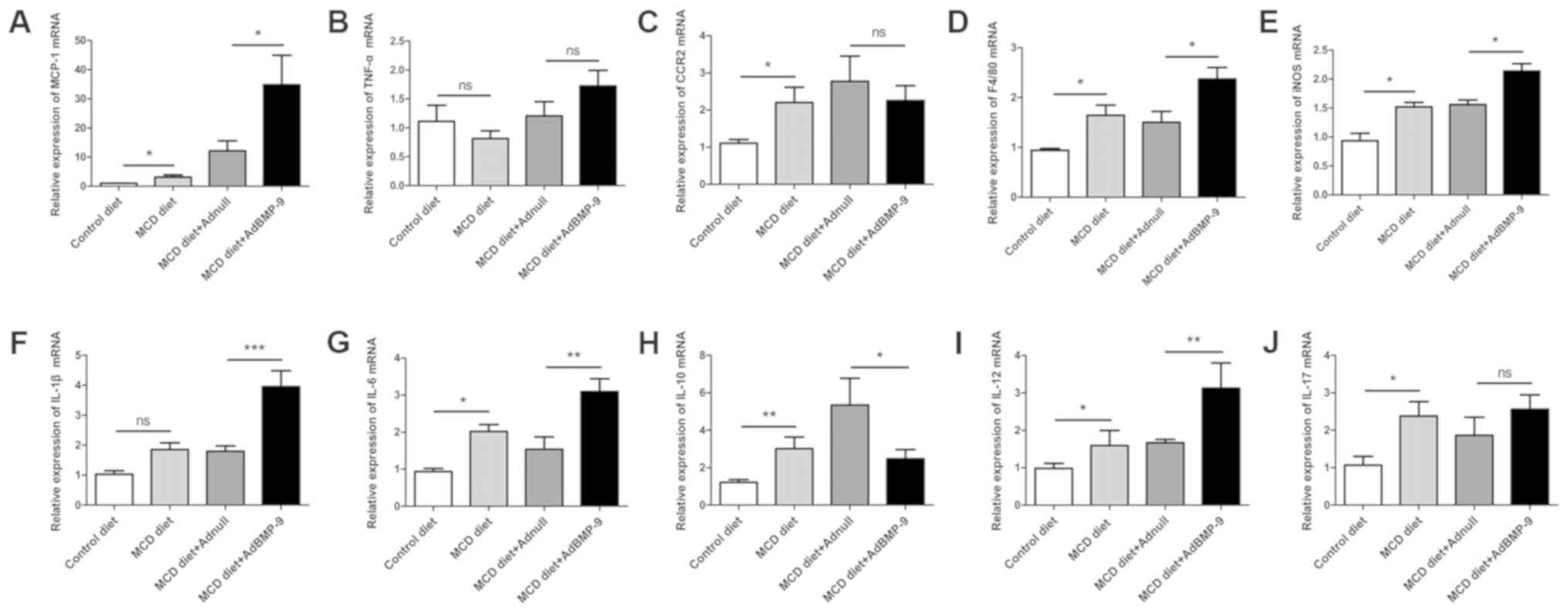 | Figure 5.Effect of BMP-9 overexpression on
hepatic pro-inflammatory gene mRNA levels in mice fed the MCD diet
for 4 weeks. BMP-9 overexpressing and wild-type mice were fed
either the control diet or the MCD diet for 4 weeks. (A) Bar graphs
presenting the results of the quantitative analysis of the mRNA
expression of MCP-1, (B) TNF-α, (C) CCR2, (D) F4/80, (E) iNOS, (F)
IL-1β, (G) IL-6, (H) IL-10, (I) IL-12 and (J) IL-17 in the liver
tissues obtained from the 4 groups. *P<0.05, **P<0.01 and
***P<0.001, as indicated. Data are expressed as the mean ±
standard error of the mean (n=6 mice in each group). BMP-9, bone
morphogenetic protein-9; MCD, methionine- and choline-deficient
diet; ns, not significant; MCP-1, monocyte chemoattractant
protein-1; TNF-α, tumor necrotic factor-α; CCR2, C-C chemokine
receptor 2; IL, interleukin; iNOS, inducible nitric oxide
synthase. |
BMP-9 overexpression mediates
macrophage accumulation and polarization in MCD-induced NASH model
mice
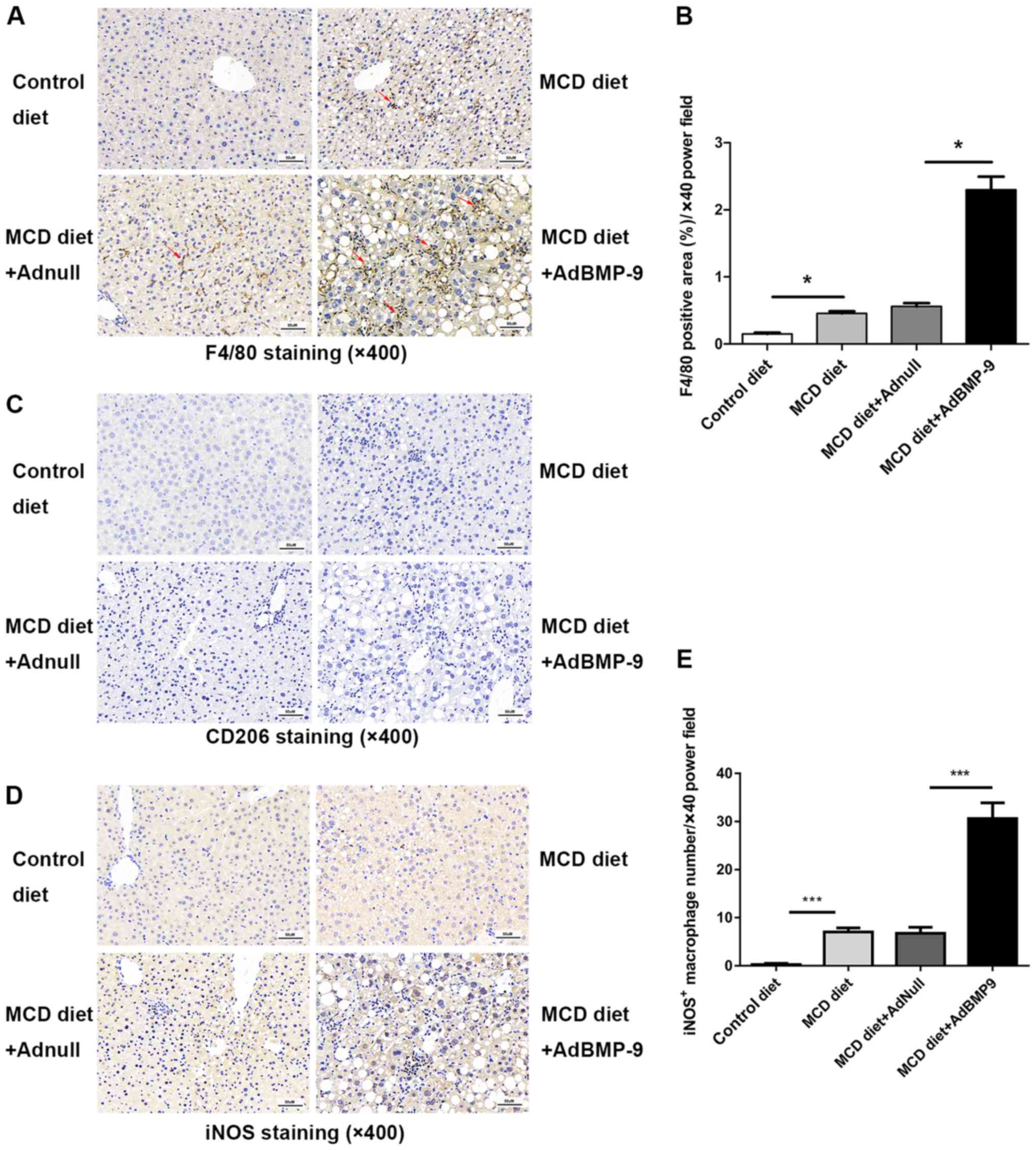
Scattered sinusoidal macrophage staining (using
antibodies against F4/80) was present in the livers of MCD mice
(Fig. 6). Hepatic macrophage
accumulation increased in mice that were administered the MCD diet,
which was further increased with BMP-9 overexpression (Fig. 6A and B). The number of iNOS
positive macrophages, marked as M1 macrophages that promote
inflammation, was significantly higher in the MCD+Ad-BMP-9-HA(c)
group when compared with the other 3 groups (Fig. 6D and E); whereas, no staining or
significant differences were observed for CD206 positive
macrophages, marked as M2 macrophages that secrete
anti-inflammatory factors to regulate immunity, in the 4 groups
(Fig. 6C). This demonstrates that
in the MCD-induced NASH model, macrophages in the liver were more
polarized to inflammation, whereby BMP-9 enhanced this
pro-inflammatory environment in the development of NASH.
BMP-9 overexpression partly mediates
pro-fibrotic gene expression in MCD-induced NASH model mice
We previously reported that BMP-9 is pro-fibrogenic
upon liver damage (19). The
present study also determined whether BMP-9 promotes liver fibrosis
in the NASH model. Since activation of hepatic stellate cells
(HSCs) is a key event during liver fibrosis, the expression of
α-SMA, a typical marker of activated HSCs was determined by IHC. No
significant difference were identified in Sirius red staining
intensities among the 4 groups (Fig.
7A and B). Although α-SMA staining increased in the MCD groups,
there was no marked difference between the MCD diet+AdBMP-9 and MCD
diet+Adnull groups (Fig. 7C and
D).
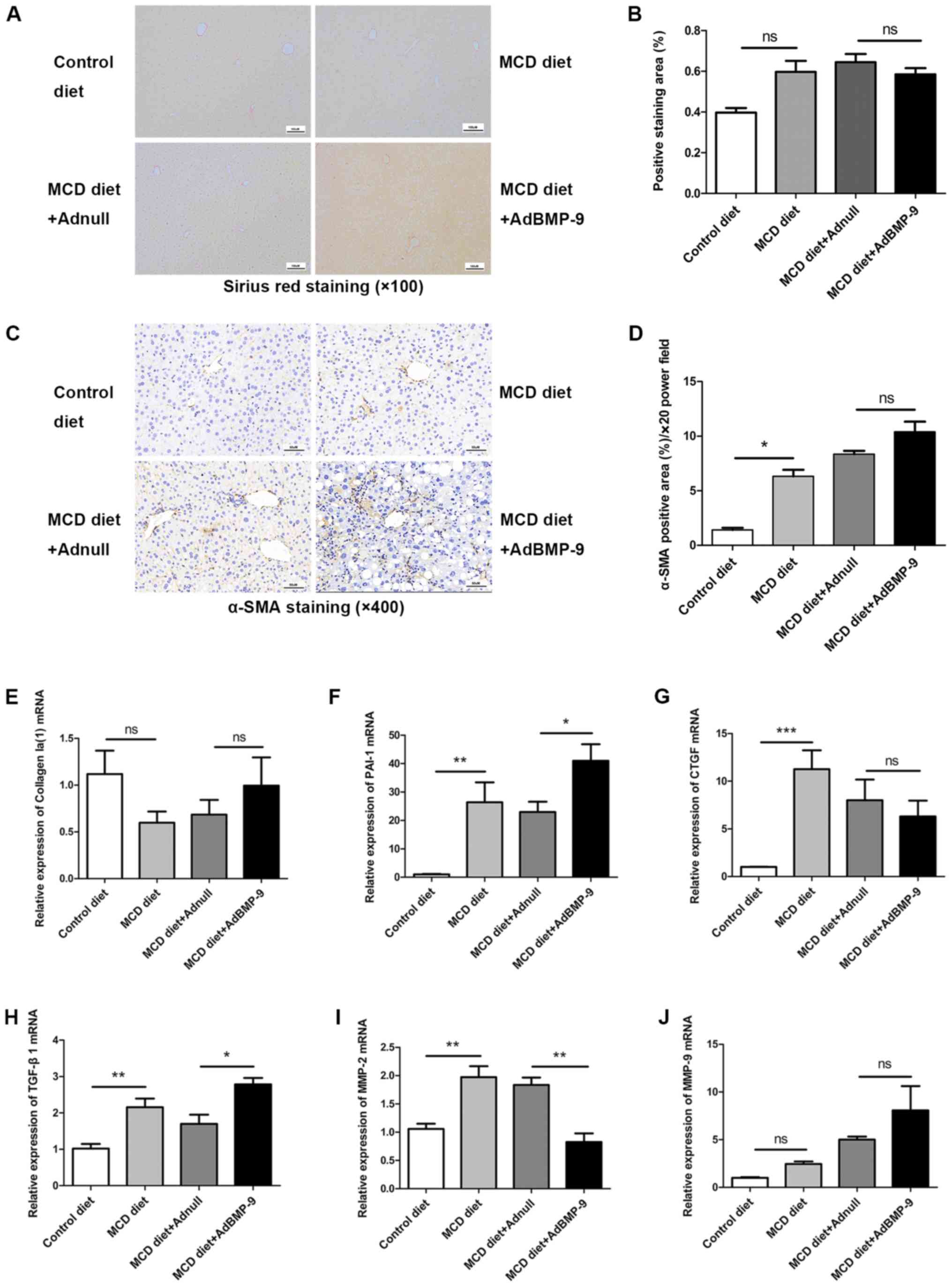 | Figure 7.Effect of BMP-9 overexpression on
liver fibrosis in mice fed the MCD diet. BMP-9 overexpressing and
wild-type mice were fed either the control diet or the MCD diet for
4 weeks. (A) Representative photomicrographs of Sirius red staining
in the livers of each group (magnification, ×100). (B) The extent
of Sirius red staining was assessed via semi-quantification; bar
graphs present the results of the semi-quantitative analysis of
Sirius red staining in the 4 groups. (C) Representative
photomicrographs of α-SMA immunostaining in the livers of each
group (magnification, ×400). (D) The extent of α-SMA immunostaining
was assessed via semi-quantification; bar graphs present the
results of the semi-quantitative analysis of α-SMA staining in the
4 groups. (E) Bar graphs presenting the results of the quantitative
analysis of the mRNA expression of Collagen Ia(1), (F) PAI-1, (G)
CTGF, (H) TGF-β1, (I) MMP-2 and (J) MMP-9 in the liver tissues of
the 4 groups. *P<0.05, **P<0.01 and ***P<0.001, as
indicated. Data are expressed as the mean ± standard error of the
mean (n=6 mice in each group). BMP-9, bone morphogenetic protein-9;
MCD, methionine- and choline-deficient diet; TGF-β, transforming
growth factor-β; CTGF, connective tissue growth factor; PAI-1,
plasminogen activator inhibitor 1; MMP, matrix metalloproteinase;
α-SMA, α-smooth muscle actin; ns, not significant. |
Regarding pro-fibrogenic gene expression, no
significant difference for Collagen I was detected in the 4 groups
(Fig. 7E and J). However, CTGF,
PAI-1 and TGF-β1 were significantly upregulated by the MCD diet.
For PAI-1 and TGF-β1, this was further intensified by BMP-9
overexpression; however, BMP-9 overexpression did not significantly
decrease CTGF expression (Fig.
7F-H). The expression of MMP-2, an extracellular matrix
remodeling enzyme, was enhanced by MCD; however, its expression was
reduced by BMP-9 overexpression (Fig.
7I). For MMP-9, no differences were observed in the 4 groups.
These results indicated that BMP-9 exerts minor pro-fibrotic
effects in experimental settings.
Discussion
In the present study, it was indicated that the tail
vein injection of Ad-BMP-9-HA(c) induced the overexpression of
BMP-9 in the liver, increased the hepatic expression of BMP-9 and
exacerbated MCD diet-induced NASH development in mice. To the best
of our knowledge, a limited number of studies on the effects of
BMP-9 on NASH have been conducted. The results of the present study
demonstrated that BMP-9 overexpression enhances MCP-1 expression
and promotes macrophage recruitment and polarization in the liver,
leading to more acute hepatocyte ballooning, hepatic inflammation
and liver fibrosis. BMP-9 overexpression in MCD-fed mice increased
the serum levels of ALT and AST; however, the TG contents in the
liver at 4 weeks was unchanged. To the best of our knowledge, there
is a limited number of reports on the potential role of BMP-9 in
fatty liver disease. Kim et al (20) reported that periodical injection of
MB109, a recombinant derivative of human BMP-9, into high fat
diet-induced obese mice not only suppressed weight gain in mice,
but also reduced the amount of lipid droplets in the liver, the
serum levels of ALT and total cholesterol. In the present MCD
models, mice lost weight in a time-dependent manner (Fig. S1), but BMP-9 overexpression in
MCD-fed mice increased the serum levels of ALT and AST. These
different results from the two studies may be due to the use of
different animal models. The high fat diet-induced obese model is
normally used to evaluate the insulin resistance of fatty liver;
however, the MCD diet has been widely accepted to evaluate
mechanisms underlying NASH in rodents. Furthermore, MB109 may not
possess all of the natural functions of the full BMP-9 protein.
In our previous study, it was indicated that BMP-9
stimulation of cultured primary hepatocytes inhibited
proliferation, epithelial to mesenchymal transition and preserved
the expression of important metabolic enzymes, including cytochrome
P450 oxidases (19). Application
of BMP-9 after partial hepatectomy also significantly enhanced
liver damage and disturbed the proliferative response (19). In the NASH model utilized in the
present study (MCD model), it was further demonstrated that BMP-9
overexpression enhanced ALT and AST serum levels and hepatocyte
ballooning, indicating that BMP-9 promoted liver damage.
Aside from enhancing liver damage, we also
previously demonstrated that BMP-9 plays a pro-fibrogenic role
in vivo. Chronic carbon tetrachloride challenge in
BMP-9-deficient mice or in mice adenovirally overexpressing the
selective BMP-9 antagonist activin receptor-like kinase-1-Fc
resulted in reduced collagen deposition and subsequent fibrosis
(19). Li et al (26) further confirmed that in patients,
higher BMP-9 levels were associated with advanced stages of liver
fibrosis, and in mouse models recombinant BMP-9 overexpression
accelerated liver fibrosis and adenoviruses-mediated BMP-9
knockdown attenuated liver fibrogenesis. In the MCD NASH model, the
present study indicated that although BMP-9 overexpression induced
TGF-β1 and PAI-1 expression, it failed to significantly enhance
collagen deposition, and stellate cell activation marked by α-SMA
positivity in the liver was not promoted by BMP-9. However, in
addition to upregulating TGF-β1 and PAI-1, BMP-9 also downregulated
the expression of MMP-2, both representing pro-fibrotic features.
Flores-Costa et al (27)
revealed that in mice with NASH, MMP-2 expression was increased,
which is consistent with the results of the present study. The
present study demonstrated that BMP-9 significantly inhibited MMP-2
expression in the liver of MCD-induced NASH model mice. Since MMP-2
is an antifibrotic enzyme, its inhibition can lead to the
progression of liver fibrosis (28). Therefore, the present study
hypothesized that BMP-9 overexpression may promote NASH fibrosis
though MMP-2 downregulation, a subject that requires further
examination. However, significantly enhanced collagen deposition at
4 weeks was simply too short. Therefore, whether BMP-9 could
promote liver fibrosis in NASH requires further investigation.
MCP-1 has been reported to contribute to the
pathogenesis of NASH through multiple mechanisms, including
enhancement of hepatic lipid accumulation, insulin resistance in
mice with a high fat-induced diet, inflammatory responses and liver
fibrosis (29). MCP-1 mediates
leukocyte recruitment to the liver via interactions with the CCR2
receptor on inflammatory cells including macrophages (30). BMP-9 has been reported to play a
role in inflammation by inducing the expression of E-selectin,
which is associated with the initial capture of leukocytes and the
inflammatory cytokines IL-8 and IL-6 (31). Appleby et al (32) reported that BMP-9 alone did not
induce neutrophil recruitment to the endothelium; however, it could
enhance lipopolysaccharide-induced leukocyte recruitment to the
vascular endothelium. Young et al (33) reported that in primary human
endothelial cells BMP-9 treatment regulated chemokine secretion,
adhesion and inflammation pathways. These responses included the
upregulation of the chemokine CXCL12/SDF1 and the downregulation of
its receptor CXCR4 (33). It
remains unclear whether BMP-9 mediates CCR2/MCP-1 interactions. In
the present study, it was revealed that BMP-9 could enhance MCP-1
expression in the MCD-induced NASH model livers, whereas it had no
effect on CCR2 expression. Future studies will aim to clarify
whether BMP-9 is indeed a mediator of CCR2/MCP-1 interactions in
NASH progression.
To the best of our knowledge, there is a limited
number of studies regarding the association between macrophage
polarization and the BMP family. Rocher and Singla (34) reported that BMP-7 treatment could
polarize monocytes into M2 macrophages and increase the expression
of anti-inflammatory cytokines via the activations of the
PI3K-Akt-mTOR signalling pathway. Martínez et al (35) observed that BMP-4 was associated
with and promoted M2 macrophages, which promote tumor progression
in bladder cancer. To the best of our knowledge, there are
currently no reports regarding whether BMP-9 was directly
associated with macrophage polarization. In the NASH mouse model,
the present study demonstrated that BMP-9 overexpression could
induce the expression of MCP-1, a chemokine that is characteristic
of M1 polarization (36). By
contrast, the number of iNOS positive macrophages was significantly
increased by BMP-9 overexpression, which further indicates that
BMP-9 may play a role in the activation of M1-macrophages, fatty
tissue inflammation and NASH. In addition, these results also imply
that BMP-9 may play a role in inflammation and macrophage
polarization.
In conclusion, the results of the present study
revealed that BMP-9 overexpression affected liver steatosis,
macrophage recruitment and polarization in MCD diet-mice. In
addition, BMP-9 influenced the gene expression of some
pro-fibrogenic genes in this model. These results highlight an
important distinction in the mechanism underlying inflammation in
the MCD diet model of NASH compared with other models. The MCD diet
therefore represents a promising model to further investigate the
pro-inflammatory effects of BMP-9 in the future.
Supplementary Material
Supporting Data
Acknowledgements
Not applicable.
Funding
The present study was supported by funding from
Research Development Fund of Capital Medical University (grant no.
PYZ2017085), Scientific Research Project of You'an Hospital, CCMU,
2018 (grant no. YNKTTS20180129), National Natural Science
Foundation (grant no. 81672725), Beijing Natural Science Foundation
Program and Scientific Research Key Program of Beijing Municipal
Commission of Education (grant no. KZ201810025037), WBE Liver
Fibrosis Foundation, (grant no. CFHPC20131023), National Natural
Science Foundation of China (grant no. 81370525), the BMBF program
LiSyM (grant no. PTJ-FKZ: 031L0043) and the Deutsche
Forschungsgemeinschaft (German Research Foundation; grant nos.
393225014 and 394046768-SFB1366).
Availability of data and materials
The datasets used and/or analyzed during the current
study are available from the corresponding author on reasonable
request.
Authors' contributions
QL, SD and HD conceived and designed the study. BL,
QJ and PD performed the experiments and collected the data. QL,
KBH, HW, HD and KX analyzed and interpreted the data. QL, HW and SD
were major contributors in drafting and revising the manuscript.
All authors read and approved the final manuscript.
Ethics approval and consent to
participate
All animal experiments were in full compliance with
the guidelines for animal care and were approved by the Animal Care
Committee of Tongji Medical College, Huazhong University of Science
and Technology.
Patient consent for publication
Not applicable.
Competing interests
The authors declare that they have no competing
interests.
Glossary
Abbreviations
Abbreviations:
|
NASH
|
non-alcoholic steatohepatitis
|
|
BMP-9
|
bone morphogenetic protein-9
|
|
TGF-β
|
transforming growth factor-β
|
|
MCD
|
methionine choline deficiency
|
|
ALT
|
alanine aminotransferase
|
|
AST
|
aspartate transaminase
|
|
CTGF
|
connective tissue growth factor
|
|
PAI-1
|
plasminogen activator inhibitor 1
|
|
MMP-2
|
matrix metalloproteinase-2
|
|
NAFLD
|
non-alcoholic fatty liver disease
|
|
NAFL
|
non-alcoholic fatty liver
|
|
HCC
|
hepatocellular carcinoma
|
|
MCP-1
|
monocyte chemoattractant protein-1
|
|
TNF-α
|
tumor necrotic factor-α
|
|
CCR2
|
C-C chemokine receptor 2
|
|
IL
|
interleukin
|
|
GDF-2
|
growth differentiation factor-2
|
|
Ad-BMP-9-HA(c)
|
adenovirus-mediated over-expression of
BMP-9 tagged with HA at the C-terminus
|
|
SPF
|
specific pathogen free
|
|
PFU
|
plaque forming unit
|
|
TG
|
triglyceride
|
|
IHC
|
immunohistochemistry
|
|
iNOS
|
inducible nitric oxide synthase
|
|
α-SMA
|
α-smooth muscle actin
|
|
MMP-9
|
matrix metalloproteinase-9
|
|
ALK-1
|
activin receptor-like kinase-1
|
References
|
1
|
Pappachan JM, Babu S, Krishnan B and
Ravindran NC: Non-alcoholic fatty liver disease: A clinical update.
J Clin Transl Hepatol. 5:384–393. 2017.PubMed/NCBI
|
|
2
|
Younossi ZM, Koenig AB, Abdelatif D, Fazel
Y, Henry L and Wymer M: Global epidemiology of nonalcoholic fatty
liver disease-Meta-analytic assessment of prevalence, incidence,
and outcomes. Hepatology. 64:73–84. 2016. View Article : Google Scholar : PubMed/NCBI
|
|
3
|
Tacke F: Targeting hepatic macrophages to
treat liver diseases. J Hepatol. 66:1300–1312. 2017. View Article : Google Scholar : PubMed/NCBI
|
|
4
|
Park JK, Shao M, Kim MY, Baik SK, Cho MY,
Utsumi T, Satoh A, Ouyang X, Chung C and Iwakiri Y: An endoplasmic
reticulum protein, Nogo-B, facilitates alcoholic liver disease
through regulation of kupffer cell polarization. Hepatology.
65:1720–1734. 2017. View Article : Google Scholar : PubMed/NCBI
|
|
5
|
Baeck C, Wehr A, Karlmark KR, Heymann F,
Vucur M, Gassler N, Huss S, Klussmann S, Eulberg D, Luedde T, et
al: Pharmacological inhibition of the chemokine CCL2 (MCP-1)
diminishes liver macrophage infiltration and steatohepatitis in
chronic hepatic injury. Gut. 61:416–426. 2012. View Article : Google Scholar : PubMed/NCBI
|
|
6
|
Liaskou E, Zimmermann HW, Li KK, Oo YH,
Suresh S, Stamataki Z, Qureshi O, Lalor PF, Shaw J, Syn WK, et al:
Monocyte subsets in human liver disease show distinct phenotypic
and functional characteristics. Hepatology. 57:385–398. 2013.
View Article : Google Scholar : PubMed/NCBI
|
|
7
|
Song JJ, Celeste AJ, Kong FM, Jirtle RL,
Rosen V and Thies RS: Bone morphogenetic protein-9 binds to liver
cells and stimulates proliferation. Endocrinology. 136:4293–4297.
1995. View Article : Google Scholar : PubMed/NCBI
|
|
8
|
Brown MA, Zhao Q, Baker KA, Naik C, Chen
C, Pukac L, Singh M, Tsareva T, Parice Y, Mahoney A, et al: Crystal
structure of BMP-9 and functional interactions with pro-region and
receptors. J Biol Chem. 280:25111–25118. 2005. View Article : Google Scholar : PubMed/NCBI
|
|
9
|
David L, Mallet C, Keramidas M, Lamandé N,
Gasc JM, Dupuis-Girod S, Plauchu H, Feige JJ and Bailly S: Bone
morphogenetic protein-9 is a circulating vascular quiescence
factor. Circ Res. 102:914–922. 2008. View Article : Google Scholar : PubMed/NCBI
|
|
10
|
Herrera B, Dooley S and Breitkopf-Heinlein
K: Potential roles of bone morphogenetic protein (BMP)-9 in human
liver diseases. Int J Mol Sci. 15:5199–5220. 2014. View Article : Google Scholar : PubMed/NCBI
|
|
11
|
Bessa PC, Cerqueira MT, Rada T, Gomes ME,
Neves NM, Nobre A, Reis RL and Casal M: Expression, purification
and osteogenic bioactivity of recombinant human BMP-4, −9, −10, −11
and −14. Protein Expr Purif. 63:89–94. 2009. View Article : Google Scholar : PubMed/NCBI
|
|
12
|
Chen C, Grzegorzewski KJ, Barash S, Zhao
Q, Schneider H, Wang Q, Singh M, Pukac L, Bell AC, Duan R, et al:
An integrated functional genomics screening program reveals a role
for BMP-9 in glucose homeostasis. Nat Biotechnol. 21:294–301. 2003.
View Article : Google Scholar : PubMed/NCBI
|
|
13
|
Suzuki Y, Ohga N, Morishita Y, Hida K,
Miyazono K and Watabe T: BMP-9 induces proliferation of multiple
types of endothelial cells in vitro and in vivo. J Cell Sci.
123:1684–1692. 2010. View Article : Google Scholar : PubMed/NCBI
|
|
14
|
Truksa J, Peng H, Lee P and Beutler E:
Bone morphogenetic proteins 2, 4, and 9 stimulate murine hepcidin 1
expression independently of Hfe, transferrin receptor 2 (Tfr2), and
IL-6. Proc Natl Acad Sci U S A. 103:10289–10293. 2006. View Article : Google Scholar : PubMed/NCBI
|
|
15
|
Li Q, Gu X, Weng H, Ghafoory S, Liu Y,
Feng T, Dzieran J, Li L, Ilkavets I, Kruithof-de Julio M, et al:
Bone morphogenetic protein-9 induces epithelial to mesenchymal
transition in hepatocellular carcinoma cells. Cancer Sci.
104:398–408. 2013. View Article : Google Scholar : PubMed/NCBI
|
|
16
|
Herrera B, Garcia-Alvaro M, Cruz S, Walsh
P, Fernández M, Roncero C, Fabregat I, Sánchez A and Inman GJ: BMP9
is a proliferative and survival factor for human hepatocellular
carcinoma cells. PLoS One. 8:e695352013. View Article : Google Scholar : PubMed/NCBI
|
|
17
|
Kuo MM, Kim S, Tseng CY, Jeon YH, Choe S
and Lee DK: BMP-9 as a potent brown adipogenic inducer with
anti-obesity capacity. Biomaterials. 35:3172–3179. 2014. View Article : Google Scholar : PubMed/NCBI
|
|
18
|
Young K, Tweedie E, Conley B, Ames J,
FitzSimons M, Brooks P, Liaw L and Vary CP: BMP9 crosstalk with the
hippo pathway regulates endothelial cell matricellular and
chemokine responses. PloS One. 10:e01228922015. View Article : Google Scholar : PubMed/NCBI
|
|
19
|
Breitkopf-Heinlein K, Meyer C, Konig C,
Gaitantzi H, Addante A, Thomas M, Wiercinska E, Cai C, Li Q, Wan F,
et al: BMP-9 interferes with liver regeneration and promotes liver
fibrosis. Gut. 66:939–954. 2017. View Article : Google Scholar : PubMed/NCBI
|
|
20
|
Kim S, Choe S and Lee DK: BMP-9 enhances
fibroblast growth factor 21 expression and suppresses obesity.
Biochim Biophys Acta. 1862:1237–1246. 2016. View Article : Google Scholar : PubMed/NCBI
|
|
21
|
Chen LL, Yang WH, Zheng J, Hu X, Kong W
and Zhang HH: Effect of catch-up growth after food restriction on
the entero-insular axis in rats. Nutr Metab(Lond). 7:452010.
View Article : Google Scholar : PubMed/NCBI
|
|
22
|
Bedossa P, Poitou C, Veyrie N, Bouillot
JL, Basdevant A, Paradis V, Tordjman J and Clement K:
Histopathological algorithm and scoring system for evaluation of
liver lesions in morbidly obese patients. Hepatology. 56:1751–1759.
2012. View Article : Google Scholar : PubMed/NCBI
|
|
23
|
Kleiner DE, Brunt EM, Van Natta M, Behling
C, Contos MJ, Cummings OW, Ferrell LD, Liu YC, Torbenson MS,
Unalp-Arida A, et al: Design and validation of a histological
scoring system for nonalcoholic fatty liver disease. Hepatology.
41:1313–1321. 2005. View Article : Google Scholar : PubMed/NCBI
|
|
24
|
Livak KJ and Schmittgen TD: Analysis of
relative gene expression data using real-time quantitative PCR and
the 2(-Delta Delta C(T)) method. Methods. 25:402–408. 2001.
View Article : Google Scholar : PubMed/NCBI
|
|
25
|
Pierantonelli I and Svegliati-Baroni G:
Nonalcoholic fatty liver disease: Basic pathogenetic mechanisms in
the progression from NAFLD to NASH. Transplantation. 103:e1–e13.
2019. View Article : Google Scholar : PubMed/NCBI
|
|
26
|
Li P, Li Y, Zhu L, Yang Z, He J, Wang L,
Shang Q, Pan H, Wang H, Ma X, et al: Targeting secreted cytokine
BMP9 gates the attenuation of hepatic fibrosis. Biochim Biophys
Acta Mol Basis Dis. 1864:709–720. 2018. View Article : Google Scholar : PubMed/NCBI
|
|
27
|
Flores-Costa R, Alcaraz-Quiles J, Titos E,
López-Vicario C, Casulleras M, Duran-Güell M, Rius B, Diaz A, Hall
K, Shea C, et al: The soluble guanylate cyclase stimulator IW-1973
prevents inflammation and fibrosis in experimental non-alcoholic
steatohepatitis. Br J Pharmacol. 175:953–967. 2018. View Article : Google Scholar : PubMed/NCBI
|
|
28
|
Roderfeld M: Matrix metalloproteinase
functions in hepatic injury and fibrosis. Matrix Biol.
68-69:452–462. 2018. View Article : Google Scholar : PubMed/NCBI
|
|
29
|
Berres ML, Nellen A and Wasmuth HE:
Chemokines as immune mediators of liver diseases related to the
metabolic syndrome. Dig Dis. 28:192–196. 2010. View Article : Google Scholar : PubMed/NCBI
|
|
30
|
Deshmane SL, Kremlev S, Amini S and Sawaya
BE: Monocyte chemoattractant protein-1 (MCP-1): An overview. J
Interferon Cytokine Res. 29:313–326. 2009. View Article : Google Scholar : PubMed/NCBI
|
|
31
|
Upton PD, Davies RJ, Trembath RC and
Morrell NW: Bone morphogenetic protein (BMP) and activin type II
receptors balance BMP9 signals mediated by activin receptor-like
kinase-1 in human pulmonary artery endothelial cells. J Biol Chem.
284:15794–15804. 2009. View Article : Google Scholar : PubMed/NCBI
|
|
32
|
Appleby SL, Mitrofan CG, Crosby A,
Hoenderdos K, Lodge K, Upton PD, Yates CM, Nash GB, Chilvers ER and
Morrell NW: Bone morphogenetic protein 9 enhances
lipopolysaccharide-induced leukocyte recruitment to the vascular
endothelium. J Immunol. 197:3302–3314. 2016. View Article : Google Scholar : PubMed/NCBI
|
|
33
|
Young K, Conley B, Romero D, Tweedie E,
O'Neill C, Pinz I, Brogan L, Lindner V, Liaw L and Vary CP: BMP9
regulates endoglin-dependent chemokine responses in endothelial
cells. Blood. 120:4263–4273. 2012. View Article : Google Scholar : PubMed/NCBI
|
|
34
|
Rocher C and Singla DK: SMAD-PI3K-Akt-mTOR
pathway mediates BMP-7 polarization of monocytes into M2
macrophages. PloS One. 8:e840092013. View Article : Google Scholar : PubMed/NCBI
|
|
35
|
Martínez VG, Rubio C, Martinez-Fernandez
M, Segovia C, López-Calderón F, Garín MI, Teijeira A,
Munera-Maravilla E, Varas A, Sacedón R, et al: BMP4 induces M2
macrophage polarization and favors tumor progression in Bladder
cancer. Clin Cancer Res. 23:7388–7399. 2017. View Article : Google Scholar : PubMed/NCBI
|
|
36
|
Moore LB, Sawyer AJ, Charokopos A, Skokos
EA and Kyriakides TR: Loss of monocyte chemoattractant protein-1
alters macrophage polarization and reduces NFkappaB activation in
the foreign body response. Acta Biomater. 11:37–47. 2015.
View Article : Google Scholar : PubMed/NCBI
|